Professional Documents
Culture Documents
Communicable Diseases
Uploaded by
Kimsha Concepcion0 ratings0% found this document useful (0 votes)
535 views176 pagesby: Kimberly Trisha R. Conccepcion
Notify me, if you've download my file, thanks
The sources are sited in other files together with the table of contents.
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentby: Kimberly Trisha R. Conccepcion
Notify me, if you've download my file, thanks
The sources are sited in other files together with the table of contents.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
535 views176 pagesCommunicable Diseases
Uploaded by
Kimsha Concepcionby: Kimberly Trisha R. Conccepcion
Notify me, if you've download my file, thanks
The sources are sited in other files together with the table of contents.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 176
Page 1
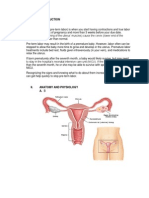
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
COMMUNICABLE DISEASES
Communicable disease- (synonym: infectious disease) An illness
due to a specific infectious agent or its toxic products that arises through
transmission of that agent or its products from an infected person, animal
or inanimate source to a susceptible host; either directly or indirectly
through an intermediate plant or animal host, through a vector, or through
contact with the inanimate environment.
Common communicable diseases found in the Philippines are discussed
according to the different systems which they affect and in the following order,
if specified:
Important information/Description
Also known as(aka)
Causative agent
Predisposing factors
Incubation period
Period of communicability
Mode of transmission
Diagnostic/Laboratory exams
Signs and symptoms
Complications
Management
Prevention
Treatment
Medical Care
Nursing Care
Page 2
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
DISEASES AFFECTING THE INTEGUMENTARY
SYSTEM
I. LEPROSY
A. Important Information
1. Chronic infectious and communicable disease. No new case of
leprosy arises without previous contact; usually prolonged and
intimate, with an open case.
2. Majority is contracted in childhood, will show manifestations
by 15 years of age and definitely diagnosed by age 20.
3. It is not hereditary.
4. No other disease shows these cardinal signs:
4.1 Presence of Hansens bacilli in stained smears or biopsy
material
4.2 Presence of localized areas of anesthesia
5. Does not cross placental tissues and therefore does not affect
the fetus. Pregnancy women with leprosy cannot be treated because
the drugs are teratogenic.
B. AKA: Hansens Disease, Hansenosis, Lepra
C. Causative Agent: Mycobacterium leprae or Hansens bacilli thrives
best in reticuloendothelial cells
D. Incubation Period - varies from 1 to 5 years
E. Period of communicability as long as there are open lesions
Children below 12 years old are more susceptible
F. Mode of transmission:
1. (Not exactly known) Skin to skin contact with untreated leprosy
patient
2. Respiratory tract: Droplet infection (nasopharyngeal secretions)
G. Diagnostic/Laboratory exams:
Page 3
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
1. Skin smear test
A skin smear is a test in which a sample of material is collected
from a tiny cut in the skin and then stained for M. leprae, an acid-
fast bacillus.
2. Skin lesion biopsy
A skin biopsy is the removal of a small portion of abnormal skin.
The removed skin is tested to see why it is not normal.
3. Lepromin Test- tissue is removed from the earlobe or from large
soft nodules thoroughly dried and ground into powder as the basic
lepromin stock. The usual dose is 0.2 ml, just enough to produce a
wheal when injected intradermally at the flexor surface of the
forearm. A (+) result develops a nodule at the site of injection on the
1
st
-3
rd
week and gradually increase in size.
Size of the wheal
3 mm. wheal 1+
3-5 mm. wheal 2+
>5mm. wheal 3+
If nodule
suppurates
4+
H. Types
1. Polar
1.1 Lepromatous or malignant
Many microorganisms are found
Open or infectious cases
Negative reaction to lepromin test
Tendency to form globi in the skin, mucous membranes,
peripheral nerves
1.2 Tuberculoid or benign
Only few organisms are found
Usually closed or noninfectious
Positive reaction to lepromin test
2. Indeterminate- unestablished lesion; usually noninfectious
3. Borderline- s/sx of tuberculoid and lepromatous
I. S/Sx:
CARDINAL SIGNS
1) Peripheral nerve enlargement
2) Loss of sensation
3) Positive smear test
EARLY STAGE
Skin changes color
Alopecia- hair loss
Muscle weakness and
paralysis of the extremities
Page 4
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Pain and redness in the eyes
Loss of sensation(anesthesia)
Epistaxis nose bleeding
Skin ulcers which do not heal even when treated
Anhydrosis loss of sweating
Skin lesions varying from bronze, purple or light red macules, 1-
10 cm in diameter; yellow or brown infiltrated nodules, 1-5 cm in
diameter; confluent nodules
LATE STAGE
Clawing of the fingers and toes due to contractures
Lagophthalmos inability to close the eyes
Leoning face pathognomonic sign
- skin becomes so thickened and nodular
Page 5
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Earlobes are thickened and nodular
Sinking of the nose bridge(saddle nose deformity) due to
absorption of the small bones
Severe neuritis: neuralgic pains, most severe in the arms
Trophic ulcers on the hands, feet, fingers or toes contract
because of bone absorption and big blisters or bullae appear on
the trunk
Gynecomastia- enlargement of male breast
Madarosis loss of hair, then thickening of eyebrows
FINAL STAGE
Injury of the eye
Involvement of the 5
th
and 7
th
cranial nerves
Gangrene of fingers or toes which may require amputation
J. Management
PREVENTION
Separate infants from lepromatous parents at birth
BCG immunization
Avoid contact
MEDICAL CARE
Domiciliary treatment as embodies in R.A. 4073 which
advocated home treatment
Multidrug therapy (MDT): sulfone drugs are given in
combination with other drugs to prevent drug resistance, hasten
recovery and lessen the period of communicability
Paucibacillary (few organisms)- given for 6-9 mos. or until
negative
Page 6
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Rifampicin once a month
Dapsone once a day
Multibacillary (many organisms)- given for 24-30 mos./2
years
Rifampicin once a month
Dapsone once a day
Lamprene once a day(causes blackish discoloration of
the skin)
Adverse Reaction
RIFAMPICIN
Discoloration of body fluids
Rashes
Muscle soreness
Anuria (nephrotoxicity)
Thrombocytopenia- relative decrease of platelets in blood
Jaundice
DAPSONE
Causes increase in the numbers of lesions
Treated symptomatically, needs referral
LAMPRENE
Skin discoloration
Dryness and flakiness of the skin (hot soak to improve
circulation)
TREATMENT COMPLETION
PB regimen- should take 6 blister packs within 9 mos.
MB regimen- should take 12 blister packs within 18 mos.
At the end of this duration, the patient should be considered as
Treatment Completed (TC)
NURSING CARE
Emotional support
Skin and Meticulous eye care
Balanced diet, exercises and rest hygiene
Adequate information regarding drug therapy
Page 7
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
II. MEASLES & III. GERMAN MEASLES
Measles
German Measles
A. Important
Information
1. An extremely
contagious exanthematous
disease of acute onset.
2. Essential a disease of
childhood.
3. Signs and symptoms
are preferable to the upper
respiratory passages.
4. It is endemic and may
occur at any time of the
year.
5. Breastfed babies of
mothers who have measles
possess a relative immunity
for the first 3 months of life.
6. The greatest incidence
occurs during 3 years of
age.
7. Second attacks are not
impossible.
8. The most common
complication is otitis media.
9. The most serious
complications are
bronchopneumonia and
encephalitis.
1. An acute contagious disease
2. Essentially a mild childhood
disease, the danger actually
being congenital defects in the
newborn if a pregnant woman
suffers from it or exposed to
someone with the disease.
2.1 Mirocephaly
2.2 Congenital heart
defect; cataract; deafness and
mutism
B. Also known
as
Rubeola; Morbilli;
Little Red Disease;
hard Measles, 7-day
measles; 9-day
measles
Rubella, 3-day measles
C. Causative
agent
filterable
Paramyxovirus,
rubeola/measles virus
Pseudoparamyxovirus,
Rubella/ Toga virus
D. Incubation
period
usually 10-12 days
(8-20 days)
usually 14-21 days
E. Period of
communicability
about 9 days (4 days
before to 5 days after the
appearance of rash). It is
4-7 days after the onset of
catarrhal symptoms ( 7
days before and 4 days
Page 8
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
most communicable at the
height of the rash
after the appearance of
rash)
F. Mode of
transmission
Spread by direct
(droplet/airborne;
nasopharyngeal
secretions) or indirect
contact (airborne)
Same with measles, mother
to infant (transplacental)
G. Signs &
symptoms
PRE-
ERUPTIVE/PRODROMA
L STAGE
3 Cs: Coryza, Cough,
Conjuctivitis
Photophobia- fear of
light
Pathognomonic sign
: Kopliks spot
whitish spots in the
inner cheeks, appear
3 days before rashes
start
ERUPTIVE/ SKIN RASH
STAGE
Usually seen on the
fourth day
Maculopapular
rashes redisn in
color and blotchy in
appearance
-Cephalocaudal
appearance: from
face to trunk to
extremities
High grade
PRE-
ERUPTIVE/PRODROMAL
STAGE
Starts with low grade
fever
Mild catarrhal symptoms
Malaise, stiffness of the
neck, and anorexia
Mild conjunctivitis and
sore throat
Most earliest and
prominent characteristic
sign:
Lymphadenopathy
ERUPTIVE STAGE
Pathognomonic sign:
Forscheimers spot
pinkish rash on the soft
palate extending to
mucous membrane
Pinkish maculopapular
rash begins on the face
and spreads to trunk,
limbs, fades rapidly
lasting about 2-3 days
No pigmentation or
desquamation
Testicular pain in adults
Transient
polyarthralgia(joint
pains) & polyarthritis(
pain affecting 5 or more
joints)
Enlargement of lymph
nodes- subocciptal,
pastauricular and
poscervical
Page 9
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
intermittent fever
Anorexia(loss of
appetite),
pruritus(itching), and
irritability
Tonsillitis(inflamma-
tion of the tonsils)
CONVALESCENT
STAGE
Cephalocaudal
disappearance of the
rashes
Desquamation of the
skin
POST-ERUPTIVE STAGE
Lymph nodes subsides
Rashes disappear on the
3
rd
day
H. Diagnosis/
Diagnostic test
Clinical observation
Nose & Throat
Swabbing-
laboratory test done
to isolate and
identify organisms
that may cause
infection in the
throat
Leukopenia or
leukocytosis
Confirmatory test:
Complement
fixation or
Same as measles
Page 10
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
hemagglutinin an
immunological test
that is used to detect
presence of specific
antigen/antibody
produced by
microorganism
I. Immunity/
Prevention
Measles vaccine at 9
months old
MMR (measles,
mumps, and rubella)
vaccine
-1
st
dose at 15 months
old
-2
nd
dose at 11 to
years
MMR vaccine
Pregnant women should be
vigilant preventing
exposure
Immunoglobulin one week
after exposure of high risk
individuals
-Immune serum globulin
(20 ml)- given to pregnant
woman in their 1
st
trimester
J. Complications Bronchopneumonia-
acute or chronic
inflammation of the
lungs
Abdominal pain
Secondary skin
infections
Otitis media
Encephalomyelitis-
inflammation of the
brain and spinal cord
Subacute sclerosing
panencephalitis
(SSPE)
Encephalitis
Neuritis
Arthritis
Athralgia
Congenital rubella
syndrome
I. Management NURSING CARE:
Isolate in a well-
ventilated room with
subdued light
NURSING CARE:
Isolate in a well-ventilated
room with subdued light
Bed rest
Page 11
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Tepid Sponge Bath
(TSB)-for fever
Skin care; daily
cleansing bed bath
Oral hygiene (for
tonsillitis)
Position patient where
direct glare of light is
avoided
Care of ears
Increase Oral Fluid
Intake and provide
adequate nutrition,
increase Vitamin C
Avoid exposure to
draft. Never sponge
with cold water
MEDICAL CARE:
No therapy is indicated
for uncomplicated
measles
Supportive &
Symptomatic
Antipyretics
Antibiotics for
secondary infections
Immune Globulin
prophylaxis
TSB (for fever)
Ear and eye care
TREATMENT: Symptomatic
Page 12
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IV. CHICKEN POX & V. HERPES ZOSTER
Chicken Pox
Herpes Zoster
A. Important
Information
1. Most highly contagious
childhood disease
2. Affects adults more
severely than children
3. One attack confers
lifelong immunity
4. Not all viruses may
leave the body; they just
become dormant and live in
the nerves which, when
weakened by low resistance,
may lead to Herpes Zoster
5. Charcaterized by
vesicular eruptions on the
skin and mucous membrane
6. Mild self-limiting disease
1. Caused by the same virus
that causes chickenpox
2. A dormant type of
chickenpox
3. More often attacks adults
than children
4. Uncommon under age 10
5. Appears in clusters
6. Acute viral infection of the
nerve structure occurring in a
partially immune individual due
to a previous varicella infection
7. Extremely painful because it
affects the sensory nerve
B. Also known
as
Varicella zoster
Shingles; Acute Posterior
Ganglionitis; Zota
C. Causative
agent
Varicella Zoster virus;
Herpes virus varicella;
Human Haemophilus
virus 3
Same as chicken pox
D. Incubation
period
From 10 to 21 days
(mean: 14 days)
Unknown; believed to be
13 to 17 days
E. Period of
communicability
1 day before the
eruption of the first lesion
up to five days after the
appearance of the last crop
A day before appearance of
rash until 5 to 6 days after
last crust
F. Mode of
transmission
Direct contact
Indirect contact
(linen or fomites)
Airborne/droplet
infection
Same as chicken pox
G. Signs &
symptoms
PRE-
ERUPTIVE/PRODROMAL
STAGE
Mild fever and malaise
ERUPTIVE/ SKIN RASH
STAGE
Rashes start from the
trunk (unexposed
area) then spread to
Rashes start from any
part of the body
More commonly on
areas along the course
of spinal sensory and
cranial nerve such as
the thoracic wall, face,
neck and lumbar area
Follows the same
course of rashes on
chickenpox
Page 13
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
other parts of the
body
In older children,
lesions may
widespread and more
severe
Rapid progression
Very pruritic
STAGES
MACULE
flat red lesion
PAPULE
elevated lesion
VESICLE
fluid-filled papule <1cm
thin walled vesicle readily
bursts and dries up in 3 to
5 days
PUSTULE
infected or pus-filled
vesicle
scar usually become big
and wide
CRUST
scar formation that is
superficial, depigmented
and takes time to fade
out
POST-ERUPTIVE STAGE
falling off of
exanthem
PAIN is a major
symptom, occurs 1 to 5
days before appearance
of rash, worse at night
and on movement, can
cause paresthesia on
the affected skin
(numbness & tingling)
and/or painful vesicles
similar to chickenpox
Post-Herpetic
Neuralgia- painful
condition which affects
the nerve fibers and
skin
Fever, malaise,
anorexia, and
headache,
lymphadenopathy
GASSERIAsN
GANGLIONITIS
result when Cranial
Nerve V (Trigeminal
Nerve) is affected
RAMSAY-HUNT
SYNDROME result
when Cranial nerve VII
paralysis and vesicles
on the external auditory
meatus
H. Prognosis the younger the
patient, the more
favorable is the
prognosis
disease lasts about 2
weeks including the
peeling of crusts
Not serious but may
cause extreme
discomfort
I. Diagnosis/
Diagnostic test
Clinical observation
Demonstration of the
virus via electron
microscope
Complement
fixation or
Same as chickenpox
Page 14
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
hemagglutinin an
immunological test
that is used to detect
presence of specific
antigen/antibody
produced by
microorganism
J. Immunity/
Prevention
Varivax
active artificial
immunity- live
attenuated varicella
vaccine
Passive immunity
Human hyper-
immune gamma
globulin
K.
Complications
Meningo-encephalitis
Pneumonia
Sepsis
Secondary infection:
Cellulitis, Furuncle/Boil
Encephalitis
Paralytic ileus, bladder
paralysis
Blindness
Deafness
L. Management NURSING CARE:
Respiratory isolation is
a must until all
vesicles have crusted
Proper hygiene
Attention should be
given to
nasopharyngeal
secretions and
discharges
Avoid complications of
vesicles by cutting
fingernails short and
wash hands more
often, child must wear
mittens, apply cool wet
dressings with NSS to
pruritic lesions
Provide activities to
keep child occupied to
lessen pruritus
Calamine lotion over
rash
Anti-pyretics for fever
MEDICAL CARE:
Antiviral Acyclovir
(Zovirax)
NURSING CARE:
Isolation
Apply cool wet dressings
with NSS to pruritic lesios
Efforts should be made to
prevent secondary
infections
MEDICAL CARE:
Symptomatic
Anti-viral meds (Acyclovir)
Analgesics
Anti-inflammatory
Potassium Permanganate
compress(ABO)
A-astringent effect
B-bacterial effect
O-oxidizing
effect(deodorize the rash)
Page 15
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Antihistamine
Calamine Lotion
Antipyretics
NOTE: No aspirin because it
can lead to Reyes
Syndrome
Page 16
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VI. SCABIES
A. Important Information
1. It is an aged-old skin infection caused by an itch mite, which
penetrates the skin, forming burrows.
2. Burrows are tiny thread-like projections ranging 2-6mm long that
appear as thin gray, brown or red lines in affected area
3. Scabies occurred worldwide and is predisposed by overcrowding and
poor hygiene
4. It is characterized by eruptive lesions produced from burrowing of the
female parasite into the skin.
5. It is common disease of troops in the field under wartime conditions
B. AKA: GALIS
C. Causative agent: Sarcoptes scabiei mite is a yellowish white in
color and barely seen by the unaided eye. The parasite does not survive
more than 3-4 days away from the skin. The males are smaller and the
females burrows beneath the epidermis to lay her eggs that causes
intense irritation.
D. Incubation period: within 24 hours of an original contact
E. Period of communicability: The disease is communicable for the
entire period that the host is infected.
F. Mode of transmission:
1. Direct contact with infected persons
2. Acquired through sleeping on an infested bed or wearing infested
clothing
3. Scabies on dogs (mange)
G. Diagnostic test:
1. Clinical observation when appearance of lesion, and the intense
itching and finding of the causative agent
2. A drop of mineral oil placed over the burrow, followed by superficial
scraping with a hypodermic needle or curette, and then examined
under lower power of the microscope or by hard lens, may reveal
mites, ova or mite feces.
Page 17
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
H. Signs and Symptoms
Eruptive lesions produced by the burrowing of the female parasite into
the skin
Scabies Burrow- pathognomonic sign
1
st
symptom is severe itching that is most intense at night
1
st
week the itch is subtle, it is more intense that after a month or two,
sleep becomes almost impossible
Secondary lesions: vesicles, papules, pustules, excoriation and crusts
may be found on affected site
Minor discomfort- skin may feel hot and burning
Secondary infection is severe- fever, headache and malaise.
Secondary dermatitis is common
I. Management
MEDICAL CARE
Application of Pediculicide such as permethrin cream or lindane
lotion( 10-12 hours)
Crotamiton cream (5 consecutive nights)
Neosporin ointment (4 to 5 times/day)
Page 18
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Eurax and Kwell lotion drug of choice
Antihistamine like dipenhydramine(Benadryl) relief from itching
NURSING CARE:
All clothes used before and during the treatment period should
be disinfected by dry cleaning or boiling.(Benzyl benzoate
emulsion- is the cleaner)
Instruct the patient to apply the cream at bedtime, from the
neck down to the toes, covering the entire body.
Advise the patient to report any skin irritation.
Suggest that family members and other close contacts of the
patient be checked for possible symptoms and treated if
necessary.
If the patient is hospitalized, practice good handwashing
technique or use gloves
Terminal disinfection should be carried out after the discharge
of the patient.
PREVENTION & CONTROL:
Good personal hygiene
Avoid contact with infected persons
All members of the household, including close contacts, should
be treated
After treatment, beddings and clothing worn next to the skin
should be properly laundered.
Page 19
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VII. PEDICULOSIS
A. Important Information
1. Propagate in hairy regions of the body.
2. Nits (louse eggs or lisa) cling tenaciously to the shaft of the hair
3. More commonly a disease of females and of children than adults.
4. Infestation by lice of the head, body, or pubic area
5. Also called Phthiriasis
Head Lice
Body Lice Crab Lice Or Pubic
Lice
A.
Etiologic
agent
Pediculus humanos
var. capitis
Pediculus
humanos
var.
corporis
Gray-white
insect
about 2-
4mm long
Female is a
little longer
Lifespan- 1
month
8-10
eggs/day
8 days
eggs
hatched
Phthirus pubis
A rounder insect
about 2-3 mm
long
4-6 legs
Lifespan 3-4
weeks
3 eggs/day
Incubate 6-8 days
before hatching
B. Mode of
trans-
mission
Passed from person to person
The source of infestation: being other infested persons or
their personal belongings, especially clothing
C. Signs
and
Symptoms
Itching- 1
st
predominant
symptom
Plica polonica-
rare condition
leading to tangled
hair and an
inflamed scalp
Initial
lesions
minute red
spots
Spot swells
Secondary
crust and
excoriation
is formed
Persistent itching
in the pubic
region chief
symptom
Grayish
pigmented spots
(maculae
caerulae) are
found in the inner
thighs or the
abdomen
Page 20
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
D.
Diagnostic
Physical examination
Using fluorescent light and microscopic examination of hair
shafts
E.
Complica-
tion
Pigmentation and honey crust of secondary pyoderma
Vagabondia- a combination of extensive excoriation, hypo-
and hyperpigmentation associated with lichenification
Enlargement of the nuchal and cervical nodes, with febrile
episodes that can lead to micrococcal infection
Blepharitis- ocular condition characterized by chronic
inflammation of the eyelid
F.
Treatment
Dusting the scalp
with 1% malathion
powder/lotion
is a reliable and
convenient method
Thorough massage
gamma-benzene
hexachloride
shampoo in the
scalp for 4 minutes,
then rinse.
Launder
(dry clean)
or boil the
clothing
and
beddings
Good body
hygiene
must be
observed
always
Apply Kwell or
Gamene (lindane)
cream or
lotion(see tx. of
scabies)
Rub crotamiton
(Eurax, Geigy)
onto the affected
area
Repeat the
application of
crotamiton after 1
week
Treat patient with
sexual contact
with the patient
Remove
remaining nits
mechanically
Infestation in the
eyelids treated
with yellow
oxide of
mercury
Apply it twice
daily for a few
days
G.
Prevention
Good personal hygiene
Avoiding contact with persons suffering from pediculosis
Page 21
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VIII. IMPETIGO
A. Important information
1. It is a superficial infection of the skin
2. Exposed areas of the body, face, hands, neck and extremities are most
frequently involved.
3. It is particularly common among children living in poor hygienic
conditions.
4. In adults, chronic health problems, poor hygiene, and malnutritions
may predispose to impetigo
B. Causative agent: Group A Streptococcus, Staphylococci
C. Mode of transmission:
1. Skin to skin contact
2. Other members of the family who touch the patient or who use towels
or combs that are soiled with the exudates of the lesion
D. Signs and Symptoms
Vesicle formation affecting only the stratum corneum
Pruritic vesicle or pustule that breaks
Leaves a thick honey-colored crust
Intense itching, burning
Scratching often causes satellite lesions
Ecthyma-deeper form of impetigo
Secondary infections: Osteomyelitis, arthritis, and pneumonia
Regional lymphadenopathy is common
Acute nephritis
Page 22
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Pathognomonic Sign (Collarette Sign)- Collar of scale forms
around ruptured Blister roof
E. Complication
Glomerulonephritis severe complication that occurs in about 3% of
impetigo cases, is a renal disease (usually of both kidneys)
characterized by inflammation of the glomeruli, or small blood vessels
in the kidneys.
F. Diagnostic
Physical examination
Grams stain and culture of the lesions
G. Management
MEDICAL CARE
Oral antibiotics and topical mupirocin(Bactroban) ointment
Systemic antibiotic therapy
Agents for nonbullous impetigo: benzathine penicillin or oral
penicillin or erythromycin
Agents for bullous impetigo: penicillinase-resistant penicillin or
erythromycin
Topical antibacterial therapy for 1 week
NURSING CARE
Use antiseptic solution (chlorhexidine/ Hibiclens) to cleanse
skin and reduce bacterial content and prevent spread.
Wear gloves when giving care
Instruct patient and family to bathe at least once daily with
bactericidal soap
Encourage cleanliness and good hygiene practices to prevent
spread of lesion from one skin area to another from one person
to another.
Instruct patient and family not to share bath towels and
washcloths and to avoid physical contact between the infected
person and other people until lesions heal.
Page 23
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IX. TINEA/FUNGAL SKIN DISEASE
A. Important information
1. Tinea infections affect the head, body, groin, feet and nails.
2. It is also called ringworm because of its appearance of ring or rounded
tunnel under the skin.
3. It is most common dermatological problems encountered by health
care professionals.
Tinea Capitis Tinea
corporis
Tinea cruris Tinea pedis Tinea
unguium
A.
Location/Al
so known
as:
Head Body Groin Area;
Jock itch
or Jock
rot
Foot;
Athletes
foot
Toenails;
Onycho-
mycosis
B.
Information
It is
contagious
fungal
infection of
the hair shaft
Common in
children
It also
involve
s the
face,
exclu-
ding
the
area of
a beard
in men,
trunk
and
limbs
Men are
affected far
more
frequently
than
women
It occurs
more
frequently
in young
joggers,
obese
people, and
those
wearing
tight under-
clothing
It is most
common
fungal
infection
It is
prevalent
in those
who use
communal
showers
or
swimming
pools
May
appear
acute or
chronic
infection
on the
soles of
the feet
or
between
the toes
It is
associa-
ted with
long-
stand-
ing
fungal
infect-
ion of
the feet
C.
Causative
agent
Tricho-
phyton
tonsurans
Tricho-
phyton
genus
Epidermo
-phyton
floccosum,
Tricho-
phyton
rubrum,
and
Tricho-
phyton
menta-
grophytes
Tricho-
phyton
genus
Tricho
phy-
ton
genus
D.
Incubation
period
10-14 days 4 10 days probably weeks but
exact limits are
unknown
Page 24
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
E. Period of
communi-
cability
A person can spread ringworm as long as lesions are present and
viable fungus persists on contaminated materials and surfaces.
E. Mode of
trans-
mission
Direct
contact with
a human or
animal
source
Inanimate
infected
objects such
as the back
of seats,
combs,
brushes, or
hats.
Direct contact with a human or
animal source
Contracted from places such as
shower stalls, benches,
contaminated floors, and articles
used by an infected person.
Direct
con-
tact
with a
human
or
animal
source
F. Signs &
Symptoms
Oval, scaling,
erythema-
tous patches
Small
papules or
pustules on
the scalp
Brittle hair
that breaks
easily
Begins
with
red
macule,
which
spreads
to aring
of
papules
or
vesicles
with
central
clearing
Lesions
found
in
cluster
Many
spread
to the
hair,
scalp or
nails
Very
pruritic
Begins with
small, red
scaling
patches,
which
spread to
form
circular
elevated
plaques
Very
pruritic
Clusters of
pustules
may be
seen
around
borders
Soles of
one or
both feet
have
scaling
and mild
redness
with
macera-
tion in the
toe webs
More
acute
infections
may have
clusters of
clear
vesicles
on dusky
base
Nails
thicken
, crum-
ble
easily,
and
lack
luster
Whole
nail
may be
destroy
ed
G.
