Professional Documents
Culture Documents
Arterioscler Thromb Vasc Biol 2013 Norman 1473 7
Uploaded by
winardi rCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Arterioscler Thromb Vasc Biol 2013 Norman 1473 7
Uploaded by
winardi rCopyright:
Available Formats
ATVB in Focus
Tobacco Related Cardiovascular Diseases in the 21st Century
Series Editor: Muredach P. Reilly
Understanding the Effects of Tobacco Smoke on the
Pathogenesis of Aortic Aneurysm
Paul E. Norman, John A. Curci
Downloaded from http://atvb.ahajournals.org/ by guest on August 21, 2016
AbstractAneurysmal arterial disease is a vascular degenerative condition that is distinct from atherosclerotic and other
occlusive arterial diseases. There is regionalization of the predisposition to aneurysm formation within the vascular tree,
and the pathological process varies with location. Infrarenal abdominal aortic aneurysm (AAA) is the most common
manifestation of aneurysmal disease, and smoking is the dominant risk factor. Smoking is a much greater risk factor
for AAA than for atherosclerosis. In addition to playing a role in the pathogenesis of AAA, smoking also increases the
rate of expansion and risk of rupture of established AAA. The mechanistic relationship between AAA and smoking
is being established by the use of enhanced animal models that are dependent on smoke or smoke components. The
mechanisms seem to involve durable alterations in vascular smooth muscle cell and inflammatory cell function. This
review examines the clinical, epidemiological, and mechanistic evidence implicating smoking as a cause of aneurysms,
focusing on AAA.(Arterioscler Thromb Vasc Biol. 2013;33:1473-1477.)
Key Words: aneurysm smoking pathogenesis risk factor
neurysmal arterial disease is clinically, histologically,
and mechanistically quite distinct from atherosclerosis
and other occlusive arterial disease. Although atherosclerotic
change may be seen in many aneurysms, the relationship is
not necessarily a causal one. Aneurysms are more common
in some arteries than others, and their pathogenesis varies
by location, with, for example, hypertension dominating in
cerebral arteries, genetic factors dominating in the ascending aorta, and smoking dominating in the abdominal aorta.1
Given the importance of smoking in abdominal aortic aneurysm (AAA), this review focuses on AAA. Although there is
less evidence implicating smoking in other manifestations of
aneurysmal disease, this does not exclude a role for smoking
in the development or progression of other aneurysms.
Swedish men aged 65 years, 87% of men with AAA were current or ex-smokers, and smoking was the dominant risk factor
for AAA (odds ratio, 3.5; 95% CI, 2.45.1).4
Results from a screening study of >3 million individuals
in the United States showed that there was a clear relationship between prevalent AAA and both duration and amount of
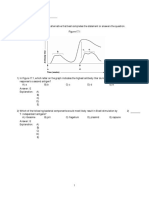
smoking (Figure 1).5 There is evidence of a strong linear dose
response effect with duration of smoking.2,5,6 The relationship
with the amount smoked is also linear in current smokers and
to a lesser extent in ex-smokers.5,6 In ex-smokers, the duration
seems to be more important than the level of exposure.5,6
The magnitude of risk with smoking eclipses all other
modifiable risk factors for prevalent AAA. Intriguingly, smoking
seems to be a substantially greater risk factor for AAA than for
occlusive atherosclerotic disease. In a systematic review by
Lederle et al,7 the association between smoking and AAA was
2.5-fold (95% CI, 2.22.8) greater than the association between
smoking and coronary heart disease. The divergent effect of
smoking on these 2 vascular diseases supports the distinct
pathogenesis of aneurysmal and occlusive arterial disease.
The US Preventive Services Task Force considered smoking
a sufficiently dominant risk factor for AAA to recommend
screening men aged 65 to 75 years who have ever smoked, rather
than all men of that age.8 Kent et al5 have demonstrated that the
efficiency of screening can be improved using algorithms based
on risk factors, such as smoking. However, other studies have
not supported selective screening based on risk factors.9,10
Although AAA is less common in women, outcomes seem
to be worse in women with AAA compared with men with
Clinical and Epidemiological Studies of
Smoking and AAA
Smoking Increases Prevalence and Incidence
All epidemiological studies of AAA have identified the importance of smoking as a risk factor. Smoking is a very strong risk
factor for the presence of an AAA in both men and women, with
odds ratios ranging from 3 to 12.2,3 In the large (n=114567)
Aneurysm Detection and Management (ADAM) screening
study, a history of ever smoking was associated with an odds
ratio of 2.97 (95% CI, 2.653.32) for 3- to 3.9-cm AAAs and
5.07 (95% CI, 4.136.21) for 4-cm AAAs.2 Smoking was
considered to be responsible for 75% of the excess prevalence of AAAs 4 cm. In a recent report of screening 22187
Received on: September 17, 2012; final version accepted on: November 20, 2012.
From the School of Surgery, University of Western Australia, Fremantle, Australia (P.E.N.); and Department of Surgery, Section of Vascular Surgery,
Washington University School of Medicine, Saint Louis, MO (J.A.C.).
Correspondence to Paul Norman, School of Surgery, University of Western Australia, Fremantle Hospital, PO Box 480, Fremantle, WA 6959, Australia.
