Professional Documents
Culture Documents
Weebly Example 4
Uploaded by
api-280761968Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Weebly Example 4
Uploaded by
api-280761968Copyright:
Available Formats
Running head: POLICY AND PROCEDURE ANALYSIS
Analysis of a Hospital-based Policy and Procedure:
The Nurse Educators Role
Ellice Hayek
Youngstown State University
POLICY AND PROCEDURE ANALYSIS
Within a hospital setting in Northeast Ohio, to promote positive patient outcomes, yearly analysis
of intensive care unit (ICU) policies and procedures must be conducted. The clinical nurse
educators are in charge of coordinating this process. The policy and procedure for the noninvasive cardiac output monitor (NICOM) had not been reviewed since June 2014. Using
evidence-based sources, a thorough analysis and subsequent updates were executed.
POLICY AND PROCEDURE ANALYSIS
Analysis of a Hospital-based Policy and Procedure: The Nurse Educators Role
Within a hospital setting in Northeast Ohio, yearly analysis of intensive care unit (ICU)
policies and procedures must be conducted. This process is conducted to promote safe, effective
nursing practice to support positive patient outcomes. It is the responsibility of the clinical nurse
educators within the hospital setting to ensure that all policies and procedures are reviewed. The
clinical nurse educators delegate and facilitate the review process.
The review process consists of two parts. First, a team of two nurses are selected to
perform the analysis. The analysis must be conducted by comparing the policy and procedure to
current evidence-based practice literature and updating as needed. Second, the policy and
procedure is brought in front of a professional practice council who reviews and then determines
whether or not the changes may remain.
The policy and procedure for non-invasive cardiac output monitoring (NICOM) had not
been reviewed since June of 2014 (See Appendix A). Using the latest critical care nursing book
by the American Association of Critical Care Nursing, among many other internet sources
including the device website and recently published literature (all of evidence-based value) the
policy and procedure was updated. Numerous changes were made which further emphasized the
importance of updating policies and procedures within the health-care setting.
The NICOM policy and procedure was reviewed by the professional practice council on
April 14th, 2015 (See Appendix B). The policy and procedure passed, with the only
recommended changes being minor grammatical errors. It is empowering to know that my
analysis of this policy and procedure played an influential role in promoting safe and effective
nursing care within this hospital.
POLICY AND PROCEDURE ANALYSIS
Appendix A
Original NICOM Policy and Procedure
NICOM (NON-INVASIVE CARDIAC OUTPUT MONITOR)
(formerly Procedure)
Effective Date: 11/10
Revised Date: 05/11, 06/14
Review Date:
________________________________________________________________________
Page 1 of 6
PURPOSE:
To provide non-invasive assessment of the patients hemodynamic status for purposes of fluid
optimization, differential diagnosis, and drug titration.
POLICY:
The primary goal of patient fluid and/or other forms of resuscitation is to restore adequate tissue
perfusion. Cardiac output (CO), which drives tissue perfusion, is equal to the product of stroke
volume (SV) and heart rate (HR). SV is dependent upon complex interactions between preload,
afterload, and cardiac contractility. Various measurements (hemodynamic parameters) and
technologies (advanced hemodynamic monitoring) have been developed to assess preload and
afterload. Advanced hemodynamic monitoring is an important part of treatment in clinical
situations where aggressive, yet guided hemodynamic interventions are required in order to
stabilize the patient and optimize outcomes. Clinical situations in which hemodynamic
monitoring may be indicated, include shock (hypovolemic, cardiogenic, septic, anaphylactic, and
neurogenic), trauma, acute myocardial infarction with shock, and increased metabolic demands
(burns, infection and peri-operative states). The NICOM is a non-invasive advanced
hemodynamic monitoring technology. A discussion of the merits of alternative means of
hemodynamic monitoring is beyond the scope of this policy
Page 2 of 6
POLICY AND PROCEDURE ANALYSIS
PROCEDURE:
Equipment:
NICOM
NICOM Electrodes/Sensors
NICOM Non-Invasive Blood Pressure (NIBP) cuff (attached to NICOM)
Passive leg raise (PLR) wedge, if available
The NICOM is not defibrillator protected: disconnect the lead wires from the electrodes
prior to defibrillation! Keep NICOM plugged in to retain full battery power.
