Professional Documents
Culture Documents
Endocrine System and Reproductive System
Uploaded by
Kim Ramos0 ratings0% found this document useful (0 votes)
22 views8 pagesG
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentG
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
22 views8 pagesEndocrine System and Reproductive System
Uploaded by
Kim RamosG
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 8
Endocrine System and Reproductive § Anterior Lobe (Adenohypophysis)
System v Responds to hormones from the
hypothalamus through the H-h
portal system (Hypothalamus –
Quick Trans by: Alyssa Balt hypophyseal portal system)
Lecture by: Doc DJ v Hormones – ACTH, FSH, LH,
Date: January 29, 2018 Prolactin, GH and TSH
TEXT ONLY | NO FIGURES | PPT AND SIDE NOTES
§ Posterior Lobe (Neurohypophysis)
Endocrine System v DOES NOT produce hormones;;
§ The Endocrine System is a collection of v Stores hormone from the
glands that produce hormones directly hypothalamus – ADH and Oxytocin
into the circulatory system to be carried v Transmitted through nerve impulse.
to distant target organs.
§ Function: regulate metabolism, growth Hypothalamic Connections
and development, tissue function,
sexual function, reproduction, sleep and Hypothalamo – hypophysial Portal System
mood. § Blood vessels connecting the anterior
lobe of pituitary gland to the
Pineal Gland hypothalamus. This transmits the
§ “Epiphysis Cerebri” releasing factors to the anterior lobe.
§ The pineal gland is pinecone-shaped
organ located posterior to the 3rd Hypothalamo – hypophysial Nerve Tract
ventricle and is overhanging the § Connection of the posterior lobe of
midbrain. pituitary to the supraoptic and
§ It produces, Melatonin, a serotonin- paraventricular nuclei of the
derived hormone which plays a role in hypothalamus.
regulating sleep patterns (circadian § Hormones Vasopressin and Oxytocin
rhythm). are released at the axon terminals in the
posterior lobe of pituitary.
§ Melatonin secretion is decreased ¯
during daytime, among elderly and
Note: The body of sphenoid has depression,
insomniacs
Sella Turcica. Sella Turcica is covered by
reflection of meningeal matter, Diaphragm
Note: Pineal gland has sexual function (activity
Sellae.
of the gonads).
Blood Supply and Venous Drainage of the
Pituitary Gland
Pituitary Gland
§ A tiny organ at the base of the brain,
§ Superior and Inferior Hypophyseal
weighs about 0.5 gms.
Arteries from the Internal Carotid Artery
§ Attached to the hypothalamus by
§ Veins drain into the Intercavernous
infundibulum (nerve tract).
Sinus
o Infundibulum / Infundibular Stalk
/ Pituitary stalk
Thyroid Gland
§ It is called the “master gland” because
§ Encapsulated bilobed gland
it produces many hormones that direct
§ Enclosed by the pretracheal fascia
certain processes/stimulating other
outside the capsule
organs to produce other hormones.
Note: Pretracheal Fascia is the layer that moves
§ It is controlled in large part by the
when swallowing. It is attached to the cricoid
hypothalamus.
cartilage.
§ An isthmus connects the 2 lobes (L and
Note: Pituitary Gland is the “Master Gland”
R) across the midline, in front of the 2nd
because it controls the activity of stimulating
– 4th tracheal rings
hormones.
§ Weighs about 25 gms.
Lobes of Pituitary Gland
Note: Thyroid Gland is smooth and usually, not Note: Maximum of 6 pairs (excess is formed in
palpable. It is heavier in females. Not visible in the thorax)
neck. § blood supply comes from superior and
inferior thyroid arteries
Blood Supply of the Thyroid Gland
The blood supply of the Thyroid Gland comes
from: Function of Parathyroid Glands
§ External Carotid – Superior § Secrete Parathormone (Parathyroid
Thyroid Artery Hormone)
§ Thyrocervical Artery – Inferior § an osteoclastic hormone, mobilize
Thyroid Artery calcium from bones, increase
Note: Left Inferior Thyroid Artery and Right absorption of calcium from intestine,
Inferior Thyroid Artery join before terminating to increase reabsorption of calcium in
Left Innominate Veins. proximal convoluted tubules.
