Professional Documents
Culture Documents
How Do I Diagnose The Cause of A Cough of Less Than 3 Weeks' Duration?
Uploaded by
Sudhir Tyagi0 ratings0% found this document useful (0 votes)
284 views14 pagescough differential diagnosis and treatment
Original Title
Cough
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentcough differential diagnosis and treatment
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
284 views14 pagesHow Do I Diagnose The Cause of A Cough of Less Than 3 Weeks' Duration?
Uploaded by
Sudhir Tyagicough differential diagnosis and treatment
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 14
How do I diagnose the cause of a cough of less than
3 weeks' duration?
If cough is associated with significant breathlessness, see the CKS topic on
Breathlessness.
• An upper respiratory tract infection is the most likely cause when:
o There are no other respiratory symptoms such as breathlessness,
pleuritic chest pain, haemoptysis, or wheeze, and
o Examination of the chest is normal.
• If the person has chest signs and/or respiratory symptoms in addition to
cough:
o Identify people who need emergency admission including people with
clinical features of:
Pulmonary embolism, pneumothorax, or foreign body
aspiration.
Severe illness, based on an assessment of their pulse rate, blood
pressure, temperature, respiratory rate, peak expiratory flow
rate, and oxygen saturation level (if pulse oximetry is
available).
• If the person has chest signs and/or respiratory symptoms in addition to
cough and does not require emergency admission, look for clinical features
of:
o Lung cancer. Arrange a chest X-ray to be reported within 5 days if
features of lung cancer are present.
If the person is older than 40 years of age with persistent
haemoptysis and smokes, also arrange urgent referral to a
respiratory physician.
If the person has a chest X-ray that is suggestive of lung cancer
(including pleural effusion and slowly resolving consolidation)
arrange urgent referral to a respiratory physician. If features of
lung cancer are present, arrange a chest X-ray to be reported
within 5 days.
o Pneumonia. The diagnosis can be confirmed by chest X-ray, but it is
not considered necessary if the person is well enough to be managed in
the community.
Arrange a chest X-ray if the person is older than 50 years of
age, smokes, and has clinical features of pneumonia, to look for
signs of underlying lung cancer.
o Acute bronchitis. The diagnosis is confirmed by clinical features alone.
o Acute asthma. The diagnosis is confirmed by demonstrating variable
airflow limitation by:
Serial peak expiratory flow rate measurements demonstrating
greater than a 20% diurnal or day-to-day change, or
Where there is doubt, by a large response (more than 400 mL)
to either bronchodilators or 30 mg of oral prednisolone daily
for 14 days.
o An acute exacerbation of chronic obstructive pulmonary disease
(COPD) if the person is older than 35 years of age, and smokes or has
smoked. The diagnosis is confirmed by:
Demonstrating air flow limitation by spirometry that is not
fully reversible with treatment.
Air flow limitation is defined as a forced expiratory volume in
1 second (FEV1) of less than 80% of the predicted value and
FEV1/forced vital capacity ratio less than 70%.
o An acute exacerbation of bronchiectasis, especially in non-smokers
with chronic productive cough or recurrent chest infections. The
diagnosis is confirmed by:
Arranging a chest X-ray to exclude other causes for symptoms,
and
Referring to a respiratory physician for confirmation of the
diagnosis by high resolution CT scanning.
o Pertussis, especially if the person has cough lasting more than 14 days
with paroxysms of coughing or vomiting after coughing or cough
associated with an inspiratory whoop, and if they have developed a
cough within 3 weeks of being in contact with someone with
confirmed pertussis. The diagnosis is confirmed by:
Taking nasopharyngeal aspirates or nasal swabs for culture if
the person presents up to 2 weeks after the onset of the cough,
or by taking blood for serology if the person presents more than
2 weeks after the onset of the cough.
What are the clinical features of the common causes
of acute cough?
• Upper respiratory tract infections
o Conditions include the common cold, influenza, pharyngitis, otitis
media, and sinusitis.
o Symptoms — may cause cough with or without sputum, general
malaise, and possibly fever. Infection and symptoms, such as pain and
discharge, may be localized to the nose, ears, throat, or sinuses.
o Signs — no focal chest signs.
• Acute bronchitis
o Symptoms — cough with or without sputum, breathlessness, wheeze,
or general malaise.
o Signs — no chest signs other than wheeze and crackles. Crackles, if
present, should clear with coughing — if they persist, diagnose
pneumonia.
• Pneumonia
o Symptoms — cough associated with at least one other symptom of
breathlessness, sputum, wheeze, or pleuritic pain.
o Signs — any focal chest sign (such as dull percussion note, bronchial
breathing, or coarse crackles) plus at least one systemic feature (such
as fever/sweating, or myalgia), with or without a temperature greater
than 38°C. There may be signs of an associated pleural effusion.
• Acute asthma
o Risk factors — personal history of rhinitis or eczema, or family
history of atopy.
o Symptoms — wheeze, breathlessness, cough. Symptoms are variable
(often worse at night, first thing in the morning, and upon exercise or
exposure to cold or allergens).
o Signs — there may be none when the person is feeling well. During an
acute episode, the respiratory rate is increased, and wheeze is usually
present.
o Peak expiratory flow rate (PEFR) is reduced during an acute episode.