STEPS:
KEY POINTS:
1. Obtain ordering provider order for NICOM
monitoring.
2. Explain procedure to patient/family.
3. Follow standard precautions during procedure
by washing/degerming hands before and after
patient contact.
4. Assemble equipment/obtain NICOM
NICOM electrodes are a charge item.
electrodes/sensors.
5. Apply NICOM BP cuff.
To apply electrodes:
1. If necessary, clip hair. If skin is oily, wipe
with alcohol prep pad.
2. Gently rub skin with sand paper included
in electrode packet.
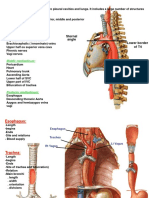
3. Place upper set of electrodes length-wise
on patients chest, shoulders, or back (midclavicular line). Place lower set of
electrodes length-wise on abdomen (midclavicular line), flanks, or back. Avoid
placement into skin folds. Ensure electrode
cable connector points downward toward
patients feet. (Refer to pictures on
electrodes and packaging for guidance).
4. Attach leads to NICOM cables: red to red,
transparent to black).
5. Secure lead cables to patients skin
approximately 2 inches below electrode
with adhesive tape.
Page 3 of 6
NICOM electrodes are positioned in a square around the
heart. Exact location is flexible. Symmetrical right-left
placement of the electrodes is preferred when possible
but is not obligatory.
KEYPOINTS:
POLICY AND PROCEDURE ANALYSIS
STEPS:
6. Write date/time of electrode
application on adhesive tape.
To begin monitoring:
1. Turn on monitor by pressing and
holding the green ON switch for
approximately 30 seconds. Wait
for beep.
2. For existing patient, select
existing patient and highlight
patients medical record number
{MRN}. If details are correct,
highlight RUN and press OK. If
details are incorrect, highlight
Update
3. details and press OK. Correct
details as needed. Skip to step #
5.
4. For new patient, select new
patient. Enter patient
information. Navigate
numbers/letters using arrow keys.
Press OK to enter selection. After
each data set is entered, click
NEXT to move to the next data
field.
MRN
Age
Weight
Height
Gender
5. After gender is entered, press
FINISH.
6. Review screen appears. Review
patient data for accuracy.
7. When completed, click RUN to
move to RUN screen. Click OK to
initiate calibration/monitoring.
6
NICOM electrodes are for single use only and
may last up to 48 hours, depending on signal quality.
Patient information and readings are stored in NICOM
until deleted.
System performs an automatic calibration for
approximately two minutes then starts monitoring the
patient. Ensure patient remains still during calibration.
Movement prolongs the calibration time. Screen
displays a message that indicates calibration is in
process. NICOM will now begin obtaining continuous
hemodynamic parameters. Parameters available include
CO, Cardiac Index (CI), SV, Stroke Volume Index
(SVI), Mean Arterial Pressure (MAP), Total Peripheral
Resistance (TPR), Total Peripheral Resistance Index
(TPRI), and Stroke Volume Variation (SVV). SVV
should not be utilized for diagnostic purposes unless
patient is in sinus rhythm and receiving positive
pressure mechanical ventilation. Ordering providers
may use these parameters to select interventions or may
POLICY AND PROCEDURE ANALYSIS
7
KEYPOINTS:
choose to utilize maneuvers such as the PLR or Bolus
Protocols to immediately determine fluid
responsiveness.
Page 4 of 6
STEPS:
To obtain NIBP reading:
1. Press MENU key.
2. Highlight NIBP.
3. Highlight MANUAL NIBP.
4. If you want NIBP readings at timed
intervals, press MENU key.
5. Highlight NIBP Timed Interval.
Highlight the desired timed
interval and press OK to activate.
