Professional Documents
Culture Documents
CT and MR Imaging of Chronic Subdural Haematomas: A Comparative Study
Uploaded by
YhafapCezOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CT and MR Imaging of Chronic Subdural Haematomas: A Comparative Study
Uploaded by
YhafapCezCopyright:
Available Formats
Original article
S W I S S M E D W K LY 2 010 ; 1 4 0 ( 2 3 2 4 ) : 3 3 5 3 4 0 w w w . s m w . c h
335
Peer reviewed article
CT and MR imaging of chronic subdural
haematomas: a comparative study
Senem Senturka, Aslan Guzel b, Aslan Bilicia, Ilker Takmazb, Ebru Guzel c, M. Ufuk Aluclu d , Adnan Cevizb
a
b
c
d
Department of Radiology, School of Medicine, University of Dicle, Diyarbakir, Turkey
Department of Neurosurgery, School of Medicine, University of Dicle, Diyarbakir, Turkey
Veni Vidi Hospital, Diyarbakir, Turkey
Department of Neurology, School of Medicine, University of Dicle, Diyarbakir, Turkey
Summary
Questions under study/principles: This study was
designed to compare CT and MR appearances of
chronic subdural haematomas as well as CT- and
MR-guided measurements of haematoma thicknesses.
Methods: CT and MR images of 48 chronic
subdural haematomas of 34 patients were reviewed retrospectively. The thickness measurements and imaging characteristics of haematomas
were compared.
Results: Levelling was observed in 25% of
haematomas, and most of them (60%) had intrahaematomal membranes. All membranes could be
delineated by MR imaging, whereas only 27%
were defined by CT. Mixed density (52%) and T1
hyperintensity (59%) were commonly observed in
membraned haematomas, but the difference was
not statistically significant. Haematomas were
measured significantly thicker on MR images. All
patients had been treated with burr-hole craniotomy and irrigation.
Conclusions: MR imaging is more sensitive
than CT in determining the size and internal
structures of chronic subdural haematomas.
Key words: chronic subdural haematoma; computed
tomography; magnetic resonance imaging; haematoma
thickness; intrahaematomal membrane
Introduction
No conict of
interest in relation
to this article.
Chronic subdural haematoma (CSDH), which
generally occurs in older patients, is one of the
most frequent clinical entities encountered in
neurosurgery departments. With early diagnosis
and adequate surgical treatment the prognosis is
favourable. Computed tomography (CT) remains
the most important imaging method in the initial
evaluation of CSDHs [1]. It is a faster, cheaper and
more available technique than magnetic resonance (MR) imaging. However, MR imaging provides more precise localisation and determination
of the extent of haematoma and its mass effect on
adjacent structures [2]. MR imaging is more advantageous in the case of isodense and bilateral
CSDHs [2, 3].
CT and MR imaging of CSDHs detect various patterns, which can be attributed to many factors including the age of the haematoma, the presence of rehaemorrhage and the haematocrit status
of the patient [46]. In this study 48 haematomas
in 34 patients were evaluated by determining CT
density and MR intensity characteristics and in-
ternal structures such as intrahaematomal membranes and layering. The thickness of each haematoma was measured on CT and MR images and
the measurements obtained by these two methods
were compared. We also attempted to determine
whether there was any difference in duration of
symptoms and hospital stay of patients with haematomas showing various MR characteristics.
Abbreviations
CSDH Chronic subdural haematoma
CT
Computed tomography
MR
Magnetic resonance
T1W
T1-weighted
T2W
T2-weighted
336
CT and MR imaging of chronic subdural haematomas
Materials and methods
From July 2002 to October 2007, 34 adult patients
who had both CT and MR evaluation of a symptomatic
CSDH were included in the study. CT and MR images
together with clinical data concerning aetiology, symptoms and signs, diagnosis and therapy of all 34 patients
(23 males and 11 females) were retrospectively obtained
from documents of the Department of Neurosurgery of
our institution. Ethics committee approval or informed
consent from patients was not required for this retrospective study.
Forty-eight haematomas of 34 patients, age range
1793 (mean 60.56 years), were included in the study:
20 patients had unilateral and 14 patients bilateral haematomas. Of the 34 patients 19 (56%) had a history of head
trauma, which in all cases, except for two motor vehicle
accidents, was minor. CT was performed at initial evaluation and MR imaging within 07 days with a mean of 1.88
days after CT scans. The capsule and chronic natures of
subdural haematomas were confirmed by surgery in all
patients.
Imaging was performed on high resolution spiral CT
systems and on 1 Tesla or 1.5 Tesla MR scanners. All MR
studies included a transverse and sagittal T1-weighted
(T1W) spin-echo sequence (400600/1520 [repetition
Figure 1
Difference of
haematoma thickness on CT and MR
imaging.
a, b. Haematoma
thickness measurement on consequent
CT scans.
c, d. Haematoma
thickness measurement on consequent
transverse T1W MR
images of the same
patient. Black line
represents the
thickness measurement performed from
the central part of the
crescent-shaped
haematoma vertical
to the convexity of
the parietal bone.
Note that haematoma
appears larger on MR
images.
time/echo time]) and a transverse or coronal T2-weighted
(T2W) spin-echo sequence (25004000/90105 [repetition time/echo time]) using 5 mm slice thickness and
1 mm gap. Slice thickness of CT images was 10 mm without gap. All transverse CT and MR images were obtained
parallel to the vertex with analogous angulations.
MR images were evaluated two weeks after CT
characteristics of haematomas were determined and all
CT-guided measurements were completed.