Acute asthma is:
Life-threatening — when PEFR is less than 33% of predicted,
and is associated with tachycardia, hypotension, a silent chest,
or impaired level of consciousness.
Severe — when PEFR is 33–50% of predicted, and is
associated with a respiratory rate of more than 25 breaths per
minute and an inability to complete full sentences.
Moderate — when PEFR is more than 50% of predicted, with a
respiratory rate of less than 25 breaths per minute.
• Acute exacerbation of chronic obstructive pulmonary disease (COPD)
o History — typically, the person is older than 35 years of age, is a
smoker or past smoker, and reports slowly progressive breathlessness
often associated with wheezing or chest tightness, and a cough
(producing purulent sputum).
o Symptoms of acute exacerbation — new or worsening cough
associated with worsening breathlessness, and wheeze.
o Signs — wheeze, hyperinflated chest (in emphysema), crackles (when
infection is present). There may be signs of right-side heart failure in
people with severe disease, including swollen ankles and increased
jugular venous pressure. The person's peripheries (the hands and feet)
are often warm to the touch and a dusky colour (cyanosed), with
distended veins.
• Acute exacerbation of bronchiectasis
o History of bronchiectasis — suspect if the person has a history of
recurrent or chronic productive cough (present in 75–100% of adults
with bronchiectasis), progressive breathlessness (72–83%),
haemoptysis (51–45%), and non-pleuritic chest pain between
exacerbations (31%).
o Symptoms of an acute exacerbation — new or worsening cough that
may be associated with worsening breathlessness and wheeze.
o Signs — coarse crackles in early inspiration commonest in the lower
lung fields (70% of adults), wheeze (34%), and large airway rhonchi
(44%). Finger clubbing occurs infrequently.
• Pulmonary embolism (PE)
o Risk factors — immobilization, surgery, cancer, symptoms or signs of
deep vein thrombosis (DVT).
o Symptoms — acute-onset breathlessness (in 73% of people with PE),
pleuritic pain (66%), cough (37%), haemoptysis (13%). Recurrent
acute episodes may lead to chronic breathlessness.
o Signs — tachypnoea of more than 20 breaths per minute (in 70% of
people with PE), crackles (51%), tachycardia (30%), signs of
DVT (11%).
• Pneumothorax/tension pneumothorax
o Risk factors — smoking, age, and body type (adults who are young,
tall, and slim), previous pneumothorax, chronic respiratory disease
(such as COPD or asthma), trauma to chest wall (including therapeutic
procedures such as injections and aspirations).
o Symptoms — collapse, sudden-onset pleuritic pain, breathlessness.
o Signs — reduced chest wall movements, reduced breath sounds,
reduced vocal fremitus, and increased resonance of the percussion note
on the affected side. Tension pneumothorax can result in rapid
development of severe symptoms associated with tracheal deviation
away from the pneumothorax, tachycardia, and hypotension.
• Aspiration of a foreign body
o Symptoms — sudden onset of cough that may be associated with
history suggestive of an inhaled foreign body.
o Signs — sudden onset of cough, distress, or stridor if the foreign body
lodges in the upper airway. There may be signs of lung or lobar
collapse if there is a foreign body in the lower airways. Signs of lung
or lobar collapse include reduced chest wall movement on affected
side, dull percussion note with bronchial breathing, and reduced or
diminished breath sounds.
• Lung cancer
o Risk factors — smoking, primary cancers at other sites, asbestos
exposure, COPD.
o Symptoms — haemoptysis or persistent and unexplained cough, chest
or shoulder pain, breathlessness, weight loss, hoarseness.
o Signs — finger clubbing, cervical or supraclavicular
lymphadenopathy, signs of superior vena cava obstruction, stridor.
• Pertussis
o History — suspect in an adult with a cough:
Lasting more than 14 days with paroxysms of coughing or
vomiting after coughing or a cough associated with an
inspiratory whoop. Paroxysms increase in frequency and
severity as the condition progresses and usually persists for 2–
6 weeks. Occasionally the cough may persist for several
months. A prolonged cough may be the only symptom in
adults.
That develops within 2 weeks of being in contact with someone
with confirmed pertussis.
o Signs — normal chest examination.
When should I arrange emergency admission for
someone with acute cough?
• If the person has chest signs or respiratory symptoms in addition to
cough, measure blood pressure, pulse rate, temperature, and oxygen
saturation. If asthma is suspected, measure peak expiratory flow rate (PEFR).
• Arrange emergency admission if the person has:
o A respiratory rate of more than 30 breaths per minute.
o Tachycardia greater than 130 beats per minute.
o Systolic blood pressure less than 90 mmHg, or diastolic blood pressure
less than 60 mmHg (unless this is normal for them).
o Oxygen saturation less than 92%, or central cyanosis (if the person has
no history of chronic hypoxia).
o PEFR less than 33% of predicted.
o Altered level of consciousness.
o A large respiratory effort (particularly if the person is becoming
exhausted).
o Clinical features of pulmonary embolism, pneumothorax, or aspiration
of a foreign body.
• Consider arranging emergency admission, depending on the severity and
number of risk factors present, if the person has any of the following:
o Elevated respiratory rate (but if it is more than 30 breaths per minute,
arrange emergency admission).
o Tachycardia (but if it is more than 130 beats per minute, arrange
emergency admission).
o Hypotension (but if blood pressure is less than 90 mmHg systolic or
60 mmHg diastolic, arrange emergency admission).
o High temperature (especially if it is higher than 38.5°C).
o PEFR less than 50% of predicted (but if it is less than 33%, arrange
emergency admission).
o Older than 65 years of age.
