Professional Documents
Culture Documents
Mammographic Screening of Breastr Cancer
Uploaded by
willyoueverlovemenkOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Mammographic Screening of Breastr Cancer
Uploaded by
willyoueverlovemenkCopyright:
Available Formats
The new england journal of medicine
clinical practice
Mammographic Screening for Breast Cancer
Suzanne W. Fletcher, M.D., and Joann G. Elmore, M.D., M.P.H.
This Journal feature begins with a case vignette highlighting a common clinical problem.
Evidence supporting various strategies is then presented, followed by a review of formal guidelines,
when they exist. The article ends with the authors’ clinical recommendations.
A 44-year-old woman who is a new patient has no known current health problems
and no family history of breast or ovarian cancer. Eighteen months ago, she had a nor-
mal screening mammogram. She recently read that mammograms may not help to
prevent death from breast cancer and that “the patient should decide.” But she does
not think she knows enough. She worries that there is a breast-cancer epidemic. What
should her physician advise?
the clinical problem
From the Department of Ambulatory Care In 1990, for the first time in 25 years, mortality from breast cancer in the United States
and Prevention, Harvard Medical School began dropping; by 1999, the age-adjusted mortality rate was at its lowest level (27.0 per
and Harvard Pilgrim Health Care, Boston
(S.W.F.); and the Department of Medicine, 100,000 population) since 1973.1 Meanwhile, by 1997, 71 percent of women in the
University of Washington, Seattle (J.G.E.). United States who were 40 years of age or older reported having undergone mammog-
Address reprint requests to Dr. Fletcher at raphy during the previous two years — an increase from 54 percent in 1989.2 Ironically,
the Department of Ambulatory Care and
Prevention, 6th Fl., 133 Brookline Ave., Bos- just as screening (or better treatment or both) seemed to be lowering mortality from
ton, MA 02215. breast cancer nationally, questions were raised about the validity of the studies that had
led to widespread screening. For more than two decades, expert groups uniformly agreed
N Engl J Med 2003;348:1672-80.
Copyright © 2003 Massachusetts Medical Society.
that screening mammography reduces mortality from breast cancer among women in
their 50s and 60s, even though they disagreed about other age groups.3 However, ques-
tions were raised in 2000, when two Danish investigators concluded that only three of
eight randomized trials were of sufficient quality to determine the effectiveness of
mammography and that the combined results of these three trials showed no benefit.
This report led to confusion about the usefulness of screening mammography.
strategies, evidence, and areas of uncertainty
Women are interested in knowing about breast cancer and want information from their
doctors.4,5 When women and their physicians are making decisions about screening,
they need information about the underlying risk of the condition being screened for, the
effectiveness of the procedure in preventing an untoward outcome such as death, and
the potential ill effects of screening, such as false positive tests. (For policymakers and
payers, cost effectiveness is an important factor in decisions about the allocation of fi-
nite resources.) Clinical information about each of these issues with regard to breast
cancer and mammography is summarized below.
the risk of development of and death from breast cancer
The average 10-year risk of the development of and death from breast cancer is shown
in Table 1, along with the 10-year risk of death from any cause (in order to provide con-
text).6,7 A computerized tool for calculating an individual woman’s risk of breast cancer,
the Breast Cancer Risk Assessment Tool (available at http://bcra.nci.nih.gov/brc/), can
1672 n engl j med 348;17 www.nejm.org april 24, 2003
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
clinical practice
10-to-15-minute clinical breast examination. The
Table 1. Chances of the Development of and Death studies differed with respect to the years in which
from Breast Cancer within the Next 10 Years.*
they were conducted, the type of mammography
Cases of Invasive Death from Death from used, the interval between mammographic exam-
Age Breast Cancer Breast Cancer Any Cause inations, the method of assigning women to the
screened and unscreened groups, the number of
no./1000 women
screening visits, the age of the women who were
40 Yr 15 2 21 included, and the methods of analysis.3,11 For wom-
50 Yr 28 5 55 en between 50 and 69 years of age, all reports of
60 Yr 37 7 126 studies comparing screening with no screening
showed protective effects of screening, and meta-
70 Yr 43 9 309
analyses that included all trials demonstrated sta-
80 Yr 35 11 670 tistically significant 20 to 35 percent reductions in
mortality from breast cancer.
* Rates for breast cancer and death from breast cancer A widely cited meta-analysis published in 200012
were calculated on the basis of data from Feuer and Wun6;
rates of death from any cause were calculated on the basis (updated in 200113) by Gotzsche and Olsen raised
of data from Anderson and DeTurk.7 questions about the efficacy of mammography. The
authors concluded that the methods used in five of
the eight studies were so flawed that they had to be
be used to calculate the five-year risk and the life- excluded from the meta-analysis. Appropriate ran-
time risk. The tool uses the woman’s age, history of domization should lead to very similar groups, but
first-degree relatives with breast cancer (up to two for five of the studies (and part of a sixth, the Malmö
relatives), number of previous breast biopsies (and II Trial), there were significant differences between
whether any revealed atypical hyperplasia), age at the screened group and the control group in some
menarche, and age at first delivery. It assumes reg- of the characteristics; Gotzsche and Olsen suggest-
ular screening and no history of breast cancer and ed that these differences might bias the trial results.
does not include several known risk factors and sev- Also, numbers varied among different reports on
eral known protective factors (see Supplementary the same trials. Finally, according to a combined
Appendix 1, available with the full text of this article analysis of the four Swedish studies, mortality from
at http://www.nejm.org).8 Overall, the tool has been breast cancer, but not overall mortality, decreased in
found to predict breast cancer well, but its ability to the screened group, raising the possibility of bias in
discriminate at the individual level was not much determining the cause of death, as well as the pos-
better than that of predictions that would have oc- sibility that treatments resulting from findings on
curred by chance,9 so its usefulness is similar to that screening could be dangerous. A meta-analysis of
of Table 1. For women with a strong family history the remaining three studies showed no protective
of breast cancer, ovarian cancer, or both, a program effect of mammography.
