Professional Documents
Culture Documents
Class IV Composite Repair for Heavily Textured Central Incisor
Uploaded by
ventynataliaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Class IV Composite Repair for Heavily Textured Central Incisor
Uploaded by
ventynataliaCopyright:
Available Formats
Accreditation Essentials
Class IV Composite Repair
A Heavily Textured Central Incisor
Robert L. Strain, DDS
Key Words: Class IV fracture, composite, incisal, Accreditation Case Type IV
Directly bonded restorations
can satisfy a patient in a single
appointment, often with little
or no tooth reduction.
14
Spring 2014 Volume 30 Number 1
Introduction
Conservative dentistry can solve many esthetic problems. Directly
bonded restorations can satisfy a patient in a single appointment,
often with little or no tooth reduction.
Composite materials currently available exhibit outstanding
characteristics for duplicating the appearance of natural teeth.
Hybrid composites exhibit excellent tensile strength and blending characteristics. Microfilled composite resins exhibit outstanding characteristics for duplicating the appearance of natural tooth
structure, especially the characteristics of translucency and reflectance.
There are occasions when a tooth could be restored with a ceramic restoration, but a direct composite is still the preferred option.1,2 Two such situations are when the pulp of an injured tooth
has not sufficiently matured, and when gingival tissues have not
adequately receded to form a mature gingival crest. These situations occur in pre-adolescent and adolescent patients.
Direct composite restorations can be used to replace substantial amounts of tooth structure if proper design, occlusal forces,
and patient habits are taken into consideration.
This article addresses AACD Accreditation Case Type IV (in this
particular case, treatment of an incisal edge fracture on a left central incisor). The case demonstrates the techniques for disguising
the fracture line and replicating highly textured surface enamel.
Mid-treatment modifications to the restoration and the adjacent
central incisor are discussed.
Figure 1a: The before smile view shows the large fracture of
tooth #9.
Strain
Figure 1b: The after smile view shows a natural, polychromatic,
and esthetic result.
Patient History and Chief Complaint
The patient was a healthy 10-year-old male with an American
Society of Anesthesiologists (ASA) Type I health evaluation.
He had no medical contraindications to dental treatment.
The patient had a history of minimal preventive and restorative dentistry. He had developing dentition with incomplete
eruption and had not had orthodontics. His left maxillary
central incisor had sustained a minor Class IV fracture of the
mesial incisal edge and the left central incisor had sustained
a major Class IV fracture involving both incisal edges in a
schoolyard accident (Figs 1a-2b). He was initially referred to
another dentist who recommended a three-month wait to see
if the tooth remained vital prior to placing a crown.
Diagnosis and Treatment Plan
Figure 2a: The 1:2 retracted preoperative view.
Diagnosis
The patient presented with a horizontally fractured left central incisor involving both incisal corners. This accounted for
35% to 40% of the missing tooth structure. A very small fracture was present on the right central incisor. Strong mamelons
remained on the right central incisor and the lateral incisors.
There was no visible pulp exposure. Tooth #9 responded as being vital to a cold sensitivity test.
Radiographs taken as part of the examination included
maxillary anterior periapicals. The required AACD guideline
photographs were obtained at the initial cosmetic consultation. Impressions for diagnostic models were made.3 A hard
and soft tissue exam revealed no underlying hard or soft tissue
pathology. An occlusal evaluation revealed a Class I molar relationship and a developing Class I cuspid relationship. There
was an approximately 40% overbite with no excess anterior
overjet.
Figure 2b: The 1:2 retracted postoperative view.
Journal of Cosmetic Dentistry
15
Accreditation Essentials
No additional fractures within the damaged teeth
or adjacent teeth were visible on the radiographs or
with transillumination. The patient had no anterior
enamel wear. Mamelons were still present on the lateral incisors and right central incisor. The incisors were
heavily textured both macroscopically (depressions)
and microscopically (striae), which added complexity
to polishing the finished restorations.
