Professional Documents
Culture Documents
Meeting ED Quality Indicators with Simplified Patient Assessments
Uploaded by
Mareeze Hatta0 ratings0% found this document useful (0 votes)
50 views8 pagesThe document describes changes made to the triage process at Medway NHS Foundation Trust emergency department in the UK. Problems had arisen with the previous triage system, including long wait times for initial assessment and difficulty meeting new quality targets for ambulance patients. The senior nursing team developed a new "navigation" system to simplify initial patient assessment. Under navigation, nurses conduct initial assessments and streaming of patients rather than relying primarily on the computer-based Manchester Triage System. The goal is to prioritize direct patient care over administrative tasks and better identify patients needing immediate treatment.
Original Description:
Navigating Triage to Meet
Original Title
Navigating Triage to Meet
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document describes changes made to the triage process at Medway NHS Foundation Trust emergency department in the UK. Problems had arisen with the previous triage system, including long wait times for initial assessment and difficulty meeting new quality targets for ambulance patients. The senior nursing team developed a new "navigation" system to simplify initial patient assessment. Under navigation, nurses conduct initial assessments and streaming of patients rather than relying primarily on the computer-based Manchester Triage System. The goal is to prioritize direct patient care over administrative tasks and better identify patients needing immediate treatment.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
50 views8 pagesMeeting ED Quality Indicators with Simplified Patient Assessments
Uploaded by
Mareeze HattaThe document describes changes made to the triage process at Medway NHS Foundation Trust emergency department in the UK. Problems had arisen with the previous triage system, including long wait times for initial assessment and difficulty meeting new quality targets for ambulance patients. The senior nursing team developed a new "navigation" system to simplify initial patient assessment. Under navigation, nurses conduct initial assessments and streaming of patients rather than relying primarily on the computer-based Manchester Triage System. The goal is to prioritize direct patient care over administrative tasks and better identify patients needing immediate treatment.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 8
June 2013 | Volume 21 | Number 3 EMERGENCY NURSE 20
Art & science | patient assessment
Until two years ago the main performance
measure for emergency departments (EDs) in
England was the four-hour waiting time target,
which required that 98 per cent of patients were
discharged or admitted in less than four hours.
in April 2011, however, as part of the nHS outcomes
Framework (Department of Health (DH) 2010),
this standard was replaced by a new set of clinical
indicators to measure the quality of care.
two of these indicators state that, for patients
who arrive at EDs by ambulance, the time to initial
assessment must be less than 15 minutes and
the time to initial treatment must be less than
60 minutes. these requirements affect how EDs
receive patients and begin their treatments.
All patients seeking emergency care are triaged so
that those with the most urgent or life threatening
conditions can be identified. the most widely used
triage tool in the UK is the Manchester triage System
(MtS) (Mackway-Jones et al 2008), which Cooke et al
(2000) found was being used by 75 per cent of UK
ED staff. over the next decade, this figure rose to
96 per cent (newell and Smith 2008).
the MtS is based on an algorithm comprising
52 flow charts that refer to patients presenting
complaints. in each flow chart there are
six key discriminators:
life-threatening.
Haemorrhage.
Pain.
Consciousness level.
temperature.
Acuity of condition.
After choosing a discriminator, triage nurses assess
the urgency with which patients should be treated.
treatments assessed to be immediate, urgent
or routine are allocated the colour categories red,
amber or yellow, or green respectively (Ganley
and Gloster 2011).
Medway nHS Foundation trust ED introduced the
MtS for initial assessment of all patients in 1997.
over the next seven years, attendance figures at
the ED increased by about 5,000 a year. Staff were
spending more and more time assessing routine
category patients, which was delaying identification
of patients with life-threatening conditions.
in 2004, therefore, a see and treat, or streaming,
system was introduced to allow staff to identify
patients with minor conditions when they arrive
and direct them away from the triage queue. A list
of conditions suitable for streaming was drawn up
to enable reception staff to register these patients
automatically before they were directed to the
minor injuries area.