E-mail paul.norman@uwa.edu.au
2013 American Heart Association, Inc.
Arterioscler Thromb Vasc Biol is available at http://atvb.ahajournals.org
1473
DOI: 10.1161/ATVBAHA.112.300158
1474 Arterioscler Thromb Vasc Biol July 2013
1.333.06) for current smoking versus ex/never smoker, an
effect that was independent of aneurysmal diameter.15
Influence of Smoking on Intervention and Prognosis
Downloaded from http://atvb.ahajournals.org/ by guest on August 21, 2016
Smoking is relevant when patients require intervention for AAA.
For patients undergoing surgical intervention for AAA, current
smoking is likely to increase the risk of perioperative death and
late mortality. In the UK Small Aneurysm Trial, continued smoking 1 year after randomization was associated with significantly
increased mortality (hazard ratio, 3.23; 95% CI, 1.736.03).17
Although smokers are less likely to develop an endoleak after
endovascular repair (presumably as a result of prothrombotic
effects), they are at increased risk of stent migration.18
The recently documented decline in incidence of AAA
interventions and deaths and the lower than expected prevalence in screening studies have been attributed to falling
rates of smoking.4,19,20 Smoking cessation is associated with a
decline in risk of an AAA of 30% for each decade after quitting (Figure 1).2,5,6 Nevertheless, the legacy of increased risk
of AAA from smoking lasts many decades.14
Mechanistic Studies of Smoking
and Aneurysm Formation
Figure 1. Age-adjusted effects of: smoking duration (A), quantity
(B), and time since quitting (C) on the risk of abdominal aortic
aneurysm (AAA). Reference groups are nonsmokers for all smoking variables. The vertical error bars show 95% CIs. Adapted with
permission from Kent et al.5
AAA.11 There is some evidence that smoking may be a greater
risk factor for AAA in women than in men. In the Rotterdam
Study, 56% of women with AAA were current smokers compared with 38% of men.12 In the ADAM study, the odds ratio
for ever smoking was 3.80 (95% CI, 1.579.20) in women
compared with 3.34 (95% CI, 3.043.67) in men.13 It is
unclear how important these differences are.
Smoking is also the dominant factor for incident AAA. In
a prospective analysis of the Troms study, there was a dose
response effect with both smoking duration and quantity.14
Even individuals who had stopped smoking 10 to 19 years
earlier had nearly a 3-fold risk of an incident AAA compared
with nonsmokers. This suggests that smoking has a durable
influence on AAA formation an effect also seen in recent
experimental studies (see below).
Smoking Increases Expansion
Rate and Rupture Risk
Smoking is an important cause of progression of AAA.
Continued smoking in individuals with an AAA is associated
with both increased rates of expansion and the risk of rupture.
In a recent meta-analysis using data from 15475 patients with
small (35.5 cm) AAAs, current smoking was associated with
an increased rate of expansion of 0.35 (95% CI, 0.230.48)
mm/year.15 In the UK Small Aneurysm Trial, current smoking
doubled the risk of rupture, although this was not statistically
significant, with a hazard ratio of 2.11 (95% CI, 0.95 4.67).16
However, this doubling of risk was confirmed as significant
in a recent meta-analysis with a hazard ratio of 2.02 (95% CI,
The most striking feature of AAA histology is the loss of normal medial arterial structure and, in particular, the near complete absence of a normal lamellar elastin matrix, a feature
that it has in common with chronic obstructive pulmonary
disease.21 In the aorta, these matrix changes are attributed to 3
general features that are believed to be interrelated: (1) elaboration of high levels of proteases, (2) chronic inflammatory
infiltration, and (3) loss/dysfunction of parenchymal cells central to matrix deposition and repair.
Although considerable research with human tissue and
animal models over the past 2 decades has begun to inform our
understanding of the initiation and progression of AAA, we are
yet to develop and verify an effective biological therapeutic
that will interrupt development of an AAA or halt the growth
of a small AAA. However, given the importance of smoking
as a risk factor, there has until recently been very little work
on the effects of smoke exposure in these models. Because
of the complex make-up of tobacco smoke (TS) and the
variety of intermediaries that may be involved, the effects on
the vasculature could be mediated through alterations of the
inflammatory response, of resident vascular smooth muscle cell
(VSMC) function, or of the vessel matrix itself. Several different
experimental approaches have been proposed to determine the
mechanisms of AAA formation related to smoking (Table).
Human Studies
There are many challenges to evaluating the mechanistic
effects of smoking on AAA formation in humans. When
looking at the associations of various circulating markers in
patients with AAA, Lindholt et al22 came to the conclusion that
smoking may activate tissue plasminogen activator. Because
tissue plasminogen activator is a potent activator of elastolytic
matrix metalloproteinase, this could link smoking to aortic
elastolysis. In support of this, others have shown endothelial
response to serum from smokers to result in increased tissue
Norman and Curci Smoking and Aneurysm Formation 1475
Table.
