Professional Documents
Culture Documents
Laparoscope
Uploaded by
dharmaCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Laparoscope
Uploaded by
dharmaCopyright:
Available Formats
5
The Role of Laparoscopy in the
Management of End-Stage Renal Disease
Patients in Peritoneal Dialysis
Rui Maio
Universidade de Lisboa
Portugal
1. Introduction
Continuous ambulatory peritoneal dialysis (CAPD) is an established and well-known
technique for renal replacement therapy in patients with end-stage renal disease (1,2). Since
the introduction of CAPD, four methods have been advocated for the placement of PD
catheters: open surgery, percutaneous, peritoneoscopic (Y-Tec; Medigroup, Oswego, Illinois,
USA), and laparoscopic placement (2,3,13,17).
The manner in which PD catheters are placed has a significant influence on catheter
function, incidence of catheter-related complications, and technique survival (6). Open
surgery and especially the percutaneous technique are associated with poor outcomes and
sometimes life-threatening complications (20,21). In fact, the incidence of omental wrapping,
catheter displacement, and intraabdominal complications, specifically bowel and bladder
perforation, is higher with these two methods. In recent years, there has been considerable
interest in the use of laparoscopy for creation of peritoneal access. Laparoscopic peritoneal
catheter placement is simple, quick, efficient, and minimally invasive. As with any new
application of a modality, laparoscopy for peritoneal access is still undergoing procedurespecific adaptation. The strength of laparoscopy is that it allows an opportunity to visibly
address problems that adversely effect catheter outcome, namely, catheter tip migration,
omental entrapment, and peritoneal adhesions. Identifying and preemptively correcting
these problems at the time of the implantation procedure are the advantages of surgical
laparoscopy over other catheter insertion techniques (7,8).
Regardless of the technique utilized to implant the PD catheter, there are best-demonstrated
practices that should be followed in every case (4,5). Adherence to these recognized
practices could reduce the risk of catheter tip migration, pericatheter leakage, hernias,
superficial cuff extrusion, and catheter-related infections.
2. Laparoscopic placement of Tenckhoff catheters: A safe, effective, and
reproducible procedure
Our catheter implantation technique will be described in detail (14,15,16).
The same team operated on all patients. The laparoscopic procedures were performed in the
operating room under general anesthesia. A prophylactic antibiotic, cefazolin or
vancomycin in the event of cephalosporin allergy was administered prior to the
www.intechopen.com
76
Laparoscopy An Interdisciplinary Approach
procedure. A Veress needle was inserted into the peritoneal cavity through a stab incision in
the right hypochondrium to create a pneumoperitoneum. Pressure limits for abdominal gas
insufflation were set between 10 and 12 mmHg. The Veress needle was replaced with a 10mm port and preliminary laparoscopy was performed to look for adhesions or other
anatomical abnormalities that could hinder performance of the Tenckhoff catheter. A 5-mm
port was inserted under direct vision in the right iliac fossa. A 1-cm skin incision was made
on the left, 2 3 cm lateral and inferior to the umbilicus, and a second 5-mm port was placed
in a paramedian location and tunneled in a caudal direction through the rectus sheath for a
distance of at least 4 cm before entry was made into the peritoneal cavity. We aligned both
5-mm ports and inserted the Endograsp (United States Surgical, Norwalk, Connecticut,
USA) through the lower right quadrant port and brought it out through the paramedian
port. The paramedian port was then removed but the tip of the Endograsp remained outside
the abdominal cavity (Figures 1 and 2). The intraperitoneal portion of the Tenckhoff catheter
tip was caught with the grasper and slowly pulled inside the peritoneal cavity through the
tunnel created in the abdominal wall (Figure 3). The deep cuff was located at the medial
edge of the muscle within the rectus sheath. The intra-abdominal portion of the catheter was
placed between the visceral and parietal peritoneum toward the pouch of Douglas. The
subcutaneous tunnel tract and skin exit site were directed downwards or laterally. The
subcutaneous cuff was positioned at a distance of at least 2 cm from the exit wound.
Between each of the preceding steps, catheter patency was checked to ensure that there was
adequate inflow and outflow without leakage. The entire procedure was done under direct
vision. The laparoscope was then removed and the pneumoperitoneum was allowed to
deflate. The fascia of the laparoscopic port site was closed with 2-0 polyglactin suture. Skin
wounds were sutured with 3-0 nylon. The protocol for catheter irrigation consisted of a
daily in-and-out flush with dialysate solution. Peritoneal dialysis was generally delayed for
a minimum of 2 weeks to allow complete wound healing.
Since January 2002, the author performed more then 400 laparoscopic placement of
Tenckhoff peritoneal catheter in patients with end-stage renal diseases.
The average operative time was 15 4 minutes and mean duration of hospital stay was 1
day. There were no conversions from laparoscopy to any other conventional method of
catheter placement. In patients with intraperitoneal adhesions, laparoscopic adhesiolysis
was performed to eliminate intraperitoneal loculations that might interfere with the
peritoneal catheter drainage function.
