Professional Documents
Culture Documents
Burns
Uploaded by
Bell SwanCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Burns
Uploaded by
Bell SwanCopyright:
Available Formats
Article
injuries
Burns
Gordon L. Klein, MD,
MPH,* David N. Herndon,
MD
Objectives
1.
2.
3.
4.
5.
6.
After completing this article, readers should be able to:
Determine the extent and depth of a burn injury.
Delineate how to evaluate a child who has an acute burn injury.
Know when to suspect abuse in a burned child.
Describe the resuscitation of a burned child.
Recognize the metabolic and immune response to a burn injury.
Discuss how to evaluate and manage an inhalation injury.
Definitions
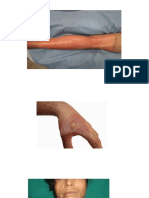
It is very important for the clinician caring for a burn victim to know the depth, or degree,
of burn. A first-degree burn is superficial, dry, painful to touch, and heals in less than
1 week. A second-degree burn is partial thickness and pink or possibly mottled red. It
exhibits bullae or frank weeping on the surface. It usually is painful unless classified as deep
and heals in 1 to 3 weeks. Second-degree burns commonly are caused by scald injuries and
result from brief exposure to the heat source. A third-degree burn is the most serious. It
appears pearly white, charred, hard, or parchmentlike. The dead skin (eschar) is white, tan,
brown, black, and occasionally red. Superficial vascular thrombosis can be observed; there
also can be focal tissue loss with prolonged exposure and a soapy-looking lesion that is
found in alkali burns.
A first-degree burn is exemplified by prolonged exposure to sunlight. Second- and
third-degree burns can result from contact with hot fluids (scald) or hot objects, such as an
iron (contact burn), flames (flame burn), high-voltage electricity (electrical burn); various
chemical agents, including acid and alkali (chemical burn); or very cold objects or
environments (frostbite).
The physician also must determine the extent of injury. The determination of total body
surface area (TBSA) involved in a burn injury is shown in the Figure.
Epidemiology
Two thirds of burn injuries in children younger than 4 years of age are scald burns, one fifth
are from contact with hot substances, and the remainder are flame burns. For children
between the ages of 6 months and 2 years, spillage of hot liquids, such as coffee and other
hot foods, is the most common scenario. Hot water burns occur primarily in the bathroom
and generally are more extensive than hot food burns. Most microwave-associated burns in
children are due to exposure to the hot foods within the appliance.
A subset of burns in young children is due to child abuse (10% to 30% overall) by
parents, siblings, or caretakers. Affected children may exhibit other signs of abuse or
neglect, such as poor body hygiene, fractures, bruises, or malnutrition. Cigarette burns
constitute the greatest number of thermal injuries in the abused population, usually are
limited in extent, and may not necessitate hospitalization for care, but clearly require
confinement of the child if abuse is suspected. Scald burns that exhibit a straight-line
distribution suggest immersion; such appearance on the feet, posterior legs, buttocks, and
hands suggest abuse. These burns often are associated with trauma, such as fractures. Cases
of placing small children inside microwave ovens also have been reported. In these cases,
* Professor of Pediatrics and Preventive Medicine.
Jesse H. Jones Distinguished Professor of Surgery, University of Texas Medical Branch and Shriners Burns Hospital, Galveston,
Tex.
Pediatrics in Review Vol.25 No.12 December 2004 411
injuries burns
burned skin. When burns exceed
25% TBSA, noninjured tissues also
swell. The cause of the fluid shift is
believed to be the presence of various mediators stimulated by the
burn injury (Table 1). These mediators also impair cardiac contractility and increase vascular resistance,
creating a scenario for hypovolemia, hypoperfusion, tissue ischemia, renal failure, cardiovascular
collapse, and death, if aggressive
resuscitation therapy is not initiated early.
Electrical burns cause additional
complications. Cardiac arrhythmia,
including ventricular fibrillation,
Figure. The rule of nines altered for the anthropomorphic differences of infancy and can occur at the time and site of the
childhood. Reprinted with permission from Herndon DN, ed. Total Burn Care. 2nd ed. injury, as can myocardial damage.
London, England: Saunders: 2002.
Tissues that are most resistant to
electric current, such as bone, sustain the greatest heat injury, and
the injuries are full-thickness, and most are demarcated
soft tissue next to the bone frequently is damaged.
close to the source of the microwave. In cases of contact
Myoglobinuria, renal failure, and neurologic damage,
burn with a hot iron, burns on the dorsal surface of the
including Guillain-Barre syndrome, transverse myelihand often indicate abuse; those on the palm usually
tis, amyotrophic lateral sclerosis, paresis, and paralysis,
suggest neglect.
can develop up to 2 years following an electrical burn.
