Professional Documents
Culture Documents
8412-Article Text-29472-1-10-20130809
Uploaded by
NenyCopyright
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document8412-Article Text-29472-1-10-20130809
Uploaded by
NenyACCIDENTS TO OVARIAN CYSTS
REVIEW ARTICLE
Mishra Jyoti
ACCIDENTS TO OVARIAN CYSTS *Mishra Jyoti
*Dr. Jyoti Mishra
Gynae Endoscopic & Robotic surgeon, Head, Dept. of Minimal Access Gynae Surgery, Pushpanjali Crosslay Hospital,
Ghaziabad (Delhi, NCR), India
INTRODUCTION ACCIDENTS TO OVARIAN CYSTS
Ovulation, a monthly physiological event, is a sequel of fine Table No. 2
balance between hormones & local factors. Hormonal
imbalance, pelvic infections, diseases of the ovary, use of ! Torsion
ovulation inducing drugs & many more factors can lead to ! Haemorrhage
formation of ovarian cysts. These cysts occur most frequently ! Rupture
in reproductive life, though no one from fetal life till old age is ! Infection
immune to them. The most common types of benign cysts ! Pregnancy related complications
encountered in clinical practice are listed in table1. ! Ovarian Hyperstimulation Syndrome (OHSS)
COMMON TYPES OF OVARIAN CYSTS SEEN IN
TORSION OF OVARIAN CYST
CLINICAL PRACTICE
Also called axial rotation, torsion is known to happen in a
Table No. 1
normal sized ovary in children & adolescents due to
physiological mobility of organs. It is more frequently
! Follicular cyst
encountered in women of reproductive age group, with ovarian
! Lutein cyst
enlargement. It is most typically seen in a cyst of 10 to15 cm.
! Granulosa lutein
size, with a long pedicle lying in abdomen, where there is more
! Theca lutein
space. Hence it is most commonly seen in dermoid cysts due to
! Endometrioma
their small to medium size & high mobility & is least likely in
! Dermoid cyst
chocolate cysts due to presence of adhesions.
! Cyst adenoma
! Serous Evidence of axial rotation is seen in 12% of ovarian tumours
! Mucinous coming for operation.1 Adnexal torsion is the fifth most
common gynecologic surgical emergency, with a prevalence
Ovarian cysts may remain asymptomatic for long or may lead of approximately 3%. 2
to pelvic pain, dysmenorrhoea, dyspareunia, menstrual
disturbances, and infertility or pressure effects on adjacent Pathophysiology
organs. Rarely, these patients report in an emergency room
Precipitating factor is often a sudden twisting movement of the
with acute pain in abdomen & sometimes even in shock. The
trunk. There is a high probability of this complication during
likely causes are shown in table 2.
Journal of Universal College Of Medical Sciences (2013) Vol.1 No.02 46
ACCIDENTS TO OVARIAN CYSTS
REVIEW ARTICLE
Mishra Jyoti
pregnancy & immediately after delivery, when the pelvic Corpus luteal haematoma: Vaginal bleeding usually follows
organs are undergoing a rapid change in size. Once begun, the short period of amenorrhoea. Haemorrhagic shock is seen in
process of torsion is completed by pulsations of the supplying rare cases. Treatment requires immediate surgical
vessels, which transmit their impulse to the pedicle. As the intervention.
veins get compressed, the cyst gets congested. Lymphatic Non-Gynecological conditions: Acute appendicitis,
obstruction leads to oedema. This is followed by interstitial diverticulitis, and ureteric colic, intestinal obstruction has to
haemorrhage into the substance of the tumour. Due to be differentiated from torsion. Detailed history points towards
increasing tension, there is severe abdominal pain. Usually symptoms specific to each involved organ. Clinical
these symptoms bring the patient to the hospital, before examination, laboratory tests & ultrasonography help in
arterial occlusion, leading to necrosis sets in. reaching the diagnosis.
Another clinical picture is that of frequent attacks of mild Investigations
abdominal pain, due to intermittent incomplete torsion. Leucocytosis is usually seen in patients with torsion of
Degeneration of cyst wall leads to adhesions, most often with ovarian cyst.
omentum. After acquiring new blood supply, the ovarian mass
may sever its pelvic connection & become parasitic. A pregnancy test may be required to rule out ectopic
pregnancy.
Diagnosis
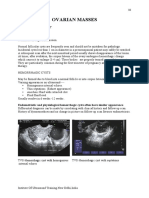
Ultrasonography shows presence of adnexal cystic mass &
Patient is often unaware of the cyst when she is seized with features of torsion. Simple cysts are unilocular and have a
sudden pain. Most of the time, there is a past history of uniformly thin wall surrounding a single cavity that contains
intermittent pain in abdomen. There may be associated nausea, no internal echoes. Most commonly, they are functional
vomiting, and signs of bladder & bowel irritability or vaginal follicular or luteal cysts or, less commonly, serous
bleeding. cystadenomas or inclusion cysts. Complex cysts may have
more than one compartment (multilocular), thickening of the
On examination, there is tachycardia, but other vital signs are
wall, projections (papulations) sticking into the lumen or on
usually maintained. Per abdomen examination reveals marked
muscle guarding & rigidity. A mass arising from pelvis may be the surface, or abnormalities within the cyst contents.
felt. On pelvic examination, a tender adnexal mass, separate Sonography findings for ovarian torsion vary depending on
from the uterus is felt. To ascertain the diagnosis of ovarian the degree of vascular compromise. Twisted adnexal masses
cyst, one must palpate its lower rounded pole through the are frequently midline, cranial to the fundus.3 Nonspecific
fornix. Large cysts often displace the uterus to the opposite
ultrasound findings include a cystic, solid, or complex mass
side. Marked tenderness & muscle guarding may impose
with free fluid, a diffusely enlarged ovary with peripheral
difficulty in defining the boundaries of the cyst. Sudden,
cystic follicles, and marked thickening of the cyst wall.
