Professional Documents
Culture Documents
Vascular Cognitive Impairment-2006 PDF
Uploaded by
dianisvillarrealOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Vascular Cognitive Impairment-2006 PDF
Uploaded by
dianisvillarrealCopyright:
Available Formats
REVIEW
www.nature.com/clinicalpractice/neuro
Vascular cognitive impairment
Ola A Selnes* and Harry V Vinters
S U M M A RY INTRODUCTION
Cognitive impairment is part of the clinical
Cognitive impairment commonly accompanies clinical syndromes
presentation of several conditions associated
associated with vascular disease of the brain. Because of evolving
with cerebrovascular disease, but the precise
definitional criteria, however, the frequency of cognitive impairment
frequency of vascular cognitive disorders is diffi-
attributable to cerebrovascular disease is difficult to determine. Dementia
occurs in up to one-third of elderly patients with stroke, a subset of whom
cult to ascertain. Clinicopathological studies of
have Alzheimers disease (AD) rather than a pure vascular dementia various selected or unselected populations have
syndrome. In fact, pure vascular dementia has been shown to be uncommon shown a remarkable heterogeneity of vascular
in most large autopsy series. A mixed etiology of AD and cerebrovascular and brain parenchymal lesions,13 and classifica-
disease is thought to become more common with increasing age, although tion schemes based on clinical,4 radiological5 and
no clinical criteria for the diagnosis of AD with cerebrovascular disease are neuropathologic1,6 criteria have been proposed.
currently available. Epidemiological studies have implicated subcortical In this Review, only the major subtypes of vascular
small-vessel disease as a risk factor for cognitive impairment and dementia, cognitive impairment will be considered.4
but the cognitive expression and clinical significance of MRI white matter Diagnostic criteria for vascular dementia
changes in individual patients is difficult to establish. The frequency have evolved over the past two decades,7 but
of specific neuropathologic features of vascular cognitive impairment several obstacles to widespread acceptance of
depends largely on study inclusion criteria. Cerebral meningocortical these definitions are recognized. Modeled after
microangiopathies with distinctive clinicopathological profiles are Alzheimers disease (AD), early definitions of
associated with dementia in both sporadic cases and familial syndromes. vascular dementia (VaD) disproportionately
In patients with AD, the contribution of amyloid- protein to the degree of emphasized deficits of new learning and
cognitive impairment has not been clearly defined. memory, rather than the pattern of motor
KEYWORDS brain ischemia, CADASIL, cerebral amyloid angiopathy,
slowing and executive deficits typically asso-
cerebrovascular disorders, dementia ciated with VaD. The requirement that patients
with VaD should have cognitive impairment
REVIEW CRITERIA of sufficient severity to interfere with activi-
We searched PubMed (19902005) for articles, including electronic early
release articles. Search terms included dementia, CADASIL, Alzheimers
ties of daily living is now acknowledged as too
disease, cerebrovascular disorders, cerebral infarction, brain ischemia, restrictive, because it does not allow cases to be
cerebral amyloid angiopathy, cognition disorders, cognition disorders/ identified early enough for diagnostic inter-
pathology, neuropsychology, dementia/pathology and brain/pathology. ventions. The severity and type of lesions on
We prioritized articles according to several criteria, including large study sample neuroimaging required for a diagnosis of VaD
sizes, inclusion of a control group, and assessment of cognition by standardized
neuropsychological tests. remain controversial, and the requirement of
a temporal link between the onset of cognitive
changes and neuroimaging changes restricts
OA Selnes is a professor in the Cognitive Neuroscience Division, Department
of Neurology, Johns Hopkins University School of Medicine, Baltimore, MD, case identification predominantly to VaD
USA, with a joint appointment in the Department of Psychiatry. HV Vinters secondary to infarcts.8
holds the Daljit S. and Elaine Sarkaria Chair in Diagnostic Medicine, and The term vascular cognitive disorder was
is Professor of Pathology and Laboratory Medicine, and Neurology, at the proposed by Sachdev9 to define vascular cogni-
University of California, Los Angeles, CA, USA. tive deficits of sufficient severity to meet criteria
for a diagnosable disorder. It was intended as an
Correspondence
*Division of Cognitive Neuroscience, Johns Hopkins University School of Medicine,
umbrella term to include the spectrum of impair-
Reed Hall East 2, 1620 McElderry Street, Baltimore, MD 21205-1910, USA ment from mild vascular cognitive impairment
oselnes@jhmi.edu (VCI) to VaD.10 The development of a single,
uniform set of criteria that apply to all subtypes
Received 13 March 2006 Accepted 21 July 2006
www.nature.com/clinicalpractice
of VCI has clearly been challenging, and some
doi:10.1038/ncpneuro0294 experts have recommended that separate criteria
538 NATURE CLINICAL PRACTICE NEUROLOGY OCTOBER 2006 VOL 2 NO 10
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
be developed for certain subtypes, such as non- smaller infarcts in particular regions, for
infarct-related subcortical small-vessel disease.11 example in the deep central gray matter, might
The aim of this Review is to provide a brief over- have an equally important role in causing
view of the current state of scientific knowledge dementia.1 Lacunar infarcts involving the
in the field of VCI, with an emphasis on its thalamus, internal capsule and basal ganglia are
neurocognitive and neuropathologic aspects. sometimes associated with surprisingly wide-
spread cognitive effects, including confusion
and memory impairment.21 Infarcts involving
SUBTYPES OF VASCULAR COGNITIVE the dorsomedial and anterior thalamus might
IMPAIRMENT also produce significant executive symptoms
Post-stroke dementia and profound amnesia, which can persist in
The prognosis for recovery of cognitive symp- some cases.22 Prospective follow-up studies
toms, including aphasia, after an initial stroke have shown that, although initially quite severe,
is generally favorable, but some patients do not cognitive symptoms associated with strategic
show the expected recovery, and instead develop infarcts are often reversible by 12 months,
persistent or progressive cognitive decline.12 and they are therefore not a common cause of
Because older patients at risk for stroke have an persistent dementia.23
increased risk of dementia even in the absence In summary, there is substantial evidence that
of a stroke, the inclusion of elderly controls is stroke in the context of advanced age confers an
crucial for interpreting the results of post-stroke increased risk of dementia. Nonetheless, the risk
dementia (PSD) studies.13,14 PSD has long been of PSD appears to be more closely related to the
considered the prototypical subtype of VaD, and severity of pre-existing white matter abnormali-
it might therefore be expected that all patients ties, atrophy and hemodynamic factors than to
with PSD would meet the criteria for VaD. the stroke characteristics themselves. Although
Surprisingly, however, only one-third of such generally easily recognized clinically, PSD repre-
patients have been reported to meet the diag- sents only the proverbial tip of the iceberg of
nostic criteria for AD.12,15 This finding is consis- the spectrum of VCI.24
tent with epidemiological data showing that risk
factors for cerebrovascular disease are common in
patients with AD,16 and also that many patients Alzheimers disease with cerebrovascular
diagnosed with PSD have cognitive impairment disease
even before their stroke.12,17 Determining the neurobehavioral and neuro-
The most important demographic predictor imaging correlates of ischemic brain lesions
of PSD is age; the association with stroke risk occurring in the context of significant AD altera-
factors is less robust.12 Degree of pre-existing tions can be a daunting task, and the usefulness
subcortical white matter disease, infarct of the traditional strict dichotomization between
volume, and global and medial temporal lobe AD and VaD has recently been challenged.25
atrophy, have been identified as some of the Evidence is accumulating that AD is commonly
relevant imaging determinants of post-stroke associated with vascular risk factors, including
dementia,18 and cortical hypoperfusion might diabetes,26 hypertension and smoking.16 Whether
also play an important role.14 Stroke character- these associations are causal or coincidental
istics, such as lesion volume and location, appear co-occurrences of common age-associated
to be less predictive of PSD. A greater degree of conditions is not known.