Contact with hot items in the home or fires are the
Eye injuries complicate 5% to 20% of electrical burns;
chief causes of burn injury among children and young
cataracts are the most common complications.
adolescents. Such burns are associated with contact with
Hypermetabolism
curlers and curling irons, room heaters, ovens, ranges,
Children who have large burns experience an increase in
gasoline, and fireworks. Electrical burn injuries are likely
energy expenditure and protein metabolism of approxito result from contact with household electrical cords or
mately 50% after the first few days following injury. This
current in wall outlets. Males are at greater risk of burn
results in negative nitrogen balance and depletion of
injury and death than are females; children younger than
body protein stores, which can last for 9 months follow4 years of age, especially those who have disabilities, are
ing the burn. This state results in weight loss of up to
at the greatest risk.
20%, impaired growth velocity, muscle wasting, impaired
Pathogenesis
immunity, delayed wound healing, and markedly reOnce sustained, the burn injury, especially full-thickness
duced bone formation, with acute skeletal bone loss and
burns that occupy 40% or more TBSA, give rise to many
increased risk of fracture. Epinephrine, cortisol, and glucomplications. The most immediate are burn shock and
cagon are produced in excess and mediate the inburn edema, as well as inhalation injury, if sustained.
creased gluconeogenesis, glycogenolysis, muscle
Within a few days of the burn injury, other responses are
breakdown, and bone loss. They also antagonize the
detected, including hypermetabolism, systemic inflamanabolic effects of insulin and growth hormone. The
matory response syndrome (SIRS), and sepsis.
body is less able to use fat for fuel, and muscle becomes
an energy source.
Acute Changes: Burn Shock and Burn Edema
Burn injury results in loss of fluid from the intravascular
space and excessive fluid accumulation in the interstitial
space, resulting in hypovolemia and swelling of the
412 Pediatrics in Review Vol.25 No.12 December 2004
SIRS
SIRS occurs as a result of burn injury, and symptoms
range from tachypnea and tachycardia, leukocytosis, and
injuries burns
Table 1.
Mediators of Burn Shock and Edema
Mediator
Source
Effect
Histamine
Mast cells from burned skin
Prostaglandins
Thromboxanes
Arachidonic acid released from burned
tissue and inflammatory cells
Platelets in the burn wound
Kinins
Serotonin
Catecholamines
Inflammatory cells
Inflammatory cells
Adrenal medulla
Oxygen radicals
Platelet aggregation
factor
Angiotensin II and
vasopressin
Burned tissue
Burn wound platelets
Increases capillary permeability, arteriolar dilatation,
and venular contraction
PGE2, PGI2: potent vasodilators; increase
microvascular permeability
Thromboxanes A2 and B2: vasoconstrictors;
contribute to tissue ischemia
Increase venular permeability
Vasoconstrictor; reduces blood flow to burn wounds
Vasoconstrictor; contributes to wound ischemia,
increased systemic vascular resistance
Increase vascular permeability and burn edema
Increases capillary permeability
Renal juxtaglomerular cells
fever to hypotension, shock, and multisystem organ failure. The hyperactive immune response causes a generalized inflammation that damages healthy tissue as well as
infected burn wounds. Microvascular permeability leads
to decreased tissue oxygenation, and blood flow is reduced due to microthrombi. During this reaction, the
intestinal and, possibly, the respiratory barriers to infection are damaged, allowing the entry of additional bacteria into the circulation, known as bacterial translocation.
Coexisting with SIRS is another reaction termed the
counter anti-inflammatory response syndrome (CARS),
which attempts to limit the damage created by inflammatory cells. However, the CARS reaction also promotes
immunosuppression. These reactions are generated by
chemokines, which are located in the macrophages and
endothelial cells, and attract inflammatory cells to the site
of damage. The inflammatory cells produce cytokines,
which also stimulate the inflammatory response and tissue destruction. Differentiating SIRS and CARS from
sepsis, which is the leading cause of death in burns, is
extremely challenging.
Inhalation Injury
Inhalation of the toxins associated with flame smoke
accounts for 80% of burn-related deaths. These include
carbon monoxide and hydrogen cyanide, which can potentiate tissue hypoxia and acidosis. It is important to
know both the source of the fire and the nature of the
gases it produces to treat the injury adequately. In addition, the inhaled hot gases cause oropharyngeal edema in
Vasoconstrictors; may be responsible for intestinal
ischemia (angiotensin) and increased systemic
vascular resistance (vasopressin)
the same way that they affect other tissues, as discussed
previously. Also, inhalation of various chemicals, such as
aldehydes, can cause contact damage to the trachea and
bronchi, resulting in inflammation and formation of
fibrin casts that can obstruct the lower airway completely
and lead to decreased oxygenation due to pulmonary
vascular vasoconstriction.
