Professional Documents
Culture Documents
Access To The Extrapleural Space at The Time of Surgery For Continuous Paravertebral Block After Flank Incision - Description of The Technique and Case Series PDF
Uploaded by
Elizabeth Baldeon0 ratings0% found this document useful (0 votes)
43 views4 pagesAn alternative to neuraxial analgesia widely used in thoracic surgery is the surgeon-placed PVB. Patients received an average of 5. Mg of subcutaneous equivalent hydromorphone. No complications because of the PVB were found.
Original Description:
Original Title
Access to the Extrapleural Space at the Time of Surgery for Continuous Paravertebral Block After Flank Incision_ Description of the Technique and Case Series.pdf
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentAn alternative to neuraxial analgesia widely used in thoracic surgery is the surgeon-placed PVB. Patients received an average of 5. Mg of subcutaneous equivalent hydromorphone. No complications because of the PVB were found.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
43 views4 pagesAccess To The Extrapleural Space at The Time of Surgery For Continuous Paravertebral Block After Flank Incision - Description of The Technique and Case Series PDF
Uploaded by
Elizabeth BaldeonAn alternative to neuraxial analgesia widely used in thoracic surgery is the surgeon-placed PVB. Patients received an average of 5. Mg of subcutaneous equivalent hydromorphone. No complications because of the PVB were found.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 4
Surgical Techniques in Urology
Access to the Extrapleural Space at the Time
of Surgery for Continuous Paravertebral Block
After Flank Incision: Description of the
Technique and Case Series
Gavin M. Langille, Gordon O. Launcelott, and Ricardo A. Rendon
OBJECTIVE To test our hypothesis that surgeon-placed paravertebral block (PVB) placement during open
renal surgery is effective, feasible, and safe. Neuraxial analgesia represents the current standard of
care for perioperative anesthesia for open renal surgery. However, potential catastrophic
complications such as neuraxial bleeding and infection may occur. An alternative to neuraxial
analgesia widely used in thoracic surgery is the surgeon-placed PVB.
TECHNICAL
CONSIDERATIONS
The surgeon-placed catheter is directed in the paravertebral space through the ank incision at
the time of surgery. The postoperative catheter management was directed by anesthesiologists. All
patients undergoing open renal surgery by a single urologist were provided a PVB for this series.
Twenty-nine consecutive patients undergoing open renal surgery were given PVBs. Patients
received an average of 5.1 mg of subcutaneous equivalent hydromorphone in the 48-hour
postoperative period. No complications because of the PVB were found.
CONCLUSION PVB represents a safe and effective surgeon-placed alternative to neuraxial analgesia for open
renal operative procedures. UROLOGY 81: 675e678, 2013. 2013 Elsevier Inc.
N
euraxial analgesia represents the gold standard
in pain control for major abdominal and ank
incisions used for open urologic procedures. It
can decrease the stress response and improve postoperative
respiratory function by reducing perioperative opioid
requirements.
1
This works to minimize the systemic side
effects of opioids suchas nausea, pruritus, urinary retention,
and ileus. Although rare, potential complications include
epidural hematoma or abscess, which can lead to perma-
nent neurological decits. Epidural abscess has been
documented at widely variable rates, some of the higher
incidences reported at 1:800 to 1:1930.
2,3
In a large series,
the rate of epidural hematoma was 1:4105.
4
Neuraxial
analgesia is contraindicated in patients requiring certain
perioperative anticoagulation or antiplatelet regimens,
which has furthered interest in alternative techniques.
Anesthesiologist-administeredparavertebral block(PVB)
has been described in the literature as a technique for post-
operative analgesia for renal surgery.
5
This technique does
not carry the potential risks of neuraxial bleeding, but
maintains benets such as decreased opioid use. Additional
benets over neuraxial analgesia include preservation of
forced vital capacity, minimizing respiratory depression, and
limiting hypotension.
6
For thoracotomy incisions, PVB has
been proposed to represent the new gold standard over
neuraxial analgesia.
