Professional Documents
Culture Documents
June-Issue 12
Uploaded by
Nephrology On-DemandOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
June-Issue 12
Uploaded by
Nephrology On-DemandCopyright:
Available Formats
Contributors: A Bansal (U of Pennsylvania) | P Dedhia (U of Cincinnati) | A Elebiary (Lahey Clinic) | X Vela (U of El Salvador) | D Thomson (ECU) | P Jawa (ECU) | S Sridharan
(Lister H ospital, UK)
F Iannuzsella (U of Parma, Italy) | D M itema (Johns H opkins U)
Courtesy: D. Divakaran | mostphotos.com/ 1987407/ human- kidney
Kidney
Konnection
Stay connected with Kidney Konnection through the N OD Plus App: http: / / goo.gl/ tfSAQT
ISSN 2372- 0824 (Print) | 2372- 0832 (Electronic)
Kidney Konnection is a monthly independent publication from N ephrology On- Demand
KIDNEY FAILURE, BLEEDING, & THE GI TRACT
(by Ahmed Elebiary)
It's a fact! The incidence of GI bleeding in chronic kidney disease patients including those on dialysis is significantly higher than the
general population. Acute upper gastrointestinal bleeding carries a very high mortality; it accounts for 3- 7% of all deaths in patients with
ESRD. In an analysis of the US Renal Data System (USRDS) Dialysis M orbidity and M ortality Study, Wasse and colleagues reported a
rate of 23 upper GI bleeding events per 1000 person- years. That's more than 10 times higher than the general population. There is a one
study showed that 19% of patients with CKD have +ve FOBTs!
Why do they bleed more? Uremia is very toxic to both the GI mucosa and platelets; that?s all you need to cause an intractable
gastrointestinal hemorrhage. Uremia causes platelet dysfunction. There is also a direct effect of uremia on the GI mucosa due to oxidative
stress. In addition to that, patients receiving hemodialysis (H D) have a higher risk because of heparin used during H D. Risk increases
with other co- morbidities like diabetes mellitus, coronary artery disease, cirrhosis and the use of non- steroidal anti- inflammatory drugs.
Where do they bleed from? Bleeding can happen anywhere from the esophagus to the rectum. Angiodysplasias and gastritis/ peptic ulcer
disease are the most common causes of upper GI bleeding. The most common site is the duodenum. Duodenal lesions were found in 61%
of ERSD patients with +ve fecal occult blood tests. The most common site of lower gastrointestinal tract bleeding is the proximal colon.
Colonic neoplasms, angiodyplasia and diverticulosis are the most common causes of lower tract bleeding. Angiodysplasia has been shown
to cause an increased risk of recurrent bleeding in patients with renal failure and is the most common cause of recurrent lower
gastrointestinal bleeding likely due to use of heparin 3 times a week during hemodialysis.
What should I do? Always keep in mind that GI bleeding is very common in CKD and ESRD patients. Anemia should always be
evaluated with a thorough history, physical exam (and yes, a digital rectal exam with stool guaiac is needed!). Avoid the common
mistake of attributing anemia to erythropoietin deficiency. Screen these high risk patients and refer them to gastroenterology early.
I THINK THEREFORE I KNOW (ANSWERS)
In the April issue we asked you about a 70- year- old patient with non- specific complaints. You spun his/ her urine (Image A) and found
an interesting finding that prompted you to biopsy his/ her kidney. The biopsy findings were shown in Image B and you were asked to
comment on the images, diagnosis, and/ or treatment.
Image A
<- - Image A shows one of many erythrocyte casts
(aka red blood cell casts).
Image B shows one of many glomeruli with - - >
crescents (a bit hard to tell if the crescents are
cellular, fibrocellular, or fibrous)
(continued on page 2)
Image B
Want a complimentary print subscription?
N ephrology On- Demand
Issue 12 | Volume 1 | 2015
Email myFellowship@ecu.edu for details
myFellowship@ecu.edu
https:/
/
www.scribd.com/
doc/
251289582/
JuneIssue12
http: / / goo.gl/ tfSAQT
Editor: Tejas Desai | Chief: Cynthia Christiano
FIND M E...I'M LOST (ANSWERS)
In the M ay issue we introduced our first Word Find (Topic: renal failure in stem cell transplantation). Admittedly, this
was a hard word find to complete. N evertheless, we want to congratulate our winners and everyone who made an
attempt. Below are the answers.
Clues
1.
The acronym for the condition that
occurs in up to 50% of stem cell
transplant recipients
This entity is indistinguishable from
hepatorenal syndrome and is a major
cause of renal failure in patients
undergoing myeloablative stem cell
transplantation
An antithrombotic and fibrinolytic
used in the management of
venoocclusive disease
The drug class of choice in the
treatment of thrombotic
microangiopathy
Chronic graft- versus- host disease is
associated with this nephrologic
syndrome
Severe forms of thrombotic
microangiopathy require this form of
therapy
The type of stem cell transplant
whereby the cells are from a donor
The type of stem cell transplant
whereby the cells are from a patient
2.