Basis for recommendation
Central cyanosis
• Central cyanosis is reported to be present when the concentration of
deoxygenated haemoglobin is more than 50 g/L. This corresponds to an
arterial oxygen saturation of less than 90% in people who are not anaemic
[Douglas and Bevan, 2009].
Peak expiratory flow rate (PEFR)
• The SIGN and BTS British guideline on the management of asthma
recommends that people with asthma and PEFR less than 30% of predicted,
have life-threatening asthma; and recommends emergency admission [SIGN
and BTS, 2009].
How should I manage someone with acute cough
waiting for emergency admission?
• If the person has an oxygen saturation of less than 92%, give oxygen and
continuously monitor their oxygen saturation levels while waiting for transfer
to hospital.
o ONLY USE A 28% VENTURI MASK AT 4 L/MIN FOR
PEOPLE WITH SUSPECTED CHRONIC OBSTRUCTIVE
PULMONARY DISEASE (COPD), morbid obesity, a chest wall
deformity, or a neuromuscular disorder. This is because they are at risk
of hypercapnic respiratory failure.
o For other people who are acutely ill, use a simple face mask. Adjust
the flow rate to 5–10 L/min to achieve a target oxygen saturation of
94–98%.
• Identify and treat if the person has clinical features of acute severe
asthma (peak expiratory flow less than 50% of predicted) or an acute
exacerbation of COPD.
Give a bronchodilator (for example nebulized salbutamol 5 mg,
or repeated doses of a metered-dose inhaler via a spacing
device).
Give prednisolone 30 mg orally (if available).
Repeat the bronchodilator treatment as necessary.
How should I manage someone with acute cough who
does not need emergency admission?
For people with:
• An upper respiratory tract infection — advise them:
o To use paracetamol or ibuprofen as required to reduce pain or
symptoms of malaise.
o To rest and drink sufficient fluids to prevent dehydration.
o To seek medical advice if symptoms deteriorate significantly or other
symptoms develop.
o That antibiotics are not likely to be helpful.
o That cough medicines may help, but they are not thought to be any
more effective than simple remedies such as a honey and lemon drink.
How do I diagnose the cause of sub-acute cough of 3-
8 weeks' duration?
• If the person has a cough that started with an obvious respiratory
infection:
o Identify people with clinical features of pneumonia or acute bronchitis.
o Identify people with pertussis (whooping cough):
Suspect in an adult with cough lasting more than 14 days with
paroxysms of coughing or vomiting after coughing or an
inspiratory whoop, and in adults presenting with cough who
have been in contact with someone with confirmed pertussis in
the preceding 3 weeks.
Confirm the diagnosis by taking blood for serology.
o Identify people with post-infectious cough (who do not have specific
features suggestive of pertussis). The following features should all be
present:
Absence of malaise.
A persistent dry cough.
A normal respiratory examination.
• If the person has sub-acute cough that did not start with an obvious
respiratory tract infection, look for a cause of chronic cough.
When should I arrange urgent referral to a
respiratory physician for someone with sub-acute
cough?
• Identify whether the person has clinical features of:
o Lung cancer, including:
Haemoptysis, or
Any of the following symptoms and signs that are unexplained
and persist for longer than 3 weeks: chest and/or shoulder pain,
breathlessness, weight loss, chest signs, hoarseness, finger
clubbing, cervical/ supraclavicular lymphadenopathy.
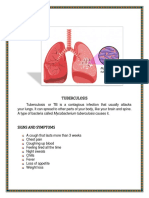
o Pulmonary tuberculosis, including:
Chronic cough which may be associated with sputum,
breathlessness, or haemoptysis.
Weight loss, fever, night sweats, anorexia, and general malaise.
Finger clubbing.
o Foreign body aspiration, including:
Sudden onset of cough that may be associated with history
suggestive of an inhaled foreign body.
Stridor, if the foreign body is in the upper airway. There may
be signs of lung or lobar collapse if the foreign body is in the
lower airways. Signs of lung or lobar collapse include reduced
chest wall movement on the affected side, a dull percussion
note with bronchial breathing, reduced or diminished breath
sounds.
•
• If the person has clinical features of lung cancer:
o Arrange a chest X-ray to be reported within 5 days.
o Arrange urgent referral to respiratory physician:
For people older than 40 years of age with persistent
haemoptysis who smoke.
For people with a chest X-ray that is suggestive of lung cancer
(including pleural effusion or slowly resolving consolidation).
• If the person has clinical features of pulmonary tuberculosis:
o Arrange a chest X-ray and, if possible, send three sputum samples
(ideally one sample should be taken in the early morning) for
microscopy to look for acid-fast bacilli and for mycobacterial culture.
o Refer to a specialist for diagnosis and management (ideally within
2 weeks). Do not delay referral to a specialist by waiting for
investigation results if symptoms are highly suggestive of active
tuberculosis.
• If the person has a suspected foreign body aspiration, arrange urgent
referral or emergency admission (depending on clinical judgement) to a
respiratory physician for bronchoscopy.
How should I manage someone with sub-acute cough
who does not need urgent referral?
• If the person has pneumonia or acute bronchitis, see the CKS topic on
Chest infections - adult.