7
Placement of the paravertebral block
into the extrapleural space has traditionally been performed
by an anesthesiologist using a percutaneous ultrasound-
guided technique. This approach requires operator experi-
ence and skill; it has had varied degrees of success and is less
reliable and prone to more side effects than catheters placed
under direct vision.
8
The use of surgeon-placed PVBs in the thoracic literature
is gaining in popularity.
9,10
Surgeon-placed PVB during
posterolateral thoracotomy has been shown to decrease
postoperative opioid requirements compared to epidural.
11
It also avoids possible neuraxial placement, which is pos-
sible with an anesthesiologist-applied block.
9
We hypoth-
esize that a surgeon-placed PVB under direct vision via
a ank approach during renal surgery is a feasible procedure
that can provide effective perioperative analgesia without
the risks associated with neuraxial analgesia.
MATERIALS AND METHODS
Neuroanatomy
A discussion on the relevant anatomy is warranted. As the
thoracic spinal nerve root leaves the intervertebral foramen, it
immediately gives off a small posterior branch (posterior primary
ramus). The main nerve crosses the paravertebral space and into
Financial Disclosure: The authors declare that they have no relevant nancial interests.
From the Department of Urology, Dalhousie University, Halifax, Nova Scotia,
Canada; and Department of Anesthesia, Dalhousie University, Halifax, Nova Scotia,
Canada
Reprint requests: Ricardo A. Rendon, M.D., F.R.C.S.C., Department of Urology,
Dalhousie University, 5015 5th Floor, Victoria General Hospital, 1276 South Park
Street, Halifax, Nova Scotia B3H 2Y9, Canada. E-mail: rrendon@dal.ca
Submitted: July 5, 2012, accepted (with revisions): November 27, 2012
2013 Elsevier Inc. 0090-4295/13/$36.00 675
All Rights Reserved http://dx.doi.org/10.1016/j.urology.2012.11.043
the intercostal space in the plane between the pleura anteriorly
and the posterior intercostal membrane. Beyond the angle of the
rib, the nerve lies inferior to the intercostal vessels sandwiched
between the intercostalis intimus anteriorly and the internal
intercostal muscle, continuing in this plane until it reaches the
anterior axillary line. At this point, the intercostalis intimus
terminates and the nerve once again comes to lie directly on the
pleura. In the ank, as the 10th thoracic nerve passes beyond
the costal cartilage, it will come to lie on the pleura, the dia-
phragm, and the transversus abdominis muscle as it makes its
way toward the anterior abdominal wall (Fig. 1). It is here that
the extrapleural space can be accessed at the time of surgery and
a catheter placed in the paravertebral gutter under direct vision
for local anesthetic inltration.
It is this anatomic relationship of the thoracic spinal nerve
roots and intercostal nerves sandwiched between the pleura and
the chest wall within the thoracic cavity that provides an
opportunity for local anesthetic to spread and block several
spinal nerve roots. Furthermore, if this space can be accessed
easily at the time of surgery, a catheter can be placed under
direct vision allowing for continuous infusion of local anesthetic
and prolonged unilateral peripheral nerve block.
Technique
Toward the end of the surgical case, after the completion of the
urologic intervention, attention is turned to PVB placement.
The anterolateral aspect of the diaphragm is identied where it
crosses the 10th and 11th ribs (Fig. 2). The parietal pleura is
subsequently identied beneath the diaphragm. The parietal
pleura are dissected bluntly from the 10th rib. This plane is
widened with blunt dissection. The extrapleural plane is devel-
oped superoposteriorly to the necks of the 8th through 12th ribs.
Exposure is aided with the use of a narrow Ribbon retractor and
adequate illumination. Under direct vision, a Tuohy (17 gauge,
3.5 inches; Becton, Dickinson and Co., Franklin Lakes, NJ)
epidural needle is passed percutaneously over the 11th rib
approximately 10 cm lateral to the spine. Care is taken to protect
the pleura and the lung. An epidural catheter is passed through
the Tuohy needle under direct vision and is directed into the
paravertebral space (Fig. 3). The Tuohy needle is removed and
the epidural catheter is xed externally to the skin with adhesive
tape, as per the technique used in neuraxial analgesia. The pleura
and lung are allowed to fall back into place. What remains is
a standard extended posterolateral retroperitoneal incision
closure in layers. The diaphragm is reapproximated to the deeper
fascial layer with a continuous suture.