§ Arch of Aorta/Left Common
Carotid/Brachiocephalic – Thymus Gland
Thyroidea Ima § A bilobed organ located in the superior
mediastinum directly behind the
Note: Thyroidea Ima is the smallest thyroid manubrium
artery and has inconsistent blood supply. § It is the primary or central lymphoid
organ
Function of the Thyroid Gland § Its function is production of T (thymic)
§ Secretion of Thyroxin (T4) and lymphocytes that are seeded to the rest
Triidothyronine (T3), which increase of the lymphatic system.
the metabolic activity of most cells in the
body Note: Thymus gland has bone and lymphoid
v Increase Oxygen consumption and origin.
Heat production
Thymic Hormone
§ Produces the hormone, § Thymosin influences the maturation
Thyrocalcitonin, that lowers the blood and function of lymphocytes within the
calcium level thymus and elsewhere in the body
v not under the control of the pituitary
but stimulated by hypercalcemia Blood Supply of Thymus Gland
and suppressed by hypocalcemia § Inferior Thyroid Artery
Note: If the blood calcium levels are normal, § Internal Thoracic Artery
calcitonin will stop.
Suprarenal Glands
Note: Hypothyroidism symptoms include: feeling § Paired glands
cold in hot weather, sleepy, gains weight despite § Yellowish retroperitoneal organs that lie
the less food intake. The opposite of which is on the upper pole of the kidneys
Hyperthyroidism. § Surrounded by Renal Fascia (Gerota’s
Fascia) but are separated from the
Note: Immunocompromised patients have kidney by perirenal fats.
enlarged thyroid gland. o Note: In between SR glands,
perirenal fats.
Parathyroid Gland
§ weighs about 25mg Note:
§ located on the posterior surface of the Right SR – pyramidal in shape and is limited to
thyroid gland the upper pole of the kidney;; drains IVC
§ usually 2 pairs, upper pair being more Left SR – crescentic;; extends to the medial
constant in position at the middle part of border of the kidney;; drains in L Renal Vein.
posterior surface of thyroid gland. Note: Review: What are the tributaries of Left
The inferior pair is found at the lower Renal Vein? Left SR, Left Gonadal, Left
border of thyroid gland. Inferior Phrenic Veins.
Superior SR – derived from Inferior Phrenic prostate. Prostate is palpable during rectal
Artery exam.
Middle SR – direct branch of Abdominal Aorta
Inferior SR – derived from Renal Artery Note: Prostate is an outpouching of the urethra
about 10ft;; doughy, no greasy sensation and no
Blood Supply and Venous Drainage nodules. At 60 yrs. Old, there’s hypertrophy of
§ Right and Left Inferior Phrenic Arteries Median lobe making urination difficult.
§ Middle Suprarenal Artery - The most glandular portion of
§ Left Inferior Adrenal prostate is Median Lobe. (à usually
the affected lobe in Benign
Parts of Suprarenal Glands Hyperthyroid)
§ Suprarenal cortex
v function controlled by anterior lobe Note: Visual Malignancy is seen on Posterior
of pituitary through a hormone, Lobe;; It will not have early symptoms of
Adrenocorticotropic Hormone obstruction because it’s too far. Usually, once
(ACTH) detected, there’s already metastatis.
v Note: Glucocorticoids, Adrenal
Androgens (à masculinity in Note: Prostatic Urethra – urethra traversing
females) prostate;; It is the widest and most dilatable
§ Suprarenal Medulla portion of the entire urethra.
§ Secretes catecholamines,
epinephrine and norepinephrine Note: Blood Supply of Prostate: Inferior Vesical
Pancreas Artery – branch of Internal Iliac Artery at
Parts: Anterior Division;; supplies the prostate (also,
• Head base of bladder, prostate and seminal vesicles in the
• Neck male;; it also gives off the artery to the vas deferens)
• Body
Note:
• Tail
Lobes
Lateral – lies on either sides of urethra;; with
Blood Supply of Pancreas
§ Superior pancreaticoduodenal Artery glands
§ Inferior pancreaticoduodenal Artery Median – between urethra and ejaculatory ducts;;
§ Splenic Artery with glands
§ Superior Mesenteric Artery Posterior – behind the urethra;; with gland
Anterior – lies in front of the urethra;; NO gland
(aglandular)
Lymph nodes of Pancreas
§ Celiac Nodes
Seminal Vesicles
Reproductive System • Lies at the posterior wall of Posterior surface
of urinary bladder
Male Reproductive Organs • NOT A RESERVOIR glandular organ;;
Internal Genitalia • Made up of long tube, coiled upon itself;;
§ Prostate Gland coiling is permanent, can’t be stretched.