CSDHs were classified into 4 groups according to
their CT density characteristics: low, high and mixed
density, and isodense (where the density of the haematoma appears equal to that of the grey matter of the
brain). They were also classified into 3 groups according
to their MR intensity characteristics on TIW images: low,
high and mixed intensity. Levelling and membranes were
searched on CT and MR images. CT density (low, high
and mixed density, and isodensity) and MR intensity (low,
high and mixed intensity) characteristics of haematomas
with and without membranes were compared by Chisquare test.
Students t-test for independent samples was used to
compare time from onset of haematoma symptoms of various MR characteristics, either with intrahaematomal
membranes or not, hyperintense (including mixed intensity haematomas which were predominantly T1 hyperintense) or hypointense on T1W images. The mean hospital stay of patients with membraned and non-membraned
haematomas was also calculated.
Two radiologists checked consecutive transverse slice
positions of CT and MR images before performing measurements to make sure that slice positions were comparable. On CT and MR images the levels representing the
largest amount of haematoma were determined on axial
images, and the maximum thickness of each haematoma
was measured at these levels (fig. 1). Haematomas could
be definitely differentiated from subarachnoid space and
other possible collections on T1W images. Therefore,
maximum thickness of each haematoma was measured on
axial T1W MR images. Measurements were performed
from the central part of the crescent-shaped haematoma
vertical to the convexity of the calvarial bones. The thickness of each haematoma was measured manually by means
of scale bars on the CT and MR images. The measurements were obtained with the consensus of two radiologists. Students t-test for pair-wise comparison was used
to compare the measurements guided by CT and MR images. The values were expressed as the mean standard
deviation.
Results
All patients were treated by burr-hole craniotomy. The capsule and chronic natures of subdural haematomas were confirmed by surgery in all
48 haematomas. Membranes were observed in
29 haematomas of 21 patients. The aetiology was
identifiable in 19 patients (56%) who had a history
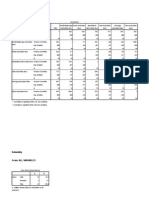
Table 1
Imaging method
Measurements
of haematoma
thicknesses.
N (number of
haematomas)
Mean haematoma
thickness (mm)
CT
48
17.1458
MR
48
21.0000
of head trauma. Except for two motor vehicle accidents, all the head traumas were minor. The
leading symptom was headache. Confusion, hemiparesis and seizures were other symptoms. Days
after trauma or onset of symptoms varied from 14
to 72 days with a mean of 33.3 days.
The mean haematoma thicknesses obtained
by CT and MR images are summarised in table 1.
The difference between measurements of haematoma thickness guided by MR imaging (mean
21.00 9.09) and CT scans (mean 17.15 8.62)
was statistically significant (t = 11.225; p <0.05).
S W I S S M E D W K LY 2 010 ; 1 4 0 ( 2 3 2 4 ) : 3 3 5 3 4 0 w w w . s m w . c h
Table 2
CT density
Number of haematomas
Distribution of
haematomas
according to CT
density characteristics.
Hypodense
18
Isodense
10
Mixed density
19
Hyperdense
Table 3
MR intensity
Number of haematomas
Distribution of
haematomas
according to MR
intensity characteristics.
Hypointense
10
Mixed Intensity
14
Hyperintense
24
There was a high correlation between CT and
MR measurements of haematoma thicknesses
(p <0.05).
Distribution of haematomas according to
their CT and MR imaging characteristics is shown
in tables 2 and 3. Eighteen haematomas (38%)
337
were hypodense and 10 (21%) were isodense on
CT scans. In addition, 19 (40%) haematomas were
mixed density and only 1 (2%) was hyperdense.
The CT appearances of hypodense, isodense and
hyperdense haematomas are shown in figure 2. All
mixed density haematomas were either isodense
or hypodense and contained hyperdense areas.
Only 10 (21%) of the 48 haematomas were
hypointense on T1W MR imaging. Half of CSDHs (n = 24) were hyperintense and 14 (29%)
were mixed intensity (fig. 3). All mixed intensity
haematomas were predominantly hyperintense. In
all, 79% of haematomas were hyperintense.
Isodense haematomas were diagnosed with
the aid of two findings on CT: (1) sulcal effacement, (2) midline shift and mass effect on the ventricles. However, all isodense haematomas were
clearly delineated on MR images (fig. 4).
All mixed density haematomas on CT were ei-
Figure 2
CT density patterns. a. Hypodense subdural haematoma. b. Isodense subdural haematoma. c. Hyperdense subdural
haematoma (arrow). d. Mixed density left frontoparietal haematoma with levelling. e. Mixed density haematoma with
hyperdense component (black arrow), and intrahaematomal membrane (white arrow).
Figure 3
MR imaging characteristics. a. Hypointense haematoma. b. Hyperintense haematoma. c. Mixed intensity left frontoparietal
haematoma with loculations and membranes. There is also a small right parietal hyperintense haematoma. d. Bilateral mixed
intensity haematomas with levelling.
Figure 4
Comparison of extent of haematoma and determination of membranes on CT and MR
imaging.
a. Isodense haematoma is barely recognised on CT with the aid of sulcal effacement.
b. Hyperintense haematoma with thin membranes (white arrows) is shown on T1W image.
c. Membranes (white arrows) are clearly discernible on T2W image.
CT and MR imaging of chronic subdural haematomas
ther layered or contained intrahaematomal membranes (fig. 2). Most of the haematomas with
membranes were mixed density on CT scans.