that can be used to estimate the risk of genetic mu- The investigators defended their trials. Several
tations in the BRCA1 and BRCA2 genes is available at trials included some subjects who were later deter-
http://astor.som.jhmi.edu/brcapro/. The program mined to be ineligible, and reports sometimes used
has been found to be effective in predicting risk on the woman’s age instead of the date of birth, ac-
an individual level.10 counting for differing numbers. The cluster ran-
domization that was used in several trials probably
mammography and mortality led to small, unimportant base-line differences be-
from breast cancer tween groups.14,15 In an updated analysis of the four
There have been eight randomized trials of the ef- Swedish studies published after the critique, unad-
fectiveness of mammography: four trials in Sweden justed overall mortality was lower in the screened
comparing mammography with no screening; one group (relative risk, 0.98 [95 percent confidence in-
in Edinburgh, Scotland, one in New York, and one terval, 0.96 to 1.00]).16 (Detailed responses to the
in Canada comparing the combination of mam- criticisms of Gotzsche and Olsen are reviewed in
mography and clinical breast examination with no Supplementary Appendix 2, available with the full
screening; and one in Canada evaluating the effect text of this article at http://www.nejm.org.) In addi-
of the addition of mammography to a standardized, tion, Gotzsche and Olsen were criticized for not
n engl j med 348;17 www.nejm.org april 24, 2003 1673
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
considering other methodologic aspects, such as tween 65 and 74 years of age led to a 55 percent de-
the age of participants (one of the trials included crease in mortality from breast cancer (relative risk
only women in their 40s); the number, type, and of death from breast cancer, 0.45 [95 percent con-
quality of screenings and the intervals between fidence interval, 0.20 to 1.02]).25
them; compliance with the assigned strategy; and
contamination (the degree to which women in risks associated with mammography
control groups underwent screening mammogra- False Positive Mammograms
phy).14,15,17,18 Finally, they included a study that Because most women do not have breast cancer at
compared two methods of screening19 and had no the time of screening, there is potential to do harm
unscreened control group. with false positive results that necessitate further in-
In summary, criticisms of all but one of the trials vestigation before a woman can be declared to be
excluded from the meta-analysis have been an- free of disease. Nationally, an average of 11 percent
swered. In-depth independent reviews of the criti- of screening mammograms are read as abnormal
cisms concluded that they do not negate the effec- and necessitate further diagnostic evaluation26;
tiveness of mammography, especially for women breast cancer is found in about 3 percent of women
older than 50 years of age.3,18,20 with an abnormal mammogram (representing 0.3
percent of all mammograms). Therefore, on aver-
women in their 40s age, a woman has about a 10.7 percent chance of a
For many years, there has been controversy over false positive result with each mammogram. Be-
the use of screening mammography for women in cause women are screened repeatedly, a woman’s
their 40s.21 In general, the effect of screening risk of having a false positive mammogram increas-
younger women has been slower to appear and es over time. One study estimated that after 10 mam-
less dramatic than the effect among women older mograms, about half of women (49 percent [95 per-
than 50 years of age. These differences may result cent confidence interval, 40 to 64]) will have had a
from mammographically denser breasts in younger false positive result, which will have led to a needle
women (leading to reduced sensitivity of mammog- biopsy or an open biopsy in 19 percent (95 percent
raphy), faster spread of some cancers in younger confidence interval, 10 to 41).27
women, or both. Meta-analyses show that screen- False positive mammograms increase patients’
ing in this age group decreased 15-year mortality anxiety; the degree of anxiety is related to the in-
from breast cancer by about 20 percent.3,22 tensity of the additional diagnostic procedures and
Because trial results are presented according to the recency of the screening mammogram.20 One
women’s ages at the time of entry into the studies, study found that in the 12 months after a false pos-
some women who entered in their late 40s received itive mammogram, women initiated more health
a diagnosis of breast cancer in their 50s; there- care visits for both breast-related and non–breast-
fore, some of the benefit ascribed to the screening related problems.28 However, false positive mam-
of women in their 40s would have occurred if the mograms increase women’s adherence to further
women had waited until 50 years of age to be screening.29-31
screened.23,24 Also, although analyses are usually The risk of a false positive mammogram varies
presented according to the decade of life, it is likely according to characteristics of the woman and ra-
that a gradual change occurs as a woman ages. The diologic factors: a younger age, an increasing num-
latest analysis of the four Swedish trials — the first ber of breast biopsies, a positive family history of
to examine screening effects according to five-year breast cancer, estrogen use, an increasing interval
age increments — found that screening was most between screenings, the lack of comparison with
effective after 55 years of age.16 previous mammograms, and a tendency by the ra-
diologist to consider mammograms abnormal (as
mammography in women older determined by the percentage of mammograms
than 70 years of age read as abnormal) were independent risk factors
Too few women older than 70 years of age partici- for a false positive result in one study.32 Having
pated in randomized trials to permit conclusions mammographically dense breasts also increases the
to be drawn about the effects of mammographic risk of false positive (or false negative) mammo-
screening in this age group. One case–control study grams.33-35 Many characteristics of patients are im-
in the Netherlands found that screening women be- mutable, but obtaining mammograms during the
1674 n engl j med 348;17 www.nejm.org april 24 , 2003
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
clinical practice
luteal phase of the menstrual cycle may decrease icy and Research recommends that the false positive
mammographic breast density.36 Also, a prelimi- rate be no more than 10 percent.38 The malpractice
nary investigation found that stopping hormone- climate in this country may work against the lower-
replacement therapy 10 to 30 days before a repeated ing of the threshold, since failure to diagnose breast
mammogram eliminated or reduced mammo- cancer is the leading reason for malpractice suits.39
graphic abnormalities.37 Comparison of current and previous mammograms
Lowering the recall rate (the percentage of mam- decreases the false positive rate, as does the use of
mograms that result in recommendations for fur- screening intervals of 18 months or less.
ther tests) is likely to reduce the risk of false positive
mammograms. Because of the trade-off between Possible Overdiagnosis — Ductal Carcinoma in Situ
sensitivity and specificity, it is important not to low- Ductal carcinoma in situ was a relatively rare diag-
er the radiographic threshold for recall so much that nosis before the introduction of mammography. In
cancers are missed. The Agency for Health Care Pol- 1973, the incidence in the United States was 2.4
Table 2. North American Recommendations for Routine Mammographic Screening in Women at Average Risk
Who Are 40 Years of Age or Older.*
Group (Date) Frequency of Screening Initiation of Screening
40–49 Yr 50–69 Yr ≥70 Yr
of Age of Age of Age
yr
Government-sponsored and private groups
U.S. Preventive Services Task Force (2002)† 1–2 Yes Yes Yes‡
Canadian Task Force on Preventive Health Care 1–2 No Yes No
(1998, 1999, 2001)
National Institutes of Health consensus conference (1997) No§ — —
American Cancer Society (1997) 1 Yes Yes Yes
National Cancer Institute (2002) 1–2 Yes Yes Yes
Medical societies
American College of Obstetricians and Gynecologists (2000) 1–2 if 40–49 yr old Yes Yes Yes
1 yr if ≥50 yr old
American Medical Association (1999) 1 Yes Yes Yes
American College of Radiology (1998) 1 Yes Yes Yes
American College of Preventive Medicine (1996) 1–2 No¶ Yes Yes
American Academy of Family Physicians (2001) 1–2 No§¶ Yes No
American Geriatrics Society (1999) 1–2 — — Yes‡
Advocacy groups
National Breast Cancer Coalition (2000) No —§ No
National Alliance of Breast Cancer Organizations (2002) 1 Yes Yes Yes
Susan B. Komen Foundation (2002) 1 Yes Yes Yes
* Adapted from the U.S. Preventive Services Task Force.3 A “no” recommendation may be a statement that there is insuf-
ficient evidence for a positive recommendation.
† Recommendations are for mammography with or without clinical breast examination.
‡ There is an explicit recommendation to screen women older than 70 years of age.
§ Recommendations note that women should be counseled about the risks and benefits of mammography.
¶ Recommendations note that women at high risk should be screened beginning at 40 years of age.
n engl j med 348;17 www.nejm.org april 24, 2003 1675
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
overdiagnosis — finding early neoplasms, many of
Table 3. Recommendations Regarding Breast-Cancer Screening in Women. which will never become invasive breast cancer.
