Professional Documents
Culture Documents
ACLS ECG Rhythms & Pharmacology Review
Uploaded by
karenjlazarusOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
ACLS ECG Rhythms & Pharmacology Review
Uploaded by
karenjlazarusCopyright:
Available Formats
S.A. Pulley, D.O.
, FACOEP
ACLS ECG Rhythms
PCOM-EM
Electrocardiography: ACLS Rhythms
I.
II.
III.
IV.
V.
Objectives
A. To establish a process for rhythm review
B. To examine tachycardias and bradycardias
C. To highlight lethal rhythms
Electrical Conduction
A. PQRS
Systematic Approach
A. Rate
1. Too Fast?
2. Too Slow?
3. Middle of the Road?
B. QRS
1. Narrow?
2. Wide?
3. QRS (<0.12 sec)
C. P Waves
1. Present?
2. Constant P-R Relationship?
3. More Ps than QRSs
D. Rhythm
1. Regular?
a. Sinus
b. Junctional
c. Idioventricular
d. Atrial Flutter
2. Irregular?
a. Sinus Dysrhythmia
b. MAT
c. PACs, PJCs, PVCs
d. Atrial Fibrillation
Sinus Rhythms
A. Narrow QRS
B. Normal P-R
C. P:QRS, 1:1
D. Regular
E. Bradycardia: <60 bpm
F. Normal (NSR): 60~100
G. Tachycardia: 100~160
Atrio-Ventricular Blocks
A. 1st Degree-Clinical insignificance
B. 2nd Degree
1. Mobitz I (Wenckebach)
2. Mobitz II
C. 3rd Degree
1. Complete AV Dissociation
2. Ventricular Standstill
D. A-V Blocks
1. Class 1-All impulses get through
2. Class 2-Some get through
3. Class 3-No impulses get through
E. 1st Degree AVB
1. P-R >0.20 sec (5 little boxes) (1 big box)
F. 2nd Degree AVB-Mobitz I, Wenckebach
1
300 - 150 - 100 - 75 - 60 - 50 ~40
S.A. Pulley, D.O., FACOEP
ACLS ECG Rhythms
PCOM-EM
VI.
VII.
1. Progressive prolongation P-R
2. Then drops a QRS
G. Pearl
1. Variable P-R interval can only be
a. 2nd Degree AVB-Mobitz I
b. 3rd Degree AVB
c. To differentiate
i.
Must check every P-P interval
ii.
Must check every R-R interval (or S-S)
d. Then look for the Wenckebach pattern
H. 3rd Degree AVB-Usually wide QRS, can be narrow
1. Variable P-R
2. Constant P-P
3. Constant S-S (or R-R )
a. Can be variable or absent
I. 2nd Degree AVB-Mobitz II
1. Constant P-R Interval
2. More Ps than QRSs
3. Described by ratio
a. 2:1, 3:1, 4:1, or Variable
Lethal (or potentially lethal)
A. Dead Rhythms-Rhythms without a pulse
1. Asystole
2. Pulseless Electrical Activity (PEA)
3. Ventricular Fibrillation (VF)
4. Pulseless Ventricular Tachycardia (VT)
B. Asystole
1. Confirm asystole in 2 leads
C. Pulseless Electrical Activity (PEA)
1. Any organized rhythm without a pulse is PEA
2. Except VT which gets treated as VF
D. VF/Pulseless VT (See below for VT)
1. Priority is Defibrillation (if available)
E. Torsades de Pointes
1. The impulse travels around the myocardium
2. You are looking at it from the same spot (Lead II)
3. Therefore, the amplitude changes rhythmically
Tachycardias
A. SVT (Narrow Complex)
1. Sinus Tachycardia (See above for ST)
a. Normal P-R
2. Multifocal Atrial Tachycardia
a. Ps variably different
3. Atrial Tachycardia
a. Ps abnormal but non-variable
b. Or too fast for Sinus Tachycardia
4. Paroxysmal-Start/Stop on own
5. Stable vs. Unstable (SVT or VT)
a. Determined by physical signs, Not The Rate
b. Stable
i.
SBP > 90, Normal Mentation, No CP, Lungs Clear
S.A. Pulley, D.O., FACOEP
ACLS ECG Rhythms
PCOM-EM
c.
Unstable
i.
SBP<90 (or so), Change in responsiveness, Crushing CP, CHF
d. Unstable Electricity Requires Electricity to fix it
e. Stable Electricity Gets Medical Therapy
B. Wide Complex Tachycardia (Fast, Wide, No P Waves
1. SVT with Aberrancy
a. Preexisting Bundle Branch Block
2. Ventricular Tachycardia
VIII.
Early Beats (Ectopy)-Premature Contractions
A. PAC-Atrial ( Different P waves)
B. PJC-Junctional ( No P waves)
C. PVC-Ventricular
1. Unifocal
2. Multifocal
3. Couplets
IX.
No P Waves
A. Junctional Rhythm
1. Junctional Escape (40-60 bpm)
2. Accelerated Junctional (>60 bpm)
B. Idioventricular
1. Ventricular Escape (20-40 bpm)
2. Idioventricular (>40 bpm)
X.
Too Many P Waves
A. Atrial Fibrillation
1. Irregularly irregular
2. P waves are not well defined
B. Atrial Flutter
1. Saw tooth pattern (Woodsmans)
2. Ratio: 2:1, 3:1, 4:1, Variable
C. Pearl
1. If a patient has a seemingly Sinus Tachycardia of 145-155
2. And the patient is symptomatic in any way at all
3. Consider that the patient may be in a 2:1 or 3:1 Atrial Flutter
4. Because at that rate and ratio the extra p waves disappear into the QRS and T
waves
S.A. Pulley, D.O., FACOEP
ACLS ECG Rhythms
PCOM-EM
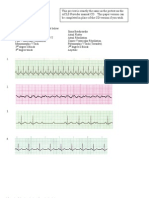
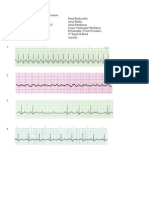
Lets see if you were paying attention
1
2
5
7
6
8
10
11
12: A
D
4
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
ACLS Pharmacology
I.
II.
III.
Snap Shot of Instability
A. ABCDEs
B. Vital Signs
i. Heart Rate, Respiratory Rate, Blood Pressure
ii. Pulse Oximetry, Blood Sugar
iii. Temperature
C. Mental Status
i. Confusion
ii. Disorientation
D. Symptoms
i. Chest Pain
ii. Dyspnea
iii. Lightheadedness
E. Physical Signs
i. Respiratory Distress
ii. Pallor
iii. Diaphoresis
Initial Management
A. Rapid Assessment
i. ABCDEs
ii. Mental Status
iii. Gross Appearance
iv. Pulse/HR/RR
B. 12 Lead ECG
C. Oxygen (O2) if Pulse Ox<94%
D. Cardiac/Pressure/Pulse Ox Monitor
E. Treatment based on findings
F. Pay Attention
i. Time => Brain Cells
ii. Time => Resistance to Defibrillation
iii. Time => Muscle
Drug Class Recommendations
A. Class I
i. Always indicated
ii. Solid proof of utility
B. Class IIa
i. Probably helpful
ii. Most data support use
C. Class IIb
i. Possibly helpful
ii. Some supportive data
iii. Not harmful
D. Class Indeterminate
i. Insufficient scientific evidence at this time
E. Class III-Contraindicated/Harmful
IV.
V.
VI.
VII.