severe abdominal pain in a patient known to have ovarian cyst,
However, these findings may also be found in other conditions
should raise high suspicion of torsion.
such as a hemorrhagic cyst, endometriosis, PID, and ectopic
Differential diagnosis pregnancy.4
Ectopic gestation: History of amenorrhoea, a positive Colour Doppler provides evidence of decreased or absent
pregnancy test & an ectopic gestational sac on blood flow to the ovary. While Doppler may show no flow in
ultrasonography help in differentiating these cases from the ovary secondary to mechanical torsion of the ovarian
torsion. vessels, arterial waveforms and color flow have been reported
in surgically proven cases of torsion.5 Continued flow despite
Acute PID: Temperature is raised & patient may complain of
vaginal discharge. Ultrasonography reveals presence of torsion may be due to venous thrombosis causing symptoms
adnexal mass with free fluid in cul de sac. prior to arterial occlusion, or due to its dual blood supply from
the ovarian artery and the ovarian branches of the uterine
Ruptured ovarian cyst: Patient presents with acute pain with artery. If there is flow within a twisted vascular pedicle, a
varying degree of collapse. If a cyst was known to exist characteristic pattern of circular or coiled twisted vessels, the
previously, its size is reduced & free fluid can often be "whirlpool sign”, may be found on Doppler.3, 4
demonstrated in cul de sac. Immediate surgery is the treatment
in both torsion & rupture of ovarian cyst.
Journal of Universal College Of Medical Sciences (2013) Vol.1 No.02 47
ACCIDENTS TO OVARIAN CYSTS
REVIEW ARTICLE
Mishra Jyoti
Treatment: held by ally's type grasper & stretched out ovarian tissue by a
fine-toothed grasper. By gentle traction, the cyst wall is peeled
Once diagnosed, patient needs immediate surgical
off. Care is taken to progress slowly, releasing one grasper at a
intervention to preserve ovarian function. Till few years ago,
time or else there will be difficulty in differentiating between
laparotomy was the only approach. With recent advances in
cyst wall & ovarian tissue. Haemostasis is usually not a
the field of endoscopy, laparoscopy has become the main tool
problem. Any obvious bleeder is tackled by cautery. Edges of
in managing cases of twisted ovarian tumours. Irrespective of
the breached ovarian surface may be held together for a few
the surgical approach, salient features of treatment include,
seconds. In a very large defect, suturing may be required.
untwisting the mass, assessment of tissue viability,
cystectomy while preserving the normal ovarian tissue & Excised wall of small cyst is extracted by holding with a claw
restoring near normal anatomy. forceps passed through the 10mm port, under the guidance of a
hysteroscope, which has been inserted through a 5mm
Laparoscopy
cannula. In case of spillage into the peritoneal cavity, it is
Surgery is performed under general anaesthesia with worth giving a lavage with ringer lactate solution.
endotracheal intubation, as this allows better control of respiratory Postoperative recovery is smooth in most cases.
& cardiovascular status of the patient, especially during
Special attention is needed in cases of dermoid cyst. Here
prolonged surgery. Instruments required are listed in table 3.
attempt should be made to prevent the spillage of cyst contents
SET OF INSTRUMENTS NEEDED FOR OPERATIVE into the peritoneal cavity. Instead of puncturing the cyst, a very
LAPAROSCOPY superficial incision is made in the cortex, preferably with CO2
laser. The incision is extended with scissor & aqua dissection,
Table No. 3
and whole of the cyst is separated. If the cyst ruptures
Veress' needle Scissor accidentally, thorough peritoneal cavity irrigation with at least
5mm trocar cannula 2 Ally's type grasper 10 liters of Ringer's lactate with direct suctioning of all fatty &
epidermal elements prevents the post operative granulomatous
10mm trocar cannula Fine toothed grasper peritonitis. Such a cyst is best removed in an endobag.
Laparoscope (30 degree) Bipolar cautery
If the cyst & ovary look necrosed, they have to be completely
Injection needle removed.
Suction cannula Technical difficulties
The site of primary port may have to be above the umbilicus, if Placement of trocars: In case of a large cyst lying in
the cyst is big. Secondary ports may also require higher abdomen, the primary port needs to be placed higher up. In
placement. Cyst appears dark coloured due to venous case of suspected adhesions, Veress' needle is inserted through
congestion. Fallopian tube is often involved in the torsion & the Palmer's point (just below the left coastal margin in the
looks oedematous, but decision to salvage the tube should not midclavicular line). Achieving a good pneumperitoneum is
be taken until the adnexal mass has been untwisted, as the essential, as the peritoneum tends to be loose in this area.
inflamed tube later regains its normal anatomy in most cases. Attempts to push in the 5mm trocar through a loose
Supporting with 2 instruments, the cyst can be untwisted peritoneum, will lead to pre peritoneal placement, & extra
completely. Normal ovarian tissue is assessed for viability. If peritoneal emphysema. The 5mm hysteroscope along with its
cystectomy seems amenable, the cyst is made steady by sheath is put in through this side port & under its guidance the
holding the ovarian ligament. All except the most benign 10mm trocar is placed at the location of choice. The position of
looking cysts are removed intact either in an endobag or other secondary ports may be safely decided depending on the
through the cul de sac. A totally benign looking large cyst with size & location of the cyst. Some surgeons use the open
thin wall can be punctured with injection needle & fluid (Hasson's) technique for primary port entry.
aspirated through the attached suction tube. After the cyst
becomes lax it is easier to grasp. Small nick is made by scissor Untwisting the cyst: The instruments may slip while trying to
& suction cannula is inserted to aspirate the remaining fluid. untwist the cyst. Holding the cyst wall at less tense areas, with
Laparoscope is then inserted to closely visualize the cyst wall. ally's type grasper gives a better grip & makes it possible to
If the cyst looks benign, the incision is enlarged. Cyst wall is rotate the cyst.