Age Recommendations
Unfortunately, ductal carcinoma in situ can
progress to invasive cancer. The eight-year rate of
Any Ask about family history of breast cancer, ovarian cancer, or both on recurrence in one study of treatment with only sur-
both maternal and paternal sides. Consider referral or counsel-
ing for possible genetic testing if risk of a BRCA1 or BRCA2 gene
gical excision was 27 percent, and half the recur-
mutation is at least 10 percent (to calculate risk, see http:// rences were invasive cancers.43 It is not clear who is
astor. som.jhmi.edu/brcapro/) or the patient has one of the fol- at risk for recurrence and whether survival results
lowing: a first-degree relative with a known deleterious mutation
for breast cancer; ≥2 relatives given a diagnosis of breast cancer
would be the same if surgery were undertaken only
before 50 yr of age, ≥1 of them a first-degree relative; ≥3 relatives after early invasive cancer had been diagnosed. In
given a diagnosis of breast cancer, ≥1 of them before 50 yr of sum, women who undergo screening mammogra-
age; ≥2 relatives given a diagnosis of ovarian cancer; ≥1 relative
given a diagnosis of breast cancer and ≥1 relative given a diag-
phy are more likely than other women to be given a
nosis of ovarian cancer. diagnosis of ductal carcinoma in situ. Whether find-
40–70 Yr Begin discussions about breast-cancer screening at 40 yr of age.
ing it saves lives or merely increases the number of
Recommend screening mammography every 1–2 yr between women who receive a diagnosis of breast cancer is
50 and 69 yr of age. Use information on the chances of develop- not yet clear.
ment of or death from breast cancer within the next 5 yr (as giv-
en in the National Cancer Institute Breast Cancer Assessment
Tool) or 10 yr.* Also give information on benefits and hazards of Other Risks
mammography.† Emphasize the increasing risk of breast can- Many women have pain during mammography, but
cer, increasing benefit of screening, and decreased harms asso-
ciated with screening with increasing age. Record decision
few report that pain deters them from obtaining
about screening in the medical record. subsequent mammograms.44-48 The risks associ-
ated with radiation are small. It has been estimated
>70 Yr For women with life expectancy of ≥10 yr, consider screening as
above, making clear that risks of breast cancer are known that 10 years’ worth of annual mammographic
but less is known about the benefits and harms of screening. screenings in 10,000 women will cause one addi-
Record decision about screening in the medical record. tional breast cancer.49 False negative interpretations
are possible and are more common in younger
* This information is presented in Table 1.
† This information is shown in Figures 1 and 2.
women and in those with dense breasts.50-52
guidelines
cases per 100,000 women; by 1998, it was 30.7 per Recommendations from several leading groups re-
100,000 women, accounting for approximately 14 garding mammographic screening are summarized
percent of all breast cancers diagnosed.1 With treat- in Table 2.3 After the analysis by Gotzsche and
ment, the prognosis is excellent. In one study, wom- Olsen, some, but not all, reconsidered and changed
en given a diagnosis of ductal carcinoma in situ had their recommendations. For example, the editorial
a 9-year survival rate that was the same as or better board of the Physician Data Query data base of the
than that in the general population,40 and in anoth- National Cancer Institute (which does not issue rec-
er study, the risk of death from breast cancer within ommendations, as such) backed away from con-
10 years after the diagnosis of ductal carcinoma in cluding that mammography is effective; instead, the
situ was 1.9 percent.41 board now concludes that mammography “may”
Such an excellent prognosis could be attribut- decrease mortality.23 The U.S. Preventive Services
able to the detection of lesions before they become Task Force moved in the opposite direction and ex-
invasive cancers, which could save lives. However, tended its recommendations for the use of screen-
if ductal carcinoma in situ were the usual precursor ing to include women ranging from 40 years of age
to early invasive cancer, the incidence of early-stage to more than 70 years of age.3
invasive breast cancer should decrease as the inci- Recommendations from expert groups with re-
dence of in situ cancer increases, but the opposite gard to screening women in their 40s have long var-
is happening. Also, autopsy studies in women who ied, but over time, more groups have moved toward
died from causes unrelated to breast cancer have endorsing the same approach for this age group as
shown a substantial “reservoir” of ductal carcino- for older women. Most groups have not issued ex-
ma in situ in such women.42 Therefore, detection plicit recommendations for women older than 70
of ductal carcinoma in situ may be an example of years and merely recommend that screening begin
1676 n engl j med 348;17 www.nejm.org april 24 , 2003
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
clinical practice
at a certain age. More groups have begun calling for relative risks (occurring over meaningful periods),
shared decision making about breast-cancer screen- and through comparisons with other risks.54
ing, but the information to be shared has not been
specified. specific recommendations
All women, regardless of age, should be asked
whether they have a family history of breast cancer,
conclusions and
recommendations ovarian cancer, or both (Table 3).55,56 For women
without strong family histories, discussions about
general conclusions breast-cancer screening should begin at 40 years of
Breast cancer is common, but when viewed over a age and continue until life expectancy is less than
10-year period, the risk for the average woman is 10 years. Evidence supporting the usefulness of
relatively small. During the past few years, scientific mammographic screening is strongest for women
controversy about the benefits of screening mam- between 50 and 69 years of age, and screening
mography has increased. As with most screening should be routinely recommended for women in
tests, there are hazards — primarily, risks of false this age group. For women 40 to 49 years of age
positive mammograms, with associated anxiety and (such as the patient described in the vignette),
unnecessary biopsies, and perhaps a risk of overdi- shared decision making is especially important,
agnosis. because the absolute benefit of screening is smaller
When the benefits of medical interventions are and the risks associated with it are greater. Screen-
controversial and when hazards exist, shared deci- ing should be routinely discussed, and the patient
sion making is needed, with the clinician providing and clinician should decide together according to
facts and the patient assessing her situation from the woman’s values.
the vantage point of her personal values. In addi- For women who want more information, Table
tion, the climate in the United States with regard to 1, the Breast Cancer Risk Assessment Tool, or both
malpractice makes discussions between clinician can be used to estimate the individual risk of breast
and patient about breast-cancer screening essential
for all women beginning at 40 years of age. To save
time, information can be provided by handouts and
≥1 False positive
an office practice that is organized to address the mammogram
concerns of patients. 600 560
Women vary in terms of how much they want to
500 470
participate in decisions about screening. In one sur-
vey of women younger than 50 years of age, 49 per- 400
No. of Women
cent wanted to share in decision making, 44 percent 360
wanted to make the decision themselves, and 7 per- 300 ≥1 Needle or open
biopsy
cent wanted the physician to decide.5 However, 79
190 190 190
percent wanted information from the doctor. Be- 200
cause of varying individual values, and because Development
of breast cancer
women have a good deal of fear about breast can- 100
37
cer,53 physicians should be prepared for a decision 15 28
0
different from the one they would recommend. 40 50 60 40 50 60 40 50 60
A woman needs some knowledge of her risk of Years of Age at Beginning of the 10-Yr Period
breast cancer and the benefits and hazards of
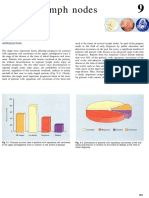
screening — specifically, her risks of the develop- Figure 1. Chances of False Positive Mammograms, Need for Biopsies,
ment of and death from breast cancer and her and Development of Breast Cancer among 1000 Women Who Undergo
Annual Mammography for 10 Years.
