Professional Documents
Culture Documents
Emergency and Disaster Nursing
Uploaded by
Nina Oaip0 ratings0% found this document useful (0 votes)
282 views19 pagesemergency nursing
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentemergency nursing
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
282 views19 pagesEmergency and Disaster Nursing
Uploaded by
Nina Oaipemergency nursing
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 19
EMERGENCY AND DISASTER NURSING Mass Casualty Incident - situation in which the number of INCIDENT COMMANDER - The head
of INCIDENT COMMANDER - The head of the incident
casualties exceeds the number of resources. command system
TERMS USE:
Post Traumatic Stress Syndrome - characteristic of He must be continuously informed of all the
Trauma - Intentional or unintentional wounds/injuries on symptoms after a psychologically stressful event was out activities and informed about any deviation from
the human body from particular mechanical mechanism
of range of an normal human experience. the established plan
that exceeds the bodys ability to protect itself from injury
EMERGENCY IT IS WHATEVER THE PATIENT OR THE
Emergency Management - traditionally refers to care
FAMILY CONSIDERS IT TO BE. SCOPE AND PRACTICE OF EMERGENCY NURSING
given to patients with urgent and critical needs. The emergency nurse has had specialized
EMERGENCY NURSING - It is the nursing care given to
Triage - process of assessing patients to determine education, training, and experience.
patients with urgent and critical needs
management priorities. The emergency nurse establishes priorities,
EMERGENCY NURSE - has a specialized education, training, monitors and continuously assesses acutely ill and
First Aid - an immediate or emergency treatment given to and experience to gain expertise in assessing and
a person who has been injured before complete medical injured patients, supports and attends to families,
identifying patients health care problems in crisis supervises allied health personnel, and teaches
and surgical treatment can be secured. situations patients and families within a time-limited, high-
BLS - level of medical care which is used for patient with establishes priorities, monitors and continuously pressured care environment.
illness or injury until full medical care can be given. assesses acutely ill and injured patients, supports
Nursing interventions are accomplished
ACLS ADVANCE CARDIAC LIFE SUPPORT- Set of clinical and attends to families, supervises allied health interdependently, in consultation with or under
interventions for the urgent treatment of cardiac arrest personnel, and teaches patients and families the direction of a licensed physician.
and often life threatening medical emergencies as well as within a time-limited, high-pressured care
the knowledge and skills to deploy those interventions. environment Appropriate nursing and medical interventions are
anticipated based on assessment data.
Defibrillation - Restoration of normal rhythm to the heart DISASTER NURSING - a branch of emergency nursing, it
in ventricular or atrial fibrillation refers to nursing care given to patients who are victims of The emergency health care staff members work as
disasters, whether it is manmade or natural phenomena. a team in performing the highly technical, hands-
Disaster - Any catastrophic situation in which the normal on skills required to care for patients in an
patterns of life (or ecosystems) have been disrupted and emergency situation.
INCIDENT COMMAND SYSTEM - It is a management tool
extraordinary, emergency interventions are required to
for organizing personnel, facilities, equipment, and
save and preserve human lives and/or the environment.
communication for any emergency situation.
Patients in the ED have a wide variety of actual or Good Samaritan Law Stages of Crisis
potential problems, and their condition may 1. Anxiety and Denial
change constantly. Gives legal protection to the rescuer who encouraged to recognize and talk about their
act in good faith and are not guilty of gross feelings.
Although a patient may have several diagnosis at a negligence or willful misconduct. asking questions is encouraged.
given time, the focus is on the most life- honest answers given
threatening ones Focus of Emergency Care
prolonged denial is not encouraged or supported
Preserve or Prolong Life 2. Remorse and Guilt
ISSUES IN EMERGENCY NURSING CARE
Alleviate Suffering verbalize their feelings
Emergency nursing is demanding because of the Do No Further Harm 3. Anger
diversity of conditions and situations which are Restore to Optimal Function way of handling anxiety and fear
unique in the ER. allow the anger to be ventilated
4. Grief
Issues include legal issues, occupational health and Golden Rules of Emergency Care
help family members work through their grief
safety risks for ED staff, and the challenge of
Dos letting them know that it is normal and acceptable
providing holistic care in the context of a fast-
- Obtain Consent Core Competencies in Emergency Nursing
paced, technology-driven environment in which
- Think of the Worst Assessment
serious illness and death are confronted on a daily
- Respect Victims Modesty & Privacy Priority Setting/Critical Thinking Skills
basis.
Donts Knowledge of Emergency Care
The emergency nurse must expand his or her - let the patient see his own injury Technical Skills
knowledge base to encompass recognizing and - Make any unrealistic promises Communication
treating patients and anticipate nursing care in the
event of a mass casualty incident. Guidelines in Giving Emergency Care Assess and Intervene
A Ask for help Check for ABCs of life
Legal Issues Includes: I Intervene A Airway
D Do no Further Harm B Breathing
Actual Consent
C - Circulation
Implied Consent
Team Members
Parental Consent
Rescuer
Emergency Medical Technician
Paramedics Estimated Blood Pressure - Re-evaluate clients LOC
Emergency Medicine Physicians - Use AVPU mnemonics
SITE SBP
Incident Commander E Exposure
Support Staff Radial 80 - Remove clothing
Inpatient Unit Staff - Maintain Privacy
- Prevent Hypothermia
Emergency Action Principle
I. Survey the Scene III. Activate Medical Assistance
Is the Scene Safe? Femoral 70 Information to be Relayed:
What Happened? What Happened?
Are there any bystanders who can help? Number of Persons Injured
identify as a trained first aider! Extent of Injury and First Aid given
Telephone number from where youre calling
II. Do a Primary Survey - organization of approach so that
immediate threats to life are rapidly identified and Carotid 60
IV. Do Secondary Survey
effectively manage.
Interview the Patient
Primary Survey S Symptoms
A - Airway/Cervical Spine A Allergies
- Establish Patent Airway Control of Hemorrhage M Medication
- Maintain Alignment P Previous/Present Illness
- GCS 8 = Prepare Intubation L Last Meal Taken
B Breathing E Events Prior to Accident
- Assess Breath Sounds Check Vital Signs
- Observe for Chest Wall Trauma
- Prepare for chest decompression
C Circulation
- Monitor VS V. Triage
- Maintain Vascular Access D Disability
- Direct Pressure - Evaluate LOC
comes from the French word trier, meaning to Upper extremity fractures, minor burns, sprains, 5. Fast-Track:
sort small lacerations without significant bleeding, Psychological support needed
process of assessing patients to determine behavioral disorders or psychological
management priorities disturbances. FIRST AID
Categories: Role of First Aid
1. Emergent - highest priority, conditions are life TRIAGE PRIORITY COLOR Bridge the Gap Between the Victim and the
CATEGORY
threatening and need immediate attention Physician
IMMEDIATE 1 RED
Immediately start giving interventions in pre-
Airway obstruction, sucking chest wound, shock, DELAYED 2 YELLOW hospital setting
unstable chest and abdominal wounds, open MINIMAL 3 GREEN
Value of First Aid Training
fractures of long bones EXPECTANT 4 BLACK
Self-help
2. Urgent have serious health problems but not Health for Others
immediately life threatening ones. Must be seen Field TRIAGE Preparation for Disaster
within 1 hour 1. Immediate: Safety Awareness
Injuries are life-threatening but survivable with
Maxillofacial wounds without airway compromise, minimal intervention. Individuals in this group can
eye injuries, stable abdominal wounds without progress rapidly to expectant if treatment is BASIC LIFE SUPPORT - an emergency procedure that
evidence of significant hemorrhage, fractures delayed. consists of recognizing respiratory or cardiac arrest or both
2. Delayed: the proper application of CPR to maintain life until a victim
3. Non-urgent patients have episodic illness than recovers or advance life support is available.
Injuries are significant and require medical care,
can be addressed within 24 hours without
but can wait hours without threat to life or limb. Artificial Respiration
increased morbidity
Individuals in this group receive treatment only
Upper extremity fractures, minor burns, sprains, a way of breathing air to persons lungs when
after immediate casualties are treated.
small lacerations without significant bleeding, breathing ceased or stopped function.
