Professional Documents
Culture Documents
Oral Case Presentation Benchmarks - : Identifying Information & Chief Concern
Uploaded by
Manisanthosh KumarOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Oral Case Presentation Benchmarks - : Identifying Information & Chief Concern
Uploaded by
Manisanthosh KumarCopyright:
Available Formats
Oral Case Presentation Benchmarks
_____ _
On completion of Foundations of Clinical Medicine, students should be able to perform an accurate, complete and
well organized comprehensive oral case presentation for a new clinic or hospital patient, and adapt the case
presentation to the clinical setting. A comprehensive OCP includes these sections:
Name & age
Identifying information &
chief concern
Known medical problems highly relevant to the chief concern (< 4)
Chief concern and duration of symptoms
Background: Health at the time of symptom onset and details of any chronic
illness directly related to the chief concern.
History of present illness
Details of the presenting problem: Beginning at symptom onset and
proceeding sequentially.
Predisposing conditions & risk factors
Pertinent negatives
Optional: Hospital course or evaluation to date
Past medical history
All active medical problems and any other problems relevant to evaluation or
ongoing management.
Summarize for each major, active problem: diagnosis, current treatment,
control, and complications
Medications & allergies
Prescribed medications and doses
Non-prescription medications and complementary therapies
Drug allergies and the type of reaction
Habits and risk factors
Substance use not already covered in HPI
Social history
Summary of social influences on your patients health and health care: living
situation, social support, occupation and avocation, any financial or other
concerns
Physical exam
General appearance and vital signs
Name each organ system in order and report all pertinent exam findings, both
normal and abnormal:
Comprehensive exam of system(s) relevant to chief concern
Other findings (normal or abnormal) that will help your listener
answer a clinical question
Report all abnormal findings
Summary statement
Restate the ID, and summarize the key features from the history and exam
Assessment
Format determined by clinical context
Plan
Format determined by clinical context
PURPOSE AND FORMAT OF EACH SECTION
The purpose of the oral case presentation is:
To concisely communicate the findings of your history and exam to other members of your team
To formulate and address the clinical questions important to your patient's care
Identifying Information and Chief Concern (ID/CC)
Purpose:
Sets the stage and gives a brief synopsis of the patients major problem.
Format:
-Identify the patient by name and age
-Include no more than four medical problems (sometimes there are zero) that are highly relevant
to the chief concern. List only the diagnoses here, and elaborate on them in the HPI or PMH.
-Report the chief concern and duration of symptoms
Template:
Mr. _____ is a ____ year-old man with a history of _______ who presents with
_______ of ______ duration.
Example:
Mr. T is a 32 year old man with Crohn's disease who presents with bloody diarrhea of 3
days duration.
History of Present Illness (HPI)
Purpose:
Provides a complete account of the presenting problem, including information from the
past medical history, family history and social history related to that problem.
Format:
The HPI should occupy 1/3 to 1/2 of your total presentation time. The content of the HPI
in the oral case presentation is the same as the HPI in the write up.
Template:
A 5-paragraph format is one common structure for the HPI. Use this structure for your case
presentations for patients seen in college tutorials. Your preceptors may ask you to adapt this
structure in different clinical contexts.
Paragraph 1: Background
Characterize the patients health at the time current symptoms began. If the presenting concern is related to a
chronic illness, give a brief summary of the illness, including when it was diagnosed, treatment, complications,
and how well it is controlled.
Example: Mr. T was in his usual state of good health, with well controlled Crohn's disease, until three days prior
to admission. He was first diagnosed with Crohn's in 2011, when he presented with diarrhea, abdominal pain,
and weight loss. He was treated with steroids and then infliximab, and his symptoms have been well controlled,
with one to two bowel movements per day. He had had no recent flares or hospitalizations before this week."
Paragraph 2: Details of the presenting problem
This is an organized and edited version of the patient's narrative, beginning at the onset of symptoms, and
proceeding sequentially to the time of presentation. This section should describe the presenting concern
completely:
Quality
Time, duration, & frequency
Aggravating or alleviating factors
Associated symptoms
Attribution
Any prior episodes
If the presenting concern is pain, also describe:
Position (or location)
Radiation
Severity
Paragraph 3: Predisposing conditions and risk factors (aka. pertinent positives)
Information from the rest of the history (PMH, medications, habits and risk factors, family history, ROS) that is
directly related to the presenting problem. For example, a family history of cirrhosis is pertinent and should
be included in the HPI of a patient who presents with jaundice. The same family history of cirrhosis would NOT
be pertinent to a patient with dysuria, so would NOT be included in the HPI.
