Professional Documents
Culture Documents
Modified Atkins Diet and Low Glycemic Index Treatment For Medication Resistant Epilepsy Current Trends in Ketogenic Diet 2155 9562.S2 007
Uploaded by
starmittOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Modified Atkins Diet and Low Glycemic Index Treatment For Medication Resistant Epilepsy Current Trends in Ketogenic Diet 2155 9562.S2 007
Uploaded by
starmittCopyright:
Available Formats
Kumada et al.
, J Neurol Neurophysiol 2013, S2
http://dx.doi.org/10.4172/2155-9562.S2-007
Neurology & Neurophysiology
Research
Case
Report Article
Open
OpenAccess
Access
Modified Atkins Diet and Low Glycemic Index Treatment for MedicationResistant Epilepsy: Current Trends in Ketogenic Diet
Tomohiro Kumada*, Tomoko Miyajima, Ikuko Hiejima, Fumihito Nozaki, Anri Hayashi and Tatsuya Fujii
Department of Pediatrics, Shiga Medical Center for Children, Shiga, Japan
Abstract
Compared to the classical ketogenic diet (KD), the modified Atkins diet (MAD) and the low glycemic index
treatment (LGIT) are more liberal and less restrictive diet therapies for the treatment of medication-resistant epilepsy.
The MAD was first reported by Kossoff et al. in 2003, and gained global popularity with sufficient evidence in its
efficacy reported recently in a controlled study. The LGIT was first reported by Pfeifer et al. in 2005, and its use has
also become widespread. We reviewed the efficacy of both diet therapies in the treatment of medication-resistant
epilepsy based on the evidence from previous literatures and our own clinical experience. From our experience,
the LGIT was more liberal, tolerable, and dietetically balanced than the MAD. To find out which of these diets is
most appropriate in different epilepsies and different patients, future controlled comparative studies on the efficacy,
tolerability, and dietetic advantages between the MAD and the LGIT are necessary.
Keywords: Ketogenic diet; Modified Atkins diet; Low glycemic index
treatment; Epilepsy
Introduction
The ketogenic diets (KDs) have been used for the treatment of
medication-resistant epilepsy since the 1920s. The classical KD is a
highly restrictive diet with a 3:1-4:1 ketogenic ratio, calculated as the
weight of fat divided by that of carbohydrates plus protein. Although
the classical KD result in at least a 50% reduction in seizure frequency
in approximately half of epileptic patients, some patients cannot
tolerate the diet over a long period of time because of its restrictiveness.
Consequently, the modified Atkins diet (MAD) and the low glycemic
index treatment (LGIT) that are more liberal and less restrictive than
the classical KD, were developed in the 1990-2000s [1,2]. Contrary
to the classical KD, these diets can be provided without restriction of
calories, protein and fluid intake, and calculation of ketogenic ratio is
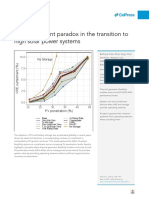
not necessary. Figure 1 shows the distribution of major nutrients in
calories in each diet [1,2]. MAD and LGIT have a similar composition
pattern and the percentage of fat is less than in KD. These new KDs
weigh greater importance in having a stable blood glucose level than
the production of ketone bodies.
Because the KDs including MAD and LGIT are the therapy that
the patients and parents must prepare by themselves, the menus of
the KDs are greatly affected by their food culture. Thus, the practical
menus of these KDs differ among countries based on various local food
cultures although the concepts of these KDs are common globally. For
example, Japanese patients and parents cannot cook daily KDs menus
by referring to the textbooks on the KDs in Western countries because
the available foods and the tastes are different between Japan and
Western countries. Therefore, we have designed the MAD and LGIT
menus which Japanese patients and parents can easily prepare and
resemble to normal Japanese ethnic menus.
In this paper, we describe the history of development of the KDs,
their methods and the evidence of clinical efficacy from the previous
literatures. In particular, we present how Japanese patients and parents
can cook the MAD and LGIT menus using Japanese ethnic foods
concretely in the section of dietary concept, compositon, and menu
of each diet. We also describe our own clinical experience in each of
these diets, and discuss which of these KDs (MAD or LGIT) should be
selected in different patients.
J Neurol Neurophysiol
History of the KDs from fasting to the LGIT
An overview of the history of the KDs shows that the focus has
changed from a diet that produces ketone bodies efficiently, which
mimics fasting, to one that is palatable and can therefore be followed
with high compliance. From the period of Hippocrates, it has been
known that seizures can be treated by fasting [3]. The KD protocols
consisting of high fat and low carbohydrate were designed to mimic the
metabolic effect of fasting. In 1921, Geyelin reported to the American
Medical Association that the beneficial effect of fasting continued even
after the fast was broken. Then, Wilder theorized that the benefit of the
diet depends on the ketonemia observed by Geyelin [3,4]. He showed
that ketosis occurred when the ratio of fatty acids to glucose was >2:1.
From this theory, the classical KD was developed and it was widely used
in the treatment of epilepsy. Huttenlocher developed a medium chain
triglyceride diet in an attempt to make the classical KD more palatable.
With the advancement of the pharmacotherapy for epilepsy, however,
the KD treatment has gradually become replaced by antiepileptic drugs,
particularly after the introduction of carbamazepine and valproic acid
in the 1970-80s.