Membrane was discernible clearly in 3 of these
mixed density haematomas. When CT scans were
compared with MR images, some hyperdense areas of mixed density haematomas were in agreement with the capsule and membranes on MR images.
Levelling was observed in 12 haematomas
(25%) on both CT and MR images. Intrahaematomal membranes were surgically confirmed in
29 CSDHs (60%). Only 8 haematomas (27%) had
membranes on CT scans, whereas all membranes
were recognisable on MR images, especially on
T2W images (fig. 4).
Haematomas with membranes showed all
types of characteristics both on CT and MR images. However, mixed density on CT (52%) and
338
high intensity on MR (59%) were common observations. Chi-square test was applied to compare
CT density and MR intensity of haematomas with
or without membranes; however, no relationship
was found statistically (p >0.05).
There was no statistically significant difference between duration of symptoms in hyperintense haematomas (mean 34.4 10.7 days) and hypointense haematomas (mean 28.5 7.1 days) on
T1W images. Duration of symptoms did not differ significantly in haematomas with membranes
(mean 34.4 11.9 days) and without membranes
(mean 31.3 7.6 days) either.
All patients had similar outcome without early
serious complications, except for one patient with
acute myeloid leukaemia who died on the fifth day
of hospitalisation due to adult respiratory distress
syndrome. Hospital stay was 37 days.
Discussion
In this study we observed that various density
and intensity patterns of CSDHs can be detected
with CT and MR imaging. Unlike chronic intraparenchymal haematomas, mixed density on CT
and T1 hyperintensity are common in CSDHs.
Either layering or membranes are observed in
mixed density haematomas. Layering can be observed both on CT and MR images, whereas most
of the membranes, all of which are clearly delineated on MR imaging, cannot be recognised on CT
scans. MR is superior to CT when detecting membranes in CSDHs. We also found that haematomas appeared thicker on MR images compared to
CT. We therefore suggest that the extent and internal structures of CSDHs can be more precisely
evaluated by MR imaging, which provides highresolution images and better delineation of haematoma margins.
The capsule of CSDH consists of the outer
membrane adhering to the dura mater and the inner membrane on the arachnoid side. The vessels
of the capsule, which have a marked proliferation
potential and a fragile nature, are the most important factor for the development of CSDH [7]. Repeated microhaemorrhages from the neocapillary
network in the outer membrane of CSDH, and increased fibrinolytic activity of fibrinogen degradation products, result in large CSDHs [1]. Thrombomodulin expressed on the sinusoidal vessels of
the outer membrane in CSDHs inhibits the blood
coagulation system in the haematoma. Excessive
activation of both the coagulation and fibrinolytic
systems and high expression of tissue-type plasminogen activator in haematomas are proposed as
possible explanations for the failure of haematomas to coagulate [810]. Thus, CSDHs grow
gradually without coagulating.
The pathogenesis of CSDHs with excessive
activation of both the coagulation and fibrinolytic
systems results in complex imaging patterns. CSDHs can be low and high density, isodense or
mixed density on CT. MR imaging appearances
are more complex [11, 12]. Acute and subacute
subdural haematomas follow signal intensity patterns of intraparenchymal brain haemorrhage on
MR imaging, but they differ in the chronic phase
due to absence of bloodbrain barrier in the subdural space [5]. The propensity of CSDHs for repeat haemorrhage further complicates the CT
density and MR signal intensity patterns. The
phenomenon of repeated haemorrhage is characterised by layering effects and membranes as well
as more frequent haemosiderin deposition [5].
On MR, the haematocrit, methaemoglobin
and free Fe3+ levels are three major factors causing
prominent shortening in relaxation times and thus
high intensity on T1W imaging [13]. T1 shortening, which results with hyperintensity, generally
represents methaemoglobin, the typical component of subacute haematoma [1315]. The CSDH
may be slightly hypointense to isointense relative
to grey matter on short repetition time/echo time
(TR/TE), corresponding to T1W, images. Fobben
et al. postulate that these signal intensity changes
are the result of a decrease in concentration of free
methaemoglobin either by dilution, absorption
and/or degradation [5]. However, persistence of
high signal intensity, typical of the subacute intracranial haematomas [15], beyond its expected
time interval is a common observation, which is
probably due to repeated haemorrhage.
A CSDH is characterised by well formed inner and outer membranes and, regardless of the
time interval when the capsule is confirmed surgically, the haematoma should be regarded as
chronic [16]. Methaemoglobin, and thus T1 hyperintensity, may be the result of either a short
time interval from the onset of haemorrhage or of
S W I S S M E D W K LY 2 010 ; 1 4 0 ( 2 3 2 4 ) : 3 3 5 3 4 0 w w w . s m w . c h
rehaemorrhage. In all, 79% of haematomas in our
study were predominantly hyperintense on T1W
images. Hosoda et al. reported 18 CSDHs, 12
(67%) of which were hyperintense on T1W images [2]. Another study by Tsutsmi et al. showed
that 164 (71%) of 230 CSDHs were hyperintense
and mixed intensity [17]. These previously published studies and our study support the hypothesis that although various intensity patterns are
detected with MR imaging, most of the CSDHs
are predominantly hyperintense on T1W images.
