Professional Documents
Culture Documents
Use of G-CSF To Hasten Neutrophil Recovery 2014
Uploaded by
amandbhaskar0 ratings0% found this document useful (0 votes)
12 views5 pagesG-CSF to hasten Neutrophil recovery
Original Title
Use of G-CSF to Hasten Neutrophil Recovery 2014
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentG-CSF to hasten Neutrophil recovery
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
12 views5 pagesUse of G-CSF To Hasten Neutrophil Recovery 2014
Uploaded by
amandbhaskarG-CSF to hasten Neutrophil recovery
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 5
ORIGINAL ARTICLE
Use of G-CSF to hasten neutrophil recovery after auto-SCT
for AML is not associated with increased relapse incidence: a
report from the Acute Leukemia Working Party of the EBMT
T Czerw
1
, M Labopin
2,3,4
, N-C Gorin
2,3,4
, S Giebel
1
, D Blaise
5
, P-Y Dumas
6
, R Foa
7
, M Attal
8
, N Schaap
9
, M Michallet
10
, C Bonmati
11
,
H Veelken
12
and M Mohty
2,3,4
Application of G-CSF in AML is controversial as leukemic blasts may express receptors interacting with the cytokine, which may
stimulate leukemia growth. We retrospectively analyzed the impact of G-CSF use to accelerate neutrophil recovery after auto-SCT
on outcome. Adults with AML in rst CR autografted between 1994 and 2010 were included. Nine hundred and seventy two
patients were treated with G-CSF after auto-SCT whereas 1121 were not. BM and PB were used as a source of stem cells in 454
(22%) and 1639 (78%) cases, respectively. The incidence of relapse at 5 years in the BM-auto-SCT group was 38% for patients
receiving post-transplant G-CSF and 43% for those not treated with G-CSF, P =0.46. In the PB-auto-SCT cohort, respective
probabilities were 48% and 49%, P =0.49. No impact of the use of G-CSF could be demonstrated with respect to the probability of
leukemia-free survival: in the BM-auto-SCT group, 51% for G-CSF(+) and 48% for G-CSF(), P =0.73; in PB-auto-SCT group, 42% for
G-CSF(+) and 43% for G-CSF( ), P =0.83. Although G-CSF administration signicantly shortened the neutropenic phase, no
benecial effect was observed with regard to non-relapse mortality. In patients with AML, the use of G-CSF after auto-SCT is not
associated with increased risk of relapse irrespective of the source of stem cells used.
Bone Marrow Transplantation (2014) 49, 950954; doi:10.1038/bmt.2014.64; published online 7 April 2014
INTRODUCTION
G-CSF is widely used to accelerate neutrophil recovery after auto-
SCT with the aim of reducing the risk of infectious complications,
requirement for supportive care and duration of hospital stay.
1
Auto-SCT is an option for consolidating remission in a subgroup of
patients with AML. It is offered especially to individuals achieving
rst CR (CR1), with good or intermediate cytogenetic and
molecular risk features, and those lacking an allogeneic stem cell
donor.
2,3
Although a signicant decrease in auto-SCT has been
reported after the year 2000, this treatment modality continues to
be used by some centers. According to data from the European
Group for Blood and Marrow Transplantation (EBMT), auto-SCT
now represents about 1520% of transplants performed in AML.
4
The major disadvantage of auto-SCT is the risk of graft
contamination with leukemic blasts and the lack of GVL effect.
Hence, relapse of the disease occurring mainly within the rst 2
years is a major cause of treatment failure. It was shown that
leukemic clones surviving high-dose chemo- and/or radiotherapy
or infused with contaminated transplant material contribute to
AML recurrence.
5,6
Application of G-CSF in AML is controversial as
leukemic blasts may express G-CSF receptors interacting with the
cytokine.
7,8
Hence, there may be some concern about increased
risk of relapse and reduced leukemia-free survival (LFS) when
using G-CSF after auto-SCT in patients with AML. The goal of our
study was to assess the impact of the use of G-CSF after auto-SCT,
based on a retrospective analysis of a large cohort of patients
reported to the EBMT registry.
SUBJECTS AND METHODS
Study design and data retrieval
This study was a retrospective multicenter analysis. Data were obtained
from the EBMT registry. The registry maintains data reported by more than
500 participating transplant centers, including all consecutive stem cell
transplantations and follow-ups updated once a year. The process of
submitting data consists of mandatory lling minimum essential data
(MED-A). Audits are routinely performed to determine the accuracy of the
stored data. The study was approved by the Acute Leukemia Working Party
of the EBMT, and followed EBMT registry study guidelines.
