Professional Documents
Culture Documents
PCAP Handout
Uploaded by
Cherr Noll0 ratings0% found this document useful (0 votes)
48 views1 pageThis document discusses pediatric community-acquired pneumonia. It notes that in neonates, group B streptococcus and gram-negative bacteria are most common, while in older infants and preschoolers, viruses like RSV are a frequent cause. After the neonatal period, S. pneumoniae is the most common bacterial cause. Clinical signs of pneumonia in children include fever, cyanosis, and respiratory distress. Diagnostic testing includes gram stain, culture, and oxygen saturation. Management involves respiratory support, antibiotics, and drainage of effusions. Complications can include hypoxia, respiratory distress, sepsis, and pleural effusions. Vaccination is the primary prevention method.
Original Description:
pediatric community acquired pneumonia
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses pediatric community-acquired pneumonia. It notes that in neonates, group B streptococcus and gram-negative bacteria are most common, while in older infants and preschoolers, viruses like RSV are a frequent cause. After the neonatal period, S. pneumoniae is the most common bacterial cause. Clinical signs of pneumonia in children include fever, cyanosis, and respiratory distress. Diagnostic testing includes gram stain, culture, and oxygen saturation. Management involves respiratory support, antibiotics, and drainage of effusions. Complications can include hypoxia, respiratory distress, sepsis, and pleural effusions. Vaccination is the primary prevention method.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
48 views1 pagePCAP Handout
Uploaded by
Cherr NollThis document discusses pediatric community-acquired pneumonia. It notes that in neonates, group B streptococcus and gram-negative bacteria are most common, while in older infants and preschoolers, viruses like RSV are a frequent cause. After the neonatal period, S. pneumoniae is the most common bacterial cause. Clinical signs of pneumonia in children include fever, cyanosis, and respiratory distress. Diagnostic testing includes gram stain, culture, and oxygen saturation. Management involves respiratory support, antibiotics, and drainage of effusions. Complications can include hypoxia, respiratory distress, sepsis, and pleural effusions. Vaccination is the primary prevention method.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 1
Pediatric Community-Acquired Pneumonia
The term community-acquired pneumonia
(CAP) refers to a pneumonia in a previously
healthy person who acquired the infection
outside a hospital.
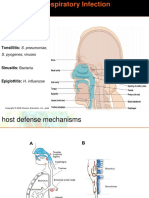
Etiology
Group B streptococcus and gram-
negative enteric bacteria are the most
common pathogens in neonates (i.e.,
birth to 20 days) and are obtained via
vertical transmission from the mother
during birth.
In infants older than four months and in
preschool-aged children, viruses are the
most frequent cause of CAP; respiratory
syncytial virus (RSV) is the most
common.
S. pneumoniae is the most common
bacterial cause of CAP after the
neonatal period. Less common bacterial
etiologies include Haemophilus
influenzae type B, Moraxella
catarrhalis, and Staphylococcus aureus.
Mycoplasma
pneumoniae and Chlamydia
pneumoniae frequently are associated
with CAP in pre-school-aged children
and are common causes of CAP in older
children and adolescents.
Mycobacterium tuberculosis also may
cause CAP in children at risk for
exposure.
Clinical Evaluation
The strongest predictors of pneumonia in
children are fever, cyanosis, and more than one
of the following signs of respiratory distress:
tachypnea, cough, nasal flaring, retractions,
rales, and decreased breath sounds.
Older children and adolescents are more likely
to have findings such as rales, dullness to
percussion, bronchial breath sounds, tactile
fremitus, and a pleural rub.