3.
4.
5.
6.
7.
8.
Answers
1. CVH D
2. Venooclusive Disease
3. Defibrotide
4. ACE inhibitor
5. N ephrotic Syndrome
6. Plasmapheresis
7. Allogeneic
8. Autologous
I THINK THEREFORE I KNOW (ANSWERS)
(continued from page 1)
The serologies finally returned and the patient was anti- neutrophil cytoplasmic antibody (AN CA) positive (titer = 1: 640). Based on this
information, the most appropriate diagnosis at this time is AN CA- associated vasculitis (AAV)
Treatment for this condition will depend on a number of factors (some of which are listed below):
-
Age: younger does better than older
Gender: women of child- bearing age must consider the detrimental effects of treatment on future reproductive ability
Race: African- Americans may do better w/ some regimens versus others
Entry creatinine & / or need for renal replacement therapy: higher the former (esp. > 5.0 mg/ dl) or need for dialysis both forecast a
poorer prognosis
- Degree of interstitial fibrosis/ tubular atrophy on biopsy: the more there is, the worse the renal outcome
- Type of crescents: cellular crescents may respond a bit better than fibrous crescents
- Presence of anti- GBM antibody: believe it or not, this actually forecasts a better prognosis (still unclear why)
In an upcoming issue we'll go over the treatment options for AN CA- associated vasculitides.
2
(Thanks to Dr. Jordan Weinstein
(@UKidney) for the images)
You might also like
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- December 2015Document2 pagesDecember 2015Nephrology On-DemandNo ratings yet
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- March-Issue 9Document2 pagesMarch-Issue 9Nephrology On-DemandNo ratings yet
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- 2017 #Nephmadness Tournament Selection ReportDocument24 pages2017 #Nephmadness Tournament Selection ReportNephrology On-Demand100% (1)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Gender Gap PosterDocument1 pageGender Gap PosterNephrology On-DemandNo ratings yet
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Dialysis CalendarDocument1 pageDialysis CalendarNephrology On-DemandNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- July 2015Document2 pagesJuly 2015Nephrology On-DemandNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Role of YouTube in The Same-Sex Referendums of North Carolina and WashingtonDocument1 pageRole of YouTube in The Same-Sex Referendums of North Carolina and WashingtonNephrology On-DemandNo ratings yet
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Enhancing Provider Education and Improving Healthcare Disparities in Chronic Myeloid Leukemia (CML) and Multiple Myeloma (MM) Through A Rural Regional North Carolina Hospital NetworkDocument1 pageEnhancing Provider Education and Improving Healthcare Disparities in Chronic Myeloid Leukemia (CML) and Multiple Myeloma (MM) Through A Rural Regional North Carolina Hospital NetworkNephrology On-DemandNo ratings yet
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Duty Hour Logs Through An AppDocument1 pageDuty Hour Logs Through An AppNephrology On-DemandNo ratings yet
- September 2015Document2 pagesSeptember 2015Nephrology On-DemandNo ratings yet
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Seven - Jan. 2015Document2 pagesSeven - Jan. 2015Nephrology On-DemandNo ratings yet
- October 2015Document2 pagesOctober 2015Nephrology On-DemandNo ratings yet
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- August 2015Document2 pagesAugust 2015Nephrology On-DemandNo ratings yet
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- May-Issue 11Document2 pagesMay-Issue 11Nephrology On-DemandNo ratings yet
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- April-Issue 10Document2 pagesApril-Issue 10Nephrology On-DemandNo ratings yet
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Outpt. Recommendation of Renal Transplant Patients.Document86 pagesOutpt. Recommendation of Renal Transplant Patients.Nephrology On-DemandNo ratings yet
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Pediatric Nephrology WorkforceDocument5 pagesPediatric Nephrology WorkforceNephrology On-DemandNo ratings yet
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- Recurrent GN After TXPDocument8 pagesRecurrent GN After TXPNephrology On-DemandNo ratings yet
- BK Virus - 1Document6 pagesBK Virus - 1Nephrology On-DemandNo ratings yet
- February-Issue 8Document2 pagesFebruary-Issue 8Nephrology On-DemandNo ratings yet
- Kidney BrochureDocument8 pagesKidney BrochureNephrology On-DemandNo ratings yet
