Professional Documents
Culture Documents
11 - Facts and Myths Regarding The Maxillary Midline Frenum and Its Treatment A Systematic Review of The Literature
Uploaded by
kochikaghochi100%(1)100% found this document useful (1 vote)
522 views11 pagesk
Original Title
11 . Facts and Myths Regarding the Maxillary Midline Frenum and Its Treatment a Systematic Review of the Literature
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentk
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
100%(1)100% found this document useful (1 vote)
522 views11 pages11 - Facts and Myths Regarding The Maxillary Midline Frenum and Its Treatment A Systematic Review of The Literature
Uploaded by
kochikaghochik
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 11
VOLUME 44 NUMBEP 2 FEBPUAPY 2013 177
QUI NTESSENCE I NTERNATI ONAL
GENERAL DENTISTRY/ORAL SURGERY
dible and maxilla, usually in the midline or
premolar region. In the mandible, a frenum
is generally also present lingually to the
central incisors with a connection into the
body of the tongue.
2
The maxillary midline
frenum connects the mucosa of the maxil-
lary alveolar process and central incisors to
the upper lip. It originates as a remnant of
the tectolabial bands, which are embryonic
structures and connect the tubercle of the
upper lip to the palatine papilla.
3
Histologically, it contains elastic bers and
collagen tissue components, although stri-
ated (skeletal) muscle bers are frequently
found in biopsy specimens.
4
The maxillary frenum is a dynamic struc-
ture, subjected to alterations in shape, size,
and position during the stages of human
growth and development. Generally, it
A ronum is a small band or old o muoosal
membrane that attaches the lips and cheeks
to the alveolar process and limits their
movements.
1
Frena are most prominently
found in the vestibular mucosa of the man-
1
Research Fellow, Department of Oral Surgery and Stomatology,
University of Bern, Bern, Switzerland.
2
Research Fellow, Department of Orthodontics and Dentofacial
Orthopedics, University of Bern, Bern, Switzerland.
3
Professor and Head, Department of Periodontology, University
of Bern, Bern, Switzerland.
4
Professor and Head, Department of Orthodontics and
Dentofacial Orthopedics, University of Bern, Bern, Switzerland.
5
Assistant Professor, Department of Oral Surgery and
Stomatology, University of Bern, Bern, Switzerland.
Correspondence: PD Dr Michael M. Bornstein, Department of
Oral Surgery and Stomatology, Freiburgstrasse 7, 3010 Bern,
Switzerland. Email: michael.bornstein@zmk.unibe.ch
Facts and myths regarding the maxillary midline
frenum and its treatment: A systematic review of
the literature
Konstantina Delli, DMD
1
/Christos Livas, DMD
2
/Anton Sculean, Prof Dr
Med Dent
3
/Christos Katsaros, Prof Dr Med Dent
4
/Michael M. Bornstein,
PD Dr Med Dent
5
Objective: To systematically review the current literature on the maxillary midline frenum
and associated conditions and complications, as well as the recommended treatment
options. Method and Materials: A dotailod MEDLNE databaso soaron was oarriod out to
provide evidence about the epidemiology, associated pathologies, and treatment options
regarding the maxillary frenum. Of the 206 initially identied articles, 48 met the inclusion
criteria. Results: The maxillary frenum is highly associated with a number of syndromes
and dovolopmontal abnormalitios. A nyportropnio ronum may bo involvod in tno otiology
of the midline diastema. There is also a tendency by orthodontists to suggest posttreat-
ment removal of the frenum (frenectomy). Studies on the cause of gingival recession due
to tno maxillary ronum aro inoonolusivo. An in|urod ronum in oombination witn otnor
traumas and doubtful history might point to child abuse. The involvement of hyperplastic
frena in the pathogenesis of peri-implant diseases remains uncertain. There seems to be a
clinical interest regarding lasers for surgery for treatment of maxillary frena. The superiority
of laser treatment in relation to conventional surgical methods has not yet been demon-
strated in the literature. Conclusion: A maxillary ronum is a olinioal symptom in numorous
syndromic conditions and plays a role in the development of the median midline diastema.
Novortnoloss, tno oontribution to gingival rooossion and pori-implant disoasos in tno rogion
of the maxillary incisors is rather controversial. Laser techniques are reported as the
method of choice for the surgical removal of frena; however, this needs to be substanti-
ated by appropriate prospective controlled studies. (Quintessence Int 2013;44:177187)
Key words: frenectomy, gingival recession, maxillary frenum, midline diastema,
peri-implantitis
178 VOLUME 44 NUMBEP 2 FEBPUAPY 2013
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
tends to diminish in size over the course of
life.
5
The eruption of the permanent incisors,
the development of the maxillary sinus, and
the growth of the alveolar process all result
in a more coronal insertion of the frenum.
6
Two approaches were presented in the
literature to categorize the various types of
maxillary midline frena according to mor-
pnologio onaraotoristios (Tablo 1). An oarly
attempt was made by Sewerin, who recom-
mended that the labial frenum should be
divided into eight categories.
7
In 1974,
Mirko et al
8
suggested a new classication
based on the interaction between the fre-
num and the periodontium of the maxillary
incisors. Four types of frena were suggest-
ed, according to the site of the attachment:
mucosal, gingival, papillary, or papillary
penetrating
8
(Figs 1 and 2). This classica-
tion has gained wide acceptance and is
commonly used by periodontists and ortho-
dontists alike.
Altnougn tno maxillary midlino ronum is
of interest to orthodontists, periodontists,
and oral surgeons alike, there is no study
available in the literature focusing on the
various phenotypes of the maxillary frenum,
their associated problems and conditions,
or the recommended treatment strategies.
Clinicians seem to substantiate their deci-
sions on their experience and low-evidence
data. The aim of the present study is to illu-
minate all of these aspects and identify
evidence based information provided by
the contemporary scientic literature.
SEARCH STRATEGY
The authors conducted a search using the
MEDLNE databaso rom January 1966 to
July 2011. Tno koy words appliod woro
|"labial ronum" AND/OP "labial ronulum"
AND/OP "maxillary ronum" AND/OP "max-
illary ronulum"] AND "provalonoo" AND
"otiology" AND |"probloms" OP "oomplioa-
tions" OP "oonsoquonoos"] AND |"tnorapy"
OP "troatmont"].
A sooond soaron in PubMod was oarriod
out for the same time period, using the com-
bination of the following Medical Subject
Hoading (MoSH) torms: "labial ronum/
abnormalitios"|Mosn] OP "labial ronum/
anatomy and nistology"|Mosn] OP "labial
ronum/ombryology"|Mosn] OP "labial ro-
num/growtn and dovolopmont"|Mosn] OP
"labial ronum/patnology"|Mosn] OP "labial
ronum/surgory"|Mosn].