Mechanistic Studies of Smoking Components and AAA
Smoke Component
Study Design
Potential Mechanism
Source
Whole smoke
Circulating inflammatory markers in humans with AAA
Increased tPA in smokers which could activate proteases
22
Whole smoke
Genome-wide association study in humans
Association of smoke and AAA on 3p12.3 and epigenetic
modifications
2325
Water-soluble smoke extract
Human VSMC
Suppression of prolyl-4-hydroxylase
Water-soluble smoke extract
Human neutrophils, endothelial cells, and VSMC
Increased MMP production
Nicotine
VSMC and inflammatory cells
Multiple
29
Nicotine
Mouse (ApoE-deficient) model of AAA
AMP-activated protein kinase 2
30
Nicotine
Mouse (ApoE-deficient and elastase perfusion) model
of AAA
miR-21 (also associated with stabilization of aortic dilation)
31
Whole smoke
Mouse (ApoE-deficient) model of AAA
Increased MMP gene expression
32
Whole smoke
Mouse (modified elastase perfusion) model of AAA
Altered T-cell response
33
26
27,28
AAA indicates abdominal aortic aneurysm; tPA, tissue plasminogen activator; VSMC, vascular smooth muscle cells; and MMP, matrix metalloproteinase.
Downloaded from http://atvb.ahajournals.org/ by guest on August 21, 2016
plasminogen activator without increased plasminogen activator inhibitor-1 or tissue factor pathway inhibitor-1.34
Genetic variants associated with AAA have also shown potential
interactions with smoking. One genome-wide association study
found a variant on 3p12.3, which demonstrated that the genetic risk
was significantly greater in those with a history of smoking.23 Other
studies, however, have not shown a clear relationship among smoking, genetic variants, and AAA.24 It is also possible that smoking
contributes to the pathogenesis of AAA via epigenetic interactions,
although conclusive evidence about this is still lacking.25
Studies of Smoke Components
Because the matrix changes in the aorta bear some resemblance to those in the lung, some studies have begun with
a presumption that the mechanisms are likely to be similar.
Applying techniques that were successfully used to define
similar pathological processes induced by TS in the lung,3541
these studies have attempted to develop a mechanistic understanding of TS on vascular biology. Typically, these studies
have relied primarily on gross extracts or purified specific
components of TS applied in vivo or to tissues or cells.
Using a water-soluble cigarette smoke extract (CSE) applied
to VSMC in culture, the expression of a key component of
prolyl-4-hydroxylase is suppressed and thereby reduces collagen production.26 This could promote AAA development
by reducing the ability of the aorta to repair medial structural
damage. Others have shown that CSE can induce metalloprotease production and release in vascular cells and inflammatory cells,27,28 thereby promoting matrix damage.
In other studies, however, there is evidence of effects of CSE
that would be contrary to what is known about AAA pathology.
In VSMC, CSE seems to promote proliferation and survival.42
This would be consistent with the enhancement of intimal
hyperplasia caused by smoking, but the VSMC in AAA are
typically sparse and senescent and reproduce poorly in vitro.43
Furthermore, the immunomodulatory effects of TS and CSE
in the acute situation vary, but it is well described that chronic
exposure effectively induces T-cell anergy,44,45 which seems
contradictory to the chronic inflammation prominent in AAA.
The cellular effects of nicotine have been well studied and
include effects that may both promote and inhibit AAA development, as has been reviewed elsewhere.29 Two recent studies
using the apolipoprotein Edeficient mouse model of AAA
have shown that nicotine can significantly increase aneurysm
formation either with31 or without angiotensin II infusion.30 A
similar AAA augmentation has also been shown with nicotine
infusion in the elastase perfusion model.31
Activation of the AMP-activated protein kinase 2
(AMPK-2) in VSMC may be responsible for the nicotine-enhanced AAA formation,30 consistent with increased
AMPK-2 in both smokers and patients with AAA. In a second
study, microRNA-21 (miR-21) was found to be enhanced late in
aneurysm development in both apolipoprotein Edeficient and
elastase perfusion models and was associated with stabilization
of further dilation.31 Although nicotine exposure increased miR21 in the aneurysms and cell culture, AAA in the model was
abrogated with administration of exogenous premiR-21. The
authors did not resolve the apparent contradiction with respect
to the effects of nicotine on AAA formation and miR-21.
The relationship between these 2 distinct mechanisms of
AAA development related to nicotine exposure remains to be
elucidated, although there are some data to suggest that they
may be regulated similarly in response to cellular stress. Both
miR-21 and AMPK are recognized to be increased in response
to hypoxia.46 There is evidence that miR-21 and AMPK can
both be elevated in the context of a stress on glioma cells.47
Further studies of the downstream effects of miR-21 and
AMPK, particularly in the context of whole-animal smoke
exposure, will probably be necessary to better clarify the role
of these molecules in nicotine-enhanced AAA.
Models Incorporating In Vivo Smoke Exposure
Although smoke component studies do offer important clues to
the effects of TS on AAA development, they are often severely
limited by 3 assumptions: First, that the toxin or limited toxin
mixture applied to the cells in culture (or selected for in vivo
exposure) would elicit the same effect as the in vivo response
when an individual inhales cigarette smoke. Second, that the
components evaluated will elicit the same response when used
in a more complex mixture. Third, that TS or TS component
exposure may activate known pathways of disease. None of
these assumptions has been rigorously investigated or validated.