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
PAY ATTENTION
A. Time is Critical
i. Time=>Brain Cells
ii. Time=>Resistance to Defibrillation
iii. Time=>Cardiac Muscle
Do drugs make a difference?
A. Not really
What makes a difference?
A. Optimal compressions
B. Avoid hyperventilation
C. Early defibrillation
Dead Rhythms (Rhythms without a pulse) Therapy
A. Treatment
i. Oxygen
ii. Epinephrine
iii. (Lidocaine/Amiodarone)
iv. Defibrillation
v. Magnesium Sulfate
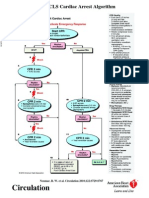
B. Dead Box (Algorithm box)
i. All dead rhythms (no pulse) have common elements of treatment
ii. All get/continue AAA-CAB/CPR
iii. All get an IV or IO
iv. All get Epinephrine 1 mg IV (1:10,000)
v. All get intubated/advanced airway when convenient
vi. Elements added at beginning or end
C. Oxygen
i. Always administer 100% FiO2 in Arrest states
ii. Cardio-Respiratory distress
iii. Class: I
iv. Contraindications-COPD
(Vasopressin 40 u IV)
1. Never withhold Oxygen in hypoxic states
2. Monitor ventilation (pCO2) and assist prn
3. Intubate if necessary
v. However, in ischemic states once patient stabilized
1. Back off on FIO2 to keep pulse ox>94%<100% (When Convenient)
D. Ventilation Technique
i. No advanced airway: 30:2 (Compressions:Ventilations)
ii. Yes advanced airway: 1 breath Q 6 seconds
1. Same if Respiratory Arrest only
2. Same for Children <8 y/o except:
a. 15:2 if two rescuers no advanced airway
iii. Normal tidal volume 6 ml/kg
iv. Code Volume:
1. No O2: 10 ml/kg over 1 second
2. Yes O2: 6-7 ml/kg over 1 second
v. Goal is PaCO2/ETCO2 of 35-40
vi. Avoid Hyperventilation=>Respiratory alkalosis and decreased cerebral perfusion
E. Epinephrine
i. Potent Vasoconstrictor
ii. Beta1, Beta2, & Alpha1, Alpha2 Stimulation
iii. Administration IV/IO, (ETT if no IV/IO
iv. Dose
1. IV:
1 mg q3 5 min
a. ETT: 2 2.5x IV dose=>Intraosseous recommended!
v. Indications-Class I
vi. V-Fib, Unstable V-Tach, Asystole, PEA
vii. (Also, IM/SQ for Anaphylaxis or Status Asthmaticus)
1. 0.3 mg (0.3 ml of 1:1K)
CAB-D/CPR
I V /I O
Epi 1 mg IV
Intubate
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
viii. Contraindications / Cautions
1. Stable Vital Signs
2. Caution in elderly
F. No IV?
i. Preference is IV or IO (Intraosseous)
ii. However, drugs that can be given via Endotracheal Tube (ETT)
iii. True ACLS Drugs (A-L-E)
1. Atropine
2. Lidocaine
3. Epinephrine
iv. (N-A-V-E-L)
1. Add Narcan and Vasopressin
G. Asystole-Check that leads are attached and check in more than one lead
i. Recommend the same for VF
H. PEA (Pulseless Electrical Activity)-If bradycardic could consider transcutaneous pacing
VIII.
Ts and Hs
A. Anytime the patient is not doing well
i. Do primary survey, ABCDE
ii. Check 6 vital signs (BP-HR-RR-T-PO-BS)
B. Consider the Ts and Hs (order reversed on purpose) (5 each)
i. Tension Pneumo, Tamponade, Thrombosis-Pulmonary, Thrombosis-Coronary,
Toxins/Tablets
ii. Hypoxia, Hypovolemia, Hyperacidemia, Hyperelectrolytemia, Hypothermia
C. PALS has 6 each adding Hypoglycemia and Trauma (for hemorrhage)
IX.
VF/Pulseless VT
A. Time => Resistance to Defibrillation
B. Quick Look for and immediate Defibrillation if appropriate
C. SHOCK at maximum for device
i. 360 J Monophasic or 120-200 (up to 360) J Biphasic depending on the machine.
ii. Time to shock is critical
iii. Try to defibrillate as close to time 0 as possible
D. Dead Box Therapy
i. CAB-D/CPR
ii. IV/IO
iii. Epinephrine 1mg IV
iv. Intubate/advanced airway when ready/convenient
E. 2 minute blocks for code
i. CAB/CPR to Circulate drug for 2 minutes
ii. Drug at beginning of the block
1. (Every other 2 minute block is Epi step)
iii. Reevaluate-TRIAD
1. Rhythm-if potentially perfusing check:
2. Pulse-to see if it is perfusing:
2 Minutes
3. BP-to see how well it is perfusing
4. If awake, dont forget to ask how they are
iv. Shock-if shockable rhythm
v. DO NOT PAUSE TO CHECK RHYTHM IMMEDIATELY AFTERWARDS
1. Wait for 2 minute mark due to myocardial stunning
vi. Go back to i. to start next block and give next drug (if indicated)
F. Amiodarone
i. Anti-Dysrhythmic
ii. Action:
1. Works @ AV Node, Bundles, & Ventricles
iii. Administration: IV
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
X.
iv. Dosage:
1. VF / Unstable VT: 300 mg IVP
a. Repeat after 4 minutes once at (150 mg IVP)
2. Stable VT/SVT: 150 mg over 10 minutes
3. Then administer @ 1 mg/min X 6 hrs
4. Then @ 0.5 mg/min X 18 hrs
v. Indications
1. VF, Stable / Unstable VT & SVT
vi. Contraindications / Cautions
1. Caution in hypotension, Hypersensitivity
G. Lidocaine
i. Class: IIb
ii. Anti-Dysrhythmic
iii. Action: works @ Bundles & Ventricles
iv. Dose:
1. Bolus: 11.5 mg/Kg IVP Max Dose 3 mg/Kg
2. Repeat: 1/2 of bolus (0.5-0.75 mg/Kg)
3. Infusion: 1 4 mg / min
v. Indications
1. VF, VT
vi. Contraindications / Cautions
1. Hypotension, Hypersensitivity
H. Magnesium Sulfate
i. Action: Cardiac membrane stabilization
ii. Administration: IV
iii. Dose
1. 1 2 grams IV over 5 60 min in 50 100 cc
iv. Indications
1. Torsades de Pointe => Class I
2. Hypomagnesemia, Status Asthmaticus
v. Contraindications / Cautions
1. Not recommended routinely in cardiac arrest
Too Fast (Tachycardic) Therapy
A. Anti-dysrhythmics
i. Lidocaine, Amiodarone, Magnesium (done above)
ii. Procainamide
1. Anti-dysrhythmic
2. Action: AV Node, Bundles & Ventricles
3. Dose
a. Code: 50 mg/min
i. 1 gm in 100 cc @ 300 cc/h = 50 mg/min
b. Therapeutic: 20 30 mg/min
i. 1 gm in 100 cc @ 150 cc/hr = 27 mg/min
c. Maximum 15 mg/kg (~1 gm)
4. Indications
a. Atrial & Ventricular Dysrhythmias
5. Contraindications / Cautions
a. Hypotension
b. Do not use with Amiodarone
c. Avoid in Torsades
6. Reasons to Stop
a. Hypotension
b. QRS width > 50% of baseline
c. Reach maximum dose of 1 gm (15 mg/kg)
d. Dysrhythmia suppression
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
B. Generally treatment of SVT is:
i. Stable SVT: Vagal Maneuvers then Adenosine then Rate Control with Beta or
Calcium channel blockers
ii. Unstable SVT (See I below): Synchronized Cardioversion
iii. Stable Tachycardia
1. SBP>90
2. Normal mentation
3. No chest pain
4. Clear lungs/No dyspnea
C. 1st Vagal Maneuvers-Hands on-Remember you are an Osteopathic Physician!
i. Eyeballs-Ocular Pressure
1. ***Caution in elderly
ii. Face-Surprise ice water immersion
iii. Neck-Carotid sinus massage
1. ***Caution in elderly
iv. Belly-Valsalva
v. Butt-Anal Massage
vi. (Not in ACLS book: V-Spread)
D. Adenosine
i. Action: AV node blockade
ii. Half-Life: < 10 seconds
iii. Administration: IV Rapid Push through at least proximal 18 ga.