chances of successful treatment with screening and
All numbers are rounded. The numbers for 10-year rates of false positive
without screening, of having a false positive mam-
mammograms and breast biopsies come from a single study in which, over-
mogram or an invasive breast procedure, and of hav- all, the rate of false positive mammograms was 6.5 percent,27 and the rate
ing ductal carcinoma in situ diagnosed. Numerical may be different in other settings. Data on the development of breast cancer
risks may be best explained with the use of pictures are broken down further in Figure 2.
or graphs, with discussion of absolute as well as
n engl j med 348;17 www.nejm.org april 24, 2003 1677
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
es that yearly screening mammography in women
Development of different ages will result in a false positive mam-
of breast cancer
40 mogram, an invasive breast procedure, or a diagno-
37
sis of ductal carcinoma in situ or invasive breast
35
cancer. Women should be made aware that at least
Breast cancer cured
30 28
by treatment, half the patients given a diagnosis of breast cancer
survive regardless of the use or nonuse of screening
No. of Women
25 regardless
of screening
— a fact that many women do not understand.57,58
20 18 Diagnosis of ductal
carcinoma in situ Recently, survival rates have been improving, but
15 14 Life saved by
15 because of screening how much of this improvement is attributable to
mammography mammography
10 8
treatment itself and how much to earlier diagnosis
7 7
4
6 due to screening are difficult to determine. The
5 3 2 number of women “saved” is calculated according
0 to the estimates that screening of women in their
40 50 60 40 50 60 40 50 60 40 50 60
40s reduces mortality from breast cancer by about
Years of Age at Beginning of the 10-Yr Period
20 percent and screening of women in their 50s or
Figure 2. Chances of Breast-Cancer–Related Outcomes among 1000 Women 60s reduces it by about 30 percent. It should be em-
Who Undergo Annual Mammography for 10 Years. phasized that these numbers may vary, depending
All numbers are rounded. The numbers for the incidence of invasive breast on the efficacy of mammography in reducing mor-
cancer and ductal carcinoma in situ, as well as the number of women whose tality. Individual women will interpret these num-
lives are saved by treatment (those surviving at least 20 years after the first di- bers differently depending on their own values.
agnosis of breast cancer) regardless of screening, were calculated on the ba-
To decrease the risk of false positive results, pa-
sis of data from the Surveillance, Epidemiology, and End Results program.1,57
The numbers of women whose lives are saved because of screening (those tients should be referred to experienced mammog-
surviving at least 15 years after diagnosis) were calculated on the assumption raphers with recall rates of no more than 10 percent.
of a reduction of 20 percent in mortality from breast cancer among women 40 They should be encouraged to obtain previous
to 49 years of age and a reduction of 30 percent among women 50 to 69 years mammograms for comparison and should undergo
of age; these numbers are approximate.
screening more frequently than every 18 months.
Women often are unaware of the difference be-
tween screening and diagnostic examinations to
cancer. Women should be reminded that the risk of evaluate a breast symptom or abnormal finding. In
breast cancer increases with age and that the one- one study, cancer was diagnosed in about 10 percent
in-eight risk is a lifetime risk for a newborn who of women older than 40 years of age who reported
lives for 90 years. a breast mass and in almost 5 percent of those with
The chances of being helped or harmed by any breast-related problem.59 Clinicians and wom-
screening mammography are summarized in Fig- en should not be falsely reassured by a previously
ures 1 and 2, which contain information that may normal screening mammogram in the case of a
be useful to patients. These figures show the chanc- new breast-related problem.
refer enc es
1. Ries LAG, Eisner MP, Kosary CL, et al., evaluations of communication channels for 8. Clemons M, Goss P. Estrogen and the
eds. SEER cancer statistics review, 1973- cancer-related information. J Behav Med risk of breast cancer. N Engl J Med 2001;344:
1999. Bethesda, Md.: National Cancer Insti- 1992;15:429-45. 276-85. [Erratum, N Engl J Med 2001;344:
tute, 2002. (Accessed April 1, 2003, at http: 5. Kinsinger L, Harris R, Karnitschnig J. 1804.]
//seer.cancer.gov/csr/1973_1999/.) Interest in decision-making about breast 9. Rockhill B, Spiegelman D, Byrne C,
2. Blackman DK, Bennett EM, Miller DS. cancer screening in younger women. J Gen Hunter DJ, Colditz GA. Validation of the
Trends in self-reported use of mammograms Intern Med 1998;13:Suppl:98. abstract. Gail et al. model of breast cancer risk predic-
(1989–1997) and Papanicolaou tests (1991– 6. Feuer EJ, Wun LM. DevCan: probability tion and implications for chemoprevention.
1997) — behavioral risk factor surveillance of developing or dying of cancer. 4.1. Bethes- J Natl Cancer Inst 2001;93:358-66.
system. MMWR CDC Surveill Summ 1999; da, Md.: National Cancer Institute, 1999. 10. Berry DA, Iversen ES Jr, Gudbjartsson
48(SS-6):1-22. 7. Anderson RN, DeTurk PB. United States DF, et al. BRCAPRO validation, sensitivity of
3. Preventive Services Task Force. Screen- life tables, 1999. National vital statistics re- genetic testing of BRCA1/BRCA2, and prev-
ing for breast cancer: recommendations ports. Vol. 50. No. 6. Hyattsville, Md.: Na- alence of other breast cancer susceptibility
and rationale. Ann Intern Med 2002;137: tional Center for Health Statistics, 2002. genes. J Clin Oncol 2002;20:2701-12.
344-6. (DHHS publication no. (PHS) 2002-1120 11. Fletcher SW, Black W, Harris R, Rimer
4. Johnson JD, Meishcke H. Differences in 02-0141.) BK, Shapiro S. Report of the International
1678 n engl j med 348;17 www.nejm.org april 24 , 2003
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
clinical practice
Workshop on Screening for Breast Cancer. LG. Screening mammography in communi- 40. Ernster VL, Barclay J, Kerlikowske K,
J Natl Cancer Inst 1993;85:1644-56. ty practice: positive predictive value of ab- Grady D, Henderson C. Incidence of and
12. Gotzsche PC, Olsen O. Is screening for normal findings and yield of follow-up diag- treatment for ductal carcinoma in situ of the
breast cancer with mammography justifi- nostic procedures. AJR Am J Roentgenol breast. JAMA 1996;275:913-8.
