Professional Documents
Culture Documents
Fetal & Maternal Energy Metabolism During Labor
Uploaded by
bellia loranthifoliaCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Fetal & Maternal Energy Metabolism During Labor
Uploaded by
bellia loranthifoliaCopyright:
Available Formats
Scheepers et al.
, Fetal and maternal metabolism during labor
457
Review article
J. Perinat. Med.
29 (2001) 457464
Fetal and maternal energy metabolism during labor in
relation to the available caloric substrate
H. C. J. Scheepers1, P. A. de Jong1, G. G. M. Essed2, and H. H. H. Kanhai3
1
Deptartment of Gynecology and Obstetrics, Leyenburg Hospital, The Hague,
of Gynecology and Obstetrics University Hospital Maastricht, and
3Department of Gynecology and Obstetrics Leiden University Medical Center,
Leiden, The Netherlands
2Deptartment
1 Introduction
During delivery, it is not unusual for women to
have little or no nutrient intake in spite of the fact
that the demand for energy increases for skeletal
and smooth muscle contractions. The question remains as to what the optimal policy in nutritional
intake during labor should be. The major reason
for restricting oral intake is the possible risk or
aspiration of gastric contents leading to the Mendelson syndrome. In many countries, a totally restrictive policy is adhered to [14, 31] although in
recent years, there is a tendency towards a more
liberal policy. The American Society of Anesthesiologists, stated in 1999 that, during normal labor, parturients should be allowed to drink clear
liquids and in Great Britain an increasing number
of institutes allow eating or drinking during labor
[5, 50].
Mortality figures due to the Mendelson syndrome
in The Netherlands, where oral intake is left to
the decision of laboring women are, comparable
to that of countries where a restrictive policy is
adhered to [47, 50]. Although many authors of
review articles conclude that the restriction of
eating and drinking during labor should be reconsidered [5, 29, 33, 52, 55], little evidence is recorded on the actual effects of eating and drinking on the course of labor [22].
Maternal and fetal metabolism during labor has
been studied, but studies on the relationship to the
availability of energetic substrate and metabolic
parameters are rare. The influence of intravenous
glucose administration on maternal and fetal metabolism has been studied, but the role of oral
caloric intake on metabolites remains relatively
unstudied. In this paper we discuss maternal and
fetal metabolic events during labor, the effects of
intravenous glucose administration and the possible role of oral caloric intake.
2 Maternal energy metabolism and acid
base balance
Energy demands can be met by different pathways [19]. The first is the use of ATP and creatinine phosphate, and the second, is the oxidative
pathway. This latter pathway is used when sufficient oxygen is available and glucose, glycogen,
triglycerids and amino acids can be used as fuel.
The third pathway is the non-oxidative pathway,
which is active when insufficient oxygen is available and in which lactate is produced. The oxidative pathway is used in prolonged moderate exercise and the non-oxidative pathway is important
for giving extra power.
During normal labor, maternal blood glucose increases [17, 23, 25, 26, 39, 58] which can be explained by the increased gluconeogenesis due to
cortisol and adrenaline, produced as a stress reaction [19]. In prolonged labor, however, a decrease
in maternal glucose levels has been described
[17]. The glucose turnover during labor, is mark-
2001 by Walter de Gruyter GmbH & Co. KG Berlin New York
Brought to you by | New York University Bobst Library Technical Services
Authenticated
Download Date | 6/19/15 3:32 AM
458
Scheepers et al., Fetal and maternal metabolism during labor
edly elevated suggesting that glucose is probably
the major energy source for the myometrium during labor [30, 56].
Gluconeogenesis may be insufficient when deliveries are long of duration and glucose supply is
lacking. During normal labor, the concentration
of both free fatty acids [23, 26, 57] and ketobodies [15, 17, 26] rise. This suggests an increased
mobilization of substrates other than glucose and
indicates a relative shortage of carbohydrates.
Maternal lactate concentrations rise in the last
part of the first stage and during the second stage
[10, 17, 25, 26, 60] and indicate an increased
need for the non-oxidative pathway. The rise in
lactate is more pronounced when the second stage
lasts longer [24] or when uterine contractions are
more frequent [26]. In hypoactive labor, the
increase in lactate is not significant [17].
When comparing glycogen concentration in the
myometrium of pregnant women to non-pregnant
women, Wilmidsky and Gutman found 13 mg
glycogen per 1 g of myometrium opposed to
3 mg in non-pregnant women. The activities of
glycogen synthase phosphatase and phosphorylase were also significantly higher [59] this would
suggest a preparation for labor. During labor, a
significant decrease in glycogen in the myometrium is noticed, the glycogen store is almost depleted and the energetic load, calculated by the
adenylate energy charge (which is equal to the
Atkinsons quotient), being the relative ATP, ADP
and AMP concentrations, is decreased [27].
Fetal acid base balance during labor has been described extensively. The maternal acid base balance and its relation to the fetus have received
relatively less attention. Since fetal acid base
status is mostly determined by fetal oxygenation
and to a far lesser extent by maternal acid base
status, [6] this is understandable.
In humans, the acid base balance can be equated
in: CO2 H20 L H2CO3 L H HCO3. The
pH is defined by the concentrations of CO2 and
HCO3. A higher CO2 concentration results in a
lower pH and HCO3 acts as a buffer by binding
H ions. The base excess (or base deficit), is an
expression of the amount of buffer that is used in
order to maintain the acid base balance. In humans, the concentration of HCO3 can be
adapted by means of changes in the excretion in
the kidney, but this process is slow. A faster way
of reducing the pH is an increased excretion of
CO2 by means of breathing [4, 19]. In adults, under normal circumstances, the HCO3 concentration is 24 mmol/l, the pCO2 is 5.3 kPa (40 mm
Hg) and the pH is 7.4. The base excess/deficit
varies from 2 to 2 mmol/l.
During pregnancy, progesterone directly stimulates the maternal respiratory centre resulting in
a hyperventilation and a lower maternal pCO2
(mean 4.3 kPa). During labor, the maternal pCO2
further decreases due to the increased hyperventilation during contractions [4, 6, 39]. The fetomaternal CO2 gradient increases, which facilitates the
fetal transfer of CO2 to the maternal circulation.