Despite this development, however, problems
with the use of MtS persisted. triage involved the
categorisation of patients on a computer system
before their conditions had been assessed, for
example, which meant that their registration took
priority over care.
Inmaculada Diaz Alonso explains how the triage process
at her emergency department was replaced by a simpler
system in which nurses undertake initial assessments
navigating triage to meet
targets for waiting times
Correspondence
i.diaz-alonso@nhs.net
Inmaculada Diaz Alonso is clinical
nurse lead in the emergency
department at Medway
NHS Foundation Trust, Kent
Date of submission
January 22 2013
Date of acceptance
April 15 2013
Peer review
This article has been subject
to double-blind review and
has been checked using
antiplagiarism software
Author guidelines
www.emergencynurse.co.uk
Abstract
An initial assessment process, called navigation,
has been introduced at Medway Maritime Hospital
emergency department (ED) to address problems
with the triage system and to meet the latest ED
quality clinical indicators. This article explains
the rationale for introducing the new assessment
process, describes the system and discusses the
change-management process needed to implement it.
Keywords
Navigation, initial assessment, triage, streaming
EN Jun 2013 20-26 asIDA1145.indd 20 03/06/2013 17:25
EMERGENCY NURSE June 2013 | Volume 21 | Number 3 21
Art & science | patient assessment
Up to 25 patients an hour registered in the
ED, with computer triage taking a minimum of
15 minutes to complete for each of them. triage
nurses had to deal with a constant stream of self-
presenting patients or patients brought in by
ambulance and found it difficult to keep on top of
the workload at peak times.
this resulted in long queues and lengthy waiting
times for initial assessment at busy periods, and
triage nurses struggled to identify ill patients on
their arrival because they had to spend so much
time in front of the computer, trying to clear the
backlog of patients.
there was often a conflict between the need to
fulfil triage categories and the requirement to meet
the four-hour waiting times target, and a balance
had to be struck between attending to patients
with higher triage categories who had recently
arrived and those with lower categories who had
been waiting longer.
Contrary to the relevant national institute for
Health and Care Excellence (2012) guidelines, many
patients had to wait more than 30 minutes to be
seen by nurses. As a result, compliance with the nHS
outcomes Frameworks (DH 2010) quality indicators
for initial assessment became almost impossible.
Against this background, and in anticipation of
the imminent introduction of new quality indicators,
the senior nursing team in the trusts ED analysed
normal triage practice to try to identify how the
system could be improved. they also drew diagrams
of the emergency care journeys made by patients
who self-present and those who arrive by ambulance
to highlight flaws in the system.
Most self-presenting patients registered at
reception and waited for triage, although those with
minor injuries were streamed to the minor injuries
unit by receptionists according to the inclusion
criteria list. this meant that administrative staff
were making clinical decisions about some patients
and analysis showed that the receptionists did not
always indicate whether the patients conditions
required immediate, urgent or routine treatment.
Because self-presenting patients had to wait to
register and wait again for triage, they were unlikely
to be seen by a nurse for at least 30 minutes. triage
itself was a lengthy and time-consuming process
because it had to be undertaken on a computer
regardless of each patients condition.
Even people who had been registered in error,
or who required simple advice, had to be triaged
so that they could be directed to the appropriate
area. At the same time, triage nurses were expected
to carry out tasks such as electrocardiography and
urine analysis.
the senior nursing team also found that, due to
a lack of documentation about initial interventions
in the ED, many triage nurses thought they could
not, for example, give patients analgesia until they
had been registered on the system.
when patients arrived by ambulance the nurse
in charge of the ED was expected to undertake full
handovers with ambulance staff before making
initial assessments. the nurses in charge of the
ED are band 6 or 7, and have sufficient knowledge
and autonomy to make initial assessments and
initiate some treatments. in practice, however, full
handovers rarely took place, and the patients had to
wait for triage and initial treatments to be carried
out by other, more junior staff.