3. Minimal:
behavioral disorders or psychological
Injuries are minor and treatment can be delayed
disturbances.
hours to days. Individuals in this group should be
3. Non-urgent patients have episodic illness than
moved away from the main triage area.
can be addressed within 24 hours without
4. Expectant:
increased morbidity
Injuries are extensive and chances of survival are Respiratory Arrest
unlikely even with definitive care.
a condition when the respiration or breathing Table of Cardiopulmonary Resuscitation for Adult, Child Open the Check for foreign bodies then remove
pattern of an individual stops to function, while & Infant Airway using finger sweep
Head-tilt-chin-lift maneuver
the pulse and circulation may continue.
Adult Child Infant Jaw-thrust Maneuver
Causes: Choking, Electrocution, strangulation, drowning Compression Lower half of the Lower half of Lower half of
Assess for Bring cheek over the mouth and nose
Area sternum but not the sternum the sternum
and suffocation. hitting the xiphoid but not hitting but not hitting
Breathing of the casualty
process: measure the xiphoid the xiphoid Look for chest movement
up to 2 fingers process: process: 1 Listen for breath sounds
from substernal measure up to finger width Feel for breathing on your cheek
WAYS TO VENTILATE THE LUNGS notch. 1 finger from below the The Casualty is NOT Breathing:
substernal imaginary
1. MOUTH-TO-MOUTH = a quick, effective way to notch. nipple line.
Go for Help if someone responds to your shout for
provide O2 and ventilation to the victim. Depth Approximately 1 Approximately Approximately
help send that person to phone for
to 2 inches 1 to 1 inches to 1 inch
2. MOUTH-TO-NOSE = recommended when it is How to Heel of 1 hand, Heel of 1 hand. 2 fingers ambulance
impossible to ventilate through the victims compress other hand on (middle & ring if youre on your own, leave the
mouth. (Trismus, mouth injury) top. fingertips) casualty and make the phone call for
Compression 30:2 (1 or 2 30:2 (1 or 2 30:2 (1 or 2 yourself
3. MOUTH-TO-NOSE and MOUTH = if the pt. is an -ventilation rescuers) rescuers) rescuers) * never leave if the patient has collapsed as a
infant ratio result of trauma or drowning or if the casualty is
Number of 5 cycles in 2 5 cycles in 2 5 cycles in 2 a child
4. MOUTH-TO-STOMA = used if the pt. has a stoma; a
cycles per minutes minutes minutes Give Rescue 5 rescue breaths 2 rescue
permanent opening that connects the trachea minute
Breaths breaths
directly to the front of the neck.
Place mouth pinch nose seal lips around
Procedure Infant(0-1yr) over the nose and the mouth and
For Rescue Breathing Alone: Child(1-8 Adult
and mouth of ventilate via blow steadily
yrs)
Rate is 10-12 breaths in ADULT the infant mouth for 1.5 2
seconds
(1.5 - 2 sec/breath) ( 1 breath every 4 to 5 secs) Safe Approach and assess situation look for chest look for look for chest
Rate is 20 breaths for a CHILD and INFANT Approach rising chest rising rising
(1 1.5 sec/breath) ( 1 breath every 3 secs) Assess for Shout and gently pinch Gently
Response shouting
are you
ok? then
shake the
victim
Positioning Placed Supine on a firm and flat surface
With your other hand grasp the far thigh just When to STOP CPR:
above the knee, then pull the casualty towards
S SPONTANEOUS BREATH RESTORED
you and on to his or her side
T TURNED OVER THE MEDICAL SERVICES
O OPERATOR IS EXHAUSTED TO CONTINUE
CRITERIA FOR NOT STARTING CPR
P PHYSICIAN ASSUMES RESPONSIBILITY
- All patients in cardiac arrest receive resuscitation
unless:
1. The pt. has a valid DNR order COMPLICATIONS OF CPR:
2. The pt. has signs of irreversible death: rigor mortis,
livor mortis, algor mortis, decapitation RIB FRACTURE
3. No physiological benefit can be expected because STERNUM FRACTURE
the vital functions have deteriorated despite LACERATION OF THE LIVER OR SPLEEN
maximal therapy PNEUMOTHORAX, HEMOTHORAX
4. Witholding attempts to resuscitate in the DR is
appropriate for newly born infants with: CHAIN OF SURVIVAL
EARLY ACCESS early recognition of cardiac
- Confirmed gestation less than 23 weeks or
arrest, prompt activation of emergency services
birthweight less than 400 grams
EARLY BLS prevent brain damage, buy time for
- Anencephaly the arrival of defibrillator
When to Stop EARLY DEFIBRILLATION - 7-10% decrease per
when the patient has spontaneous breathing minute without defibrillation
The Casualty is Breathing: EARLY ACLS technique that attempts to stabilize
when the first aider is too exhausted to continue
Place in recovery position patient
when another first aider takes over
Before moving casualty remove any objects safely
when EMS arrives and takes over
from her pockets
Kneel beside casualty, place arm nearest at right
angles, and then bend elbow keeping the palm
uppermost.
Bring far arm across the casualtys chest and hold
back of the casualtys hand against the nearest
cheek
AIRWAY OBSTRUCTION For patient lying (unconscious): D. ENDOTRACHEAL INTUBATION
position patient at the back (supine); kneel astride Indications:
KINDS OF AIRWAY OBSTRUCTION: the patients thigh To establish an airway for patients cannot be
1. Anatomic Airway Obstruction Place HEEL of one HAND against the pts adequately ventilated with an oropharyngeal
2. Mechanical Airway Obstruction abdomen, place the second hand directly on the airway
top of the fist. To bypass upper airway obstruction
TYPES OF AIRWAY OBSTRUCTION Make a quick UPWARD thrust To permit connection to ambubag or mechanical
1. Partial Airway Obstruction with Good Air Exchange ventilator
2. Partial Airway Obstruction with Poor Air Exchange FINGER SWEEP: used only in unconscious adult client To prevent aspiration
3. Complete Airway Obstruction Make a TONGUE-JAW LIFT. Opening the pts To facilitate removal of tracheobronchial
mouth by grasping both tongue and lower jaw secretions
Clinical Manifestations: UNIVERSAL DISTRESS SIGNAL between the thumb and fingers, and lifting the
(patient may clutch the neck between the thumb and mandible. E. CRICOTHYROIDOTOMY
fingers), choking, stridor, apprehensive appearance, Insert index finger of other hand to scrape across a puncture or incision of the cricothyroid
restlessness. CYANOSIS and LOSS of CONSCIOUSNESS the back of the throat membrane to establish an emergency airway in
develop as hypoxia worsens. Use a hooking action certain emergency situations where endotracheal
intubation or tracheostomy is not possible.
CHEST THRUST: used only in patients in advanced stages of indicated to pts. with trauma to head and neck,
MANAGEMENT FOR AIRWAY OBSTRUCTION pregnancy or in markedly obese clients and in allergic reaction causing laryngeal edema
a. Conscious Patient standing or sitting use of gauge 11 needle or scalpel blade
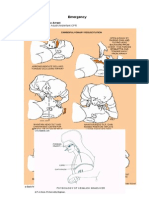
HEIMLICH MANEUVER Stand behind the client with arms under patients
(Subdiaphragmatic Abdominal Thrusts) axilla to encircle patients chest Nursing Actions:
Place thumb side of fist on the MIDDLE of Extend the neck. Place towel roll beneath the
For Standing or sitting conscious patient: STERNUM, grasp with the other hand and perform shoulders
Stand behind the patient; wrap your arms around BACKWARD thrust until foreign body is expelled. Insert the needle at a 10 to 30 degree caudal
the patients waist direction in the midline jest above the upper part
Make a FIST, placing thumb side of the fist against of the cricoid cartilage
the pts abdomen, in the midline SLIGHTLY ABOVE MEASURES TO ESTABLISH AIRWAY Listen for air passing back and forth
the UMBILICUS and WELL BELOW the XIPHOID A. HEAD-TILT-CHIN-LIFT MANEUVER Direct the needle downward and posteriorly, and
PROCESS B. JAW-THRUST MANEUVER tape it.
Make a quick INWARD and UPWARD thrust. Each C. OROPAHRYNGEAL AIRWAY
thrust is separated.