Paragraph 4: Pertinent negatives
Pertinent negatives are symptoms, conditions and risk factors that your patient does NOT have that directly
affect your assessment of the patients problem. For example, No family history of liver disease is a pertinent
negative in a patient presenting with jaundice.
To start with, report the absence symptoms from the major organ system involved and the absence of
constitutional symptoms in the pertinent negative section.
Paragraph 5: Evaluation of this problem to date
(Optional)
3. Past Medical History (PMH)
Purpose:
To provide a succinct overview of other important medical and surgical history that will
aid in the care of the patient.
Format:
Report active medical problems and other medical history that is pertinent to evaluation
or ongoing management. Medical or surgical history that is relevant to the chief concern
should be included in the HPI. If a past diagnosis or surgery is not active or relevant, it is
included in the write-up but NOT in the OCP.
Include a brief synopsis of each active major problem:
Diagnosis
Current treatment
Control
Complications
4. Medications and Allergies
- List all prescribed medications (by generic name if possible) and doses
- List all non-prescription medications and complementary/alternative therapies
- Report any drug allergies and the type of reaction
5. Habits and Risk Factors
- Summarize substance use not already mentioned in HPI, including tobacco, alcohol, drug use
- Risk factors relevant to the presenting concern should be included in the HPI
6. Social History
Purpose:
To provide your listener with the social context of the illness and its impact on ongoing
care
Format:
In 2-3 sentences summarize the patients living situation and support systems, occupation,
and any social issues that could impact care.
7. Physical Examination
Purpose:
Succinctly and accurately describe the patients physical examination, emphasizing
pertinent findings
Format:
Begin with general appearance and vital signs.
Name each organ system in order, and report the relevant exam:
HEENT and neck,
Chest
Cardiac
Abdomen
Neurologic
Musculoskeletal
Skin
Report all pertinent physical examination findings, both normal and abnormal:
Complete exam of the organ system(s) relevant to the chief concern
Other findings (normal or abnormal) that help your listener answer a clinical question.
Use concise but complete descriptions of positive findings.
Report all abnormal findings regardless of organ system.
If the examination of a system NOT relevant to the chief concern was normal, you may say
Normal.
8. Summary Statement: The first sentences of your assessment
Purpose:
To synthesize the important history and exam findings, to frame the clinical problem and
to lead your listener into your assessment. This is NOT simply a restatement of the ID chief
concern.
Format:
Restate the identifying data and summarize the key features from the patient's history and
physical exam.
Template:
In, summary,
year old man who presents with a history of PRESENTING
CONCERN (REFINED WITH SEMANTIC QUALIFIERS) AND MAJOR ASSOCIATED SYMPTOMS. His history
is notable for ELEMENTS OF THE HPI, PREDISPOSING CONDITIONS AND RISK FACTORS THAT IMPACT
YOUR ASSESSMENT. Physical exam is notable for KEY FINDINGS, NORMAL AND ABNORMAL, THAT
NAME
is a
AGE
IMPACT YOUR ASSESSMENT.
9. Assessment
Purpose:
Address the clinical problem(s) important in this encounter, and demonstrate your clinical
reasoning. The clinical problem may range from a new and undiagnosed problem to
routine follow-up of a chronic problem.
Format:
Format may vary based on type of problem. For example:
1. An undiagnosed problem. Your assessment would address the top 3-4 items on the
differential diagnosis suggested by your patients history and exam findings.
Example: The most likely reason for Lilys rash is eczema. Her skin dryness and pruritis,
and her family history of atopy are all consistent with eczema, as is the history of
worsening in the winter and after frequent swimming. She also has a classic
distribution on the hands and elbow creases. A less likely possibility is scabies, which
frequently affects the hands. However, Lilys skin between the wrists and elbows is
spared, which would be atypical for scabies.