Criteria of selection
Adults with AML (excluding acute promyelocytic leukemia) treated with
auto-SCT in CR1 between January 1994 and December 2010 were included
in the analysis. Information regarding use of G-CSF in the immediate post-
transplant period to hasten neutrophil recovery, which is documented in
research forms (MED-B), was mandatory. Patients who received growth
factors for engraftment failure were excluded from analysis.
1
Department of Bone Marrow Transplantation and Oncohematology, Maria Sklodowska-Curie Memorial Cancer Centre and Institute of Oncology, Gliwice, Poland;
2
Clinical
Hematology and Cellular Therapy Department, Hopital Saint-Antoine APHP, Paris, France;
3
INSERM UMRs 938, Paris, France;
4
Universit Pierre et Marie Curie (UPMC, Paris VI),
Paris, France;
5
Unit de transplantation et de thrapie cellulaire, Institut Paoli-Calmettes, Marseille, France;
6
Hmatologie clinique et Thrapie celllulaire, Hpital Haut-Lvque,
Pessac, France;
7
Dipartimento Biotecnologie Cellulari ed Ematologia, Universit LaSapienza, Rome, Italy;
8
CHU Department Hematologie, Hopital de Purpan, Toulouse, France;
9
Department of Hematology, Radboud UniversityNijmegen Medical Centre, Nijmegen, The Netherlands;
10
Service Hematologie, Centre Hospitalier Lyon Sud, Lyon, France;
11
Department of Hematology, Centre Hospitalier Universitaire Brabois, Vandoeuvre les Nancy, France and
12
BMT Centre Leiden, Leiden University Hospital, Leiden, The
Netherlands. Correspondence: Dr T Czerw, Department of Bone Marrow Transplantation and Oncohematology, Maria Sklodowska-Curie Memorial Cancer Centre and Institute of
Oncology, Gliwice Branch; Wybrzeze Armii Krajowej 15 Street, Gliwice 44101, Poland.
E-mail: tomcmed@gmail.com
Received 31 August 2013; revised 20 February 2014; accepted 20 February 2014; published online 7 April 2014
Bone Marrow Transplantation (2014) 49, 950954
2014 Macmillan Publishers Limited All rights reserved 0268-3369/14
www.nature.com/bmt
Patients and auto-SCT procedure
Two thousand and ninety-three auto-SCT procedures fulling search
criteria were registered in the EBMT database. Among the population of
2093 patients, 972 were treated with G-CSF after auto-SCT whereas 1121
patients did not receive cytokines to support neutrophil recovery. BM and
PB were used as the source of stem cells in 454 (22%) and 1639 (78%)
cases, respectively. Within the BM-auto-SCT group, clinical characteristics
were comparable, except for less common use of TBI as a preparative
regimen in patients who received G-CSF support after auto-SCT (32 vs 44%,
P =0.007). The same trend could be noted in PB-auto-SCT group, TBI was
used in 11% of patients who received G-CSF and in 16% of those who did
not receive G-CSF after transplantation (P =0.002). Among PB-auto-SCT,
patients in the G-CSF subgroup had also statistically signicant longer
interval between diagnosis and CR1 (42 vs 39 days, P =0.04) and a higher
percentage of them had received more than one course of induction
chemotherapy to achieve CR1 (17 vs 13%, P =0.009). This may reect a
worse AML risk prole in this subgroup. There were no differences in all the
subgroups regarding the distribution of FrenchAmericanBritish classi-
cation subtypes (data not shown). Table 1 summarizes patients
characteristics according to stem cell source.
Statistical analysis
The incidence of relapse (RI) was the primary study end point. Other points
of interest were neutrophil engraftment rate and risk of primary graft
failure, probability of LFS and non-relapse mortality (NRM).
LFS was dened as survival with no evidence of relapse. NRM was
dened as probability of death while in CR. Cumulative incidence functions
were used to estimate RI and NRM in a competing risks setting, as death
and relapse are competing together.
9
Probabilities of LFS were calculated
using the KaplanMeier estimate. Univariate analyses were done using log-
rank test for LFS, Grays test for CIF. Multivariate analyses were performed
using Cox proportional hazard model for LFS, FineGray model for RI and
NRM.
10
Patient-, disease- and transplant-related variables of the two
groups (receiving G-CSF or not) were compared using
2
or Fischers exact
test for categorical variables and MannWhitney test for continuous
variables. Factors differing between two groups in terms of distribution
and all factors known to be potentially associated with the outcome were
included in the nal model. All tests were two-sided with type I error rate
xed at 0.05.