To assess fluid responsiveness
using either PLR or bolus protocol:
To perform PLR Test:
(Not recommended for traumatic brain
injury, below knee amputees, or patients with
portal hypertension. If patient is wearing
intermittent pneumatic compression devices
(IPCDs) on the lower extremities, the device is
turned off for a couple of minutes to allow normal
blood flow to
return prior to initiating test. Push TED hose
down. Take any pillows from under legs and verify
foot of bed is flat. Put IV maintenance
fluids on hold.
1. With patient lying supine, raise
head of bed (HOB) to 45 degrees.
2. Make sure NIBP cuff is attached to
patients arm.
3. Press the MENU key. Highlight
PROTOCOL. Press OK.
4. Highlight PLR. Press OK.
5. Keep patient still while monitor
The PLR test is based upon the assumption that the
average patient has approximately 250 ml of vascular
volume in the lower extremities. Raising the legs results
in a reversible fluid bolus. Proper positioning and
removal of compression devices prior to the test is
essential to ensure an adequate vascular volume in the
lower extremities to assess for fluid responsiveness.
Follow the monitor prompts in order to obtain the series
of readings needed to determine baseline and PLR
readings.
In order to truly challenge patient, position change must
occur as quickly as possible. Lift legs to 45 degree angle
immediately; do NOT lift gradually.
KEYPOINTS:
POLICY AND PROCEDURE ANALYSIS
obtains NIBP and baseline data.
6. Monitor counts down 3 minutes
and sounds an audible alarm to
indicate when the 3 minutes is up.
7. When monitor prompts, lower the
patients HOB to flat. Elevate the
patients legs to a 45 degree
angle. May hold patients legs
Page 5 of 6
STEPS:
up or use PLR wedge pillow, if
available.
8. Press OK on monitor to continue
the test.
9. The monitor counts down 3
minutes.
10.
After 3 minutes is up, lower
the patients legs back down and
raise the HOB to a comfortable
position. Turn IPCDs back on, if
applicable. Resume IV fluids.
To perform BOLUS Test:
1. Press MENU key. Highlight
PROTOCOL. Press OK.
2. Highlight Bolus Test. Press OK.
3. Per provider order, give 200 to
300 ml of fluid over 5 to 10
minutes.
4. Once bolus is complete, must
manually stop Bolus Test. Select
MENU, PROTOCOL, END
PROTOCOL.
To turn off monitor:
1. Press MENU key
2. Highlight EXIT
3. MAIN MENU highlights
4. Select SHUT DOWN
5. Highlight and click YES
Test is positive if SVI rises greater than 10 %, indicating
patient is fluid responsive. Test is negative if SVI rises
less than 10 %, indicating patient is not fluid responsive.
Patient position does not matter during bolus test as long
as position does not change during test. Will need at
least 2 minutes of data. If bolus finishes in less than 3 to
4 minutes, allow this time to elapse before stopping test.
Test is positive if stroke volume index (SVI) rises
greater than 10 %, indicating patient is fluid responsive.
Test is negative if SVI rises less than 10 %, indicating
patient is not fluid responsive. SVI typically increases
by 15 % in response to 500 mL IV fluid administration.
POLICY AND PROCEDURE ANALYSIS
6. Machine powers off
Clean or disinfect the unit:
1. Routine cleaning includes removal of any soil or dirt from the external surfaces. Use a soft
cloth dampened lightly with water.
2. When disinfecting the unit or when passing a patient cable between patients, clean all nondisposable parts, such as patient cable and clips with alcohol on a soft towel or wipe.
3. Do not expose the instrument, patient cable, clips or electrodes to sprays, or any other type of
solvents.