Diagnostic Testing
Gram stain and culture
Rapid antigen tests
Oxygen saturation
Management
Respiratory: inhaled oxygen
concentration, positive pressure
ventilation, Bi-level positive airway
pressure
Pharmacologic: Antibiotic agents, Anti-
inflammatory therapy, Antiviral agents,
Bronchodilators
For Pleural Effusion: Drainage of
parapneumonic effusions with or
without intrapleural instillation of a
fibrinolytic agent, Chest tube placement
for drainage of an effusion or empyema
Complications
refractory hypoxia
decompensated respiratory distress (eg,
lessening tachypnea due to fatigue,
hypercapnia)
sepsis
Pleural effusion
Empyema
Pneumatocele
Lung abscess
Prevention
Aside from avoiding infectious contacts (difficult
for many families who use daycare facilities),
vaccination is the primary mode of prevention.
Since the introduction of the conjugated HIB
vaccine, the rates of HIB pneumonia have
significantly declined. However, the diagnosis
should still be considered in unvaccinated
persons, including those younger than 2
months, who have not received their first shot.
You might also like
- Respiratory SystemDocument30 pagesRespiratory SystemHani El-asferNo ratings yet
- Chapter 1Document30 pagesChapter 1Ayro Business CenterNo ratings yet
- Addis Ababa University: Collage of Health Science Pediatrics and Neonatology On PneumoniaDocument21 pagesAddis Ababa University: Collage of Health Science Pediatrics and Neonatology On PneumoniaCheru DugaseNo ratings yet
- Case Study PcapDocument3 pagesCase Study PcapClaire PalaciosNo ratings yet
- Pediatric Community-Acquired Pneumonia: Causes, Symptoms & TreatmentDocument43 pagesPediatric Community-Acquired Pneumonia: Causes, Symptoms & TreatmentRazel Kinette AzotesNo ratings yet
- Epidemiology of TBDocument4 pagesEpidemiology of TByam pdNo ratings yet
- Pneumonia in ChildrenDocument22 pagesPneumonia in ChildrenHarsha HinklesNo ratings yet
- Updated September 2016: PneumoniaDocument5 pagesUpdated September 2016: PneumoniaYidnekachew Girma Assefa100% (1)
- Oleh: Ns. Hana Ariyani, M. KepDocument23 pagesOleh: Ns. Hana Ariyani, M. KepMuhammad Rizal alimuddinNo ratings yet
- Case On PcapDocument1 pageCase On PcapLorenn AdarnaNo ratings yet
- Community Acquires PneumoniaDocument3 pagesCommunity Acquires PneumoniabaniniycsebNo ratings yet
- Pneumonia: Key FactsDocument28 pagesPneumonia: Key FactsAri Widiastuti NiPutuNo ratings yet
- RSV Bronchiolitis Causes, Symptoms & TreatmentDocument6 pagesRSV Bronchiolitis Causes, Symptoms & TreatmentRonNo ratings yet
- Childhood Pneumonia Diagnosis and TreatmentDocument65 pagesChildhood Pneumonia Diagnosis and TreatmentYemata HailuNo ratings yet
- Case Ana Neonatal PneuDocument2 pagesCase Ana Neonatal PneuCharmie GandaNo ratings yet
- Reading Article (Pedia)Document2 pagesReading Article (Pedia)Babon , Christelle Anne S.No ratings yet
- Acute Respiratory InfectionsDocument50 pagesAcute Respiratory InfectionsLinus PuleNo ratings yet
- Cap MRDocument4 pagesCap MRKit BarcelonaNo ratings yet
- Pneumonia With Pleural EffusionDocument24 pagesPneumonia With Pleural EffusionMund CheleNo ratings yet
- READINGS PcapDocument2 pagesREADINGS PcapEden RelacionNo ratings yet