Engraftment was dened as achieving granulocyte recovery in PB higher
than 500 cells/L for 3 consecutive days, while primary graft failure
occurred when these criteria were never met.
Separate analyses were performed for BM and PB groups because
of different kinetics of engraftment and potentially different risk of
relapse.
11
Statistical analyses were performed with SPSS 19 (SPSS Inc, Chicago, IL,
USA), and R 2.13.2 (R Development Core Team, Vienna, Austria) software
packages.
RESULTS
Relapse incidence
No impact of the use of G-CSF could be demonstrated with
respect to the RI. In the BM-auto-SCT setting, with the median
follow-up of 64 months (range, 1201) for patients treated
with G-CSF and 102 months (2214) for those not receiving
G-CSF prophylaxis, the RI at 5 years was 38% (95% CI 3144)
and 43% (3749), respectively (P =0.46). In the PB-auto-SCT cohort,
the respective median follow-up was 60 (1194) and 71 (1203),
and the RI rates were 48% (4452) and 49% (4653), P =0.49
(Figure 1).
Administration of growth factor had also no impact
on RI, irrespective of the conditioning regimen used. In the BM-
auto-SCT and TBI preparative regimen, RI reached 35% (2348) for
G-CSF(+) and 40% (3149) for G-CSF( ), P =0.59. In the
chemotherapy subgroup, RI was 38% (3047) and 46% (3754),
P =0.43, respectively. Patients transplanted with PB and condi-
tioned with TBI had RI of 41% (3051) for G-CSF(+) and 54%
(4562) for G-CSF( ), P =0.14. For those treated with chemother-
apy, corresponding gures were 49% (4553) and 48% (4552),
P =0.93.
Older age and more than one induction course needed to
achieve CR were factors that independently were associated with
higher RI both in BM- and PB-auto-SCT groups. Favorable
karyotype was predictive of lower RI within PB-auto-SCT group
(Table 2).
Hematopoietic reconstitution
In the overall population, 94% patients met the criteria of
neutrophil engraftment after BM-auto-SCT and 98% after
PB-auto-SCT. The rate of graft failure in the BM-auto-SCT
Table 1. Patient and transplant characteristics according to the use of G-CSF
BM-auto-SCT PB-auto-SCT
G-CSF ( ) G-CSF (+) P-value G-CSF ( ) G-CSF (+) P-value
N 254 200 867 772
Follow-up months (range) 102 (2214) 64 (1201) 71 (1203) 60 (1194)
Age (years) 44 (1871) 43 (1869) 0.61 48 (1878) 49 (1877) 0.05
Initial WBC (g/L) 15 (0.5350) 15 (0.4350) 0.49 17 (0.4390) 15 (0.5900) 0.42
Interval diagnosis CR1 (days) 40 39 0.3 39 42 0.04
Interval CR1-auto-SCT (days) 135 147 0.05 106 105 0.97
Induction courses (no.)
1 189 (82%) 151 (84%) 0.56 680 (87%) 567 (83%) 0.009
2 41 (18%) 28 (16%) 98 (13%) 120 (17%)
Karyotype
Favorable 14 (6%) 16 (8%) 0.27 73 (9%) 74 (10%) o0.001
Intermediate 108 (42%) 85 (42%) 476 (55%) 498 (65%)
Unfavorable 11 (4%) 3 (2%) 64 (7%) 43 (5%)
Unknown 121 (48%) 96 (48%) 254 (29%) 157 (20%)
Conditioning
Chemotherapy-based 141 (56%) 135 (68%) 0.007 724 (84%) 686 (89%) 0.002
TBI-based 112 (44%) 63 (32%) 142 (16%) 85 (11%)
Abbreviation: CR1 rst CR. Statistically signicant values are indicated in bold.
Impact of G-CSF use after auto-SCT on AML relapse
T Czerw et al
951
2014 Macmillan Publishers Limited Bone Marrow Transplantation (2014) 950 954
setting was comparable for patients receiving G-CSF prophylaxis
and those not treated with G-CSF (7 vs 5%, P =0.33).
Also, no difference could be demonstrated for the risk of graft
failure in the PB-auto-SCT cohort (2% irrespective of the
use of G-CSF, P =0.77). Among BM-auto-SCT recipients, the use
of G-CSF was associated with signicantly faster neutrophil
recovery (median 29 vs 32 days, P =0.02). The same could be
observed in the PB-auto-SCT cohort (median 12 vs 14 days,
Po0.001).
The probability of reaching platelet counts of >20 10
9
/L 6
months after BM-auto-SCT did not differ between patients
receiving G-CSF or not (80% (6788) vs 72% (5982), P =0.51).
