Professional Documents
Culture Documents
ACLS 2015 Algorithm and Anesthesia ACLS PDF
Uploaded by
Taufiqurrahman RizkiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
ACLS 2015 Algorithm and Anesthesia ACLS PDF
Uploaded by
Taufiqurrahman RizkiCopyright:
Available Formats
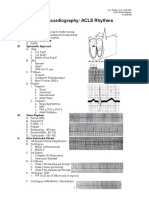
Cardiac Arrest *
Circular Algorithm
Shout for Help/Activate Emergency Response
Start CPR
Give Oxygen Attach Monitor/Defibrillator
2 minutes Return of Spontaneous
Circulation (ROSC)
Check Post-Cardiac
Rhythm Arrest Care
If VF/VT
Shock
Drug Therapy
IV/IO access
Epinephrine every 3–5 minutes
uous CPR
Amiodarone for refractory VF / VT
Continuous CPR
Consider Advanced Airway
Quantitative waveform capnography
Contin
Treat Reversible Causes
Mo
nitor y
CPR Qualit
Doses/Details for the Cardiac Arrest Algorithms
CPR Quality Return of Spontaneous Circulation(ROSC)
Push hard (2” to 2.4” or 5–6cm) and fast (100–120/min) and allow Pulse and blood pressure
complete chest recoil. Abrupt sustained increase in PETCO2 (typically ≥ 40 mm Hg)
Minimize interrruptions in compressions.**
Spontaneous arterial pressure waves with intra-arterial
Avoid excessive ventilation monitoring
Rotate compressor every 2 minutes
If no advanced airway, 30:2 compression-ventilation ratio
Quantative waveform capnography
If PETCO2<10mm Hg, attempt to improve CPR quality
Shock Energy
If relaxation phase(diastolic) pressure<20mm Hg,
attempt to improve CPR quality. Biphasic: Manufacturer recommendation (eg. initial dose of
120–200 J): if unknown, use maximum available.
Second and subsequent doses should be equivalent, and
Drug Therapy higher doses may be considered
Monophasic: 360 J
Epinephrine IV/IO Dose: 1 mg every 3–5 minutes
Amiodarone IV/IO Dose***: First dose: 300 mg bolus
Second dose: 150 mg Reversible Causes
Hypovolemia Tension pneumothorax
Advanced Airway**** Hypoxia Tamponade, cardiac
Supraglottic advanced airway or endotracheal intubation Hydrogen ion (acidosis) Toxins
Waveform capnography to confirm and monitor ET tube placement Hypo-/Hyperkalemia Thrombosis, pulmonary
10 breaths per minute with continuous chest compressions Hypothermia Thrombosis, coronary
* Link MS, Berkow LC, Kudenchuk PJ, Halperin HR, Hess EP, Moitra VK, Neumar RW, O’Neil BJ, Paxton JH, Silvers SM, White RD, Yannopoulos D, Donnino MW. Part 7: adult advanced cardiac life support. 2015 American
Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015 132 (suppl 2):S444-S464
** Bobrow BJ, Clark LL, Ewy GA, Chikani V, Sanders AB, Berg RA, Richman PB Minimally Interrupted cardiac resuscitation by emergency medical services for out of hospital cardiac arrest. JAMA 2008;299:1158-1165
***Dorian P, Cass D, Schwartz B, Cooper R. Gelaznikas R, Barr A. Amiodarone as compared with Lidocaine for shock resistant ventricular fibrillation N Engl J Med 2002;346:884-890.
**** Dorges V, Wenzel V, Knacke P, Gerlach K, Comparison of different airway management strategies to ventilate apneic, nonpreoxygenated patients. Crit Care Med. 2003;31:800-804
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020.
If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document. Version 2018.02.a
© ACLS Training Center 877-560-2940 support@acls.net
Complete your ACLS recertification online with the highest quality course at http://www.acls.net and use promo code PDF2016 during checkout for 15% off.
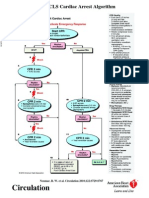
Cardiac Arrest
Algorithm
Shout for Help/Activate Emergency Response
Start CPR
1 Give Oxygen
Attach Monitor/Defibrillator
2 VF/VT Rhyhm Shockable? Asystole/PEA 9
3 Shock*
CPR 2 min
IV/IO access
4
CPR 2 min 10 Epinephrine every 3–5 min
IV/IO access Consider advanced airway,
capnography
Rhythm Shockable?