No infections of the exit site or subcutaneous tunnel, hemorrhagic complications, abdominal
wall hernias, or extrusion of the superficial catheter cuff were detected.
No mortality occurred in this series of patients. Catheter survival was 97%, 95%, and 91% at
1, 2, and 3 years, respectively (Figure 4).
Peritoneal catheter placement must be regarded as an important surgical intervention,
demanding care and attention to detail equal to that of any other surgical procedure and as
a consequence a competent and experienced operator must perform the catheter
implantation procedure.
Due to its characteristics (simple, quick, efficient, and minimally invasive to the patient), it
seems that laparoscopic peritoneal catheter placement should become the preferred
approach. In addition, the laparoscopic method offers an excellent view of the abdomen and
optimal placement of the catheter within the cavity. The single blind step is the Veress
needle insertion; however, the probability of damaging the abdominal organs or epigastric
and retroperitoneal blood vessels is very low.
www.intechopen.com
The Role of Laparoscopy in the Management
of End-Stage Renal Disease Patients in Peritoneal Dialysis
77
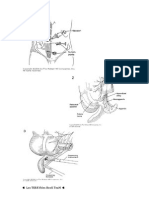
Fig. 1. Operative photograph demonstrates the alignment of the two 5-mm ports and
insertion of the grasping forceps.
Fig. 2. Operative photograph shows that the tunneled5-mm port has been removed and the
dialysis catheter has been grasped in preparation of pulling it into the peritoneal cavity.
www.intechopen.com
78
Laparoscopy An Interdisciplinary Approach
This method is particularly useful in patients that have already undergone previous
abdominal operations (8). Patients with peritoneal adhesions that might interfere with
drainage function can be treated with adhesiolysis and displaced catheters can be
repositioned.
In addition, laparoscopy is useful for the diagnosis and treatment of abdominal wall hernias
and peritoneo vaginal canal persistence.
Another advantage of laparoscopy is the possibility of performing a selective prophylactic
omentopexy, a technique that has been separately described by Ogunc and Crabtree (10,11).
In conjunction with rectus sheath tunneling and adhesiolysis, it is possible that selective use
of omentopexy could have prevented the omental obstruction and the need for revisionary
surgery that occurred in 6 of our patients.
Some centers use laparoscopic insertion with local anesthesia on the assumption that it is
safer (12). We suggest that modern general anesthesia is safe for the vast majority of patients
and allows a better view of the peritoneal cavity. Different techniques have been described
for the placement of peritoneal catheters by laparoscopy using specially designed devices.
The distinctive characteristic of our technique is that we used nothing more than
conventional laparoscopic equipment available in any facility that routinely performs
laparoscopic surgery. Laparoscopy is a commonly performed procedure in general practice
but it also has an inherently steep learning curve. A junior surgeon, under close supervision
of a consultant, performed some of the later procedures without technical difficulties.
Fig. 3. Operative photograph shows the catheter tip pulled inside the peritoneum through
the tunnel created in the abdominal wall.
www.intechopen.com
The Role of Laparoscopy in the Management
of End-Stage Renal Disease Patients in Peritoneal Dialysis
79
Time to catheter dysfunction
Survival
Function
1,0
Censored
Cum Survival
0,8
0,6
0,4
0,2
0,0
0,00
10,00
20,00
30,00
40,00
50,00
60,00
Months
Fig. 4. Cumulative probability of peritoneal dialysis catheter survival following laparoscopic
placement. The ticks on the survival curve represent censored data points.
Abdominal wall leaks, our major complication occurred at the beginning of our experience.
At that time, the length of the musculofascial tunnel was shorter and in our opinion resulted
in a higher incidence of leaks. Successful management of these leaks consisted of delaying
the beginning of dialysis.
We did not experience intraoperative complications such as intra-abdominal organ injury,
as has been reported for conventional techniques. In fact, in our series we had no intraabdominal catastrophes and the incidence of catheter displacement was lower than that
reported using open surgery technique. Furthermore, we did not encounter problems
commonly reported for open catheter placement, such as hematoma, seroma, or infections.
No perioperative mortality occurred in this case series. Our long-term catheter survival
exceeds the targets recommended by published guidelines and is higher than most reported
experiences.
3. Abdominal adhesions
Despite widespread acceptance of peritoneal dialysis, patients with previous history of
abdominal operations are frequently excluded from consideration.
www.intechopen.com
80
Laparoscopy An Interdisciplinary Approach
Abdominal surgery can lead to the formation of adhesions. Adhesive scarring within the
peritoneal space can complicate catheter placement. Compartmentalization of the peritoneal
cavity by adhesions can impede insertion of the catheter, produce kinking or malpositioning
of the tubing, block the side drainage holes resulting in flow dysfunction, and limit the
available dialyzable space. It is not unreasonable to surmise that intraperitoneal adhesions
would not only increase the difficulty and risk of catheter insertion but also adversely affect
catheter survival.