Layering type and mixed density haematomas
have a stronger tendency to rebleed [18]. The
study by Lee et al. [19] demonstrated that 67% of
mixed density CSDHs required reoperation. Tsutsumi et al. suggested that T1W MR imaging was
useful in predicting the propensity of CSDHs to
recur [17]. They showed that high-intensity haematomas on T1 images had a lower recurrence
rate. However, Havenbergh et al. suggested that
CT findings had no influence on the patients outcome [20]. In this study we did not observe any
relationship between the prognosis and CT and
MR imaging characteristics of CSDHs either. The
absence of recurrences in this study may be due to
the small number of patients or to the absence of
long-time follow-up. Whether CT and MR imaging findings are important indicators of prognosis
is still unclear.
Despite general agreement concerning the indication for surgical treatment, the extent of surgery is controversial [12, 19, 2124]. Some authors
postulate that a small craniotomy can be preferred
for thick-membraned, loculated or multilayered
haematomas and solid haematomas with rehaemorrhage, whereas burr hole craniotomy or twist
drill craniotomy is suitable for more homogeneous-appearing haematomas [19, 25]. However,
others believe that less invasive procedures are adequate [12, 19, 24]. It is known that some loculated
haematomas with membranes recur and require
craniotomy, and MR imaging is useful in predicting the propensity of CSDHs to recur [17]. This
study shows that MR imaging is superior in delineating membranes of CSDHs. A small craniectomy instead of less invasive procedures may be
preferred when MR shows thick membranes.
Thus, MR imaging may influence the type of surgery.
An important limitation of our study is that
imaging of all patients could not be performed on
the same CT and MR scanners. CT and MR images could not be obtained simultaneously either.
MR images were obtained 07 days after CT scanning. In the time period between CT and MR
scans the clinical status of the patients remained
the same, and rebleeding was not considered.
When the long period from onset of symptoms or
339
trauma to CT scan (1472 days) is taken into account, this delay is not expected to influence the
appearance of haematoma on MR imaging.
Slice position was an important factor that
could influence the measurement results. All
transverse CT and MR images were obtained parallel to the vertex with similar angulations, and
two radiologists checked consecutive slice positions to make sure that slice positions were comparable if not identical. Slice thickness of CT and
MR scans was not identical either. However, since
measurements were performed on tranverse plane
vertical to the convexity of the calvarial bones,
slice thickness has little or no influence on haematoma thickness.
The diagnosis of CSDH is generally established by CT, which is a very fast scanning method
but has some important limitations. Exclusion of
other subdural collections such as effusions and
hygromas may be difficult in the case of hypodense subdural haematomas [5, 26]. Isodense
haematomas and small amounts of subdural collections are barely recognisable on CT [6, 16, 27],
whereas they are clearly discerned on MR images
[2, 28]. Subdural hygroma or effusions can also be
easily diagnosed by MR imaging [5, 29]. Previously published studies showed that MR imaging
is superior to CT in diagnosing small CSDHs [25,
30, 31]. It is also difficult to delineate haematoma
margins of isodense haematomas on CT, especially when they are bilateral [30]. In this study we
evaluated 29 isodense and mixed density haematomas, and we also observed that it was difficult to
delineate the exact margins of most of these haematomas on CT. We observed that haematoma
margins were clearly delineated with MR, and
haematomas appeared thicker on MR. We also
showed that all membranes could be determined
by MR imaging, whereas only 27% of them were
delineated by CT. MR is therefore superior to CT
when evaluating CSDHs.
CT is adequate for diagnosis when the extent
of CSDH can be clearly shown and other subdural
collections can be excluded. Since the thickness of
a haematoma is not very important when planning
surgery, and most patients can be treated with less
invasive procedures, MR imaging is not essential.
However, a small craniotomy may be preferred for
thick-membraned, loculated or multilayered haematomas, and, since most membranes could not
be identified on CT, MR imaging is useful. The
inner structures of the haematoma can change
the plan of surgery. We therefore suggest that if
the clinical status of the patient is not urgent, MR
imaging, when available, is useful in delineating
the exact margins of haematomas and determining
internal structures of haematomas.
340
CT and MR imaging of chronic subdural haematomas
Conclusions
Various density and intensity patterns are detected with CT and MR imaging, but most CSDHs are mixed density and predominantly hyperintense on T1W images.
MR imaging is more accurate than CT when
delineating the extent and determination of membranes of CSDHs, and with it hypodense CSDHs
can be differentiated from other subdural collections. Small and isodense CSDHs are better evaluated by MR. Mixed density CSDHs on CT are
generally layered, and membraned haematomas
and the internal structures can be clearly shown by
MR imaging, thus possibly changing the treatment strategy.
Correspondence:
Senem Senturk
Dicle Universitesi Tip Fakultesi
Radyoloji AD
21280, Diyarbakir, Turkey
E-Mail: snmsenturk@gmail.com
References
1 Markwalder TM. Chronic subdural hematomas: a review.
J Neurosurg. 1981;54:63745.
2 Hosoda K, Tamaki N, Masumura M, Matsumoto S, Maeda F.
Magnetic resonance images of chronic subdural hematomas.
J Neurosurg. 1987;67:67783.
3 Sipponen JT, Sepponen RE, Sivula AS. Chronic subdural hematoma: demonstration by magnetic resonance. Radiology.
1984;150:7985.
4 Ebisu T, Naruse S, Horikawa Y, Tanaka C, Higuchi T. Nonacute subdural hematoma: fundamental interpretation of MR
images based on biochemical and in vitro MR analysis. Radiology. 1989;171:44953.
5 Fobben ES, Grossman RI, Atlas SW, Hackney DB, Goldberg
HI, Zimmerman RA, Bilaniuk LT. MR characteristics of subdural hematomas and hygromas at 1.5T. AJR Am J Roentgenol.