A revival boom of the KDs occurred in the 1990s, starting with an
NBC Dateline report in 1994. Soon after, the television movie, First,
Do No Harm, starring Meryl Streep, which was a dramatization of
the life of a patient with epilepsy, turned the publics eye to the diet
in 1997. In the last decade, the KDs became popular globally; the 1st
international symposium on dietary treatments for epilepsy and
other neurological disorders was held in 2008, and the international
consensus recommendation was published in Epilepsia in 2009 [5].
*Corresponding author: Dr. Kumada, Department of Pediatrics, Shiga Medical
Center for Children, Moriyama, Japan, Tel: +81 77 582 6200; Fax: +81 77 582
6304; E-mail: tkumada@mccs.med.shiga-pref.jp
ReceivedMarch 13, 2013; Accepted June 13, 2013; Published June 20, 2013
Citation: Kumada T, Miyajima T, Hiejima I, Nozaki F, Hayashi A, et al. (2013)
Modified Atkins Diet and Low Glycemic Index Treatment for Medication-Resistant
Epilepsy: Current Trends in Ketogenic Diet. J Neurol Neurophysiol S2: 007
doi:10.4172/2155-9562.S2-007
Copyright: 2013 Kumada T, et al. This is an open-access article distributed under
the terms of the Creative Commons Attribution License, which permits unrestricted
use, distribution, and reproduction in any medium, provided the original author and
source are credited.
Epilepsy: Current Trends
ISSN: 2155-9562 JNN, an open access journal
Citation: Kumada T, Miyajima T, Hiejima I, Nozaki F, Hayashi A, et al. (2013) Modified Atkins Diet and Low Glycemic Index Treatment for MedicationResistant Epilepsy: Current Trends in Ketogenic Diet. J Neurol Neurophysiol S2: 007 doi:10.4172/2155-9562.S2-007
Page 2 of 6
Regular Diet
Classical KD
MAD
LGIT
Figure 1: Percentage of carbohydrate, fat, and protein in the regular diet, the classical KD, the MAD, and the LGIT.
Meanwhile, Kossoff from Johns Hopkins University Hospital
designed and reported on a new and more liberal KD called MAD in
2003 [6]. Since then, numerous articles on MAD have been published
from all over the world, including USA [7,8], Denmark [9,10], France
[11], Belgium [12], Korea [13,14], India [15], Iran [16], and Japan
[17]. Separately, in 2005, Pfeifer from Massachusetts General Hospital
developed and reported on an alternative ketogenic diet, LGIT, which
was more palatable than the MAD [18]. The diet has also gained a
widespread attention. Currently, the MAD and the LGIT are the main
KDs used in therapy especially in adolescent and adult patients [19].
The MAD
Dietary concept, composition and menu
The MAD was developed at Johns Hopkins Hospital to create
a KD that was more liberal and less restrictive than the classical KD
for children who were reluctant to follow the classical KD due to its
restrictiveness [1]. Dr. Atkins originally developed the diet in the
1970s as a method for weight reduction for people suffering from
obesity. This diet was modified so that the fat intake was increased
while the carbohydrate restriction was maintained the same as in the
introduction phase of the original method. The carbohydrate content
of the diet is restricted to 10 g per day at the initiation of the MAD,
and is subsequently maintained at 10-30 g per day. Calories, protein
and fluids are not restricted. As shown in (Figure 1), the proportion of
calories from fat is decreased in the MAD compared to the classical KD.
The amount of calories remained from the decrease in fat are assigned
to protein so that the ketogenic ratio resulted in 1:1 to 2:1 in the MAD
diet. Figure 2a and 2b shows an example of a lunch menu of the MAD
in our hospital. The content of carbohydrates, protein, and fat in this
menu was 2.5 g, 26.8 g, and 42.8 g respectively, and the ketogenic ratio
was 1.46:1, which was lower than that of the classical KD, 3:1 to 4:1.
Evidence of efficacy based on previous literatures
More than 50 articles on the use of MAD for medication-resistant
J Neurol Neurophysiol
epilepsy have been published since Kossoff et al. first reported on
the diet in 2003, and there is accumulating evidence for its efficacy
[5]. Auvin reviewed 7 prospective and 2 retrospective reports, and
summarized the efficacy of MAD as follows [20]; the responder rate
(the proportion of patients with >50% seizure reduction) was 51/87
(59%) after 1 month, 73/152 (48%) after 3 months, and 46/119 (39%)
after 6 months of MAD therapy. Chen et al. investigated the long-term
efficacy of the MAD and reported that the responder rate was 64/87
(74%) after 1 month, 36/54 (67%) after 6 months, 28/35 (80%) after
12 months, and 8/16 (50%) after 24 months in intent-to-treat analysis
[21]. Recently, a randomized controlled trial of the use of MAD for
the treatment of medication-resistant childhood epilepsy published
by Sharma et al. [22], showed that the proportion of patients with
>90% seizure reduction (30% vs. 7.7%, p=0.005) and that with>50%
seizure reduction (52% vs. 11.5%, p<0.001) was significantly higher in
the MAD group than in the control group after 3 months. A number
of published reports have shown the efficacy of the MAD in specific
epilepsy syndromes and underlying diseases including infantile spasms
[15], absence epilepsy [23], juvenile myoclonic epilepsy [24], SturgeWeber syndrome [25], and nonconvulsive status epilepticus [26].
Our experience
In our group, we have been treating medication-resistant epilepsy
with the MAD since 2007. Upon admission, the MAD was initiated
with a restriction of the carbohydrate content of the diet to10 g per day,
and the total calorie content was adjusted to match the patients usual
caloric intake before the diet. After 3 to 4 weeks on the diet, we let the
parents decide whether or not to continue the diet. We then follow the
patients after discharge every 1-3 months at the out-patient clinic.
