Professional Documents
Culture Documents
Approved IFCC Recommendation On Reporting Results For Blood Glucose
Uploaded by
Pham PhongOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Approved IFCC Recommendation On Reporting Results For Blood Glucose
Uploaded by
Pham PhongCopyright:
Available Formats
Clinical Chemistry 51:9
15731576 (2005)
Special Report
Approved IFCC Recommendation on Reporting
Results for Blood Glucose (Abbreviated)
Paul DOrazio,1 Robert W. Burnett,2 Niels Fogh-Andersen,3* Ellis Jacobs,4
Katsuhiko Kuwa,5 Wolf R. Kulpmann,6 Lasse Larsson,7 Andrzej Lewenstam,8
Anton H.J. Maas,9 Gerhard Mager,10 Jerzy W. Naskalski,11 and
Anthony O. Okorodudu12; the International Federation of Clinical Chemistry
Scientific Division Working Group on Selective Electrodes and
Point of Care Testing
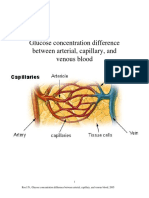
In current clinical practice, plasma and blood glucose
are used interchangeably with a consequent risk of
clinical misinterpretation. In human blood, glucose, like
water, is distributed between erythrocytes and plasma.
The molality of glucose (amount of glucose per unit of
water mass) is the same throughout the sample, but the
concentration is higher in plasma because the concentration of water and, therefore, glucose is higher in
plasma than in erythrocytes. Different devices for the
measurement of glucose may detect and report fundamentally different quantities. Different water concentrations in calibrators, plasma, and erythrocyte fluid can
explain some of the differences. Results of glucose
measurements depend on sample type and on whether
methods require sample dilution or use biosensors in
undiluted samples. If the results are mixed up or used
indiscriminately, the differences may exceed the maximum allowable error of glucose determinations for
diagnosing and monitoring diabetes mellitus, and com-
Instrumetation Laboratory, Lexington, MA.
Hartford Hospital, Hartford, CT.
3
Herlev Hospital, Herlev, Denmark.
4
Wadsworth Center, Albany, NY.
5
University of Tsukuba, Tsukuba, Japan.
6
Medizinizche Hochschule, Hannover, Germany.
7
Univeristy of Linkoping, Linkoping, Sweden.
8
bo Akademi University, bo-Turku, Finland.
9
Department of Cardiology, Isala Klinieken, Zwolle, The Netherlands.
10
Fresenius, Bad Homburg, Germany.
11
Jagiellonian University, Krakow, Poland.
12
Department of Pathology, University of Texas Medical Branch,
Galveston, TX.
*Address correspondence to this author at: Department of Clinical
Biochemistry, Herlev Hospital, DK-2730 Herlev, Denmark. E-mail nifa@
herlevhosp.kbhamt.dk.
Received April 4, 2005; accepted June 6, 2005.
Previously published online at DOI: 10.1373/clinchem.2005.051979
2
plicate the treatment. The goal of the IFCC Scientific
Division Working Group on Selective Electrodes and
Point of Care Testing (IFCC-SD, WG-SEPOCT) is to
reach a global consensus on reporting results. The
document recommends reporting the concentration of
glucose in plasma (with the unit mmol/L), irrespective
of sample type or measurement technique. A constant
factor of 1.11 is used to convert concentration in whole
blood to the equivalent concentration in the pertinent
plasma. The conversion will provide harmonized results, facilitating the classification and care of patients
and leading to fewer therapeutic misjudgments.
2005 American Association for Clinical Chemistry
The WHO and the American Diabetes Association (ADA)
define the diagnosis of diabetes mellitus by at least 2
measurements of fasting plasma glucose concentration
7.0 mmol/L. As an alternative, a random venous
plasma glucose concentration 11.1 mmol/L in the presence of symptoms or a 2-h post-oral glucose tolerance test
result 11.1 mmol/L suffice to make a definite diagnosis
of diabetes mellitus (1, 2 ). The new classifications of
impaired fasting glucose have narrower intervals [6.1
6.9 mmol/L (WHO) or 5.6 6.9 mmol/L (ADA)] for venous plasma glucose concentration than the previous
fasting interval (5.6 7.7 mmol/L) for classifying normoglycemia and diabetes (3 ). The narrower diagnostic limits
increase the need for reliable results to classify individuals
correctly.
Currently, various types of instruments detect and
report fundamentally different glucose quantities. Biosensors for glucose are direct reading when they measure
glucose directly, i.e., without previous dilution of the
sample. The new generation of direct-reading glucose
sensors responds to the molality of glucose, which is
identical in whole blood and plasma, whereas the glucose
1573
1574
DOrazio et al.: IFCC Recommendation on Reporting Blood Glucose Results
concentrations in these two systems are different. Methods requiring high sample dilution will produce results
equivalent to concentration when calibrated against aqueous standards because the water concentrations in the
sample and calibrator are almost identical after dilution.