The maternal pH increases during the first stage
of labor [10, 39]. Maternal base deficit, however,
increases [10, 39]. This indicates an increase in
the need for the buffer mechanism. Therefore,
during the first stage of labor in the mother, a
combination of a metabolic acidosis and a respiratory alkalosis is present, in which the respiratory component is more dominant. During the second stage, maternal pH decreases back to normal values and the base deficit further decreases
[10, 39]. This indicates an increasing metabolic
acidosis, which agrees with the findings of an
increase in lactate concentrations that are measured during the second stage. Table I summa-
Table I. Maternal energy metabolism and acid base
balance during labor
1) glucose most important fuel, but ketobodies suggest
shortage
2) increased concentration of glycogen in myometrium
of pregnant women
3) mainly oxidative pathway
4) non-oxidative pathway : formation of lactate
in: polysystolic contractions
second stage
5) first stage: metabolic acidosis/respiratory alkalosis
(hyperventilation)
A pH
A base deficit
6) second stage: due to increase of lactate: increase
metabolic acidosis
B pH ( to normal levels)
further A base deficit
J. Perinat. Med. 29 (2001)
Brought to you by | New York University Bobst Library Technical Services
Authenticated
Download Date | 6/19/15 3:32 AM
Scheepers et al., Fetal and maternal metabolism during labor
rizes maternal energy metabolism and acid base
balance during labor.
3 Fetal metabolism and its relation to
maternal metabolites
The fetus needs maternal supply of nutrients for
metabolic processes and growth [2]. The most important substrate for the fetal energy metabolism
is glucose. In neonates, the respiratory quotient
(RQ) approaches one, suggesting an almost exclusive use of carbohydrates for metabolic needs.
A premature infant has a RQ of 0.91.0 and an
infant at term has a RQ of 0.7 [7].
Hay has described the process of fetal carbohydrate and lipid metabolism [20]. The main source
of fetal glucose is the maternal circulation. The
glucose-transfer through the placenta is directly
related to the maternal glucose concentration. In
cases of low fetal glucose concentration, a
smaller portion of the delivered glucose is used
by the uterus and placenta resulting in a buffer
mechanism to maintain fetal glucose supply.
Furthermore, due to a higher fetal capacity to use
glucose because of higher levels of insulin and an
increase of insulin-sensitive tissue, the maternalfetal glucose gradient increases.
The relationship between maternal and fetal metabolites was studied in the late 1960s1970s.
Glucose was found to be higher in maternal than
in fetal blood [34, 42] and venous umbilical cord
blood glucose was higher than arterial umbilical
blood, suggesting fetal usage of glucose. Hay has
described the effects of changes in maternal
blood glucose concentrations [20] and concluded
that short term severe hypoglycemia resulted in
lower fetal glucose supply. This lead to a decrease
in fetal glucose utilisation, fetal hypoinsulinemia,
a decrease in placental lactate formation and a
decrease in fetal lactate uptake. However, during
most parturitions, maternal blood glucose levels
increased and in even in prolonged labor, in
which a decline was described, the glucose concentration did not reach hypoglycemic levels
[17].
Short-term maternal hyperglycemia resulted in an
increasing amount of glucose which is shunted
into the non-oxidative pathway, leading to an
increase in the lactate concentration. An increase
459
in glucose uptake and utilization occurred and an
increase in fetal insulin was observed. Furthermore, fetal oxygen consumption was increased
[20].
Free fatty acids have been reported to higher in
maternal than fetal blood [42, 53]. Free fatty acid
concentration was found to be higher in cases of
prolonged labor and fetal arterial concentration
higher than the fetal venous concentration, suggesting fetal mobilization of free fatty acids. In
studies where glucose was administered intravenously during labor, a decline in the concentrations of both maternal and fetal blood free fatty
acids was observed [18, 42]. This would suggest
that improved glucose availability results in a decline of both maternal and fetal mobilization of
free fatty acids. This is confirmed by the fact that
the difference between arterial umbilical cord and
venous umbilical cord concentrations declines
[42, 53].
A plasma ketone rise during normal labor has
been described which correlated to the duration
of labor [18, 34]. Maternal blood concentrations
have been found to be higher than those in fetal
blood with a gradient of 2:1 [34]. The concentration of ketones in venous umbilical blood was
found to be higher than in arterial blood; this
would suggest a transplacental uptake by the fetus. In well-nourished mothers, it was found that
oxidation of ketone bodies was low and glucose
provided the major part of the fetal energetic substrate [1]. However, when there has been of maternal fasting, ketobodies can become a fetal fuel
source [46]. These ketobodies were mainly derived from the maternal circulation and fetal ketogenesis was almost inactive [9].
Schneider et al have described the homeostasis of
fetal lactate metabolism during labor [48]. They
concluded that during labor there was a gradual
rise in both maternal and fetal lactate. In most
cases fetal lactate concentrations were higher
than the maternal concentrations. Furthermore,
fetal arterial umbilical cord concentration was
higher than the venous umbilical cord concentration. This would suggest that during normal delivery the fetus produced lactate. Since lactate is
transferred by means of facilitated diffusion, in
most cases transport from the fetal to the maternal
circulation takes place. Fetal metabolic acidosis is
J. Perinat. Med. 29 (2001)
Brought to you by | New York University Bobst Library Technical Services
Authenticated
Download Date | 6/19/15 3:32 AM
460
Scheepers et al., Fetal and maternal metabolism during labor
therefore mostly of fetal origin and high lactate
concentrations during delivery suggest fetal nonoxidative metabolism and a (relative) shortage of
oxygen. It may however be the case that when
maternal lactate concentrations are high, the ability of the fetus to transfer lactate to the maternal
circulation diminishes. Very high maternal lactate
concentrations may even lead to a transport of
lactate from the maternal to the fetal circulation,
but only in about 6 % of deliveries [38]. However,
high maternal lactate concentration may have a
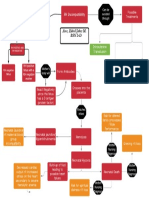
negative effect on fetal metabolic acidemia. Figure 1 summarizes the relationship between glucose and lactate in a maternal normoglycemic and
hyperglycemic situation.
estrogen and cortisol. This induces a diabetic-like
state in which peripheral glucose uptake is lower
whereby maternal blood glucose can be reserved
for the fetus. Pregnancy exaggerates the response
of the body to fasting, which make pregnant
women more prone to ketosis [15, 13]. Women
who eat during parturition have lower ketobodies
than those who do not [44]. Winkler and Hebeler
stated that uterine activity was reduced by the ac-
Conclusion: In most deliveries maternal blood glucose increases. A decline in maternal blood glucose can occur in long lasting deliveries without
adequate glucose supply, but this does not result in
severe hypoglycemia. Furthermore, due to the capacity of the placenta to regulate fetal glucose supply and fetal glucose sensitivity, it is unlikely that
fetal glucose supply will be jeopardized.