12
Rhyhm Shockable?
5 Shock
If no signs of return of
spontaneous circulation
(ROSC), go to 10 or 11.
CPR 2 min
Epinephrine every 3-5 min CPR 2 min
6 Consider advanced airway, Treat reversible causes 11
capnography
If ROSC, go to Post-
Cardiac Arrest Care.
Rhyhm Shockable? Rhyhm Shockable?
7 Shock
CPR 2 min
Amiodarone 8 Go to 5 or 7
Treat reversible causes
* Link MS, Atkins DL, Plassman RS, Halperin HR, SAmson RA, White RD, Cudnik MT, Berg MD, Kudenchuk PJ, Kerber RE. “Part 6: electrical therapies: automated external defibrillators, defibrillation, cardioversion, and pacing:
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care”. Circulation. 2010;122(suppl 3): S706-S719.
http://circ. ahajournals.org/content/122/18_suppl_3/S706
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020.
If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document. Version 2018.02.a
© ACLS Training Center 877-560-2940 support@acls.net
Complete your ACLS recertification online with the highest quality course at http://www.acls.net and use promo code PDF2016 during checkout for 15% off.
Acute Coronary
Syndromes Algorithm
Syndroms Suggestive of Ischemia or Infarction
EMS assessment and care and hospital prepartion*
Oxygen
Aspirin (If O sat< 94% Activate Cardiac Pain
2
12–Lead ECG Control
160–325 mg or O Sat>90%
2
Cath Lab
with COPD)
Concurrent ED assessment Immediate ED general
(<10 minutes) treatment
Aspirin Nitroglycerin
Check Vital Physical If O2 sat<94% Pain
IV Access 160–325 mg Sublingual or
Signs Exam Start Oxygen (If not already taken) Control spray
Activate Cardiac Cardiac Marker Chest X-ray
Cath Lab 12–Lead ECG
Levels (<30 mins)
ECG Interpretation**
ST-elevation MI (STEMI) High-risk unstable angina/non-ST-elevation Low-/Intermediate-risk ACS
Start adjunctive therapies
MI (UA/NSTEMI)
Consider admission to ED chest pain unit
as indicated or to appropriate bed and follow:
Do not delay reperfusion Serial cardiac markers (including troponin)
Troponin elevated or high-risk patient Repeat ECG/continuous ST-segment monitoring
Consider early invasive strategy if: Consider noninvasive diagnostic test
Refractory ischemic chest discomfort
Time from onset Recument/persistent ST deviation
of symptoms
>12 Ventricular tachycardia
hours Develops 1 or more:
≤ 12 hours? Hemodynamic instability
Signs of heart failure Clinical high-risk features
Dynamic ECG chages
consistent with ischemia
Troponin elevated
Start adjunctive treatments as indicated
≤12 Nitroglycerin
hours Heparin (UFH or LMWH)
Consider: PO β-blockers
Consider: Clopidogrel Abnormal diagnostic
Consider: Glycoprotein llb/llla inhibitor noninvasive imaging or
physiologic testing?
Reperfusion goals:
Door-to-balloon inflation (PCI)*** Admit to monitored bed Assess risk status Continue
goal of 90 minutes ASA heparin, and other therapies as indicated If no evidence of ischemia or
Door-to-needle (fibrinolysis) ACE inhibitor/ARB; HMG CoA reductase inhibitor (statin therapy) infarction by testing, can
goal of 30 minutes Not at high risk: cardiology to risk stratity discharge with follow-up
* O’Connor RE, Brady W, Brooks SC, Diercks D, Egan J, Ghaemmaghami C, Menon V, O’Neil BJ, Travers AH, Yannopoulos D. “Part 10: acute coronary syndromes: 2010 American Heart Association Guidelines for
Cardiopulmonary Resuscitation and Emergency Cardiovascular Care”. Circulation. 2010;122(suppl 3):S787-S817. http://circ.ahajoumals.org/content/122/18_suppl_3/S787
**Afolabi BA, Novaro GM, Pinski SL, Fromkin KR, Bush HS. Use of the prehoapital ECG improves door to balloon times in ST segment elevation myocardial infarction irrespective of time of day or day of week. Emerg Med J. 2007;24:588-591
*** O’Connor, RE AL, Ali, brady , WJ, Ghaemmaghami CA, Menon V, Welsford M, shuster M. . Part 9: acute coronary syndromes: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation
and Emergency Cardiovascular Care. Circulation 2015;132(suppl2):S483-S500
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020.