In the current report, we summarized data from 16 patients who
started the MAD in our hospital. Table 1 shows the profile and shortterm efficacy and tolerability after 3 months on the diet in all of the
patients, including 10 patients reported elsewhere [17]. Eight patients
could not continue the diet for more than 3 months. Four of them,
Epilepsy: Current Trends
ISSN: 2155-9562 JNN, an open access journal
Citation: Kumada T, Miyajima T, Hiejima I, Nozaki F, Hayashi A, et al. (2013) Modified Atkins Diet and Low Glycemic Index Treatment for MedicationResistant Epilepsy: Current Trends in Ketogenic Diet. J Neurol Neurophysiol S2: 007 doi:10.4172/2155-9562.S2-007
Page 3 of 6
a. Regular diet
protein
24.1 g
carbohydrate
77.6 g
ketogenic ratio
0.12:1
fat
Total calorie
b. MAD
11.8 g
520 kcal
protein
26.8 g
carbohydrate
2.5 g
ketogenic ratio
1.46:1
c. LGIT
fat
Total calorie
42.8 g
517 kcal
protein
19.3 g
carbohydrate
22.2 g
ketogenic ratio
0.95:1
fat
39.5 g
Total calorie
520 kcal
Figure 2: Examples of a lunch menu for the regular diet, the MAD, and the LGIT Each style of lunch menu was provided to case-13 at our hospital. A regular diet
which she ate before the start of the MAD at 11 years of age. The lunch consisted of polished rice, boiled mackerel, salad with bean sprouts, nimono (boiled dish), and
banana. The ketogenic ratio was 0.12:1. This is an example of a diet usually preferred by Japanese. b. A MAD menu which she ate during MAD therapy at 11 years
of age. The lunch consisted of sauteed chicken with green beans and bacon, scrambled eggs with mayonnaise, and miso (soybean paste) soup. The ketogenic ratio
was 1.46:1. c. A LGIT menu which she ate during the LGIT at 13 years of age. The lunch consisted of unpolished rice with natto, pork beans, tuna salad, miso soup,
and sauteed chicken. The ketogenic ratio was 0.95:1.
including one who was infected with viral gastroenteritis, refused the
menus. In the remaining 4 patients, their families gave up preparing
the MAD after discharge. Excluding these drop-outs, the efficacy
at 3 months was as follows: 3 individuals were excellent responders
(seizure-free), 1 was a good responder (>50% seizure reduction), and
the diet was not efficacious in the remaining 4. The values of serum
beta-hydroxybutyrate were elevated over 2000umol/L at 3 months on
the diet in all cases investigated. The long-term efficacy of the MAD in
our patients is shown in Figure 3. The responder rate was 4/8 (50%) after
3 months, 3/6 (50%) after 6 months, 3/4 (75%) after 12 months, and 2/4
(50%) after 24 months on the diet. All of 4 patients who completed 24
months of the diet discontinued the diet afterwards. One patient (case2) of those who achieved seizure control at the 24 months has been
seizure-free since then, although the other patient (case-3) suffered
a relapse of seizures soon after the diet was stopped. There were no
side effects on the laboratory examinations during the course of the
diet except serum total-cholesterol which were slightly elevated (270300 mg/dl) in some patients. There were no patients who experienced
weight loss or failure of appropriate weight gain during the diet. Severe
side effects, which led to an interruption of the MAD occurred in 3
patients: generalized fatigue with severe acidosis (pH 7.20 on blood
gas analysis) on the third day of the diet (case-2). Generalized fatigue
with unknown cause within 1 week on the diet (case-9), and fainting
with hypoglycemia due to refusal of food intake after one month on
the diet (case-16). Although case-9 and -16 gave up the restart of the
MAD, case-2 could resume the MAD ten days later. Our results suggest
that even the MAD has potentially severe life-threatening side effects,
especially in the early period from the start of the diet, although many
authors have emphasized that the MAD can be safely introduced
without hospital admission in contrast to the classical KD [1].
The Low Glycemic Index Treatment (LGIT)
The GI values of foods available in Western countries can be found
in the literature [27]. In addition to this report, we used the list of the
GI values of Japanese foods prescribed in our previous report [28].
Japanese ethnic foods such as udon (flour noodle), soba (buckwheet
noodle), and unpolished Japonica rice mixed with various supplements
such as natto (fermented soybeans) and grated yam are all available in
the LGIT.
Figure 2c shows an example of a lunch menu for the LGIT used
in our hospital, in which the total daily calorie intake is 1600 kcal. The
carbohydrate used in the lunch was unpolished Japonica rice mixed
with natto. The GI value of the unpolished rice is lower than that of
polished rice because it has more fiber than its polished counterpart,
which can delay the absorption of glucose from the intestine and
decrease the speed at which blood glucose increases. Moreover, when
mixed with natto, the rate of glucose absorption was reduced, and the
GI value of unpolished rice decreases further to fewer than 50 relative
to glucose. The content of carbohydrates, protein, and fat in Figure 1c
was 22.2 g, 19.3 g, and 39.5 g respectively, and the ketogenic ratio was
0.95:1, which is lower than that of the classical KD and the MAD.
Evidence of efficacy based on previous literatures
Dietary concept, composition and menu
The glycemic index (GI), designed by Jenkins in 1981 [2], is an
indicator of the degree of the increase of blood glucose levels by a
specific food as compared to that of a standard food. Low GI foods
have since been used for the treatment of diabetes mellitus and obesity.