severity of cognitive impairment after stroke has Many individuals with AD, especially those
been associated with increased risk of PSD.15,19 beyond 85 years of age, show significant
The apolipoprotein E 4 allele is a risk factor for vascular comorbidity, to the extent that they are
AD, but it does not appear to be associated with more accurately characterized as having mixed
increased risk of PSD.20 vascularAD dementia. 27 In longitudinal
studies and large clinicopathological series
with necropsy confirmation, the observed
Strategic infarct dementia morpho-anatomical substrates are largely
The view that a certain threshold volume of determined by study entry criteria. Autopsy
brain tissue loss (e.g. >50100 ml) predictably investigations in individuals who develop
causes dementia is no longer widely accepted; dementia after large cortical or subcortical
OCTOBER 2006 VOL 2 NO 10 SELNES AND VINTERS NATURE CLINICAL PRACTICE NEUROLOGY 539
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
cystic infarcts will show different patterns more-severe white matter lesions had a twofold
of lesions from studies in which patients are increased risk of dementia.37 In prospective
selected for a high likelihood of deep lacunar studies, the presence of periventricular white
infarcts or subcortical white matter alterations, matter lesions at baseline was found to double
including leukoaraiosis.6,28 Such populations the risk of future dementia.21 There is also
of patients are also likely to differ in their evidence that progression of white matter
clinical progression; those with small deep disease is accompanied by a decline in cogni-
lacunar infarcts (especially within the white tive performance, supporting an etiological
matter) or multiple microinfarcts are less link between the white matter changes and
likely to show a stepwise progression of cogni- cognitive decline.32,38
tive impairment than are those with regions Although epidemiological studies have clearly
of substantial cystic encephalomalacia. In one established an association of subcortical white
large autopsy series, pure VaD was seen in 9.4% matter lesions with poorer performance in
of 900 individuals with dementia, but in only specific cognitive domains,39 the cognitive
2.9% of patients with the clinical diagnosis of expression of subcortical small vessel disease in
probable or possible AD.29 Some investigators individual patients is highly variable. In a patient
suggest that VaD might account for only 23% who presents with mild cognitive impairment
of dementias,30 and others claim that pure VaD and mild subcortical white matter lesions, the
is almost nonexistent in large dementia series, etiological significance of the white matter
even when careful necropsies are performed.31 lesions cannot be easily determined. Neither a
Even though a mixed etiology is likely to be history of risk factors for cerebrovascular disease
more common than either pure AD or VaD nor the clinical presentation can establish that
among older patients, there are no current the cognitive symptoms are causally related to
clinical criteria for ante-mortem diagnosis the white matter findings. On the one hand,
of mixed dementia.4 there are case reports of patients with MRI-
documented widespread white matter disease
whose cognitive functioning is normal even
Subcortical small-vessel ischemic disease by detailed neuropsychological testing.40 On
White matter hyperintensities and lacunar the other hand, it is also well known that white
infarcts demonstrated by MRI are generally matter abnormalities are commonly seen in
considered to be evidence of small-vessel or patients with AD.41
microvascular ischemic disease, although some Although there is no cognitive profile that is
are related to dilated perivascular spaces.1 White entirely specific for subcortical vascular disease,
matter abnormalities on MRI are common in neuropsychological testing can nevertheless
otherwise healthy community-dwelling indi- identify whether the overall pattern is predomi-
viduals.32 The prevalence of these abnormali- nantly cortical or subcortical. In patients who
ties increases sharply with age, and other risk present with cognitive changes in the context
factors include hypertension, diabetes and of risk factors for cerebrovascular disease,
genetic factors.33,34 In patients with known and with MRI findings of subcortical white
cardiovascular disease, such as candidates for matter disease, the finding of a predominantly
coronary artery bypass grafting, the preva- subcortical profile will significantly increase
lence has been reported to be as high as 50%.35 the likelihood that the cognitive symptoms
Pathologically, MRI white matter signal abnor- are of vascular origin. The profile of neuro-
malities reflect focal and diffuse lesions of the psychological test findings alone cannot rule
subcortical and periventricular white matter, as out possible primary or coexisting AD, but if
well as lacunes and microinfarcts of the central follow-up testing demonstrates stable or rela-
gray matter.36 tively minor change over time, this can further
Because white matter abnormalities are support a diagnosis of VCI.
so common in otherwise asymptomatic An important but unresolved question is
individuals, they are often considered to be whether subcortical small-vessel disease by
benign. There is increasing evidence, however, itself can lead to cognitive impairment of
that white matter abnormalities on MRI are sufficient severity to meet the criteria for
associated with an increased risk of dementia. dementia. Overall, the cognitive expression of
In cross-sectional studies, individuals with isolated white matter hyperintensities appears
540 NATURE CLINICAL PRACTICE NEUROLOGY SELNES AND VINTERS OCTOBER 2006 VOL 2 NO 10
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
to be limited to mild motor and psychomotor of AD principally by milder memory impair-
slowing rather than a pervasive, severe degree ment but more-pronounced impairment of
of cognitive impairment.42 There is growing executive functions.56,57
evidence, however, that the subcortical white For several reasons, it has been difficult to
matter changes visualized on conventional resolve the question of the specificity of the
MRI might be incomplete markers of more- cognitive profile of VCI. First, if all etiologies
widespread, covert hypoxiaischemia-related of VCI are considered together, there is little
injury.43,44 With improvements in the ability reason to expect a consistent cognitive profile.
to quantify the overall burden of vascular The cognitive profile of dementia secondary
disease affecting the brain, including the pres- to large cortical infarcts might depend on
ence of hypoperfusion,45,46 microinfarcts47,48 both the location and volume of the lesion,
and amyloid angiopathy,49 a more-precise and would consequently be highly variable.
