Professional Documents
Culture Documents
Beta Blockers
Uploaded by
vicky_ani19860 ratings0% found this document useful (0 votes)
54 views4 pagesDocument of beta blockers
Original Title
Beta blockers
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentDocument of beta blockers
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
54 views4 pagesBeta Blockers
Uploaded by
vicky_ani1986Document of beta blockers
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 4
Beta Blockers
Reassessing Pharmacological Differences
April, 1998
blockers have grown steadily in number and application since
the introduction of propranolol in 1965. This edition will
compare the efficacy, safety, and cost of commonly prescribed
blockers. Carvedilol (Coreg), the latest addition to the
newly evolving class of combination - blockers is also
reviewed.
Comparative Pharmacology:
Despite a common chemical structure, blockers possess a
number of properties that differentiate one agent from another.
Advantages and disadvantages of these properties are often of
more theoretical than clinical significance.
Cardioselective blockers include acebutolol
(Sectral/Monitan), atenolol (Tenormin), and metoprolol
(Lopresor/Betaloc). These agents preferentially block
1
receptors found primarily in cardiac muscle, adipose tissue, and
the kidney. They have less effect on
2
receptors found in
pulmonary and vascular smooth muscle and the pancreas.
Cardioselective agents should theoretically cause less coldness
of the extremities and less bronchospasm. Unfortunately,
selectivity is dose-dependent and varies widely among patients
1
so this property cannot be relied upon to consistently provide
improved safety and reduced side effects. Non-cardioselective
agents are generally required if used to treat essential tremor or
prevent migraine.
Pindolol (Visken), oxprenolol (Trasicor), and acebutolol
have intrinsic sympathomimetic activity (ISA). These agents
act as partial agonists and cause smaller reductions in heart rate
and cardiac output. The clinical significance of these effects
has yet to be clearly demonstrated.
1
Agents with ISA should
be avoided in patients post-MI, or with CHF.
Acebutolol, pindolol, and propranolol (Inderal) also have a
local anaesthetic effect or membrane stabilizing activity
(MSA). Supratherapeutic doses are required to produce this
effect so it is usually not clinically relevant.
1
Adverse CNS effects are often thought to be related to
blockers lipophilicity, as fat-soluble agents cross the blood-
brain barrier more readily. However, frequency and severity of
CNS adverse effects may not be solely related to lipophilicity
as fatigue, mood changes, depression, and nightmares have
been reported with all blockers
1
including water-soluble
Highlights
blockers are considered first line agents along with
thiazide diuretics in patients with uncomplicated HTN,
due to proven morbidity & mortality and low cost.
Cardioselectivity may improve safety and tolerability,
however, this is not guaranteed.
Metoprolol SR combines cardioselectivity with well-
documented efficacy in angina, myocardial infarction
and CHF, and provides excellent 24h BP control.
blockers, unless contraindicated, are often preferred in
patients with stable or unstable angina, supraventricular
arrhythmia, and previous MI.
Carvedilol may be beneficial in patients with heart
failure who are refractory to other drug therapies.
agents. Cardioprotective efficacy has been associated with a
blockers degree of lipophilicity (see MI).
Hypertension:
blockers have a well established role in the treatment of
hypertension. They are still considered first line agents along
with thiazides in the management of uncomplicated
hypertension because of clinically proven reductions in
morbidity and mortality.
2
At equipotent doses, all blockers
are equally effective in reducing blood pressure.
1
blockers
may be particularly effective antihypertensives in younger
patients with high renin activity. The elderly may also benefit
from blockers especially when used in combination with
diuretics. blockers may be preferred in patients with
angina, supraventricular arrhythmia, previous MI,
migraine, anxiety, or other comorbid conditions where
blockers are of benefit.
Optimal antihypertensive therapy requires consistent BP
reduction over a 24 hour period. Although several agents may
be given once daily (acebutolol, atenolol, nadolol, pindolol,
timolol), care should be taken to ensure adequate 24 hour
control is maintained. Once daily atenolol may not control
blood pressure adequately during the early morning hours.