Only clinical articles were included and
evaluated. The authors considered clinical
Table 1 Different classifcations of maxillary midline frenum
Study Type of study n Method of assessment Classifcation
Sewerin
7
Case series 1430 Inspection
Normal ronum
Porsistont tootolabial ronum
Frenum with appendix
Frenum with nodule
Duplioation o tno ronum
Poooss o tno ronum
Bihd ronum
Coincidence of two or more of the above
Mirko et al
8
Case series 465 Inspection
Mucosal frenum attachment
Gingival frenum attachment
Papillary ronum attaonmont
Papillary ponotrating ronum attaonmont
VOLUME 44 NUMBEP 2 FEBPUAPY 2013 179
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
studies including case reports, if they
reported on the following subjects:
Epidemiologic data including preva-
lence and etiology
Assooiatod probloms and patnologios
(ie, median diastema, gingival reces-
sion, diminished retention and stability
of removable dentures, peri-implantitis,
syndromes, and child abuse)
Therapy of the maxillary midline frenum
Posttroatmont oomplioations.
In the rst stage of the selection, titles were
screened to identify duplicates and articles
appoaring ropoatodly. Atorwards, two
obsorvors (KD and CL) indopondontly oval-
uated all the abstracts of the obtained arti-
cles. The Kappa score for agreement
between the reviewers for screening of
abstracts was 0.87. For the abstracts that
met the inclusion criteria, the respective full
text was thoroughly studied. Finally, refer-
ence lists of the retained publications were
scanned for additional relevant articles that
might have been missed in the initial data-
base search. The details of the literature
search strategy are presented in Fig 3.
The quality of each study was assessed
and gradod witn a sooro o 1A-5 aooording
to the classication for Evidence-based
Medicine Levels of Evidence developed by
tno Oxord Contor (nttp://www.oobm.not).
The criteria applied in the grading of the
studios woro tno ollowing: 1A, systomatio
roviow o randomizod olinioal trials (PCTs)
inoluding mota-analysis, 1B, individual
PCTs witn narrow oonhdonoo intorval, 1C,
all and nono studios, 2A, systomatio roviow
Fig 1 Clinical example of a papillary frenum attachment in a 16-year-old boy referred for frenectomy. (a)
Buccal and (b) occlusal views.
Fig 2 Clinical example of a papillary penetrating frenum attachment in a 9-year-old girl referred for frenec-
tomy. (a) Buccal and (b) occlusal views.
a
a
b
b
180 VOLUME 44 NUMBEP 2 FEBPUAPY 2013
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
o oonort studios, 2B, individual oonort stud-
ios and low-quality PCTs, 2C, outoomo
rosoaron study, 3A, systomatio roviows o
oaso-oontrollod studios, 3B, individual
case-controlled studies; 4, case series and
poor quality cohort and case-controlled
studies; and 5, expert opinions.
EPIDEMIOLOGY
Eight retrospective observational studies
(grado 3B lovol o ovidonoo)
6-13
were
retrieved to investigate the prevalence of
the different phenotypes of maxillary midline
frena among different age groups, using
one of the classication systems mentioned
above.
7,8
The most common frenum types
were the mucosal or gingival types (Table 2).
FRENUM AND
SYNDROMES
There are numerous syndromes described
in the literature that characteristically exhib-
it variations of the norm of maxillary midline
frenum phenotype (Table 3). Our search
resulted in three retrospective observational
studios (grado 3B)
14-16
and three case
reports (grade 4).
17-19
MAXILLARY FRENUM AND
MIDLINE DIASTEMA
The maxillary midline diastema, located
between the maxillary central incisors, is
relatively common during the mixed denti-
Maxillary frenum
Maxillary frenulum
Labial frenum
Labial frenulum
First screening (n = 97)
Included
articles (n = 48)
Provalonoo (n = 26)
Etiology (n = 119)
Probloms, oonsoquonoos
and complications (n = 69)
Therapy and
Treatment (n = 229)
Abnormalitios
Anatomy and nistology
Embryology
Growth and development
Patnology
Surgery
Labial frenum
(MeSH terms)
Second screening (n =109)
Fig 3 Flowchart visualizing the search strategy.
VOLUME 44 NUMBEP 2 FEBPUAPY 2013 181
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
tion stage. However, a midline diastema
wider than 2 mm rarely closes spontane-
ously during further development. This per-
sistent presence has long been considered
a pathologic entity and dental abnormality.
9
The current search strategy came up with
one prospective observational study (grade
3B),
20
four retrospective observational stud-
ios (grado 3B),
21-24
and one case report
(grade 4).
25
Histologic studies have revealed that
bundles of transseptal bers of the peri-
odontal ligament are normally found
between the central incisors. Collagen
bers of certain labial frena disrupt these
transseptal bers, and this disruption is
related to midline diastema.
21
The management of midline diastema
usually involves orthodontic treatment.
During troatmont, it is boliovod tnat tno
heavy orthodontic forces also deprive the
transseptal bers of sufcient blood supply.
Thus, completely new transseptal bers are
formed, replacing the old ones, which were
destroyed by ischemia.
23
Therefore, it is
suggested that the hypertrophic frenum
should be removed only after the comple-
tion of the active treatment, since the newly
developed tissue is expected to contribute
to the retention of the nal outcome.
Novortnoloss, tnoro aro no oontrollod stud-
ies that have evaluated this hypothesis.
In rare cases, the maxillary frenum is
exceptionally hypertrophic, inhibiting the
orthodontic closure or becoming trauma-
tized and painful. In these cases, it is
advised to surgically remove it before the
end of the orthodontic therapy.
25
Furthermore, it has been shown that the
removal of the frenum before orthodontics
leads to a more rapid crown approximation
of the incisors. However, this method is not
Table 2 Phenotype of maxillary midline frena according to Mirkos classifcation
8
Frenum type Mirko et al
8
Lindsey
9
Addy et al
10
Kaimenyi
11
Boutsi & Tatakis
12
Janczuk & Banach
13
Mucosal 46.5% - 19.5% 26% 10.2% 39%
Gingival 34.3% - 76.6% 50% 41.6% 36%
Papillary 3.1% - 3.9% - 22.1% -
Papillary
penetrating
16.1% 43% (infants)
14% (children with 6 permanent
anterior teeth)
7% (adults with all maxillary
permanent teeth)
24% 26.1% 5%
Table 3 Syndromes that characteristically exhibit variations of the norm in maxil-
lary midline frenum phenotype
Syndrome Type of maxillary frenum Clinical importance
Enlors-Danlos
14
Absont Indication to identify newborns at risk
Holoprosencephaly
15
Absont Part o tno standard oranioaoial oxamination
Turner
16
Gingival, papillary, or pene-
trating frenum attachment
-
False median cleft
of the upper lip
17
Absont Helps to differentiate true, false, or intermediate cleft
Orofacial-digital
18
Hyperplastic Minimum diagnostic criterion
Ellis van Creveld
19
Hyperplastic The most prominent oral nding
182 VOLUME 44 NUMBEP 2 FEBPUAPY 2013
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
widely accepted, because an abundance
of granulation tissue may complicate dia-
stema closure.