J Neurol Neurophysiol
In 2005, Pfeifer et al. from Massachusetts General Hospital first
reported on an alternative ketogenic diet, LGIT for the purpose of
maintaining compliance to diet therapy [18]. This diet allows a more
liberal daily intake of carbohydrates (40-60 g per day) than the other
KDs, on condition that the GI of carbohydrates is restricted to less than
50 relative to glucose. In the LGIT, a typical proportions of calories are
as follows; 60-65% from fat, 20-30% from protein, and 10-15% from
carbohydrates (Figure 1). Calories and fluids are not restricted. As a
result, the diet is a more palatable and less rigid KD (ketogenic ratio is
almost 1:1). The foods do not need to be weighed since the amount is
based on portion sizes, which are based on diabetic exchanges.
The LGIT was first reported to be effective for the treatment of
medication-resistant epilepsy at Massachusetts General Hospital [18].
In their recent report, the responder rate was 42%, 50% ,54% 64%, and
66% at 1, 3, 6, 9 and 12 months after treatment, respectively in intentto-treat analysis [29]. Coppola et al. from Italy showed that 8 of 15
Epilepsy: Current Trends
ISSN: 2155-9562 JNN, an open access journal
Citation: Kumada T, Miyajima T, Hiejima I, Nozaki F, Hayashi A, et al. (2013) Modified Atkins Diet and Low Glycemic Index Treatment for MedicationResistant Epilepsy: Current Trends in Ketogenic Diet. J Neurol Neurophysiol S2: 007 doi:10.4172/2155-9562.S2-007
Page 4 of 6
patients (53%) with the LGIT achieved >50% seizure reduction in the
first report published outside of Massachusetts General Hospital [30].
Recently, successful treatments with the LGIT for seizures associated
with tuberous sclerosis complex [31], Angelman syndrome [32], and
mitochondrial disorder [33] have also been reported. However, no
controlled studies on the efficacy of the LGIT for the treatment of
medication-resistant epilepsy are available. To qualify the evidence for
the LGIT, randomized controlled studies are necessary.
Our experience
We first introduced the LGIT to case-13 in Table 1 because she had
refused to comply with the MAD only 2 weeks after the diet therapy
even though her seizures remitted with the MAD. She continued to
tolerate the LGIT for over 1 year and achieved >50% seizure reduction.
Her detailed clinical course with this diet therapy will be published
elsewhere [28]. We have tried the LGIT in only 3 patients and no
reports other than ours are available in Japan so far. It seems, therefore,
that the LGIT has not yet become a popular therapy for medicationresistant epilepsy in Japan. However, we assume that this diet will
gain popularity in this country where the rice is a staple food; rice is
acceptable with this diet therapy although only unpolished and a small
amount of rice were permitted.
Which diet should we use, the MAD or the LGIT?
Several reports in the literature compared the efficacy of the classical
KD and the MAD: Two articles reported a tendency for a higher
responder rate with the classical KD than the MAD after 6 months
(7/17 vs. 2/10, p=0.41 in Porta et al. [11], 30/50 vs. 13/33, p=0.06 in
Miranda et al. [34]), although the differences were not significant.
Kossoff et al. reported that patients with Doose syndrome achieved
more seizure control by switching from the MAD to the classical KD
[35]. In addition, Auvin insisted that the classical KD, not the MAD
100%
90%
80%
70%
60%
discontinued
50%
poor
40%
good
30%
excellent
20%
10%
0%
1 month
3 month
6 months
12 months
24 months
Figure 3: Percent of patients with excellent response (seizure-free), good response (>50% seizure reduction), poor response (<50% seizure reduction) on LGIT, and
discontinued at each follow up interval.
Case/sex
Age at the
Underlying
Epilepsy
Seizure
Seizure
Efficacy
Reasons of
beta-hydroxy-
start of MAD
disease
classification
phenotype
frequency
at 3 months
discontinuation
butyrate at 3 months
Reject By Patient
1/Male
1y6m
leukodystrophy
SLRE
Complex Partial
Weekly
Discontinued
2/Female
1y6m
Trisomy 21
IS
Spasms
Daily
Excellent
4929 umol/L
3/Male
1y11m
IS
Spasms, Tonic
Daily
Excellent
3986 umol/L
4/Male
2y2m
IS
Spasms, Tonic
Daily
Unchanged
5/Female
3y
Doose
MAS, Myoclonic
Daily
Discontinued
6/Female
3y
IS
Spasms, Tonic
Daily
Unchanged
7/Female
3y
IS
Spasms, Tonic
Daily
Unchanged
not done
8/Male
3y
IS
Spasms, Tonic
Daily
Unchanged
6174 umol/L
5470 umol/L
Reject By Family
not done
9/Female
3y
tuberous sclerosis
LGS
Tonic, Atypical Absence
Daily
Discontinued
10/Female
5y
band heterotopia
unclassified
NCSE, Gtcs, Drop
Daily
Excellent
11/Female
5y
SLRE
NCSE, Tonic, Hypermotor
Daily
Good
12/Male
7y
SLRE
Tonic
Weekly
Discontinued
Reject By Family
13/Female
11y
tuberous sclerosis
LGS
Tonic, Atypical Absence
Daily
Discontinued
Reject By Patient
14/Female
17y
tuberous sclerosis
LGS
Tonic, Atypical Absence
Daily
Discontinued
Reject By Family
15/Female
29y
15q inv dup
syndrome
SLRE
Daily
Discontinued
Reject By Family
16/Female
32y
Weekly
Discontinued
Reject By Patient
SLRE
Complex Partial, Gtcs
Reject By Patient
2376 umol/L
2795 umol/L
Table 1: Profiles of patients who started the MAD in our hospital and the short-term efficacy and tolerability after 3 months on the diet Abbreviations: SLRE, symptomatic
localization-related epilepsy; IS, infantile spasms; LGS, Lennox-Gastaut syndrome; Doose, Doose syndrome; NCSE, nonconvulsive status epilepticus; GTCs, generalized
tonic clonic seizure; excellent, seizure-free; good, >50% seizure reduction; unchanged; <50% seizure reduction.