• If the person has post-infectious cough:
o Explain that the cough may persist for several months.
o Advise them to re-attend for assessment if the cough does not improve
after 2 months.
• If the person has a sub-acute cough that did not start with an obvious
respiratory tract infection, assess and manage as for chronic cough.
How should I assess someone presenting with chronic
cough of more than 8 weeks' duration?
• If the person is taking an angiotensin-converting enzyme (ACE) inhibitor
— stop the treatment and prescribe an alternative.
o The diagnosis is confirmed by resolution or marked improvement of
the cough after stopping the treatment.
o For most people the cough resolves within 1 month, but occasionally it
may persist for several months.
• If the person smokes:
o Advise them to stop smoking and offer them support to do so.
Smoker's cough is confirmed by resolution or marked
improvement of the cough following smoking cessation.
Usually cough resolves within 4 weeks, but it may take longer.
o Identify whether the person has clinical features of chronic obstructive
pulmonary disease (COPD). The diagnosis is confirmed by:
Spirometry demonstrating airflow limitation that is not fully
reversible with treatment.
Air flow limitation is defined as a forced expiratory volume in
1 second (FEV1) of less than 80% of the predicted value and
FEV1/forced vital capacity ratio less than 70%.
A chest X-ray to exclude other causes for symptoms, such as
lung cancer.
• If the person has clinical features of chronic sinusitis or allergic rhinitis
suggesting a diagnosis of upper airway cough syndrome (post-nasal drip),
arrange a 2 week trial of a nasal corticosteroid.
o The diagnosis is confirmed by resolution or marked improvement of
the cough within 2 weeks.
• If the person has clinical features of asthma:
o Arrange serial peak expiratory flow rate (PEFR) measurements
morning and night and prescribe a 2 week trial of an inhaled
corticosteroid and a bronchodilator.
o The diagnosis is confirmed by:
Serial PEFR measurements demonstrating airflow limitation
that is variable or, where there is doubt, by a large response
(more than 400 mL) to either bronchodilators or 30 mg of oral
prednisolone daily for 14 days, and
Resolution or marked improvement of the cough with
treatment.
• If the person has dyspepsia, or a cough that is worse during or after
eating, when bending, or has other clinical features of gastro-oesophageal
reflux disease (GORD):
o Arrange an 8 week trial of a proton pump inhibitor such as omeprazole
20–40 mg twice daily (or equivalent). If the cough only partially
resolves, add in a prokinetic agent such as metoclopramide 10 mg three
times daily.
o The diagnosis is confirmed by resolution or marked improvement of
the cough within 4 months of starting treatment.
• If the person has a chronic productive cough, look for features of
bronchiectasis and arrange a chest X-ray and spirometry.
o If clinical features of bronchiectasis are present and the chest X-ray
and spirometry do not indicate another cause refer to a specialist to
arrange high-resolution CT scanning to confirm the diagnosis.
• If the person has a chronic dry cough:
o Look for features of interstitial lung disease and if present arrange a
chest X-ray and spirometry.
Refer the person for specialist investigations if they have
spirometry with a restrictive pattern and/or a chest X-ray
suggestive of an underlying cause for interstitial lung disease
(such as sarcoidosis or asbestosis).
o Look for clinical features of pertussis (whooping cough) especially if
the person has a cough lasting more than 14 days with paroxysms of
coughing or vomiting after coughing or a cough associated with an
inspiratory whoop, and in people who develop a cough within 3 weeks
of being in contact with someone with confirmed pertussis. The
diagnosis is confirmed by taking blood for serology.
• If the person has a persistent unexplained cough, arrange a chest X-ray, and
spirometry.
o If there is no cause suggested from the history, examination, and
investigations, see Further assessment.
Basis for recommendation
• Recommendations are based on expert opinion published in the UK guidelines
for use of erythromycin chemoprophylaxis in persons exposed to pertussis
[Dodhia et al, 2002].
How do I assess someone with chronic cough, when
no cause is suggested from the history, examination,
spirometry, chest X-ray, and blood tests?
• If the person has chronic cough with no cause suggested from the history,
examination, spirometry, chest X-ray, and blood tests — arrange a
sequential trial of drug treatment:
o Upper airway cough syndrome — prescribe a nasal corticosteroid
and review after 2 weeks of treatment.
The diagnosis is confirmed by resolution or marked
improvement of the cough within 2 weeks.
o Asthma — prescribe a topical corticosteroid and review after 2 weeks
of treatment.
The diagnosis of asthma, cough variant asthma, or eosinophilic
bronchitis is confirmed by resolution or marked improvement
of the cough within 2 weeks.
o Gastro-oeophageal reflux disease — prescribe a proton pump
inhibitor such as omeprazole 20 to 40 mg twice daily (or equivalent)
and review after 8 weeks.
The diagnosis is confirmed by resolution or marked
improvement of the cough within 8 weeks.
• If the person has a chronic cough that partially responds to a trial of
therapy, consider if there is more than one cause of the cough.
• If the person has a chronic cough that has no identifiable cause following
the above assessment — arrange referral to a respiratory physician
(preferably to a specialist who runs a cough clinic).
What are the clinical features of the non-pulmonary
causes of chronic cough?