1989;153:58995.
6 Smith WP Jr, Batnitzky S, Rengachary SS. Acute isodense subdural hematomas: a problem in anemic patients. AJR Am J
Roentgenol. 1981;136:5436.
7 Yamashima T, Yamamoto S. How do vessels proliferate in
the capsule of a chronic subdural hematoma? Neurosurgery.
1984;15:6728.
8 Kawakami Y, Chikama M, Tamiya T, Shimamura Y. Coagulation and fibrinolysis in chronic subdural hematoma. Neurosurgery. 1989;25:259.
9 Murakami H, Hirose Y, Sagoh M, Shimizu K, Kojima M,
Gotoh K, et al. Why do chronic subdural hematomas continue
to grow slowly and not coagulate? Role of thrombomodulin in
the mechanism. J Neurosurg. 2002;96:87784.
10 Vaquero J, Zurita M, Cincu R. Vascular endothelial growthpermeability factor in granulation tissue of chronic subdural
hematomas. Acta Neurochir. (Wien) 2002;144:3436.
11 Fujisawa H, Nomura S, Kajiwara K, Kato S, Fujii M, Suzuki
M. Various magnetic resonance imaging patterns of chronic
subdural hematomas: indicators of pathogenesis? Neurol Med
Chir. (Tokyo) 2006;46:3338.
12 Ernestus RI, Beldzinski P, Lanfermann H, Klug N. Chronic
subdural hematoma: surgical treatment and outcome in 104 patients. Surg Neurol. 1997;48:2205.
13 Bradley WG Jr. Schmidt PG. Effect of methemoglobin formation on the MR appearance of subarachnoid hemorrhage. Radiology. 1985;156:99-103.
14 Gomori JM, Grossman RI. Mechanisms responsible for the
MR appearance and evolution of intracranial hemorrhage. Radiographics. 1988;8:42740.
15 Gomori JM, Grossman RI, Hackney DB, Goldberg HI, Zimmerman RA, Bilaniuk LT. Variable appearances of subacute intracranial hematomas on high-field spin-echo MR. AJR Am J
Roentgenol. 1988;150:1718.
16 Fogelholm R, Heiskanen O, Waltimo O. Chronic subdural hematoma in adults. Influence of patients age on symptoms, signs,
and thickness of hematoma. J Neurosurg. 1975;42:436.
17 Tsutsumi K, Maeda K, Iijima A, Usui M, Okada Y, Kirino T.
The relationship of preoperative magnetic resonance imaging
fndings and closed system drainage in the recurrence of chronic
subdural hematoma. J Neurosurg. 1997;87:8705.
18 Nomura S, Kashiwagi S, Fujisawa H, Ito H, Nakamura K. Characterization of local hyperfibrinolysis in chronic subdural hematomas by SDS-PAGE and immunoblot. J Neurosurg. 1994;
81:9103.
19 Lee JY, Ebel H, Ernestus RI, Klug N. Various surgical treatments of chronic subdural hematoma and outcome in 172 patients: is membranectomy necessary? Surg Neurol. 2004;61:
5238.
20 van Havenbergh T, van Calenbergh F, Goffin J, Plets C. Outcome of chronic subdural hematoma: analysis of prognostic factors. Br J Neurosurg. 1996;10:359.
21 Erol FS, Topsakal C, Faik Ozveren M, Kaplan M, Tiftikci MT.
Irrigation vs. closed drainage in the treatment of chronic subdural hematoma. J Clin Neurosci. 2005;12:2613.
22 Markwalder TM, Steinsiepe KF, Rohner M, Reichenbach W,
Markwalder H. The course of chronic subdural hematomas after burr-hole craniostomy and closed-system drainage. J Neurosurg. 1981;55:3906.
23 Muzii VF, Bistazzoni S, Zalaffi A, Carangelo B, Mariottini A,
Palma L. Chronic subdural hematoma: Comparison of two
surgical techniques. Preliminary results of a prospective randomized study. J Neurosurg Sci. 2005;49:416.
24 Reinges MH, Hasselberg I, Rohde V, Kker W, Gilsbach JM.
Prospective analysis of bedside percutaneous subdural tapping
for the treatment of chronic subdural hematoma in adults. J
Neurol Neurosurg Psychiatry. 2000;69:407.
25 Tanikawa M, Mase M, Yamada K, Yamashita N, Matsumoto
T, Banno T, Miyati T. Surgical treatment of chronic subdural
hematoma based on intrahematomal membrane structure on
MRI. Acta Neurochir. (Wien) 2001;143:6138.
26 Mori K, Maeda M. Delayed magnetic resonance imaging with
GdD-DTPA differentiates subdural hygroma and subdural effusion. Surg Neurol. 2000;53:30310.
27 Amendola MA, Ostrum BJ. Diagnosis of isodense subdural hematomas by computed tomography.AJR Am J Roentgenol. 1977;
129:6937.
28 Han JS, Benson JE, Kaufman B, Rekate HL, Alfidi RJ, Huss
RG, Sacco D, Yoon YS, Morrison SC. MR imaging of pediatric
cerebral abnormalities. J Comput Asist Tomogr. 1985;9:10314.
29 Hasegawa M, Yamashima T, Yamashita J, Suzuki M, Shimada S.
Traumatic subdural hygroma: pathology and meningeal enhancement on magnetic resonance imaging. Neurosurgery. 1992;31:
5805.