Patients were then allocated trolley spaces or
taken to the waiting room, where they waited to be
registered on the computer system, and were then
triaged by either the nurse responsible for the trolley
spaces or the triage nurse in the waiting room.
the senior nursing team analysing the system
concluded that computer triage was little more
than an administrative exercise. Decision making
should include cognitive, intuitive and experiential
processes (Pugh 2002) but, instead of drawing on
their experience and intuition to assign patients to
triage categories, many nursing staff were assigning
new categories to the patients.
triage was most often effective when it was
undertaken by senior nurses, who have the
necessary clinical skills and knowledge.
Navigation
the senior nursing team realised that nurses need
tools such as the MtS to help them make safe
and effective initial assessments, and they need
computers to process the information they are given
and to assign patients priority codes.
the team concluded, therefore, that the cause of
problems in the ED was the way the MtS was being
used, rather than the system itself, and that the ED
triage process should be simplified and prioritise
patient care.
the senior nursing team worked with other
senior staff to develop an initial-assessment
system that would involve fewer steps than are
required by the MtS and in which nurses, rather
than non-clinical staff, would identify patients who
require immediate management or who should be
streamed to other areas.
initially, the team approached the intensive
Support team (iSt), part of the nHS interim
Management and Support (iMS) service, which
helps nHS organisations change clinical processes
(nHS iMS 2011).
EN Jun 2013 20-26 asIDA1145.indd 21 03/06/2013 17:25
June 2013 | Volume 21 | Number 3 EMERGENCY NURSE 22
Art & science | patient assessment
the iSts main recommendation was to introduce
streaming of patients on their initial assessments in
the ED. the team then studied how other hospitals
in Kent assessed ED patients on their arrival and
found some had piloted streaming systems for a
few months but had returned to triage. only one
hospital had continued to stream patients but had
also adopted a computer-based triage system. Rather
than streamlining the triage process, therefore, the
hospital had added an extra step.
the steps involved in the MtS are shown in
Figure 1 and those involved in the new system,
called navigation, are shown in Figure 2. As these
algorithms show, the introduction of navigation
has reduced the number of steps required before
patients are seen by decision-making clinicians,
which has ensured in turn that people with
life-threatening conditions can be identified earlier.
in the navigation system, patients who present
to the ED are assessed by a senior nurse, called
a navigating nurse, before they are registered.
this practice ensures that lower category patients
are streamed by senior clinicians rather than non-clinical staff, and that people with serious
conditions can be identified as soon as they
arrive at the ED.
navigating nurses have the competencies
to treat pain by prescribing and administering
analgesia, and to order investigations as soon as
patients arrive.
in each case, navigating nurses record the results
of their assessments, including basic observations
and descriptions of the pathway each patient should
follow, on navigating forms. the navigating form
used at Medway Maritime Hospital ED has been
adapted for Figure 3.
the navigating forms are then passed to
reception staff, who register the patients and direct
them to the appropriate areas. they also scan and
save the forms in the relevant patients electronic
records so that details of the patients care pathways
are available instantly to clinicians who work in all
areas of the ED.
Some patients follow pathways that involve
specific investigations, which must be carried out
before decisions about the patients care can be
made. these investigations are made by another
healthcare professional, called a navigating
assistant, according to the principles of the MtS.
the navigating assistant role is, as far as the authors
know, unique to the trust.
Managing change
implementation of the navigation system required
a change in practice and culture at the trust,
and its success depended on careful planning
Figure 1 Steps involved in the Manchester Triage
System
Patient arrives by ambulance
Handover to nurse in charge
Patient allocated to waiting room or trolley space
Patient registration
Triage and prioritisation of care
Further investigations
Final relocation
Patient is seen by a clinician
Figure 2 Steps involved in navigation
Patient arrives by ambulance
Handover to nurse in charge. Prioritisation of
care according to patients clinical condition and
observations made during handover
Patient allocated to waiting room or trolley space
Further investigations
Patient is seen by a clinician
EN Jun 2013 20-26 asIDA1145.indd 22 03/06/2013 17:25
EMERGENCY NURSE June 2013 | Volume 21 | Number 3 23
Art & science | patient assessment
Figure 3 Medway NHS Foundation Trust emergency department navigating form
Date .......................................................... Time ......................................................... Crew .......................................................