1. With immediate slam IVP NSS bolus 10-20 ml
2. And raise arm to enhance return
iv. Dose: 6 mg => 12 mg => 12 mg?
v. Indications: SVT, PSVT
vi. Contraindications / Cautions
1. May slow Atrial Fibrillation only
2. Dont use diagnostically in Wide Complex Tachycardia
3. Effectiveness with Theophylline, Dipyridamole, Carbamazepine
4. May cause bronchospasm
vii. WARN the patient as it transiently stops the heart (Dont tell the patient THAT!)
E. Verapamil
i. Action: Calcium Channel Blocker, AV Node Blockade
ii. Administration: IV
iii. Dose
1. 2.5 5 mg IV / 1 minute (0.075 0.15 mg / Kg)
2. Re-dose 5-10 mg in 15-30 mg
iv. Indications
1. Rate control of Narrow Complex Tachycardia
v. Contraindications / Cautions
1. Wide Complex Tachycardia (re-entry)
2. Hypotension (may result in hypotension)
3. Calcium IV may be given if adverse effects
F. Diltiazem
i. Action: Calcium Channel Blocker, AV Node Blockade
ii. Administration: IV, PO
iii. Dose
1. 1st Dose: 0.25 mg/Kg IV (5 10 mg)
2. 2nd Dose: 0.35 mg/Kg IV (10 15 mg)
3. Infusion: 5 15 mg/hr
iv. Indications
1. Rapid Atrial Fibrillation, other SVT's
v. Contraindications / Cautions
1. Hypotension
2. Wide Complex Tachycardia
vi. May administer Calcium IV to reverse effects
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
G. Metoprolol/Atenolol and Labetolol
i. Action: Beta Blocker, AV Node Blockade
ii. Dose
1. Labetalol: 10 20 mg IV over 1 2 min
a. Double with each subsequent dose q10 min
b. Infusion: 2 8 mg / min
2. Metoprolol: 5 mg IV over 2 5 min q 5 min (x 3 for ACS)
a. PO Dose given after IV loading
iii. Indications
1. Hypertensive Emergency
2. Heart Rate Control (esp. AMI) or SVT
iv. Contraindications / Cautions
1. Hypotension, Bradycardia
H. Esmolol
i. Titratable Beta Blocker
ii. Short half life
iii. Little hypotension or bronchospasm
iv. 250-500 mcg/kg IVB over 1 minute
v. Then 25-50 mcg/kg/min
vi. Re-bolus q 5 min PRN
vii. Increase in 50 mcg/kg/min steps to max of 200 mcg/kg/min
I. Sotalol
i. Action:
1. Blockade at AV Node, Bundles & Ventricles
ii. Dose
1. IV: 1 1.5 mg/Kg @ 10 mg/min
2. PO: 40 80 mg PO BID
iii. Indications
1. Ventricular & Supraventricular Dysrhythmias
iv. Contraindications / Cautions
1. Bradycardia
2. Hypotension
3. Pro-Dysrhythmic (Torsades)-So not used much
v. Limited by Slow infusion rate
J. If you use Calcium Channel or Beta Blocker be prepared to synchronized cardiovert
i. You can make them and Unstable Tachycardia mostly through hypotension
ii. Because they all have antihypertensive properties
iii. Or, if they have a bypass tract tachycardia (e.g. WPW, LGL, etc.)
1. Blocking the AV node pushes all the impulses to the bypass tract
2. Which causes the HR to zoom up, and the BP crash
K. Synchronized Cardioversion for Unstable Tachycardias
i. When presented with a tachycardia, decision point as to whether stable or
unstable
ii. Unstable Electricity requires Electricity to fix it
iii. SVT or VT
iv. Unstable-Only need one of the following to be unstable
1. Hypotension (SBP<90)
2. Significant change in mental status
3. Cardiogenic chest pain
4. Dyspnea from pulmonary edema/CHF
v. Joules-Monophasic or Biphasic
1. 100 J (If A-Flutter 50 J)
2. 200 J
3. 300 J
4. 360 J
XI.
XII.
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
Shock (Hypotension) Therapy
A. Oxygen (Above)
B. Normal Saline Solution
i. Crystalloid
ii. Preferred resuscitation solution
iii. First line treatment of hypotension
iv. 250 ml-1000 ml fluid bolus IV
1. Amount driven by clinical situation
v. Caution (Doesnt mean dont give it)
1. CHF (or History of CHF), Elderly
2. Renal Failure
C. Dopamine
i. Action:
1. Dopaminergic (Renal Artery Dilatation)
2. Beta (Inotropic & chronotropic heart stimulation)
3. Alpha (Peripheral arterial constrictor)
ii. Dose
1. Dopaminergic: 3 5 ug/kg/min
2. Beta: 5 10 ug/kg/min
3. Alpha: 10 20 ug/kg/min (Shock Dose)
iii. Indications: Hypotension
D. Dobutamine
i. Action: Inotropic beta stimulation, increases cardiac contractility
ii. Dose: 5 20 ug/kg/min
iii. Indications: Cardiogenic Shock
iv. Adverse Effects: Hypotension due to arterial dilatation
v. Do not administer unless SBP > 90 mmHg
E. Norepinephrine
i. Action: Pure alpha stimulation, potent arterial constrictor
ii. Dose: 4 8 ug/min
iii. Indications: Refractory Hypotension
iv. Very good for poor vascular tone shock such as neurologic or septic
F. Epinephrine (Above)
Too Slow (Bradycardia) Therapy
A. Atropine
i. Action: AV Node stimulation
ii. Dose: IV
1. 0.02 mg/Kg IV (minimum dose = 0.1 mg)
2. Bradycardia Dose: 0.5 mg IV (Dont want to overshoot)
a. No longer indicated for Asystole
iii. Indications
1. Sinus Bradycardia with significant HypoTN (Class I)
2. Other Symptomatic Bradycardia (Class IIb)
3. Contraindications / Cautions
a. Use caution in Mobitz II and 3rd AV Block
b. May increase degree of block
B. Dopamine-Beta Property (Above)
C. Dobutamine-Beta Property(Above)
D. Epinephrine-Beta Property (Above)
E. Isoproteronol-Pure Beta-Just mentioning, rarely utilized
i. 2-10 mcg/minute
ii. 2 mg in 250 ml starting at 15 ml/hr
iii. Sympathomimetic with pure beta
iv. Potent inotropic and chronotropic effects
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
XIII.
XIV.