Such difference was also not seen in PB-auto-SCT group (94%
(9195) vs 93% (9095), P =0.12).
Leukemia-free survival
The probabilities of LFS 5 years after BM-auto-SCT were 51%
(4358) for patients who received G-CSF after transplantation and
48% (4255) for those who did not receive G-CSF support, P =0.73.
In PB-auto-SCT group, corresponding values were 42% (3846) for
G-CSF(+) and 43% (4047) for G-CSF(), P =0.83.
Older age, above the median of 48 years (hazard ratio (HR) 1.61,
95% CI 1.222.12, P =0.0006 for BM-auto-SCT; HR 1.47, 95% CI
1.271.69, Po0.0001 for PB-auto-SCT), and more than one
induction course needed to achieve CR (HR 1.7, 95% CI 1.212.39,
P =0.002 for BM-auto-SCT; HR 1.41, 95% CI 1.171.69, P =0.0003
for PB-auto-SCT) were independently associated with worse LFS
both in BM- and PB-auto-SCT groups. Favorable karyotype was
predictive of better LFS within PB-auto-SCT group (HR 0.43, 95% CI
0.310.6, Po0.0001).
Non-relapse mortality
No signicant effect was observed for NRM. In the BM-auto-SCT
group, NRM was calculated as 12% (717) for G-CSF(+) and 8%
(512) for G-CSF( ), P =0.12. In the PB-auto-SCT group, 9% (711)
for G-CSF(+) and 7% (59) for G-CSF( ), P =0.26.
In a multivariate analysis, year of transplantation (after median
2001) was found to be independently associated with a lower
probability of NRM among patients transplanted with BM as a
stem cell source (HR 0.48, 95% CI 0.260.91, P =0.02). In the PB-
auto-SCT cohort, older age was the only factor that signicantly
affected higher NRM (HR 2.47, 95% CI 1.673.65, Po0.0001).
DISCUSSION
Myeloid blasts express receptors for hematopoietic growth factors,
and may exhibit variable responses when being exposed to them.
This includes either malignant clone proliferation or granulocytic
maturation.
7,8,12
In the current study, we have addressed the issue of the
potential impact of the use of G-CSF early after auto-SCT to
accelerate hematopoietic recovery on the probability of AML
recurrence. To the best of our knowledge this is the rst study
focusing on this issue taking into account a large, homogenous
population of autografted patients. In all, we could not
demonstrate an impact of the G-CSF prophylaxis on the RI. This
held true for both BM and PB used as a source of stem cells.
Moreover, the effect could not be shown when patients treated
with chemotherapy and TBI-based conditioning were analyzed
separately. The potential limitation of these ndings is that precise
determination of the reasons to use G-CSF after auto-SCT by the
Years after transplantation
C
u
m
u
l
a
t
i
v
e
i
n
c
i
d
e
n
c
e
o
f
r
e
l
a
p
s
e
0 1 2 3 4
P=0.46 P=0.49
5
0.0
0.2
0.4
0.6
0.8
1.0
BM-auto-SCT PB-auto-SCT
0.0
0.2
0.4
0.6
0.8
1.0
Years after transplantation
C
u
m
u
l
a
t
i
v
e
i
n
c
i
d
e
n
c
e
o
f
r
e
l
a
p
s
e
0 1 2 3 4 5
no GCSF
GCSF
no GCSF
GCSF
Figure 1. Cumulative incidence of relapse in patients receiving BM or PB-auto-SCT for AML with and without G-CSF.
Table 2. Multivariate analysis of outcomes
BM-auto-SCT PB-auto-SCT
P-value HR 95% CI P-value HR 95% CI
RI
G-CSF use 0.49 0.89 0.651.23 0.29 0.92 0.791.07
Age>median (48 years) 0.01 1.51 1.12.06 0.007 1.23 1.061.43
Year>median (2001) 0.21 1.22 0.891.68 0.58 1.05 0.891.22
Induction courses>1 0.0006 1.97 1.342.89 0.0004 1.44 1.181.76
Favorable karyotype 0.7 0.88 0.451.71 o0.0001 0.46 0.330.65
Unfavorable karyotype 0.88 1.06 0.52.24 0.1 1.26 0.951.67
TBI 0.57 0.91 0.671.25 0.97 1 0.811.24
Abbreviations: CI =condence interval; HR=hazard ratio; RI =relapse incidence. Statistically signicant values are indicated in bold.
