Professional Documents
Culture Documents
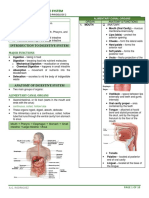
Digestion Absorption and Secretion of The Human GI Tract
Uploaded by
Hani Alex0 ratings0% found this document useful (0 votes)
20 views3 pagesQuick overview of the GI tract functions
Original Title
Digestion Absorption and Secretion of the human GI Tract
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentQuick overview of the GI tract functions
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
20 views3 pagesDigestion Absorption and Secretion of The Human GI Tract
Uploaded by
Hani AlexQuick overview of the GI tract functions
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 3
Explain the processes of digestion, absorption and excretion occurring in the
digestive tract, focusing particularly on fats, carbohydrates, proteins, vitamins
and iron
I.
Mechanical Digestion
a. Initial mechanical digestion is done by mastication in the mouth. Food is ground by the
teeth and manipulated by the tongue, following which the bolus is swallowed
i. Saliva solubilizes the food particles, as digestive enzymes can only act in liquid media
b. Following the entry of food into the stomach, peristaltic movements pass over the
stomach every 15-25 seconds to soften the food and mix it with gastric juices to
produce chyme
c. Progressive gastric emptying releases about 3ml of chime into the duodenum at a time
d. Finally, peristaltic movements of the small intestine mix the chyme with digestive
enzymes and allow contact with the mucosal wall to facilitate absorption
II.
Carbohydrates
a. Digestion
i. Begins in the mouth with secretion
of salivary amylase, which breaks
down starches into maltose,
maltotriose, and dextrins
ii. Salivary amylase is denatured in
the acidic environment of the
stomach
iii. Further digestion in duodenum by
pancreatic amylase
iv. The resultant -dextrins are
digested by dextrinase, a brushborder enzyme which produces
single glucose molecules
v. Sucrose, lactose, and maltose are
digested in the duodenum by
sucrose, lactase, and maltase
respectively
vi. Cellulose is indigestible plant fibre
b. Absorption
i. Digestion
ends
once
monosaccharides
glucose,
fructose,
and
galactose
are
produced as these are absorbable
ii. Fructose is moved into the
absorptive cells of the small
intestine via facilitated diffusion
iii. Glucose and galactose undergo
secondary transport with sodium
iv. Once in the cell, facilitated diffusion moves all three molecules across the membrane
into the capillary network
III.
Lipids
a. Digestion
i. Lingual glands in the tongue secrete lingual lipase, which converts triglycerides into
fatty acids and monoglycerides
ii. Gastric juices contain gastric lipase, which further digests triglycerides
iii. The majority of lipid digestion is in the duodenum, carried out by pancreatic lipase
iv. Before digestion in the small intestine, the lipid globules need to be emulsified in order
to increase the reactive surface area, this is done by the bile salts (chenodeoxycholic
acid, and cholic acid, and their conjugated derivatives) which are amphipathic
b. Absorption
i. Short chain fatty acids (fewer than 12 carbons) easily diffuse into the absorptive cells
of the small intestine and into the lacteals of the villus leading to the lymph system
ii. Long-chain fatty acids combine with the bile salts to form micelles, which are ~2-10nm
in diameter
iii. Once the micelles come in contact with the brush border the monoglycerides and fatty
acids diffuse into the cells, leaving the bile salts behind to continue the process
IV.
V.
VI.