able? Lancet 2000;355:129-34. 1995;165:1373-7. 41. Ernster VL, Barclay J, Kerlikowske K,
13. Olsen O, Gotzsche PC. Cochrane review 27. Elmore JG, Barton MB, Moceri VM, Wilkie H, Ballard-Barbash R. Mortality
on screening for breast cancer with mam- Polk S, Arena PJ, Fletcher SW. Ten-year risk among women with ductal carcinoma in
mography. Lancet 2001;358:1340-2. of false positive screening mammograms situ of the breast in the population-based
14. Screening mammography re-evaluated. and clinical breast examinations. N Engl J Surveillance, Epidemiology and End Re-
Lancet 2000;355:747-8, 752. Med 1998;338:1089-96. sults program. Arch Intern Med 2000;160:
15. Screening for breast cancer with mam- 28. Barton MB, Moore SM, Polk S, Shtat- 953-8.
mography. Lancet 2001;358:2164-8. land E, Elmore JG, Fletcher SW. Increased 42. Welch HG, Black WC. Using autopsy se-
16. Nystrom L, Andersson I, Bjurstam N, patient concern after false-positive mammo- ries to estimate the disease “reservoir” for
Frisell J, Nordenskjold B, Rutqvist LE. Long- grams: clinician documentation and subse- ductal carcinoma in situ of the breast: how
term effects of mammography screening: quent ambulatory visits. J Gen Intern Med much more breast cancer can we find? Ann
updated overview of the Swedish randomised 2001;16:150-6. Intern Med 1997;127:1023-8.
trials. Lancet 2002;359:909-19. [Erratum, 29. Burman ML, Taplin SH, Herta DF, 43. Fisher B, Costantino J, Redmond C, et
Lancet 2002;360:724.] Elmore JG. Effect of false-positive mammo- al. Lumpectomy compared with lumpecto-
17. Basinski A. Commentary on “Review: grams on interval breast cancer screening in my and radiation therapy for the treatment
High-quality studies do not show reduc- a health maintenance organization. Ann In- of intraductal breast cancer. N Engl J Med
tions in breast cancer mortality for women tern Med 1999;131:1-6. 1993;328:1581-6.
screened with mammography.” ACP J Club 30. Pisano ED, Earp JA, Schell M, Vokaty K, 44. Andrews FJ. Pain during mammogra-
2000;133:67. [Comment on: Gotzsche PC, Denham A. Screening behavior of women phy: implications for breast screening pro-
Olsen O. Is screening for breast cancer with after a false-positive mammogram. Radiol- grammes. Australas Radiol 2001;45:113-7.
mammography justifiable? Lancet 2000; ogy 1998;208:245-9. 45. Kemmers-Gels ME, Groenendijk RP,
355:129-34.] 31. Lerman C, Trock B, Rimer BK, Boyce A, van den Heuvel JH, Boetes C, Peer PG,
18. The benefit of population screening for Jepson C, Engstrom PF. Psychological and Wobbes TH. Pain experienced by women at-
breast cancer with mammography. The behavioral implications of abnormal mam- tending breast cancer screening. Breast
Hague, the Netherlands: Health Council of mograms. Ann Intern Med 1991;114:657- Cancer Res Treat 2000;60:235-40.
the Netherlands, 2002. (Publication no. 61. 46. Dullum JR, Lewis EC, Mayer JA. Rates
2002/03E.) 32. Christiansen CL, Wang F, Barton MB, et and correlates of discomfort associated with
19. Miller AB, Baines CJ, To T, Wall C. Cana- al. Predicting the cumulative risk of false- mammography. Radiology 2000;214:547-
dian National Breast Screening Study. 2. positive mammograms. J Natl Cancer Inst 52.
Breast cancer detection and death rates 2000;92:1657-66. 47. Kornguth PJ, Keefe FJ, Conaway MR.
among women 50 to 59 years. CMAJ 1992; 33. Fajardo LL, Hillman BJ, Frey C. Correla- Pain during mammography: characteristics
147:1477-88. [Erratum, CMAJ 1993;148: tion between breast parenchymal patterns and relationship to demographic and medi-
718.] and mammographers’ certainty of diagno- cal variables. Pain 1996;66:187-94.
20. Vainio H, Bianchini F. Breast cancer sis. Invest Radiol 1988;23:505-8. 48. Rutter DR, Calnan M, Vaile MS, Field S,
screening. Lyons, France: IARC Press, 2002. 34. Laya MB, Gallagher JC, Schreiman JS, Wade KA. Discomfort and pain during mam-
21. Breast cancer screening for women ages Larson EB, Watson P, Weinstein L. Effect of mography: description, prediction, and pre-
40-49. Vol. 15. No. 1. Bethesda, Md.: Na- postmenopausal hormonal replacement vention. BMJ 1992;305:443-5.
tional Institutes of Health Consensus Devel- therapy on mammographic density and pa- 49. Feig SA. Assessment of radiation risk
opment Program, 1997. (Accessed April 1, renchymal pattern. Radiology 1995;196: from screening mammography. Cancer
2003, at http://consensus.nih.gov/cons/103/ 433-7. 1996;77:818-22.
103_intro.htm.) 35. Laya MB, Larson EB, Taplin SH, White 50. Ma L, Fishell EK, Wright B, Hanna W,
22. Berry DA. Benefits and risks of screen- E. Effect of estrogen replacement therapy on Allan S, Boyd NF. Case-control study of fac-
ing mammography for women in their for- the specificity and sensitivity of screening tors associated with failure to detect breast
ties: a statistical appraisal. J Natl Cancer Inst mammography. J Natl Cancer Inst 1996;88: cancer by mammography. J Natl Cancer Inst
1998;90:1431-9. 643-9. 1992;84:781-5.
23. Breast Cancer (PDQ): screening. Be- 36. White E, Velentgas P, Mandelson MT, et 51. Holland R, Hendriks JH, Mravunac M.
thesda, Md.: National Cancer Institute, al. Variation in mammographic breast den- Mammographically occult breast cancer: a
2003. (Accessed April 1, 2003, at http:// sity by time in menstrual cycle among wom- pathologic and radiologic study. Cancer
www.cancer.gov/cancerinfo/pdq/screening/ en aged 40-49 years. J Natl Cancer Inst 1998; 1983;52:1810-9.
breast/.) 90:906-10. 52. Kerlikowske K, Grady D, Barclay J, Sick-
24. Fletcher SW. Breast cancer screening 37. Harvey JA, Pinkerton JV, Herman CR. les EA, Ernster V. Effect of age, breast densi-
among women in their forties: an overview Short-term cessation of hormone replace- ty, and family history on the sensitivity of
of the issues. In: National Institutes of Health ment therapy and improvement of mammo- first screening mammography. JAMA 1996;
Consensus Conference on breast cancer graphic specificity. J Natl Cancer Inst 1997; 276:33-8.
screening for women ages 40–49. Journal of 89:1623-5. 53. Black WC, Nease RF Jr, Tosteson ANA.
the National Cancer Institute Monographs. 38. Bassett LW, Hendrick RE, Bassford TL, Perceptions of breast cancer risk and screen-
No. 22. Bethesda, Md.: National Cancer In- et al. Quality determinants of mammogra- ing effectiveness in women younger than 50
stitute, 1997;22:5-9. phy. Clinical practice guideline. No. 13. years of age. J Natl Cancer Inst 1995;87:720-
25. van Dijck JA, Verbeek AL, Beex L, et al. Rockville, Md.: Agency for Health Care Pol- 31.