Complica-
tion
Bacterial skin infections, cellulitis
Skin disorders such as pyoderma or dermatophytid
Spread of tinea to feet, scalp, groin, or nails
Whole-body (systemic) side effects of medications
H.
Diagnostic
A special lamp
called a
Wood's
lamp test can
help diagnose
a fungal scalp
infection.
Skin biopsy
Looking at a skin scrap-ing of the rash
under the micro-scope using a KOH
(pota-ssium hydro-xide) test
Skin lesion biopsy
Skin Culture test
Physi-
cal
exam-
ination
Culture
test
Page 25
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
I. Medical
Manage-
ment
Griseofulvin
for 6 weeks
Shampoo
hair 2 or 3
times with
Nizoral or
selenium
sulfide
shampoo
Mild condi-tions:
Topical antifungal
creams
Severe condi-tions:
Griseofulvin or
terbinafine
Soak feet
in vinegar
and water
solution
Resistant
infections:
Griseofulv
in or
terbina-
fine
Terbina-
fine
(Lamisil)
daily for 3
months
Itracona
-zole
(Sporan
ox) in
pulses
of 1
week a
month
for 3
months
J. Nursing
Manage-
ment
Instruct the
family and
patient to
set up a
hygiene
regimen for
home use
Each person
should have
a separate
comb and
brush
Avoid
exchanging
hats and
other
headgears
All infected
members
should be
examined
Household
pets should
also be
examined
Instruct
to use
clean
towel
and
wash-
cloth
daily
Clean
cotton
clothing
should
be worn
next to
the skin
Instruct
the
patient
to avoid
excessiv
e heat
and
humidity
Avoid
wearing
nylon
under-
wear,
tight-
fitting
clothing,
and wet
bathing
suit
The
groin
area
should
be
cleaned,
dried
thorough
ly, and
dusted
with a
topical
antifung
al agent
such as
tolnaf-
tate
Instruct to
keep feet
as dry as
possible
Place a
small
cotton can
be placed
between
the toes
at night to
absorb
moisture
Socks
should be
made of
cotton
Plastic- or
rubber-
soled
footwear
should be
avoided
Talcum
powder
applied
twice
daily
Strict
followin
g of
prevent-
ive
measure
s may
help in
averting
relapse
of the
fungal
nail
disease
The
nails
should
be kept
trimmed
and the
side skin
edges
should
not be
cut.
It is
better to
take off
shoes
for small
periods
of time
during
the day
Page 26
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
X. ANTHRAX
A. Important Information
1. It is an acute bacterial disease usually affecting the skin but which
may very rarely involve the oropharynx, lower respiratory tract,
mediastinum or intestinal tract.
B. AKA: Malignant pustule; Malignant edemia; Woolsorter disease;
Ragpicker disease
C. Causative agent: Bacillus anthracis
Large, aerobic, spore-forming, Gram (+) rod-shaped MO
Survive for years in dry soil
Destroyed by boiling for 10 mins.
Tx: KMnO
4
hydrogen peroxide
Susceptible to penicillin
D. Human cases:
Agricultural cases- contact with infected animals
Industrial cases exposure to contaminated hides, goat hair,
wool, or bones
E. Mode of transmission:
Direct
Indirect
Airborne
Page 27
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
F. Signs and symptoms
Cutaneous anthrax Inhalation anthrax
(Woolsorters disease)
Gastrointestinal
anthrax
Incubation period: 9
hrs-2 wks (2-7 days)
2-3 days- a small
pimple or macule
appears
4
th
day ring of
vesicles develops
Marked edema stops
to develop
5
th
7
th
days
original papules
ulcerate forming
eschar
Edema extends from
the lesion
Severe sx. if it is
located on face, neck
or chest
High fever, toxemia,
regional painful
lymphadenopathy,
extensive edema-
severe forms
Shock and death may
also occur
Presenting sx those of
severe viral
respiratory disease
1-3 day acute phase-
increasing fever,
dyspnea, stridor,
hypoxia, hypotension
occur
Leading to death
within 24 hrs
Producing hemorrhagic
necrosis of the nodes
Primary infxn- lesions
in the intestine
accompanied by
hemorrhagic
lymphadenitis
Fever, N&V, abdominal
pain, bloody diarrhea,
ascites
G. Complications
1. Anthrax meningitis
2. Anthrax sepsis
H. Management
TREATMENT
Parenteral penicillin G -2 million units every 6 hrs, oral penicillin
for 7-10 day course
Sensitive to penicillin- can be treated with
erythromycin,tetracycline, or chloramphenicol
NURSING CARE
Careful hx. taking
Thorough Physical exam
Skin care, psychological and emotional support
Supportive measures
Report cases of anthrax
Page 28
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XI. ROCKY-MOUNTAIN SPOTTED FEVER
A. Important Information
1. It is a tick-borne disease.
2. Despite the name, the disease is not limited to the Rocky Mountains
but rather occurs throughout most of the U.S.
B. Causative agent: Rickettsia rickettsii
C. Incubation period: 2-14 days; average: 7 days
D. Period of communicability: Not directly transmitted from person-
person. The tick remains infective for life, commonly as long as 18
months.
E. Mode of transmission:
Bite of an infected tick
Contamination of breaks in the skin or mucous membrane with tick
feces
F. Signs and symptoms
1. Abrupt onset of fever
2. Severe headache, muscle aches, and vomiting
3. Other symptoms that are less common are abdominal pain,
swollen lymph nodes, cough, stiff neck, confusion, and coma.
G. Diagnostic
1. Complete blood count
- low white blood cell count
- low platelet count
- elevated liver function tests
Page 29
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
H. Management
PREVENTION
Children and adults who are outside in tick-infested areas
should wear long clothing and tuck the end of the pants into
the socks
Insect repellant should be applied to shoes and socks
Permethrin products are more effective against ticks than DEET
products.
Check for ticks attached to the skin every 2-3 hours while
outside, then check thoroughly once a day
Favorite hiding places for ticks are in the hair so check the
scalp, neck, armpits, and groin.
TREATMENT
Antibiotics such as doxycycline, tetracycline, or chloramphenicol.
Pregnant women should not take doxycycline or tetracycline
Since chloramphenicol is available in the US only in IV form,
pregnant women should be admitted to the hospital.
Page 30
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XII. SCARLET FEVER
A. Important Information
1. It is an acute, contagious bacterial disease characterized by a skin
rash and a strawberry tongue.
B. Causative agent: Group A beta hemolytic streptococcus (GABHS)
C. Period of communicability: from the point of infxn through the active
disease, and post disease in individuals with sinusitis or otitis media
D. Mode of transmission:
Airborne droplets
Contact with nasopharyngeal secretions
Ingestion of contaminated milk or other food
E. Signs and symptoms
Prodromal period Enanthema stage Exanthema phase
Appear 1-3 days
after exposure
High fever
Chills
Tachycardia
N&V
Headache
Abdominal pain
Malaise
Sore throat
Enlarged, reddened
tonsils
After 1
st
day, tongue is
coated and white with
red
Raspberry tongue-
pathognomonic sign
4
th
day- sloughs off
Red punctuate lesions
on the palate
Rash appear 12
hrs after
prodromal sx:
Pinhead-size red
lesions rash
cover the body
except for the
face
Last 4-10 days
Face is flushed
on the cheeks
with a cicumoral
pallot
After a wk,
desquamation
and peeling
begin on the
palms and soles
Pastias lines
Page 31
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
F. Diagnostic
1. Schultz-Charlton reaction skin test- skin test for the diagnosis of
scarlet fever, performed by the intradermal injection of human scarlet fever
immune serum; a positive reaction consists of blanching of the rash in the
area surrounding the point of injection.
2. Throat culture
G. Complication
1. Otitis media- inflammation of the middle ear, or middle ear
infection
2. Sinusitis - inflammation of the paranasal sinuses, which may be
due to infection, allergy, or autoimmune issues
3. Peritonsillar abscess- collection of infected material in the area
around the tonsils
4. Septicemia and hepatic damage
H. Management
GOALS
to prevent acute rheumatic fever
to reduce the spread of infection
to prevent poststreptococcal glomerulonephritis and
suppurative sequelae (eg, adenitis, mastoiditis, ethmoiditis,
abscesses, cellulitis), and
to shorten the course of illness.
TREATMENT
Penicillin remains the drug of choice
Page 32
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XIII. LYME DISEASE
A. Important Information
1. Lyme disease is caused by a bacterial infection that occurs due to a
bite of a tick.
2. It leads to fever, headache as well as a typical rash associated with
the disease.
B. Causative agent: Borrelia burgdorferi
C. Incubation period: 3-32 days
D. Period of communicability: No evidence exists of natural transmission
from person to person
E. Mode of transmission:
By the bite of ticks infected with Lyme disease bacteria. (Deer
tick)
F. Signs and symptoms
1. Red, slowly expanding "bull's-eye" rash (called erythema
migrans) pathognomonic sign
2. Fever, headache, stiff neck, muscle aches, and joint pain
3. Untreated- develop arthritis, including intermittent episodes of
swelling and pain in the large joints; neurologic abnormalities, such
as aseptic meningitis, facial palsy, motor and sensory nerve
inflammation (radiculoneuritis) and inflammation of the brain
(encephalitis); and, rarely, cardiac problems, such as atrioventricular
block, acute inflammation of the tissues surrounding the heart
(myopericarditis) or enlarged heart (cardiomegaly).
Page 33
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
G. Diagnostic
1. Bulls-eye rash is the best way to diagnose Lyme disease.
2. ELISA test to check the level of antibodies in the body against the
bacteria.
Second test includes Western blot
H. Management
PREVENTION
One should avoid getting into wooded, bushy as well as grassy
areas during warm months.
One should stick to trails when walking and not get diverted into
the grassy paths.
Wear protective clothing like socks, full sleeve shirts as well as
cover your legs to prevent ticks from sticking to your skin.
If one observes ticks sticking to their body, make sure they are
removed properly. Do not break the mouth parts from its body.
As it will still lead to transfer of bacteria into the blood.
Wear an insect repellent containing DEET for skin when moving
outdoors. Also, make sure you wear a cap and tie your long hair
properly to avoid ticks sticking to your scalp.
TREATMENT
For adults, early localized and early disseminated disease can be
treated effectively with doxycycline (100 mg twice daily)
Amoxicillin (500 mg 3 times daily), or cefuroxime axetil (500 mg
twice daily) for 14 days (range 1021 days for doxycycline and 14
21 days for amoxicillin or cefuroxime axetil).
Children less than eight years of age should be treated with
amoxicillin (50 mg/kg per day in 3 divided doses [maximum of 500
mg per dose]), or cefuroxime axetil (30 mg/kg per day in 2 divided
doses [maximum of 500 mg per dose]). For children 8 years of age,
the dosage of doxycycline is 4 mg/kg per day in 2 divided doses
(maximum of 100
mg per dose)
Page 34
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
DISEASE AFFECTING THE EYES
I. ACUTE CONJUNCTIVITIS
A. Important Information
1. Self-limiting viral infection: disappears in a weeks time even without
tx.
2. More common during the summer months
B. AKA: Sore eyes
C. Causative agent: Some are Streptococcus pneumonia,
Haemophilus influenza and Staphylococcus aureus
D. Period of communicability: from the time symptoms first appear up to
14 days
E. Mode of transmission:
Transmitted through eye discharges of pt
Contact with contaminated articles and in swimming pools
F. Signs and symptoms
1. Eyes are itchy, red and painful
2. Blurring of vision
3. May or may not have fever, headache and weakness or malaise
G. Diagnostic
1. Swab smear preparation and culture
H. Management
No definite drug of choice
Avoid using personal belongings ( towel, eyedrops, eye
cosmetics, sunglasses) of infected persons
Avoid crowded places or rubbing the eyes when itchy
Page 35
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
DISEASES AFFECTING THE CIRCULATORY SYSTEM
I. DENGUE FEVER
A. Important Information
1. Only the first person bitten by the mosquito will be affected
2. Never give Aspirin(ASA) to patient because it can aggravate
bleeding since Aspirin is a plate inhibitor. Also, can cause Reyes
syndrome.
3. Dengue cases usually peaks in the months of July-November and
lowest during the month of February-April.
4. It is an acute febrile disease caused by infection with one of the
serotypes of dengue virus, which is transmitted by mosquito genus
Aedes.
REMEMBER THIS:
D- Day biter
L- Low flying
S- Stagnant water
U- Urban
B. AKA: Breakbone fever; Hemorrhagic Fever; Dandy Fever;
Infectious Thrombocytopenic Purpura
C. Causative Agent: Arbovirus group B, 4 Serotypes(1, 2, 3, 4)
namely Flavivirus, Chikungunya, Onyong-onyong, and West Nile)
Flavivirus 1, 2, 3, 4 from a family of Togaviridae, it is the most
dangerous
D. Mode of Transmission: mosquito bite. The first 2 are biological
transmitters
1. Aedes aegypti in urban, day biting mosquito, appear 2 hrs after
sunrise & 2 hrs before sunset, breeds in stagnant water, it has fine dots
at the base of the wings and white bands on the legs and it is has low
flying movement
2. Aedes albopictus in rural areas
3. Cultex fatigans mechanical transmitter
Other contributory mosquitoes: Aedes polynensis, Aedes scutellaris
simplex
Page 36
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
E. Incubation Period: 3-14 days, commonly 7-10 days
F. Period of communicability: A day before the febrile period to the end
of it and it becomes infective from day 8-12 after the blood meal remains
infective throughout its life
G. Sources of Infection
1. Infected persons
2. Standing water
H. Incidence
1. Age any age, common among children and peaks to 4 9 years old
2. Sex both sexes can be affected
3. Season frequent during rainy season
4. Location prevalent in urban
I. Diagnostic
1. Torniquet test (Rumpel Leede Test) screening test, done by
occluding the arm veins for about 5 minutes, to detect capillary fragility.
With use of BP cuff, take the BP. Add the systolic and diastolic BPs
and then divide by 2.
Keep the cuff inflated for 6-10 minutes(child) or 10-15 minutes
(adult)
Count the petechiae formation on a 1 square inch (as big as a 5-peso
coin)
If there are 20 or more than 20/square inch = (+) for Dengue Fever
2. Platelet count (decreased) confirmatory test
Platelet count is 100,000/mm
3
or less
Less than 50,000/mm
3
or (+) bleeding need a blood transfusion
3. Hemoconcentration an increase of at least 20% in the hematocrit
or a steady rise in the hematocrit
4. Occult blood in stool
5. Hemoglobin determination
6. Serologic test/ Rapid diagnostic test/ Complement fixation
test can confirm dx of Dengue Fever
Page 37
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
J. Classification according to severity
Dengue Grade 1
(Classic Dengue
Fever)
Dengue Grade 2
(Dengue
Hemorrhagic
Fever)
Dengue
Grade 3
Dengue
Grade 4
(Dengue
Shock
Syndrome)
Hermans sign
(Pathognomonic sign)
general flushing of the
body, it starts at the
distal portion of
extremities, sparring
the axilla and chest
(+) tourniquet test
Non-specific
symptoms/Flu-like
symptoms:
abdominal pain,
anorexia, N&V, pain
behind the eyes and
joint pains
Maculopapular or
petechial rash
All signs of Grade
1
Spontaneous
bleeding from
the nose, gums,
and GIT are
present
All signs of
Grade 2
Circulatory
failure: weak
pulse,
narrow pulse
pressure,
low BP, cold
clammy skin
and
restlessness.
All signs
of Grade
3
Profound
shock
with
undetecta
ble BP
and pulse
K. Complications
Dengue Fever Dengue
Hemorrhagic Fever
Severe
Manifestations
Epistaxis(nose
bleeding);
menorrhagia
Gastrointestinal
bleeding
Concomitant
gastrointestinal
disorder (peptic
ulcer)
Metabolic acidosis
Hyperkalemia
Tissue anoxia
Hemorrhage into
the CNS or adrenal
glands
Uterine bleeding
may occur
Myocarditis
Dengue
encephalopathy
L. Management:
PREVENTION AND CONTROL
Health education
Early detection and treatment of cases will not worsen the
victims condition.
Treat mosquito nets with insecticides.
House spraying is advised.
Page 38
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Eliminate water by changing water in vases, destroying breeding
places of mosquitoes and keeping the water containers covered.
Avoid hanging too many clothes inside the house.
Case finding
TREATMENT
No specific antiviral drugs
Symptomatic Treatment for fever
IV infusion to prevent dehydration and replacement of plasma
Blood transfusion for severe bleeding
O2 therapy for patient in shock
Sedatives to allay anxiety and apprehension
NURSING MANAGEMENT
Patient should be kept in a mosquito-free environment to avoid
further transmission
Keep patient at rest during bleeding episodes
Monitor VS
To restore blood volume: Put patient in Trendelenburg position
For nose bleeding: Keep the patients trunk elevated; apply ice
bag to the bridge of the nose and to the forehead
Avoid Aspirin use
No isolation required
Observe signs of shock: slow pulse, cold clammy skin, prostration
and fall of BP
Avoid dark-colored foods
Page 39
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
II. MALARIA
A. Important Information
1. Known as the King of Tropical Disease
2. Infectious but not contagious
3. A person infected with Malaria remains a carrier for as long as the
organism remains in his blood in sufficient amount to infect mosquitoes.
4. It is an acute and chronic parasitic disease transmitted by the bite of
infected mosquitoes and is confined mainly to tropical and subtropical
areas.
REMEMBER THIS:
N- Night biter
H- High flying
F- Free flowing water
R- Rural
B. AKA: Ague, Bad air
C. Causative Agent: 4 Species of protozoa/ Protizoa of genus
plasmodia
Plasmodium
falciparum
Plasmodium
vivax
Plasmodium
malariae
Plasmodium
ovale
Malignant
tertian
Most serious
type
Development
of high
parasitic
densities in the
blood(RBC)
Cause
agglutination-
resulting to
microembolus
formation
Most common
Benign tertian
Non-life
threatening
except for
very young
and the very
old
Chills every
48 hours on
the 3
rd
onward
Regular
intermittent
Quartan
Non-life
threatening
Fever and
chills occur
every 72
hours, usually
on the 4
th
day
after onset
Regular
intermittent
rare
Page 40
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
in the Phil.
Irregular
remittent
D. Incubation period:
Plasmodium
falciparum
Plasmodium
vivax and ovale
Plasmodium
malariae
12 days 14 days 30 days
E. Period of communicability:
Plasmodium
falciparum
Plasmodium
vivax a
Plasmodium
malariae
Not more than a 1
year
1-2 years More than 3 years
F. Mode of Transmission: Bite of an infected Female Anopheles
Mosquito
Transmitted parenterally through blood transfusion
Rarely-shared contaminated needle
Rarely- transplacental
G. Diagnostic
1. Malarial smear- a film of blood is placed on a slide, stained and
examined microscopically
2. Rapid diagnostic test- blood test for malaria that can be conducted
outside the laboratory. It gives results within 10-15 minutes. It is done
to detect malarial parasite antigen in the blood.
H. Signs and Symptoms
1. Hemolysis pathologic change made by Plasmodium Falciparum
2. 3 stages of paroxysms: a) Cold stage- chills to extreme shaking,
myalgia(feelings of well-being in between), b) Hot stage- rapidly rising
high grade fever and c) Wet stage-profuse sweating
3. Hepatomegaly and Splenomegaly
4. stepladder like fever with chills-pathognomonic sign
5. Orthostatic hypotension
Page 41
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
I. Complication:
Cerebral Malaria- caused by blocked capillaries in the brain from
parasitized RBCs and rupture of RBCs in the brain
Manifestations: Changes in sensorium, seizures and severe
headache
Blackwater Fever- most dreaded complication of malaria
Caused by massive hemolysis, large amount of hemoglobin are
released into the plasma, spilling over into the urine and it
passage of reddish-black or mahogany colored urine
J. Management:
PREVENTION AND CONTROL
All malaria cases should be reported
A thorough screening of all infected persons from mosquitoes is
important.
Breeding places should be destroyed.
Home should be sprayed with insecticides
Use mosquito nets
Insect repellants should be applied
People living in malaria-infested areas should not donate blood
for atleast 3 years
Blood donors should be properly screened.
MEDICAL MANAGEMENT
Anti-malarial drugs are safe in all trimesters of pregnancy
Chloroquine Primaquine Sulfadoxine Quinine
Most potent drug
Acts on
Erythrocytic
stages
Not given to pt.
with Plasmodium
Acts on the
exo-erythrocytic
stage
For relapse of
P.vivax and
P.ovale
For
Chloroquine
-resistant
malaria
Drug of
choice
for
preg-
nant
women
Page 42
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
malariae(Quar-
tan)
Destroys the
merozoites of
the P.
Falciparum
NURSING MANAGEMENT
Patient should be closely monitored
Monitor I&O to prevent pulmonary edema
Monitor Serum bilirubin, BUN creatinine and parasitic count
Determine ABG and plasma electrolyte pt exhibits respiratory
and renal symptoms
Wear gloves
Provide comfort and psychological support
Cold Stage Hot Stage Diaphoretic/Wet stage
Provide blanket
Warm drinks
Warm bath
Tepid sponge
bath(TSB)
Alcohol rubs
Cold compress
Light loose
clothing
Keep pt dry
Increase fluid intake
Warm sponge bath
CLEAN BY DOH
C Chemically treated mosquito nets
L Larvivarous fish (carps)
E Environmental sanitation
A Anti mosquito soaps and repellants (basil soap)
N Neem tree (Oregano/Eucalyptus)
Page 43
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
DISEASES AFFECTING THE CENTRAL NERVOUS
SYSTEM
I. MENINGITIS
A. Important Information
1. It is an inflammation of the meninges of the brain and spinal cord as
a result of viral or bacterial infxn.
2. It is an acute contagious disease
3. Usually endemic which may become epidemic at anytime.
4. It involves 3 layers: Dura mater, Subarachnoid mater and pia
mater
B. AKA: Cerebro-spinal Fever; Spotted Fever
C. Causative agent:
Most common among neonates & infants Escherichia coli
Most common among children (5 months-5 years old)-
Haemophilus influenza
Most common among adults- Streptococcus Pneumoniae
Others: Neisseria meningitides for Meningococcemia, Streptococcus
agalactiae Listeria Monocytogenes, Staphylococcus species,
Salmonella species, Pseudomonas aeruginosa, Klebsiella pneumonia,
Mycobacterium tuberculosis, For Aseptic meningitis: Viral, Rickettsial,
Spirochetes, Fungal and Protozoa
D. Mode of transmission:
Droplet
Direct invasion via Otitis media, Mastoiditis and sinusitis
Hematogenous spread- producing blood, originating in or spread
by the blood.
Direct Inoculation Head injury/Skull fracture, Lumbar
fracture and neurosurgical procedures
E. Incubation period: It varies, extreme limits being set from 1-10 days
F. Diagnostic
1. Lumbar puncture- insertion of a needle into the lumbar
subarachnoid space and withdrawal of CSF, ICP can cause CSF to spurt
from the needle
Page 44
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Obtaining the CSF specimen
Taking x-rays of the spinal canal and cord
2. Therapeutic purposes
Reducing intracranial pressure
Introducing serum and other medications
Injecting an anesthetic agent
3. Gram-staining
4. Smear and blood culture
5. Smear from petechiae
6. Urine culture
G. Signs & Symptoms:
Sudden fever of 40
o
C
Alteration in consciousness
Drowsiness
Confusion- disorientation
Stupor- pain stimulus response
Visual disturbances: Blurring vision, diplopia(double vision)
and photophobia
Delirium, stupor and coma
Arrhythmia, irritability and tachycardia
Characteristics sign of meningeal irritation
Nuchal
rigidity
Opisthotonos
position
(+) Kernigs sign (+) Brudzinkis sign
Stiff neck
Neck
resistance
during
flexion
Hyperextension
of the back and
neck muscles
Resistance to full
extension of leg
at knee when hip
is flexed
Flexion of both
hips and knees
when back is
passively flexed
Signs of intracranial pressure
Bulging fontanels in infants
Page 45
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
N&V(projectile)
Severe frontal headache
Blurring vision
Alteration in sensorium
H. Complications
Subdural effusion- accumulation of fluid in subdural mater
Hydrocephalus
Deaf-mutism
Blindness
Otitis media, mastoiditis
Pneumonia or Bronchitis
Page 46
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
I. Management
PREVENTION
Immunization
HiB- for H. influenza
Pneumovaccine for S. pneumonia
BCG for M. tuberculosis
Proper treatment for otitis media, mastoiditis and sinusitis
MEDICAL MANAGEMENT
O2 therapy
IV antibiotics for 2 weeks: ampicillin, cephalosporin(ceftriaxone)
