Professional Documents
Culture Documents
Neonatal Cardiac Arrhythmias: Intensive Care Nursery House Staff Manual
Uploaded by
Kranti PrajapatiOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Neonatal Cardiac Arrhythmias: Intensive Care Nursery House Staff Manual
Uploaded by
Kranti PrajapatiCopyright:
Available Formats
Intensive Care Nursery House Staff Manual
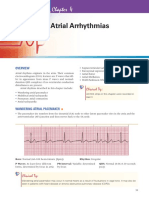
Neonatal Cardiac Arrhythmias
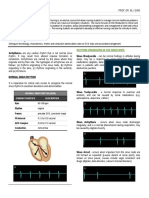
INTRODUCTION: Identification and treatment of arrhythmias in newborns is challenging and differs from older children, and the natural history of arrhythmias presenting in the neonatal period is often dramatically different. METHODS OF DIAGNOSIS AND THERAPY: For management of arrhythmias, consult Cardiology team. 1. Diagnostic methods: 15 lead electrocardiogram (standard 12 lead plus V3R, V4R, V7) Heart rate determination (ECG strip, count number of QRS complexes in 6 sec x 10) Blood pressure (intra-arterial or indirect) 2. Treatment: Electrical (See below for drug therapy) Artificial pacing : -Temporary transvenous pacing -Esophageal pacing Cardioversion: -Setting: 0.5 - 2.0 Joules/kg -Mode: synchronous for narrow QRS; asynchronous for ventricular fibrillation IMMEDIATE MANAGEMENT OF ARRHYTHMIAS: Tachyarrhythmia narrow-QRS wide-QRS Bradyarrhythmia
stable vagal maneuvers adenosine, propranolol or digoxin
unstable synchronized cardioversion
stable Procainamide, lidocaine in VT
unstable synchronized cardioversion no response asynchronous mode
unstable A B C*, O2, atropine & isoproterenol, temporary transvenous pacing
*A B C, airway, breathing, circulation
105
Copyright 2004 The Regents of the University of California
Neonatal Cardiac Arrhythmias
A. Tachy-arrhythmias with narrow QRS: I. Diagnosis
Atrial flutter
Reentry tachycardias Findings on ECG
-"Sawtooth" flutter waves -AV block does not terminate atrial rhythm -Atrial rate up to 500 in newborns -Variable AV conduction common -P follows QRS, typically on upstroke of T -Superior or rightward P wave axis -AV block always terminates tachycardia -Typically terminates with P wave -After termination, WPW have pre-excitation -Incessant - P wave precedes QRS -Inverted P waves in II, III, AVF -AV block always terminates tachycardia -May terminate with QRS or P wave -No pre-excitation after termination -P usually not visible, superimposed on QRS -AV block usually terminates tachycardia.
Treatment
-Unstable: esophageal pacing or electrical cardioversion -Stable: digoxin, propranolol, or digoxin + procainamide
Accessory pathway mediated tachycardia (WPW)
-Unstable: esophageal pacing or electrical cardioversion -Stable: vagal maneuvers. adenosine propranolol or digoxin -No response: procainamide or flecainide
Permanent form of junctional reciprocating tachycardia (PJRT)
Atrioventricular node reentry
Atrial and sinoatrial reentry
-P present, precedes next QRS -Terminates with QRS rather than P -AV block does not terminate atrial rhythm -P axis may be superior or inferior -"Irregularly irregular" -No two RR intervals exactly the same -P waves difficult to see, bizarre and chaotic
-Unstable: electrical cardioversion -Stable: propranolol, procainamide or amiodarone -Unstable: electrical cardioversion -Stable: digoxin + procainamide
Atrial fibrillation
II. Increased automaticity
