Professional Documents
Culture Documents
Gynecology HX
Uploaded by
lovelots1234Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Gynecology HX
Uploaded by
lovelots1234Copyright:
Available Formats
GYNECOLOGY
Helen B. Albano, MD, FPOGS
Medical History
The quality of the medical care provided by the
physician
Type of relationship between physician and the
patient
o Can be determined largely the depth of
gynecological history
Patient-Doctor Relationship
o Complete history
o Complete PE
o Labs
New Patient
o Take Time
Obtain comprehensive history
Perform comprehensive PE
o Establish data base, along with DPR basd on
a good communication
Old Patient or the established patient
o Updates
Gynecological changes
Pregnancy history
Additional surgery, accidents or new
medications
History Taking
Overview
o Most important part of gynecological
evaluation
o Provides tentative diagnosis (impression)
before PE
o LEGAL document
Subject to subpoena, may be
defended in court
General Data
Name
Age
Gravidity (G)
o State of being pregnant
Parity (P)
o Outcome of pregnancy
o FPAL (in digits)
F = number of full term pregnancy
P = number of preterm pregnancy
A = Abortion
L = total number of living children
o Ex: G1P0 0001
LMP (Last Menstrual Period)
o Also take the first and last day of normal
menstruation
PNMP (Previous Normal Menstrual Period)
EDC/EDD and AOG Expected Date of
Confinement/Delivery
o Nigellas EDC
3 mos back + 7 + 1year ???
o AOG (wks of gestation)
Date and Time of Consultation/Admission
Chief Complaint
Only one
Reason for admission
Common gynecological complaints
o Bleeding (vaginal)
o Pain (specify: use 9 regions of abdomen)
o Mass (abdominal or pelvic)
o Vaginal discharge
o Urinary or GI symptoms
o Protrusion out of the vagina
o Infertility
HPI (History of Present Illness)
Refers to the chief complaint
o Duration
o Severity
o Precipitating factors
o Occurrence in relation to other events
Menstrual cycle
Voiding
Bowel movements
History of similar symptoms
Outcome of previous therapies
Impact on the patients:
o Quality of life
o Self-image
o Relationship with the family (sexual history
to husband)
o Daily activities
Menstrual History
Age of menarche
Date of onset of menstrual periods
Duration and quantity (i.e. number of pads used per
day) of flow
Degree of Discomfort
Premenstrual symptoms
Cycle
o Counted from the first day of menstrual flow
of one cycle to the first day of menstrual
flow of the next
Range of normal is wide
o Normal range of ovulatory cycles
Between 21 & 35 days
o 28-day cycle represent the median cycle
o A recent change in the usual pattern maybe
a more reliable sign of a problem
Average menstrual blood loss
o 30 ml (entire)
o 10-80 ml (normal range)
Excessive menses
o Need to frequently change saturated
sanitary pads or tampons
o Passage of many or large blood clots
Dysmenorrhea
o Painful menstruation
o Discomfort or pain at the hypogastric area,
often associated with backache
o Common
o Begins just before or soon after the onset of
bleeding
o Subsides by day 2 or 3 of flow
o May be associated with systemic symptoms
Obstetric History
Number of pregnancies
FPAL
Complications of previous pregnancies
o Antepartum, intrapartum or postpartum
Duration of labor
Type of delivery
o Place: hospital, house, hilot, TBA, physician
Anesthesia used
Perinatal status of fetus
o Birthweight
o Early growth and development of children
including feeding habits, growth, overall
well-being, current status
History of Infertility
o Evaluation, diagnosis, treatment, outcome
Medical History
Allergies
Past and current medical and surgical problems
Previous hospitalizations
o Reason, date, outcome
Vaccination
o Type, date
Surgical History
Operative procedure
o Outcomes
o Complications
o Surgical diagnosis
o Pathologic diagnosis
Review of Systems (subjective)
Pulmonary
Cardiovascular
Gastrointestinal
Genital
Urinary
o Dont combine, as in GU
Vascular
Neurologic
Endocrinologic
Immunologic
Breast Symptoms
Masses
Galactorrhea
Pain
Family history
Social History
Marital status
o Number of years married
o Period of infertility
Drug (causes abruption placenta), alcohol use,