Models that examine the in vivo effects of smoking on
AAA development have a critical role to play with regard
to exploring the biological response of the aorta to inhaled
smoke and in validating the mechanistic pathways defined by
1476 Arterioscler Thromb Vasc Biol July 2013
Downloaded from http://atvb.ahajournals.org/ by guest on August 21, 2016
smoke component evaluations. Unfortunately, although exposure to smoke in the mouse has been used for years to model
pulmonary disease, no aneurysm phenotype emerged. Several
investigators have demonstrated smoke-enhanced AAA formation with the elastase perfusion model or the angiotensin
IItreated apolipoprotein E knockout model.32,48,49
In the elastase perfusion model, like the human disease where
the increased risk of aneurysm formation persists decades after
cessation of smoke exposure,14 the effects of relatively short
exposure to smoke (6 weeks) result in persistently increased AAA
development at least 8 weeks after smoke cessation. Somewhat
surprisingly, the effects of smoke on aneurysm development are
not inhibited with protease inhibitors or through genetic knockout of elastolytic enzymes.33 The ultrastructure of the aorta is not
altered by smoke exposure alone, but smoke exposure increases
the T-cell infiltrate in the aorta in response to elastase injury.
Even more remarkable was the finding that adoptive transfer
of leukocytes from smoke-exposed animals to smoke-free animals confers the enhanced aneurysm phenotype on the recipient.33 These results suggest that durable alterations in leukocyte
function, particularly the effects on T cells, may contribute to the
enhancement of aneurysm formation by smoking (Figure 2).
Consolidating Current Experimental
Results of Smoking on AAA
The impact of the inhalation of a complex cocktail of potential
toxins in cigarette smoke on the vasculature presents a significant challenge to scientific interrogation. It must be recognized
that the in vivo inhalation of TS results in episodic exposure of
combustion products with a variety of bioactivities (eg, oxygen
radicals) and affinities with the circulation (eg, lipophilic versus
hydrophilic) in the process of delivery to the tissue of interest
the aorta. Cells and enzymes in circulation may also interact
with the absorbed smoke in ways that are not well understood.
Prominent components of tobacco smoke, such as nicotine,
are relatively easy to study in isolation, with some elegant results
in cell culture and animals models that can confirm our bias
regarding the role of smoking on arterial disease. These studies of individual smoke components must be interpreted with
caution, however. The apparent contradictory results of smoke
component experiments seen in some of these studies may well
be because of unique responses to the simplified exposure chosen (Figure 2). The novel aneurysm models based on inhaled
cigarette smoke exposure provide a critical means of validating
the potential mechanisms related to smoke components.
Figure 2. Both nicotine infusion and experimental smoke exposure can lead to enhanced aneurysm development in murine
models. Nicotine seems to directly enhance abdominal aortic
aneurysm (AAA) development via AMP-activated protein kinase
2 (AMPK-2) activation in aortic smooth muscle cells. Nicotine
also increases local production of the microRNA-21 (miR-21),
which may stabilize the aneurysm through improved matrix repair
processes. Inhalation of tobacco smoke enhances AAA development through altered leukocyte function, which seems to be predominantly T-celldependent. It is unclear whether AMPK-2 is
activated by nicotine when inhaled during tobacco smoking.
Sources of Funding
This work was supported by the National Health and Medical
Research Council of Australia grants 458505 and1006266 (to P.E.
Norman), the National Heart, Lung, and Blood Institute K08 HL84004
(to J.A. Curci), Flight Attendants Medical Research Institute (to J.A.
Curci), the American Heart Association 0765432Z (to J.A. Curci),
the American College of Surgeons/Society for Vascular Surgery
Foundation (to J.A. Curci), the Department of Veterans Affairs (J.A.
Curci), and the Peripheral Vascular Surgery Society (J.A. Curci).
Conclusion
There is little doubt that smoking is an important cause of AAA
development and progression. It is, however, not the only cause
of AAA, with 10% to 15% of cases seen in individuals who have
never smoked.4 This highlights the fact that our understanding
of the pathogenesis of AAA is still incomplete. The resistance
of smoke-enhanced AAA models to inhibition of elastolytic
proteases is an important new clue. An understanding of the
unique mechanisms related to smoking is needed to shed light on
new strategies to prevent or retard the growth of AAA. Although
there is no direct evidence that smoking cessation prevents AAA
or decreases the need for AAA intervention, health economic
modeling suggests that it would be a cost-effective strategy and
it remains a priority for all patients with AAA.50
Disclosures
None.
References
1. Norman PE, Powell JT. Site specificity of aneurysmal disease.
Circulation. 2010;121:560568.
2. Lederle FA, Johnson GR, Wilson SE, Chute EP, Hye RJ, Makaroun MS,
Barone GW, Bandyk D, Moneta GL, Makhoul RG. The aneurysm detection and management study screening program: validation cohort and
final results. Aneurysm Detection and Management Veterans Affairs
Cooperative Study Investigators. Arch Intern Med. 2000;160:14251430.
3. Jamrozik K, Norman PE, Spencer CA, Parsons RW, Tuohy R, LawrenceBrown MM, Dickinson JA. Screening for abdominal aortic aneurysm:
lessons from a population-based study. Med J Aust. 2000;173:345350.
4. Svensj S, Bjrck M, Grtelschmid M, Djavani Gidlund K, Hellberg
A, Wanhainen A. Low prevalence of abdominal aortic aneurysm among
Norman and Curci Smoking and Aneurysm Formation 1477
Downloaded from http://atvb.ahajournals.org/ by guest on August 21, 2016
65-year-old Swedish men indicates a change in the epidemiology of the
disease. Circulation. 2011;124:11181123.
5. Kent KC, Zwolak RM, Egorova NN, Riles TS, Manganaro A, Moskowitz
AJ, Gelijns AC, Greco G. Analysis of risk factors for abdominal aortic
aneurysm in a cohort of more than 3 million individuals. J Vasc Surg.