Peritoneal adhesions have been reported to form after 70-90% of abdominal operations.
Catheter implantation using conventional approaches in patients with intra-abdominal
adhesions has been associated with an increased incidence of postoperative complications.
In the presence of adhesions, catheter insertion can be complicated by visceral injury,
hemorrhage and catheter malposition with flow dysfunction. Visualization of peritoneal
cavity during implantation of PD catheters using laparoscopic methods can determine the
presence and extent of intra-abdominal adhesions and help direct the placement of
catheters. Patients with peritoneal adhesions that might interfere with drainage function can
be treated with adhesiolysis and displaced catheters can be repositioned. Therefore this
method is particularly useful in patients that have already undergone previous abdominal
operations.
4. Omental wrap
Omental wrap is a common cause of catheter obstruction. The mechanism of omental wrap
is uncertain. A redundant omentum can adhere to the distal end of the catheter and displace
it out of the pelvis. A catheter that has migrated out of the pelvis is at risk of being wrapped
by the omentum. Catheter displacement as seen on plain abdominal radiograph could in
fact be omental wrap.
Laparoscopic intervention is an effective treatment for omental wrap. The tiny projections of
the omentum insinuate through the side holes of the catheter and obstruct its lumen. On
close-up view, the omental fat forms a dumb-bell shaped plug in the side hole. The plug is
snug and firm. While the catheter is being steadied by laparoscopic graspers, the omental
plugs have to be pulled in the right direction to be released. A less precise manoeuvre, such
as pulling the catheter away from the omentum, is unlikely to free the catheter entirely, and
bleeding might occur as the omental plugs together with the small vessels supplying them
are avulsed. This can happen in fluoroscopic stiff-wire manipulation, since the movement
involved is similar. Reports of stiff wire manipulation under fluoroscopic guidance showed
a high incidence of recurrent malfunction and the need for repeat manipulation.
Omental wrap remains one of the likely reasons for failure of non-laparoscopic treatments.
In one study, 50% of the patients who had undergone unsuccessful fluoroscopic wire
manipulation were found to have omental wrap at laparoscopic salvage. One definitive
laparoscopic procedure is likely to be more effective than multiple wire manipulations. For
recurrent catheter migration or malfunction, laparoscopy should be the next step. Open
removal and replacement of catheter risks recurrent malfunction since the cause of
malfunction has not been resolved.
Laparoscopy provides visual diagnosis of the cause of catheter malfunction and when used
as first-line management, has shown high success rates.
A procedure on the greater omentum appears important in preventing catheter malfunction.
A low rate of obstruction has been demonstrated by series of primary open insertion of
www.intechopen.com
The Role of Laparoscopy in the Management
of End-Stage Renal Disease Patients in Peritoneal Dialysis
81
catheter where prophylactic omentopexy or subtotal omentectomy had been performed.
Crabtree and Fishman reported an obstruction rate of only 0.7% in 153 patients when selective
prophylactic omentopexy during laparoscopic implantation of catheter was performed.
Reports of laparoscopic salvage have found an incidence of omental wrap ranging from 57 to
92%. The incidence of obstruction causing poor flow of dialysate is 6.0 to 20.5%. Occlusion by
the greater omentum is therefore an important etiology of catheter malfunction. Current
laparoscopic techniques for salvaging catheters include simple repositioning with or without
catheter fixation, omentopexy, omentectomy and omental folding.
Omentopexy is a laparoscopically enabled procedure shown to be of value in preventing
omental entrapment. Ogunc recommended it for all implantation procedures whereas
Crabtree et al used it selectively when redundant omentum was found to extend to the deep
pelvis in the vicinity of the catheter tip. In Ogunc' s Technique which is minilaparoscopic
extraperitoneal tunelling with omentopexy, the lateral inferior edges of the omentum are
fixed onto the parietal peritoneum of the lateral abdominal wall at two points with a 3-0
polypropylene suture with 2 mm needle holder at the level of the umbilicus (18). If the
omentum is large or bulky, one more fixation suture is applied between the middle inferior
edge of the omentum and the falciform ligament. There was no complication related to the
small bowel volvulus, internal herniation and the other mechanical outflow obstruction in
44 consecutive patients.
In contrast to omentopexy, which fixes the omentum to the anterior or lateral abdominal
wall, or to the falciform ligament, omental folding fixes the omentum to itself. Omental
folding creates a safe distance between the catheter and the omentum by shortening the
latter. Technically, omental folding is a form of omentopexy. The other effect of folding is
that the distal omentum with its slender projections is converted into a rounded edge.