Journal of Universal College Of Medical Sciences (2013) Vol.1 No.02 48
ACCIDENTS TO OVARIAN CYSTS
REVIEW ARTICLE
Mishra Jyoti
If there is less space to rotate the cyst, one may need to aspirate distensible quality of the tunica, there may not be any pain or
the cyst contents prior to untwisting, to reduce the bulk. tenderness. Bleeding from small vessels is usually self-
limiting & only leads to change in colour of the cyst contents.
Improper tissue planes: Pseudoendometriomas are Rupture of bigger vessels or intraperitoneal haemorrhage
invaginations of the ovarian cortex, which carry ovarian gives rise to severe pain. These patients may also present with
follicles. Hence there is no true cyst wall, which can be haemorrhagic shock. In the absence of shock, laparoscopy is
excised. Only aspiration & coagulating the surface is the preferred approach. Sucking all the blood & clots, clears
sufficient. Intraovarian cysts are cysts in the ovary where haemoperitoneum. The bleeding vessel is identified &
endometriotic tissue reaches by hematogenous route. These coagulated and cystectomy is performed.
cysts are usually free from adhesions & it is possible to strip off
the cyst wall. Identification of cyst wall is difficult in dermoid Corpus luteal haematoma
cyst. It is best to remove these cysts in endobag. In functional Sometimes haemorrhage may occur in a normal corpus luteum
cysts, the cyst wall may be very thin at places. It is better to which fails to resolve & gives rise to corpus haemorrhagicum.
excise such areas than to peel them. Persistent production of hormones leads to increased growth
Haemostasis: Bleeding can be severe near infundibulopelvic of endometrium. This causes amenorrhoea followed by heavy
ligament & ovarian ligament. Any bleeding vessels & prolonged bleeding. There is marked tenderness & on per
encountered here should be coagulated with bipolar. vaginal examination a tender cyst may be felt through the
fornix. Differential diagnosis is with cases of ectopic
Extraction of cyst wall: After grasping a specimen larger than pregnancy & abortion.
5 mm channel, the sleeve is slipped upward on the grasper
shaft out of the peritoneal cavity. The grasping forceps with the On sonography, the combination of clotted blood & liquid
specimen is then pulled out in one motion through the soft contents may appear as: an irregular echogenic area with
tissue of the anterior abdominal wall. Forcep is then reinserted scalloped edging along the inner walls, 2) a spherical cyst with
through the exit tract & the sleeve is pushed over it. Initial many lobes, 3) one or more septa within the cyst.6
placement of the trocar sleeve lateral to the deep epigastric Management
vessels avoids going through the rectus muscle. Trocar
penetrates the external oblique, internal oblique & Analgesics & simple observation usually suffices. Follow up
transversalis fascia only, thus leaving an easily identifiable sonography after menses, shows resolution of corpus luteum
tract. Extraction through cul de sac is rarely required. cyst in most cases. Surgery is required if patient presents with
acute abdomen & the possibility of torsion or rupture cannot be
A large cyst wall may be cut into long strips & then removed. ruled out. Due to variable presentations of ectopic pregnancy,
Dermoid cyst, due to its variable consistency, is difficult to these patients are often operated for the same. It is only on
extract. The cyst is placed in an endobag, inserted through the histopathology, that true nature of pathology is revealed.
10mm port & the threads are pulled out. As the bag reaches the
level of abdominal wound, contents are removed partially & RUPTURED OVARIAN CYST
then the bag withdrawn. Rupture is more likely to happen if the cyst wall is damaged by
Sequelae: Most of these patients, when treated early, resume previous ischaemic degeneration or if it is malignant. It can
normal ovarian function & have normal fertility. Cases also happen spontaneously as is typically seen in the cases of
reporting late may develop ovarian necrosis & sepsis. actively growing pseudomucinous cystadenomas, where the
epithelial elements of the cyst grow faster than the connective
HAEMORRHAGIC OVARIAN CYST tissue of the capsule. Spontaneous rupture results, discharging
Ovary has an outer cortex, rich in primordial follicles & inner pseudomucinous material into the peritoneal cavity. In most
medulla, which is more vascular. The outermost connective cases, there is no serious side effect, but rarely the coagulated
tissue layer is called tunica albuginea. Unlike male testis, pseudomucinous material forms adhesions with omentum &
where tunica forms a resistant layer, in females it is poorly intestines leading to pseudomyxoma peritonei.1 External
formed & is quite distensible. This allows for monthly factors such as trauma, pelvic examination, coitus or childbirth
distension of ovaries by the growing follicle. When a small can also precipitate rupture. During labour the presenting part
vessel in the wall of the tumour ruptures, blood may collect presses upon the cyst lying in the pouch of Douglas, & can lead
into the cyst itself or into the peritoneal cavity. Due to to rupture.
Journal of Universal College Of Medical Sciences (2013) Vol.1 No.02 49
ACCIDENTS TO OVARIAN CYSTS
REVIEW ARTICLE
Mishra Jyoti
Signs & Symptoms when there is evidence of spreading peritonitis despite
adequate medical treatment, ruptured ovarian abscess or when
Presentation depends on the contents & size of the cyst.
diagnosis is in doubt. Some surgeons prefer to do laparoscopy
Rupture of a small cyst may cause sudden severe pain without
for confirming the diagnosis & draining the purulent fluid
any after effects. There may be a sensation of something
along with excision of abscess cavity (necrotic inflammatory
giving way, followed by vomiting, diarrhoea, and severe
exudates).The peritoneal cavity is well irrigated with Ringer's
abdominal pain. Because the amount of blood loss is minimal,
hypovolemia does not supervene. Peritoneal irritation due to lactate solution. Caution is needed in cases of suspected
leakage of cyst fluid can lead to significant tenderness, adhesions. Temperature elevation rarely persists past the first
abdominal distension, and hypoperistalsis. If the cyst was postoperative day.
known to exist, its size is found reduced & free fluid is seen in OVARIAN CYST IN PREGNANCY
the peritoneal cavity.
