Professional Documents
Culture Documents
Airway Management
Uploaded by
Michael SedanoCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Airway Management
Uploaded by
Michael SedanoCopyright:
Available Formats
AIRWAY MANAGEMENT a) Nasopharynx
Rashelle Lopez-Salvatierra, MD An upper area, separated from the lower
oropharynx by soft palate
b) Oropharynx
Airway management Extends from the soft palate to the base of the
Expertise in airway management is important in every tongue
medical specialty Tongue is the principal source of airway
Maintaining a patent airway is essential for adequate obstruction, usually due to decreased tone of the
oxygenation and ventilation genioglossus muscle
Failure to do so, even for a brief period of time, can be life C) Laryngopharynx
threatening.
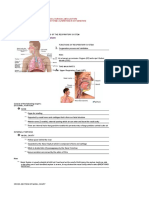
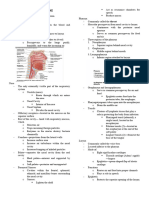
Anatomy of the Airway LARYNX
Airway Begins at the base of the tongue and ends at the
Extrapulmonary air passages beginning of the trachea
( nasal and oral cavities, pharynx, larynx, trachea LARYNX (C3-C6)
and large bronchi) Functions as:
- Open valve in respiration
- Partially closed valve during
phonation
- Closed valve during swallowing,
protecting the lower airway against
aspiration
Its closure also insists in the development of
intrathoracic pressure associated with coughing,
defacation, micturation and lifting heavy objects
Comparative anatomy of the pediatric and adult airway
Anatomic Newborn Adult
Features
Size 4 cm 10-13 cm
Shape funnel cylindrical
Position of the C3-C4 C6
Function glottis
1. Acts as a conducting system for air to enter the lower
Narrowest point 1 cm below At vocal cords
airway the vocal cords
2. Acts as a protective mechanism to prevent foreign material (cricoid
from entering the pulmonary tree cartilage)
3. Acts as an “air conditioner” of inspired gases
4. Plays an important role in the processes of speech Vocal cords slanting Transverse or
anteriorly slightly slanting
Nose and Mouth
posteriorly
Normal breathing: Air is warmed and humidified as it
passes through the nares Mucous Loose (swells More firmly bound
The ophthalmic and maxillary divisions of the trigeminal membranes easily)
nerve- innervates nasal mucosa
Palatine nerves- innervates the hard and soft palate A) Laryngeal Cartilages
Lingual nerve- branch of the mandibular division of the Made up of 9 cartilages to form a box-like structure at the
trigeminal nerve upper end of the trachea. There are 3 single and 3 paired
- provides sensation to the anterior 2/3 of the cartilages
tongue Single (ETC) Paired (CAC)
Posterior 3rd of the tongue, soft palate, oropharynx- - Epiglottis -Arytenoids
innervated by the glossopharyngeal nerve - Thyroid - Corniculate
PHARYNX - Cricoid - Cuneiform
Serves as a common musculomembranous passage way for
the digestive & respiratory systems.
Anesth: Airway Management
Page 1
o Action – draws hyoid bone inferiorly &
1. Epiglottis draws thyroid cartilage superiorly (elevators
Landmark in performing tracheal intubation of the larynx)
Fibrous cartilage shaped like a leaf attached to the top of c. Inferior constrictors
the larynx in a hinge like fashion o A pharyngeal muscle
Small depression - called the valleculae, which is the site o Action – solely as constrictor of pharynx
of placement of curved MAC laryngoscope blade Extrinsic Muscles of the Larynx
During swallowing as laryngeal muscles contract,
downward movement of the epiglottis and closure &
upward movement of the glottis prevents food from
entering the larynx
When acutely inflamed and swollen, life-threatening
airway obstruction may occur
2. Thyroid Cartilage
Largest cartilage of the larynx
Shield-like structure
Consists of two laminae fused in the midline of neck to
form a subcutaneous projection termed laryngeal
prominence (Adam’s apple)
3. Cricoid Cartilage
Shaped like a signet ring with the bulky portion placed
posteriorly
Forms a complete ring – only tracheal ring is complete
Narrowest portion of the upper airway in the infant and 2. Intrinsic muscles
small child Responsible for moving the cartilages of larynx
Smaller but thicker and stronger than thyroid one against the other
Separated from the thyroid cartilage by the cricothyroid 3 fold function:
membrane Open cords in inspiration
4. Arytenoid Cartilage Close the cords and laryngeal inlet during
Pyramidal structures located on the supero-lateral aspect of swallowing
the cricoid cartilages Alter the tension of cords during speech
Provide anatomic attachment for the inter-arytenoids and
vocalis muscle
5. Corniculate Cartilage
Small conical nodules attached to superior aspect of
arytenoid
Also known as cartilage Santorini
6. Cuneiform Cartilage
Small and spheroidal embedded within aryepiglottic fold
on each side
Also known as cartilage of Wrisberg
TWO GROUPS OF MUSCLES
Extrinsic Muscles
o Moves the larynx as a whole
Intrinsic Muscles
o Moves the various cartilages in relation to one
another
B) Laryngeal Muscles
Blood supply of laryngeal muscles
1. Extrinsic muscles
1. Superior Laryngeal Artery
a. Sternothyroid
o Branch of superior thyroid artery
o An infrahyoid muscle
o Accompanies internal branch of superior laryngeal