assessment of the relationship between cerebro- Second, because comprehensive cognitive
vascular changes and cognitive impairment testing cannot easily be performed in large
might become possible. clinical or community samples, many of the
studies with detailed testing have been limited
by modest sample sizes.58,59 A third reason why
Cerebral autosomal dominant some investigators have not found consistent
arteriopathy with subcortical infarcts differences between the cognitive profiles of
and leukoencephalopathy vascular and AD-type cognitive impairment
Cerebral autosomal dominant arteriopathy with is that not all cognitive domains have been
subcortical infarcts and leukoencephalopathy explored in sufficient detail. One of the more
(CADASIL) is a hereditary non-amyloid type of robust neuropsychological characteristics of
small-vessel disease that is commonly associated patients with subcortical disease is a slowing
with cognitive impairment or dementia.50,51 of motor and psychomotor speed,39 a feature
It results from either a gain or a loss of one that is not typically associated with cortical
or three cysteine residues in the extracellular dementias. Because most studies have not
N-terminal region of the NOTCH3 gene, which included measures of motor speed in their
is located on chromosome 19p13.52 Affected test battery, however, psychomotor speed has
deep cerebral arteries show destruction of the not generally been considered to be a unifying
smooth cell layer in their media, accompanied feature of VCI.55,59
by progressive wall thickening, and luminal Studies that have focused on patients with
narrowing caused by this thickening and VCI of sufficient severity to meet the criteria
fibrosis. Clinically, the condition is character- for dementia have generally found impairments
ized by recurrent subcortical strokes in patients across most cognitive domains, with more
aged between 40 years and 60 years. The clinical similarities to than differences from AD. These
manifestations include cognitive impairment studies are likely to have included a subset of
and psychiatric symptoms, with a generally patients with dementia of mixed etiology.55,60
variable clinical course.53 Some patients may In patients with less-severe cognitive impair-
initially present with only migraine headaches ment, a more distinctive cognitive profile might
and no cognitive symptoms. The diagnosis is be discernable. Garrett and colleagues reported
made by a combination of characteristic MRI that the neuropsychological performance of a
findings and genetic testing. small group of patients with cognitive impair-
ment (but no dementia) was characterized by
disproportionate executive dysfunction and
NEUROCOGNITIVE CONSIDERATIONS deficits in verbal retrieval.59 Data from Looi
There has been considerable debate with respect and colleagues61 also confirm an overall profile
to the specificity of the cognitive profile asso- of less-severe memory impairment and greater
ciated with VCI. Some people have argued that executive impairment in VaD. Several inves-
there is significant overlap between the cogni- tigators have reported a profile of memory
tive profiles of subcortical vascular disease and impairment that includes better preservation
cortical dementias such as AD.54,55 Others have of recognition memory performance relative to
suggested that the cognitive profile of subcortical free recall in patients with VCI.58,62 In studies
vascular disease can be distinguished from that of patients with CADASIL, who are generally
OCTOBER 2006 VOL 2 NO 10 SELNES AND VINTERS NATURE CLINICAL PRACTICE NEUROLOGY 541
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
patient in whom the history, imaging findings
Ischemic vascular dementia (IVD)
Multi-infarct dementia (MID) and clinical presentation are otherwise consis-
tent with subcortical vascular disease, a neuro-
Microglial/astroglial proliferation
cognitive profile of relatively preserved language
Secreted factors and recognition memory, but with significant
Blood vessel-derived factors motor and psychomotor slowing and impaired
executive performance, can be considered to
be supportive of a diagnosis of probable VCI
Pathogenesis of Consequences for CNS
rather than AD.
vascular disease parenchyma
macro/micro [?] (ischemia partial/complete)
NEUROPATHOLOGIC SUBSTRATES
OF VASCULAR COGNITIVE
IMPAIRMENT
Atheroma AS/LH Synapse and dendritic spine loss
CAA (spor/fam) Wallerian degeneration From a neuropathologic perspective, the
FMD
?Vasculitis CADASIL Trans-synaptic degeneration problem of studying ischemic VaD can be
Cardiogenic emboli Others Retrograde cortical neuronal changes reducedwith the understanding that this is
Others a huge oversimplificationto examining three
major inter-related, yet functionally separable,
pathophysiologic components: cerebrovascular
disease, systemic mediators of ischemic brain
Systematic factors necrosis (which of course might interact with
(hypotension, hypoxia) cerebrovascular disease), and the CNS paren-
chymal lesions that we recognize as being the
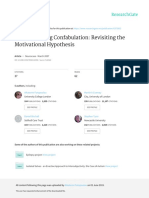
Figure 1 Conceptual framework for etiology and pathogenesis of result of cerebrovascular disease and systemic
ischemic vascular dementia, taking into account cerebrovascular factors. Once irreversible parenchymal injury
disease, systemic factors and ischemic necrosis of the brain, as well as has occurred, there are downstream and
retrograde or downstream effects of focal ischemic lesions. Abbreviations: retrograde effects in the CNS that result from
AS, arteriosclerosis; CAA, cerebral amyloid angiopathy; CADASIL,
the insultas a function of Wallerian, trans-
cerebral autosomal dominant arteriopathy with subcortical infarcts and
leukoencephalopathy; FMD, fibromuscular dysplasia; LH, lipohyalinosis; synaptic and other types of degeneration
spor/fam, sporadic/familial. (Figure 1)which almost certainly affect subse-
quent neurobehavioral morbidity in ways that
we do not yet understand.4,67 Subcortical axonal
injury and loss might be key elements in VaD
younger and therefore less likely to have pathogenesis and progression.68 The identity of
concomitant AD pathologic changes, speed of the neuropathologic substrates of leukoaraiosis,
processing has consistently been identified as which also affects subcortical white matter, is
impaired, with somewhat less-pronounced but still controversial, but might include apoptosis
significant deficits in areas of executive perfor- of oligodendroglia.69
mance and attention. It has been suggested Ischemic parenchymal lesions in patients
that this pattern of impairment represents the with VaD vary in size. In a longitudinal
core of the cognitive syndrome associated with California-wide study of patients pre-selected
small-vessel subcortical ischemic disease.6365 for a high likelihood of subcortical ischemic
Only a few studies have examined the cogni- lesions, especially lacunar infarcts (based on
tive profile of autopsy-confirmed cases of VCI ante-mortem neuroimaging studies), we have
and dementia.66 These studies have emphasized arbitrarily subcategorized infarcts seen at
considerable variability in the clinical presenta- autopsy as cystic infarcts (larger than 1.0 cm in
tion and the profile of neuropsychological greatest dimension), lacunar infarcts (grossly
test findings. visible on cut sections of the brain but smaller
Although the cognitive profile of subcortical than 1.0 cm in size), and microinfarcts (not
VCI might vary somewhat according to both seen on gross inspection of the cut brain,
etiology and severity of the disease, the pattern but identified by microscopy; see Figure 2).6
of relative preservation and impairment is Immunohistochemical stains that are especially
nonetheless helpful in a clinical setting. In a helpful for demonstrating microinfarcts include
542 NATURE CLINICAL PRACTICE NEUROLOGY SELNES AND VINTERS OCTOBER 2006 VOL 2 NO 10
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
those using primary antibodies against CD68 A B
or other macrophagemicroglial markers, and
those using primary antibodies against glial
fibrillary acidic protein (GFAP). Both of these
stains highlight areas of localized proliferation
of cells that react to irreversible ischemic injury.
The roles of astrocytes and microgliaand the
factors that they secretein the progression
of subinfarctive ischemia are not yet known.
Abundant old cortical microinfarcts render C D
the cortical surface irregular; an affected brain
is sometimes described as showing granular
atrophy, even though the causal lesions are
infarctive rather than atrophic.