Patient/family education
1. Purpose of monitoring
2. Procedure, including position changes and need to lie still as directed
Page 6 of 6
Normal Hemodynamic Parameters Adult
Parameter
Cardiac Output (CO)
Cardiac Index (CI)
Stroke Volume (SV)
Stroke Volume Index (SVI)
Mean Arterial Pressure (MAP)
Total Peripheral Resistance (TPR)
Total Peripheral Resistance Index (TPRI)
Stroke Volume Variation (SVV)*
*During positive pressure mechanical ventilation
Equation
HR x SV/1000
CO/BSA
CO/HR x 1000
SV/BSA
Directly from oscillometric profile
80 x (MAP)/CO
80 x MAP/CI
(SVmax-SVmin)/{(SVmaxSVmin)/2} x 100
Normal Range
4.0 8.0 l/min
2.5 4.0 l/min
60 100 ml/beat
33 47 ml/m2/beat
70 105 mmHg
800 1200 dynes sec/cm5
1970 2390 dynes sec/cm5/m2
<10% unlikely to be preload responsive
>15% likely to be preload responsive
Notify ordering provider of the following:
1. Hemodynamic parameters obtained
2. Response to interventions
3. Sudden or significant changes in clinical condition and related hemodynamic parameters
Documentation:
1. Patient tolerance/response to monitoring/PLR/interventions
2. Hemodynamic parameters as ordered by the ordering provider in the Complex Vital Signs
Doc Flowsheet and/or progress note
3. Notification of ordering provider
4. Patient/family education
REFERENCES:
1. American Association of Critical Care Nurses. (2006). Core Curriculum for Critical Care
Nursing 6th Edition. Saunders, Elsevier, pp. 195-199.
2. Cheetah Medical. (2014, June 4). Cheetah NICOM Normal Hemodynamic Parameters.
Retrieved from Cheetah Medical: http://cheetah-medical.com/sites/default/files/Normal-
POLICY AND PROCEDURE ANALYSIS
10
Ranges_poster-Feb21_2012-70x100.pdf.
3. Cheetah Medical. (2014, June 4). Cheetah NICOM Online Training. Retrieved from Cheetah
Medical - Non-invasive Hemodynamic Monitoring:
http://www.cheetahmedical.com/resources/training.
4. Cheetah Medical. (2014, June 4). Passive Leg Raise (PLR) Protocol with the Cheetah
NICOM System. Retrieved from Cheetah Medical : http://files.cheetahmedical.netdnacdn.com/cdn/ farfuture/JADXGHEm_jezvAwdq2- xuNWCvnJCk6jZ0dE3flB6kbI/mtime:
1398868310/sites/default/files/PLR_Challenge_F.pdf.
APPROVAL:
SICU Operations Committee
Infection Prevention and Control Services, Manager
Professional Practice Council
Appendix B
Updated NICOM Policy and Procedure
NICOM (NON-INVASIVE CARDIAC OUTPUT MONITOR)
(formerly Procedure)
Effective Date: 11/10
Revised Date: 05/11, 06/14
Review Date:
________________________________________________________________________
Page 1 of 6
PURPOSE:
To provide non-invasive assessment of the patients hemodynamic status for purposes of fluid
optimization, differential diagnosis, and drug titration.
POLICY:
The primary goal of hemodynamic monitoring is to assess the ability of the cardiovascular
system to respond to the tissue oxygen demands within the body. Cardiac output (CO), a key
indicator of tissue perfusion, represents the volume of blood pumped by the ventricles every
minute. CO is the product of stroke volume (SV) and heart rate (HR). SV, the amount of blood
pumped by each ventricle with each cardiac cycle, is dependent upon complex interactions
between preload, afterload, and cardiac contractility. Various measurements (hemodynamic
parameters) and technologies (advanced hemodynamic monitoring) have been developed to
assess preload and afterload. With this information appropriate interventions to obtain
hemodynamic stability may be executed. Clinical situations in which hemodynamic monitoring
may be indicated include shock (cardiogenic, hypovolemic, and distributive), trauma, and times
of increased metabolic demands (peri-operative) The NICOM is a non-invasive advanced
hemodynamic monitor. A discussion of the merits of alternative means of hemodynamic
monitoring is beyond the scope of this policy.
POLICY AND PROCEDURE ANALYSIS
11
Page 2 of 6
PROCEDURE:
Equipment:
NICOM
NICOM Electrodes (Sensors)
NICOM Non-Invasive Blood Pressure (NIBP) cuff (attached to NICOM)
Passive leg raise (PLR) wedge, if available
The NICOM is not defibrillator protected: disconnect the lead wires from the electrodes
prior to defibrillation! Keep NICOM plugged in to retain full battery power.