§ Seminal Vesicle • Secretion:
§ Ejaculatory Duct v added to the bulk of ejaculate and
seminal fluid
Note: Prostate Gland is wedge-shaped below v rich in sugar (fructose) – for motililty
urinary bladder. It has 5 lobes: 2 Lateral lobes, 1 and life of sperm and nourishment
Medial lobe, 1 Posterior Lobe and 1 Anterior of the spermatozoa
Lobe. Prostatic Secretion: The prostate
produces a thin, milky fluid containing citric acid Seminal Duct
and acid phosphatase that is added to the • joined by Vas Deferens
seminal fluid at the time of ejaculation. The v Vas Deferens is the distal
secretion is drained into urethra (note: seminal continuation of epididymis.
veins, testis and spermatozoa also drain into
urethra) during ejaculation by contraction of the Ductus Deferens
• Joins with duct of Seminal Vesicle § Skin of scrotum is corrugated and
provided with few scattered crisp hairs.
Seminal Duct + Ductus Deferens à Ejaculatory § Skin is provided with sebaceous gland
Duct (secretion: less sugar) and modified sweat (apocrine) gland.
§ Dartos layer contains smooth muscle –
Ejaculatory Duct the dartos muscle.
• pierces the base of prostate, terminates
in the prostatic urethra and is drained Note: Testes are housed in scrotum.
into prostatic sinuses
Note: Layers of Scrotum
Prostatic Sinus 1. Skin
• where secretion of Prostatic Gland is 2. Superficial Fascia
drained 3. Spermatic Fascia
a. External Spermatic Fascia
Vas Deferens - Derived from the aponeurosis of the
• only excretory duct of Testis external oblique muscle
v Urerter is the excretory duct of b. Cremasteric Fascia
kidney. - Derived from internal oblique muscle
• the one cut during Vasectomy c. Internal Spermatic Fascia
- Derived from Fascia Transversalis
Blood Supply:
Inferior Vesical Artery – branch of Internal Iliac
Arery (à supplies the internal genitalia among Penis (Dorsal)
males) • Anatomical position: directed upward
Urogenital Diaphragm Penis is the male organ of copulation.
• below the prostate It consists of 3 erectile bodies:
• contains muscles of deep transverse § 2 Corpus Cavernosa
perineal embedded at pea size gland, § 1 Corpus Spongiosum
Bulbourethral Gland
Note: Each erectile body is surrounded by a
Bulbourethral Gland tough fibrous tissue, Tunica Albuginea.
• aka: Cowper’s Gland • Tunica Albuginea can expand only to a
• secretion: serves as a lubricant fluid and limit;; It’s made up of cavernous sinus
precedes ejaculation;; drains into Penile (finer spaces that become engorged
Urethra with blood during erection but to a
certain extent only limited by tunica
Penile Urethra albuginea).
• traverses the penis (Corpus • Filling of cavernous sinus will cause
Spongiosum, specifically) erection.
• opens at the tip of the penis
It consists of 3 parts of the penis:
• receives the secretion of Bulbourethral
§ Glands
Gland
§ Body/Shaft
§ Root of Penis
Membranous Urethra
• shortest and least dilatable Erectile Structures of the Penis
1. Corpora Cavernosa
External Genitalia a. Proximal parts consist of 2
§ Penis tapering ends that are attached
§ Scrotum to the ischiopubic rami, the
§ Testis and Epididymis crura.;; divergent
§ Vas (Ductus) Deferens Note: Crura is attached to isthiopubic ramus
which covers the muscle.
Scrotum is a cutaneous pouch consisting of
skin and dartos fascia.
b. Distal ends are embedded in the aspect of Testis;; where Spermatozoa is formed).
glans penis, part of the corpus The tubules open into a network of channels in
spongosum. the mediastinum called the Rete Testis. Rete
2. Corpus Spongiosum Testis is conveyed to unite and form body of
a. Proximal expansion is the bulb Epididymis. à Efferent Ductules connect the
of penis, the distal expansion is rete testis to the upper end of the epididymis à
the glans penis Epididymis (at posterolateral aspect of testis;;
b. It is traversed by the penile inside Epididymis, there’s duct – ductus
urethra from the bulb to the tip epipididymis, which has head, body and tail
of the glans.