Diagnosis and Management of the Burn
Wound
The appearance of the skin should be sufficient to classify
the depth and extent of the burn. It is important to
obtain a complete history of the burn injury because
certain sources, such as alkali, may require additional
treatment to stop the penetration of skin layers.
The superficial burn wound that extends to less than
10% TBSA usually can be treated on an outpatient basis
unless abuse is suspected. Therapy consists of applying a
cotton gauze occlusive dressing to protect the damaged
skin from bacterial contamination, eliminate air movement over the wound (thus reducing pain), and decrease
water loss. Dressings are changed daily. A topical antimicrobial agent should be applied to the wound prior to the
dressing for prophylaxis. The agent used most commonly
is silver sulfadiazine, which has activity against Staphylococcus aureus, Escherichia coli, Klebsiella sp, Pseudomonas
aeruginosa, Proteus sp, and Candida albicans. The primary adverse effect of silver sulfadiazine is leukopenia,
which occurs in 5% to 15% of treated patients. However,
there is no increase in the incidence of infection. Daily
clinical inspection and wound culture, if necessary,
Pediatrics in Review Vol.25 No.12 December 2004 413
injuries burns
should determine when the wound is healed, but such
wounds generally heal in fewer than 2 weeks. Also, the
application of Biobrane by experienced practitioners
can be of value in partial-thickness burns. The product
consists of a coat of cellophane topped by a protein that
adheres to the wound and protects it while healing.
Initial Treatment of a Child Who Has
Extensive Burns
Treatment of a child who has major burn injury consists
of fluid resuscitation to prevent shock, early excision and
grafting of the burn wound coupled with early nutrition
support, identification of airway involvement due to inhalation injury, and measures to treat sepsis. Additionally, with knowledge of the nature of the burn and any
potential chemical exposure or electrical injury, more
specific measures can be taken to diagnose acute complications, such as cardiac arrhythmias, or to use antidotes
for toxic inhalants.1
through a feeding tube. This is known as the Galveston
formula.
Early Excision and Grafting
Early excision and grafting of the burn wound should be
performed at a burn center. The rationale for rapid
closure of all unequivocal deep burns is to reduce wound
infection, fluid loss, and concomitant complications.
Most burn surgeons close deep wounds within 1 to
2 weeks of the injury.
Early and Aggressive Nutrition Support
With early and aggressive nutrition support, burn centers
have been able to reduce the resting energy expenditure
from 1.6 to 2 times normal to less than 1.5 times normal.
Because other processes beyond hypermetabolism, such
as fluid loss, sepsis, and inflammation, contribute to
energy expenditure, intensive nutrition support can help
minimize protein catabolism and weight loss. A highcarbohydrate diet is needed because of the relative inabil-
Initial Management
The victim must be removed from
the scene, the burning extinguished, any jewelry removed
(sources of heat), and in the case
of a chemical burn, any saturated
clothing removed and skin thoroughly irrigated with water, taking care not to spread any chemical to unburned skin. In addition,
the patients chest should be exposed to assess respiratory effort, and pulse should be
obtained. Any accompanying injuries, such as fractures,
also should be assessed. Intravenous access should be
obtained as quickly as possible. Determination of past
medical history, allergies, and current medications at the
scene is advisable if time permits.
Once the nature and extent of injury are assessed, fluid
resuscitation is begun. Fluid administration, usually
through at least two large-bore intravenous catheters,
begins with Ringers lactate 5,000 mL/m2 burned surface area per day, with an additional 2,000 mL/m2 TBSA
per day of Ringers lactate and 5% dextrose for maintenance. The first half of the fluid load is infused over the
first 8 hours postburn; the remainder is infused over the
ensuing 16 hours. The infusion rates should be adjusted
to maintain a urine flow of 1 mL/kg per hour. During
the second 24 hours, fluid administration is reduced to
3,750 mL/m2 surface area burn, with 1,500 mL/m2
TBSA per day as maintenance, which almost always
can be administered in the form of enteral feeding
The
superficial burn wound that extends
to less than 10% TBSA usually can be treated
on an outpatient basis unless abuse is
suspected.
414 Pediatrics in Review Vol.25 No.12 December 2004
ity of the burn victim to use fat, as discussed previously. If
indirect calorimetry is not available, use of the Galveston
formula is recommended:
Infants: 0 to 1 y: 2,100 kcal/m2 plus 1,000 kcal/m2
burn
1 to 11 y: 1,800 kcal/m2 plus 1,300 kcal/m2 burn
12 years and older: 1,500 kcal/m2 plus 1,500 kcal/
m2 burn
Vitamins, minerals, and trace elements are provided
according to the recommended daily intakes. However,
severe burn injury may produce additional requirements,
which have not been investigated completely, including
calcium, magnesium, and vitamin D as well as zinc and,
possibly, other micronutrients. Following burn injury, patients experience hypocalcemia and magnesium depletion,
despite receiving large quantities of enteral and parenteral
calcium and magnesium. This is believed to be due to an
upregulation of the parathyroid gland calcium-sensing receptor, but treatment is limited to providing the minerals in
quantities to cause serum levels to return to normal.
