Professional Documents
Culture Documents
Osteoarthritis of The Knee - Patient Information and Exercises - PHYSIO 001 PDF
Uploaded by
Zola Ismu ArjunantoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Osteoarthritis of The Knee - Patient Information and Exercises - PHYSIO 001 PDF
Uploaded by
Zola Ismu ArjunantoCopyright:
Available Formats
Osteoarthritis of the Knee
Patient Information and Exercises
Integrated Musculoskeletal Service
Physiotherapy Department
Osteoarthritis (OA) of the Knee
Information and Exercise Leaflet for
Patient’s and Carers
What is osteoarthritis?
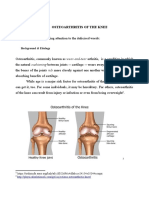
Arthritis means inflammation of the joints. Osteoarthritis (OA) is the most common form of
arthritis in the UK. OA mainly affects the joint cartilage and the bone tissue next to the cartilage.
What causes osteoarthritis?
All normal joints and joint tissues are constantly undergoing some form of repair because of the
wear and tear that is placed on them through our daily activities. However, in some people, it
seems that this repair process becomes faulty in some way (perhaps because of severe wear
and tear to the joints or a problem with the repair process) and OA develops.
In joints with OA, the joint cartilage becomes damaged and worn. The bone tissue next to the
cartilage can also be affected and bony growths can develop around the joint edges. These
growths are called osteophytes and may be seen on X-rays. The joints and the surrounding
tissues can also become inflamed. This inflammation is called synovitis.
Factors that may play a role in the development of OA include:
Age: OA becomes more common with increasing age. By the age of 65, at least half of
people will have some OA in some joint(s).
Genetics: There may be some inherited tendency for OA to develop in some people.
Obesity: Knee OA is more likely to develop, or be more severe, in obese people. This is
because there is an increased load on the joints and a potential for more joint damage.
Your sex: Women are more likely to develop OA than men.
Previous joint injury, damage or deformity: This may include previous joint infection, a
previous fracture (break in the bone) around a joint, or a previous ligament injury that
caused a joint to become unstable.
MSK / Osteoarthritis of the Knee / Aug 2014 / Page 1 of 5
Osteoarthritis of the Knee
Patient Information and Exercises
What are the symptoms of osteoarthritis?
In some cases no symptoms may occur. Quite a number of people can have X-ray
changes that indicate some degree of OA but have no, or only very mild, symptoms.
Pain, stiffness, and limitation in full movement of the joint are typical. The stiffness tends
to be worse first thing in the morning but tends to loosen up after half an hour or so.
Swelling and inflammation of an affected joint can sometimes occur.
An affected joint tends to look a little larger than normal. This is due to overgrowth of the
bone next to damaged cartilage.
You may have poor mobility and problems walking if your knee is badly affected.
Do I need any tests?
Your doctor can often diagnose osteoarthritis based on your age, your typical symptoms and
examination of your affected joints. Tests such as X-rays or blood tests are usually not needed.
However, sometimes your doctor may suggest X-rays or other tests if they are uncertain about
the diagnosis and want to exclude other problems.
What is the outlook for people with osteoarthritis?
The severity of symptoms can vary. In many people, OA is mild and does not make you any
more disabled than expected for your age. However, in some people, the severity of OA and
the disability it causes is out of proportion to your age.
What are the aims of physiotherapy?
The aim of physiotherapy is to increase joint mobility, improve muscle strength and try and
relieve pain.
General measures to help treat osteoarthritis:
Exercise
If possible, exercise regularly. This helps to strengthen the muscles around affected joints, to
keep you fit, and to maintain a good range of joint movement.
Weight control
If you are overweight, try to lose some weight as the extra burden placed on your knees can
make symptoms worse. Even a modest weight loss can make quite a difference.
Walking aids
If you have OA of your hip or knee, when walking try using a walking stick. Hold it in the hand
on the opposite side of the body to the affected joint. This takes some pressure of the affected
joint and helps to ease symptoms in some cases.
MSK / Osteoarthritis of the Knee / Aug 2014 / Page 2 of 5
Osteoarthritis of the Knee
Patient Information and Exercises
Other therapies
Some people find that they can also get some pain relief from using hot or cold packs.
