Professional Documents
Culture Documents
Acrokeratoelastoidosis With Nail Dystrophy
Uploaded by
600WPMPO0 ratings0% found this document useful (0 votes)
18 views3 pagesAcrokeratoelastoidosis With Nail Dystrophy
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentAcrokeratoelastoidosis With Nail Dystrophy
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
18 views3 pagesAcrokeratoelastoidosis With Nail Dystrophy
Uploaded by
600WPMPOAcrokeratoelastoidosis With Nail Dystrophy
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 3
Gefitinib: A Cause of Pyogenic
Granulomalike Lesions of the Nail
G eftinib (Iressa; AstraZeneca Pharmaceuticals LP,
Wilmington, Del) is an epidermal growth fac-
tor receptor (EGFR) tyrosine kinase inhibitor
used to treat non–small cell lung cancer (NSCLC). Re-
cently, this agent has been a point of controversy. In pa-
tients who demonstrate a response, the results are often
dramatic; however, such a response has occurred in as
few as 10% of treated patients.1
In June 2005, using data from a phase 3 trial that failed
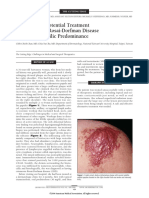
Figure. A 78-year-old woman presented with friable papules erupting from
to demonstrate prolonged survival, the US Food and Drug the proximal nail fold of each thumb following 8 weeks of gefitinib use for
Administration revised the labeling to indicate contin- non–small cell lung cancer.
ued use only in those with a prior response to gefitinib
or in further clinical trials.2 Similar related monoclonal medications, including systemic retinoids, antiretrovi-
antibodies include cetuximab, panitumumab, or erlo- ral agents such as indinavir, and capecitabine, a novel fluo-
tinib. Despite recognized cutaneous manifestations at- ropyrimidine used in the treatment of advanced breast
tributed to this entire class of EGFR inhibitors, there is and colorectal cancers.5 While underappreciated within
a paucity of discussion regarding such events within the much of the dermatology literature, gefitinib and other
major American dermatology journals. EGFR inhibitors should be recognized as a cause of such
an occurrence, and further study might yield other rel-
Report of a Case. A 78-year-old woman with NSCLC pre- evant cutaneous manifestations as well. Familiarity with
sented to our clinic with the complaint of exquisitely pain- these cutaneous reaction patterns may improve patient
ful erythematous papules erupting from the proximal nail care, particularly with the expanding use of such agents.
fold of both thumbs (Figure). The tissue was friable and
bled easily. For this reason, she kept the lesions covered Whitney A. High, MD
with bandages most of the time. She had consulted her
Correspondence: Dr High, Department of Dermatol-
oncologist and had also been examined by 2 dermatolo-
ogy, University of Colorado Health Sciences Center Can-
gists. Concern had focused on trauma-induced pyo-
cer Pavilion, PO Box 6510, Mail Stop F.703, Denver, CO
genic granulomas or possibly metastases from her can-
80045-0510 (whitney.high@uchsc.edu).
cer. There was no history of trauma. Interestingly, she
Financial Disclosure: None reported.
also reported tender erythema surrounding the nail folds
of her great toes and had a faint, follicularly centered, ery- 1. Frantz S. Drug discovery: playing dirty. Nature. 2005;437:942-943.
thematous and papular eruption on the face, neck, and 2. United States Food and Drug Administration. FDA Alert: Gefitinib (mar-
keted as Iressa) Information. http://www.fda.gov/cder/drug/infopage/ gefitinib
upper chest. A review of her medications revealed that /default.htm. Accessed October 30, 2005.
she had begun gefitinib treatment 2 months prior to the 3. Segaert S, Van Cutsem E. Clinical signs, pathophysiology and management
development of the lesions. of skin toxicity during therapy with epidermal growth factor receptor inhibitors.
Ann Oncol. 2005;16:1425-1433.