The common types of ovarian cysts seen during pregnancy are
Worst peritoneal reaction is seen with the rupture of dermoid serous cyst, dermoid cyst & corpus luteum cyst.
cyst. Sebaceous material collects into the peritoneal cavity, The incidence of dermoid cyst is two times higher than in non-
leading to acute abdomen & fever. pregnant state. The incidence of benign ovarian tumours with
pregnancy is about 0.2%, 1/3rd being dermoids 1/3rd corpus
Investigations:
luteum cysts.7
There is often leucocytosis & sonography reveals free fluid in
Pathophysiology
the peritoneal cavity. If urgent sonography is not possible,
culdocentesis gives important information to reach a Following fertilization the normal corpus luteum continues to
diagnosis. grow & forms corpus luteum of pregnancy. If haemorrhage
occurs in its substance, then it can become cystic & acquire
Management
quite a large size, up to 3-5cms. Such cysts disappear
The aim of treatment is to clear the peritoneal cavity of all the spontaneously at 14-16 weeks.
cyst contents along with removal of the cyst. In patients
reporting early, laparoscopy is preferred for all its benefits of Any of these cysts can undergo complications like torsion,
minimally invasive approach. In late cases, where there is high haemorrhage, rupture & infection. The incidence of torsion is
likelihood of dense bowel adhesions, laparotomy is preferred. higher during the first trimester when the gravid uterus
After removing the cyst contents, repeated lavage is done, till dislodges the cyst from the pelvis into more spacious abdomen
the peritoneal cavity appears clean. Prognosis in & still higher soon after delivery when pelvic organs are
pseudomyxoma peritonei is poor, even after the ovaries are rapidly changing in size.
removed. Cyst can undergo haemorrhage or rupture during labour.
INFECTED OVARIAN CYST Infection is more likely in the puerperium.
Infection may happen by direct spread of organisms through Signs & symptoms
adjacent structures as in acute salpingitis or pelvic peritonitis. Majority of the patients are asymptomatic. During pregnancy
A cyst, which has undergone ischaemic necrosis, is more the some of the patients may present with urinary retention,
likely to get infected with bowel organisms. A cyst, which has mechanical distress due to over distension of abdomen or
been treated by tapping rather than by removal, is more likely preterm labour. During labour there is high chance of
to undergo infection. These cases present with fever &
malpresentation & obstructed labour. If any of the
abdominal pain. There is leucocytosis & a tender mass is felt
complications occur, patient presents with features of acute
through the fornix. Ultrasound documents a tubo - ovarian
abdomen.
pathology, with features of a complex mass.
Diagnosis is easy in early pregnancy, when one can feel the
Treatment
cyst separately from the uterus. In second trimester, putting the
Treatment of infection is conservative & consists of patient in Trendelenburg position, shifts the cyst more towards
intravenous antibiotic coverage, along with supportive the abdomen, & becomes more obvious. Ultrasonography
therapy. Surgery is indicated only in special circumstances as helps to confirm the diagnosis.
Journal of Universal College Of Medical Sciences (2013) Vol.1 No.02 50
ACCIDENTS TO OVARIAN CYSTS
REVIEW ARTICLE
Mishra Jyoti
Differential diagnosis preferably in the first week. If cyst is found impacted in pouch
A complicated ovarian cyst during pregnancy is to be of Douglas, Caesarean section should be performed. Even if
differentiated from ectopic pregnancy, sacculation of gravid caesarean is done for other obstetric reasons, cyst should be
uterus, red degeneration of fibroid, acute hydramnios & removed at the same time.
accidental haemorrhage.
Laparoscopic surgery is possible upto 16 weeks gestation. Till
Treatment then, the size of gravid uterus does not hinder the introduction
of trocar at the usual sites.8
Cyst smaller than 5 cms is usually corpus luteum of pregnancy
& does not require any treatment. Such a cyst disappears OVARIAN HYPERSTIMULATION SYNDROME
spontaneously by14 to 16 weeks. A larger cyst can be safely (OHSS)
removed after 16 weeks, when placenta has taken over the
function of corpus luteum. Cystectomy with ovarian Introduction of gonadotrophins for ovulation induction, in the
reconstruction is the preferred treatment, but even if treatment of infertility has been a major medical breakthrough
ovariectomy is performed, there is no risk to pregnancy. After in this century. Serious OHSS is an outcome of ovulation
28 weeks, it is better to keep the patient under observation. stimulation, which can affect 100-200 cases in 100,000
Due to increased risk of complications after delivery, these stimulation cycles annually through World Registries of
cysts should be removed early in the puerperium. If Assisted Conception.9
complications like torsion, haemorrhage or rupture occur,
surgery is done irrespective of the gestational age. Classification
If cyst is not impacted in the pelvis, vaginal delivery may be Schenker & Weinstein have classified OHSS according to the
allowed. Cyst should be removed early in the puerperium, symptoms, signs & laboratory findings 10(table 4).
Table 4. Schenker & Weinstein's Classification of OHSS10
Grade I - Serum oestrogen > 150micrograms/ day
Urine pregnendiol excretion > 10 mg/ day
Mild Hyperstimulation
Grade II - Grade I with ovarian enlargement / small cysts.