Twenty-nine consecutive patients who had PVB during
open partial or radical nephrectomy by a single surgeon were
reviewed. Research ethics board approval for this study was
obtained. All incisions were made superior to the 11th rib.
A 20 mL bolus of 0.5% bupivacaine was administered to all
patients via the extrapleural catheter intraoperatively. A
maintenance infusion of 0.375% ropivicaine at 12 mL per hour
was provided. Anesthesiologists maintained control over the
management of the paravertebral catheters. All patients
received acetaminophen 975 mg orally every 6 hours, as per our
care map to supplement the PVB postoperatively. Additional
opioid administration was at the discretion of the anesthesiol-
ogist directed Acute Pain Service while the PVB was in place.
Opioid requirements were converted to parenteral equivalent
hydromorphone based on accepted ratios.
12,13
The parenteral to
oral equivalent ratio of morphine and hydromorphone is 1:3 and
1:5, respectively. The conversion ratio of oral morphine to oral
hydromorphone is 1.5:10. Paravertebral catheters were removed
once the anesthesiology team felt the analgesia to be adequate,
and all were removed by 72 hours postoperatively.
RESULTS
Twenty-nine consecutive patients who had open partial
or radical nephrectomy by a single surgeon were reviewed.
The cases were dated from November 2008 to July 2011.
All patients had PVB placement performed intra-
operatively. All incisions were made superior to the 11th
rib. Twenty-ve partial and 4 radical nephrectomies were
included in this study. In all cases, the surgical dissection
of the extrapleural plane and intraoperative paravertebral
catheter placement were successful. The average amount
of intravenous hydromorphone used in the postanesthetic
care unit was 1.24 mg. Over half of these patients
received 1 mg or less of hydromorphone, with 6 of these
patients receiving none. Parenteral equivalent hydro-
morphone used in the initial 48 hours on the surgical
oor was 3.87 mg. For the 6 hours before PVB removal,
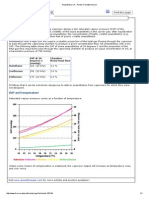
Figure 1. A window has been cut through the external and
internal oblique muscles showing the 9th and 10th thoracic
nerves, lying successively on the pleura, diaphragm, and
transverses abdominis. This gure was reproduced with
permission: initially published as Figure 43 in Local Anal-
gesia Abdominal Surgery MacIntosh and Bryce-Smith,
Copyright: Elsevier, E & S Livingstone Ltd, Edinburgh and
London (1962).
676 UROLOGY 81 (3), 2013
systemic narcotic administration was 38% less than the
6 hours after PVB removal. The average length of stay in
the hospital was 4.4 days. No complications were found
to be associated with the use of this technique.
COMMENT
We present this technique as a feasible and safe surgeon-
applied procedure that provides excellent postoperative
analgesia to patients undergoing lateral lower thoracotomy.
PVB provides similar benets of neuraxial analgesia
including minimal systemic opioid use with excellent
pain control while avoiding complications from neuraxial
analgesia such as epidural abscess and hematoma. An-
other advantage is the ability to place a PVB under direct
vision, a surgeon-directed maneuver performed during
the operation. This facilitates the short learning curve
associated with this procedure.
PVB placement is safe in our experience, with no per-
ioperative complications related to its placement or use.
Potential complications of PVB include bleeding most
commonly in the form of a limited hematoma, which
is reported at 2.4% for anesthesiologist-placed blocks.
6
Pneumothorax and pleural puncture rates were reported
as 0.5% and 1%, respectively, for anesthesiologist-placed
PVB. Anesthetic toxicity is also a possibility.
14
Although
infection is possible, the risk of infection in the epidural
space is avoided by using the surgeon-placed approach.
Placement of the paravertebral catheter in the extrap-
leural space is a relatively straightforward procedure that
we feel has a much shorter learning curve than the
ultrasound-guided anesthesiologist-directed technique.