Omental folding can thus be performed with the most basic laparoscopic equipment found
in most surgical units. With practice, the folding of the omentum can be performed within
10 minutes and the whole salvage procedure can take less than 40 minutes and is a safe and
effective technique for salvaging PD catheters (19).
5. Conclusions
A laparoscopic approach for placing Tenckhoff catheters can be accomplished with
complete compliance to recommended best practices for PD access. Moreover, laparoscopy
permits advantages over conventional implantation techniques through the use of
adjunctive procedures such as rectus sheath tunneling to prevent catheter tip migration,
adhesiolysis to assure adequate dialysate drainage function of the catheter, and
omentopexy, omentectomy or omental folding to prevent omental wrapping. The catheter
implantation method described in this chapter uses standard laparoscopic equipment and
techniques completely familiar to any surgeon who routinely performs laparoscopic
surgery. The procedure can be performed with low risks of morbidity and mortality. The
patient benefits from a minimally invasive approach and the assurance of obtaining
successful long-term catheter function. The results reported here support our opinion that
laparoscopic Tenckhoff catheter implantation should become the standard of care for clinical
practice.
6. References
[1] Gokal R. CAPD overview. Perit Dial Int 1996; 16(Suppl 1):1318.
www.intechopen.com
82
Laparoscopy An Interdisciplinary Approach
[2] Cruz C. Implantation techniques for peritoneal dialysis catheters. Perit Dial Int 1996;
16(Suppl 1):31921.
[3] Gokal R, Alexander S, Ash SR, Chen TW, Danielson A, Holmes C, et al. Peritoneal
catheters and exit-site practices toward optimum peritoneal access: 1998 update.
Perit Dial Int 1998; 18:1133.
[4] Dombros N, Dratwa M, Feriani M, Gokal R, Heimburger O, Krediet R, et al.; EBPGExpert Group on Peritoneal Dialysis. European best practice guidelines for
peritoneal dialysis. . Nephrol Dial Transplant 2005; 20:ix812.
[5] Lund L. Per itoneal dialysis catheter placement: is laparoscopy an option? Int Urol
Nephrol 2007; 39:6258.
[6] Asif A. Peritoneal dialysis catheter insertion. Minerva Chir 2005; 60:41728.
[7] Adamson AS. Endoscopic placement of CAPD catheters: an overview of one hundred
procedures. Nephrol Dial Transplant 1992; 7:8557.
[8] Brandt CP. Laparoscopic placement of peritoneal dialysis catheters in patients who have
undergone prior abdominal operations. J Am Coll Surg 1994; 178:51516.
[9] Kimmelstiel FM. Laparoscopic management of peritoneal dialysis catheters. Surg
Gynecol Obstet 1993; 176:56570.
[10] Ogunc G. Videolaparoscopy with omentopexy: a new technique to allow placement
of a catheter for continuous ambulatory peritoneal dialysis. Surg Today 2001; 31:
9424.
[11] Crabtree JH, Fishman A. Selective performance of prophylactic omentopexy during
laparoscopic implantation of peritoneal dialysis catheters. Surg Laparosc Endosc
Percutan Tech 2003; 13:1804.
[12] Crabtree JH. Laparoscopic approach under local anesthesia for peritoneal dialysis
access. Perit Dial Int 2000; 20: 75765.
[13] Cala Z. Laparoscopic placement of the peritoneal dialysis catheter using a specially
designed trocar: a review of 84 patients. Dial Transplant 2000; 11:722 7.
[14] Maio R. Colocao de cateteres de dilise peritoneal. Mtodo cirrgicovantagens e
inconvenientes. III curso ps-graduado de dilise peritoneal. Lisboa; 2005.
[15] Maio R. Laparoscopic placement of peritoneal dialysis cathetersingle centre
experience. 7th European Peritoneal Dialysis Meeting; October 1518, 2005; Prague,
Czech Republic.
[16] Maio et al. Laparoscopic placement of Tenckhoff catheters for peritoneal dialysis: a
safe, effective and reproducible procedure. Perit Dial Int 2008; 28:170-3.
[17] Poole et al. Laparoscopic Tenckhoff catheter insertion: a prospective study of a new
technique. Aust NZ J Surg 2000; 70:371-3.
[18] Ogunc. Minilaparoscopic extraperitoneal tunneling with omentopexy: a new technique
for CAPD catheter placement. Perit Dial Int 2005; 25:551-5.
[19] Comert et al. A new laparoscopic technique for the placement of a permanent
peritoneal dialysis catheter: the preperitoneal tunneling method. Surg Endosc 2005;
19:245-248.
[20] Soontrapornchai et al. Comparison of open and laparoscopic secure placement of
peritoneal dialysis catheters. Surg Endosc 2005; 19:137-9.