Gingival heights of #8 and #9 were nearly symmetrical, with slight differences in gingival architecture
that would not affect a finished restoration. There was
an apparent slight mesial angulation of both teeth,
which might correct as the canines completed eruption. Otherwise, orthodontics could provide better
angulation for these teeth. Tooth #8 had considerable
variations in hues, chroma, and opacity/translucency.
All teeth remained vital three months after the traumatic injury. The parents chose to wait despite being
advised to treat immediately. They did choose to complete treatment with conservative cosmetic bonding as
described below.
Treatment Plan
The patient had a pleasant display of teeth when smiling, other than the fractured central incisors, which
was the chief complaint. He smiled easily, even with
the damage. The advantages of direct composite restorations were discussed. The patients mother was
encouraged to have this treatment completed as soon
as possible.
Initially, I believed that an excellent result could be
obtained with minor enamelplasty on #8 and direct
resin on #9. Over the next couple of years, some improvement in the axial angle of the incisors could be
expected to partially correct the angled incisal edges.
The initial treatment plan and treatment was as follows:
minor incisal enamelplasty at #8
mesial incisal distal (MID) composite at #9.
After completion of this treatment and advice from
an Accreditation mentor that the case could be better,
a decision was made to create more ideal outline form.
Additions would be made to both central incisors.
The revised treatment plan and treatment was as
follows:
mesial incisal composite at #8
MID at #9.
16
Spring 2014 Volume 30 Number 1
Treatment
Preparation
A diagnostic wax-up for #9 was developed (based upon the initial treatment plan) and a polyvinyl silane (PVS) (Exafast; GC America; Alsip, IL)
matrix4 was made from this model prior to the treatment appointment
(Fig 3).
A 2-mm shoulder preparation with a .5-mm depth was placed beyond
the fracture line on #9 with a 856L-016 diamond bur (Henry Schein; Melville, NY). A 1-mm bevel was placed on the shoulder. Then a series of irregular feathered bevels was placed randomly on the facial surface.
Minor enamelplasty was performed on #8 to determine whether proper esthetics and occlusion would result solely by restoring #9.
Tooth #9 was restored to match the recontoured #8. Matrix strips
(Henry Schein) were placed to isolate individual teeth. The surfaces to be
bonded were etched with 40% phosphoric acid gel (Henry Schein). They
were then coated with a two-step bonding system (Clearfil SE Bond, Kuraray Noritake; Okayama, Japan) containing a water-based primer.
Reference to the color maps (Fig 4) can help in understanding the
incremental build,5,6 as follows:
1. The internal dentin mamelons were reestablished with A-1 hybrid
composite (Venus, Heraeus Kulzer; South Bend, IN), taking care to
overlap the fracture line with the composite. Three individual lobes
were developed and light-cured to mimic natural teeth and the
adjacent central incisor. A hybrid composite was chosen because of
its distinct benefit over microfill composites due to its ability to mask
sharp edges, preventing the dark background of the mouth from
revealing the fracture line.
2. The PVS matrix was placed and a very thin shell was built for the lingual wall in light translucent microfill composite (Renamel, Cosmedent; Chicago, IL).
3. The facial surface was built up in stages, beginning with the most
gingival area, using B1 microfill composite (Renamel). Small depressions were left near the incisal to be filled with very minimal ochre
chroma (Kolor + Plus, Kerr; Orange, CA) covered by light translucent
microfill composite (Renamel).7 Because of the tooths high texture,
the outer surface texture was modified to an irregular, non-worn
texture using the tip of a #2 flat sable brush (Loew-Cornell; Erlanger,
NY) just prior to curing. The translucent nature of these microfill
resins allow the dentin layers to show through, creating excellent
blending and high polishability.
4. The mesial and distal contacts on #9 were developed with B-1 microfill utilizing clear plastic matrix strips (Henry Schein) separating the
tooth from adjacent teeth.
5. The resulting buildup appeared too low in value, so the lingual wall
and some of the translucent composite were then replaced with white
enamel-colored resin composite (Renamel). This change blocked the
dark background show-through and provided the desired result.