INJURIES TO HEAD, SPINE, AND FACE CUSHINGS TRIAD ( bradypnea, bradycardia, B. SKULL FRACTURES
widened pulse pressure) indicating increased SIMPLE closed
A. HEAD INJURIES intracranial pressure COMPOUND open
1. OPEN HEAD INJURY skull is fractured unequal or unresponsive pupils; impaired vision LINEAR Fx common hairline break, w/o
2. CLOSED HEAD INJURY skull is intact Battles sign bluish discoloration of the mastoid, displacement of structure
3. CONCUSSION temporary loss of consciousness indicating a possible BASAL SKULL FRACTURE COMMINUTED Fx splinters or crushes the bone
that results in transient interruption if the brains Rhinorrhea or otorrhea indicative of CSF leak in several fragments
normal functioning Periorbital Ecchymosis indicates anterior basilar DEPRESSED Fx pushes the bone toward the
4. CONTUSSSION bruising of the brain tissue fracture brain
5. INTRACRANIAL HEMORRHAGE significant CRANIAL VAULT Fx top of the head
bleeding into a space or potential space between ALERT: If basilar skull fracture or severe midface fractures are BASILAR Fx base of the skull and frontal sinuses
the skull and the brain suspected, a nasogastric tube(NGT) is CONTRAINDICATED! ALERT:
a. Epidural hematoma Damage to the brain is the first concern, it is
the most serious type of hematoma; forms MANAGEMENT: considered a neurosurgical condition
rapidly and results from arterial bleeding Open airway by Jaw-Thrust Manuever, suction In children, skulls thinness and elasticity allows a
orally if needed depression w/o a break in the bone
forms between the dura and the skull Administer high flow oxygen: most common
from a tear int the meningeal area death is CEREBRAL ANOXIA CAUSES: Traumatic blows to the head, VA, severe
b. Subdural hematoma In general, hyperventilate the patient to 20-25 beatings
forms slowly and results from a venous bpm, causing cerebral vasoconstriction and S/Sx: scalp wounds, agitation and irritability, loss
bleed minimizing cerebral edema of consciousness, labored breathing, abnormal
Apply a bulky, loose dressing; dont apply deep tendon reflexes, altered pupillary and moor
a surgical emergency
pressure response
c. Intracerebral hemorrhage IV line of PNSS or Plain LR IF CONSCIOUS: complains of persistent localized
bleeding directly into the brain matter prepare to manage seizures headache
maintain normothermia IF JAGGED BONE FRAGMENTS: may cause cerebral
ALERT: Assume cervical spine fracture for any patient Medications: bleeding
with a significant head injury, until proven otherwise. a. Diazepam HALO SIGN blood-tinged spot surrounded by lighter
b. Steroids ring
PRIMARY ASSESSMENT: Assess for ABC c. Mannitol IF SPHENOIDAL Fx: damages the optic nerve and may
SECONDARY ASSESSMENT: Prepare of immediate surgery if pt. shows cause BLINDNESS
Change in LOC most sensitive indicator in the evidence of neurologic deterioration IF TEMPORAL Fx: may cause unilateral deafness or
pts condition
facial paralysis
TREATMENT: SUBSEQUENT ASSESSMENT: INJURIES TO SOFT TISSUES, BONES AND JOINTS
For LINEAR FRACTURES: Hypotension, bradycardia, hypothermia - A. SOFT TISSUE INJURIES
supporative (mild analgesics) suggests SPINAL SHOCK 1. CLOSED WOUND
cleaning and debridement of wounds Total sensory loss and motor paralysis below the A. CONTUSION bleeding beneath the skin into the soft
If conscious: observed for 4 hours; if not, admit for level of injury tissue
evaluation MANAGEMENT: B. HEMATOMA well-defined pocket of blood and fluid
if VS stable, may go home with instruction sheet Nasotracheal intubation beneath the skin
For VAULT and BASILAR FRACTURES: initaite IV access, monitor blood gas 2. OPEN WOUND
Craniotomy to remove fragemnts indwelling urinary catheterization A. ABRASION superficial loss of skin from rubbing or
anti-biotics prepare to manage seizures scraping
Dexamethasone Meds: High dose steroids and diazepam B. LACERATION tear in the skin, can be insicional or
Osmotic Diuretics (MANNITOL) if increased ICP is jagged
present D. MAXILLOFACIAL TRAUMA C. PUNCTURE penetration of a pointed object, can be
NURSING CONSIDERATIONS: PRIMARY ASSESSMENT: penetrating or perforating
maintain patent airway; nasal airway Immobilization of spine while performing D. AVULSION tearing off or loss of a flap of skin
contraindicated to basilar fx assessment E. AMPUTATION traumatic cutting or tearing off of a
support with O2 administration ABC (tongue swelling, bleeding, broken or finger, toe, arm or leg
suction pt. through mouth not nose if CSF leak is missed teeth)
present SUBSEQUENT ASSESSMENT: PRIMARY MANAGEMENT
RHINORRHEA wipe it, dont let him blow it! Paralysis if the upward gaze indicative of D- IRECT PRESSURE
OTORRHEA cover it lightly with sterile gauze, INFERIOR ORBIT FX E- LEVATION
dont pack it! Crepitus on nose indicates nasal fracture P- RESSURE POINTS
Position head on side Flattening of the cheek and loss of sensation S- OAK, SOAP, SCRUB, SURGERY
Maintain a supine position with bed elevated to below the orbit indicates ZYGOMA (cheekbone)
A- NTI-TETANUS, ANTIBIOTICS
30 degrees FX
I- RRIGATE
dont give narcotics or sedative Malocclussion of teeth, trismus indicative of
assist in surgery, maintaining sterile technique MAXILLA FX D- RESS
PRIMARY INTERVENTIONS:
C. CERVICAL SPINE INJURIES Insertion of oral airway or intubation B. INJURIES TO BONES AND JOINTS
PRIMARY ASSESSMENT: Nasopharyngeal airway should only be used if no 1. FRACTURE a break in he continuity of the bone;
immediate immobilization of the spine evidence of nasal fracture or rhinorrhea occurs when stress is placed on a bone is greater
A B C ( Intercoastal paralysis w/ diapragmatic Apply bulky, loose dressing; apply ice to areas of than the bone can absorb
breathing) swelling
ALERT: fractured cervical spine, pelvis and femur may Endoprosthetic Replacement implantation of Management: Immobilize part, Secure reduction of
produce life threatening injuries; posterior dislocations of metal device dislocations manually (usually preferred under anesthesia)
the hip are life- and limb-threatening emergencies due to NURSING CONSIDERATIONS: Nursing Considerations:
potential blood loss. Elevate to prevent or limit swelling Assess neurovascular status before and after
Apply ice packs or cold compress; not place reduction of dislocation
Clinical Manifestations: directly in skin Administer pain medications (NSAIDs)
Pain and tenderness over fracture site Splint and maintain in good alignment, immobilize Ensure proper use of immobilization device
Crepitus or grating over fracture site the joint above and below the fracture (elastic bandage, splints)
swelling and edema Give pain medications as ordered
Deformity, shortening of an extremity or rotation Assist in casting; use the palm of your hands in 3. SPRAIN an injury to the ligamentous structure
of extremity holding a wet cast surrounding a joint; usually caused by a wrench or twist
Avoid resting cast on hard surfaces or sharp edges resulting in a decrease joint stability
EMERGENCY Management: IMMOBILIZE, INITIATE IV Do neurovascular checks hourly for the first 24
hours Clinical Manifestations:
MANAGEMENT PROCESS OF FRACTURES Assess for COMPARTMENT SYNDROME check Rapid swelling due to extravasation of blood w/n
for 6 Ps tissues
REDUCTION If Compartment syndrome is suspected, do not Pain on passive movement of joint
setting the bone; refers to the restoration of the elevate limb above the level of the cast discoloration, and limited use or movement
fracture fragments into anatomic position and Notify the physician
alignment Bivalve the cast 4. STRAIN a microscopic tearing of the muscle cause by
IMMOBILIZATION excessive force, stretching, or overuse
maintains reduction until bone healing occurs 2. TRAUMATIC JOINT DISLOCATION - occurs when the
REHABILITATION surfaces of the bones forming the joint no longer in Clinical Manifestations:
Regaining normal function of the affected part anatomic position Pain with isometric contractions
Swelling and tenderness
use of cast and splint to immobilize extremity and ALERT: this is a medical emergency because of associated Hemorrhage in muscle
maintain reduction disruption of surrounding blood and nerve supplies
Skin Traction force applied to the skin using * Subluxation partial disruption of the articulating
foam rubber, tapes surfaces
Skeletal Traction force applied to the bony Clinical Manifestations:
skeleton directly, using wires, pins, tongs placed in Pain and deformity
the bone Loss of normal movement
ORIF operative intervention to achieve X-ray confirmation of dislocation w/o assoc.