Sinus tachycardia -Normal P wave axis -P waves precede QRS -Due to extrinsic factor such as heart failure, fever, anemia, catecholamines, theophylline -Incessant -Abnormal P axis which predicts location of focus -P wave precedes QRS -Continues in presence of AV block -Incessant -Usually with atrio-ventricular dissociation and slower atrial than ventricular rate. -Capture beats with no fusion. -Treat causative extrinsic factor
Atrial ectopic tachycardia
-Unstable: IV amiodarone -Stable: propranolol, sotalol or amiodarone, or digoxin + procainamide. -Unstable: cooling, IV amiodarone -Stable: propranolol, sotalol or amiodarone
Junctional ectopic tachycardia
106
Copyright 2004 The Regents of the University of California
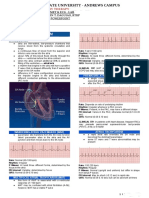
Neonatal Cardiac Arrhythmias
B. Tachy-arrhythmias with wide QRS: Diagnosis
Ventricular tachycardia (VT)
Findings on ECG
-Often with AV dissociation -Capture beats with narrower QRS than other beats; fusion beats -Complete chaotic rhythm -Rapid and irregular rhythm
Treatment
-Unstable: electrical cardioversion -Stable: lidocaine, procainamide
Ventricular fibrillation
SVT with pre-existing bundle branch block
Antidromic SVT in WPW
-QRS morphology similar to that in sinus rhythm -QRS morphology is that of right or left bundle branch block -QRS morphology similar to pre-excited sinus rhythm, but wider -Never with AV dissociation
(1) asynchronous cardioversion 2j/kg (2) asynchronouss cardioversion 2j/kg (3)asynchronous cardioversion 4j/kg (4)lidocaine + asynch. cardioversion. -Unstable: esophageal pacing or electrical cardioversion -Stable: vagal maneuvers, adenosine, propranolol or digoxin -No response: procainamide or flecainide
C. Bradyarrhythmias: Diagnosis
Sinus bradycardia
Findings on ECG
Treatment
-Vigorous resuscitation and supportive care -A B C -O2 -Treat underlying causes -Unstable: A B C O2 Atropine, isoproterenol infusion Temporary transvenous pacing -Stable: Treat underlying causes -Permanent pacemaker in AV block with ventricular rate < 55 (newborn)
-Slow atrial rate with normal P waves -1:1 conduction -Due to underlying causes such as hypoxia, acidosis, increased intracranial pressure, abdominal distension, hypoglycemia, hypothermia, digoxin, propranolol Atrioventricular block -Atrioventricular dissociation -Regular R-R intervals Complete atrioventricular block -Regular P-P intervals -Atrial rate > ventricular rate -P which occur after T have no effect on R-R interval -Infants of maternal lupus 2nd degree atrioventricular block - Mobitz type I (Wenckebach) -Progressive PR interval prolongation followed by a blocked beat -Usually indicates block in the AV node - Mobitz type II - No characteristic PR prolongation as seen in type I. - Usually not reversible with medications. - Type II has worse prognosis than type I. - Sinus P waves intermittently disappear due to block of impulses leaving the node. -Premature P wave superimposed on the previous T wave, deforming it
Sinus exit block Premature atrial contractions
-Usually does not need treatment.
107
Copyright 2004 The Regents of the University of California
You might also like
- Neonatal Cardiac Arrhythmias: Intensive Care Nursery House Staff ManualDocument3 pagesNeonatal Cardiac Arrhythmias: Intensive Care Nursery House Staff ManualAhmed MohammedNo ratings yet
- Heart Dysrhythmias Cheat Sheet ExplainedDocument5 pagesHeart Dysrhythmias Cheat Sheet ExplainedpcmundotNo ratings yet
- Nclex RN Review Notes 2018 Triple eDocument30 pagesNclex RN Review Notes 2018 Triple eEndla SriniNo ratings yet
- NCM 112 MSN Prelim Topic 4 Cardiac Rhythm DisordersDocument5 pagesNCM 112 MSN Prelim Topic 4 Cardiac Rhythm DisordersKim Erida QuezonNo ratings yet