and aminoglycosides
Digitalis control arrythmias
Mannitol- to decrease cerebral edema
Anticonvulsant or sedatives- to reduce restlessness and
convulsions
Paracetamol
Acetaminophen helpful in relieving headache and fever
NURSING MANAGEMENT
Neuro assessment check level of consciousness
Watch out for deterioration of patients condition
Monitor fluid balance
Ensure adequate nutritional intake
Ensure comfort
Provide reassurance
Strict aseptic technique when handling patients with head
wounds or skull fractures
Isolation
Page 47
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
II. MENINGOCOCCEMIA
A. Important Information
1. Meningococci invade the bloodstream without involving the meninges.
B. AKA: Meningococcal Menigitis
C. Causative agent: Neisseria Meningitidis
D. Mode of transmission: same as meningitis
E. Incubation Period: 2-10 days with an average of 3-4 days
F. Diagnostic: same as meningitis
G. Signs and Symptoms
Purple rashes pathognomonic sign
Onset starts with nasopharyngitis followed by sudden attack of high-
grade fever with chills, N&V, malaise and headache
Petechial, purpuric or ecchymotic hemorrhages scatter over the
entire body
Adrenal lesions start to bleed into the medulla, extending to the
cortex
Waterhouse-Friderichsen syndrome is a combination of
meningococcemia and adrenal medullary hemorrhage
Is a rapid devt of petechiae that
become purpuric and ecchymotic
spots in association with shock
Runs in short course
Is fatal
Abrupt onset of hypotension and
tachycardia-septic shock
Death is within 10-12 hrs
H. Management: same as meningitis
Page 48
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
III. Encephalitis
A. Important Information
1. Inflammation of the brain tissues
2. Produces its characteristic effects upon the cranial and not the spinal
nerves
3. Resulting in abnormal functioning of the brain and spinal cord
B. AKA: Brain Fever
C. Causative agent: Mostly viral (arbovirus)
D. Mode of transmission: Bite an infected Culex mosquito
Becomes infected by biting an infected bird
Not transmitted from man-to-man
Does not carry the virus from humans
E. Incubation period: 5-15 days
F. Classification
Primary Encephalitis Secondary Encephalitis
Direct invasion of the CNS by a
virus resulting in an inflammatory
reaction
Acute nonsupurative which
follows or is part of some
infectious disease
Page 49
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
TYPES
a. Eastern equine encephalitis
(EEE)
Serious epidemic disease of
horses
Affects children under 5 years
of age
Can multiply in the Aedes
sullicitans mosquito
From horse
b. Western equine encephalitis
(WEE)
Milder and affects adults
From horse
c. St. Louis encephalitis
Gain entrance through olfactory
tract
Virus transmitted by the bite of
infected mosquito
Disease from birds
d. Japanese encephalitis
Bite of Culex triteaniorhynchus
which lives in rural rice-growing
and pig-farming regions
Breeds in flooded and stagnant
rice
Affects 5-10 years old
3 male: 1 female ratio
30-35% fatality rate
Peak during rainy season
(March-April) & (September-
October)
No specific tx
AKA: Post-infection
encephalitis
a) Post Infection Encephalitis
Usually a complication or
sequel to some viral diseases
like measles, chickenpox, and
mumps
b) Post-vaccinal encephalitis
Clients receives a vaccine,
most commonly with the anti-
rabies vaccine
G. Diagnostic Procedure
1. CSF analysis
2. Serologic test confirmatory test
90% confirmatory, done on the 7
th
day of illness
Diagnostic identification of antibodies in the serum
3. ELISA (IgM)
4. Polymerase chain reaction
Page 50
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
H. Signs & Symptoms
PRODROMAL PERIOD (1-4 days)
Fever
Headache
Dizziness
Vomiting
Apathy
Other S/Sx:
Chills
Sore throat
Conjuctivitis
Athralgia- joint pain
Myalgia-muscle pain
Abdominal pain
Encephalitic signs are:
Nuchal rigidity
Ataxia uncontrollable muscle contraction and twitching
Tremors
Mental confusion
Speech difficulties
Stupor
Hyper-excitability
Convulsions
Coma
Death
Cranial nerve paralysis are:
Ocular palsy
Ptosis- drooping of eyelids
Page 51
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Flaccid paralysis
Disturbances in:
Swallowing
Mastication
Phonation
Respiration
Facial and ocular movement
Respiration
Movements of the muscles of the eyes or face
H. Sequelae
Motor Disturbances Mental Disturbances Endocrine
Disturbances
Persistent
convulsions
Parkinsonian
syndrome or
paralysis agitans
Epilepsy
Mental dullness
Mental deterioration
Lethargy
Mental depression
Sleep disturbances
May grow
either fat or
thin
Sexual
interest or
activity is lost
I. Management:
PREVENTION
Vector control (same as Dengue)
TREATMENT
Symptomatic and supportive
Convulsions must be controlled
Proper disposal of respiratory secretions
TSB
Oral care
Mouth gag and protective devices, such as bedrails are available
Monitor I&O
Record beginning, duration, and frequency of convulsion
Gently turn patients head on side in case of convulsion
Monitor neurologic signs:
GCS
Motor and sensory
VS
NURSING MANAGEMENT
Provide comfort
Prevent complications
Monitor I&O
Page 52
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IV. TETANUS
A. Important information
1. Infectious but not contagious
2. Brought about by direct inoculation of material containing the causative
agent
3. Always a serious disease
4. An infectious disease with prominent systemic neuromuscular effects
manifested by generalized spasmodic contractions of the skeletal muscles
5. Exotoxins involved are:
Tetanospasmin responsible for muscular spasm
Tetanolysin responsible for the destruction of the RBC
B. AKA: Lockjaw
C. Causative agent: Clostridium tetani
D. Mode of transmission:
Acquired from any type of wound contaminated by dust, soil, or
animal excreta
Rugged traumatic wounds and burns such as scratch or bite, tooth
decay and open fractures
Through cleaning ear canal with dirty or rusty hairpin
Dental extraction
Ear piercing
Circumcision
Umbilical stump in newborns
Babies delivered at home with faulty cord dressing
Babies delivered by mothers without tetanus toxoid immunization
Page 53
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
E. Sources of infection:
1. Animal or human feces
2. Soil and dust
3. Items contaminated with the MO
F. Fatality rate: 60% if unimmunized and death within 10 days
G. Incubation period: 5-10 days
H. Signs & Symptoms
TETANUS NEONATORUM- for neonate/infant
feeding and sucking difficulty
Sucking results in spasm and cyanosis
Jaw becomes stiff
Excessive and voiceless crying
Muscle spasm or convulsions provoked by stimuli
Flaccidity, exhaustion and death may occur
OLDER CHILDREN AND ADULT
Increased muscle tone and spasm near the wound
Hyperactive deep tendon reflexes, tachycardia, profuse sweating,
fever, painful involuntary contractions
Trismus- neck and jaw muscle rigidity and last symptom to
disappear
Risus sardonicus/Sardonic grin pathognomonic sign
grinning expression
facial muscle spasm
Opisthotonos position- arching of the trunk
Board-like abdomen
Convulsion cyanosis and asphyxiation (suffocation)
Laryngospasm resulting to respiratory distress
Vertebral fracture may occur during severe spasms, yielding to coma
and death
Death occurs during the first 10 days of the disease
I. Complications
Page 54
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Resulting from
laryngospasm and
involvement of the
muscles of respiration
1. Pneumonia
2. Hypoxia
3. Atelectasis and pneumothorax
4. Traumatic glossitis and
microglossia
Changes related to SNS 1. Transitory hallucinosis
2. Cardiac standstill and bradycardia
Due to trauma 1. Laceration of the tongue
2. Intramuscular hematoma
Fracture of the spine and ribs
Septicemia
J. Diagnostic Procedure
CBC
Creatinine and Potassium
Wound Gram Stain
Culture Stain
K. Management
TREATMENT & PREVENTION
Active immunization with tetanus toxoid for adults and pregnant
women
DPT for babies and children
Active immunization with
tetanus toxoid
6 wks after birth (together with
DP): 0.5 ml for 3 doses (4-8
wk interval)
Tetanus toxoid for non
pregnant women
1
st
dose Given
anytime, 0.5
ml IM
2
nd
dose After 1 month
3
rd
dose After 6 months
4
th
dose After 1 year
5
th
dose After another
year
Passive immunization
- Anti-tetanus serum (ATS) for horse
- Tetanus Immune Globulin (TIG) for human, within
24 hours after wound with skin test
MEDICAL CARE
Penicillin(DOC)
Diazepam and Phenobarbital muscle relaxant
Wound debridement
If admitted: O2, NGT and tracheostomy
Antibiotic prophylaxis are Penicillin, Erythromycin and
Tetracycline
NURSING CARE
Maintain adequate airway
Cardiac monitoring
Maintain IV line
Wound care
Avoid stimulation
Page 55
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
V. Rabies
A. Important information
1. It is a specific, acute infectious/viral disease.
2. It is preventable but not curable.
3. Always fatal after it has once developed
4. Considered as the deadliest disease because it is universally fatal
5. Seen in dogs (most common), cats (next common), horse and cattle
Dumb stage Complete change of disposition, tries to hide, is
nervous and apprehensive, being unable to
remain long in one place or position
Furious stage Gradually gets restless and barks in a peculiar,
characteristic manner (head and snot pointed
toward the sky, haunting and moaning in
sound). Starts running aimlessly around
Death When hydrophobia (fear of water) develops, the
dog dies within 14 days
B. AKA: Rabies encephalitis; Infectious hydrophobia; Lyssa
C. Causative agent: Rhabdovirus/Lyssavirus (bullet-shaped)
D. Mode of transmission: transmitted by direct inoculation with infected
saliva usually by bites or scratches from man.
E. Incubation period: 10-15 days(human), 1 wk- 7 months (dogs)
The closer the bite to the brain, the shorter the incubation
F. Period of Communicability: The patient is communicable from 3-5 days
before the onset of symptoms until the entire course of illness.
G. Signs & Symptoms:
Negri bodies-pathognomonic sign
Present in hippocampus, basal ganglia, pons, medulla and
salivary gland
Page 56
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Invasion
phase/Prodromal
phase
Excitement
phase/Neurological
phase
Terminal
phase/Paralytic
phase
Coma, Death
Non specific s/sx
Pain and/or
paresthesia at the
site of
inoculation/bite
Sensitivity to
light, sound, and
temperature
Body malaise
Mild difficulty in
swallowing may
be felt
Marked excitation
and apprehension
Objective signs of
CNS dysfunction
occur
Muscle
contraction/spasm
Maniacal behavior:
eyes are fixed and
cold clammy skin
Sense of terror
Severe and painful
spasm of muscles
of the mouth,
pharynx, and
larynx induced by :
swallowing, mere
sign of water or
food and even a
light breeze in the
air
Making the patient
salivate
profusely/frothing
and fearing
drinking, although
thirst is great
Patient
becomes quiet
and
unconscious
Loss of bowel
and bladder
control
Spasms cease
with
progressive
paralysis
Tachycardia,
labored or
irregular
respirations
Ventilatory
assistance
prolongs the
clinical course
of the disease,
rarely will they
affect the
outcome of
the disease
Due to:
Respiratory
paralysis
Circulatory
collapse
Heart
failure
H. Diagnostic
1. Clinical observation definitive history of exposure (bite by an animal
or close contact with animals) and development of characteristic s/sx of
rabies
2. Virus isolation from saliva or throat
3. Fluorescent Rabies Antibody (FRA)- most definitive diagnosis
4. Negri bodies in the dogs brain a (-) result does not absolutely
exclude infection
I. Management
TREATMENT
Page 57
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Thorough washing of wound from bite or scratch with soap and
running water for atleast 3 minutes
Provide tetanus prophylaxis (ATS &TT) and antibacterial therapy
aside from anti-rabies vaccines
PREVENTION/MANAGEMENT OF THE BITING DOG
Restrain the dog with a leash
or confine in a cage
Observe the dog for 14 days
for any signs of rabies or
submit the dog to a licensed
veterinarian for observation
Do not kill the dog, it is better
to wait for the dog to die
naturally
If the dog dies within 14 days,
call a veterinarian for proper submission of sample to the nearest
diagnostic laboratory
RECOMMENDED POST-EXPOSURE PROPHYLAXIS FOR RABIES (WHO)
Category I Category II Category III
Touching or
feeding
animals
Licks on intact
skin (i.e. no
exposure)
Post-exposure
measures:
none
Nibbling of
uncovered skin
Minor scratches or
abrasions without
bleeding
Post-exposure
measures:
Immediate
vaccination
Local treatment
of the wound
Single or multiple
transdermal bites
or scratches
Licks on broken
skin
Contamination of
mucous membrane
with saliva from
licks
Exposure to bats
Post-exposure measures:
Immediate
vaccination
Immediate
administration
of rabies
immunoglobulin
Local treatment
of the wound
NURSING CARE
Isolation of the patient
Provide comfort for the patient
Provide a restful environment
Patient should not be bathed
There should not be any running water in the room or within
hearing distance
If IV fluid has to be given, wrap and secure IV in the vein
Provide assurance and emotional support to the members of the
family
Page 58
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VI. POLIOMYELITIS
A. Important information
1. An acute paralytic condition which is very contagious and infectious.
2. Characterize by changes in the central nervous system.
3. Disease of the lower motor neuron involving the anterior horn cells.
4. No patient dies except if respiration is affected by involvement of the
spinal cord. No matter how severely paralyzed, if respiration is not
involved the prognosis is good.
B. AKA: Infantile Paralysis; Heine-Medin Disease
C. Causative agent: Polio virus (Legio debilitans)
3 strains of the virus are: Brunhilde, Lansing and Leon
D. Mode of transmission:
Ingestion
Fecal-oral route (Food- or water- borne, Vector borne)
Ingestion of infected throat secretions
Direct and indirect contact with respiratory secretions and feces
E. Incubation Period: 7-12 days
F. Period of communicability: First 3 days-3 months of illness
Most contagious: 3-4 days before onset of symptoms
G. Predisposing causes:
1. Age 60% below 10 years old
2. Sex 3 Males: 2 Females ratio
3. Heredity not heredity
4. Environment and hygienic condition rich are more often spared than
the poor, excessive work, strain and marked overexertion
H. Signs and Symptoms
TYPES OF POLIOMYELITIS
Silent type/
Asymptomatic
type
Abortive/
Minor Illness of
Polio
Non-paralytic/
Pre-paralytic
type/ Major
Illness of Polio
Paralytic type
(-) clinical
manifestations
Does not
invade the
Abortive sx
plus:
Non-paralytic sx
plus:
Page 59
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Poliomyelitis CNS yet
Non-specific
s/sx
Patient
recovers
within 72 hrs
Muscle spasms:
pain on neck,
beck, arms, legs
and abdomen
Inability to place
head between
knees
(+) Pandys
test-done on
the CSF
(cerebrospinal
fluid) to detect
the elevated
levels of
proteins (mainly
globulins)
Last about a
week
Paralysis
(+) Kernig and
Brudzinki tests
Muscle weakness
Hypersensitivity
to touch
(+) Hoynes sign-
positive the head
falls back limply
TYPES OF PARALYTIC
Spinal paralytic Bulbar Bulbospinal
Involvement of motor
neurons in the spinal
cord
Paralysis of one or
both lower
extremities
Autonomic
involvement
Respiratory difficulty
Involvement of motor
neurons in the
brainstem
Paralysis of the facial,
pharyngeal, and ocular
muscles
Mostly affects CNS IX
and X
Respiratory and cardiac
abnormalities
Involvement of the
neurons in the
brainstem and spinal
cord
Together with Bulbar
paralysis, they are
more serious
compared to spinal
paralysis especially if
respiratory muscles
are involved
I. Diagnostic
1. Isolation of the virus from throat washing
2. Stool culture
3. Culture from the CSF
J. Complication
1. Respiratory failure
2. Circulatory collapse
3. Electrolyte imbalance
4. Bacterial infxn
5. Urinary problems
6. Abdominal distention
K. Management
PREVENTION
Salk vaccine killed viruses given IM
Page 60
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Sabin vaccine- attenuated live virus administered orally
TREATMENT
Analgesic for headache and pain
Moist heat
Bed rest
Rehabilitation therapy
NURSING CARE
Enteric isolation
Observe for signs of paralysis and other neurologic damage
Neurologic assessment OD (at least)
Check VS especially if brainstem is affected
Provide good skin care; prevent pressure sores
Give sufficient fluids to prevent fecal impaction
Emotional support
Maintain good oral and skin care
Page 61
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VII. BOTULISM
A. Important information
1. It came from the Latin word botulus (sausage).
2. It is a rare but serious paralytic illness caused by a potent neurotoxin.
B. Causative agent: Clostridium botulinum; Canned-good bacillus
Characteristic of Clostridium botulinum: Gram(+), spore-forming,
anerobic, natural habitat is the soil. Spore withstands boiling for several
hours. Botulinal toxin is the most potent toxin known to man
C. Human forms of botulism
TYPES OF BOTULISM
Food-
borne/Classical
botulism
Wound/ Cutaneous
botulism
Infant botulism
Results from
ingestion of
inadequately
cooked
contaminated
food containing
botulinal toxin
Especially with
low-acid content
E.g. are canned
goods, sausage
and preserved
foods
Manifestations
begin 18-36 hrs
after eating
contaminated
food
Manifests with
skin ulcers as a
deposition of
toxin in the area
Also known as
Hypotonic(Flopp
y) Infant
Syndrome
Commong among
infants who ingest
or place objects in
their mouth with
dust or soil
contaminated with
the toxin.
Constipation,
feeble/weak cry,
depressed gag
reflex, inability to
suck
Can cause death
by weakening or
paralyzing tongue
and pharyngeal
muscles
innervated by CNs
IX to XII
D. Signs & Symptoms
Flaccid paralysis
Generalized muscle weakness leading to paralysis
Diplopia, blurred vision
Ptosis, dry mouth, dysphagia and dysathria
Page 62
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
E. Complications
1. Pneumonia
2. UTI
3. Pulmonary embolism
4. Decubitus ulcer
5. Flexion contractures
F. Management
PREVENTION
Persons who do home canning should follow strict hygienic
(sterile) procedures to reduce contamination of foods
Oils infused with garlic and herbs should be refrigerated. Potatoes
which have been baked while wrapped in aluminum should be
kept hot until served or refrigerated
Persons who eat home-canned foods should consider boiling the
food for 10 minutes before eating it to ensure safety
Because honey can contain spores of Clostridium botulinum, it
should not be fed to children less than 12 months old
TREATMENT/NURSING CARE
Supportive care is needed with particular attention to respiratory
a nutritional needs
Emetics and gastric lavage for food-borne botulism
Exploration and debridement for wound botulism
If diagnosed early, food-borne and wound botulism can be
treated with an antitoxin
If respiratory failure and paralysis that occur with severe
botulism may require a patient to be on a ventilator for weeks
(intubation)
Page 63
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VIII. TOXIC SHOCK SYNDROME
A. Important information
1. It is an acute bacterial infxn that may progress rapidly to severe
shock.
2. May become systemic
B. Causative agent: Staphylococcus aureus
C. Mode of transmission:
Prolonged placement of tampons or barrier contraceptives
D. Signs and symptoms
1. Onset:
High fever
Headache
Sore throat
Nonpurulent conjunctivitis
Lethargy
Confusion
Vomiting
Diarrhea
Sunburn like skin rash
2. within 48 hrs
Syncope
Orthostatic hypotension
Diminished urine output
Shock
Peripheral and pulmonary edema
Hepatitis
Myolysis-breakdown of muscle tissue
3. after 3-7 days
Skin sloughs off on the palms and soles
Page 64
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
E. Complication/Leading to:
1. Neurologic deficit
2. Renal failure
3. Respiratory failure
4. Death
F. Diagnostic
1. Clinical examination
2. Biopsy confirmation test
3. Pap smear and colposcopy
4. Acetic acid-whitish color
G. Management
TREATMENT
Antibiotics to treat causative organism
Fluid replacement
Hygiene counseling including changing tampons more frequently
Good handwashing
Appropriate removal of diaphragm (within 24 hr) and sponge
(within 30 hr) after intercourse
Page 65
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IX. TOXOPLASMOSIS
A. Important information
1. It is an intestinal coccidium that parasitizes members of the cat family
as definitive hosts and has a wide range of intermediate hosts.
B. Causative agent: Toxoplasma gondii
C. Reservoir
Cats
D. Mode of transmission:
Ingestion of cysts on focally contaminated fingers or in food
Transplacental
E. Signs and symptoms
1. Confusion, headache, lethargy, low-grade fever
2. Focal manifestations of weakness, ataxia, speech problems, apraxia,
seizures, and sensory changes
3. Multiple brain abscesses
4. Congenitally infected children may suffer impaired vision and mental
retardation
5. For immunosuppressed pts may have CNS disease (encephalitis)
F. Diagnostic
1. Serology
2. Histologic examination of tissues
G. Management
TREATMENT
Pyrimethamine
Sulfadiazine
Leucovorin or clindamycin
Symptomatic tx
Page 66
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
X. CREUTZFELDT-JAKOB DISEASE
A. Important information
1. It is a rare, fatal brain disease that produces progressive dementia,
myoclonus, and distinctive electroencephalographic (EEG) changes.
2. Two separate mechanisms: genetic and infectious.
B. AKA: Mad cow disease
C. Causative agent: Virion, slow virus and prion
D. Incubation period: 4-21 yrs
E. Mode of transmission:
Ingestion of infected beef
F. Incidence
1 per million worldwide
G. Signs and Symptoms
1. Weight loss, anorexia, insomnia, malaise, and dizziness for period of
wks months
2. Early stage: Progressive memory loss, visual impairment, and
dysphagia
3. Within few wks or months progressive dementia, marked
deterioration
4. Myclonus (twitching) is present
H. Diagnostic
1. EEG- sharp waves and spikes
2. Polyclonal antibody in CSF
3. CT Scan- rule out mimic sx
Page 67
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
4. MRI- to identify lesions in the basal ganglia
5. Brain biopsy or autopsy definitive dx
I. Management
TREATMENT
No effective tx
Palliative and supportive care
Prevention of injury
NURSING CARE
Psychological and emotional support
Conventional methods of sterilization do not destroy the prion
Isolation is not necessary
Page 68
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XI. EBOLA
A. Important information
1. It is a viral haemorrhagic fever and one of the most virulent viral
diseases known to humankind.
2. Severe and often deadly illness that can occur in humans and
primates (monkeys, gorillas).
B. AKA: Ebola Hemorrhagic Fever
C. Causative agent: Ebola virus
D. Incubation period: 2 - 21 days
E. Mode of transmission:
close contact with the blood, secretions, organs or other bodily fluids
of infected animals
infected chimpanzees, gorillas, fruit bats, monkeys, forest antelope
and porcupines found dead or ill in the rainforest
F. Signs and Symptoms
1. sudden onset of fever, intense weakness, muscle pain, headache
and sore throat
2. vomiting, diarrhoea, rash, impaired kidney and liver function
3. both internal and external bleeding
G. Diagnostic
1. enzyme-linked immunosorbent assay (ELISA)
2. antigen detection tests
3. serum neutralization test
4. reverse transcriptase polymerase chain reaction (RT-PCR) assay
5. virus isolation by cell culture.
Page 69
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
H. Management
PREVENTION
Avoid areas in which there are epidemics. Wear a gown, gloves,
and mask around sick patients. These precautions will greatly
decrease the risk of transmission.
TREATMENT
Patients are frequently dehydrated and in need of intravenous
fluids or oral rehydration with solutions containing electrolytes.
No specific treatment or vaccine is yet available for EHF
Bleeding problems may require transfusions of platelets or fresh
blood.
Page 70
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
DISEASES AFFECTING THE RESPIRATORY SYSTEM
I. DIPHTHERIA
A. Important information
1. An acute contagious disease
2. Characterized by a generalized systemic toxemia emanating from a
localized inflammatory focus.
3. Infants born of immune mothers remain for the first 6 months of life.
4. One attack does not necessarily confer lifelong immunity.
5. It is an acute bacterial disease that can infect the body in two areas:
the throat (respiratory diphtheria) and the skin (skin or cutaneous
diphtheria).
B. Causative agent: Corynebacterium diphtheria(Klebs-Leoffler
bacillus)
It is a gram (=), non-sporulating, aerobic, unstable and easily
destroyed by light, heat and aging
3 strains are: a) Gravis(severe)- most severe in Europe, b)
Mitis(mild)-produces lesions extending to the larynx and lungs, and
c) Intermedius (intermediate) has tendency to bleed
C. Incubation period: 2-5 days
D. Period of communicability: More than 2-4 wks (untreated pt.), 1-2
days (treated pt.)
E. Source of infection:
Discharges of the nose, pharynx, eyes and lesions of infected
persons
F. Mode of transmission:
1. Direct contact with contaminated secretions
2. Indirect transmission from drinking fountains, cups, toilet seats,
toys and infected milk supplies
G. Predisposing Factors
1. Nose & Throat operation
2. Economic status
3. Lack of proper nutrition
Page 71
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
4. Overcrowding
H. Diagnostic
1. Nose & Throat swab
2. Virulence test
3. Shick test- diagnostic test designed to evaluate susceptibility to
diphtheria
4. Moloney test- one for detection of delayed hypersensitivity to
diphtheria toxoid.
5. Loeffler slant
I. Types
Nasal Tonsilar Facial
Nasopharyngeal
Laryngeal Wound or
cutaneous
diphtheria
Foul-
smelling
serosanguin
ous
secretions
from the
nose
Low fatality
rate
Lesions to
the tonsils
Most severe
type
Cervical lymph
nodes swollen
Bulls neck
Marked degree
toxemia
Fetid breath
Common in
children
ages 2-5
yrs old
Increased
respirations
Moderate
hoarseness
until it
becomes
lost
Affects
the
mucous
mem-
brane
Affects
any
break
on the
skin
J. Signs and Symptoms:
Feeling of fatigue
Malaise
Slight sore throat
Forming necrosis
Grayish thickened membrane
becomes dull white
Cervical adenitis with pain
Page 72
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Swollen neck (Bulls neck) form
Difficulty in breathing
Husky voice
Increased heart rate
Stridor
Nasal discharge (foul-smelling)
Palate swelling
Low-grade fever
K. Complications
1. Myocarditis most common
2. Polyneuritis
3. Asphyxiation (suffocation)
4. Otitis media
5. Bronchopneumonia
L. Management
PREVENTION
Mandatory DPT immunization of babies only effective to
control diphtheria
3 doses of soluble toxoid at 4-8 wks interval to stimulate
own antitoxin
Report Diphtheria cases
Isolate pt. for 14 days
Avoid contact
Children under 5 years should be given boosters of diphtheria
tetanus vaccine
TREATMENT
Penicillin-treats respiratory diphtheria
Antitoxin
Skin test before administration of anti-toxin
Fractional doses for (+) cases
0.05 ml (1:20 dilution) Subcutaneously
0.05 ml (1:10 dilution) Subcutaneously
0.10 ml undiluted Subcutaneously
0.20 ml undiluted Subcutaneously
0.50 ml undiluted IM
0.10 ml undiluted IV
Note: 15 minutes interval, (-) reaction give after an hr
Erythromycin, 40 mg/kg bw in 4 doses for x 7-10 days
Supportive therapy
tracheostomy done for laryngeal obstruction
Page 73
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Bed rest
Oxygen inhalation
Adequate nutrition and Fluid & Electrolyte balance
NURSING CARE
Full bed rest for 2 wks
Pt. not permitted to bathe by himself
Avoid exertion during defecation
Soft diet recommended
Encourage to dink fruit juices
Apply Ice collar to the neck
Nose & Throat care
Page 74
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
II. PERTUSSIS
A. Important information
1. It is an infectious disease characterized by repeated attacks of
spasmodic coughing which consists of a series of explosive expirations
2. Produces a crowing sound whoop and usually followed by vomiting
B. AKA: Whooping Cough
C. Causative agent: Bordetella pertussis
D. Incubation period: 7-14 days
E. Period of communicability: 7 days after exposure to 3 wks after typical
paroxysms
F. Mode of transmission:
Direct contact and droplet
Indirectly through soiled linens and contaminated particles
G. Sources of Infection:
Nose & throat secretions of infected persons
H. Incidence
Highly in infants
1st attack produces lifetime immunity
2
nd
attack causing whooping cough syndrome
I. Signs and Symptoms
Catarrhal stage Paroxysmal stage Convalescent stage
Non-specific sx:
mucoid rhinoria,
sneezing,
lacrimation, dry
bronchial cough
Irritating cough
Lasts for 1-2 wks
Occurs on 7
th
-14
th
day
Spasmodic cough
5-10 coughs in 1
expiration
Loud, crowing
inspiratory whoop
and choking on
mucus that causes
vomiting
Paroxysmal coughing
induce hemorrhage
Face becomes
Gradual decrease in
the paroxysms of
coughing
Vomiting ceases
After 6 wks from the
onset, attack
subsides
Page 75
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
cyanotic, Distended
face and neck veins,
bulge eyes, tongue
protrudes
Convulsion result of
intracranial
hemorrhage
Lasts 4-6 wks
J. Complication
1. Atelectasis-lung collapse
2. Convulsions
3. Otitis media
4. Bronchopneumonia most dangerous complication
5. Severe malnutrition and starvation
K. Diagnostic
1. Nasopharyngeal swabs
2. Sputum culture
3. CBC (leukocytosis)
K. Management
PREVENTION
Report pertussis cases
Pt should be isolated 4-6 wks
Public education for active immunization
TREATMENT
Supportive therapy
Fluid and Electrolyte replacement
Adequate nutrition
Oxygen therapy
NURSING CARE
Isolation and medical sepsis
Pt should not be left alone-paroxysms
Ready suctioning equipment
Protect pt from drafts, sunshine & fresh air are important
Child should be kept as still & quiet
Provide warm baths
Keep bed dry and free from soiled linens
Monitor I&O
Page 76
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
III. INFLUENZA
A. Important information
1. It is an acute viral infectious disease affecting the respiratory system
B. AKA: La Grippe
C. Causative agent: RNA-containing myxoviruses type A, A-prime, B
and C
D. Incubation period: 24-48 hours
E. Period of communicability: until 5
th
day of illness, up to 7
th
day in
children
F. Mode of transmission:
Airborne
Direct contact with the infected droplet
Persists for hrs in dried mucus
G. Signs and Symptoms
Onset- chilly sensation, hyperpyrexia, malaise, sore throat, coryza,
rhinorrhea, myalgia and headache
Severe back pain
Severe sweating
Gastrointestinal sx. and vomiting
Worst sx last from 3-5 days
H. Complication
Viral Bacterial
1. Hemorrhagic pneumonia
2. Encephalitis
3. Reyes syndrome
4. Myocarditis or heart failure
5. Sudden infant death
syndrome
6. Myoglobinuria
1. Otitis media
2. Sinusitis
3. Pneumonia
Page 77
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
I. Diagnostic
1. Blood exam
2. Oropharyngeal washings or swabs
3. Viral serology
a) Complement fixation test
b) Hemo-agglutination test
c) Neutralization test
J. Management
PREVENTION
Immunization
Avoid crowded places
Public education
Annual vaccination for elderly, poor immunity and with conditions
such as diabetes and lung, kidney, heart or liver disease
TREATMENT
No specific tx
Advice to stay home
Oral fluid intake
Paracetamol- to relieve fever and headache
Aspirin, unless contraindicated (not given to children below 16
years of age)
Ibuprofen anti-inflammatory
Tepid sponge bath
Limit strenuous activity
Watch out for complications
Page 78
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IV. AVIAN INFLUENZA
A. Important information
1. It is recognized both as an emerging and re-emerging viral infection
2. It is an infectious disease of birds ranging from mild to severe form of
illness
B. AKA: Bird flu
C. Causative agent: Avian influenza virus H5N1; Influenza virus A -from
Orthomyxoviridae family
D. Incubation period: 3-5 days
E. Source of infection:
Viruses that normally infect only birds and less commonly pigs.