[21] Jwo SC et al. Prospective randomized study for comparison of open surgery with
laparoscopic-assisted placement of Tenckhoff peritoneal dialysis catheter--a single
center experience and literature review. J Surg Res. 2010 Mar;159(1):489-96. Epub
2008 Oct 9
www.intechopen.com
Laparoscopy - An Interdisciplinary Approach
Edited by Dr. Ivo Meinhold-Heerlein
ISBN 978-953-307-299-9
Hard cover, 146 pages
Publisher InTech
Published online 12, September, 2011
Published in print edition September, 2011
Over the last decades an enormous amount of technical advances was achieved in the field of laparoscopy.
Many surgeons with surgical, urological, or gynaecological background have contributed to the improvement of
this surgical approach which today has an important and fixed place in the daily routine. It is therefore
comprehensible to compose a book entitled laparoscopy serving as a reference book for all three disciplines.
Experts of each field have written informative chapters which give practical information about certain
procedures, indication of surgery, complications and postoperative outcome. Wherever necessary, the
appropriate chapter is illustrated by drawings or photographs. This book is advisable for both beginner and
advanced surgeon and should find its place in the libraries of all specialties surgery, urology, and
gynecology.
How to reference
In order to correctly reference this scholarly work, feel free to copy and paste the following:
Rui Maio (2011). The Role of Laparoscopy in the Management of End-Stage Renal Disease Patients in
Peritoneal Dialysis, Laparoscopy - An Interdisciplinary Approach, Dr. Ivo Meinhold-Heerlein (Ed.), ISBN: 978953-307-299-9, InTech, Available from: http://www.intechopen.com/books/laparoscopy-an-interdisciplinaryapproach/the-role-of-laparoscopy-in-the-management-of-end-stage-renal-disease-patients-in-peritonealdialysis
InTech Europe
University Campus STeP Ri
Slavka Krautzeka 83/A
51000 Rijeka, Croatia
Phone: +385 (51) 770 447
Fax: +385 (51) 686 166
www.intechopen.com
InTech China
Unit 405, Office Block, Hotel Equatorial Shanghai
No.65, Yan An Road (West), Shanghai, 200040, China
Phone: +86-21-62489820
Fax: +86-21-62489821
You might also like
- Biliopancreatic Endoscopy: Practical ApplicationFrom EverandBiliopancreatic Endoscopy: Practical ApplicationKwok-Hung LaiNo ratings yet
- Sotelo Et Al, Laparoscopic Rectovesical Fistula RepairDocument5 pagesSotelo Et Al, Laparoscopic Rectovesical Fistula RepairjordynixnNo ratings yet
- Use Only: Intracorporeal Hybrid Single Port Conventional Laparoscopic Appendectomy in ChildrenDocument4 pagesUse Only: Intracorporeal Hybrid Single Port Conventional Laparoscopic Appendectomy in ChildrenYelisa PatandiananNo ratings yet
- Urushihara 10.1007 s00383-015-3779-8Document4 pagesUrushihara 10.1007 s00383-015-3779-8CherNo ratings yet
- Nephrectomy ProcedureDocument4 pagesNephrectomy ProcedureRon Java FantillanNo ratings yet
- ANew Guidewire Cannulation TechniDocument7 pagesANew Guidewire Cannulation TechniJorge CisnerosNo ratings yet
- Laparoscopic Surgery in Gynaecologic OncologyDocument7 pagesLaparoscopic Surgery in Gynaecologic OncologyManan BoobNo ratings yet
- Management of Anastomotic Leaks After Esophagectomy and Gastric Pull-UpDocument9 pagesManagement of Anastomotic Leaks After Esophagectomy and Gastric Pull-UpSergio Sitta TarquiniNo ratings yet
- Surgical Endoscopy Oct.1997Document87 pagesSurgical Endoscopy Oct.1997Saibo BoldsaikhanNo ratings yet
- Omentum OverlayDocument10 pagesOmentum OverlayAlin MihetiuNo ratings yet
- 2021 Techniques of Esophageal Anastomosis For EsophagectomyDocument14 pages2021 Techniques of Esophageal Anastomosis For EsophagectomyykommNo ratings yet
- 2014 172 0 Retroperitoneal and Retrograde Total Laparoscopic Hysterectomy As A Standard Treatment in A Community Hospital 97 101 1Document5 pages2014 172 0 Retroperitoneal and Retrograde Total Laparoscopic Hysterectomy As A Standard Treatment in A Community Hospital 97 101 1Sarah MuharomahNo ratings yet
- Pi Is 2213576614000049Document3 pagesPi Is 2213576614000049Ditha FadhilaNo ratings yet
