Professional Documents
Culture Documents
Arterial Line Waveform Interpretation UHL Childrens Intensive Care Guideline
Uploaded by
DhonyOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Arterial Line Waveform Interpretation UHL Childrens Intensive Care Guideline
Uploaded by
DhonyCopyright:
Available Formats
Arterial Line Waveform
Interpretation PICU CPM
October 2014
1. Introduction
The document is primarily aimed at education to provide some basic understanding of arterial line wave form
2. Scope
The interpretation of arterial traces requires experience and should not be considered in isolation. i.e. The
patient needs to be examined and if in doubt discussed with the Duty Intensivist
3. Index
Page 1 Introduction Scope Index
Page 2 Normal trace variation Dampened trace Hyperactive trace Arterial line swing
Page 3 Relationship of Contraction, Anacrotic Limb
Valves and Pressure
Page 4 Dicrotic Limb
Page 5 Legal Liability Statement
Arterial Line Waveform Interpretation Page 1 of 5
Author: James Whitelaw Written: Oct2014 Last Reviewed Nov 2017
Final Version Approved by Paediatric Clinical Practice Board on Next Review: November 2020
Trust Ref: C109/2016
NB: Paper copies of this document may not be most recent version. The definitive version is held on INsite Documents
Normal trace variation Ascending Aorta
114
Mean 93
The diagram to the right shows the variation that occurs 83
in different arterys.
This is related to turbulent flow. Note that although there
Pressure (mmHg)
Abdominal Aorta 119
can be large variations between the sytolic and diastolic Mean 92
79
pressure the mean stays stable.
Radial Artery
126
Mean 89
71
Dampened Trace
• Air Bubles
• Catheter Kinks
• Clots
• Injection Ports
• Low Flush Bag Pressure Or No Fluid In The Flush Bag
• Overly Compliant, Distensible Tubing
This type of trace UNDERESTIMATES blood pressure.
Hyperactive Trace
• Long tubing
• Overly stiff, non-compliant tubing
• Increased vascular resistance
• Reverberations in tubing causing harmonics that
distort the trace (i.E. High systolic and low diastolic)
• Non-fully opened stopcock valve
This type of trace OVERESTIMATES blood pressure.
Arterial Line Swing
Reduction in Venous return
Dehydration - check CVP and Capillary Refil
Asthma or Hyperexpansion of the Lungs (Pulsus
Paradoxus)
Pneumothorax or Pleural effusions
Pericardial effusions
Arterial Line Waveform Interpretation Page 2 of 5
Author: James Whitelaw Written: Oct2014 Last Reviewed Nov 2017
Final Version Approved by Paediatric Clinical Practice Board on Next Review: November 2020
Trust Ref: C109/2016
NB: Paper copies of this document may not be most recent version. The definitive version is held on INsite Documents
Relationship of Contraction, Valves and Pressure
Anacrotic Limb
Represents Tf to T2 (the shaded area of the diagram)
It occurs as the ventricles eject the blood into the arterial tree and gives a visual record
of the arterial pressure rising to that of the end systole.
The steepness of the ascending phase can
be affected by:-
• Heart rate,
• Increased systemic vascular resistance
(more steep incline)
ͦͦ Cooling
ͦͦ Vasopressors such as
noradrenaline
• Decreased systemic vascular
resistance(less steep incline)
ͦͦ Septic shock
ͦͦ Vasodilators - Milrinone,
GTN, Dobutamine.
Myocardial contractility also effects the
steepness of the anacrotic limb – during
impaired contractility (post bypass) the up-
Arterial Line Waveform Interpretation Page 3 of 5
Author: James Whitelaw Written: Oct2014 Last Reviewed Nov 2017
Final Version Approved by Paediatric Clinical Practice Board on Next Review: November 2020
Trust Ref: C109/2016
NB: Paper copies of this document may not be most recent version. The definitive version is held on INsite Documents
sweep, or the rate of pressure increase can be prolonged.
As the pressure reaches maximum, and the wave makes sharp turn to level off, this is
called the anacrotic notch (T1)
Dicrotic Limb
T2 to Tf
The rate of dicrotic ‘fall-off’, or the rate at
which the arterial line trace falls from end-
systole to early-diastole changes in relation
to systemic vascular resistance.
In patients with a severely reduced arteriolar
resistance, fall-off time is rapid. This occurs
as soon as end-systole finishes due to the
greatly reduced pressure in the arterial
tree (representing reduced afterload, i.e.
systemic to pulmonary shunts). The arterial
waveform in this clinical state looks thin and
pointed (don’t confuse this with resonance).
In patients with increased vascular
resistance, such as main vessel stenosis for
example, the dicrotic fall-off time is greatly
increased. This occurs due to the length of
time it takes to return to end-diastolic pressure. The arterial waveform in this clinical state
may be normal, or quite fat!