2010;52:539548.
6. Wilmink TB, Quick CR, Day NE. The association between cigarette smoking and abdominal aortic aneurysms. J Vasc Surg. 1999;30:10991105.
7. Lederle FA, Nelson DB, Joseph AM. Smokers relative risk for aortic
aneurysm compared with other smoking-related diseases: a systematic
review. J Vasc Surg. 2003;38:329334.
8. US Preventive Services Task Force. Screening for abdominal aortic
aneurysm: recommendation statement. Ann Int Med. 2005;142:198202.
9. Vardulaki KA, Walker NM, Day NE, Duffy SW, Ashton HA, Scott RA.
Quantifying the risks of hypertension, age, sex and smoking in patients
with abdominal aortic aneurysm. Br J Surg. 2000;87:195200.
10. Spencer CA, Jamrozik K, Norman PE, Lawrence-Brown MM. The
potential for a selective screening strategy for abdominal aortic aneurysm. J Med Screen. 2000;7:209211.
11. Norman PE, Powell JT. Abdominal aortic aneurysm: the prognosis in
women is worse than in men. Circulation. 2007;115:28652869.
12. Pleumeekers HJ, Hoes AW, van der Does E, van Urk H, Hofman A, de
Jong PT, Grobbee DE. Aneurysms of the abdominal aorta in older adults.
The Rotterdam Study. Am J Epidemiol. 1995;142:12911299.
13. Lederle FA, Johnson GR, Wilson SE; Aneurysm Detection and
Management Veterans Affairs Cooperative Study. Abdominal aortic
aneurysm in women. J Vasc Surg. 2001;34:122126.
14. Forsdahl SH, Singh K, Solberg S, Jacobsen BK. Risk factors for abdominal aortic aneurysms: a 7-year prospective study: the Tromso Study,
19942001. Circulation. 2009;119:22012208.
15. Sweeting MJ, Thompson SG, Brown LC, Powell JT; RESCAN collaborators. Meta-analysis of individual patient data to examine factors affecting growth and rupture of small abdominal aortic aneurysms. Br J Surg.
2012;99:655665.
16. The United Kingdom Small Aneurysm Trial Participants. Risk factors
for aneurysm rupture in patients kept under ultrasound surveillance. Ann
Surg. 1999;230:28996.
17. The United Kingdom Small Aneurysm Trial Participants. Long-term
outcomes of immediate repair compared with surveillance of small
abdominal aortic aneurysms. N Eng J Med. 2002;346:144552.
18. Koole D, Moll FL, Buth J, Hobo R, Zandvoort H, Pasterkamp G, van
Herwaarden JA; EUROSTAR collaborators. The influence of smoking on endovascular abdominal aortic aneurysm repair. J Vasc Surg.
2012;55:15811586.
19. Norman PE, Spilsbury K, Semmens JB. Falling rates of hospitalization
and mortality from abdominal aortic aneurysms in Australia. J Vasc
Surg. 2011;53:274277.
20. Anjum A, von Allmen R, Greenhalgh R, Powell JT. Explaining the
decrease in mortality from abdominal aortic aneurysm rupture. Br J
Surg. 2012;99:637645.
21. Snider GL. Distinguishing among asthma, chronic bronchitis, and
emphysema. Chest. 1985;87:35S39S.
22. Lindholt JS, Jrgensen B, Shi GP, Henneberg EW. Relationships between
activators and inhibitors of plasminogen, and the progression of small
abdominal aortic aneurysms. Eur J Vasc Endovasc Surg. 2003;25:546551.
23. Elmore JR, Obmann MA, Kuivaniemi H, Tromp G, Gerhard GS,
Franklin DP, Boddy AM, Carey DJ. Identification of a genetic variant
associated with abdominal aortic aneurysms on chromosome 3p12.3 by
genome wide association. J Vasc Surg. 2009;49:15251531.
24. Gretarsdottir S, Baas AF, Thorleifsson G, et al. Genome-wide association study identifies a sequence variant within the DAB2IP gene
conferring susceptibility to abdominal aortic aneurysm. Nat Genet.
2010;42:692697.
25. Krishna SM, Dear AE, Norman PE, Golledge J. Genetic and epigenetic mechanisms and their possible role in abdominal aortic aneurysm.
Atherosclerosis. 2010;212:1629.
26. Raveendran M, Senthil D, Utama B, Shen Y, Dudley D, Wang J, Zhang Y,
Wang XL. Cigarette suppresses the expression of P4Halpha and vascular
collagen production. Biochem Biophys Res Commun. 2004;323:592598.
27. Murphy EA, Danna-Lopes D, Sarfati I, Rao SK, Cohen JR. Nicotinestimulated elastase activity release by neutrophils in patients with
abdominal aortic aneurysms. Ann Vasc Surg. 1998;12:4145.
28. Lematre V, Dabo AJ, DArmiento J. Cigarette smoke components
induce matrix metalloproteinase-1 in aortic endothelial cells through
inhibition of mTOR signaling. Toxicol Sci. 2011;123:542549.
29. Li ZZ, Dai QY. Pathogenesis of abdominal aortic aneurysms: role of
nicotine and nicotinic acetylcholine receptors. Mediators Inflamm.
2012;2012:103120.