19,25
Sustained release (SR) metoprolol, given once daily combines
excellent 24 hour BP control with cardioselectivity.
25,26
blockers, particularly in low doses, may be better tolerated
than commonly believed. Results of TOMHS (Treatment of
Mild Hypertension Study) indicated acebutolol was associated
with the greatest overall improvement in quality of life
measures when compared with agents from 4 other classes of
antihypertensives (amlodipine, enalapril, chlorthalidone, and
doxazosin).
17
Adverse effects are further outlined in Table 2.
Angina:
blockers appear to be the most efficacious agents for the
treatment of stable and unstable angina. They are the only
antianginal agents shown to improve clinical outcomes in
patients with myocardial ischemia.
3
Their negative
chronotropic and inotropic effects decrease heart rate and
contractile force, reducing myocardial oxygen demand and
relieving angina. All blockers improve exercise tolerance
and reduce signs and symptoms of angina regardless of
differences in ISA and selectivity.
1
Combinations of a
blocker and a long-acting dihydropyridine calcium antagonist
are useful in some patients. blockers should be avoided in
vasospastic angina as uncompensated alpha receptor
stimulation may result in further vasoconstriction.
4
Myocardial Infarction (MI): Secondary prevention
Many studies in the last decade have shown the benefit of
blockers in prevention of recurrent MI and other related
complications, acutely and in the postinfarction period. Results
from major trials show a reduction in overall mortality of more
than 20-30%.
6-9
blockers with moderate to high
lipophilicity (timolol, metoprolol, propranolol) have shown
marked reductions in sudden cardiac death.
7-9
It is
postulated that these agents enter the brain rapidly and increase
vagal tone. This prevents ventricular fibrillation associated
with the increased sympathetic drive and reduced vagal tone
during an acute MI.
10
blockers appear underused in survivors
of acute MI.
5
Studies looking at pindolol and oxprenolol
showed no effect on mortality.
11,12
As both agents have ISA,
blockers with this property may not be appropriate for use post-
MI.
1
Arrhythmia:
All blockers have some inherent (Class II) antiarrhythmic
activity. They slow conduction through both the SA node and
the AV node. All blockers appear beneficial in treatment of
supraventricular arrhythmias, regardless of MSA, ISA, or
selectivity.
1
Sotalol (Sotacor) may be the preferred
blocker for arrhythmias because it has both Class II and Class
III antiarrhythmic activity. Caution is required as sotalol also
has pro-arrhythmic potential.
Heart Failure (HF):
The role of blockers in HF has yet to be clearly established.
In the past, blockers were considered contraindicated due to
their negative inotropic effects. Recent application in HF has
resulted from the beneficial effects seen in patients with MI.
Studies report improvement in hemodynamic parameters and
exercise tolerance but this is not always accompanied by
significant reductions in mortality.
6
Studies are currently
underway to assess the effect of blockers on survival in
HF.
13,14
blockers appear to have greater clinical benefits in idiopathic
dilated cardiomyopathy than in ischemic cardiomyopathy.
15
Effects on exercise tolerance and quality of life favor the
cardioselective agents.
14
blockers with ISA should be
avoided as they do not appear to have any benefical effect in
HF.
15
Initially, blockers may worsen symptoms of HF but
improvement is usually seen with long term therapy (i.e. after
1-2 months). Patients should be stabilized on a regimen of
ACE inhibitors, diuretics, and/or digoxin before starting
blockers. Initial doses should be very small, 1/10-1/20th the
antihypertensive dose, and titrated up gradually over a period of
several weeks (eg. metoprolol 6.25mg BID x 7 days; double
dose weekly till 50 mg BID or adverse affects appear
).
