Professional Documents
Culture Documents
2
Uploaded by
JHon Hendrik TambunanCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
2
Uploaded by
JHon Hendrik TambunanCopyright:
Available Formats
Remote Nursing Certified Practice Adult Decision Support Tools: ACUTE BRONCHITIS
This decision support tool is effective as of October 2014. For more information or to provide feedback on
this or any other decision support tool, e-mail certifiedpractice@crnbc.ca
ADULT ACUTE BRONCHITIS
DEFINITION
Inflammation of trachea and bronchi (larger airways)
Potential Causes
Viral infection: 90% of cases
Influenza A or B, adenovirus, rhinovirus, para-influenzae, corona virus, Respiratory
Syncytial Virus (RSV), human metapneumovirus
Bacterial infection: 10% of cases
Mycoplasma pneumoniae, Chlamydia pneumoniae, Bordetella pertussis possible causes
Streptococcus pneumoniae and H. Influenziae usually only causative organisms if there is
underlying lung disease
Predisposing Risk Factors
Chronic sinusitis
Chronic Obstructive Pulmonary Disease (COPD)
Asthma
Bronchiectasis
Immunocompromised (chronic asthma)
Smoking
Second hand smoke
Air pollutants, environmental factors
Alcoholism
Gastro Esophageal Reflux Disease (GERD)
Wood stoves
Mould
Typical Findings of Acute Bronchitis
Initially the presentation of acute bronchitis is difficult to distinguish from an Upper Respiratory
Tract Infection (URTI).
Later the presentation of acute bronchitis and pneumonia are often similar. In general, clients
with pneumonia are sicker and usually have more chest abnormalities.
CRNBC monitors and revises the CRNBC certified practice decision support tools (DSTs) every two years and as necessary based
on best practices. The information provided in the DSTs is considered current as of the date of publication. CRNBC-certified nurses
(RN(C)s) are responsible for ensuring they refer to the most current DSTs.
The DSTs are not intended to replace the RN(C)'s professional responsibility to exercise independent clinical judgment and use
evidence to support competent, ethical care. The RN(C) must consult with or refer to a physician or nurse practitioner as
appropriate, or whenever a course of action deviates from the DST.
THIS DST IS FOR USE BY REGISTERED NURSES CERTIFIED BY CRNBC
CRNBC October 2014/Pub. 740 1
Remote Nursing Certified Practice Adult Decision Support Tools: ACUTE BRONCHITIS
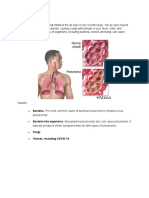
The organisms that cause bronchitis can also cause pneumonia. The difference is in where the
infection lies anatomically. Bronchitis involves the larger airways, whereas pneumonia involves
the smaller airways and air sacs.
History
Previous infection of Upper Respiratory Tract (URT)
General malaise
Fever
Cough: initially dry, later productive of white, yellow or green sputum
Cough for more than 5 days
- Cough often lasts 10-20 days
- 45% still have a cough after two weeks, and 25% still have a cough after 3 weeks
Muscular aching in the chest wall or discomfort with coughing
Wheezing may be present
PHYSICAL ASSESSMENT
Temperature may be mildly to moderately elevated
Pulse may be mildly elevated if febrile
Respirations may be slightly elevated
Purulent sputum is common in 50% of cases
Rhinitis may be present
Expiratory phase may be slightly prolonged
Wheezes (scattered, low pitched) may be present
Abnormal vital signs (fever, tachypnea or tachycardia) and signs of consolidation or rales on
physical exam suggest the possibility of pneumonia
Diagnostic tests
Electrocardiogram (ECG), Culture and Sensitivity (C&S) of sputum
Consider swab for pertussis, particularly if cough lasts more than 6 days and is accompanied
by vomiting
Consider Tuberculosis (TB) skin test for cough greater than 2 weeks and in high risk or
susceptible populations
MANAGEMENT AND INTERVENTIONS
Goals of Treatment
Relieve symptoms (coughing, fever)
Prevent pneumonia
Non-pharmacological interventions
Increased rest (especially if febrile)
Adequate hydration (8-10 glasses of fluid per day)
Increased humidity in the environment
Avoidance of pulmonary irritants (e.g., stop or decrease smoking)
THIS DST IS FOR USE BY REGISTERED NURSES CERTIFIED BY CRNBC 2
CRNBC October 2014/Pub. 740
Remote Nursing Certified Practice Adult Decision Support Tools: ACUTE BRONCHITIS
PHARMACOLOGICAL INTERVENTIONS
To manage fever or pain
- Acetaminophen 325 mg 1-2 tabs po q4-6h prn
OR
- Ibuprofen 200 mg 1-2 tabs po q4-6h prn
If bronchospasm, dyspnea or wheezing is significant, short-acting 2-agonist bronchodilators
can be used until acute symptoms resolve
- Salbutamol 100mcg Metered-Dose Inhaler (MDI) 1 or 2 puffs q4h prn via aero chamber-
maximum dose of 8 puffs/day
Avoid antibiotics
In most cases, antibiotics are not recommended for acute bronchitis in an otherwise healthy
client, as the cause is usually viral.