o Action – depressors of larynx
nerve
b. Thyrohyoid
o Pierces the thyrohyoid membrane
o An infrahyoid muscle
o Supplies the interior of larynx
Anesth: Airway Management
Page 2
2. Inferior Laryngeal Artery
Superior Minimal effects
o Inferior thyroid branch of the thyro cervical trunk
laryngeal nerve Hoarseness/tiring of voice
o Accompanies recurrent laryngeal nerve into larynx Unilateral
Bilateral
Innervation
1. Superior Laryngeal Nerve Recurrent Hoarseness
Arises from ganglion nodusum laryngeal nerve Stridor, respiratory distress
Unilateral Aphonia
Divides into an external (motor) branch to supply the
Bilateral
cricothyroid membrane; internal (sensory) branch a) Acute
pierces the thyrohyoid membrane b) Chronic
Internal branch divides into: Vagus nerve Hoarseness
o Upper branch Unilateral Aphonia
supplies mucous Bilateral
o Lower branch membrane of base of
tongue, pharynx,
epiglottis & larynx
2. Recurrent Laryngeal Nerve
Trachea
Loops around subclavian artery on right side & aortic p Suspended from the cricoid cartilage by the cricotracheal
arch on left side
Innervates all intrinsic muscles of larynx except
p ligament
Measures 15 cm in adults
cricothyroid l
Supported by 17-18 C shaped cartilages
Supplies sensory branch to mucous membrane of i Cartilages are interconnected by fibroelastic tissue which
larynx below the vocal cords
e allows for expansion of the trachea with expiration or
Laryngeal Innervationv
s inspiration and flexion and extension of the thoracocervical
NERVE SENSORY MOTOR spine
1st tracheal ring is anterior to the 6th cervical vertebrae
Superior Epiglottis, base of None m Ends at the carina T5
laryngeal the tongue Right and Left Main Bronchus
u
(internal division) Supraglottis Right is larger, wider and deviates from the plane of the
musoca c trachea in less acute angle
Thyroepiglottic o
joint u Airway assessment
Cricothyroid joint Why should we asses a patient’s airway preoperatively ?
s
Super laryngeal Anterior subglottic Cricothyroid
The goal of evaluating a patient's airway
(external musoca (adductor, tensor)
m -attempt to identify any possible problems with
division)
e maintaining, protecting, and providing a patent airway
during anesthesia.
Recurrent Subglottic musoca Thyarytenoid m NOTE:
laryngeal Lateral b 1) The Laryngoscope’s function is to visualize the
cricoarytenoid r mouth/Pharynx/Epiglottis
Inter arytenoids 2) With your left hand insert the Blade to the right of the tongue so
(adductors) a
that the tongue moves toward the left
Posterior n 3) Once the tip of the blade is at the base of the tongue pull the
cricoarytenoids e laryngoscope forward and upward in 45 degrees from the horizontal
(abductors) line(don’t rotate as u might damage the upper teeth).
L
Effects of Laryngeal Nerve Injury on the Voice Assessment
o Begins with a comprehensive history and physical
NERVE EFFECT OF NERVE INJURY w examination
e
HISTORY: History related to airway problems (aspiration risk)
r
o hx of voice changes
o Vocal cord polyps
b
Anesth: Airway Management
r
Page 3
a
n
c
o Frequent pneumonias Pierre-Robin syndrome Micrognathia, macroglossia, cleft soft
o Coughing after eating/ drinking palate
o Acute narcotic therapy Treacher-Collins syndrome Auricular and ocular defects, malar and
o Acute trauma mandibular hypoplasia
o ICU admission (current) Goldenhar’s syndrome Auricular and ocular defects, malar and
o Pregnancy mandibular hypolasia
o Immediate postpartum Down’s syndrome Poorly developed or absent bridge of
o Systemic diseases associated with gastroparesis: DM, the nose, macroglossia
postvagotomy thyroid dysfunction, liver disease,CNS Kippel-Feil syndrome Congenital fusion of a variable number
tumors, chronic renal insufficiency, collagen vascular of cervical vertebrae, restriction of neck
disease Parkinson disease movement
Goiter Compression of trachea, deviation of
HISTORY: larynx/trachea
difficult laryngoscopy/SGA ventilation SYNDROMES ASSOCIATED WITH DIFFICULT AIRWAY
History of surgical manipulation in or around the MANAGEMENT
airway
History of radiation therapy of the head/neck Acquired :
Various congenital and acquired syndromes Infections:
Supraglottis Laryngeal edema
obstructive sleep apnea Croup Laryngeal edema
Body mass index > 35 kg/m2 Abscess (intraoral,
Loud snoring retropharyngeal) ` Distortion of the airway and
Pauses in breathing during normal sleep trismus
Sleep interruption Ludwig’s angina Distortion of the airway and
Daytime somnolence/napping trismus
Airway affecting craniofacial abnormalities Arthritis:
Rheumatoid arthritis Temporomandibular joint
lingual tonsil hyperplasia ankylosis,cricoarytenoid arthritis,
Chronic sore throat deviation of larynx, restricted mobility
Voice change of cervical spine
Dysphagia Ankylosing spondylitis Ankylosis of cervical spine, less
Obstructive sleep apnea commonly ankylosis
Hx of tonsillectomy temporomandibular joints, lack of
thyroglossal duct cyst mobility of cervical spine
Asymptomatic anterior cervical mass that moves with Benign tumors:
deglutination Cystic hygroma, lipoma, adenoma, goiter
Complications: cyst infection, fistula, spontaneous Stenosis or distortion of the airway, fixation of larynx or