reduction, alignment and stabilization fracture
MANAGEMENT OF SPRAINS AND STRAINS - Can be classified as: MANAGEMENT:
A. HYPOVOLEMIC - occurs when significant amount Administer O2 via ET or nonrebreather face mask
COMPRESSION (Elastic Bandage) of fluid is lost in the intravascular space (Ex. (if intubated, may be hyperventilated to control
Hemorrhage, burns, fluid shifts) acidosis)
REST B. CARDIOGENIC occurs when the heart fails as a Fluid resuscitation (2 large-bore IV lines, Ringers
ICE (for the first 24 hrs; 1 hr on, 2 hrs off during waking pump. Primary causes includes MI, dysrhythmias; Lactate, BT)
hours) Secondary causes includes mechanical restriction Insertion of an indwelling catheter
MEDICATIONS ( NSAIDs) of cardiac function or venous obstruction like in Maintain patient in a supine position with legs
ELEVATION Cardiac Tamponade, tension pneumothrorax, VCO elevated
C. SEPTIC SHOCK from bacteria and their products Continue to monitor VS, ECG, CVP, ABG, UO, HCT,
SUPPORT (Use of crutches, splints) circulating in the blood Hgb,and electrolytes; refer changes on the
following
NURSING CONSIDERATIONS: PRIMARY INTERVENTIONS: Maintain normothermia (high fever will increase
Apply ice compress for the first 24 hrs to produce Assess for ABC the cellular metabolism effects of shock
vasoconstriction, decrease edema, and reduce Resuscitate as necessary Medications: Inotropics, Vasopressor, and Anti-
discomfort Administer O2 to augment O2-carrying capacity of biotics
Apply warm compress after 24 hrs to promote arterial blood
circulation and absorption (20 to 30 minutes at a Start cardiac monitoring ELECTROCARDIOGRAM
time) Control hemorrhage - It is a useful tool in the diagnosis of those
Educate to rest injured part for a month to allow conditions that may cause abberations in the
healing SUBSEQUENT ASSESSMENT: electrical activity
Educate to resume activities gradually and to o Assess LOC, decreasing LOC indicates progression
warm up of shock WAVE INTERPRETATIONS:
o Monitor arterial blood pressure (narrowing pulse P WAVE : Atrial Depolarization; first positive deflection
SHOCK AND INTERNAL INJURIES pressure, fall in systolic pressure) Q WAVE: first negative deflection
A. SHOCK o Assess pulse quality and rate change (tachycardia, R WAVE: first positive deflection
- Inadequate tissue perfusion, resulting in failure of weak and thready) S WAVE: negative deflection, after R wave
one or more of the ff: o Assess urinary output (25ml/hr may indicate QRS COMPLEX: Ventricular Depolarization
a. pump failure of the heart shock) T WAVE: Ventricular Repolarization
b. Blood volume o Assess capillary perfusion
c. arterial resistance levels o Assess for metabolic acidosis due to anaerobic
d. capacity of venous beds metabolism of cells
o Assess for excessive thirst, hyperthermia on septic
shock
Nursing Responsibilities during ECG COMPLICATIONS: Thoracentesis yeilds blood and serosanguinous
Check order for ECG, in cases of arrest, prepare 1. TENSION PNEUMOTHORAX fluid
the machine at the bedside at ER a condition in which air enters the chest but cant ECG
Provide Privacy be ejected during exhalation Retrograde aortography reveals aortic
Instruct patient to lie still and avoid movement There is lung collapse and mediastinal shift laceration
Remove metal objects on the patients (jewelries) S/Sx: tracheal deviation, cyanosis and severe dyspnea, Echocardiography
Place Chest leads as labeled: absent breath sound on the affected side, agitation, Computed Tomography
Lead 1: Red, Right Arm JVD
Lead 2: Yellow, Left Arm 2. HEMOTHORAX TREATMENT:
Lead 3: Green, Left Foot collection of blood in the pleural cavity, usually Simple Rib Fractures
Neutralizer: Black, Right foot results from ribs, lacerating lung tisssue or an mild analgesics, bed rest, apply heat
V1: Red, 4th ICS, Right Sternal Border intercoastal artery incentive spirometry
V2: Yellow, 4th ICS, Left sternal border It is the most common cause of shock following deep breathing, coughing and splinting
V3: Green, midway between V2 and V4 chest trauma Severe Rib Fractures
V4: Brown, 5th ICS, Left MCL 2. LACERATION or RUPTURE of AORTA intercoastal nerve blocks
V5: Black, 5th ICS, LAAL immediately fatal position for semi-fowlers, administer O2
V6: Violet, 5th ICS, LMAL 3. DIAPHRAGMATIC RUPTURE Hemothorax
causes severe respi. Distress; if untreated Chest tube insertion at 5th-6th ICS anterior to MAL
B. BLUNT CHEST INJURIES abdominal viscera may herniate, compromising administer IV fuids, O2, Blood Transfusion
- It is a trauma in the chest without an open wound both circulation and vital capacity of lungs Thoracotomy
- usually cause by VA, blast injuries 4. CARDIAC TAMPONADE Thoracentesis
SIGNS/SYMPTOMS: rapid unchecked rise in intrapericardia pressure
RIB FRACTURES: tenderness, slight edema, pain that that impairs diastolic filling of the heart TREATMENT:
worsens with deep breathing and movement, shallow results from blood or fluid accumulation in the Tension Pneumothorax
and splinted respirations pericardial sac insertion of spinal, 14G or 16G needle into the 2nd
STERNAL FRACTURES: persistent chest pain ICS at MCL to release pressure
MULTIPLE RIB FRACTURES: ASSESSMENT AND DIAGNOSIS: Chest Tubes
- FLAIL CHEST (loss of chest wall integrity) Percussion: Surgical Repair
- decreased lung inflation, paradoxical - Hemothorax: Dullness Aortic Rupture/Laceration
chest movements - Tension Pnuemothorax: tymphany immediate surgery
- extreme pain Auscultation: - synthetic grafts
- rapid and shallow respirations - Tension Pnemothorax: PMI is deviated - aortic anastomosis
- hypotension, cyanosis - Cardiac tamponade: muffled heart tones O2, BT, IV
- respiratory acidosis X-ray
NURSING CONSIDEARTIONS: GENERAL INTERVENTIONS: Monitor VS every 15 mins and cardiac rhythm
monitor VS, (q 15, first hour post thoracentesis Keep pt. quiet in the stretcher, any movement Educate to avoid immediate reexposure to high
and post CTT) may dislodge a clot temperatures
After CTT insertion, encourage cough and Cut the clothing, count the number of wounds,
breathing exersises look for entrance and exit wounds 2. HEATSTROKE - It is a combination of hyperpyrexia and
Chest tubes should have continuous Apply compression to external bleeding wounds neurologic symptoms. It caused by a shutdown or failure
FLUCTUATIONS double IV line and infuse Ringers Lactate of the heat-regulating mechanisms of the body.
if BUBBLING, air leak is suspected Insert NGT to decompress the abdomen
if FLUCTUATION STOPS, mechanical blockage or Cover protruding abdominal viscera w/ sterile CLINICAL MANIFESTATIONS:
lung has already expanded saline dressings; dont attempt to place back the bizarre behavior or irritability, progressing to
have an extra bottle with PNSS, clamps and sterile protruding organs confusion, delirium and coma
gauze at bedside Cover open wounds with dry dressings 40.6 degrees Celcius, hypotension, tachycardia,
in case of dislodgment, cover the opening with Insert indwelling catheter; if pelvic fracture is tachypnea
sterile/petroleum gauze to prevent rapid lung suspected, catheter should not be placed until skin may appear flushed and hot; at start it maybe
collapse integrity of urethra is ensured. moist progressing to dryness (Anhidrosis)
Assist with proper positioning Meds: Tetanus Prophylaxis, Antibiotics NURSING ALERT:
Bed Rest Assist in peritoneal lavage Elderly clients are high-risk to develop heat-stroke
Prepare pt. for surgery if the condition persists. Once diagnosis is confirmed, it is imperative to
C. ABDOMINAL INJURIES (Exploratory Laparotomy) reduce patients temperature
1. PENETRATING ABDOMINAL INJURY usually the
result of gunshot wound or stab wounds; may ENVIROMENTAL EMERGENCIES MANAGEMENT:
cross the diaphragm and enters the chest 1. HEAT EXHAUSTION - It is the inadequacy or the collapse EVAPORATIVE COOLING, most effective, by
2. BLUNT ABDOMINAL INJURY caused by vehicular of peripheral circulation due to volume and electrolyte spraying tepid water on skin while fans are used to
accidents or falls depletion blow
ASSESSMENT: temperature may be normal or slightly Apply ice packs to necks, groin, axillae, and scalp
PRIMARY ASSESSMENT AND INTERVENTIONS: elevated, hypotension, tachycardia, tachypnea, pale and Soak sheets/towels in ice water and place on
ASSESS ABC moist skin, fatigue, headache, dizziness, syncope patient
INITITATE RESUSCITATION AS NEEDED DIAGNOSTICS: hemoconcentration, hyponatremia or If temp. fails to decrease, initiate core cooling:
CONTROL BLEEDING AND PREPARE TO TREAT hypernatremia, ECG may show dysrhythmias iced saline lavage, cool fluid peritoneal dialysis,
SHOCK MANAGEMENT: cool fluid bladder irrigation
IF THERE IS AN IMPALED OBJECT IN THE Move patient to a cool environment, remove all Discontinue active cooling when the temp.