Impact of G-CSF use after auto-SCT on AML relapse
T Czerw et al
952
Bone Marrow Transplantation (2014) 950 954 2014 Macmillan Publishers Limited
centers (per protocol or due to anticipated poor engraftment) was
impossible. Important changes in diagnostic tools, which have
been incorporated in the clinic over a 17-year period of accrual,
especially the possibility of detecting minimal residual disease
before auto-SCT, represent the other factors that could have
inuenced the results. For this reason we performed additional
sub-cohort analyses dividing study populations according to the
median year of transplantation (1996 for BM-auto-SCT and 2001
for PB-auto-SCT group). Once again, we did not nd any adverse
effect of G-CSF use on RI (data not shown).
Thus far, in the only publication related to the use of G-CSF after
auto-SCT in AML, Majhail et al. included in the analysis patients
who had survived in continuous CR for at least 2 years after
transplantation.
13
In this retrospective study, the use of growth
factors to hasten neutrophil recovery was found to be the only
factor associated with an increased risk of late relapses (HR 3.64,
P =0.013). However, as most AML relapses occur during the rst
2 years after auto-SCT, this nding might have resulted from a
selection bias, which was also stated by the authors.
Our data correspond to previous observations on the use of
G-CSF to support initial chemotherapy of AML.
1420
G-CSF
prophylaxis during and following induction and consolidation
was not shown to adversely affect the CR rate, the RI or the LFS in
meta-analysis of 19 randomized trials.
21
On the other hand,
however, there are also recent data indicating that under
particular circumstances G-CSF may stimulate leukemogenesis in
AML. AML-BFM 98 study (patients younger than 18 years) reported
a trend toward increased RI in the standard-risk patients assigned
to receive prophylactic G-CSF after initial therapy.
22
Furthermore,
overexpression of differentiation-defective G-CSF receptor isoform
IV on blast clones was found to be a signicant and pivotal risk
factor for relapse among patients receiving G-CSF (5-year RI 50 vs
14% in patients with low-level expression, P =0.04). In patients not
receiving G-CSF, the level of expression of this molecule had no
inuence on RI.
23
It was previously shown that AML cell lines and
AML patient samples express increased relative amounts of the
class IV isoform G-CSF receptor.
24,25
These data suggest that
despite the lack of evidence for an increased risk of relapse
associated with G-CSF administration in general, there may be
particular AML patient subsets susceptible to this effect. In our
study, the number of cases with standard-risk AML was relatively
small, so we were able to analyze it separately only in the PB-auto-
SCT group. However, once again, the potential adverse role of
G-CSF use was not observed (data not shown). It may be
hypothesized that the potential negative effect of G-CSF in de
novo AML may not necessarily be relevant among patients
referred for auto-SCT, who are in rst CR with a low tumor burden.
As expected, in the current analysis the use of G-CSF
signicantly shortened the duration of the neutropenic phase
after transplantation both in BM- and PB-auto-SCT groups (by
median 3 and 2 days, respectively). The differences, however, were
relatively small and clinically unimportant, as the incidences of
graft failure and NRM were comparable. These ndings are
consistent with previously published data in lymphoid malig-
nancies and solid tumors.
2628
In the meta-analysis of randomized
controlled trials, the prophylactic use of growth factors after auto-
SCT was associated with faster neutrophil recovery, reduction of
days of parenteral antibiotics and hospital stay.
29
These benets,
however, did not translate into a reduction of NRM.
In conclusion, our results indicate that in the general population
of patients with AML, the use of G-CSF after auto-SCT is not
associated with an increased risk of relapse and may be
considered safe, irrespective of the source of stem cells used for
transplantation. However, on the basis of the recent ndings,
individual susceptibility related to the biology of leukemic blasts
cannot be excluded. Future investigations should focus on
particular genetic subtypes and optimally take into account the
expression of G-CSF receptors and their isoforms.
CONFLICT OF INTEREST
The authors declare no conict of interest.
REFERENCES
1 Smith TJ, Khatcheressian J, Lyman GH, Ozer H, Armitage JO, Balducci L et al.
2006 update of recommendations for the use of white blood cell growth
factors: an evidence-based clinical practice guideline. J Clin Oncol 2006; 24:
31873205.
2 Breems DA, Lwenberg B. Acute myeloid leukemia and the position of auto-
logous stem cell transplantation. Semin Hematol 2007; 44: 259266.
3 Seshadri T, Keating A. Is there a role for autotransplants in AML in rst remission?
Biol Blood Marrow Transplant 2009; 15: 1720.
4 Passweg JR, Baldomero H, Gratwohl A, Bregni M, Cesaro S, Dreger P et al. The
EBMT activity survey: 1990-2010. Bone Marrow Transplant 2012; 47: 906923.