Grade III - Grade II with abdominal distension
Moderate Hyperstimulation
Grade IV Grade III with nausea, vomiting and/ or diarrhoea
Grade V Grade IV with large ovarian cysts and ascities and/ or hydrothorax
Severe Hyperstimulation
Grade VI Grade with hemoconcentration, with or without coagulation abnormalities
Golan proposed another classification, where he also included sonographic findings 11 (table 5).
Table 5. OHSS classification by Golan et al11
Grade I Abdominal distension & discomfort.
Mild OHSS
Grade II - Grade I with nausea, vomiting and/ or diarrhoea; ovaries are enlarged 5- 12 cm.
Moderate OHSS Grade III features of mild OHSS plus ultrasonic evidence of ascites.
Grade IV Features of moderate hyperstimulation with clinical ascites and/ or hydrothorax
and respiratory difficulties.
Severe OHSS
Grade V All of the above plus change in the blood volume, increased blood viscosity
due to hemoconcentration, coagulation abnormalities & diminished renal perfusion.
Journal of Universal College Of Medical Sciences (2013) Vol.1 No.02 51
ACCIDENTS TO OVARIAN CYSTS
REVIEW ARTICLE
Mishra Jyoti
Complications CONCLUSION
Vascular complications - Haemoconcentration, thromboembolic With increasing use of ovulation inducing drugs, the incidence of
phenomena due to coagulation abnormalities may lead to serious ovarian cyst is increasing. Though many factors contribute to it, there
cerebrovascular accident. are still, not too many effective ways to prevent the occurrence of
ovarian cysts. Oral contraceptive pills are known to provide some
Liver dysfunction - Although the liver functions are abnormal, protection. OHSS can be prevented by close monitoring of all high-
morphological changes are seen only at the ultrastructural level. This risk patients.
is a compensatory change in response to increased demand of liver
enzymes. Early diagnosis & treatment is the only way of reducing accidents to
ovarian cyst & long-term complications like adhesions & infertility.
Respiratory complications - Pleural effusion, mechanical distress
due to ascites, hydrothorax & Adult Respiratory Distress Syndrome
may appear due to OHSS.
POINTS TO REMEMBER
Gastrointestinal complications - Pain in abdomen, nausea,
vomiting & diarrhoea could be the initial symptoms of OHSS. Ovarian cysts may remain asymptomatic for long or
occasionally present with acute abdominal pain or even shock.
Adnexal torsion - Multiple follicular or luteal cysts make the ovaries
enlarged. This predisposes them to torsion. Pregnancy further Adnexal torsion is the fifth most common gynec surgical
increases the chances. Mashiach et al noted torsion in 16% of the emergency.
pregnant patients compared with 2.3% in the nonpregnant patients.12
Torsion (of ovarian cyst ) can occur during pregnancy and
Prevention of OHSS immediate post delivery due to a rapid change in pelvic organ
Recognition of high-risk patients & following preventive measures size.
are the only ways of reducing the incidence of OHSS.
Torsion needs differentiation from ectopic pregnancy, acute
Young thin patients, presence of polycystic ovaries, oligomenorrhoic PID ruptures ovarian cyst, corpus luteal hematoma and non
anovulation & use of hMG & GnRH agonists, all increase the risk of gynecological causes for acute abdomen.
developing OHSS.
Hemorrhage, rupture and infection of ovarian cyst are other
Other high risk factors include presence of large number of small &
gynecological causes for acute abdomen.
intermediate follicles on sonography & serum estradiol levels >/
=2500pg/ml, on the day of hCG administration. Localized infection and small corpus luteal hematoma can be
More reliable is the slope of rise in E2 concentration, to check if the managed conservatively while torsion and rupture need
values are more than doubling. Conception cycles lead to a higher risk surgical intervention preferably by laparoscopic approach,
of OHSS. occasionally by laparotmy.
Withholding or delaying hCG, using GnRH agonists to trigger Incidence of benign ovarian tumours with pregnancy is about
ovulation can prevent OHSS. Follicular aspiration, use of 0.2% and most patients are asymptomatic.
progesterone to support luteal phase, administration of human
albumin & glucocorticoids at the time of oocyte recovery is some of Presence of ovarian cyst during pregnancy can lead to urinary
the other ways of reducing the chances of OHSS. retention, mechanical distress, preterm labour,
Treatment malpresentations and obstructed labour.
Treatment is mainly supportive to maintain the intravascular volume Corpus luteal cysts <5 cms during pregnancy do not need any
& avoid the complications of hypercoaguability. treatment and regress spontaneously by 14-16 week.
Surgical therapy is indicated only in the following situations- When ovarian cysts persist during pregnancy, cystectomy with
Intraperitoneal haemorrhage ovarian reconstruction is performed after 16 weeks in second
Rupture of ovarian cyst trimester.
Torsion of ovarian cyst
Ectopic pregnancy. Emergency surgery is performed when cyst complications
occur during pregnancy.
One may choose laparoscopic or laparotomy route, depending on the
patient's condition. Just untwisting the enlarged ovary is mostly In OHSS due to presence of enlarged ovaries surgery is indicated
sufficient to carry on the pregnancy. when rupture, torsion or intraperitoneal hemorrhage occur.
Journal of Universal College Of Medical Sciences (2013) Vol.1 No.02 52
ACCIDENTS TO OVARIAN CYSTS
REVIEW ARTICLE
Mishra Jyoti
REFERENCES
1) Howkins & Bourne Shaw, Disorders of the ovary. In Padubidri VG, 7) Hopkins MP, Duchon MA. Adnexal surgery in pregnancy. Reprod
Daftary Shirish N. Eds. Shaw's Textbook of Gynaecology, Twelfth Ed. Med.1986; 31:1035.