injuries burns
Ileus, decreased blood
pressure and urine
output, anorexia,
irrationality
Wounds
exudative,
macerated
Burn wound biopsy
with >105
organisms per
gram of tissue
Burn wound biopsy
with >105
organisms per
gram of tissue
Wounds develop
focal gangrene
Gradual
onset
Gram-positive
Temperature usually
104F (40C) or
higher
White blood cell count
either low or high;
blood cultures may
be negative
White blood cell count
usually >20 103/
mcL (20 109/L);
blood cultures may
be negative
Temperature increased
or normal, followed
by hypothermia
8 to 12 h
onset
Gram-negative
Features of Bacterial Sepsis Following Large Burns
Table 2.
Sepsis
Burn wound sepsis is defined as the site showing proliferating microorganisms that exceed 105/g tissue and
invasion of underlying unburned tissue. Bacteremia is
indicated by the transient presence of microorganisms in
the blood; sepsis is defined as invasion of the blood by
pathogenic bacteria from local foci of infection, such as
the burn wound. Sepsis frequently is accompanied by
hyperthermia, hypothermia, and prostration.
Table 2 lists the symptoms and signs associated with
sepsis with gram-positive and gram-negative organisms.
Some of the more common infections seen with severe
burn injury include pneumonia, subacute bacterial endocarditis, catheter infections, thrombophlebitis, suppura-
Ileus, decreased blood
pressure and urine
output, obtundation
Recognition of Airway Involvement
A history of closed-space exposure to smoke should raise
suspicion of inhalation injury. Physical signs that are
most suggestive of airway injury are hoarseness and stridor, which indicate partial obstruction of the airway and
a risk for total obstruction. Patients who exhibit these
signs require immediate endotracheal intubation. Patients who are obtunded or comatose may have been
exposed to carbon monoxide, which is diagnosed by
measurement of blood carboxyhemoglobin concentrations. However, the correlation between inhalation injury and symptoms and signs often is poor, which necessitates bronchoscopic examination during evaluation at
the burn center. Intravenous radionuclide scans using
xenon133 can identify small airways that are affected by
inhalation injury. Areas retaining xenon for more than
90 seconds are assumed to be obstructed. Treatment of
inhalation injury is supportive. With combined burn and
inhalation injury, fluid requirements are increased by
40% to 75% in the first 24 hours postinjury. For carbon
monoxide exposure, patients should receive 100% oxygen until the blood carboxyhemoglobin levels are less
than 10%.
Patients who have hypoxia require supplemental oxygen. Chest physiotherapy and spirometry generally are
used to treat airway secretions. Wheezing is an indication
for diagnostic bronchoscopy to determine whether there
is plugging of the airway or bronchospasm and edema. If
there is plugging, therapeutic bronchoscopy and aerosolized heparin and humidification are administered. For
bronchospasm, treatment initially is with nebulized beta2
agonists and, if needed, intravenous aminophylline. If
respiratory failure ensues, the treatments of choice are
intubation, mechanical ventilation, and tracheostomy. If
ventilation remains inadequate, permissive hypercapnia
may stimulate respiratory effort.
Pediatrics in Review Vol.25 No.12 December 2004 415
injuries burns
tive chondritis and sinusitis, urinary tract infections, cholecystitis, and intestinal infections. Antibiotic therapy
should be based on sensitivity of the organism(s) involved.
Prognosis
Despite the seriousness of large burn injury in children,
the prognosis for survival is good and improving steadily.
Recent data analyzed at the United States Army Institute
for Surgical Research showed that adults older than 50
years of age who had burns of less than 50% TBSA
accounted for 19% of the admissions to burn units, but
greater than 50% of the deaths. In contrast, children
younger than 4 years of age who were similarly burned
accounted for 19% of admissions but only 12.5% of the
deaths. Other challenges remain, including physical and
emotional rehabilitation, reconstructive surgery, treatment of the hypermetabolic state with anabolic agents
such as growth hormone, and reintegration of children
into their communities. Work is ongoing in these and
other areas.
Suggested Reading
Herndon DN, ed. Total Burn Care. 2nd ed. London, England:
Saunders; 2002
PIR Quiz
Quiz also available online at www.pedsinreview.org.
1. A 9-month-old boy is brought to the emergency department for burns involving his feet and lower legs.
According to the father, the boy sustained his injuries when he was being bathed in the bathtub and the
father accidentally turned on the hot water. Which of the following is most suggestive of nonaccidental
(child abuse) injury?
A.
B.
C.
D.
E.
