Professional Documents
Culture Documents
Cerebral Aneurysm Arteriovenous Malformation: Signs and Symptoms
Uploaded by
MohammadAwitOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Cerebral Aneurysm Arteriovenous Malformation: Signs and Symptoms
Uploaded by
MohammadAwitCopyright:
Available Formats
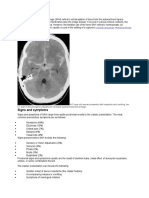
The term subarachnoid hemorrhage (SAH) refers to extravasation of blood into the subarachnoid space
between the pial and arachnoid membranes (see the image below). It occurs in various clinical contexts,
the most common being head trauma. However, the familiar use of the term SAH refers to nontraumatic
(or spontaneous) hemorrhage, which usually occurs in the setting of a rupturedcerebral
aneurysm or arteriovenous malformation (AVM).
A 47-year-old woman presented with headache and vomiting; her
CT scan in the emergency department revealed subarachnoid hemorrhage.
Signs and symptoms
Signs and symptoms of SAH range from subtle prodromal events to the classic presentation. The most
common premonitory symptoms are as follows:
Headache (48%)
Dizziness (10%)
Orbital pain (7%)
Diplopia (4%)
Visual loss (4%)
Signs present before SAH include the following:
Sensory or motor disturbance (6%)
Seizures (4%)
Ptosis (3%)
Bruits (3%)
Dysphasia (2%)
Prodromal signs and symptoms usually are the result of sentinel leaks, mass effect of aneurysm
expansion, emboli, or some combination thereof.
The classic presentation can include the following:
Sudden onset of severe headache (the classic feature)
Accompanying nausea or vomiting
Symptoms of meningeal irritation
Photophobia and visual changes
Focal neurologic deficits
Sudden loss of consciousness at the ictus
Seizures during the acute phase
Physical examination findings may be normal or may include the following:
Mild to moderate BP elevation
Temperature elevation
Tachycardia
Papilledema
Retinal hemorrhage
Global or focal neurologic abnormalities
Complications of SAH include the following:
Hydrocephalus
Rebleeding
Vasospasm
Seizures
Cardiac dysfunction
See Clinical Presentation for more detail.
Diagnosis
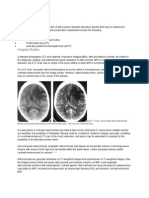
Diagnosis of SAH usually depends on a high index of clinical suspicion combined with radiologic
confirmation via urgent noncontrast CT, followed by lumbar puncture or CT angiography of the brain. After
the diagnosis is established, further imaging should be performed to characterize the source of the
hemorrhage.
Laboratory studies should include the following:
Serum chemistry panel
Complete blood count
Prothrombin time (PT)/activated partial thromboplastin time (aPTT)
Blood typing/screening
Cardiac enzymes
Arterial blood gas (ABG) determination
Imaging studies that may be helpful include the following:
CT (noncontrast, contrast, or infusion)
Digital subtraction cerebral angiography
Multidetector CT angiography
MRI (if no lesion is found on angiography)
Magnetic resonance angiography (MRA; investigational for SAH)
Other diagnostic studies that may be warranted are as follows:
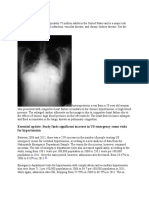
Baseline chest radiograph
ECG on admission
Lumbar puncture and CSF analysis
See Workup for more detail.
Management
Current treatment recommendations include the following:
Antihypertensive agents (eg, IV beta blockers) when mean arterial pressure exceeds 130 mm Hg
Avoidance of nitrates (which elevate ICP) when feasible
Hydralazine and calcium channel blockers
Angiotensin-converting enzyme (ACE) inhibitors (not first-line agents in acute SAH)
In patients with signs of increased ICP or herniation, intubation and hyperventilation
Other interventions for increased ICP are as follows:
Osmotic agents (eg, mannitol)
Loop diuretics (eg, furosemide)
IV steroids (controversial but recommended by some)
Additional medical management is directed toward the following common complications:
Rebleeding
Vasospasm
Hydrocephalus
Hyponatremia
Seizures
Pulmonary complications
Cardiac complications
Surgical treatment to prevent rebleeding includes the following options:
Clipping the ruptured aneurysm
Endovascular treatment [1] (ie, coiling)
The choice between coiling and clipping usually depends on the location of the lesion, the neck of the
aneurysm, and the availability and experience of hospital staff.
Screening is not recommended in the general population. However, it can lower cost and improve quality
of life in patients at relatively high risk for aneurysm formation and rupture.