The original intention of the IFCC Scientific Division
Working Group on Selective Electrodes and Point of Care
Testing (IFCC-SD WGSE) was to make a recommendation
for direct-reading biosensors in blood gas/electrolyte/
metabolite analyzers. However, an isolated recommendation would be meaningless and not lead to the goal of
harmonized results, which requires a consensus on reporting results for all analyzers. Inexpensive instruments
with direct-reading biosensors are available for self-monitoring or point-of-care testing of glucose (4 6 ). The
clinical chemistry laboratory is expected to perform glucose determinations by direct-reading sensors concurrently with other routine instruments that measure substance concentration in diluted samples.
In current clinical practice, plasma and blood glucose
are used interchangeably (7 ) with a consequent risk of
misinterpretation. The two systems are frequently mistaken in the clinical literature, despite an average 11%
difference in glucose concentration (plasma blood). The
ADA provides clinical decision limits for the concentration of glucose in venous plasma, but the WHO in
addition provides the concentration of glucose in whole
blood (13 ).
With the present use of multiple methods providing
results of different quantities, there is a serious risk of
clinical misinterpretation. For example, some blood gas/
electrolyte/metabolite instruments with direct-reading
glucose biosensors are calibrated with aqueous calibrators
to provide results according to the relative molality of
glucose in the sample. The predicted ratios of results
obtained by such instruments to the results obtained by
instruments that analyze diluted specimens are
1.18 (0.99/0.84) for normal whole blood and 1.06 (0.99/
0.93) for normal plasma, in agreement with results from
the literature (8, 9 ).
We recommend a constant factor of 1.11 for conversion
between the glucose concentration in blood and the
equivalent concentration in the pertinent plasma and
reporting of only the glucose concentration in plasma to
avoid misjudgments. The converted result equals the
concentration of glucose in plasma when the hematocrit
and water concentrations are normal. The recommendation includes point-of-care devices and methods that
measure the concentration of glucose in whole blood. The
conversion does not eliminate current preanalytical influences or hematocrit effects, which are specific to certain
methods [see the summary by Chance et al. (4 )]. However, the conversion will provide consistent harmonized
results, facilitating the classification and care of patients
and leading to fewer therapeutic misjudgments.
Activity and Molality of Glucose
Biosensors respond to activity of the pertinent analyte.
The activity of glucose is assumed equal to molality, with
a molal activity coefficient equal to 1. Activity is physiologically relevant for determining enzymatic reaction
rates, direction of chemical processes, transport, and
binding to receptors. Glucose permeates the erythrocyte
membrane quickly via passive transport (facilitated by the
erythrocyte glucose transporter); therefore, the molality of
glucose (amount of glucose per unit mass of water) is
identical in erythrocytes and plasma. Results obtained by
a direct-reading glucose biosensor responding to molality
are identical for whole blood and its separated plasma.
The converted results based on measured glucose
activity and the average concentration of water in normal
plasma are called the active concentration of glucose in
normal plasma to distinguish them from the substance
concentration of glucose in actual plasma. We recommend
converting and reporting results from all systems and
devices using direct-reading glucose biosensors as the
active concentration of glucose in normal plasma (10, 11 )
and using the unit mmol/L. The converted results of
direct-reading glucose biosensors are proportional to the
activity and molality of glucose (contrary to the less
physiologic substance concentration of glucose) because
of the constant factor relationship. The advantage of
direct-reading glucose biosensors responding to activity
and molality is maintained. The ratio between the active
and conventional concentrations of glucose in a given
plasma sample equals the ratio of the average plasma
water concentration to the actual plasma water concentration (with a mean of 1.00 and SD of 0.01 if the water
concentration is normal). In practice, the two can be
considered identical. Subgroups such as neonates or pregnant women may have slightly higher than average
plasma water concentrations. A lower-than-average actual plasma water concentration attributable to, e.g., hyperlipidemia will lead to a lower conventionally used
substance concentration but has no impact on the active
concentration of glucose. The active concentration of
glucose is unaffected by changes in water concentration,
but the conventionally used concentration will change in
proportion to the water concentration.
For the same reason, control materials with assigned
glucose concentrations must have a normal water concentration of 0.93 kg/L to be valid for quality assessment of
direct-reading glucose biosensors. Otherwise, the water
concentration must be taken into account.
Concentration of Glucose
Most current photometric methods to measure glucose
use enzymatic conversion with NADH or NADPH as
coenzymes and absorbance measurements near or at 340
nm. The molar absorptivity permits direct calculation of
the glucose concentration after complete reaction.
The concentration can also be determined by a kinetic
measurement, comparing sample to a calibrator. A kinetic
1575
Clinical Chemistry 51, No. 9, 2005
measurement obviates subtraction of background, at the
cost of introducing a small positive bias. Enzymatic reaction rates depend on substrate activity (or molality). The
slightly lower water concentration in a diluted sample
compared with a diluted calibrator provides a relatively
(slightly) higher enzymatic reaction rate in the diluted
sample. Methods that include protein precipitation also
have a positive bias, depending on the degree of dilution
and concentration of protein. Despite these (minor) theoretical queries, routine clinical chemical analyzers measure glucose concentration (amount of glucose per volume of sample) with sufficient trueness and precision.