Cystic infarcts often result from occlusion
of large meningeal arteries affected by athero-
sclerosis, sometimes as a result of atheroemboli
that lodge within themsuch atheroemboli might Figure 2 Microscopic appearance of brain lesions commonly encountered in
also originate in severely atherosclerotic carotid the brains of individuals with cerebrovascular disease and dementia. (A,B) Two
small arteries with marked onion skin-type thickening in the brain of a 68-year-
or vertebral arteries in the neck.70 Cystic infarcts
old man. (C) A slit-like microinfarct (arrows) perpendicular to the pial surface (left),
can also occur as wedge-shaped regions of with a larger triangular region of necrosis at its base near the cortexwhite matter
encephalomalacia in the border zone between junction. (D) Small old linear parenchymal infarct (arrows) filled with macrophages.
two large territories of supply by cerebral
arteries. As discussed above, strategically placed
small infarcts might be just as likely to lead to
dementia as larger infarcts.1,71 A
Lacunar infarcts have historically been
attributed to arteriosclerotic microangiopathy
affecting cerebral parenchymal arteries, a
process sometimes described as lipohyalinosis
and linked etiologically to longstanding hyper-
tension, although that association has recently
been called into question.28,72 Therefore, the
term hypertensive microvascular disease as
a synonym for lipohyalinosis is best avoided.
Lacunar infarcts (Figure 3) have been further
classified into various subtypes on the basis of
their neuropathologic components; the different
types include Ia (small cystic cavity containing B
small blood vessels and a few macrophages),
Ib (incomplete necrosis with perivascular rare-
faction and patchy astrocytic gliosis), and II (an
old microhemorrhage with abundant hemo-
siderin-laden macrophages).72 Hippocampal
injury, often resembling hippocampal scle-
rosis, identified in the medial temporal lobes of Figure 3 Lacunar infarcts. (A) Lacunar infarct
patients with intractable temporal lobe epilepsy (arrowhead) in the left basal ganglia of a patient
(with severe segmental neuron loss in the CA1 with dementia. Larger cystic infarcts (arrows) are
segment of the pyramidal cell layer and frequent seen at the junction of the right basal ganglia with
the adjacent white matter, and in the white matter
preservation of CA2) is now recognized as a
of the right centrum semiovale. (B) Lacunar infarcts
common neuropathologic finding in the CNS in the pons of a different patient (arrows). Lacunar
of elderly patients with dementia, and should infarcts are thought to be one consequence of
probably be considered as part of the spectrum longstanding hypertension, although the strength
of VaD.6,73 of this association has recently been questioned.
OCTOBER 2006 VOL 2 NO 10 SELNES AND VINTERS NATURE CLINICAL PRACTICE NEUROLOGY 543
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
A B that almost all AD patients have some degree of
CAA when this is diligently sought by multiple
sections from autopsy brains.7779 In rare cases,
individuals with prominent CAA lack other
neuropathologic characteristics of AD (senile
plaques and neurofibrillary tangles), and might
not show signs of dementia during their life-
time.80 Severe CAA, in which the medial layer
of many or most cortical arterioles is completely
replaced by amyloid, is also comparatively rare.
Replacement of the smooth muscle cell layer
C D
of the arteriolar media by fibrillar amyloid
renders the vessel susceptible to spontaneous
rupture, which can occur with mild increases
in intravascular pressure or when thrombo-
lytic agents are administered.76 This can result
in nontraumatic lobar cerebral hemorrhage,
although this is an infrequent occurrence
considering the vast numbers of individuals
who have some degree of CAA.74,77 In biopsy
or autopsy brain specimens, antibodies to
E amyloid- (A) protein (especially A140,
as opposed to A142) effectively immuno-
label arteriolar and capillary walls, showing
that vascular amyloid in CAA is similar to the
amyloid in senile plaques.75
A small subset of patients with sporadic or
age-related CAA develop superimposed vascu-
litis. This granulomatous vasculitis, often with
a significant giant cell component, appears to
result from amyloid deposition in arteriolar
Figure 4 Cerebral amyloid angiopathy, sporadic, with extensive old walls, rather than being a cause of amyloid
microinfarcts throughout the CNS. The specimens were taken from a
deposition.81 Recent studies have indicated
77-year-old patient who was considered clinically to have Alzheimers
disease (AD), and who showed significant AD changes in the hippocampus that vasculitis with CAA might present with a
and neocortex at autopsy. (A,B) Hematoxylin and eosin-stained sections (at clinically distinctive syndrome of rapid cogni-
low and high magnification, respectively) show severe thickening of cerebral tive decline and seizures, rather than cerebral
parenchymal arterioles, in which the media has been replaced by eosinophilic hemorrhage.82 There is also growing interest
glassy hyaline material (arrows). (C) Amyloid- (A) immunohistochemistry in the likelihood that patients with severe CAA
shows replacement of many arteriolar walls by A-immunoreactive material
might represent an underappreciated variant
(arrows). (D) Multiple remote microinfarcts (similar to those indicated by
arrows) and microhemorrhages were found throughout all areas of the cortex.
of VaD (Figure 4).83 In our California-wide
(E) Infarcts were highlighted by CD68 and glial fibrillary acidic protein (GFAP) longitudinal study of individuals at high risk
immunohistochemistry (this panel shows anti-GFAP immunoreactivity). for VaD, as many as 810% of those exam-
ined at necropsy showed severe CAA, often
with associated cortical microinfarcts, severe
subcortical leukoencephalopathy or both.