You might also like
- Cerebral Aneurysm Arteriovenous Malformation: Signs and SymptomsDocument3 pagesCerebral Aneurysm Arteriovenous Malformation: Signs and SymptomsMohammadAwitNo ratings yet
- Ich & SahDocument70 pagesIch & Sahmirabel IvanaliNo ratings yet
- Subarachnoid HemorrhageDocument12 pagesSubarachnoid HemorrhageStephanie SarjonoNo ratings yet
- Drgirma StrokeDocument35 pagesDrgirma StrokeGirma LemaNo ratings yet
- Case PresentationDocument6 pagesCase PresentationbaleteaprileuniceNo ratings yet
- Investigations in Cardiology M1 Lecture 08082017Document40 pagesInvestigations in Cardiology M1 Lecture 08082017frankozed1No ratings yet
- Understanding Intra-Cerebral HemorrhageDocument41 pagesUnderstanding Intra-Cerebral HemorrhageAnggia AnggraeniNo ratings yet
- Ax & DX SAHDocument5 pagesAx & DX SAHMohammadAwitNo ratings yet
- Intracerebral HemorrhageDocument5 pagesIntracerebral HemorrhageyulitawijayaNo ratings yet
- Cerebro-Vascular Disease & Stroke: Faizan Zaffar KashooDocument57 pagesCerebro-Vascular Disease & Stroke: Faizan Zaffar KashooDrGasnasNo ratings yet
- Diagnostic TestsDocument1 pageDiagnostic TestsMae Anne MahinayNo ratings yet
- Stroke IskemikDocument237 pagesStroke IskemikVania ValentinaNo ratings yet
- Stroke, Subarachnoid Hemorrhage and Hypothermia For Cardiac ArrestDocument82 pagesStroke, Subarachnoid Hemorrhage and Hypothermia For Cardiac ArrestDrGasnasNo ratings yet
- DynaMed Plus - Stroke (Acute Management)Document126 pagesDynaMed Plus - Stroke (Acute Management)Sarah Shafa MarwadhaniNo ratings yet
- Stroke ManagementDocument18 pagesStroke ManagementAETCM Emergency medicineNo ratings yet
- Management of Stroke: in The Name of God The Most Gracious The Most MercifulDocument29 pagesManagement of Stroke: in The Name of God The Most Gracious The Most MercifulHaider Nadhem AL-rubaiNo ratings yet
- Nanda, A, Niranjan NS, Transient Ischemic Attack. Medscape. 2013Document6 pagesNanda, A, Niranjan NS, Transient Ischemic Attack. Medscape. 2013rahmatNo ratings yet
- Hypertensive Crisis: Megat Mohd Azman Bin AdzmiDocument34 pagesHypertensive Crisis: Megat Mohd Azman Bin AdzmiMegat Mohd Azman AdzmiNo ratings yet
- NeuroDocument2 pagesNeuroHa Jae kyeongNo ratings yet
- Cerebral AngiographyDocument9 pagesCerebral AngiographyVincent LopezNo ratings yet
- Emergency Neurological Life Support Subarachnoid Hemorrhage: Last Updated: 19-Mar-2016Document22 pagesEmergency Neurological Life Support Subarachnoid Hemorrhage: Last Updated: 19-Mar-2016michaelNo ratings yet
- Stroke Syndrome - BenyDocument22 pagesStroke Syndrome - BenyyericosabathinoNo ratings yet
- Update Management of Acute StrokeDocument48 pagesUpdate Management of Acute StrokerintyosoNo ratings yet
- Practice Essentials: Signs and SymptomsDocument20 pagesPractice Essentials: Signs and SymptomsYoga Zunandy PratamaNo ratings yet
- Cerebrovascular AccidentDocument42 pagesCerebrovascular AccidentGideon HaburaNo ratings yet
- Readings About Cerebral Venous Sinus Thrombosis (CVST) (ER-RMPH)Document8 pagesReadings About Cerebral Venous Sinus Thrombosis (CVST) (ER-RMPH)Raquel Beldia FuentesNo ratings yet
- Liver Disease Guide: Symptoms, Tests, and TreatmentsDocument1 pageLiver Disease Guide: Symptoms, Tests, and TreatmentsPooya WindyNo ratings yet
- Carotid Artery Disease: Causes, Symptoms, Tests, and TreatmentDocument6 pagesCarotid Artery Disease: Causes, Symptoms, Tests, and TreatmentVijay Baskar SNo ratings yet