- 2019 Simplified Minimally Invasive Surgical Approach For Prophylactic Laparoscopic Gastropexy in 21 CasesDocument8 pages2019 Simplified Minimally Invasive Surgical Approach For Prophylactic Laparoscopic Gastropexy in 21 CasesrizalakbarsyaNo ratings yet
- Retroperitoneal HeminephrectomyDocument4 pagesRetroperitoneal HeminephrectomyIoannis ValioulisNo ratings yet
- Cistectomia Radical Art08 PDFDocument7 pagesCistectomia Radical Art08 PDFJoshua GardnerNo ratings yet
- DAnnibale2004 Article RoboticAndLaparoscopicSurgeryFDocument7 pagesDAnnibale2004 Article RoboticAndLaparoscopicSurgeryFWarren SeowNo ratings yet
- Laparoscopic Entry TechniquesDocument9 pagesLaparoscopic Entry TechniquesDougNo ratings yet
- McKeown EsophagectomyDocument9 pagesMcKeown EsophagectomyDa JunNo ratings yet
- Main PDFDocument4 pagesMain PDFhhNo ratings yet
- Laparoscopic Repair of Vesicovaginal FistulaDocument4 pagesLaparoscopic Repair of Vesicovaginal FistulaGloria AteNo ratings yet
- Surgical Endoscopy 6Document102 pagesSurgical Endoscopy 6Saibo BoldsaikhanNo ratings yet
- Component SeparationDocument23 pagesComponent Separationismu100% (1)
- Actas Urológicas EspañolasDocument4 pagesActas Urológicas EspañolasTrahmono SrNo ratings yet
- Open Versus Laparoscopic Mesh Repair of Ventral Hernias: A Prospective StudyDocument3 pagesOpen Versus Laparoscopic Mesh Repair of Ventral Hernias: A Prospective Study'Adil MuhammadNo ratings yet
- Carlucci2020 Article MinimalInvasiveSurgeryOfTheDis PDFDocument9 pagesCarlucci2020 Article MinimalInvasiveSurgeryOfTheDis PDFrickysuryamin4745No ratings yet
- Robotic-Assisted Laparoscopic Radical Cystectomy With Extracorporeal Urinary Diversion: Initial ExperienceDocument11 pagesRobotic-Assisted Laparoscopic Radical Cystectomy With Extracorporeal Urinary Diversion: Initial ExperiencesandyrraoNo ratings yet
- S0090429521002594Document7 pagesS0090429521002594Mounia MarsouNo ratings yet
- Treatmen 3Document6 pagesTreatmen 3Livia GudacNo ratings yet
- RectopexyDocument7 pagesRectopexyInzamam Ul HaqNo ratings yet
- Ciencia e Technica Omentum Overlay PDFDocument10 pagesCiencia e Technica Omentum Overlay PDFAlin MihetiuNo ratings yet
- Jurnal 1 PDFDocument5 pagesJurnal 1 PDFsabila_chaNo ratings yet
- Wind2007 PDFDocument5 pagesWind2007 PDFanatolioNo ratings yet
- Williams2013 Article LaparoscopicManagementOfHighTrDocument3 pagesWilliams2013 Article LaparoscopicManagementOfHighTrVishnu priya kokkulaNo ratings yet
- Surgery Insight: Natural Orifice Transluminal Endoscopic Surgery - An Analysis of Work To DateDocument12 pagesSurgery Insight: Natural Orifice Transluminal Endoscopic Surgery - An Analysis of Work To Datedocramanujam@rediffmailNo ratings yet
- Blumgart Anastomosis For Pancreaticojejunostomy Minimizes Severe Complications After Pancreatic Head ResectionDocument10 pagesBlumgart Anastomosis For Pancreaticojejunostomy Minimizes Severe Complications After Pancreatic Head ResectionRegina UgarteNo ratings yet
- Editorial What Is The Best Endoscopic Treatment For Pancreatic PseudocystDocument4 pagesEditorial What Is The Best Endoscopic Treatment For Pancreatic PseudocystLogical MonsterNo ratings yet
- Laparoscopic Repair of Inguinal HerniaDocument12 pagesLaparoscopic Repair of Inguinal Herniawadhe omara100% (1)
- Laparoscopic Common Bile Duct ExplorationDocument2 pagesLaparoscopic Common Bile Duct ExplorationmhmmdfaizalNo ratings yet
- Laparoscopic Orchidopexy: Current Surgical Opinion.: AbstractDocument6 pagesLaparoscopic Orchidopexy: Current Surgical Opinion.: AbstractGemiNo ratings yet
- Combined Laparoscopic Pyelolithotomy and Endoscopic Pyelolithotripsy For Staghorn Calculi: Long-Term Follow-Up Results From A Case SeriesDocument6 pagesCombined Laparoscopic Pyelolithotomy and Endoscopic Pyelolithotripsy For Staghorn Calculi: Long-Term Follow-Up Results From A Case SeriesantonNo ratings yet
- Review StrikturDocument13 pagesReview StrikturFryda 'buona' YantiNo ratings yet
- Trans-Fistulary Endoscopic Drainage For Post-Bariatric Abdominal Collections Communicating With The Upper Gastrointestinal TractDocument8 pagesTrans-Fistulary Endoscopic Drainage For Post-Bariatric Abdominal Collections Communicating With The Upper Gastrointestinal TractAlexandra JichituNo ratings yet