• Angiotensin-converting enzyme (ACE) inhibitor induced cough
o History — cough may start almost immediately after the person starts
an ACE inhibitor or after a dose increase, or it may occur after several
years of treatment. Cough settles after the person stops the ACE
inhibitor, but may take up to 4 months to completely resolve.
o Symptoms — bouts of coughing associated with the perception of
airway irritation. Between coughing bouts, the person is asymptomatic.
o Signs — no signs of chest disease.
• Gastro-oesophageal reflux disease
o Symptoms.
Cough that may or may not be associated with symptoms of
gastro-oesophageal reflux. Symptoms of gastro-oesophageal
reflux commonly occur after eating a large meal or with
bending.
Cough that is worse during or after eating, with talking, and
with bending.
o Signs — no signs of chest disease.
• Upper airway cough syndrome (also called post-nasal drip) caused by:
o Chronic sinusitis
Symptoms — chronic (more than 12 weeks) nasal blockage or
nasal discharge with facial pain or pressure over the affected
sinus. A reduced sense of smell is common. Pain may radiate
into the upper teeth.
Signs — There may be tenderness to palpation of the effected
sinus.
o Allergic rhinitis
History — allergic rhinitis is more likely if there is a personal
or family history of atopy (asthma, eczema, or allergic rhinitis).
Symptoms — nasal itching, sneezing, discharge, and blockage.
Symptoms may be associated with exposure to a known
allergen such as house dust mite, animal dander, or pollens.
What are the clinical features of the pulmonary
causes of chronic cough?
• Asthma
o Risk factors — personal and family history of atopy.
o Symptoms — wheeze, breathlessness, and cough. Symptoms are
variable, often worse at night, with exercise, or with exposure to cold
or allergens.
o Signs — wheeze is present during an acute episode, except when
asthma is extremely severe when the chest may be silent.
o The peak expiratory flow rate (PEFR) is reduced during an acute
episode. Acute asthma is:
Life-threatening when the PEFR is less than 33% of predicted.
Severe when the PEFR is 33–50% of predicted.
Moderate when the PEFR is more than 50% of predicted.
• Cough variant asthma
o Clinical features — chronic cough with a normal chest examination,
and normal spirometry.
o May be confirmed by demonstrating hyper-responsiveness to airway
provocation, sputum eosinophilia (only available to a specialist), and
symptomatic improvement with a trial of an inhaled topical
corticosteroid.
• Eosinophilic bronchitis
o Clinical features: chronic cough, normal chest examination, normal
spirometry, and normal response to airway provocation test (only
available to a specialist).
o May be confirmed by demonstrating sputum eosinophilia (only
available to a specialist), and symptom improvement with a trial of an
inhaled corticosteroid.
• Smoker's cough and chronic bronchitis
o Smoker's cough
Symptoms — morning cough with little sputum.
Signs — normal chest examination.
o Chronic bronchitis
Symptoms — chronic productive cough on most days for
3 months in each of two consecutive years, if the person does
not have another cause for chronic cough.
Signs — normal chest examination.
• Chronic obstructive pulmonary disease
o History — slow progressive breathlessness in a person older than
35 years of age who smokes or who has smoked.
o Symptoms — persistent progressive breathlessness usually associated
with wheezing or chest tightness. Acute exacerbations of symptoms are
common, and usually caused by respiratory tract infections.
o Signs — wheeze, hyperinflated chest, may have signs of right sided
heart failure such as swollen ankles and increased jugular venous
pressure.
•
•
• Bronchiectasis
o History — suspect in people with a history of recurrent or chronic
productive cough, especially if they do not smoke.
o Symptoms — cough with daily sputum production (present in 75–
100% of adults with bronchiectasis), progressive breathlessness (72–
83%), haemoptysis (51–45%), non-pleuritic chest pain between
exacerbations (31%).
o Signs — coarse crackles in early inspiration most common in the
lower lung fields (70% of adults), wheeze (34%), large airway rhonchi
(44%). Finger clubbing occurs infrequently.
• Interstitial lung disease (ILD)
o Causes — include idiopathic pulmonary fibrosis, sarcoidosis,
pneumoconioses, ILD associated with drug therapy, ILD associated
with connective tissue disease, and hypersensitivity
pneumonitis/extrinsic allergic alveolitis (following sensitization to
inhaled environmental allergens, for example from birds, hay, or
mushrooms).
o Symptoms — cough and slowly progressive breathlessness. When it is
caused by extrinsic allergic alveolitis there may be a history of
recurrent episodes of flu-like illness following exposure to the
responsible allergen. There may be symptoms of the underlying cause
(for example joint pains when the ILD is associated with connective
tissue disease).
o Signs — there may be none in sarcoidosis. When present, there may be
fine end inspiratory crepitations (indicative of fibrosis), finger
clubbing, cyanosis, and signs of right heart failure.
• Pertussis
o History — suspect in an adult with a cough:
Lasting more than 14 days with paroxysms of coughing or
vomiting after coughing or a cough associated with an
inspiratory whoop. Paroxysms increase in frequency and
severity as the condition progresses and usually persist for 2–
6 weeks. Occasionally the cough may persist for several
months. A prolonged cough may be the only symptom in
adults.
That develops within 2 weeks of being in contact with someone
with confirmed pertussis.
o Signs — normal chest examination.
When should I arrange urgent referral to a
respiratory physician for someone with chronic
cough?