ABDOMEN, LEAVE IT THERE AND STABILIZE THE clothing reaches 39 degrees Celcius
OBJECT WITH BULKY DRESSINGS Position the patient supine with the feet slightly Oxygenate the pt. via ET or nonrebreather mask
elevated Monitor VS, ECG, and neurologic status
Start IV infusion using Ringers Lactate GOAL of MANAGEMENT: Rewarm without 4. NEAR-DROWNING
Anti-pyretics are not useful precipitating cardiac dysrhythmias. - It is a survival for atleast 24 hours after
Indwelling catheterization submersion, with most common consequence of
WOF hypokalemia, metabolic acidosis, seizures MANAGEMENT: hypoxemia.
Passive External Rewarming (temp above 28 - Hypoxia and acidosis are common problems of the
3. HYPOTHERMIA degrees) victim.
- It is a condition where the core temp. is less than - Remove all wet clothing, and replace with warm - Resultant pathophysiologic changes and
35 degrees Celcius as a result in the exposure to clothing pulmonary injury depend on type of fluid and the
cold. - Provide insulation by wrapping the patient in volume aspirated.
- 3 compensatory mechanisms: several blankets a. Fresh water aspiration- results in loss of surfactant,
a. shivering produces heat thru muscular activity - Provide warm fluids hence an inability to expand lungs
b. peripheral vasoconstriction to decrease heat Disadvantage: slow process b. Saltwater aspiration- leads to pulmonary edema from
loss Active External Rewarming (temp above 28 the osmotic effect of salt within the lungs.
c. raising basal metabolic rate degrees)
- Provide external heat for patient- warm hot water Clinical Manifestations:
NURSING ALERT: bottles to the armpits, neck, or groin -difficulty of breathing
Elderly are greater risk for hypothermia due to - Warm water immersion -hypothermia
altered compensatory mechanisms - Disadvantages: -cyanosis
Extreme caution should be used in moving or 1. causes peripheral vasodilation, returning cool blood to -chills
transporting hypothermic pts., because the heart the core, causing an initial lowering of the core temp.
is near fibrillation threshold 2. Acidosis due to washing out of lactic acid from the MANAGEMENT:
peripheral tissue Immediate CPR
CLINICAL MANIFESTIONS: 3. An increased in metabolic demands before the heart is Endotracheal intubation with PEEP
slow, spontaneous respirations warmed to meet these needs. VS, check degree of hypothermia
heart sounds may not be audible even if its Active Core Rewarming (temp below 28 degrees) Rewarming procedures
beating - Inhalation of warm, humidified O2 by mask or Intravascular volume expansion and inotropic
BP is extremely difficult to hear ventilator agents
fixed dilated pupils, no pulse, no BP; initiate CPR - warmed IV fluids ECG
drowsiness progressing to coma - Warm gastric lavage Indwelling catheterization
shivering is suppressed on temp. below 32.3 - Peritoneal dialysis with warmed standard dialysis NGT insertion
degrees solution
ataxia - Cardiopulmonary bypass
cold diuresis Disadvantage: invasiveness of the procedure
fruity or acetone odor of breath
TOXICOLOGIC EMERGENCIES 1. Forced diuresis with urine pH alteration to 1. Stomach may be left empty.
ASSESSMENT: enhance renal clearance. 2. An Adsorbent may be instilled in the tube and
ABC 2. Hemoperfusion (process of passing blood through allowed to remain in the stomach.
Identify the poison an extracorporeal circuit and a cartridge 3. A saline cathartic may be instilled in the tube.
Obtain blood and urine tests; gastric contents may containing an adsorbent, such as charcoal, after Pinch off the tube during removal or maintain
be sent to laboratory which the detoxified blood is returned to the suction while tubing is being withdrawn.
Monitor neurologic status patient) Give the patient a cathartic if prescribed.
Monitor fluid and electrolytes 3. Hemodialysis to purify and accelerate the Warn patient that stool will turn black from the
elimination of circulating toxins. charcoal.
GENERAL INTERVENTIONS: 4. Repeated dose of charcoal.
Initiate large-bore IV access, monitor shock 5. Providing an antidote antidote is a chemical or 2. CARBON MONOXIDE POISONING
Prevent aspiration of gastric contents by physiologic antagonist that will neutralize the - It is an example of inhaled poison and results in
positioning head on side poison. the incomplete hydrocarbon combustion
Maintain seizures precaution - Carbon monoxide exerts its toxic effects by
GASTRIC LAVAGE binding to circulating hemoglobin to reduce the
MINIMIZING ABSORPTION PURPOSES: oxygen carrying capacity of the blood.
Administration of activated charcoal with a 1. To remove unabsorbed poison after ingestion. - Carbon monoxide and hemoglobin is 200 300
cathartic to hasten secretion. 2. To diagnose and treat gastric hemorrhage and for times affinity compared to oxygen and
Induction of emesis with syrup of ipecac; done the arrest of hemorrhage. hemoglobin.
only in patients with good gag reflex and is 3. To cleanse stomach before endoscopic - Creation of carboxyhemoglobin resulting to tissue
conscious. procedures. anoxia.
Adult dose is 30 ml by mouth followed by 2 4. To remove liquid or small particles of material CLINICAL MANIFESTATIONS
glasses of water; Pedia dose is15 ml followed by 8 from the stomach. - Respiratory depression, stridor.
16 oz. of water. NURSING CONSIDERATIONS - Confusion progressing to coma.
Insertion of NGT or OGT. - Headache, muscular weakness, palpitation, and
NURSING ALERT: Do not induce emesis after ingestion of Place patient on left lateral position with head dizziness.
caustic substances, hydrocarbons, iodides, silver nitrates, lower 15 degrees downward. - Skin is pink in color, cherry red, or cyanotic.
petroleum distillates; to a patient having seizure or to Elevate funnel and pour approx. 150 200 ml. - ABG: carboxyhemoglobin level is 12% (Normal),
pregnant patient. Lavage fluid is left in place for about one minute 30 40% severe carbon monoxide poisoning.
Gastric lavage for the obtunded patient. Save before allowed to drain
gastric aspirate for toxicology screen. Save samples of first two washings. MANAGEMENT:
Procedure to enhance the removal of ingested Repeat lavage procedure until the returns are Provide 100% oxygen by tight-fitting mask (the
substance if the patient is deteriorating. relatively clear and no particular matter is seen. elimination half life of carboxyhemoglobin, in
At the completion of the lavage: serum, for a person breathing room air is 5 hours
and 20 minutes. If patient breaths 100% oxygen - Have epinephrine on hand Symptoms begins as early as 4 hours after
the half life is reduced to 80 minutes - Wear emergency medical bracelet indicating reduction of alcohol intake and peaks at 24 - 48
100% oxygen in hyperbaric chamber reduces hypersensitivity. hours but may last up to 2 weeks.