- Infections in Solid Organ TransplantDocument14 pagesInfections in Solid Organ TransplantNephrology On-DemandNo ratings yet
- Medical Care 1st Year Post TransplantDocument18 pagesMedical Care 1st Year Post TransplantNephrology On-DemandNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Liver TransplantDocument16 pagesLiver TransplantNephrology On-DemandNo ratings yet
- BK VirusDocument6 pagesBK VirusNephrology On-DemandNo ratings yet
- Cardio Vascular Complications After Kidney Trans.Document9 pagesCardio Vascular Complications After Kidney Trans.Nephrology On-DemandNo ratings yet
- Transplant Immunology - 1Document16 pagesTransplant Immunology - 1Nephrology On-DemandNo ratings yet
- Transplant Immuno - 2Document30 pagesTransplant Immuno - 2Nephrology On-DemandNo ratings yet
- Script - TEST 5 (1st Mid-Term)Document2 pagesScript - TEST 5 (1st Mid-Term)Thu PhạmNo ratings yet
- Explore the rules and history of American football and basketballDocument2 pagesExplore the rules and history of American football and basketballAndrei IoneanuNo ratings yet
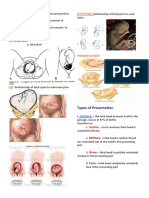
- The 4Ps of Labor: Passenger, Passageway, Powers, and PlacentaDocument4 pagesThe 4Ps of Labor: Passenger, Passageway, Powers, and PlacentaMENDIETA, JACQUELINE V.No ratings yet
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- A Model For Blockchain-Based Distributed Electronic Health Records - 2016Document14 pagesA Model For Blockchain-Based Distributed Electronic Health Records - 2016Asif KhalidNo ratings yet
- Lantern October 2012Document36 pagesLantern October 2012Jovel JosephNo ratings yet
- NAS Drive User ManualDocument59 pagesNAS Drive User ManualCristian ScarlatNo ratings yet
- IkannnDocument7 pagesIkannnarya saNo ratings yet
- Catalogo 4life en InglesDocument40 pagesCatalogo 4life en InglesJordanramirezNo ratings yet
- I CEV20052 Structureofthe Food Service IndustryDocument98 pagesI CEV20052 Structureofthe Food Service IndustryJowee TigasNo ratings yet
- 01 ElectricalDocument15 pages01 ElectricalKrishna KrishNo ratings yet
- TAFJ-H2 InstallDocument11 pagesTAFJ-H2 InstallMrCHANTHANo ratings yet
- Doulci Activator For IOS 9Document2 pagesDoulci Activator For IOS 9Syafiq Aiman100% (2)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Dukic WarehouselayoutsDocument14 pagesDukic Warehouselayoutsrohitkamath7No ratings yet
- 2005 Australian Secondary Schools Rugby League ChampionshipsDocument14 pages2005 Australian Secondary Schools Rugby League ChampionshipsDaisy HuntlyNo ratings yet
- Karnataka Email Id DataDocument5,173 pagesKarnataka Email Id DataSumalatha Venkataswamy100% (6)
- Presentation 1Document13 pagesPresentation 1lordonezNo ratings yet
- Guest Speaker SpeechDocument12 pagesGuest Speaker SpeechNorhana Manas83% (82)
- Hays Grading System: Group Activity 3 Groups KH PS Acct TS JG PGDocument1 pageHays Grading System: Group Activity 3 Groups KH PS Acct TS JG PGkuku129No ratings yet
- New Member OrientationDocument41 pagesNew Member OrientationM.NASIRNo ratings yet
- Nursing Effective Leadership in Career DevelopmentDocument4 pagesNursing Effective Leadership in Career DevelopmentAlan Divine BNo ratings yet
- TypeDocument20 pagesTypeakshayNo ratings yet
- AIESEC - Exchange Participant (EP) GuidebookDocument24 pagesAIESEC - Exchange Participant (EP) GuidebookAnonymous aoQ8gc1No ratings yet
- Glowing Stones in Ancient LoreDocument16 pagesGlowing Stones in Ancient LorerippvannNo ratings yet
- Georgetown University NewsletterDocument3 pagesGeorgetown University Newsletterapi-262723514No ratings yet
- Polystylism in The Context of Postmodern Music. Alfred Schnittke's Concerti GrossiDocument17 pagesPolystylism in The Context of Postmodern Music. Alfred Schnittke's Concerti Grossiwei wuNo ratings yet
- CLNC 2040 Reflection of Assistant ExperiencesDocument4 pagesCLNC 2040 Reflection of Assistant Experiencesapi-442131145No ratings yet
- Abhivyakti Yearbook 2019 20Document316 pagesAbhivyakti Yearbook 2019 20desaisarkarrajvardhanNo ratings yet
- Yoga Practice Guide: DR - Abhishek VermaDocument26 pagesYoga Practice Guide: DR - Abhishek VermaAmarendra Kumar SharmaNo ratings yet
- CH 2 Short Questions IXDocument2 pagesCH 2 Short Questions IXLEGEND REHMAN OPNo ratings yet
- Expectations for Students and ParentsDocument15 pagesExpectations for Students and ParentsJasmine TaourtiNo ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (327)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (13)
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)