J Neurol Neurophysiol
Epilepsy: Current Trends
ISSN: 2155-9562 JNN, an open access journal
Citation: Kumada T, Miyajima T, Hiejima I, Nozaki F, Hayashi A, et al. (2013) Modified Atkins Diet and Low Glycemic Index Treatment for MedicationResistant Epilepsy: Current Trends in Ketogenic Diet. J Neurol Neurophysiol S2: 007 doi:10.4172/2155-9562.S2-007
Page 5 of 6
%DRI
(%)
150
100
MAD
LGIT
50
0
Ca
Mg
Fe
Zn
Cu
Vit.B1
Vit.B2
Vit.B6
Folate
Vit.C
Figure 4: %DRI of daily micronutrient distribution based on the mean amount in each of the diets (the MAD and the LGIT) prepared for case-13 at our hospital. %DRI
was calculated as the daily amount of each micronutrient (the mean value for 2 weeks) divided by the recommended dietary allowance provided by Dietary reference
intakes for Japanese, 2010. Based on this, insufficiency in intake of a specific micronutrient resulted in a %DRI <100%. Blue rod: the MAD, Red rod: the LGIT
should be tried in the epileptic emergency such as recent onset of
infantile spasms and refractory status epilepticus because the former
can resolve the seizures faster [20].
Although increasing number of evidences are becoming available
that indicates an appropriate choice between the classical KD and the
MAD as mentioned above, we still do not have clear answers to govern
our choice between the MAD or the LGIT. Our experience with case13 in Table 1 who tolerated the LGIT better than the MAD suggested
that the LGIT should be considered for patients with medicationresistant epilepsy who cannot tolerate more restrictive diet therapies.
On the other hand, there has not been any comparative data from the
dietetic perspective between the MAD and the LGIT. Figure 4 shows
the micronutrient distribution in the MAD and the LGIT given to
case-13 at our hospital. The % dietary reference intakes (%DRI) of all
of the minerals and soluble vitamins listed were higher in the LGIT
than in the MAD. Furthermore, among all of the subjects, the %DRI
of some soluble vitamins (B2, C, and folate) was >100% in the LGIT,
making supplementation unnecessary. Therefore, we believe that the
LGIT would be superior to the MAD based on its tolerability and
dietetic balance. However, we do not have data from a controlled trial
or retrospective analysis, comparing the efficacy of the MAD and the
LGIT.
Conclusion
Currently, there is a large volume of evidence, including one
controlled trial, on the efficacy of the MAD for seizure control, and
the diet was established as an important treatment for medicationresistant epilepsy. In contrast, there is less evidence for use of the LGIT
without any controlled trials. This therapy is less popular than the
MAD, especially in Japan. Further comparative data on the efficacy,
tolerability and dietetic balance of both the MAD and the LGIT are
needed in order to select the best type of diet therapy for patients with
medication-resistant epilepsy.
Acknowledgements
We gratefully thank Miyuki Takada, the dietitian of our hospital, for designing
the MAD and LGIT menus. The authors report no conflicts of interest.
References
1. Kossoff EH, Dorward JL (2008) The modified Atkins diet. Epilepsia 49 Suppl
8: 37-41.
J Neurol Neurophysiol
2. Pfeifer HH, Lyczkowski DA, Thiele EA (2008) Low glycemic index treatment:
implementation and new insights into efficacy. Epilepsia 49 Suppl 8: 42-45.
3. Wheless JW (2004) Epilepsy and the ketogenic diet. Humana Press, New
Jersey.
4. Freeman JM, Kossoff EH, Hartman AL (2007) The ketogenic diet: one decade
later. Pediatrics 119: 535-543.
5. Kossoff EH, Zupec-Kania BA, Amark PE, Ballaban-Gil KR, Christina Bergqvist
AG, et al. (2009) Optimal clinical management of children receiving the
ketogenic diet: recommendations of the International Ketogenic Diet Study
Group. Epilepsia 50: 304-317.
6. Kossoff EH, Krauss GL, McGrogan JR, Freeman JM (2003) Efficacy of the
Atkins diet as therapy for intractable epilepsy. Neurology 61: 1789-1791.
7. Kossoff EH, McGrogan JR, Bluml RM, Pillas DJ, Rubenstein JE, et al. (2006)
A modified Atkins diet is effective for the treatment of intractable pediatric
epilepsy. Epilepsia 47: 421-424.
8. Kossoff EH, Rowley H, Sinha SR, Vining EP (2008) A prospective study of the
modified Atkins diet for intractable epilepsy in adults. Epilepsia 49: 316-319.
9. Weber S, Mlgaard C, Karentaudorf, Uldall P (2009) Modified Atkins diet to
children and adolescents with medical intractable epilepsy. Seizure 18: 237240.