• Identify whether the person has clinical features of:
o Lung cancer, including:
Haemoptysis, or
Any of the following symptoms and signs that are unexplained
and persist for longer than 3 weeks; chest and/or shoulder pain,
breathlessness, weight loss, chest signs, hoarseness, finger
clubbing, cervical/ supraclavicular lymphadenopathy.
o Pulmonary tuberculosis, including:
Chronic cough which may be associated with sputum,
breathlessness, or haemoptysis.
Weight loss, fever, night sweats, anorexia, and general malaise.
o Foreign body aspiration, including:
Recurrent pneumonia in the same lobe, which may indicate an
aspirated foreign body.
Sudden onset of cough that may be associated with history
suggestive of an inhaled foreign body.
Stridor, if the foreign body is in the upper airway. There may
be signs of lung or lobar collapse if the foreign body is in the
lower airways. Signs of lung or lobar collapse include reduced
chest wall movement on the affected side, a dull percussion
note, and reduced or diminished breath sounds.
• If the person has clinical features of lung cancer:
o Arrange a chest X-ray to be reported within 5 days.
o Arrange urgent referral to a respiratory physician:
If the person is older than 40 years of age with persistent
haemoptysis, and they smoke.
If the person has a chest X-ray that is suggestive of lung cancer
(including pleural effusion or slowly resolving consolidation).
• If the person has clinical features of pulmonary tuberculosis:
o Arrange a chest X-ray and, if possible, send three sputum samples
(ideally one sample should be taken in the early morning) for
microscopy to look for acid-fast bacilli and for mycobacterial culture.
o Refer to a specialist for diagnosis and management (ideally within
2 weeks). Do not delay referral to a specialist by waiting for
investigation results if symptoms are highly suggestive of active
tuberculosis.
• If the person has a suspected foreign body aspiration, arrange urgent
referral to a respiratory physician for bronchoscopy.
You might also like
- Expanded 3P Study Guide YasminaIrinaDocument79 pagesExpanded 3P Study Guide YasminaIrinaikNo ratings yet
- Inflamed Trachea, (Tracheitis) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandInflamed Trachea, (Tracheitis) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Pleurisy, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandPleurisy, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Pulmonary Diseases - Dental ManagementDocument45 pagesPulmonary Diseases - Dental Managementfilyouth4life100% (3)
- Dizziness and Difficulty Breathing CaseDocument4 pagesDizziness and Difficulty Breathing CaseLucyellowOttemoesoeNo ratings yet
- PericarditisDocument29 pagesPericarditisPavin KumarNo ratings yet
- PD OSCE GuideDocument19 pagesPD OSCE GuideChorong ParkNo ratings yet
- Medicine1 Grand PE ScriptDocument10 pagesMedicine1 Grand PE ScriptCarmeline Santi BeronillaNo ratings yet
- Charting Examples For Physical AssessmentDocument16 pagesCharting Examples For Physical Assessmentim3in1No ratings yet
- Common Signs and SymptomsDocument36 pagesCommon Signs and SymptomsJamil AimanNo ratings yet
- H&P OutlineDocument5 pagesH&P Outlineginadaislu100% (1)
- Headache History: Introduction - WIPPPDocument4 pagesHeadache History: Introduction - WIPPPAmjad_2020No ratings yet
- Gastro MnemonicsDocument8 pagesGastro MnemonicsRufina SoomroNo ratings yet
- CVS, Respi Heent ExamDocument8 pagesCVS, Respi Heent ExamDranreb Berylle MasangkayNo ratings yet
- Carbuncle, Incision, Drainage, DebridementDocument11 pagesCarbuncle, Incision, Drainage, DebridementAlvin Germo PasuquinNo ratings yet
- Comprehensive H&P Note Template For Phase 1 Spring Assessment 2016Document5 pagesComprehensive H&P Note Template For Phase 1 Spring Assessment 2016Derek JonesNo ratings yet
- Pediatric Cardio-Respiratory AssessmentDocument9 pagesPediatric Cardio-Respiratory AssessmentRicky SpideyNo ratings yet
- Deconditioning Syndrome For Patients PDFDocument2 pagesDeconditioning Syndrome For Patients PDFEdmonLagarto100% (1)
- PE Form - NeonateDocument3 pagesPE Form - NeonateStef ReyesNo ratings yet
- SOAP NotesDocument4 pagesSOAP Notesemmag79No ratings yet
- Adult Soap Note GuideDocument5 pagesAdult Soap Note Guidelizdp21No ratings yet
- Hopkins History Taking ArtDocument5 pagesHopkins History Taking ArtAnastasia TjanNo ratings yet
- History & Physical Diagnostic#Document106 pagesHistory & Physical Diagnostic#Olsa Alshapira100% (1)