Biosensors that require dilution provide results that
closely resemble concentration. These devices report concentration based on the concentration of glucose in the
calibrator.
Plasma and whole-blood glucose concentrations are
not interchangeable because of the difference in glucose
concentrations between plasma and whole blood (in contrast to current practice in many institutions). Different
reference intervals and clinical decision limits apply. The
recommendation here is to report only the concentration
of glucose in plasma, irrespective of material investigated.
Glucose and water distribute freely between erythrocytes
and plasma; therefore, the molality (but not the concentration) of glucose is identical in erythrocytes and plasma.
Because erythrocytes have a lower water concentration
than plasma, the concentration of glucose in whole blood
is lower than in plasma for a given concentration of
glucose in plasma. The concentration of glucose in plasma
is independent of hematocrit. Another reason for choosing plasma rather than whole blood as the system of
reference is the relationship between glucose activity and
concentration. Glucose activity and concentration are
practically proportional in plasma, where the water concentration varies relatively little, but not in whole blood,
where hematocrit may vary considerably and confound
the relationship. The concentration of glucose in plasma
(rather than the concentration in whole blood) therefore
more closely reflects the activity of glucose. For most
purposes, the concentration of glucose in plasma is physiologically more relevant to measure and report than the
concentration in whole blood.
Serum should not be used because the glucose concentration decreases 0.6 mmol L1 h1 as a result of
glycolysis during its preparation (12 ). Likewise, the concentration of glucose in capillary whole blood should not
be used as a substitute for the concentration in venous
plasma (13 ).
The system of reference and type of specimen have not
always received the attention they deserve. The ADA
recommends for self-monitoring a maximum allowable
CV of 10% at glucose concentrations of 1.722 mmol/L
and a maximum bias of 15% from a reference method
value (14, 15 ). In other words, the ADA accepts no more
than 5% analytical error for self-monitoring of blood
glucose (14 ). The recently proposed quality criteria for
Fig. 1. Conversion factors for different glucose quantities.
laboratory analysis of The National Academy of Clinical
Biochemistry (NACB) (12 ), based on intraindividual biological variation (16 ), are even more demanding. The
maximum allowable imprecision (CV) according to the
NACB Laboratory Medicine Practice Guideline is 3.3%,
the maximum bias is 2.5%, and the maximum total error
(difference from the true value) is 7.9%. The systematic
11% difference between normal blood and plasma already
exceeds the recommended allowable maximum error.
Mistaking or not properly distinguishing sample type
may lead to misinterpreting the result and a wrong
diagnosis. According to an editorial on the subject (17 ),
reporting whole-blood glucose values is anachronistic
and comparable to reporting the whole-blood rather than
the plasma concentration of potassium. Manufacturers
and clinical chemists always should report the concentration of glucose in plasma to avoid this risk, irrespective of
sample type and method of measurement.
The present IFCC document recommends using a
constant factor of 1.11 (Fig. 1) for converting glucose
concentration, based on water concentrations of normal
whole blood and of normal plasma. The relationship has
been supported experimentally (8, 9 ). Conversion based
on measured hematocrit may introduce additional error
(9 ), in addition to being less convenient and requiring
additional information. Converted (whole blood 3
plasma) glucose concentrations have the same dependence on hematocrit as the currently reported wholeblood glucose concentrations (18 ). With this recommendation, all results can be harmonized and reported as the
concentration of glucose in plasma. The laboratory, however, must keep information about which sample type
and measurement procedure were used.
References
1. World Health Organization. Definition, diagnosis and classification
of diabetes mellitus and its complications: report of a WHO
consultation. Part 1: diagnosis and classification of diabetes
mellitus. Geneva: World Health Organization, 1999.
1576
DOrazio et al.: IFCC Recommendation on Reporting Blood Glucose Results
2. American Diabetes Association. Standards of medical care in
diabetes. Diabetes Care 2005;28(Suppl 1):S4 36.
3. Diabetes mellitus. Report of a WHO Study Group, World Health
Organization Expert Committee. Tech Report Ser 727. Geneva,
Switzerland: WHO, 1985.
4. Chance JF, Li DJ, Jones KA, Dyer KL, Nichols JH. Technical
evaluation of five glucose meters with data management capabilities. Am J Clin Pathol 1999;111:54756.
5. Johnson RN, Baker JR. Accuracy of devices used for self-monitoring of blood glucose. Ann Clin Biochem 1998;35:68 74.
6. Kost GJ, Vu HT, Lee JH, Bourgeois P, Kiechle FL, Martin C, et al.
Multicenter study of oxygen-insensitive handheld glucose point-ofcare testing in critical care/hospital/ambulatory patients in the
United States and Canada. Crit Care Med 1998;26:5819.
7. Burrin JM, Alberti KGMM. What is blood glucose: can it be
measured? Diabetic Med 1990;7:199 206.
8. Fogh-Andersen N, Wimberley PD, Thode J, Siggaard-Andersen O.
Direct reading glucose electrodes detect the molality of glucose in
plasma and whole blood. Clin Chim Acta 1990;189:33 8.