rupture, voice change, dysphagia, dyspnea and snoring adjacent tissues secondary to infiltration or fibrosis from
signs and symptoms related to airway irradiation
o Snoring Malignant tumor, facial injury, cervical spine injury,
o Changes in voice laryngeal/tracheal trauma
o Dysphagia Edema of the airway, hematoma, unstable fraction(s) of the
o Stridor maxillae, mandible and cervical vertebrae.
o Bleeding
o Cervical spine pain or limited range of motion Obesity Short thick neck, redundant tissue in the
o Upper extremity neuropathy oropharynx,sleep apnea
o TMJ dysfunction Acromegaly Macroglossia, prognathism
sequelae of previous intubation Acute burns edema of airway
o Chipped teeth
o Significant prolonged sore throat Physical Examination:
Patency of nares : polyps, deviated nasal septum
SYNDROMES ASSOCIATED WITH DIFFICULT AIRWAY Teeth (edentulous)
MANAGEMENT Palate (high arched palate or a long narrow
Congenital : mouth)
Prognathism
Anesth: Airway Management
Page 4
Observation of patient’s neck (short, thick)
(masses, extension, neck mobility, ability to Quick airway assessment
assume a sniffing position) Can the patient open the mouth widely?
Presence of hoarse voice/stridor or previous Can the patient maximally protrude the tongue?
tracheostomy Patients ability to move jaw forward?
Infections of the airway Can the patient fully bend/ extend the head and move it
Physiologic conditions ( pregnancy and obesity) sidewards?
TMJ movement Indicative of TMJ movement
Ask the patient to sit up with his head in the neutral Inspects posterior aspect of mouth/pharyngeal structures
position and open his mouth as wide as possible. Indicates ease to maneuver the laryngoscope
The condyle should rotate forward freely such that the Indicates neck movement
space created between the tragus of the ear and the
mandibular condyle is approximately one fingerbreadth in Management of the airway:
width. Preoxygenation
Mouth opening and tongue protrusion “denitrogenation”
The aperture of the patient's mouth should admit at least 2 Replacement of the nitrogen volume of the lung with
fingers between his teeth oxygen in order to provide reservoir for diffusion into the
Thyromental distance/ Sternomental distance alveolar capillary blood after the onset of apnea
It is measured from the lower border of the chin. Preoxygenation for 5 minutes- furnish up to 10 minutes of
This measurement is done with the adult patient's neck oxygen reserve following apnea
fully extended Four vital capacity breaths of 100% oxygen over a 30 sec
Adults who have less than 3 fingerbreadths between their period
mentum and thyroid notch may have either an anterior Eight deep breaths in a 60 second period
larynx or a small mandible, which will make intubation Aids in prolonging the time of desaturation
difficult. Methods of supporting the airway
Anesthesia face Mask
SPECIFIC TEST FOR ASSESSTMENT: Supraglottic airways
Mallampati Classification LMA
relates tongue size to pharyngeal size ET tube
performed with the patient in the sitting position, the head Uses of face mask
held in a neutral position, the mouth wide open, and the Pre-oxygenation prior to induction of anaesthesia
tongue protruding to the maximum. Inhalational induction of anaesthesia
classification is assigned based upon the pharyngeal Bag-mask ventilation (BMV) prior to intubation
structures that are visible. Maintenance of anaesthesia
If the patient phonates, this falsely improves the view Non-invasive ventilation for respiratory failure
Class I = visualization of the soft palate, fauces, Techniques in using face mask:
uvula, anterior and posterior pillars. One-handed technique
Class II = visualization of the soft palate, fauces and correct sized mask over the nose and mouth
uvula non-dominant hand to position the facemask,
Class III = visualization of the soft palate and the Holding the body of the mask between thumb and
base of the uvula. index finger
Class IV = only the hard palate is visible; soft palate Use remaining 3 fingers to support the jaw, with
is not visible at all the little finger hooked behind the angle of the
mandible
Direct Laryngoscopy • Lift the mandible upwards, towards and into the mask to create
Cormack and Lehane an air-tight seal
Grades of Laryngoscopic View • Slight head extension may improve airway patency
Grade I = visualization of the entire laryngeal • Ventilate the patient with dominant hand by squeezing the
aperture. bag or using bellows
Grade II = visualization of just the posterior portion of • Continually assess the adequacy of the technique by observing
the laryngeal aperture. bilateral chest movement, listening for air leaks and assessing for
Grade III = visualization of only the epiglottis. signs of inadequate facemask ventilation
Grade IV = visualization of just the soft palate only,
not even the epiglottis is visible
Anesth: Airway Management
Page 5
two -handed technique If unsuccessful, consider using laryngeal mask
uses a similar approach to the one-handed technique airway early
described above, with the additional hand adopting an Presence of facial hair
identical position on the other side of the mask and face Consider using larygneal mask airway or endotracheal tube
early.