- Acute Bronchiolitis EditedDocument19 pagesAcute Bronchiolitis EditedSurgicalgownNo ratings yet
- Sign and SymptomsDocument8 pagesSign and SymptomsCaral Grace Gatdula-PenalbaNo ratings yet
- Patient Case Presentation StructureDocument30 pagesPatient Case Presentation StructureAmira HelayelNo ratings yet
- Physical Examination Health AssessmentDocument2 pagesPhysical Examination Health AssessmentRosa Willis0% (1)
- Pre-Op Case Protocol #4Document2 pagesPre-Op Case Protocol #4IC BNo ratings yet
- CVA Case PresentationDocument16 pagesCVA Case PresentationgolokipokNo ratings yet
- CURRENT MEDICAL TREATMENT ON BPHDocument33 pagesCURRENT MEDICAL TREATMENT ON BPHDeviruchi GamingNo ratings yet
- H&P SampleDocument3 pagesH&P Samplelindsay_weiss_6No ratings yet
- How To Read A CTGDocument31 pagesHow To Read A CTGAbdullah As'ad100% (1)
- Mo Intern Handbook - FinalDocument37 pagesMo Intern Handbook - FinalGideon K. MutaiNo ratings yet
- Health HistoryDocument19 pagesHealth HistoryAngelene Caliva100% (1)
- UrosepsisDocument22 pagesUrosepsisWita Ferani KartikaNo ratings yet
- Gordons Case Pres 1Document5 pagesGordons Case Pres 1JM Asentista0% (1)
- Acute Pneumonia: Richard T. Ellison III and Gerald R. DonowitzDocument30 pagesAcute Pneumonia: Richard T. Ellison III and Gerald R. DonowitzNilay ChatterjeeNo ratings yet
- SOAP Note NSG 6420 Week 8Document6 pagesSOAP Note NSG 6420 Week 8Jan FloydNo ratings yet
- Bates Thorax Lungs With TermsDocument4 pagesBates Thorax Lungs With Termscrystalshe100% (1)
- Treating Acute BronchiolitisDocument3 pagesTreating Acute BronchiolitisHajar Hanis SofiaNo ratings yet
- Ob Gyn Soap NoteDocument1 pageOb Gyn Soap NoteMichelle Tanzil100% (1)
- The Detailed Neurologic Examination in Adults - UpToDate PDFDocument29 pagesThe Detailed Neurologic Examination in Adults - UpToDate PDFMiguel GarciaNo ratings yet
- Bates Physical Examination RED NOTESDocument2 pagesBates Physical Examination RED NOTESAmanda Gomez100% (1)
- AhafinalheadtoeDocument4 pagesAhafinalheadtoeapi-620081868No ratings yet
- Obstetrics History Taking in and Examination PowerpointDocument15 pagesObstetrics History Taking in and Examination Powerpointياسر كوثر هانيNo ratings yet
- OSCE Gynae HXDocument3 pagesOSCE Gynae HXmpage3100% (1)
- ConceptMap AMLDocument1 pageConceptMap AMLnursing concept mapsNo ratings yet
- Pneumonia Cheat Sheet: by ViaDocument3 pagesPneumonia Cheat Sheet: by ViaGayle MarieNo ratings yet
- Lower Respiratory Tract Diseases - KeyDocument45 pagesLower Respiratory Tract Diseases - KeyYugmaPandyaNo ratings yet
- PEDIATRIC ASSESSMENT OVERVIEWDocument2 pagesPEDIATRIC ASSESSMENT OVERVIEWAghnia Nafila100% (1)
- Case 36 AscitesDocument4 pagesCase 36 AscitesMichaelNo ratings yet
- Dermatological History and Examination PDFDocument5 pagesDermatological History and Examination PDFHesbon MomanyiNo ratings yet
- 2016 CPG Ent PDFDocument21 pages2016 CPG Ent PDFCamelle CelisNo ratings yet
- Medical History Outline-2020Document9 pagesMedical History Outline-2020sumiti_kumarNo ratings yet
- Differential Diagnosis of Cervical CancerDocument8 pagesDifferential Diagnosis of Cervical Cancerrey martinoNo ratings yet
- Cell Wall Inhibitors and Protein Synthesis Inhibitors Antibiotics Mechanisms of ActionDocument3 pagesCell Wall Inhibitors and Protein Synthesis Inhibitors Antibiotics Mechanisms of Actionyanks1120No ratings yet
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Practical Gastroenterology and Hepatology Board Review ToolkitFrom EverandPractical Gastroenterology and Hepatology Board Review ToolkitKenneth R. DeVaultNo ratings yet
- Anaerobic Infections in HumansFrom EverandAnaerobic Infections in HumansSydney FinegoldRating: 5 out of 5 stars5/5 (1)
- Treatment of Psoriasis DermDocument11 pagesTreatment of Psoriasis DermSudhir TyagiNo ratings yet
- Report of Development of Gujarat Under Narendra Modi Till 2007Document49 pagesReport of Development of Gujarat Under Narendra Modi Till 2007ravighiyarNo ratings yet
- Report of Development of Gujarat Under Narendra Modi Till 2007Document49 pagesReport of Development of Gujarat Under Narendra Modi Till 2007ravighiyarNo ratings yet
- Neral PractitionersDocument216 pagesNeral PractitionersSudhir Tyagi100% (1)
- भारतीय इतिहास की भयंकर भूलDocument177 pagesभारतीय इतिहास की भयंकर भूलInsearchof_Knowledge100% (1)
- Oxygen TherapyDocument7 pagesOxygen TherapySudhir TyagiNo ratings yet