Name ......................................................... Date of birth ................................................ Navigator ..................................................
Navigator or ambulance handover details
Ambulance observations
Blood pressure Temperature Electrocardiography given? Yes No
Heart rate Body mass index Cannula given? Yes No
Respiratory rate Pupil size Pain score
/10
Blood oxygen saturation Glasgow Coma Scale score
Medications and fluids given Time they were given
Navigator instructions
For navigation assistant? Yes No
Observations: have these been made? Bloods: have these been undertaken or assessed?
General observations Yes No Cannula Yes No Troponin I levels Yes No
Neurological observations Yes No Full blood count Yes No Paracetamol and salicylate Yes No
Electrocardiography result Yes No Urea and electrolyte test Yes No Beta HCG level Yes No
Ketone level Yes No International normalised ratio Yes No Progesterone Yes No
Body mass index Yes No Clotting Yes No Other tests
Urinalysis result Yes No Amylase level Yes No
Human chorionic gonadotropin
(HCG)
Yes No C-reactive protein level Yes No
X-ray result Yes No Liver function Yes No
Weight Yes No Glucose level Yes No
Treatment location
Priority number Ambulance overflow Emergency triage unit
trolley number
Trolley number GP majors Paediatric navigator
Resuscitation number See and treat Paediatric trolley
Majors waiting room GP minors Paediatric see and treat
Pain score Drug Dosage Route Signature Given by Time
EN Jun 2013 20-26 asIDA1145.indd 23 03/06/2013 17:25
June 2013 | Volume 21 | Number 3 EMERGENCY NURSE 24
Art & science | patient assessment
and management of change. to guide the
change-management process, the senior nursing
team adopted Kotters (1995) eight-step change
model. these steps involve:
1. Establishing a sense of urgency.
2. Forming a guiding coalition.
3. Creating a vision.
4. Communicating the vision.
5. Empowering others to act on the vision.
6. Planning for and creating short-term wins.
7. Consolidating improvements and creating
more change.
8. institutionalising new approaches.
Establishing a sense of urgency this was
provided by the introduction of new clinical quality
indicators, as a result of which a new triage process
had to be completed within three months.
Forming a guiding coalition After the senior
nursing team had analysed the current triage
process, it presented its findings to senior ED sisters
and explained why it should be streamlined. the
team drew on advice from the iSt and senior ED
sisters, and its observations of triage processes
at other sites, to develop the navigation system.
By involving senior sisters at this early stage,
Table 1 Most common staff questions and responses to them
Question Response
How do very ill patients
get flagged up in the
system?
New locations have been created in the computer system for flagging up patients
for clinicians. When patients are registered, there is an option to place them in
a location, such as trolley 1, or in a priority location, such as priority trolley 1.
The patients remain in the same place but the change in the name of their locations
alerts clinicians to the higher priority of their care.
What happens when
there is no capacity for
patients who need to be
monitored?
This problem would be familiar to most emergency departments, regardless of the
type of initial assessment they use, and it should be discussed separately because
it does not form part of the navigation process. However, it is better to know that
patients require monitoring straight away rather than to find this out at triage,
when they will have been in the department for a while.
How do you record details
of patient assessments?
The navigating form is used for every patient and is scanned onto their electronic
records. The navigating room is next to the reception and, as soon as the navigating
nurses have completed their assessments, they put the forms in a tray to be collected
by reception staff, who then enter the details on the computer system. Details on the
form are entered on to the computer retrospectively and the time of initial assessment
by the navigating nurse is recorded as time of arrival.
Does recording the time
of assessment as time
of arrival constitute a
falsifying of records, given
the delay between them?