30 Orrison WW, Gentry LR, Stimac GK, Tarrel RM, Espinosa
MC, Cobb LC. Blinded comparison of cranial CT and MR in
closed head injury evaluation. AJNR Am J Neuroradiol. 1994;
15:3516.
31 Provenzale J. CT and MR imaging of acute cranial trauma.
Emerg Radiol. 2007;14:112.
You might also like
- 114 FullDocument9 pages114 FullFebri W FinisiaNo ratings yet
- 249 FullDocument7 pages249 Fullwan hanisaNo ratings yet
- JAKO201528551641066Document6 pagesJAKO201528551641066PradanaNurOviyantiNo ratings yet
- The Role of Diffusion-Weighted Magnetic Resonance Imaging in The Differentiation of Head and Neck MassesDocument10 pagesThe Role of Diffusion-Weighted Magnetic Resonance Imaging in The Differentiation of Head and Neck MassestaufikolingNo ratings yet
- Tsutsumi 1997Document6 pagesTsutsumi 1997Ahmad AlzawahrehNo ratings yet
- RAD Head and Neck Vascular Lesions by CT Korean J RadiolDocument10 pagesRAD Head and Neck Vascular Lesions by CT Korean J RadiolyellowbieNo ratings yet
- LN3Document6 pagesLN3Haseeb QuadriNo ratings yet
- 145 Full PDFDocument7 pages145 Full PDFWildaHanimNo ratings yet
- Tractography of The BrainDocument11 pagesTractography of The BrainLina ArancibiaNo ratings yet
- Original Contribution: Ix. MR Tissue Characterization of Intracranial Tumors by Means of Texture AnalysisDocument8 pagesOriginal Contribution: Ix. MR Tissue Characterization of Intracranial Tumors by Means of Texture AnalysisrmaheshinNo ratings yet
- CT Angiography in The Evaluation of Acute StrokeDocument10 pagesCT Angiography in The Evaluation of Acute StrokeDio SukardiNo ratings yet
- Diagnostic Value and Forensic Relevance of A Novel Photorealistic 3D Reconstruction TechniqueDocument7 pagesDiagnostic Value and Forensic Relevance of A Novel Photorealistic 3D Reconstruction TechniqueYosef CnnNo ratings yet
- 476 FullDocument7 pages476 FullBen Chaaben AssilNo ratings yet
- EO10-my M1-Sa DWI AvastinDocument3 pagesEO10-my M1-Sa DWI Avastinserv2008tutbyNo ratings yet
- A Novel Technique For Short Nose CorrectionDocument74 pagesA Novel Technique For Short Nose CorrectionJWPlasticsurgeryNo ratings yet
- Real-Time Ultrasound Elastography - A Noninvasive Diagnostic Procedure For Evaluating Dominant Thyroid NodulesDocument7 pagesReal-Time Ultrasound Elastography - A Noninvasive Diagnostic Procedure For Evaluating Dominant Thyroid NodulesastriNo ratings yet
- Effective Utilization of Chest X-Ray For Follow-UpDocument4 pagesEffective Utilization of Chest X-Ray For Follow-UpAida Fitriyane HamdaniNo ratings yet
- Jurding RafioDocument6 pagesJurding RafioEveLyn PRadanaNo ratings yet
- CT Doses in Children - A Multicentre Study PDFDocument9 pagesCT Doses in Children - A Multicentre Study PDFRadoi Sandina RodicaNo ratings yet
- 3D Transthoracic Echocardiography Provides Accurate Cross-Sectional Area of The RV Outflow Tract - 1Document3 pages3D Transthoracic Echocardiography Provides Accurate Cross-Sectional Area of The RV Outflow Tract - 1Thumper KatesNo ratings yet
- Research ArticleDocument11 pagesResearch Articletsania nkdNo ratings yet
- 10.1007@s11060 004 3390 7Document9 pages10.1007@s11060 004 3390 7AlejitaplafuenteNo ratings yet
- Ctangiographyincomplexupperextremity Reconstruction: Keywords: CT Angiography, Upper Extremity ReconstructionDocument5 pagesCtangiographyincomplexupperextremity Reconstruction: Keywords: CT Angiography, Upper Extremity ReconstructionIrinel BuscaNo ratings yet
- PDF DIR 5932Document5 pagesPDF DIR 5932Yogi PrasetioNo ratings yet
- PDF PHDocument10 pagesPDF PHWennyNo ratings yet
- 11 - Espectroscopia Desmiel Tumefactive - Ikeguchi2018Document8 pages11 - Espectroscopia Desmiel Tumefactive - Ikeguchi2018Henry DanielNo ratings yet
- A Comparison Between The Reference Values of MRI and EUS and Their Usefulness To Surgeons in Rectal CancerDocument9 pagesA Comparison Between The Reference Values of MRI and EUS and Their Usefulness To Surgeons in Rectal CancerСергей СадовниковNo ratings yet
- Esti2012 E-0030Document8 pagesEsti2012 E-0030Anonymous p52JDZOdNo ratings yet
- Presentation 01Document15 pagesPresentation 01KDNo ratings yet
- Intratumoral Microhemorrhages On T2 - Weighted Gradient-Echo Imaging Helps Differentiate Vestibular Schwannoma From MeningiomaDocument6 pagesIntratumoral Microhemorrhages On T2 - Weighted Gradient-Echo Imaging Helps Differentiate Vestibular Schwannoma From MeningiomaBoyke SitompulNo ratings yet
- RM Rayos Carcinoma Canal AnalDocument9 pagesRM Rayos Carcinoma Canal Analouf81No ratings yet