Assessment and Predictability of Difficult Mask Ventilation Patients with dentures, edentulous patients or sunken cheeks
Criteria for Difficult Mask Ventilation Consider leaving dentures in place if secure.
Inability for one anesthesiologist to maintain Use oropharyngeal airway and/or nasopharyngeal airway.
oxygen saturation > 92% Consider placing lower pole of face mask over lower lip
Significant gas leak around face mask itself in edentulous patients.
Need for ≥ 4 LPM gas flow ( or use of fresh gas Ask assistant to support soft tissue of cheeks against mask.
flow button more than twice) Obese patients
No chest movement Pre-oxygenation is essential
Two handed mask ventilation is needed Recognize that facemask ventilation and maintaining
Changed of operator required adequate oxygenation can be difficult.
When facemask ventilating, keep patient 5-10° head up
Patient factors associated with difficult facemask ventilation position, with anaesthetist standing on a platform or step if
• Presence of facial hair/ beard necessary to achieve this.
• Lack of teeth (edentulous) Use two-handed technique with oropharyngeal airway.
• Patients with sunken cheeks Endotracheal intubation is often indicated for surgery.
• Obesity (BMI >26)
• History of obstructive sleep apnea LARYNGEAL MASK AIRWAY
• Age >55yrs The LMA was invented by Dr. Archie Brain at the London
• History and signs of upper airway obstruction (snoring) Hospital, Whitechapel in 1981
The LMA consists of two parts:
Problems and suggested solutions for inadequate facemask The mask
ventilation The tube
Poor mask seal The LMA has proven to be very effective in the
Indicated by audible leak, poor chest management of airway crisis
expansion or difficulty generating positive pressure in bag The LMA design:
Solutions: Provides an “oval seal around the laryngeal inlet”
Use two-handed technique and ensure good jaw once the LMA is inserted and the cuff inflated.
thrust. Once inserted, it lies at the crossroads of the
Ask assistant to support soft tissues of cheek digestive and respiratory tracts.
around rim of mask. Contraindications of the LMA
Consider using an oropharyngeal or Risk of gastric content aspiration (full stomach, hiatal
nasopharyngeal airway to improve airway hernia with significant gastroesophageal reflux, intestinal
patency. obstruction, delayed gastric emptying, poor history)
Ensure no leaks in equipment or circuit Preparation of the LMA for Insertion
If unsuccessful, consider using laryngeal mask Step 1: Size selection
airway early Step 2: Examination of the LMA
Partial or complete airway obstruction Step 3: Check deflation and inflation of
Indicated by high airway pressures, poor chest movement, the cuff
cyanosis or low oxygen saturations Step 4: Lubrication of the LMA
Solutions: Step 5: Position the Airway
Optimize patient head position with slight head Size Selection
extension. Verify that the size of the LMA is correct for the patient
Use two-handed technique and ensure good jaw Recommended Size guidelines:
thrust Size 1: under 5 kg (4 ml)
Use an oropharyngeal or nasopharyngeal airway Size 1.5: 5 to 10 kg (7 ml)
Consider possibility of laryngospasm – often Size 2: 10 to 20 kg (10 ml)
giving additional intravenous anaesthetic agent Size 2.5: 20 to 30 kg (14 ml)
(e.g. propofol) can improve this. Size 3: 30 kg to 50 kg (20 ml)
Ensure no occlusion in equipment or circuit – Size 4: 50-70 kg (30 ml)
consider reverting to self-inflating bag and mask. Size 5: 70 to 100 kg (40 ml)
Anesth: Airway Management
Page 6
LMA Insertion Technique Syringe for tracheal tube inflation
LMA Insertion Suction apparatus
Laryngoscope handle
Different laryngoscope blades
Step 1 stethoscope
Grasp the LMA by the tube, holding it like a pen as near as
possible to the mask end.
Place the tip of the LMA against the inner surface of the
patient’s upper teeth
Step 2
Under direct vision:
Press the mask tip upwards against the hard
palate to flatten it out.