halflife to 20 minutes. - If sting occurs, remove stinger with one quick
Intubate if necessary to protect airway. scrape of fingernail. ALCOHOLISM a chronic disease or disorder
Continuous ECG monitoring, treat dysrhythmias. - Do not squeeze venom sack, because this may characterized by excessive alcohol intake and
Correct acid-base and electrolyte imbalances. cause additional venom to be injected. interference in the individuals health, interpersonal
Continuous observation of psychoses, spastic - Avoid insect feeding areas. realtionship and economic functioning
paralysis, visual disturbances, and deterioration of
personality may persist after resuscitation and 4. SNAKE BITES - Considered to be present when there is .1% or 10
may be symptoms of permanent CNS damage. CLINICAL MANIFESTATIONS: ml for every 1000 ml of blood
- Burning pain, swelling, and numbness of the site. - At .1 - .2%, there is low coordination
3. INSECT STINGS - Hemorrhagic blisters may occur after few hours of - At .2 - .3%, there is ataxia, tremors, irritability,
- These are injected poisons that can produce either bite and entire extremity may become edematous. and stupor
local or systemic reactions. - WOF signs of systemic reactions (nausea,
- Local reactions are characterized by pain, sweating, weakness, lightheadedness, initial At .3 and above, there is unconsciousness
erythema and edema at the site of injury. euphoria followed by drowsiness, dysphagia, COMMON BEHAVIORAL PROBLEMS: 5 Ds
- Systemic reactions usually begin within minutes. paralysis of various muscle groups, shock, seizures, D-enial
(Unconsciousness, laryngeal edema, and coma). D-ependency
bronchospasm, and cardiovascular collapse. MANAGEMENT: D-emanding
MANAGEMENT: Wash the site of bite, keep the patient calm and D-estructive
ABC immobilize extremity. D-omineering
Epinephrine is the drug of choice give SQ. Administer O2 and start IV line. COMMON WITHDRAWAL SIGNS AND SYMPTOMS:
Administer bronchodilator. Administer anti-venin and be alert to allergic HALLUCINATIONS (VISUAL AND TACTILE)
Initiate IV with Ringers Lactate. reaction.
Prepare for CPR. Administer vasopressors in the treatment of
INCREASED VITAL SiGNS
NURSING CONSIDERATIONS: shock. TREMORS
Apply ice packs to site to relieve pain. SWEATING AND SIEZURE
Elevate extremities with large edematous local 5. ALCOHOL WITHDRAWAL DELIRIUM COMMON DEFENSE MECHANISMS:
reaction. a.k.a Delirium Tremens or Alcoholic Hallucinosis DENIAL
Administer anti histamine for local reaction. An acute toxic state that follows a prolonged bout
Clean wounds thoroughly with soap and water or of steady drinking or sudden withdrawal from
RATIONALIZATION
antiseptic solution. prolonged intake of alcohol. ISOLATION
Educate patient. PROJECTION
PRIORITY NURSING DIAGNOSIS: 1. VIOLENT PATIENTS PRIORITY NURSING DIAGNOSIS:
- INEFFECTIVE INDIVIDUAL COPING - Is usually episodic and is a means of expressing Risk for Injury, Self-directed
DRUG OF CHOICE for aversion therapy of an alcoholic: feelings of anger, fear and hopelessness about a NURSING INTERVENTIONS:
- DISULFIRAM (antabuse)
situation. Provide one-on-one monitoring
Instruct patient to avoid, when taking Disulfiram:
Manage through: Have frequent unscheduled rounds
MOUTH WASH
a. Establish control, keeping the door open, and be in Avoid use of metals and glass utensils
OVER THE COUNTER COLD REMIDIES clear veiw of staff Remove shampoos, perfumes, medicines at the
FOOD SAUCES MADE UP OF WINE b. Ask if he has a weapon, avoid touching an agitated pt. bedside
FRUIT FLAVORED EXTRACTS c. Adopt a calm, nonconfrontational approach Monitor for signs of impending suicide (giving
AFTERSHAVE LOTIONS d. Provide emotional support; CRISIS INTERVENTION away of valued possession)
VINEGAR
SKIN PRODUCTS 2. SUICIDE 3. RAPE TRAUMA SYNDROME
MANAGEMENT: - Ultimate form of self-destruction; cry for help According to RA 8353, RAPE refers to the insertion
Protect patient from injury, diazepam or - Major Interventions: PREVENTION and LISTEN of penis into the mouth, vagina, anus of a victim
phenytoin for seizure control as prescribed. Insertion of any object into the mouth or anus
Monitor VS every 30 minutes. RISK FACTORS It is generally considered as an act of hostility,
Use a non-alcohol skin preparation, draw blood
SEX (female attempts, male commits suicide) anger, or violence
for measurement of ethanol concentration,
toxicologic screen for other drug abuse. ELEMENTS OF RAPE:
UNSUCCESSFUL PREVIOUS ATTEMPT
Maintain electrolyte balance and hydration. Use of threat/force
Observe for hypoglycemia. IDENTIFICATION with family member committed suicide lack of consent of the victim
Administer thiamine followed by parenteral CHRONIC Actual penetration of the penis into the vagina
dextrose if liver glycogen is depleted. Different Kinds of Rape:
Give orange juice, gatorade, or other
ILLNESS
POWER done to prove ones masculinity
carbohydrates to stabilize blood sugar. DEPRESSION/DEPENDENT PRERSONALITY ANGER done as a means of retaliation
Place patient in a private room with close
observation.
AGE (18-25 AND ABOVE 40)/ALCOHOLISM SADISTIC done to express erotic feelings
LETHALITY OF PREVIOUS ATTEMPTS
BEHAVIORAL EMERGENCIES - It is an urgent, serious RAPE TRAUMA SYNDROME
disturbances of behavior, affect, or thought that makes - It refers to a group of signs and symptoms
the patient unable to cope with his life situation and experienced by a victim in reaction to rape
interpersonal relationship
4 Phases the perineal area is prone to
1. ACUTE PHASE characterized by shock, numbness autocontamination by urine and feces;
and disbelief circumferential burns of the extremities
2. DENIAL characterized by victims refusal to talk can produce a tourniquet-like effect and
about the event lead to vascular compromise
3. HEIGHTENED ANXIETY characterized by fear, (compartment syndrome).
tension, and nightmares 4. Depth
4. REORGANIZATION victims life normalizes
PRIORITY NURSING CARE: Preservation of evidences Classification Affected Part Description of Wound What to Expect
TREATMENT: Crisis Intervention
1st degree Epidermis Pin, painful sunburn Discomfort last after 48 hrs; heals
BURN TRAUMA - Is the damage caused to skin and deeper superficial Blisters form after 24 hours in 3-7 days
body structures by heat (flames, scald, contact with heat) ,
electrical, chemical or radiation
2nd degree Pediermis and part Red, wet blisters, bullae very Heals in 2-3 weeks, in no
FACTORS DETERMINING SEVERITY OF BURN: partial thickness of the dermis painful complication
1. age mortality rates are higher for children < 4 yrs of
age and for clients > 65 yrs of age
2. Patients medical condition debilitating disorders such 2nd degree Only the skin Waxy white, difficult to Slow to heal 94-8 weeks) surgical
as cardiac, respiratory, endocrine and renal disorders deep partial appendages in the distinguish from 3rd degree incision and grafting unless has
negatively influence the clients response to injury and thickness hair follicle remain except hair growth becomes complication
treatment. apparent in 7-10 days, little or
mortality rate is higher when the client no pain
has a pre-existing disorder at the time of the burn
injury 3rd degree Epidermis, dermis Dry, leathery, may be Requires excision and grafting.