smoking
Occupational History
o Exposure to radiation
o Infectious agents
Sexual History
o Partners, protection from STDs
Emotional or sexual abuse
Family History
Significant medical and surgical disorders that runs
in the family
Heredofamilial diseases
Evaluation of the General Appearance
General Impression
o Level of consciousness
o Ambulatory
o Nutritional state
o Presence of facial or excessive body hair
o Vital signs
Physical Examination (PE)
(objective)
Follows IPPA (with exception of certain organs)
Head and Neck
Chest and Lungs
Heart
Breast
Abdomen
Lower extremities
Pelvic examination
Gynecological Examination
Pelvic Examination
o Most commonly performed medical
procedure
o Performed during the first visit
o Patient should be encouraged to give
feedback during PE to reduce anxiety
o Lithotomy position
Patient lying on her back with both
knees flexed
Buttocks are positioned at the edge
of the table
The feet are supported by stirrups
o The patient should empty her bladder just
before the examination
Pelvic Examination consist of:
o Inspection
Visual inspection of the vulva
Speculum examination vagina and
cervix
o Palpation
Bimanual pelvic examination
o Lithotomy position to allow adequate
exposure
o She should be comfortable and properly
draped
o Should not be painful except in:
Virgins and has not used tampons
for menstrual protection
In women with inflammatory
processes
Menopausic nulligravid
Inspection of the Vulva
o The vulva should be examined for:
General state of hygiene
Growth of hair
Regions of ulceration and rash
Discoloration
Labial abnormality
Excessive vaginal discharge
Lochia discharged after
delivery
Evidence of perineal trauma from
previous deliveries
Evidence of rectal disease
hemorrhoids
Bartholins and Skeenes glands can
be inspected and palpated
Presence of ectovaginal fistula or
prolapsed
Guidelines in Daily Pelvic Examination
Warning
o The physician should prepare the patient for
any pelvic examination by warning her in
advance and examining fingers and
speculum
Important:
o Not only because the patient cannot see
what is going on
o But also because the area to be examined is
extremely sensitive, both psychologically
and physically
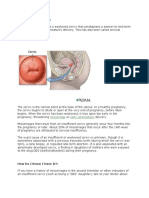
Inspection of the Vagina and Cervix
Graves Speculum
o Employed for visualization of the vagina and
cervix
o Bivalve
Anterior valve shorter than the
posterior valve
Speculum Examination
Techniques that should be remembered in speculum
exam
If for pap smear, the speculum
should be warmed, either by a
warming device or placing in warm
water, if and then it should be
lubricated
By spreading the labia and placing
some tension on the posterior
fourchet, the speculum can be
gently inserted at an angle of about
45O to avoid the urethra
o Speculum insertion
Placing the tranverse diameter of
the blades in the anteroposterior
position and guding the blades
through the introitus in a downward
motion with the tips pointing toward
the rectum
The anterior wall of the vagina is
backed by the pubic symphysis,
upward pressure causes patient
discomfort.
In the resting state, the vagina lies
on the rectum and actually extends
to the rectum
The speculum should be turned so
that the transverse axis of the
blades is in transverse axis of the
vagina
It should now lie inferior to the
cervix
With gentle opening of the
speculum, the valves separate and
the cervix can be visualized
The blades should be inserted to
their full length
The cervix is inspected next
It should be pink, shiny and clear
Nulliparous external os should be
round
Parous external os takes on a
fishmouth appearance
With previous cervical
lacerations, healed stellate
laceration may be found
Inspection
o The cervix should be inspected for
Color
Erosion
Degree of discharge (leucorrhea
discharges other than blood)
Evidence of trauma
Presence of lesion
*Pap smear is encouraged if not done yet
Pap Smear
Major objectives:
1. sample exfoliated cells from the
endocervical canal
2. Scrape the transitional zone
A collection of cells from the posterior fornix
(maturation index)
Bimanual Pelvic Exam
After the speculum has been.