2. An exacerbation of a chronic problem. Your assessment would address the most likely
reasons for the exacerbation, as suggested by your patients history and exam findings.
Example: The most likely reason for Mr. Cs CHF exacerbation is medication nonadherence due to both costs and confusion. He reports filling his medications less often
than monthly because even the co-pay is expensive, which is confirmed by his
pharmacy. Although he manages his own medications, he is unable to accurately
describe what each is for, or his dosing schedule. A second possibility is new ischemia;
however, hes had no chest pain or tightness, and initial ECG and enzymes were
negative. Finally, a URI could have precipitated this exacerbation, as he had low grade
fever, cough, and rhinorrhea last week. However, those symptoms have resolved as his
edema and shortness of breath have progressed, making this possibility less likely.
3. Routine follow-up of a chronic problem. Your assessment would address current control of
the problem, evidence of complications, and adequacy of current education and treatment.
Example: Ms. Bs type 2 diabetes is well controlled, with most recent HgbA1c of 6.8.
She reports excellent adherence to diet and exercise, as well as metformin. She has no
evidence of retinopathy or neuropathy on exam and urine for microalbumin was
negative.
10. Plan
Purpose:
To outline your next steps in addressing your patients clinical problem(s).
Format:
The plan is usually presented as a bulleted list, and may include interventions in these
categories:
Lab tests
Diagnostic
evaluation
Imaging
Consultation with specialists
Behavior change
Therapy
Medications
Counseling
Referral to another provider (e.g. physical therapy)
Monitoring
and follow-up
Repeat laboratory tests to monitor response to
treatment
Routine screening tests
Primary care clinic follow-up
Education about diagnoses done by you
Education
Referral to other providers for additional teaching, e.g.
diabetes educator, pharmacist
Adapting The Comprehensive OCP To Other Contexts
Example #1: An outpatient presenting for routine follow-up of a known problem
S: Subjective
ID/CC: Include scheduled follow up for and list problem(s) as well as any additional
issues identified during agenda setting.
HPI: Start with a brief synopsis of the problem that the patient is being seen for:
Diagnosis
Current treatment
Control
Complications
When the patient was last seen in clinic
Status of the known problem since the last visit:
Symptoms/control
Intervening problems
Pertinent positive/negative symptoms
PMH: Brief synopsis of other ongoing medical problems
Medications and allergies
Any changes in PMH/FH/SH since the last visit
O: Objective
A: Assessment:
Physical Exam
Vital signs
General appearance
Exam of the pertinent systems ONLY
Start with your summary statement
Address current control of the problem(s), evidence of complications, and
adequacy of current education and treatment.
P: Plan
Example #2: An outpatient presenting with an exacerbation of a chronic problem
S: Subjective
ID/CC: Same as comprehensive OCP
HPI: Same as comprehensive OCP
PMH: Brief synopsis of other ongoing medical problems
Medications and allergies
Any changes in PMH/FH/SH since the last visit
O: Objective
A: Assessment
Physical Exam
Vital signs
General appearance
Exam of the pertinent systems ONLY
Start with your summary statement
Address possible causes of the exacerbation
P: Plan
Example #3: A patient presenting to her primary care clinic with a new problem
S: Subjective
ID/CC
History of present illness as in comprehensive OCP. Include predisposing
conditions and risk factors, pertinent negatives, and evaluation and treatment
to date.
PMH: Brief synopsis of other ongoing medical problems
Medications and allergies
Any changes in PMH/FH/SH since the last visit
O: Objective
A: Assessment
Physical Exam
General Description
Vital signs
Exam of organ systems relevant to the presenting problem
Start with your summary statement
Address differential diagnosis of the new problem
P: Plan
Delivery Tips for Oral Case Presentations:
At the bedside, introduce your patient and any family members to your team.
Maintain good posture.
Establish eye contact with your team and your patient, glancing at your notes only as necessary.
Present with a clear, energetic, and interested voice.
When presenting at the bedside, recognize the impact of your choice of words on your patient:
o
Avoid medical language that might frighten your patient, unless he has used it. Examples: Endstage liver disease and Another possibility is lung cancer
Avoid language your patient might find insulting. Examples: Morbidly obese and Pleasantly
confused elderly woman.