15,16
Approximately 15% of patients will not tolerate blocker
therapy, developing low output syndrome with bradycardia,
hypotension, edema, and progressive heart failure. Patients
intolerant to blockers tend to have right-sided failure with
ascites, jugular venous distension, tricuspid regurgitation,
increased right filling pressure,and EF of <20%. blockers are
best avoided in this population.
15
1
- lockers:
Labetalol (Trandate) was the first blocker to combine both
non-selective and vasodilatory
1
adrenergic blockade in a
single drug. Its : blockade ratio is 3:1. Labetolol IV is
indicated in various hypertensive emergencies.
Carvedilol (Coreg ) is a more potent non-selective blocker
and
1
antagonist. Unlike other blockers, carvedilol also
possesses several unique cardioprotective, anti-ischemic, and
antioxidant properties.
22
Many recent studies lend support
to the use of carvedilol in HF.
23
Most impressive of these, the
US Carvedilol Heart Failure Study was terminated early after a
6 month follow-up showed a 65% reduction in overall mortality
in carvedilol vs. placebo treated patients. All study patients
were stabilized on diuretics, ACE inhibitors, and digoxin. Until
further trials are completed, carvedilol serves as a promising
alternative in HF patients refractory to other therapy. Although
carvedilol is a potent antihypertensive, it is not currently
approved in Canada for the treatment of hypertension.
Carvedilol is generally well tolerated. Effective doses are
lower then comparable doses of blockers because of its
combined mechanisms of action. Carvedilols blocking
activity reduces reflex tachycardia and fluid retention usually
seen with blockers. Complaints of cold extremities,
bradycardia, and reduced cardiac output seen with pure
blockers are minimized by carvedilols vasodilatory effect.
21
Adverse effects are more common early in therapy and are
often dose-related. Common complaints include dizziness,
headache, and orthostatic hypotension as well as fatigue and
asthenia.
20
Unlike other blockers, carvedilol does not appear
to adversely affect lipid profiles or glucose metabolism.
20
Cautious use is still advised in diabetics due to masking of signs
of hypoglycemia. Carvedilol does not appear to cause
deteriorations in renal function because of its vasodilatory
effect, and it actually reduces microalbuminuria.
20
References available on request.
The Rx Files: Beta Blockers (BBs)
Supplementary Tables
Table 1
Contraindications and Precautions
Contraindications
Sick sinus syndrome or 2nd/3rd degree AV block
Cardiogenic shock
Uncompensated CHF
Reactive airway disease (asthma,COPD,emphysema)
Precautions
Severe hypotension (SBP<100 mm or HR <60)
Peripheral vascular disease - exacerbated especially by
non-selective blockers
Vasospastic angina - uncompensated alpha vasoconstriction
Diabetes may prolong/exacerbate hypoglycemia in insulin
dependent pts. due to inhibition of gluconeogenesis, masking of
warning signs (tachycardia/tremor), profound bradycardia and
hypertension; In non-insulin dependent pts. may hyper-
glycemia due to inhibition of insulin release and tissue uptake
Mental depression - may be exacerbated
Pregnancy - FDA categorys B-C; Use cautiously when benefit
outweighs risk
Breastfeeding - excreted in breast milk to varying
degrees;Monitor infant for hypotension and bradycardia
Pediatrics - use cautiously under guidance of specialist
Table 2
Adverse Effects
General: fatigue, cold extremities, depression, sleep
disturbance, impotence, etc.