The ease of use is facilitated by the ability to place the
catheter under direct vision during the procedure. In the
current series, paravertebral catheters were successfully
placed in the paravertebral space. The development of the
extrapleural space and catheter insertion adds only several
minutes to the overall procedure.
Patients in this series had a variety of requirements for
systemic postoperative opioids, many with near negligible
amounts considering the usual pain derived from a ank
incision. A variety of factors including body habitus and
length of incision could inuence opioid requirements.
Twenty-six of the 29 patients received just 2.0 mg or less
of intravenous hydromorphone in the postoperative
recovery room. Analgesic requirements on the surgical
oor showed that almost half (48%) of the patients in this
series had 4 mg or less of equivalent parenteral hydro-
morphone in the 48-hour postoperative period. For
this same period, 2 patients required 10 mg or more of
equivalent parenteral hydromorphone. The total anal-
gesic requirements for these 2 patients was still slightly
less than the previously reported amount for open
nephrectomy without neuraxial analgesia, with our
median requirement just half of this value.
15
Compared to
previous data on neuraxial and PVB for posterolateral
thoracotomy, the 48-hour total opioid requirements in
our patients was 29% and 12% less, respectively.
11
Compared to another series of surgeon-placed PVB for
thoracotomy, our opioid requirements were nearly iden-
tical.
16
Total narcotic requirements were similar
compared to open nephrectomy in another series.
17
The
possibility exists that suboptimal placement or displace-
ment of the catheter could lead to decreased efcacy,
although we feel that the straightforward placement of
the PVB minimizes this risk. Further investigations into
factors that inuence the effectiveness of PVB include
correlating individual characteristics such as age, weight,
and body mass index, etc., in a larger data set.
The limitations of this study include its retrospective,
nonblinded nature with no control group. Although this
review serves as a proof of principle for the use of
surgeon-placed PVB in the urologic literature, further
prospective and randomized trials would help solidify
Figure 2. Dissection of the diaphragm to develop the plane
leading to the extrapleural space during ank surgery. The
highlighted anatomic relations demonstrating a patient lying
in the left lateral decubitus position are maintained for
Figure 3. The bolstering suture can be visualized on the
cranial aspect of the right kidney. Rt, right.
Figure 3. The epidural catheter is passed through the Tuohy
needle below the 10th rib and fed into the paravertebral
space. Rt, right.
UROLOGY 81 (3), 2013 677
the use of PVB by urologists for renal surgery. At our
institution, the PVB is now used for all open renal and
adrenal surgeries. Because of the excellent results
observed, this technique has been expanded to other
procedures using lower lateral thoracotomies (such as
abdominal aortic aneurysm repair).
CONCLUSION
The use of surgeon-placed PVB intraoperatively is feasible
and provides safe and effective perioperative analgesia for
open renal and adrenal surgery using the ank approach
based on these initial results. PVB placement has become
the mainstay for anesthetic delivery for all open renal and
adrenal surgery at our institution.
Acknowledgments. The authors thank Sebastian Launcelott
and Lynn Langille for their contributions to this project.
References
1. Hahnenkamp K, Herroeder S, Hollmann MW. Regional anaes-
thesia, local anaesthetics and the surgical stress response. Best Pract
Res Clin Anaesthesiol. 2004;18:509-527.
2. Phillips JM, Stedeford JC, Hartsilver E, et al. Epidural abscess
complicating insertion of epidural catheters. Br J Anaesth. 2002;89:
778-782.
3. Wang LP, Hauerberg J, Schmidt JF. Incidence of spinal epidural
abscess after epidural analgesia: a national 1-year survey. Anesthesi-
ology. 1999;91:1928-1936.
4. Cameron CM, Scott DA, McDonald WM, et al. A review
of neuraxial epidural morbidity: experience of more than 8,000
cases at a single teaching hospital. Anesthesiology. 2007;106:
997-1002.
5. Lonnqvist PA, Olsson GL. Paravertebral vs epidural block in chil-
dren. Effects on postoperative morphine requirement after renal
surgery. Acta Anaesthesiol Scand. 1994;38:346-349.