Strain
Figure 3: The putty matrix in place, displaying the random feathered bevels
to mask the finish line. Bonding resin has been applied.
Initial contouring to establish primary anatomy
was completed with a medium-grit flame diamond
(#260.8, Premier Dental; Plymouth Meeting, PA).
An attempt was made to first develop the vertical
anatomy, then horizontal and irregular features were
placed with a round-tipped, multi-fluted #7378 bur
(SS White; Lake Township, NJ), used with a very light
touch and much discretion. Margins only were finished initially with a coarse-grit polishing disc (SofLex; 3M ESPE; St. Paul, MN) rotating toward the
margin. No medium- or fine-grit discs were applied
due to the desire to retain the irregular reflection pattern to match #8. The tip of a fine-grit flexible point
(FlexiPoint, Cosmedent) was used to smooth recessed
surface areas. An initial polish was established with a
goat hair with chamois wheel (#10250022HP, Cosmedent) brush mounted on a straight mandrel. An effort
was made to minimize pressure to avoid flattening the
texture that had been created in the previous step. A
second polish step was completed using a chamois/
brush combination on a straight mandrel, with a polishing paste suitable for microfill enamel.6,8
A photograph was taken for study prior to the patients return for post-treatment photos, which was
to occur after tooth #8 had rehydrated. The patients
mother expressed her delight with the results. The patient enjoyed the attention he received posing for his
after photos.
Refinement
Figure 4: The color maps show the layers of composite used in the
restoration. The frontal view shows a cutaway portion and the surface layer.
There are occasions when a tooth could
be restored with a ceramic restoration,
but a direct composite is still the
preferred option.
At the follow-up visit, minor facial anatomical corrections were made based upon a study of the photograph taken at the end of the previous visit. The restoration was repolished and new photographs were
taken.
This case was shown in its non-final form at an
Advanced Accreditation Workshop at the 2013 AACD
Annual Meeting. Comments from other attendees
and the instructor/mentor were extremely positive,
but it was suggested that the case could be improved.
The patient was very willing to return to the office so
that changes could be made as detailed below.
Despite an excellent match to tooth #8, after reviewing the postoperative photos, it was determined
that the patient would benefit even more if the mesial incisal corners of both #8 and #9 were restored to
more ideal tooth form in accordance with Accreditation criteria.1 This would allow for a more attractive
incisal embrasure. Also, there was slightly too much
ochre chroma. There was a bit of excessive flash past
the mesial margin.
Journal of Cosmetic Dentistry
17
Accreditation Essentials
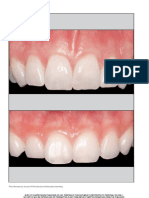
Figure 5: Side-by-side comparison showing the initial result compared to intermediate completion and the final restoration where #8 also
has a small composite repair on the mesial incisal.
A simple irregular bevel was placed on the mesial incisal of both teeth. An area of excess chroma was removed
with the blunt end of a diamond. The areas were restored
with B1 microfill composite (Renamel) bonded with
bonding resin (only). The gingival mesial margin was
trimmed with a #12B surgical blade (Henry Schein) and
smoothed with a fine-grit sandpaper strip (Sof-Lex).
The patient was rescheduled to return the following
week and a new set of final AACD Accreditation photographs were taken. The stages to achieve the final restoration are compared in Figure 5.
Summary
Direct bonded composite resin restorations are a conservative and valuable service that can be provided at a very
reasonable cost. This case demonstrated the solution to
two problems that dentists encounter in correcting Class
IV enamel fractures: 1) hiding the fracture line and 2) replicating heavy surface texture (Figs 6a-7b).
Having this treatment option available allows patients
to enjoy an attractive smile and can delay more extensive
removal of tooth structure, which could weaken the tooth
and create greater potential for pulpal necrosis. For juveniles, it allows maturation of gingival architecture and additional dentin development should more invasive tooth
preparation be desired in the future. For the dentist, it is
an opportunity to maximize the application of todays
materials to mimic nature and provide great personal satisfaction.