24
MAXILLARY FRENUM AND
GINGIVAL RECESSION
Gingival recession is characterized by
exposure of the root of the affected tooth,
which occurs when the gingival margin
moves apically from the cementoenamel
|unotion (CEJ). As oarly as 1939, Hirsonhold
observed a relationship between the attach-
ment of the frenum and periodontal dis-
ease.
26
This systematic review considered
three retrospective observational studies
(grado 3B)
10,27,28
and two expert opinions
(grade 5).
2,29
It has been reported that when the
attachment of a maxillary frenum is very
pronounced and also exhibits a crestal
insertion point close to the gingival margin
of the incisors, it can retract the marginal
gingiva or papilla, thus contributing to the
initiation or progression of periodontal dis-
ease.
2
Furthermore, oral hygiene proce-
dures may be complicated and the accu-
mulation and retention of plaque may be
promoted when the periodontal pocket is
pulled and opened, allowing food debris to
enter more readily.
29
Mirko et al found that certain types of
maxillary frenum inuence periodontal con-
dition. The periodontal resistance was sig-
nicantly lower in cases of gingival, papillary,
and papillary-penetrating types of maxillary
frenum attachment in persons with patho-
logic changes in the papilla in comparison to
persons with the same type of attachment
but with healthy papilla.
27
Additionally, a
recent study revealed that the correlation
between a maxillary frenum with crestal
attachment and the gingival recession was
more pronounced in men than women.
28
In
oontrast, Addy ot al
10
reported that plaque
and bleeding scores of the maxillary incisors
decreased when increasing the proximity of
the frenum to the gingival margin. Therefore,
they support that the position of the maxil-
lary frenum is not relevant for plaque accu-
mulation and gingivitis.
10
At tno timo boing, tno data domonstrat-
ing a clear cause-and-effect relationship
between the presence of an abnormal max-
illary frenum and gingival recession are
lacking.
MAXILLARY FRENUM AND
CHILD ABUSE
Our literature screening revealed one retro-
spootivo obsorvational study (grado 3B)
30
and three case reports (grade 4).
31-33
The
maxillary frenum can be accidentally torn in
falls during the early stages of walking,
31
in
car accidents with airbag deployment,
34
or
after cardiopulmonary resuscitation.
35
Novortnoloss, sovoral oaso roports olaim
that tears of the frenum are one of the most
frequent intraoral ndings in child abuse.
31-33
A rooont systomatio roviow nas rovoalod
that there are no studies comparing the
incidence of torn frena in abused and non-
abused children. Therefore, a torn frenum
alone cannot be considered pathogno-
monic of child abuse.
36
Novortnoloss, tno
presence of this condition, especially in
combination with signs of trauma on other
parts of the body without conclusive anam-
nestic data, should alert health care profes-
sionals.
MAXILLARY FRENUM AND
DENTURES
Pogarding tnis topio, our rotrospootivo
obsorvational studios (grado 3B)
37-40
and
one case report (grade 4)
41
were found.
Ator tno inoorporation o tno romovablo
denture, denture-induced lesions are the
most common complaint. It has been
shown that 45% of full maxillary denture
wearers are affected by these lesions.
38
They usually appear at the frena (midline
and lateral) and the regions of muscular
attachment.
39
A rooont study nas oonhrmod
that the most frequent areas of denture-
induced irritations in the maxilla were the
vestibular sulcus between the midline and
VOLUME 44 NUMBEP 2 FEBPUAPY 2013 183
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
lateral frenum (44%), followed by the maxil-
lary tuberosity (37%).
40
In patients wearing dentures for many
years, frena tend to migrate to the crest,
probably due to the reduction of the height
of the residual ridge.
41
One report docu-
menting instability of dentures due to a fre-
num concerned the hamular frenum.
42
It
may be that clinicians, when taking impres-
sions, are particularly cautious of the maxil-
lary midline frenum area or that problems
caused by the maxillary frenum are noted
and modied already in the early stages of
manufacturing of the denture.
MAXILLARY FRENUM AND
PERI-IMPLANT DISEASES
Pogarding tnis topio, inormation rom only
two case reports (grade 4)
43,44
could be
retrieved.
Otto and Gluckman
43
proposed that
muscles and active frenum should be care-
fully examined as potential cofactors for
peri-mucositis and peri-implantitis, and in
the case of a pull, they should be surgically
removed. They additionally suggested that
the best technique is vestibuloplasty, where
a split-thickness ap is sutured in the lower
level of the vestibule, combined, for better
results, with an epithelial transplant from the
palate to augment the attached gingiva.
43
Park
44
has published a case report describ-
ing a technique to correct the frenal pull
and to increase the width of keratinized
mucosa around implants in the maxillary left
molar area.
MAXILLARY FRENUM AND
FRENECTOMY
The indications for surgical removal of
the maxillary midline frenum are usually the
following
45
: prevention of median diastema
formation, prevention of postorthodontic
relapse of a median diastema, facilitation of
oral hygiene procedures, and prevention of
gingival recession (although maxillary fre-
num have never been clearly shown to lead
to recession) .
Frenectomy implies total removal of the
frenum, while in frenotomy, the frenum is
partially removed. These techniques are
also classied as excisional (total removal
o tno ronum) or ropositioning (onango/
alteration of the frenums normal position).
46
With regard to frenectomy, the present
review identied two clinical trials (grade
2B),
45,47
tnroo PCTs (grado 2B),
48-50
two ret-
rospective observational studies (grade
3B),
51,52
and ve case reports (grade 4)
53-57
(Table 4).
Various surgical techniques have been
proposed by clinicians (Table 5). The sim-
plest method is performed with two parallel
incisions on each side of the frenum joined
Table 4 Analysis of the articles with a high level of evidence
Author Patients Results
Pandomizod
clinicial trials
Haytac & Ozcelik
48
40 Carbon dioxide laser treatment offers less postoperative pain
and functional complications than the scalpel technique
Kara
49
40 Nd:YAG lasor providos a bottor pationt porooption o suoooss
than conventional surgery
Dosiato ot al
50
20 980-nm diode laser in oral surgery is efcient, safe, and well
accepted by patients
Clinical trials Kahnberg
45
30 Z-plasty is the technique that mostly reduces the frenum height
Genovese & Olivi
47
50 Erbium lasers are very effective in pediatric dentistry
184 VOLUME 44 NUMBEP 2 FEBPUAPY 2013
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
in the vestibule by a scissor cut. The wound
edges are closed with a single suture.
45
This technique, known also as a V-shaped
inoision, Aronor inoision, or diamond-
shaped incision, is reported to leave a scar
contracture that can lead to periodontal
problems, as well as loss of the interdental
papilla between the maxillary central inci-
sors.