5 Brenner MK, Rill DR, Moen RC, Krance RA, Mirro J Jr, Anderson WF et al. Gene-
marking to trace origin of relapse after autologous bone-marrow transplantation.
Lancet 1993; 341: 8586.
6 Feller N, Schuurhuis GJ, van der Pol MA, Westra G, Weijers GW, van Stijn A et al.
High percentage of CD34-positive cells in autologous AML peripheral blood stem
cell products reects inadequate in vivo purging and low chemotherapeutic
toxicity in a subgroup of patients with poor clinical outcome. Leukemia 2003; 17:
6875.
7 Vellenga E, Young DC, Wagner K, Wiper D, Ostapovicz D, Grifn JD. The effects of
GM-CSF and G-CSF in promoting growth of clonogenic cells in acute myeloblastic
leukemia. Blood 1987; 69: 17711776.
8 Lwenberg B, Touw IP. Hematopoietic growth factors and their receptors in acute
leukemia. Blood 1993; 81: 281292.
9 Gooley TA, Leisenring W, Crowley JA, Storer BE. Estimation of failure probabilities
in the presence of competing risks: new representations of old estimators. Stat
Med 1999; 18: 665706.
10 Fine JP, Gray RJ. A proportional hazards model for subdistribution of a
competing risk. J Am Stat Assoc 1999; 94: 496509.
11 Gorin NC, Labopin M, Blaise D, Reiffers J, Meloni G, Michallet M et al. Higher
incidence of relapse with peripheral blood rather than marrow as a source of
stem cells in adults with acute myelocytic leukemia autografted during the rst
remission. J Clin Oncol 2009; 27: 39873993.
12 Graf M, Hecht K, Reif S, Pelka-Fleischer R, Pster K, Schmetzer H. Expression and
prognostic value of hemopoietic cytokine receptors in acute myeloid leukemia
(AML): implications for future therapeutical strategies. Eur J Haematol 2004; 72:
89106.
13 Majhail NS, Bajorunaite R, Lazarus HM, Wang Z, Klein JP, Zhang MJ et al. High
probability of long-term survival in 2-year survivors of autologous hematopoietic
cell transplantation for AML in rst or second CR. Bone Marrow Transplant 2011;
46: 385392.
14 Heil G, Hoelzer D, Sanz MA, Lechner K, Liu Yin JA, Papa G et al. A randomized,
double-blind, placebo-controlled, phase III study of lgrastim in remission
induction and consolidation therapy for adults with de novo acute myeloid leu-
kemia. The International Acute Myeloid Leukemia Study Group. Blood 1997; 90:
47104718.
15 Godwin JE, Kopecky KJ, Head DR, Willman CL, Leith CP, Hynes HE et al. A double-
blind placebo-controlled trial of granulocyte colony-stimulating factor in elderly
patients with previously untreated acute myeloid leukemia: a Southwest oncol-
ogy group study (9031). Blood 1998; 91: 36073615.
16 Usuki K, Urabe A, Masaoka T, Ohno R, Mizoguchi H, Hamajima N et al.
Efcacy of granulocyte colony-stimulating factor in the treatment of acute mye-
logenous leukaemia: a multicentre randomized study. Br J Haematol 2002; 116:
103112.
17 Alonzo TA, Kobrinsky NL, Aledo A, Lange BJ, Buxton AB, Woods WG. Impact of
granulocyte colony-stimulating factor use during induction for acute myelogen-
ous leukemia in children: a report from the Childrens Cancer Group. J Pediatr
Hematol Oncol 2002; 24: 627635.
18 Kutlay S, Beksac M, Dalva K, Ilhan O, Koc H, Akan H et al. The detection of ow
cytometric G-CSF receptor expression and its effect on therapy in acute myeloid
leukemia. Leuk Lymphoma 2003; 44: 791795.
19 Wheatley K, Goldstone AH, Littlewood T, Hunter A, Burnett AK. Randomized
placebo-controlled trial of granulocyte colony stimulating factor (G-CSF) as sup-
portive care after induction chemotherapy in adult patients with acute myeloid
leukaemia: a study of the United Kingdom Medical Research Council Adult Leu-
kaemia Working Party. Br J Haematol 2009; 146: 5463.
20 Beksac M, Ali R, Ozcelik T, Ozcan M, Ozcebe O, Bayik M et al. Short and long term
effects of granulocyte colony-stimulating factor during induction therapy in acute
myeloid leukemia patients younger than 65: results of a randomized multicenter
phase III trial. Leuk Res 2011; 35: 340345.