6. Chelly JE. Paravertebral blocks. Anesthesiol Clin. 2012;30:75-90.
7. Rawal N. Epidural technique for postoperative pain: gold standard
no more? Reg Anesth Pain Med. 2012;37:310-317.
8. Boezaart AP, Lucas SD, Elliott CE. Paravertebral block: cervical,
thoracic, lumbar, and sacral. Curr Opin Anaesthesiol. 2009;22:
637-643.
9. Elsayed H, McKevith J, McShane J, et al. Thoracic epidural or
paravertebral catheter for analgesia after lung resection: is the
outcome different? J Cardiothorac Vasc Anesth. 2012;26:78-82.
10. Marret E, Bazelly B, Taylor G, et al. Paravertebral block with
ropivacaine 0.5% versus systemic analgesia for pain relief after
thoracotomy. Ann Thorac Surg. 2005;79:2109-2113.
11. Richardson J, Sabanathan S, Jones J, et al. A prospective,
randomized comparison of preoperative and continuous balanced
epidural or paravertebral bupivacaine on post-thoracotomy pain,
pulmonary function and stress responses. Br J Anaesth. 1999;83:
387-392.
12. Gordon DB, Stevenson KK, Grife J, et al. Opioid equianalgesic
calculations. J Palliat Med. 1999;2:209-218.
13. Gammaitoni AR, Fine P, Alvarez N, et al. Clinical application of
opioid equianalgesic data. Clin J Pain. 2003;19:286-297.
14. Kotze A, Scally A, Howell S. Efcacy and safety of different tech-
niques of paravertebral block for analgesia after thoracotomy:
a systematic review and metaregression. Br J Anaesth. 2009;103:
626-636.
15. Nicholson ML, Kaushik M, Lewis GR, et al. Randomized clinical
trial of laparoscopic versus open donor nephrectomy. Br J Surg.
2010;97:21-28.
16. Garutti I, Gonzalez-Aragoneses F, Biencinto MT, et al. Thoracic
paravertebral block after thoracotomy: comparison of three different
approaches. Eur J Cardiothorac Surg. 2009;35:829-832.
17. McDougall E, Clayman RV, Elashry OM. Laparoscopic radical
nephrectomy for renal tumor: the Washington University experi-
ence. J Urol. 1996;155:1180-1185.
Video Clips cited in this article can be found
on the internet at: http://www.goldjournal.net
678 UROLOGY 81 (3), 2013
You might also like
- Effectiveness of Continuous Wound Infusion of Ropivacaina by On-Q Pain Relief PDFDocument7 pagesEffectiveness of Continuous Wound Infusion of Ropivacaina by On-Q Pain Relief PDFElizabeth BaldeonNo ratings yet
- Anaesthesia UK - Printer Friendly Version3Document1 pageAnaesthesia UK - Printer Friendly Version3Elizabeth BaldeonNo ratings yet
- Anaesthesia UK - Printer Friendly Version6Document4 pagesAnaesthesia UK - Printer Friendly Version6Elizabeth BaldeonNo ratings yet
- Fetal Health Surveillance - Antepartum and Intrapartum Consensus GuidelineDocument60 pagesFetal Health Surveillance - Antepartum and Intrapartum Consensus Guidelinebel4ronaldoeNo ratings yet
- Fetal Health Surveillance - Antepartum and Intrapartum Consensus GuidelineDocument60 pagesFetal Health Surveillance - Antepartum and Intrapartum Consensus Guidelinebel4ronaldoeNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (120)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Medication ErrorsDocument2 pagesMedication Errors88AKKNo ratings yet
- Ham D PDFDocument1 pageHam D PDFRabiatul AdawiyahNo ratings yet
- Zoll M Series Defibrillator Manual PDFDocument111 pagesZoll M Series Defibrillator Manual PDFAhmad TanveerNo ratings yet
