Professional Documents
Culture Documents
CV 2
Uploaded by
Anonymous Di1zSIkRBHOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CV 2
Uploaded by
Anonymous Di1zSIkRBHCopyright:
Available Formats
Review
For reprint orders, please contact:
reprints@future-drugs.com
Preeclampsia and future
cardiovascular risk
J Newstead, P von Dadelszen and Laura A Magee
CONTENTS
Cardiovascular disease in
women: magnitude of
the problem
Recognized cardiovascular
risk markers in women
Is preeclampsia a new,
novel cardiovascular
risk factor?
What should clinicians do?
Conclusions
Expert commentary
Key issues
Pregnancy is a metabolic and vascular stress test for women and those who fail are at
increased risk of long-term cardiovascular complications. Specifically, women who
develop preeclampsia (and/or other manifestations of placental dysfunction) are at
increased risk of coronary heart disease, stroke and cardiovascular disease in general.
The risk is highest among women who develop both maternal (e.g., hypertension and
proteinuria) and fetal (e.g., intrauterine growth restriction) manifestations of abnormal
placentation, especially with preterm delivery. Most women who develop a maternal
placental syndrome return to a normal clinical state in the weeks following pregnancy and
their absolute risk of cardiovascular disease in the short term is very low. However, perhaps
having a placentally complicated pregnancy affords women the opportunity to
personalize risk and take action. Action is needed. The fact that we, as a population, are
getting heavier and more sedentary is an urgent public health issue. The American Heart
Association recommends that all women (even those at low cardiovascular risk) pursue
dietary and lifestyle changes, in addition to smoking cessation. Engaging women of childbearing age who may be motivated by a complicated pregnancy would be very
valuable, from a public health perspective, given the prevalence and importance of
cardiovascular disease in women, and the central role of the woman as caregiver to
children, spouses and other family members.
Expert Rev. Cardiovasc. Ther. 5(2), 283294 (2007)
Five-year view
References
Affiliations
Author for correspondence
University of British Columbia,
Departments of Obstetrics and
Gynaecology and Medicine, and the
Centre for Applied Health Research
and Evaluation, Child and Family
Research Institute of British
Columbia, and British Columbias
Womens Hospital and Health
Centre, 4500 Oak Street,
Room 1U59, Vancouver
V6H 3N1, BC, Canada
Tel.: +1 604 875 2960
Fax: +1 604 875 2961
lmagee@cw.bc.ca
KEYWORDS:
hypertension, ischemic heart
disease, long-term cardiovascular
mortality, preeclampsia,
pregnancy, stroke
www.future-drugs.com
More than half of the adult population in the
developed world is sedentary or inactive [1].
Metabolic syndrome is on the rise and this will
only lead to further stress on an already
strained healthcare system. Public health advocates are seeking ways to interest the population in this alarming trend and promote health
behaviors that have been proven to improve
long-term outcomes.
Preeclampsia represents just such an opportunity for personalization of risk. Preeclampsia and other forms of placental dysfunction
have been associated consistently with excess
long-term cardiovascular risk. It would appear
that these women have failed the physiological
stress test of pregnancy. This affords the
healthcare provider the opportunity to both
initiate primary prevention in women at
increased risk and educate the entire family
about healthy lifestyle choices so that society at
large also benefits.
10.1586/14779072.5.2.283
Cardiovascular disease in women:
magnitude of the problem
Cardiovascular disease (CVD) is the cause of
death for just over 50% of women worldwide
[2]. The majority of these cardiovascular deaths
are due to coronary heart disease (23%) and
stroke (18%). Prevention is key. Nearly two
thirds of women who die suddenly of coronary
heart disease have no previously recognized
symptoms. Also, we now recognize the existence of subclinical disease that is amenable to
treatment, rather than viewing CVD as an all
or nothing phenomenon.
Recognized cardiovascular risk markers
in women
There are many global risk-assessment tools
that take a risk marker tally approach to the
assessment of CVD risk [3]. The most well
known is the Framingham global risk assessment tool that incorporates the following
2007 Future Drugs Ltd
ISSN 1477-9072
283
Newstead, von Dadelszen & Magee
traditional cardiovascular risk markers: gender, age, systolic
blood pressure (BP) and its treatment, total cholesterol and
high-density lipoproteins (HDL) [101]. These are used to
determine the 10-year CVD risk estimate, which is then used
in guidelines to recommend management.
These global risk assessment tools must be viewed as imperfect and still in development for a number of reasons [4]. First,
most of the available tools (including the Framingham score)
are prone to error, particularly at the extremes of risk. Young
women are likely to fall into the low (or optimal) risk category
and, as such, the global risk assessment tools will only be
moderately accurate in predicting the 10-year risk of a major
coronary event. Second, many tools do not take into account
other established risk markers for CVD, such as family history
of premature CVD, diabetes, chronic renal failure and obesity.
Third, most tools do not take into account new and novel
cardiovascular risk markers. These include microalbuminuria
and preclinical atherosclerosis (e.g., measures of vascular function and endothelial health). These novel risk markers may
also include a history of hypertensive pregnancy. What is the
evidence for this?
Is preeclampsia a new, novel cardiovascular risk factor?
What is preeclampsia?
preeclampsia, or the hypertension may remain isolated.
Therefore, the classification of a womans hypertensive disorder
of pregnancy may change.
The hypertensive disorders of pregnancy are common, complicating up to 10% of pregnancies worldwide. They represent
a leading cause of maternal mortality and morbidity in pregnancy. The most common is gestational hypertension (56%).
Using population-based data, approximately 1% of pregnancies are complicated by pre-existing hypertension, 56% by
gestational hypertension without proteinuria and 12% by
preeclampsia [8].
Understanding the pathogenesis of preeclampsia is key to an
understanding of preeclampsias multisystem and varied clinical
manifestations. The most popular theory for the pathogenesis
of preeclampsia describes a two-stage process (FIGURE 1) [911].
The first stage consists of a relative failure of the maternal
uterine spiral arteries (termed uteroplacental arteries in pregnancy) to undergo their normal vascular remodeling adequately for the subsequent fetoplacental demands. In normal
pregnancy, syncytiotrophoblast from the placenta invades the
vascular luminal wall of uterine spiral arteries, resulting in loss
of the inner elastic lamina and vascular smooth muscle. Their
diameter increases fourfold to create an intervillous (maternal)
blood supply that is high capacitance, low resistance and unresponsive to vasoactive stimuli. These changes extend to the
inner third of the myometrium. By contrast, in preeclampsia,
particularly early onset, the vascular remodeling of the uterine
Hypertension during pregnancy is classified as: pre-existing
(chronic) hypertension (that was present either prior to pregnancy
or before 20 weeks gestation, or which persists for more than
6 weeks postpartum) or gestational (pregnancy-induced) hypertension (appeared
Cytotrophoblast invasion
after 20 weeks gestation) [5,6]. Gestational
(pregnancy-induced) hypertension is furImmunological factors
ther subcategorized according to the presPoor placentation
ence of proteinuria and/or adverse features. Proteinuria is defined as 0.3 g/day
Thrombophilia
or more by a 24-h urine collection or,
Uteroplacental mismatch
Acute atherosis
Multiple pregnancy
alternatively, by at least 2+ by urinary
Fetal macrosomia
dipstick or at least 30 mg/mmol urinary
creatinine by spot urinary protein:creatiPlacental
Intervillous
PBLs
Cytokines PGs
ROS
nine ratio [7]. Adverse features refer to
debris
soup
maternal complications of preeclampsia,
such as eclampsia (seizure), severe hyperEndothelial cell activation
tension, elevated liver enzymes or low
platelets. The Canadian classification
system defines preeclampsia as gestaCardiomyopathy
Hypertension
Maternal syndrome
tional hypertension with proteinuria or
adverse features. The American classifiLiver damage/
cation system defines preeclampsia as
Eclampsia/
hematoma/
stroke
gestational (pregnancy-induced) hyperrupture
Glomerular
tension and proteinuria, but goes on to
Edema
ARDS Microangiopathic
endotheliosis/
hemolysis/
describe the potential multiorgan materproteinuria/
thrombocytopenia/
nal and fetal complications of preATN
DIC
eclampsia. Women who develop isolated
gestational (pregnancy-induced) hyper- Figure 1. Pathogenesis of the maternal syndrome of preeclampsia (modified from [9]).
tension may develop proteinuria or ARDS: Acute respiratory distress syndrome; ATN: Acute tubular necrosis; DIC: Disseminated intravascular
end-organ complications that define coagulation; PBL: Peripheral blood leukocyte; PG: Eicosanoid; ROS: Reactive oxygen species.