- Cerebral arteriovenous malformation (AVMDocument7 pagesCerebral arteriovenous malformation (AVMCj UritaNo ratings yet
- Differential Diagnosis FormatDocument2 pagesDifferential Diagnosis FormatRalph Francis Flores Palma100% (1)
- Instrumental MethodDocument24 pagesInstrumental Methodzerish0208No ratings yet
- Stroke Hemoragik: Yuneldi Anwar Sps Departemen Neurologi FK UsuDocument28 pagesStroke Hemoragik: Yuneldi Anwar Sps Departemen Neurologi FK UsuJuliana Sari HarahapNo ratings yet
- CVA SsDocument39 pagesCVA SsAnushri ManeNo ratings yet
- Diagnosing subarachnoid hemorrhage with CT and lumbar punctureDocument8 pagesDiagnosing subarachnoid hemorrhage with CT and lumbar punctureMohammadAwitNo ratings yet
- Evidencia en Craniectomia DescompresivaDocument22 pagesEvidencia en Craniectomia DescompresivaJosé Luis ChavesNo ratings yet
- Intracerebral Hemorrhage - Classification, Clinical Symptoms, DiagnosticsDocument27 pagesIntracerebral Hemorrhage - Classification, Clinical Symptoms, DiagnosticsJoisy AloorNo ratings yet
- Cerebrovascular Accident Types, Causes, Signs, and ManagementDocument5 pagesCerebrovascular Accident Types, Causes, Signs, and ManagementPrakuz Harmony SubedifiedNo ratings yet
- StrokeDocument5 pagesStrokeChristian Roi ArcillaNo ratings yet
- Stroke Hemoragik: Yuneldi Anwar Sps Departemen Neurologi FK UsuDocument28 pagesStroke Hemoragik: Yuneldi Anwar Sps Departemen Neurologi FK UsuDwi Meutia IndriatiNo ratings yet
- QXCI stroke treatment optionsDocument5 pagesQXCI stroke treatment optionsEnrique Gonzalez Marquier100% (1)
- 2019 Evc Isquemico NeuroimagenDocument15 pages2019 Evc Isquemico NeuroimagenJuan Pablo B. FloresNo ratings yet
- Cerebrovascular Accident (Cva) : Tanja Čujić Iva Ferček Petra ČrnacDocument28 pagesCerebrovascular Accident (Cva) : Tanja Čujić Iva Ferček Petra ČrnacDrGasnasNo ratings yet
- DR NzooloDocument21 pagesDR NzooloJohn chrisant Mwansa the future presdoNo ratings yet
- Stroke Hemoragik: Dr. Puji Pinta O. Sinurat, Sps Bagian Neurologi Fk-Umi 2019Document28 pagesStroke Hemoragik: Dr. Puji Pinta O. Sinurat, Sps Bagian Neurologi Fk-Umi 2019Desima Tamara sinuratNo ratings yet
- Guar Raci No 2016Document14 pagesGuar Raci No 2016ema moralesNo ratings yet
- ACUTE CORONARY SYNDROMEDocument12 pagesACUTE CORONARY SYNDROMEElsy MayjoNo ratings yet
- Renovascular Hypertension (RVH) SeminarDocument58 pagesRenovascular Hypertension (RVH) SeminarfaizalmasoodiNo ratings yet
- Guidelines for Diagnosis and Treatment of Acute and Chronic Heart FailureDocument52 pagesGuidelines for Diagnosis and Treatment of Acute and Chronic Heart FailureDedy KristoferNo ratings yet
- Transient Ischemic AttackDocument7 pagesTransient Ischemic AttackDandelionNo ratings yet
- PDF Takayasu Arteritis 2 PDFDocument5 pagesPDF Takayasu Arteritis 2 PDFPadmaja PriyadarshiniNo ratings yet
- Supraventricular ArrhythmiasDocument56 pagesSupraventricular ArrhythmiasGading AuroraNo ratings yet
- Hypertension WorkshopDocument15 pagesHypertension WorkshopDonaJeanNo ratings yet
- TIADocument22 pagesTIAArabylle Maranca AbuelNo ratings yet
- I. Textbook Discussion & Schematic Diagram of The Diagnosis A.Definition Cerebrovascular Disease (CVA), An IschemicDocument5 pagesI. Textbook Discussion & Schematic Diagram of The Diagnosis A.Definition Cerebrovascular Disease (CVA), An IschemicJanet CamposanoNo ratings yet
- MATSS TIA Education Booklet Updated April 2010Document22 pagesMATSS TIA Education Booklet Updated April 2010BeyLha Ituwh AquhNo ratings yet