F. Symptoms
i. Mild=>Perhaps no treatment, just monitoring
ii. Moderate=>Atropine and if it doesn't work a Beta drug
iii. Severe "Unstable"-SBP<90, Confusion, CP, CHF
1. Unstable Electricity Requires Electricity=>Pacing
G. Pacemakeri. Transcutaneous easiest to place
ii. Any symptomatic bradycardic rhythm
1. Especially if with severe symptoms or perfusion issues
iii. Absolute consideration for Mobitz 2 and 3rd degree AVB
iv. Downside is that TCP is uncomfortable
Too Wet (Fluid Overload) Therapy
A. Oxygen (Above)
B. Nitroglycerin
i. Coronary Artery Vasodilator
1. Decreases preload first, Then afterload at higher doses
ii. Dosage:
1. SL: 300400ug (0.30.4mg) q5 min
2. IV: 1020 ug/min & titrate by 10ug q 5 min
3. TC: - 2 inch paste to chest wall
iii. Indications
1. Ischemic Cardiac Chest Pain, CHF
2. Hypertension (Including Hypertensive Emergency)
iv. Contraindications / Cautions
1. Hypotension (SBP < 90)
2. Viagra/Cialis/Levitra
3. Revatio/Adcirca (used for pulmonary hypertension)
C. Positive Pressure Airway-CPAP, BiPAP, or Ventilator
D. Furosemide
i. Loop Diuretic
ii. Dose:
1. 0.5 - 1 mg/kg IV (~40 mg)
2. Avoid over diuresing
iii. Indications:
1. Pulmonary Edema, Hypertensive Crisis
2. Increased ICP
iv. Cautions:
1. Low BP
2. Hypovolemia
3. Electrolyte lows
E. Dopamine-Beta Property (Above)
F. Dobutamine-Beta Property (Above)
Too High (Pressure) Therapy
A. Nitroglycerin-Afterload reduction (Above)
B. Nitroprusside-Just mentioning, rarely utilized
i. Potent vasodilator
ii. Indications:
1. High SVR cardiogenic shock, pulmonary edema, acute MVR or AVR
2. Reduces afterload
iii. Indicated for severe hypertension
iv. Mix 50-100 mg in 250 D5W
1. Range 5-10 mcg/kg/min
2. Begin 0.1 mcg/kg/min
3. Light sensitive: Cover the IV bag
C. Beta Blockers-Afterload reduction (Metoprolol/Atenolol, Labetolol Above)
XV.
XVI.
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
Acute Coronary Drugs- (Covered in the ACS Lecture)
A. Oxygen (Above)
B. Nitroglycerin (Above)
C. Aspirin
D. Heparin/Lovenox
E. Beta Blockers (Above)
F. Opiates
G. Thrombolytics
Miscellaneous Drug
A. Calcium Chloride
i. Indications:
1. Hyperkalemia, Hypocalcemia
2. Antagonize Ca+ Channel Blockers
ii. Dose:
1. 8 - 16 mg/kg (5 - 10 ml) IV
iii. Precautions:
1. Do not use routinely in cardiac arrest
2. Do not mix with Sodium Bicarbonate
B. Sodium Bicarbonate
i. Action: Uncertain
ii. Dose
1. Initial: 1 meq/Kg IV Bolus
2. Repeat: 0.5 meq/Kg q 10 min
iii. Indications
1. Class I
a. TCA or Phenobarbital Overdose
b. Hyperkalemia
c. Known pre-existent Metabolic Acidosis
2. Class II b =>Protracted Code
iv. Contraindications / Cautions
1. Avoid admixture or infiltration with Calcium or Epinephrine
2. Use only after other Class I / Class II drugs
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
ACLS Pharmacology (List Only)
I.
II.
III.
IV.
V.
Dead Rhythms (Rhythms without a pulse) Therapy
A. Asystole, Pulseless Electrical Activity, Ventricular Fibrillation,
Ventricular Tachycardia, Torsades De Pointes
B. Dead Box (Algorithm box)
i. All dead rhythms (no pulse) have common elements of treatment
ii. All get/continue CAB-D/CPR
iii. All get an IV/IO
iv. All get Epinephrine 1 mg IV
v. All get intubated/advanced airway when convenient
vi. Elements added at beginning or end
C. Medications
i. Oxygen
ii. Epinephrine
iii. Lidocaine or Amiodarone
iv. Defibrillation (Non pharmacologic therapy)
v. Magnesium Sulfate
Too Fast (Tachycardic) Therapy
A. Anti-dysrhythmics
i. Lidocaine, Amiodarone, and Magnesium (Covered earlier)
ii. Procainamide
B. Stable SVT
i. 1st Vagal Maneuvers (Non pharmacologic therapy)
C. Adenosine
D. Rate Control Calcium Channel Blockers
i. Verapamil
ii. Diltiazem
E. Rate Control Beta Blockers
i. Metoprolol/Atenolol
ii. Labetolol
F. Sotalol
G. Unstable Tachycardia
i. Synchronized Cardioversion (Non Pharmacologic therapy)
Shock (Hypotension) Therapy
A. Oxygen (Covered earlier)
B. Normal Saline Solution
C. Dopamine-(=>)
D. Dobutamine-() (Cardiogenic Shock Only)
E. Norepinephrine-()
F. Epinephrine-( & )
Too Slow (Bradycardia) Therapy
A. Atropine
B. Dopamine-() (Covered earlier)
C. Dobutamine-() (Covered earlier)
D. Epinephrine-() (Covered earlier)
E. Isoproteronol-() -Rarely utilized
F. Transcutaneous Pacemaker-(Non Pharmacologic therapy)-For Unstable
Too Wet (Fluid Overload) Therapy
A. Oxygen (Covered earlier)
B. Nitroglycerin
C. Positive Pressure-CPAP, BiPAP, or Ventilator
D. Furosemide
E. Dopamine-() (Covered earlier)
F. Dobutamine-() (Covered earlier)
1
S.A. Pulley, D.O., FACOEP
ACLS Pharmacology
PCOM-EM
VI.
VII.
VIII.
Too High (Pressure) Therapy
A. Nitroglycerin (Covered earlier)
B. Nitroprusside-Rarely utilized
C. Beta Blockers (Metoprolol/Atenolol, Labetolol covered earlier)
Acute Coronary Drugs (Covered in the ACS Lecture)
A. Oxygen (Covered earlier)
B. Nitroglycerin (Covered earlier)
C. Aspirin
D. Heparin/Lovenox
E. Beta Blockers (Covered earlier)
F. Narcotics
G. Thrombolytics
Miscellaneous Drugs
A. Calcium Chloride-Calcium Channel Blocker Toxicity, Hyperkalemia
B. Na Bicarbonate-Hyperkalemia, TCA OD
S.A. Pulley, D.O., FACOEP
Acute Brain Syndrome
PCOM-EM
Acute Brain Syndrome
Acute Stroke
I.
II.
III.
IV.
V.
VI.
VII.
Objectives
A. To identify symptoms and diagnostics
B. To establish priorities and treatments
Brain Attack
A. Stroke has a similar pathogenesis as Acute Coronary Syndrome
B. It also is very time sensitive
C. We are just starting to be able to treat Acute Stroke
Epidemiology
A. 3rd Leading Cause of Death
B. Leading cause of disability
C. 3.8 million stroke survivors
1. 10 % No deficits
2. 48 % Hemiparetic
3. 22 % Gait dysfunction
4. 16 % Aphasic
8 Ds of Stroke Care
A. Detection- Signs and Symptoms
B. Dispatch- 9-1-1
C. Delivery- Rapid transport
D. DoorUrgent triage
E. DataBrain CT
F. Decision (and Discussion)
G. DrugAdministration
H. Disposition
Pathophysiology
A. Blockage causes cell death within minutes
1. We can not treat this
B. The goal is to prevent the ischemic penumbra from converting to cell death
1. This is the focus of therapies
Cincinnati Stroke Scale-FAST Exam
A. Facial Droop
i.