284
Expert Rev. Cardiovasc. Ther. 5(2), (2007)
Preeclampsia and future cardiovascular risk
Vascular risk factors
spiral arteries is more superficial in terms
of depth and the numbers of uterine
Population with complicated pregnancy (e.g., preeclampsia)
arterioles involved.
Failure of normal placentation can be
Healthy population
caused by many factors, such as genetics
Threshold for vascular or metabolic disease
(including a paternal contribution),
maternal thrombophilia, pre-existing
hypertension and chronic renal disease, as
shown in FIGURE 1. It must also be recognized that, at term, among women with
preeclampsia, there is an excess of largefor-date fetuses and multiple pregnancies.
Under these circumstances, it may be
that the demands of the normally formed
fetoplacental unit outstrips the ability of
Neonatal life
Pregnancies
Middle age
fully remodeled uteroplacental arteries to
Age
supply those demands.
In the second stage, which occurs later Figure 2. Risk markers for vascular disease.
in pregnancy, fetal demands outstrip the Adapted from [14].
uteroplacental supply, resulting in uteroplacental mismatch. As a result of this, a soup is released from metabolic stress is removed and virtually all women return to a
the placenta containing substances that are proinflammatory, subclinical and normotensive state. However, with the passage
prothrombotic, vasoconstrictive and/or antiangiogenic of time, they may again be pushed above the threshold for clini(e.g., sFlt-1) [12], or result in oxidative stress (i.e., reactive oxy- cal disease, manifested later in life as CVD. This hypothesis is
gen species). This soup causes systemic maternal endothelial illustrated in FIGURE 2 [14].
cell dysfunction and vasospasm, activation of the coagulation
cascade with the formation of occlusive microthrombi and loss Similar risk markers
of intravascular fluid. Ultimately, this leads to the end-organ Risk markers for preeclampsia and for CVD are similar. Noncomplications of preeclampsia. It is worth emphasizing that modifiable risk markers include: age, family history of the conhypertension is but one of these complications and is not part dition and ethnicity [15]. Of greater interest are those that are
of the pathogenesis of preeclampsia. Also, this placental soup potentially modifiable or treatable, including (pre-existing)
forms part of a forward feedback loop, which causes decreased hypertension, diabetes mellitus, renal disease, obesity, dyslipiplacental perfusion, and so the cycle continues.
demia, metabolic syndrome, microalbuminuria, thromIt follows from this discussion that the maternal manifesta- bophilia (such as antiphospholipid syndrome and hyperhomotions of preeclampsia are varied and can involve any organ sys- cystenemia) and elevated antibodies to Chlamydia pneumoniae
tem. The most common manifestations are, of course, those and cytomegalovirus [1618]. The idea that preelcampsia is a
that most commonly define preeclampsia: hypertension and failed stress test and pregnancy is a form of the metabolic synproteinuria. However, FIGURE 1 highlights that there can be any drome is helpful in understanding the relationship between
combination or permutation of complications, including the two.
hypertension with elevated liver enzymes. There is also a fetal
syndrome of preeclampsia, resulting from the consequences of Similar pathology
inadequate placentation, and consisting of: oligohydramnios The pathognomonic placental lesion of preeclampsia is called
(i.e., low amniotic fluid), intrauterine fetal growth restriction, acute atherosis owing to its histological similarity to the
abnormal Doppler velocimetry of the umbilical artery or still- lesions of atherosclerosis. Acute atherosis affects the uteroplabirth. This fetal syndrome can present before the maternal cental arteries (termed spiral arteries before pregnancy) of the
manifestations of preeclampsia; alternatively, they can present decidua (termed endometrium before pregnancy) and myoin isolation and represent part of the spectrum of placental metrium. Similar to atherosclerosis, acute atherosis is characabnormalities [13].
terized by focal endothelial disruption, fibrinoid necrosis of
the arterial wall (containing both immunoglobulin [Ig]M and
Why might preeclampsia be a cardiovascular risk marker?
complement that reflect inflammation), infiltration of
Preeclampsia and CVD share risk markers and have a similar perivascular spaces by mononuclear cells, accumulation of
clinical picture and pathology. The hypothesis is that there is an lipid-laden macrophages and lipoprotein(a) deposition [19].
underlying maternal predisposition to vascular disease. The met- The resultant plaque contains lipid and cellular debris. The
abolic stress of pregnancy causes this predisposition to vascular vessels can become partially or completely occluded or can
disease to become manifest as preeclampsia. After pregnancy, the rupture [20].
www.future-drugs.com
285
Newstead, von Dadelszen & Magee
Similar clinical picture
Preeclampsia is characterized by metabolic changes that closely
resemble those of the metabolic syndrome:
Hyperlipidemia (i.e., reduced HDL cholesterol and elevated
triglycerides, free fatty acids and low-density lipoprotein
[LDL] cholesterol)
Insulin resistance
An increase in coagulation factors [10]
These metabolic changes are seen to a lesser extent in normal
pregnancy, which can be regarded as a transient metabolic syndrome or a stress test of sorts. Normal pregnancy is associated
with hyperlipidemia, relative insulin resistance, an increase in
coagulation factors and upregulation of the inflammatory cascade (and neutrophilia) [14]. It is thought that in women with
more abnormal prepregnancy carbohydrate, lipid and/or vascular function, the metabolic stress of pregnancy may push them
past a clinical threshold for the manifestation of vascular or
metabolic disease (FIGURE 2). These women manifest, for example, what we know as gestational hypertension or preeclampsia,
gestational diabetes (GDM) or thromboembolism.
What is the evidence for an association between
preeclampsia & CVD?
In the 1970s, Leon Chesley, the father of our scientific and
clinical approach to the hypertensive disorders of pregnancy,
recognized that women who suffer from eclampsia have an
excess of long-term CVD [21]. Over the last 10 years, there
have been many publications linking preeclampsia (and other
manifestations of abnormal placentation) with future CVD.
We are aware of 12 retrospective studies (ten cohort [2233]
and two casecontrol [22,34]) that have examined an association
between gestational hypertension or preeclampsia (with or
without other adverse placental complications) and subsequent
cardiovascular events (TABLE 1). The term adverse placental
events refers to stillbirth, placental abruption, preeclampsia or
normotensive intrauterine growth restriction, all of which have
collectively been referred to as the maternal placental syndrome. The outcomes analyzed have included any CVD or the
most common specific ones: ischemic heart disease and stroke.
These studies have been conducted in Canada [29], Iceland
[22,26], Israel [23], Norway [25], Scotland [28,30,33], Sweden [32], the
UK [24,34] and the USA [27].
A consistent association has been described between gestational hypertension or preeclampsia and an increased risk of
cardiovascular mortality or morbidity, compared with women
whose pregnancies were not complicated by a maternal placental
syndrome or population norms over a corresponding period of
time [26]. The point estimates for the relative risk (RR) of future
cardiovascular events following a pregnancy complicated by gestational hypertension or preeclampsia have ranged from 1.3 to
3.3, with almost all studies finding the association to be significant, particularly for preeclampsia. The CVD was also reported
to occur earlier in life [24]. There also seems to be a consistent
doseresponse relationship. More mild manifestations of the
286
maternal placental syndrome (i.e., gestational hypertension or
isolated intrauterine fetal growth restriction) have been associated less consistently and less strongly with increased cardiovascular risk. More severe manifestations of the maternal placental
syndrome (i.e., severe preeclampsia or preeclampsia associated
with intrauterine fetal growth restriction, preterm birth and/or
fetal death) have consistently demonstrated future cardiovascular risk to be elevated, with much higher RR values (i.e., point
estimates ranging from 2.78.1). Also, a doseresponse relationship was demonstrated for recurrent gestational hypertension or
preeclampsia in subsequent pregnancies. Women with hypertensive disease in both their first and second pregnancies (vs only
their first pregnancy) had an even higher RR of future ischemic
heart disease [32].