It is helpful to place a stool at the base of the
examining table and support the examining arm and
elbow during the examination
o This support of the elbow allows greater
sensitivity in the examining fingers
At the same time, a second dimension is added by
employing the other hand to pressure the abdomen
One hould rquire proficiency with the index and
middle fingers of one hand and then always use that
hand for the vaginal examination as the:
1. Vaginal hand (non-dominant hand)
2. The other as an abdominal hand (dominant
hand)
Palpation by Bimanual Examination
Basically allows the physician to palpate the uterus
and the adnexa
The lubricated index and middle fingers of the
dominant hand are placed within the vagina, and
the thumb is folded under
o So as not to cause the patient distress in the
area of the mons pubis, clitoris and pubic
symphysis
The fingers are inserted deeply into the vagina so
that they rest beneath the cervix in the posterior
fornix
The physician should be in a comfortable position,
generally with the leg on the side of the vaginal
examining hand on a table lift and the elbow of that
arm resting on the knee.
The opposite hand is in the patients abdomen
above the pubic symphysis
The first palpable is the cervix
Next is the anteriorly displaced uterus
The flat of the fingers are used for palpation
The uterus is then elevated by pressing up on the
cervix and delivers the uterus to the abdominal
hand so that the uterus may be placed placed
between the two hands
o Identify position, size , shape, consistency
and mobility
The shape of the uterus shuld be described in detail.
The consistency of the uterus is generally firm but
not rock-hard
Any underlying tenderness
o May imply an inflammatory process
Examination of the adnexa
If the right hand is the pelvic hand, the first two
fingers of the right hand are then moved into the
right vaginal fornix as deeply as they can be
inserted
Cervical and adnexal tenderness:
o Ectopic pregnancy
o PID/Salphigitis
o Endometriosis
A normal ovary is approximately 3 cm b 2 cm (about
the size of a walnut) and will sweep between the
two fingers with ease unless it is fixed in an
abnormal position by adhesions.
When the adnexa is palpated, its size, mobility and
consistency must be determined
Adnexa are usually not palpable in postmenopausal
women
If palpable adnexa in menopause may need further
investigation for ovarian pathology, if enlarged
Rectovaginal Examination (read book its beyond my
powers)
Confirm bimanual examination
Hemorrh
Should be employed in all patients
After
o Uterosacral ligament
Any thickening or beadiness
(endometriosis/inflammation)
If the uterus is retroverted
Summary (inspection and palpation only)
Vagina
o Leukorrhea
o Color
Cervix
o
o
o
Uterus
o
o
o
Adnexa
o
o
o
You might also like
- Hirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Gastric Outlet Obstruction, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandGastric Outlet Obstruction, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Ectopic PregnancyDocument5 pagesEctopic PregnancyFaith FuentevillaNo ratings yet
- Nursing Care of Family During Labor and BirthhhDocument6 pagesNursing Care of Family During Labor and BirthhhAudreySalvadorNo ratings yet
- Normal Conduct of LaborDocument62 pagesNormal Conduct of LaborFaye Cabotaje LinganNo ratings yet