Mammographic screening after the age of icy and Research, October 1994. (AHCPR 54. Edwards A, Elwyn G, Mulley A. Explain-
65 years: evidence for a reduction in breast publication no. 95-0632.) ing risks: turning numerical data into mean-
cancer mortality. Int J Cancer 1996;66:727- 39. Breast cancer study. Washington, D.C.: ingful pictures. BMJ 2002;324:827-30.
31. Physician Insurers Association of America, 55. Statement of the American Society of
26. Brown ML, Houn F, Sickles EA, Kessler June 1995. Clinical Oncology: genetic testing for cancer
n engl j med 348;17 www.nejm.org april 24, 2003 1679
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
clinical practice
susceptibility, adopted on February 20, 1996. Md.: National Cancer Institute, 1997. (NIH Breast symptoms among women enrolled in
J Clin Oncol 1996;14:1730-6. publication no. 97-2789.) a health maintenance organization: fre-
56. BRCA1 genetic screening. Guideline 58. Silverman E, Woloshin S, Schwartz LM, quency, evaluation, and outcome. Ann In-
NGC-0461. Rockville, Md.: Kaiser Perma- Byram SJ, Welch HG, Fischhoff B. Women’s tern Med 1999;130:651-7.
nente, 1998. views on breast cancer risk and screening Copyright © 2003 Massachusetts Medical Society.
57. Ries LAG, Kosary CL, Hankey BF, Miller mammography: a qualitative interview study.
BA, Harras A, Edwards BK, eds. SEER can- Med Decis Making 2001;21:231-40.
cer statistics review, 1973-1994. Bethesda, 59. Barton MB, Elmore JG, Fletcher SW.
1680 n engl j med 348;17 www.nejm.org april 24, 2003
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
New England Journal of Medicine
CORRECTION ever, the rate of death due to breast cancer, as a percentage of the
rate of death from any cause, is highest among women in their 40s.
Mammographic Screening for Breast Cancer A reduction in mortality of 20 percent among women in their 40s is
a low estimate. The Gothenberg Breast Cancer Screening Trial,1 the
To the Editor: I was troubled by the lack of a cost–benefit analysis in Malmö Mammographic Screening Program,2 and the Swedish trials3
the article by Fletcher and Elmore on the effectiveness of mammog- showed statistically significant reductions in mortality of 44 percent,
raphy for screening for breast cancer (April 24 issue).1 In fairness, 35 percent, and 29 percent, respectively, among women younger than
their recommendations are more fiscally conservative than those of 50 years of age. Furthermore, because of noncompliance and con-
the U.S. Preventive Services Task Force. Still, their omission of any tamination, the trials underestimate the benefit. Women need to be
discussion of relative costs and benefits gives the implicit message provided with all the data in order to make informed decisions. The
that cost does not matter. concerns raised by Gøtzsche and Olsen were either unwarranted or
of no consequence,4 and the trial data remain valid.
William A. Hensel, M.D.
Moses Cone Health System Daniel B. Kopans, M.D.
Greensboro, NC 27401 Harvard Medical School
bill.hensel@mosescone.com Boston, MA 02115
References References
1. Fletcher SW, Elmore JG. Mammographic screening for breast
1. Bjurstam N, Björneld L, Duffy SW, et al. The Gothenberg Breast
cancer. N Engl J Med 2003;348:1672-1680.
Cancer Screening Trial: preliminary results on breast cancer mor-
tality for women ages 39–49. In: National Institutes of Health con-
To the Editor: The article by Fletcher and Elmore on mammographic
sensus conference on breast cancer screening for women ages
screening is potentially misleading because it lumps ``recalls´´ to-
40–49. Journal of the National Cancer Institute monographs. No.
gether with false positive mammograms (Figure 1 of their article). A
22. Bethesda, Md.: National Cancer Institute, 1997:53-5.
false positive mammogram refers to an interpretation of a screening
mammogram as abnormal in a case in which there is no accompany- 2. Andersson I, Janzon L. Reduced breast cancer mortality in women
ing diagnosis of cancer.1 A recall occurs when a screening mammo- under 50: update from the Malmö Mammographic Screening Pro-
gram demonstrates an area of potential concern necessitating addi- gram. In: National Institutes of Health consensus conference on
tional mammographic views for clarification. An interpretation is not breast cancer screening for women ages 40–49. Journal of the
rendered until these additional views are obtained. A recall is there- National Cancer Institute monographs. No. 22. Bethesda, Md.:
fore distinct from a false positive mammogram. National Cancer Institute, 1997:63-7.
This point is more than one of simple semantics. If the distinction be-
3. Hendrick RE, Smith RA, Rutledge JH III, Smart CR. Benefit of
tween recalls and false positive interpretations is blurred, the negative
screening mammography in women ages 40–49: a new meta-
effect of mammography is amplified. Such an analysis creates a sub-
analysis of randomized controlled trials. In: National Institutes
tle bias against mammography, which could be mitigated by careful
of Health consensus conference on breast cancer screening for
adherence to these definitions.
women ages 40–49. Journal of the National Cancer Institute
Michael J. Fishbein, M.D. monographs. No. 22. Bethesda, Md.: National Cancer Institute,
Falmouth Hospital 1997:87-92.
Falmouth, MA 02540
mjf@massmed.org 4. Kopans DB. The most recent breast cancer screening contro-
versy about whether mammographic screening benefits women
at any age: nonsense and nonscience. AJR Am J Roentgenol
References
2003;180:21-26.
1. Sickles EA, Ominsky SH, Sollitto RA, Galvin HB, Monticciolo
DL. Medical audit of a rapid-throughput mammography screening To the Editor: Figure 2 in the article by Fletcher and Elmore misleads
practice: methodology and results of 27,114 examinations. Radi- the reader by exaggerating the number of lives saved by mammog-
ology 1990;175:323-327. raphy by a factor of 5 to 10. First, the authors assume a 30 percent
reduction in mortality among women 50 to 69 years of age. The lat-
To the Editor: The tone of the article by Fletcher and Elmore suggests est meta-analysis estimates that the reduction is 16 percent.1 Second,
that screening women in their 40s is still of questionable value. How- the authors apply this 30 percent reduction in relative risk to the rate of
N Engl J Med 2003;349:610
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
New England Journal of Medicine
death due to breast cancer calculated on the basis of a screened pop- cancer with mammography. Lancet 2001;358:1340-1342.
ulation rather than a control population, thus compounding the error.
They estimate that four lives are saved by screening 1000 women 50 2. Gøtzsche PC. Screening for breast cancer with mammography.
to 60 years of age for 10 years and that six lives are saved by similar Lancet 2001;358:2167-2168.
screening among women 60 to 70 years of age. In reality, the number
3. Gøtzsche PC. Update on effects of screening mammography.
needed to screen is 1224 to save 1 life over a 14-year period1 (ap-
Lancet 2002;360:338-338.
proximately 1713, over a 10-year period); in other words, 5.8 lives will
be saved per 10,000 women screened, not 4 or 6 per 1000 screened
4. Shapiro S. Discussion II. In: Selection, follow-up, and analysis in
— almost a case of the missing zero. Among women younger than 50
prospective studies: a workshop. National Cancer Institute mono-
years of age, the number needed to screen is approximately 2508 —
graph 67. Bethesda, Md.: National Cancer Institute, May 1985:75-
that is, over a 10-year period, 4 lives will be saved per 10,000 women
9. (NIH publication no. 85-2713.)
screened, not 20 per 10,000, as estimated by the authors.