Churchill Livingstone Pvt.Ltd. New Delhi. 1999: 326.
8) Rao AR. Laparoscopic Management of Ovarian Masses. In Desai SV,
2) Pena J, Ufberg D, Cooney N & Denis A. Usefulness of Doppler Joseph KA. Eds. Gynecological Endoscopic Surgery- Current
sonography in the diagnosis of ovarian torsion. Fertility & Sterility, concepts. A FOGSI Publication, Jaypee Brothers, New Delhi. 2002; Ch
2000: 73(5): 1047-50. 3:13.
3) Dill-Macky M J, Atri M. Ovarian Sonography. In Ultrasonography in 9) Schenker JG, Ezra Ezra. Complications of assisted reproduction
Obstetrics and Gynecology, Callen PW Ed, 4th Edition. WB Saunders techniques. Fertil Steril, 1994: 61:411-422.
Company, Philadelphia 2000; Ch 31: 872-873.
10) Schenker and Weinstein. Ovarian Hyperstimulation Syndrome: a current
4) Lee EJ, Kwon HC, Joo HJ, Suh JH, & Fleischer AC. Diagnosis of survey. Fertil Steril 1978: 30: 255-68.
Ovarian Torsion with Color Doppler Sonography: Depiction of
11) Golan A, Ron-EI Rherman A. Ovarian Hyperstimulation Syndrome: an
Twisted Vascular Pedicle. J Ultrasound Med 1998: 17: 83-89.
update review. Obstet Gynecol Surv 1989: 44:430-440.
5) Rumack CM, Wilson SR, & Charboneau JW. Diagnostic Ultrasound,
12) Ben-Raphael Z, Bider D, Mashiach S. Laparoscopic unwinding of
2nd edition. Mosby, 1998:550-1.
twisted ischaemic haemorrhagic adnexum after in vitro fertilization.
6) Cydney Afriat Menihan. Gynaecologic Pain and Dysfunctional Uterine Fertil Steril 1990: 53: 569-571.
Bleeding. In Limited Sonography in Obstetric and Gynaecologic
Triage. Brogan JE, Barta.SV, Barishek V Eds. Lippincott - Raven
Publishers. Philadelphia. 1998; Ch 7:109-110.
Universal College of Medical Sciences and Teaching Hospital
Facilities available
! General Surgery ! Cardiology ! Colour Doppler
! Internal Medicine ! Intensive Care Unit ! C.T. Scan
! Neuro Surgery ! Neonatal Intensive Care Unit ! M.R.I.
! Neurology ! C.C.U. ! Digital X-ray
! Plastic Surgery ! Fully equipped Operation Theatres ! Bone Densitometry
! Gynaecology & Obstetrics ! Endoscopy ! Fluoroscopy
! Paediatrics ! E.C.G. ! Hemo Dialysis
! Ophthalmology ! ECHO ! 24x7 hours Emergency Services
! Dermatology ! Holter ! Ambulance Serivce
! Orthopaedics ! Tread Mill Test ! Laparoscopic Surgery
! ENT ! Ultra Sound ! Bronchoscopy
! Psychiatry ! E.E.G. ! Colonoscopy
Journal of Universal College Of Medical Sciences (2013) Vol.1 No.02 53
You might also like
- EndometriomaDocument7 pagesEndometriomaErick Rafael AncaNo ratings yet
- M 1: T A S: Odule HE Cute CrotumDocument10 pagesM 1: T A S: Odule HE Cute CrotumROMANNo ratings yet
- Acute Scrotum Guide for Medical StudentsDocument9 pagesAcute Scrotum Guide for Medical StudentsJody FelizioNo ratings yet
- Acute ScrotumDocument9 pagesAcute ScrotumIsabel ReyNo ratings yet
- EndometriosisDocument46 pagesEndometriosisManoj Ranadive0% (1)
- Scrotal AbnormalitiesDocument6 pagesScrotal AbnormalitiesmoominjunaidNo ratings yet
- Pediatric Surgery Notes For NursesDocument8 pagesPediatric Surgery Notes For NursesAhmed SamyNo ratings yet
- Clinicopathologic Case Presentation of Uterine MassDocument47 pagesClinicopathologic Case Presentation of Uterine Massvicheryl100% (1)
- Ovarian Masses: Types, Ultrasound Features & Differential DiagnosisDocument5 pagesOvarian Masses: Types, Ultrasound Features & Differential DiagnosisPriyanka GeorgeNo ratings yet
- Ovarian TorsionDocument48 pagesOvarian Torsionmaria ilyasNo ratings yet
- Torsion Ovarian CystDocument10 pagesTorsion Ovarian CystDani SetiawanNo ratings yet
- Torsio TestisDocument55 pagesTorsio TestisAulia RizkiaNo ratings yet
- Appendicitis, Acute: Pelvic Inflammatory DiseaseDocument16 pagesAppendicitis, Acute: Pelvic Inflammatory DiseaseLittle SleepybirdNo ratings yet
- Module 1 Acute Scrotum PDFDocument11 pagesModule 1 Acute Scrotum PDFbayutrihatmajaNo ratings yet
- Intussusception PresentationDocument9 pagesIntussusception PresentationAme NasokiaNo ratings yet
- Benign Lesions of The OvariesDocument12 pagesBenign Lesions of The OvariesdocjosmaNo ratings yet
- GENITAL EMERGENCYDocument4 pagesGENITAL EMERGENCYcorsaruNo ratings yet
- Acute Appendicitis Diagnosis and TreatmentDocument3 pagesAcute Appendicitis Diagnosis and TreatmentMavi HayalNo ratings yet
- DR Sankalpa R WankhedeDocument76 pagesDR Sankalpa R Wankhedechaitanya suryawanshiNo ratings yet
- Nital Disorders and Injuries-1Document43 pagesNital Disorders and Injuries-1qruz Mohamed DiisNo ratings yet
- Ovaries & AdnexaeDocument124 pagesOvaries & AdnexaeabafzNo ratings yet