Try wrapping crushed ice in a damp towel and hold it for five to ten minutes against the
part of your hip that hurts. You can do this every two to three hours. Make sure you use
a damp towel between the ice and the skin to avoid ice burn.
Alternatively you could use a heat pad or a hot water bottle with an insulated cover on it.
Make sure this is not too hot and not directly touching your skin. You should this for 10 to
15 minutes, three to four times a day.
Some people have found that transcutaneous electrical nerve stimulator (TENS)
machines help to ease pain from OA. A TENS machine delivers small electrical pulses to
the body via electrodes placed on the skin.
Acupuncture may also help to ease symptoms in some cases.
Warning Signs
If you have severe pain which is getting worse over several weeks, if you are unwell with
back or full leg pain, or under the age of 16 years, you should consult your doctor.
The following symptoms are very rare, but if you suddenly develop any of them, you
should consult your doctor straightaway.
Significant swelling to the leg not just the knee
Feeling generally unwell
Signs of infection i.e. night sweats that are out of the ordinary, high temperature and
feeling unwell.
Constant night pain (unable to rest/sleep)
Unexplained weight loss
If your symptoms fail to improve within 6 weeks with this regime you should contact
your doctor for a physiotherapy referral.
If this is the case remember to bring a pair of shorts to change in to, this will help the
physiotherapist diagnose your problem.
MSK / Osteoarthritis of the Knee / Aug 2014 / Page 3 of 5
Osteoarthritis of the Knee
Patient Information and Exercises
MSK / Osteoarthritis of the Knee / Aug 2014 / Page 4 of 5
Osteoarthritis of the Knee
Patient Information and Exercises
Integrated Musculoskeletal Service Author: Physiotherapy
ID No: PHYSIO - 001 – Osteoarthritis of the Knee
Date of Issue: December 2014 Review Date: November 2016
Contact details
Physiotherapy Department Physiotherapy Department
Burnley General Hospital – Tel: 01282 803294 Royal Blackburn Hospital – Tel: 01254 735091
MSK / Osteoarthritis of the Knee / Aug 2014 / Page 5 of 5
You might also like
- Medical Application FormDocument3 pagesMedical Application FormBogdan Brdar100% (1)
- Endodontic Clinic Manual 2015 - 1Document134 pagesEndodontic Clinic Manual 2015 - 1Adina Popa100% (2)
- Knee Pain: Treating Knee Pain: Preventing Knee Pain: Natural Remedies, Medical Solutions, Along With Exercises And Rehab For Knee Pain ReliefFrom EverandKnee Pain: Treating Knee Pain: Preventing Knee Pain: Natural Remedies, Medical Solutions, Along With Exercises And Rehab For Knee Pain ReliefRating: 5 out of 5 stars5/5 (1)
- Oman New Reimbursement Claim FormDocument3 pagesOman New Reimbursement Claim Formtoalok4723No ratings yet
- OsteoarthritisDocument17 pagesOsteoarthritisNishaThakuriNo ratings yet
- All About Arthritis- Find Updated Causes, Symptoms, Diagnostic Tests, New Alternative Treatments, Cures and BreakthroughsFrom EverandAll About Arthritis- Find Updated Causes, Symptoms, Diagnostic Tests, New Alternative Treatments, Cures and BreakthroughsNo ratings yet
- Maternal and Child Nursing QuestionsDocument87 pagesMaternal and Child Nursing QuestionsAnn Michelle Tarrobago50% (2)
- Obstetric Analgesia PDFDocument45 pagesObstetric Analgesia PDFBoneyJalgar100% (1)
- CANINE-Medical Management of Chronic Otitis in DogsDocument11 pagesCANINE-Medical Management of Chronic Otitis in Dogstaner_soysuren100% (1)
- ArthritisDocument54 pagesArthritisPeby M. Ramdhan100% (1)