Using the index finger, keep pressing upwards as
you advance the mask into the pharynx to ensure
the tip remains flattened and avoids the tongue.
Step 3
Keep the neck flexed and head extended:
Press the mask into the posterior pharyngeal wall
using the index finger.
Step 4 Tracheal Tube size and length
Continue pushing with your index finger. Age Internal Diameter Length
Guide the mask downward into position. Child 4+ age/4 14+age/4
Step 5 Adult
Grasp the tube firmly with the other hand female 7.0-7.5 21-24
then withdraw your index finger from the male 7.5-9.0 23-24
pharynx.
Press gently downward with your other hand to The height of the supine patient’s airway should be at the
ensure the mask is fully inserted. level of the laryngoscopist’s xyphoid cartilage. The
Step 6 clinician performing the intubation must have unobstructed
Inflate the mask with the recommended volume of air. access to the head
Do not over-inflate the LMA. Extension of the head at the atlanto-occipital joint (sniffing
Do not touch the LMA tube while it is being inflated unless position) serve to align the oral, pharyngeal and laryngeal
the position is obviously unstable. axes such that the passage and line of vision from the lips
Normally the mask should be allowed to rise up to the glottic opening are most nearly a straight line.
slightly out of the hypopharynx as it is inflated to Laryngoscope is held in the left hand
find its correct position. The blade is inserted in the right side of the patient’s mouth
Choose the largest size that will fit comfortably in the oral and the tongue is deflected to the left
cavity then inflate to the minimum pressure that allows Pressure on the teeth and gums must be avoided
ventilation to 20 cm water Tube is advanced until the proximal end is 1-2 cm past the
vocal cords (midway between the vocal cords and carina)
ENDOTRACHEAL INTUBATION Low pressure high volume cuff that prevents leaks during
IndicationS for endotracheal intubation positive ventilation pressure (20 to 30 cm H2O), minimizes
Provide a patent airway the likelihood of mucosal ischemia
Prevent aspiration of gastric contents Gold standard: VISUALIZATION OF THE VOCAL
Need for frequent suctioning CORDS AND END TIDAL CO2 DETECTION
Operative position other than supine
Facilitate positive-pressure ventilation of the lungs The ASA calls a Failed/Difficult Laryngoscopy if:
Operative site near or involving the upper airway Any airway that takes more than 3 attempts
Airway maintenance by mask is difficult Any airway that takes more than 10 minutes to secure
Equipment for laryngoscopy Npo status and the Rapid sequence induction
Oxygen source and self inflating ventilation bag Performed to gain control of the airway in the shortest
Face mask amount of time
Oropharyngeal and nasopharyngeal airway
Tracheal tube and stylets
Anesth: Airway Management
Page 7
Administration of intravenous anesthetic induction agent is
immediately followed by a rapidly acting neuromuscular
blocking drugs
Intubation should be performed as soon as muscle
relaxation is confirmed
Cricoid pressure (Sellick’s maneuver) is applied by an
assistant from the beginning of induction until confirmation
of the ETT placement
Awake intubation
Maintenance of spontaneous ventilation in the event that
the airway cannot be secured rapidly
Confers maintenance of upper and lower esophageal
sphincter tone, thus reducing the risk of reflux
Transtracheal Techniques
Cricothyrotomy
DIFFICULT EXTUBATION Transtracheal jet ventilation
LARYNGOSPASM- can be triggered by respiratory Needle cricothyrotomy— involves passing an over-the-
secretions, vomitus, blood, or foreign body in the airway needle catheter through the cricothyroid membrane
Contraction of the lateral Surgical cricothyroidotomy — is an emergent airway
criciarytenoid,thyroarytenoid and cricothyroid approach in which the clinician makes an incision in the
muscles cricothyroid membrane and passes a tracheostomy or
Tx: removal of the offending stimulus, endotracheal tube into the trachea.
administratyion of O2, small dose of short acting Percutaneous transtracheal ventilation — involves
muscle relaxants oxygenation and ventilation via a needle or surgical
DIFFICULT AIRWAY cricothyroidotomy using an improvised ventilation device.
‘Difficult airway’ Transtracheal jet ventilation — refers to high frequency,
one in which there is a problem in establishing or low tidal volume ventilation provided via a laryngeal
maintaining gas exchange via a mask, an artificial catheter by specialized ventilators that are usually only
airway or both. available in the operating room or intensive care unit .This
Recognizing before anaesthesia the potential for a procedure is occasionally employed in the operating room
difficult airway (DA) allows time for optimal when a difficult airway is anticipated
preparation, proper selection of equipment and
technique and participation of personnel
experienced in DA management.
ASA defines…
difficult airway as “the situation in which the
conventionally trained anesthesiologist experiences
difficulty with intubation, mask ventilation or both”.