- 2002 23 132 Benjamin Gaston: Pediatr. RevDocument11 pages2002 23 132 Benjamin Gaston: Pediatr. RevDiego DíazNo ratings yet
- Practice Essentials: Pediatric Pneumonia MedicationDocument56 pagesPractice Essentials: Pediatric Pneumonia MedicationAnonymous HgX3mN1oNo ratings yet
- File 18587Document10 pagesFile 18587Mohammed MuthanaNo ratings yet
- Essential Update: Pediatric Pneumonia May Be Effectively Treated With Twice-Daily AmoxicillinDocument54 pagesEssential Update: Pediatric Pneumonia May Be Effectively Treated With Twice-Daily AmoxicillinYostesara Maurena SantosaNo ratings yet
- Pediatric PneumoniaDocument3 pagesPediatric PneumoniaErika GardeNo ratings yet
- Listeria Monocytogenes Escherichia Coli: Signs and SymptomsDocument15 pagesListeria Monocytogenes Escherichia Coli: Signs and SymptomsPuput's BourboneNo ratings yet
- Laryngitis: S. PneumoniaeDocument48 pagesLaryngitis: S. PneumoniaeTiyaTyraSidoraNo ratings yet
- Pneumonia 1Document17 pagesPneumonia 1Jonathan katanaNo ratings yet
- CH 11 PneumoniaDocument18 pagesCH 11 PneumoniaBader AljarboaNo ratings yet
- Community Acquired Pneumonia Nelson 400Document37 pagesCommunity Acquired Pneumonia Nelson 400fatima chrystelle nuñalNo ratings yet
- BronchioitisDocument24 pagesBronchioitismitiku aberaNo ratings yet
- Pneumonia Causes and TypesDocument30 pagesPneumonia Causes and TypesCabdiNo ratings yet
- Community Acquired PneumoniaDocument9 pagesCommunity Acquired PneumoniaSuzette Rae TateNo ratings yet
- Pediatric Pneumonia - Practice Essentials, Background, PathophysiologyDocument1 pagePediatric Pneumonia - Practice Essentials, Background, PathophysiologyShiferaw TesfayeNo ratings yet
- Pediatric PneumoniaDocument12 pagesPediatric PneumoniaKrystal Migo Denolo ContrerasNo ratings yet
- Weekly Epidemiological Report: A Publication of The Epidemiology Unit Ministry of Health, Nutrition & Indigenous MedicineDocument4 pagesWeekly Epidemiological Report: A Publication of The Epidemiology Unit Ministry of Health, Nutrition & Indigenous MedicineVijayakanth VijayakumarNo ratings yet
- Pneumonia WW ReportDocument29 pagesPneumonia WW ReportAradhanaRamchandaniNo ratings yet
- The Wheezing Infant: Airway Problems in ChildrenDocument4 pagesThe Wheezing Infant: Airway Problems in ChildrenDenise DelaneyNo ratings yet
- Pneumonia PresentationDocument54 pagesPneumonia PresentationSêrâphîm HâdíNo ratings yet
- Acute PharyngitisDocument3 pagesAcute PharyngitisMohammed Taha Al-nuaimyNo ratings yet
- Acute bronchiolitis causes and treatmentDocument3 pagesAcute bronchiolitis causes and treatmentHandre PutraNo ratings yet
- 2002 23 132 Benjamin Gaston: Pediatrics in ReviewDocument11 pages2002 23 132 Benjamin Gaston: Pediatrics in ReviewLuis Fernando Rojas ArroyoNo ratings yet
- PneumoniaDocument5 pagesPneumoniasamtaynbNo ratings yet
- Community Acquired Pneumonia, A Case StudyDocument26 pagesCommunity Acquired Pneumonia, A Case StudyMenggay SanDiego57% (7)
- _MICROMIDTERMSLABDocument27 pages_MICROMIDTERMSLABmicaellaabedejosNo ratings yet
- Child Health Nursing Teaching Staff Respiratory DisordersDocument47 pagesChild Health Nursing Teaching Staff Respiratory DisordersSimaNo ratings yet