Blister formation.
Myoglobinuria.
Pearly white surface.
Splash burns.
Straight-line circumferential burns.
2. You are examining a 1-year-old girl during a health supervision visit. As a part of anticipatory guidance,
you discuss burn injuries in children. Which of the following is the most common source of accidental burn
injuries at this age?
A.
B.
C.
D.
E.
Chemical burns
Contact with hot surfaces.
Electrical burns.
Exposure to microwave.
Spillage of hot liquids.
3. A 4-year-old girl is brought to the emergency department after being rescued from a house fire. Physical
examination shows: rectal temperature 96.8F (36C), heart rate of 100 beats/min, respiratory rate of 24
breaths/min, and blood pressure of 110/70 mm Hg. She has medium-pitched inspiratory stridor and
suprasternal retractions. Air entry is equal on both sides. She is obtunded and responds to painful stimuli
by appropriate withdrawal. Her face is covered with soot. No skin burns are noted. Supplemental oxygen is
provided by a face mask. Pulse oximetry shows an oxygen saturation of 100%. Intravenous access is
obtained. Which of the following is the most appropriate next step?
A.
B.
C.
D.
E.
Administration of 20 mL/kg Ringers lactate.
Computed tomography of head, neck, and chest.
Endotracheal intubation.
Fiberoptic bronchoscopy.
Radionuclide xenon scan.
416 Pediatrics in Review Vol.25 No.12 December 2004
injuries burns
4. An 8-year-old boy is brought to the emergency department after suffering burn injuries while lighting a
firecracker at a backyard barbecue party. Physical examination shows third-degree burns on 60% of his
body surface involving the trunk and lower extremities. His rectal temperature is 96.8F (36C), heart rate
is 180 beats/min, respiratory rate is 48 breaths/min, and blood pressure is 90/60 mm Hg. Which of the
following is the most accurate statement regarding his metabolic state over the next several weeks?
A.
B.
C.
D.
E.
Decreased cortisol level.
Decreased energy requirements.
Increased epinephrine and glucagon levels.
Increased nitrogen retention.
Increased utilization of fat as the energy source.
Note: In the October 2004 issue of Pediatrics in Review, on page 357, question 12 repeated the value PCO2, 50 mm Hg;
one of the values should have been PO2, 50 mm Hg.
Pediatrics in Review Vol.25 No.12 December 2004 417
You might also like
- Burn Injury: Burn Injury Is The Result of Heat Transfer From One Site To AnotherDocument10 pagesBurn Injury: Burn Injury Is The Result of Heat Transfer From One Site To AnotherSachin SinghNo ratings yet
- Burns Practice TeachingDocument58 pagesBurns Practice TeachingSakthi Devi100% (1)
- Physical ExamDocument43 pagesPhysical Examapi-3726369No ratings yet
- Case Pres PartDocument12 pagesCase Pres PartJeannezelle Anne Mariz GazaNo ratings yet
- Askep KGD Luka Bakar TeoriDocument43 pagesAskep KGD Luka Bakar TeoriRiskaNo ratings yet
- Anesthetic Management of Patients With Major Burn InjuryDocument10 pagesAnesthetic Management of Patients With Major Burn InjuryPablo Eduardo AmadorNo ratings yet
- Burns: Review ClassDocument3 pagesBurns: Review ClassEdison BonoNo ratings yet
- Nursing Care of Patients With BURNDocument21 pagesNursing Care of Patients With BURNShuciee ImoedtsNo ratings yet
- A. Background: Preliminary BurnsDocument8 pagesA. Background: Preliminary BurnsFaisal IrhamNo ratings yet
- The White Army-BurnsDocument69 pagesThe White Army-BurnsVishnu PriyaNo ratings yet
- BURNSDocument69 pagesBURNS57- Kalanidhi mNo ratings yet
- BMJ BurnDocument3 pagesBMJ BurnNila SariNo ratings yet
- BURN INJURY CONCEPTS AND DISTINGUISHING ANTEMORTEM FROM POSTMORTEMDocument16 pagesBURN INJURY CONCEPTS AND DISTINGUISHING ANTEMORTEM FROM POSTMORTEMHarwento Eka putraNo ratings yet
- Burns & PoisoningDocument19 pagesBurns & PoisoningFrancis Caster MatutesNo ratings yet
- BURNS MetDocument50 pagesBURNS MetmihikaNo ratings yet
- Environmental and Nutritional Factor in Disease: by Dr. Theresia Indah B, DRG., M.KesDocument48 pagesEnvironmental and Nutritional Factor in Disease: by Dr. Theresia Indah B, DRG., M.KesJay MNo ratings yet