- Stroke Guidelines 2018Document36 pagesStroke Guidelines 2018Mickola VorokhtaNo ratings yet
- DD Nyeri Kepala Skenario 1Document8 pagesDD Nyeri Kepala Skenario 1Ika Putri YulianiNo ratings yet
- Stroke Syndromes and PresentationsDocument12 pagesStroke Syndromes and PresentationsSam JamesNo ratings yet
- Cardiac Care and COVID-19: Perspectives in Medical PracticeFrom EverandCardiac Care and COVID-19: Perspectives in Medical PracticeNo ratings yet
- Pharmacotherapeutic Management of Cardiovascular Disease Complications: A Textbook for Medical StudentsFrom EverandPharmacotherapeutic Management of Cardiovascular Disease Complications: A Textbook for Medical StudentsNo ratings yet
- HTDocument3 pagesHTMohammadAwitNo ratings yet
- US ER visits for hypertension rise 25% 2006-2011Document4 pagesUS ER visits for hypertension rise 25% 2006-2011MohammadAwitNo ratings yet
- Skabies DXDocument6 pagesSkabies DXMohammadAwitNo ratings yet
- Volkmann Contracture: Historical AspectsDocument2 pagesVolkmann Contracture: Historical AspectsMohammadAwitNo ratings yet
- Oli God End Ro GliomasDocument1 pageOli God End Ro GliomasMohammadAwitNo ratings yet
- Scabiei Hominis. Approximately 300 Million Cases of Scabies (See The Image Below) Are ReportedDocument3 pagesScabiei Hominis. Approximately 300 Million Cases of Scabies (See The Image Below) Are ReportedMohammadAwitNo ratings yet
- Neurilemmomas DXDocument1 pageNeurilemmomas DXMohammadAwitNo ratings yet
- Neurilemmomas DXDocument1 pageNeurilemmomas DXMohammadAwitNo ratings yet
- MRI Findings Help Diagnose Rare Intraosseous LesionsDocument1 pageMRI Findings Help Diagnose Rare Intraosseous LesionsMohammadAwitNo ratings yet
- Neurofibroma Ganglion Cyst Giant Cell Tumor of Tendon Sheath LipomaDocument1 pageNeurofibroma Ganglion Cyst Giant Cell Tumor of Tendon Sheath LipomaMohammadAwitNo ratings yet
- Neurilemmomas DXDocument1 pageNeurilemmomas DXMohammadAwitNo ratings yet
- Oli God End Ro GliomasDocument1 pageOli God End Ro GliomasMohammadAwitNo ratings yet
- AstrocytomaDocument1 pageAstrocytomaMohammadAwitNo ratings yet
- Oli God End Ro GliomasDocument1 pageOli God End Ro GliomasMohammadAwitNo ratings yet
- Oli God End Ro GliomasDocument1 pageOli God End Ro GliomasMohammadAwitNo ratings yet
- SAH DXDocument2 pagesSAH DXMohammadAwitNo ratings yet
- Oli God End Ro GliomasDocument1 pageOli God End Ro GliomasMohammadAwitNo ratings yet
- Oli God End Ro GliomasDocument1 pageOli God End Ro GliomasMohammadAwitNo ratings yet
- United States StatisticsDocument1 pageUnited States StatisticsMohammadAwitNo ratings yet
- AstrocytomaDocument1 pageAstrocytomaMohammadAwitNo ratings yet
- AstrocytomaDocument1 pageAstrocytomaMohammadAwitNo ratings yet
- Oli God End Ro GliomasDocument1 pageOli God End Ro GliomasMohammadAwitNo ratings yet
- AstrocytomaDocument2 pagesAstrocytomaMohammadAwitNo ratings yet
- United States StatisticsDocument1 pageUnited States StatisticsMohammadAwitNo ratings yet
- Lymphoblastic Leukemia: This MRI Shows A Juvenile Pilocytic Astrocytoma of The CerebellumDocument1 pageLymphoblastic Leukemia: This MRI Shows A Juvenile Pilocytic Astrocytoma of The CerebellumMohammadAwitNo ratings yet
- Prognosis: Clinical Grading ScalesDocument3 pagesPrognosis: Clinical Grading ScalesMohammadAwitNo ratings yet
- Brainstem Gliomas: Brain Cancer Treatment ProtocolsDocument2 pagesBrainstem Gliomas: Brain Cancer Treatment ProtocolsMohammadAwitNo ratings yet