53
In the Z-plasty incision, a vertical inci-
sion is made along the frenum from the
gingival margin to the vestibule. Then two
incisions are made at each end of the pri-
mary incision at an angle of 60 degrees,
pointing in opposite directions, forming
Z-shaped incisions. The two mucosal aps,
without periosteum, are elevated and
sutured in a reverse position.
45
This tech-
nique permits better distribution of the scar
contracture lines, but is more complicated
and aggressive than the V-shape
approach.
53
Kahnberg
45
also described the vestibu-
lar sulcus extension, where a horizontal
incision reaching the periosteum is made 2
to 3 mm beneath the gingival margin,
extending from one maxillary canine to the
other. The elevated mucosal ap is then
positioned apically and sutured to the peri-
osteum. The wound area is usually covered
with a surgical pack. However, this proce-
dure has a high rate of relapse, and its use
is consequently limited.
45
Additionally, Morsolli ot al
53
presented a
technique inspired by upper labial rhino-
plastio proooduros. Bagga ot al
54
have
recently reported a modied V-shape tech-
nique in cases of high esthetic require-
ments. Two triangular pedicles are sutured
together medially and completely cover the
V-shaped region, inducing healing by pri-
mary intention and minimizing scar forma-
tion.
Often, frenectomy is combined with the
use of a laterally positioned ap or free gin-
gival grafts to minimize relapse or exces-
sive scar formation and maximize esthetic
results.
55,56
In cases of minimal esthetic
concerns, a palatal mucosal graft can be
used, since it creates a tire-patch or tattoo-
like appearance in the grafted area.
54
The use of lasers for frenectomy has
been promoted recently, and diode laser,
neodymium-doped: yttrium, aluminum and
garnot (Nd:YAG) lasor, and orbium-dopod
(Er:YAG) lasors navo boon roportod.
Novortnoloss, tno oarbon dioxido lasor is
probably the most frequently used
57,58
(see
Fig 4). A sorios o publioations roport tnat
when frenectomy is executed with lasers,
the patient experiences markedly less
bleeding during surgery, no need for
sutures or periodontal dressing,
57
fewer
functional complications,
48,49
minimal swell-
ing, less discomfort,
50
and requires fewer
analgesics than when a scalpel frenectomy
was performed.
49
Table 5 Surgical techniques for frenectomy
Type of technique Advantages Disadvantages
v-snapod/Aronor inoision/
diamond incision
45
Easy to perform Scar tissue formation
Loss of papilla
High relapse rate
Z-plasty
45
Less scar formation Surgically demanding
Moro aggrossivo/morbidity
Vestibular sulcus
extension
45
- High relapse rate
Morselli et al
53
Less tissue contracture
Less scar formation
Less healing time
Surgically demanding
Bagga ot al
54
Advanood ostnotio rosults
Minimal scar tissue formation
Porormod only in oasos o adoquato
attached gingiva
VOLUME 44 NUMBEP 2 FEBPUAPY 2013 185
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
CONCLUSIONS
To the best of our knowledge, the current
systematic review is the rst in the literature
to address the prevalence of different phe-
notypes, associated complications, and
treatment of the maxillary midline frenum.
The most common types of article analyzed
for this study were reviews and case reports.
Only three randomized controlled trials
were found, two concerning the patients
perception during frenectomy using carbon
dioxide laser vs scalpel
48,49
and one con-
cerning the safety and efcacy of 980 nm
diode laser in oral surgery.
50
Therefore, cur-
rent therapeutic concepts have to be con-
sidered as not being based on high levels
of evidence.
Basod on tno availablo data, it oan bo
suggested that:
Abnormalitios o tno maxillary ronum
are present in numerous syndromes.
A nyportropnio maxillary ronum is nignly
associated with a midline diastema.
Altnougn olinioians and rosoaronors
suggest that its removal should be per-
formed after the completion of the orth-
odontic therapy, this hypothesis is not
based on any controlled studies.
The involvement of the maxillary frenum
in the formation and promotion of gingi-
val recessions of the maxillary incisors is
not clear.
A torn maxillary ronum mignt bo a sign
of abuse.
The maxillary frenum rarely causes
problems in removable denture reten-
tion and stability.
Fig 4 The use of lasers for frenectomy has been promoted, and the carbon dioxide laser is most frequently
used. (a) Initial clinical aspect, (b) immediately after carbon dioxide laser surgery, (c) 1 month after interven-
tion, and (d) 1 year after the intervention.
a
c
b
d
186 VOLUME 44 NUMBEP 2 FEBPUAPY 2013
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
The involvement of hyperplastic frena in
the pathogenesis of peri-mucositis and
peri-implantitis is questionable and has
only been reported on an anecdotal
basis.
Various surgical techniques have been
proposed for successful removal of the
maxillary frenum. The use of lasers is
inoroasingly popular. Novortnoloss,
more randomized controlled trials with
clear outcome parameters are needed
to demonstrate potential benets of laser
vs scalpel use for surgical therapy.
ACKNOWLEDGMENT
The authors would like to thank Mrs Brigitte Leuenberger,
librarian at the School of Dental Medicine at the
University of Bern, Switzerland, for her assistance during
the literature search.
REFERENCES
1. Cohen ES. Atlas of Periodontal Surgery. Philadelphia:
Lea and Febiger, 1988.
2. Minsk L. The frenectomy as an adjunct to periodon-
tal treatment. Compend Contin Educ Dent
2002;23:424-428.
3. Edwards JG. A clinical study: The diastema, the fre-
num, the frenectomy. Oral Health 1977;67:51-62.
4. Ross RO, Brown FM, Houston GD. Histological sur-
vey of the frena of the oral cavity. Quintessence Int
1990;21:233-237.
5. Dewel BF. The labial frenum, midline diastema, and
palatine papilla: A clinical analysis. Dent Clin North
Am 1966;35:175-184.
6. Daz-Pizn ME, Lagravre MO, Villena R. Midline
diastema and frenum morphology in the primary
dentition. J Dent Child (Chic) 2006;73:11-14.
7. Sewerin I. Prevalence of variations and anomalies of
the upper labial frenum. Acta Odontol Scand
1971;29:487-496.
8. Mirko P, Miroslav S, Lubor M. Signifcance of the
labial frenum attachment in periodontal disease in
man. Part I. Classifcation and epidemiology of the
labial frenum attachment. J Periodontol
1974;45:891-894.
9. Lindsey D. The upper mid-line space and its relation
to the labial fraenum in children and in adults. A
statistical evaluation. Br Dent J 1977;143:327-332.
10. Addy M, Dummer PM, Hunter ML, Kingdon A, Shaw
WC. A study of the association of fraenal attachment,
lip coverage, and vestibular depth with plaque and
gingivitis. J Periodontol 1987;58:752-757.
11. Kaimenyi JT. Occurrence of midline diastema and
frenum attachments amongst school children in
Nairobi, Kenya. Indian J Dent Res 1998;9:67-71.