- Bradycardia and TachycardiaDocument66 pagesBradycardia and TachycardiaKarissaNo ratings yet
- Ecg Dysrythmias Nursing Responsibilitu Sinus Node 1.) Sinus BradycardiaDocument2 pagesEcg Dysrythmias Nursing Responsibilitu Sinus Node 1.) Sinus BradycardiaNickha LazoNo ratings yet
- This Study Resource Was Shared Via: Sinus BradycardiaDocument3 pagesThis Study Resource Was Shared Via: Sinus BradycardiaPascal St Peter NwaorguNo ratings yet
- Atrial Arrhythmias Definition and Pathology Significance Etiology Clinical Manifestations InterventionDocument5 pagesAtrial Arrhythmias Definition and Pathology Significance Etiology Clinical Manifestations Interventionmakyofrancis20No ratings yet
- Cardiac Arrhythmias Guide: Tachycardias and Supraventricular RhythmsDocument83 pagesCardiac Arrhythmias Guide: Tachycardias and Supraventricular Rhythmsmargareth hoyan SilabanNo ratings yet
- Cardiac Dysrhythmia Chart Med Surg NUR4 PDFDocument3 pagesCardiac Dysrhythmia Chart Med Surg NUR4 PDFlml100% (1)
- NCM 118 - Lesson 11 (Arrhythmia)Document5 pagesNCM 118 - Lesson 11 (Arrhythmia)Bobby Christian DuronNo ratings yet
- 40 - Arrythmias (PICU COURSE)Document44 pages40 - Arrythmias (PICU COURSE)surasuarezlopezNo ratings yet
- Workshop Pit IV THN 2017Document57 pagesWorkshop Pit IV THN 2017anettepardedeNo ratings yet
- Arrhythmia: CausesDocument21 pagesArrhythmia: CausesDagmawit GirmaNo ratings yet
- The ECG Made Easy by John R. HamptonDocument1 pageThe ECG Made Easy by John R. HamptonLpNo ratings yet
- ELECTROCARDIOGRAM by Aldrin Jayson AlmadenDocument23 pagesELECTROCARDIOGRAM by Aldrin Jayson AlmadenItsMe AJNo ratings yet
- Understanding Tachycardia and Bradycardia ClassificationsDocument18 pagesUnderstanding Tachycardia and Bradycardia ClassificationsZega AgustianNo ratings yet
- Drugs used to treat cardiac arrhythmiasDocument74 pagesDrugs used to treat cardiac arrhythmiasGunel Sadiqova100% (1)
- Cardiac Life Support Cme Latest Edited VersionDocument53 pagesCardiac Life Support Cme Latest Edited VersionSyed Shahrul Naz SyedNo ratings yet
- Cardiac Life Support Cme Latest Edited VersionDocument53 pagesCardiac Life Support Cme Latest Edited VersionSyed Shahrul Naz SyedNo ratings yet
- Arrhythmias: BY Zarish FazilDocument64 pagesArrhythmias: BY Zarish FazilZarish Amanat100% (1)
- Cardiology-5 DysrhythmiaDocument16 pagesCardiology-5 DysrhythmiaMahmoud RamadanNo ratings yet
- ACLS For TachycardiaDocument31 pagesACLS For TachycardiaTausif HaqueNo ratings yet
- EKG Arrhythmia Identification and Treatment GuideDocument28 pagesEKG Arrhythmia Identification and Treatment GuideJason LinNo ratings yet
- ECG Mastery Improving Your ECG Interpretation SkillsDocument23 pagesECG Mastery Improving Your ECG Interpretation SkillsHitesh Deora100% (2)
- 3881 - Prosedur Pendaftaran Internship Per November 2016Document57 pages3881 - Prosedur Pendaftaran Internship Per November 2016Munawir_Syam91No ratings yet
- Cardiology Notes USMLE Step CKDocument135 pagesCardiology Notes USMLE Step CKArianna BetancourtNo ratings yet
- Sinus Rhythm and Sinus and Atrial DysrhythmiasDocument41 pagesSinus Rhythm and Sinus and Atrial Dysrhythmiasclaudia brongNo ratings yet
- Electrocardiogram Interpretation and Nursing InterDocument4 pagesElectrocardiogram Interpretation and Nursing InterJulia Rae Delos SantosNo ratings yet
- Curs 7 - Bradiaritmii TahiaritmiiDocument88 pagesCurs 7 - Bradiaritmii Tahiaritmiijhonny12321No ratings yet
- Ecg Arrhythmia: Dr. Lowry Yunita, SPJP, FihaDocument48 pagesEcg Arrhythmia: Dr. Lowry Yunita, SPJP, FihaMaria JozilynNo ratings yet