- BURNDocument45 pagesBURNMuhammad Abbas WaliNo ratings yet
- Patel - Physiotherapy in BurnsDocument96 pagesPatel - Physiotherapy in BurnsFaridah saidNo ratings yet
- Burn Injuries and Management - Dr. Ihab AzzamDocument12 pagesBurn Injuries and Management - Dr. Ihab Azzambiii boooNo ratings yet
- Thermal Burns: Risk FactorsDocument21 pagesThermal Burns: Risk FactorsSriarbiatiNo ratings yet
- Pediatric Burn InjuriesDocument12 pagesPediatric Burn Injuriesokwadha simionNo ratings yet
- Classification: by DepthDocument7 pagesClassification: by Depthstephanie_neri_2No ratings yet
- Assessment of Burn Patients Complications and Outcomes From Bihar RegionDocument4 pagesAssessment of Burn Patients Complications and Outcomes From Bihar RegionumeshNo ratings yet
- Trauma and Emergecny Nursing: Course TittleDocument64 pagesTrauma and Emergecny Nursing: Course TittleAbdisamed AllaaleNo ratings yet
- Anestesia en Ninos QuemadosDocument10 pagesAnestesia en Ninos QuemadosMaria Alejandra EchetoNo ratings yet
- Burn management guideDocument36 pagesBurn management guideAshok SabalNo ratings yet
- Luka Bakar (DR Aplin)Document25 pagesLuka Bakar (DR Aplin)Angel TsukiyomiNo ratings yet
- Nursing Management of Patient With BurnsDocument30 pagesNursing Management of Patient With BurnsjsoalNo ratings yet
- Burns: BY Idris Abdulrashid, Department of Nursing Sciences Bayero University KanoDocument44 pagesBurns: BY Idris Abdulrashid, Department of Nursing Sciences Bayero University KanoNaija Nurses TV100% (3)
- Burns An Introduction To Burns and Basic Wound - 2023 - Physician Assistant CliDocument11 pagesBurns An Introduction To Burns and Basic Wound - 2023 - Physician Assistant CliJose AnaconaNo ratings yet
- Burns PresentationDocument34 pagesBurns PresentationMiriam ArchibongNo ratings yet
- Heat Stroke: Early Recognition and Cooling TechniquesDocument13 pagesHeat Stroke: Early Recognition and Cooling TechniquesAniNo ratings yet
- Acute burn managementDocument61 pagesAcute burn managementNara NoroNo ratings yet
- Burns (ALS) History of Present IllnessDocument12 pagesBurns (ALS) History of Present IllnessIlyes FerenczNo ratings yet
- Understanding Burns: Initial Considerations For Burn InjuryDocument14 pagesUnderstanding Burns: Initial Considerations For Burn InjurySanthosh.S.UNo ratings yet
- About BurnsDocument14 pagesAbout BurnsSamNo ratings yet
- Tgs B.inggris 3Document10 pagesTgs B.inggris 3Lisu Ardiyanti PolopadangNo ratings yet
- Introduction To BurnsDocument47 pagesIntroduction To BurnsanushavergheseNo ratings yet
- Types of BurnsDocument10 pagesTypes of BurnsMamata BeheraNo ratings yet
- Jemal Yimam Jibril Berhanu Kalkidan Zenebe: Presented byDocument57 pagesJemal Yimam Jibril Berhanu Kalkidan Zenebe: Presented byVincent SerNo ratings yet
- Sitti Misfiyani Kusuma's VideoDocument18 pagesSitti Misfiyani Kusuma's VideoaniNo ratings yet
- First Aid: BY Prof. A. Emad Omar ZakiDocument31 pagesFirst Aid: BY Prof. A. Emad Omar ZakiMohamedNo ratings yet
- 1 s2.0 S0263931921002404 MainDocument8 pages1 s2.0 S0263931921002404 MainMarina UlfaNo ratings yet
- Burn MonographDocument19 pagesBurn MonographDrMufaddal RampurwalaNo ratings yet
- Burn Treatment and Recovery GuideDocument5 pagesBurn Treatment and Recovery GuideMarcel Quario OrinaNo ratings yet
- Burn in PediatricDocument5 pagesBurn in PediatricAbdulkadir HasanNo ratings yet
- Pamantasan NG Lungsod NG Maynila: (University of The City of Manila)Document23 pagesPamantasan NG Lungsod NG Maynila: (University of The City of Manila)Em Hernandez AranaNo ratings yet
- Advanced Wound Care Awc Industry in IndiaDocument15 pagesAdvanced Wound Care Awc Industry in IndiaSunil KumarNo ratings yet
- Treatment and Prevention of Heat-Related Illness1Document10 pagesTreatment and Prevention of Heat-Related Illness1Karyn AlbaNo ratings yet
- Advances A. BackgroundDocument24 pagesAdvances A. Backgroundalistia andiniNo ratings yet