3. location Full thickness and subcutaneous red or black 10- 14 days for graft to
burns on the head, neck and chest are tissue . no skin May have thrombosed revascularize
associated with pulmonary complications; appendages veins
burns on the face are associated with Marked edema
corneal abrasion; Distal circulation may
burns on the ear are associated with be decreased
auricular chondritis; Painless
hands and joints require intensive
therapy; 4th degree Skin, muscle, Dry, charred, bone may be Requires excision, grafting and
deep full thickness tendon, bonde visible sometimes amputation
5. Size: Rule of nine Types of Burns and their Treatment: Spasm in the air passages as a result of
Assessment Child < 3 Adult Scald irritation by smoke or gases
years burn caused by hot liquid Severe burns to the air passages causing
old immediately flush the burn area with swelling and obstruction
water (under a tap or hose for up to 20 Victim will show signs and symptoms of
Head and neck 18% 9% min) lack of O2. He may also be confused or
if no water is readily available, remove unconscious
1 arm 9% 9% clothing immediately as clothing soaked Electrical
Posterior trunk 18% 18% with hot liquid retains heat check for Danger
Flame turn of the electricity supply if possible
Anterior trunk 18% 18% Smother the flames with a coat or blanket, avoid any direct contact with the skin of
get the victim on the floor or ground (stop, the victim or any conducting material
1 leg 14% 18% drop, and Roll) touching the victim until he is
Perineum 1% 1% Prevent victim from running disconnected
If water is available, immediately cool the once the area is safe, check the ABCs
burn area with water if necessary, perform rescue breathing or
6. Temperature If water is not available, remove clothing; CPR
determines the extent of injury avoid pulling clothing across the burnt face Chemical
7. Exposure to the Source Cover the burn area with a loose, clean, Flood affected area with water for 20-30
Thermal Burns caused by exposure to dry cloth to prevent contamination min
flames, hot liquids, steam or hot objects Do not break blisters or apply lotions, Remove contaminated clothing
Chemical Burns caused by tissue contact ointments, creams or powder If possible, identify the chemical for
with strong acids, alkalis or organic Airway possible subsequent neutralization
compounds if face or front of the trunk is burnt, there Avoid contact with the chemical
Electrical Burns result in internal tissue could be burns to the airway Sunburn
damaging, alternating current is more there is a risk of swelling or air passage, Exposure to ultraviolet rays in natural
dangerous than direct current for it is leading to difficulty in breathing sunlight is the main cause of sunburn
associated with cardiopulmonary arrest, Smoke inhalation General skin damage and eventually skin
ventricular fibrillation, titanic muscle Urgent treatment is required with care of cancer develops
contractions, and long bone and vertebral the airway, breathing and circulation The signs and symptoms of sunburn are
fractures. When 02 in the air is used up by fire, or pain, redness and fever
Radiation Burns are caused by exposure replaced by other gases, the oxygen level
to ultraviolet light, x-rays or a radioactive in the air will be dangerously low
source.
You might also like
- Mastering ICU Nursing: A Quick Reference Guide, Interview Q&A, and TerminologyFrom EverandMastering ICU Nursing: A Quick Reference Guide, Interview Q&A, and TerminologyNo ratings yet
- COMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideFrom EverandCOMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideNo ratings yet
- Emergency and Disaster Nursing 2012Document218 pagesEmergency and Disaster Nursing 2012Darran Earl Gowing100% (2)
- Emergency and Disaster NursingDocument138 pagesEmergency and Disaster NursingDarran Earl Gowing95% (20)
- Emergency and Disaster NursingDocument20 pagesEmergency and Disaster NursingNeil Cuasito89% (9)
- Emergency and Disaster NursingDocument10 pagesEmergency and Disaster Nursingbabyrainbow100% (2)
- Emergency NursingDocument40 pagesEmergency NursingJaimely ReyesNo ratings yet
- Disaster TriageDocument20 pagesDisaster TriageNabella100% (1)
- Emergency Nursing PDFDocument39 pagesEmergency Nursing PDFJustin John NavarroNo ratings yet
- IV InsertionDocument18 pagesIV InsertionRochelle Valero100% (2)
- Perioperative NursingDocument41 pagesPerioperative Nursingbajaoc100% (8)
- Emergency Room QuestionsDocument5 pagesEmergency Room QuestionsCharles Anthony Lopez EstebanNo ratings yet
- Emergency NursingDocument9 pagesEmergency NursingJamaica WineNo ratings yet
- Triage WorkbookDocument202 pagesTriage WorkbooklatifahNo ratings yet
- Pre and Post Operative ManagementDocument3 pagesPre and Post Operative Managementdrsb54No ratings yet
- Emergency NursingDocument5 pagesEmergency NursingSpislgal PhilipNo ratings yet
- Perioperative Nursing SkillsDocument278 pagesPerioperative Nursing SkillsNacel Celeste100% (3)
- Disaster NursingDocument7 pagesDisaster NursingAmal B Chandran100% (1)
- 1-The Introduction of Disaster NursingDocument20 pages1-The Introduction of Disaster NursingHanifah AmbangNo ratings yet
- Peri Operative NursingDocument22 pagesPeri Operative NursingIvyBanez100% (1)
- Perioperative Nursing QuizDocument4 pagesPerioperative Nursing Quizgladz25100% (1)
- Perioperative Nursing - OrIGINALDocument176 pagesPerioperative Nursing - OrIGINALJamil Lorca100% (4)
- Emergency NursingDocument41 pagesEmergency NursingDr. Jayesh Patidar100% (2)
- Perioperative Nursing Management Ksu 0Document35 pagesPerioperative Nursing Management Ksu 0moath qadourah100% (1)
- CASE SCENARIO 3 PreopDocument3 pagesCASE SCENARIO 3 PreopEdgarNo ratings yet
- What Happens in The Operating RoomDocument137 pagesWhat Happens in The Operating RoomMelchor Felipe Salvosa100% (1)
- NCM 118Document7 pagesNCM 118Hazel MiraranNo ratings yet
- Competency Appraisal Questions Plus RationalesDocument68 pagesCompetency Appraisal Questions Plus RationalesCara Aspili100% (3)
- Emergency NursingDocument90 pagesEmergency NursingGen-GenMedranoGiray100% (1)
- Perioperative NursingDocument8 pagesPerioperative NursingJaney Ceniza تNo ratings yet
- Emergency NursingDocument5 pagesEmergency NursingmirageplayerNo ratings yet
- Disaster NursingDocument5 pagesDisaster NursingLorelie Asis100% (1)
- Practice Test Questions Downloaded From FILIPINO NURSES CENTRALDocument12 pagesPractice Test Questions Downloaded From FILIPINO NURSES CENTRALFilipino Nurses CentralNo ratings yet
- Perioperative Nursing 2Document54 pagesPerioperative Nursing 2Michelle Montemayor100% (1)
- Disaster Nursing NotesDocument19 pagesDisaster Nursing NotesRoscelin LumenNo ratings yet
- Scope and Practice of Emergency NursingDocument15 pagesScope and Practice of Emergency NursingLouis Justin E. ArevaloNo ratings yet
- Disaster NursingDocument2 pagesDisaster Nursingcgteacher7446100% (1)
- CHAPTER 16 MEDICAL Û SURGICAL EMERGENCIESDocument10 pagesCHAPTER 16 MEDICAL Û SURGICAL EMERGENCIESjev_belardoNo ratings yet
- Peri Operative NursingDocument184 pagesPeri Operative Nursingfelxhu100% (3)
- Geria NursingDocument23 pagesGeria NursingMaia Saivi OmegaNo ratings yet
- Ed QuestionsDocument5 pagesEd Questionsherbert100% (1)
- Introduction To Critical Care HandoutDocument30 pagesIntroduction To Critical Care HandoutAvy PHNo ratings yet
- Emergency NursingDocument5 pagesEmergency NursingRoAn DulayNo ratings yet
- Perioperative Nursing ConceptDocument21 pagesPerioperative Nursing ConceptArgee Alonsabe100% (8)
- Ppt1.1 Emergency and Disaster Nursing INTRODUCTIONDocument64 pagesPpt1.1 Emergency and Disaster Nursing INTRODUCTIONSkye M. Peters100% (2)
- Rubric For Drug StudyDocument2 pagesRubric For Drug StudyMart Juaresa Yambao100% (2)
- Name: - DateDocument10 pagesName: - DateTni JolieNo ratings yet
- Operating Room TeamDocument7 pagesOperating Room TeamFaruqueHossain100% (1)