9. Fogh-Andersen N, DOrazio P. Proposal for standardizing directreading biosensors for blood glucose. Clin Chem 1998;44:6559.
10. Siggaard-Andersen O, Durst RA, Maas AHJ. International Federation of Clinical Chemistry, Scientific committee, analytical section:
and approved recommendation (1984) on physico-chemical quantities and units in clinical chemistry with special emphasis on
activities and activity coefficients. J Clin Chem Clin Biochem
1987;25:369 91.
11. Siggaard-Andersen O, Durst RA, Maas AHJ. International Federation of Clinical Chemistry, Scientific committee, analytical section:
and approved recommendation (1984) on physico-chemical quantities and units in clinical chemistry with special emphasis on
activities and activity coefficients. Ann Biol Clin 1987;45:89
109.
12. Sacks DB, Bruns DE, Goldstein DE, Maclaren NK, McDonald JM,
Parrott M. Guidelines and recommendations for laboratory analysis in the diagnosis and management of diabetes mellitus. Clin
Chem 2002;48:436 72.
13. Stahl M, Brandslund I, Jorgensen LG, Hyltoft Petersen P, BorchJohnsen K, de Fine Olivarius N. Can capillary whole blood glucose
and venous plasma glucose measurements be used interchangeably in diagnosis of diabetes mellitus? Scand J Clin Lab Invest
2002;62:59 66.
14. American Diabetes Association. Consensus statement: self monitoring of blood glucose. Diabetes Care 1990;13(Suppl 1):41 6.
15. American Diabetes Association. Self-monitoring of blood glucose.
Diabetes Care 1994;17:81 6.
16. Ricos C, Alvarez V, Cava F, Garcia-Lario JV, Hernandes A, Jimenez
CV, et al. Current databases on biological variation: pros, cons
and progress. Scand J Clin Lab Invest 1999;59:491500.
17. Rainey PM, Jatlow P. Monitoring blood glucose meters [Editorial].
Am J Clin Pathol 1995;103:125 6.
18. Fogh-Andersen N. Evaluation of HemoCue glucose meter (201)
converting B-glucose to P-glucose. Point of Care 2004;3:1725.
You might also like
- p1541 - Vol 84 - 9 PDFDocument5 pagesp1541 - Vol 84 - 9 PDFmresearchNo ratings yet
- Complementary and Alternative Medical Lab Testing Part 6: Liver and GallbladderFrom EverandComplementary and Alternative Medical Lab Testing Part 6: Liver and GallbladderNo ratings yet
- Pmls ArticleDocument8 pagesPmls ArticleEd dela PenaNo ratings yet
- Blood Glucose Determination - Plasma or SerumDocument4 pagesBlood Glucose Determination - Plasma or SerumJamesNo ratings yet
- Glucose Lab ReportDocument12 pagesGlucose Lab ReportKing Everest86% (7)
- An Evaluation of The Accuracy of A Flash Glucose Monitoring System in Children With Diabetes in Comparison With Venous Blood GlucoseDocument8 pagesAn Evaluation of The Accuracy of A Flash Glucose Monitoring System in Children With Diabetes in Comparison With Venous Blood GlucosesovalaxNo ratings yet
- Original Article: Measurement of Blood Glucose: Comparison Between Different Types of SpecimensDocument10 pagesOriginal Article: Measurement of Blood Glucose: Comparison Between Different Types of SpecimenstampskebaNo ratings yet
- Comparison of The Accuracy of The Hemocue Glucose Analyzer With The Yellow Springs Instrument Glucose Oxidase Analyzer, Particularly in HypoglycemiaDocument7 pagesComparison of The Accuracy of The Hemocue Glucose Analyzer With The Yellow Springs Instrument Glucose Oxidase Analyzer, Particularly in HypoglycemiaSeven NightNo ratings yet
- Introduction: Diabetes Mellitus (DM) Is The Most Common Endocrine ProblemDocument6 pagesIntroduction: Diabetes Mellitus (DM) Is The Most Common Endocrine ProblemHeribertus Andi WidagdoNo ratings yet
- Glycemic Variability in The Use of Point-of-Care Glucose MetersDocument6 pagesGlycemic Variability in The Use of Point-of-Care Glucose MetersCifha Rajesh SaldhanhaNo ratings yet
- tmp7639 TMPDocument6 pagestmp7639 TMPFrontiersNo ratings yet
- 290-Article Text-929-1-10-20191031Document6 pages290-Article Text-929-1-10-20191031Nurul Nadia HamdanNo ratings yet
- Effects of Total Plasma Protein ConcentrDocument4 pagesEffects of Total Plasma Protein ConcentrThuy NguyenNo ratings yet
- Anion GapDocument13 pagesAnion GapLuis Gerardo Alcalá GonzálezNo ratings yet
- Newsletter10-1 SebiaDocument4 pagesNewsletter10-1 SebiaNidiam2100% (1)