Figure 6a: The large Class IV fracture as seen on a 1:1 view.
Acknowledgment
This case, prior to treatment plan revisions, was presented at an
Accreditation Workshop at the 2013 AACD Annual Scientific
Session. Comments by Bradley J. Olson, DDS, FAACD, during
and after the seminar were instrumental in the final results.
The author also thanks James Peyton, DDS, FAACD, for his
assistance in preparing the color maps and this article.
18
Spring 2014 Volume 30 Number 1
Figure 6b: The 1:1 postoperative image shows the intricate surface
texture that had to be duplicated.
Strain
References
1. Spoor R. The use of direct composites in the conservative esthetic correction of the anterior dentition. J Cosmetic Dent. 2006
Fall;22(3):90-6.
2. Malterud M. Minimally invasive restorative dentistry: a biomimetic approach. Pract Proced Aesthet Dent. 2006 Aug;18(7):40914.
3. American Academy of Cosmetic Dentistry (AACD). Diagnosis
and treatment evaluation in cosmetic dentistry: a guide to Accreditation criteria. Madison (WI): AACD, 2001.
4. Fahl N Jr, Denehy G, Jackson R. Protocol for predictable restora-
Figure 7a: Full-face preoperative view; the large fracture is clearly visible.
tion of anterior teeth with cosmetic resin. Pract Proced Aesthet
Dent. 1995;7(8):13-21.
5. Fahl N Jr. Coronal reconstruction of a severely compromised central incisor with composite resins: a case report. J Cosmetic Dent.
2010 Spring;26(1):92-113.
6. LeSage B, Milnar F, Wohlberg J. Achieving the epitome of cosmetic art: creating natural tooth esthetics, texture, and anatomy using appropriate preparation and layering techniques. J Cosmetic
Dent. 2008 Fall;24(3):132-41.
7. Blank J. Creating translucent edge effects and maverick internal
tints using microhybrid resin. Pract Proced Aesthet Dent. 2006
Mar;18(2):31-6.
8. Peyton JH. Finishing and polishing techniques: direct composite resin restorations. Pract Proced Aesthet Dent. 2004
May;16(4):293-8.
jCD
Figure 7b: The full-face postoperative view shows a very happy patient.
Having this treatment option available
allows patients to enjoy an attractive
smile and can delay more extensive
removal of tooth structure.
Dr. Strain maintains a practice in Rancho Mirage, California.
Disclosure: The author did not report any disclosures.
Journal of Cosmetic Dentistry
19
Accreditation Essentials
Examiners Commentary
Microesthetics and Case Type IV
J.A. Reynolds, DDS, AAACD
This case type tests the clinicians ability to seamlessly blend and
shape composite resin with the natural tooth.
Figure 1: Classic incisal fracture.
Figure 2: Microesthetics: Note the blending of the shading and
texture of the resin.
20
Spring 2014 Volume 30 Number 1
uccessful completion of Accreditation
Case Type IV requires using composite resin to repair a Class IV fracture or
close a diastema of at least 1 mm. The Class
IV resin must replace at least 10% of the facial
structure of an anterior tooth, and this young
patient met the criteria.1 This case type tests
the clinicians ability to seamlessly blend and
shape composite resin with the natural tooth.
There should be special emphasis on managing the microesthetics of shade selection, surface finish, luster, and fracture line block-out.
Global smile design principles play less of a
role in the examiners evaluations.
This is an example of the candidate choosing the right case for Accreditation submission. Although Dr. Strain had some detailed
surface textures to emulate, varying color characterizations on the contralateral tooth were
minimal. He chose a combination of hybrid
Reynolds/Strain
and microfill composites to combine strength and
enamel replication.2 Using a long, irregular bevel to
create a gradual transition from sound tooth structure
to the restoration, he did a good job overcoming the
glass effect, a graying at the margin that can occur
when blending composite over a bevel.3
If preoperative and postoperative photographic
documentation are used in both the planning and
final analysis of treatment, the level of dentistry we
provide for our patients will certainly improve. Dr.