Jayant S. Vaidya, M.B., B.S., Ph.D.
The authors reply: We strongly agree with Dr. Hensel regarding the
Michael Baum, M.D.
importance of cost effectiveness. However, as we point out in our ar-
University College London
ticle, information about cost effectiveness is especially important for
London W1W 7EJ, United Kingdom
policymakers and payers when they are making decisions about the
j.vaidya@ucl.ac.uk
allocation of finite resources. The key issues for clinical practice are
the underlying risk of the condition being screened for, the effective-
References ness of screening in the prevention of major untoward outcomes such
as death, and the hazards associated with the screening procedure,
1. Humphrey LL, Helfand M, Chan BKS, Woolf SH. Breast cancer such as false positive results.
screening: a summary of the evidence for the U.S. Preventive Ser-
Dr. Fishbein’s concern about differentiating between recalls and false
vices Task Force. Ann Intern Med 2002;137:347-360.
positive mammograms is understandable. The recall rate (which we
defined as the percentage of mammograms that result in recommen-
To the Editor: Fletcher and Elmore’s account of the issues is not bal-
dations for further testing) includes both false positive and true posi-
anced. They describe a number of criticisms of our work that have
tive mammograms, but because most positive mammograms are false
been raised and — conversely — contend that all the criticisms of
positives, lowering the recall rate would most likely reduce the risk of
the mammography trials we raised have been answered, apart from
false positive mammograms; this is important, because many studies
those of one trial (in Edinburgh, Scotland) that was excluded from our
have shown that false positive mammograms make women anxious.1
meta-analysis.
Mammographers have a difficult task: they must not miss cancers, but
First, the criticisms Fletcher and Elmore mention concern our first ar- they must also not recall too many women.
ticle in the Lancet, which were answered in our Cochrane Review and
Dr. Kopans is concerned that the 20 percent reduction in the rate of
in our second Lancet article.1 Second, the most important criticisms
2,3
death due to breast cancer that we used to calculate the number of
we raised against the trials remain unanswered : the biased mis-
women in their 40s whose lives would be saved by regular mammo-
classification of the cause of death, discrepancies in numbers in the
graphic screening is too low, and Drs. Vaidya and Baum think our
analyses of the Swedish trials, and differential exclusions from analy-
estimates are too high. Estimates differ mainly according to which tri-
sis of women with breast cancer before randomization. For example,
als are included in a given analysis. Whatever the estimate, Figure 2
Fletcher and Elmore indicate that there was no problem with exclu-
of our article makes it possible to translate the relative effect into abso-
sions in the New York trial, but the trial’s lead investigator admitted
lute numbers. For example, we estimated that 2 of 1000 women who
that even in 1985, more than 20 years after the study started, the in-
regularly underwent mammography during their 40s might owe their
vestigators were unaware of some previous cases of breast cancer in
lives to mammography. If mortality due to breast cancer is reduced by
controls, who should have been excluded.4
40 percent, the number would be about four.
Peter C. Gøtzsche, M.D.
In addition, Vaidya and Baum are concerned that we missed a zero in
Nordic Cochrane Centre
our calculations. They are mistaken, since the numbers in the figure
2100 Copenhagen, Denmark
are based on 10,000 mammograms. Because mammography is rec-
pcg@cochrane.dk
ommended repeatedly, we chose to demonstrate the effect of 10,000
mammograms in 1000 women tested annually for 10 years, rather
References than that of 10,000 mammograms in 10,000 women tested once each.
We also included many other effects of a program of regular screening
1. Olsen O, Gøtzsche PC. Cochrane Review on screening for breast mammography.
N Engl J Med 2003;349:610
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
New England Journal of Medicine
We made a list of Dr. Gøtzsche’s concerns about the randomized
trials, along with responses we found, and presented them in a table
in a supplementary appendix on the Journal’s Web site (available with
the full text of our article at http://www.nejm.org). Interested readers
can review the list there.
Finally, we wish to point out an error in our article. The statement (be-
ginning on the last line of page 1674) that ``obtaining mammograms
during the luteal phase of the menstrual cycle may decrease mammo-
graphic density´´ should have read ``obtaining mammograms during
the luteal phase of the menstrual cycle may decrease mammographic
sensitivity.´´
Suzanne W. Fletcher, M.D.
Harvard Medical School
Boston, MA 02115
Joann G. Elmore, M.D., M.P.H.
University of Washington
Seattle, WA 98104
References
1. Vainio H, Bianchini F. Breast cancer screening. Lyons, France:
IARC Press, 2002.
N Engl J Med 2003;349:610
Downloaded from www.nejm.org at TATA MEMORIAL HOSPITAL on June 16, 2009 .
Copyright © 2003 Massachusetts Medical Society. All rights reserved.