- Tugas Translate JurnalDocument13 pagesTugas Translate JurnalWenny Eka FildayantiNo ratings yet
- Pcap Didactics ChanDocument61 pagesPcap Didactics ChanValerie Anne BebitaNo ratings yet
- WHO - PneumoniaDocument4 pagesWHO - Pneumoniadyan ayu puspariniNo ratings yet
- Community-Acquired Pneumonia in ChildrenDocument1 pageCommunity-Acquired Pneumonia in Childrenlouie john abilaNo ratings yet
- PneumoniaDocument2 pagesPneumoniaJen Ballesteros100% (1)
- Community-Acquired Pneumonia in Infants and ChildrenDocument9 pagesCommunity-Acquired Pneumonia in Infants and ChildrenLorenn AdarnaNo ratings yet
- Classification: PneumoniaDocument2 pagesClassification: PneumoniaAlbean DelojeroNo ratings yet
- Congenital and Neonatal Pneumonia PAEDIATRIC RESPIRATORY REVIEWS (2007) 8, 195-203 Michael D. NissenDocument9 pagesCongenital and Neonatal Pneumonia PAEDIATRIC RESPIRATORY REVIEWS (2007) 8, 195-203 Michael D. Nissenroggers72No ratings yet
- PneumoniaDocument3 pagesPneumoniaZel's FieldNo ratings yet
- Medical Mnemonic Sketches : Pulmonary DiseasesFrom EverandMedical Mnemonic Sketches : Pulmonary DiseasesNo ratings yet
- Leighs Construction Reference CheckDocument2 pagesLeighs Construction Reference CheckCherr NollNo ratings yet
- Gastroenteritis Causes, Symptoms, Treatment and PreventionDocument7 pagesGastroenteritis Causes, Symptoms, Treatment and PreventionCherr NollNo ratings yet
- Leadership Styles: AuthoritarianDocument5 pagesLeadership Styles: AuthoritarianCherr NollNo ratings yet
- Concept Map (Heartdiseases)Document3 pagesConcept Map (Heartdiseases)Cherr NollNo ratings yet
- Connective Tissue MatrixDocument2 pagesConnective Tissue MatrixCherr Noll0% (1)
- Gbs HandoutDocument2 pagesGbs HandoutCherr NollNo ratings yet
- GBSDocument21 pagesGBSCherr NollNo ratings yet
- Gastroenteritis Causes, Symptoms, Treatment and PreventionDocument7 pagesGastroenteritis Causes, Symptoms, Treatment and PreventionCherr NollNo ratings yet
- TeacherDocument1 pageTeacherCherr NollNo ratings yet
- Medical and Applied Sciences: Name: - DateDocument3 pagesMedical and Applied Sciences: Name: - DateCherr NollNo ratings yet
- Describe The Body Region Each of These Terms Refer To:: NameDocument2 pagesDescribe The Body Region Each of These Terms Refer To:: NameCherr NollNo ratings yet
- Theory of WagesDocument1 pageTheory of WagesCherr NollNo ratings yet
- Skeletal System Structure Functions and Types of Joints & BonesDocument14 pagesSkeletal System Structure Functions and Types of Joints & BonesCherr NollNo ratings yet
- Normal Values of CBCDocument1 pageNormal Values of CBCCherr NollNo ratings yet
- Theory of WagesDocument1 pageTheory of WagesCherr NollNo ratings yet
- Oiling The NavelDocument4 pagesOiling The NavelHazel100% (3)
- Vital Signs Procedures ChecklistDocument3 pagesVital Signs Procedures ChecklistharpreetNo ratings yet
- Case Study StrokeDocument5 pagesCase Study StrokelilutzuNo ratings yet
- Malaria in Children: Department of Paediatrics and Child Health, Mbarara UniversityDocument13 pagesMalaria in Children: Department of Paediatrics and Child Health, Mbarara UniversityMwanja MosesNo ratings yet
- BEmONC - Training ManualDocument263 pagesBEmONC - Training ManualdiribaNo ratings yet