(which is connected to Vas Deferens) à Vas
Note: Towards the end of Urethra before Deferens/Ductus Deferens à ascends to
termination at its distal end, you will see a slight inguinal canal à enters pelvic cavity à
expansion: Fossa Navicular – external urethral Seminal Duct à Ejaculatory Duct à Penile
orifice of penile urethra;; most constricted Urethra
Note: Urethra has both Urinary and Note: Tyson’s Glands are modified sebaceous
Reproductive functions. glands. Their secretion is one of the components
of Smegma.
Note: The root of the penis consists (a) Bulb of
Penis and (b) L and R crura of the penis. Superficial Fascia of the Perineum
§ The Dartos Layer of Scrotum – the
Parts of Penis inferior continuation of the Camper’s
§ Body: consist of 3 erectile bodies such Fascia of Anterior Abdominal Wall.
as the 2 dorsal corpora cavernosa and 1
ventral corpus spongiosus. § In the Perineum, the superficial fascia
§ Root: consist of the proximal ends of loses its fats and acquires the dartos
the corpora cavernosa, the crura and smooth muscle.
proximal ends of corpus spongiosum,
the bulb § The Dartos Muscle contraction is
§ Glans: the distal expansion of the responsible for the corrugation of the
corpus spongiosum that contains the scrotal skin.
navicular fossa and external urethral
orifice. Colles’ Fascia is a superficial fascia in the
perineum deep to the darto’s fascia. It is derived
Penis, cross section from the Scarpa’s Fascia on the Anterior
§ Blood vessels and nerves Abdominal Wall.
v Superficial dorsal vein: 2 dorsal
bodies embedded in the superficial Note: In Perineal Cavity, arteries and nerves that
fascia supply the pelvis are the Internal Pudendal
Note: In uncircumcised, Superficial Dorsal Vein Artery and Internal Pudendal Nerves.
is attached to ventral surface of glans. SDV is
the one cut during circumcision. Erection
v Deep dorsal vein and dorsal artery • Pelvic nerves
and nerve are in the deep fascia. • Parasympathetic
§ Deep Fascia of Penis (Buck’s Fascia)
v Limits the penis Ejaculation
§ Tunica Albuginea – a tough fibrous • Sympathetic
covering of each corpus spongiosum
and cavernosa;; Note: Convoluted Seminiferous Tubule Is at the
Posterior aspect of testis
Note: Tunica Albuginea extends into the Female Reproductive Organs
substance of testis and sends out processes to Internal Genitalia
“Septula Testis”, and then into a space called § Ovary
“Testicular Lobule”. Within each lobule are § Uterine (Fallopian) Tube
convoluted Seminiferous Tubules (at Posterior § Uterus
§ Upper Part of the Vagina ovum to bo be fertilized. Ovum is expelled from
ovary à Menstruation (“thick cry of frustrated
External Genitalia uterus”).
§ Mons Pubis
§ Labia majora and Labia minora Note: Cilia – pushes towards the uterus.
§ Clitoris
§ Bulb of Vestibule Uterus, in Layman’s Term – “Womb”, is about
§ Vestibule of the Vagina 7.5 to 8 cm long and is entirely a pelvic organ;;
§ Lower part of the Vagina From lower part of Pelvis to fundus of Uterus.
§ Greater Vestibular Gland (Bartholin’s
Gland) Note: Uterus is bent forward (downward).
Ovary is the female homologue of the testis in § 3 main parts:
male. v Fundus – above the attachment of
§ Releases egg every month fallopian tubes
§ produces the hormones: estrogen and v Body – between the fallopian tubes;;
progesterone. between the body and cervix,
Note: Interstitial Cell Stimulating there’s Isthmus of Uterus
Hormone (or Luteinizing Hormone in (*landmark).
females) v Cervix – inside the cervix:
§ releases the matured ovum. Opening between cervical canal and
§ located in the lateral pelvic wall. uterine cavity: Internal Os
Opening between cervix and vagina:
Note: Oviduct transports immature ovum External Os
released from the ovaries.