STEPS:
KEY POINTS:
6. Obtain order from ordering provider.
7. Explain procedure to patient/family.
8. Follow standard precautions during procedure
by performing hand hygiene before and after
patient contact.
9. Gather and assemble NICOM equipment.
10. Apply NICOM BP cuff.
NICOM electrodes are a charge item.
To apply electrodes:
7. If necessary, clip hair.
8. Gently rub skin with sand paper included
in electrode packet.
9. Place upper set of electrodes on patients
upper chest, shoulders, upper back, or
axillary region. Place lower set of
electrodes on patients lower ribs, flanks,
or back. Place in a lengthwise direction.
Ensure electrode cable connector points
downward toward patients feet. (Refer to
NICOM electrodes are positioned in a square around the
heart. Exact location is flexible. Symmetrical right-left
placement of the electrodes is ideal, but is not
mandatory.
POLICY AND PROCEDURE ANALYSIS
12
pictures on electrodes and packaging for
guidance).
10. Attach leads to NICOM cables: red to red,
transparent to black).
Page 3 of 6
STEPS:
To begin monitoring:
8. Turn on monitor by pressing and
holding the green ON switch. Wait
for beep.
9. For existing patient, select
existing patient and highlight
patients medical record number
[MRN]. If details are correct, press
RUN. If details are incorrect, press
Update
Details and correct details as
needed. When finished updating
details, press FINISH, then press
RUN. From this point, skip to step
#7.
10.
For new patient, select new
patient. Enter patient information using
touch screen technology. After each data
set is entered, select NEXT to move to the
next data field.
MRN
Age
Weight
Height
Gender
11.
After gender is entered,
KEYPOINTS:
NICOM electrodes are for single use only and
may last up to 48 hours, depending on signal quality.
Patient information will delete from the monitor
automatically after an extended period of time.
System performs an automatic calibration for
approximately 90 seconds then starts monitoring the
POLICY AND PROCEDURE ANALYSIS
press FINISH.
12.
Review screen appears.
Review patient data for accuracy.
13.
When completed, select
RUN.
14.
Confirm electrode
placement/connection and press
OK to initiate
calibration/monitoring.
13
patient. Screen displays a message that indicates
calibration is in process. Ensure patient remains still
during calibration. Parameters available include CO,
Cardiac Index (CI), SV, Stroke Volume Index (SVI),
Mean Arterial Pressure (MAP), Total Peripheral
Resistance (TPR), Total Peripheral Resistance Index
(TPRI), and Stroke Volume Variation (SVV). SVV
should not be utilized for diagnostic purposes unless
patient is in sinus rhythm and receiving positive
pressure mechanical ventilation. Ordering providers
may use these parameters to select interventions or may
choose to utilize maneuvers such as the PLR or Bolus
Protocols to immediately determine fluid
responsiveness.
KEYPOINTS:
Page 4 of 6
STEPS:
To obtain NIBP reading:
6. Press MENU key.
7. Press NIBP.
8. Press MANUAL NIBP.
9. If you want NIBP readings at timed
intervals, press MENU key.
10.
Press NIBP.
11.
Press NIBP Time Interval.
12.
Press the desired timed
interval to activate.
To assess fluid responsiveness using
either PLR or bolus protocol:
To perform PLR Test:
(Not recommended for traumatic brain injury,
leg amputees, uncontrolled atrial fibrillation,
deep vein thrombosis, pregnancy, or patients
with portal hypertension. Intermittent
pneumatic compression devices (IPCDs) on
The PLR test is based upon the assumption that the
average patient has approximately 200-300 ml of
vascular volume in the lower extremities. Raising the
legs results in a reversible fluid bolus. Proper
positioning and removal of compression devices prior to
the test is essential to ensure an adequate vascular
volume in the lower extremities to assess for fluid
responsiveness.