Normal: Both sides of face move equally
ii.
Abnormal: One side of face does not move at all
B. Arm Drift
i.
Normal: Both arms move equally or not at all
ii.
Abnormal: One arm drifts compared to the other
C. Speech
i.
Normal: Patient uses correct words with no slurring
ii.
Abnormal: Slurred or inappropriate words or mute
Los Angeles Prehospital Stroke Screen
A. Look for obvious asymmetry
B. Facial smile / grimace
i.
Left and Right
ii.
Normal or Facial Droop
C. Grip Strength
i.
Left and Right
ii.
Normal, Weak, No Grip
D. Arm weakness
i.
Left and Right
ii.
Normal, Drifts Down, Falls Rapidly
S.A. Pulley, D.O., FACOEP
Acute Brain Syndrome
PCOM-EM
VIII.
IX.
X.
XI.
Immediate Assessment-Within 10 minutes of arrival (Arrival to T+10 minutes)
A. ABCs, Vital Signs
B. Oxygen: If pulse ox<94%
C. Blood Sugar, Thiamine/Naloxone
D. 12 Lead ECG
E. Neuro Assessment
F. Alert Stroke Team
Immediate Neurologic Assessment-(Within Arrival to T+25 minutes)
A. History
B. Physical Exam
C. Neurologic Exam
D. LOC/GCS
E. NIH Stroke Severity Score
F. Urgent Non-contrast CT
G. C-spine evaluation (if trauma)
CT Brain interpretation negative for bleed (Within Arrival to T+45 minutes)
Therapy
A. TPA-Within 3 hours of onset and 60 minutes of arrival (T+60 minutes)
1. Only medication currently approved
2. Significant time constraint
3. Use driven by symptoms and age
4. Stroke Scores/Scales
B. Dose
a. 0.9 mg/kg IV
b. 10% given as IVB
c. Remainder given over 1 hour
C. Symptomatic ICH
a. TPA for CVA-~6.4%, half of which are life threats or death
b. TPA for MI-~0.6% in presumably normal brain
D. Contraindications
a. Current ICH or SAH
b. <3 Months Neurosurgery or CVA
c. History of ICH
d. HTN: >185/>110 (Until controlled)
e. IC Neoplasm
f. Active internal bleeding
g. Coagulopathy/Thrombocytopenia <100K
h. Heparin within 48 hours
E. Within 3 Hours
1. Patient must recognize problem
2. Get to the hospital
3. Have Acute Stroke recognized by staff
4. Thorough neuro exam
5. CT Scan done and interpreted as (-)
6. Have a neurologic consultation
7. Consideration for utility of TPA
8. Determination of any contraindications
F. TPA-Door to needle time goal of <60 minutes
S.A. Pulley, D.O., FACOEP
Acute Brain Syndrome
PCOM-EM
G. Some centers have extended 3 to 4.5 hours due to Evidenced-Based literature
1. FDA is strongly against that
2. Subgroups that did poorly and are thus exclusions:
a. BP >185/110 even if controlled
b. DM with prior CVA
c. NIHSS>25
d. Age>80
e. Any anticoagulant regardless of INR
A. < 3 hours you can correct warfarin to INR < 1.2
B. Not so in the 3-4.5 hour timeframe
C. Antiplatelet agents are OK
H. Intracerebral artery (invasive) TPA can be given to 6-8 hours (depends on location)
XII.
NIH Stroke Scale-NIHSS (Score of 0, 1, 2, 3)
1A. LOC
-Alert, Arousable, Repeated stimulation or pain, Not
1B. LOC Questions (2)
-Month and Age
1C. Commands (2 tasks)