Impact of G-CSF use after auto-SCT on AML relapse
T Czerw et al
953
2014 Macmillan Publishers Limited Bone Marrow Transplantation (2014) 950 954
21 Gurion R, Belnik-Plitman Y, Gafter-Gvili A, Paul M, Vidal L, Ben-Bassat I et al.
Colony-stimulating factors for prevention and treatment of infectious complica-
tions in patients with acute myelogenous leukemia. Cochrane Database Syst Rev
2011; 7: CD008238.
22 Creutzig U, Zimmermann M, Lehrnbecher T, Graf N, Hermann J, Niemeyer CM
et al. Less toxicity by optimizing chemotherapy, but not by addition of granulo-
cyte colony-stimulating factor in children and adolescents with acute myeloid
leukemia: results of AML-BFM 98. J Clin Oncol 2006; 24: 44994506.
23 Ehlers S, Herbst C, Zimmermann M, Scharn N, Germeshausen M, von Neuhoff N
et al. Granulocyte colony-stimulating factor (G-CSF) treatment of childhood acute
myeloid leukemias that overexpress the differentiation-defective G-CSF receptor
isoform IV is associated with a higher incidence of relapse. J Clin Oncol 2010; 28:
25912597.
24 White SM, Ball ED, Ehmann WC, Rao AS, Tweardy DJ. Increased expression of the
differentiation-defective granulocyte colony-stimulating factor receptor mRNA
isoform in acute myelogenous leukemia. Leukemia 1998; 12: 899906.
25 Beekman R, Touw IP. G-CSF and its receptor in myeloid malignancy. Blood 2010;
115: 51315136.
26 Stahel RA, Jost LM, Cerny T, Pichert G, Honegger H, Tobler A et al. Randomized
study of recombinant human granulocyte colony-stimulating factor after high-
dose chemotherapy and autologous bone marrow transplantation for high-risk
lymphoid malignancies. J Clin Oncol 1994; 12: 19311938.
27 Linch DC, Milligan DW, Wineld DA, Kelsey SM, Johnson SA, Littlewood TJ
et al. G-CSF after peripheral blood stem cell transplantation in lymphoma
patients signicantly accelerated neutrophil recovery and shortened
time in hospital: results of a randomized BNLI trial. Br J Haematol 1997; 99:
933938.
28 Schmitz N, Ljungman P, Cordonnier C, Kempf C, Linkesch W, Alegre A et al.
Lenograstim after autologous peripheral blood progenitor cell transplantation:
results of a double-blind, randomized trial. Bone Marrow Transplant 2004; 34:
955962.
29 Dekker A, Bulley S, Beyene J, Dupuis LL, Doyle JJ, Sung L. Meta-analysis
of randomized controlled trials of prophylactic granulocyte colony-stimulating
factor and granulocyte-macrophage colony-stimulating factor after auto-
logous and allogeneic stem cell transplantation. J Clin Oncol 2006; 24:
52075215.
Impact of G-CSF use after auto-SCT on AML relapse
T Czerw et al
954
Bone Marrow Transplantation (2014) 950 954 2014 Macmillan Publishers Limited
You might also like
- S GCSF and Alzheimer's Disease 2012Document8 pagesS GCSF and Alzheimer's Disease 2012amandbhaskarNo ratings yet
- Embo 1986Document7 pagesEmbo 1986amandbhaskarNo ratings yet
- J. Biol. Chem.-1997-Morley-17887-93Document8 pagesJ. Biol. Chem.-1997-Morley-17887-93amandbhaskarNo ratings yet
- Transforming Bacteria RowDocument6 pagesTransforming Bacteria Rowme_dayakarNo ratings yet
- Arabidiopsis Thaliana CBF 1 Encodes An AP2Document6 pagesArabidiopsis Thaliana CBF 1 Encodes An AP2amandbhaskarNo ratings yet
- Session III Ichq6b SpecificationsDocument84 pagesSession III Ichq6b Specificationsamandbhaskar100% (1)
- The Role of Granulocyte Colony Stimulating Factor Receptor Signalling in Neytrophil DevDocument136 pagesThe Role of Granulocyte Colony Stimulating Factor Receptor Signalling in Neytrophil DevamandbhaskarNo ratings yet
- GCSF Cloning and CharacterizationDocument12 pagesGCSF Cloning and CharacterizationsanpukoNo ratings yet
- Estimation of GCSF Effectivness in NeutropeniaDocument171 pagesEstimation of GCSF Effectivness in NeutropeniaamandbhaskarNo ratings yet