Fetal lactate is mostly of fetal origin, suggesting
fetal non-oxidative metabolism (a lack of oxygen). Hyperglycemia, however, may lead to an
increased production of lactate either in the maternal circulation and/or in the fetus/placenta. A
high maternal lactate furthermore diminishes the
ability of the fetus to transfer lactate to the maternal circulation. Combined with the increase in fetal oxygen consumption this may lead to a higher
risk of fetal acidemia.
4 Effects of fasting during labor and the
parallel to exercise
Deprivation of fluid and food during labor, theoretically, may have a negative impact on the progress
and outcome of labor. In animals, maternal and fetal blood glucose levels decline in fasting [54]. The
fetus is dependent upon glucose as its major energy
source and fetal activity has been shown to be
greater in higher maternal blood glucose levels
[32]. A lack of glucose, results in a higher mobilization of free fatty acids resulting in ketosis.
In pregnancy, the carbohydrate metabolism is altered [21]. There is a higher resistance to insulin
due to the effects of human placental lactogen,
Figure 1. Glucose and lactate metabolism in maternal
normo- and hyperglycemia
J. Perinat. Med. 29 (2001)
Brought to you by | New York University Bobst Library Technical Services
Authenticated
Download Date | 6/19/15 3:32 AM
Scheepers et al., Fetal and maternal metabolism during labor
cumulation of ketone bodies, but the cause and
effect relationship between prolonged labor and
the concentration of ketones is uncertain [60].
Since glucose is the main energy source not only
for the fetus, but also for the myometrium, gluconeogenesis is important. Although maternal glucose concentration, in most parturitions do not
decline, the rise in ketobodies and the increase in
mobilization of free fatty acids would suggest a
relative shortage of glucose.
A similar relationship between energy supply and
availability and the occurrence of fatigue occurs
in skeletal muscles during exercise. In this situation, fasting or a declining carbohydrate supply
leads to accelerated fatigue, enhanced lipolysis
and increased protein catabolism [58]. Studies
during exercise have shown that in a fasting state,
the usage of free fatty acids is enhanced [49].
During both exercise and labor, a sympathetic activation exists, resulting in a redistribution of
blood. Despite the lower blood supply to the intestinal tract, it has been shown that oral carbohydrate feeding during exercise results in a slower
occurrence of fatigue [8, 12, 45, 58]. The American College of Sports Medicine advises athletes,
who exercise for longer than one hour to ingest
carbohydrate solutions during exercise [11].
461
hyperglycemia resulting in fetal hyperinsulinemia
and neonatal hypoglycemia [3, 35, 43].
Maternal hyperglycemia, which can be caused by
an infusion of a highly concentrated glucose solution, may lead to a rise in both maternal and fetal
lactate and therefore to a metabolic acidosis. Fetal
metabolic acidosis was observed after a rapid infusion of 100 g glucose per hour [28, 36]. When
using lower dosages, this does not seem to be the
case. It was suggested by Piquard et al, that an
infusion of 10 % glucose at a rate of 30 g glucose
per hour, did not result in acidosis. Should fetal
acidosis occur, however, this would be more
likely be as a result from hypoxia than of maternal glucose administration [37]. Recently it has
been shown that the use of a 5 % glucose infusion
reduces fetal cord acidemia compared to the use
of Ringers lactate without glucose [16].
Yancey and Harlass have reviewed fetal acid base
status in relation to glucose administration and
have concluded that results are conflicting [61].
They stated that infusions which result in maternal
and fetal hyperglycemia have been correlated to alterations in fetal metabolic and acid-base status.
5 Glucose administration
To our knowledge, the only randomized controlled study on oral intake and maternal metabolic parameters has been published by Scrutton
et al [51]. They did not find a rise in maternal
lactate, nor maternal hyperglycemia, in women
who ate versus those who were starved. The formation of ketones was prevented by eating. Due
to the physiologic increase in the insulin concentration, it seems unlikely that oral intake can lead
to hyperglycemia in non-diabetic pregnant
women. Given the fact that most women in labor
do not eat or drink large amounts, oral caloric
intake is likely to be safe with regard to possible
effects on the fetal acid-base balance.
In the past, parenteral glucose administration was
considered a reasonable way to combat ketosis.
Even hyperglycemia was induced to fortify patients and it was considered good treatment for
both maternal and fetal distress [41]. However,
later studies showed fetal deterioration and fetal
Conclusion: the infusion of hyperglycemic solutions may cause fetal acidemia. Using 510 %
glucose solutions would appear to be safe. Oral
supplementation of carbohydrates may be considered. It is unlikely that oral intake would cause
hyperglycemia, but relevant data is scarce.
Conclusion: it would appear that pregnant women
are more prone to ketosis. No data are available on
the effects of caloric intake on the course of labor.
In athletes, the use of oral carbohydrates has
proven to be effective in reducing fatigue, without
adverse effects upon the gastro-intestinal tract.
Abstract
Aim: To discuss maternal and fetal metabolic events
during labor and the possible role of glucose administration.
Results: The oxidative pathway covers the largest part
of the energy demand of labor, although in the second
stage or, in polysystolic labor, the non-oxidative path-
J. Perinat. Med. 29 (2001)
Brought to you by | New York University Bobst Library Technical Services
Authenticated
Download Date | 6/19/15 3:32 AM
462
Scheepers et al., Fetal and maternal metabolism during labor
way becomes important as well. Glucose is the main
maternal energy source, but the rise in ketobodies, even
during normal labor, suggests a relative shortage. In the
first stage of labor, a combination of a respiratory alkalosis, and to a lesser extent, a metabolic acidosis, result
in a rise in the maternal pH. In the second stage of labor,
the maternal pH decreases due to an increasing metabolic acidosis. Glucose is also the main fetal energetic
fuel. In fetal hypoxia, lactate is produced, which in most
cases is transferred to the maternal circulation. High
maternal lactate concentrations, however, may interfere
with this process. Furthermore, fetal hyperglycemia
may lead to an increased fetal lactate production.