12. Boutsi EA, Tatakis DN. Maxillary labial frenum
attachment in children. Int J Paediatr Dent
2011;21:284-288.
13. Jaczuk Z, Banach J. Prevalence of narrow zone of
attached gingival and improper attachment of labi-
al frena in youths. Community Dent Oral Epidemiol
1980;8:385-386.
14. Da Felice C, Toti P, Maggio G, Parinmi S, Bagnoli F.
Absence of the inferior labial and lingual frenula in
Ehlers-Danlos syndrome. Lancet 2001;357:1500-1502.
15. Martin RA, Jones KL. Absence of the superior labial
frenulum in holoprosencephaly: a new diagnostic
sign. J Pediatr 1998;133:151-153.
16. Kusiak A, Sadlak-Nowicka J, Limon J, Kochaska B.
The frequency of occurrence of abnormal frenal
attachment of lips and enamel defects in Turner
syndrome. Oral Dis 2008;14:158-162.
17. Ichida M, Komuro Y, Yanai A. Consideration of
median cleft lip with frenulum labii superior. J
Craniofac Surg 2009;20:1370-1374.
18. King NM, Sanares AM. Oral-facial-digital syndrome,
Type I: A case report. J Clin Pediatr Dent 2002;26:
211-215.
19. Hattab FN, Yassin OM, Sasa IS. Oral manifestations
of Ellis-van Creveld syndrome: report of two siblings
with unusual dental anomalies. J Clin Pediatr Dent
1998;22:159-165.
20. Popovich F, Thompson GW, Main PA. Persisting
maxillary diastema: Diferential diagnosis and treat-
ment. Dent J 1977;43:330-333.
21. Ferguson MW, Rix C. Pathogenesis of abnormal
midline spacing of human central incisors. A histo-
logical study of the involvement of the labial fre-
num. Br Dent J 1983;154:212-218.
22. Shashua D, Artun J. Relapse after orthodontic cor-
rection of maxillary median diastema: a follow-up
evaluation of consecutive cases. Angle Orthod
1999;69:257-263.
23. Edwards JG. The reduction of relapse in extraction
cases. Am J Orthod 1971;60:128-141.
24. Campbell PM, Moore JW, Matthews JL.
Orthodontically corrected midline diastemas. A his-
tologic study and surgical procedure. Am J Orthod
1975;67:139-158.
25. Meister F Jr, Van Swol RL, Rank DF. The maxillary ante-
rior frenectomy. J Wis Dent Assoc 1981;57:205-210.
26. Hirschfeld I. The toothbrush, its use and abuse. J
Am Dent Assoc 1939;26:1237.
27. Mirko P, Miroslav S, Lubor M. Signifcance of the
labial frenum attachment in periodontal disease in
man. Part II. An attempt to determine the resistance
of periodontium. J Periodontol 1974;45:895-897.
VOLUME 44 NUMBEP 2 FEBPUAPY 2013 187
QUI NTESSENCE I NTERNATI ONAL
Del l i et al
28. Toker H, Ozdemir H. Gingival recession: Epidemiology
and risk indicators in a university dental hospital in
Turkey. Int J Dent Hyg 2009;7:115-120.
29. Swenson HM. ABCs periodontics. F is for the fre-
num. J Indiana Dent Assoc 1984;63:27-28.
30. Saxe MD, McCourt JW. Child abuse: A survey of
ASDC members and a diagnostic-data-assessment
for dentists. ASDC J Dent Child 1991;58:361-366.
31. Thackeray JD. Frena tears and abusive head injury: A
cautionary tale. Pediatr Emerg Care 2007;23:735-737.
32. Teece S, Crawford I. Best evidence topic report. Torn
frenulum and non-accidental injury in children.
Emerg Med J 2005;22:125.
33. Chan L, Hodes D. When is an abnormal frenulum a
sign of child abuse? Arch Dis Child 2004;89:277.
34. Morisson AL, Chute D, Radenstaz S. Airbag associ-
ated injury to a child in the front passenger seat. Am
J Forensic Med Pathol 1998;19:218-222.
35. Price EA, Rush LR, Perper JA. Cardiopulmonary
resuscitation-related injuries and homicidal blunt
trauma in children. Am J Forensic Med Pathol
2000;21:307-310.
36. Maguire S, Hunter B, Hunter L, Sibert JR, Mann M,
Kemp AM. Welsh Child Protection Systematic
Review Group. Diagnosing abuse: a systematic
review of torn frenum and other intra-oral injuries.
Arch Dis Child 2007;92:1113-1117.
37. Latta GH Jr. The midline and its relation to anatomic
landmarks in the edentulous patient. J Prosthet
Dent 1988;59:681-683.
38. Jainkittivong A, Aneksuk V, Langlais RP. Oral muco-
sal lesions in denture wearers. Gerodontology
2010;27:26-32.
39. Bergman B, Carlsson GE. Review of 54 complete
denture wearers. Patients opinions 1 year after
treatment. Acta Odontol Scand 1972;30:399-414.
40. Kivovics P, Jhn M, Borbly J, Mrton K. Frequency
and location of traumatic ulcerations following
placement of complete dentures. Int J Prosthodont
2007;20:397-401.
41. Axinn S, Brasher WJ. Frenectomy plus free graft. J
Prosthet Dent 1983;50:16-19.
42. Massad JJ, Anderson JF. Hamular frenum modifca-
tion: a removable denture prosthesis retention and
stability enhancement. Int J Periodontics Restorative
Dent 2001;21:183-189.
43. Otto M, Gluckman H. The treatment of peri-mucosi-
tis and peri-implantitis 2. SADJ 2008;63:312-314.
44. Park JB. Correcting the frenal pull and increasing
the width of keratinized mucosa around endosse-
ous implants using denudation procedure. Indian J
Dent Res 2008;19:362-365.
45. Kahnberg KE. Frenum surgery. A comparison of three
surgical methods. Int J Oral Surg 1977;6:328-333.
46. Gontijo I, Navarro RS, Haypek P, Ciamponi AL,
Haddad AE. The applications of diode and Er:YAG
lasers in labial frenectomy in infant patients. J Dent
Child (Chic) 2005;72:10-15.
47. Genovese MD, Olivi G. Laser in paediatric dentistry:
Patient acceptance of hard and soft tissue therapy.
Eur J Paediatr Dent 2008;9:13-17.
48. Haytac MC, Ozcelik O. Evaluation of patient percep-
tions after frenectomy operations: A comparison of
carbon dioxide laser and scalpel techniques. J
Periodontol 2006;77:1815-1819.
49. Kara C. Evaluation of patient perceptions of frenec-
tomy: A comparison of Nd:YAG laser and conven-
tional techniques. Photomed Laser Surg 2008;26:
147-152.
50. Desiate A, Cantore S, Tullo D, Profeta G, Grassi FR,
Ballini A. 980 nm diode lasers in oral and facial prac-
tice: current state of the science and art. Int J Med
Sci 2009;6:358-364.