May be less frequent/severe with cardioselective agents
May respond to dose reduction
Metabolic: loss of glycemic control
Usually hypoglycemia in IDDM and hyperglycemia in
NIDDM
May occur less frequently with cardioselective agents
Lipids: in triglycerides, VLDL, and HDL
Moderate with non-selective BBs, minor with selective
BBs, and neutral with BBs with ISA
unknown if effect detrimental in the long-term;
cardioprotective benefits appear to outweigh risk
6
Renal: may precipitate/exacerbate renal failure due to
GFR and renal perfusion
exception: nadolol GFR by unknown mechanism
may occur less often with cardioselective or ISA BBs
Withdrawal phenomena:
abrupt withdrawal may cause rebound hypertension,
exacerbate angina, induce arrhythmia, precipitate MI
patients with coronary artery disease at high risk
gradually reduce dose over a number of days before
stopping
Table 3
Drug Interactions
18
Amiodarone - risk of bradycardia, ventricular arrhythmia,
cardiac arrest
Barbiturates, rifampin - effect of hepatically cleared BBs
due to metabolism
Benzodiazepines, phenothiazines - effect may be with
hepatically cleared BBs due to metabolism
Calcium Channel Blockers - potentiate effects and possible
toxicity of either group of drugs
Cimetidine - effect of hepatically metabolized BBs due to
metabolism
Clonidine - hypertensive reactions when clonidine withdrawn
Digoxin - risk of bradycardia especially with non-ISA BBs
Epinephrine, phenylephrine, phenylpropanolamine -
hypertensive reactions especially with non-selective BBs
Oral Hypoglycemics - hyperglycemia due to BB inhibition
of insulin release and tissue uptake
Magnesium, calcium, aluminun, antacids - effect of BB
due to bioavailability; Space administration times by 2-4hrs
NSAIDs - hypotensive effect of BB
Quinolone (floxacin) antibiotics - effect of hepatically
cleared BBs due to metabolism
Theophylline - all BBs antagonize effects; hepatically
cleared BBs metabolism and may theophylline toxicity
Table 4
Comparative Cost For 30 Days Treatment With
Commonly Used Antihypertensives (Retail cost to consumer, SK)
hydrochlorothiazide 12.5-25mg po daily
atenolol 50mg po daily
metoprolol SR 100 mg po od
acebutolol 200mg po bid
lisinopril 10mg po daily
enalapril 10mg po daily
enalapril 5mg po bid
felodipine ER 10mg po daily
diltiazem CD 180mg po daily
$ 8.00
$ 18.00
$ 16.00
$ 25.00
$ 36.00
$ 42.00
$ 64.00
$ 43.00
$ 48.00
We wish to acknowledge those who have assisted in the development and
review of this newsletter: Dr. Z. Tymchak (FM), Dr. M. Jutras (FM), Dr. M.
Lyon (Pharmacol.), Dr. R.C. Orchard (Cardiol.), Brenda Thiessen BSP, MSc
and the CDUP Advisory Committee.
Loren D. Regier BSP,BA
Sharon L. Downey BSP
The Rx Files - April, 1998
Beta Blockers
References:
1
Sproat T and Lopez L. Around the blockers one more time. DICP. 1991; 25: 962-71.
2
The sixth report of the joint national committee on prevention, detection, evaluation and treatment of high blood pressure. Arch Intern
Med. 1997; 157: 2413-2445.
3
Deedwania P and Carbajal E. Role of beta blockers in the treatment of myocardial ischemia. Am J Cardiol. 1997; 80(9b): 23J-28J.
4
Kern M, Gunz P, Horowitz J et al. Potentiation of coronary vasoconstriction by beta adrenergic blockade in patients with coronary artery
disease. Circulation. 1983:67: 1178-85..
5
Soumerai SB, McLaughlin TJ, Spiegelman D et al. Adverse outcomes of underuse of beta-blockers in elderly survivors of acute
myocardial infarction. JAMA 1997; 277:2, 115-21.
6
Freis, E. Current status of diuretics, blockers, a blockers, and a- blockers in the treatment of hypertension. Med Clin North Amer.
1997:81(6):1305-17.
7
Norwegian Multicentre Study Group. Timolol induced reduction in mortality and reinfarction in patients surviving acute myocardial
infarction. N Engl J Med. 1981; 304: 801-7.
8
Beta-blocker Heart Attack Trial Research Group. A randomized trial of propranolol in patientw with acute myocardial infarction. I.