Follow the standard format of the OCP precisely.
Orient your listeners to the next section of the OCP with a brief pause followed by the title of that
section.
Use precise language.
Do not rationalize, editorialize, or justify as you present. Just present the facts.
Be aware of your patients confidentiality, especially if the patient is in a shared room.
You might also like
- ECG Interpretation DR - Rawan AlshreemDocument25 pagesECG Interpretation DR - Rawan AlshreemMarymii Al-sahlawiiNo ratings yet
- High Yield NotesDocument211 pagesHigh Yield Notesroad2successNo ratings yet
- Presenting The PatientDocument3 pagesPresenting The PatientAli ZeinNo ratings yet
- Md2017 Carms Mock Interview GuideDocument6 pagesMd2017 Carms Mock Interview GuideLizamna ReynosoNo ratings yet
- Brain Sheet2011Document1 pageBrain Sheet2011nursekatieNo ratings yet
- Trusted Evidence For Confident Clinical Decisions: Resources For Medication, Disease, and ToxicologyDocument10 pagesTrusted Evidence For Confident Clinical Decisions: Resources For Medication, Disease, and ToxicologyCurcubeuAuroraNo ratings yet
- SOAP Presentation 5.19.16 PDFDocument1 pageSOAP Presentation 5.19.16 PDFnems92No ratings yet
- Care Plan Handbook TemplateDocument34 pagesCare Plan Handbook TemplateBreanna Hopkins100% (1)
- Herbal GuideDocument42 pagesHerbal GuideladygreenNo ratings yet
- Cardiology ConsultsDocument2 pagesCardiology ConsultsjuweriyNo ratings yet
- Amazing Esqs With Answers Pediatrics-ShelfDocument31 pagesAmazing Esqs With Answers Pediatrics-ShelfDrSajid BuzdarNo ratings yet
- Bilateral Peritonsillar Abscess: A Case ReportDocument2 pagesBilateral Peritonsillar Abscess: A Case ReportshashaNo ratings yet
- Weekly Clinical Prep Packet 12 REVISEDDocument12 pagesWeekly Clinical Prep Packet 12 REVISEDMei SarteNo ratings yet
- Orientation To General SurgeryDocument0 pagesOrientation To General SurgeryIrham TahkikNo ratings yet
- 01 Interview FormDocument7 pages01 Interview FormSavage SkylenNo ratings yet
- Mo Intern Handbook - FinalDocument37 pagesMo Intern Handbook - FinalGideon K. MutaiNo ratings yet
- History and ExamDocument27 pagesHistory and ExamEmereole FrancesNo ratings yet
- Diagnosis and Management of Acute Abdominal PainDocument43 pagesDiagnosis and Management of Acute Abdominal PainTe HineahuoneNo ratings yet
- Diagnosis and Management of Acute Abdominal PainDocument43 pagesDiagnosis and Management of Acute Abdominal PainTe HineahuoneNo ratings yet
- ResumeDocument3 pagesResumeAstig Kuging63% (8)
- Presence Saint Francis Hospital ProgramDocument12 pagesPresence Saint Francis Hospital ProgramRamanpreet Kaur MaanNo ratings yet
- Magic Stage Hypnotism Training Class HandoutsDocument46 pagesMagic Stage Hypnotism Training Class HandoutsArun Sharma100% (1)
- OSCE Final 1 PDFDocument204 pagesOSCE Final 1 PDFamalNo ratings yet
- Smhs - Gwu.edu Sample NotesDocument3 pagesSmhs - Gwu.edu Sample NotesWaqas HaleemNo ratings yet
- Problem-based Approach to Gastroenterology and HepatologyFrom EverandProblem-based Approach to Gastroenterology and HepatologyJohn N. PlevrisNo ratings yet
- 22 Disritmia 2018Document60 pages22 Disritmia 2018Nur akilaNo ratings yet
- The AOA Guide: How To Succeed Inthe3 Year Clerkships: Example Notes For The MsiiiDocument20 pagesThe AOA Guide: How To Succeed Inthe3 Year Clerkships: Example Notes For The Msiiinybiker100% (1)