- Antibiotics may be considered in those at high risk of serious complications because of
pre-existing co-morbidity (heart, lung, renal, liver, or neuromuscular disease, Congestive
Heart Failure, diabetes mellitus, current use of oral glucocorticoids,
immunocompromised)
- In clients with an acute bronchitis overlying chronic bronchitis, antibiotics may be
considered for clients who have two or more of the following symptoms:
Increased sputum volume
Increased sputum purulence
Increased dyspnea
Choices:
- Amoxicillin 500 mg po tid for 5-7 days
OR
- Doxycycline 200 mg once, then 100 mg po bid for 5-7 days
OR
- Trimethoprim 160 mg / Sulphamethoxazole 800 mg (DS) po bid for 5-7 days
Pregnant or Breastfeeding Women:
- Amoxicillin may be used as listed above.
- DO NOT USE doxycycline and Trimethoprim 160 mg / Sulphamethoxazole 800 mg.
Potential Complications
Pneumonia
Post-bronchitis cough
Client Education and Discharge Information
Recommend hand washing to prevent spread of infection throughout a household
Inform client that cough may persist for more than 2 weeks
Inform client that routine antibiotic therapy is not necessary or recommended
THIS DST IS FOR USE BY REGISTERED NURSES CERTIFIED BY CRNBC 3
CRNBC October 2014/Pub. 740
Remote Nursing Certified Practice Adult Decision Support Tools: ACUTE BRONCHITIS
Monitoring and Follow-Up
Arrange for follow up in 2-3 days if antibiotics are used and the clients condition is not
resolving.
Consultation and/or Referral
Consult with or refer to physician and/or nurse practitioner if unresponsive to treatment or if
pneumonia is suspected.
Documentation
As per agency policy.
REFERENCES
For help obtaining any of the items on this list, please contact CRNBC Helen Randal Library at
circdesk@crnbc.ca
More recent editions of any of the items in the Reference List may have been published since
this DST was published. If you have a newer version, please use it.
Balter, M. S., La Forge, J., Low, D. E., Mandell, L., & Grossman, R. F. (2003). Canadian
guidelines for the management of acute exacerbations of chronic bronchitis. Canadian
Respiratory Journal, 10 (Suppl B), 3B-32B.
Blondel-Hill, E., & Fryters, S. (2012). Bugs and drugs: An antimicrobial infectious diseases
reference. Edmonton, AB: Alberta Health Services.
Blush III, R. R. (2013). Acute bronchitis. Nurse Practitioner, 38(10), 14-20.
Canadian Pharmacists Association. (2011). Therapeutic choices (6th ed.). Ottawa, ON: Author.
Carolan, P. L. (2014, March 18). Pediatric bronchitis. Retrieved from
http://www.emedicine.com/ped/topic288.htm
Cash, J. C., & Glass, C. A. (Eds.). (2014). Family practice guidelines (3rd ed.). New York, NY:
Springer.
Chen, Y. A., & Tran, C. (Eds.). (2011). The Toronto notes 2011: Comprehensive medical
reference and review for the Medical Council of Canada Qualifying Exam Part 1 and the
United States Medical Licensing Exam Step 2 (27th ed.). Toronto, ON: Toronto Notes for
Medical Students.
DynaMed. (2014, April 17). Acute bronchitis. Retrieved from
http://search.ebscohost.com/login.aspx?direct=true&AuthType=cpid&custid=s5624058&
db=dme&AN=113814
THIS DST IS FOR USE BY REGISTERED NURSES CERTIFIED BY CRNBC 4
CRNBC October 2014/Pub. 740
Remote Nursing Certified Practice Adult Decision Support Tools: ACUTE BRONCHITIS
Esherick, J. S., Clark, D. S., & Slater, E. D. (2012). Current practice guidelines in primary care
2012. New York, NY: McGraw-Hill Medical.
Fayyaz, J. (2014, March 28). Bronchitis. Retrieved from
http://www.emedicine.com/emerg/topic69.htm
Kuehn, B. M. (2013). Excessive antibiotic prescribing for sore throat and acute bronchitis
remains common. JAMA: The Journal of the American Medical Association, 310(20),
2135-2136.