-Open and close eyes and hands, or similar
2. Best Gaze
-Normal (EOMI), Palsy, Total paresis
3. Visual
-Normal
-Hemianopia: Partial, Complete Unilateral, Bilateral
4. Facial Palsy
-Normal, Minor, Partial, Complete Paralysis
5. Motor Arm-Each Arm with own score
-No Drift, Drift, Effort against gravity, No effort against gravity, No movement
6. Motor Leg
-No Drift, Drift, Effort against gravity, No effort against gravity, No movement
7. Limb Ataxia (Finger-Nose, Heel-Shin)
-Absent, Present in 1 limb, Present in 2 limbs
8. Sensory (Pinprick or Withdrawal)
-Normal, Mild to Moderate Loss, Severe to Total Loss
9. Best Language (Aphasia)
-None, Mild/Moderate, Severe, Global
10. Dysarthria
-None, Mild/Moderate, Severe
11. Extinction/Inattention (Formerly Neglect)
-None, Inattention to stimulus, Profound Inattention
XII. Permissive HTN
A. If TPA candidate, BP needs to be <185/110
1. Can use a number of IV agents
B. If not a TPA candidate, allow BP to be high up to maximum of 220/140
1. Increases cerebral perfusion pressure to drive through the ischemic penumbra
XIV. Future Therapies?
A. Hypothermia-At least prevention of hyperthermia
B. Magnessium
C. Caffeinol
D. Statins-Antiinflammatory wonder drug
E. Recanalization Devices
1. MERCI-Clot Extractor
2. The Penumbra Device-Think Roto-Rooter
S.A. Pulley, D.O., FACOEP
Acute Brain Syndrome
PCOM-EM
XV. CT Scan
A. Fast, widely available, cheaper than MRI
B. Detects ICH/SDH/EDH about 100% of the time
C. Does not show CVA
D. Misses about 3-6% of SAH
XVI. MRI
A. Can show tissue that is dead and that at risk (penumbra)
B. MRA shows the circulation
C. Takes longer, not readily available, more expensive
XVII. Hemorrhagic CVA
A. CT (+) For Bleed
B. ICH 10%, SAH 6% of CVAs
C. Requires Neurosurgical Consultation and Neuro ICU admission
S.A. Pulley, D.O., FACOEP
Acute Brain Syndrome
PCOM-EM
Stroke Distributions
Vascular Territories
XVIII. Anterior Cerebral Artery-2%
A. Contralateral paresis, Legs>Arms
B. Sensory deficit in the same distribution
C. Gait disturbance due to weakness, not cerebellar balance dysfunction
XIX. Middle Cerebral Artery-90%
A. Contralateral paralysis, Face/Arms>Legs
B. Sensory deficit in the same distribution
C. Aphasia (if dominant hemisphere)
D. Hemineglect (if nondominant hemisphere)
E. Homonymous hemianopsia
1. Eyes look towards the side of the stroke
2. Vision preserved on the side of the stroke
F. Right-handed=>Left hemisphere dominant=>Left MCA CVA
1. Right hemiparesis & sensory deficit
2. Aphasia
3. Right homonymous hemianopsia-(Looks to right)
G. Right-handed=>Left hemisphere dominant=>Right MCA CVA
1. Left hemiparesis & sensory deficit
2. Left hemineglect
3. Left homonymous hemianopsia-(Looks to left)
H. Reverse for opposite handedness and dominance
I. Left-handed=>Right hemisphere dominant=>Right MCA CVA
1. Left hemiparesis & sensory deficit
2. Aphasia
3. Left homonymous hemianopsia-(Looks to left)
J. Left-handed=>Right hemisphere dominant=>Left MCA CVA
1. Right hemiparesis & sensory deficit
`
2. Right hemineglect
3.Right homonymous hemianopsia-(Looks to right)
XX. Posterior Cerebral Artery-5%
A. Supplies occipital cortex=>one of the following:
1. Homonymous hemianopsia on contralateral side
2. Right artery looks left, Left artery looks right
3. Visual agnosia-Can't recognize objects
4. Cortical blindness
5. Plus:
a. Confusion
b. Paresthesias
c. Dizziness
d. Nausea
e. Memory loss
f. Language dysfunction
g. Minimal motor involvement in the form of a tremor
S.A. Pulley, D.O., FACOEP
Acute Brain Syndrome
PCOM-EM
XXI. Vertebrobasilar Artery
A. Supplies brainstem, cerebellum, visual cortex
B. Mortality >85%
C. Symptoms depend on the area of ischemia, can be variable
D. Typically waxing/waning course
E. Up to 50% have TIA's days before the CVA
F. ***Vertigo, Vomiting, HA, CN findings***
G. Large number of manifestations
1. Abnormal oculomotor, dysarthria, dysphagia
2. Face and tongue weakness, face and scalp sensory loss
3. Decreased LOC, ataxia, contralateral weakness, incontinence
XXII. Cerebellar Artery-3%
A. 3 vessels: Superior, Inferior, Posterior
B. ***Vertigo, Vomiting, HA, Ataxia***
1. Note similarity to the VBA CVA minus CN findings
XXIII. Lacunar Syndromes-15-25%
A. Small deep penetrating vessels
B. Microinfarctions in HTN/DM patients
C. Stuttering course, CT (-)
D. Prognosis is better
E. 5 Types:
1. Pure motor hemiparesis: Pons or Internal Capsule
2. Pure sensory: Thalamus
3. Dysarthria-Hemiparesis: Pons, Internal Capsule
4. Ataxia-Hemiparesis: Pons, Internal Capsule
5. Mixed Sensorimotor: Hemiparesis with Ipsilateral complaints
XXIV. Transient Ischemic Attack-TIA
A. 2009 AHA/ASA:
1. A transient episode of neurological dysfunction caused by focal brain, spinal cord, or
retinal ischemia, without acute infarction
B. Now a tissue based, not time based, diagnosis
C. Requires imaging
1. Immediate neuroimaging is key
2. MRI is better
3. CT is faster but is limited in the posterior circulation
D. Need to figure out why:
1. ECG to look for A-fib that could be embolic cause
2. MRA or CTA to look for stenosis
3. Carotid doppler if MRA/CTA does not show the carotids well
4. Echocardiography for clots and function
5. Bubble test echocardiography to look for right to left shunts (e.g. PFO)
E. ABCD2 is not accurate enough for low risk
F. All TIA's require urgent work-up within 48 hours
1.Usually accomplished through short admission
G. TIA=Warning sign
H. Risk of progression:
1. Within 2 days: 1 - 8% (=1/100-1/12 risk of CVA within 48 hrs)
2. Within 7 days: 1.2 - 11%
3. Within 90 days: 3 - 18%
XXV. Brain Attack
A. TIA-warning sign=>Equate to USA
B. Silent CNS Infarction=>Equate to NSTEMI
1. Damage without sx
C. CVA-Damage with sx=>Equate to STEMI
S.A. Pulley, D.O., FACOEP
Acute Coronary Syndrome
PCOM-EM
Acute Coronary Syndrome
Cardiogenic Chest Pain
I.
II.
II.
III.
IV.
V.
VI.
VII.
VIII.
Objectives
a. To discuss the epidemiology, pathogenesis and risk factors
b. To identify symptoms and diagnostics
c. To establish priorities and treatments
Acute MI
A. Time wasted is heart muscle lost
B. TIME=MUSCLE
C. Muscle=Quality of Life (or ability to live)
Scope of Problem
A. 735K MIs annually
B. 47% die outside of hospital
C. Another 10-15% die within 12 months
D. 318+ Billion dollar disease
E. Approximately 600K annual cardiac deaths
1. ~370K are CAD related
Sudden Cardiac Death
A. ~424K cases annually for SCD
B. ~326K EMS cases annually for SCD
C. Only 1/3 of victims get CPR in the field
D. EMS intact save rate nationwide averages
a. Was 8%, Now up to 11%
b. 31% for witnessed VF/VT
Pathogenesis of AMI
A. Interaction of multiple factors
1. Progressive artherosclerotic process
2. Plaque fissuring and subintimal hemorrhage
3. Platelet aggregation at site of existing narrowing
B. Coronary artery spasm
C. Coronary artery embolism
D. Spontaneous Inflammation
Chest Pain
A. A patient presents to the Emergency Department with a complaint of chest pain
B. What do you do first?
Screening for AMI
A. Need a specific triage protocol
B. Should be placed immediately in a treatment area so they can...
C. Have a 12-lead ECG performed
ECG Patterns of AMI
A. Pattern of injury
1. ST elevation in only 50% of MIs
2. Nonspecific ST-T changes in about 25%
3. About 25% have normal ECGs
B. Old Myocardial infarction
C. Non Q-wave infarction
D. New BBB
Pattern of Injury
A. ST segment elevation (in 2 or more contiguous leads) leads
1. 2 mm in precordial leads
2. 1 mm in limb
B. New LBBB
S.A. Pulley, D.O., FACOEP
Acute Coronary Syndrome
PCOM-EM
IX.
X.
XI.
XII.
XIII.
XIV.
XV.
C. ECG Regions
1. II, III, F: Inferior wall
2. V1 - V2: Interventricular septum
3. V3 -V4: Anterior wall
4. I, L: High lateral wall
5. V5 - V6: Low lateral wall
6. R V3 - RV4: Right Ventricle
7. Mirror V1 - V2 or V9: Posterior Wall
Differential Diagnosis
A. Acute Coronary Syndrome***(Short term life threat)
B. Thoracic Aneurysm Dissection***(Short term life threat)
C. Pneumothorax***(Short term life threat if Tension)
D. Pulmonary Embolism***(Short term life threat)
E. Booerhaves***(Short term life threat)
F. Trauma
G. Pleurisy/Pneumonia
H. Pericarditis
I. GERD/Esophagitis
Risk Factors for AMI
A. Not Modifiable
1. Prior disease (MI, bypass, angioplasty), Family history, Age/Sex
B. Modifiable
1. Sedentary, Obesity, HTN, Smoking, Hyperlipidemia, DM
C. Other Modifiable
1. Stress, Poor nutrition, Excessive alcohol, Cocaine, Methamphetamine
Cardiogenic Chest Pain-Chest Discomfort
A. Pressure
B. Tightness
C. Heaviness
D. Squeezing
E. Bricks or elephant sitting on chest
F. Any discomfort from umbilicus to upper teeth, front or back, in the right patient, can be
considered cardiac related
G. The older the patient is, females, or the longer that the patient has had diabetes, the less
typical the symptoms tend to be
Cardiogenic Symptoms
A. Chest discomfort
B. Levine sign
C. Shortness of breath
D. Diaphoresis
E. Nausea/vomiting
F. Radiation
Public Awareness
A. 92% recognize chest pain as a symptoms of heart attack
B. Only 27% were aware of all the major symptoms and knew to call 9-1-1
C. With about 47% of people dying outside the hospital from cardiac arrest, it appears that most
do not heed the warning symptoms of heart attack
Atypical Symptoms
A. Any discomfort from umbilicus to upper teeth, front or back, in the right patient, can be
considered cardiac related
B. The older the patient is, females, or the longer that the patient has had diabetes, the less
typical the symptoms tend to be
Decision Process
A. More likely to have
1. Risk factors
2. Suspicious story (Symptoms) which is the most important factor
S.A. Pulley, D.O., FACOEP
Acute Coronary Syndrome
PCOM-EM
XVI.