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- DragonDreaming International Ebook v02.03-2Document28 pagesDragonDreaming International Ebook v02.03-2Tim LueschenNo ratings yet
- Obstructive Sleep Aponea SurgeriesDocument638 pagesObstructive Sleep Aponea Surgerieswillyoueverlovemenk100% (2)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Distinguish Opinion From TruthDocument12 pagesDistinguish Opinion From TruthMAR ANTERO R. CENIZA100% (2)
- Adolescent HealthDocument19 pagesAdolescent Healthhou1212!67% (3)
- Seismic Aspects of Dam Design PDFDocument12 pagesSeismic Aspects of Dam Design PDFAlokNo ratings yet
- Pediatric Sinusitis and Sinus SurgeryDocument293 pagesPediatric Sinusitis and Sinus SurgerywillyoueverlovemenkNo ratings yet
- DualSPHysics v4.0 GUIDE PDFDocument140 pagesDualSPHysics v4.0 GUIDE PDFFelipe A Maldonado GNo ratings yet
- Changes between the 6th and 7th editions of the TNM Classification of Malignant TumoursDocument46 pagesChanges between the 6th and 7th editions of the TNM Classification of Malignant TumoursKen HidakaNo ratings yet
- Nbde ReleasedDocument4 pagesNbde ReleasedwillyoueverlovemenkNo ratings yet
- 5J - Tongue FlapDocument11 pages5J - Tongue FlapwillyoueverlovemenkNo ratings yet
- 5A - Median Forhead FlapDocument12 pages5A - Median Forhead FlapwillyoueverlovemenkNo ratings yet
- 5G - Sternocleidomastoid FlapDocument11 pages5G - Sternocleidomastoid FlapwillyoueverlovemenkNo ratings yet
- 5I - Temporalis Muscle FlapDocument12 pages5I - Temporalis Muscle Flapwillyoueverlovemenk100% (1)
- 02 - The Reconstruction TriangleDocument28 pages02 - The Reconstruction TrianglewillyoueverlovemenkNo ratings yet
- Voice Disorders and Their Management, Third Edition: Margaret Freeman Margaret Fawcus, EditorsDocument1 pageVoice Disorders and Their Management, Third Edition: Margaret Freeman Margaret Fawcus, EditorswillyoueverlovemenkNo ratings yet
- 5B - Standard Forehead FlapDocument18 pages5B - Standard Forehead Flapwillyoueverlovemenk100% (1)
- 5D - Orbicularis Oris FlapDocument20 pages5D - Orbicularis Oris FlapwillyoueverlovemenkNo ratings yet
- General Principles: BasicDocument3 pagesGeneral Principles: BasicwillyoueverlovemenkNo ratings yet
- Salivary Glands: Fig. 11.1 Histologic Structure of The Normal Salivary GlandDocument35 pagesSalivary Glands: Fig. 11.1 Histologic Structure of The Normal Salivary GlandwillyoueverlovemenkNo ratings yet
- Head and Neck Soft Tissue Tumor Diagnosis and TreatmentDocument37 pagesHead and Neck Soft Tissue Tumor Diagnosis and TreatmentwillyoueverlovemenkNo ratings yet
- Neurogenic Tumors and Paragangliomas: BenignDocument36 pagesNeurogenic Tumors and Paragangliomas: BenignwillyoueverlovemenkNo ratings yet
- Salivary Glands: Fig. 11.1 Histologic Structure of The Normal Salivary GlandDocument35 pagesSalivary Glands: Fig. 11.1 Histologic Structure of The Normal Salivary GlandwillyoueverlovemenkNo ratings yet
- Chap 14Document40 pagesChap 14willyoueverlovemenkNo ratings yet
- Oral Cavity and Oropharynx CancersDocument61 pagesOral Cavity and Oropharynx CancerswillyoueverlovemenkNo ratings yet
- Thyroid and Parathyroid Glands AnatomyDocument43 pagesThyroid and Parathyroid Glands AnatomywillyoueverlovemenkNo ratings yet
- Chap 8Document86 pagesChap 8willyoueverlovemenkNo ratings yet
- Neurogenic Tumors and Paragangliomas: BenignDocument36 pagesNeurogenic Tumors and Paragangliomas: BenignwillyoueverlovemenkNo ratings yet
- The Lips: Fig. 5.1 Site and Gender Distribution: Squamous Cell Carcinoma of TheDocument24 pagesThe Lips: Fig. 5.1 Site and Gender Distribution: Squamous Cell Carcinoma of ThewillyoueverlovemenkNo ratings yet
- Cervical Lymph NodesDocument41 pagesCervical Lymph NodeswillyoueverlovemenkNo ratings yet
- Oral Cavity and Oropharynx CancersDocument61 pagesOral Cavity and Oropharynx CancerswillyoueverlovemenkNo ratings yet
- Head and Neck Soft Tissue Tumor Diagnosis and TreatmentDocument37 pagesHead and Neck Soft Tissue Tumor Diagnosis and TreatmentwillyoueverlovemenkNo ratings yet
- The Skull BaseDocument56 pagesThe Skull BasewillyoueverlovemenkNo ratings yet
- Nasal Cavity and Paranasal Sinuses: Fig. 3.1 The Anatomic Location of The Paranasal SinusesDocument35 pagesNasal Cavity and Paranasal Sinuses: Fig. 3.1 The Anatomic Location of The Paranasal SinuseswillyoueverlovemenkNo ratings yet
- Chap2 PDFDocument20 pagesChap2 PDFwillyoueverlovemenkNo ratings yet
- The Scalp and Skin of The FaceDocument31 pagesThe Scalp and Skin of The FacewillyoueverlovemenkNo ratings yet
- Zimbabwean Indigenous Languages Syllabus: Form 1 - 4Document46 pagesZimbabwean Indigenous Languages Syllabus: Form 1 - 4Takudzwa ZengeraniNo ratings yet
- Eq 1Document4 pagesEq 1jppblckmnNo ratings yet
- French demonstrative pronouns guideDocument8 pagesFrench demonstrative pronouns guidedfñoiiuglkjs.No ratings yet
- 15 Tips To Get Fair Skin Naturally PDFDocument2 pages15 Tips To Get Fair Skin Naturally PDFLatha SivakumarNo ratings yet
- Edgar Allan Poe's "The RavenDocument3 pagesEdgar Allan Poe's "The RavenЖанна ФодееваNo ratings yet
- Crane's Manual - CV ValuesDocument14 pagesCrane's Manual - CV Valuesnghiemta18No ratings yet
- Chapter 8Document3 pagesChapter 8sasafoadjeiNo ratings yet
- Philippians 1:27-2:18Document3 pagesPhilippians 1:27-2:18Buddy OvermanNo ratings yet
- LESSON 1 Definition and Functions of ManagementDocument2 pagesLESSON 1 Definition and Functions of ManagementJia SorianoNo ratings yet
- LP Direct & Indirect SpeechDocument7 pagesLP Direct & Indirect SpeechJoana JoaquinNo ratings yet
- 1st Part PALIAL CasesDocument255 pages1st Part PALIAL CasesAnonymous 4WA9UcnU2XNo ratings yet
- Agenda For Regular Board Meeting February 18, 2022 Western Visayas Cacao Agriculture CooperativeDocument2 pagesAgenda For Regular Board Meeting February 18, 2022 Western Visayas Cacao Agriculture CooperativeGem Bhrian IgnacioNo ratings yet
- Chong Co Thai Restaurant LocationsDocument19 pagesChong Co Thai Restaurant LocationsrajragavendraNo ratings yet
- Reading at the BeachDocument3 pagesReading at the BeachhihiijklkoNo ratings yet
- 1.7 The Lagrangian DerivativeDocument6 pages1.7 The Lagrangian DerivativedaskhagoNo ratings yet
- Data Structures Assignment 2: (Backtracking Using Stack)Document4 pagesData Structures Assignment 2: (Backtracking Using Stack)Sai CharanNo ratings yet
- Executive Summary WynnDocument5 pagesExecutive Summary Wynnapi-505730347No ratings yet
- Vector DifferentiationDocument2 pagesVector DifferentiationJayashree MisalNo ratings yet
- TEACHING AS A NOBLE PROFESSIONDocument6 pagesTEACHING AS A NOBLE PROFESSIONShaiNo ratings yet
- 11th Commerce Mathematics and Statistics Part II Maharashtra BoardDocument10 pages11th Commerce Mathematics and Statistics Part II Maharashtra BoardTanmay Gholap100% (3)
- Pilar Fradin ResumeDocument3 pagesPilar Fradin Resumeapi-307965130No ratings yet
- Development Through The Lifespan Test 1Document3 pagesDevelopment Through The Lifespan Test 1Alexandra CastroNo ratings yet
- Mughals in IndiaDocument4 pagesMughals in IndiaSalony RoongtaNo ratings yet
- New Dll-Math Week 4-1Document3 pagesNew Dll-Math Week 4-1AstroNo ratings yet