- SAH DXDocument4 pagesSAH DXMohammadAwitNo ratings yet
- Astrocytoma SDocument6 pagesAstrocytoma SMohammadAwitNo ratings yet
- Spek Pheno and Confidence SG E-KatDocument3 pagesSpek Pheno and Confidence SG E-KatSamu SimamesaNo ratings yet
- Charles B. Higgins, Albert de Roos MRI and CT of The Cardiovascular SystemDocument180 pagesCharles B. Higgins, Albert de Roos MRI and CT of The Cardiovascular SystemdrAlbertoVVNo ratings yet
- Emergency Radiology PDFDocument41 pagesEmergency Radiology PDFRobiul AlamNo ratings yet
- A Proposed Grading System For Endovascular Treatment of Cerebral Arteriovenous Malformations - Buffalo Score PDFDocument9 pagesA Proposed Grading System For Endovascular Treatment of Cerebral Arteriovenous Malformations - Buffalo Score PDFRafael Mujica OreNo ratings yet
- Peripheral Angiography: IndicationsDocument2 pagesPeripheral Angiography: IndicationsjyothiNo ratings yet
- 300+ TOP RADIOLOGY Objective Questions and AnswersDocument26 pages300+ TOP RADIOLOGY Objective Questions and Answersمحمد سلمان100% (1)
- 4 HTA RenDocument37 pages4 HTA RenBordean LilianaNo ratings yet
- Guía Hemorragia Intestino DelgadoDocument8 pagesGuía Hemorragia Intestino DelgadoSMIBA MedicinaNo ratings yet
- Ruiz 1998Document2 pagesRuiz 1998Sarly FebrianaNo ratings yet
- Imaging and RadiologyDocument7 pagesImaging and RadiologyOdyNo ratings yet
- Q.P. Code: 801521Document15 pagesQ.P. Code: 801521CARDIAC SRINITHI DHANA DHARSHIKAA N100% (1)
- Role of Multi Detector (MDCT)Document52 pagesRole of Multi Detector (MDCT)ramon100% (5)
- STROKEDocument61 pagesSTROKEK.MERCYNo ratings yet
- DSADocument7 pagesDSANantini GopalNo ratings yet
- Bushong ReviewDocument10 pagesBushong ReviewbbkanilNo ratings yet
- Nursing Practice 1Document4 pagesNursing Practice 1Nurul IzzahNo ratings yet
- X-Ray Contrast Media Made ClearDocument14 pagesX-Ray Contrast Media Made CleartughtedNo ratings yet
- Imaging in Brain TumorDocument142 pagesImaging in Brain TumorMagrinov AzaniaNo ratings yet
- Pelvic Trauma - PPT 2010Document47 pagesPelvic Trauma - PPT 2010Chamila Senarathna100% (2)
- X-Ray Technology PresentationDocument372 pagesX-Ray Technology PresentationAnonymous 3ZKNMd100% (1)
- Is Iso 10555 2 1996Document14 pagesIs Iso 10555 2 1996Hemant SharmaNo ratings yet
- Nervus 3Document3 pagesNervus 3Palneuro UnsriNo ratings yet
- DNB Systemwise Questions Customized (Space For Notes) Upto Dec 2019 PDFDocument252 pagesDNB Systemwise Questions Customized (Space For Notes) Upto Dec 2019 PDFGovindNo ratings yet
- Handbook of Interventional Radiologic ProceduresDocument1,101 pagesHandbook of Interventional Radiologic Proceduresizzat basahai100% (2)
- Contrast MediaDocument97 pagesContrast MediaAME DENTAL COLLEGE RAICHUR, KARNATAKANo ratings yet
- 1 CathDocument12 pages1 CathHashem AlsmadiNo ratings yet
- Cardiac CTDocument7 pagesCardiac CTdaniel7pintiliiNo ratings yet
- Carotid Cavernous Fistula Treatment OptionsDocument78 pagesCarotid Cavernous Fistula Treatment OptionsDeny Handayanto0% (1)
- A Morphological Study of Anatomical Variations in 96 Circles of Willis An Autopsic Evaluation and Literature ReviewDocument6 pagesA Morphological Study of Anatomical Variations in 96 Circles of Willis An Autopsic Evaluation and Literature ReviewRoxana RoxNo ratings yet
- 2018 Interventional Rad - For Medical StudentDocument183 pages2018 Interventional Rad - For Medical StudentDaniyal HaiderNo ratings yet