If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document. Version 2018.02.a
© ACLS Training Center 877-560-2940 support@acls.net
Complete your ACLS recertification online with the highest quality course at http://www.acls.net and use promo code PDF2016 during checkout for 15% off.
Tachycardia With a
Pulse Algorithm
Assess appropriateness for clinical condition.
Heart rate typically ≥ 150/min if tachyarrhythmia.
Identify and Treat Underlying Cause
Maintain patient airway; assist breathing as necessary
Oxygen (if O2 sat < 94%)
Cardiac monitor to identify rhythm; monitor blood pressure and oximetry
Persistent Tachyarrhythmia Causing:
Synchronized
Hypotension? Cardioversion*
Acutely altered mental status? Consider sedation
Signs of shock? If regular narrow complex,
Ischemic chest discomfort? consider adenosine
Acute heart failure?
IV access and 12–lead ECG if available.
Consider adenosine only if regular
Wide QRS? and monomorphic.
0.12 second Consider antiarrhythmic infusion.
Consider expert consultation.
IV access and 12–lead ECG if available.
Vagal maneuvers.
Adenosine (if regular)
β-Blocker or calcium channel blocker.
Consider expert consultation.
Doses/Details Adenosine IV Dose: Amiodarone IV Dose:
Synchronized First dose : 6 mg rapid IV push; First dose : 150 mg over 10 minutes.
Cardioversion** follow with NS flush.
Repeat as needed if VT recurs. Follow
Second dose : 12 mg if required by maintenance infusion of 1 mg/min
Initial recommended doses: for first 6 hours.
Narrow regular : 50–100 J Antiarrhythmic Infusions
Narrow irregular : 120–200 J for Stable Wide-QRS Sotalol IV Dose:
biphasic or 200 J monophasic Tachycardia
Wide regular : 100 J
Wide irregular : Defibrillation
Procainamide IV Dose: 100 mg (1.5 mg/kg) over 5 minutes.
Avoid if prolonged QT.
dose (not synchronized)
20-50 mg/min until arrhythmia
suppressed, hypotension ensues, QRS
duration increases > 50% or
maximum dose 17 mg/kg given.
Maintenance infusion: 1–4 mg/min.
Avoid if prolonged QT or CHF.
* Link MS, Atkins DL, Passman RS, Halperin HR, SAmson RA, White RD, Cudnik MT, Berg MD, Kudenchuk PJ, Kerbenchuk PJ, Kerber RE. “Part 6: electrical therapies: automated external defibrillators,
defibrillation, cardioversion, and pacing: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care”. Circulation. 2010;122(suppl 3):
S706-S719. http://circ.ahajournals.org/content/122/18_suppl_3/S706
** Scholten M, Szili-Torok T, Klootwijk P, Jordaens L, Comparison of monophasic and biphasic shocks for transthoracic cardioversion of atrial fibrillation. Heart 2003;89:1032-1034
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020.
If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document. Version 2018.02.a
© ACLS Training Center 877-560-2940 support@acls.net
Complete your ACLS recertification online with the highest quality course at http://www.acls.net and use promo code PDF2016 during checkout for 15% off.
Bradycardia With
a Pulse Algorithm
Assess appropriateness for clinical condition.
Heart rate typically < 50/min if bradyarrhythmia.
Identify and treat underlying cause
Maintain patent airway; assist breathing as necessary*
Oxygen (if hypoxemic)
Cardiac monitor to identify rhythm; monitor blood pressure and oximetry
IV access
12–Lead ECG if available; don’t delay therapy
Persistent bradyarrhythmia causing:
Monitor Hypotension?
and Acutely altered mental status?
Signs of shock?
observe
Ischemic chest discomfort?
Acute heart failure?