- Clinical Abstract: Bañag, Daraga, Albay Contact Nos.: (Globe) 09271684061 (Smart) 09475160066Document1 pageClinical Abstract: Bañag, Daraga, Albay Contact Nos.: (Globe) 09271684061 (Smart) 09475160066kolintang1No ratings yet
- DR Walsh Autism Ocd Pandas Depression MethylationDocument6 pagesDR Walsh Autism Ocd Pandas Depression MethylationAnupama PouloseNo ratings yet
- Chapter 8A Neonatal Emergencies.Document35 pagesChapter 8A Neonatal Emergencies.Sai NathNo ratings yet
- Torrent Downloaded From ExtraTorrent - CCDocument26 pagesTorrent Downloaded From ExtraTorrent - CCZorofan Roronoa AzNo ratings yet
- Circulatory and Respiratory System Crossword PuzzleDocument4 pagesCirculatory and Respiratory System Crossword Puzzlejoel jacobNo ratings yet
- ATI RN Mental Health Online Practice BDocument38 pagesATI RN Mental Health Online Practice Bseansdrew2No ratings yet
- Large Databases in Anaesthesiology: ReviewDocument6 pagesLarge Databases in Anaesthesiology: ReviewSoumya DasNo ratings yet
- Activity # 3 - Research JournalDocument3 pagesActivity # 3 - Research Journalcayla mae carlosNo ratings yet
- Pelvic Traction SlingDocument3 pagesPelvic Traction SlingArturo Jr Garces RNNo ratings yet
- Thyroid Disorders Part II Hypothyroidism and Thyroiditis LIttle 2006Document6 pagesThyroid Disorders Part II Hypothyroidism and Thyroiditis LIttle 2006Jing XueNo ratings yet
- 4 - The Circulatory System - PPTDocument110 pages4 - The Circulatory System - PPTRinopro 555No ratings yet
- Query ReplyDocument5 pagesQuery ReplyParakhModyNo ratings yet
- CPG - Acute Infectious DiarrheaDocument52 pagesCPG - Acute Infectious DiarrheaJim Christian EllaserNo ratings yet
- Fever: Clinical DescriptionDocument6 pagesFever: Clinical DescriptionNama ManaNo ratings yet
- DKA AssignmentDocument4 pagesDKA AssignmentHisham ShahinNo ratings yet
- Extrahepatic Biliary AtresiaDocument3 pagesExtrahepatic Biliary AtresiaTiti Afrianto100% (1)
- Ohio Voter Rights CoalitionDocument19 pagesOhio Voter Rights CoalitionsrichardsonNo ratings yet
- International Classification of Function, Disabiltiy and HealthDocument31 pagesInternational Classification of Function, Disabiltiy and Healthsri subhikshaNo ratings yet
- Cebu Normal University: Drug StudyDocument2 pagesCebu Normal University: Drug StudyGwen Marie Taboada100% (1)
- Oncology: Nursing Management in Cancer CareDocument27 pagesOncology: Nursing Management in Cancer CareAmy50% (2)
- CHICKENPOX: SIGNS, SYMPTOMS, TREATMENT AND NURSING CAREDocument16 pagesCHICKENPOX: SIGNS, SYMPTOMS, TREATMENT AND NURSING CAREAlbert TerbioNo ratings yet
- Hypertensive Renal DiseaseDocument2 pagesHypertensive Renal DiseaseHenry KaweesaNo ratings yet
- Occupational Noise Exposure: A Review of Its Effects, Epidemiology, and Impact With Recommendations For Reducing Its BurdenDocument28 pagesOccupational Noise Exposure: A Review of Its Effects, Epidemiology, and Impact With Recommendations For Reducing Its BurdenRizal KendariNo ratings yet
- PBL 2 Scarred Glands - Draft 1Document5 pagesPBL 2 Scarred Glands - Draft 1Shellz2428No ratings yet
- Medical Emergency Part 2Document10 pagesMedical Emergency Part 2navyaNo ratings yet