Dicrotic means ‘twice beating’ – meaning that this phase of the arterial pressure pulse
should have a second, smaller wave, known as the dicrotic notch. This can occur at any
point that there is a fluctuation in pressure during the descending arterial limb. The most
common time for this to occur is when the aortic and pulmonary valves snap shut causing
pressure reverberations through the arterial system
Flat or non-existent notch can mean that the patient is dehydrated (line trace will also
‘swing’)
Low notch can also mean high pulse pressure (due to the low diastole in septic shock for
example)
Flattened notch can be present in cardiopulmonary valve insufficiency
Arterial Line Waveform Interpretation Page 4 of 5
Author: James Whitelaw Written: Oct2014 Last Reviewed Nov 2017
Final Version Approved by Paediatric Clinical Practice Board on Next Review: November 2020
Trust Ref: C109/2016
NB: Paper copies of this document may not be most recent version. The definitive version is held on INsite Documents
4. Legal Liability Statement
Guidelines or Procedures issued and approved by the Trust are considered to represent best practice.
Staff may only exceptionally depart from any relevant Trust guidelines or Procedures and always only
providing that such departure is confined to the specific needs of individual circumstances. In healthcare
delivery such departure shall only be undertaken where, in the judgement of the responsible healthcare
professional’ it is fully appropriate and justifiable - such decision to be fully recorded in the patient’s
notes
Arterial Line Waveform Interpretation Page 5 of 5
Author: James Whitelaw Written: Oct2014 Last Reviewed Nov 2017
Final Version Approved by Paediatric Clinical Practice Board on Next Review: November 2020
Trust Ref: C109/2016
NB: Paper copies of this document may not be most recent version. The definitive version is held on INsite Documents
You might also like
- Graphic Anaesthesia, second edition: Essential diagrams, equations and tables for anaesthesiaFrom EverandGraphic Anaesthesia, second edition: Essential diagrams, equations and tables for anaesthesiaNo ratings yet
- 1) Vasoplegia During Cardiac Surgery Current Concepts and Management 2010Document5 pages1) Vasoplegia During Cardiac Surgery Current Concepts and Management 2010Carolina QuirogaNo ratings yet
- Technique For Awake Fibre Optic IntubationDocument3 pagesTechnique For Awake Fibre Optic Intubationmonir61No ratings yet
- Extubation After AnaesthesiaDocument7 pagesExtubation After AnaesthesiaaksinuNo ratings yet
- Fluid Resuscitation - Dita AditianingsihDocument48 pagesFluid Resuscitation - Dita AditianingsihGalih Wicaksono100% (1)
- FCA 2 Trials MindmapDocument1 pageFCA 2 Trials MindmapameenallyNo ratings yet
- Advance in Haemodynamic Monitoring CompressedDocument66 pagesAdvance in Haemodynamic Monitoring Compressedmeta ikaNo ratings yet
- ICU One Pager EVD V11Document1 pageICU One Pager EVD V11Mohamed Mahmoud100% (1)
- Anesthetic Consideration in Hypertensive PatientDocument11 pagesAnesthetic Consideration in Hypertensive PatientYosiAsmaraNo ratings yet
- Anaesthesia For Trauma PatientsDocument5 pagesAnaesthesia For Trauma Patientscahya candraNo ratings yet
- Journal ClubDocument26 pagesJournal Clubysindhura23gmailcom100% (1)
- Monitoring in Critical CareDocument10 pagesMonitoring in Critical CareYohanes NugrohoNo ratings yet
- Abg PrimerDocument22 pagesAbg PrimerAraceli Ecot CalunodNo ratings yet
- Module 9 Mechanical Ventilation PDFDocument46 pagesModule 9 Mechanical Ventilation PDFChabboo SutabrataNo ratings yet
- PAC and Hemodynamic Monitoring 2-4-08Document32 pagesPAC and Hemodynamic Monitoring 2-4-08anum786110No ratings yet
- Cardiac AnesthesiologyDocument48 pagesCardiac AnesthesiologyNiaNo ratings yet
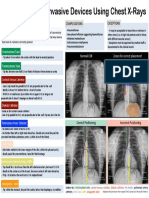