Atropine IV Dose:
First dose: 0.5 mg bolus
Repeat every 3–5 minutes
Maximum: 3 mg
If atropine ineffective:
Transcutaneous pacing**
OR
Dopamine IV infusion:
2–20 mcg/kg per minute
OR
Epinephrine IV infusion:
2–10 mcg per minute
Consider:
Expert consultation
Transvenous pacing
* Dorges V, Wenzel V, Knacke P, Gerlach K, Comparison of different airway management strategies to ventilate apneic, nonpreoxygenated patients. Crit Care Med. 2003;31:800-804
** Link MS, Atkins DL, Passman RS, Halperin HR, Samson RA, White RD, Cudnik MT, Berg MD, Kudenchuk PJ, Kerber RE. “Part 6: electrical therapies: automated external defibrillators, defillation, cardioversion, and pacing:
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care”. Circulation. 2010; 122(suppl 3):S706-S719. http://circ.ahajournals.org/content/122/18_suppl_3/S706
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020.
If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document. Version 2018.02.a
© ACLS Training Center 877-560-2940 support@acls.net
Complete your ACLS recertification online with the highest quality course at http://www.acls.net and use promo code PDF2016 during checkout for 15% off.
Immediate Post-Cardiac
Arrest Care Algorithm
Return of Spontaneous Circulation (ROSC)*
Optimize Ventilation and
Oxygenation Treat Hypotension (SBP < 90 mm Hg)
Maintain oxygen saturation 94% IV/IO bolus
Consider advanced airway Vasopressor infusion
waveform capnography Consider treatable causes
Do not hyperventilate 12-Lead ECG
Follow Commands ?
Induced Hypothermia**
Cardiac Catheterization Laboratory
Advanced Critical Care
Doses/Details Epinephrine IV Dopamine IV
Infusion Infusion
0.1–0.5 mcg/kg per minute 2–20 mcg/kg per minute
Ventilation/Oxygenation (in 70-kg adult: 7-35 mcg
per minute)
Avoid excessive ventilation Norepinephrine
Start at 10 94% breaths/min IV Infusion
and titrate to target PETCO2 Reversible Causes
of 35–40 mm Hg.
When feasible, titrate FIO2 0.1–0.5 mcg/kg per minute
to minimum necessary to Hypovolemia (in 70–kg adult: 7–35mcg
achieve SpO2 ≥ 94%. Hypoxia per minute)
Hydrogen ion (acidosis)
Hypo-/Hyperkalemia
IV Bolus Hypothermia
Tension pneumothorax
1–2 L normal saline or Tamponade, cardiac
lactated Ringer’s. Toxins
If inducing hypothermia, Thrombosis, pulmonary
may use 4°C fluid. Thrombosis, coronary
* Sasson C, Rogers MA, Dahl J, Kellermann AL. Predictors of survival from out of hospital cardiac arrest: a systematic review and metanalysis Circ Cardiovasc Qual Outcomes. 2010;3:63-81.
** Bruel C, Parienti JJ, Marie W, Arrot X, Mild hypothermia during advanced life support, a preliminary study in out of hospital cardiac arrest. Crit Care. 2008;12: R31
*** Callaway CW, Donnino MW, Fink EL, Geocadin RG, Golan E, Kern KB, Leary M, Meurer WJ, Peberdy MA, Thompson TM, Zimmerman JL. Part 8: post-cardiac arrest care: 2015 American Heart Association
Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015;132(suppl2):S465-S482
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020.
If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document. Version 2018.02.a
© ACLS Training Center 877-560-2940 support@acls.net
Complete your ACLS recertification online with the highest quality course at http://www.acls.net and use promo code PDF2016 during checkout for 15% off.
Stroke Assessment
The Cincinnati Prehospital Stroke Scale
Facial Droop
(have patient show teeth or smile)
NORMAL ABNORMAL
Both sides of face move equally. One side of face does not move
as well as the other side.
Arm Drift
(patient closes eyes and extends both arms straight out, with palms up for 10 seconds)
NORMAL ABNORMAL
Both arms move the same or both One arm does not move or one
arms do not move at all. arm drifts down compared
with the other.
Abnormal Speech
(have the patient say “you can’t teach an old dog new tricks”)
Normal - Patient uses correct Abnormal - Patient slurs
words with no slurring. words, uses the wrong words,
or is unable to speak.