- INGUINAL HERNIA and Umbilical HerniaDocument13 pagesINGUINAL HERNIA and Umbilical HerniaKathNo ratings yet
- Testicular Torsion, Hydrocele & Fournier GangreneDocument41 pagesTesticular Torsion, Hydrocele & Fournier GangreneNur Insyirah100% (1)
- Testicular Torsion - StatPearls - NCBI BookshelfDocument6 pagesTesticular Torsion - StatPearls - NCBI Bookshelfwijana410No ratings yet
- Ovarian TorsionDocument25 pagesOvarian TorsionshaggypazokiNo ratings yet
- Ectopic Pregnancy 2022 Edited 3Document40 pagesEctopic Pregnancy 2022 Edited 3apule geraldhumbleNo ratings yet
- 2.4.5.2.3.a Bowel ObstructionDocument35 pages2.4.5.2.3.a Bowel ObstructionProject ByNo ratings yet
- Rectovaginal Fistulae: Bidhan Das, MD Michael Snyder, MDDocument7 pagesRectovaginal Fistulae: Bidhan Das, MD Michael Snyder, MDNovaNo ratings yet
- Abnormalities Involving UterusDocument20 pagesAbnormalities Involving UterusDrRajkumar PatelNo ratings yet
- Abnormalities Of The Testis And Scrotum: A Concise GuideDocument34 pagesAbnormalities Of The Testis And Scrotum: A Concise GuideIma MoriNo ratings yet
- 25 UrologyDocument47 pages25 UrologyMahmoud AbuAwadNo ratings yet
- Benign Gynecological LesionsDocument9 pagesBenign Gynecological LesionsLanceNo ratings yet
- Pathophysiology: Each Month, Normally Functioning Ovaries Develop SmallDocument9 pagesPathophysiology: Each Month, Normally Functioning Ovaries Develop SmallAl-nazer Azer Al100% (1)
- IntussusceptionDocument10 pagesIntussusceptionshenlie100% (1)
- LP NokDocument20 pagesLP NokGracia Ayu ChristinaNo ratings yet
- Gynecologic-Nursing Part 2Document40 pagesGynecologic-Nursing Part 2jomariNo ratings yet
- Benign Gynecologic Lesions: Vulva, Vagina, Cervix, Uterus, Oviduct, OvaryDocument28 pagesBenign Gynecologic Lesions: Vulva, Vagina, Cervix, Uterus, Oviduct, OvaryvannieloveNo ratings yet
- Ileal Atresia ReferenceDocument50 pagesIleal Atresia ReferenceOvamelia JulioNo ratings yet
- Case 3 AlexiDocument17 pagesCase 3 AlexiHenry HNo ratings yet
- Abnormalities of Placenta and CordDocument47 pagesAbnormalities of Placenta and CordShrooti Shah75% (4)
- Appendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenDocument7 pagesAppendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenAndi HairunNo ratings yet
- Department of Prasuti Tantra and Striroga Dayanand Ayurvedic College, Jalandhar SESSION 2016-17Document40 pagesDepartment of Prasuti Tantra and Striroga Dayanand Ayurvedic College, Jalandhar SESSION 2016-17jyothiNo ratings yet
- Urological Physical ExaminationDocument5 pagesUrological Physical ExaminationSirajum MuneeraNo ratings yet
- EndometriosisDocument5 pagesEndometriosisLok100% (2)
- HerniaDocument11 pagesHerniaHapsari Wibawani 'winda'100% (1)
- Ovarian Torsion in Pregnancy A Case ReportDocument3 pagesOvarian Torsion in Pregnancy A Case ReportCakraEkkyNo ratings yet
- Chapter X.4. Intussusception: Case Based Pediatrics For Medical Students and ResidentsDocument5 pagesChapter X.4. Intussusception: Case Based Pediatrics For Medical Students and ResidentsNawaf Rahi AlshammariNo ratings yet
- Multiloculated Peritoneal Inclusion Cyst Treated Successfully With Laparoscopic SurgeryDocument3 pagesMultiloculated Peritoneal Inclusion Cyst Treated Successfully With Laparoscopic SurgerySreekumar SreekandanNo ratings yet
- Male GU ExamDocument5 pagesMale GU ExamOmar Farid ElgebalyNo ratings yet
- Female Genital Cysts Tract PDFDocument6 pagesFemale Genital Cysts Tract PDFRaraNo ratings yet
- Chronic Uterine InversionDocument4 pagesChronic Uterine InversionnurelianaNo ratings yet
- Hernias (Inguinal and Femoral)Document37 pagesHernias (Inguinal and Femoral)Muwanga faizoNo ratings yet
- 07 Intussusception and Midgut Volvulus - 2015-05-12 - AHC Media: Continuing Medical Education PublishingDocument10 pages07 Intussusception and Midgut Volvulus - 2015-05-12 - AHC Media: Continuing Medical Education PublishingPridina SyadirahNo ratings yet
- EndometriosisDocument10 pagesEndometriosisSivaram Shanmugha VilasNo ratings yet
- Bowel Obstruction and Tumors SheetDocument19 pagesBowel Obstruction and Tumors SheetAbu Ibtihal OsmanNo ratings yet
- Uterine Fibroid - Viva VoceDocument77 pagesUterine Fibroid - Viva VoceK Haynes Raja100% (1)
- 2017 Pediatric Ovarian TorsionDocument13 pages2017 Pediatric Ovarian TorsionVladimir BasurtoNo ratings yet
- UB DisordersDocument13 pagesUB Disordershussain AltaherNo ratings yet