POLICY AND PROCEDURE ANALYSIS
the lower extremities should be shut off and
TED hose should be pushed down to ankles a
few minutes prior to beginning the test. Take
any pillows from under legs and ensure foot of
bed is flat. Put IV maintenance fluids on hold.
11. With patient lying supine, raise
head of bed (HOB) to 45 degrees.
12. Make sure NIBP cuff is attached to
patients arm.
13. Press the MENU, PROTOCOL, then PLR
Test.
14. To obtain baseline data, press NO.
15. Verify that the patient is in a semirecumbent position and press NEXT.
16. Keep patient still while monitor
obtains baseline data.
17. Monitor counts down three minutes. When
complete, a pop-up screen will indicate that it
is time to lower the patients HOB.
14
Follow the monitor prompts in order to obtain the series
of readings to determine baseline and PLR readings.
In order to truly challenge patient, position change must
occur as quickly as possible. Lift legs to 45 degree angle
immediately; do NOT lift gradually.
KEYPOINTS:
Test is positive if SVI rises 10% or more, indicating
patient is fluid responsive. Test is negative if SVI rises
less than 10%, indicating patient is not fluid responsive.
Page 5 of 6
STEPS:
18. When monitor prompts, lower the patients
HOB to flat. Elevate the patients legs to a 45
degree angle. May hold patients legs up or use
PLR wedge pillow, if available.
19. Press NEXT on monitor to continue the
test.
20. The monitor counts down 3
minutes.
21. After 3 minutes is up, lower the
patients legs back down and raise
the HOB to a comfortable position.
Turn IPCDs back on, if applicable.
Resume IV fluids.
To perform BOLUS Test:
5. Press MENU, PROTOCOL, and BOLUS
TEST.
6. To obtain baseline data, press NO.
Patient position does not matter during bolus test as long
as position does not change during test. Will need at
least 5 minutes of data. If bolus finishes in less than 5
minutes, continue running bolus test on NICOM until 5
minutes has elapsed.
Bolus amount of 200-300 mL may be given
in 3-5 minutes. However, verify bolus
amount to be given with ordering
provider.
Test is positive if SVI rises 10% or more, indicating
patient is fluid responsive. Test is negative if SVI rises
less than 10%, indicating patient is not fluid responsive.
POLICY AND PROCEDURE ANALYSIS
15
7. When ready to start obtaining baseline
data, press NEXT.
8. Monitor will countdown three minutes
while baseline data is obtained.
9. Once three minutes is up, a pop-up screen
will prompt to start bolus injection, press
NEXT.
10.
Once bolus complete, press MENU,
PROTOCOLS, END BOLUS TEST.
To turn off monitor:
1. Press MENU key.
2. Press EXIT
3. Press MAIN MENU
4. Press SHUT DOWN
5. Press YES
6. Machine powers off.
Clean or disinfect the unit:
1. Routine cleaning includes removal of any soil or dirt from the external surfaces. Use a soft
cloth dampened lightly with water.
2. When disinfecting the unit or when passing a patient cable between patients, clean all nondisposable parts, such as patient cable and clips with alcohol on a soft towel or wipe.
3. Do not expose the instrument, patient cable, clips or electrodes to sprays, or any other type of
solvents.