Cerebral amyloid angiopathy It might be predicted that all of these indi-
Cerebral amyloid angiopathy (CAA) describes viduals would also have advanced (Braak
an enigmatic microangiopathy that affects stage VVI) AD, but instead, a subset of them
meningeal and cortical arterioles, venules and showed Alzheimerization of the CNS that did
capillaries, whereby the normal vessel wall not extend to the isocortical stage. Further
becomes replaced by fibrillar amyloid.7476 The characterization of this interesting patient
most common form of CAA is an age-related group is in progress. In large casecontrol
vasculopathy that appears to be confined to the studies, A CAA has been established as a risk
brain. CAA is strongly associated with AD, such factor for cerebral ischemic infarcts.84
544 NATURE CLINICAL PRACTICE NEUROLOGY SELNES AND VINTERS OCTOBER 2006 VOL 2 NO 10
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
An autosomal dominant syndrome of KEY POINTS
dementia and stroke (cerebral hemorrhage), Several clinical subtypes of vascular cognitive
characterized by extensive, often over- impairment due to vascular disease are now
whelming and widely distributed meningo- recognized, ranging in severity from mild
cortical CAA, results from a point mutation in cognitive impairment to dementia
codon 693 of the gene that codes for amyloid The risk of dementia after stroke is increased
precursor protein (APP). The resulting in older patients and in those with pre-existing
disease, which is observed in circumscribed cognitive impairment or cerebrovascular
regions of the Netherlands, is described as here- disease
ditary cerebral hemorrhage with amyloidosis,
The cognitive consequences of subcortical
Dutch-type (HCHWA-D).74,85 Interestingly, small-vessel disease is variable, suggesting
dementia in these patients clearly appears to that the subcortical white matter changes
be linked to the severity or burden of CAA visualized on conventional MRI might be
rather than to the density of senile plaques incomplete markers of the total burden of
and neurofibrillary tangles.86 This indicates cerebrovascular disease
that sporadic, age-related or AD-associated
The cognitive profile of vascular cognitive
CAA, especially when severe, might be a impairment is predominantly subcortical, with
significantperhaps even definingfactor prominent psychomotor slowing and executive
in the cognitive decline in this disorder. Other deficits, but relatively preserved language and
familial syndromes in which A-immuno- recognition memory
reactive CAA is a dominant neuropathologic
From a neuropathologic perspective, the
finding result from mutations in codons
morphologic substrates or correlates of
692694 of the APP gene.74,76 Very recently, a vascular dementia are extremely heterogeneous
neuropathologically pure form of CAA was
identified in association with an autosomal Cerebral microvascular diseases, both
dominant APP L705V point mutation within sporadic and genetically determined, including
the A sequence.87 cerebral autosomal dominant arteriopathy with
subcortical infarcts and leukoencephalopathy
(CADASIL) and cerebral amyloid angiopathy,
are instructive in terms of providing pathologic
CONCLUSIONS models of age-related arteriopathies and their
The field of cerebrovascular disease and consequences for brain parenchyma
cognitive impairment has made significant
progress over the past decade, including the The brains of aged individuals are likely to
show impaired function as a consequence
discovery of CADASIL, the first genetic form
of combined Alzheimerization and
of a vascular cognitive disorder. Several chal- cerebrovascular disease
lenges lie ahead, however. Population-based
epidemiological studies suggest a continuum
of AD-type pathology and vascular brain
References
disease, and the relatively arbitrary separation 1 Chui H (2005) Neuropathology lessons in vascular
of AD and vascular dementia may no longer be dementia. Alzheimer Dis Assoc Disord 19: 4552
2 Fernando MS and Ince PG (2004) Vascular pathologies
the most productive approach. Improvements and cognition in a population-based cohort of elderly
in neuroimaging have demonstrated that brain people. J Neurol Sci 226: 1317
microvascular disease becomes increasing ly 3 Neuropathology Group of the Medical Research
Council Cognitive Function and Ageing Study (2001)
common with advancing age, but the poor Pathological correlates of late-onset dementia in a
correlation with degree of cognitive impair- multicentre, community-based population in
ment indicates that better measures to capture England and Wales. Neuropathology Group of the
Medical Research Council Cognitive Function and
the total burden of vascular disease of the Ageing Study (MRC CFAS). Lancet 357:
brain are needed. Ultimately, the importance 169175
of better understanding of the pathophysiology 4 OBrien JT et al. (2003) Vascular cognitive impairment.
Lancet Neurol 2: 8998
of dementia with cerebrovascular disease 5 Rockwood K et al. (2005) Clinical and radiographic
is the potential that some of the risk factors subtypes of vascular cognitive impairment in a clinic-
might be treatable, so that the incidence of based cohort study. J Neurol Sci 240: 714
6 Vinters HV et al. (2000) Neuropathologic substrates of
this age-related disorder might eventually ischemic vascular dementia. J Neuropathol Exp Neurol
be reduced. 59: 931945
OCTOBER 2006 VOL 2 NO 10 SELNES AND VINTERS NATURE CLINICAL PRACTICE NEUROLOGY 545
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
7 Pohjasvaara T et al. (2000) Comparison of different 32 Longstreth WT Jr et al. (2005) Incidence,
clinical criteria (DSM-III, ADDTC, ICD-10, NINDS- manifestations, and predictors of worsening white
AIREN, DSM-IV) for the diagnosis of vascular matter on serial cranial magnetic resonance imaging
dementia. National Institute of Neurological Disorders in the elderly: the Cardiovascular Health Study. Stroke
and Stroke-Association Internationale pour la 36: 5661
Recherche et lEnseignement en Neurosciences. 33 Schmidtke K and Hull M (2005) Cerebral small vessel
Stroke 31: 29522957 disease: how does it progress? J Neurol Sci 229230:
8 Bowler JV (2002) The concept of vascular cognitive 1320
impairment. J Neurol Sci 203204: 1115 34 Ringelstein EB and Nabavi DG (2005) Cerebral small
9 Sachdev P (1999) Vascular cognitive disorder. Int J vessel diseases: cerebral microangiopathies. Curr
Geriatr Psychiatry 14: 402403 Opin Neurol 18: 179188
10 Roman GC et al. (2004) Vascular cognitive disorder: a 35 Goto T et al. (2001) Magnetic resonance imaging
new diagnostic category updating vascular cognitive findings and postoperative neurologic dysfunction in
impairment and vascular dementia. J Neurol Sci 226: elderly patients undergoing coronary artery bypass
8187 grafting. Ann Thorac Surg 72: 137142
11 Roman GC et al. (2002) Subcortical ischaemic 36 Udaka F et al. (2002) White matter lesions and
vascular dementia. Lancet Neurol 1: 426436 dementia: MRIpathological correlation. Ann NY Acad
12 Leys D et al. (2005) Poststroke dementia. Lancet Sci 977: 411415
Neurol 4: 752759 37 Kuller LH et al. (2005) Determinants of vascular
13 Linden T et al. (2004) Cognitive impairment and dementia in the Cardiovascular Health Cognition
dementia 20 months after stroke. Neuroepidemiology Study. Neurology 64: 15481552
23: 4552 38 Prins ND et al. (2005) Cerebral small-vessel disease
14 Desmond DW et al. (2002) Incidence of dementia after and decline in information processing speed, executive
ischemic stroke: results of a longitudinal study. Stroke function and memory. Brain 128: 20342041
33: 22542260 39 de Groot JC et al. (2000) Cerebral white matter lesions
15 Henon H et al. (2001) Poststroke dementia: incidence and cognitive function: the Rotterdam Scan Study. Ann
and relationship to prestroke cognitive decline. Neurol 47: 145151
Neurology 57: 12161222 40 Duning T et al. (2005) Excellent cognitive performance
16 Luchsinger JA et al. (2005) Aggregation of vascular despite massive cerebral white matter changes.
risk factors and risk of incident Alzheimer disease. Neuroradiology 47: 749752
Neurology 65: 545551 41 de Leeuw FE et al. (2004) Alzheimers diseaseone
17 Barba R et al. (2000) Poststroke dementia: clinical clinical syndrome, two radiological expressions:
features and risk factors. Stroke 31: 14941501 a study on blood pressure. J Neurol Neurosurg
18 Pohjasvaara T et al. (2000) How complex interactions Psychiatry 75: 12701274
of ischemic brain infarcts, white matter lesions, and 42 Mosley TH Jr et al. (2005) Cerebral MRI findings and
atrophy relate to poststroke dementia. Arch Neurol 57: cognitive functioning: the Atherosclerosis Risk in
12951300 Communities study. Neurology 64: 20562062
19 Lin JH et al. (2003) Prediction of poststroke dementia. 43 Roman GC (2004) Brain hypoperfusion: a critical factor
Neurology 61: 343348 in vascular dementia. Neurol Res 26: 454458
20 Rowan E et al. (2005) Impact of hypertension and 44 Kalaria RN et al. (2001) Multiple substrates of late-
apolipoprotein E4 on poststroke cognition in subjects onset dementia: implications for brain protection.