- MedStart UMAT Sample and Practice QuestionsDocument55 pagesMedStart UMAT Sample and Practice QuestionsLyn JiangNo ratings yet
- Normal Values HR RR BPDocument28 pagesNormal Values HR RR BPKthrine CrronNo ratings yet
- Changes in Brain Function (Quantitative EEG Cordance) During Placebo Lead-In and Treatment Outcomes in Clinical Trials For Major DepressionDocument7 pagesChanges in Brain Function (Quantitative EEG Cordance) During Placebo Lead-In and Treatment Outcomes in Clinical Trials For Major DepressiondebdotnetNo ratings yet
- Generic Name Brand Name Classification/ Indication Mechanism of Action Adverse Effects Nursing ResponsibilitiesDocument3 pagesGeneric Name Brand Name Classification/ Indication Mechanism of Action Adverse Effects Nursing ResponsibilitiesRia Nicole100% (1)
- Cms Sop FinalDocument65 pagesCms Sop FinalJennifer LopataNo ratings yet
- Concept of Unitive and Preventive HealthDocument5 pagesConcept of Unitive and Preventive HealthalorNo ratings yet
- Kuliah 8. Anestesi - Syok Dan Tata LaksananyaDocument63 pagesKuliah 8. Anestesi - Syok Dan Tata LaksananyaDesi Suryani DewiNo ratings yet
- ParacetamolDocument24 pagesParacetamolFriné MirandaNo ratings yet
- Orbit Key ArticlesDocument37 pagesOrbit Key ArticlesArjun MUNo ratings yet
- Anxiety Disorders in ChildrenDocument3 pagesAnxiety Disorders in ChildrenooiseowwweiNo ratings yet
- Rehabilitation of Spinal Cord Injuries: Kemal Nas, MD, Professor, Series EditorDocument10 pagesRehabilitation of Spinal Cord Injuries: Kemal Nas, MD, Professor, Series EditorMuhammad AbduhNo ratings yet
- Fabry DiseaseDocument63 pagesFabry DiseaseKunal PaulNo ratings yet
- US NCP-5 Owner Manual PN 21980-04 With Treatment Pants and Indications A PDFDocument103 pagesUS NCP-5 Owner Manual PN 21980-04 With Treatment Pants and Indications A PDFThanh Dao100% (1)
- Peripheral Arterial ExamDocument2 pagesPeripheral Arterial ExamliyeexzNo ratings yet
- Histology of PulpDocument61 pagesHistology of PulpLom SimloteNo ratings yet
- Model Paper ADocument7 pagesModel Paper AAndrewwwCheahNo ratings yet
- Management of Bleeding Disorders in Children - MannoDocument7 pagesManagement of Bleeding Disorders in Children - MannoRhiannon Bam OoiNo ratings yet
- Nursing Care Plan On: Ca OvaryDocument13 pagesNursing Care Plan On: Ca Ovaryvaishali TayadeNo ratings yet
- Company Profile Complete VersionDocument13 pagesCompany Profile Complete VersionJanna FabiaNo ratings yet
- Evidence-Based Care SheetDocument6 pagesEvidence-Based Care SheetTITINNo ratings yet
- @MedicalBooksStore 2012 Pelvic PainDocument243 pages@MedicalBooksStore 2012 Pelvic PainEnrique SwayneNo ratings yet
- Texas Has The Highest Maternal Mortality Rate in The Developed WorldDocument5 pagesTexas Has The Highest Maternal Mortality Rate in The Developed WorldDixanetNo ratings yet
- Lyme DiseaseDocument133 pagesLyme Diseaseernestval100% (3)
- Diagnosis Management of HypertensionDocument23 pagesDiagnosis Management of Hypertensionarahman168No ratings yet
- Infection Control Risk Assessment Tool 1208Document7 pagesInfection Control Risk Assessment Tool 1208sostro0% (1)
- App Ashcraft's Pediatric Surgery 5th EditionDocument8 pagesApp Ashcraft's Pediatric Surgery 5th EditionAndri Feisal NasutionNo ratings yet
- Alternativas A TotalesDocument12 pagesAlternativas A TotalesJuan Jose Stuven RodriguezNo ratings yet