The delay between times of arrival and assessment is not taken into account because
assessment occurs almost as soon as patients arrive at the department.
What happens when there
is a queue for assessment?
Will patients wait longer?
Before navigation was implemented, patients queued to register at reception and
then for triage, so one queue has been eliminated. We know how many patients
are waiting for navigation because there is a marked off area in the waiting room
in which they can be counted easily. If there are more than five patients waiting for
assessment, the navigating nurse alerts the nurse in charge, who assigns another
navigating nurse.
What happens if patients
need further investigations
before clinical decisions
can be made?
If patients conditions are thought to be life threatening, they are taken immediately
to a monitored bay. If they need full observations or diagnostic tests, they will be seen
by the navigating assistant, who can undertake on-the-spot, vital observations and
make quick decisions, for example to refer patients to GPs or discharge them.
EN Jun 2013 20-26 asIDA1145.indd 24 03/06/2013 17:25
EMERGENCY NURSE June 2013 | Volume 21 | Number 3 25
Art & science | patient assessment
the team ensured they had a sense of ownership
of the project, and encouraged them to engage
with their teams throughout the change process.
Medway Hospital board members were in favour
of the change on the grounds that it would improve
patient experience and help staff achieve the new
quality indicators.
Creating a vision the vision or outcome for change
was improved patient safety and satisfaction.
Communicating the vision the vision was shared
in all departmental team meetings and illustrated
on posters placed in the staff rest room. Feedback
and suggestion forms were also provided so
that staff could share their ideas and concerns.
the main concerns, and team members responses,
are described in table 1.
Empowering others to act on the vision the senior
nursing team asked senior nurses who were
enthusiastic about the project to become navigating
champions, who were responsible for devising
the navigation form and leading the pilot project.
the senior sisters conducted research into
attendance trends and chose the quietest day of
the week to start the pilot.
Planning for and creating short-term wins
navigation was regarded as a quick win, partly
because it allows staff to draw on their clinical
expertise during initial assessments and partly
because it helps them to ensure that patients
who arrive by for ambulance wait no longer than
15 minutes for assessment, as stipulated in the
relevant new quality indicator.
in addition, all diagnostic tests are carried out by
navigating assistants under the navigating nurses
instructions so, by the time patients are given full
assessments, the results of the initial assessments
have been returned and clinicians can make
decisions more quickly.
Consolidating improvements and creating more
change Changing well-established practice can
be problematic and, as changes to practice were
consolidated, various problems arose. For example,
during the pilot project, the navigating nurse greeted
patients as they arrived in the waiting room and
attempted to assess them according to the kinds of
information that, under the old system, they would
have volunteered during registration.
this practice raised privacy and confidentiality
issues, however, because the information required
by the navigating nurse is more detailed than that
Figure 4 Allocation of resources in navigation
One band 6 or 7
nurse in charge
One navigating nurse
One navigating
assistant
One resuscitation
nurse
Four trolley area
nurses
Two emergency
triage unit nurses
who work
from 11am
Two observation
ward nurses
Two minor injuries
nurse practitioners
One treatment nurse
usually volunteered to receptionists, and patients
were reluctant to provide such information
while among other patients in the waiting room.
this problem was overcome by removing computers
and other equipment from the old triage room,
and converting it into a navigating room, where
patients could be assessed quickly and in private.
nevertheless, many patients and relatives did
not understand the change to the triage process.
the MtS had been in place for many years and
patients generally understood that they would see
a nurse after they had registered at reception. Some
were shocked to be seen by a nurse on arrival and,
afterwards, were unsure about whether they had
been assessed. others insisted on presenting at
the reception desk rather than being seen by the
navigating nurse.