30. Wang S, Zhang C, Zhang M, Liang B, Zhu H, Lee J, Viollet B, Xia L,
Zhang Y, Zou MH. Activation of AMP-activated protein kinase 2 by
nicotine instigates formation of abdominal aortic aneurysms in mice in
vivo. Nat Med. 2012;18:902910.
31. Maegdefessel L, Azuma J, Toh R, Deng A, Merk DR, Raiesdana A, Leeper
NJ, Raaz U, Schoelmerich AM, McConnell MV, Dalman RL, Spin JM,
Tsao PS. MicroRNA-21 blocks abdominal aortic aneurysm development
and nicotine-augmented expansion. Sci Transl Med. 2012;4:122ra22.
32. Stolle K, Berges A, Lietz M, Lebrun S, Wallerath T. Cigarette smoke
enhances abdominal aortic aneurysm formation in angiotensin II-treated
apolipoprotein E-deficient mice. Toxicol Lett. 2010;199:403409.
33. Arif B, Garcia-Fernandez F, Ennis TL, Jin J, Davis EC, Thompson RW,
Curci, JA. Novel mechanism of aortic aneurysm development in mice
associated with smoking and leukocytes. Arterioscler Thromb Vasc Biol.
2012;32:29012909.
34. Barua RS, Ambrose JA, Saha DC, Eales-Reynolds LJ. Smoking is associated with altered endothelial-derived fibrinolytic and antithrombotic
factors: an in vitro demonstration. Circulation. 2002;106:905908.
35. Shapiro SD. The pathogenesis of emphysema: the elastase:antielastase
hypothesis 30 years later. Proc Assoc Am Physicians. 1995;107:346352.
36. Shapiro SD. Evolving concepts in the pathogenesis of chronic obstructive pulmonary disease. Clin Chest.Med. 2000;21:621632.
37. Shapiro SD. Proteinases in chronic obstructive pulmonary disease.
Biochem Soc Trans. 2002;30:98102.
38. Finlay GA, ODriscoll LR, Russell KJ, DArcy EM, Masterson JB,
FitzGerald MX, OConnor CM. Matrix metalloproteinase expression
and production by alveolar macrophages in emphysema. Am J Respir
Crit Care Med. 1997;156:240247.
39. Finlay GA, Russell KJ, McMahon KJ, Darcy EM, Masterson JB,
FitzGerald MX, OConnor CM. Elevated levels of matrix metalloproteinases in bronchoalveolar lavage fluid of emphysematous patients.
Thorax. 1997;52:502506.
40. Segura-Valdez L, Pardo A, Gaxiola M, Uhal BD, Becerril C, Selman M.
Upregulation of gelatinases A and B, collagenases 1 and 2, and increased
parenchymal cell death in COPD. Chest. 2000;117:684694.
41. Betsuyaku T, Nishimura M, Takeyabu K, Tanino M, Venge P, Xu S,
Kawakami Y. Neutrophil granule proteins in bronchoalveolar lavage
fluid from subjects with subclinical emphysema. Am J Respir Crit Care
Med. 1999;159:19851991.
42. Chen QW, Edvinsson L, Xu CB. Cigarette smoke extract promotes human
vascular smooth muscle cell proliferation and survival through ERK1/2- and
NF-B-dependent pathways. ScientificWorldJournal. 2010;10:21392156.
43. Liao S, Curci JA, Kelley BJ, Sicard GA, Thompson RW. Accelerated
replicative senescence of medial smooth muscle cells derived from
abdominal aortic aneurysms compared to the adjacent inferior mesenteric artery. J Surg Res. 2000;92:8595.
44. Kalra R, Singh SP, Savage SM, Finch GL, Sopori ML. Effects of cigarette smoke on immune response: chronic exposure to cigarette smoke
impairs antigen-mediated signaling in T cells and depletes IP3-sensitive
Ca(2+) stores. J Pharmacol Exp Ther. 2000;293:166171.
45. Geng Y, Savage SM, Razani-Boroujerdi S, Sopori ML. Effects of nicotine on the immune response. II. Chronic nicotine treatment induces T
cell anergy. J Immunol. 1996;156:23842390.
46. Polytarchou C, Iliopoulos D, Hatziapostolou M, Kottakis F, Maroulakou
I, Struhl K, Tsichlis PN. Akt2 regulates all Akt isoforms and promotes
resistance to hypoxia through induction of miR-21 upon oxygen deprivation. Cancer Res. 2011;71:47204731.
47. Godlewski J, Nowicki MO, Bronisz A, Nuovo G, Palatini J, De Lay M,
Van Brocklyn J, Ostrowski MC, Chiocca EA, Lawler SE. MicroRNA-451
regulates LKB1/AMPK signaling and allows adaptation to metabolic
stress in glioma cells. Mol Cell. 2010;37:620632.
48. Buckley C, Wyble CW, Borhani M, Ennis TL, Kobayashi DK, Curci JA,
Shapiro SD, Thompson RW. Accelerated enlargement of experimental abdominal aortic aneurysms in a mouse model of chronic cigarette
smoke exposure. J Am Coll Surg. 2004;199:896903.
49. Bergoeing MP, Arif B, Hackmann AE, Ennis TL, Thompson RW,
Curci JA. Cigarette smoking increases aortic dilatation without affecting matrix metalloproteinase-9 and -12 expression in a modified mouse
model of aneurysm formation. J Vasc Surg. 2007;21:328338.