VII.
iv. Micelles also solubilize vitamins A,D,E,K and cholesterol
v. Once long-chain FAs enter the cell they are recombined to form triglycerides,
aggregate with cholesterol and phospholipids, and become coated with proteins,
forming chylomicrons
1. Roughly 80nm diameter and enter the pores of the lacteals to the
thoracic duct
vi. Chylomicrons are broken down by lipoprotein lipase and the products absorbed by the
liver and adipocytes
vii. Bile salts are actively reabsorbed in the ileum and returned to the liver by the portal
vein
Proteins
a. Digestion
i. Digestion begins in the stomach , where a mixture of pepsin and hydrochloric acid
break down peptide bonds
ii. In the duodenum trypsin, chymotrypsin, elastase, and carboxypeptidases continue to
break down proteins
iii. Brush enzymes aminopeptidase and dipeptidase finishes digestion, producing single
amino acids
b. Absorption
i. Single amino acids are absorbed by direct active transport or secondary active
transport (Na-dependant)
ii. Dipeptides and tripeptides are absorbed via secondary active transport (H-dependant)
iii. The amino acids diffuse into the blood supply
Vitamins, water and Electrolyte absorption
a. Most vitamins absorb by passive diffusion, either through micelles or dissolved in water
i. Exception being B12, which binds to intrinsic factor from the stomach
b. Electrolytes
i. Sodium is actively transported out of absorptive cells by basolateral Na-K pumps,
which causes passive diffusion of negatively charged molecules into the cells
ii. Calcium, iron, magnesium, and phosphate are actively transported into the absorptive
cells (see previous weeks for iron and calcium)
c. Water
i. Water is absorbed via osmosis in the small and large intestine. Roughly 8.3 liters is
absorbed by the small intestine daily, another 0.9 is done by the large intestine
Excretion
a. By the time chyme reaches the large intestine it is semisolid as most liquid has been
reabsorbed
b. Now called feces, it is composed of water, inorganic salts, epithelial cells, bacteria, and
indigestible foods
c. In the large intestine electrolytes and some vitamins are absorbed as well as water
Regulation of digestion
a. Cephalic
i. Smell, sight, thought and taste, of food activates neural centres in the cerebral cortex,
hypothalamus, and brain stem
ii. This causes secretion of saliva and vagal stimulation of the stomach to release gastric
juices
b. Gastric
i. Stretch receptors and chemoreceptors in the stomach are activated when the stomach
is distended with food and the pH increases due to buffering by proteins
ii. Nerve impulses cause parietal cells to secrete HCl and the stomach wall to contract
iii. Hormonal regulation by G-cells, which secrete gastrin
1. Stimulated by distention of stomach, pH rise, parasympathetic
activation, or caffeine
2. Gastrin enters bloodstream and reaches target organs of digestive
tract
3. Causes gastric glands to secrete gastric juice, strengthens
esophageal sphincter and relaxes pyloric
4. Gastrin secretion inhibited at pH 2.0, providing optimal pH for pepsin,
and denaturing of proteins
c. Intestinal
i. Neural Regulation
1. Duodenal distension causing enterogastric reflex which increases the
contractilitiy of the stomach by neural inhibition of the PSNS
ii. Hormonal Regulation
1. Cholecystokinin is secreted by CCK cells in the intestine in response
to partially digested proteins and FAs
2. CCK stimulates pancreatic juice secretion and contraction of the
gallbladder which causes bile release
a. Also causes relaxation of the sphincter of Oddi