- Obstetics Simplified El-MowafiDocument515 pagesObstetics Simplified El-Mowafiapi-370504650% (2)
- Taking Obstetrical HistoryDocument20 pagesTaking Obstetrical Historymawada abdallaNo ratings yet
- Abdominal Mass Differential PresentationDocument42 pagesAbdominal Mass Differential Presentationdeb haartNo ratings yet
- HERNIA - Case StudyDocument8 pagesHERNIA - Case StudyMa Jaimeliz Mae MuñizNo ratings yet
- History & Physical Exam in Ob/Gyn: By: - DR AmanuDocument75 pagesHistory & Physical Exam in Ob/Gyn: By: - DR AmanuKåbåñå TürüñåNo ratings yet
- Hydramnios and Premature Rupture of MembranesDocument5 pagesHydramnios and Premature Rupture of Membranessarguss14No ratings yet
- Ogexamination 110401040414 Phpapp02 PDFDocument26 pagesOgexamination 110401040414 Phpapp02 PDFDika RizkiardiNo ratings yet
- Key Points of Obstetrics and Gynaecological HistoryDocument44 pagesKey Points of Obstetrics and Gynaecological HistoryRoisah Yunan NegariNo ratings yet
- Cerebral PalsyDocument14 pagesCerebral PalsyWaode SittrisnawatiNo ratings yet
- O and G Notes Notebank NumberedDocument173 pagesO and G Notes Notebank NumberedPerscitus Ali القحطانيNo ratings yet
- HHHHDocument36 pagesHHHHdger11No ratings yet
- Gyne History Taking PDFDocument6 pagesGyne History Taking PDFGokul AdarshNo ratings yet
- OSCE OB - PDF Version 1Document15 pagesOSCE OB - PDF Version 1FNaF is love FNaF is lifeNo ratings yet
- History Examination of Gynecology and Obstetrics PatientsDocument3 pagesHistory Examination of Gynecology and Obstetrics PatientsAgus WijayaNo ratings yet
- Gyni History TalkingDocument61 pagesGyni History TalkingEthiopia TekdemNo ratings yet
- Benign Gynecologic Lesions FinalDocument11 pagesBenign Gynecologic Lesions Final2012100% (4)
- EUOGS OSCE Booklet 2020Document26 pagesEUOGS OSCE Booklet 2020Amanda Leow100% (1)
- OBGYN Objective - Module Study GuideDocument79 pagesOBGYN Objective - Module Study GuideHema LaughsalotNo ratings yet
- Cervical Insufficiency:: Miscarriage Early (Premature)Document2 pagesCervical Insufficiency:: Miscarriage Early (Premature)Ardelean EmanuelNo ratings yet
- Ob SGDDocument88 pagesOb SGDFerdinand Luis SuarezNo ratings yet
- Abdominal Examination Print PDFDocument8 pagesAbdominal Examination Print PDFPooja HbNo ratings yet
- OB History Endorsement FormatDocument6 pagesOB History Endorsement FormatVin CustodioNo ratings yet
- Antenatal Care: Physiological Changes in PregnancyDocument2 pagesAntenatal Care: Physiological Changes in PregnancyAlexander Ennes100% (1)
- Joint Pain - ApproachDocument32 pagesJoint Pain - ApproachHassan Bin AjmalNo ratings yet
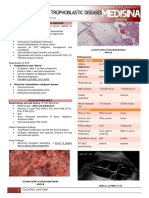
- 02 Gestational Trophoblastic DiseaseDocument8 pages02 Gestational Trophoblastic Diseasemisakichan FrandoNo ratings yet
- 7 Leopold ManeuverDocument2 pages7 Leopold ManeuverGrazyna ChojnNo ratings yet
- Abnormal OBDocument34 pagesAbnormal OBLawrence NemirNo ratings yet
- Drug Therapy For GI Disorders PDFDocument5 pagesDrug Therapy For GI Disorders PDFmeeraNo ratings yet
- Recurrent Pregnancy LossDocument61 pagesRecurrent Pregnancy LossHerman FiraNo ratings yet
- OB GYN CasePre FinalDocument82 pagesOB GYN CasePre FinalMarjorie Lahaylahay AlabataNo ratings yet
- Hypertensive Disorder in PregnancyDocument56 pagesHypertensive Disorder in PregnancyESCA GabrielNo ratings yet