>75 years of age. Stroke 36: 18641868 Novartis Found Symp 235: 4960
21 Vermeer SE et al. (2003) Silent brain infarcts and the 45 de Leeuw FE et al. (2000) Atrial fibrillation and the
risk of dementia and cognitive decline. N Engl J Med risk of cerebral white matter lesions. Neurology 54:
348: 12151222 17951801
22 Perren F et al. (2005) The syndrome of combined polar 46 Markus HS et al. (2000) Reduced cerebral blood flow in
and paramedian thalamic infarction. Arch Neurol 62: white matter in ischaemic leukoaraiosis demonstrated
12121216 using quantitative exogenous contrast based perfusion
23 Madureira S et al. (1999) A follow-up study of cognitive MRI. J Neurol Neurosurg Psychiatry 69: 4853
impairment due to inferior capsular genu infarction. 47 Werring DJ et al. (2004) Cognitive dysfunction in
J Neurol 246: 764769 patients with cerebral microbleeds on T2*-weighted
24 Longstreth WT Jr (2005) Brain vascular disease overt gradient-echo MRI. Brain 127: 22652275
and covert. Stroke 36: 20622063 48 Kovari E et al. (2004) Cortical microinfarcts and
25 Gold G et al. (1998) Re-evaluating the role of vascular demyelination significantly affect cognition in brain
changes in the differential diagnosis of Alzheimers aging. Stroke 35: 410414
disease and vascular dementia. Eur Neurol 40: 121129 49 Vinters HV (2001) Cerebral amyloid angiopathy: a
26 Ott A et al. (1999) Diabetes mellitus and the risk of microvascular link between parenchymal and vascular
dementia: The Rotterdam Study. Neurology 53: dementia? Ann Neurol 49: 691693
19371942 50 Chabriat H and Bousser MG (2003) CADASIL. Cerebral
27 Langa KM et al. (2004) Mixed dementia: emerging autosomal dominant arteriopathy with subcortical
concepts and therapeutic implications. JAMA 292: infarcts and leukoencephalopathy. Adv Neurol 92:
29012908 147150
28 Kalimo H (Ed.; 2005) Pathology and Genetics: 51 Dichgans M (2002) CADASIL: a monogenic condition
Cerebrovascular Diseases. Basel: ISN Neuropath Press causing stroke and subcortical vascular dementia.
29 Jellinger KA (2002) The pathology of ischemic- Cerebrovasc Dis 13 (Suppl 2): 3741
vascular dementia: an update. J Neurol Sci 203204: 52 Miao Q et al. (2004) Fibrosis and stenosis of the
153157 long penetrating cerebral arteries: the cause of
30 Hansen LA and Crain BJ (1995) Making the diagnosis the white matter pathology in cerebral autosomal
of mixed and non-Alzheimers dementias. Arch Pathol dominant arteriopathy with subcortical infarcts and
Lab Med 119: 10231031 leukoencephalopathy. Brain Pathol 14: 358364
31 Nolan KA et al. (1998) Absence of vascular dementia in 53 Opherk C et al. (2004) Long-term prognosis and
an autopsy series from a dementia clinic. J Am Geriatr causes of death in CADASIL: a retrospective study in
Soc 46: 597604 411 patients. Brain 127: 25332539
546 NATURE CLINICAL PRACTICE NEUROLOGY SELNES AND VINTERS OCTOBER 2006 VOL 2 NO 10
2006 Nature Publishing Group
REVIEW
www.nature.com/clinicalpractice/neuro
54 Arango-Lasprilla JC et al. (2005) Cortical and 71 Del ST et al. (1990) Vascular dementia: a Acknowledgments
subcortical diseases: do true neuropsychological clinicopathological study. J Neurol Sci 96: 117 Work in H Vinters laboratory
differences exist? Arch Clin Neuropsychol 21: 2940 72 Lammie GA (2002) Hypertensive cerebral small vessel is supported by PHS grants
55 Laukka EJ et al. (2004) Similar patterns of cognitive disease and stroke. Brain Pathol 12: 358370 P50 AG 16570 and P01
deficits in the preclinical phases of vascular dementia 73 Dickson DW et al. (1994) Hippocampal sclerosis: a AG 12435. The research of
and Alzheimers disease. J Int Neuropsychol Soc 10: common pathological feature of dementia in very old O Selnes is supported by
382391 (> or = 80 years of age) humans. Acta Neuropathol PHS grant 35610 (NINCDS).
56 Frisoni GB et al. (2002) Mild cognitive impairment with (Berl) 88: 212221 Technical assistance
subcortical vascular features: clinical characteristics 74 Verbeek MM et al. (2000) Cerebral Amyloid Angiopathy provided by Justine
and outcome. J Neurol 249: 14231432 in Alzheimers Disease and Related Disorders. Pomakian and Negar
57 Graham NL et al. (2004) Distinctive cognitive profiles Dordrecht: Kluwer Academic Publishers Khanlou. We thank Pamela
in Alzheimers disease and subcortical vascular 75 Revesz T et al. (2002) Sporadic and familial cerebral Talalay for her editorial
dementia. J Neurol Neurosurg Psychiatry 75: 6171 amyloid angiopathies. Brain Pathol 12: 343357 assistance.
58 Tierney MC et al. (2001) Recognition memory and 76 Rensink AA et al. (2003) Pathogenesis of cerebral
verbal fluency differentiate probable Alzheimer disease amyloid angiopathy. Brain Res Brain Res Rev 43: Competing interests
from subcortical ischemic vascular dementia. Arch 207223 The authors declared
Neurol 58: 16541659 77 Vinters HV (1987) Cerebral amyloid angiopathy: they have no competing