Over what period of time is this potentially increased cardiovascular risk manifested? The answer is many years, until the
underlying maternal predisposition reaches the critical threshold
for clinical manifestations (FIGURE 3).
In summary, preeclampsia specifically (and the maternal placental syndrome in general) has been associated with an
increased risk of future CVD in general and stroke and
ischemic heart disease in particular. There are two important
points to make. Firstly, association does not imply causation. At
present, the most plausible explanation for the association
between preeclampsia and CVD is that preeclampsia unmasks a
maternal predisposition to vascular disease. This situation is
analogous to GDM, which is a risk marker for, but not a cause
of, long-term Type II diabetes. Secondly, the increase in cardiovascular risk associated with preeclampsia or other placental
syndromes is small; the immediate risk is very low (<10% over
10 years). However, given the prevalence of CVD and its
importance as the number one cause of mortality in women,
the public health implications are enormous. The question is,
what should clinicians do?
What should clinicians do?
Clinicians need to follow evidence-based practice and consider
practice guidelines that have recommendations based on such
evidence. This point has been emphasized in the area of
womens health by the fact that hormone-replacement therapy
in peri- and post-menopausal women may actually increase cardiovascular risk rather than reducing it as was anticipated prior
to definitive randomized controlled trials [35].
Unfortunately, there are no published evidence-based guidelines
for long-term management of women who have no traditional
cardiovascular risk markers but who do have a history of gestational hypertension or preeclampsia (or another component of the
maternal placental syndrome). Women with pre-existing hypertension are guided by various national guidelines [36,37]. As such,
the discussion that follows is meant to inform the reader about
possible approaches for women with gestational hypertension or
preeclampsia. These approaches have either been used in other
settings or are novel but may be appropriate. Whether adopting
any of these practices following hypertensive pregnancy would
improve long-term cardiovascular health has not been established.
Expert Rev. Cardiovasc. Ther. 5(2), (2007)
Preeclampsia and future cardiovascular risk
Table 1. Retrospective cohort studies linking abnormal placentation with cardiovascular disease .
Study
Study participants
Median
follow-up
(year)
MPS at baseline
Future CV risk
Adjusted RR
[95% CI]
Mann et al.
(1976)
77 women <45 years old
discharged from hospital with a
myocardial infarction (cases), and
207 controls
Preeclampsia (requiring
drug treatment
or hospitalization)
Myocardial
infarction
2.8 [-,-];
p < 0.05
[34]
Jonsdottir
et al. (1995)
7543 women with a delivery
41.9
Any hypertension
in pregnancy
Death from
ischemic
heart disease
1.5 [1.1,2.0]
[26]
Preeclampsia
Death from
ischemic
heart disease
1.9 [1.0,3.5]
Eclampsia
Death from
ischemic
heart disease
2.6 [1.1,6.1]
Ref.
Hannaford
et al. (1997)
23,000 women who participated in 27
(but never used) oral contraception
Toxemia
Any ischemic
heart disease
1.7 [1.3,2.2]
[24]
Smith et al.
(2001)
129,920 women with livebirth
Preeclampsia
Ischemic
heart disease
2.0 [1.5,2.5]
[30]
Preeclampsia + SGA
+ preterm delivery*
Ischemic
heart disease
7.0 [3.0,14.5]
Preeclampsia
CV death
1.6 [1.0,2.7]
Preeclampsia +
preterm delivery
CV death
8.1 [4.3,15.3]
Gestational hypertension
Cerebrovascular
death
1.5 [0.7,3.3]
Preeclampsia
Cerebrovascular
death
2.1 [1.0,4.3]
Gestational hypertension
CV disease
2.8 [1.6,4.8]
Mild preeclampsia
CV disease
2.2 [1.3,3.6]
Severe preeclampsia
CV disease
3.3 [1.7,6.5]
Low infant BW
Major stroke
1.3 [1.0,1.6]
Preterm delivery*
Major stroke
1.9 [1.4,2.7]
Low infant BW +
preterm delivery
Major stroke
2.7 [1.4,5.1]
Irgens et al.
(2001)
Wilson et al.
(2003)
Kestenbaum
et al. (2003)
Pell et al.
(2004)
626,272 women with registered
first delivery
3593 women with a delivery
807,010 women with a delivery
15-19
13
15-19
7.8
119,668 women with first livebirth 15-19
[25]
[33]
[27]
[28]
Smith et al.
(2005)
783,340 women with a
first delivery
20.4
Low BW
CV death
1.3 [1.2,1.4]
[31]
Ray et al.
(2005)
1,026,265 women with a
first delivery
8.7
MPS composite
Premature
CV disease
2.0 [1.7,2.2]
[29]
Reproduced with permission from [29].
*Preterm delivery is defined as delivery before 37 weeks gestation.
This study reported incidence rate ratios, instead of a standard RR.
BW: Birthweight; CI: Confidence interval; CV: Cardiovascular; HDP: Hypertensive disorder of pregnancy; MPS: Maternal placental syndrome; RR: Relative risk;
SGA: Small for gestational age.
www.future-drugs.com
287
Newstead, von Dadelszen & Magee
Table 1. Retrospective cohort studies linking abnormal placentation with cardiovascular disease (cont.).
Study
Study participants
Median
follow-up
(year)
MPS at baseline
Future CV risk
Adjusted RR
[95% CI]
MPS composite +
poor fetal growth
Premature
CV disease
3.1 [2.2,4.5]
MPS composite + stillbirth
Premature
CV disease
4.4 [2.4,7.9]
Ref.
Funai et al.
(2005)
37,061 women with a delivery
24.5-36.5
Preeclampsia
3.1 [2.1,4.3]
[23]
Wikstrom
et al. (2005)
403,550 primips
15
Any HDP
1.7 [1.5,2.0]
[32]
Gestational hypertension
2.0 [1.7-2.5]
1.6 [1.3-2.0]
Mild preeclampsia
2.1 [1.8-2.5]
1.9 [1.6-2.2]
Severe preeclampsia
3.1 [2.4-4.1]
2.8 [2.2-3.7]
Any HDP + SGA + preterm
delivery
2.6 [1.8,4.7]
Arnadottir
et al. (2005)
325 women with hypertension
(cases) and 629 matched controls
50 for cases
55 for
controls
Any HDP
[22]
Mild/moderate
preeclampsia
Severe preeclampsia
Eclampsia
Reproduced with permission from [29].
*Preterm delivery is defined as delivery before 37 weeks gestation.
This study reported incidence rate ratios, instead of a standard RR.
BW: Birthweight; CI: Confidence interval; CV: Cardiovascular; HDP: Hypertensive disorder of pregnancy; MPS: Maternal placental syndrome; RR: Relative risk;
SGA: Small for gestational age.
Prevention requires both recognition of the problem and adoption of strategies to decrease risk. Physician awareness of womens
cardiovascular risk is inadequate, according to a national survey
of American physicians (primary care, obstetricians and cardiologists). These physicians were more likely to underestimate the
cardiovascular risk of women in an intermediate risk category,
compared with men of the same risk [38]. It is likely that women
themselves must be targeted in educational initiatives.
Personalization of cardiovascular risk
General knowledge is a necessary initial step towards active risk
reduction. General awareness alone is probably not sufficient.
However, perceived personal risk has been shown to increase
risk-reduction behaviors [39].
Womens awareness of cardiovascular risks, personal risks and
preventative action was examined in a random sample of
1008 American women who were interviewed via a telephone
questionnaire [38]. Only 45% of women correctly identified
their CVD risk, with 30% underestimating it and 25% overestimating it. Taking action (e.g., by seeing a healthcare provider
and making lifestyle changes) was associated with perceived
288
high risk and general awareness (particularly when they had
seen, heard or read information regarding heart disease in the
previous year). At least 90% of women stated that they took
action to improve their own health, feel better and/or live
longer. However, 67% of women said that they took action for
their family. There was no single self-reported barrier to cardiovascular health that was cited by more than 50% of women; of
note, 42% cited family obligations and 36% a lack of self-perceived risk among the top four reasons for not taking action.