Page 6 of 6
Patient/family education
3. Purpose of monitoring
4. Procedure, including position changes and need to lie still as directed
Normal Hemodynamic Parameters Adult
Parameter
Cardiac Output (CO)
Cardiac Index (CI)
Stroke Volume (SV)
Stroke Volume Index (SVI)
Mean Arterial Pressure (MAP)
Total Peripheral Resistance (TPR)
Total Peripheral Resistance Index (TPRI)
Stroke Volume Variation (SVV)*
*During normal sinus rhythm and positive
Equation
HR x SV/1000
CO/BSA
CO/HR x 1000
SV/BSA
Directly from oscillometric profile
80 x (MAP)/CO
80 x MAP/CI
SVmax-SVmin/[(SVmax +
SVmin)/2] x 100
Normal Range
4.0 8.0 l/min
2.5 4.0 l/min/m2
60 100 ml/beat
33 47 ml/m2/beat
70 105 mmHg
800 1200 dynes sec/cm5
1970 2390 dynes sec/cm5/m2
<10% unlikely to be preload responsive
>12% likely to be preload responsive
POLICY AND PROCEDURE ANALYSIS
16
pressure mechanical ventilation
Notify ordering provider of the following:
4. Hemodynamic parameters obtained
5. Response to interventions
6. Sudden or significant changes in clinical condition and related hemodynamic parameters
Documentation:
5. Patient tolerance/response to monitoring/PLR/interventions
6. Hemodynamic parameters as ordered by the ordering provider in the Complex Vital Signs
Doc Flowsheet and/or progress note
7. Notification of ordering provider
8. Patient/family education
REFERENCES:
1. Cheetah Medical. (n.d.-a). CHEETAH NICOM reference cards. Retrieved from
http://cheetah-medical.com/sites/default/files/Cheat%20Sheet_18x24.pdf
2. Cheetah Medical. (n.d. b). Passive leg raise (PLR) protocol with the cheetah NICOM
system. Retrieved from http://files.cheetahmedical.netdnacdn.com/cdn/farfuture/JADXGHEm_jezvAwdq2xuNWCvnJCk6jZ0dE3flB6kbI/mtime:1398868310/sites/default/files/PLR_Challenge_F.
3. Cheetah Medical. (2012). NICOM sensors. Retrieved from http://www.cheetahmedical.com/sites/default/files/trainings/Leaflet-July5_2012-Rev02.pdf
4. Cheetah Medical. (2013a). Normal hemodynamic parameters. Retrieved from
http://www.cheetah-medical.com/content/hemodynamic-normal-parameters
5. Cheetah Medical. (2013b). Clinical application. Retrieved from http://www.cheetahmedical.com/clinical-applications
6. Cheetah Medical. (2013c). Passive leg raise. Retrieved from http://www.cheetahmedical.com/faq-type/passive-leg-raise-plr
7. Cheetah Medical. (2014). CHEETAH NICOM inservice video. Retrieved from
https://www.youtube.com/watch?v=RYLE2be3JLs
8. Kuhn, C., & Werdan, K. (2001). Hemodynamic monitoring. In R. G. Holzheimer & J. A.
Mannick (Eds.), Surgical treatment: Evidence-based and problem-oriented. Munich:
Zuckschwerdt.
9. Leeper, B. (2014). Cardiovascular system. In S. Burns (Ed.), AACN essentials of critical
care nursing (3rd ed.). United States: McGraw-Hill Education.
10. Marik, P. (2012). Fluid resuscitation in sepsis: The path to the holy grail. Intensive Care
Monitor, 19(3). Retrieved from http://www.intensive-care-monitor.com/portfolio/fluidresuscitation-in-sepsis-the-path-to-the-holy-grail
11. Miller, L. (2014). Hemodynamic monitoring. In S. Burns (Ed.), AACN essentials of
critical care nursing (3rd ed.). United States: McGraw-Hill Education.