F. Mode of transmission:
Spreads in the air and in manure
Through contaminated feeds, water, equipment and clothing
Cats-possible vectors for H5N1 strains of avian flu
G. Signs and Symptoms
Fever
Sore throat
Cough
Muscle pain
Sore eyes
Severe cases- pneumonia or difficulty breathing
H. Management
PREVENTION
Influenza tests
Yearly vaccination of poultry workers
Rapid destruction
TREATMENT
Antiviral drugs
Vaccines- take at least 4 months to produce and be prepared for
each subtype
NURSING CARE
Patient should be isolated
Early recognition of cases during outbreak among poultry
Utilize personal protective equipment
Page 79
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
V. SEVERE ACUTE RESPIRATORY
SYNDROME
A. Important information
1. It is confirm that a novel coronavirus is the primary cause of the
disease
2. It was 1
st
reported in China in November 2002, with over 8,300 cases
and 812 deaths reported by the beginning of July 2003
3. 1
ST
Case in the Phil on April 11, 2003 in a Caucasian business
commuter between Hong Kong and Manila
B. AKA: SARS
C. Causative agent: Novel human coronavirus
D. Incubation period: 2-10 days but may be long as 13 days
E. Mode of transmission:
Direct
Contact with infectious droplets
Casual and social contact - result of intense exposure to a case of
SARS
Contamination of inanimate materials (Infectious respiratory
secretions or body fluids
F. Signs and symptoms
1. High grade fever < 38
o
C
2. Headache and overall feeling of discomfort and body aches
3. Mild respiratory symptoms at the onset: after 2 days, dry cough and
respiratory difficulty
Page 80
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
G. Management
PREVENTION
Early tx is the key, consult a doctor
Build up good immunity
Practice good personal hygiene
Wear a mask if develop a runny nose, sore throat or cough
Wear a protective mask
Wash hands properly and keep them clean
TREATMENT
No specific tx
Empiric therapy
Consultation
SARS CLINICAL COURSE MANAGEMENT
Difficult to decide when will the SARS patient to be discharge in
an appropriate time
SARS appear to have lingering after-effects once the acute phase
of the disease ends
Psychosocial aspects of this illness should not be
underestimated
Page 81
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VI. TUBERCULOSIS
A. Important information
1. One of the most communicable diseases which tends to run a chronic
course.
2. Badly nourished, neglected and fatigued individuals are more prone
than their healthier counterparts.
3. Susceptibility is highest in children under 3 years.
4. Primary infection usually does not develop into a full blown clinical
disease; it is usually followed by a period of latency, until such time
when there is reinfection (phthisis).
Endogenous reinfection if primary infection does not entirely
heal but rather spreads
Exogenous reinfection reinfection from outside the pts body
5. Active PTB commonly involves the upper lobe of the lung, the apices
or the subapical region.
6. Classified as either pulmonary or extra-pulmonary TB.
7. It is a chronic, subacute or acute respiratory disease commonly
affecting the lungs characterized by the formation of tubercles in the
tissues which tend to undergo caseation, necrosis and calcification.
B. AKA: Kochs Disease; Phthisis; Consumption Disease
C. Causative agent: Mycobacterium tuberculosis and M. africanum in
humans
M. bovis in cattle
D. Incubation period: 2-10 wks
E. Period of communicability: Pt. is capable of discharging the organism
all throughout his/her life if remains untreated. It is highly
communicable during its active phase
F. Mode of transmission:
It is transmitted through inhalation directly into the lungs from
contaminated air
Direct or indirect contact with infected persons
Coughing, sneezing or kissing
Contact with contaminated eating or drinking utensils
Through skin lesions (rarely)
G. Sources of infection:
Sputum
Blood from hemoptysis
Nasal discharge
Page 82
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Saliva
H. Quantitative Classifications of Tuberculosis
1. Minimal characterized by small lesions without demonstrable
excavation that are confined to a small part of one or both lungs.
2. Moderately advanced
a. One or both lungs may be involved.
b. The volume affected should not extend to one lobe.
c. The total diameter of the cavity should not exceed four
centimeters.
3. Advanced characterized by lesions that are more extensive than
moderate
I. Clinical Classification
1. Inactive TB
a. Symptoms of tuberculosis are absent.
b. Sputum is negative for tubercle bacilli after repeated
examinations.
c. There is no evidence of cavities on chest x-ray.
2. Active
a. The tuberculin test is positive.
b. X-ray of the chest is generally progressive.
c. Symptoms due to lesions are usually present.
d. Sputum and gastric contents are positive for tubercle bacilli.
3. Activity not determined
Activity has not been determined from a suitable period of
observation or adequate laboratory and x-ray studies.
J. Signs and symptoms
1. Afternoon rise in temperature
2. Night sweating
3. Body malaise and weight loss
4. Dry to productive cough
5. Dyspnea and hoarseness of voice
6. Hemoptysis coughing up blood
ATS
CLASS
EXPO
SURE
PPD CXR Active
Disease
0 - - - - No
exposure
1 + - - - TB
Exposure
2 + + - - Tb
Infection
3 + + + + PTB
active
4 + + + - Previous
PTB
disease
5 + + + PTB
suspect
Page 83
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
7. Occasional chest pains
8. Ghons complex pathognomonic sign
9. Sputum positive for AFB
K. Diagnostic
1. Sputum analysis for Acid Fast Bacilli (confirmatory)
2. Chest x-ray-most definitive test
3. Tuberculin testing
a. Mantaux test (PPD)
L. Management
PREVENTION AND CONTROL
Submit all babies for BCG immunization
Avoid overcrowding.
Improve nutritional and health status.
Advise persons who have been exposed to infected persons to
receive the tuberculin test and, if necessary, chest x-ray and
prophylactic isoniazid.
TREATMENT
Page 84
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Short-course chemotherapy consisting of isoniazid (INH), rifampicin,
pyrazinamide (PZA) and ethambutol may be given for a period of six
months.
Patients with drug resistance may be given second-line drugs such
as capreomycin, streptomycin, cycloserine, amikacin and quinoline.
WHO recommends the directly observed treatment, short course
(DOTS) to prevent non-compliance. The health worker ensures that the
patient takes his/her drugs.
If the medicine is taken incorrectly, the patient becomes resistant to
anti-TB drugs. This is very dangerous because if the disease recurs it
becomes hard to treat the second time around.
Relapsing patients usually become resistant to individual drugs
(INH, rifampicin, ethambutol and PZA). They are given a combination of
the abovementioned drugs.
Multiple Drug Therapy(side effects)
Rifampicin (RIF)
a. red-orange urine
Isoniazid (INH)
a. hepatotoxicity
b. peripheral neuropathy
Ethambutol (EMB)
a. optic neuritis
Pyrazinamide (PZA)
a. severe hepatotoxicity
Streptomycin
a. CN VIII damage
b. vertigo
NURSING CARE
Maintain respiratory isolation until the patient responds to treatment
or until he/she is no longer contagious.
Administer medicines as ordered.
Always check the sputum for blood or purulent expectoration.
Encourage questions and conversation so that the patient can air
his/her feelings.
Teach or educate the patient about PTB.
Encourage the patient to stop smoking.
Teach the patient to cough or sneeze onto tissue paper and dispose
secretions properly.
Advise the patient to get plenty of rest and eat balanced meals.
Be alert for signs of drug reaction.
If the patient is receiving ethambutol, watch out for optic neuritis. If
it develops, discontinue the drug.
If the patient is receiving rifampicin (Rifampin), watch out for
hepatitis and purpura. Observe the patient for other complications like
hemoptysis (Yuan, 2003).
Emphasize the importance of regular follow-up examinations and
instruct the patient and his/her family about the signs and symptoms of
recurring TB.
Page 85
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VII. PNEUMONIA
A. Important information
1. It is an acute infectious disease caused by Pneumococcus and is
associated with general toxemia and a consolidation of one or more
lobes of either or both lungs.
2. It is an inflammation of the lungs in which the air sacs are filled with
pus or exudate so that air is excluded and the lungs become solid.
B. Causative agent: Streptococcus pneumoniae
o Staphylococcus aureus
o Haemophilus influenzae
o Klebsiella pneumoniae (Friedlanders bacilli)
Pneumonia is not a single disease. It can have over 30 different causes,
the five main ones being:
1. Bacteria
2. Viruses
3. Mycoplasma
4. Other infectious agents, such as fungi
5. Various chemicals
C. Incubation period: 1-3 days
D. Mode of transmission:
Droplet
indirect contact
inhalation of caustic or toxic chemicals, and aspiration of food, fluid or
vomitus.
Pneumonia is sometimes classified according to where and how
the client was exposed to the disease:
1. Community-acquired pneumonia acquired in the course of ones
daily lifeat work, at school or at the gym.
Page 86
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
If a hospitalized patient develops pneumonia in less than 36
hours during his stay in the hospital, he is diagnosed as having
community-acquired pneumonia.
Streptococcus pneumoniae (pneumococcus) is the most common
bacterial cause of community-acquired pneumonia, although
Hemophillus influenzae, and Legionella can also be the cause of
community-acquired pneumonia.
2. Nosocomial pneumonia is a pneumonia that develops while the client
is in the hospital. Such pneumonia reflects the kind of nursing care given
to the client.
3. Aspiration pneumonia occurs when a foreign matter is inhaled
(aspirated) into the lungs, most commonly when gastric contents enter
the lungs after vomiting.
Clients Prone to Aspiration Pneumonia
a. Decreased level of consciousness
b. Clients with poor gag reflex
c. The elderly
d. The very young
4. Pneumonocystis carnii pneumonia. Caused by opportunistic
organisms, this type of pneumonia strikes people with a compromised
immune system. (Organisms that are not normally harmful for healthy
people can be extremely dangerous to those with HIV/AIDS, sickle cell
disease and other conditions that impair the immune system.)
5. Actinomycosis
Caused by an anaerobic Gram-positive bacterial species that is
present in the mouth, known as Actinomyces Israeli
Usually associated with poor dental hygiene
The organisms cause pleural infection, resulting in a thickened
pleura, empyema and a fistulous tract.
6. Nocardia
A type of pneumonia caused by inhalation of soil particles where
the microorganisms, Nocardia asteroids, may be found.
Pulmonary infection can seed the bloodstream and form a brain
abscess, which is often mistaken as a CNS metastasis of lung
cancer.
ANATOMICAL CLASSIFICATION OF PNEUMONIA
1. Bronchopneumonia (lobular or catarrhal pneumonia)
a. This is the most common type of pneumonia.
b. Infection usually starts from the bronchus and bronchioles and
spreads to the alveoli in the periphery.
c. The lobules are inflamed and consolidated.
d. Sometimes these lobules are not inflamed but are collapsed due
to mucopurulent plugging of the bronchioles which supply them.
e. This pneumonia is caused by Pneumococcus, Klebsiella
pneumoniae, and Haemophilus influenzae.
f. The onset of this type of pneumonia is slow and the fever is
lower.
g. The period of communicability remains unknown; however, it is
believed that the disease remains infectious while the exciting
agent is given off in the discharges from the nose and throat.
2. Lobar pneumonia (Croupous pneumonia)
a. This is a consolidation of the entire lobe.
Page 87
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
b. It manifests as chills, chest pain or breathing and cough with
blood-streaked sputum (prune juice or rusty in appearance).
c. As the disease progresses, the prune-juice color of the sputum
may be replaced by a thinner or yellowish color.
d. In severe cases, the heart weakens and death occurs from heart
failure, edema of the lungs or severe general exhaustion.
3. Primary atypical pneumonia (viral pneumonia)
a. It is a solidification of the lungs that comes in patches.
b. Cough is often delayed in appearing and greenish to whitish
secretions are often expelled by coughing on the 3
rd
to the 5
th
days.
GENERAL CLASSIFICATION OF PNEUMONIA
1. Primary pneumonia is produced as a direct result of inhalation or
aspiration of pathogens or noxious substances. It includes some cases of
pneumococcal pneumonia, mycoplasma pneumonia and pneumonia
caused by tubercle bacilli.
2. Secondary pneumonia develops as a complication of the disease.
There are three types of secondary pneumonia.
a. Primary pulmonary infection, which is usually viral, is predisposed
to superinfection with an unrelated organism. (Example:
Staphylococcal pneumonia superimposed upon viral pneumonia
caused by type A influenza virus.)
b. Secondary bacterial infection may follow damage caused by an
initial noxious chemical insult to the lungs, such as aspiration of
gastric contents.
c. Hematogenous spread of bacterial pathogens from a distant focus
may result in secondary pneumonia.
E. Signs and Symptoms:
1. Sudden onset of chills with rising fever.
2. Stabbing chest pain aggravated by respirations and coughing.
3. Paroxysmal or choking cough.
4. Sputum is rusty or prune juice in color- pathognomonic sign
of pneumonia.
5. Pain on the abdomen mistaken as appendicitis.
6. Herpes may appear on the lips.
7. Body malaise
Page 88
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
8. Respiratory grunting with marked tachypnea and flaring of the
nares.
9. Labored respiration.
10. Pulse is rapid and bounding.
11. Diaphoresis-excessive sweating
12. Convulsion and vomiting in children.
F. Diagnostic
1. Physical findings for patient with lobar pneumonia
a. The patient has malar paleness, a flushed face, dilated
pupils, high-grade fever, tachypnea, and a relatively low
pulse.
b. The patients sputum is rusty and experiences hacking
paroxysmal cough.
c. Chest movement on the affected side is diminished;
percussion is dull
2. Chest x-ray definitive test (see Tuberculosis)
3. Sputum analysis, smear and culture is important.
4. The patient may be subjected to blood/serologic exam.
G. Management
PREVENTION
Preventing common colds, influenze and other upper respiratory
infections;
Immunization with pneumonia vaccine; and
Addressing environmental factors, such as exposure to cold,
pollution and physical conditions of fatigue and alcoholism (These are
contributory factors in lowering ones resistance to pneumonia.)
TREATMENT
Antimicrobial therapy varies with each agent
Example:
Streptococcus. Pneumonia caused by this agent can be
treated with macrodiles for seven to ten days.
Klebsiella. Treatment of pneumonia caused by this agent
includes aminoglycosides and cephalosporins.
Streptococcus. The patient may be given nafcillin or oxacillin
for 14 days.
Pneumocystis carinii. Cotrimoxazole or pentamidine may be
given to patients with pneumonia caused by this agent.
Pen G is still the drug if choice.
Supportive measures include:
o Humidified oxygen therapy for hypoxia
o Mechanical ventilation for respiratory failure
o High-calorie diet and adequate fluid intake, unless
contraindicated
Page 89
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
o Absolute bedrest
Bronchodilators aminophyllin may be of some benefit
Expectorants
Pain relievers for pleuritic pain
NURSING CARE
Maintain the patients airway and adequate oxygenation.
Teach the patient how to cough and perform deep-breathing
exercises to clear secretions. Advise him/her to do this often.
Obtain sputums specimens as needed. Teach the correct collection
of specimen.
Maintain adequate nutrition to offset high-calorie utilization.
Provide a calm environment as the patient needs rest.
Control the spread of infection by disposing secretions properly.
Control temperature by implementing cooling measures.
Monitor vital signs closely and watch for danger signs like:
a. Marked dyspnea,
b. Thread, small, irregular pulse,
c. Delirium with extreme restlessness,
d. Cold, moist skin, and
e. Cyanosis and exhaustion.
Page 90
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VIII. COMMON COLD
A. Important information
1. It is a self-limiting, acute viral infxn of the upper respiratory tract.
2. Resulting inflammation involves the nasal passages, throat, sinuses,
trachea, and bronchi.
3.Children: 6-8 colds a year, adults: 2-3 colds per year
B. AKA: Viral rhinitis; Coryza
C. Causative agent: 7 Viruses
1. Rhinovirus
2. Parainfluenza virus- fall colds
3. Coronavirus- winter colds
4. Respiratory syncytial virus (RSV)
5. Influenza virus
6. Adenovirus
7. Picornaviruses spring and summer colds
D. Mode of transmission:
Direct contact
Airborne infxn by droplet
E. Signs and Symptoms:
1. Nasal congestion
2. Runny nose
3. Sneezing
4. Nasal discharge
5. Nasal itchiness
6. Tearing watery eyes
7. Scratchy or sore throat
8. General malaise
9. Low-grade fever
10. Chills
11. Often headache and muscle aches
F. Diagnostic
1. Clinical examination
G. Management
PREVENTION
Page 91
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Anti- Influeza vaccination
Handwashing
TREATMENT
No specific tx
Adequate fluid intake
Encouraging rest
Preventing chills
Increasing intake of vitamin C
Using expectorants
Warm-salted water gargles soothe the sore throat
NSAIDS such as ibuprofen relieve the aches, pains, and fever in
adults
Antihistamines to relieve sneezing, rhinorrhea, and nasal
congestion
Topical (nasal) decongestant agents
Zinc lozenges may reduce the duration of cold sx if taken within
24 hrs of onset
Antimicrobial agents
Page 92
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IX.RESPIRATORY SYNCYTIAL DISEASE
A. Important information
1. It is a localized infection of the upper or lower respiratory tract or
both.
2. The degree of illness varies with the age and immune status of the
host.
3. The virus infects the ciliated mucosal epithelial cells of the nose, eyes,
and mouth.
B. Causative agent: Respiratory syncytial virus from genus
Pneumovirus
C. Incubation period: 3-7 days
D. Mode of transmission:
Self-inoculation by mouth or nose after contact with infectious
respiratory secretions
Droplets
Direct contact
E. Signs and Symptoms:
Minor cases
1. Congested or runny nose
2. Dry cough
3. Low-grade fever
4. Sore throat
5. Mild headache
Severe cases
1. High fever
2. Severe cough
3. Wheezing a high-pitched noise that's usually heard on breathing
out (exhaling)
4. Rapid breathing or difficulty breathing, which may make the child
prefer to sit up rather than lie down
5. Bluish color of the skin due to lack of oxygen (cyanosis)
Page 93
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
F. Diagnostic
1. Laboratory dx detecting viral antigen, isolating virus, detecting RNA
with polymerase chain reaction (PCR), and detecting a rise of antibody
titer or elevated IgM antibodies in a single serum.
G. Management
PREVENTION
Wash your hands frequently
Avoid exposure
Keep things clean
Don't share drinking glasses with others
Don't smoke
Wash toys regularly
TREATMENT
Acetaminophen (Tylenol, others) or ibuprofen (Advil, Motrin,
others) to reduce fever
Offer plenty of fluids and watch for signs of dehydration, such as
dry mouth, little to no urine output, sunken eyes and extreme
fussiness or sleepiness
Hospital care for RSV in severe cases may be necessary to
provide intravenous (IV) fluids and humidified oxygen
Hospitalized infants and children may also be hooked up to
mechanical ventilation a breathing machine to ease
breathing
In some severe cases, a nebulized bronchodilator such as
albuterol (Proventil, Ventolin) may be used to relieve wheezing
Page 94
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
X. PARAGONIMIASIS
A. Important information
1. The lungs are the most frequently involved; mistaken for TB on chest
x-ray.
2. May also affect the CNS, subcutaneous tissues, intestinal wall, lymph
nodes and genitourinary tract.
B. AKA: Lung fluke disease
C. Causative agent: Paragonimus a trematode
D. Incubation period: Flukes mature and begin to lay eggs about 6 wks
after man ingests infective larvae
E. Period of communicability: up to 20 yrs
F. Mode of transmission:
Ingestion of raw or insufficiently cooked crabs
Contaminated food or utensils with meta-cercariae during food
preparation
Consumption of inadequately cooked meat of animal reservoirs
Using meat or juice of infected animals for certain means
Accidental transfer of excysted meta-cercariae to the mouth during
food preparation
Drinking contaminated water with infective larvae (metacercariae)
G. Signs and Symptoms:
1. Cough of long duration
2. Hemoptysis or recurrent blood streaked sputum
3. Chest/Back pain
4. PTB-like s/sx not responding to anti-TB meds
H. Diagnostic
Page 95
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
1. Sputum exam eggs in brown spots
2. Immunology
3. Cerebral Paragonimiasis eosinophilia in CSF
I. Management
PREVENTION
Tx of infected person
Disinfection/Sanitary disposal of excreta
Anti-mollusk campaigns
Education of the population
Avoid eating infected foods
Avoid bathing in infected water
TREATMENT
Praziquantel (Biltrizide) DOC
25 mg./kg. Body weight 3 times daily for 3 days-Adults
and children over 4 yrs of age. Preparation: 600 mg tab
Bithionol (BITIN) alternative
30-50 mg./kg. Body weight on alternate days for a total of
10-15 doses
Surgical removal for heterotopic cases
Page 96
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XI. CRYPTOCOCCUS
A. Important information
1. It is a type of fungus that is found in the soil worldwide, usually in
association with bird droppings.
B. Causative agent: Cryptococcus neoformans
C. Mode of transmission:
Inhalation of airborne fungi
Human-to-human
D. Signs and Symptoms:
1. Pneumonia-like illness, with shortness of breath, coughing and fever
2. Skin lesions may also occur
3. Central nervous system infection, such as meningoencephalitis.
4. Fever, headache, orchange in mental status.
E. Diagnostic
1. Microscopic examination and/or culture of tissue or body fluids
such as blood, cerebrospinal fluid and sputum
2. Cryptococcal antigen test is a rapid test that can be performed
on blood and/or on cerebrospinal fluid to make the diagnosis
F. Management
PREVENTION
People who have weakened immune systems
should avoid areas contaminated by bird
droppings, and should avoid contact with
birds
TREATMENT
Treatment of meningoencephalitis and other severe infections is
usually initiated with an amphotericin B formulation, with or
without flucytosine.
Fluconazole is used for maintenance therapy in HIV-infected
patients with cryptococcal meningoencephalitis, and may be used
for patients with milder forms of infection not involving the
central nervous system.
Page 97
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XII. HANTAVIRUS PULMONARY
SYNDROME
A. Important information
1. It is a severe, sometimes fatal, respiratory disease in humans caused by
infection with a hantavirus.
B. Causative agent: Hantavirus
C. Mode of transmission:
Airborne transmission
If a rodent with the virus bites someone, the virus may be spread to
that person, but this type of transmission is rare.
Researchers believe that people may be able to get the virus if they
touch something that has been contaminated with rodent urine,
droppings, or saliva, and then touch their nose or mouth.
Researchers also suspect people can become sick if they eat food
contaminated by urine, droppings, or saliva from an infected rodent.
D. Signs and Symptoms:
Early sx
1. Fatigue, fever and muscle aches
2. Headaches, dizziness, chills, and abdominal problems, such as
nausea, vomiting, diarrhea, and abdominal pain
Late sx
3. Coughing and shortness of breath
E. Diagnostic
1. Blood tests can reveal if your body has made antibodies to a
hantavirus
F. Management
PREVENTION
Block access. Mice can squeeze through holes as small as a
quarter-inch (6 millimeters) wide. Seal holes with wire screening,
metal flashing or cement.
Close the food buffet. Wash dishes promptly, clean counters
and floors, and store your food including pet food in rodent-
proof containers. Use tightfitting lids on garbage cans.
Reduce nesting material. Clear brush, grass and junk away from
the building's foundation.
Set traps. Spring-loaded traps should be set along baseboards.
Exercise caution while using poison-bait traps, as the poison also can
harm people and pets.
Page 98
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Safe cleanup procedures
TREATMENT
Supportive therapy: People with severe cases need immediate
treatment in an intensive care unit
Assisted respiration, whether through intubation or mechanical
ventilation, can help with breathing and ward off pulmonary edema
Intubation involves placing a breathing tube through your nose,
mouth or trachea to help keep your airways open and functioning.
Blood oxygenation: In extremely severe cases of pulmonary
distress, you'll need a method called extracorporeal membrane
oxygenation to help ensure you retain a sufficient supply of oxygen
Page 99
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XIII. HISTOPLASMOSIS
A. Important information
1. It is an infection caused by a fungus.
2. The fungus lives is the soil, and is breathed in through a person' s
lungs. Most people with histoplasmosis develop no symptoms and may
never know they are infected.
B. AKA: Cave disease; Darling's disease; Ohio valley disease;
Reticuloendotheliosis; Spelunkers Lung and Caver's disease
C. Causative agent: Histoplasma capsulatum (H. capsulatum)
D. Mode of transmission:
Not transmitted person to person except for a few rare instances
when a transplant patient has contracted histoplasmosis from a
transplanted organ
Inhalation/Airborne
E. Signs and Symptoms:
1. Fever and chills
2. Cough and chest pain that gets worse when breathing in
3. Joint pain
4. Mouth sores
5. Red skin bumps called erythema nodosum, most often on the
lower legs
6. Chronic lung infection -- develops slowly over weeks to months
and produces a cough that gets worse, weight loss, night sweats,
and sometimes shortness of breath
7. Trouble breathing -- this can happen to people who breathe in
very large amounts of the fungus. It is sometimes called
"spelunker's lung" because it can happen after exploring caves.