During this period, patients and relatives
required constant explanation and reassurance,
and a leaflet describing the change was drawn up
and given to them on their arrival, either by the
navigating nurse or reception staff.
the navigating form has also been changed
according to requirements. At time of going to
press, the third version of the form is being used
and a fourth version, which will cover issues such
as the management of people who have mental
health problems or who require close monitoring,
EN Jun 2013 20-26 asIDA1145.indd 25 03/06/2013 17:25
June 2013 | Volume 21 | Number 3 EMERGENCY NURSE 26
Art & science | patient assessment
References
Cooke MW, Higgins J, Bridge P (2000)
A&E: The Present State. Emergency Medicine
Research Group, Universities of warwick
and Birmingham.
Department of Health (2010) A&E Clinical
Quality Indicators: Implementation
Guidance. tinyurl.com/ousal69
(last accessed: May 23 2013.)
Ganley L, Gloster A (2011) An overview
of triage in the emergency department.
Nursing Standard. 26, 12, 49-56.
Kotter J (1995) leading change: why
transformation efforts fail. Harvard
Business Review. tinyurl.com/aqmqevc
(last accessed: May 23 2013.)
Newell J, Smith P (2008) Triage in the
Light of Four Hour Targets: Results of
a Survey of Current Practice in Emergency
Departments in the UK. tinyurl.com/p5g3465
(last accessed: May 23 2013.)
Mackway-Jones K, Marsden J, Manchester
Triage Group (2008) Emergency Triage.
wiley-Jones, Hoboken nJ.
NHS Interim Management and Support
(2011) Effective Approaches in Urgent and
Emergency Care. tinyurl.com/p4f92y8
(last accessed: May 23 2013.)
National Institute for Health and
Care Excellence (2012) Quality
Standards. tinyurl.com/qzucvnk
(last accessed: May 23 2013.)
Pugh D (2002) A phenomenologic study of
flight nurses clinical decision: making in
emergency situations. Air Medical Journal.
21, 2, 28-36.
is under development. this version will also allow
navigating nurses to record assessments of patient
risk of absconding so the nurses in charge know
how often welfare checks should be carried out.
when triage was based on the MtS, nurses
would attend a workshop to learn how to undertake
triage and how to use the trusts computer system
to build on their knowledge. when navigation
was introduced, however, the workshops became
unnecessary and junior nurses had no way of
developing experience in patient assessment.
to address this problem, a clinical prioritisation
workshop for junior nurses was introduced.
As navigating assistants, junior nurses are also
expected to work alongside navigating nurses, and
to gain experience through peer review and senior
support rather than computer program training.
Institutionalising new approaches Allocation of
staff in the ED since navigation was introduced is
shown in Figure 4. initially, staff were re-allocated
to the system, although one extra nurse was
subsequently hired to become a navigating assistant
on the night shifts.
During the pilot and after navigation was
introduced, triage was based on the new system only
during the day and nurses could revert to the more
familiar MtS at night.
After six weeks, however, nursing staff decided
to adopt navigation for 24 hours a day because
it allowed them to identify high risk patients on
arrival, and to make quicker and safer assessments.
this decision to make navigation the established
form of initial assessment for the department was
considered a sign of success and, in november
2011, MtS was replaced by navigation in the EDs
operational policy.
Conclusion
navigation prioritises initial assessments and
ensures that the first person patients contact in the
ED is an experienced nurse. it also reduces initial
assessment time because it does not rely on the use
of a computer program, and reduces the number of
patients who need to be seen by the navigating nurse
by removing from queues those patients who have
arrived by ambulance. Patients are then streamed
to the most appropriate areas from their arrival and
those with more urgent needs are identified more
quickly and more effectively.
navigation is based and reliant on the principles
of triage, but eliminates extra steps. it allows
senior nurses to draw on their expertise and helps
them to identify high risk patients at an early
stage. At Medway Hospital ED, navigating nurses
became better able to interact with patients after
the departments computerised assessment process
has been removed.
Finally, managing change from a well-established
system to a new concept, and ensuring its viability
and success, required careful planning and
implementation by the senior nursing team.