10. Miranda MJ, Mortensen M, Povlsen JH, Nielsen H, Beniczky S (2011) Danish
study of a modified Atkins diet for medically intractable epilepsy in children:
can we achieve the same results as with the classical ketogenic diet? Seizure
20: 151-155.
11. Porta N, Valle L, Boutry E, Fontaine M, Dessein AF, et al. (2009) Comparison
of seizure reduction and serum fatty acid levels after receiving the ketogenic
and modified Atkins diet. Seizure 18: 359-364.
12. Carrette E, Vonck K, de Herdt V, Dewaele I, Raedt R, et al. (2008) A pilot trial
with modified Atkins diet in adult patients with refractory epilepsy. Clin Neurol
Neurosurg 110: 797-803.
13. Kang HC, Lee HS, You SJ, Kang du C, Ko TS, et al. (2007) Use of a modified
Atkins diet in intractable childhood epilepsy. Epilepsia 48: 182-186.
14. Kim YM, Vaidya VV, Khusainov T, Kim HD, Kim SH, et al. (2012) Various
indications for a modified Atkins diet in intractable childhood epilepsy. Brain
Dev 34: 570-575.
15. Sharma S, Sankhyan N, Gulati S, Agarwala A (2012) Use of the modified Atkins
diet in infantile spasms refractory to first-line treatment. Seizure 21: 45-48.
16. Tonekaboni SH, Mostaghimi P, Mirmiran P, Abbaskhanian A, Abdollah Gorji
F, et al. (2010) Efficacy of the Atkins diet as therapy for intractable epilepsy in
children. Arch Iran Med 13: 492-497.
17. Kumada T, Miyajima T, Oda N, Shimomura H, Saito K, et al. (2012) Efficacy
Epilepsy: Current Trends
ISSN: 2155-9562 JNN, an open access journal
Citation: Kumada T, Miyajima T, Hiejima I, Nozaki F, Hayashi A, et al. (2013) Modified Atkins Diet and Low Glycemic Index Treatment for MedicationResistant Epilepsy: Current Trends in Ketogenic Diet. J Neurol Neurophysiol S2: 007 doi:10.4172/2155-9562.S2-007
Page 6 of 6
and tolerability of modified Atkins diet in Japanese children with medicationresistant epilepsy. Brain Dev 34: 32-38.
27. Foster-Powell K, Holt SH, Brand-Miller JC (2002) International table of glycemic
index and glycemic load values: 2002. Am J Clin Nutr 76: 5-56.
18. Pfeifer HH, Thiele EA (2005) Low-glycemic-index treatment: a liberalized
ketogenic diet for treatment of intractable epilepsy. Neurology 65: 1810-1812.
28. Kumada T, Hiejima I, Nozaki F, Hayashi A, Fujii T (2013) Glycemic index
treatment using Japanese foods in a girl with Lennox-Gastaut syndrome.
Pediatr Neurol 48: 390-392.
19. Payne NE, Cross JH, Sander JW, Sisodiya SM (2011) The ketogenic and
related diets in adolescents and adults--a review. Epilepsia 52: 1941-1948.
20. Auvin S (2012) Should we routinely use modified Atkins diet instead of regular
ketogenic diet to treat children with epilepsy? Seizure 21: 237-240.
29. Muzykewicz DA, Lyczkowski DA, Memon N, Conant KD, Pfeifer HH, et al.
(2009) Efficacy, safety, and tolerability of the low glycemic index treatment in
pediatric epilepsy. Epilepsia 50: 1118-1126.
21. Chen W, Kossoff EH (2012) Long-term follow-up of children treated with the
modified Atkins diet. J Child Neurol 27: 754-758.
30. Coppola G, DAniello A, Messana T, Di Pasquale F, della Corte R, et al. (2011)
Low glycemic index diet in children and young adults with refractory epilepsy:
first Italian experience. Seizure 20: 526-528.
22. Sharma S, Sankhyan N, Gulati S, Agarwala A (2013) Use of the modified Atkins
diet for treatment of refractory childhood epilepsy: a randomized controlled trial.
Epilepsia 54: 481-486.
31. Larson AM, Pfeifer HH, Thiele EA (2012) Low glycemic index treatment for
epilepsy in tuberous sclerosis complex. Epilepsy Res 99: 180-182.
23. Groomes LB, Pyzik PL, Turner Z, Dorward JL, Goode VH, et al. (2011) Do
patients with absence epilepsy respond to ketogenic diets? J Child Neurol 26:
160-165.
32. Thibert RL, Pfeifer HH, Larson AM, Raby AR, Reynolds AA, et al. (2012) Low
glycemic index treatment for seizures in Angelman syndrome. Epilepsia 53:
1498-1502.
24. Kossoff EH, Henry BJ, Cervenka MC (2013) Efficacy of dietary therapy for
juvenile myoclonic epilepsy. Epilepsy Behav 26: 162-164.
33. Martikainen MH, Pivrinta M, Jskelinen S, Majamaa K (2012) Successful
treatment of POLG-related mitochondrial epilepsy with antiepileptic drugs and
low glycaemic index diet. Epileptic Disord 14: 438-441.
25. Kossoff EH, Borsage JL, Comi AM (2010) A pilot study of the modified Atkins
diet for Sturge-Weber syndrome. Epilepsy Res 92: 240-243.
34. Miranda MJ, Turner Z, Magrath G (2012) Alternative diets to the classical
ketogenic diet--can we be more liberal? Epilepsy Res 100: 278-285.