Conclusions: Maternal hyperglycemia, may lead to an
increase in maternal and fetal lactate production resulting in metabolic acidosis. Unlike high dosage intravenous glucose administration, it is not likely that oral
intake of carbohydrates leads to maternal and fetal hyperglycemia and subsequently to metabolic acidosis, but
studies are rare.
Keywords: Acid-base balance, fetal, glucose, lactate, maternal, metabolism.
Acknowledgements: The authors gratefully acknowledge the assistance of M. C. J. Thans and Dr. G. E. Beverstock
for reviewing this manuscript.
References
[1] Adam PAJ, P Felig: Carbohydrate, fat and aminoacid metabolism in the pregnant women and fetus.
In: Falkner F, JM Tanner: Human Growth. Principles and Prenatal Growth. Bailliere Tindall London 1978, pp 461
[2] Aldoretta PW, WW Hay: Metabolic substrates for
fetal energy metabolism and growth. Clinics in
Perinatology 22 (1995) 15
[3] Anderson GG, L Cordero, EH Hon: Hypertonic
glucose infusion during labour. Effects on acidbase status, fetal heart rate and uterine contractions. Obstet Gyn 36 (1970) 405
[4] Berg vd PP, JG Aarnoudse: Het foetale zuur-base
evenwicht. In: Nijhuis JG, GGM Essed, HP van
Geijn, GHA Visser: Foetale bewaking. Elsevier/
Bunge, Maarssen 1998, pp 123
[5] Berry H: Feast or famine? Oral intake during labour: Current evidence and practice. Br J Nurse
Midw (1997) 413
[6] Blechner JN: Maternal Fetal Acid Base Physiology: Clin Obst Gyn 36 (1993) 3
[7] Boisieu de D, F Rocchiccioli, N Kalach, PF Bougneres: Ketone body turnover at term and in premature newborns in the first 2 weeks after birth. Biol
Neonate 67 (1995) 84
[8] Bosch AN, SM Weltan, SC Dennis, TD Noakes:
Fuel substrate turnover and oxidation and glycogen sparing with carbohydrate ingestion in noncarbohydrate loaded cyclist. Pflugers Arch 432
(1996) 1003
[9] Bougneres PF, C Lemmel, P Ferre, DM Bier: Ketone body transport in the human neonate and infant. J Clin Invest 77 (1986) 42
[10] Cohen AV, H Schulman, SL Romney: Maternal
acid-base metabolism in normal human parturation. Am J Obstet Gynaecol 107 (1970) 933
[11] Convertino VA, LE Armstrong, EF Coyle, GW
Mack, MN Sawka, LC Senay jr, WM Sherman:
[12]
[13]
[14]
[15]
[16]
[17]
[18]
[19]
[20]
[21]
American College of Sports Medicine position
stand. Exercise and fluid replacement. Med Sci
Sports Exerc 28 (1996) i-vii
Dennis SC, TD Noakes, JA Hawley: Nutritional
strategies to minimize fatigue during prolonged
exercise: fluid electrolyte and energy replacement.
J Sports Sci 15 (1997) 305
Dumoulin JG; JE Foulkes: Ketonuria during labor.
Br J Obstet Gyn 91 (1984) 97
Elkington KW: At the waters edge: where obstetrics and anaesthesia meet. Obstet Gynecol 77
(1991) 304
Felig P, V Lynch: Starvation in human pregnancy;
hypoglycemia, hypoinsulinemia and hyperketonemia. Science 170 (1970) 990
Fisher AJ, JF Huddleston: Intrapartum maternal
glucose infusion reduces umbilical cord acidemia.
Am J Obst Gyn (1997) 765
Friedberg V, RH Ackermann: Aspekte des endokrin-metabolischen Zusammenspiels unter der Geburt. Geburtshilfe Frauenheilk 43 (1983) 8
Gardmark S, G Gennser, L Jacobson, G Rooth, J
Thorell: Influence on fetal carbohydrate and fat
metabolism and on acid-base balance of glucose
administration to the mother during labour. Biol
Neonate 26 (1975) 129
Guyton AC. Lipid Metabolism In: Guyton AC:
Textbook of medical physiology. Seventh edition.
Philidelphia W. B. Saunders 1986, pp 822
Hay WW: Nutrition and development of the fetus:
carbohydrate and lipid "metabolism In: Nutrition
in pediatrics. Walker 24 (1997) 364
Helmerhorst FM, MJNC Keirse: De normale
zwangerschap. In: Treffers PE et al, Obstetrie en
Gynaecologie. De voortplanting van de mens. Utrecht: Wetenschappelijke uitgeverij Bunge 1993,
pp 116
J. Perinat. Med. 29 (2001)
Brought to you by | New York University Bobst Library Technical Services
Authenticated
Download Date | 6/19/15 3:32 AM
Scheepers et al., Fetal and maternal metabolism during labor
[22] Johnson CJ, MJNC Keirse, M Enkin, I Chalmers:
Nutrition and hydration in labour. In: Chalmers I,
Effective care in pregnancy and childbirth. Oxford
University Press Oxford 1989, pp 827
[23] Kashyap ML: Carbohydrate and lipid metabolism
during human labor: free fatty acids, glucose, insulin and lactic acid metabolism during normal and
oxytocin-induced labor for postmaturity. Metabolism 25 (1976) 865
[24] Katz M, E Lunenfeld, I Meizner, N Bashan, J
Gross: The effect of the duration of the second
stage of labour on the acid-base state of the fetus.