- OsteoarthritisDocument5 pagesOsteoarthritisprincess0fdeathNo ratings yet
- OsteoarthritisDocument5 pagesOsteoarthritisRobby Dwitria MaulanaNo ratings yet
- Hip Osteonecrosis A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHip Osteonecrosis A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- 7-Steps For DI Systematic ApproachDocument8 pages7-Steps For DI Systematic ApproachDrDeepak Pawar71% (7)
- 4R's of RadiobiologyDocument32 pages4R's of Radiobiologyarif081190No ratings yet
- Pernicious AnemiaDocument36 pagesPernicious Anemiaopesh3No ratings yet
- Arthritis: Types of Arthritis: The most important information you need to improve your healthFrom EverandArthritis: Types of Arthritis: The most important information you need to improve your healthNo ratings yet
- Osteoarthritis: Natural Drugless Treatments That Really Work!From EverandOsteoarthritis: Natural Drugless Treatments That Really Work!No ratings yet
- Answer and Rationale Psychiatric NursingDocument23 pagesAnswer and Rationale Psychiatric NursingCharles Gerard B. BeluanNo ratings yet
- Pain in Your Butt PreformisDocument3 pagesPain in Your Butt PreformiscloudoverhillNo ratings yet
- Diet DM 1700 P 40: Energi: 1700 Kkal Protein: 40 Gram Lemak: 51 Gram Karbohidrat: 257.5 GramDocument7 pagesDiet DM 1700 P 40: Energi: 1700 Kkal Protein: 40 Gram Lemak: 51 Gram Karbohidrat: 257.5 GramBrevi Istu PambudiNo ratings yet
- Osteoarthritis ExplanationDocument6 pagesOsteoarthritis ExplanationmedicembuNo ratings yet
- Osteoarthritis EssayDocument8 pagesOsteoarthritis EssayMeysha PNo ratings yet
- Osteoarthritis - Surgical Therapy, Alternative Medicine and Proper ExerciseDocument5 pagesOsteoarthritis - Surgical Therapy, Alternative Medicine and Proper ExerciseElsa Novi WulansariNo ratings yet
- Living With Osteoarthritis 2013Document36 pagesLiving With Osteoarthritis 2013Hoinaru FerdinandNo ratings yet
- Osteoarthritis: T Person's of Developing Osteoarthritis. It IncludesDocument5 pagesOsteoarthritis: T Person's of Developing Osteoarthritis. It IncludesLove Shery SabrosoNo ratings yet
- Osteoarthritis: Done By: Shameem Faheem Group 6Document32 pagesOsteoarthritis: Done By: Shameem Faheem Group 6Alisha ShamsNo ratings yet
- Common Causes of Severe Knee PainDocument8 pagesCommon Causes of Severe Knee PainRatnaPrasadNalamNo ratings yet
- OsteoarthritisDocument63 pagesOsteoarthritisDuaa BalochNo ratings yet
- Osteoarthritis PocDocument4 pagesOsteoarthritis PocIrene Joy GomezNo ratings yet
- OsteoarthritisDocument6 pagesOsteoarthritisgovindhaNo ratings yet
- OsteoarthritisDocument6 pagesOsteoarthritisgovindhaNo ratings yet
- Osteoarthritis: and OsteoporosisDocument4 pagesOsteoarthritis: and OsteoporosisJansen LeeNo ratings yet
- Osteoarthritis: CausesDocument5 pagesOsteoarthritis: CausesYahya i.nNo ratings yet
- Osteoarthtritis Symptoms: Older Age. The Risk of Osteoarthritis Increases With AgeDocument4 pagesOsteoarthtritis Symptoms: Older Age. The Risk of Osteoarthritis Increases With AgeJessica AdhykaNo ratings yet
- Dr. Jonaidi T, SPKFR Instalasi Rehabilitasi Medik Rsud Dr. Soedarso, PontianakDocument29 pagesDr. Jonaidi T, SPKFR Instalasi Rehabilitasi Medik Rsud Dr. Soedarso, PontianakHerlam SyahNo ratings yet
- Aunty ProjectDocument13 pagesAunty Projectdevansh kumarNo ratings yet
- YOU Don'T Have To Live With Joint Pain: A Patient'S Guide To The Causes and Treatment of Joint PainDocument18 pagesYOU Don'T Have To Live With Joint Pain: A Patient'S Guide To The Causes and Treatment of Joint PainbaboosabNo ratings yet