Cutaneous adverse effects of EGFR inhibitors in- 4. Lee MW, Seo CW, Kim SW, et al. Cutaneous side effects in non-small cell
clude acneiform eruptions, xerosis, trichomegaly, telan- lung cancer patients treated with Iressa (ZD1839), an inhibitor of epidermal
growth factor. Acta Derm Venereol. 2004;84:23-26.
giectasias, dyspigmentation, painful paronychia, nail 5. Piguet V, Borradori L. Pyogenic granuloma-like lesions during capecitabine
cracking, and pyogenic granulomalike lesions of the nail therapy. Br J Dermatol. 2002;147:1270-1272.
fold.3 An acneiform rash is identified in 50% to 100% of
patients taking EGFR inhibitors, and it appears to be dose
dependent.3 Nail changes are seen in 10% to 15% of pa-
tients and are typically a later event, beginning 4 to 8 weeks
Acrokeratoelastoidosis With Nail Dystrophy:
after initiation of therapy.4 The mechanism underlying
A Coincidence or a New Entity?
these cutaneous manifestations is unknown.3,4 Our pa-
tient demonstrated not only the acneiform rash but also
bilateral nail splitting with pyogenic granulomalike le-
sions of the thumbs after 8 weeks of gefitinib use.
Discontinuance of gefitinib therapy yielded slow but
complete resolution. The rash cleared in several weeks,
A crokeratoelastoidosis (AKE) was first de-
scribed in 1954.1 This dominant disorder is char-
acterized by the presence of small, skin-
colored to yellowish, round to polygonal papules on the
thenar and hypothenar eminences of the palms and on
and the lesions of the nails resolved over 6 weeks. It is
unclear whether other therapy, such as debridement or the plantar surfaces of the feet. Histologic examination
laser treatment, would have hastened resolution. Dis- typically shows broadening of the granular layer, with
continuance alone was satisfactory to her, and was ac- circumscribed hyperkeratosis in a cup-shaped depres-
ceptable to her oncologist. sion of the epidermis. Fragmentation of elastic fibers is
also found.2 Histologic studies are needed to differenti-
Comment. Pyogenic granulomalike lesions are a well- ate AKE from similar disorders such as focal acral hy-
recognized occurrence following treatment with certain perkeratosis, acrokeratosis verruciformis of Hopf, and
(REPRINTED) ARCH DERMATOL/ VOL 142, JULY 2006 WWW.ARCHDERMATOL.COM
939
©2006 American Medical Association. All rights reserved.
Figure 1. Nail dystrophy with pterygium formation (inset).
Figure 3. Typical histopathologic appearance, with hyperkeratosis overlying a
cup-shaped depression (hematoxylin-eosin, original magnification ⫻50). Inset,
Fragmentation of elastic fibrils (elastic van Gieson, original magnification ⫻100).
B
(Figure 2). A pronounced fetor was noted, prompting
an examination with a Wood light, which showed a coral-
red fluorescence between the toes, extending onto the
plantar surface of the feet (not shown). Histologic ex-
amination of a papule revealed broadening of the granu-
lar layer, with a circumscribed hyperkeratosis project-
ing into a cup-shaped depression of the epidermis. The
underlying dermis contained fragmented elastic fibers
(Figure 3). Based on these results, a diagnosis of AKE
with pitted keratolysis was made. Treatment with topi-
cal antibiotics resulted in clearance of the pits and dis-
Figure 2. A,Translucent polygonal papules on the thenar eminence;
appearance of the fetor.
B, hyperkeratosis with papules on the plantar surface.
Comment. The present case is unusual. The patient had
punctate palmoplantar keratoderma.3,4 To our knowl- pitted keratolysis, also referred to as keratoma sulcatum.
edge, no other skin abnormalities have been described We consider it unlikely that there is a direct association
in conjunction with AKE to date,4 but we recently saw a between pitted keratolysis and AKE, but in this case, the
patient with AKE that was accompanied by pitted kera- pitted keratolysis obscured the plantar keratoderma that
tolysis and nail dystrophy. can be part of AKE5 and resulted in a delay in diagnosis.