Strains successful Accreditation case is no exception.
Self-analysis is an important step in building skill
level and confidence. The Accreditation journey is an
additional way to continue growth through consistent
guidance and mentorship. Dr. Strains conservative
use of composite resin will serve this young patient
for many years to come.
References
1. American Academy of Cosmetic Dentistry (AACD). Diagnosis
and treatment evaluation in cosmetic dentistry: a guide to Accreditation criteria. Madison (WI): AACD; 2001.
The Accreditation Examiners noted the following
deficiencies during the examination:
Criterion #44: Does the surface exhibit
the appropriate finish, polish, and luster?
The surface of the restoration appeared
slightly pitted with some embedded blue
polishing residue remaining.
Criterion #51: Has underlying tooth color
been properly managed to allow for an
optimal cosmetic result? Examiners noted
that the fracture line could have been
blocked out more completely.
Criterion #53: Is the color (hue, chroma,
value) selection appropriate/natural, not
monochromatic? The chroma appeared
high in the middle third as compared to
the contralateral tooth.
2. Miller M. Universal materialsdo they really exist? J Acad Gen
Dent. 2013 Sept-Oct 3013;61(6):14-5.
3. Helvey GA. The value of a restoration. Inside Dent. 2013
Nov;9(11):80-4.
jCD
Dr. Reynolds is an AACD Accredited Member and has been an AACD Accreditation Examiner since
2003. He practices in Franklin, Tennessee.
Disclosure: The author did not report any disclosures.
Journal of Cosmetic Dentistry
21
You might also like
- Demin/Remin in Preventive Dentistry: Demineralization By Foods, Acids, And Bacteria, And How To Counter Using RemineralizationFrom EverandDemin/Remin in Preventive Dentistry: Demineralization By Foods, Acids, And Bacteria, And How To Counter Using RemineralizationNo ratings yet
- Clinical Cases in Restorative and Reconstructive DentistryFrom EverandClinical Cases in Restorative and Reconstructive DentistryRating: 5 out of 5 stars5/5 (1)
- Supra-Gingival Minimally Invasive Dentistry: A Healthier Approach to Esthetic RestorationsFrom EverandSupra-Gingival Minimally Invasive Dentistry: A Healthier Approach to Esthetic RestorationsRating: 5 out of 5 stars5/5 (1)
- Biomechanics in Restorative DentistryDocument34 pagesBiomechanics in Restorative DentistryUlfa RahmaNo ratings yet
- 2013 Direct Anterior Composites A Practical GuideDocument16 pages2013 Direct Anterior Composites A Practical Guidemaroun ghalebNo ratings yet
- Nanohybrid Versus Nano LL Composite in Class I CavitiesDocument5 pagesNanohybrid Versus Nano LL Composite in Class I CavitiessonygabrielNo ratings yet
- ISSN: 0975-833X: Research ArticleDocument9 pagesISSN: 0975-833X: Research ArticleSuryo HannaNo ratings yet
- ReviewDocument6 pagesReviewArchana SrinivasanNo ratings yet
- Relining and Rebasing of Complete DenturesDocument28 pagesRelining and Rebasing of Complete DenturesPurnama SyahbaniNo ratings yet
- Dental Update - Periodontal Splinting in General Dental PracticeDocument7 pagesDental Update - Periodontal Splinting in General Dental PracticeJacob_Fletcher_529No ratings yet
- Advanced Restorative Dentistry A Problem For The ElderlyDocument8 pagesAdvanced Restorative Dentistry A Problem For The ElderlyAli Faridi100% (1)
- 16 Access Related Endodontic Mishaps.20170115064301Document8 pages16 Access Related Endodontic Mishaps.20170115064301Amrutha DasariNo ratings yet