b. Slows gastric emptying and induces satiety by acting on
hypothalamus
3. Acidic chyme in the duodenum stimulates secretin release from S
cells, which stimulates secretion of bicarbonate rich juices from the
pancreas
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Concrete EssayDocument1 pageConcrete EssayHani AlexNo ratings yet
- Brochure Vue Pacs Clinical AppsDocument8 pagesBrochure Vue Pacs Clinical AppsHani AlexNo ratings yet
- Linus Pauling EssayDocument2 pagesLinus Pauling EssayHani AlexNo ratings yet
- BTS Guidelines For The Investigation and Management of Pulmonary NodulesDocument64 pagesBTS Guidelines For The Investigation and Management of Pulmonary NodulesHARIHARAN NARENDRANNo ratings yet
- Concrete EssayDocument1 pageConcrete EssayHani AlexNo ratings yet
- Brochure Vue Pacs Clinical AppsDocument8 pagesBrochure Vue Pacs Clinical AppsHani AlexNo ratings yet
- Stroke PSDocument5 pagesStroke PSHani AlexNo ratings yet
- ReportDocument7 pagesReportHani AlexNo ratings yet
- Bio Lab - Enzyme ActivityDocument3 pagesBio Lab - Enzyme ActivityHani AlexNo ratings yet
- Bio Lab - Enzyme ActivityDocument3 pagesBio Lab - Enzyme ActivityHani AlexNo ratings yet
- Organic ChemistryDocument1 pageOrganic ChemistryHani AlexNo ratings yet
- Hydrogenase MechanismDocument8 pagesHydrogenase MechanismHani AlexNo ratings yet
- Essay On PIP3Document5 pagesEssay On PIP3Hani AlexNo ratings yet
- Explain How Calcium Homeostasis Is Maintained, and Outline The Common Disorders of ThisDocument3 pagesExplain How Calcium Homeostasis Is Maintained, and Outline The Common Disorders of ThisHani AlexNo ratings yet
- Do Elastic Compression Stockings Lower The Risk of Deep Vein Thrombosis in Over 50 Year Olds Undertaking LongDocument3 pagesDo Elastic Compression Stockings Lower The Risk of Deep Vein Thrombosis in Over 50 Year Olds Undertaking LongHani AlexNo ratings yet
- Motor Neuron LesionsDocument4 pagesMotor Neuron LesionsHani AlexNo ratings yet
- Motor Neuron LesionsDocument4 pagesMotor Neuron LesionsHani AlexNo ratings yet
- Figure 3: The Hydrogen Bonding, and Electrostatic Interactions of TheDocument3 pagesFigure 3: The Hydrogen Bonding, and Electrostatic Interactions of TheHani AlexNo ratings yet
- Monoamine HypothesisDocument2 pagesMonoamine HypothesisHani AlexNo ratings yet
- Beta AmyloidDocument2 pagesBeta AmyloidHani AlexNo ratings yet
- Hydrogenase MechanismDocument8 pagesHydrogenase MechanismHani AlexNo ratings yet
- Report Robert Lefkowitz WorkDocument8 pagesReport Robert Lefkowitz WorkHani AlexNo ratings yet
- Beta AmyloidDocument2 pagesBeta AmyloidHani AlexNo ratings yet
- A Crystallographic Structure-Function Analysis of SH2 Domain Containing Inositol Polyphosphate 5-Phosphatase 2 (SHIP2)Document6 pagesA Crystallographic Structure-Function Analysis of SH2 Domain Containing Inositol Polyphosphate 5-Phosphatase 2 (SHIP2)Hani AlexNo ratings yet
- ReportDocument9 pagesReportHani AlexNo ratings yet
- Explain How Calcium Homeostasis Is Maintained, and Outline The Common Disorders of ThisDocument3 pagesExplain How Calcium Homeostasis Is Maintained, and Outline The Common Disorders of ThisHani AlexNo ratings yet
- Digestion and Absorption OverviewDocument1 pageDigestion and Absorption OverviewHani AlexNo ratings yet
- Pathogenesis of Acute Tubular NecrosisDocument2 pagesPathogenesis of Acute Tubular NecrosisHani AlexNo ratings yet
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (120)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- 5090 s11 QP 11Document20 pages5090 s11 QP 11mstudy123456No ratings yet