- Abdul Hakeem Hady.: Done byDocument29 pagesAbdul Hakeem Hady.: Done byعمر احمد شاكرNo ratings yet
- Case 1 History & PEDocument3 pagesCase 1 History & PEcbac1990No ratings yet
- Hiv in Pregnancy FinalDocument73 pagesHiv in Pregnancy Finalapi-3797079No ratings yet
- Concept Map CholesectomyDocument3 pagesConcept Map CholesectomyDoreen Claire100% (1)
- OBS and GYN - HX TakingDocument3 pagesOBS and GYN - HX Takingboro1522No ratings yet
- BY: Shazlin Bt. Sabaah Salwa Hanim Bt. Mohd. Saifuddin Kamarulzaman B. MuzainiDocument61 pagesBY: Shazlin Bt. Sabaah Salwa Hanim Bt. Mohd. Saifuddin Kamarulzaman B. MuzainiJohn Christopher LucesNo ratings yet
- ICM 01 History Taking (AOlajubelo-140611)Document39 pagesICM 01 History Taking (AOlajubelo-140611)AkbarNo ratings yet
- Biliary DisoderDocument50 pagesBiliary DisoderZanida ZainonNo ratings yet
- Clerkship Obgyn OsceDocument6 pagesClerkship Obgyn OsceErika Leah Manalo100% (1)
- How To Read A CTGDocument11 pagesHow To Read A CTGiwennieNo ratings yet
- Vasculitis MindnodeDocument1 pageVasculitis MindnodeToño VargasNo ratings yet
- Neck Examination PDFDocument2 pagesNeck Examination PDFNizam Mischievous'Lovely Schremo BoyysNo ratings yet
- Obstetrics History Taking in and Examination PowerpointDocument15 pagesObstetrics History Taking in and Examination Powerpointياسر كوثر هانيNo ratings yet
- OSCE Gynae-OSCE-MMSSDocument24 pagesOSCE Gynae-OSCE-MMSSMohammad Saifullah100% (1)
- The Abnormal PuerperiumDocument25 pagesThe Abnormal PuerperiumMartijn JohanNo ratings yet
- Ob-Gyn Review Part 3Document101 pagesOb-Gyn Review Part 3filchibuffNo ratings yet
- Maternal and Fetal Assessment During LaborDocument66 pagesMaternal and Fetal Assessment During LaborHazelynne Mamucud100% (2)
- 1 GYNE 7 - EndometriosisDocument6 pages1 GYNE 7 - EndometriosisIrene FranzNo ratings yet
- Breech - Management Of: 1. PurposeDocument15 pagesBreech - Management Of: 1. PurposeMuathNo ratings yet
- Case History Ob & Gyne 4Document6 pagesCase History Ob & Gyne 4maksventileNo ratings yet
- Kernicterus, (Bilirubin Encephalopathy) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandKernicterus, (Bilirubin Encephalopathy) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Problem-based Approach to Gastroenterology and HepatologyFrom EverandProblem-based Approach to Gastroenterology and HepatologyJohn N. PlevrisNo ratings yet
- Hydrocele, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHydrocele, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- A Simple Guide to Acalculous Cholecystopathy, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Acalculous Cholecystopathy, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Maternal AnatomyDocument68 pagesMaternal Anatomylovelots1234No ratings yet
- Polycystic Ovarian Syndrome: Iggy Candice Songco Resident Physician Trainee IIDocument78 pagesPolycystic Ovarian Syndrome: Iggy Candice Songco Resident Physician Trainee IIlovelots1234No ratings yet
- Maternal Anatomy ReportDocument52 pagesMaternal Anatomy Reportlovelots1234No ratings yet
- Prenatal Care, Maternal Nutrition, IDADocument91 pagesPrenatal Care, Maternal Nutrition, IDAlovelots1234No ratings yet
- LaborDocument115 pagesLaborlovelots1234No ratings yet
- CPG-3rd Trimester Bleeding and Postpartum Hemorrage 2009Document107 pagesCPG-3rd Trimester Bleeding and Postpartum Hemorrage 2009lovelots1234100% (8)