- Volumetric Shrinkage and Film THDocument8 pagesVolumetric Shrinkage and Film THcalebleon101113No ratings yet
- Principles of Cavity PreparationDocument5 pagesPrinciples of Cavity Preparationمعاذ العسافNo ratings yet
- Dahl's ApplianceDocument7 pagesDahl's AppliancerekabiNo ratings yet
- Mucogingival Conditions in The Natural DentitionDocument10 pagesMucogingival Conditions in The Natural DentitionMartty BaNo ratings yet
- Internal Root Resorption - A ReviewDocument15 pagesInternal Root Resorption - A Reviewjaime097830690% (1)
- Operative DentistryDocument51 pagesOperative Dentistryqra_beliebersNo ratings yet
- Maciej Zarow Metal Post and Core How To Improve Aesthetics Via WWW Styleitaliano OrgDocument27 pagesMaciej Zarow Metal Post and Core How To Improve Aesthetics Via WWW Styleitaliano OrgghfhfdghNo ratings yet
- Starb Urst BevelDocument4 pagesStarb Urst BevelventynataliaNo ratings yet
- Nano DentistryDocument6 pagesNano Dentistrypriyanka shelkeNo ratings yet
- Dan Lazar Workflow Composite Veneering On Non Vital Teeth ViaDocument12 pagesDan Lazar Workflow Composite Veneering On Non Vital Teeth Viaclaudia360No ratings yet
- Molar Incisor Hypomineralization Supplementary, Restorative, Orthodontic, and Esthetic Long-Term Treatment 2019Document6 pagesMolar Incisor Hypomineralization Supplementary, Restorative, Orthodontic, and Esthetic Long-Term Treatment 2019player osamaNo ratings yet
- Posterior CompositeDocument21 pagesPosterior CompositeNaji Z. ArandiNo ratings yet
- Contacts and ContoursDocument73 pagesContacts and ContoursKasturi VenkateswarluNo ratings yet
- Speeds in DentistryDocument38 pagesSpeeds in DentistryRiya Jain100% (1)
- Challenges in dentin bondingDocument11 pagesChallenges in dentin bondingDanish SattarNo ratings yet
- Modern Dental Ceramics: An OverviewDocument6 pagesModern Dental Ceramics: An OverviewDilesh PradhanNo ratings yet
- Papper PeriodDocument12 pagesPapper PeriodLoretoReyesMoralesNo ratings yet
- Direct Cuspal CoverageDocument8 pagesDirect Cuspal CoverageLuLu NikhlaturNo ratings yet
- Rethinking FerruleDocument10 pagesRethinking FerruleteodudeNo ratings yet
- Dr. Samahi's lecture on post-insertion denture problems and follow-up visitsDocument10 pagesDr. Samahi's lecture on post-insertion denture problems and follow-up visitsRahul MahajanNo ratings yet
- Crown & Bridge 13Document6 pagesCrown & Bridge 13reham_ali31No ratings yet
- Fiber-Reinforced Onlay Composite (Unlocked by WWW - Freemypdf.com)Document7 pagesFiber-Reinforced Onlay Composite (Unlocked by WWW - Freemypdf.com)Adrian DjohanNo ratings yet
- Recent Criterias of Tooth Preparation inDocument6 pagesRecent Criterias of Tooth Preparation inFelyciaNo ratings yet
- Clinical Evaluation of Abutment Teeth of Removable PartialDocument7 pagesClinical Evaluation of Abutment Teeth of Removable PartialAlex KwokNo ratings yet
- Articulators and Related InstrumentsDocument4 pagesArticulators and Related InstrumentsUmut ASLANNo ratings yet
- MANAGING DENTAL CARE FOR SENIOR PATIENTSDocument77 pagesMANAGING DENTAL CARE FOR SENIOR PATIENTSKulashekar ReddyNo ratings yet
- Newer Advances in Glass Ionomer Cement A Review PDFDocument5 pagesNewer Advances in Glass Ionomer Cement A Review PDFانس سامي عوادNo ratings yet
- Notes On Biological Considerations of Restorative DentistryDocument5 pagesNotes On Biological Considerations of Restorative DentistryTracie YWNo ratings yet