Br J Obst Gyn 94 (1987) 425
[25] Katz M, D Kroll, Y Shapiro, N Cristal, I Meizner:
Energy expenditure in normal labor. Isr J Med Sci
26 (1990) 254
[26] Krolikowska von M. T Laudanski, J Mikaszewska-Pietraszum, T Paprocka-Raba: Einfluss der
Wehentatigkeit auf Parameter des Kohlenhydratund Fettstoffwechsels im Blut. Zbl. Gynakol 101
(1979) 1151
[27] Laudanski T: Energetischer Metabolismus des
Myometriums wahrend der Schwangerschaft und
der Geburt. Zbl. Gynakol 107 (1985) 568
[28] Lawrence GF, VA Brown, RJ Parsons, ID Cooke:
Feto-maternal consequences of high-dose glucose
infusion during labour. Br J Obstet Gyn 89 (1982)
27
[29] Ludka LM, CC Roberts: Eating and drinking in
labor. A literature review. J Nurse-Midw 38(4)
(1993) 199
[30] Maheux PC, B Bonin, A Dizazo, P Guimond,
D Monier, J Bourque, JL Chiasson: Glucose homeostatis during spontaneous labour in normal human pregnancy. J Clin Endocrin Metab 81(1996)
209
[31] Michael S, CS Reilly, JA Caunt: Policies for oral
intake during labour. A survey of maternity units
in England and Wales. Anaesthesia. 46(12) (1991)
1071
[32] Miller FM, H Skiba, H Klapholz: The effect of
maternal blood sugar-levels on fetal activity. Obstet Gyn 52 (1978) 662
[33] OSullivan G: The stomach, fact and fantasy: eating and drinking during labor. Int Anesthesiol Clin
32(2) (1994) 31
[34] Paterson P, J Sheath, P Taft, C Wood: Maternal
and foetal ketone concentrations in plasma and
urine. Lancet i (7495) (1967) 862
[35] Pearson JF, R Shuttleworth: The metabolic effects
of a hypertonic fructose infusion on the mother
and fetus during labor. Am J Obst Gynec 15
(1971) 259
[36] Philipson EH, SC Kalhan, MM Riha, R Pimentel:
Effects of maternal glucose infusion on fetal"acidbase status in human pregnancy. Am J Obst Gyn
157 "(1987) 866
463
[37] Piquard F, R Hsiung, A Schaefer, P Haberey, P
Dellenbach: Does fetal acidosis develop with maternal glucose infusion during normal labor? Obstet Gyn 74 (1989) 909
[38] Piquard F, A Schaefer, P Dellenbach, P Haberey:
Is fetal acidosis in the human fetus maternogenic
during labor? A reanalysis. Am J Physiol 261
(1991) R1294
[39] Pontonnier G, F Puech, H Grandjean, M Rolland:
Some physical and biochemical parameters during
normal labour. Biol-Neonate 26 (1975) "159
[40] Practice guidelines for obsetrical anesthesia: A report by the American Society of Anesthesiologist
Task Force on Obstetrical Anesthesia. Anesthesiology 90 (1999) 600
[41] Romney SL, MS Gabel: Maternal glucose loading
in the management of fetal distess. Am J Obst Gyn
96 (1966) 698
[42] Roux JF, SL Romney: Plasma free fatty acids and
glucose concentrations in the human fetus and
newborn exposed to various environmental conditions. Am J Obst Gynec 97 (1967) 269
[43] Rutter N: Glucose during labor. Lancet 2 (1980)
155
[44] Sabata V, H Wolf, S Lausmann: The role of free
fatty acids, glycerol, ketone bodies and glucose in
the energy metabolism of the mother and fetus
during delivery. Biol Neonatol 13 (1968) 7
[45] Sayed el MS, D MacLaren, AJ Rattu: Exogeneous
carbohydrate utilisation: effects on metabolism
and exercise performance. Comp Biochem Physiol
A Physiol 118 (1997) 789
[46] Schambaugh GE: Ketone body metabolism in the
mother and fetus. FASEB J. 44 (1985) 2347
[47] Scheepers HCJ, GGM Essed, F Brouns: Food and
fluid intake during labour; policies on oral intake
during labour in The Netherlands: Eur J Obst Gyn
and Repr Biol 78 (1998) 37
[48] Schneider H, J Danko, R Huch, A Huck: Homeostasis of fetal lactate metabolism in late pregnancy
and the changes during labor and delivery. Eur J
Obst Gyn Repr Biol (1984) 183
[49] Schneiter P, Di-Vetta V, Jequier E, Tappy L. Effect
of physical exercise on glycogen turnover and net
substrate utilization according to the nutritional
state. Am J Physiol 269 (1995) E1031
[50] Schuitemaker N, J Roosmalen, G Dekker, P
Dongen van, H Geijn van, J Bennebroek Gravenhorst: Maternal mortality after cesarean section
in The Netherlands. Acta Obstet Gynecol Scand
76 (1997) 332
[51] Scrutton MJL, GA Metcalfe, C Lowy, PT Seed, G
OSullivan: Eating in labor. A randomized controlled trial assessing the risk and benefits. Anaesthesia 54 (1999) 329
[52] Sharp DA: Restriction of oral intake for women in
labour. Br J. Midwifery 5 (1997) 408
J. Perinat. Med. 29 (2001)
Brought to you by | New York University Bobst Library Technical Services
Authenticated
Download Date | 6/19/15 3:32 AM
464
Scheepers et al., Fetal and maternal metabolism during labor
[53] Sheath J, J Grimwade, K Waldron, M Bickley, P
Taft, C Wood: Arteriovenous nonesterified fatty
acids and glycerol differences in the umbilical
cord at term and their relationship to fetal metabolism. Am J Obstet Gynecol 113 (1972) 358
[54] Simmons M, G Meschia, E Makowski: Fetal metabolic response to maternal starvation. Pediatr Res
(1974) 830
[55] Sleutel M, SS Golden. Fasting in labor: relic or
requirement: J Obstet Gynecol Neonatal Nurs 28
(1999) 507
[56] Steingrimsdottir Th, G Ronquist, U Ulmsten, A
Waldenstrom: Different energy metabolite pattern
between uterine smooth muscle and striated rectus
muscle in term pregnant women. Eur J Obst Gyn
Reprod Med (1995) 241
[57] Wagemakers AJM, EJ Beckers, F Brouns, H Kuipers, PB Soeters, GJ van der Vusse, WHM Saris:
Carbohydrate supplementation, glycogen depletion, and amino acid metabolism during exercise.