F. Diagnostic
1. Biopsy of the lung, skin, liver, or bone marrow
Page 100
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
2. Blood or urine tests to detect histoplasmosis proteins or
antibodies
3. Cultures of the blood, urine, or sputum (this test provides the
clearest diagnosis of histoplasmosis, but results can take 6
weeks)
To help diagnose this condition, your doctor may perform:
Bronchoscopy
Chest CT scan
Chest x-ray
Spinal tap to look for signs of infection in cerbrospinal fluid (CSF)
G. Management
PREVENTION
Prevented by reducing exposure to dust in chicken coops, bat caves,
and other high-risk locations.
Wear masks and other protective equipment if you work in these
environments.
TREATMENT
The main treatment for histoplasmosis is antifungal drugs.
Amphotericin B, itraconazole, and ketoconazole are the usual
treatments.
Antifungals may need to be given through a vein, depending on
the form or stage of disease.
Some of these medicines can have side effects.
Sometimes, long-term treatment with antifungal drugs may be
needed. You may need to take these medications for up to 1 to 2
years.
Page 101
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XIV. LEGIONNAIRES DISEASE
A. Important information
1. It is a type of pneumonia caused by bacteria.
2. You usually get it by breathing in mist from water that contains the
bacteria.
3. The mist may come from hot tubs, showers or air-conditioning units
for large buildings.
4. The bacteria don't spread from person to person.
B. Causative agent: Legionella bacterium
C. Mode of transmission:
Breathing in small droplets of contaminated water
Inhalation: of aerosols, fine sprays, mists or other microscopic
droplets of water contaminated with LDB, providing direct access
into the lungs.
Aspiration: such as may occur when choking or spontaneously
during the drinking, ingesting, swallowing process. This allows oral
fluids and particles to by-pass natural gag reflexes and enter into
the respiratory tract and lungs instead of the esophagus and
stomach.
D. Signs and Symptoms:
1. Early symptoms include slight fever, headache, aching joints and
muscles, lack of energy or tiredness, and loss of appetite.
2. Later symptoms include:
High fever (102 to 105 F, or 39 to 41 C)
Cough (dry at first, later producing phlegm)
Difficulty in breathing or shortness of breath
Chills
Chest pain
Common gastrointestinal symptoms include vomiting, diarrhea,
nausea, and abdominal pain.
Page 102
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
3. Pontiac fever is a non-pneumonia disease with a short incubation
period of one to three days. Full recovery usually occurs in two to five
days without medical intervention and no deaths have been reported.
Pontiac fever produces flu-like symptoms that may include fever,
headache, tiredness, loss of appetite, muscle and joint pain,
chills, nausea, and a dry cough.
Pontiac fever has been associated with exposure to non-viable
LDB and may be a hypersensitivity response to bacterial or other
antigens rather than an infection.
E. Diagnostic
1. Chest x-ray and positive laboratory test results
F. Management
PREVENTION
The best way to prevent an outbreak of Legionnaires disease is
to ensure any water system under your control is properly maintained
and conforms to relevant health and safety regulations.
This mainly involves keeping water either cooled below 20C or
heated above 60C. The water supply should also be kept free of any
impurities and kept moving so it doesn't stagnate.
TREATMENT
The drugs of choice belong to a class of antibiotics called
macrolides. They include azithromycin, erythromycin, and
clarithromycin.
Pontiac fever goes away on its own without treatment and causes
no lingering problems.
Page 103
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XV. HERPANGINA
A. Important information
1. It is an acute febrile illness associated with small vesicular or
ulcerative lesions on the posterior oropharyngeal structures (enanthem).
2. Herpangina typically occurs during the summer and usually develops
in children, occasionally occurring in newborns, adolescents, and young
adults
B. Causative agent: Coxsackie virus
C. Mode of transmission:
"fecal-oral route" or via "respiratory route."
Contact with mucous of an individual infected with one of these
viruses is usually all that is needed to contract the illness
D. Signs and Symptoms:
1. grayish-white ulcers on the child's tongue and on the roof of the
mouth toward the back
2. painful swallowing
3. fever diarrhea
4. pink rash on the trunk.
E. Diagnostic
1. Physical exam
F. Management
PREVENTION
Good handwashing practices
TREATMENT
Take acetaminophen (Tylenol) or ibuprofen (Motrin) by mouth for
fever and discomfort as the doctor recommends.
Increase fluid intake, especially cold
milk products. Gargle with cool water
or try eating popsicles. Avoid hot
beverages and citrus fruits.
Eat a non-irritating diet. (Cold milk
products, including ice cream, are
often the best choices during
herpangina infection. Fruit juices are
too acidic and tend to irritate the
mouth sores.) Avoid spicy, fried, or
hot foods.
Use topical anesthetics for the mouth (these may contain benzocaine
or xylocaine and are usually not required).
Page 104
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
DISEASES AFFECTING THE GASTROINTESTINAL
SYSTEM
I. TYPHOID FEVER
A. Important information
1. It is a bacterial infection transmitted by contaminated water, milk,
shellfish and other foods.
2. It is an infection of the GIT affecting the lymphoid tissues of the small
intestines called Peyers patches.
B. AKA: Enteric Fever
C. Causative agent: Salmonella typhosa/typhi
Gram-negative, motile non-spore-forming pathogenic only to man
D. Incubation period: 5-40 days, mean: 10-20 days
E. Period of communicability: As long as the patient is excreting the MO,
he is capable of infecting others.
F. Sources of infection:
Patient with typhoid or infected or recovered from the disease
Ingestion of contaminated shellfish (oysters)
Infected patients stool or vomitus
G. Mode of transmission
Fecal-oral route
5 Fs:
1. Feces
2. Food
3. Files
4. Fomites
5. Fingers
H. Signs and Symptoms:
Onset Typhoid state
Headache, chilly sensation and
aching all over the body
N&V, Diarrhea
Worst all symptoms -4
th
and 5
th
days
Fever high in the morning than in
the afternoon
Symptoms decline in severity
Tongue protrudes, dry and brown
Accumulation of dirty-brown
collection of dried mucus and
bacteria (sordes) in the teeth and
lips
Staring blankly (coma vigil)
Page 105
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Breathing is accelerated
Tongue furred
Skin dry and hot
Distended abdomen with
tenderness
Rose spots appear on the
abdominal wall on the 7
th
-9
th
days
2
nd
wk- symptoms become more
aggravated, stable temp.,
prominent rose spots
Tendons twitching
Wrist twitching (subsultus
tendinum)
Mutters deliriously
Carphologia picks up aimlessly
at bedclothes with his finger in a
continuous fashion
Tendency to slip down to the foot
part of the bed
Rambling delirium, death
I. Complications
1. Hemorrhage or perforation 2 most dreaded complications
2. Peritonitis
3. Bronchitis and pneumonia
4. Meteorism or excessive distention of the bowels (tympanites)
5. Thrombosis and embolism
6. Early heart failure
7. Typhoid spine
8. Septicemia
9. Reiters syndrome joint pain, eye irritation and painful urination
leading to chronic arthritis
J. Diagnostic
1. Typhidot confirmatory test
- medical test consisting of a dot ELISA kit that
detects IgM and IgG antibodies against the outer membrane
protein (OMP) of the Salmonella typhi
Page 106
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
2. ELISA
3. Widal test- presumptive serological test for enteric
fever or undulant fever whereby bacteria causing typhoid fever are
mixed with serum containing specific antibodies obtained from an
infected individual.
4. Rectal swab
K. Management
PREVENTION
Sanitary and proper disposal of excreta
Proper supervision of food handlers
Enteric isolation
Provision of adequate amounts of safe drinking water supply
Reporting of cases to health authorities
Monitoring of typhoid carriers
Public education
TREATMENT
Chloramphenicol drug of choice
Ampicillin
Co-trimoxazole
Ciprofloxacin or ciftriaxone
3
rd
and 4
th
generations of drugs no response to chloramphenicol
NURSING CARE
Isolation
Oral fluid intake
Monitor VS
Prevent further injury(fall)
Maintain personal hygiene and mouth care
Cooling measures
Watch out for signs of intestinal bleeding
Terminal and concurrent disinfection
Page 107
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
II. FOOD POISONING
A. Important information
1. Onset is usually abrupt and ascribed to food recently eaten.
2. The most common predisposing cause consists of infected food
handlers and insufficient cooking of food.
3. The most common vehicles for transmitting staphylococcus food
poisoning are custard-filled pastries, processed meats especially ham and
milk from cows.
4. The exotoxin of botulism is a true poison known to be one of the
deadliest substances and usually released into the food smoothly after it
has been canned or preserved.
Most cases occur from eating uncooked foods from jars or cans
that have been inadequately processed during preserving.
Majority come from home-canned vegetables like string beans
A bulging can or jar of preserved food which smells rancid, shows
gas bubbles, tastes abnormal and a part of the solid portion appears
soft or liquefied is dangerous.
5. Signs and symptoms vary among individuals depending on the
resistance or the amount of infected food eaten.
B. AKA: Salmonellosis; Botulism
C. Causative agent:
Salmonellosis S. tryhimurium, S. cholerasesuis, S. Montevideo,
S. Newport, S. cranieburg
Staphylococcus
Botulism Clostridium botulinum
Toxin is produced only under anerobic conditions and in
alkaline or neutral nonacid foods
Easily destroyed by boiling
D. Incubation period: - 48 hrs
E. Period of communicability: no secondary person-to-person
transmission
F. Signs and Symptoms
Salmonellosis Botulism
Abrupt onset of severe
diarrhea and abdominal
cramps
Stools are offensive and
putrefactive at first, later
becoming watery, greenish
Extreme weakness; dizziness
Difficulty in breathing, swallowing
and speaking
Marked vertigo, disturbances of
vision
Page 108
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
and bloody, tenesmus
(straining at stool)
Concurrent N&V; abdominal
tenderness; slight fever
G. Management
PREVENTION
Proper canning
Proper preservation
Refrigeration of foods
MEDICAL CARE
Fluid and electrolytes; Potassium is a life-saving measure
Treatment of shock is present
Antibiotics
NURSING CARE
Complete Bed rest for patient
Provide comfort measures
Monitor Urine output
Page 109
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
III. LEPTOSPIROSIS
A. Important information
1. Increase incidence during the rainy season because of floods.
2. Sewer workers, farmers, miners and slaughterhouse workers are
among at risk.
3. Disease of a low-form animal.
4. It is a zoonotic infectious bacterial disease carried by animals, both
domestic and wild.
5. Infected urine contaminates water or food, which causes disease
when ingested or inoculated through the skin.
B. AKA:
1. Mud Fever
2. Weils Disease
3. Swamp Fever
4. Canicola Disease
5. Pretibial Disease
6. Swinherds Disease
7. Ictero-hemorrhagic Spirochetosis
8. Hemorrhagic Jaundice
C. Causative agent: Leptospira interrogans
Found in river, lake waters, sewage and sea
Saprophytic aquatic organisms
150 serotypes among 18 serogroups
Pathogenic to man and animals
Weils disease caused by the serovar icterohaemorrhagiae
D. Incubation period: 6-15 days
E. Period of communicability: 10-20 days after onset
F. Source of infection:
Contaminated food and water
Rats (L/ icterohaemorrhagiae) source of Weils disease among mine,
sewer, and abattoir workers
Rats (L. bataviae) attacks ricefield workers
Dogs (L. canicola) among veterinarians, breeders and owners of
dogs
Mice (L. grippotyphosa) affects farmers and flax workers
Page 110
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
G. Mode of transmission:
Contact of the skin (even if not abraded) or of mucous membranes
with water, moist soil or vegetation contaminated with urine of
infected animals as when wading in floods
Direct contact with excreta, urine or tissues of infected animals;
ingestion of food contaminated with urine of infected rats
Prolonged immersion in contaminated water
Human-to-human transmission is rare
H. Signs and symptoms
Symptoms range in severity from asymptomatic to fatal
Clinical course-biphasic, Unicteric- majority cases
Orange-colored skin and sclera pathognomonic sign
Septic stage Immune or toxic stage Convalescence
Febrile (4-7 days)
Onset of remittent
fever
Chills
Headache
Anorexia
Abdominal pain
Severe prostration
Respiratory distress
Fever subsides with
lysis
With or without jaundice
Lasts for 4-30 days
Iritis
Headache
Meningeal
manifestations:
disorientation,
convulsions and aseptic
meningitis
Oliguria and anuria with
progressive renal failure
Shock, coma, CHF
Death between 9
th
and 16
th
days
Relapse may
occur during the
4
th
-5
th
weeks
I. Diagnostic
1. Blood urea-nitrogen and creatinine
2. Enzyme-linked immunosorbent assay (ELISA)
3. Liver function tests usually are slightly to moderately elevated:
Aspirate aminotransferase (AST)
Alanine aminotranferase (ALT)
Page 111
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Gamma-glutamyltransferase (GGT)
4. Leptospira antigen-antibody test (LAAT)
5. Leptospira antibody test (LAT)
J. Complications
1. Meningitis
2. Respiratory distress
3. Renal interstitial tubular necrosis that results in renal failure (Weils
disease)
4. Cardiovascular problems
K. Management
PREVENTION
Sanitation
Proper drainage system and control of rodents (40-60%)
Animals must be vaccinated
Infected humans and pets should be treated
Information dissemination campaign
MEDICAL CARE
Suppressing causative agent
Fighting possible complications
Aetiotropic drugs penicillin, doxycycline, ampicillin,
amoxicillin
For prophylaxis doxycycline 100 mg p.o. every 12 hours
for 1 wk
Administration of fluid and electrolytes and blood
NURSING CARE
Isolate the patient, disposed urine properly
Darken the room
Observe skin care to ease pruritus
Keep homes clean
Regularly replace water in pools, vases, aquaria, etc. to prevent
stagnation
Eradicate rats and rodents
Provide health education
Encourage oral fluid intake
Page 112
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IV. PARALYTIC SHELLFISH POISONING
A. Important information
1. A syndrome of characteristic symptoms predominantly neurologic
which occur within minutes or several hours after ingestion of
poisonous shellfish.
2. Victims who survive the first 12 hrs after ingestion have a greater
chance of survival.
3. It caused by a population explosion or toxic, naturally occurring
microscopic phytoplanktons, specifically a subgroup known as
dinoflagellates.
B. AKA: Red tide
C. Causative agent: Gonyaulax, Protogonyaulax and Gessnerium
known by accepted name Alexandrium sp.
Alexandrium tamarense Atlantic coast
Alexandrium catenella Pacific West Coast
Ptychodiscus brevis Gulf of Mexico along the West Florida
D. Factors which are favorable for growth are:
1. warm surface temperature
2. high-nutrient content;
3. low salinity and calm seas; and
4. rainy days followed by sunny weather
E. Incubation period: 30 mins to several hrs. after ingestion of
poisonous shellfish (tahong, talaba, halaan, etc.)
F. Mode of transmission: Ingestion of raw or inadequately cooked
seafoods specifically bivalve shellfish or mollusks during red tide
season.
Shellfish include: quahogs, soft shell clamps,oysters, mussels, scallops, and
moon snails
4 syndromes of shellfish poisoning:
1. Paralytic shellfish poisoning
2. Diarrheal shellfish poisoning
3. Amnestic shellfish poisoning
4. Neurologic shellfish poisoning
Note: Lobster, crabs, shrimps and fish do not accumulate toxins and
are safe to eat even if they are from affected waters.
Page 113
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
G. Signs and symptoms
Initial sign tingling of the lips and tongue spreads to the face,
neck, fingertips and toes
Headache, dizziness, nausea follow same as drunken condition
Such symptoms aggravated by alcohol consumption
Muscular paralysis and DOB may occur in 5-12 hrs due to diaphragm
paralysis- can survive through with the aid of a respirator
Fatalities from respiratory arrest
H. Management
PREVENTION
Monitor for shellfish contamination
Department of Environmental Quality Engineering (DEQE)- year
round testing of shellfish
When blooms subside-shellfish becomes purifies toxin, when in
safe levels, areas are reopened
Seek medical attention immediately for suspected ingestion of
toxic shellfish
Recreational shellfish gatherers
TREATMENT
Induce vomiting
Charcoal hamoperfusion -pumping arterial blood through charcoal
filter
Alkaline fluids such as sodium bicarbonate are helpful- toxins
become unstable
Artificial respiration for respiratory stress
Page 114
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
V. MUMPS
A. Important information
1. A generalized systemic infection involving the parotid glands
2. Usually occurs in epidemic form
3. An acute contagious disease
4. A single attack causes permanent immunity if both glands were
affected.
B. AKA: Infectious Parotitis; Epidemic Parotitis
C. Causative agent: Paramyxovirus
D. Incubation period: 14-25 days (average: 18 days)
E. Period of communicability: 6 days before and 9 days after the onset of
parotid gland swelling, 48 hr period- highest communicability
F. Mode of transmission:
Droplet infection
Direct contact
G. Signs and symptoms:
1
st
symptom- sudden headache, earache, loss of appetite, fever and
swelling of the parotid glands located in front and below the ears.
Pain-peak 2 days and continues 7-10 days
Moderately elevated temp.
One gland may be affected at first, 1-3 days later-other side becomes
involved
Occasionally, enlargement of the glands may be the only symptom
noted.
Page 115
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Gelatinous edema- pathognomonic sign
H. Complication
1. Orchitis(swollen testes) most notorious complication
2. Oophoritis (abdomen tenderness/pain) in females
3. Mastitis-breast infxn
4. CNS involvement
5. Nuchal rigidity
6. Deafness
7. Meningoencephalitis most common complication
8. Pancreatitis
9. Transvers myelitis, ataxia, thrombocytopenia, myocarditis, arthritis
and nephritis (rare)
I. Diagnostic
1. Compliment fixation test presumptive evidence of infection
2. Hemogglutination inhibition test determine immune status
3. Neutralization test- determines immunity to mumps
4. A viral culture
5. Serum amylase determination most useful test in making an
early presumptive diagnosis for mumps
J. Management
PREVENTION
Active immunization (MMR)
Isolation of patient
Reporting cases
TREATMENT
Anti-viral drugs
Application of a hot or cold pack ro relief pain from parotid
swelling
NURSING CARE
Care for in a single-occupancy room
Use masks and must wash hands regularly
Terminal disinfection
Oral care and overall personal hygiene
Bed rest
Diversion activities
No restriction of food except during the acute stage(painful to
chew or swallow)
Soft and semisolid foods are easily managed.
Acidic foods, like juices, may increase discomfort
Page 116
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VI. PINWORM INFESTATION
A. Important information
1. An intestinal roundworm which infects only man
2. If found in one family member, the rest are probably infected also.
B. AKA: Nocturnal ani; Enterobiasis; Oxyuriasis
C. Causative agent: Enterobius vermicularis- a nematode, also known as
seatworm or threadworm
Lives and breeds in the small intestine.
When eggs are swallowed, they hatch in the stomach and small
intestines.
Gravid worms migrate during the night down the rectum and even the
peranal area to lay their eggs, causing severe itching.
May enter the vagina within a few hours after leaving the GIT.
Eggs are easily blown around by mild breezes and are very infectious.
Not destroyed by ordinary laundering.
D. Incubation period: 2-6 wks to be completed -cycle of worm
E. Period of communicability: As long as gravid females are discharging
eggs on the perianal skin.
F. Mode of transmission:
Direct transfer of infective eggs by hand from anus to mouth of the
same or another person
Indirectly contaminated clothing, linen, food, etc.
Dustborne infection is also possible
G. Diagnostic exam:
Test Tape
Best done upon waking up in the
morning before bathing or bowel
movement
Scotch tape placed against the anus and then examined
microscopically for eggs.
H. Management:
Handwashing
Wear well-fitting underwear
All members of the household should be treated
with Piperazine hexahydrate (500mg/tsp) for 1 wk
tsp OD - for childr en
2 tsps BID for adults
Page 117
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VII. ASCARIASIS
A. Important information
1. A chronic condition often producing no symptoms
2. More prevalent in tropical countries like the Philippines
3. It is an infection caused by a parasitic roundworm
4. Most commonly affects children 4-12 years old
B. AKA: Roundworm Infection
C. Causative agent: Ascaris lumbricoides
Elongated. Cylindrical worms tapered at the oral portion & anal end
Creamy and pinkish yellow when fresh
Thick as a pencil and live for 1-2 yrs
Female worm produces up to 240,000 eggs per day
D. Incubation period: reach about 2 months after ingestion
E. Period of communicability: As long as mature gravid worms are in the
intestines.
F. Mode of transmission:
Contaminated fingers put into the mouth
Ingestion of food and drinks contaminated with embryonated eggs
can transmit ascariasis
G. Signs and symptoms
Developmental Stage
Embryonated
ova
Larval stage Adult
Information Soil
contamination
with human
excreta
Contamination
of food, water
and other
objects
Ingested to
intestine
Larvae
penetrate the
walls of the
intestine
(duodenum)
Larvae are
picked up by
lymphatics or
bloodstream
Carried to the
liver
May reach the
heart
Carried to the
biliary tract
Adult ascaris
stays in the
small
intestine
Become
erratic that
go to the
stomach to
the
esophagus,
sometimes to
the common
bile duct and
the gall
bladder
Page 118
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
(sometimes)
Reach the
stomach,
esophagus, and
Upper
respiratory tract
Stay in
capillaries of
the lungs, reach
alveoli-grow for
10 days
From alveoli,
migrate to the
bronchioles,
bronchi,
trachea, and
epiglottis
Ascaris may be
swallowed or
ingested
Copulate in
the GIT
Female lays
egg about 2-
3 months
after
embryonated
eggs are
ingested
Symptomatology N&V, poor
appetite
Periumbilical
pain
RUQ pain
Cough, fever,
rales, blood-
tinged sputum
Nasal pruritus if
larvae reach
the nose
Colicky,
periumbilical
pain
aggravation
by cold
stimulation
(Nakamura
sign)
Intestinal
obstruction
may be
caused by a
bolus of
entangled
worms which
may be
palpable
Severe
abdominal
pain
associated
with vomiting
H. Complications
1. Biliary tract obstruction develops cholestatic jaundice
2. Hepatic abscess and cholangitis
3. Intestinal obstruction, perforation, peritonitis
4. Malnutrition
I. Diagnostic test
1. Stool for ova demonstration of fertilized or unfertilized eggs in
the stools (Kato-Katz technique)
Page 119
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
2. Abdominal x-ray densed shadow of adult ascaris which looks like
strands of spaghetti (dot sign)
3. Routine blood counts significant eosinophelia
J. Management
PREVENTION
Sanitation and hygienic practices
Improved nutrition
Deworming is advised
Avoid contaminated water or food when travelling
TREATMENT
Albendazole or mebendazole 15 cc as a single dose
Piperazine citrate 75 mg/kg twice daily, orally
Pyrantel pamoate 1mg/kg as a single dose, orally
NURSING CARE
Isolation
Preventive measures in each home and community
Family must be taught on sanitary practices: washing hands
before handling food, washing all fruits and vegetables that are
eaten raw and effective sewage disposal
Availability of toilet facilities
Importance of personal hygiene
Proper disposal of diapers
Page 120
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VIII. TRICHINOSIS
A. Important information
1. It is caused by helminthes or parasitic worms
B. AKA: Trichiniasis
C. Causative agent: Trichinella spiralis
A small roundworm
Can be killed by extremes of temperature
Encapsulated larvae from infected meat dissolve when ingested
embryos released into the stomach and intestines where they grow
and copulate female worm releases several hundreds of
embryos bloodstream skeletal muscles
D. Incubation period: 10-14 days
E. Mode of transmission
Eating raw or insufficiently cooked pork or beef, e.g. hamburger
F. Signs and symptoms
1. NVD within 48 hrs
2. Moderate intermittent, remittent or continuous fever
3. Swelling over forehead and around the eyes
4. Intense muscular pain specially when moving
G. Diagnostic test: same as ascariasis
H. Management: same as ascariasis
Page 121
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IX. TRICHURIASIS
A. Important information
1. It is caused by helminthes or parasitic worms
B. AKA: Whipworm disease
C. Causative agent: Trichuris trichiuria
Nematode
Ingestion of infective eggs from contaminated soil larvae are
hatched attach to the mucosa of the cecum and proximal colon
D. Incubation period: Indefinite
E. period of communicability: Several years in untreated carriers
F. Mode of transmission:
Indirect
Not transmissible from person to person
G. Signs and symptoms
1. Diarrhea with bloody, mucoid stools
2. Rectal prolapsed
H. Diagnostic: same as ascariasis
I. Management: same as ascariasis
Drug of choice: Mebendazoloe (Vermox) or Albendazole
Page 122
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
X. TAENIASIS
A. Important information
1. It is caused by helminthes or parasitic worms
B. Causative agent:
Taenia solium (pork tapeworm)
Taenia saginata (beef tapeworm)
Diphyllobotrium latum (fish)
C. Incubation period: several days to 10 yrs after infxn
D. Period of communicability: Not directly transmitted from person to
person
E. Mode of transmission:
Ingestion of raw or undercooked infected pork, beef or fish
F. Signs and symptoms:
Many are asymptomatic
Nervousness
Insomnia
Weight loss
Abdominal pain
Digestive disturbances
G. Diagnostic: same as ascariasis
H. Management: same as ascariasis
Niclosamide (Niclocide, Yomesan)
Praziquantel Biltricide
Page 123
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XI. HOOKWORM DISEASE
A. Important information
1. It is an intestinal parasite of humans that usually causes diarrhea or
cramps.
2. It occurs mostly in tropical and subtropical countries.
B. AKA: Ancyclostomiasis; Miners disease; Egyptian Chlorosis
C. Causative agent:
Ancylostoma duodenale prevalent in Europe and Asia
Necator americanus Central and South America and West Africa
Female hookworm 10,000-20,000 eggs per day
Source of infection: Soil contaminated with feces that contains
hookworm ova
Pathogenic to man
Develop embryos- 24-72 hrs
Life span few to 10 yrs
D. Incubation period: 40-100 days or 2-8 wks
Appear in the stools: 4-6 wks after larvae penetrate the skin
E. Period of communicability: Persons remain spreaders of infections as
long as they are infected
F. Mode of transmission:
Direct through the skin of the foot(ground itch)
Ingestion of contaminated drinking water or food
Page 124
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
G. Signs and symptoms:
Devt of small lesions
50 ml daily of hosts blood resulting to iron deficiency anemia
Signs of anemia: pallor, easy fatigability, bradycardia
Abdominal pain, diarrhea and and urticaria
Mentally and physically underdeveloped for children
Infected children- be malnourished, undersized, lazy, no energy
and lack of ambition
Pupils are more or less dilated
Perverted appetites
Pedal edema and edema present
H. Diagnostic
1. Microscopic examination of feces for the eggs
2. Blood exam reveals eosinophilia
I. Management
PREVENTION
Health education
Pollution regulations
Avoid walking barefoot
Good hygiene
Animals should not allowed to defecate on the streets
Drink only purified or boiled water
Do not eat raw vegetables
Do not use night soil and sewage for fertilizers
TREATMENT
Pyrantel embonate (Quantrel)
Tetrachloroethylene
Carbon tetrachloride
NURSING CARE
Isolation is not necessary
Diet should be high in calories, vitamins and minerals
Maintain personal hygiene
Page 125
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XII. STRONGYLOIDIASIS
A. Important information
1. A helminthic infection of the duodenum and upper jejunum
2. Often asymptomatic
B. Causative agent: Strongyloides stercoralis and S. fuelleborni
C. Incubation period: 2 wks from skin penetration by filariform larvae
until rhabditiform larvae appear
D. Period of communicability: As long as living worms remain in the
intestine (up to 35 yrs)
E. Mode of transmission
Infective filariform larvae from feces or moist soil contaminated with
feces penetrate the skin enter venous circulation
lungs through capillary walls Alveoli Trachea
Epiglottis Descend into the digestive tract Upper part of
the small intestine where development of the adult female is
completed
F. Signs and symptoms
1. Classic: Epigastric pain, diarrhea and urticaria; N&V
2. Voracious appetite- Consuming or eager to consume great
amounts of food
3. Weakness
4. Pot belly
5. Anemia
6. Stunted growth in children below 10 yrs old
Page 126
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
7. Intensely pruritic dermatitis radiating from the anus
G. Diagnostic:
1. Stool exam
2. Jejunal biopsy
H. Management
PREVENTION
Proper handwashing
Personal hygiene
Proper wearing of footwear
Proper handling of foods
TREATMENT
Antihelminthics e.g. Antiox (dosage depends on body weight)
NURSING CARE
Isolation is not necessary
Diet should be high in calories, vitamins and minerals
Maintain personal hygiene
Page 127
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XIII. SCHISTOSOMIASIS
A. Important information
1. Affects mostly farmers and their families in the rural area.
2. Endemic in 10 regions, 24 provinces, 183 municipalities and 1,212
barangays.