- Etched Cast RestorationsDocument41 pagesEtched Cast Restorationssharanya chekkarrajNo ratings yet
- Dentin Bonding Agents - An OverviewDocument4 pagesDentin Bonding Agents - An OverviewIOSRjournalNo ratings yet
- Direct Cuspal-Coverage Posterior Resin Composite Restorations: A Case ReportDocument8 pagesDirect Cuspal-Coverage Posterior Resin Composite Restorations: A Case ReportDinar ArdhananeswariNo ratings yet
- Endo Crown: An Approach For Restoring Endodontically Treated Right Mandibular First Molars With Large Coronal Destruction - A Case ReportDocument7 pagesEndo Crown: An Approach For Restoring Endodontically Treated Right Mandibular First Molars With Large Coronal Destruction - A Case ReportIJAR JOURNALNo ratings yet
- 5-Plaque and CalculusDocument174 pages5-Plaque and CalculusAJPEDO LIFE100% (1)
- Good Occlusal Practice in Restorative DentistryDocument3 pagesGood Occlusal Practice in Restorative DentistryCarmen Breban CirțiuNo ratings yet
- Incisal GuidanceDocument5 pagesIncisal Guidancejinny1_0No ratings yet
- Deliperi S - PPAD - 2005 PDFDocument9 pagesDeliperi S - PPAD - 2005 PDFAlfredo PortocarreroNo ratings yet
- Department of Conservative Dentistry 2009 FinalDocument160 pagesDepartment of Conservative Dentistry 2009 FinalDr. Nikhil saran67% (3)
- Bonded Composites Versus Ceramic Veneers PDFDocument7 pagesBonded Composites Versus Ceramic Veneers PDFAnnaAffandieNo ratings yet
- Erosion Abrasion Attrition and Abfrcation1Erosion Abrasion Attrition and Abfrcation1Document82 pagesErosion Abrasion Attrition and Abfrcation1Erosion Abrasion Attrition and Abfrcation1Madalina A DobreNo ratings yet
- Treating The Mother of Black Triangles With Bioclear VeneersDocument4 pagesTreating The Mother of Black Triangles With Bioclear VeneersThe Bioclear ClinicNo ratings yet
- Material Options For Class II Composite Restorations - Varied Clinical Parameters Require Different TechniquesDocument6 pagesMaterial Options For Class II Composite Restorations - Varied Clinical Parameters Require Different TechniquesMohammed NabeelNo ratings yet
- Precision attachments overviewDocument4 pagesPrecision attachments overviewPhoebe DavidNo ratings yet
- Intracanal MedicamentDocument11 pagesIntracanal MedicamentAsh PeiNo ratings yet
- Cavity design techniques for optimizing Class IV composite restorationsDocument6 pagesCavity design techniques for optimizing Class IV composite restorationselokfaiqNo ratings yet
- The Standardized-Taper Root Canal Preparation - Part 2. GT File Selection and Safe Handpiece-Driven File UseDocument9 pagesThe Standardized-Taper Root Canal Preparation - Part 2. GT File Selection and Safe Handpiece-Driven File UseMaria VeronicaNo ratings yet
- Dahl ConceptDocument3 pagesDahl ConceptmusaabsiddiquiNo ratings yet
- Esthetic Failure in Implant DentistryDocument20 pagesEsthetic Failure in Implant Dentistrykavya ravuriNo ratings yet
- Temporary and Permanent SplintingDocument7 pagesTemporary and Permanent SplintingGanisht AzmiNo ratings yet
- Principles of Occlusion in Implant Dentistry PDFDocument7 pagesPrinciples of Occlusion in Implant Dentistry PDFnakul wareNo ratings yet
- Laser-Assisted Removal of All Ceramic Fixed Dental Prostheses: A Comprehensive ReviewDocument7 pagesLaser-Assisted Removal of All Ceramic Fixed Dental Prostheses: A Comprehensive ReviewValeria CrespoNo ratings yet