- Paragonimus WestermaniDocument3 pagesParagonimus WestermaniHanisha EricaNo ratings yet
- Kamus ManusiaDocument822 pagesKamus ManusiaAhmad Abdullah100% (1)
- One Hundred Magic-UsersDocument4 pagesOne Hundred Magic-UsershigherdepthsNo ratings yet
- Vaginal Examination Wit RationaleDocument1 pageVaginal Examination Wit RationaleAna Maria Teresa H RollanNo ratings yet
- Nematode StructureDocument31 pagesNematode StructureShadab HanafiNo ratings yet
- WJMH 32 110Document6 pagesWJMH 32 110Yacine Tarik AizelNo ratings yet
- Cordlife BrochureDocument16 pagesCordlife BrochureMelodie YlaganNo ratings yet
- Haematology and Biochemistry in Alpacas and Llamas: Red Blood CellsDocument6 pagesHaematology and Biochemistry in Alpacas and Llamas: Red Blood CellsDarwin Antezana De la RosaNo ratings yet
- Percubaan Kedah Peraturan Permarkahan Sains Paper 2 Set1Document12 pagesPercubaan Kedah Peraturan Permarkahan Sains Paper 2 Set1Ishraqi IlyasNo ratings yet
- Fitness Form & Hospital ListDocument24 pagesFitness Form & Hospital ListAbhijeetMhatreNo ratings yet
- Lesson 4 Digestive SystemDocument10 pagesLesson 4 Digestive SystemJulio De GuzmanNo ratings yet
- 03etiology and Pathogenesis of Neonatal EncephalopathyDocument22 pages03etiology and Pathogenesis of Neonatal EncephalopathyDaniela MuñozNo ratings yet
- U R H O B O (T O) E N G L I S H 8-2-12 (RE-EDITED) For Upload PDFDocument64 pagesU R H O B O (T O) E N G L I S H 8-2-12 (RE-EDITED) For Upload PDFAghogho Biakolo100% (1)
- Topographic Anatomy of Abdominal OrgansDocument18 pagesTopographic Anatomy of Abdominal OrgansHasnain IdreesNo ratings yet
- ST Louis Cty FairDocument36 pagesST Louis Cty FairGarrett RossNo ratings yet
- Tooth-Support Over Dentures: An Approach To Preventive ProsthodonticsDocument5 pagesTooth-Support Over Dentures: An Approach To Preventive ProsthodonticsAdvanced Research PublicationsNo ratings yet
- Pneumo HemothoraxDocument126 pagesPneumo HemothoraxLyra Jan Roo100% (1)
- Bulletin - Diseases of Mud Crabs in India - InnerDocument36 pagesBulletin - Diseases of Mud Crabs in India - InnerDr. K.P.JithendranNo ratings yet
- Stigma in Access To Antiretroviral Therpy in Abuja Nigeria The Importance of Social Connections PDFDocument318 pagesStigma in Access To Antiretroviral Therpy in Abuja Nigeria The Importance of Social Connections PDFKingsley OturuNo ratings yet
- Urinary System: Human Anatomy & Physiology (Biol 20025)Document21 pagesUrinary System: Human Anatomy & Physiology (Biol 20025)Aila Grace PeriodicoNo ratings yet
- What Is Animal Identification SystemDocument51 pagesWhat Is Animal Identification SystemRohit SachdevaNo ratings yet
- 2 Sets Word Problems PrintDocument2 pages2 Sets Word Problems PrintS. SHUMAILA ZEHRA/TCHR/EKNNCNo ratings yet
- 4eso Unit 5Document5 pages4eso Unit 5Llanetes Cortes100% (1)
- NLR Proteins - Methods and ProtocolsDocument269 pagesNLR Proteins - Methods and ProtocolsG DelisNo ratings yet
- Revise Anatomy in 15 Days K Raviraj VD AgrawalDocument7 pagesRevise Anatomy in 15 Days K Raviraj VD AgrawalShehnaaz Khan29% (14)
- The Patient Created By: Chloe Coleman Screenplay By: Chloe ColemanDocument9 pagesThe Patient Created By: Chloe Coleman Screenplay By: Chloe Colemanapi-263876709No ratings yet
- Seduced by A Volleyball Goddess 1Document11 pagesSeduced by A Volleyball Goddess 1Gar LewisNo ratings yet
- Affirmative To Being A VegetarianDocument10 pagesAffirmative To Being A VegetarianIra ajahNo ratings yet
- BronchiolitisDocument4 pagesBronchiolitistingtingcrazyNo ratings yet