Mortality results. JAMA 1982; 247: 1707-1714.
9
Olsson G, Wikstrand J, Warnol I et al. Metoprolol-induced reduction in postinfarction mortality: pooled results from five double-blind
randomized trials. Eur Heart J 1992; 13: 28-32.
10
Kendall, MJ. Clinical relevance of pharmacokinetic differences between blockers. Am J of Cardiol. 1997; 80(9B): 15J-19J.
11
European Infarction Study Group (EIS). European infarction study; a secondary prevention study with slow release oxprenolol after
MI: morbitity and mortality. Eur Heart J. 1984; 5:189-202.
12
Austrian and Swedish Pindolol Study Group. The effect of pindolol on the two years mortality after complicated MI. Eur Heart J.
1983; 4:367-75.
13
Hjalmarson A and Waagstein F. The role of blockers in treatment of cardiomyopathy and ischemic heart failure. Drugs. 1994;
47(suppl 4): 31-40.
14
Waagstein F. Efficacy of beta blockade in idiopathic dilated cardiomyopathy and ischemic cardiomyopathy. Am J Cardiol. 1997;
80(9B): 45J-49J.
15
Rasymas A. Rethinking the use of beta blockers in heart failure. Hospital Pharmacy Practice. 1995; March/April: 28-33.
16
Gheorghiade M, Benatar D, Konstam M et al. Pharmacotherapy for systolic dysfunction: a review of randomized clinical trials. Am J
cardiol 1997; 80(9B0: 14H-27H.
17
Grimm RH, Grandis GA, Cutler JA et al. Relationships of quality of life measures to long term lifestyle and drug treatment in the
Treatment of Mild Hypertension Study. Arch Intern Med. 1997; 157: 638-48.
18
Hansten and Horns DRUG INTERACTIONS ANALYSIS AND MONOGRAPHS. Applied Therapeutics Inc. 1997.
19
Neutel J, Smith D, Ram C et al. Application of ambulatory blood pressure monitoring in differentiating between antihypertensive
agents. Am J Med. 1993; 94: 181-7.
20
Dunn C, Lea A, and Wagstaff A. Carvedilol; a reappraisal of its pharmacologic properties and therapeutic use in cardiovascular
disorders. Drugs. 1997; 54:161-85.
21
Louis W, Krum H, and Conway E. A risk-benefit assessment of carvedilol in treatment of cardiovascular disorders. Drug Saf. 1994;
11(2): 86-93.
22
Ruffolo r and Feuerstein G. Pharmacology of carvedilol; a rationale for its use in hypertension, coronary artery disease, and chronic
heart failure. Cardiovasc Drug Ther. 1997; 11:247-56.
23
Chen B and Chow M. Focus on carvedilol, a novel blocking agent for treatment of congestive heart failure. Formulary. 1997; 32:
795-805.
24
Packer M, Bristow M, Cohn J et al. US Carvedilol Heart Failure Study Group; the effect of carvedilol on morbidity and mortality in
patients with chnoric heart failure. N Engl J Med. 1996; 334: 1349-55.
25
Kaplan N. Beta blockade in the primary prevention of hypertensive cardiovascular events with the focus on sudden cardiac death. Am J
Cardiol 1997; 80(9B):20J-22J.
26
Plosker G, Clissold S. Controlled release metoprolol formulations: A review of their pharmacodynamic and pharmacokinetic properties,
and therapeutic use in hypertension and ischaemic heart disease. Drugs 1992; 43(3):382-414.