Am J Physiol 1991 (1991) E883
[58] Whaley WH, FP Zuspan, GH Nelson, RP Ahlquist:
Alterations of plasma free fatty acids and glucose
during labor. Am J Obstet Gyn 67 (1967) 875
[59] Wilmidsky A, Guman A: Glycogen metabolism of
normal human myometrium and leiomyoma. Possible hormonal control. Gyn Obstet Invest 15
(1983) 147
[60] Winkler H, Hebeler F: Investigation of the acetone
and lactic acid concentrations in blood during
birth and their importance for uterine action. Archiv Gynekol 168 (1939) 64
[61] Yancey MK, Harlass FE: Extraneous factors and
their influences on fetal acid-base status. Clin Obst
Gyn 36 (1993) 60
H. C. J. Scheepers,
Leyenburg Hospital
Leyweg 275
2545 CH The Hague
The Netherlands
Fax:
31 70-3592204
e-mail: HCJ. Scheepers@hetnet.nl
J. Perinat. Med. 29 (2001)
Brought to you by | New York University Bobst Library Technical Services
Authenticated
Download Date | 6/19/15 3:32 AM
You might also like
- Obesity - Short Scientific Findings to Ameliorate the Body WeightFrom EverandObesity - Short Scientific Findings to Ameliorate the Body WeightNo ratings yet
- Translational Glycobiology in Human Health and DiseaseFrom EverandTranslational Glycobiology in Human Health and DiseaseMichelle KilcoyneNo ratings yet
- Metabolism in Normal PregnancyDocument10 pagesMetabolism in Normal Pregnancywilliam pinillaNo ratings yet
- 02 - Added Sugars and Risk Factors For Obesity, Diabetes and Heart DiseaseDocument6 pages02 - Added Sugars and Risk Factors For Obesity, Diabetes and Heart DiseaseFloridalma FajardoNo ratings yet
- Diet and Acne New FindingsDocument14 pagesDiet and Acne New FindingsAlbert WielandNo ratings yet
- The Pathophysiology of Intrahepatic Cholestasis of PregnancyDocument13 pagesThe Pathophysiology of Intrahepatic Cholestasis of PregnancyEnrique RosasNo ratings yet
- Artigo 1Document13 pagesArtigo 1Ana Cláudia MatiasNo ratings yet
- Κατανάλωση φρουκτόζηςDocument17 pagesΚατανάλωση φρουκτόζηςxrysakouNo ratings yet
- Beyond Weight Loss: A Review of The Therapeutic Uses of Very-Low-Carbohydrate (Ketogenic) DietsDocument8 pagesBeyond Weight Loss: A Review of The Therapeutic Uses of Very-Low-Carbohydrate (Ketogenic) DietsChrisostomus AltiusNo ratings yet
- New Insights Into Gestational Glucose Metabolism: Lessons Learned From 21st Century ApproachesDocument8 pagesNew Insights Into Gestational Glucose Metabolism: Lessons Learned From 21st Century ApproachessanthiyasandyNo ratings yet
- The Effect of High-Fructose Corn Syrup Consumption On Triglycerides and Uric AcidDocument4 pagesThe Effect of High-Fructose Corn Syrup Consumption On Triglycerides and Uric AcidAddin RayindaNo ratings yet
- Protein Metabolism in Pregnancy: Satish C KalhanDocument7 pagesProtein Metabolism in Pregnancy: Satish C KalhanAdib FraNo ratings yet
- Approach To Hypoglycemia in Infants and Children - UpToDateDocument20 pagesApproach To Hypoglycemia in Infants and Children - UpToDateDenny IntanNo ratings yet
- Meal MacronutsDocument13 pagesMeal MacronutsTere NavaNo ratings yet
- Glikemik Indeks Pada DMDocument6 pagesGlikemik Indeks Pada DMAliyahRajutButikNo ratings yet
- Fasting Substrate Oxidation at Rest Assessed by Indirect Calorimetry Is Prior Dietary Macronutrient Level and Composition A ConfounderDocument4 pagesFasting Substrate Oxidation at Rest Assessed by Indirect Calorimetry Is Prior Dietary Macronutrient Level and Composition A ConfounderAlan SalazarNo ratings yet
- Beyond Weight Loss A Review of The Therapeutic Uses of Very-Low-Carbohydrate (Ketogenic) DietsDocument8 pagesBeyond Weight Loss A Review of The Therapeutic Uses of Very-Low-Carbohydrate (Ketogenic) DietsmrsilvNo ratings yet
- F A C N - M: Rom The Merican Ollege of Urse IdwivesDocument8 pagesF A C N - M: Rom The Merican Ollege of Urse Idwivesbellia loranthifoliaNo ratings yet
- HFCS Everything You Wanted To Know But Were Afraid To AskDocument1 pageHFCS Everything You Wanted To Know But Were Afraid To AskSofía I. Morales NavarroNo ratings yet
- Neonatal Energy Triangle Part 1Document6 pagesNeonatal Energy Triangle Part 1Belfast324100% (1)
- The Role of Maternal Dietary Proteins in Development of Metabolic Syndrome in OffspringDocument33 pagesThe Role of Maternal Dietary Proteins in Development of Metabolic Syndrome in OffspringNurfadhilah YusufNo ratings yet
- Ijo 201233 ADocument8 pagesIjo 201233 AYondri Mandaku TasidjawaNo ratings yet
- 1 s2.0 S0955286317303868 MainDocument14 pages1 s2.0 S0955286317303868 MainAdib FraNo ratings yet
- Lipo GenesisDocument2 pagesLipo GenesisArthur James De TorresNo ratings yet
- Nature 2000 - Central Nervous System Control of Food IntakeDocument11 pagesNature 2000 - Central Nervous System Control of Food IntakeAlan NiemiesNo ratings yet
- 2018 Article 9455Document21 pages2018 Article 9455ნათია დემეტრაძეNo ratings yet
- Maternal and Fetal Acid Base Chemistry ReviewDocument10 pagesMaternal and Fetal Acid Base Chemistry ReviewcarlosarmijoNo ratings yet
- When To Eat The Influence of Circadian Rhythms On Metabolic Health Are Animal Studies Providing The EvidenceDocument14 pagesWhen To Eat The Influence of Circadian Rhythms On Metabolic Health Are Animal Studies Providing The EvidenceAndré LeiteNo ratings yet