- Osteoarthritis: Applied Medicine BY: Dr. Kinza IftikharDocument16 pagesOsteoarthritis: Applied Medicine BY: Dr. Kinza IftikharsabaamjadNo ratings yet
- Arthritis AdviceDocument6 pagesArthritis Adviceapi-309082881No ratings yet
- Arthritis (Cabansag, Ma. Flor-And-Cabansag, Joyce)Document38 pagesArthritis (Cabansag, Ma. Flor-And-Cabansag, Joyce)Carlojay IniegoNo ratings yet
- Mayumi - How To Cure OsteoarthritisDocument4 pagesMayumi - How To Cure OsteoarthritisMayumi SariputraNo ratings yet
- Erbil Polytechnic University Erbil Health Technical College Physiotherapy Department Study Year 2020-2021Document13 pagesErbil Polytechnic University Erbil Health Technical College Physiotherapy Department Study Year 2020-2021Muhamad SdeqNo ratings yet
- Symptoms: Medications To Help Relieve PainDocument2 pagesSymptoms: Medications To Help Relieve PaincithzNo ratings yet
- KneeDocument3 pagesKneedoos1No ratings yet
- What Causes Osteoarthritis?Document9 pagesWhat Causes Osteoarthritis?jajabsNo ratings yet
- Osteoarthritis DissertationDocument8 pagesOsteoarthritis DissertationPaperHelpJackson100% (1)
- OsteoarthritisDocument6 pagesOsteoarthritisKristine ValenciaNo ratings yet
- A Positive Response To Ankylosing Spondylitis: Guidebook For PatientsDocument18 pagesA Positive Response To Ankylosing Spondylitis: Guidebook For PatientsdipanshuroyNo ratings yet
- Osteoarthritis of The Knee CopieDocument20 pagesOsteoarthritis of The Knee CopieNarcisYonutzNo ratings yet
- Assignment Submitted To DR Iqra Naz 70063678 Habiba Jameel DPT 10 Semester. Topic: ArthritisDocument10 pagesAssignment Submitted To DR Iqra Naz 70063678 Habiba Jameel DPT 10 Semester. Topic: ArthritisMuiz SaddozaiNo ratings yet
- Causes and Tips For Coping With Chronic Knee PainDocument6 pagesCauses and Tips For Coping With Chronic Knee PainRatnaPrasadNalamNo ratings yet
- Osteoarthritis and Fibromyalgia: by Tamara MitchellDocument13 pagesOsteoarthritis and Fibromyalgia: by Tamara MitchellmailbabuNo ratings yet
- OsteoarthritisDocument4 pagesOsteoarthritisdrnareshNo ratings yet
- Osteoarthritis PDFDocument15 pagesOsteoarthritis PDFعبدالرحمن علىNo ratings yet
- PBL Joint PainDocument11 pagesPBL Joint PainMuhd FawwazNo ratings yet
- Cotul Reumatic EnglezaDocument7 pagesCotul Reumatic EnglezaElena GaneaNo ratings yet
- Word To PDFDocument119 pagesWord To PDFshravaniNo ratings yet
- OsteoarthritisDocument3 pagesOsteoarthritisVanessa Da CruzNo ratings yet
- Arthritis HWDocument9 pagesArthritis HWraphaelNo ratings yet
- Arthritis of The Knee - OrthoInfo - AAOSDocument5 pagesArthritis of The Knee - OrthoInfo - AAOSMarcelo KrauseNo ratings yet
- OsteoarthritisDocument23 pagesOsteoarthritisGoutham VGouthamNo ratings yet
- Distal Clavicle Osteolysis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandDistal Clavicle Osteolysis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Thesis On Osteoarthritis KneeDocument4 pagesThesis On Osteoarthritis Kneednrrt4fr100% (2)
- Steopathic Nformation Ervice: OSTEOPATHY: SportsDocument5 pagesSteopathic Nformation Ervice: OSTEOPATHY: SportsAnonymous GzRz4H50FNo ratings yet
- Skeletal Joint: Dr. Vareishang Tangpu Assistant Professor in Zoology RIE, Mysore - 06Document53 pagesSkeletal Joint: Dr. Vareishang Tangpu Assistant Professor in Zoology RIE, Mysore - 06Floriza de LeonNo ratings yet
- 3 LWG Knee Pain Part 1Document1 page3 LWG Knee Pain Part 1Woo Guan LeeNo ratings yet
- Arthritis: Osteoarthritis (OA or Degenerative Arthritis) Osteoarthritis FactsDocument6 pagesArthritis: Osteoarthritis (OA or Degenerative Arthritis) Osteoarthritis FactsFelisitas FellNo ratings yet