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- American Heart Association: Advanced Cardiovascular Life Support Written ExamsDocument36 pagesAmerican Heart Association: Advanced Cardiovascular Life Support Written ExamsAndrew Sefain56% (9)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- BLS MCQ For Final Exam PDFDocument33 pagesBLS MCQ For Final Exam PDFMoaz Albaba86% (14)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Acute Pulmonary OedemaDocument31 pagesAcute Pulmonary OedemaNiwashiny Cny100% (2)
- Electrocardiogram (Ecg)Document6 pagesElectrocardiogram (Ecg)rnrmmanphd100% (1)
- Med Surg 2 MIDTERM REVIEWDocument6 pagesMed Surg 2 MIDTERM REVIEWHannah PerkinsNo ratings yet
- 8085 MicroprocessorDocument23 pages8085 Microprocessorauromaaroot196% (55)
- Structured Oral Examination in Clinical Anaesthesia Practice Ex NDocument578 pagesStructured Oral Examination in Clinical Anaesthesia Practice Ex Nkaran27091% (11)
- CPCRDocument51 pagesCPCRAnushaNo ratings yet
- Biomedical Engineering Theory and Practice-Biomedical Instrumentation-ElectrocardiographyDocument4 pagesBiomedical Engineering Theory and Practice-Biomedical Instrumentation-Electrocardiographyvicky_ani1986No ratings yet
- Density of StatesDocument5 pagesDensity of Statesvicky_ani1986No ratings yet
- 1832Document4 pages1832vicky_ani1986No ratings yet
- Everyday EBM - EKG Challenge #3 Case Conclusion - Mind Your P's and K'sDocument4 pagesEveryday EBM - EKG Challenge #3 Case Conclusion - Mind Your P's and K'svicky_ani1986No ratings yet
- ECG Wave GenDocument4 pagesECG Wave Genvicky_ani1986No ratings yet
- Digital Image Processing QuestionsDocument7 pagesDigital Image Processing Questionsvicky_ani1986No ratings yet
- Bioelectricity: action potential propagation and refractory periodDocument5 pagesBioelectricity: action potential propagation and refractory periodvicky_ani1986No ratings yet
- Atrial Bigeminy ECG Pattern and CausesDocument1 pageAtrial Bigeminy ECG Pattern and Causesvicky_ani1986No ratings yet
- Carrier Recombination and GenerationDocument5 pagesCarrier Recombination and Generationvicky_ani1986No ratings yet
- Neuro-Fuzzy Computing Model Learning and Inference Through ANFISDocument10 pagesNeuro-Fuzzy Computing Model Learning and Inference Through ANFISChanaka RupasingheNo ratings yet
- Syllabus SemiconductorDocument1 pageSyllabus Semiconductorvicky_ani1986No ratings yet
- DSPL 1 ADocument32 pagesDSPL 1 AShafiq MihatNo ratings yet
- Cardio LectDocument10 pagesCardio Lectvicky_ani1986No ratings yet
- Bilingual Version of 001Document3 pagesBilingual Version of 001Shanmugam BalasubramaniamNo ratings yet
- Sysgen UserDocument424 pagesSysgen Uservicky_ani1986No ratings yet
- PIC Stands For Peripheral Interface ControllerDocument14 pagesPIC Stands For Peripheral Interface Controllervicky_ani1986No ratings yet
- DR NonNet PDFDocument3 pagesDR NonNet PDFvicky_ani1986No ratings yet
- RRC-Application Form PDFDocument1 pageRRC-Application Form PDFvicky_ani1986No ratings yet
- EcgrevDocument13 pagesEcgrevvicky_ani1986No ratings yet
- 13Pg-04-Physics - Final Key: NO Set A Set B Set C Set DDocument6 pages13Pg-04-Physics - Final Key: NO Set A Set B Set C Set Dvicky_ani1986No ratings yet
- Matlab Daq TutorialDocument9 pagesMatlab Daq TutorialVitaly DrukerNo ratings yet
- AE75Document3 pagesAE75vicky_ani1986No ratings yet