50. Mani K, Wanhainen A, Lundkvist J, Lindstrm D. Cost-effectiveness of
intensive smoking cessation therapy among patients with small abdominal aortic aneurysms. J Vasc Surg. 2011;54:628636.
Downloaded from http://atvb.ahajournals.org/ by guest on August 21, 2016
Understanding the Effects of Tobacco Smoke on the Pathogenesis of Aortic Aneurysm
Paul E. Norman and John A. Curci
Arterioscler Thromb Vasc Biol. 2013;33:1473-1477; originally published online May 16, 2013;
doi: 10.1161/ATVBAHA.112.300158
Arteriosclerosis, Thrombosis, and Vascular Biology is published by the American Heart Association, 7272 Greenville
Avenue, Dallas, TX 75231
Copyright 2013 American Heart Association, Inc. All rights reserved.
Print ISSN: 1079-5642. Online ISSN: 1524-4636
The online version of this article, along with updated information and services, is located on the
World Wide Web at:
http://atvb.ahajournals.org/content/33/7/1473
Permissions: Requests for permissions to reproduce figures, tables, or portions of articles originally published in
Arteriosclerosis, Thrombosis, and Vascular Biology can be obtained via RightsLink, a service of the Copyright
Clearance Center, not the Editorial Office. Once the online version of the published article for which permission is
being requested is located, click Request Permissions in the middle column of the Web page under Services.
Further information about this process is available in the Permissions and Rights Question and Answerdocument.
Reprints: Information about reprints can be found online at:
http://www.lww.com/reprints
Subscriptions: Information about subscribing to Arteriosclerosis, Thrombosis, and Vascular Biology is online at:
http://atvb.ahajournals.org//subscriptions/
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Topnotch Radiology For Moonlighters - Sept 2019Document72 pagesTopnotch Radiology For Moonlighters - Sept 2019Cara Marrero IguidNo ratings yet
- Test Bank For Nursing Assistant A Nursing Process Approach 11th EditionDocument7 pagesTest Bank For Nursing Assistant A Nursing Process Approach 11th EditionLarry Cessor100% (26)
- First Aid QuizDocument5 pagesFirst Aid QuizIan AriNo ratings yet
- c17 Microbiology Tortora TestbankDocument18 pagesc17 Microbiology Tortora Testbankwhitewave25No ratings yet
- Psoriasis: A Comprehensive Review: Nternational Ournal OF Harmacy & IFE CiencesDocument21 pagesPsoriasis: A Comprehensive Review: Nternational Ournal OF Harmacy & IFE Ciences24hintheghettoworkoutNo ratings yet
- Dental Caries IndexDocument35 pagesDental Caries Indexdr parveen bathla100% (1)
- C-Section Case StudyDocument4 pagesC-Section Case StudyChin Villanueva Ulam0% (1)
- Hemoglobin, Red Blood Cell Count, Hematocrit and Derived Parameters For Diagnosing Anemia in Elderly MalesDocument10 pagesHemoglobin, Red Blood Cell Count, Hematocrit and Derived Parameters For Diagnosing Anemia in Elderly Maleswinardi rNo ratings yet
- European Respiratory Society Guidelines For The Management of Adult BronchiectasisDocument23 pagesEuropean Respiratory Society Guidelines For The Management of Adult Bronchiectasiswinardi rNo ratings yet
- Stroke 2017Document4 pagesStroke 2017Jamie LittleNo ratings yet
- Diagnosis and Initial Treatment of Ischemic Stroke: Health Care GuidelineDocument71 pagesDiagnosis and Initial Treatment of Ischemic Stroke: Health Care GuidelineRosyid PrasetyoNo ratings yet
- STR 0000000000000069 FullDocument34 pagesSTR 0000000000000069 FullcignalNo ratings yet
- 1Document27 pages1Nada ApriliaNo ratings yet
- Typhoid FeverDocument6 pagesTyphoid FeverReeshabhdev GauttamNo ratings yet
- Respiratory Chest PainDocument16 pagesRespiratory Chest Painwinardi rNo ratings yet
- PneumoniaDocument9 pagesPneumoniawinardi rNo ratings yet
- Global TB Report 2017Document262 pagesGlobal TB Report 2017doc_next_doorNo ratings yet
- 1Document27 pages1Nada ApriliaNo ratings yet
- Smoking and Periodontal DiseaseDocument7 pagesSmoking and Periodontal DiseaseIgnaciaPerotNo ratings yet
- 03 Pathophysiology of CommunityDocument3 pages03 Pathophysiology of CommunityVenerandaNo ratings yet
- Respiratory Chest PainDocument16 pagesRespiratory Chest Painwinardi rNo ratings yet
- Int. J. Epidemiol. 2009 Cornfield 1175 91Document17 pagesInt. J. Epidemiol. 2009 Cornfield 1175 91winardi rNo ratings yet
- The Darkside of NeuroplasticityDocument19 pagesThe Darkside of Neuroplasticitywinardi rNo ratings yet
- Proposal IMO 2016Document38 pagesProposal IMO 2016winardi rNo ratings yet