Also, 56% of women stated that someone elses health was
more important to them than their own, most commonly, their
childrens (30%) and their spouses/partners (17%).
The fact that having had preeclampsia or another aspect of
the maternal placental syndrome may put their childs future
health at risk is something that may further motivate women
following complicated pregnancy. The Barker Hypothesis
states that a babys nourishment before birth and during early
life affects the development of (or programs) physiology,
including metabolism and vascular function. As such, poor
fetal and infant nutrition has been associated with an increased
risk of hypertension and diabetes key determinants of CVD.
Expert Rev. Cardiovasc. Ther. 5(2), (2007)
Preeclampsia and future cardiovascular risk
Probability of being free of cardiovascular disease (%)
There are inconsistencies and questionable assumptions in the testing of this theory. These include the assumption that
100
intrauterine growth restriction (which
has many causes) is due to poor nutrition
99
and an inability to adequately account for
Unaffected pregnancy
the impact of smoking and social class.
MPS
MPS and poor fetal growth
However, there is tremendous support for
98
MPS and fetal death
this theory and this may motivate women
to act altruistically to provide a healthy
97
lifestyle for their child.
Consequently, we may have a window of
opportunity for the identification of
96
women (and children) at risk following a
pregnancy complicated by gestational
95
hypertension, preeclampsia and/or another
component of the maternal placental syndrome. Identification of such individuals
0
at an early stage (before complications have
4
0
1
2
3
5
6
7
8
9
10 11 12 13 14
occurred) has been a major barrier to risk
Times since index delivery (years)
reduction [14].
It is well established that GDM is assoFigure 3. Risk of premature cardiovascular disease associated with abnormal placentation.
ciated with an increased risk (approxi- MPS: Maternal placental syndrome.
mately 30%) of Type II diabetes in the Adapted from [29].
long term [40,41]. It is well accepted that
these women should be counseled about this risk, the need to Strategies to decrease cardiovascular risk
monitor serum glucose at regular intervals postpartum and the There are a number of theoretical options for CVD prevention
benefits of modifying lifestyle [14]. Presumably, if there is per- in women with a history of adverse placental outcome: ensure
sonalization of risk and women are to effect change in their compliance with existing recommendations for traditional
behaviors, then the information that they receive should affect cardiovascular risk marker screening and/or treatment, as they
their long-term health perception. This was confirmed in a apply to all women of childbearing age; consider early screening
prospective cohort of 106 women with GDM, who received for traditional cardiovascular risk markers (and/or their treatthe appropriate information in a specialty clinic and were fol- ment); and/or consider early treatment of modifiable cardiolowed up 35 years after pregnancy by postal survey [42]. vascular risk markers. These will be addressed consecutively but
Compared with normal pregnancy controls (and corrected for they are not mutually exclusive. For example, the first and third
factors independently related to health perception), women approaches may be undertaken in conjunction.
with GDM were more worried about their own health, rated
their children as less healthy and perceived themselves as more Screening
likely to have diabetes. The study did not examine whether In 2004, the American Heart Association published evidencethe change in health perception was associated with a change based clinical guidelines for CVD prevention in women [2].
in health behaviors.
These guidelines recommended treatment of individual risk
In summary, women change their lifestyle for themselves markers (e.g., hyperlipidemia). When should screening for
and for their family. Having a history of a maternal placental these risk markers begin in the otherwise healthy postpartum
syndrome may be a way to emphasize or personalize risk, even woman with a history of a maternal placental syndrome?
if that risk is already apparent (e.g., owing to a history of
In Canada, the evidence-based periodic health examination
pre-existing hypertension, obesity or diabetes mellitus). for women aged 2164 years suggests routine screening only
Womens health perceptions can be changed through coun- for tobacco use and hypertension, in the absence of other
seling related to pregnancy complications, using GDM as an cardiovascular risk markers (TABLE 2).
example. Through an altered perception of personal risk,
If one looks to other sources of information for screening recwomen with a history of preeclampsia or another placental ommendations, consensus guidelines are available that are not
syndrome may be more receptive (than other women of child- graded based on available evidence. The Canadian Diabetes
bearing age) to cardiovascular risk-reduction strategies, for Association recommends screening for diabetes (by fasting
themselves and for their families. What are the options for plasma glucose) at age 40 years and then every 3 years thereafintervention once increased risk has been identified and, ter in the absence of cardiovascular risk markers [102]. The
hopefully, personalized?
American Diabetes Association is similar in recommending
www.future-drugs.com
289
Newstead, von Dadelszen & Magee
Table 2. Recommendations of the Canadian Task Force on the Periodic Health Exam: cardiovascular risk
factor screening*.
Risk marker
Minimal approach
Smoking
Smoking cessation counseling, with/without nicotine-replacement therapy offered as an adjunct (I, A)
Blood pressure
Case-finding should be considered in all persons aged 2164 years, because of high prevalence, effective detection
manoevre and efficacious treatment (III, B)
Blood sugar (diabetes)
Not recommended for asymptomatic and nonpregnant population without other cardiovascular risk markers
(II-2, D). Otherwise, screening should be individualized
Lipids
Not clear whether or not this should be performed for women of child-bearing age (III, C)
Obesity
With obesity-related disease, weight reduction can alleviate symptoms and reduce the need for drug therapy for
related diseases (I, B). Insufficient evidence to recommend against weight-reduction therapy in obese adults without
obesity-related disease owing to the limited long-term effectiveness of weight reduction methods (I, C)
*The following levels refer to the type of studies on which the recommendation is based: I (at least one properly randomized controlled trial) II-2 (well-designed cohort or
casecontrol analytic studies, preferably from more than one center or research group) III (opinions of respected authorities, based on clinical experience, descriptive
studies or reports of expert committees). The following levels refer to the quality of the evidence on which to base the recommended clinical action: A (good), B (fair),
C (conflicting).
Diabetes mellitus, hypertension, hyperlipidemia, obstructive sleep apnea or coronary artery disease.
screening at 45 years of age, particularly for individuals with a
body mass index (BMI) of 25 kg/m2 or more [103]. Individuals
with (nonpregnancy) hypertension or dyslipidemia should be
screened for diabetes at any age. The 2001 National Cholesterol Education Program guidelines (NCEP ATP III) guidelines recommend that screening with total and HDL-cholesterol testing be performed from 20 years of age and then at least
every 5 years thereafter [3]. However, screening of women
(without traditional cardiovascular risk markers) from 45 years
of age is recommended by the 2003 Canadian [43] and other
American guidelines (from the American Academy of Family
Physicians in 2003, American College of Physicians in 1996
and the US Preventive Services Task Force in 2001). Women
with risk markers should be screened for dyslipidemia,
regardless of age.
Elevated levels of the traditional cardiovascular risk markers of
hypertension, diabetes mellitus and hyperlipidemia should be
treated according to national or international evidence-based
guidelines. More aggressive intervention should not be considered unless the estimated 10-year risk of CVD is more than
10%. One point to keep in mind here is that the caregiver
should consider and discuss the possibility of future pregnancy,
given that 50% of pregnancies are unplanned. For many cardiovascular drugs (e.g., statins), there is limited information about
teratogenicity and/or fetotoxicity. However, angiotensin-converting enzyme (ACE) inhibitors (and, by association, angiotensin
receptor blockers) are contraindicated for use in pregnancy
owing to fetotoxicity and, probably, teratogenicity [44].
In summary, evidence-based and even consensus recommendations do not advocate screening for traditional cardiovascular
risk markers (other than smoking and elevated BP) before the
age of 40 years, with the possible exception of screening for
lipid abnormalities. Screening otherwise healthy women with a
history of a maternal placental syndrome for traditional cardiovascular risk markers other than hypertension and possibly,
290
hypercholesteremia, would be a step-up from existing suggestions, as most of these women will be under 4050 years of age.