- PaperII KeyDocument11 pagesPaperII Keymaaster321No ratings yet
- The EEG Signal: Nervous SystemDocument1 pageThe EEG Signal: Nervous Systemvicky_ani1986No ratings yet
- BibliografiaDocument1 pageBibliografiavicky_ani1986No ratings yet
- Matlab Daq TutorialDocument9 pagesMatlab Daq TutorialVitaly DrukerNo ratings yet
- Manual Pic 18F2550Document430 pagesManual Pic 18F2550Pancho NuncioNo ratings yet
- Left Ventricle Wall MotionDocument4 pagesLeft Ventricle Wall MotionSolenero SatelNo ratings yet
- Arrhythmia Clinical PracticeDocument12 pagesArrhythmia Clinical PracticeSaba ElmahadiNo ratings yet
- Cad NCPDocument1 pageCad NCPKrizzia Mae F. MayoresNo ratings yet
- Angised 90Document8 pagesAngised 90Darwesh FaqeerNo ratings yet
- Electrocardiogram ExaminationDocument13 pagesElectrocardiogram ExaminationayunisallehNo ratings yet
- Cardiotronic MedicationsDocument13 pagesCardiotronic MedicationsTee WoodNo ratings yet
- Basic Life Support PresentationDocument34 pagesBasic Life Support PresentationMona ElhassanNo ratings yet
- Cardiac Murmurs in Children: FactfileDocument2 pagesCardiac Murmurs in Children: FactfileResya I. NoerNo ratings yet
- Atrial Septal DefectDocument7 pagesAtrial Septal DefectRis Amy AyaNo ratings yet
- Management of StemisDocument20 pagesManagement of Stemisapi-269001337No ratings yet
- BBraun Medical Products PricelistDocument4 pagesBBraun Medical Products PricelistJanna FabiaNo ratings yet
- Update On Heart Failure Management and Future Directions: Hong-Mi Choi, Myung-Soo Park, and Jong-Chan YounDocument33 pagesUpdate On Heart Failure Management and Future Directions: Hong-Mi Choi, Myung-Soo Park, and Jong-Chan YounBryan NguyenNo ratings yet
- Cardiovascular Physiology: Regulation of Arterial Blood PressureDocument25 pagesCardiovascular Physiology: Regulation of Arterial Blood Pressureyuhuma_qyu6841No ratings yet
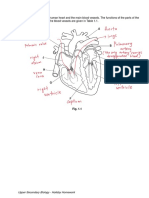
- Transport in Animals 1 StructuredDocument12 pagesTransport in Animals 1 Structuredlogy of bioNo ratings yet
- Format English Homework Chapter Four Cardiology Page 29-30Document3 pagesFormat English Homework Chapter Four Cardiology Page 29-30Alvi Jalilul HakimNo ratings yet
- Cardiac Rehabilitation and Exercise Therapy in Pediatric and Adult PatientsDocument24 pagesCardiac Rehabilitation and Exercise Therapy in Pediatric and Adult PatientsebookNo ratings yet
- Heart Failure Clinical Presentation - History, Physical Examination, Predominant Right-Sided Heart Failure PDFDocument11 pagesHeart Failure Clinical Presentation - History, Physical Examination, Predominant Right-Sided Heart Failure PDFislamiah 89No ratings yet
- EkgppDocument93 pagesEkgppLindsay WishmierNo ratings yet
- With A Healthy Heart, The Beat Goes On.Document4 pagesWith A Healthy Heart, The Beat Goes On.manish dafdaNo ratings yet
- ACLS Study Guide: New Updated 2015 AHA GuidelinesDocument33 pagesACLS Study Guide: New Updated 2015 AHA GuidelinesAdamRabbetNo ratings yet
- JV Properties of Cardiac MuscleDocument43 pagesJV Properties of Cardiac MuscleRiya GuptaNo ratings yet
- Velez College of Nursing F. Ramos Street, Cebu CityDocument57 pagesVelez College of Nursing F. Ramos Street, Cebu Cityinah krizia lagueNo ratings yet
- Secondary Stroke PreventionDocument17 pagesSecondary Stroke PreventionNidia BracamonteNo ratings yet