- Guidlines For The Use of FilgrastimDocument7 pagesGuidlines For The Use of FilgrastimamandbhaskarNo ratings yet
- Genomic DNA isolation from human bloodDocument2 pagesGenomic DNA isolation from human bloodamandbhaskarNo ratings yet
- Antioxidant Potential of Zingiber Nimmonii (J. Graham) DalzellDocument3 pagesAntioxidant Potential of Zingiber Nimmonii (J. Graham) DalzellamandbhaskarNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5783)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
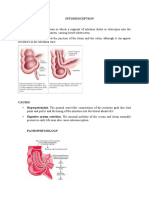
- INTUSSUSCEPTIONDocument3 pagesINTUSSUSCEPTIONS GNo ratings yet
- Health Promotion Methods and ApproachesDocument18 pagesHealth Promotion Methods and ApproachesDrGagandeep Singh100% (1)
- Absence of A Menstrual PeriodDocument2 pagesAbsence of A Menstrual PeriodDragan PetrovicNo ratings yet
- Being Afraid: Everyday WorriesDocument10 pagesBeing Afraid: Everyday Worriesdina171279No ratings yet
- MSQ's Pediatric SurgeryDocument28 pagesMSQ's Pediatric Surgeryrohit0% (1)
- Treatment Planning Heterogeneity Vs Homogeneity Lung ProjectDocument13 pagesTreatment Planning Heterogeneity Vs Homogeneity Lung Projectapi-299138743No ratings yet
- AmenorrheaDocument41 pagesAmenorrheaDewi Felayati Gusni100% (2)
- Pancha Karma (Sree Subramania Ayurvedic Nursing Home)Document15 pagesPancha Karma (Sree Subramania Ayurvedic Nursing Home)Sanand Ratnam Thekkayil100% (1)
- Stefan Et Al-2019-Journal of Clinical PsychologyDocument16 pagesStefan Et Al-2019-Journal of Clinical PsychologyYuni Indriani RombeNo ratings yet
- Iontophoresis Definition and PrinciplesDocument4 pagesIontophoresis Definition and PrinciplesSiva Shanmugam100% (1)
- DisolusiDocument47 pagesDisolusiNoonaNuzha Lestary NuzhaAyuNo ratings yet
- Sop Icu H & FW 12725 28.04.2018Document20 pagesSop Icu H & FW 12725 28.04.2018shah007zaadNo ratings yet
- Gabapantin and PregabalinDocument23 pagesGabapantin and PregabalinayushiNo ratings yet
- !!!-MBS Skin Item Numbers Nov 2016Document3 pages!!!-MBS Skin Item Numbers Nov 2016abu ubaidahNo ratings yet
- Asian Music Research - J.C GarciaDocument5 pagesAsian Music Research - J.C GarciaJomel GarciaNo ratings yet
- Guideline PERKENI 2015Document34 pagesGuideline PERKENI 2015Iin Citra Liana HasibuanNo ratings yet
- Asthma: Setya Puspa Dewi AprilyaniDocument19 pagesAsthma: Setya Puspa Dewi Aprilyaninadia kurnia100% (1)
- Endocrine MCQDocument11 pagesEndocrine MCQiman14100% (3)
- C Perfringens Cladosporium SPP - PDFDocument21 pagesC Perfringens Cladosporium SPP - PDFEman QasmNo ratings yet
- 290 297Document12 pages290 297YASMINDPNo ratings yet
- Ezzat PaperDocument15 pagesEzzat PaperMohamedAbdelmonaemNo ratings yet
- Osmotic DiureticsDocument30 pagesOsmotic Diureticsrhimineecat71100% (1)
- Complete Urinalysis: A. Physical Characteristics of UrineDocument8 pagesComplete Urinalysis: A. Physical Characteristics of UrineKryza Dale Bunado BaticanNo ratings yet
- Atrial FibrillationDocument14 pagesAtrial FibrillationNur Atiqah ZainalNo ratings yet
- Heaven & Earth Spa Treatments Under 40Document2 pagesHeaven & Earth Spa Treatments Under 40Janhavi SoniNo ratings yet
- 09 SterilizationDocument34 pages09 Sterilizationitung2350% (2)
- Balanced Diet: Includes Foods From All Food Groups During The DayDocument19 pagesBalanced Diet: Includes Foods From All Food Groups During The DayMayuri VohraNo ratings yet
- Fluid and Electrolyte BalanceDocument295 pagesFluid and Electrolyte BalanceAnuchithra RadhakrishnanNo ratings yet
- SEMINARDocument19 pagesSEMINARTaiwoNo ratings yet
- Pediatrics MnemonicsDocument13 pagesPediatrics MnemonicsMuhammad Luqman Nul HakimNo ratings yet