There is currently no evidence to advocate this approach and the
cost implications are unknown. One could argue against early
screening and more aggressive intervention based on the fact that
women with a history of a maternal placental syndrome have a
10-year cardiovascular risk that still appears to be low (<10%).
Treatment
In the 2004 American Heart Association guidelines for CVD
prevention in women, all women are recommended to pursue
dietary and lifestyle changes, consisting of: smoking cessation,
heart-healthy diet, physical activity and weight reduction
(Class I recommendation) [2]. This recommendation applies
even to women without traditional CVD risk markers who are
at low cardiovascular risk (i.e., <10% risk over 10 years). The
details of the recommended interventions are provided in
TABLE 3. These interventions are intended to decrease adverse
cardiovascular outcomes but they may also improve subsequent
pregnancy outcome [45].
How successful are these interventions? Can women maintain
them? Can we afford them? First, it must be said that, in an
American national survey that followed publication of the 2004
guidelines, physicians did not rate themselves as very effective in
their ability to help patients prevent CVD [38]. Approximately
25% of primary-care physicians and obstetricians identified the
following as the major barriers to cardiovascular risk reduction
efforts: office time constraints, inadequate remuneration and the
patient him/herself as a barrier. Only half of low-risk women
were reported to receive recommendations for dietary changes
and only two-thirds received other lifestyle recommendations;
physicians reported spending a mean of 8 min providing this
information at routine annual visits. Mutually desired change is
most likely to occur when there is a therapeutic alliance between
caregiver and patient [46].
Expert Rev. Cardiovasc. Ther. 5(2), (2007)
Preeclampsia and future cardiovascular risk
Table 3. American Heart Association lifestyle recommendations for cardiovascular disease prevention in all women.
Intervention
Consistently encourage women*
Smoking
cessation
Not to smoke and avoid environmental tobacco (I, B)
Heart:
healthy diet
To adopt an overall healthy eating pattern that includes intake of a variety of fruits, vegetables, grains, low-fat or nonfat
diary projects, fish, legumes and sources of protein low in saturated fat (e.g., poultry, lean meats, plant sources). Limit
saturated fat intake to <10% and calories, limit cholesterol intake to <300 mg/day and limit intake of trans fatty acids (I, B)
Physical activity To accumulate 30 min of moderate-intensity physical activity (e.g., brisk walking) on most, and preferably all, days of the
week (I, B)
Weight
reduction
To maintain/reduce their weight through an appropriate balance of physical activity, caloric intake and formal behavioral
programmes when indicated to achieve a body mass index of 18.5-24.9 kg/m2 and a waist circumference <78.4 cm (I, B)
Reproduced with permission from [2].
*Classification of recommendations: Class I (intervention is useful and effective); Level of evidence B (limited evidence from a single randomized controlled trial or other
nonrandomized studies).
Smoking cessation strategies inform our understanding of
how to most effectively counsel and affect behavior. Abstinence
rates are lowest when there is no particular format to the counseling, higher with self-help material, proactive telephone counseling or group counseling, and highest with individual counseling. Lessons learned from this literature have led to the
Surgeon Generals 5As for intervention: Ask (about tobacco
use), Advise (to quit), Assess willingness (to make a quit
attempt), Assist (in quit attempt) and Arrange follow-up. These
As highlight the fact that attempts to change lifestyle are just
that and that assistance is needed, and needed over time, as subsequent attempts are likely to be necessary.
Can we afford lifestyle interventions? The Finnish Diabetes
Prevention Study informs our understanding of the benefits
reaped by lifestyle changes but at high cost to the healthcare system. The study examined dietary and lifestyle modification as a
way to prevent or delay diabetes in individuals with impaired
glucose intolerance [47]. The intervention group was advised on
how to achieve the following goals: 5% weight reduction,
decrease in fat intake to less than 30% of calories, increase in
fiber intake and at least 30 min/day of moderate exercise. Dietary counseling was intensive: seven sessions in year 1, then quarterly thereafter (and guided by quarterly 3-day food diaries).
Physical activity counseling was individualized based on degree
of fitness and supervised resistance training sessions were also
offered (and accepted by 5085% of subjects, depending on the
center). The control group received general verbal and written
information on diet and exercise at baseline and at annual visits,
but no specific program was offered to them. They completed
food diaries annually. Overall, the intervention group was more
likely than controls to report changes in diet and lifestyle and
weight reduction (by 3.5 vs 0.8 kg) and less likely to develop diabetes mellitus (i.e., 32 vs 78 cases per 1000 person-years).
The costeffectiveness of strategies for managing people at high
risk of diabetes was examined using data from the published literature, including basic and epidemiological studies, clinical trials
and Kaiser Permanente administrative data [48]. These figures are
based on individuals at high risk of diabetes; individuals at lower
www.future-drugs.com
risk would presumably benefit less and, therefore, the cost would
be greater. Taking the societal perspective, compared with not
undertaking a lifestyle change program, implementing the plan
undertaken in the Diabetes Prevention Program study [47] for
high-risk individuals would cost US$62,600 per quality-adjusted
life-year (QALY). The program would be cost-saving over
30 years if the annual cost of the intervention could be reduced to
approximately US$100. This would be difficult indeed.
Special note: weight gain in pregnancy
Obesity is a risk marker for both the maternal placental syndrome and CVD so it will be present in many women with a history of preeclampsia or the maternal placental syndrome. Treatment of obesity is modestly effective (e.g., a loss of 35 kg for
1 year or more) [49]. The public-health focus has moved to prevention. As pregnancy-related weight gain is a trigger for weight
retention, it follows that weight during pregnancy warrants
special consideration.
Weight gain during a healthy pregnancy is unavoidable and
expected. The average weight gain is 12.5 kg. The recommended weight gain for women with a normal prepregnancy
BMI (19.926.6 kg/m2) is 1116 kg. Weight-gain goals are
lower for women who are overweight at the start of pregnancy.
The Stockholm Pregnancy and Weight Development Study
was a long-term follow-up study of women who had a mean
weight increase of 14.1 4.1 kg during pregnancy, 15 years
previously [50]. A number of important findings were made.
First, based on prepregnancy characteristics, it was difficult to
predict who was likely to retain pregnancy-related weight gain
after pregnancy. Not surprisingly, women who were overweight
on follow-up at 15 years had a higher prepregnancy BMI
(22.3 1.5 vs 20.5 1.6 kg/m2), gained more weight during
pregnancy (15.4 4.4 vs 13.6 3.7 kg), retained more weight
at 1 year postpartum and had more rapid age-related weight
gain between 1 and 15 years postpartum. However, most
women who became overweight had a normal prepregnancy
BMI of 2025 kg/m2. Also, the differences in prepregnancy
weight between women who became overweight (versus those
291
Newstead, von Dadelszen & Magee
who did not) were small and variation was wide. Women who
became overweight were more likely to quit smoking during
pregnancy and less likely to breastfeed; otherwise, there were no
other demographics or pregnancy characteristics that differed
between groups. Previous reports on this cohort at 1 year postpartum identified an association between weight retention at
1 year postpartum and both less frequent exercise and a change
to more irregular eating habits. The overall conclusion was that
it is difficult to predict who will gain weight during pregnancy
and who will retain weight postpartum, and that there is much
that we do not know. Dietary and lifestyle changes associated
with having a new baby may play a role. At this stage, observation over time, rather than prevention by identifying those at
risk, appears to be the best option. Perhaps close follow-up of
women who are indeed gaining and retaining weight is the key
to halting and reversing this worrisome trend in their health.
In summary, in nonpregnant populations, dietary and lifestyle
changes are effective in decreasing surrogate markers of CVD
(e.g., glucose tolerance and BP), as well as cardiovascular outcomes per se. However, how best to make these dietary and lifestyle changes, and maintain those changes at a reasonable cost to
the public healthcare system is uncertain. These interventions
require time and effort on behalf of the patients and caregivers,
including those providing routine gynecological care.