- Vertebrobasilar Dolichoectasia Diagnosed by Magnetic Resonance Angiography and Risk of Stroke and Death: A Cohort StudyDocument6 pagesVertebrobasilar Dolichoectasia Diagnosed by Magnetic Resonance Angiography and Risk of Stroke and Death: A Cohort StudyRajesh SharmaNo ratings yet
- Daisne 2004Document8 pagesDaisne 2004alinaNo ratings yet
- Robot-Assisted Microwave Thermoablation of Liver Tumors: A Single-Center ExperienceDocument9 pagesRobot-Assisted Microwave Thermoablation of Liver Tumors: A Single-Center ExperienceMamanya Fadhil HaniNo ratings yet
- Relationship Between Patient Centering, Mean Computed Tomography Numbers and Noise in Abdominal Computed Tomography Influence of Anthropomorphic ParametersDocument7 pagesRelationship Between Patient Centering, Mean Computed Tomography Numbers and Noise in Abdominal Computed Tomography Influence of Anthropomorphic Parameterslorenz_gtlNo ratings yet
- Can Magnetic Resonance Spectroscopy Differentiate Endometrial Cancer?Document9 pagesCan Magnetic Resonance Spectroscopy Differentiate Endometrial Cancer?Csiszár MártonNo ratings yet
- Jurnal RadioDocument5 pagesJurnal RadioMatra Adi PrawiraNo ratings yet
- MRI Diffusion-Weighted Imaging in Intracranial Hemorrhage (ICH)Document10 pagesMRI Diffusion-Weighted Imaging in Intracranial Hemorrhage (ICH)Rika FitriaNo ratings yet
- 0040JKSMRM JKSMRM 17 8Document11 pages0040JKSMRM JKSMRM 17 8M P ChakravortyNo ratings yet
- Highres Mri Surgery Early RectalccDocument10 pagesHighres Mri Surgery Early RectalccCsiszár MártonNo ratings yet
- M Granulomatosa PDFDocument14 pagesM Granulomatosa PDFmorelialrNo ratings yet
- Yoon 2021Document5 pagesYoon 2021Muhammad Azhar ImranNo ratings yet
- Primary Leiomyosarcoma of The Spine: An Analysis of Imaging Manifestations and Clinicopathological FindingsDocument9 pagesPrimary Leiomyosarcoma of The Spine: An Analysis of Imaging Manifestations and Clinicopathological Findingst7xs5mchfzNo ratings yet
- Norbash 99 AjnrDocument7 pagesNorbash 99 Ajnrthor112No ratings yet
- 1785 FullDocument10 pages1785 FullAgustina 'tina' HartutiNo ratings yet
- Comparative Treatment Planning Study of Photons and ProtonsDocument15 pagesComparative Treatment Planning Study of Photons and ProtonsJesse Helmut Hansen-BartelNo ratings yet
- 1 s2.0 S0720048X16300286Document6 pages1 s2.0 S0720048X16300286Yuda ArifkaNo ratings yet
- Comparison of Susceptibility Artifact On Rectal Dwi Mri and Rectal Volume Before and After Ultraso PDFDocument6 pagesComparison of Susceptibility Artifact On Rectal Dwi Mri and Rectal Volume Before and After Ultraso PDFНикола ЋопићNo ratings yet
- CT MRI TBsadadDocument5 pagesCT MRI TBsadadArief RachmanNo ratings yet
- Imaging and Radiotherapy Physics - Proposal For PHD Degree: Kathrine - Redalen@Ntnu - NoDocument6 pagesImaging and Radiotherapy Physics - Proposal For PHD Degree: Kathrine - Redalen@Ntnu - Noali alasdyNo ratings yet
- 2011 Article 271Document4 pages2011 Article 271Diah HayustiningsihNo ratings yet
- TouijerDocument7 pagesTouijerVinko GrubišićNo ratings yet
- Abstract Knee PrativaDocument1 pageAbstract Knee PrativaRks RathoreNo ratings yet
- Pi Is 0012369215513937Document7 pagesPi Is 0012369215513937Tiar OktavianNo ratings yet
- Tumor Doubling TimeDocument6 pagesTumor Doubling TimeArismunandar SosiloNo ratings yet
- MRI CT-Scan SinusitisDocument8 pagesMRI CT-Scan SinusitisFongmeicha Elizabeth MargarethaNo ratings yet
- An Investigation of The Relationship Between Thoracic Outlet Syndrome and The Dimensions of The First Rib and ClavicleDocument7 pagesAn Investigation of The Relationship Between Thoracic Outlet Syndrome and The Dimensions of The First Rib and ClavicleFrancisco Javier Flores IzarNo ratings yet
- 1369 Full PDFDocument9 pages1369 Full PDFIqbal AbdillahNo ratings yet
- JCDR 10 TC01Document5 pagesJCDR 10 TC01Muhammad Azhar ImranNo ratings yet
- Ventriculoperitoneal Shunt Infection in Adult PatientDocument10 pagesVentriculoperitoneal Shunt Infection in Adult PatientYhafapCezNo ratings yet
- An Rifki/L/11 Th/12526678: No Identitas TGL Mrs Ruang Kasus Diagnosa Rencanatindaka N Lain-LainDocument1 pageAn Rifki/L/11 Th/12526678: No Identitas TGL Mrs Ruang Kasus Diagnosa Rencanatindaka N Lain-LainYhafapCezNo ratings yet
- MC Goon RatioDocument7 pagesMC Goon RatioYhafapCezNo ratings yet
- CT and MR Imaging of Chronic Subdural Haematomas: A Comparative StudyDocument6 pagesCT and MR Imaging of Chronic Subdural Haematomas: A Comparative StudyYhafapCezNo ratings yet
- The Computed Tomographic Attenuation and The Age of Subdural HematomasDocument2 pagesThe Computed Tomographic Attenuation and The Age of Subdural HematomasYhafapCezNo ratings yet