Anesth: Airway Management
Page 8
You might also like
- Airway ManagementDocument4 pagesAirway Managementpaveethrah100% (1)
- Airway Management TechniquesDocument1 pageAirway Management TechniquesDebashish PaulNo ratings yet
- Difficult AirwayDocument77 pagesDifficult AirwayParvathy R Nair100% (1)
- Endotracheal IntubationDocument43 pagesEndotracheal IntubationBishow100% (1)
- Airway ManagementDocument36 pagesAirway ManagementShobhaNo ratings yet
- Airway ManagementDocument49 pagesAirway ManagementusuisatimNo ratings yet
- Arterial Lines GuideDocument38 pagesArterial Lines GuideRabeed MohammedNo ratings yet
- One Lung Ventilation: Llalando L. Austin Ii, MHSC, Aa-C, RRT Nova Southeastern UniversityDocument47 pagesOne Lung Ventilation: Llalando L. Austin Ii, MHSC, Aa-C, RRT Nova Southeastern UniversityZulkarnainBustamam100% (1)
- Anesthesia Management in Bronchoscopy Procedure NewDocument29 pagesAnesthesia Management in Bronchoscopy Procedure NewChlara Obisuru100% (1)
- Difficult Airway Management TechniquesDocument54 pagesDifficult Airway Management TechniquesAnonymous V5xDcrNo ratings yet
- Arterial Line and Central LineDocument32 pagesArterial Line and Central LineOrachorn AimarreeratNo ratings yet
- Overview of Mechanical Ventilation Settings, Modes, TroubleshootingDocument24 pagesOverview of Mechanical Ventilation Settings, Modes, TroubleshootingRochim CoolNo ratings yet
- ArdsDocument81 pagesArdsAmit KlNo ratings yet
- Arterial LinesDocument13 pagesArterial LinesYee LengNo ratings yet
- Mechanical VentilationDocument19 pagesMechanical VentilationDoha EbedNo ratings yet
- 21 Obstetric Anaesthesia PDFDocument0 pages21 Obstetric Anaesthesia PDFjuniorebindaNo ratings yet
- Mechanical Ventilation and Intracranial PressureDocument30 pagesMechanical Ventilation and Intracranial PressureFlavius AnghelNo ratings yet
- Acute Exacerbation of COPD Nursing Application of Evidence-Based GuidelinesDocument17 pagesAcute Exacerbation of COPD Nursing Application of Evidence-Based GuidelinesCandice ChengNo ratings yet
- Basics Mechanical VentilationDocument51 pagesBasics Mechanical VentilationademNo ratings yet
- Tension Pneumothorax Diagnosis and ManagementDocument21 pagesTension Pneumothorax Diagnosis and ManagementnovelraaaNo ratings yet
- Rapid Seq InductionDocument6 pagesRapid Seq InductionandikszuhriNo ratings yet
- Airway AdjunctsDocument17 pagesAirway AdjunctsChannelGNo ratings yet
- Acute Respiratory Distress SyndromeDocument77 pagesAcute Respiratory Distress SyndromeAnnisa Dyah ChairiniNo ratings yet
- Incentive Spirometry (Respirometer)Document4 pagesIncentive Spirometry (Respirometer)Anandhu G100% (1)
- Airway ManagementDocument42 pagesAirway ManagementOwy100% (4)
- Flow LoopDocument6 pagesFlow LoopfarexNo ratings yet
- Liver AnesthesiaDocument141 pagesLiver Anesthesiadrimrangafoor75% (4)
- Conduct of AnaesthesiaDocument30 pagesConduct of AnaesthesiaAnirban PalNo ratings yet
- The Management of Acute Respiratory Distress SyndromeDocument48 pagesThe Management of Acute Respiratory Distress SyndromeLauraAlvarezMulettNo ratings yet
- ICU TriageDocument27 pagesICU TriageAkmal FahrezzyNo ratings yet
- Technique For Awake Fibre Optic IntubationDocument3 pagesTechnique For Awake Fibre Optic Intubationmonir61No ratings yet
- Endotracheal TubeDocument14 pagesEndotracheal TubeValerie BlasNo ratings yet
- Arteri LineDocument13 pagesArteri Linemuthia octavianaNo ratings yet
- Rapid Sequence Intubation and Cricoid PressureDocument16 pagesRapid Sequence Intubation and Cricoid PressureErlin IrawatiNo ratings yet
- Airway Assessment MeDocument46 pagesAirway Assessment MePeter AbikoyeNo ratings yet
- Epidural AnesthesiaDocument5 pagesEpidural AnesthesiaImran MukhlessNo ratings yet
- Ventilation Servo-I With Nava Neurally Controlled VentilationDocument14 pagesVentilation Servo-I With Nava Neurally Controlled Ventilationraju_pnNo ratings yet
- Airway ManagementDocument129 pagesAirway ManagementSyabie YassinNo ratings yet
- Basics of ICU CareDocument19 pagesBasics of ICU CareUmar Farooq GondalNo ratings yet