- Biopharm. YhatsssDocument4 pagesBiopharm. YhatsssNash IsmaelNo ratings yet
- Set-Point Theory and ObesityDocument6 pagesSet-Point Theory and ObesityDouglas MarinNo ratings yet
- Osama Hamdy, MD, PHD Chief Editor Romesh Khardori, MD, PHD, FACP Etiology Obestity MedscapeDocument4 pagesOsama Hamdy, MD, PHD Chief Editor Romesh Khardori, MD, PHD, FACP Etiology Obestity MedscapeEvi BaeNo ratings yet
- Neonatal HypoglycemiaDocument12 pagesNeonatal HypoglycemiayogaNo ratings yet
- Review Article Effect of The Dietary Fat Quality On Insulin SensitivityDocument9 pagesReview Article Effect of The Dietary Fat Quality On Insulin SensitivityGilberto BicalhoNo ratings yet
- Cambios RespiratoriosDocument12 pagesCambios RespiratoriosRandolph Saki Ruiz RodríguezNo ratings yet
- Parenteral Nutrition Patients: ObstetricDocument14 pagesParenteral Nutrition Patients: ObstetricAripinSyarifudinNo ratings yet
- Am J Clin Nutr 2014 Lecoultre 268 75Document8 pagesAm J Clin Nutr 2014 Lecoultre 268 75Kang Opik TaufikNo ratings yet
- Effect of Fat Intake On Energy BalanceDocument7 pagesEffect of Fat Intake On Energy BalancekarlosNo ratings yet
- Calcio Enel Emba RazoDocument31 pagesCalcio Enel Emba RazoCarlos Elio Polo VargasNo ratings yet
- Cholestasis of PregnancyDocument14 pagesCholestasis of PregnancyLina MartinezNo ratings yet
- Role of Dietary Fructose and Hepatic de Novo Lipogenesis in Fatty Liver DiseaseDocument12 pagesRole of Dietary Fructose and Hepatic de Novo Lipogenesis in Fatty Liver DiseaseYazmin Alcalde BritoNo ratings yet
- Nutrients 09 00385 Glicación AvanzDocument16 pagesNutrients 09 00385 Glicación AvanzLuis franNo ratings yet
- ABM Clinical Protocol #1: Guidelines For Blood Glucose Monitoring and Treatment of Hypoglycemia in Term and Late-Preterm Neonates, Revised 2014Document7 pagesABM Clinical Protocol #1: Guidelines For Blood Glucose Monitoring and Treatment of Hypoglycemia in Term and Late-Preterm Neonates, Revised 2014Gita KurniasariNo ratings yet
- Glycemic Index and Glycemic LoadDocument18 pagesGlycemic Index and Glycemic LoadKristine ReyesNo ratings yet
- Maternal Carbohydrate Intake and Pregnancy OutcomeDocument6 pagesMaternal Carbohydrate Intake and Pregnancy OutcomeSofía Simpértigue CubillosNo ratings yet
- Frutose DiseasesDocument9 pagesFrutose DiseasesPaolla MirandaNo ratings yet
- Polydextrose and Weight ManagementDocument4 pagesPolydextrose and Weight Managementchef Sergio rojasNo ratings yet
- 247 Ketogenic Diet and Its Role in Eliminating PDFDocument14 pages247 Ketogenic Diet and Its Role in Eliminating PDFAnil Batta100% (1)
- Cloves 1Document9 pagesCloves 1irmaNo ratings yet
- Timing of Food Intake Predicts Weight Loss EffectivenessDocument8 pagesTiming of Food Intake Predicts Weight Loss Effectivenessellla 38No ratings yet
- Theresa Davis USDA Grant Through 3:2019Document5 pagesTheresa Davis USDA Grant Through 3:2019The Nutrition CoalitionNo ratings yet
- Effect of A Carbohydrate-Rich Beverage On Rate of Cesarean Delivery in Primigravidae With Epidural Labor AnalgesiaDocument12 pagesEffect of A Carbohydrate-Rich Beverage On Rate of Cesarean Delivery in Primigravidae With Epidural Labor AnalgesiaandriruslyNo ratings yet
- Glucose As A Major Antioxidant - When, What For and Why It FailsDocument20 pagesGlucose As A Major Antioxidant - When, What For and Why It FailsDaniel GilbertoNo ratings yet
- Neonatal Glucose Metabolism Differential Diagnoses, Evaluation, and Treatment of Hypoglycemia 2002Document11 pagesNeonatal Glucose Metabolism Differential Diagnoses, Evaluation, and Treatment of Hypoglycemia 2002Guillermo CalderaroNo ratings yet
- Radiant WarmersDocument5 pagesRadiant WarmersUday KumarNo ratings yet
- Fatty Acids, Obesity, and Insulin Resistance: Time For A ReevaluationDocument9 pagesFatty Acids, Obesity, and Insulin Resistance: Time For A ReevaluationBlagojeNo ratings yet
- International Archives of Medicine: Fat Feeding Potentiates The Diabetogenic Effect of Dexamethasone in Wistar RatsDocument12 pagesInternational Archives of Medicine: Fat Feeding Potentiates The Diabetogenic Effect of Dexamethasone in Wistar RatsShanmugam SivabalanNo ratings yet
- Perspective: Leptin's Physiologic Role: Does The Emperor of Energy Balance Have No Clothes?Document3 pagesPerspective: Leptin's Physiologic Role: Does The Emperor of Energy Balance Have No Clothes?ShuiNo ratings yet
- Tremblay-2011-Obesity The Allostatic Load of Weight Loss DietingDocument6 pagesTremblay-2011-Obesity The Allostatic Load of Weight Loss DietingluizfernandosellaNo ratings yet
- Research Article: The Effect of Oral Leucine On Protein Metabolism in Adolescents With Type 1 Diabetes MellitusDocument6 pagesResearch Article: The Effect of Oral Leucine On Protein Metabolism in Adolescents With Type 1 Diabetes MellitushartithpNo ratings yet
- Associations of Serum Fibroblast Growth Factor 23 Levels With Obesity and Visceral Fat Accumulation PDFDocument6 pagesAssociations of Serum Fibroblast Growth Factor 23 Levels With Obesity and Visceral Fat Accumulation PDFAkiko Syawalidhany TahirNo ratings yet
- 8 Honey Nutrient FunctionalDocument47 pages8 Honey Nutrient Functionalbellia loranthifoliaNo ratings yet