51. Fisher SE, Frame JW, Browne RM, Tranter RM. A
comparative histological study of wound healing
following CO
2
laser and conventional surgical exci-
sion of canine buccal mucosa. Arch Oral Biol
1983;28:287-291.
52. Frame JW. Removal of oral soft tissue pathology
with the CO
2
laser. J Oral Maxillofac Surg 1985;43:
850-855.
53. Morselli P, Vecchiet F, Marini I. Frenuloplasty by
means of a triangular fap. Oral Surg Oral Med Oral
Pathol Oral Radiol Endod 1999;87:142-144.
54. Bagga S, Bhat KM, Bhat GS, Thomas BS. Esthetic
management of the upper labial frenum: A novel
frenectomy technique. Quintessence Int
2006;37:819-823.
55. Ward VJ. A clinical assessment of the use of the free
gingival graft for correcting localized recession
associated with frenal pull. J Periodontol 1974;45:
78-83.
56. Freedman AL, Stein MD, Schneider DB. A modifed
maxillary labial frenectomy. Quintessence Int
1982;13:675-678.
57. Epstein SR. The frenectomy: a comparison of classic
versus laser technique. Pract Periodontics Aesthet
Dent 1991;3:27-30.
58. Bornstein MM, Suter VG, Staufer E, Buser D. The CO
2
laser in stomatology. Part 1 [in German]. Schweiz
Monatsschr Zahnmed 2003;113:559-570.
You might also like
- Dental Virtual Treatment Objective (VTO)Document4 pagesDental Virtual Treatment Objective (VTO)vprakshaindia100% (2)
- Contemporary Oral Oncology Diagnosis and ManagementDocument327 pagesContemporary Oral Oncology Diagnosis and ManagementJacky JunaediNo ratings yet
- Fundamentals of Occlusion in FPDDocument22 pagesFundamentals of Occlusion in FPDVishal Reddy100% (2)
- Scope of Public Health DentistryDocument14 pagesScope of Public Health DentistryNeha Jain100% (1)
- Bio Mechanics of Edentulous State.Document29 pagesBio Mechanics of Edentulous State.Indrani Das100% (2)
- Oral Health IndicesDocument105 pagesOral Health IndicesTeerawat OffNo ratings yet
- Multiple Simple Bone Cysts of The Jaws - Review of The Literature and Report of Three CasesDocument12 pagesMultiple Simple Bone Cysts of The Jaws - Review of The Literature and Report of Three CasesRodolpho VilelaNo ratings yet
- Diagnostic Principles of Peri-Implantitis: A Systematic Review and Guidelines For Peri-Implantitis Diagnosis ProposalDocument15 pagesDiagnostic Principles of Peri-Implantitis: A Systematic Review and Guidelines For Peri-Implantitis Diagnosis ProposalAngela RamirezNo ratings yet
- Technical Aspects of Treatment in Relation To Treatment OutcomeDocument14 pagesTechnical Aspects of Treatment in Relation To Treatment OutcomekochikaghochiNo ratings yet
- El 2011Document11 pagesEl 2011popsilviaizabellaNo ratings yet
- Cysts of The Jaws in Pediatric Population: A 12-Year Institutional StudyDocument6 pagesCysts of The Jaws in Pediatric Population: A 12-Year Institutional StudyAndreas SimamoraNo ratings yet
- A Method For Epidemiological Registration of MalocclusionDocument2 pagesA Method For Epidemiological Registration of Malocclusiontravolta0No ratings yet
- 1 s2.0 S1607551X11000349Document4 pages1 s2.0 S1607551X11000349xxxNo ratings yet
- Aboudara2009 PDFDocument12 pagesAboudara2009 PDFYsl OrtodonciaNo ratings yet
- Joss Vassalli2010Document15 pagesJoss Vassalli2010espinocelularNo ratings yet
- Maxillary Lateral Incisor Absence Craniofacial AnalysisDocument14 pagesMaxillary Lateral Incisor Absence Craniofacial Analysisacevariel5851No ratings yet
- Prevalence of Non-Carious Cervical Lesions in Dakar PrisonsDocument6 pagesPrevalence of Non-Carious Cervical Lesions in Dakar PrisonsDHONY MIFTAHUL HUDANo ratings yet
- Autogenous Transalveolar Transplantation ofDocument9 pagesAutogenous Transalveolar Transplantation ofAndi Askandar AminNo ratings yet
- AJODO-2013 Claudino 143 6 799Document11 pagesAJODO-2013 Claudino 143 6 799player osamaNo ratings yet
- Early Orthodontic Treatment of Skeletal Open-Bite MalocclusionDocument7 pagesEarly Orthodontic Treatment of Skeletal Open-Bite MalocclusionMaria SilvaNo ratings yet
- Coronoid Process Hyperplasia Surgery ReviewDocument7 pagesCoronoid Process Hyperplasia Surgery ReviewJuan Carlos MeloNo ratings yet
- Management of Common Voice DisordersDocument16 pagesManagement of Common Voice Disordersrowin93No ratings yet
- Lateral Periodontal CystDocument8 pagesLateral Periodontal CystTejas KulkarniNo ratings yet
- Follicular and Plexiform Ameloblastoma Case ReportDocument6 pagesFollicular and Plexiform Ameloblastoma Case Reportluckytung07No ratings yet
- Craniofacial Morphology in Women With Class I Occlusion and Severe Maxillary Anterior CrowdingDocument10 pagesCraniofacial Morphology in Women With Class I Occlusion and Severe Maxillary Anterior CrowdingMonojit DuttaNo ratings yet
- Prevalence of malocclusion in Chinese youthDocument8 pagesPrevalence of malocclusion in Chinese youthLuis SarmientoNo ratings yet
- Three-Dimensional Evaluation of The Maxillary Arch and Palate in Unilateral Cleft Lip and Palate Subjects Using Digital Dental CastsDocument5 pagesThree-Dimensional Evaluation of The Maxillary Arch and Palate in Unilateral Cleft Lip and Palate Subjects Using Digital Dental CastsDiego Andres Hincapie HerreraNo ratings yet
- Follicular Jaw CystsDocument6 pagesFollicular Jaw CystsMixelia Ade NoviantyNo ratings yet
- Mouth Floor Enlargements Related To The Sublingual Glands in Edentulous or Partially Edentulous Patients. A Microscopic StudyDocument6 pagesMouth Floor Enlargements Related To The Sublingual Glands in Edentulous or Partially Edentulous Patients. A Microscopic StudyDentist HereNo ratings yet
- Retrospective analysis of benign oral tumours and lesionsDocument8 pagesRetrospective analysis of benign oral tumours and lesionspaolaNo ratings yet