3. High prevalence in Region 5 (Bicol), Region 8 (Samar and Leyte) and
Region 11 (Davao).
4. It is a slowly progressive disease.
B. AKA: Bilharziasis; Snail Fever
C. Causative agent: Schistosoma japonicum
3 MAJOR TYPES
Schistosoma
japonicum
Schistosoma
mansoni
Schistosoma
haematobium
Infects the intestinal
tract (Katayama
disease)
Only type that is
endemic in the Phil.
AKA: oriental
schistosomiasis
Affects the
intestinal tract
Common in some
parts of Africa
Affects urinary tract
Found in some parts of
Middle East like Iraq &
Iran
D. Incubation period: At least 2 months
E. Sources of infection:
Feces of infected persons
Dogs, pigs, carabaos, cows, monkeys and wild rats serve as hosts
F. Mode of transmission:
Ingestion of contaminated water
Skin pores
Intermediary host, a tiny snail called Oncomelania quadrasi
Characteristics:
1. Thrives along riverbanks, freshwater streams, creeks, canals and
swamp
2. Clinging to water hyacinths, grasses, decaying leaves, pieces of
rotting wood, bamboo and coconut husks.
3. Areas with sandy-loamy soil
4. Greenish-brown in color as big as smallest grain of palay
Page 128
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
G. Signs and symptoms
1. Swimmers itch pruritic rash-pathognomonic sign
2. Low-grade fever, myalgia and cough
3. Abdominal discomfort due to hepatomegaly, splenomegaly and
lymphadenopathy.
4. Bloody-mucoid stools
5. Icteric and jaundice
6. Belly becomes big because of inflamed liver
7. Weak, pale and muscle wasting
8. Severe headaches, dizziness and convulsions
H. Complication
1. Liver cirrhosis and portal HPN
2. Cor pulmonale and pulmonary HPN
3. Heart failure
4. Ascitis
5. Hematemesis rupture of esophageal varices
6. Renal failure
7. Cerebral schistosomiasis caused by the hosts reaction to
schistosoma eggs with a s/sx of Increased ICP with focal neurological
signs.
I. Diagnostic
1. Fecalysis or direct stool exam
2. Kato-Katz technique
3. Liver and rectal biopsy
3. Enzyme-linked immunosorbent assay (ELISA)
4. Circumoval precipitin test (COPT) confirmatory test
J. Management
PREVENTION
Have a stool examination
Reduce snail density by clearing vegetation, proper irrigation
and drainage, removal of weeds
Diminish infection rate through proper waste disposal
Health education
TREATMENT
Praziquantel tablet for 6 months; 1 tab 2x a day for 3 months,
then 1 tab a day for another 3 months
Fuadin injection given either IM or IV. The patient should
consume 360 mg for the entire treatment
If the patient continues to live in the endemic area, he frequently
gets reinfected and has to be retreated.
Page 129
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XIV. AMOEBIASIS
A. Important information
1. It is a protozoal infection of human beings initially involves the colon,
but may be spread to soft tissues, most commonly the liver and lungs, by
contiguity or hematogenous or lymphatic dissemination.
B. AKA: Amoebic dysentery
C. Causative agent: Entamoeba histolytica
Common in warm climates, unsanitary areas, by swallowing
Causes amoebic liver abscess
DEVELOPMENTAL STAGES
Trophozoites/Vegetative form Cyst
Invade tissues
Found in parasitized tissues
and liquid colonic contents
Passed out with formed or
semi-formed stools
Resistant to
environmental conditions
Infective stage
D. Source: Human excreta
E. Incubation period: 3-4 wks
Severe infxn: 3 days
Sub-acute and chronic: lasts for several months
F. Period of communicability: Entire duration of the illness
G. Mode of transmission:
Fecal-oral transmission passed from one person to another
Direct contact: sexual contact, orogenital, oroanal, and proctogenital
sexual activity
Indirect contact: ingestion of contaminated food with fecal material
H. Signs and symptoms
Acute amoebic
dysentery
Chronic amoebic
dysentery
Extraintestinal
forms/Hepatic
Slight attacks of
diarrhea
Periods of
constipation
Tenesmus
Diarrhea, watery
Lasts for several
days
Tenesmus
Anorexia, weight
loss and
weakness
Pain in the RUQ
with liver
tenderness
Jaundice
Intermittent fever
Loss of weight or
Page 130
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
and foul-smelling
stools often
contains blood-
streaked mucus
Colic and
gaseous
distension
Nausea,
flatulence,
Abdominal
distention,
tenderness in
the right iliac
region over the
colon
Enlarged liver
Semifluid stools
become watery,
bloody and
mucoid
Vague abdominal
distress,
flatulence,
constipation
Mild toxemia,
constant fatigue
and lassitude
Loses abdominal
elasticity
Scattered
ulceration with
yellowish and
erythematous
borders noted
Gangerous type
(fatal)
anorexia
Coughs
anchovy-sauce
sputum
I. Diagnostic
1. Stool exam (cyst; white and yellow pus with plenty of amoeba)
2. Blood exam (leukocytosis)
3. Proctoscopy/Sigmoidoscopy
J. Management
PREVENTION
Health education
Sanitary disposal of feces
Protect, chlorinate and purify drinking water
Scrupulous cleanliness in food preparation
Detection and tx of carriers
Fly control
TREATMENT
Metronidazole (Flagyl) 800 mg TID x 5 days
Tetracycline 250 mg every 6 hrs
Ampicillin, quinolone, sulfadiazine
Streptomycin SO
4
, chloramphenicol
Lost fluids and electrolytes should be replaced
NURSING CARE
Observe isolation
Provide health education
Proper collection of stool specimen
Page 131
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Never give paraffin or any oil prep. for at least 48 hrs
prior
Avoid mixing urine with stools
Select large portions containing blood and mucus as
possible
Send specimen immediately
Label specimen properly
Skin care
Mouth care
Provide optimum comfort: Keep pt. warm
Diet: Oral fluid intake, cereals and strained meat broths without
fat should be given, add chicken and fish when in convalescence
and a bland-diet without cellulose or bulk-producing foods should
be maintained for a long time
Page 132
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XV. BACILLARY DYSENTERY
A. Important information
1. It is an acute bacterial infection of the intestines
2. Characterized by diarrhea and fever associated with bloody-mucoid
stools accompanied by tenesmus.
B. AKA: Shigellosis; Bloody Flux
C. Causative agent: Shigella group
Serologic groups:
1. Shigella flexneri (Group B) common in the Phil.
2. Shigella boydii
3. Shigella connei
4. Shigella dysenteriae
Most infectious
GIT of man-habitat
Develop resistance against antibiotics
Rarely invade blood stream
D. Incubation period: 7 hrs 7 days, average: 3-5 days
E. Period of communicability: During acute infxn, pt remains carriers for a
year or 2.
F. Mode of transmission
Ingestion of contaminated food or water or milk
By flies or objects with feces of the pt.
Fecal-oral transmission
G. Signs and symptoms
1. Fever especially children
2. Tenesmus, N&V, headache
3. Colicky or cramping abdominal pain with anorexia and body
weakness
Page 133
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
4. Diarrhea with bloody-mucoid stools that is watery
5. Rapid dehydration and weight loss
H. Complication
1. Rectal prolapsed in undernourished children
2. Cough and pneumonia
3. Non-suppurative arthritis and peripheral neuropathy
I. Diagnostic
1. Fecalysis
2. Rectal swab or culture
3. Peripheral blood exam
4. Blood culture
5. Sheets of polymorphoneuclear leukocytes seen in staining with
methylene blue
J. Management
PREVENTION
Sanitary disposal
Proper preparation of food
Safe washing facilities
Fly control
Isolation during acute stage
Protection of water supply
TREATMENT
Ampicillin, tetracycline and cotrimoxazole may be useful in
severe cases
IV infused with normal saline
Low-residue diet
Anti-diarrheal drugs are contraindicated because they delay
fecal excretion that can lead to prolonged fever
NURSING CARE
Maintain fluid and electrolytes
Keep pt. warm
Restrict food until N&V subsides
Isolation
Maintain personal hygiene
Properly disposal of excreta
Concurrent and terminal disinfection
Return to normal activities must be gradual
Page 134
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XVI. CHOLERA
A. Important information
1. It is an acute bacterial enteric disease of the GIT
2. It is characterized by profuse diarrhea, vomiting, massive loss of fluid
and electrolytes which could result in hypovolemic shock, acidosis and
death.
B. AKA: El Tor
C. Causative agent: Vibrio cholera/ Vibrio coma
Slightly curved rod (comma-shaped)
Multiplies in temp from 22-40 degrees centigrade
Can survive in refrigerated foods
An enterotoxin, choleragen that grows in the intestinal tract.
D. Incubation period: few hrs -5 days, usually 1-3 days
E. Period of communicability: Communicable during the stool-positive
stage, usually a few days after recovery; carrier for several months
F. Mode of transmission:
Fecal transmission via oral route from contaminated water, milk, and
other foods
Ingestion of contaminated water or food with stools
Flies, soiled hands and utensils
G. Signs and symptoms
Rice water stools pathognomonic sign
1. Acute, profuse, watery diarrhea with no tenesmus
2. Brown stool becomes pale gray and rice-water like with slightly fishy
odor
3. Vomiting after diarrhea
4. Diarrhea causes fluid loss of 1-30 liters per day
Page 135
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
5. Poor turgor, sunken eyes
6. washerwomans hand skin is cold; fingers and toes are
wrinkled
7. Cyanosis
8. Radial pulse-imperceptible
9. BP unobtainable
10. Rapid breathing
11. Hoarseness of voice and Aphonia
12. Diminished peripheral circulation
13. Oliguria or Anuria
14. Death 4 hrs after onset, usually 1
st
or 2
nd
day if not properly
treated
H. PRINCIPAL DEFICITS
Extracellular volume- lead to severe dehydration or circulatory
collapse or shock
Metabolic acidosis loss of large volume of bicarbonate-rich stools
Hypokalemia- massive loss of potassium through the stools
Renal failure- untreated shock or unrelieved hypokalemia
Convulsions and tetany- loss of magnesium
Hypoglycemia stupor for several days for untreated children
Corneal scarring- lost wink reflex
Acute pulmonary edema uncorrected metabolic acidosis that follow
hydration
I. Diagnostic
1. Rectal swab
2. Dark-field or phase microscopy
3. Stool exam
J. Management
PREVENTION
Page 136
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Protect food and water supply for fecal contamination
Water should be boiled or chlorinated
Pasteurized milk
Proper disposal of feces
Sanitary supervision
TREATMENT
Intravenous tx. By rapid infusion of an alkaline solution
Oral therapy rehydration (ORESOL, HYDRITES)
Maintenance of the volume of fluid and electrolytes
Antibiotics
Tetracycline 500 mg every 6 hrs- for adults; 125 mg/kg
body weight for children every 6 hrs for 72 hrs
Furazolidone 100 mg for adults; 125 mg/kg for children
every 6 hrs for 72 hrs
Chloramphenicol 500 mg for adults; 18 mg/kg for
children every 6 hrs for 72 hrs
Cotrimoxazole 8 mg/kg for 72 hrs
NURSING CARE
Handwashing
Enteric isolation
Vital signs be recorded accurately
Monitor I&O
Careful personal hygiene
Properly disposal of excreta
Concurrent disinfection
Properly preparing of food
Environmental sanitation
Weighing the pt.
Appropriate diet is given to the stage of recovery
Page 137
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XVI. HEPATITIS
A. Important information
1. It is defined as inflammation of the liver, and is classified as either
viral or non-viral.
SUMMARY OF THE COMPARISON OF MAJOR FORMS OF VIRAL
HEPATITIS
HEPATITIS A HEPATITIS B HEPATITIS C HEPATITIS
D
HEPATITIS
E
AKA: Infectious
hepatitis;
Catarrhal
jaundice
Serum hepatitis Non-A, non-B
hepatitis
Causative
agent
Hepatitis A
virus (HAV)
Hepatitis B virus
(HBV
Hepatitis C
virus (HCV)
Hepatitis D
virus
(HDV)
Hepatitis E
virus (HEV)
Mode of
transmission
Fecal-oral
route;
poor
sanitation.
Person-
person
contact
Water-
borne
Foodborne
Oral-anal
contact
during sex
Parenterally;
by intimate
contact with
carriers or
those with
acute
disease
Sexual and
oral-oral
contact
Perinatal
contact from
mothers to
infant
Transfusion
of blood and
blood
products;
exposure to
contaminated
blood
through
equipment or
drug
paraphernalia
Sex with
infected
partners
Same as
HBV,
HDV
surface
antigen
for
replica-
tion;
pattern
similar to
hepa B
Fecal-
oral
route
Person-
person
contact
Incubation
period
(days)
And
Immunity
15-60 days
Average: 30
days
Homologous
50-189 days
Average: 90
days
Homologous
15-160
days
Average:
50 days
Second
attack may
indicate
weak
immunity
of infection
with
another
agent
21-140
days
Average
: 35
days
Homolo-
gous
15-65
days
Average:
42 days
Unknown
S/Sx May occur
with or
without sx;
flu-like
illness
Preicteric
phase:
Headache,
Malaise,
Fatigue,
Anorexia,
Fever
Icteric
phase: Dark
urine,
jaundice of
skin, tender
liver
May occur
without sx
May develop
athralgias,
rash
Similar to
HBV; less
severe and
anicteric
Similar
to HBV
Similar to
HAV.
Very
severe in
pregnant
women
Page 138
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
I. HEPATITIS A (Infectious hepatitis/Catarrhal jaundice)
Groups at Risk for HAV
1. Children in day care centers can transmit the infection through diapers
and toys.
2. Troops living in crowded conditions at military camps or in the field are
at great risk.
3. Homosexual men are at an increased at risk of HAV infection from oral-
anal sexual contact.
4. People who live in areas with a breakdown of sanitary conditions, such
as after a flood or other natural disasters.
Clinical Manifestations
1. Flu-like illness with chills and high fever
2. Diarrhea, fatigue and abdominal pain
3. Loss of appetite
4. Nausea, diarrhea and fever
5. Jaundice and dark-colored urine
6. The infection in young children is often mild and asymptomatic.
7. Hepatitis A does not have chronic stage and does not cause permanent
liver damage.
8. Following infection, the immune system makes antibodies against the
hepatitis A virus that confer immunity against future infection. The
disease can be prevented by hepatitis A vaccine.
Complications
1. Progressive encephalopathy characterized by drowsiness and cerebral
edema
2. GIT bleeding progressing to stupor and later coma. Bleeding is not
responsive to parenteral vitamin K administration.
3. Clonus and hyperreflexia are later replaced by loss of deep tendon
reflexes.
4. Edema and ascitis
5. Aplastic anemia
6. In the late course of the disease, loss of corneal and papillary reflexes,
elevated arterial blood, respiratory failure, and cerebrovascular collapse
may be present.
Diagnostic Procedures
1. HAV and HBV complement fixation rate
Page 139
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
2. Liver function test to determine the presence and extent of liver
damage and check the progress of the liver
3. Bile examination of stool and urine samples
4. SGOT serum glutamic oxoloacetic transaminase
SGPT serum glutamic pyruvic transaminase
ALT serum alanine transaminase
5. IgM level
Treatment Modalities
1. There is no specific treatment, although bed rest is essential.
2. Diet must be high in carbohydrates, low in fat and low in protein.
3. Patient must take vitamin supplements, especially the B complex group.
4. Intravenous therapy is occasionally necessary.
5. Isoprinosine (methisoprenol) may enhance the cell-mediated immunity
of the T-lymphocytes.
6. Alkalies, belladonna, and anti-emetics should be administered to control
dyspepsia and malaise.
Nursing Management
1. The patient must be isolated (enteric isolation).
2. Patient should be encouraged to rest during the acute or symptomatic
phase.
3. The patients nutritional status must be improved.
4. Appropriate measures to minimize spread of the disease must be taken.
5. Observe the patient for melena and check stools for the presence of
blood.
6. Provide optimum skin and oral care.
7. Increase the ability to carry out activities.
a. Encourage the patient to limit activity when fatigued.
b. Assist the client in planning of rest and activity.
c. Encourage gradual resumption of activities and mild exercise
during recovery.
Prevention and Control
1. Hands should be washed thoroughly after using the toilet.
2. Travelers should avoid water and ice if unsure of their purity.
3. Food handlers should be carefully screened.
4. Safe preparation and serving of food must be practiced.
5. The public should be educated on the mode of transmission of the
disease.
II. HEPATITIS B (Serum hepatitis)
Clinical Manifestations
1. Prodromal period
Page 140
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
a. Fever, malaise, and anorexia
b. Nausea, vomiting, abdominal discomfort, fever and chills
c. Jaundice, dark urine and pale stools
d. Recovery is indicated by a decline of fever and improved
appetite.
2. Fulminant hepatitis may be fatal and manifested by severe symptoms
like ascites and bleeding.
Diagnostic Procedures
1. Compliment fixation test
2. Radio-immunoassay-hemaglutinin test
3. Liver function test
4. Bile examination in blood and urine
5. Blood count
6. Serum transaminase SGOT, SGPT, ALT
7. HBsAg
Prevention
1. Blood donors must be screened to exclude carriers.
2. Caution must be observed in giving care to patients infected with HBV.
3. Hands and other skin areas must be washed immediately and
thoroughly after contact with body fluids.
4. Avoid injury with sharp objects or instruments.
5. Use disposable needles and syringes only once and dispose properly.
6. Avoid sharing toothbrushes, razors and other instruments that may be
contaminated with blood.
7. Practice safe sex.
8. Get adequate rest, sleep, and exercise, and eat nutritious foods.
9. Hepatitis B vaccine is recommended for pre-exposure.
10. Hepatitis immune globulin (HBIg) should be administered within 72
hours to those exposed directly to hepatitis B virus by either ingestion,
prick or inoculation.
III. HEPATITIS C
The infection is often asymptomatic, but once established,
can cause scarring of the liver (fibrosis) and eventually,
cirrhosis (advance scarring).
The heap C virus is associated with high rate of chronic liver
diseases (chronic hepatitis, cirrhosis, and an increased risk for
hepatocellular carcinoma).
Clients with chronic hepatitis C are considered infectious.
No vaccine is available for hepatitis C.
IV. HEPATITIS D
A patient can acquire hepatitis D virus infection at the same
time that he/she is infected with the hepatitis D virus. This is
called co-infection. A patient can also be infected with
hepatitis D virus at any time during acute hepatitis B virus
infection. This is called superinfection.
Found only in patients with an acute episode of or chronic
hepatitis B and requires the presence of HbsAg.
This virus depends on the double-shelled type B to replicate.
For this reason, type D infection does not outlast type B
infection.
Type D is rare in the United Stated, except among drug users.
Page 141
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
V. HEPATITIS E
Hepatitis E never becomes chronic (long-lasting) illness, but
on rare occasions the acute illness damages and destroys so
many liver cells that the liver can no longer function. This is
called fulminant liver failure and may cause death.
Pregnant women are at much higher risk of dying from
fulminant liver failure.
The great majority of patients who recover from acute
infection do not continue to carry HEV and cannot pass the
infection to others.
Signs and Symptoms
Assessment findings are similar for the different types of hepatitis. Signs
and symptoms progress in three stages.
Prodromal stage
Patient complains of easy fatigue,
anorexia, body malaise, headache,
arthralgia, myalgia, photophobia and
nausea with vomiting.
There are changes in patients senses of
smell and taste.
There is moderate grade fever ranging
from 37.8 38.9C.
As the prodromal stage draws to a close, urine may become
dark-colored and stools are clay-colored
Clinical jaundice stage
Patient manifests with pruritus, abdominal pain or tenderness
and indigestion.
There is yellowish discoloration of the sclera, mucous membrane
and the skin, which can last for one to two weeks.
On inspection of the skin, rashes, erythematous patches and
urticaria may be seen, especially if the client is suffering from
hepatitis B or C.
Pain, tenderness of the RUQ, an enlarged and tender liver,
splenomegaly and cervical adenopathy are present.
Recovery stage
During this stage, most of the patients symptoms decrease or
subside.
Recovery stage commonly lasts for 2-12 weeks.
Diagnosis
1. Hepatitis A: Detection of antibodies to hepatitis A confirms the
diagnosis.
Page 142
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
2. Hepatitis B: The presence of HbsAg and Hepatitis B antibodies confirms
the diagnosis.
3. Hepatitis C: The diagnosis depends on serologic testing for the specific
antibody one or more months after the onset of acute hepatitis.
4. Hepatitis D: Detection of intrahepatic delta or immunoglobulin M (IgM)
establishes the diagnosis.
5. Hepatitis E: Detection of hepatitis E antigen supports the diagnosis.
Following are additional findings from liver functions tests that
support the diagnosis:
1. Serum aspartate aminotransferase and serum alanine
aminotranferase are increased in the prodromal stage of acute viral
hepatitis.
2. Serum alkaline phosphatase levels are slightly increased.
3. Serum bilirubin levels are elevated and may continue to rise in
severe cases.
4. Prolonged prothrombin time (PT) (more than 3 seconds) indicates
severe liver damage.
5. WBC reveals transient neutropenia and lymphopenia followed by
lymphocytosis.
6. Liver biopsy is performed only if diagnosis is questionable.
General Nursing Management
1. Suggest that a large meal be eaten in the morning because nausea
tends to intensity as the days progresses.
2. Provide diversional activities to relieve boredom and anxiety.
3. Encourage anorexic patients to take juices with occasional ice chips to
maintain hydration without inducing vomiting.
4. Monitor the patients weight daily. Record intake and output.
5. Observe stools for color, consistency and amount. Record the frequency
of bowel movement.
6. Before the patient is discharge, discuss restrictions and how to prevent
recurrence of hepatitis.
B. NON-VIRAL HEPATITIS
Non-viral hepatitis is classified as either toxic or drug-induced
(idiocyncratic) hepatitis. Most of the patients recover from this type of
hepatitis, although a few develop fulminant hepatitis or cirrhosis.
Causes
1. Alcohol overuse follows heavy alcohol consumption
2. Direct hepatotoxicity hepatocellular damage and necrosis usually
caused by toxins; it is a dose-dependent and occurs primarily in
acetaminophen overdose.
3. Idiosyncratic hepatotoxicity follows a sensitization period of several
weeks caused by the hosts hypersensitivity to medication, such as, INH,
methyldopa, lovastatin and halothane.
4. Choleestatic reactions caused by a lack of bile excretion; direct
hepatotoxicity from hormonal contraceptives or anabolic steroids; and
hypersensitivity to antibiotics, thyroid medications, anti-diabetics and
cytotoxic drugs.
5. Metabolic and autoimmune disorders acute exacerbations of sub-
clinical liver disease.
Page 143
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XVII. CRYPTOSPORIDIOSIS
A. Important information
1. It is an illness caused by a parasite.
2. The parasite lives in soil, food and water.
3. It may also be on surfaces that have been contaminated with waste.
You can become infected if you swallow the parasite.
B. AKA: Crypto
C. Causative agent: Cryptosporidium
D. Mode of transmission:
By putting something in your mouth or accidentally swallowing
something that has come into contact with stool of a person or animal
infected with Crypto.
By swallowing recreational water contaminated with Crypto.
By swallowing water or beverages contaminated with stool from
infected humans or animals.
By eating uncooked food contaminated with Crypto.
By touching your mouth with contaminated hands.
By exposure to human feces through sexual contact.
E. Signs and symptoms
1. Watery diarrhea
2. Other symptoms include:
Dehydration
Weight loss
Stomach cramps or pain
Fever
Nausea
Vomiting
F. Diagnostic
1. Examination of stool samples
different techniques (e.g., acid-fast staining, direct fluorescent
antibody [DFA] , and/or enzyme immunoassays for detection
of Cryptosporidium sp. antigens).
G. Management
PREVENTION
Wash hands with soap and water for at least 20 seconds, rubbing
hands together vigorously and scrubbing all surfaces:
Before preparing or eating food
Page 144
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
After using the toilet
After changing diapers or cleaning up a child who has
used the toilet
Before and after tending to someone who is ill with
diarrhea
After handling an animal or animal waste
To reduce the risk of disease transmission, children with diarrhea
should be excluded from child care settings until the diarrhea has
stopped.
not swimming if you are experiencing diarrhea (this is essential
for children in diapers). If diagnosed with cryptosporidiosis, do not
swim for at least 2 weeks after diarrhea stops.
Shower before entering the water.
Wash children thoroughly (especially their bottoms) with soap
and water after they use the toilet or their diapers are changed and
before they enter the water.
Take children on frequent bathroom breaks and check their
diapers often.
Change diapers in the bathroom, not at the poolside.
Minimize contact with the feces of all animals, particularly young
animals.
When cleaning up animal feces, wear disposable gloves, and
always wash hands when finished.
Wash hands after any contact with animals or their living areas.
Wash hands after gardening, even if wearing gloves.
Avoid close contact with any person or animal that has
cryptosporidiosis. Cryptosporidiosis can become a life threatening
disease for immunocompromised persons.
Do not handle animal feces because infection can be life
threatening for immunocompromised persons.
TREATMENT
Nitazoxanide has been FDA-approved for treatment of diarrhea
caused byCryptosporidium in people with healthy immune systems
and is available by prescription.
Consult with your health care provider for more information. Most
people who have healthy immune systems will recover without
treatment.
Diarrhea can be managed by drinking plenty of fluids to prevent
dehydration
Page 145
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
XVIII. LISTERIOSIS
A. Important information
1. It is a serious infection usually caused by eating food contaminated.
B. AKA: Listeria
C. Causative agent: Listeria monocytogenes
D. Mode of transmission:
Consumption of contaminated food
Nosocomial transmission have been reported(rare)
E. Signs and symptoms
Fever and muscle aches, sometimes preceded by diarrhea or other
gastrointestinal symptoms. Almost everyone who is diagnosed with
listeriosis has "invasive" infection, in which the bacteria spread beyond
the gastrointestinal tract.