Cervix projects into vagina, so there will be
recesses around the cervix.
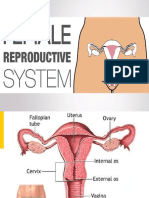
Uterine (Fallopian) Tubes
§ Uterine tube, paired tubes that convey Note: Cervix of a virgin – has an opening like
matured ovum to the uterus. that of a little finger;; soft and smooth and like
§ Spermatozoa travels upward to meet that of the tip of the nose.
the ovum.
§ Mucosal lining is provided with cilia that § Wall has 3 layers:
propel the ovum/fertilized ovum towards v Epimetrium – outermost layer
the uterus. v Myometrium – THICKEST layer
§ Has 2 openings, the abdominal os and v Endometrium – innermost layer
the uterine os.
Uterine Cavity is triangular and has upper 2
Parts of Uterine (Fallopian) Tubes angles, the uterine os of the fallopian tubes and
§ Outside the Uterus an inferior angle, the internal os, which is the
v Infundibulum communication between uterine cavity and the
- characterized by finger-like projections called cervical canal.
“Fimbriae”
v Ampulla Communications of the Uterus
-Rendezvous for fertilization § Uterine Tubes (Fallopian Tubes)
v Isthmus § Cervical Canal
§ Within the wall of uterus Cervix is the lower part of the uterus below the
v Intramural portion isthmus.
§ Cervical Canal – fusiform in shape;;
Note: Egg is taken to Oviduct by Fimbriae. passageway in the cervix.
Oviduct transports the egg into the Uterine § Internal Os – superior opening of the
Cavity. canal through which it communicates
with the uterus.
Note: After the release of ovum, there’s
thickening of internal layer for preparation for
§ External Os – inferior opening of the Note: Clitoris is formed like Penis, except that it
canal through which it communicates has no opening of urethra. Urethra opens at
with the vagina. vestibule of vagina.
Normal Position of the Uterus Greater Vestibular Glands are the homologues
§ Anteflexion, uterus being bent on its of bulbo-urethral glands in male. It’s pea-sized
cervix. lobulated structures at the posterior poles of the
§ Anteversion, uterus bent on the vagina. bulb of vestibule. Their ducts open into the
vestibular fossa posterior to the vagina orifice.
Vagina is the organ of copulation. It’s 7.5 to 8 It secretes mucus that lubricates the vulva.
cm long. It has NO mucosal glands. It is
moistened by secretion from the Cervical Gland HOMOLOGUES:
of the cervix. Superiorly forms recess around
the vaginal part of the cervix – the fornices. Bulb of Vestibule Bulb of Penis
Ovary Testis
Recesses of the Vagina Uterus Prostatic Utricle
§ Fornices of the vagina Bulbourethral gland Greater Vestibular
v Anterior, anterior to the cervix (“Cowper’s Gland”) Gland (“Bartholin’s
v Lateral, on each side of the cervix Gland)
v Posterior, posterior to the cervix. Labia Minora Prepuce
§ The deepest among the Labia Majora Scrotum
fornices Pudendal Cleft Median Raphe
§ The opening of the cervix is directed to Vagina Penis
the posterior wall of the posterior fornix.
Mons Pubis is a conspicuous, subcutaneous fat
pad over the pubic bones and symphysis. It is
CASE DISCUSSION:
covered with pubic hair, largely absent in male.
A 48-year old female presented to her physician
Labia Majora is a broad longitudinal fold of skin
complaining of difficulty in breathing and
filled with subcutaneous fat and fibrous tissue.
swallowing. She was also concerned at the
Its medial surface is smooth and provided with
increase in size of her neck. On physical
plenty of sebaceous gland. It encloses a space,
examination, an irregular firm mass in an
the pudendal cleft.
anterior aspect of the lower neck was palpated.
The mass moved up and down during
Labia Minora is a smaller fold of skin, devoid of
swallowing. An ultrasound scan and needle
fat on the pudendal cleft. It encloses a space,
biopsy revealed the mass to be a multinodular
the vestibule of the vagina. The union of the
goiter. A subtotal thyroidectomy was performed.
labia minora posteriorly is the frenulum of the
After the procedure, the patient complained of
labia or the fourchette. It’s the homologue of
tingling in her hands and feet, and
skin of Penis.
carpopedal spasm. These symptoms
disappeared after 24 hours.