- Disaster NursingDocument7 pagesDisaster NursingachiemandacNo ratings yet
- Perioperative NursingDocument74 pagesPerioperative NursingTina Talmadge100% (4)
- Community Focused Nursing: Passbooks Study GuideFrom EverandCommunity Focused Nursing: Passbooks Study GuideNo ratings yet
- A Guide for the Nurse Entrepreneur: Make a DifferenceFrom EverandA Guide for the Nurse Entrepreneur: Make a DifferenceNo ratings yet
- EmergencyDocument8 pagesEmergencyZanie CruzNo ratings yet
- Printed LecturesDocument10 pagesPrinted LecturesCla SeNo ratings yet
- Emergency Nursing: Compiled Notes of Bernie C. ButacDocument14 pagesEmergency Nursing: Compiled Notes of Bernie C. ButacFARAH MAE MEDINANo ratings yet
- Compiled Notes of Bernie C. ButacDocument12 pagesCompiled Notes of Bernie C. ButacVeigner Whyng CabugayanNo ratings yet
- Emergency NursingDocument46 pagesEmergency NursingJoshua P AloveroNo ratings yet
- Emergency and Disaster Nursing RodDocument21 pagesEmergency and Disaster Nursing RodRodney Beltran SubaranNo ratings yet
- Emergency and Disaster NursingDocument8 pagesEmergency and Disaster NursingJOvie RectinNo ratings yet
- GAD TemplateDocument12 pagesGAD TemplateNina OaipNo ratings yet
- 50 Item Integumentary ExamDocument10 pages50 Item Integumentary ExamAijem RyanNo ratings yet
- University of The Visayas: Gerontological Nursing - MidtermDocument1 pageUniversity of The Visayas: Gerontological Nursing - MidtermNina OaipNo ratings yet
- University of The VisayasDocument2 pagesUniversity of The VisayasNina OaipNo ratings yet
- Psychopathophysiology in Ms-FinalsDocument3 pagesPsychopathophysiology in Ms-FinalsNina OaipNo ratings yet
- 50 Item Pharmacology ExamDocument10 pages50 Item Pharmacology Examshark_tale04100% (1)
- MDT For D.O Personnel MasterlistDocument15 pagesMDT For D.O Personnel MasterlistNina OaipNo ratings yet
- Client Planning ChecklistDocument6 pagesClient Planning ChecklistNina OaipNo ratings yet
- Guest Req Track 3Document2 pagesGuest Req Track 3Nina OaipNo ratings yet
- Registration Card Sample 2Document2 pagesRegistration Card Sample 2Nina OaipNo ratings yet
- Musculoskeletal SystemDocument124 pagesMusculoskeletal Systemnursereview93% (15)
- Registration Card Sample 5Document1 pageRegistration Card Sample 5Nina OaipNo ratings yet
- Orders To Flush Central/hep Loc line/PICC: Admission D/CDocument2 pagesOrders To Flush Central/hep Loc line/PICC: Admission D/CKaren Joy DelayNo ratings yet
- Competency Appraisal (Physiologic Disorders in Children) (Ongoing)Document1 pageCompetency Appraisal (Physiologic Disorders in Children) (Ongoing)Nina OaipNo ratings yet
- CS Form No. 212 Revised Personal Data Sheet 2Document13 pagesCS Form No. 212 Revised Personal Data Sheet 2ferosiacNo ratings yet
- Lhh-General Ward December 4th YearDocument2 pagesLhh-General Ward December 4th YearNina OaipNo ratings yet
- NCM Lec Demo GradeDocument2 pagesNCM Lec Demo GradeNina OaipNo ratings yet
- QuizDocument1 pageQuizNina OaipNo ratings yet
- Wedding SongsDocument1 pageWedding SongsNina OaipNo ratings yet
- Soymph-Medical Ward Duty FinalDocument1 pageSoymph-Medical Ward Duty FinalNina OaipNo ratings yet
- Exam NCM-Lec DemoDocument8 pagesExam NCM-Lec DemoNina OaipNo ratings yet
- August: Monday Wednesday Thursday Friday Saturday Sunday MondayDocument12 pagesAugust: Monday Wednesday Thursday Friday Saturday Sunday MondayNina OaipNo ratings yet
- Activities For The Christmas PartyDocument1 pageActivities For The Christmas PartyNina OaipNo ratings yet
- Family Nursing Care PlanDocument15 pagesFamily Nursing Care Planshielaebelandres90% (10)
- Certificate of AppearanceDocument1 pageCertificate of AppearanceNina OaipNo ratings yet
- Scribd1 2Document1 pageScribd1 2Nina OaipNo ratings yet
- Rle-Medical Ward Duty: Baluran Calapre Caturan Florendo Gloria Legua Paderog Rose Sumabat Tabo-OnDocument2 pagesRle-Medical Ward Duty: Baluran Calapre Caturan Florendo Gloria Legua Paderog Rose Sumabat Tabo-OnNina OaipNo ratings yet
- CA CardiovascularDocument10 pagesCA CardiovascularNina OaipNo ratings yet
- Scribd2 1Document1 pageScribd2 1Nina OaipNo ratings yet
- Scribd 8Document1 pageScribd 8Nina OaipNo ratings yet
- Collet and David Stephan ArgumentsDocument493 pagesCollet and David Stephan ArgumentsKaren Bartko100% (3)
- Department of A HospitalDocument24 pagesDepartment of A HospitalAnonymous YcdK9FWtH100% (2)
- Patient Transport PolicyDocument15 pagesPatient Transport Policydrwaheedhegazy100% (2)
- Deep and Dreamless SleepDocument7 pagesDeep and Dreamless SleepBilly ActualNo ratings yet
- Acute Care Surgery Handbook: General Aspects, Non-Gastrointestinai and Critical Care EmergenciesDocument512 pagesAcute Care Surgery Handbook: General Aspects, Non-Gastrointestinai and Critical Care EmergenciesOscar Villacres100% (6)
- Impact of Language Barrier On Acutecaremedical Professionals Is Dependent Upon RoleDocument4 pagesImpact of Language Barrier On Acutecaremedical Professionals Is Dependent Upon Roleravibunga4489No ratings yet
- Medical English Vocabulary: Nurses and Medical ProfessionalsDocument15 pagesMedical English Vocabulary: Nurses and Medical ProfessionalsEchan MitnickNo ratings yet
- OxfordMedicineLIVETitleList Aug 2018Document297 pagesOxfordMedicineLIVETitleList Aug 2018Anonymous BOXUxa0% (1)
- Suny CVDocument5 pagesSuny CVRanjith RamachandranNo ratings yet
- Foreign Bodies of The Ear and Nose - A Novel Technique of RemovalDocument4 pagesForeign Bodies of The Ear and Nose - A Novel Technique of RemovalAnonymous lAfk9gNPNo ratings yet
- Memo To SOGH Staff Re ED Conversion To UCDocument3 pagesMemo To SOGH Staff Re ED Conversion To UCElishaDaceyNo ratings yet
- Tugas SL 8Document3 pagesTugas SL 8Desmita AuliaNo ratings yet
- Danish National Action Plan 2013-2020Document116 pagesDanish National Action Plan 2013-2020Alina BurlacuNo ratings yet
- Tarlac Provincial Hospital 2014 Manual NewDocument143 pagesTarlac Provincial Hospital 2014 Manual NewAl Sah Him100% (5)
- Aussie Emergency CareDocument9 pagesAussie Emergency CarePuspita Sari FiazNo ratings yet
- Rakesh Joshi - Thesis Synopsis (NEW)Document19 pagesRakesh Joshi - Thesis Synopsis (NEW)Bhaskar NamanNo ratings yet
- Aontú Election 2020 ManifestoDocument69 pagesAontú Election 2020 ManifestoBusinessPost100% (1)
- Nur 460 Capstone Final PaperDocument15 pagesNur 460 Capstone Final Paperapi-429837528No ratings yet
- 2018 MUSE Inspire Conference - Educational PresentationsDocument83 pages2018 MUSE Inspire Conference - Educational PresentationsMichele LambertNo ratings yet
- EPPA6214 Cost ConceptDocument6 pagesEPPA6214 Cost ConceptIbrahim AmmarNo ratings yet
- The Abbreviated Injury Scale and Its Correlation With Preventable Traumatic Accidental DeathsCorrelation WithDocument9 pagesThe Abbreviated Injury Scale and Its Correlation With Preventable Traumatic Accidental DeathsCorrelation WithmkumNo ratings yet
- Specimen Bmat 2015 Past Paper Section 1 PDFDocument28 pagesSpecimen Bmat 2015 Past Paper Section 1 PDFSkruzdelyte MielaNo ratings yet
- National Emergency Guidelines, FMOH 2020Document248 pagesNational Emergency Guidelines, FMOH 2020Ramo Edum80% (5)
- Design BrifeDocument27 pagesDesign Brifesai pranayNo ratings yet
- 10 Ideas For Healthcare, 2012Document32 pages10 Ideas For Healthcare, 2012Roosevelt Campus NetworkNo ratings yet
- Jurnal Sports Injury 1Document18 pagesJurnal Sports Injury 1Giita AidhaNo ratings yet
- Room & Department in Hospital 3ADocument66 pagesRoom & Department in Hospital 3AAjeng AyuNo ratings yet
- Final Activity Set B ECE069 1S1920Document5 pagesFinal Activity Set B ECE069 1S1920Jericho Ernest Cariño SibayanNo ratings yet
- Reception and Resuscitation of The Seriously Injured PatientDocument14 pagesReception and Resuscitation of The Seriously Injured PatientEdwardRazvanNo ratings yet
- Oral Station ScenarioDocument3 pagesOral Station ScenariojrworthingtonNo ratings yet