- Surgical Treatment of BurnsDocument20 pagesSurgical Treatment of BurnsHudiansyahNo ratings yet
- Salinan Terjemahan 91287 - Artikel 4 p2k2Document12 pagesSalinan Terjemahan 91287 - Artikel 4 p2k2anon_659186730No ratings yet
- BurnsDocument69 pagesBurnsMuhammad Umer Farooq NadeemNo ratings yet
- Burn Depth and Survival FactorsDocument59 pagesBurn Depth and Survival Factorsvina zulfianiNo ratings yet
- Rehabilitation Methods For The Burn Injured Individual PDFDocument25 pagesRehabilitation Methods For The Burn Injured Individual PDFNestor BalboaNo ratings yet
- Nursing Manag BURNDocument34 pagesNursing Manag BURNumi margi rahayuNo ratings yet
- Burns: Priyanka JayakumarDocument132 pagesBurns: Priyanka JayakumarPriyankaNo ratings yet
- Classification of BurnsDocument4 pagesClassification of BurnsErtania NirmalaNo ratings yet
- JOP 28 Mar-01 Apr - WYDocument6 pagesJOP 28 Mar-01 Apr - WYBell SwanNo ratings yet
- E PosterDocument2 pagesE PosterBell SwanNo ratings yet
- Colonic StenosisDocument3 pagesColonic StenosisBell SwanNo ratings yet
- Are Routine Dilatations Necessary PostDocument6 pagesAre Routine Dilatations Necessary PostBell SwanNo ratings yet
- CAT Jurnal ReadingDocument9 pagesCAT Jurnal ReadingBell SwanNo ratings yet
- Jss 03 02 193Document11 pagesJss 03 02 193Bell SwanNo ratings yet
- Medicine: Full-Endoscopic Discectomy Via The Interlaminar Approach For Disc Herniation at L4-L5 and L5-S1Document7 pagesMedicine: Full-Endoscopic Discectomy Via The Interlaminar Approach For Disc Herniation at L4-L5 and L5-S1Bell SwanNo ratings yet
- Journal Reading: Dr. Firdaus RamliDocument22 pagesJournal Reading: Dr. Firdaus RamliBell SwanNo ratings yet
- HIP Joint AnatomyDocument4 pagesHIP Joint AnatomyBell SwanNo ratings yet
- Slipped Capital Femoral Epiphysis: MSC Otho, MRCS Assistant Lecturer of Orthopaedic at Ain Shams UniversityDocument30 pagesSlipped Capital Femoral Epiphysis: MSC Otho, MRCS Assistant Lecturer of Orthopaedic at Ain Shams UniversityBell Swan100% (1)
- Assessment Oncology KoassDocument4 pagesAssessment Oncology KoassBell SwanNo ratings yet
- MainDocument9 pagesMainBell SwanNo ratings yet
- Baby with abdominal distension and suspected Hirschsprung's diseaseDocument12 pagesBaby with abdominal distension and suspected Hirschsprung's diseaseBell SwanNo ratings yet
- Bab10 InflammatoryDisordersofBonesandJoints PDFDocument50 pagesBab10 InflammatoryDisordersofBonesandJoints PDFBell SwanNo ratings yet
- Romiyo/ MALE/21 Yo: Thursday, 10 TH January 2014Document13 pagesRomiyo/ MALE/21 Yo: Thursday, 10 TH January 2014Bell SwanNo ratings yet
- CoverDocument1 pageCoverBell SwanNo ratings yet
- Data LabDocument3 pagesData Labyun chae rinNo ratings yet
- LaporanDocument1 pageLaporanBell SwanNo ratings yet
- Data LabDocument3 pagesData Labyun chae rinNo ratings yet
- Data LabDocument3 pagesData Labyun chae rinNo ratings yet
- Full Download Holes Human Anatomy and Physiology 15th Edition Shier Solutions ManualDocument35 pagesFull Download Holes Human Anatomy and Physiology 15th Edition Shier Solutions Manualbarovert.o87w100% (29)
- Aip Summer 2017 PDFDocument116 pagesAip Summer 2017 PDFShibli KushtiaNo ratings yet
- Phylum Platyhelminthes Phylum Nematoda Phylum MolluscaDocument44 pagesPhylum Platyhelminthes Phylum Nematoda Phylum MolluscaAngel FebiolaNo ratings yet
- 4BI0 1B Que 20130523Document28 pages4BI0 1B Que 20130523traphouse982No ratings yet
- Lab Report - Smooth MuscleDocument8 pagesLab Report - Smooth MuscledhebbertNo ratings yet
- Classification and Types of StrokeDocument11 pagesClassification and Types of StrokeJose Enrique OrtizNo ratings yet
- NO Nama Alat Jumlah Kondisi Baik RusakDocument6 pagesNO Nama Alat Jumlah Kondisi Baik RusakRumah Sakit Umum KartiniNo ratings yet
- Frog Dissection (Remote)Document21 pagesFrog Dissection (Remote)Mohammad NiyaifarNo ratings yet
- The Problem and Its BackgroundDocument43 pagesThe Problem and Its BackgroundkjjkjkljkjjklNo ratings yet
- Osmosis Lab DiscussionDocument2 pagesOsmosis Lab Discussionsoha zubairNo ratings yet