Nail dystrophy has not been previously described in AKE,
Report of a Case. A 47-year-old Dutch woman sought but subtle changes may well have escaped attention. The
help for abnormal nails. She had also noted thickening lifelong presence of the nail dystrophy, the fact that all nails
of the skin on the soles of her feet, which had an un- were affected, and the absence of skin changes, as seen in
pleasant smell. “Bumps” had been present on the pal- psoriasis or lichen planus, suggest that the nail abnormali-
mar surface of her hands for a long time, but she had paid ties in our patient are part of the phenotype. Careful ex-
no particular attention to them. Other family members amination for nail dystrophy in patients with AKE will help
were not affected. Her general health was good. Physi- to delineate the extent of nail disease in AKE.
cal examination revealed dystrophic nails with longitu-
dinal ridging, onychorrhexis, and distal onycholysis. Some Maurice A. M. van Steensel, MD, PhD
nails showed pterygia (Figure 1). Multiple polygonal Valerie L. R. M. Verstraeten, MD
to round, translucent, skin-colored papules of varying size Jorge Frank, MD, PhD
were present on the thenar and hypothenar eminences
of both hands. The soles of the feet demonstrated a yel- Correspondence: Dr van Steensel, Department of Derma-
low hyperkeratosis with grayish pits on the balls of the tology, University Hospital Maastricht, PO Box 5800, 6202
feet and polygonal papules along the edges of the soles AZ Maastricht, the Netherlands (mvst@sder.azm.nl).
(REPRINTED) ARCH DERMATOL/ VOL 142, JULY 2006 WWW.ARCHDERMATOL.COM
940
©2006 American Medical Association. All rights reserved.
Financial Disclosure: None reported. Comment. Trigeminal trophic syndrome is a rare com-
Funding/Support: Dr van Steensel’s research is sup- plication after peripheral or central damage to the tri-
ported by Barrier Therapeutics NV, Geel, Belgium, and geminal nerve.3 There are approximately 125 cases re-
by the International Pachyonychia Congenita Founda- ported in the literature, and of those, only 2 cases have
tion. Dr Verstraeten is supported by funds from the been reported in children with associated Herpes sim-
University Hospital Maastricht. Dr Frank is a member plex trigeminal neuritis and trigeminal neuralgia.1,2 The
of the Network for Ichthyoses and Related Keratiniza- ulcers usually present 2 to 30 weeks after injury to the
tion Disorders (NIRK), which is supported by the Ger- trigeminal ganglion.4 The lesions are characterized by cres-
man Federal Ministry of Education and Research cent-shaped erosions occurring in the dermatomal dis-
(BMBF). tribution of the trigeminal nerve, typically involving the
nasal ala, but they can also involve other areas such as
1. Costa OG. Acrokeratoelastoidosis. AMA Arch Derm Syphilol. 1954;70:228-231.
2. Fiallo P, Pesce C, Brusasco A, Nunzi E. Acrokeratoelastoidosis of Costa: a pri- the scalp, forehead, ear, palate, and jaw. Trigeminal tro-
mary disease of the elastic tissue? J Cutan Pathol. 1998;25:580-582. phic syndrome may also involve the mucous mem-
3. Korc A, Hansen RC, Lynch PJ. Acrokeratoelastoidosis of Costa in North America: branes, as was seen in this patient. Interestingly, our pa-
a report of two cases. J Am Acad Dermatol. 1985;12:832-836.
4. Lewis KG, Bercovitch L, Dill SW, Robinson-Bostom L. Acquired disorders of tient also went on to develop neurotrophic keratitis of
elastic tissue, II: decreased elastic tissue. J Am Acad Dermatol. 2004;51:165-
188.