- The Association Between Estimated Average Glucose Levels and Fasting Plasma Glucose LevelsDocument4 pagesThe Association Between Estimated Average Glucose Levels and Fasting Plasma Glucose LevelsRina MachdalenaNo ratings yet
- Validation of A Glucose Meter at An Intensive Care UnitDocument7 pagesValidation of A Glucose Meter at An Intensive Care UnitRodas GetachewNo ratings yet
- Effect of The Different Assays of Hba1C On Diabetic Patients MonitoringDocument4 pagesEffect of The Different Assays of Hba1C On Diabetic Patients MonitoringAndi Raodah ImranNo ratings yet
- A Review - Qualitative and Quantitative Analysis of Antimalarial Drugs and Their Metabolites in Body FluidsDocument10 pagesA Review - Qualitative and Quantitative Analysis of Antimalarial Drugs and Their Metabolites in Body FluidsRavi ShankarNo ratings yet
- 1 s2.0 S1262363613000219 MainDocument7 pages1 s2.0 S1262363613000219 MainfghfghfNo ratings yet
- Molecular Adsorbent Recirculating System and Single-Pass Albumin Dialysis in Liver Failure - A Prospective, Randomised Crossover StudyDocument13 pagesMolecular Adsorbent Recirculating System and Single-Pass Albumin Dialysis in Liver Failure - A Prospective, Randomised Crossover StudyRicardo RodriguezNo ratings yet
- Lane 2015Document6 pagesLane 2015Andres Vásquez ChNo ratings yet
- Relationship Between Serum and Saliva Chloramphenicol ConcentrationsDocument4 pagesRelationship Between Serum and Saliva Chloramphenicol Concentrationsmonarch01No ratings yet
- HbA1C Direct Reagent KitDocument1 pageHbA1C Direct Reagent KitSamar Sharaf50% (2)
- Use of A Blood Gas Analyzer and A Laboratory Autoanalyzer in Routine Practice To Measure Electrolytes in Intensive Care Unit PatientsDocument7 pagesUse of A Blood Gas Analyzer and A Laboratory Autoanalyzer in Routine Practice To Measure Electrolytes in Intensive Care Unit PatientsZheng GuNo ratings yet
- (Q1) Pone.0169593Document16 pages(Q1) Pone.0169593wiradewi lestariNo ratings yet
- IFCC HbA1Document9 pagesIFCC HbA1msaidsaidyoussefNo ratings yet
- Relationship Between Levels of Fasting Blood Glucose and Hba1C in Prediabetes PatientsDocument4 pagesRelationship Between Levels of Fasting Blood Glucose and Hba1C in Prediabetes Patientsمحمد رحيم حسن محمودNo ratings yet
- Hemolysis of Blood Samples Has No Significant Impact On The Results of Pharmacokinetic DataDocument4 pagesHemolysis of Blood Samples Has No Significant Impact On The Results of Pharmacokinetic DataDiego OrtechoNo ratings yet
- Berk Ow 2013Document10 pagesBerk Ow 2013langit rizki yuditamaNo ratings yet
- The Accuracy of Serum Osmolarity Calculation in Small Children Ta Nost Izra Unavanja Serumskog Osmolariteta U Male DeceDocument11 pagesThe Accuracy of Serum Osmolarity Calculation in Small Children Ta Nost Izra Unavanja Serumskog Osmolariteta U Male DeceMilica AdzibabaNo ratings yet
- Standards of Medical Care in Diabetesd2021: 6. Glycemic TargetsDocument12 pagesStandards of Medical Care in Diabetesd2021: 6. Glycemic TargetsFajar NugrahantoNo ratings yet
- Tauk 2015Document7 pagesTauk 2015Andres Vásquez ChNo ratings yet
- The Role Of Hba1C Testing In Diagnosing Diabetes: 종 설 (Review)Document5 pagesThe Role Of Hba1C Testing In Diagnosing Diabetes: 종 설 (Review)Choi WonNo ratings yet
- Roe Glucose Conc in Different Blood Compartments 2005Document18 pagesRoe Glucose Conc in Different Blood Compartments 2005jeffnroe1No ratings yet
- 2010-Fasting For Haematological TestDocument6 pages2010-Fasting For Haematological Testpedro vargasNo ratings yet
- Glu KosaDocument6 pagesGlu Kosajulianprist777No ratings yet
- The Impact of Delayed Analysis On Glucose Levels of Blood SamplesDocument4 pagesThe Impact of Delayed Analysis On Glucose Levels of Blood SamplesInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Clinical Validation and Implications of Dried Blood SpotDocument8 pagesClinical Validation and Implications of Dried Blood SpotGhufranNo ratings yet
- Carbohydrates: Disease Compilation: Submitted ToDocument33 pagesCarbohydrates: Disease Compilation: Submitted ToTob MoradosNo ratings yet
- Lactate MonitoringDocument6 pagesLactate Monitoringaliv8s3624No ratings yet
- Jurnal LisinoprilDocument7 pagesJurnal LisinoprildidiisafitriNo ratings yet