- Cor Pulmonale Lesson PlanDocument49 pagesCor Pulmonale Lesson PlanRadha Sri50% (2)
- Pathophysiology ARDSDocument2 pagesPathophysiology ARDSKim AmboyaNo ratings yet
- Anesthesia PresentationDocument19 pagesAnesthesia PresentationJohnyNo ratings yet
- Management of Emergencies in ChildrenDocument39 pagesManagement of Emergencies in ChildrensastroboyzNo ratings yet
- Adult Invasive Mechanical VentilationDocument73 pagesAdult Invasive Mechanical Ventilationmed2004100% (1)
- Over View of IAP ALSDocument12 pagesOver View of IAP ALSMohamed RasoolNo ratings yet
- Airway Management (RS)Document68 pagesAirway Management (RS)yoan purnomoNo ratings yet
- Anaesthesia For Trauma PatientsDocument42 pagesAnaesthesia For Trauma PatientsMerindukan Surga MuNo ratings yet
- Chest DrainageDocument28 pagesChest DrainageCristy Guzman100% (1)
- Ventricular Septal DefectsDocument7 pagesVentricular Septal DefectsMuhammadAldoGiansyahNo ratings yet
- Respiratory FailureDocument16 pagesRespiratory FailurealzaabiBMNo ratings yet
- Essential Concepts for Airway ManagementDocument42 pagesEssential Concepts for Airway Managementkader abdiNo ratings yet
- Acute Respiratory Distress Syndrome (Ards)Document12 pagesAcute Respiratory Distress Syndrome (Ards)Vin Grace Tiqui - GuzmanNo ratings yet
- Transportation of Critically Ill PatientDocument18 pagesTransportation of Critically Ill Patientfirdaus che daud100% (2)
- Difficult Airway ManagementDocument79 pagesDifficult Airway Managementedwardjohnson2310No ratings yet
- ACLS HandoutsDocument4 pagesACLS HandoutsMeynard AndresNo ratings yet
- Hemodynamic Monitoring Techniques and Their Clinical ApplicationsDocument44 pagesHemodynamic Monitoring Techniques and Their Clinical Applicationsinvisigoth17No ratings yet
- Medical Surgical (MS) Lecture Respiratory System: Alteration in OxygenationDocument44 pagesMedical Surgical (MS) Lecture Respiratory System: Alteration in OxygenationYman Gio BumanglagNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemJed Kachel BugayongNo ratings yet
- Lec 1 Respiratory SystemDocument3 pagesLec 1 Respiratory SystemfaiNo ratings yet
- Anatomy of Voice: How to Enhance and Project Your Best VoiceFrom EverandAnatomy of Voice: How to Enhance and Project Your Best VoiceRating: 4 out of 5 stars4/5 (3)
- Dyspepsia and HypertensionDocument32 pagesDyspepsia and HypertensionMichael SedanoNo ratings yet
- Sexually Transmitted Infections Treatment Guidelines, 2021Document192 pagesSexually Transmitted Infections Treatment Guidelines, 2021Jorge Augusto Israel 狼No ratings yet
- Basic Skills in NursingDocument82 pagesBasic Skills in NursingMichael SedanoNo ratings yet
- Gerd CPG PDFDocument17 pagesGerd CPG PDFJamie SebastianNo ratings yet
- CPG AID - Full VersionDocument120 pagesCPG AID - Full VersionJoniee SnowNo ratings yet
- High Yield Immunology PDFDocument75 pagesHigh Yield Immunology PDFPaulette Pinargote100% (2)
- Gastro and COVIDDocument21 pagesGastro and COVIDMichael SedanoNo ratings yet
- Sexually Transmitted Infections Treatment Guidelines, 2021Document192 pagesSexually Transmitted Infections Treatment Guidelines, 2021Jorge Augusto Israel 狼No ratings yet
- Infectious DiarrheaDocument2 pagesInfectious DiarrheaMichael SedanoNo ratings yet
- 1 The Systemic Response To InjuryDocument17 pages1 The Systemic Response To InjuryMichael SedanoNo ratings yet
- JNC 8 Guideline Algorithm for Treating HypertensionDocument2 pagesJNC 8 Guideline Algorithm for Treating HypertensionTaradifaNurInsi0% (1)
- Community-Acquired Pneumonia - CPG 2016Document26 pagesCommunity-Acquired Pneumonia - CPG 2016Jamie SebastianNo ratings yet
- Anatomy MCQ 2Document63 pagesAnatomy MCQ 2Pirabakar MahendranNo ratings yet
- Ethics 3Document4 pagesEthics 3Michael SedanoNo ratings yet
- Last GlaucomaDocument6 pagesLast GlaucomaMichael SedanoNo ratings yet
- Medical Surgical NXDocument16 pagesMedical Surgical NXMichael SedanoNo ratings yet
- Risk factors for gallstone formationDocument1 pageRisk factors for gallstone formationMichael SedanoNo ratings yet