Tackett, K. L., & Atkins, A. (2012). Evidence-based acute bronchitis therapy. Journal of
Pharmacy Practice, 25(6), 586-590.
THIS DST IS FOR USE BY REGISTERED NURSES CERTIFIED BY CRNBC 5
CRNBC October 2014/Pub. 740
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Croup: Straight To The Point of CareDocument36 pagesCroup: Straight To The Point of CareNana OkujavaNo ratings yet
- Suppurative Lung DiseasesDocument39 pagesSuppurative Lung Diseasesmatchees-gone rogueNo ratings yet
- Vaccine: Greg G. WolffDocument5 pagesVaccine: Greg G. WolffRennan Lima M. CastroNo ratings yet
- Croup Diagnosis and Management 2018Document6 pagesCroup Diagnosis and Management 2018Jose Fernando DiezNo ratings yet
- Rhu Matalam Pending 2nd Dose 10.01.2021Document1,402 pagesRhu Matalam Pending 2nd Dose 10.01.2021aleiah jean libatiqueNo ratings yet
- Acute Bronchiolitis: Zakaria Omar Elzwie Najwa Abdulallah Alfergany (Mub) NovemberDocument28 pagesAcute Bronchiolitis: Zakaria Omar Elzwie Najwa Abdulallah Alfergany (Mub) Novemberزكريا عمرNo ratings yet
- Respiratory Case StudiesDocument2 pagesRespiratory Case Studiesk_manchesterNo ratings yet
- Sedentary Issue47Document6 pagesSedentary Issue47Tang TreyNo ratings yet
- When Well What Should I Do?: Call An Ambulance On 000Document2 pagesWhen Well What Should I Do?: Call An Ambulance On 000Sophia RoseNo ratings yet
- NCP For Bronchopneumonia With 7 Nursing DiagnosisDocument4 pagesNCP For Bronchopneumonia With 7 Nursing DiagnosisBeng AlontoNo ratings yet
- PULMODocument3 pagesPULMOGianna Louisse Marie Dacalos DiazNo ratings yet
- Tabel SKDR 2022Document4 pagesTabel SKDR 2022Basroni FaizalNo ratings yet
- G1 Health Teaching PlanDocument4 pagesG1 Health Teaching Planbernadil01No ratings yet
- Pneumonia in PlabDocument6 pagesPneumonia in PlabBeaulahNo ratings yet
- Ob2 Sas 26Document9 pagesOb2 Sas 26????No ratings yet
- Employees Health Declaration FormDocument1 pageEmployees Health Declaration FormELENITA VILLANo ratings yet
- Everything You Need to Know About CoughsDocument12 pagesEverything You Need to Know About CoughsLany T. CataminNo ratings yet
- NCPDocument4 pagesNCPMarius Clifford BilledoNo ratings yet
- Makalah B. Inggris SputumDocument8 pagesMakalah B. Inggris SputumDian FaqihNo ratings yet
- Bronchitis (Biochem Presentation)Document42 pagesBronchitis (Biochem Presentation)SiewLiZhenNo ratings yet
- Bacteria. The Most Common Cause of Bacterial Pneumonia Is StreptococcusDocument4 pagesBacteria. The Most Common Cause of Bacterial Pneumonia Is StreptococcusLouise OpinaNo ratings yet
- OrthomyxovirusDocument28 pagesOrthomyxoviruskiedd_04No ratings yet
- Recognizing Interstitial Versus Airspace Disease Recognizing Interstitial Versus Airspace DiseaseDocument30 pagesRecognizing Interstitial Versus Airspace Disease Recognizing Interstitial Versus Airspace DiseaseYoga KharismaNo ratings yet
- Vi. Ûrxm: ®vôtôw ® Øû/LsDocument4 pagesVi. Ûrxm: ®vôtôw ® Øû/Lsbgk_usNo ratings yet
- NCPPDocument11 pagesNCPPAngelo Miguel MuñozNo ratings yet
- 3 NCP Form (1) (5) .Docareway NoorDocument3 pages3 NCP Form (1) (5) .Docareway NoorALI-A ALINo ratings yet
- Respiratory PathophysiologyDocument17 pagesRespiratory PathophysiologyJohn Christopher LucesNo ratings yet
- Recurrent Pneumonia in Children: A Systematic Diagnostic ApproachDocument35 pagesRecurrent Pneumonia in Children: A Systematic Diagnostic ApproachVishal SidanaNo ratings yet
- Laporan Harian Pasien Puskesmas JatinegaraDocument8 pagesLaporan Harian Pasien Puskesmas JatinegaraanggaNo ratings yet
- 2ms Third ExamDocument2 pages2ms Third ExamGood ChanceNo ratings yet