- ES Task 4 - ArticleDocument4 pagesES Task 4 - ArticleTaraa_CNo ratings yet
- Abstract Bhs IngDocument1 pageAbstract Bhs IngZola Ismu ArjunantoNo ratings yet
- Studi Fenomenologi Pengalaman Keluarga Merawat Anggotanya Yang Menderita Halusinasi Di Rumah Sakit Jiwa JambiDocument7 pagesStudi Fenomenologi Pengalaman Keluarga Merawat Anggotanya Yang Menderita Halusinasi Di Rumah Sakit Jiwa JambiZola Ismu ArjunantoNo ratings yet
- Meningitis & EncephalitisDocument18 pagesMeningitis & EncephalitisZola Ismu ArjunantoNo ratings yet
- Osteoarthritis of The Knee - Patient Information and Exercises - PHYSIO 001Document5 pagesOsteoarthritis of The Knee - Patient Information and Exercises - PHYSIO 001Zola Ismu ArjunantoNo ratings yet
- Lecture 9 Reading Assignment 2Document9 pagesLecture 9 Reading Assignment 2Dennis KorirNo ratings yet
- Bladder Calculus Resulting From The Migration of An IntrauterineDocument8 pagesBladder Calculus Resulting From The Migration of An IntrauterineFabrien Hein WillemNo ratings yet
- Single Phase Correction of Tongue Thrust Habit AloDocument7 pagesSingle Phase Correction of Tongue Thrust Habit AloAkhil SinghNo ratings yet
- Comprehensive Assessment Diagnosis and Treatment Planning of Severe Periodontal DiseaseDocument9 pagesComprehensive Assessment Diagnosis and Treatment Planning of Severe Periodontal DiseaseJOHAYMEN MANGORSINo ratings yet
- Leptospirosis CaseDocument29 pagesLeptospirosis CaseJp RectraNo ratings yet
- Truncated Middle Turbinnate SNPDocument4 pagesTruncated Middle Turbinnate SNPSriram RajanNo ratings yet
- Levels of EvidenceDocument4 pagesLevels of EvidenceshineeicaNo ratings yet
- Narayana Hrudalaya - Section D Group 7Document4 pagesNarayana Hrudalaya - Section D Group 7Prateek100% (1)
- Assessing Nutrition in Patients With Chronic Kidney Disease by Kimberly Thompson, MS, RD, LDNDocument23 pagesAssessing Nutrition in Patients With Chronic Kidney Disease by Kimberly Thompson, MS, RD, LDNCarlos RaiolNo ratings yet
- Deep Back Massage 3Document11 pagesDeep Back Massage 3Anonymous ecK9pw1O3QNo ratings yet
- Adamantinoma: Sebok Daniel Sucher ErwinDocument34 pagesAdamantinoma: Sebok Daniel Sucher ErwinGheorghe SebokNo ratings yet
- A Systematic Review: Optimal Management of Fatigue in Patients With Systemic Lupus ErythematosusDocument14 pagesA Systematic Review: Optimal Management of Fatigue in Patients With Systemic Lupus ErythematosusMelz Melz MutzNo ratings yet
- Osteoporosis and Fragility Fractures Surgical PerpspectiveDocument54 pagesOsteoporosis and Fragility Fractures Surgical PerpspectiveSonal DudaniNo ratings yet
- Introduction To Pharmacokinetics: Deborah RobertsonDocument3 pagesIntroduction To Pharmacokinetics: Deborah RobertsonTheresa Tyra SertaniNo ratings yet
- Biology 12 Unit 10 Assignment 1 Blood Pressure Virtual LabDocument6 pagesBiology 12 Unit 10 Assignment 1 Blood Pressure Virtual Labapi-338578874100% (1)
- Multidimensional Family Therapy - Working With AdolescentsDocument7 pagesMultidimensional Family Therapy - Working With AdolescentsLen PetersNo ratings yet
- Internet Addiction and Its Cognitive Behavioral Therapy: Ömer Şenormancı, Ramazan Konkan and Mehmet Zihni SungurDocument21 pagesInternet Addiction and Its Cognitive Behavioral Therapy: Ömer Şenormancı, Ramazan Konkan and Mehmet Zihni SungurShari' Si WahyuNo ratings yet
- Acupuncture Standards China Baoyan 2009Document50 pagesAcupuncture Standards China Baoyan 2009Marlon RamirezNo ratings yet