- Tension Type HeadacheDocument9 pagesTension Type Headachewinardi rNo ratings yet
- ChapmanDocument62 pagesChapmanraspatiNo ratings yet
- Thorax 2001 Qvarfordt 445 9Document6 pagesThorax 2001 Qvarfordt 445 9winardi rNo ratings yet
- The Effect of Reducing The Number of Cigarettes Smoked On Risk of LungDocument10 pagesThe Effect of Reducing The Number of Cigarettes Smoked On Risk of Lungwinardi rNo ratings yet
- ICHD IIR1finalDocument232 pagesICHD IIR1finalcrslazaNo ratings yet
- A Common Neurobiology For Pain PDFDocument7 pagesA Common Neurobiology For Pain PDFwinardi rNo ratings yet
- The Effect of Reducing The Number of Cigarettes Smoked On Risk of LungDocument10 pagesThe Effect of Reducing The Number of Cigarettes Smoked On Risk of Lungwinardi rNo ratings yet
- Circulation 2004 Aug 110 (5) 588-636Document1 pageCirculation 2004 Aug 110 (5) 588-636winardi rNo ratings yet
- RHD PDFDocument16 pagesRHD PDFwhy1328No ratings yet
- Overlap Between Brugada Syndrome and Arrhytmogenic RVDocument4 pagesOverlap Between Brugada Syndrome and Arrhytmogenic RVwinardi rNo ratings yet
- Overlap Between Brugada Syndrome and Arrhytmogenic RVDocument6 pagesOverlap Between Brugada Syndrome and Arrhytmogenic RVwinardi rNo ratings yet
- Difficulty in SwallowingDocument1 pageDifficulty in SwallowingmawelNo ratings yet
- Surgical Site MarkingDocument12 pagesSurgical Site Markingh1m4w4nNo ratings yet
- Approach To Floppy InfantDocument44 pagesApproach To Floppy InfantNavya Hegde100% (2)
- AERGDocument12 pagesAERGsupaidi97No ratings yet
- Name: Insong, Osannah Irish B. Section: BSMT 3CDocument1 pageName: Insong, Osannah Irish B. Section: BSMT 3COsannah Irish InsongNo ratings yet
- Programmed Postoperative Physiotherapy May Improve Functional Outcomes in Pneumonectomy Patients of Rare Causes Case SeriesDocument7 pagesProgrammed Postoperative Physiotherapy May Improve Functional Outcomes in Pneumonectomy Patients of Rare Causes Case SeriesAtu KaushalNo ratings yet
- Suspected Preeclampsia AlgorithmDocument1 pageSuspected Preeclampsia Algorithmmisstina.19876007100% (1)
- Parafin Sept 2011Document28 pagesParafin Sept 2011Sarin AvniNo ratings yet
- 0 Small FoundationsDocument9 pages0 Small FoundationsFrancesc Xavier Bofill De RosNo ratings yet
- ParkinsonDocument12 pagesParkinsonStephanie NieNo ratings yet
- Abortion Using Misoprostol Pills: Before SmaDocument1 pageAbortion Using Misoprostol Pills: Before SmaAhmad Shah SyedNo ratings yet
- Therapeutic Interventions in Vascular MalformationsDocument47 pagesTherapeutic Interventions in Vascular MalformationsDr KhanNo ratings yet
- Antimicrobial Resistance Trends in Bacterial Keratitis Over 5 Years in Sydney, AustraliaDocument9 pagesAntimicrobial Resistance Trends in Bacterial Keratitis Over 5 Years in Sydney, AustraliaBima RizkiNo ratings yet
- Within A Year, Nusantics Has Evolved To Be A Key Shaper of Future Health-Biotechnology in IndonesiaDocument23 pagesWithin A Year, Nusantics Has Evolved To Be A Key Shaper of Future Health-Biotechnology in IndonesiaGatot SubagyoNo ratings yet
- 1 Acknowledgement 2 2 3 3 Signs and Symptoms 4 4 Pathophysiology 5 5 Real Cases A-Patient History B - Physical Examination 6-9Document22 pages1 Acknowledgement 2 2 3 3 Signs and Symptoms 4 4 Pathophysiology 5 5 Real Cases A-Patient History B - Physical Examination 6-9radicalmpNo ratings yet
- Types of AnaesthesiaDocument1 pageTypes of AnaesthesiaElaine BriososNo ratings yet
- Step Up To Medicine Chapter 03Document868 pagesStep Up To Medicine Chapter 03yanks1120No ratings yet
- Malpractice CaseDocument4 pagesMalpractice CaseAr-jay JubaneNo ratings yet
- Unit 6: Resistance of The Body To Infection: II. Immunity and AllergyDocument34 pagesUnit 6: Resistance of The Body To Infection: II. Immunity and AllergyEsteban Tabares GonzalezNo ratings yet
- Efficacy of Unani Formulation in Infertility Among Obese Women: A Clinical StudyDocument10 pagesEfficacy of Unani Formulation in Infertility Among Obese Women: A Clinical StudyWaseem AhmedNo ratings yet
- Health - Very Very Important Tips: WaterDocument8 pagesHealth - Very Very Important Tips: WaterLohidas PailaNo ratings yet
- 7 Physiotherapy in PeriodontologyDocument31 pages7 Physiotherapy in PeriodontologyXulkanain ZE100% (1)
- 2020-68 Annex B - Health Declaration Form110320Document4 pages2020-68 Annex B - Health Declaration Form110320Aileen MayaNo ratings yet
- SOCT Copernicus: OPTOPOL Technology S.ADocument4 pagesSOCT Copernicus: OPTOPOL Technology S.AakhterNo ratings yet