- The Yale Way - New Patient PresentationsDocument9 pagesThe Yale Way - New Patient PresentationsAndrew McGowanNo ratings yet
- UroflowDocument41 pagesUroflowSri HariNo ratings yet
- HY Mixed USMLE Review Part I 1Document20 pagesHY Mixed USMLE Review Part I 1Jennifer Ross-ComptisNo ratings yet
- Computer Generated in Nursing Care PlansDocument4 pagesComputer Generated in Nursing Care PlansCake Man100% (1)
- Cardio History TakingDocument4 pagesCardio History Takingwaleed sonbol100% (2)
- Lecture - 1 Components of Sewage Collection SystemDocument19 pagesLecture - 1 Components of Sewage Collection SystemDanial Abid100% (1)
- Policies and ProceduresDocument24 pagesPolicies and ProceduresAbdulazizNo ratings yet
- How To Make An Oral Case Presentation To Healthcare ColleaguesDocument5 pagesHow To Make An Oral Case Presentation To Healthcare ColleaguesYuliana Citra AnggraeniNo ratings yet
- Soap Note Template 01Document1 pageSoap Note Template 01Matthew MarrNo ratings yet
- Annex"B": Subject: Application For Voluntary Confinement For Treatment and RehabilitationDocument3 pagesAnnex"B": Subject: Application For Voluntary Confinement For Treatment and RehabilitationShaila GonzalesNo ratings yet
- Practice Test Questions Downloaded From FILIPINO NURSES CENTRALDocument37 pagesPractice Test Questions Downloaded From FILIPINO NURSES CENTRALFilipino Nurses Central50% (8)
- The AOA Guide:: How To Succeed in The Third-Year ClerkshipsDocument25 pagesThe AOA Guide:: How To Succeed in The Third-Year Clerkshipshector100% (1)
- Wu Step 2 CK Study PlanDocument5 pagesWu Step 2 CK Study PlanLeti Sefa TaNo ratings yet
- MRCP2 Rapid Revision NotesDocument125 pagesMRCP2 Rapid Revision NotesManisanthosh Kumar100% (1)
- MRCP2 Rapid Revision NotesDocument125 pagesMRCP2 Rapid Revision NotesManisanthosh Kumar100% (1)
- Transgenerational and Structural Family TherapyDocument19 pagesTransgenerational and Structural Family Therapynorociel8132100% (3)
- DeVirglio NotesDocument77 pagesDeVirglio NotesAlvand SehatNo ratings yet
- Aquifer InternalMedicine11 - 45Document8 pagesAquifer InternalMedicine11 - 45JulieNo ratings yet
- Brunner Step 2 CK Study PlanDocument2 pagesBrunner Step 2 CK Study PlanhellayeahNo ratings yet
- History and Physical AssessmentDocument31 pagesHistory and Physical AssessmentShalini RavNo ratings yet
- Aquifer InternalMedicine09 - 55Document7 pagesAquifer InternalMedicine09 - 55JulieNo ratings yet
- Prevention of CancerDocument2 pagesPrevention of Cancercmmc_3No ratings yet
- Icm Course Syllabus PDFDocument8 pagesIcm Course Syllabus PDFZoya Morani100% (1)
- Radiology: Dr. Abdulaziz Alsaad Neuroradiology Fellow King Fahad Medical CityDocument22 pagesRadiology: Dr. Abdulaziz Alsaad Neuroradiology Fellow King Fahad Medical CityAjmal EnsanahNo ratings yet
- ANU Web Page-TexstDocument80 pagesANU Web Page-TexstČiča HemuliNo ratings yet
- Internal Medicine Topic List 2015Document3 pagesInternal Medicine Topic List 2015Krystal Mae LopezNo ratings yet
- Invitation To Participate in ECFMG's New Electronic Credentials Verification ProgramDocument2 pagesInvitation To Participate in ECFMG's New Electronic Credentials Verification ProgramCatya AñilabNo ratings yet