You might also like
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Anti Angina (Hany)Document51 pagesAnti Angina (Hany)Angga AhadiyatNo ratings yet
- Neuro Questionnaire 1Document1 pageNeuro Questionnaire 1Michael Baylon DueñasNo ratings yet
- FLUKE ProSim 8 Technical DataDocument12 pagesFLUKE ProSim 8 Technical DataZurab SanikidzeNo ratings yet
- NCP For Dizziness and HeadacheDocument4 pagesNCP For Dizziness and HeadacheDharyl Joshua67% (12)
- Preoperative Physiology, Imaging, andDocument13 pagesPreoperative Physiology, Imaging, andSiLfia SahrinNo ratings yet
- Chest Pain. Surgical Treatment of Acute Coronary Syndrome (ACS)Document21 pagesChest Pain. Surgical Treatment of Acute Coronary Syndrome (ACS)Hanif ZamriNo ratings yet
- PALS Nitty Gritty Study Guide FINALDocument11 pagesPALS Nitty Gritty Study Guide FINALuncmikee1997100% (1)
- CHF CSDocument4 pagesCHF CSLaren CyrNo ratings yet
- Pulmonary Mbolism: Presented By: Miss. M.K.Kaku Nursing TutorDocument9 pagesPulmonary Mbolism: Presented By: Miss. M.K.Kaku Nursing TutorKaku ManishaNo ratings yet
- Body Fluids and CirculatoinDocument34 pagesBody Fluids and CirculatoinPrasmita BeheraNo ratings yet
- PathophysiologyDocument137 pagesPathophysiologyAhmed S. Hamid0% (1)
- 56 MediastinumDocument6 pages56 MediastinumRahmi Dwi AzkiahNo ratings yet
- MRCP Passmedicine Part II 2017Document8,783 pagesMRCP Passmedicine Part II 2017Prakash MahatoNo ratings yet
- Alterations in Ventricular Pumping in Patients With Atrial Septal Defect at Rest, During Dobutamine Stress and After Defect ClosureDocument10 pagesAlterations in Ventricular Pumping in Patients With Atrial Septal Defect at Rest, During Dobutamine Stress and After Defect ClosureYusrina Njoes SaragihNo ratings yet
- Mechanical and Electrical Events of The Cardiac CycleDocument39 pagesMechanical and Electrical Events of The Cardiac CyclebhatsindhoorNo ratings yet
- Histology of The Cardiovascular System-t22-HDocument22 pagesHistology of The Cardiovascular System-t22-HSekry EyaNo ratings yet
- Intepretasi EKG (DR Eka)Document93 pagesIntepretasi EKG (DR Eka)Danil Anugrah JayaNo ratings yet
- ARTIGO Accelerometer-Derived "Weekend Warrior" Physical ActivityDocument6 pagesARTIGO Accelerometer-Derived "Weekend Warrior" Physical Activitylucas.ec.sousa25No ratings yet
- Diet For Cardiovaskular Disease - ErinetaDocument8 pagesDiet For Cardiovaskular Disease - ErinetaErin NettaNo ratings yet
- Hilarie Rankin CVDocument2 pagesHilarie Rankin CVapi-555062409No ratings yet
- Cardiac RehabilitationDocument114 pagesCardiac RehabilitationAfiqul RashyedNo ratings yet
- Data Set 1: Health Exam Results: Male Age HT WT Waist Pulse SYS Dias Chol BMI Leg Elbow Wrist ArmDocument2 pagesData Set 1: Health Exam Results: Male Age HT WT Waist Pulse SYS Dias Chol BMI Leg Elbow Wrist ArmBishop PantaNo ratings yet
- Ebook Cardiology Board Review and Self Assessment A Companion Guide To Hursts The Heart PDF Full Chapter PDFDocument67 pagesEbook Cardiology Board Review and Self Assessment A Companion Guide To Hursts The Heart PDF Full Chapter PDFjohn.eastman290100% (26)
- Vascular SurgeryDocument458 pagesVascular SurgeryZoltan KardosNo ratings yet
- Curriculum Vitae Consultant Adult Cardiology: Ihab Fathi Ibrahim SulimanDocument6 pagesCurriculum Vitae Consultant Adult Cardiology: Ihab Fathi Ibrahim SulimankarlosihabNo ratings yet
- Bicuspid Aortic Valve and Dilatation of The Ascending Aorta (PDFDrive)Document82 pagesBicuspid Aortic Valve and Dilatation of The Ascending Aorta (PDFDrive)jimurgaNo ratings yet
- Shirure Et AlDocument7 pagesShirure Et AleditorijmrhsNo ratings yet
- Okeyla. Terkona DenDocument84 pagesOkeyla. Terkona DenASHRAF SANYEONGNo ratings yet
- Topic: Recent Advances - Cardiac CT: Journal ClubDocument130 pagesTopic: Recent Advances - Cardiac CT: Journal Clubjai256No ratings yet
- Endovenous Microwave Ablation of Great Saphenous VeinDocument3 pagesEndovenous Microwave Ablation of Great Saphenous VeinMalekseuofi مالك السيوفيNo ratings yet