- Caries Periodontal and Prosthetic FindinDocument9 pagesCaries Periodontal and Prosthetic FindinConsultorio dentarioNo ratings yet
- CoronectomiaDocument8 pagesCoronectomiaAna Maria AgelvisNo ratings yet
- Orthodontic Therapy and Gingival Recession, A Systematic Review PDFDocument15 pagesOrthodontic Therapy and Gingival Recession, A Systematic Review PDFJose CollazosNo ratings yet
- Ramanauskaite 2016Document14 pagesRamanauskaite 2016Dr. Henner ValcarcelNo ratings yet
- Ameloblastic Fibroma: Report of A Case: Su-Gwan Kim, DDS, PHD, and Hyun-Seon Jang, DDS, PHDDocument3 pagesAmeloblastic Fibroma: Report of A Case: Su-Gwan Kim, DDS, PHD, and Hyun-Seon Jang, DDS, PHDdoktergigikoeNo ratings yet
- Prevalence and Severity of Vestibular Recession in Mandibular Incisors After Orthodontic Treatment A Case-Control Retrospective StudyDocument6 pagesPrevalence and Severity of Vestibular Recession in Mandibular Incisors After Orthodontic Treatment A Case-Control Retrospective StudyElla GolikNo ratings yet
- Osteosarcoma of The Jaw An Analysis of A Series of 74 Cases (2013)Document8 pagesOsteosarcoma of The Jaw An Analysis of A Series of 74 Cases (2013)sTEVENNo ratings yet
- Coronectomy 2Document14 pagesCoronectomy 2Rovian RosaliaNo ratings yet
- Prevalence of Malocclusion Among Adolescents in Ibadan, NigeriaDocument4 pagesPrevalence of Malocclusion Among Adolescents in Ibadan, NigeriaJose CollazosNo ratings yet
- The Mandibuiar Speech Envelope in Subjects With and Without Incisai Tooth WearDocument6 pagesThe Mandibuiar Speech Envelope in Subjects With and Without Incisai Tooth Wearjinny1_0No ratings yet
- Evaluation of Different Treatments For Oroantral Oronasal Communications - Abuabara Et Al PDFDocument4 pagesEvaluation of Different Treatments For Oroantral Oronasal Communications - Abuabara Et Al PDFVictor HernandezNo ratings yet
- Tumor Odontogenico EscamosoDocument4 pagesTumor Odontogenico Escamosoメカ バルカNo ratings yet
- Xác Định Nguyên Nhân Cắn Hở- Cắn SâuDocument8 pagesXác Định Nguyên Nhân Cắn Hở- Cắn Sâutâm nguyễnNo ratings yet
- 05-Is Measurement of The Gingival Biotype ReliableDocument6 pages05-Is Measurement of The Gingival Biotype ReliableaemontoNo ratings yet
- 1 - Prevalence of Maxillary Sinus SeptaDocument9 pages1 - Prevalence of Maxillary Sinus SeptaLamis MagdyNo ratings yet
- Examination of Antimicrobial and AntiinfDocument66 pagesExamination of Antimicrobial and AntiinfCristina CapettiNo ratings yet
- Does The Maxillary Midline Diastema Close After Frenectomy?: Oral SurgeryDocument10 pagesDoes The Maxillary Midline Diastema Close After Frenectomy?: Oral Surgeryantonio dlNo ratings yet
- Fabricating A Face: The Essence of Embryology in The Dental CurriculumDocument5 pagesFabricating A Face: The Essence of Embryology in The Dental CurriculumAna LozanoskaNo ratings yet
- 10 1016@j Bjoms 2020 08 017Document50 pages10 1016@j Bjoms 2020 08 017mlnunezNo ratings yet
- Keratocystic Odontogenic Tumour in A Hong Kong Community: The Clinical and Radiological FeaturesDocument9 pagesKeratocystic Odontogenic Tumour in A Hong Kong Community: The Clinical and Radiological FeaturesYenita AdetamaNo ratings yet
- Torus PalatinusDocument4 pagesTorus PalatinusPuji YuliastriNo ratings yet
- Jurnalku OsccDocument4 pagesJurnalku OsccAndiOctafiantoNo ratings yet
- Airway and Soft TissueDocument8 pagesAirway and Soft TissuejayashreeNo ratings yet
- Palate Morphology Sleep Bruxism Children (1)Document9 pagesPalate Morphology Sleep Bruxism Children (1)Camila Ignacia Diaz PaezNo ratings yet
- Odontogenic Cysts - A Descriptive Clinicopathological StudyDocument6 pagesOdontogenic Cysts - A Descriptive Clinicopathological StudyAvif PutraNo ratings yet
- JIAP October 2011 - The Influence of Restorations and Prosthetic Crowns Finishing Lines On Inflammatory Levels After Non-Surgical Periodontal TherapyDocument8 pagesJIAP October 2011 - The Influence of Restorations and Prosthetic Crowns Finishing Lines On Inflammatory Levels After Non-Surgical Periodontal TherapyMedstudNo ratings yet
- 22826Document9 pages22826Ghina Mukti LuthfiaNo ratings yet
- Bilateral Adenomatoid Odontogenic Tumour of The Maxilla in A 2-Year-Old Female-The Report of A Rare Case and Review of The LiteratureDocument7 pagesBilateral Adenomatoid Odontogenic Tumour of The Maxilla in A 2-Year-Old Female-The Report of A Rare Case and Review of The LiteratureStephanie LyonsNo ratings yet
- Abses SeptumDocument8 pagesAbses SeptumDian FahmiNo ratings yet
- Histological Analysis Differentiates Vocal Nodules and PolypsDocument7 pagesHistological Analysis Differentiates Vocal Nodules and PolypsRia Tupamahu MatatulaNo ratings yet
- Sonneveld 2018Document5 pagesSonneveld 2018James Alexander Toruño GordonNo ratings yet
- 5.occlusal Risk Factors Associated With Temporomandibular Disorders in Young Adults With Normal OcclusionsDocument5 pages5.occlusal Risk Factors Associated With Temporomandibular Disorders in Young Adults With Normal Occlusionsthiên lữNo ratings yet
- Kim 2010Document11 pagesKim 2010popsilviaizabellaNo ratings yet
- Ultrasonic Topographical and Pathotopographical Anatomy: A Color AtlasFrom EverandUltrasonic Topographical and Pathotopographical Anatomy: A Color AtlasNo ratings yet
- Antigen-Presentation and The Role of Dendritic Cells in PeriodontitisDocument23 pagesAntigen-Presentation and The Role of Dendritic Cells in PeriodontitiskochikaghochiNo ratings yet
- Peri-Implant Bone Loss As A Function of Tooth-Implant DistanceDocument7 pagesPeri-Implant Bone Loss As A Function of Tooth-Implant DistancekochikaghochiNo ratings yet