- BMI Chart for Boys Birth to 2 YearsDocument1 pageBMI Chart for Boys Birth to 2 YearsMalisa LukmanNo ratings yet
- Horner Syndrome As The Only Focal Neurologic Manifestation of Hypothalamic HemorrhageDocument3 pagesHorner Syndrome As The Only Focal Neurologic Manifestation of Hypothalamic HemorrhageNenyNo ratings yet
- Algorithm 1: Initial Evaluation and Management: Symptoms of Possible ACSDocument6 pagesAlgorithm 1: Initial Evaluation and Management: Symptoms of Possible ACSNenyNo ratings yet
- Atrial and Ventricular EnlargementDocument47 pagesAtrial and Ventricular EnlargementNenyNo ratings yet
- 203 380 1 SM PDFDocument10 pages203 380 1 SM PDFCdma Nastiti FatimahNo ratings yet
- Drug Therapy Protocols:: MorphineDocument5 pagesDrug Therapy Protocols:: MorphineNenyNo ratings yet
- ASA Physical Status Classification System: An Overview and ReferencesDocument2 pagesASA Physical Status Classification System: An Overview and ReferencesalvionitarosaNo ratings yet
- The Philosophy of EmoDocument2 pagesThe Philosophy of EmoTed RichardsNo ratings yet
- Fauconnier - Mental SpacesDocument237 pagesFauconnier - Mental SpacesClaudia Mauléon-Stäheli100% (1)
- Gen. Math TestDocument5 pagesGen. Math TestAlfred LabadorNo ratings yet
- 489-F Latest JudgmentDocument15 pages489-F Latest JudgmentMoving StepNo ratings yet
- Review Notes in ABG Interpretation - NCLEXDocument1 pageReview Notes in ABG Interpretation - NCLEXFilipino Nurses CentralNo ratings yet
- Kinder DLP Lesson-Exemplar-Week-25-Day-2Document16 pagesKinder DLP Lesson-Exemplar-Week-25-Day-2Leonor BagnosNo ratings yet
- Understanding The SelfDocument10 pagesUnderstanding The Selfgame master50% (2)
- Senior Java Developer With 4 Years Experience ResumeDocument5 pagesSenior Java Developer With 4 Years Experience ResumedivaNo ratings yet
- Augustinian Learning Playlist: Ms. Juvelyn A. Abugan English Grade 9Document3 pagesAugustinian Learning Playlist: Ms. Juvelyn A. Abugan English Grade 9Jemar Quezon Lifana100% (2)
- RMXPRT Manual PDFDocument481 pagesRMXPRT Manual PDFsch12332163% (16)
- Department of Information TechnologyDocument1 pageDepartment of Information TechnologyMuhammad ZeerakNo ratings yet
- Literary Analysis Essay - Student PacketDocument11 pagesLiterary Analysis Essay - Student Packetapi-2614523120% (1)
- MWSS v. CADocument15 pagesMWSS v. CAAlexander AbonadoNo ratings yet
- Draft Certificates Bg. Terang 306 - 7,557. 258mt Mt-2Document5 pagesDraft Certificates Bg. Terang 306 - 7,557. 258mt Mt-2BOBY RAHMAN PURBANo ratings yet
- Chap 006Document50 pagesChap 006Martin TrịnhNo ratings yet
- Customer Satisfaction and Firm Performance: Insights From Over A Quarter Century of Empirical ResearchDocument22 pagesCustomer Satisfaction and Firm Performance: Insights From Over A Quarter Century of Empirical ResearchMohamedAliBenAmorNo ratings yet
- Sid The Science Kid - The Ruler of Thumb Cd1.avi Sid The Science Kid - The Ruler of Thumb Cd2.aviDocument27 pagesSid The Science Kid - The Ruler of Thumb Cd1.avi Sid The Science Kid - The Ruler of Thumb Cd2.avisheena2saNo ratings yet
- Ais 9 ImDocument117 pagesAis 9 ImSimonNisjaPutraZai100% (1)
- Shero Shayari by GhalibDocument65 pagesShero Shayari by GhalibEngr Muhammad Shafeeq NaqeebiNo ratings yet
- Anthony Browder - The Mysteries of MelaninDocument4 pagesAnthony Browder - The Mysteries of MelaninHidden Truth82% (11)
- Person On The StreetDocument12 pagesPerson On The StreetalyssajdorazioNo ratings yet
- Maghrib Time Nairobi - Google SearchDocument1 pageMaghrib Time Nairobi - Google SearchHanan AliNo ratings yet
- How The Government Was Formed After Prophet MuhammadDocument48 pagesHow The Government Was Formed After Prophet MuhammadMUSALMAN BHAINo ratings yet
- 101 Poisons Guide for D&D PlayersDocument16 pages101 Poisons Guide for D&D PlayersmighalisNo ratings yet
- Preparation Total Consecration PDFDocument872 pagesPreparation Total Consecration PDFgbarcelonNo ratings yet
- Papal InfallibilityDocument6 pagesPapal InfallibilityFrancis AkalazuNo ratings yet
- Updated Syllabus - ME CSE Word Document PDFDocument62 pagesUpdated Syllabus - ME CSE Word Document PDFGayathri R HICET CSE STAFFNo ratings yet
- Genealogy On June 09-2003Document25 pagesGenealogy On June 09-2003syedyusufsam92100% (3)
- Puregold SWOT AnalysisDocument3 pagesPuregold SWOT AnalysisRizza Mae CabigasNo ratings yet
- Electronics Engineering Technician: Semiconductor ComponentsDocument253 pagesElectronics Engineering Technician: Semiconductor Componentsnagsanthosh3No ratings yet