- Medical Student CV Free PDFDocument4 pagesMedical Student CV Free PDFAngelo SalvadorNo ratings yet
- BCM Som Student Resume Template 002Document3 pagesBCM Som Student Resume Template 002pro sanNo ratings yet
- (MED II) 1.05 Emergencies in Cancer PatientsDocument17 pages(MED II) 1.05 Emergencies in Cancer PatientsJearwin AngelesNo ratings yet
- Dr. Ali's Uworld Notes For Step 2 CKDocument40 pagesDr. Ali's Uworld Notes For Step 2 CKmarina shawkyNo ratings yet
- Deepak Step 2 CK UwDocument347 pagesDeepak Step 2 CK Uwusmleaddict proNo ratings yet
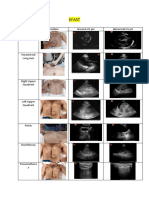
- Efast: Name Position Normal US Pic Abnormal US Pic SubcostalDocument4 pagesEfast: Name Position Normal US Pic Abnormal US Pic SubcostalMaryam FadahNo ratings yet
- Jane Elizabeth Doe: 639 Street ST - Town, CT 00000Document2 pagesJane Elizabeth Doe: 639 Street ST - Town, CT 00000Kasagga BrianNo ratings yet
- 250 ExperienceDocument5 pages250 ExperienceHuginn MuninnNo ratings yet
- Gynecology StudyguideDocument39 pagesGynecology StudyguideGameron777No ratings yet
- Turkey Book 03 Internal Medicine PDFDocument47 pagesTurkey Book 03 Internal Medicine PDFPreaisNo ratings yet
- Contoh FMEA UIHC Burn Unit Patient Education DocumentationDocument2 pagesContoh FMEA UIHC Burn Unit Patient Education DocumentationAnisaNo ratings yet
- Chief Complaint FormatDocument3 pagesChief Complaint Formatkazniels100% (1)
- Obstetrics Cases by Caroline de CostaDocument9 pagesObstetrics Cases by Caroline de CostaJeffrey HingNo ratings yet
- Medicine Review 2018 1Document470 pagesMedicine Review 2018 1Norjetalexis Maningo CabreraNo ratings yet
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Documents - MX Ataxia 558495943784eDocument75 pagesDocuments - MX Ataxia 558495943784eManisanthosh KumarNo ratings yet
- Food SafetyDocument71 pagesFood SafetyManisanthosh KumarNo ratings yet
- Documents - MX Risks Due To Chemicals in Food by Sharanya NagarajDocument20 pagesDocuments - MX Risks Due To Chemicals in Food by Sharanya NagarajManisanthosh KumarNo ratings yet
- Documents - MX Urbanisation and Its Effect On Peoples HealthDocument44 pagesDocuments - MX Urbanisation and Its Effect On Peoples HealthManisanthosh KumarNo ratings yet
- PORPHYRIA2Document43 pagesPORPHYRIA2Srm GeneticsNo ratings yet
- New Microsoft Word DocumentDocument2 pagesNew Microsoft Word DocumentManisanthosh KumarNo ratings yet
- Acute and Chronic Liver Disease - Orla CrosbieDocument46 pagesAcute and Chronic Liver Disease - Orla CrosbiewasimqureshiNo ratings yet
- Des MurgyDocument24 pagesDes MurgyManisanthosh KumarNo ratings yet
- Electromagnetic PollutionDocument29 pagesElectromagnetic PollutionManisanthosh KumarNo ratings yet
- How Ict Is Changing Education: How To Name ItDocument9 pagesHow Ict Is Changing Education: How To Name ItManisanthosh KumarNo ratings yet
- KidneyDocument94 pagesKidneyManisanthosh KumarNo ratings yet
- Rengan9095wcp 131126092723 Phpapp02Document22 pagesRengan9095wcp 131126092723 Phpapp02Manisanthosh KumarNo ratings yet
- BurnsDocument27 pagesBurnsManisanthosh KumarNo ratings yet
- Rengan9095wcp 131126092723 Phpapp02Document22 pagesRengan9095wcp 131126092723 Phpapp02Manisanthosh KumarNo ratings yet
- Genetic DisordersDocument10 pagesGenetic Disordersphantomspb100% (2)
- HTN CsseDocument3 pagesHTN CsseManisanthosh KumarNo ratings yet