- 3 Piece Intrusion Arch - Bhavana ShroffDocument8 pages3 Piece Intrusion Arch - Bhavana ShroffSai Seshadri Bharath ThotaNo ratings yet
- Generalized Calcinosis Cutis Associated With Probable Leptospirosis in A Dog (Pages 401-406)Document6 pagesGeneralized Calcinosis Cutis Associated With Probable Leptospirosis in A Dog (Pages 401-406)jenNo ratings yet
- Nexgen Complete Knee Solution Epicondylar Instrumentation Surgical Technique For Legacy Posterior Stabalized Knees Surgical TechniqueDocument32 pagesNexgen Complete Knee Solution Epicondylar Instrumentation Surgical Technique For Legacy Posterior Stabalized Knees Surgical TechniqueTudor MadalinaNo ratings yet
- Unit I Clothing Science Two Marks With Answer and Question BankDocument3 pagesUnit I Clothing Science Two Marks With Answer and Question BankSivakumar KNo ratings yet
- E147 Full PDFDocument21 pagesE147 Full PDFcahyatiNo ratings yet
- Football Interval Throwing ProgramDocument2 pagesFootball Interval Throwing ProgrammilitaruandreiNo ratings yet
- 22.3 Anatomy Study Resources - A PDFDocument3 pages22.3 Anatomy Study Resources - A PDFNothingNo ratings yet
- Understanding CLL: A Guide For Patients Who Want To Take Charge of Chronic Lymphocytic LeukemiaDocument4 pagesUnderstanding CLL: A Guide For Patients Who Want To Take Charge of Chronic Lymphocytic LeukemiaNakul Singh ParkwayIndiaNo ratings yet
- Data Interpret-Medical StudentsDocument606 pagesData Interpret-Medical StudentsIrfan Ali100% (4)
- Abdominals: Ab Crunch MachineDocument24 pagesAbdominals: Ab Crunch Machinearies_02No ratings yet
- Pathomorphology Final ExamDocument262 pagesPathomorphology Final ExamMann SarwanNo ratings yet
- Chapter 3 - Sensation and PerceptionDocument40 pagesChapter 3 - Sensation and PerceptionKaiNo ratings yet
- DR - BD S Step 1 Guide - PDF Filename UTF-8 DR - BD S Step 1 GuideDocument24 pagesDR - BD S Step 1 Guide - PDF Filename UTF-8 DR - BD S Step 1 GuideAdeelMunawarNo ratings yet
- CCDocument4 pagesCCJaymih Santos AbasoloNo ratings yet
- Plant Transport Vascular BundlesDocument31 pagesPlant Transport Vascular BundlesJoel RobinsonNo ratings yet
- Case StudyDocument3 pagesCase StudyAnonymous Gof8o3No ratings yet
- Nephrology Block Ia. History: A. InformantDocument4 pagesNephrology Block Ia. History: A. InformantKatherine FabrosNo ratings yet
- Sleep Studies: in The Sleep Laboratory and in The Home: Patient EducationDocument2 pagesSleep Studies: in The Sleep Laboratory and in The Home: Patient EducationALINo ratings yet
- BiobutanolDocument11 pagesBiobutanolPabloDoriaNo ratings yet
- Trauma y Memoria Procedural 2015 Paper Peter LevineDocument18 pagesTrauma y Memoria Procedural 2015 Paper Peter LevineMaría Regina Castro CataldiNo ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (13)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 3.5 out of 5 stars3.5/5 (2)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 5 out of 5 stars5/5 (3)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsNo ratings yet
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- Daniel Kahneman's "Thinking Fast and Slow": A Macat AnalysisFrom EverandDaniel Kahneman's "Thinking Fast and Slow": A Macat AnalysisRating: 3.5 out of 5 stars3.5/5 (130)
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 5 out of 5 stars5/5 (4)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (327)
- Troubled: A Memoir of Foster Care, Family, and Social ClassFrom EverandTroubled: A Memoir of Foster Care, Family, and Social ClassRating: 4.5 out of 5 stars4.5/5 (22)
- The Happiness Trap: How to Stop Struggling and Start LivingFrom EverandThe Happiness Trap: How to Stop Struggling and Start LivingRating: 4 out of 5 stars4/5 (1)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 3.5 out of 5 stars3.5/5 (31)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- Summary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisFrom EverandSummary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisRating: 5 out of 5 stars5/5 (3)