The symptoms vary with the infected person:
Pregnant women: Pregnant women typically experience only a mild, flu-
like illness. However, infections during pregnancy can lead to
miscarriage, stillbirth, premature delivery, or life-threatening infection of
the newborn.
Persons other than pregnant women: Symptoms, in addition to fever
and muscle aches, can include headache, stiff neck, confusion, loss of
balance, and convulsions.
F. Diagnostic
1. A blood or spinal fluid test (to look for the bacteria)
G. Management
PREVENTION
Proper washing of foods
Keep your kitchen and environment cleaner and safer.
Cook meat and poultry thoroughly.
Store foods safely.
Choose safer foods.
TREATMENT
Listeriosis is treated with antibiotics. A person in a high-risk
category who experiences flu-like symptoms within 2 months of
eating contaminated food should seek medical care and tell the
physician or health care provider about eating the contaminated
food.
If a person has eaten food contaminated with Listeria and does
not have any symptoms, most experts believe that no tests or
treatment are needed, even for persons at high risk for listeriosis.
Page 146
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
DISEASES AFFECTING THE LYMPHATIC/IMMUNE
SYSTEM
I. FILARIASIS
A. Important information
1. Often progresses to become chronic, debilitating and disfiguring
because its symptoms are not only unfamiliar, they are also not
noticeable.
2. Because of the pts physical appearance, a social stigma is attached to
it.
3. It is a parasitic disease caused by the microscopic, threadlike African
eye worm
B. AKA: Elephantiasis
C. Causative agent: Wuchereria bancrofti; Brugia malayi; Brugia
timori; Loa loa (deer fly)
D. Incubation period: From the entry of the infective larvae to the devt of
symptoms ranges from 8-16 months
E. Mode of transmission:
Mosquito bite- from person to person
F. Signs and symptoms
1. On-and-off chills
2. Headache
3. Fever lasts between 3 months and 1 yr after insect bite
4. Swelling, redness and pain in the arms, legs or scrotum
5. Areas of abscesses may appear-result of dying worms
Asymptomatic stage Acute stage Chronic stage
For yrs or even
lifetime
Characterized
only by presence
of microfiliriae in
Lymphadenitis
(inflammation of
lymph nodes)
Lymphagitis
(inflammation of
Develop 10-15 yrs
from the onset of
the 1
st
attack
Hydrocele
(swelling of
Page 147
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
the blood lymph vessels)
Male genitalia:
Funiculitis,
epidydimitis,
orchitis (red,
painful and tender
scrotum)
scrotum)
Lymphedema (
temporary
swelling of the
upper and lower
extremities)
Elephantiasis
enlargement and
thickening of the
skin of the lower
and/or upper
extremities,
scrotum and
breasts
G. Diagnostic
1. Circulating filarial antigen (CFA) test/ Immunochromatographic
test (ICT) performed on a finger-prick blood droplet taken anytime of
the day, results are available in a few minutes
2. Nocturnal Blood Exam (NBE)- done after 8:00 pm
3. Pts hx taken for signs of lymphatic obstruction
H. Management
PREVENTION
Sleep under a mosquito net
Use mosquito repellant in the hrs between dusk and dawn
Take yearly dose of meds that kills the worms circulating in the
blood
TREATMENT
Ivermectin, albendazole or diethylcarbamazine (DEC) tx
for eliminating the larvae, killing the adult worms, impairing to
reproduce (started at low dose)
Surgery to remove surplus tissue and provide to drain the fluid
around the damaged lymphatic vessels
Surgery to minimize enlargement of the scrotum
Elevating the legs and providing support with elastic bandages
DEC-fortified salt is helpful
NURSING CARE
Health education
Environmental sanitation
Pyschological and emotional support
Personal hygiene
Explain the course of the disease to the client and his/her family
Page 148
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
II. INFECTIOUS MONONUCLEOSIS
A. Important information
1. It is an acute self-limiting disease of the lymphatic system
B. AKA: Glandular Fever; mono
C. Causative agent: Epstein-Barr virus member of the herpes group
D. Incubation period: 30-50 days, average: 6 wks
E. Mode of transmission:
Close personal contact via oral route in children and kissing in young
adults, synonym kissing disease
Via saliva, blood and genital secretions
Contagious is low among exposed individuals
High and lasting immunity develops
F. Signs and symptoms
1. Fatigue, Anorexia, Inability to concentrate, chilly sensation and
headache
2. Fever lasts for 5 days
3. Sore throat and enlarged lymphnodes
4. Sore throat accompanied by exudative tonsillitis- whitish, pasty
exudates and foul-smelling and spreading greenish-gray membrane
often leave ulceration
5. Dysphagia diffulty swallowing
Page 149
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
6. Palatine petechiae are seen in the 1
st
wk
7. Reto-orbital headache, photophobia and puffy eyelids
8. Splenomegaly, hepatomegaly and jaundice appear 10-15% of cases
G. Complication
1. Pneumonia
2. Meningitis, encephalitis and Guillain-Barr Syndrome (GBS)
3. hematological manifestations
H. Diagnostic
1. Lymphocytosis
2. (+) for cephalin-cholesterol flocculation test- laboratory test
for the nonspecific measurement of blood globulins, a group of
proteins that appear in abnormally high concentrations
(hyperglobulinemia) in association with certain diseases. The test
consists of adding blood serum to a suitably prepared emulsion of
cephalin-cholesterol. A flocculent precipitate will form if the serum is
abnormally high in globulins.
3. Increased in transaminase
4
levels, especially SGOT, SGPT and LDH
4. Increased in total Ig M levels
I. Management
TREATMENT
Tx is purely symptomatic and non-specific
Use of antibiotics is no help
Steroids are beneficial in the presence of airway obstruction
and CNS involvement
Bed rest and sufficient fluids
NURSING CARE
Properly disposal of oral secretions
Cautioned to avoid pts straining or refrain from strenuous
activity
Cooling measures
Encourage soft diet and Increase fluid intake
Page 150
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
DISEASES AFFECTING THE GENITO-URINARY
SYSTEM
I. ACQUIRED IMMUNE DEFICIENCY
SYNDROME
A. Important information
1. It is acquired, which means it is neither hereditary nor inborn.
2. It involves an immune deficiency.
3. When a persons immune system breaks down, he or she becomes
susceptible to many infections, which eventually lead to death.
4. It is a syndrome, a combination of signs and symptoms that form a
distinct clinical picture of disorder.
5. HIV refers to human immunodeficiency virus (HIV), which causes
AIDS.
B. AKA: AIDS
C. Causative agent: Human immunodeficiency virus (HIV)
It is a retrovirus belonging to the family of lentiviruses (slow viruses)
D. Mode of transmission:
Sexual contact with an infected person,
Injection of infected blood or blood products, and
Perinatal or vertical transmission.
E. Modified Classification (Stages) Of HIV Infection
CLINICAL STAGE 1:
ASYMPTOMATIC
CLINICAL STAGE
2: EARLY (MILD)
CLINICAL
STAGE 3:
INTERMEDIA
TE
(MODERATE)
CLINICAL
STAGE 4: LATE
(SEVERE) AIDS
Asymptomatic/ac
ute HIV infection
is characterized
by general
lymphadenopathy
Weight loss
greater than
10% of body
weight
Minor
mucocutaneous
manifestation,
Weight loss
greater
than 10%
Chronic
unexplaine
d diarrhea
for more
HIV wasting
syndrome
Pneumocystis
carinii
pneumonia
Toxoplasmosis
of the brain
Page 151
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
like;
a. Seborrhic
dermatitis
b. Fungal nail
infection
c. Recurrent
oral
ulceration
d. Angular
cheilitis
e. Recurrent
respiratory
infection
(rhinitis,
tonsilophary
ngitis)
than one
month
Oral
candidiasis
(thrush)
Oral hairy
leukoplakia
Severe
bacterial
infection,
like
pneumonia
Cryptosporidio
sis with
diarrhea for
more than one
month
Herpes
simplex virus
infection
Progressive
multifocal
leukoencephal
opathy
Disseminated
endemic
myocosis
F. Signs and symptoms
MINOR SIGNS
1. Persistent cough for one month
2. Generalized pruritic dermatitis
3. Recurrent herpes zoster infection
4. Oropharyngeal candidiasis
5. Chronic disseminated herpes simplex infection
6. Generalized lymphadenopathy
MAJOR SIGNS
1. Loss of weight 10% of body weight
2. Chronic diarrhea for more than one month
3. Prolonged fever for one month
TOP 10 SYMPTOMS OF HIV/AIDS
1. Depression
2. Diarrhea
3. Thrush
4. Weight loss
5. Lipodystrophy (fat redistribution syndrome)
6. Sinus infection
7. Fatigue
8. Nausea and vomiting
9. Lactic acidosis lactic acid builds up in the clients body due to
damage in the mitochondria, the powerhouse of the cell
10. Burning and tingling of the feet and hands (peripheral neuropathy)
G. Common Opportunistic Infections
1. Bacterial
Page 152
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
a. MAC mycobacterium avium complex, a TB-like manifestation
that usually occurs when the patients CD count is below 50
b. Tuberculosis
c. Salmonillosis
2. Viral
a. Herpes
b. Hepatitis
c. Genital warts
d. CMV (Cryptomegalovirus) can cause retinitis, pain on swallowing
and numbness of the legs. This can be transmitted through
semen, vaginal secretions, blood and breast milk.
e. Molluscum contagiosum a disease of the skin and mucous
membranes characterized by dome-shape papules that usually
occur on the face, trunk and extremities.
3. Fungal
a. Candidiasis
b. Cryptococcal meningitis
c. Histoplasmosis small lesions that appear on the skin or usually
transmitted by direct contact; it is autoinoculable. The organism
is resistant to treatment. When the CD count falls below 200,
lesions tend to proliferate and start to spread. Other symptoms
are fever, adenopathy, cough, shortness of breath, and weight
loss.
4. Pneumonias
a. Bacterial
b. Pneucyystis carinii pneumonia (PCP) an typical type of
pneumonia
5. Cancers
a. Kaposis sarcoma cancerous lesion caused by overgrowth of
blood vessels. KS typically appears as painless pink or purple
spots or nodules on the surface of the skin or oral cavity. It can
also occur internally, especially on the intestine, lymph nodes and
lungs. The cancer can spread and can also attack the eyes.
b. Cervical dysplasia and cancer Researchers found out that
women with HIV have higher rated of this type of cancer.
Cervical carnicoma is associated with Human Papilloma Virus
(HPV).
c. Non-Hodgkins lymphoma cancerous tumor of the lymph nodes.
This is usually a late manifestation of HIV infection.
6. Parasitic
a. Toxoplasmosis parasitic disease that causes neurologic
symptoms
b. Cryptosporidiosis is caused by the microscopic parasite
Cryptosporidium, commonly known as crypto.
It can cause severe illness in people with HIV. If CD count is
below 200, crypto may cause symptoms for a long time. If the
CD count is above 200, symptoms may appear only for one to
three weeks. Cryptosporidiosis spreads by having contact with
feces containing crypto. It is not transmitted by contact with
blood. There is no drug cure for crypto. However, anti-retroviral
medicine decrease or get rid of symptoms.
Signs and Symptoms
Watery diarrhea
Abdominal cramps
Low-grade fever
Page 153
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
Weight loss due to persistent diarrhea
Preventive Measure Against Crypto
1. Wash hands thoroughly after contact with feces.
2. Practice safe sex.
3. Be careful not to swallow water when swimming.
4. Wash and/or cook food properly.
5. Drink safe water.
H. Mode of Transmission
Sexual intercourse
Blood transfusion and sharing of infected syringes and needles among
intravenous drug users
Vertical or perinatal transmission (from pregnant woman to the fetus
during pregnancy, child delivery, or breastfeeding)
There are several ways of receiving infected blood:
1. Blood transfusion
2. Sharing of unsterilized syringes or needles used for intravenous
injections
3. Transmission during pregnancy
a. May be transplacental
b. There is greater risk of transmission when the mother has
developed advanced AIDS
4. Organ donation
5. Accidental exposure in hospitals or clinics
I. Diagnostic
1. EIA or ELISA enzyme-linked immunosorbent assay
2. Particle agglutination (PA) test
3. Western blot analysis confirmatory diagnostic test
Page 154
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
4. Immunoflourescent test
5. Radio immuno-precipitation assay (RIPA)
6. HIV antibody test
When HIV antibodies are not detectable in the blood at the time of
examination, it is considered a negative antibody test.
When HIV antibodies are present in the blood in the positive
antibody test, the person is considered HIV-positive.
J. Management
TREATMENT
AIDS drugs are medicines used to treat but not cure HIV infection.
These drugs are sometimes referred to as anti-retroviral/anteroviral
drugs. These work by inhibiting the reproduction of the virus. These are
two groups of anteroviral drugs reverse transcriptase inhibitors and
protease inhibitors:
1. Reverse transcriptase inhibitors They inhibit the enzyme
called reverse transcriptase, which is needed to copy information for
the virus to replicate. These drugs are:
a. Zedovudine (ZDV) Retirvir
b. Zalcitabine Havid
c. Stavudine Zerit
d. Lamivudine Epivir
e. Nevirapine Viramune
f. Didanosine Videx
2. Protease inhibitors. They work by inhibiting the enzyme
protease which are needed for the assembly of viral particles. These
drugs are:
a. Saquinavir Invarase
b. Ritonavir Norvir
c. Indinavir Crixivan
NURSING CARE
1. Health education. The healthcare worker must:
a. Give practical advice;
b. Inform the client of the disease process and the mode of
transmission;
c. Emphasize the AIDS Awareness Program;
d. Avoid judgmental and moralistic message;
e. Be consistent and concise in giving instructions, especially
those about taking medications;
f. Use positive statement; and
g. Encourage client to trace or identify previous contacts for
proper management
2. Practice universal/standard precaution
a. There is a need for a thorough medical handwashing after
every contact with each patient and after removing the gown and
gloves, and before leaving the room of an AIDS suspect or known
AIDS patient.
Page 155
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
b. Use of universal barriers or personal protective equipment
(PPE) e.g., cap, mask, gloves, CD gown, face shield/goggles, is
very necessary.
3. Prevention
a. Care should be taken to avoid accidental pricks from sharp
instruments contaminated with potentially infection materials
from an AIDS patient.
b. Gloves should be worn when handling blood specimens and
other body secretions, as well as surfaces, materials, and object
exposed to them.
c. Blood and other specimens should be labeled with a special
warning such as AIDS Precaution.
d. Blood spills should be cleaned immediately using common
household disinfectants, such as chlorox.
e. Needles should not be bent after use, but should be disposed
into a puncture-resistant container.
f. Personal articles, like razors or razor blades and
toothbrushes, should not be shared with other members of the
family. Razor blades may be disposed in the same manner as
needles.
g. Patients with active AIDS should be isolated.
h. Clients considered at risk for HIV should not be allowed to
donate blood or any organ of the body.
i. Encourage monogamous relationships.
j. HIV-infected pregnant women should go into regular prenatal,
interpartal, and postpartal care.
k. Speak openly with partners about safer sex techniques and
HIV status.
THE FOUR CS IN THE MANAGEMENT OF HIV/AIDS
1. Compliance making sure the client sticks with the program.
2. Counseling/education
a. Giving instructions about the treatment
b. Disseminating information about the disease
c. Providing guidance on how to avoid contracting STD again
d. Sharing facts about HIV and AIDS
3. Contact tracing tracing and providing treatment with
partners.
4. Condoms promoting the use of condoms by giving away
samples and providing information on their proper use.
Page 156
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
II. CANDIDIASIS
A. Important information
1. It is an infection that ranges from a mild superficial fungal infection, to
systemic and potentially life-threatening disease.
2. Infects the nails (onychomycosis), the skin (diaper rash), mucous
membrane, particularly those of the oropharynx (thrush), vagina
(monillasis), esophagus, and the GIT.
B. AKA: Moniliasis; Candidosis
C. Causative agent: Candida albicans
Organisms are part of the normal flora of the GIT, mouth, vagina, and
skin
Cause infection when:
Rise in Blood glucose (DM)
Lowered Resistance (cancer)
Taking immunosuppressive drugs, exposed to radiation, aging
or infected with HIV
Level of estrogen rises in pregnant women
Introduced systematically by IV or urinary catheters, drug
abuse, hyperalimentation, or surgery
Broad-spectrum antibiotics are used
D. Mode of transmission:
Overgrowth associated with damaged skin or mucous membranes
or use of antibiotics
E. Signs and symptoms
1. Scaly, erythematous and popular skin
2. Red and swollen nails
3. Nailbeds darkened
4. Oropharngeal mucosa (thrush) cream-colored or bluish white
patches
Page 157
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
5. Retrosternal pain and regurgitation
6. Vaginal mucosa white or yellow discharge with pruritus
7. Renal system fever, flank pain, dysuria, hematuria, pyuria
8. Pulmonary hemoptysis, fever, cough
9. Brain headache, nuchal rigidity, seizures
10. Eyes- blurred vision, orbital or periorbital pain
G. Diagnostic
1. Stool culture
2. Gram-staining of skin, vaginal discharge, or scrapings
H. Management
PREVENTION
Check high-risk pt. daily for patchy areas of irritation, sore
throat, and gum bleeding
Check vaginal discharge and note the color, odor, and amount
TREATMENT
Nystatin, for oral thrush
Clitrimazole, fluconazole, ketoconazole, for mucous membrane
and vaginal infection
Fluconazole or amphotericin for systemic infxn.
NURSING CARE
Properly disposal of oral secretions
Cautioned to avoid pts straining or refrain from strenuous
activity
Cooling measures
Encourage soft diet and Increase fluid intake
Page 158
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
III. CHANCROID
A. Important information
1. It is a sexually-transmitted disease characterized by painful genital
ulcers and inguinal adenitis.
2. It affects males more than females
B. AKA: Soft Chancre; Soft Sore; Sulcus Mole
C. Causative agent: Haemophilus discreyi Gram(-) non-spore-forming
streptobacillus
D. Incubation period: 1-14 days, average: 3-5 days
E. Mode of transmission:
Sexual
F. Signs and symptoms
1. Small lesions appear at the groin or inner thigh
Males- appear on penis
Females vulva, vagina, and cervix
2. Sometimes lesions erupt on the lips, tongue, breast or navel
3. Papule rapidly ulcerates
4. Papules bleed easily and with pus
5. Within 2-3 wks, inguinal adenitis may develop
6. During healing stage, phimosis may develop- inability to retract
the distal foreskin over the glans penis
G. Diagnostic
1. Gram stain of ulcer exudates
2. Biopsy
3. Darkfield examination and serologic test
Page 159
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
H. Management
PREVENTION
Advice client to avoid sexual contact with infected persons.
Use condoms during sexual activity
Wash genitalia with soap and water after sexual activity
TREATMENT
Azithromycin 500 mg, taken orally as a single dose
Erythromycin 500 mg, 1 cap BID x 7 days
Ceftriaxone 250 mg IM as a single dose
NURSING CARE
Standard precaution
Check for drug allergy
Lotion, cream or oil should be applied on lesions
Instruct pt. to abstain from sexual contact until healing is
complete (2 wks)
Pt should wash his/her genitalia daily with soap and water
Page 160
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IV. CHLAMYDIA
A. Important information
1. It is a sexually-transmitted disease
2. When transmitted through sexual contact, the bacteria can infect the
urinary and reproductive organs.
B. AKA: Chlamydial infections
C. Causative agent: Chlamydia trachomatis
2 bacterias are: a) Chlamydia pneumonia-through coughing and
sneezing and b) Chlamydia psittaci birds can pass to humans
D. Incubation period: 7-21 days
2-3 wks for males; usually no symptoms in females
E. Mode of transmission:
Vaginal or rectal intercourse
Through oral-genital contact with an infected person
Infants can become infected during vaginal delivery develop
conjunctivitis, otitis media and pneumonia
F. Signs and symptoms
Women Men Some patients
With cervitis develop
cervical erosion,
mucopurulent discharges,
pelvic pain, and
dyspareunia
With endometritis or
salphingitis signs of
pelvic inflammatory
disease:
Pain and tenderness
of the abdomen,
cervix, and lymph
nodes
Chills and fever
Breakthrough
With Urethritis:
Dysuria
Erythema
Tenderness of
urethral meatus
Urinary frequency
Pruritus
Urethral
discharge
With epididymis:
Painful scrotal
swelling and
urethral
discharge
Diarrhea
Tenesmus
Pruritus
Bloody
discharge
Diffuse
ulceration in
the
rectosigmoid
colon
Page 161
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
bleeding and
bleeding after
intercourse
With urethral syndrome:
Dysuria
Pyuria
Urinary frequency
G. Diagnostic
1. Swab from the site of infection
2. Culture of aspirated materials
3. ELISA
4. Direct fluorescent antibody test
H. Management
TREATMENT
Doxycycline oral for 7 days
Azithromycin in single dose
NURSING CARE
Practice universal precaution
Suggest that both partners should submit for HIV testing
Check newborn for signs of chlamydial infxn.
Page 162
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
V. GARDENELLA VAGINITIS
A. Important information
1. It is a common condition in adults.
2. It is common cause of vaginal discharge in women although clients are
asymptomatic.
B. AKA: Bacterial vaginosis; Non-specific vaginitis
C. Causative agent: Gardnerella vaginalis and vaginal anaerobes
D. Mode of transmission:
Having multiple sexual partners
Douching
After other genital infxn and invasive gynecological procedures
E. Signs and symptoms
1. Usually no edema or erythema of vulva or vagina
2. Grey-white to yellow-white discharge clinging to external vulva and
vaginal walls
3. Clue cells
4. pH of discharge is above 4.7
5. Fish like odor
F. Diagnostic
1. Microscopic slide
2. Chemical analysis of vaginal material
3. Culture test from infxn site
G. Management
TREATMENT
Metronidazole (Flagyl) p.o. twice a day for 1 wk; vaginal gel is
also available
Clindamycin (Cleocin) vaginal cream or ovules (oval
suppositories) are also effective
Recurrent bacterial vaginosis should be tested for gonorrhea and
Chlamydia and her partners
NURSING CARE
Standard precaution
Tx of sexual partners
Page 163
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VI. GENITAL WARTS
A. Important information
1. It is a sexually transmitted disease of the genitalia and perianal
regions characterized by multiple fleshy, painless growths.
B. AKA: Condylomata Acuminata
C. Causative agent: Human Papilloma virus (HPV)
D. Mode of transmission:
Sexual contact
E. Signs and symptoms
1. Soft, moist, fleshy pink to brown projections that appear in clusters
on genital, perianal or oral mucosa
2. Can cause laryngeal papillomatosis in infants born to mothers with
vaginal warts
F. Complication
Secondary infxn, giant condylomata that destroys large segments of
penile tissues and malignant transformation
G. Diagnostic
Page 164
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
1. Clinical examination
2. Biopsy confirmation test
3. Pap smear and colposcopy
4. Acetic acid-whitish color
G. Management
TREATMENT
Topical therapy: Podofilox solution mixture or imiquimod cream,
both which are applied directly to the visible warts but
contraindicated during pregnancy
Podophyllin resin, trichloroacetic acid (TCA) or bichloroacetic acid
(BCA).
Other tx are with cryotherapy, carbon dioxide lasers and
electrocautery, and simple surgical excision can be used on
extensive warts
NURSING CARE
Inform that no cure exists and there is increased risk for genital
malignancy
They should receive pap smear, other dx procedure
Encourage to use condom
Page 165
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VII. GONORRHEA
A. Important information
1. Bacterial disease limited to columnar and transitional epithelium.
2. Has greater tendency to remain localized than syphilis and occasionally
self-limiting or spontaneously cured without treatment.
3. It is a sexually-transmitted disease involving the mucosal lining of the
genitor-urinary tract, the rectum and pharynx
B. AKA: Clap; Flores Blancas; Gleet
C. Causative agent: Neisseria gonorrhoeae or gonococcus
Gram(-) non-spore forming, does not survive outside the body
Readily killed by drying, sunlight, ultraviolet light and ordinary
disinfectants
D. Incubation period: 3-21 days; average: 3-5 days
E. Period of communicability: Varies, infected person remains
communicable as long as the organisms are present in secretions and
discharges
F. Mode of transmission:
Contact from mucous membranes of infected persons(result of
sexual activity)
Utero upon rupture of membranes-in infants delivered by CS
after the membrane ruptures
Direct contact with contaminated vaginal secretions of the
mother as the baby comes out of the birth canal
Through fomites
G. Signs and symptoms
Females Males
a. Burning sensation and frequent
urination
b. Yellowish purulent vaginal
discharge
c. Redness and swelling of the
genitals
After 3- to 6- day incubation
period
a. Dysuria with purulent
discharge(gleet) from the
urethra (2-7 days after
exposures)
Page 166
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
d. Burning sensation and itching of
the vaginal area
e. Urinary frequency or with pain
f. Urethritis or cervicitis
g. Endometritis salpingitis or pelvic
peritonitis leading to infertility
h. Pelvic infxn: Fever, N&V,
Abdominal pain
i. Pregnant with gonorrhea may
infect the eye of her baby during
the vaginal delivery
b. Rectal infxn (Homosexuals)
c. Urethral inflammation
d. Prostatitis
e. Urethritis
f. Pelvic pain and fever
OTHER S/SX VARY ACCORDING TO SITE INVOLVED (Longworth,
2004)
a. Urethra Dysuria
Urinary frequency
Purulent discharge
Itching
Red and edematous meatus
b. Vulva Occasional itching
Burning and pain
Vulval symptoms are more
severe before puberty and after
menopause
c. Vagina Engorgement, redness, and
swelling
Profuse purulent discharge
d. Pelvis Severe pelvic and lower
abdominal pain
Muscle rigidity, tenderness and
abdominal distention
Tachycardia may develop in pts
with PID and salpingitis
e. Liver RUQ pain
f. Other possible symptoms Pharyngitis
Tonsilitis
Rectal burning
SIGNS OF GONOCOCCAL PHALMIA NEONATORUM
Lid edema
Bilateral conjunctival edema
Abundant purulent discharge 2-3 days after birth
Untreated gonococcal conjunctivitis can progress to corneal
ulceration and blindness
H. Complication
1. Sterility and PID in women
2. Epididymitis
3. Arthritis
4. Endocarditis
5. Conjunctivitis
6. Meningitis
I. Diagnostic
Females Males
Culture of specimen taken
from the cervix and anal
canal (inoculation of
specimen on Thayer-Martin
medium. The medium
contains antibiotic that
inhibits the growth of MO)
Gram stain
J. Management
Page 167
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
PREVENTION
Sex education
Case finding, contact tracing
Report incidence of gonorrhea
TREATMENT
For uncomplicated gonorrhea in adults: ceftriaxone 125-250
mg IM single dose; doxycycline 100 mg orally BID x 7 days
For pregnant: ceftriaxone 125-250 mg IM, single dose, plus
erythromycin 500 mg orally for 7 days
Aqueous procaine penicillin 4 million units IM after (-) skin test
Initial regimen: 1 gram ceftriaxone IM or IV every 24 hrs
Pts allergic to beta-lactams: 2 g spectinomycin IM every 12 hrs
All regimen should be continued for 24-48 hrs then switched to
complete 1 full week of antimicrobial therapy:
400 mg cefixime p.o. twice daily or 500 mg ciprofloxacin
p.o 2x daily. Ciprofloxacin contraindicated for children,
adolescents, pregnant and lactating women
Tx for gonococcal conjunctivitis requires 1 g single dose
of ciftriaxone IM and irrigation of infected eye with NSS
NURSING CARE
Before tx, ask for drug sensitivity and watch for adverse effects
Explain that until culture negative, he/she is still infectious
Practice standard precautions
Pt is considered confidential
Pt should be isolated
Pt with gonococcal arthritis, apply moist heat to relieve pain on
the affected site
Infants born with mother with gonorrhea should be instilled with
1% silver nitrate or any ophthalmic prophylaxis onto both eyes at
the time of birth
Report cases, for gonorrhea in children to Child Abuse Authorities
Encourage pt to inform sexual contacts so they can seek tx.