59 Garrett KD et al. (2004) The neuropsychological profile a critical review. Stroke 18: 311324 interests.
of vascular cognitive impairmentno dementia: 78 Vinters HV et al. (1996) Brain parenchymal and
comparisons to patients at risk for cerebrovascular microvascular amyloid in Alzheimers disease. Brain
disease and vascular dementia. Arch Clin Pathol 6: 179195
Neuropsychol 19: 745757 79 Greenberg SM et al. (1993) The clinical spectrum of
60 Fahlander K et al. (2002) Cognitive functioning in cerebral amyloid angiopathy: presentations without
Alzheimers disease and vascular dementia: further lobar hemorrhage. Neurology 43: 20732079
evidence for similar patterns of deficits. J Clin Exp 80 Vinters HV (1992) Cerebral amyloid angiopathy and
Neuropsychol 24: 734744 Alzheimers disease: two entities or one? J Neurol Sci
61 Looi JC and Sachdev PS (1999) Differentiation of 112: 13
vascular dementia from AD on neuropsychological 81 Anders KH et al. (1997) Giant cell arteritis in
tests. Neurology 53: 670678 association with cerebral amyloid angiopathy:
62 Traykov L et al. (2002) Neuropsychological deficit in immunohistochemical and molecular studies. Hum
early subcortical vascular dementia: comparison to Pathol 28: 12371246
Alzheimers disease. Dement Geriatr Cogn Disord 14: 82 Eng JA et al. (2004) Clinical manifestations of cerebral
2632 amyloid angiopathy-related inflammation. Ann Neurol
63 Peters N et al. (2005) The pattern of cognitive 55: 250256
performance in CADASIL: a monogenic condition 83 Haglund M et al. (2004) Severe cerebral amyloid
leading to subcortical ischemic vascular dementia. Am angiopathy characterizes an underestimated variant
J Psychiatry 162: 20782085 of vascular dementia. Dement Geriatr Cogn Disord 18:
64 Buffon F et al. (2006) Cognitive profile in CADASIL. 132137
J Neurol Neurosurg Psychiatry 77: 175180 84 Cadavid D et al. (2000) Cerebral beta amyloid
65 OSullivan M et al. (2004) Diffusion tensor imaging of angiopathy is a risk factor for cerebral ischemic
thalamus correlates with cognition in CADASIL without infarction: a case control study in human brain
dementia. Neurology 62: 702707 biopsies. J Neuropathol Exp Neurol 59: 768773
66 Reed BR et al. (2004) Clinical and neuropsychological 85 Vinters HV et al. (1998) Secondary microvascular
features in autopsy-defined vascular dementia. Clin degeneration in amyloid angiopathy of patients with
Neuropsychol 18: 6374 hereditary cerebral hemorrhage with amyloidosis,
67 Vinters HV et al. (1998) Diagnostic Neuropathology, Dutch type (HCHWA-D). Acta Neuropathol (Berl) 95:
149. New York: Marcel Dekker Inc. 235244
68 Medana IM and Esiri MM (2003) Axonal damage: a key 86 Natte R et al. (2001) Dementia in hereditary cerebral
predictor of outcome in human CNS diseases. Brain hemorrhage with amyloidosis-Dutch type is
126: 515530 associated with cerebral amyloid angiopathy but is
69 Brown WR et al. (2000) Apoptosis in leukoaraiosis. independent of plaques and neurofibrillary tangles.
AJNR Am J Neuroradiol 21: 7982 Ann Neurol 50: 765772
70 Hulette C et al. (1997) Clinical-neuropathologic 87 Obici L et al. (2005) A novel APP mutation exclusively
findings in multi-infarct dementia: a report of six associated with cerebral amyloid angiopathy. Ann
autopsied cases. Neurology 48: 668672 Neurol 58: 639644
OCTOBER 2006 VOL 2 NO 10 SELNES AND VINTERS NATURE CLINICAL PRACTICE NEUROLOGY 547
2006 Nature Publishing Group
You might also like
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- PlaneacionestrategicaDocument9 pagesPlaneacionestrategicadianisvillarrealNo ratings yet
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Emotional Empathy and Facial Reactions To Facial ExpressionsDocument6 pagesEmotional Empathy and Facial Reactions To Facial ExpressionsdianisvillarrealNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Dimberg Et Al 2012 Empathy EMG PDFDocument10 pagesDimberg Et Al 2012 Empathy EMG PDFdianisvillarrealNo ratings yet
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Rehabilitación de Funciones Ejecutivas - TirapuDocument4 pagesRehabilitación de Funciones Ejecutivas - TirapudianisvillarrealNo ratings yet
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Weiss Btox EHS American PsychologistDocument14 pagesWeiss Btox EHS American PsychologistdianisvillarrealNo ratings yet
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- A Social-Neuroscience Perspective On EmpathyDocument5 pagesA Social-Neuroscience Perspective On EmpathydianisvillarrealNo ratings yet
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Déficit en FAUX PAS, en Personas Con Lesión Frontal MedialDocument7 pagesDéficit en FAUX PAS, en Personas Con Lesión Frontal MedialdianisvillarrealNo ratings yet
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Recognition of Emotion From Facial Expression Following Traumatic Brain InjuryDocument14 pagesRecognition of Emotion From Facial Expression Following Traumatic Brain InjurydianisvillarrealNo ratings yet
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Tomm 1.1Document107 pagesTomm 1.1dianisvillarrealNo ratings yet
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Executive Functions and ADHD in Adults EvidenceDocument13 pagesExecutive Functions and ADHD in Adults Evidencedianisvillarreal100% (1)
- Proficiency and Control in Verbal Fluency Performance Across The Lifespan For Monolinguals and BilingualsDocument24 pagesProficiency and Control in Verbal Fluency Performance Across The Lifespan For Monolinguals and BilingualsdianisvillarrealNo ratings yet
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Executive Functions and ADHD in Adults Evidence FoDocument9 pagesExecutive Functions and ADHD in Adults Evidence FodianisvillarrealNo ratings yet
- Evidence-Based Cognitive Rehabilitation: Updated Review of The Literature From 2003 Through 2008Document12 pagesEvidence-Based Cognitive Rehabilitation: Updated Review of The Literature From 2003 Through 2008hsvm1989No ratings yet
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Executive Functions and ADHD in Adults EvidenceDocument13 pagesExecutive Functions and ADHD in Adults Evidencedianisvillarreal100% (1)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Instruction Manual Instructions For Patient Health Questionnaire (PHQ) and GAD-7 MeasuresDocument9 pagesInstruction Manual Instructions For Patient Health Questionnaire (PHQ) and GAD-7 MeasuresJefry JapNo ratings yet
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- DañocerebralylesiondifusaDocument15 pagesDañocerebralylesiondifusadianisvillarrealNo ratings yet
- Evidence-Based Cognitive Rehabilitation: Updated Review of The Literature From 2003 Through 2008Document12 pagesEvidence-Based Cognitive Rehabilitation: Updated Review of The Literature From 2003 Through 2008hsvm1989No ratings yet
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- DimbergDocument4 pagesDimbergdianisvillarrealNo ratings yet