- Colecistectomía Laparoscópica Transumbilical: Una Técnica ReproducibleDocument4 pagesColecistectomía Laparoscópica Transumbilical: Una Técnica ReproducibleKatherine Arapa ApazaNo ratings yet
- An Algorithm For The Management of Bile Leak Following Laparoscopic CholecystectomyDocument19 pagesAn Algorithm For The Management of Bile Leak Following Laparoscopic CholecystectomyJanuar RizkyNo ratings yet
- Anterior Abdominal Wall HerniaDocument8 pagesAnterior Abdominal Wall HerniaOttofianus Hewick KalangiNo ratings yet
- Jejunum Jurnal 3Document3 pagesJejunum Jurnal 3rofitaNo ratings yet
- Radical and PartialDocument8 pagesRadical and PartialLunaFiaNo ratings yet
- How I Do ItDocument13 pagesHow I Do ItvennyherlenapsNo ratings yet
- Img 0072Document1 pageImg 0072O'jays NavarroNo ratings yet
- Ruurda Et Al-2015-Journal of Surgical OncologyDocument9 pagesRuurda Et Al-2015-Journal of Surgical OncologyJohnny TeoNo ratings yet
- Los Terrybles Book TeamDocument6 pagesLos Terrybles Book TeamWildor Herrera GuevaraNo ratings yet
- Robotics and InfertilityDocument6 pagesRobotics and InfertilityConsultorio Ginecología y ObstetriciaNo ratings yet
- Total Laparoscopic HysterectomyDocument8 pagesTotal Laparoscopic HysterectomySamir CastilloNo ratings yet
- Proximal Hypospadias Repair With Bladder Mucosal Graft: Our 10 Years ExperienceDocument6 pagesProximal Hypospadias Repair With Bladder Mucosal Graft: Our 10 Years ExperienceLastri HillaryNo ratings yet
- Retrospective Study To Determine The Short-Term Outcomes of A Modified Pneumovesical Glenn-Anderson Procedure For Treating Primary Obstructing Megaureter. 2015Document6 pagesRetrospective Study To Determine The Short-Term Outcomes of A Modified Pneumovesical Glenn-Anderson Procedure For Treating Primary Obstructing Megaureter. 2015Paz MoncayoNo ratings yet
- Natural Orifice Transluminal Endoscopic SurgeryDocument11 pagesNatural Orifice Transluminal Endoscopic SurgeryMishel Rodriguez GuzmanNo ratings yet
- Pediatric Laparoscopic Inguinal Hernia Repair - A Review of Techniques - A SAGES Wiki ArticleDocument30 pagesPediatric Laparoscopic Inguinal Hernia Repair - A Review of Techniques - A SAGES Wiki ArticleAndri Feisal NasutionNo ratings yet
- Exp LapDocument9 pagesExp LapShreeja SajitNo ratings yet
- Pharmacodynamic & PharmacokineticDocument124 pagesPharmacodynamic & Pharmacokineticdharma100% (1)
- Bia Dan Lung CometDocument6 pagesBia Dan Lung CometdharmaNo ratings yet
- 25 (OH) D ActivatorDocument8 pages25 (OH) D ActivatordharmaNo ratings yet
- Safety ChecklistDocument8 pagesSafety ChecklistdharmaNo ratings yet
- Acs QualityDocument8 pagesAcs QualitydharmaNo ratings yet
- Timing RRT AkiDocument9 pagesTiming RRT AkidharmaNo ratings yet
- Current&TX DNDocument25 pagesCurrent&TX DNdharmaNo ratings yet
- Journal HyponatremiaDocument39 pagesJournal HyponatremiadharmaNo ratings yet
- Mba Final Project PresentationDocument34 pagesMba Final Project PresentationabijithNo ratings yet
- How To Bring Down High Creatinine LevelsDocument30 pagesHow To Bring Down High Creatinine Levelskavitha_vk76No ratings yet
- Dial YseDocument314 pagesDial YseSeda Muse KusNo ratings yet
- Risk Assessment Feb. 2 2017 PDFDocument34 pagesRisk Assessment Feb. 2 2017 PDFStephanie BadilloNo ratings yet
- Chronic Kidney Disease: Dr. Des Riyadi Anas, Sp. PD M. HashemyDocument43 pagesChronic Kidney Disease: Dr. Des Riyadi Anas, Sp. PD M. HashemyAris DaooNo ratings yet
- Studi Deskriptif Kualitas Hidup Pasien Penyakit Ginjal Kronik Yang Menjalani Hemodialisis Di Rumah Sakit Pku Muhammadiyah YogyakartaDocument8 pagesStudi Deskriptif Kualitas Hidup Pasien Penyakit Ginjal Kronik Yang Menjalani Hemodialisis Di Rumah Sakit Pku Muhammadiyah YogyakartaM PNo ratings yet
- Cellulitis Care PlanDocument6 pagesCellulitis Care PlanNaya Kayala0% (1)
- Changing: Your Partner ForDocument16 pagesChanging: Your Partner ForsunilNo ratings yet
- Adverse Effects of Hemodialysis On Kidney PatientsDocument30 pagesAdverse Effects of Hemodialysis On Kidney PatientsTania Alsyabilla aaNo ratings yet
- Jurnal Self Excercise (Hemodialisis)Document8 pagesJurnal Self Excercise (Hemodialisis)Sebut Saja MawarNo ratings yet