Bulb of Vestibule is an oval shaped mass of
erectile tissue partly embedded in the substance
1. What is a goiter?
of labia minora. They taper and are joined to
2. Why did the mass move up and down during
one another toward the clitoris. It’s attached to
swallowing?
the undersurface of clitories by parts of
3. Why was the patient having difficulty in
intermedia and commissure of the bulb.
breathing and swallowing?
4. Despite only a subtotal thyroidectomy
Clitoris is the homologue of Penis, but consists
performed on the patient, she experienced
only of 2 erectile bodies, the corpora
cavernosa clitoridis. It begins as a crura of tingling sensation and carpopedal spasm.
Why?
clitoris attached to ischiopubic rami, uniting to
5. What is Chvostek’s sign?
form the body of clitoris, connected to the
6. How can one avoid damaging the recurrent
symphysis by suspensory ligament. It ends in
laryngeal nerve during a thyroidectomy?
a tiny glans.
7. What is the consequence of injuring the
recurrent laryngeal nerve during a Neck has 3 layers:
thyroidectomy? Fasciculi/Deep Cervical Fascia
§ Pre – vertebral layer
§ Pre – tracheal layer
Mass: o Plasters the structure
• “firm” – hard § Superficial Deep Cervical Layer
• “cystic” – soft
“Iatrogenic” – caused by the treatment itself;;
Thyroid Scan – to determine if mass s hot or § Recurrent Laryngeal Nerve
cold nodule. If it’s hot, it’s malignant. You will § Parathryoid
see if iodine will localize in that nodule.
Chvostek sign vs. Trousseau’s
FNAB or Fine Needle Aspiration Biopsy § Chvostek sign is the twitching of the
• Mass is aspirated with needle facial muscles in response to tapping
• Histopath: (+) over the area of the facial nerve.
§ Trousseau’s sign is carpopedal spasm
Fine Needle Aspiration of a thyroid nodule is the caused by inflating the blood pressure
investigation of choice in a patient with a solitary cuff to a level above systolic pressure.
nodule of the thyroid, as it is very successful in
obtaining cells for cytologic examination and
thus in the diagnosis of thyroid carcinoma. It can Recurrent Laryngeal Nerve
usually be performed under local anaesthesia. § (review of Mediastinum)
This patient had a recurrent nodule after § If injured,
previous partial thyroidectomy for thyrotoxicosis. o Difficulty in breathing
o Hoarseness
Multi-nodule
Superior Thyroid Artery – External Laryngeal
• Nodule is a solid mass.
Nerve
• If it has only 1 solid mass: “Nodular
§ If injured, it will affect the pitch.
Goiter”
MINI QUIZ:
Subtotal Thyroidectomy
§ removes PART of thyroid
1. Structure located on the posterior surface of
§ Total Thyroidectomy – removes ALL
the thyroid gland? Parathyroid Gland.
thyroid
2. Electrolyte deficiency seen in the patient?
Hypocalcemia.
Thyroid Gland
3. Structure that is if injured will cause difficulty
§ Butterfly in shape
in breathing? Recurrent Laryngeal Nerve
§ Bilobed;;
4. Where does RLN arise from? Vagus Nerve
§ Connected by Isthmus in the middle
5. Give 1 blood supply of the thyroid gland?
Superior Thyroid Artery, Inferior Thyroid
The Thyroid Gland is the main part of the body
Artery, Thyroidea Ima
that takes up Iodine. In a thyroid scan, Iodine is
labeled with a radioactive tracer, and a special
-----------------------------xxx-------------------------------
camera is used to measure how much tracer is
absorbed from the bloodstream by the thyrid
gland. If a patient is allergic to Iodine,
technetium can be used as an alternative.
Tingling of hands and feet and Carpopedal
Spasm: signs of HYPOCALCEMIA.