- The Neuropsychological Profile of Vascular Cognitive Impairment in Stroke and TIA PatientsDocument9 pagesThe Neuropsychological Profile of Vascular Cognitive Impairment in Stroke and TIA PatientsdianisvillarrealNo ratings yet
- Cog RehabDocument55 pagesCog RehabHarsha RamchurnNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Self-Enhancing Confabulation: Revisiting The Motivational HypothesisDocument12 pagesSelf-Enhancing Confabulation: Revisiting The Motivational HypothesisdianisvillarrealNo ratings yet
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- 2015 Article 288-2 PDFDocument9 pages2015 Article 288-2 PDFRamos SilalahiNo ratings yet
- Manual NPIDocument6 pagesManual NPIdianisvillarrealNo ratings yet
- Vascular Cognitive Impairment-2006 PDFDocument10 pagesVascular Cognitive Impairment-2006 PDFdianisvillarrealNo ratings yet
- Mini Mental Parkinson Test Standardization and NorDocument4 pagesMini Mental Parkinson Test Standardization and NordianisvillarrealNo ratings yet
- Cognitive Performance After Ischaemic StrokeDocument11 pagesCognitive Performance After Ischaemic StrokedianisvillarrealNo ratings yet
- Tree Book Information SheetDocument2 pagesTree Book Information SheetdianisvillarrealNo ratings yet
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Cognitive Performance After Ischaemic StrokeDocument11 pagesCognitive Performance After Ischaemic StrokedianisvillarrealNo ratings yet
- Vascular Cognitive Impairment-2006 PDFDocument10 pagesVascular Cognitive Impairment-2006 PDFdianisvillarrealNo ratings yet
- Posner Article Orienting of Attention PDFDocument24 pagesPosner Article Orienting of Attention PDFdianisvillarrealNo ratings yet
- Biology - Igcse - Past PaperDocument6 pagesBiology - Igcse - Past Papersollu786_889163149100% (1)
- (19437714 - HortTechnology) Foliar Sprays of Silver Thiosulfate Produce Male Flowers On Female Hemp PlantsDocument5 pages(19437714 - HortTechnology) Foliar Sprays of Silver Thiosulfate Produce Male Flowers On Female Hemp PlantsNilton FerreiraNo ratings yet
- Personal Identification RVWRDocument26 pagesPersonal Identification RVWRShaira Mae GallegoNo ratings yet
- PRL 8Document2 pagesPRL 8anna ticaNo ratings yet
- USP General Chapter (1115) Bioburdin Control For Non Sterile Drug SubstanceDocument8 pagesUSP General Chapter (1115) Bioburdin Control For Non Sterile Drug SubstanceDr usama El Shafey100% (7)
- NPK Plant Basic DesignDocument4 pagesNPK Plant Basic DesignDidier SanonNo ratings yet
- GlanceDocument30 pagesGlanceKajan_MuneeswaranNo ratings yet
- Falcon Pocket Guide - Trees (PDFDrive)Document107 pagesFalcon Pocket Guide - Trees (PDFDrive)wikibiNo ratings yet
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- 2010 Lennette's - Laboratory - Diagnosis PDFDocument512 pages2010 Lennette's - Laboratory - Diagnosis PDFHumberto Azuara Jiménez100% (1)
- Nursing Health History ReyDocument10 pagesNursing Health History ReyNikki MarieNo ratings yet
- Dr. John's Mother Tinctures & Dilutions List Dr. John's Mother Tinctures & Dilutions ListDocument6 pagesDr. John's Mother Tinctures & Dilutions List Dr. John's Mother Tinctures & Dilutions ListAnand KumarNo ratings yet
- Formulation and Evaluation of Floating in Situ Gel Based Gastroretentive Drug Delivery of Ciprofloxacin HCLDocument11 pagesFormulation and Evaluation of Floating in Situ Gel Based Gastroretentive Drug Delivery of Ciprofloxacin HCLiajpsNo ratings yet
- Gianna Pomata (Editor), Nancy G. Siraisi (Editor) - Historia - Empiricism and Erudition in Early Modern Europe (Transformations - Studies in The History of Science and Technology) (2006)Document493 pagesGianna Pomata (Editor), Nancy G. Siraisi (Editor) - Historia - Empiricism and Erudition in Early Modern Europe (Transformations - Studies in The History of Science and Technology) (2006)Marcelo Rizzo100% (1)
- Benthic Macroinvertebrates in Freshwaters - Taxa Tolerance Values, Metrics, and ProtocolsDocument128 pagesBenthic Macroinvertebrates in Freshwaters - Taxa Tolerance Values, Metrics, and Protocolstiago_henrique_3100% (1)
- BAI TAP ON VE DAU TRONG AM - TU CO 3 AM TIET (CO DAP AN) - T I 123doc - VNDocument3 pagesBAI TAP ON VE DAU TRONG AM - TU CO 3 AM TIET (CO DAP AN) - T I 123doc - VNNgô Huyền ThươngNo ratings yet
- Encircle The Correct Answer: PPSC Lecturer BIOLOGY 2020Document5 pagesEncircle The Correct Answer: PPSC Lecturer BIOLOGY 2020Sajjad AhmadNo ratings yet
- HybridizationDocument19 pagesHybridizationSamer EhabNo ratings yet
- 11th International Symposium On Urolithiasis Nice France 25 Sept 2008Document76 pages11th International Symposium On Urolithiasis Nice France 25 Sept 2008assemNo ratings yet
- AdatinaDocument1 pageAdatinaCRISTIELI IZABEL FOGUESATTONo ratings yet
- AMINOGLYCOSIDESDocument2 pagesAMINOGLYCOSIDESDiana Marcela Gomez PintoNo ratings yet
- Womersley Arterial Flow - SimpleDocument10 pagesWomersley Arterial Flow - SimplebhatsindhoorNo ratings yet
- Creature IDs - Official ARK - Survival Evolved WikiDocument19 pagesCreature IDs - Official ARK - Survival Evolved WikikirosandiskNo ratings yet
- PT3.1 SurnameDocument2 pagesPT3.1 SurnamePADERES MARGARETTE GALARIONo ratings yet
- A Quick Overview of Genetic Engineering and EctoDocument1 pageA Quick Overview of Genetic Engineering and EctoHannah Grace AquinoNo ratings yet
- ProfessionDocument6 pagesProfessionRI NANo ratings yet
- DP Biology - Speciation Lesson PlanDocument2 pagesDP Biology - Speciation Lesson Planapi-257190713100% (1)
- Pengembangan Sediaan Vitamin C Lepas Lambat Dengan Pemanfaatan Material Nanosilika DAUN BAMBU (Bambusa SP.)Document10 pagesPengembangan Sediaan Vitamin C Lepas Lambat Dengan Pemanfaatan Material Nanosilika DAUN BAMBU (Bambusa SP.)hanifahNo ratings yet
- Gynecology PDFDocument537 pagesGynecology PDFCrystal Nguyen100% (1)
- Postbiotics-Parabiotics The New Horizons in Microbial Biotherapy and Functional FoodsDocument22 pagesPostbiotics-Parabiotics The New Horizons in Microbial Biotherapy and Functional FoodsLevente BalázsNo ratings yet
- An Autobiography of Trauma: A Healing JourneyFrom EverandAn Autobiography of Trauma: A Healing JourneyRating: 5 out of 5 stars5/5 (2)
- Summary: The Myth of Normal: Trauma, Illness, and Healing in a Toxic Culture By Gabor Maté MD & Daniel Maté: Key Takeaways, Summary & AnalysisFrom EverandSummary: The Myth of Normal: Trauma, Illness, and Healing in a Toxic Culture By Gabor Maté MD & Daniel Maté: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (9)
- Rewire Your Anxious Brain: How to Use the Neuroscience of Fear to End Anxiety, Panic, and WorryFrom EverandRewire Your Anxious Brain: How to Use the Neuroscience of Fear to End Anxiety, Panic, and WorryRating: 4.5 out of 5 stars4.5/5 (157)
- Somatic Therapy Workbook: A Step-by-Step Guide to Experiencing Greater Mind-Body ConnectionFrom EverandSomatic Therapy Workbook: A Step-by-Step Guide to Experiencing Greater Mind-Body ConnectionNo ratings yet