Conflict of interest
None declared
online archive
For related information, visit
our online archive of more
than 7,000 articles and
search using the keywords
EN Jun 2013 20-26 asIDA1145.indd 26 03/06/2013 17:25
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Key Nursing SkillsDocument359 pagesKey Nursing Skillsmordanga100% (6)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Central BankDocument65 pagesCentral BankFarazNaseer100% (1)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Modulus of Subgrade Reaction KsDocument1 pageModulus of Subgrade Reaction KsmohamedabdelalNo ratings yet
- Nursing Care Plan For Ineffective Airway ClearanceDocument7 pagesNursing Care Plan For Ineffective Airway Clearancearlee marquez96% (117)
- Nexus Undercarriage Cross Reference GuideDocument185 pagesNexus Undercarriage Cross Reference GuideRomanNo ratings yet
- Design of Shear Walls Using ETABSDocument97 pagesDesign of Shear Walls Using ETABSYeraldo Tejada Mendoza88% (8)
- NCP-Risk For InfectionDocument2 pagesNCP-Risk For Infectioneihjay-bravo-804175% (80)
- Factory Hygiene ProcedureDocument5 pagesFactory Hygiene ProcedureGsr MurthyNo ratings yet
- Funded African Tech Startups 2020Document13 pagesFunded African Tech Startups 2020LoNo ratings yet
- 2010 Yoshimura Book of SpeedDocument83 pages2010 Yoshimura Book of Speedacornwoods_brentNo ratings yet
- TAHBSO PathophysiologyDocument5 pagesTAHBSO Pathophysiologybregette50% (2)
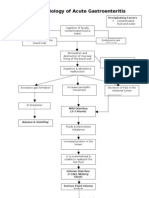
- Pathophysiology of Acute GastroenteritisDocument1 pagePathophysiology of Acute GastroenteritisJohn Glenn Bianzon79% (29)
- Immediate Newborn CareDocument8 pagesImmediate Newborn Caree jeighNo ratings yet
- Product of Your Own Personal Library Research and Creative Thinking. If You Are Not Certain About The LevelDocument5 pagesProduct of Your Own Personal Library Research and Creative Thinking. If You Are Not Certain About The LevelMareeze HattaNo ratings yet
- BLOOD AND IMMUNITY EXAM REVIEW FOR NURSESDocument4 pagesBLOOD AND IMMUNITY EXAM REVIEW FOR NURSESMareeze HattaNo ratings yet
- List of Successful Examinees in The May 2014 Nurse Licensure ExaminationDocument225 pagesList of Successful Examinees in The May 2014 Nurse Licensure ExaminationofwwatchNo ratings yet
- Development of A Conceptual Nursing Model For TheDocument10 pagesDevelopment of A Conceptual Nursing Model For TheMareeze HattaNo ratings yet
- TPDocument2 pagesTPMareeze HattaNo ratings yet
- Nursery JournalDocument11 pagesNursery JournalSte WardNo ratings yet
- Clinical Trial Oral Ondansetron For Reducing Vomiting SecondaryDocument11 pagesClinical Trial Oral Ondansetron For Reducing Vomiting SecondaryMareeze HattaNo ratings yet
- 03 Chemo PrincDocument17 pages03 Chemo PrincMareeze HattaNo ratings yet
- Family Planning Allows People To Attain Their Desired Number of Children and Determine The Spacing of PregnanciesDocument6 pagesFamily Planning Allows People To Attain Their Desired Number of Children and Determine The Spacing of PregnanciesMareeze HattaNo ratings yet
- Acute Gastroenteritis Pathophysiology ExplainedDocument2 pagesAcute Gastroenteritis Pathophysiology ExplainedMareeze Hatta100% (1)
- Acute Gastroenteritis Pathophysiology ExplainedDocument2 pagesAcute Gastroenteritis Pathophysiology ExplainedMareeze Hatta100% (1)