Conclusions
CVD is responsible for more than 50% of deaths among
women worldwide. It would appear that pregnancy is a metabolic and vascular stress test for women, and that those who
fail are at increased risk of long-term cardiovascular complications. Specifically, women who develop preeclampsia
(and/or other manifestations of maternal placental syndrome)
are at increased risk of coronary heart disease, stroke and
CVD in general. Risk is highest among women who develop
both maternal (e.g., hypertension and proteinuria) and fetal
(e.g., intrauterine growth restriction) manifestations of
abnormal placentation, especially with preterm delivery. Most
women who develop maternal placental syndrome return to a
normal clinical state in the weeks following pregnancy and
their absolute risk of CVD in the short term is very low.
It is unclear how the increased long-term cardiovascular
risk should be handled in women with a history of maternal
placental syndrome, given that this is a novel cardiovascular
risk factor. The American Heart Association recommends
that all women (even those at low cardiovascular risk) pursue
dietary and lifestyle changes, in addition to smoking cessation. Perhaps having a placentally complicated pregnancy
affords women the opportunity to personalize risk and take
action. This action requires a huge commitment and
sustained effort by not only the woman but also her family
and her caregiver.
Expert commentary
At present, a history of preeclampsia, or another of the placentally mediated adverse pregnancy outcomes, can be regarded as
a novel cardiovascular risk factor. There are no existing guidelines or strategies in place for how to deal with this problem.
CVD is the number one killer of women. We must find ways,
through postpartum counseling and routine gynecological care,
to engage this section of the population and to ensure better
uptake of the general recommendation for all women to pursue
a healthy diet and lifestyle.
Five-year view
Engaging women of child-bearing age who may be motivated
by a complicated pregnancy would be very valuable from a
public health perspective, given the prevalence and importance of CVD in women, and the central role of the woman
Key issues
Cardiovascular disease (CVD) is a womens health issue.
Pregnancy appears to be a metabolic and vascular stress test for women and those who fail are at increased risk of long-term
cardiovascular complications.
Women who develop preeclampsia (and/or other manifestations of a maternal placental syndrome) are at an increased risk of
coronary heart disease, stroke and CVD in the long term, although the absolute risk is low and not immediate.
The long-term risk of CVD is highest among women who develop both maternal (e.g., hypertension and proteinuria) and fetal
(e.g., intrauterine growth restriction) manifestations of abnormal placentation, especially with preterm delivery.
Most women who develop a maternal placental syndrome return to a normal clinical state in the weeks following pregnancy and
their absolute risk of CVD in the short term is very low.
Among women with a history of preeclampsia (or another maternal placental syndrome), it is unclear how this increased long-term
cardiovascular risk should be handled with respect to cardiovascular risk marker screening and/or treatment.
The American Heart Association recommends that all women (even those at low cardiovascular risk) pursue dietary and lifestyle
changes, in addition to smoking cessation.
Personalization of risk is an important component of engagement in risk reduction strategies.
292
Expert Rev. Cardiovasc. Ther. 5(2), (2007)
Preeclampsia and future cardiovascular risk
as a caregiver to children, their spouse and other family members. Lifestyle interventions, which are useful for all women,
may improve subsequent pregnancy outcomes, as well as
References
Papers of special note have been highlighted as:
of interest
of considerable interest
1
Miller TD, Balady GJ, Fletcher GF.
Exercise and its role in the prevention and
rehabilitation of cardiovascular disease.
Ann. Behav. Med. 19(3), 220229 (1997).
Mosca L, Appel LJ, Benjamin EJ et al.
Evidence-based guidelines for
cardiovascular disease prevention in
women. Circulation 109(5), 672693
(2004).
Excellent summary of current
cardiovascular disease (CVD) prevention
recommendations specifically for women.
Third Report of the National Cholesterol
Education Program (NCEP) Expert Panel
on detection, evaluation, and treatment of
high blood cholesterol in adults (Adult
Treatment Panel III) final report.
Circulation 106(25), 31433421 (2002).
11
12
Sattar N, Greer IA. Pregnancy
complications and maternal cardiovascular
risk: opportunities for intervention and
screening? Br. Med. J. 325(7356), 157160
(2002).
26
15
Ness RB, Hubel CA. Risk for coronary
artery disease and morbid preeclampsia: a
commentary. Ann. Epidemiol. 15(9),
726733 (2005).
Jonsdottir LS, Arngrimsson R,
Geirsson RT, Sigvaldason H, Sigfusson N.
Death rates from ischemic heart disease in
women with a history of hypertension in
pregnancy. Acta Obstet. Gynecol. Scand.
74(10), 772776 (1995).
27
Rodie VA, Freeman DJ, Sattar N, Greer IA.
Pre-eclampsia and cardiovascular disease:
metabolic syndrome of pregnancy?
Atherosclerosis 175(2), 189202 (2004).
Kestenbaum B, Seliger SL, Easterling TR
et al. Cardiovascular and thromboembolic
events following hypertensive pregnancy.
Am. J. Kidney Dis. 42(5), 982989 (2003).
28
Pell JP, Smith GC, Walsh D. Pregnancy
complications and subsequent maternal
cerebrovascular events: a retrospective
cohort study of 119,668 births. Am. J.
Epidemiol. 159(4), 336342 (2004).
29
Ray JG, Vermeulen MJ, Schull MJ,
Redelmeier DA. Cardiovascular health after
maternal placental syndromes (CHAMPS),
population-based retrospective cohort
study. Lancet 366(9499), 17971803
(2005).
Excellent review of maternal placental
syndrome and its association with CVD.
16
Helewa ME, Burrows RF, Smith J,
Williams K, Brain P, Rabkin SW. Report of
the Canadian Hypertension Society
Consensus Conference: 1. Definitions,
evaluation and classification of hypertensive
disorders in pregnancy. CMAJ 157(6),
715725 (1997).
18
10
von Dadelszen P, Magee LA, Lee SK et al.
Activated protein C in normal human
pregnancy and pregnancies complicated by
severe preeclampsia: a therapeutic
opportunity? Crit. Care Med. 30(8),
18831892 (2002).
Roberts JM, Gammill HS. Preeclampsia:
recent insights. Hypertension 46(6),
12431249 (2005).
www.future-drugs.com
Hannaford P, Ferry S, Hirsch S.
Cardiovascular sequelae of toxaemia of
pregnancy. Heart 77(2), 154158 (1997).
14
17
Allen VM. The effect of hypertensive
disorders in pregnancy on perinatal
outcomes: a population-based cohort
study. National Library of Canada Ottawa
(2002).
24
Irgens HU, Reisaeter L, Irgens LM, Lie RT.
Long term mortality of mothers and fathers
after pre-eclampsia: population based
cohort study. Br. Med. J. 323(7323),
12131217 (2001).
Report of the National High Blood Pressure
Education Program Working Group on
high blood pressure in pregnancy. Am. J.
Obstet. Gynecol. 183(1), S1S22 (2000).
Karumanchi SA, Bdolah Y. Hypoxia and
sFlt-1 in preeclampsia: the chicken-andegg question. Endocrinology 145(11),
48354837 (2004).
Funai EF, Friedlander Y, Paltiel O et al.
Long-term mortality after preeclampsia.
Epidemiology 16(2), 206215 (2005).
25
Brown MA, Hague WM, Higgins J et al.
The detection, investigation and
management of hypertension in pregnancy:
executive summary. Aust. NZ J. Obstet.
Gynaecol. 40(2), 133138 (2000).
23
Redman CWG. The placenta, preeclampsia and chronic villitis. In: The
Human Placenta. Redman CWG,
Sargent ILSP (Eds). Blackwell Scientific,
Oxford, UK, 433467 (1993).
Feldman R, Genest J. Global risk
assessment in 2005: where do we stand?
Expert Opin. Clin. Impact 1(7), 35 (2005).
286292 (2005).
Roberts JM, Lain KY. Recent Insights into
the pathogenesis of pre-eclampsia. Placenta
23(5), 359372 (2002).
13
decreasing cardiovascular risk in the long term. Whether
women and their families will engage in such a strategy is an
important question to be addressed by future research.