- Invasive Devices On CXRDocument1 pageInvasive Devices On CXRLaurensia Erlina NataliaNo ratings yet
- Oxygen Delivery in Septic ShockDocument4 pagesOxygen Delivery in Septic ShockKarimah NasarNo ratings yet
- Kuliah Ekg UnswagatiDocument75 pagesKuliah Ekg UnswagatiiikNo ratings yet
- Update EmergenciesDocument84 pagesUpdate EmergenciesElaineNo ratings yet
- Antrim ED Handbook 2019Document238 pagesAntrim ED Handbook 2019Chris Jardine LiNo ratings yet
- Conduct of AnaesthesiaDocument30 pagesConduct of AnaesthesiaAnirban PalNo ratings yet
- SRNA Orientation ChecklistDocument40 pagesSRNA Orientation Checklistihtisham1No ratings yet
- Regional Anesthesia - FinalDocument46 pagesRegional Anesthesia - Finalvan016_bunnyNo ratings yet
- Ventricular Assist DeviceDocument12 pagesVentricular Assist DevicesamadonyNo ratings yet
- Anaesthesiology ProspectusDocument60 pagesAnaesthesiology ProspectusShamalka DahanayakeNo ratings yet
- Cardiac/Cardiogenic Shock: Clinical Practice GuidelinesDocument3 pagesCardiac/Cardiogenic Shock: Clinical Practice GuidelinesAnonymous Yo0mStNo ratings yet
- Awareness Under AnesthesiaDocument27 pagesAwareness Under AnesthesiaagatakassaNo ratings yet
- ELSO Guidelines General All ECLS Version1.1 PDFDocument24 pagesELSO Guidelines General All ECLS Version1.1 PDFBranka KurtovicNo ratings yet
- Should We Use Driving Pressure To Set Tidal Volume? PDFDocument7 pagesShould We Use Driving Pressure To Set Tidal Volume? PDFYaxkin NikNo ratings yet
- Intravenous Anesthetic AgentsDocument23 pagesIntravenous Anesthetic Agentsdrhiwaomer100% (7)
- Recruitment Maneuvers and PEEP TitrationDocument17 pagesRecruitment Maneuvers and PEEP TitrationDiego Cruces OrdoñezNo ratings yet
- Ventilator Grafik WeaponDocument6 pagesVentilator Grafik WeaponiqbalNo ratings yet
- Plante PacemakersDocument57 pagesPlante Pacemakersdragon66100% (1)
- Perioperative ManagementDocument3 pagesPerioperative ManagementRaymond De GulaNo ratings yet
- Anesthesia For GeriatricDocument21 pagesAnesthesia For GeriatricintanNo ratings yet
- FCA (SA) Portfolio 7-5-2013Document39 pagesFCA (SA) Portfolio 7-5-2013matentenNo ratings yet
- Sedation in ICUDocument14 pagesSedation in ICUIhtesham Ul HaqNo ratings yet
- MainOR SyllabusDocument208 pagesMainOR Syllabuster100% (1)
- CCPACatheter Basics 07 MedicineDocument44 pagesCCPACatheter Basics 07 MedicinerinbijoyNo ratings yet
- Oliguria 6oct2010 FinalDocument75 pagesOliguria 6oct2010 Finalsallam8008No ratings yet
- Paediatric Anaesthesia PDFDocument33 pagesPaediatric Anaesthesia PDFMarcelitaTaliaDuwiriNo ratings yet
- 9 - Role of Non InvasiveDocument46 pages9 - Role of Non InvasiveHavara Kausar AkbarNo ratings yet
- Stoelting Anasthesia and Co Existing Disease PDFDocument28 pagesStoelting Anasthesia and Co Existing Disease PDFEgidia SetyaNo ratings yet
- Color Code Anesthesia PDFDocument6 pagesColor Code Anesthesia PDFYusnia Gulfa MaharaniNo ratings yet
- FINAL CA-1 Tutorial Textbook 2017Document74 pagesFINAL CA-1 Tutorial Textbook 2017Farjad IkramNo ratings yet
- Evidence-Based Obstetric AnesthesiaFrom EverandEvidence-Based Obstetric AnesthesiaStephen H. HalpernNo ratings yet
- Hemodynamic Drug InfusionsDocument45 pagesHemodynamic Drug InfusionsDawit MucheNo ratings yet
- Pitfalls in Anesthesia MonitoringDocument56 pagesPitfalls in Anesthesia MonitoringDr.Sandeep Kumar Kar100% (1)
- A Review of Neuromuscular MonitoringDocument10 pagesA Review of Neuromuscular Monitoringdrcds99No ratings yet
- Ecmo and SepsisDocument37 pagesEcmo and SepsisMarckus BrodyNo ratings yet
- ICU One Pager NIPPVDocument1 pageICU One Pager NIPPVNicholas HelmstetterNo ratings yet
- OB1 Lec - AnalgesiaDocument3 pagesOB1 Lec - Analgesiaapi-3700579No ratings yet