- Dental BS Delta 1500 PPO Benefit Summary 2018Document4 pagesDental BS Delta 1500 PPO Benefit Summary 2018deepchaitanyaNo ratings yet
- Single Tooth ImplantsDocument82 pagesSingle Tooth ImplantstomdienyaNo ratings yet
- Complicated ProstheticsDocument9 pagesComplicated Prostheticscata056No ratings yet
- Digital Versus Conventional Impressions in Fixed Prosthodontics: A ReviewDocument7 pagesDigital Versus Conventional Impressions in Fixed Prosthodontics: A Reviewruthy arias anahuaNo ratings yet
- Review Restoration EndoDocument9 pagesReview Restoration EndotarekrabiNo ratings yet
- Hemisection of A Severely Decayed Mandibular Molar: A Case ReportDocument4 pagesHemisection of A Severely Decayed Mandibular Molar: A Case Reportkartika tiaraNo ratings yet
- Mixed Dentition Analysis. / Orthodontic Courses by Indian Dental AcademyDocument81 pagesMixed Dentition Analysis. / Orthodontic Courses by Indian Dental Academyindian dental academyNo ratings yet
- Ijcmr 2369Document7 pagesIjcmr 2369Ngọc LinhNo ratings yet
- Reading MaterialDocument11 pagesReading MaterialShobhana RamachandranNo ratings yet
- 11 - Novel Decision Tree Algorithms For The Treatment Planning of Compromised TeethDocument10 pages11 - Novel Decision Tree Algorithms For The Treatment Planning of Compromised TeethkochikaghochiNo ratings yet
- Splinting Teeth - A Review of Methodology and Clinical Case ReportsDocument4 pagesSplinting Teeth - A Review of Methodology and Clinical Case ReportsRishabh Madhu SharanNo ratings yet
- Assignment 3 - Kori FrederickDocument3 pagesAssignment 3 - Kori Frederickapi-250117740No ratings yet
- Inlays & Onlays, The Unsung Heroes: What Are They?Document6 pagesInlays & Onlays, The Unsung Heroes: What Are They?MADANo ratings yet
- Emax-Press-Monolithicsol Gi en - 672600 Rev1Document86 pagesEmax-Press-Monolithicsol Gi en - 672600 Rev1Fabio WenoNo ratings yet
- Concept: Captek™ Are Crowns and Bridges That Mimic and Surpass Natural Teeth in Esthetic and FunctionDocument50 pagesConcept: Captek™ Are Crowns and Bridges That Mimic and Surpass Natural Teeth in Esthetic and FunctionPolet Aline Sánchez SosaNo ratings yet
- Laminates AND Veneers: Dr. Sakshi Rawal Department of Prosthodontics MDS II YearDocument76 pagesLaminates AND Veneers: Dr. Sakshi Rawal Department of Prosthodontics MDS II Yearsapna100% (2)
- Dental DecksDocument84 pagesDental Deckspriyaedwin56% (9)
- Fully Digital Workflow, Integrating Dental Scan, Smile Design and CAD-CAM: Case ReportDocument13 pagesFully Digital Workflow, Integrating Dental Scan, Smile Design and CAD-CAM: Case ReportCarlosChavezRiosNo ratings yet
- Precision Attachments (2) PRDocument23 pagesPrecision Attachments (2) PRpriyaNo ratings yet
- Kerr v. Ultradent ProductsDocument57 pagesKerr v. Ultradent ProductsPriorSmartNo ratings yet
- Connector Design PrinciplesDocument24 pagesConnector Design PrinciplesVikas Aggarwal100% (1)
- Functional Crown Lengthening Surgery Periodontic and Prosthodontic ConsiderationsDocument5 pagesFunctional Crown Lengthening Surgery Periodontic and Prosthodontic ConsiderationsNajeeb UllahNo ratings yet
- Kishor's PG ProfileDocument22 pagesKishor's PG ProfileKishor KumarNo ratings yet
- Cementation All Ceramics PDFDocument5 pagesCementation All Ceramics PDFMarius OprișorNo ratings yet
- Marginal Configurations in Fixed Partial DenturesDocument37 pagesMarginal Configurations in Fixed Partial DenturesSonila JosephNo ratings yet