Advise to refrain from sexual intercourse until tx is completed
Page 168
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
VIII. HERPES SIMPLEX
A. Important information
1. It is a viral disease characterized by the appearance of sores and
blisters anywhere on the skin.
2. These sores usually occur either around the mouth and nose, or on the
genitals and buttocks.
3. It is related to the viruses that causes infectious mononucleosis
(Epstein-Barr virus), chickenpox and shingles.
B. AKA: Virus of love
C. Causative agent: Herpes simplex virus (HSV)
Type 1 Type 2
a. Information Cause cold sores, usually
infect during infancy and
childhood
Tiny, clear, fluid-filled
blisters sore
Affects the lips, mouth,
nose, chin or cheeks, occurs
shortly after exposure, may
develop on wounds
Notice symptoms or need
medical attention for relief
of pain
Appear in 2-20 days, lasts
from 7-10 days
Causes genital
sores
Affecting the
buttocks, penis,
vagina or cervix
Last 2-20 days
Affects 20% of
sexually active
person
Manifestations
include minor rash
or itching and
painful sores, fever,
muscular pain and
burning sensation
b. Mode of
transmission
By kissing and sharing
kitchen utensils and towels
Catch from family
members and friends who
carry the virus
Sexual contact
with infected
person
Spread by
touching an
unaffected part of
the body after
touching the
herpes lesion
Page 169
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
D. Signs and symptoms
I. MILD TO MODERATE
a. Oral herpes Gingivostomatitis in young children
Most common intial infxn with HSV
Vesicular and ulcerative lesions in the
buccal mucosa and tongue
Inflammation of the gums, cervical
adonopathy and fever are present
Excessive salivation results from pain
on swallowing in infants and young
children
Feeding is painful and fluid intake is
poor
b. Labial herpes Cold sores or fever blisters
Crust and heal within 3-10 days
c. Ocular herpes Herpetic keratitis major medical problem
leads to loss of vision
Accompanied by conjunctivitis and
preauricular lymphadenopathy
Recurrent keratitis is usually
unilateral, but 2-6% of cases may be
bilateral
More serious if stroma is involved
d. Cutaneous
herpes
Affect the skin on any part of the body
Accompanied by deep burning pain,
fever, skin edema, ascending
lymphagitis and regional
lymphadenopathy
Samples isolated from the above the
waistline is type 1 and those below is
type 2
e. Erythema herpes Allergic reaction
HSV lesions appear as a zosteriform
f. Gential herpes One of the most common sexually
transmitted diseases
II. SEVERE TO FATAL DISEASE
a. Newborns Neonatal herpetic infxn from maternal infxn
at time of delivery
b. Eczema
varicelliform
With atopic dermatitis
Occurs with seborrheic dermatitis
Page 170
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
eruption and diaper rash
Fatality rate from 5-10%
Death due to disseminated viremia to
the brain and visceral organs or a
superimposed bacterial infxn
c. Encephalitis One of the most common non-epidemic
forms of herpes infxn in the US
Observed in infected pt. of any age,
even who already have HSV in the
blood
E. Diagnostic
1. Clinical examination and hx
2. Culture lesions
3. Biopsy
F. Management
PREVENTION
Sex education
Case finding, contact tracing
TREATMENT
Oral anti-viral drugs such as acyclovir, famciclovir or valacyclovir
Personal hygiene
Restoration of fluid and electrolyte balance
Isolation of clients, especially those with eczema herpeticum or
neonatal herpes
Practice of universal precaution and through handwashing
Page 171
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
IX. SYPHILLIS
A. Important information
1. It is a chronic, infectious, sexually transmitted disease that usually
begins in the mucous membranes and quickly becomes systemic.
2. It is caused by a spirochete and is acquired through sexual contact.
3. It is also be congenital in nature.
B. AKA: Lues Venereal; Morbus Gallicus; Pox; S.X; Bad Blood Disease
C. Causative agent: Treponema pallidum
Beautiful fast-moving but delicate spiral thread
Has no other host but man
Passes through the mucosa even if there is no break
Does not withstand dying but can withstand considerable
temperature variation (spirochetes have been found in glass hr
after it has been rinsed in cool water)
D. Sources of infection:
Discharges from obvious or concealed lesion of the skin or mucous
membranes
Semen, blood, tears and urine of infected persons
Mucous discharges from the nose, eyes, genital tract or bowels
Surface lesions contain spirochetes in very high numbers
E. Incubation period: 10-90 days; average: 3 wks
F. Period of communicability: Variable and indefinite
G. Mode of transmission:
Direct, intimate contact with infected person
Mucus or glandular secretions transmitted to the skin or
mucous surface
Indirect contact, e.g. articles freshly soiled with discharges or
blood containing the organism
H. Signs and symptoms
I. PRIMARY SYPHILIS
a) Starts with 1 or more chancres that erupt in the genitalia, anus, nipples,
tonsils or eyelids
b) Chancres are painless, start as papule and then erode
c) Chancres have endurated, raised edges and clear bases
Page 172
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
d) Disappear after 3-6 wks even without tx
e) It is associated with lymphadenopathy that is either unilateral or
bilateral
f) In women, develop on internal surfaces, such as the cervix and the
vaginal wall.
II. SECONDARY SYPHILIS
a) Devt of mucocutaneous lesions and generalized lymphadenopathy
occurs few days 8 wks after the onset of the initial chancre
b) Rash of secondary syphilis can be macular, popular, pustular, or nodular
c) Lesions are uniform in size, well-defined and generalized
d) Macules often erupt between rolls of fat on the trunk and on the arms,
palms, soles, face and scalp
e) In warm, moist areas of the body, such as the perineum, vulva and rolls
of fats in the scrotum, lesions enlarge and erode, producing highly
contaminated pink or grayish-white lesions (condylomata lata)
f) Mild constitutional sx in the 2
nd
stage. It includes headache, anorexia,
malaise, weighlt loss, N&V, sore throat, and possibly slight fever
g) Alopecia (temporary)-hair loss
h) Nails become brittle and pitted
III. LATENT SYPHILIS
a) No clinical sx, but serologic test will prove reactive
b) 2/3 of pts remain asymptomatic until death
IV. LATE SYPHILIS
LATE, BENIGN
SYPHILIS
LATE SYPHILIS CARDIOVASCULAR
SYPHILIS
Develops between 1-
10 yrs after infxn
Gumma- typical
lesion, a chronic,
superficial nodule, or
deep granulomatous
that is solitary,
asymmetric, painless
and endurated
Appear on the skin,
bones, mucous
membranes, upper
respiratory
tract(URT), liver or
stomach
Can be found in any
bone, especially the
long bones of the
legs
Involves the liver
Cause epigastric
pain, tenderness, an
enlarged spleen and
anemia
Affects the URT,
cause perforation of
the nasal septum or
the palate
Severe- destruction
of bones and other
organs that may
lead to death
Develops about 10
yrs after the initial
infxn
May appear
asymptomatic but
may fuffer from
aortic regurgitation
and aneurysm
V. CONGENITAL SYPHILIS
a) It infects many organs when enters the fetal circulation
b) Fetus may be overwhelmed by the inxn and die
c) A syphilic stillborn may have a macerated appearance, with a collapsed
skull and a protuberant abdomen
d) Skin is a livid red color
Page 173
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
e) On autopsy, spleen and liver found to be enlarged, with intense
pancreatitis and thickening of the intestines
f) If treponemal infxn does not prove fatal, may still show alteration in
fetal devt at various stages
A. Early Congenital Syphilis B. Late Congenital Syphilis
a. Lesions of the skin and mucous
membranes:
Syphilitic pemphigus
bullous rash
Old man look
Syphilitic nonychia- nails
may be loosened and shed
Mucous patches on the lips,
mouth, throat and nasal
passages
b. Liver and spleen
Infants abdomen is
protuberant
Hepatic insufficiency
a. Interstitial keratitis most
common late lesion
Begin from 4-30 yrs or even
later
Appears circumcorneal
vascularization of the sclera
Severe lesions cause
corneal scarring, giving rise
to opacities which may
cause slight impairment of
vision or even complete
blindness
I. Complication
1. Severe damage to several organs and the nervous system
2. Heart disease, insanity and brain damage
3. Severe illness or death in newborn
J. Diagnostic
1. Dark field illumination test most effective if moist lesions are
present
2. Fluorescent treponemal antibody absorption test, in which the
specimen consists of exudates from a lesion
3. VDRL slide test and rapid plasma reagent test
4. CSF analysis
Page 174
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
K. Management
PREVENTION
Report cases
Control prostitution
Require sex workers to have regular check-ups
Proper sex education
Look for cases of syphilis infxn
Contact tracing
TREATMENT
For early syphilis, tx consists of Pen G benzathine IM (2.4 million
units)
Syphilis of more than a years duration treated with Pen G
benzathine, 2.4 million units/wk for 3 wks
Non-pregnant pats develop allergy to penicillin may be treated
with oral tetracycline or doxycycline for 15 days for early syphilis
and for 30 days for late infxn. Tetracycline is contraindicated in
pregnant women.
Must abstain from sexual contact until infxn is completely healed
NURSING CARE
Stress to the client the importance of completing the tx even
after the symptoms subside
Inform their partner that they should be tested and if necessary,
treated
Practice universal precaution
In secondary syphilis, keep lesions dry as much as possible. If
they are draining, dispose of contaminated materials properly.
In cardiovascular syphilis, check for signs of decreased cardiac
output : decreased sensorium, urine output and hypoxia, and
pulmonary congestion
In neurosyphilis, check the LOC, mood and coherence. Watch for
signs of ataxia
Encourage to undergo VDRL testing after 3, 6, 12, and 24
months to detect any possible relapse
Be sure to report all cases syphilis
Page 175
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
X. TRICHOMONIASIS
A. Important information
1. It is a protozoal infxn causing vulvo-vaginitis.
2. Not life threatening, the incidence is high worldwide and the infxn
remains a major health problem.
3. Often asymptomatic, affects 3 million people annually, and its role in
PID and infertility may be greatly underestimated.
B. AKA: Trich
C. Causative agent: Trichomonas vaginalis
Prefers alkaline environment
Alterations in the vaginal flora
D. Incubation period: 4-20 days; average: 7 days
E. Mode of transmission:
Direct sexual contact
Through contact with wet objects, such as towels, wash
clothes and douching equipment
F. Signs and symptoms
Females Males
White or greenish-yellow
odorous discharge
Vaginal itching and soreness
Painful urination
Strawberry cervix
Dyspareunia- pain during
sexual intercourse
Slight itching of penis
Painful urination
Clear discharge from penis
G. Complication
1. Long term effects in adults is known.
2. Develop cervical cancer
J. Diagnostic
1. Microscopic slide of discharge
2. Culture tests
Page 176
Systems Plus College Foundation COMMUNICABLE DISEASE
ASEO BATCH 2014
3. Vaginal examination
K. Management
TREATMENT
Single oral dose of metronidazole (Flagyl) or tinidazole
(Tindimax) with simultaneous tx of all sexual partners for cure
It may given in a 7-day regimen
Contraindicated during 1
st
trimester of pregnancy
NURSING CARE
Instruct the pt. taking metronidazole not to drink alcoholic
beverages for 24 hrs after completing therapy
Might cause N&V and headaches
Prohibition include alcohol-containing products such as cough
syrup
Personal hygiene
Tx continue through the pts menstrual period
Can be taken without regard to meals
The urine may turn dark, reddish brown
You might also like
- Measles (Rubeola Morbilli 7 Days Fever)Document3 pagesMeasles (Rubeola Morbilli 7 Days Fever)Cedric BautistaNo ratings yet
- Lerelyn Case Reading4Document53 pagesLerelyn Case Reading4Ma Lerelyn DatinguinooNo ratings yet
- Leprosy Written ReportDocument7 pagesLeprosy Written Reportnicah05No ratings yet
- Syphilis - ReportDocument4 pagesSyphilis - ReportAnna CahucomNo ratings yet
- Measles 17Document30 pagesMeasles 17Neetu GuptaNo ratings yet
- W9 Measles German Measles Influenza Chicken Pox Covid19Document16 pagesW9 Measles German Measles Influenza Chicken Pox Covid19Jamie De LunaNo ratings yet
- Dermato Venerology ScienceDocument11 pagesDermato Venerology ScienceAQis AQishNo ratings yet
- LeprosyDocument45 pagesLeprosyrouhanbinrashidNo ratings yet
- LeprosyDocument7 pagesLeprosytankmpNo ratings yet
- Leprosy 2017Document47 pagesLeprosy 2017Mangala bote Nair PSMNo ratings yet
- ScabiesDocument16 pagesScabiescarla_sarmiento4847No ratings yet
- Diphtheria and MeaslesDocument35 pagesDiphtheria and MeaslesMurugesanNo ratings yet
- Communicable Disease NursingDocument50 pagesCommunicable Disease NursingGreggy Ventura100% (1)
- Hansen's Diseases/HansenosisDocument12 pagesHansen's Diseases/HansenosisSienaNo ratings yet
- LeprosyDocument10 pagesLeprosyRizweta DestinNo ratings yet
- Eruptive Fever DiseaseDocument61 pagesEruptive Fever DiseasePearl DiBerardino100% (2)
- A. Infectious ProcessDocument22 pagesA. Infectious ProcessKyla Malapit GarvidaNo ratings yet
- Viral ExanthemsDocument133 pagesViral ExanthemsDesiree AfagaNo ratings yet
- LEPROSYDocument7 pagesLEPROSYEzra Manalansan-Beltran BaulNo ratings yet
- LeprosyDocument51 pagesLeprosySoujanya Kundu ChoudhuryNo ratings yet
- Chickenpox & ChlamydialDocument5 pagesChickenpox & ChlamydialEliezah RodriguezNo ratings yet
- Communicable Disease Lectures 2Document2 pagesCommunicable Disease Lectures 2Sheana TmplNo ratings yet
- Group 2Document10 pagesGroup 2amponsahgrace0015No ratings yet
- MEASLESDocument3 pagesMEASLESAirah CatubayNo ratings yet
- Locally Endemic Diseases ControlhandoutDocument3 pagesLocally Endemic Diseases ControlhandoutEshiebel OrganistaNo ratings yet
- Leprae and Mycobacterium Lepromatosis. Named After Physician Gerhard Armauer HansenDocument5 pagesLeprae and Mycobacterium Lepromatosis. Named After Physician Gerhard Armauer HansenTim-Tim FerrerNo ratings yet
- Sexually Transmitted DiseasesDocument174 pagesSexually Transmitted DiseasesfroizkiNo ratings yet
- School PrerequistesDocument65 pagesSchool Prerequistesmanaribrahim309No ratings yet
- Small Pox (CHN)Document13 pagesSmall Pox (CHN)Getom NgukirNo ratings yet
- Leprosy: Communicable Diseases FactsheetDocument2 pagesLeprosy: Communicable Diseases FactsheetelisabethNo ratings yet
- Leprosy Ppt2Document18 pagesLeprosy Ppt2blueprincess450No ratings yet
- Meehleib, Rachelle Ayn S. Pepino, Stephanie Kate ADocument16 pagesMeehleib, Rachelle Ayn S. Pepino, Stephanie Kate ARachelle AynNo ratings yet
- What The Heck!Document36 pagesWhat The Heck!kami alee utoNo ratings yet
- Trachoma Assignment On CHNDocument6 pagesTrachoma Assignment On CHNSovon SamantaNo ratings yet
- Differential Diagnosis 1. Atopic Dermatitis History TakingDocument13 pagesDifferential Diagnosis 1. Atopic Dermatitis History TakingCocoi MellaNo ratings yet
- SmallpoxDocument3 pagesSmallpoxKailash NagarNo ratings yet
- Master Plan Onn Skin DisordersDocument5 pagesMaster Plan Onn Skin DisordersSakthi DeviNo ratings yet
- A Simple Guide to Childhood Infectious DiseasesFrom EverandA Simple Guide to Childhood Infectious DiseasesRating: 5 out of 5 stars5/5 (1)
- Sexually Transmitted Disease (STD)Document102 pagesSexually Transmitted Disease (STD)uhurtme100% (10)
- PPS UPEC PIDSP Rashes in Children ModuleDocument232 pagesPPS UPEC PIDSP Rashes in Children ModuleIda Marionne ArriolaNo ratings yet
- ImpetigoDocument66 pagesImpetigozbestgurlNo ratings yet
- CD Integu 1Document5 pagesCD Integu 1gwen manalonNo ratings yet
- Infectious Diseases 2Document12 pagesInfectious Diseases 2Jean GolezNo ratings yet
- DermatologyDocument4 pagesDermatologyRemelou Garchitorena AlfelorNo ratings yet
- ReadingsDocument2 pagesReadingsniestephNo ratings yet
- Skin Lichen Planus, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandSkin Lichen Planus, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- CD Learning Material 2 AirborneDocument36 pagesCD Learning Material 2 Airborne2C1 - YABES, JenniferNo ratings yet
- Bacillary DysenteryDocument8 pagesBacillary DysenteryRijane Tabonoc OmlangNo ratings yet
- Exanthematous Viral Diseases: Measles/ Rubeola EtiologyDocument6 pagesExanthematous Viral Diseases: Measles/ Rubeola EtiologyElle ReyesNo ratings yet
- Dermatology RevisionDocument6 pagesDermatology RevisionLedia EssamNo ratings yet
- Communicable Disease ChartDocument2 pagesCommunicable Disease ChartkauragiousNo ratings yet
- Gusti Izza - English Medical ArticleDocument6 pagesGusti Izza - English Medical Articlenuna_idaNo ratings yet
- Pediatric Dermatology Lecture HandoutDocument62 pagesPediatric Dermatology Lecture Handoutskin_docNo ratings yet
- Measles Otherwise Known As Rubeola or Morbilli Is ADocument2 pagesMeasles Otherwise Known As Rubeola or Morbilli Is AKAREEM WAHEEDNo ratings yet
- Childhood Sicknesses1111Document17 pagesChildhood Sicknesses1111abdulrahmanbelewa96No ratings yet
- Name: Carlo M. Yao Bachelor of Science in NursingDocument33 pagesName: Carlo M. Yao Bachelor of Science in Nursingcarlo24_briggsNo ratings yet
- MEASLESDocument28 pagesMEASLESAjitesh MahalingamNo ratings yet
- CHN - Communicable DiseaseDocument117 pagesCHN - Communicable DiseaseGetom NgukirNo ratings yet
- NCMB 312 - : Bachelor of Science in Nursing Communicable Disease NursingDocument17 pagesNCMB 312 - : Bachelor of Science in Nursing Communicable Disease NursingDona Mae TaberaNo ratings yet
- CASE 2 AnatomyDocument14 pagesCASE 2 AnatomyKimsha ConcepcionNo ratings yet
- Medicine Ward NCPDocument11 pagesMedicine Ward NCPKimsha ConcepcionNo ratings yet
- CASE 1anatomyDocument34 pagesCASE 1anatomyKimsha ConcepcionNo ratings yet
- Root of The Neck (Gross)Document21 pagesRoot of The Neck (Gross)Kimsha ConcepcionNo ratings yet
- RNDocument2 pagesRNKimsha ConcepcionNo ratings yet
- Musculoskeletal Disorders in ChildrenDocument2 pagesMusculoskeletal Disorders in ChildrenAudree BustamanteNo ratings yet
- Find Jobs in PampangaDocument3 pagesFind Jobs in PampangaKimsha ConcepcionNo ratings yet
- Drug Study DMDocument5 pagesDrug Study DMKimsha ConcepcionNo ratings yet
- BiologyDocument3 pagesBiologyKimsha ConcepcionNo ratings yet
- ChloroplastsDocument12 pagesChloroplastsKimsha ConcepcionNo ratings yet
- Health EducationDocument4 pagesHealth EducationKimsha ConcepcionNo ratings yet
- Deficient Diversional ActivityDocument2 pagesDeficient Diversional ActivityKimsha Concepcion100% (2)
- Peripheral VascularDocument36 pagesPeripheral VascularKimsha ConcepcionNo ratings yet
- Health EducationDocument4 pagesHealth EducationKimsha ConcepcionNo ratings yet
- Herbal Medicines (Final)Document22 pagesHerbal Medicines (Final)Kimsha ConcepcionNo ratings yet
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Definition of TermsDocument13 pagesDefinition of TermsKimsha ConcepcionNo ratings yet
- Websites For CDDocument2 pagesWebsites For CDKimsha ConcepcionNo ratings yet
- Systems Plus College Foundation Communicable Disease: Aseo Batch 2014Document3 pagesSystems Plus College Foundation Communicable Disease: Aseo Batch 2014Kimsha ConcepcionNo ratings yet
- Definition of TermsDocument2 pagesDefinition of TermsKimsha ConcepcionNo ratings yet
- Imbalance D Nutrition Related To Fatigue As Evidenced by Poor Muscle ToneDocument2 pagesImbalance D Nutrition Related To Fatigue As Evidenced by Poor Muscle ToneKimsha ConcepcionNo ratings yet
- Ate Gara NCP (Activity Intolerance)Document2 pagesAte Gara NCP (Activity Intolerance)Kimsha ConcepcionNo ratings yet
- Academic InformationDocument15 pagesAcademic InformationKimsha ConcepcionNo ratings yet
- Pre Term Case OlieDocument10 pagesPre Term Case OlieKimsha ConcepcionNo ratings yet
- World Health Statistics Report 2007Document88 pagesWorld Health Statistics Report 2007Dr Abdul Aziz AwanNo ratings yet
- Bigay PusoDocument1 pageBigay PusoKimsha ConcepcionNo ratings yet
- Pta 41107 3233666 78096Document11 pagesPta 41107 3233666 78096Casey CoxNo ratings yet
- Tracer Survey of First Degree Graduates-Comparison ReportDocument23 pagesTracer Survey of First Degree Graduates-Comparison ReportKimsha ConcepcionNo ratings yet
- APA Style Format Daftar Pustaka PDFDocument4 pagesAPA Style Format Daftar Pustaka PDFfilantropiNo ratings yet
- Impact of Digital Media On Sleep Pattern Disturbance in Medical and Nursing StudentsDocument10 pagesImpact of Digital Media On Sleep Pattern Disturbance in Medical and Nursing StudentsValarmathiNo ratings yet
- LUS HSE FM4 455 005.01 Audit Gap Analysis ChecklistDocument10 pagesLUS HSE FM4 455 005.01 Audit Gap Analysis ChecklistRichu PaliNo ratings yet
- GHP557 - Fundamentals of Global Health - Syllabus - 28aug2021 - FinalDocument32 pagesGHP557 - Fundamentals of Global Health - Syllabus - 28aug2021 - Finalps.harsha2004No ratings yet
- Senile Cataract (Age-Related Cataract) : Practice Essentials, Background, PathophysiologyDocument6 pagesSenile Cataract (Age-Related Cataract) : Practice Essentials, Background, PathophysiologyadliahghaisaniNo ratings yet
- Menstrual Disorders WDDDocument43 pagesMenstrual Disorders WDDadystiNo ratings yet
- Chapter 1Document6 pagesChapter 1Abegail Joy AragonNo ratings yet
- Complete Guide To Pediatric NusringDocument135 pagesComplete Guide To Pediatric NusringSANKARNo ratings yet
- Bài tập tiếng anhDocument8 pagesBài tập tiếng anhLinh KhánhNo ratings yet
- The Trade Effluents (Prescribed Processes and Substances) Regulations 1992Document2 pagesThe Trade Effluents (Prescribed Processes and Substances) Regulations 1992Lúcio FernandesNo ratings yet
- Postpartum Depression in Primigravida WomenDocument22 pagesPostpartum Depression in Primigravida WomenMrs RehanNo ratings yet
- MAPEH Study NotesDocument5 pagesMAPEH Study NotesBithao DaisyNo ratings yet
- Chilomastix Mesnili: Chilomastix Mesnili Is Cosmopolitan in Distribution Although Found More Frequently inDocument3 pagesChilomastix Mesnili: Chilomastix Mesnili Is Cosmopolitan in Distribution Although Found More Frequently inNurul HidayatiNo ratings yet
- Farfalle With Creamy Bacon Sauce - Spend With PenniesDocument2 pagesFarfalle With Creamy Bacon Sauce - Spend With PenniesrectagleNo ratings yet
- 2011 Sewarage SystemDocument29 pages2011 Sewarage Systemceafalld CE AF100% (1)
- ID Pengaruh Self Selected Individual MusicDocument12 pagesID Pengaruh Self Selected Individual MusicNur AiniNo ratings yet
- Nurs FPX 4020 Assessment 2 Root Cause Analysis and Safety Improvement PlanDocument5 pagesNurs FPX 4020 Assessment 2 Root Cause Analysis and Safety Improvement PlanEmma WatsonNo ratings yet
- Novel Approaches To Clinical Trial Design and ImplementationDocument7 pagesNovel Approaches To Clinical Trial Design and ImplementationEditor IJTSRDNo ratings yet
- 2-On Site Storage Methods: 1.containersDocument12 pages2-On Site Storage Methods: 1.containersPenchalaiah100% (1)
- Workbook Answer KeyDocument27 pagesWorkbook Answer Keysalcedo4479% (56)
- A Sample Hospital Business Plan Template - ProfitableVentureDocument15 pagesA Sample Hospital Business Plan Template - ProfitableVentureMacmilan Trevor Jamu100% (1)
- BHS InggrisDocument4 pagesBHS InggrisarifinilhamNo ratings yet
- Sodium Metabisulfite SDSDocument8 pagesSodium Metabisulfite SDSChaib AhmedNo ratings yet
- IP Environmental Chem PDFDocument15 pagesIP Environmental Chem PDFAshish Kumar JhaNo ratings yet
- Sudeep SrivastavaDocument202 pagesSudeep Srivastavasandeepsrivastava41No ratings yet
- Life - Line ECMO Sell - Sheet ECMO FEB22 1 WebDocument2 pagesLife - Line ECMO Sell - Sheet ECMO FEB22 1 WebJavier Dario Cifuentes SandovalNo ratings yet
- Industrial Counseling HWDocument3 pagesIndustrial Counseling HWJoyce SisonNo ratings yet
- Patomorfologia Prezentacja - KopiaDocument14 pagesPatomorfologia Prezentacja - KopiaOlgaNo ratings yet
- Errors of Eye Refraction and HomoeopathyDocument11 pagesErrors of Eye Refraction and HomoeopathyDr. Rajneesh Kumar Sharma MD HomNo ratings yet
- Mapping Bellvitge 2023Document8 pagesMapping Bellvitge 2023Lluís Cavallé MorenoNo ratings yet
- An Overview of Refeeding SyndromeDocument7 pagesAn Overview of Refeeding Syndromeannisa ferdaNo ratings yet