- Transportation and Stabilitation in Critically Ill Patient - 2015Document36 pagesTransportation and Stabilitation in Critically Ill Patient - 2015Gustav Valentino100% (1)
- General-Anesthesia Part 4Document5 pagesGeneral-Anesthesia Part 4Dianne GalangNo ratings yet
- Ventilator Weaning and Spontaneous Breathing Trials An Educational Review 2016Document7 pagesVentilator Weaning and Spontaneous Breathing Trials An Educational Review 2016Tarran PhagooNo ratings yet
- Anesthesia For Tracheoesophageal Fistula RepairDocument29 pagesAnesthesia For Tracheoesophageal Fistula RepairArop AkechNo ratings yet
- Assessment Algorithm For Sedated Adult ICU Patients: No YesDocument18 pagesAssessment Algorithm For Sedated Adult ICU Patients: No YeshendraNo ratings yet
- Hemodynamics For The Bedside Nurse 1CEUDocument7 pagesHemodynamics For The Bedside Nurse 1CEURN333100% (1)
- Q Bank Physio 30Document30 pagesQ Bank Physio 30haleemeltayebNo ratings yet
- LAB SEVEN Homeostasis and ExerciseDocument6 pagesLAB SEVEN Homeostasis and ExerciseSonia SunnyNo ratings yet
- Pregnancy Induced HypertensionDocument7 pagesPregnancy Induced HypertensionRalph Emerson RatonNo ratings yet
- The JKL Medical DictionaryDocument186 pagesThe JKL Medical Dictionarymoekyaw7171No ratings yet
- Marieb ch11bDocument28 pagesMarieb ch11bapi-229554503No ratings yet
- Review Notes (Circulatory System)Document11 pagesReview Notes (Circulatory System)Ian GarciaNo ratings yet
- Printable Flash CardsDocument28 pagesPrintable Flash CardsZaini JuttNo ratings yet
- Final ExamDocument124 pagesFinal ExamalisamsternNo ratings yet
- First Aid ManualDocument68 pagesFirst Aid ManualAntonio Bernard100% (1)
- Life Processes XDocument124 pagesLife Processes XAyush SinghNo ratings yet
- Lab Activity 2 HeartDocument5 pagesLab Activity 2 HeartRaraNo ratings yet
- Circulatory System MCQDocument9 pagesCirculatory System MCQFake GamerNo ratings yet
- NEET UG Biology Body Fluids and CirculationDocument18 pagesNEET UG Biology Body Fluids and Circulationchetan mahavarNo ratings yet
- Arterial Stiffness-1Document21 pagesArterial Stiffness-1yoeldp100% (2)
- EXPLORING THE HUMAN HEART Key To CorrectionDocument3 pagesEXPLORING THE HUMAN HEART Key To CorrectionAsh KetchumNo ratings yet
- P.E Answer KeyDocument3 pagesP.E Answer KeyAustinly Bermejo67% (6)
- Cardiovascular System-Heart: Miss Wheeler Unit 8Document29 pagesCardiovascular System-Heart: Miss Wheeler Unit 8Ngatchou GaelleNo ratings yet
- SherpaSpecialityCurvesBrochure OriginalDocument2 pagesSherpaSpecialityCurvesBrochure OriginalDigipact DigiNo ratings yet
- Review of Anatomy and Physiology of Blood Vessels and BloodDocument9 pagesReview of Anatomy and Physiology of Blood Vessels and BloodDan Ataniel EnsaladaNo ratings yet
- Nursing 2 Spanish Unit 3Document4 pagesNursing 2 Spanish Unit 3Milka Rocha FloresNo ratings yet
- CSEC Biology June 2002 P1 Specimen PaperDocument13 pagesCSEC Biology June 2002 P1 Specimen PaperJoy BoehmerNo ratings yet
- Human Heart, Cosmic Heart - Chapter 2: CirculationDocument14 pagesHuman Heart, Cosmic Heart - Chapter 2: CirculationChelsea Green PublishingNo ratings yet
- Vasa VasorumDocument4 pagesVasa Vasorum1a_deaNo ratings yet
- Science Quiz Bee ReviewerDocument26 pagesScience Quiz Bee ReviewerCatherine Joy Dela Cruz92% (13)
- 2nd Term Biology Note For Ss2Document33 pages2nd Term Biology Note For Ss2Ukwuma Michael Chijioke100% (21)
- AnuerysmthesisDocument14 pagesAnuerysmthesisLeahbelle ReginioNo ratings yet
- Blood VesselsDocument7 pagesBlood VesselsRohee TariqNo ratings yet
- Long QuizDocument30 pagesLong QuizJames Dave FajardoNo ratings yet
- Science 9 First Quarter Exam SY 2021-2022Document5 pagesScience 9 First Quarter Exam SY 2021-2022Encluna Lindon JayNo ratings yet
- Workbook - A Guide To The Vascular SystemDocument202 pagesWorkbook - A Guide To The Vascular SystemDenis PogoreviciNo ratings yet