- Hemoglobine A1cDocument7 pagesHemoglobine A1chector_mijanNo ratings yet
- Non-Invasive Blood Glucose Level Measurement From LASER Reflected Spectral Patterns ImagesDocument5 pagesNon-Invasive Blood Glucose Level Measurement From LASER Reflected Spectral Patterns ImagesIOSRJEN : hard copy, certificates, Call for Papers 2013, publishing of journalNo ratings yet
- Diabetic Post Mortem PDFDocument7 pagesDiabetic Post Mortem PDFPrakarsa Adi Daya NusantaraNo ratings yet
- Lab 9 (Biochemical Test) - Edited PDFDocument2 pagesLab 9 (Biochemical Test) - Edited PDFrzhrsNo ratings yet
- 110 320 1 PB PDFDocument10 pages110 320 1 PB PDFMirna AisyahNo ratings yet
- 110 320 1 PB PDFDocument10 pages110 320 1 PB PDFMirna AisyahNo ratings yet
- Lipemia: Causes, Interference Mechanisms, Detection and ManagementDocument16 pagesLipemia: Causes, Interference Mechanisms, Detection and ManagementkartikaparamitaNo ratings yet
- Verification of A Novel Point-Of-Care HbA1c DeviceDocument9 pagesVerification of A Novel Point-Of-Care HbA1c DeviceОксана КожокаруNo ratings yet
- Differences Between Human Plasma and Serum Metabolite ProfilesDocument6 pagesDifferences Between Human Plasma and Serum Metabolite ProfilesjoaquimmendesNo ratings yet
- BİOLABDocument3 pagesBİOLABmalaver528No ratings yet
- HbA1c: Past, Present and Future Units for Measuring Average Blood GlucoseDocument6 pagesHbA1c: Past, Present and Future Units for Measuring Average Blood GlucoseArjunaPamungkasNo ratings yet
- Hba1c StandarizaciónDocument13 pagesHba1c StandarizaciónAsesoria TecnicaNo ratings yet
- AM (179) Glu PDFDocument4 pagesAM (179) Glu PDFIftikhar AliNo ratings yet
- Amj-Hiponatremia Corregida Por Hiperglicemia-1999Document5 pagesAmj-Hiponatremia Corregida Por Hiperglicemia-1999Mayra Alejandra Prada SerranoNo ratings yet
- Translating The A1C Assay Into Estimated Average Glucose ValuesDocument6 pagesTranslating The A1C Assay Into Estimated Average Glucose ValuesFaryalBalochNo ratings yet
- Diabetes Care Glucosa Promedio EstimadaDocument6 pagesDiabetes Care Glucosa Promedio EstimadaGemeneza GonzalesNo ratings yet
- FPG HbaicDocument9 pagesFPG Hbaicanon_235643778No ratings yet
- SA Health Cleaning Standard 2014 - (v1.1) CDCB Ics 20180301 PDFDocument48 pagesSA Health Cleaning Standard 2014 - (v1.1) CDCB Ics 20180301 PDFPham PhongNo ratings yet
- GuitarTechniques Page 14 PDFDocument1 pageGuitarTechniques Page 14 PDFPham PhongNo ratings yet
- Healthcare To VietnamDocument5 pagesHealthcare To VietnamPham PhongNo ratings yet
- JAHR 2014 Medical Annual Report of Viet NamDocument317 pagesJAHR 2014 Medical Annual Report of Viet NamPham PhongNo ratings yet
- 2007 Michigan Health Care Facility Design StandardsDocument150 pages2007 Michigan Health Care Facility Design StandardsMohamed MasryNo ratings yet
- Critical CharacteristicsDocument3 pagesCritical CharacteristicsPham PhongNo ratings yet
- GuitarTechniques Page 14 PDFDocument1 pageGuitarTechniques Page 14 PDFPham PhongNo ratings yet
- Ref-Agent Based BPMDocument26 pagesRef-Agent Based BPMPham PhongNo ratings yet
- PESTEL of VietnamDocument18 pagesPESTEL of VietnamPham Phong100% (1)
- Process MappingDocument4 pagesProcess MappingPham PhongNo ratings yet
- Neurofax EEG 9200K BrochureDocument10 pagesNeurofax EEG 9200K BrochurePham PhongNo ratings yet
- Healthcare To VietnamDocument5 pagesHealthcare To VietnamPham PhongNo ratings yet
- Nidek SL 450 BrochureDocument2 pagesNidek SL 450 BrochurePham Phong0% (1)
- Organize System HealthcareDocument167 pagesOrganize System HealthcarePranav JainNo ratings yet
- Methemoglobin - It's Not Just BlueDocument11 pagesMethemoglobin - It's Not Just BluePham PhongNo ratings yet
- Timeliness As A Quality Attribute and StrategyDocument5 pagesTimeliness As A Quality Attribute and StrategyPham PhongNo ratings yet
- Scala GeneralDocument34 pagesScala GeneralPham PhongNo ratings yet
- Materials Management in Voluntary HospitalsDocument20 pagesMaterials Management in Voluntary HospitalsPham PhongNo ratings yet
- Lemon Tree BassDocument6 pagesLemon Tree BassPham PhongNo ratings yet