19
James PR, Nelson-Piercy C. Management
of hypertension before, during, and after
pregnancy. Heart 90(12), 14991504
(2004).
von Dadelszen P, Magee LA, Krajden M
et al. Levels of antibodies against
cytomegalovirus and Chlamydophila
pneumoniae are increased in early onset preeclampsia. Br. J. Obstet. Gynaecol. 110(8),
725730 (2003).
von Dadelszen P, Magee LA. Could an
infectious trigger explain the differential
maternal response to the shared placental
pathology of preeclampsia and
normotensive intrauterine growth
restriction? Acta Obstet. Gynecol. Scand.
81(7), 642648 (2002).
20
De Wolf F, Robertson WB, Brosens I. The
ultrastructure of acute atherosis in
hypertensive pregnancy. Am. J. Obstet.
Gynecol. 123(2), 164174 (1975).
21
Chesley LC, Annitto JE, Cosgrove RA. The
remote prognosis of eclamptic women.
Sixth periodic report. Am. J. Obstet.
Gynecol. 124, 446459 (1978).
22
Arnadottir GA, Geirsson RT, Arngrimsson
R, Jonsdottir LS, Olafsson O.
Cardiovascular death in women who had
hypertension in pregnancy: a casecontrol
study. Br. J. Obstet. Gynaecol. 112(3),
30
Smith GC, Pell JP, Walsh D. Pregnancy
complications and maternal risk of
ischaemic heart disease: a retrospective
cohort study of 129,290 births. Lancet
357(9273), 20022006 (2001).
31
Smith GD, Sterne J, Tynelius P,
Lawlor DA, Rasmussen F. Birth weight of
offspring and subsequent cardiovascular
mortality of the parents. Epidemiology
16(4), 563569 (2005).
32
Wikstrom AK, Haglund B, Olovsson M,
Lindeberg SN. The risk of maternal
ischaemic heart disease after gestational
hypertensive disease. Br. J. Obstet. Gynaecol.
112(11), 14861491 (2005).
33
Wilson BJ, Watson MS, Prescott GJ et al.
Hypertensive diseases of pregnancy and risk
of hypertension and stroke in later life:
results from cohort study. Br. Med. J.
326(7394), 845 (2003).
293
Newstead, von Dadelszen & Magee
34
35
36
37
38
Mann JI, Doll R, Thorogood M,
Vessey MP, Waters WE. Risk factors for
myocardial infarction in young women.
Br. J. Prev. Soc. Med. 30(2), 94100 (1976).
Grady D, Herrington D, Bittner V et al.
Cardiovascular disease outcomes during 6.8
years of hormone therapy: Heart and
Estrogen/progestin Replacement Study
follow-up (HERS II). JAMA 288(1), 4957
(2002).
Chobanian AV, Bakris GL, Black HR et al.
The Seventh Report of the Joint National
Committee on Prevention, Detection,
Evaluation, and treatment of high blood
pressure: the JNC 7 report. JAMA 289(19),
25602572 (2003).
Khan NA, McAlister FA, Rabkin SW et al.
The 2006 Canadian Hypertension
Education Program recommendations for
the management of hypertension: part II
therapy. Can. J. Cardiol. 22(7), 583593
(2006).
Mosca L, Linfante AH, Benjamin EJ et al.
National study of physician awareness and
adherence to cardiovascular disease
prevention guidelines. Circulation 111(4),
499510 (2005).
Provides insight into womens awareness
and their basis for decision making about
preventative health interventions.
39
Rosentock IM. Historical origins of the
health belief model. Health Ed. Monogr. 2,
328333 (1974).
40
Ali Z, Alexis SD. Occurrence of diabetes
mellitus after gestational diabetes mellitus
in Trinidad. Diabetes Care 13(5), 527529
(1990).
41
Kaufmann RC, Schleyhahn FT,
Huffman DG, Amankwah KS.
Gestational diabetes diagnostic criteria:
long-term maternal follow-up. Am. J.
Obstet. Gynecol. 172(2 Pt 1), 621625
(1995).
294
42
43
Feig DS, Chen E, Naylor CD. Selfperceived health status of women three to
five years after the diagnosis of gestational
diabetes: a survey of cases and matched
controls. Am. J. Obstet. Gynecol. 178(2),
386393 (1998).
Genest J, Frohlich J, Fodor G,
McPherson R. Recommendations for the
management of dyslipidemia and the
prevention of cardiovascular disease:
summary of the 2003 update. CMAJ
169(9), 921924 (2003).
44
Scialli AR, Lione A. ACE inhibitors and
major congenital malformations. N. Engl. J.
Med. 355(12), 1280 (2006).
45
Clapp JF III, Kim H, Burciu B, Lopez B.
Beginning regular exercise in early pregnancy:
effect on fetoplacental growth. Am. J. Obstet.
Gynecol. 183(6), 14841488 (2000).
46
Rosenstock IM. Adoption and maintenance
of lifestyle modifications. Am. J. Prev. Med.
4(6), 349352 (1988).
47
Tuomilehto J, Lindstrom J, Eriksson JG
et al. Prevention of type 2 diabetes mellitus
by changes in lifestyle among subjects with
impaired glucose tolerance. N. Engl. J. Med.
344(18), 13431350 (2001).
48
Eddy DM, Schlessinger L, Kahn R. Clinical
outcomes and cost-effectiveness of
strategies for managing people at high risk
for diabetes. Ann. Intern. Med. 143(4),
251264 (2005).
Provides an example of strategies used for
gestational diabetes, which is undisputed
as a strong risk marker for Type 2 diabetes.
49
McTigue KM, Harris R, Hemphill B et al.
Screening and interventions for obesity in
adults: summary of the evidence for the
U.S. Preventive Services Task Force. Ann.
Intern. Med. 139(11), 933949 (2003).
50
Linne Y, Dye L, Barkeling B, Rossner S.
Weight development over time in parous
women the SPAWN study 15 years
follow-up. Int. J. Obes. Relat. Metab. Disord.
27(12), 15161522 (2003).