5. Highet AS, Rook A, Anderson JR. Acrokeratoelastoidosis. Br J Dermatol. 1982;
106:337-344.
Trigeminal Trophic Syndrome:
A Pediatric Case
T rigeminal trophic syndrome (TTS) is a rare con-
dition characterized by unilateral facial ulcer-
ation, usually involving the nasal ala, resulting
from damage to the trigeminal nerve or its central sen-
sory root. To our knowledge, there are only 2 previ-
ously reported1,2 pediatric cases of TTS.
Report of a Case. An 8-year-old girl presented with a
2-month history of multiple ulcerations involving the left
side of her face. Significant medical history included a
possible pilocytic astrocytoma of the lower brainstem par-
tially resected at age 7 years. During a second resection,
the residual tumor was reclassified as a ganglioglioma.
Several months later, she presented to her primary care
physician with a crusted erosion on the left side of her
nose. Despite multiple courses of antibiotics for sus-
pected impetigo, the ulcerated lesions enlarged. Subse-
quently, the patient was referred to the dermatology and Figure 1. Crescent-shaped ulcerations involving the left medial infraorbital
otolaryngology departments for evaluation. region, chin, and cheek extending into the internal lateral nasal ala.
On initial examination, she was noted to have ery-
thematous, crescent-shaped ulcerations with crust on the
left medial infraorbital region, chin, cheek, and internal
left lateral nasal ala (Figure 1). An eroded white plaque
on the lateral left side of the tongue was also noted
(Figure 2). Superficial sensation did not seem to be de-
creased on the left side of her face. Vasculitis was not found
on serologic evaluation, and indirect immunofluores-
cence findings were negative. Histopathologic findings
revealed nonspecific necrosis and acute inflammation of
the involved skin and nasal mucosa. Viral, fungal, and
acid-fast bacilli tissue culture findings were negative. A
bacterial tissue culture was positive for methicillin-
resistant Staphylococcus aureus. Despite wound care and
antibiotic coverage for methicillin-resistant S aureus, the
ulcerations continued to worsen. A second opinion from
another pediatric dermatologist was therefore obtained,
and a clinical diagnosis of trigeminal trophic syndrome
was made. Figure 2. Eroded white plaque of the lateral left side of the tongue.
(REPRINTED) ARCH DERMATOL/ VOL 142, JULY 2006 WWW.ARCHDERMATOL.COM
941
©2006 American Medical Association. All rights reserved.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Role of The Palatine Tonsils in The Pathogenesis and Treatment of PsoriasisDocument6 pagesRole of The Palatine Tonsils in The Pathogenesis and Treatment of Psoriasis600WPMPONo ratings yet
- Nevus MarginatusDocument3 pagesNevus Marginatus600WPMPONo ratings yet
- Consistent Cutaneous Imaging With Commercial Digital CamerasDocument5 pagesConsistent Cutaneous Imaging With Commercial Digital Cameras600WPMPONo ratings yet
- A Unique Pattern of Hyperhidrosis and Herpes ZosterDocument1 pageA Unique Pattern of Hyperhidrosis and Herpes Zoster600WPMPONo ratings yet
- Acitretin and Pioglitazone in PsoriasisDocument7 pagesAcitretin and Pioglitazone in Psoriasis600WPMPONo ratings yet
- A Seeming Failure of LogicDocument2 pagesA Seeming Failure of Logic600WPMPONo ratings yet