26. Kumada T, Miyajima T, Kimura N, Saito K, Shimomura H, et al. (2010) Modified
Atkins diet for the treatment of nonconvulsive status epilepticus in children. J
Child Neurol 25: 485-489.
35. Kossoff EH, Bosarge JL, Miranda MJ, Wiemer-Kruel A, Kang HC, et al. (2010)
Will seizure control improve by switching from the modified Atkins diet to the
traditional ketogenic diet? Epilepsia 51: 2496-2499.
Submit your next manuscript and get advantages of
OMICS Group submissions
Unique features:
Citation: Kumada T, Miyajima T, Hiejima I, Nozaki F, Hayashi A, et al. (2013)
Modified Atkins Diet and Low Glycemic Index Treatment for MedicationResistant Epilepsy: Current Trends in Ketogenic Diet. J Neurol Neurophysiol
S2: 007 doi:10.4172/2155-9562.S2-007
This article was originally published in a special issue, Epilepsy: Current
Trends handled by Editor(s). Dr. Espinosa PS, Centro Internacional en
Neurociencias, USA
J Neurol Neurophysiol
User friendly/feasible website-translation of your paper to 50 worlds leading languages
Audio Version of published paper
Digital articles to share and explore
Special features:
250 Open Access Journals
20,000 editorial team
21 days rapid review process
Quality and quick editorial, review and publication processing
Indexing at PubMed (partial), Scopus, EBSCO, Index Copernicus and Google Scholar etc
Sharing Option: Social Networking Enabled
Authors, Reviewers and Editors rewarded with online Scientific Credits
Better discount for your subsequent articles
Submit your manuscript at: http://www.omicsonline.org/submission
Epilepsy: Current Trends
ISSN: 2155-9562 JNN, an open access journal
You might also like
- Age Stratified IFRDocument13 pagesAge Stratified IFRstarmittNo ratings yet
- Low Vol HIIT Mito BiogenesisDocument12 pagesLow Vol HIIT Mito BiogenesisstarmittNo ratings yet
- Change in Chol Vs MortalityDocument11 pagesChange in Chol Vs MortalitystarmittNo ratings yet
- Curtailment SolarDocument26 pagesCurtailment SolarstarmittNo ratings yet
- Meat and Cancer in QDDocument14 pagesMeat and Cancer in QDstarmittNo ratings yet
- 1 PDFDocument11 pages1 PDFJoeljar Enciso SaraviaNo ratings yet
- Clinical Utility of Inflammatory MarkersDocument30 pagesClinical Utility of Inflammatory MarkersstarmittNo ratings yet
- The Global Influence of The Seventh-Day AdventistDocument25 pagesThe Global Influence of The Seventh-Day AdventistSem JeanNo ratings yet
- Sleep Paterns StudyDocument9 pagesSleep Paterns StudyHiram CastroNo ratings yet
- P Intake RDA ReviewDocument11 pagesP Intake RDA ReviewstarmittNo ratings yet
- Effectiveness of Chol W:o Drugs PDFDocument5 pagesEffectiveness of Chol W:o Drugs PDFstarmittNo ratings yet
- K2 in DairyDocument6 pagesK2 in DairystarmittNo ratings yet
- Gut Biome Mod PaleoDocument14 pagesGut Biome Mod PaleostarmittNo ratings yet
- Jama Woolf 2019 SC 190006Document21 pagesJama Woolf 2019 SC 190006JasonNo ratings yet
- Delay Reverse FrailtyDocument9 pagesDelay Reverse FrailtystarmittNo ratings yet
- Flavanoids and EDDocument8 pagesFlavanoids and EDstarmittNo ratings yet
- Walking and T2DDocument9 pagesWalking and T2DstarmittNo ratings yet
- Centenarian ConcentrationsDocument17 pagesCentenarian ConcentrationsstarmittNo ratings yet
- RS Blood Lipids Glucose ControlDocument7 pagesRS Blood Lipids Glucose ControlstarmittNo ratings yet
- Meta-Analysis Prospective Cohort Studies PDFDocument12 pagesMeta-Analysis Prospective Cohort Studies PDFstarmittNo ratings yet
- The Effect of Regular Exercise On Insulin Sensitivity in Diabetes Tipo II. Revisión Sistemática y Meta-AnálisisDocument17 pagesThe Effect of Regular Exercise On Insulin Sensitivity in Diabetes Tipo II. Revisión Sistemática y Meta-AnálisisJuanma GonzalezNo ratings yet
- Simon Abundance Index PDFDocument28 pagesSimon Abundance Index PDFstarmittNo ratings yet
- VO2 TrainabilityDocument7 pagesVO2 TrainabilitystarmittNo ratings yet
- Time-Restricted Feeding Is A Preventative and Therapeutic Intervention Against Diverse Nutritional ChallengesDocument15 pagesTime-Restricted Feeding Is A Preventative and Therapeutic Intervention Against Diverse Nutritional ChallengessmashdwarfNo ratings yet
- Etiological Effects Optimal Intakes For RiskDocument25 pagesEtiological Effects Optimal Intakes For RiskstarmittNo ratings yet
- Carb Restriction Metabolic SyndromeDocument17 pagesCarb Restriction Metabolic Syndromestarmitt100% (1)
- Accepted Manuscript: Journal of HepatologyDocument31 pagesAccepted Manuscript: Journal of HepatologyNCNo ratings yet