- Oxygen Saturation in BADocument3 pagesOxygen Saturation in BASudhir TyagiNo ratings yet
- Agra Ka Lal Kila Hindu Bhavan Hai - P N OakDocument144 pagesAgra Ka Lal Kila Hindu Bhavan Hai - P N OakPramodNo ratings yet
- भारतीय इतिहास की भयंकर भूलDocument177 pagesभारतीय इतिहास की भयंकर भूलInsearchof_Knowledge100% (1)
- Taj Mahal The True Story - P N OakDocument137 pagesTaj Mahal The True Story - P N Oakrudragni10850% (2)
- Acute Pericarditis and Cardiac TamponadeDocument49 pagesAcute Pericarditis and Cardiac TamponadesajidmuNo ratings yet
- Internal Medicine Essentials For Clerkship Students 2Document369 pagesInternal Medicine Essentials For Clerkship Students 2Sudhir Tyagi100% (29)
- Hypertensive Emergencies 1Document12 pagesHypertensive Emergencies 1Sudhir TyagiNo ratings yet
- Pre and Post Operative CareDocument6 pagesPre and Post Operative CareSudhir Tyagi0% (1)
- Topical CorticosteroidsDocument14 pagesTopical CorticosteroidsSudhir TyagiNo ratings yet
- Grammarism Ed Ing Adjectives Test 4 1189424Document2 pagesGrammarism Ed Ing Adjectives Test 4 1189424Royal Stars Drama AcademyNo ratings yet
- PCS PADDLE SHIFTER INSTALL GUIDEDocument21 pagesPCS PADDLE SHIFTER INSTALL GUIDEAndreas T P ManurungNo ratings yet
- ETHICS NOTES PART 1 - IAS PCS PathshalaDocument15 pagesETHICS NOTES PART 1 - IAS PCS PathshalaATULNo ratings yet
- Datasheet De14h (II) HC 1500v May2019 NTDocument2 pagesDatasheet De14h (II) HC 1500v May2019 NTkrishnakumar paamireddyNo ratings yet
- Unit explores Christian morality and conscienceDocument1 pageUnit explores Christian morality and conscienceRose Angela Mislang Uligan100% (1)
- LirikDocument537 pagesLirikMuhamad Iqbal FahmiNo ratings yet
- Data Sheet ID FanDocument5 pagesData Sheet ID FanrudiawanNo ratings yet
- Monsterology Activity KitDocument2 pagesMonsterology Activity KitCandlewick PressNo ratings yet
- Baby NamesDocument9 pagesBaby Namesppremamca_617705407No ratings yet
- BBO 2011 ROUND 2 QUESTIONSDocument16 pagesBBO 2011 ROUND 2 QUESTIONSMalvina YuanNo ratings yet
- Plant LayoutDocument16 pagesPlant LayoutAli MahmoudNo ratings yet
- ###Questions Model PDFDocument2 pages###Questions Model PDFDave DMNo ratings yet
- Cardiopulmonary System: Relevant Anatomy & Physiology: HeartDocument12 pagesCardiopulmonary System: Relevant Anatomy & Physiology: HeartJulia SalvioNo ratings yet
- Diff Types of Transmission Lines Used in CommsDocument9 pagesDiff Types of Transmission Lines Used in CommsLe AndroNo ratings yet
- Lession Plan - MIDocument21 pagesLession Plan - MINithya SannidhiNo ratings yet
- South African Flora GlossaryDocument47 pagesSouth African Flora Glossarymr.bryceNo ratings yet
- 10 01 Breather Filters GBDocument8 pages10 01 Breather Filters GBosuengNo ratings yet
- Procedure - AC Circuits and Signal Modulation - W20Document6 pagesProcedure - AC Circuits and Signal Modulation - W20ChocoNo ratings yet
- General Psychology - Unit 2Document23 pagesGeneral Psychology - Unit 2shivapriya ananthanarayananNo ratings yet
- Tracking sports training efficiency with surface EMGDocument8 pagesTracking sports training efficiency with surface EMGsdjuknicNo ratings yet
- 1.1 Hardware and SoftwareDocument13 pages1.1 Hardware and SoftwareNurhanis SyazwaniNo ratings yet
- Consumer preference towards branded milk: A comparative analysis of Verka milk and Amul milkDocument12 pagesConsumer preference towards branded milk: A comparative analysis of Verka milk and Amul milkBhawna RehanNo ratings yet
- Reference Design Hardware Guide for EVM CE-2Document7 pagesReference Design Hardware Guide for EVM CE-2Angie FoleyNo ratings yet
- Practice: Circles and ArcsDocument2 pagesPractice: Circles and ArcsTIANA ARILENo ratings yet
- Syllabi - EE 5004 - Power ElectronicsDocument2 pagesSyllabi - EE 5004 - Power ElectronicsKalum ChandraNo ratings yet
- Type 2 Diabetes MellitusDocument6 pagesType 2 Diabetes MellitusJoy NisoladaNo ratings yet
- Clay ShonkwilerDocument9 pagesClay ShonkwilerJeoff Libo-onNo ratings yet
- Gold Grade of Epithermal Gold Ore at Lamuntet, Brang Rea, West Sumbawa District, West Nusa Tenggara Province, IndonesiaDocument10 pagesGold Grade of Epithermal Gold Ore at Lamuntet, Brang Rea, West Sumbawa District, West Nusa Tenggara Province, Indonesiasukri arjunaNo ratings yet
- Data Biostataplus Sbi2014-EDocument4 pagesData Biostataplus Sbi2014-ELucila Milagros PinillosNo ratings yet
- Pd3c CV Swa (22kv)Document2 pagesPd3c CV Swa (22kv)เต่า วีไอNo ratings yet