- NCM 118Document8 pagesNCM 118Zanie CruzNo ratings yet
- Atrioventricular Nodal Reentry Tachycardia (AVNRT)Document24 pagesAtrioventricular Nodal Reentry Tachycardia (AVNRT)Radya Agna100% (1)
- Width of The QRS Complex: - Wide VT, SVT With Aberrant Conduction - Narrrow SVTDocument11 pagesWidth of The QRS Complex: - Wide VT, SVT With Aberrant Conduction - Narrrow SVTWidelmark FarrelNo ratings yet
- DYSRHYTHMIASDocument9 pagesDYSRHYTHMIASgudobenNo ratings yet
- Antiarrhythmic Agents Lecture NotesDocument6 pagesAntiarrhythmic Agents Lecture NotesErnest Patrick MatiasNo ratings yet
- Arrythmias and EKGs 2Document20 pagesArrythmias and EKGs 2Nur Ima ErvianaNo ratings yet
- Basic EKG ECG Rhythms CheatsheetDocument1 pageBasic EKG ECG Rhythms CheatsheetAhmad83% (6)
- 26) Approach To Pediatric ArrhythmiasDocument44 pages26) Approach To Pediatric ArrhythmiasJude AlyousefNo ratings yet
- Arrhythmias: Sing Khien Tiong Gpst1Document34 pagesArrhythmias: Sing Khien Tiong Gpst1preethi preethaNo ratings yet
- W2 Emergency ECG (DR Refli)Document47 pagesW2 Emergency ECG (DR Refli)indahflsaragihNo ratings yet
- Atria Arrythmia TestDocument8 pagesAtria Arrythmia TestAnnette SandovalNo ratings yet
- CardiologyDocument149 pagesCardiologyMuhammad SyafiqNo ratings yet
- Approach To ArrhythmiasDocument1 pageApproach To ArrhythmiasADITYA SARANGINo ratings yet
- Unit Learning Outcome: Course MapDocument3 pagesUnit Learning Outcome: Course MapBunnie AlphaNo ratings yet
- Atrial-Rhythm 230518 191520-1Document2 pagesAtrial-Rhythm 230518 191520-1Maxinne GorospeNo ratings yet
- TACHYARRHYTMIASDocument40 pagesTACHYARRHYTMIASRoy Sandy PermanaNo ratings yet
- MCEM B CVS TachycardiaDocument12 pagesMCEM B CVS TachycardiaRajin MaahiNo ratings yet
- How To: Read ECG?Document63 pagesHow To: Read ECG?Let BNo ratings yet
- Peri Operative Arryhthmias: Dr. Juzny Alkatiri, SPPD, SPJPDocument102 pagesPeri Operative Arryhthmias: Dr. Juzny Alkatiri, SPPD, SPJPAstari Pratiwi NuhrintamaNo ratings yet
- Arrhythmia Types and Features Cheat SheetDocument2 pagesArrhythmia Types and Features Cheat SheetNur Fatima SanaaniNo ratings yet
- Diagnosis Dan Tatalaksana Awal SVTDocument47 pagesDiagnosis Dan Tatalaksana Awal SVTZuly Vita AulyaNo ratings yet
- Detect VT vs SVT with Wide QRSDocument1 pageDetect VT vs SVT with Wide QRSLwin Maung Maung ThikeNo ratings yet
- Quick Ekg ReferenceDocument23 pagesQuick Ekg Referencekowaikowar100% (1)
- EKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookFrom EverandEKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookNo ratings yet
- Syncope CasesFrom EverandSyncope CasesRoberto García-CiveraNo ratings yet
- Microsoft Word - CC2046 EWC Health Reflection GuidelineDocument2 pagesMicrosoft Word - CC2046 EWC Health Reflection GuidelinegalaxytwyNo ratings yet
- Transport in MammalsDocument109 pagesTransport in Mammalsgalaxytwy100% (1)
- II. Mechanisms For ArrhythmiasDocument29 pagesII. Mechanisms For ArrhythmiasgalaxytwyNo ratings yet
- HRC2009, Birmingham, October 20th 2009Document48 pagesHRC2009, Birmingham, October 20th 2009galaxytwyNo ratings yet
- .Noitamrofni Erom Rof 0059-404-008 Ta ERAC LlacDocument2 pages.Noitamrofni Erom Rof 0059-404-008 Ta ERAC LlacgalaxytwyNo ratings yet
- Ventricular ArrhythmiasDocument6 pagesVentricular ArrhythmiasgalaxytwyNo ratings yet
- Ventricular ArrhythmiasDocument6 pagesVentricular ArrhythmiasgalaxytwyNo ratings yet
- TalkingwomenDocument1 pageTalkingwomengalaxytwyNo ratings yet
- Plan 1Document11 pagesPlan 1galaxytwyNo ratings yet