- AABB Billing Guide For Blood Products and Related Services: July 2020 1Document45 pagesAABB Billing Guide For Blood Products and Related Services: July 2020 1Rija KhanNo ratings yet
- Chiropractic Treatment Techniques-2016Document9 pagesChiropractic Treatment Techniques-2016Dr. Mateen ShaikhNo ratings yet
- CU DFScience Notes Bacteria General Dairy Micro 06 10 PDFDocument10 pagesCU DFScience Notes Bacteria General Dairy Micro 06 10 PDFjoel osortoNo ratings yet
- Foodborne IllnessDocument2 pagesFoodborne IllnessBjorni VaniNo ratings yet
- Folk Biology and The Anthropology of Science Cognitive Universals and Cultural ParticularsDocument63 pagesFolk Biology and The Anthropology of Science Cognitive Universals and Cultural ParticularsGaby ArguedasNo ratings yet
- 2023 Summit Program Draft 5 Apr18Document43 pages2023 Summit Program Draft 5 Apr18Raheem KassamNo ratings yet
- Nursing Care Plan Neonatal PneumoniaDocument2 pagesNursing Care Plan Neonatal Pneumoniaderic93% (41)
- Genetics of Mitochondrial Disease: Russell P. SanetoDocument54 pagesGenetics of Mitochondrial Disease: Russell P. SanetoGréta BotyánszkiNo ratings yet
- Arthur Adolphus Lindsay - Mind The Transformer The New Psychology Complete (1911)Document172 pagesArthur Adolphus Lindsay - Mind The Transformer The New Psychology Complete (1911)truepotentialzNo ratings yet
- Hiv Awareness Project ProposalDocument17 pagesHiv Awareness Project ProposalPrincess Gesa Macula100% (1)
- 4446 16364 1 PBDocument8 pages4446 16364 1 PBSafira Rosyadatul AissyNo ratings yet
- Case Scenario: Self-Risk AssessmentDocument2 pagesCase Scenario: Self-Risk AssessmentAlyanna Alcazar CapateNo ratings yet
- Angina Pectoris: Dr. Naitik D Trivedi & Dr. Upama N. TrivediDocument15 pagesAngina Pectoris: Dr. Naitik D Trivedi & Dr. Upama N. TrivediNaveen KumarNo ratings yet
- BL42-Chi Nei Tsang III (ID-PDF) 12-17-15 PDFDocument90 pagesBL42-Chi Nei Tsang III (ID-PDF) 12-17-15 PDFJosé Tao75% (8)
- MCQ (Endocrine)Document7 pagesMCQ (Endocrine)aminata680% (5)
- Basic Life Support Field GuideDocument56 pagesBasic Life Support Field GuidelmaoheartsNo ratings yet
- 1.A Ndera CaseDocument13 pages1.A Ndera CaseNsengimana Eric MaxigyNo ratings yet
- GEHC Brochure Senographe CareDocument7 pagesGEHC Brochure Senographe CareVremedSoluCionesNo ratings yet
- Laser: DR Uzair Ahmad Qureshi Consultant Dermatologist, STDS, Laser and Aesthetic SpecialistDocument18 pagesLaser: DR Uzair Ahmad Qureshi Consultant Dermatologist, STDS, Laser and Aesthetic SpecialistFakhra TehseenNo ratings yet
- Daftar Pustaka HipertensiDocument43 pagesDaftar Pustaka HipertensiFeni Nurmia PutriNo ratings yet
- Barangay Anti-Smoking OrdinanceDocument4 pagesBarangay Anti-Smoking Ordinancejacquelyn samson100% (1)
- Epstein Barr VirusDocument13 pagesEpstein Barr VirusDianaLorenaNo ratings yet
- Pornography Statistics: 250+ Facts, Quotes, and Statistics About Pornography Use (2013 Edition)Document33 pagesPornography Statistics: 250+ Facts, Quotes, and Statistics About Pornography Use (2013 Edition)Zinc MarquezNo ratings yet
- Embryonic Development and OrganogenesisDocument33 pagesEmbryonic Development and OrganogenesisMariam QaisNo ratings yet
- Module 2 - Community Health NursingDocument9 pagesModule 2 - Community Health NursingMarie Kelsey Acena Macaraig100% (1)
- PATH-365 Objective @agrounderDocument13 pagesPATH-365 Objective @agrounderNalini PathakeNo ratings yet
- 5388 Tech ManualDocument198 pages5388 Tech ManualMichal SzymanskiNo ratings yet
- MNT For Sucrase Isomaltase DeficiencyDocument14 pagesMNT For Sucrase Isomaltase DeficiencySarah DresselNo ratings yet
- Blastomycosis: Narendra Shanmugam Group 22Document17 pagesBlastomycosis: Narendra Shanmugam Group 22Naren ShanNo ratings yet
- Diabetes Mellitus: DefinitionDocument95 pagesDiabetes Mellitus: DefinitionMalik Rizwan ElahiNo ratings yet
- Is That a Fact?: Frauds, Quacks, and the Real Science of Everyday LifeFrom EverandIs That a Fact?: Frauds, Quacks, and the Real Science of Everyday LifeRating: 4.5 out of 5 stars4.5/5 (3)
- Stuff Matters: Exploring the Marvelous Materials That Shape Our Man-Made WorldFrom EverandStuff Matters: Exploring the Marvelous Materials That Shape Our Man-Made WorldRating: 4 out of 5 stars4/5 (289)