XVII.
XVIII.
XIX.
XX.
XXI.
B. Less likely to have
1. Lack of risk factors
2. Atypical story
C. Always err towards the conservative side
Management of Cardiac Chest Pain
A. Oxygen: If pulse ox less than 94%
B. Aspirin: Chewable- 2-4 (162-324 mg)
C. Nitroglycerin: 0.4 mg SL q 5 min until relief or HA/BP intolerance
D. Opiates: e.g. Morphine/Hydromorphone
Diagnostics
A. ECG
B. VS monitoring/Rhythm monitoring/Pulse Ox, IV
C. CXR
D. Cardiac lab markers
Continuing Management of Cardiac Chest Pain
A. Acute MI (ST Elevation-STEMI)
1. Choose reperfusion strategy-FIRST
2. IV NTG
3. IV Beta Blockers
4. IV Heparin/SQ Enoxaprin
5. PO Clopidogrel
a. Normal 75 mg/day
b. Acutely 300-600 mg PO
B. NSTEMI (Non STEMI), USA, ACS
1. Same initial medications as STEMI
2. May add Glycoprotein IIb/IIa Inhibitor
3. Serial ECGs looking for STEMI conversion
C. Non-diagnostic ECG
1. Topical or IV NTG
2. ASA
3. Others as above if intermediate to high risk
4. On-going pain
a. Consider other causes (e.g. MSK or GERD)
1) Use caution as these can coexist with acute coronary syndrome
b. Urgent Catheterization
c. And/or Double/Triple rule-out CT Angiogram of Chest
C. Coronary Artery Reperfusion
1. PTCA/PCI
2. Emergent Bypass (CABG)
3. Thrombolytics
a. What do you think is the major determinant of the method chosen?
b. Location Location Location
Thrombolytics
A. Best within 4-6 hours
B. Door to needle time < 30 minutes
C. Need teamwork
D. Bleeding history
1. Stroke
2. Clotting abnormalities
3. Surgery
Emergent Cardiac Catheterization
A. PTCA
B. Possible Emergent CABG
Summary-ED Management of Acute MI
A. High index of suspicion
B. Immediate 12 lead ECG and regular repeats if normal
C. Know/Choose reperfusion strategy
3
You might also like
- ACLS NotesDocument9 pagesACLS Notestasha0% (1)
- ACLS Test BankDocument13 pagesACLS Test BankSofiaSheikh94% (51)
- Tips For PALS ExamDocument3 pagesTips For PALS ExamAy Men Alej91% (11)
- EKG and ECG Interpretation: Learn EKG Interpretation, Rhythms, and Arrhythmia Fast!From EverandEKG and ECG Interpretation: Learn EKG Interpretation, Rhythms, and Arrhythmia Fast!No ratings yet
- Torsade De Pointes, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandTorsade De Pointes, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- EKG | ECG Interpretation. Everything You Need to Know about 12-Lead ECG/EKG InterpretationFrom EverandEKG | ECG Interpretation. Everything You Need to Know about 12-Lead ECG/EKG InterpretationRating: 3 out of 5 stars3/5 (1)
- ECG & EKG Interpretation: How to interpret ECG & EKG, including rhythms, arrhythmias, and more!From EverandECG & EKG Interpretation: How to interpret ECG & EKG, including rhythms, arrhythmias, and more!No ratings yet
- The 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsFrom EverandThe 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsNo ratings yet
- ACLS Provider Manual 2015 NotesDocument5 pagesACLS Provider Manual 2015 Notescrystalshe93% (14)
- AHA ACLS Megacode ScenariosDocument6 pagesAHA ACLS Megacode ScenariosChad Sanford78% (18)
- Acls Study GuideDocument24 pagesAcls Study GuideMohammad Gita100% (17)
- ACLS Memory AidsDocument2 pagesACLS Memory Aidsmaur_jmp78% (9)
- ACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)Document11 pagesACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)김민길100% (2)
- ACLS Answer KeyDocument23 pagesACLS Answer KeyKirana Budhiarta94% (17)
- ACLS PrecourseAssessmentDocument19 pagesACLS PrecourseAssessmentBrigitte Elaine81% (21)
- ACLS Practice TestDocument5 pagesACLS Practice Testprettynpink0867% (3)
- Acls - Megacode - UpdatedDocument4 pagesAcls - Megacode - UpdatedDivine Dela Pena100% (1)
- ACLS PharmacologyDocument6 pagesACLS PharmacologyEunice Angela Fulgueras80% (5)
- ACLS Class Packet 2015Document9 pagesACLS Class Packet 2015Chi Wiin100% (3)
- ACLS - Precourse Questions and AnswersDocument18 pagesACLS - Precourse Questions and Answerssuperdockk58% (12)
- ACLS Exam ADocument8 pagesACLS Exam AAgil Rumboko Sumitro100% (3)
- ACLS Review TestDocument5 pagesACLS Review Testtostc60% (5)
- ACLS Test PrintscreenedDocument13 pagesACLS Test Printscreenedhellfireomega67% (9)
- ACLS 2020 Algorithms: American Heart Association 2020 GuidelinesDocument8 pagesACLS 2020 Algorithms: American Heart Association 2020 GuidelinesNofi Nurina100% (4)
- ACLS Cheat SheetDocument8 pagesACLS Cheat SheetLenTheRN85% (27)
- ACLS Precourse Test AnswersDocument60 pagesACLS Precourse Test AnswersTip Piraya60% (5)
- AclsDocument73 pagesAclsKamel Hady50% (2)
- Study Guide: MandatoryDocument24 pagesStudy Guide: Mandatorybooksir86% (7)
- ECG Rhythms and Pharmacology GuideDocument20 pagesECG Rhythms and Pharmacology Guidequeennita69100% (4)
- Acls Pre Course Self Assessment Study GuideDocument7 pagesAcls Pre Course Self Assessment Study Guidenova939100% (5)
- ACLS Practice Test 1Document6 pagesACLS Practice Test 1tarrynwortmann5319100% (3)
- ACLS ECGsDocument4 pagesACLS ECGsEman Elzeftawy100% (3)
- National CPR Association ACLS Study GuideDocument18 pagesNational CPR Association ACLS Study Guidekumar23No ratings yet
- ACLS Rhythms Cheat SheetDocument21 pagesACLS Rhythms Cheat SheetSisca MetasariNo ratings yet
- Soalan MCQ Acls Fit Set BDocument3 pagesSoalan MCQ Acls Fit Set BAnonymous 89ilBIGhrmNo ratings yet
- PALS Study GuideDocument25 pagesPALS Study GuideVitor Hugo G CorreiaNo ratings yet
- ACLS Post Test (Copy) 낱말 카드 - QuizletDocument18 pagesACLS Post Test (Copy) 낱말 카드 - Quizlet김민길No ratings yet
- PALS Pre StudyDocument28 pagesPALS Pre Studynursesed100% (7)
- PALS Helpful Hints 2015 Guidelines Posted Nov 2016Document5 pagesPALS Helpful Hints 2015 Guidelines Posted Nov 2016Mj Teate100% (1)
- AHA ACLS Megacode ScenariosDocument6 pagesAHA ACLS Megacode ScenariosVitor Hugo G Correia86% (7)
- ACLS Exam ADocument8 pagesACLS Exam ASean Johnson83% (30)