Websites
101
10-year cardiovascular disease
risk calculator
http://hp2010.nhlbihin.net/atpiii/calculato
r.asp?usertype=prof
102
Canadian Diabetes Association
www.diabetes.ca
103
American Diabetes Association
www.diabetes.org
Affiliations
J Newstead, MD, FRCP(C)
Assistant Professor of Medicine, University of
Saskatchewan, Department of Medicine,
Saskatoon, SK, Canada
Tel.: +1 306 966 2180
Fax: +1 306 966 1943
jill.newstead@shaw.ca
P von Dadelszen, MBChB, DPhil, FRCSC, FRCOG
Associate Professor of Obstetrics and
Gynaecology, Department of Obstetrics and
Gynaecology and the Centre for Applied Health
Research and Evaluation, Vancouver,
BC, Canada
Tel.: +1 604 875 3054
Fax: +1 604 875 2725
pvd@cw.bc.ca
Laura A Magee, MD, FRCP(C), MSc, FACP
Clinical Associate Professor of Medicine,
University of British Columbia, Departments of
Obstetrics and Gynaecology and Medicine, and
the Centre for Applied Health Research and
Evaluation, Child and Family Research Institute
of British Columbia, and British Columbias
Womens Hospital and Health Centre, 4500 Oak
Street, Room 1U59, Vancouver V6H 3N1,
BC, Canada
Tel.: +1 604 875 2960
Fax: +1 604 875 2961
lmagee@cw.bc.ca
Expert Rev. Cardiovasc. Ther. 5(2), (2007)
Reproduced with permission of the copyright owner. Further reproduction prohibited without permission.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Check - Unit - 554 - October - Renal - Problems V2 PDFDocument26 pagesCheck - Unit - 554 - October - Renal - Problems V2 PDFdragon660% (1)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Pearson - Vue - 200 QUESTIONS PDFDocument40 pagesPearson - Vue - 200 QUESTIONS PDFDr-Jahanzaib Gondal100% (2)
- Annex A - Driver's Medical Evaluation Form (August 8 2018) - 2Document2 pagesAnnex A - Driver's Medical Evaluation Form (August 8 2018) - 2Dhon de CastroNo ratings yet
- DiaDENS-PC Operation ManualDocument72 pagesDiaDENS-PC Operation Manualgetdenas100% (7)
- Malaria: Prima Dewi Yuliani 1210312120 Widyatul Aina Alfioni ParsiskaDocument27 pagesMalaria: Prima Dewi Yuliani 1210312120 Widyatul Aina Alfioni ParsiskaAnonymous Di1zSIkRBHNo ratings yet
- Classification of Congenital Heart DiseaseDocument1 pageClassification of Congenital Heart DiseaseAnonymous Di1zSIkRBHNo ratings yet
- Sepsis Update 2017 - 2Document49 pagesSepsis Update 2017 - 2Ahmad Fathul Adzmi100% (1)
- Instruction Set Architecture (ISA) : ISA Level Elements of Instructions Instructions Types Number of Addresses Registers Types of OperandsDocument51 pagesInstruction Set Architecture (ISA) : ISA Level Elements of Instructions Instructions Types Number of Addresses Registers Types of OperandsAnonymous Di1zSIkRBHNo ratings yet
- Who 2014Document100 pagesWho 2014Anonymous Di1zSIkRBHNo ratings yet
- Report of Treasurer RusDocument5 pagesReport of Treasurer RusAnonymous Di1zSIkRBHNo ratings yet
- 54 5 5 PDFDocument7 pages54 5 5 PDFTri Umi Maslakhatut DiniahNo ratings yet
- Presentasi Modul 1Document16 pagesPresentasi Modul 1Anonymous Di1zSIkRBHNo ratings yet
- PLENO21CKULITDocument20 pagesPLENO21CKULITAnonymous Di1zSIkRBHNo ratings yet
- After Studying This ChapterDocument2 pagesAfter Studying This ChapterAnonymous Di1zSIkRBHNo ratings yet
- CoolmanDocument7 pagesCoolmanAnonymous Di1zSIkRBHNo ratings yet
- Implikasi Bla2Document7 pagesImplikasi Bla2Anonymous Di1zSIkRBHNo ratings yet
- Hepatoprotective Constituents of Firmiana Hepatocytes WebsiteDocument2 pagesHepatoprotective Constituents of Firmiana Hepatocytes WebsiteAnonymous Di1zSIkRBHNo ratings yet
- PlenoDocument17 pagesPlenoAnonymous Di1zSIkRBHNo ratings yet
- Pleno PresentationDocument14 pagesPleno PresentationAnonymous Di1zSIkRBHNo ratings yet
- Hepatoprotective Constituents of Firmiana Hepatocytes WebsiteDocument2 pagesHepatoprotective Constituents of Firmiana Hepatocytes WebsiteAnonymous Di1zSIkRBHNo ratings yet
- Presentation 1Document2 pagesPresentation 1Anonymous Di1zSIkRBHNo ratings yet
- Presentation 2Document2 pagesPresentation 2Anonymous Di1zSIkRBHNo ratings yet
- Kuliah OiDocument61 pagesKuliah OiNovasuryatiNo ratings yet
- JadwalDocument1 pageJadwalAnonymous Di1zSIkRBHNo ratings yet
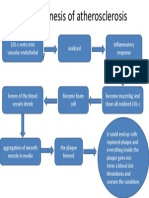
- Pathogenesis of AtherosclerosisDocument1 pagePathogenesis of AtherosclerosisAnonymous Di1zSIkRBHNo ratings yet
- Slide Progosis Dan KomplikasDocument2 pagesSlide Progosis Dan KomplikasAnonymous Di1zSIkRBHNo ratings yet
- Third Party Legal NoticesDocument1 pageThird Party Legal NoticesvincexianNo ratings yet
- SkemaDocument1 pageSkemaAnonymous Di1zSIkRBHNo ratings yet
- GetAmped2ClientSoftwareLicenseAgreement HKDocument2 pagesGetAmped2ClientSoftwareLicenseAgreement HKAnonymous Di1zSIkRBHNo ratings yet
- InfeksiDocument2 pagesInfeksiAnonymous Di1zSIkRBHNo ratings yet
- Inflation ExpectationsasaDocument29 pagesInflation ExpectationsasaAnonymous Di1zSIkRBHNo ratings yet
- F4 SC Nota Bab 3 Techniques of Measuring The Parameters of Body HealthDocument13 pagesF4 SC Nota Bab 3 Techniques of Measuring The Parameters of Body HealthJIanyun ChanNo ratings yet
- Case Study: Treating Hypertension in Patients With DiabetesDocument10 pagesCase Study: Treating Hypertension in Patients With Diabetesfirda rydNo ratings yet
- Community Health Survey ToolDocument6 pagesCommunity Health Survey ToolYna EstabilloNo ratings yet
- 312 Lec Cu10Document4 pages312 Lec Cu10Carl SantosNo ratings yet
- Sab Theek ReportDocument8 pagesSab Theek ReportAyusmanNo ratings yet
- Diagnosis of Pulmonary HypertensionDocument12 pagesDiagnosis of Pulmonary HypertensionFaridaFaradillaPutryCherewetNo ratings yet
- Health Problem Family Nursing Problem Goal of Care Objectives of Care Intervention PlanDocument2 pagesHealth Problem Family Nursing Problem Goal of Care Objectives of Care Intervention PlanCarol MalcoNo ratings yet
- Operative Orthopaedics Stanmore Guide 2010Document329 pagesOperative Orthopaedics Stanmore Guide 2010Shourjendra Datta100% (11)
- Ehx 273Document4 pagesEhx 273Robby Paguh TariganNo ratings yet
- Pre Eclampsia Eclampsia Guideline For The Management of SevereDocument15 pagesPre Eclampsia Eclampsia Guideline For The Management of SevereAris SaptianNo ratings yet
- Discussion: Cardiovascular Disease Mini-Case Study Case Study #2 Cardiovascular DiseaseDocument3 pagesDiscussion: Cardiovascular Disease Mini-Case Study Case Study #2 Cardiovascular Diseaseapi-546898544No ratings yet
- Ineffective Breathing Pattern Related To Shortness of Breath Possible Evidence by CuesDocument7 pagesIneffective Breathing Pattern Related To Shortness of Breath Possible Evidence by CuesLouie ParillaNo ratings yet
- Acute Ischemic Stroke: Clinical PracticeDocument8 pagesAcute Ischemic Stroke: Clinical PracticeDorina FrunzeNo ratings yet
- Nur 111 Session 15 Sas 1Document8 pagesNur 111 Session 15 Sas 1Zzimply Tri Sha UmaliNo ratings yet
- Unit 8 BSC 3rd YearDocument20 pagesUnit 8 BSC 3rd Yearsimonjosan100% (2)
- Afif Zikri Bin Abd Aziz - Eh2204wwDocument8 pagesAfif Zikri Bin Abd Aziz - Eh2204wwMOHD MU'IZZ MOHD SHUKRINo ratings yet
- Case Study HypertensionDocument29 pagesCase Study HypertensionnilamNo ratings yet
- Angel Hill's ThesisDocument45 pagesAngel Hill's ThesisJoan MelendresNo ratings yet
- 21 TranslatedDocument71 pages21 TranslatedMerry MonroeNo ratings yet
- Stroke in Pregnancy and The Puerperium: S D Treadwell, B Thanvi, T G RobinsonDocument8 pagesStroke in Pregnancy and The Puerperium: S D Treadwell, B Thanvi, T G RobinsonNabillah MukhlisNo ratings yet
- 12 Physical Education English Medium Chapter PDFDocument36 pages12 Physical Education English Medium Chapter PDFRohit0% (1)
- Medical Examination Report: A. Examinee DetailsDocument4 pagesMedical Examination Report: A. Examinee DetailsMohammed Bilal ShaikNo ratings yet
- NTRN 516 Case Study 2 - DM 10 12 15 UpdateDocument18 pagesNTRN 516 Case Study 2 - DM 10 12 15 Updateapi-315324296No ratings yet
- MAPEH 9 Second GradingDocument9 pagesMAPEH 9 Second GradingSittie Rahma AlawiNo ratings yet
- MidtermDocument53 pagesMidtermwriter topNo ratings yet
- 2022 05 CK May GK Shots PDFDocument262 pages2022 05 CK May GK Shots PDFCommon PhoneNo ratings yet