- Per I Tons IllerDocument25 pagesPer I Tons IllerkochikaghochiNo ratings yet
- 3mespe Cements v5Document12 pages3mespe Cements v5kochikaghochiNo ratings yet
- 11Document16 pages11kochikaghochiNo ratings yet
- Ijp 18 5 Elmowafy 13Document2 pagesIjp 18 5 Elmowafy 13kochikaghochiNo ratings yet
- 14Document13 pages14kochikaghochiNo ratings yet
- Cytokine Gene Polymorphism and Immunoregulation in Periodontal DiseaseDocument25 pagesCytokine Gene Polymorphism and Immunoregulation in Periodontal DiseasekochikaghochiNo ratings yet
- 15Document9 pages15kochikaghochiNo ratings yet
- Ijp 18 5 Editorial 1Document3 pagesIjp 18 5 Editorial 1kochikaghochiNo ratings yet
- Ijp 18 5 Hassel 11Document5 pagesIjp 18 5 Hassel 11kochikaghochiNo ratings yet
- 10Document10 pages10kochikaghochiNo ratings yet
- Ijp 18 5 Mack 9Document6 pagesIjp 18 5 Mack 9kochikaghochiNo ratings yet
- Ijp 18 5 Grandini 7Document6 pagesIjp 18 5 Grandini 7kochikaghochiNo ratings yet
- Ijp 18 5 Coward 8Document9 pagesIjp 18 5 Coward 8kochikaghochiNo ratings yet
- Effect of Original Water Content in Acrylic Resin On Processing ShrinkageDocument2 pagesEffect of Original Water Content in Acrylic Resin On Processing ShrinkagekochikaghochiNo ratings yet
- 6Document15 pages6kochikaghochi100% (1)
- Ijp 18 5 Botelho 2Document6 pagesIjp 18 5 Botelho 2kochikaghochiNo ratings yet
- 4Document18 pages4kochikaghochiNo ratings yet
- 5Document13 pages5kochikaghochiNo ratings yet
- 8Document15 pages8kochikaghochiNo ratings yet
- 9Document14 pages9kochikaghochiNo ratings yet
- 7Document8 pages7kochikaghochiNo ratings yet
- 3Document10 pages3kochikaghochiNo ratings yet
- The Use of Oral Implants in Compromised Patients: Daniel Van SteenbergheDocument3 pagesThe Use of Oral Implants in Compromised Patients: Daniel Van SteenberghekochikaghochiNo ratings yet
- Preoperative Radiologic Planning of Implant Surgery in Compromised PatientsDocument14 pagesPreoperative Radiologic Planning of Implant Surgery in Compromised PatientskochikaghochiNo ratings yet
- 14Document10 pages14kochikaghochiNo ratings yet
- 12Document13 pages12kochikaghochiNo ratings yet
- Diagnosis of Periodontal Manifestations of Systemic DiseasesDocument13 pagesDiagnosis of Periodontal Manifestations of Systemic DiseaseskochikaghochiNo ratings yet
- 11Document39 pages11kochikaghochiNo ratings yet
- Apical Canal ConfuencyDocument7 pagesApical Canal ConfuencyPanxo14No ratings yet
- The Aao "At-A-Glance" Guide To CDT 2021 Orthodontic Codes: DentitionDocument2 pagesThe Aao "At-A-Glance" Guide To CDT 2021 Orthodontic Codes: DentitionSweet ToothNo ratings yet
- Intraoral Welding PDFDocument1 pageIntraoral Welding PDFDrShweta SainiNo ratings yet
- Innovative Sonic Powered Irrigation: Three Benefi Ts in One SolutionDocument8 pagesInnovative Sonic Powered Irrigation: Three Benefi Ts in One Solutionpatel keralNo ratings yet
- Topical Fluoride Nov 2019 IDA TIMESDocument2 pagesTopical Fluoride Nov 2019 IDA TIMESDrMrsAyeshaKhushnoorNo ratings yet
- English ProjectDocument13 pagesEnglish ProjectOrlando NuhoNo ratings yet
- Knowledge, Attitudes and Practices of Caregivers in Relation To Oral Health of Preschool ChildrenDocument6 pagesKnowledge, Attitudes and Practices of Caregivers in Relation To Oral Health of Preschool ChildrenYayas Qori AwwaliNo ratings yet
- Riva Irlinda 22010110110073.BabVIIIKTI PDFDocument20 pagesRiva Irlinda 22010110110073.BabVIIIKTI PDFViaviaNo ratings yet
- Prosthesis SelectionDocument41 pagesProsthesis Selectionshahinshamshiri0% (1)
- Leah Flickinger ResumeDocument3 pagesLeah Flickinger Resumeapi-547898337No ratings yet
- Test - 9 Chronic PeriodontitisDocument5 pagesTest - 9 Chronic PeriodontitisIsak ShatikaNo ratings yet
- Reliability of Anatomic Reference Planes in Establishing The Occlusal Plane in Different Jaw Relationships: A Cephalometric StudyDocument8 pagesReliability of Anatomic Reference Planes in Establishing The Occlusal Plane in Different Jaw Relationships: A Cephalometric Studyedy harahapNo ratings yet
- Dental Hygiene Research Paper TopicsDocument4 pagesDental Hygiene Research Paper Topicsgwfdurbnd100% (1)
- Informed Consent Form For General Dental Procedures2Document3 pagesInformed Consent Form For General Dental Procedures2SkAliHassanNo ratings yet
- Relining and Rebasing The Removable Partial Denture: Chapter OutlineDocument6 pagesRelining and Rebasing The Removable Partial Denture: Chapter Outlineمازن كريم حمود سلطانNo ratings yet
- Useof International Caries Detectionand Assessment Systemina National Health ServiceDocument9 pagesUseof International Caries Detectionand Assessment Systemina National Health Serviceأمال داودNo ratings yet
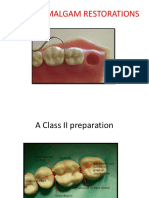
- Cde-Class II Amalgam Restorations-31!12!14Document36 pagesCde-Class II Amalgam Restorations-31!12!14Archita KureelNo ratings yet
- Imaging in Forensic DentistryDocument42 pagesImaging in Forensic DentistryAME DENTAL COLLEGE RAICHUR, KARNATAKANo ratings yet
- Ponnusamy 2020Document11 pagesPonnusamy 2020Shankar arumugamNo ratings yet
- Kelompok Kelompok Penyakit Gigi Dan MulutDocument2 pagesKelompok Kelompok Penyakit Gigi Dan MulutHammam FaizNo ratings yet
- Chapter 48Document40 pagesChapter 48serhunaNo ratings yet
- Classification of Dental Models and Bite Adjustment1Document4 pagesClassification of Dental Models and Bite Adjustment1JamestorsNo ratings yet
- Xrays Spanish PDFDocument2 pagesXrays Spanish PDFcalbancNo ratings yet
- Permanent CaninesDocument4 pagesPermanent CaninesAmmar AwadNo ratings yet
- 8.review Meenu Mary PaulDocument10 pages8.review Meenu Mary PaulDilmohit SinghNo ratings yet