- CPG-Abnormal Labor and Delivery 2009Document29 pagesCPG-Abnormal Labor and Delivery 2009lovelots123488% (8)
- 2.4 (Biochemistry) Tca HMP and Uronic Acid PathwayDocument15 pages2.4 (Biochemistry) Tca HMP and Uronic Acid Pathwaylovelots1234100% (1)
- Upper Extremities Nerve SupplyDocument19 pagesUpper Extremities Nerve Supplylovelots1234No ratings yet
- Ebcpg Antibiotic ProphylaxisDocument31 pagesEbcpg Antibiotic Prophylaxispot_domingoNo ratings yet
- Biochemistry 1.4 Enzymes Classification and KineticsDocument11 pagesBiochemistry 1.4 Enzymes Classification and Kineticslovelots1234100% (1)
- POGS CPG Abnormal Uterine BleedineDocument36 pagesPOGS CPG Abnormal Uterine Bleedinejandale57% (7)
- CPG For Antibiotic Prophylaxis in Surgical ProceduresDocument27 pagesCPG For Antibiotic Prophylaxis in Surgical Procedureslovelots1234No ratings yet
- 2.7 (BIOCHEMISTRY) Gluconeogenesis - Better PicturesDocument12 pages2.7 (BIOCHEMISTRY) Gluconeogenesis - Better Pictureslovelots1234No ratings yet
- Upper Extremities Blood SupplyDocument35 pagesUpper Extremities Blood Supplylovelots1234No ratings yet
- Biochemistry 1.3 NeurotransmittersDocument10 pagesBiochemistry 1.3 Neurotransmitterslovelots1234No ratings yet
- 2.2 (BIOCHEMISTRY) Carbohydrate Chemistry and MetabolismDocument8 pages2.2 (BIOCHEMISTRY) Carbohydrate Chemistry and Metabolismlovelots1234No ratings yet
- 2.5 (BIOCHEMISTRY) Electron Transport Chain and Oxidative PhosphorylationDocument7 pages2.5 (BIOCHEMISTRY) Electron Transport Chain and Oxidative Phosphorylationlovelots1234100% (2)
- Biochem 2.1 Introduction To MetabolismDocument5 pagesBiochem 2.1 Introduction To Metabolismlovelots1234No ratings yet
- 2.6 (BIOCHEMISTRY) Glycogen MetabolismDocument10 pages2.6 (BIOCHEMISTRY) Glycogen Metabolismlovelots1234No ratings yet
- Biochem 1.5 Bioenergetics PDFDocument7 pagesBiochem 1.5 Bioenergetics PDFlovelots1234No ratings yet
- 2.1 (BIOCHEMISTRY) Introduction To MetabolismDocument6 pages2.1 (BIOCHEMISTRY) Introduction To Metabolismlovelots1234100% (1)
- Legal Medicine Review Questions WITH KEY ANSWERDocument6 pagesLegal Medicine Review Questions WITH KEY ANSWERlovelots123493% (28)
- Anatomy 1.4 Upper Limbs - Muscle and FasciaDocument10 pagesAnatomy 1.4 Upper Limbs - Muscle and Fascialovelots1234No ratings yet
- Biochemistry 1.1 Introduction To Water and BuffersDocument7 pagesBiochemistry 1.1 Introduction To Water and Bufferslovelots1234No ratings yet
- Anatomy 1.1 Anatomy in MotionDocument5 pagesAnatomy 1.1 Anatomy in Motionlovelots1234100% (2)
- Legal MedDocument102 pagesLegal Medlovelots1234No ratings yet
- Anatomy 1.1 - Anatomicomedical TerminologyDocument2 pagesAnatomy 1.1 - Anatomicomedical Terminologylovelots1234No ratings yet
- Anatomy 1.2 Anatomy in MotionDocument4 pagesAnatomy 1.2 Anatomy in Motionlovelots1234No ratings yet
- 1991 Hanaor - DOUBLE-LAYER TENSEGRITY GRIDS - STATIC LOADDocument15 pages1991 Hanaor - DOUBLE-LAYER TENSEGRITY GRIDS - STATIC LOADDaniel MartinsNo ratings yet
- Stability TestDocument28 pagesStability TestjobertNo ratings yet
- The Journeyto Learning Throughthe Learning StylesDocument93 pagesThe Journeyto Learning Throughthe Learning Stylesastria alosNo ratings yet
- Dell Inspiron 5547 15Document7 pagesDell Inspiron 5547 15Kiti HowaitoNo ratings yet