Circumoral numbness: sign for spasm
Surgery of Thryoid
You might also like
- 2nd Sem. Neuroana CDocument27 pages2nd Sem. Neuroana CKim RamosNo ratings yet
- Assignment - Math in Our WorldDocument4 pagesAssignment - Math in Our WorldKim RamosNo ratings yet
- 32999Document4 pages32999Kim RamosNo ratings yet
- 1 - Atherosclerosis Pathogenesis PDFDocument21 pages1 - Atherosclerosis Pathogenesis PDFKim RamosNo ratings yet
- 1 PATHO 2b - Repair - Dr. BailonDocument9 pages1 PATHO 2b - Repair - Dr. BailonKim RamosNo ratings yet
- Control or Prevention of Identified BiasesDocument1 pageControl or Prevention of Identified BiasesKim RamosNo ratings yet
- Research On Problems of The Dialysis Patient: FormedDocument2 pagesResearch On Problems of The Dialysis Patient: FormedKim RamosNo ratings yet
- Puerperium and AnalgesiaDocument12 pagesPuerperium and AnalgesiaKim RamosNo ratings yet
- Sampling Methods GuideDocument35 pagesSampling Methods GuideKim RamosNo ratings yet
- B. Mayosi PenicllinDocument31 pagesB. Mayosi PenicllinKim RamosNo ratings yet
- Dyspnea and Hypoxia (MMGP)Document7 pagesDyspnea and Hypoxia (MMGP)Kim RamosNo ratings yet
- 2 - Adrenergic PharmaDocument29 pages2 - Adrenergic PharmaKim RamosNo ratings yet
- Learning and Teaching 3 PDFDocument63 pagesLearning and Teaching 3 PDFKim RamosNo ratings yet
- Lab ExamDocument2 pagesLab ExamKim RamosNo ratings yet
- XBs and OxidantsDocument6 pagesXBs and OxidantsKim RamosNo ratings yet
- Y2 NS2 4th Exam ReviewerDocument17 pagesY2 NS2 4th Exam ReviewerKim RamosNo ratings yet
- Cell Adaptation, Injury and Death PathologyDocument10 pagesCell Adaptation, Injury and Death PathologyKim RamosNo ratings yet
- InstructionsDocument1 pageInstructionsKim RamosNo ratings yet
- Reaction Paper On Unethical Experiments' Painful Contributions To Today's MedicineDocument2 pagesReaction Paper On Unethical Experiments' Painful Contributions To Today's MedicineKim RamosNo ratings yet
- Opioids and synthetic analgesicsDocument4 pagesOpioids and synthetic analgesicsKim RamosNo ratings yet
- ParaDocument7 pagesParaKim RamosNo ratings yet
- Pedia G&DDocument2 pagesPedia G&DKim RamosNo ratings yet
- 3rd MNC Meeting, May 3, 2018Document11 pages3rd MNC Meeting, May 3, 2018Kim RamosNo ratings yet
- (Pharma-B) 6s-1-Draft - Experiment C & eDocument3 pages(Pharma-B) 6s-1-Draft - Experiment C & eKim RamosNo ratings yet
- LetterDocument1 pageLetterKim RamosNo ratings yet
- CENTRO ESCOLAR UNIVERSITY- SCHOOL OF MEDICINE PHYSIOLOGIC OBSTETRICS LONG EXAMDocument9 pagesCENTRO ESCOLAR UNIVERSITY- SCHOOL OF MEDICINE PHYSIOLOGIC OBSTETRICS LONG EXAMKim Ramos100% (1)
- Quizzes: Lab. Examsd and F Cardiovascular and Git Expts. On Herbal PlantsDocument2 pagesQuizzes: Lab. Examsd and F Cardiovascular and Git Expts. On Herbal PlantsKim RamosNo ratings yet
- NS 2 3rd Shift - RAMOSDocument3 pagesNS 2 3rd Shift - RAMOSKim RamosNo ratings yet
- Fetal Morphological and Physiological Development PDFDocument10 pagesFetal Morphological and Physiological Development PDFKim RamosNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5784)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Anatomy & Physiology QuestionsDocument10 pagesAnatomy & Physiology Questionskrishna chandrakani100% (2)
- Investigation of InfertilityDocument17 pagesInvestigation of InfertilityRamona GaluNo ratings yet
- Current Practices and Controversies in Assisted ReproductionDocument404 pagesCurrent Practices and Controversies in Assisted Reproductionalessia_chiriu8567No ratings yet
- Case Analysis Group 1Document47 pagesCase Analysis Group 1bunso padillaNo ratings yet