- Role of Repeat CT Scans in The ManagementDocument10 pagesRole of Repeat CT Scans in The ManagementYhafapCezNo ratings yet
- Gentamycin ItDocument14 pagesGentamycin ItYhafapCezNo ratings yet
- Valid ReliabelDocument2 pagesValid ReliabelYhafapCezNo ratings yet
- 1.1 Anterior Skull Base: 1.1.1 Cribriform Plate/Crista GalliDocument9 pages1.1 Anterior Skull Base: 1.1.1 Cribriform Plate/Crista GalliYhafapCezNo ratings yet
- Flail Chest 2Document16 pagesFlail Chest 2talithanrNo ratings yet
- MaxillofacialDocument11 pagesMaxillofacialManjeevNo ratings yet
- Difference Between 300 and 299Document3 pagesDifference Between 300 and 299vedanth saiNo ratings yet
- GRE Word ListDocument58 pagesGRE Word ListVibeesh SundarNo ratings yet
- RIB FractureDocument46 pagesRIB Fracturebanjar1982No ratings yet
- Basic Workshop Practice TME 121: Dr. David Fadare Mechanical Engineering Department University of IbadanDocument27 pagesBasic Workshop Practice TME 121: Dr. David Fadare Mechanical Engineering Department University of Ibadandude GFANo ratings yet
- Date/Schedule Activities Expected Output Verified/Checked by Area in ChargeDocument2 pagesDate/Schedule Activities Expected Output Verified/Checked by Area in ChargeJobelle AcenaNo ratings yet
- AMSSM Poster 2020Document1 pageAMSSM Poster 2020Thang TruongNo ratings yet
- Jsa Radiography ActivitiesDocument4 pagesJsa Radiography Activitiesnasar_mahsood80% (15)
- EC270Document13 pagesEC270AmilmcNo ratings yet
- Design and Development of A Portable Exoskeleton Based CPM Machine For Rehabilitation of Hand Injuries 2007Document6 pagesDesign and Development of A Portable Exoskeleton Based CPM Machine For Rehabilitation of Hand Injuries 2007newkid2202No ratings yet
- Forensic MedicineDocument15 pagesForensic MedicineJose Li ToNo ratings yet
- 19th Century Musket ManualDocument60 pages19th Century Musket Manualhwelch5792No ratings yet
- Sports Injury Management 071055Document10 pagesSports Injury Management 071055rickyguevarra620No ratings yet
- Basic Machine Training GuideDocument22 pagesBasic Machine Training GuideFernando Lopez CamposNo ratings yet
- Eka Pada Rajakapotasana (Pigeon Pose) GregoroviousDocument2 pagesEka Pada Rajakapotasana (Pigeon Pose) GregoroviousJaason GregoroviousNo ratings yet
- Tweet Topics2Document1,104 pagesTweet Topics2John NgNo ratings yet
- Short CasesDocument102 pagesShort CasesAanandi Arun MagotraNo ratings yet
- Congenital AbnormalitiesDocument37 pagesCongenital AbnormalitiesrezkadehaNo ratings yet
- Case Study of Hip FractureDocument2 pagesCase Study of Hip FractureBernardete Freitas Barros100% (1)
- Indo European Breweries Limited, Aurangabad: Likelihood/ Consequenc EsDocument1 pageIndo European Breweries Limited, Aurangabad: Likelihood/ Consequenc EsBALAJINo ratings yet
- Mgma-015 6 (1-2)Document497 pagesMgma-015 6 (1-2)galvangrr100% (2)
- FMT Bhalani AnswerDocument174 pagesFMT Bhalani Answerpatilysh1No ratings yet
- Bone MuscleDocument433 pagesBone Muscleridho budiNo ratings yet
- MILLER Testable ConceptsDocument109 pagesMILLER Testable ConceptsMohammedGooda100% (1)
- What Is The Difference Between Jha and JsaDocument2 pagesWhat Is The Difference Between Jha and JsaSalvacion JaroNo ratings yet
- Safe Working ProcedureDocument23 pagesSafe Working ProcedureBea MokNo ratings yet
- Tannis Edwards Victim Impact StatementDocument3 pagesTannis Edwards Victim Impact StatementThe Hamilton SpectatorNo ratings yet
- A Practical Guide To Binocular CollimationDocument23 pagesA Practical Guide To Binocular CollimationAlemx Ter67% (3)
- Neuroimaging of Spinal Instability-Journal ReadingDocument18 pagesNeuroimaging of Spinal Instability-Journal ReadingAmanda Aldilla MeutiadiNo ratings yet
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (2)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (28)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (81)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (393)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningFrom EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningRating: 4 out of 5 stars4/5 (3)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)From EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)No ratings yet
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- The Marshmallow Test: Mastering Self-ControlFrom EverandThe Marshmallow Test: Mastering Self-ControlRating: 4.5 out of 5 stars4.5/5 (58)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (170)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingFrom EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingRating: 4 out of 5 stars4/5 (1138)