- Amezcua Amezcua Whyyouneedpreventioneme 130916135419 Phpapp02Document18 pagesAmezcua Amezcua Whyyouneedpreventioneme 130916135419 Phpapp02Manisanthosh KumarNo ratings yet
- Dressing SelectionDocument34 pagesDressing SelectionManisanthosh KumarNo ratings yet
- Woundproducts 150408214021 Conversion Gate01Document35 pagesWoundproducts 150408214021 Conversion Gate01Manisanthosh KumarNo ratings yet
- Pediatric Nephrology Volume 25 Issue 9 2010 (Doi 10.1007/s00467-009-1327-2) Seza Ozen - The ВЂњother” Vasculitis Syndromes and Kidney InvolvementDocument7 pagesPediatric Nephrology Volume 25 Issue 9 2010 (Doi 10.1007/s00467-009-1327-2) Seza Ozen - The ВЂњother” Vasculitis Syndromes and Kidney InvolvementManisanthosh KumarNo ratings yet
- BurnsDocument27 pagesBurnsManisanthosh KumarNo ratings yet
- Dressing SelectionDocument34 pagesDressing SelectionManisanthosh KumarNo ratings yet
- Amezcua Amezcua Whyyouneedpreventioneme 130916135419 Phpapp02Document18 pagesAmezcua Amezcua Whyyouneedpreventioneme 130916135419 Phpapp02Manisanthosh KumarNo ratings yet
- Des MurgyDocument24 pagesDes MurgyManisanthosh KumarNo ratings yet
- Airway ObstructionDocument57 pagesAirway ObstructionManisanthosh KumarNo ratings yet
- 6 BehavCoursepackDocument343 pages6 BehavCoursepackManisanthosh KumarNo ratings yet
- Swan - PricelistDocument7 pagesSwan - PricelistsyringomyeliaNo ratings yet
- Tele HealthDocument2 pagesTele HealthBoom PastranaNo ratings yet
- Situation 2Document8 pagesSituation 2Rodessa Mandac TarolNo ratings yet
- Sample of An Expository EssayDocument2 pagesSample of An Expository Essayfatin nadiaNo ratings yet
- A Critical Review of Swarnaprashan As A BoonDocument24 pagesA Critical Review of Swarnaprashan As A BoonRashmi SharmaNo ratings yet
- Buset Na ResearchDocument5 pagesBuset Na Researchmk soberanoNo ratings yet
- Ice TherapyDocument5 pagesIce TherapyDiane CastillonNo ratings yet
- ResumeDocument4 pagesResumeapi-283952616No ratings yet
- Author's Overall Organizational PatternDocument6 pagesAuthor's Overall Organizational PatternTashieka GrahamNo ratings yet
- Termimesh TMA 725 MSDS January 2015Document5 pagesTermimesh TMA 725 MSDS January 2015sschkadeNo ratings yet
- Criterios de Elegibilidad de ACODocument88 pagesCriterios de Elegibilidad de ACOquimegiNo ratings yet
- NCPDocument1 pageNCPVictor MurilloNo ratings yet
- DR - Kavita Priya Iicm 1Document68 pagesDR - Kavita Priya Iicm 1Kavita PriyaNo ratings yet
- Sharma Et Al-2016-Journal of Applied MicrobiologyDocument11 pagesSharma Et Al-2016-Journal of Applied MicrobiologyJoanaNo ratings yet
- How To Control Hypertension (High Blood Pressure) - Nutrition StudiesDocument3 pagesHow To Control Hypertension (High Blood Pressure) - Nutrition StudiesMatevž BrojanNo ratings yet
- 5090 w12 QP 11Document20 pages5090 w12 QP 11mstudy123456No ratings yet
- MedsDocument2 pagesMedsRuel MaddawinNo ratings yet
- Tintin Cooking Beans and LegumesDocument3 pagesTintin Cooking Beans and LegumesBiZayangAmaZonaNo ratings yet
- Ehz 467Document65 pagesEhz 467Coy Calapatia-TorresNo ratings yet
- MushroomDocument36 pagesMushroomthamaraibala9788100% (1)
- ANAESTHESIA FOR GASTROINTESTINAL CANCER SURGERIES AutosavedDocument40 pagesANAESTHESIA FOR GASTROINTESTINAL CANCER SURGERIES AutosavedKavyasree KatamNo ratings yet