- Meeting ED Quality Indicators with Simplified Patient AssessmentsDocument8 pagesMeeting ED Quality Indicators with Simplified Patient AssessmentsMareeze HattaNo ratings yet
- Developing Preventive Mental Health InterventionsDocument22 pagesDeveloping Preventive Mental Health InterventionsMareeze HattaNo ratings yet
- Medicine ManagementDocument10 pagesMedicine ManagementMareeze HattaNo ratings yet
- Programmes For Parents With A Mental IllnessDocument9 pagesProgrammes For Parents With A Mental IllnessMareeze HattaNo ratings yet
- Ultrasonic Examination of Heavy Steel Forgings: Standard Practice ForDocument7 pagesUltrasonic Examination of Heavy Steel Forgings: Standard Practice ForbatataNo ratings yet
- Racial and Ethnic Challenges in the UAE vs UKDocument16 pagesRacial and Ethnic Challenges in the UAE vs UKATUL KORINo ratings yet
- Organization Structure GuideDocument6 pagesOrganization Structure GuideJobeth BedayoNo ratings yet
- WSM 0000410 01Document64 pagesWSM 0000410 01Viktor Sebastian Morales CabreraNo ratings yet
- SINGGAR MULIA ENGINEERING HORIZONTAL 2-PHASE SEPARATORDocument3 pagesSINGGAR MULIA ENGINEERING HORIZONTAL 2-PHASE SEPARATORElias EliasNo ratings yet
- Article 4Document31 pagesArticle 4Abdul OGNo ratings yet
- Libros de ConcretoDocument11 pagesLibros de ConcretoOSCAR GABRIEL MOSCOL JIBAJANo ratings yet
- Rtlo 18918B 1202Document42 pagesRtlo 18918B 1202gustavomosqueraalbornozNo ratings yet
- Diagram of Thermal RunawayDocument9 pagesDiagram of Thermal RunawayVeera ManiNo ratings yet
- Research Grants Final/Terminal/Exit Progress Report: Instructions and Reporting FormDocument13 pagesResearch Grants Final/Terminal/Exit Progress Report: Instructions and Reporting FormBikaZee100% (1)
- MSDS Metafuron 20 WPDocument10 pagesMSDS Metafuron 20 WPAndi DarmawanNo ratings yet
- DS 20230629 SG3300UD-MV SG4400UD-MV Datasheet V16 ENDocument2 pagesDS 20230629 SG3300UD-MV SG4400UD-MV Datasheet V16 ENDragana SkipinaNo ratings yet
- 2.4 Adams Equity TheoryDocument1 page2.4 Adams Equity TheoryLoraineNo ratings yet
- Password CrackingDocument13 pagesPassword CrackingBlue MagicNo ratings yet
- Incident Report Form: RPSG-IMS-F-24 Accident and Investigation Form 5ADocument2 pagesIncident Report Form: RPSG-IMS-F-24 Accident and Investigation Form 5ARocky BisNo ratings yet
- Exercise No. 7: AIM: To Prepare STATE CHART DIAGRAM For Weather Forecasting System. Requirements: Hardware InterfacesDocument4 pagesExercise No. 7: AIM: To Prepare STATE CHART DIAGRAM For Weather Forecasting System. Requirements: Hardware InterfacesPriyanshu SinghalNo ratings yet
- Checklist PBL 2Document3 pagesChecklist PBL 2Hazrina AwangNo ratings yet
- A Dream Takes FlightDocument3 pagesA Dream Takes FlightHafiq AmsyarNo ratings yet
- Stellar Competent CellsDocument1 pageStellar Competent CellsSergio LaynesNo ratings yet
- Hollow lateral extrusion process for tubular billetsDocument7 pagesHollow lateral extrusion process for tubular billetsjoaopedrosousaNo ratings yet
- ViscosimetroDocument7 pagesViscosimetroAndres FernándezNo ratings yet
- (NTA) SalaryDocument16 pages(NTA) SalaryHakim AndishmandNo ratings yet
- 59 - 1006 - CTP-Final - 20200718 PDFDocument11 pages59 - 1006 - CTP-Final - 20200718 PDFshubh.icai0090No ratings yet