- Effect of Regular Group Exercise On Maternal Psychological OutcomesDocument6 pagesEffect of Regular Group Exercise On Maternal Psychological Outcomesbellia loranthifoliaNo ratings yet
- Energy Production in Human BodyDocument30 pagesEnergy Production in Human Bodymohitime100% (2)
- Comparison of The Effects of Blending and Juicing On The 2014Document7 pagesComparison of The Effects of Blending and Juicing On The 2014Riana Pasca RoshianNo ratings yet
- Antioxidant and Tissue Protective Studies On Ajwa Extract Dates From Al Madinah Al Monwarah Saudia Arabia 2161 0525.1000163 PDFDocument8 pagesAntioxidant and Tissue Protective Studies On Ajwa Extract Dates From Al Madinah Al Monwarah Saudia Arabia 2161 0525.1000163 PDFbellia loranthifoliaNo ratings yet
- Nutrition in LabourDocument8 pagesNutrition in Labourbellia loranthifoliaNo ratings yet
- Fetal & Maternal Energy Metabolism During LaborDocument8 pagesFetal & Maternal Energy Metabolism During Laborbellia loranthifoliaNo ratings yet
- F A C N - M: Rom The Merican Ollege of Urse IdwivesDocument8 pagesF A C N - M: Rom The Merican Ollege of Urse Idwivesbellia loranthifoliaNo ratings yet
- (Day 1 - Part 1) - Phlebotomy-Patient Preparation and ConsiderationDocument5 pages(Day 1 - Part 1) - Phlebotomy-Patient Preparation and ConsiderationAlexia MagtibayNo ratings yet
- Types of ShocksDocument33 pagesTypes of Shocksmark OrpillaNo ratings yet
- Hematology Lecture: DR Ma. Teresa S. FajardoDocument7 pagesHematology Lecture: DR Ma. Teresa S. FajardoJocel CastilloNo ratings yet
- Anemia Diagnosis, Classification, and Monitoring Using Cell-Dyn Technology Reviewed For The New MillenniumDocument16 pagesAnemia Diagnosis, Classification, and Monitoring Using Cell-Dyn Technology Reviewed For The New MillenniumNeveen_Hussein_1880No ratings yet
- 03.practice Set SSC-CGL Tier IDocument16 pages03.practice Set SSC-CGL Tier IdragonbourneNo ratings yet
- Anatomy and Physiology of HeartDocument5 pagesAnatomy and Physiology of HeartAmit MartinNo ratings yet
- CALC - Fluor. Calcium FluorideElasticity Salt - Contributes To Elasticity WallsDocument22 pagesCALC - Fluor. Calcium FluorideElasticity Salt - Contributes To Elasticity Wallsapi-11375880100% (1)
- Retraction: Retracted: Detection of Abnormal Hemoglobin Variants by HPLC Method: Common Problems With Suggested SolutionsDocument11 pagesRetraction: Retracted: Detection of Abnormal Hemoglobin Variants by HPLC Method: Common Problems With Suggested SolutionsHaziq WahidNo ratings yet
- CryoprecipitateDocument7 pagesCryoprecipitateBrandon BNo ratings yet
- Effects of SmokingDocument3 pagesEffects of SmokingKristine HeideeNo ratings yet
- Exerise No.5 Reticulocyte Count: Routine Hematology Laboratory Student Manual Volume 1Document6 pagesExerise No.5 Reticulocyte Count: Routine Hematology Laboratory Student Manual Volume 1Jam RamosNo ratings yet
- Form 3 Science Chapter 1Document25 pagesForm 3 Science Chapter 1Mukilan MurugasanNo ratings yet
- Science9 - ACTIVITY SHEET - Physics - Quarter I Week 1 2Document24 pagesScience9 - ACTIVITY SHEET - Physics - Quarter I Week 1 2Ezzy SantosNo ratings yet
- Prothrombin Time and International Normalized Ratio (PT - INR) - Lab Tests OnlineDocument11 pagesProthrombin Time and International Normalized Ratio (PT - INR) - Lab Tests OnlineAlyaNo ratings yet
- Report of Measurement of Plasma Total ProteinDocument11 pagesReport of Measurement of Plasma Total ProteinDoreen AmulenNo ratings yet
- 1 Diabetes Screening PO4047576719 696Document4 pages1 Diabetes Screening PO4047576719 696rishiranjan04No ratings yet
- ActivityDocument6 pagesActivityandreskalikasansaraNo ratings yet
- Hemorrhagic Conditions in Neonates: DR Hodan Ahmed, Department of Pediatrics and Child Health, Amoud Medical School, AUDocument27 pagesHemorrhagic Conditions in Neonates: DR Hodan Ahmed, Department of Pediatrics and Child Health, Amoud Medical School, AUAbdisalan hassanNo ratings yet
- The Hazards: OF Blood TransfusionDocument7 pagesThe Hazards: OF Blood TransfusionPranjal Kr SahariaNo ratings yet
- Forensic Chemistry and ToxicologyDocument15 pagesForensic Chemistry and ToxicologyLombroso's follower100% (2)
- Chapter-1 (Cell and Enzymes) - 2Document34 pagesChapter-1 (Cell and Enzymes) - 2ToXicNo ratings yet
- HEMADocument44 pagesHEMAJilycamae COSMODNo ratings yet
- Jesus Still Heals All Terminal Diseases Including CoronavirusDocument166 pagesJesus Still Heals All Terminal Diseases Including CoronavirusOyelade Oluwafunmilayo100% (1)
- 1.6 What Do The Kidneys DoDocument3 pages1.6 What Do The Kidneys DoNilar SanNo ratings yet
- ScienceDocument395 pagesScienceRachelNo ratings yet
- MCQ Exam 2011 PDFDocument22 pagesMCQ Exam 2011 PDFBranka Kurtovic80% (10)
- Homeostasis, AnatomyDocument16 pagesHomeostasis, AnatomyKapemba White BothaNo ratings yet
- Test Medicina Lingua Inglese 2014 - Domande e RisposteDocument40 pagesTest Medicina Lingua Inglese 2014 - Domande e RisposteSkuola.netNo ratings yet
- Blood Transfusion - Marino - The Icu BookDocument3 pagesBlood Transfusion - Marino - The Icu BookWilliam OmarNo ratings yet
- Basic Concept Map - RH IncompatibilityDocument1 pageBasic Concept Map - RH IncompatibilityTechnoShindoNo ratings yet