- VerbalDocument6 pagesVerbalMichael SedanoNo ratings yet
- CHN RatioDocument2 pagesCHN RatioMichael SedanoNo ratings yet
- CHN RatioDocument2 pagesCHN RatioMichael SedanoNo ratings yet
- Biochem NotesDocument5 pagesBiochem NotesMichael SedanoNo ratings yet
- Blank 4Document5 pagesBlank 4Michael SedanoNo ratings yet
- Gastro Intestinal PDFDocument41 pagesGastro Intestinal PDFMichael SedanoNo ratings yet
- What Are Families Why Are They Important?Document47 pagesWhat Are Families Why Are They Important?Michael SedanoNo ratings yet
- True pelvis anatomy and clinical significanceDocument27 pagesTrue pelvis anatomy and clinical significanceMichael SedanoNo ratings yet
- In Vitro FertilizationDocument26 pagesIn Vitro FertilizationCecilia Delos ReyesNo ratings yet
- BiologyreviewDocument5 pagesBiologyreviewMichael SedanoNo ratings yet
- Bombardier CityfloDocument14 pagesBombardier CityfloBiju KmNo ratings yet
- People vs. LorenzoDocument8 pagesPeople vs. LorenzoMRose SerranoNo ratings yet
- Sexual Self PDFDocument23 pagesSexual Self PDFEden Faith Aggalao100% (1)
- GII-07 Training MaterialDocument191 pagesGII-07 Training MaterialIris Amati MartinsNo ratings yet
- Epithelial and connective tissue types in the human bodyDocument4 pagesEpithelial and connective tissue types in the human bodyrenee belle isturisNo ratings yet
- Curriculum VitaeDocument8 pagesCurriculum VitaeChristine LuarcaNo ratings yet
- PallavaDocument24 pagesPallavaAzeez FathulNo ratings yet
- VDA ChinaDocument72 pagesVDA Chinatuananh1010No ratings yet
- 2018 World Traumatic Dental Injury Prevalence and IncidenceDocument16 pages2018 World Traumatic Dental Injury Prevalence and IncidencebaridinoNo ratings yet
- Semi-Detailed Lesson Plan Template: Pagsanjan Intergrated National High School 8Document3 pagesSemi-Detailed Lesson Plan Template: Pagsanjan Intergrated National High School 8Mae Ganate RoblesNo ratings yet
- Historyofluthera01morg PDFDocument420 pagesHistoryofluthera01morg PDFJhonNo ratings yet
- BSC Part IiDocument76 pagesBSC Part IiAbhi SinghNo ratings yet
- Test Unit 3Document2 pagesTest Unit 3RAMONA SECUNo ratings yet
- Ad844 PDFDocument20 pagesAd844 PDFkavi_mishra92No ratings yet
- Sri Dakshinamurthy Stotram - Hindupedia, The Hindu EncyclopediaDocument7 pagesSri Dakshinamurthy Stotram - Hindupedia, The Hindu Encyclopediamachnik1486624No ratings yet
- Chap 4 eDocument22 pagesChap 4 eHira AmeenNo ratings yet
- Urban Process Design - Hamid ShirvaniDocument1 pageUrban Process Design - Hamid ShirvaniCaramel LatteNo ratings yet
- Week 1 Amanda CeresaDocument2 pagesWeek 1 Amanda CeresaAmanda CeresaNo ratings yet
- Chapter 5 Quiz Corrections ADocument4 pagesChapter 5 Quiz Corrections Aapi-244140508No ratings yet
- Silvianita - LK 0.1 Modul 2 English For Personal CommunicationDocument3 pagesSilvianita - LK 0.1 Modul 2 English For Personal CommunicationSilvianita RetnaningtyasNo ratings yet
- ESL Lesson PlanDocument4 pagesESL Lesson PlanuarkgradstudentNo ratings yet
- Soal Paket 1Document10 pagesSoal Paket 1Nurul HayatiNo ratings yet
- Word Formation - ExercisesDocument4 pagesWord Formation - ExercisesAna CiocanNo ratings yet
- Unit Test, Part 2: Literature With A Purpose: Total Score: - of 40 PointsDocument3 pagesUnit Test, Part 2: Literature With A Purpose: Total Score: - of 40 PointsAriana Stephanya Anguiano VelazquezNo ratings yet
- Sustainability of A Beach Resort A Case Study-1Document6 pagesSustainability of A Beach Resort A Case Study-1abhinavsathishkumarNo ratings yet
- The Army Crew Team Case AnalysisDocument3 pagesThe Army Crew Team Case Analysisarshdeep199075% (4)
- Philosophical Perspectives Through the AgesDocument13 pagesPhilosophical Perspectives Through the Agesshashankmay18No ratings yet
- Adjustment DisordersDocument2 pagesAdjustment DisordersIsabel CastilloNo ratings yet
- ViscosityDocument7 pagesViscositykiran2381No ratings yet
- 59-33 ATO Implementation Journal KSA 100Document18 pages59-33 ATO Implementation Journal KSA 100nicolas valentinNo ratings yet