If any 1 of these 3 signs is abnormal, the probability of a stroke is 72%
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020.
If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document. Version 2018.02.a
© ACLS Training Center 877-560-2940 support@acls.net
Complete your ACLS recertification online with the highest quality course at http://www.acls.net and use promo code PDF2016 during checkout for 15% off.
Suspected Stroke Algorithm:
Goals for Management of Stroke
Identify Signs and Symptoms of Possible Stroke
Active Emergency Response
Critical EMS assessments and actions
Support ABCs: Establish time of
Perform prehospital Triage to Activate stroke
Give Oxygen Check glucose symptom onset Alert hospital
stroke assessment stroke center team
if indicated (last normal)
NINDS TIME GOALS
If onset >3 hours consider triage to hospital
with interventional capabilities for stroke.
Immediate general assessment and stabilization* Immediate neurologic assessment by stroke team
or designee
Assess ABCs, vital signs
Provide oxygen if O sat <94%
2
Obtain IV access and perform laboratory Review patient history
assessments Establish time of symptom onset or last
Check glucose; treat if indicated known normal
Obtain 12–lead ECG Perform neurologic examination (NIH Stroke
Scale or Canadian Neurological Scale)
Perform neurologic screening assessment
Order emergent CT without contrast
Does CT Scan Show Hemorrhage?
No hemorrhage Hemorrhage
Probably acute ischemic stroke; Consult neurologist or neurosurgeon;
consider fibrinolytic therapy consider transfer if not available.
Check fibrinolytic exclusions
Repeat neurologic exam: are deficits Begin stroke or hemorrhage
rapidly improving to normal? pathway
Admit to stroke unit or
intensive care unit
Patient remains candidate Not a candidate
for fibrinolytic therapy? Administer aspirin
Candidate*
Begin post-rTPA stroke pathway
Review risks/benefits with patient & family. Aggressively monitor:
If acceptable: BP per protocol
Give rTPA** For neurologic deterioration
No anticoagulants or antiplatelet Emergent admission to stroke
treatment for 24 hours unit or intensive care unit
* Jauch EC, Cucchiara B, Adeoye O, Meurer W, Brice J, Chan Y-F, Gentile N, Hazinski MF. “ Part 11: adult stroke: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitationand Emergency Cardiovascular
Care” . Circulation. 2010;122(suppl 3):S818-S828. http://circ.ahajournals.org/content/122/18_suppl_3/S818
** Tissue Plasminogen Activator for Acute Ischemic Stroke. N Engl J Med. 1995:333(24)1581-1587
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020.
If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document. Version 2018.02.a
© ACLS Training Center 877-560-2940 support@acls.net
Complete your ACLS recertification online with the highest quality course at http://www.acls.net and use promo code PDF2016 during checkout for 15% off.
You might also like
- A Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Checklist & Algoritma ACLSDocument16 pagesChecklist & Algoritma ACLSNadhif JovaldyNo ratings yet
- Advanced Paediatric Life Support - A0 PDFDocument1 pageAdvanced Paediatric Life Support - A0 PDFiulia-uroNo ratings yet
- ACLS Written 2006 Precourse Self AssessmentDocument14 pagesACLS Written 2006 Precourse Self AssessmentmonickamsNo ratings yet
- ACLS and MegacodeDocument33 pagesACLS and MegacodeMark Joseph100% (1)
- ToxidromesDocument1 pageToxidromesMayer Rosenberg100% (7)
- AclsDocument85 pagesAclsJulia CostaNo ratings yet
- Faculty Guide For ACLS Instructor Course (PDF Library)Document58 pagesFaculty Guide For ACLS Instructor Course (PDF Library)Ogine L. LoNo ratings yet