- FacebookDocument2 pagesFacebookAbhijeet SingareNo ratings yet
- 5024Document2 pages5024Luis JesusNo ratings yet
- Calculating Staff Strength:: Find Latest Hospitality Resources atDocument8 pagesCalculating Staff Strength:: Find Latest Hospitality Resources atPriyanjali SainiNo ratings yet
- Equipment Maintenance and Measuring Equipment ProcedureDocument2 pagesEquipment Maintenance and Measuring Equipment ProcedureRaja Mani100% (1)
- Service Marketing - Term End Examination 2021 School of Business Management Narsee Monjee Institute of Management Studies, HyderabadDocument2 pagesService Marketing - Term End Examination 2021 School of Business Management Narsee Monjee Institute of Management Studies, Hyderabadnatasha bennyNo ratings yet
- 2 MercaptoEthanolDocument8 pages2 MercaptoEthanolMuhamad ZakyNo ratings yet
- A B&C - List of Residents - VKRWA 12Document10 pagesA B&C - List of Residents - VKRWA 12blr.visheshNo ratings yet
- Ashfaque Ahmed-The SAP Materials Management Handbook-Auerbach Publications, CRC Press (2014)Document36 pagesAshfaque Ahmed-The SAP Materials Management Handbook-Auerbach Publications, CRC Press (2014)surajnayak77No ratings yet
- Refrigerant Unit Lab ReportDocument19 pagesRefrigerant Unit Lab Reportakmal100% (2)
- Bluesil Ep 150 A3: Insulator Grade Silicone RubberDocument2 pagesBluesil Ep 150 A3: Insulator Grade Silicone RubberNagendra KumarNo ratings yet
- MINDSET 1 EXERCISES TEST 1 Pendientes 1º Bach VOCABULARY AND GRAMMARDocument7 pagesMINDSET 1 EXERCISES TEST 1 Pendientes 1º Bach VOCABULARY AND GRAMMARanaNo ratings yet
- To Tell The TruthDocument5 pagesTo Tell The TruthNabeel Ahmed KhanNo ratings yet
- Homeopatia Vibracional RatesDocument45 pagesHomeopatia Vibracional RatesAugusto Bd100% (4)
- PICUDocument107 pagesPICUsarikaNo ratings yet
- Lesson Plan - Sight Word ObservationDocument2 pagesLesson Plan - Sight Word Observationapi-253277023No ratings yet
- Test Iii Cultural Social and Political OrganizationDocument2 pagesTest Iii Cultural Social and Political OrganizationTin NatayNo ratings yet
- 2 TolentinoDocument12 pages2 TolentinoMA. ANGELINE GRANADANo ratings yet
- Design of A Low Cost Hydrostatic Bearing: Anthony Raymond WongDocument77 pagesDesign of A Low Cost Hydrostatic Bearing: Anthony Raymond WongRogelio DiazNo ratings yet
- Two Occult Philosophers in The Elizabethan Age: by Peter ForshawDocument10 pagesTwo Occult Philosophers in The Elizabethan Age: by Peter ForshawFrancesco VinciguerraNo ratings yet
- Chemistry Previos Papaer 313Document19 pagesChemistry Previos Papaer 313Ashu GuptaNo ratings yet
- თინათინ ზურაბიშვილი, თვისებრივი მეთოდებიDocument111 pagesთინათინ ზურაბიშვილი, თვისებრივი მეთოდებიNino LomaiaNo ratings yet
- Happiest Refugee Coursework 2013Document10 pagesHappiest Refugee Coursework 2013malcrowe100% (2)
- Masters Thesis Benyam 2011Document156 pagesMasters Thesis Benyam 2011TechBoy65No ratings yet
- This Study Resource Was: MCV4U Exam ReviewDocument9 pagesThis Study Resource Was: MCV4U Exam ReviewNathan WaltonNo ratings yet
- BOMA - Office Building Standard Methods of Measurement AppendixDocument41 pagesBOMA - Office Building Standard Methods of Measurement Appendixxavest100% (7)
- Adolescents and Career DevelopmentDocument10 pagesAdolescents and Career DevelopmentMasrijah MasirNo ratings yet