- Chemistry for Breakfast: The Amazing Science of Everyday LifeFrom EverandChemistry for Breakfast: The Amazing Science of Everyday LifeRating: 4.5 out of 5 stars4.5/5 (14)
- Guidelines for Asset Integrity ManagementFrom EverandGuidelines for Asset Integrity ManagementRating: 5 out of 5 stars5/5 (1)
- Monkeys, Myths, and Molecules: Separating Fact from Fiction in the Science of Everyday LifeFrom EverandMonkeys, Myths, and Molecules: Separating Fact from Fiction in the Science of Everyday LifeRating: 4 out of 5 stars4/5 (9)
- The Disappearing Spoon: And Other True Tales of Madness, Love, and the History of the World from the Periodic Table of the ElementsFrom EverandThe Disappearing Spoon: And Other True Tales of Madness, Love, and the History of the World from the Periodic Table of the ElementsRating: 4 out of 5 stars4/5 (146)
- Science Goes Viral: Captivating Accounts of Science in Everyday LifeFrom EverandScience Goes Viral: Captivating Accounts of Science in Everyday LifeRating: 5 out of 5 stars5/5 (1)
- Coating and Drying Defects: Troubleshooting Operating ProblemsFrom EverandCoating and Drying Defects: Troubleshooting Operating ProblemsRating: 5 out of 5 stars5/5 (1)
- Organic Chemistry for Schools: Advanced Level and Senior High SchoolFrom EverandOrganic Chemistry for Schools: Advanced Level and Senior High SchoolNo ratings yet
- An Introduction to the Periodic Table of Elements : Chemistry Textbook Grade 8 | Children's Chemistry BooksFrom EverandAn Introduction to the Periodic Table of Elements : Chemistry Textbook Grade 8 | Children's Chemistry BooksRating: 5 out of 5 stars5/5 (1)
- Guidelines for Defining Process Safety Competency RequirementsFrom EverandGuidelines for Defining Process Safety Competency RequirementsRating: 3 out of 5 stars3/5 (1)
- Napoleon's Buttons: 17 Molecules That Changed HistoryFrom EverandNapoleon's Buttons: 17 Molecules That Changed HistoryRating: 4 out of 5 stars4/5 (25)
- The Regenerative Grower's Guide to Garden Amendments: Using Locally Sourced Materials to Make Mineral and Biological Extracts and FermentsFrom EverandThe Regenerative Grower's Guide to Garden Amendments: Using Locally Sourced Materials to Make Mineral and Biological Extracts and FermentsRating: 5 out of 5 stars5/5 (3)
- Essential Oil Chemistry Formulating Essential Oil Blends that Heal - Aldehyde - Ketone - Lactone: Healing with Essential OilFrom EverandEssential Oil Chemistry Formulating Essential Oil Blends that Heal - Aldehyde - Ketone - Lactone: Healing with Essential OilRating: 5 out of 5 stars5/5 (1)
- It's Elemental: The Hidden Chemistry in EverythingFrom EverandIt's Elemental: The Hidden Chemistry in EverythingRating: 4 out of 5 stars4/5 (10)
- Meltdown: Nuclear disaster and the human cost of going criticalFrom EverandMeltdown: Nuclear disaster and the human cost of going criticalRating: 5 out of 5 stars5/5 (5)
- Chemical Elements Pocket Guide: Detailed Summary of the Periodic TableFrom EverandChemical Elements Pocket Guide: Detailed Summary of the Periodic TableNo ratings yet
- Chemistry: a QuickStudy Laminated Reference GuideFrom EverandChemistry: a QuickStudy Laminated Reference GuideRating: 5 out of 5 stars5/5 (1)
- The Periodic Table: A Very Short IntroductionFrom EverandThe Periodic Table: A Very Short IntroductionRating: 4.5 out of 5 stars4.5/5 (3)
- Chemistry for Breakfast: The Amazing Science of Everyday LifeFrom EverandChemistry for Breakfast: The Amazing Science of Everyday LifeRating: 4.5 out of 5 stars4.5/5 (90)
- The Elements We Live By: How Iron Helps Us Breathe, Potassium Lets Us See, and Other Surprising Superpowers of the Periodic TableFrom EverandThe Elements We Live By: How Iron Helps Us Breathe, Potassium Lets Us See, and Other Surprising Superpowers of the Periodic TableRating: 3.5 out of 5 stars3.5/5 (22)
- Guidelines for Integrating Process Safety into Engineering ProjectsFrom EverandGuidelines for Integrating Process Safety into Engineering ProjectsNo ratings yet
- Monkeys, Myths, and Molecules: Separating Fact from Fiction, and the Science of Everyday LifeFrom EverandMonkeys, Myths, and Molecules: Separating Fact from Fiction, and the Science of Everyday LifeRating: 4 out of 5 stars4/5 (1)