- KDIGO AKI Guideline DownloadDocument141 pagesKDIGO AKI Guideline DownloadSandi AuliaNo ratings yet
- HKCE BioDocument289 pagesHKCE BioKaito Magic100% (1)
- Intradialytic Hypotension: Arwedi ArwantoDocument17 pagesIntradialytic Hypotension: Arwedi ArwantopiusiNo ratings yet
- Brochure Diacap PolysulfoneenglDocument10 pagesBrochure Diacap PolysulfoneenglAchmad DainuriNo ratings yet
- Registered NurseDocument5 pagesRegistered Nurseapi-121390694No ratings yet
- PeritonitisDocument14 pagesPeritonitisaiya_sorayaNo ratings yet
- Development of PDDocument10 pagesDevelopment of PDNatik Bi Illah100% (1)
- HemodialysisDocument19 pagesHemodialysisK.R.Raguram88% (26)
- Fresenius Medical Care Renal Products CatalogDocument39 pagesFresenius Medical Care Renal Products CatalogLeonardo Jose HernandezNo ratings yet
- Dileesh.C Dialysis Technician Medical Allied Healthcare DHA Eligibility DHA/LS/1572017/731817 +971 54 302 2150Document4 pagesDileesh.C Dialysis Technician Medical Allied Healthcare DHA Eligibility DHA/LS/1572017/731817 +971 54 302 2150Gloria JaisonNo ratings yet
- 2008K@Home Technician's Manual, 490078 Revision E - November 22, 2017 PDFDocument53 pages2008K@Home Technician's Manual, 490078 Revision E - November 22, 2017 PDFIanculescu AlexNo ratings yet
- Pekan 1. Pleno Anatomi KlinisDocument62 pagesPekan 1. Pleno Anatomi KlinisasshyriaNo ratings yet
- End Stage Renal DiseaseDocument9 pagesEnd Stage Renal DiseaseShantanu DixitNo ratings yet
- Renal Psychology: Carolyn Evans, Sarah Cook, Joanne Taylor - Review Date Jan 2016Document5 pagesRenal Psychology: Carolyn Evans, Sarah Cook, Joanne Taylor - Review Date Jan 2016oanacrisNo ratings yet
- (Mebooksfree Net) Chr&kid&dis&dia&tre&yan&he&1st PDFDocument250 pages(Mebooksfree Net) Chr&kid&dis&dia&tre&yan&he&1st PDFmainoNo ratings yet
- DialysisDocument19 pagesDialysisSachin Singh100% (2)
- Acute Renal FailureDocument33 pagesAcute Renal FailureAqsa Akbar AliNo ratings yet
- Ijnrd 8 125Document13 pagesIjnrd 8 125Muhammad Halil GibranNo ratings yet
- Transportation in Animals and Plants Worksheet 7Document2 pagesTransportation in Animals and Plants Worksheet 7Parul ShahNo ratings yet
- BMSolutions PDFDocument48 pagesBMSolutions PDF曾hahaNo ratings yet
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)From EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Rating: 3 out of 5 stars3/5 (1)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (4)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 4 out of 5 stars4/5 (5)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 4.5 out of 5 stars4.5/5 (82)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (35)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (46)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (170)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeFrom EverandThe Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeRating: 4.5 out of 5 stars4.5/5 (2)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesFrom EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesRating: 4.5 out of 5 stars4.5/5 (1412)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (44)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisFrom EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisRating: 5 out of 5 stars5/5 (8)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- How to ADHD: The Ultimate Guide and Strategies for Productivity and Well-BeingFrom EverandHow to ADHD: The Ultimate Guide and Strategies for Productivity and Well-BeingRating: 1 out of 5 stars1/5 (2)
- To Explain the World: The Discovery of Modern ScienceFrom EverandTo Explain the World: The Discovery of Modern ScienceRating: 3.5 out of 5 stars3.5/5 (51)
- Self-Care for Autistic People: 100+ Ways to Recharge, De-Stress, and Unmask!From EverandSelf-Care for Autistic People: 100+ Ways to Recharge, De-Stress, and Unmask!Rating: 5 out of 5 stars5/5 (1)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- Critical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsFrom EverandCritical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsRating: 4.5 out of 5 stars4.5/5 (39)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (254)