- The Effect of Regular Exercise On Insulin Sensitivity in Diabetes Tipo II. Revisión Sistemática y Meta-AnálisisDocument17 pagesThe Effect of Regular Exercise On Insulin Sensitivity in Diabetes Tipo II. Revisión Sistemática y Meta-AnálisisJuanma GonzalezNo ratings yet
- 2015 Adaptações Cardiovasculares Ao ExercícioDocument32 pages2015 Adaptações Cardiovasculares Ao ExercícioLeonardoCampanelliNo ratings yet
- Articulo SeminarioDocument10 pagesArticulo SeminariomaiksoNo ratings yet
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (120)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- 1 Title and SynopsisDocument11 pages1 Title and SynopsisMuhammad Arief ArdiansyahNo ratings yet
- Practice Test 05 - Hints & Solutions - Lakshya NEET 2024Document15 pagesPractice Test 05 - Hints & Solutions - Lakshya NEET 2024Pandey 14No ratings yet
- The Endocrine System and Feedback MechanismsDocument8 pagesThe Endocrine System and Feedback MechanismsJame SmithNo ratings yet
- One Answer To Cancer by William Donald Kelley, D.D.S., M.S.Document53 pagesOne Answer To Cancer by William Donald Kelley, D.D.S., M.S.Teti Haxhidauti94% (16)
- Lifebuoy 120324115017 Phpapp02Document38 pagesLifebuoy 120324115017 Phpapp02Binush ThampanNo ratings yet
- Running Head:: Prothrombotic Effect of Mimosa PudicDocument28 pagesRunning Head:: Prothrombotic Effect of Mimosa PudicGINAROSE DEGUZMANNo ratings yet
- Is Fast Food The New Tobacco PDFDocument6 pagesIs Fast Food The New Tobacco PDFCustom Writing ServicesNo ratings yet
- Foods High in Uric AcidDocument12 pagesFoods High in Uric AcidAndrelyn Macadaeg100% (1)
- Transient Tachypnea of The Newborn (TTN)Document6 pagesTransient Tachypnea of The Newborn (TTN)Wivan Havilian DjohanNo ratings yet
- PN NCLEX - Integrated (A)Document63 pagesPN NCLEX - Integrated (A)fairwoods89% (19)
- Child Protection Training ManualDocument229 pagesChild Protection Training Manualbabuin1No ratings yet
- Requirements For Human LifeDocument5 pagesRequirements For Human LifeJayrelle D. SafranNo ratings yet
- Test Name Result Unit Reference Interval EndocrinolgyDocument1 pageTest Name Result Unit Reference Interval Endocrinolgygeetha kodaliNo ratings yet
- Left Thigh Pain: I. Chief Complaint/ Other ComplaintsDocument9 pagesLeft Thigh Pain: I. Chief Complaint/ Other ComplaintsDominic BristolNo ratings yet
- Surgery Toacs APRIL 2012: Hassaan Bari Aga Khan UniversityDocument18 pagesSurgery Toacs APRIL 2012: Hassaan Bari Aga Khan UniversitySyedNo ratings yet
- Food Crisis in The World !Document6 pagesFood Crisis in The World !ChrissBright E. HermanNo ratings yet
- September 26, 2018 by Sagar Aryal: Antigen-Properties, Types and Determinants of AntigenicityDocument23 pagesSeptember 26, 2018 by Sagar Aryal: Antigen-Properties, Types and Determinants of AntigenicityEzekiel GantiedNo ratings yet
- 4UFZ75PF0FYRH8 4UFZ75PF0FYRH8 : Division of Forensic SciencesDocument7 pages4UFZ75PF0FYRH8 4UFZ75PF0FYRH8 : Division of Forensic SciencesAttila KissNo ratings yet
- GB PerforationDocument13 pagesGB Perforationmudasir61No ratings yet
- Blood Grouping ReagentsDocument7 pagesBlood Grouping ReagentsDominic EmerencianaNo ratings yet
- Semmelweis' Handwashing & Lister's Antiseptic TechniqueDocument22 pagesSemmelweis' Handwashing & Lister's Antiseptic TechniqueNewNo ratings yet
- 9 Steps To Reverse DementiaDocument36 pages9 Steps To Reverse DementiaLavinia PirlogNo ratings yet
- PEDIA Nursing NCLEX Bullets Part 1Document166 pagesPEDIA Nursing NCLEX Bullets Part 1Russel Myron Adriano AdvinculaNo ratings yet
- Spontaneous Pneumothorax - Management Feb15Document12 pagesSpontaneous Pneumothorax - Management Feb15samuelNo ratings yet
- Congenital Insensitivity To Pain With Anhidrosis (CIPA) : A Case ReportDocument5 pagesCongenital Insensitivity To Pain With Anhidrosis (CIPA) : A Case ReportAhmad DiazNo ratings yet
- Assisting IV BTDocument89 pagesAssisting IV BTmhelshy villanuevaNo ratings yet
- Statistics Notes in The British Medical Journal (Bland JM, Altman DG. - NEJ)Document95 pagesStatistics Notes in The British Medical Journal (Bland JM, Altman DG. - NEJ)pegazus_arNo ratings yet
- Fisiologi StarvasiDocument47 pagesFisiologi Starvasicynthia maharaniNo ratings yet
- Clandestine Sorbolene !!: Sorbolene Cream, What Is It & What Is It Made From ?Document6 pagesClandestine Sorbolene !!: Sorbolene Cream, What Is It & What Is It Made From ?Indika Lakshmana PathirathneNo ratings yet
- Stadardization of Ayurvedic Clinical TerminologiesDocument242 pagesStadardization of Ayurvedic Clinical TerminologiesAbhishek100% (1)