- Development of Atopic Dermatitis During The First 3 Years of LifeDocument6 pagesDevelopment of Atopic Dermatitis During The First 3 Years of Life600WPMPONo ratings yet
- In Clinical: Lmages DermatologyDocument2 pagesIn Clinical: Lmages Dermatology600WPMPONo ratings yet
- Diltiazem Induces Severe Photodistributed HyperpigmentationDocument5 pagesDiltiazem Induces Severe Photodistributed Hyperpigmentation600WPMPONo ratings yet
- Dapsone As A Potential Treatment For Cutaneous Rosai-Dorfman Disease With Neutrophilic PredominanDocument3 pagesDapsone As A Potential Treatment For Cutaneous Rosai-Dorfman Disease With Neutrophilic Predominan600WPMPONo ratings yet
- A Unique Pattern of HyperhidrosisDocument1 pageA Unique Pattern of Hyperhidrosis600WPMPONo ratings yet
- Breakthrough in The Treatment of WartsDocument2 pagesBreakthrough in The Treatment of Warts600WPMPONo ratings yet
- A Model To Teach Elliptical Excision and Basic Suturing TechniquesDocument3 pagesA Model To Teach Elliptical Excision and Basic Suturing Techniques600WPMPONo ratings yet
- A Novel Visual Clue For The Diagnosis of Hypertrophic Lichen PlanusDocument1 pageA Novel Visual Clue For The Diagnosis of Hypertrophic Lichen Planus600WPMPONo ratings yet
- Psoriasis of The ScalpDocument7 pagesPsoriasis of The Scalp600WPMPONo ratings yet
- A Clinician's View of Urticarial DermatitisDocument2 pagesA Clinician's View of Urticarial Dermatitis600WPMPONo ratings yet
- ComicRack Manual (2nd Ed)Document124 pagesComicRack Manual (2nd Ed)600WPMPONo ratings yet
- A Comparison of Oral Methylprednisolone Plus Azathioprine or Mycophenolate Mofetil For The TreatmDocument8 pagesA Comparison of Oral Methylprednisolone Plus Azathioprine or Mycophenolate Mofetil For The Treatm600WPMPONo ratings yet
- Acne Vulgaris in Richly Pigmented PatientsDocument6 pagesAcne Vulgaris in Richly Pigmented Patients600WPMPONo ratings yet
- Acne Keloidalis NuchaeDocument5 pagesAcne Keloidalis Nuchae600WPMPONo ratings yet
- ComicRack Manual (3rd Ed) PDFDocument150 pagesComicRack Manual (3rd Ed) PDF600WPMPONo ratings yet
- ComicRack Manual 0.9.1 PDFDocument101 pagesComicRack Manual 0.9.1 PDF600WPMPONo ratings yet
- ComicRack Manual (5th Ed)Document179 pagesComicRack Manual (5th Ed)pescuma8153100% (2)
- ComicRack Manual (6th Ed)Document100 pagesComicRack Manual (6th Ed)600WPMPO100% (1)
- ComicRack Manual (4th Ed ULQ)Document178 pagesComicRack Manual (4th Ed ULQ)600WPMPONo ratings yet
- ComicRack Tips and Tricks (1st Ed)Document28 pagesComicRack Tips and Tricks (1st Ed)Johnny JohnsonNo ratings yet
- ComicRack Manual (3rd Ed Revised)Document150 pagesComicRack Manual (3rd Ed Revised)600WPMPONo ratings yet
- ComicRack Manual (2nd Ed)Document124 pagesComicRack Manual (2nd Ed)600WPMPONo ratings yet
- ComicRack Bugle 001 (2013)Document1 pageComicRack Bugle 001 (2013)600WPMPONo ratings yet
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Ds B2B Data Trans 7027Document4 pagesDs B2B Data Trans 7027Shipra SriNo ratings yet
- Kasapreko PLC Prospectus November 2023Document189 pagesKasapreko PLC Prospectus November 2023kofiatisu0000No ratings yet
- Orbit BioscientificDocument2 pagesOrbit BioscientificSales Nandi PrintsNo ratings yet
- Toyota TPMDocument23 pagesToyota TPMchteo1976No ratings yet