- ACLS Student GuideDocument28 pagesACLS Student GuideSamuel de Lima71% (7)
- ACLS Rhythms Cheat SheetDocument21 pagesACLS Rhythms Cheat SheetShannon Hagan Wilson100% (8)
- PALS Study Guide: 2020 GuidelinesDocument3 pagesPALS Study Guide: 2020 GuidelinesVictoria Kidd100% (2)
- American Heart Association Acls Post Test AnswersDocument4 pagesAmerican Heart Association Acls Post Test AnswersArun Jude Alphonse0% (9)
- ACLS PRE-TEST KEYDocument19 pagesACLS PRE-TEST KEYMohammed Abdou92% (13)
- ACLS Study Guide 2016: Essentials for Passing ExamDocument2 pagesACLS Study Guide 2016: Essentials for Passing Examnova939100% (2)
- ACLS DrugsDocument16 pagesACLS Drugstostc100% (1)
- ACLS Practice Test2Document6 pagesACLS Practice Test2Ronald Rey Menor100% (11)
- Acls Test: 1. Start CPR, Beginning With Chest CompressionsDocument15 pagesAcls Test: 1. Start CPR, Beginning With Chest CompressionsBoby Jomol100% (11)
- ACLS Megacode Testing ScenariosDocument12 pagesACLS Megacode Testing Scenariosealm10100% (2)
- ACLS Advanced Cardiovascular Life Support Provider Manual 2023From EverandACLS Advanced Cardiovascular Life Support Provider Manual 2023No ratings yet
- Advance Cardiac Life Support: Short, Sweet and to the PointFrom EverandAdvance Cardiac Life Support: Short, Sweet and to the PointRating: 3 out of 5 stars3/5 (2)
- Electrocardiography in Emergency, Acute, and Critical Care, 2nd EditionFrom EverandElectrocardiography in Emergency, Acute, and Critical Care, 2nd EditionRating: 5 out of 5 stars5/5 (1)
- Point-of-Care Ultrasound in Critical CareFrom EverandPoint-of-Care Ultrasound in Critical CareLuke FlowerNo ratings yet
- Pediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesFrom EverandPediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesRating: 5 out of 5 stars5/5 (2)
- Emergency Department Resuscitation of the Critically Ill, 2nd Edition: A Crash Course in Critical CareFrom EverandEmergency Department Resuscitation of the Critically Ill, 2nd Edition: A Crash Course in Critical CareNo ratings yet
- 3 Phases of Operating Room Technique: Preoperative Phase Intraoperative Phase Post Operative PhaseDocument76 pages3 Phases of Operating Room Technique: Preoperative Phase Intraoperative Phase Post Operative Phasejamaica cabriga100% (1)
- 0417RT CodingDocument5 pages0417RT CodingcmirceaNo ratings yet
- Causality assessment of single case reportsDocument11 pagesCausality assessment of single case reportsM LyaNo ratings yet
- @MedicalBooksStoreS 2017 Acute IschemicDocument273 pages@MedicalBooksStoreS 2017 Acute IschemicAditya Perdana Dharma Wiguna100% (1)
- Tobacco Reflection PaperDocument4 pagesTobacco Reflection Paperapi-356164412No ratings yet
- Tugas GinjalDocument22 pagesTugas GinjalAnastasia MargaretNo ratings yet
- CV Disease Drug StudyDocument11 pagesCV Disease Drug StudyMaria Francheska OsiNo ratings yet
- Remdesivir - Mechanism and Effectiveness For Coronavirus Disease 2019 (COVID-19)Document10 pagesRemdesivir - Mechanism and Effectiveness For Coronavirus Disease 2019 (COVID-19)RizkiOktasariNo ratings yet
- Sports Massage Therapist - Sports Injury ChiropractorDocument3 pagesSports Massage Therapist - Sports Injury ChiropractorDr. Dale MacdonaldNo ratings yet
- Upper Respiratory Infection Definition and FactsDocument2 pagesUpper Respiratory Infection Definition and FactsBerlian PurnamasariNo ratings yet
- DDX Mata Tenang Dengan Visus Turun PerlahanDocument15 pagesDDX Mata Tenang Dengan Visus Turun PerlahanRhinRinNo ratings yet
- Puberty and The HPG AxisDocument36 pagesPuberty and The HPG AxiskjhkaNo ratings yet
- 2022 - CCR8 Treg Cells in Tumor Tissues With Long-Lasting MemoryDocument12 pages2022 - CCR8 Treg Cells in Tumor Tissues With Long-Lasting Memory1262615286No ratings yet
- Guidelines Malaria Di MalaysiaDocument61 pagesGuidelines Malaria Di MalaysianalmifaNo ratings yet
- Lindo Wing Brochure Web VersionDocument16 pagesLindo Wing Brochure Web VersionNetwerk24No ratings yet
- Expression of Vascular Endothelial Growth Factor (VEGF) and New Blood Vessels Formation On Wound Incision Post Ropivacaine Administration in Animal ModelDocument8 pagesExpression of Vascular Endothelial Growth Factor (VEGF) and New Blood Vessels Formation On Wound Incision Post Ropivacaine Administration in Animal ModelInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- 7th Lecture Physics of Cardiovascular System1Document12 pages7th Lecture Physics of Cardiovascular System1Asfoor gake1No ratings yet
- Activated Charcoal OverviewDocument3 pagesActivated Charcoal OverviewCarlos Laureano Martinez FloresNo ratings yet
- Propaira - NCI Apr 2012 FINAL v1.0Document2 pagesPropaira - NCI Apr 2012 FINAL v1.0Mustafa TurabiNo ratings yet
- Neonatal Tetanus SurveillanceDocument14 pagesNeonatal Tetanus SurveillanceNadiah Husnul KhotimahNo ratings yet
- No. Kode Barang Nama Barang Exp. Date StockDocument12 pagesNo. Kode Barang Nama Barang Exp. Date StocknafilaNo ratings yet
- 50 Prometric MCQ For GPDocument10 pages50 Prometric MCQ For GPDrkhslid8971% (7)
- Case Studies - MIC3002Document28 pagesCase Studies - MIC300217206404 STUDENTNo ratings yet
- Evidence-Based Medicine: David L. SackettDocument3 pagesEvidence-Based Medicine: David L. SackettNicolas MarinNo ratings yet
- Kaolin - Pectin v2 FINALDocument2 pagesKaolin - Pectin v2 FINALAFNo ratings yet
- Nursing Care Plan Guide for Holistic Patient CareDocument23 pagesNursing Care Plan Guide for Holistic Patient CareRej PanganibanNo ratings yet
- Febrile Seizure CPGDocument7 pagesFebrile Seizure CPGLM N/ANo ratings yet
- Ectopia LentisDocument38 pagesEctopia LentisSaransh Sharma100% (1)
- NicuuuuDocument17 pagesNicuuuuJyoti Prem UttamNo ratings yet
- Second MBBS Microbiology SyllabusDocument29 pagesSecond MBBS Microbiology SyllabusUday KolheNo ratings yet