- NCMDocument62 pagesNCMlunamoonvaleria00No ratings yet
- NP2 Nursing Board Exam June 2008 Answer KeyDocument14 pagesNP2 Nursing Board Exam June 2008 Answer KeyBettina SanchezNo ratings yet
- Name: Class:: Natural Science Primary 6 - Downloadable and Printable © Ediciones Bilingües, S.LDocument2 pagesName: Class:: Natural Science Primary 6 - Downloadable and Printable © Ediciones Bilingües, S.LMªDolores86% (14)
- INFERTILITYDocument48 pagesINFERTILITYAyisha EdwinNo ratings yet
- Human ReproductionDocument16 pagesHuman ReproductionNajeela khaleelNo ratings yet
- Female Reproductive System Lesson PlanDocument7 pagesFemale Reproductive System Lesson PlanAlizah Belle Garfin100% (1)
- 1 Reproductive and Sexual HealthDocument57 pages1 Reproductive and Sexual HealthFion NixonNo ratings yet
- CBSE 8 Science CBSE - Reproduction in Animals, Free Test Papers, Sample Questions, HOTS Questions and Notes, CBSE - Reproduction in AnimalsDocument5 pagesCBSE 8 Science CBSE - Reproduction in Animals, Free Test Papers, Sample Questions, HOTS Questions and Notes, CBSE - Reproduction in AnimalsR.Shruti 1040-12No ratings yet
- Fallopian Tube Infection Causes, Symptoms & TreatmentDocument10 pagesFallopian Tube Infection Causes, Symptoms & TreatmentmustikaweniNo ratings yet
- 2 3 Yt How Do Organisms ReproduceDocument59 pages2 3 Yt How Do Organisms ReproduceCool VighneshNo ratings yet
- CASE STUDY AbortionDocument32 pagesCASE STUDY AbortionSapna thakur94% (18)
- Presentation On Hysterosalpingography: BY Mahmud M Alkali I.D: 12/01/09/069 Radiography, Unimaid. 2014/2015 SESSIONDocument23 pagesPresentation On Hysterosalpingography: BY Mahmud M Alkali I.D: 12/01/09/069 Radiography, Unimaid. 2014/2015 SESSIONMubarak M AlkaliNo ratings yet
- NP2 Recalls 9Document10 pagesNP2 Recalls 9AhrisJeannine EscuadroNo ratings yet
- Cervical Cancer Case PresDocument40 pagesCervical Cancer Case PresEna100% (1)
- Accuracy of Tubal Patency Assessment in Diagnostic Hysteroscopy Compared With Laparoscopy in Infertile WomenDocument20 pagesAccuracy of Tubal Patency Assessment in Diagnostic Hysteroscopy Compared With Laparoscopy in Infertile Womenria.janitaNo ratings yet
- Anatomy of the Pelvis & PerineumDocument162 pagesAnatomy of the Pelvis & PerineumKolawole Adesina KehindeNo ratings yet
- Case Pres TamparanDocument22 pagesCase Pres TamparanAlano S. LimgasNo ratings yet
- Female Reproductive System OverviewDocument49 pagesFemale Reproductive System OverviewJohaifha CompaniaNo ratings yet
- Concept Map Ectopic PregnancyDocument16 pagesConcept Map Ectopic PregnancyLawrence CapuchinoNo ratings yet
- Bio QnsDocument13 pagesBio QnsRamakrishnan RangarajanNo ratings yet
- The Female Reproductive System: It Consists ofDocument4 pagesThe Female Reproductive System: It Consists ofDawnNo ratings yet
- NURSING PRACTICE I - Foundation of PROFESSIONAL Nursing Practice SITUATIONALDocument102 pagesNURSING PRACTICE I - Foundation of PROFESSIONAL Nursing Practice SITUATIONALAlyssa BusalpaNo ratings yet
- Hysterosalpingography A Re - Emerging Study With CDocument7 pagesHysterosalpingography A Re - Emerging Study With CTuyul Yelsi 1No ratings yet
- Asc101 Lab Exercise No. 3Document10 pagesAsc101 Lab Exercise No. 3MELITO JR. CATAYLONo ratings yet
- Pa Tho Physiology of Ectopic PregnancyDocument2 pagesPa Tho Physiology of Ectopic Pregnancynelyang17100% (6)
- Marketing Channel Strategy 8th Edition Palmatier Solutions ManualDocument26 pagesMarketing Channel Strategy 8th Edition Palmatier Solutions ManualStacyCarrgpjkb100% (49)