- Service Manual Pioneer CDJ 2000-2 (RRV4163) (2010)Document28 pagesService Manual Pioneer CDJ 2000-2 (RRV4163) (2010)GiancaNo ratings yet
- Mce Igcse Chemistry PPT c08Document57 pagesMce Igcse Chemistry PPT c08Shabanito GamingNo ratings yet
- Dalit LiteratureDocument16 pagesDalit LiteratureVeena R NNo ratings yet
- Earth & Life Science Q1 Module 2 - DESIREE VICTORINODocument22 pagesEarth & Life Science Q1 Module 2 - DESIREE VICTORINOJoshua A. Arabejo50% (4)
- Preterite vs Imperfect in SpanishDocument16 pagesPreterite vs Imperfect in SpanishOsa NilefunNo ratings yet
- Criminal Evidence Course OutlineDocument3 pagesCriminal Evidence Course OutlineChivas Gocela Dulguime100% (1)
- Resume John BunkerDocument8 pagesResume John BunkerJohn BunkerNo ratings yet
- Classic Failure FORD EdselDocument4 pagesClassic Failure FORD EdselIliyas Ahmad KhanNo ratings yet
- Volatility Clustering, Leverage Effects and Risk-Return Trade-Off in The Nigerian Stock MarketDocument14 pagesVolatility Clustering, Leverage Effects and Risk-Return Trade-Off in The Nigerian Stock MarketrehanbtariqNo ratings yet
- Siege by Roxane Orgill Chapter SamplerDocument28 pagesSiege by Roxane Orgill Chapter SamplerCandlewick PressNo ratings yet
- Unit 3 Test A Test (Z Widoczną Punktacją)Document4 pagesUnit 3 Test A Test (Z Widoczną Punktacją)Kinga WojtasNo ratings yet
- Apola Ose-Otura (Popoola PDFDocument2 pagesApola Ose-Otura (Popoola PDFHowe JosephNo ratings yet
- IAS Exam Optional Books on Philosophy Subject SectionsDocument4 pagesIAS Exam Optional Books on Philosophy Subject SectionsDeepak SharmaNo ratings yet
- Masters of Death: The Assassin ClassDocument5 pagesMasters of Death: The Assassin Classjbt_1234No ratings yet
- Music Literature (Western Music)Document80 pagesMusic Literature (Western Music)argus-eyed100% (6)
- Bhagavad Gita: Chapter 18, Verse 47Document3 pagesBhagavad Gita: Chapter 18, Verse 47pankaj kararNo ratings yet
- Modern Dental Assisting 11Th Edition Bird Test Bank Full Chapter PDFDocument37 pagesModern Dental Assisting 11Th Edition Bird Test Bank Full Chapter PDFRichardThompsonpcbd100% (9)
- Ramesh Dargond Shine Commerce Classes NotesDocument11 pagesRamesh Dargond Shine Commerce Classes NotesRajath KumarNo ratings yet
- Case Study 1Document2 pagesCase Study 1Diana Therese CuadraNo ratings yet
- Effects of Violence On Transgender PeopleDocument8 pagesEffects of Violence On Transgender PeopleAdel Farouk Vargas Espinosa-EfferettNo ratings yet
- ThumbDocument32 pagesThumbdhapraNo ratings yet
- Risk Assessment: Act/Hse/Ra 001: Use of Suspended Access Cradles and Platforms (Temporary Works)Document2 pagesRisk Assessment: Act/Hse/Ra 001: Use of Suspended Access Cradles and Platforms (Temporary Works)Saravana0% (1)
- A Story Behind..: Dimas Budi Satria Wibisana Mario Alexander Industrial Engineering 5Document24 pagesA Story Behind..: Dimas Budi Satria Wibisana Mario Alexander Industrial Engineering 5Owais AwanNo ratings yet
- Compatibility Testing: Week 5Document33 pagesCompatibility Testing: Week 5Bridgette100% (1)
- Hbet1103 Introduction To General LinguisticsDocument11 pagesHbet1103 Introduction To General LinguisticsNasidah NasahaNo ratings yet
- I Could Easily FallDocument3 pagesI Could Easily FallBenji100% (1)