- ALS Protocols Complete-RAPID CITY PDFDocument413 pagesALS Protocols Complete-RAPID CITY PDFCh WuNo ratings yet
- ACLS QuizletDocument7 pagesACLS Quizletek.9006001No ratings yet
- Acls Review 2015Document29 pagesAcls Review 2015JB Reyes100% (2)
- ACLS Study Guide: Ecg Strip InterpretationDocument12 pagesACLS Study Guide: Ecg Strip InterpretationMariana Berger100% (1)
- Acls Pretest Answer Key: Rhythm Identification (Part I)Document3 pagesAcls Pretest Answer Key: Rhythm Identification (Part I)aditNo ratings yet
- American Heart Association Guidelines For CPR 2015: Wanida Chongarunngamsang, MD. Faculty of Srinakarinwirot UniversityDocument49 pagesAmerican Heart Association Guidelines For CPR 2015: Wanida Chongarunngamsang, MD. Faculty of Srinakarinwirot UniversityZulkarnainBustamamNo ratings yet
- CPR ACLS Study GuideDocument18 pagesCPR ACLS Study GuideJohn Phamacy100% (1)
- American Heart Association Acls Post Test AnswersDocument4 pagesAmerican Heart Association Acls Post Test AnswersArun Jude Alphonse0% (9)
- AclsDocument11 pagesAclsdyah rahayu hutamiNo ratings yet
- AclsDocument62 pagesAclsAlemayehu beharuNo ratings yet
- Acls DrugsDocument5 pagesAcls DrugsDebby Christiana SNo ratings yet
- 2016 Updated ACLS HandoutsDocument24 pages2016 Updated ACLS Handoutskarenjlazarus86% (14)
- Scape Vs FospeDocument5 pagesScape Vs FospeDr. FarhanNo ratings yet
- ACLS AlgorithmsDocument4 pagesACLS Algorithmsmonickams100% (1)
- Acls Study Guide 2016Document2 pagesAcls Study Guide 2016Caridad RodasNo ratings yet
- In Is: Question 1 (1 Point)Document7 pagesIn Is: Question 1 (1 Point)schwad1No ratings yet
- ACLS Training - Most Important Points To RememberDocument5 pagesACLS Training - Most Important Points To RememberEman ElzeftawyNo ratings yet
- Rhythm Recognition - ACLS Medical Training 1Document9 pagesRhythm Recognition - ACLS Medical Training 1Catalina BorquezNo ratings yet
- Megacode Testing Checklist Scenarios 4-7-10 Tachycardia, VF, PEA, PC...Document1 pageMegacode Testing Checklist Scenarios 4-7-10 Tachycardia, VF, PEA, PC...krgduraiNo ratings yet
- Megacode Testing Checklist: Scenarios 1/3/8 Bradycardia Pulseless VT PEA PCACDocument6 pagesMegacode Testing Checklist: Scenarios 1/3/8 Bradycardia Pulseless VT PEA PCACberril_fannyNo ratings yet
- Defibrillatorppt 131028115457 Phpapp01Document41 pagesDefibrillatorppt 131028115457 Phpapp01Simon JosanNo ratings yet
- ACLS ChartDocument1 pageACLS ChartJev DespiNo ratings yet
- (Advanced Cardiac Life Support) : ACLS Algorithms 2018Document18 pages(Advanced Cardiac Life Support) : ACLS Algorithms 2018cristina100% (1)
- AHA ELearning ACLS Precourse Self-Assessment and Precourse WorkDocument1 pageAHA ELearning ACLS Precourse Self-Assessment and Precourse Work9kjsntkrzcNo ratings yet
- ACLS Study GuideDocument28 pagesACLS Study GuideNicole Berry100% (1)
- 2010 Integrated Updated Circulation ACLS Acute Coronary Syndromes AlgorithmDocument1 page2010 Integrated Updated Circulation ACLS Acute Coronary Syndromes Algorithmms_lezahNo ratings yet
- AHA ACLS Written Test: Ready To Study? Start With FlashcardsDocument8 pagesAHA ACLS Written Test: Ready To Study? Start With FlashcardssallyNo ratings yet
- ACLS PharmacologyDocument5 pagesACLS PharmacologyKuruva MallikarjunaNo ratings yet
- ACLS ScenarioDocument21 pagesACLS Scenariomarves15No ratings yet
- Pepp Als PretestDocument4 pagesPepp Als PretestDave BoppNo ratings yet
- Advanced Cardiac Life SupportDocument8 pagesAdvanced Cardiac Life Supportcool kipsNo ratings yet
- ACLS Protocols Pocket VersionDocument2 pagesACLS Protocols Pocket Versionjohndoe1995No ratings yet
- Basic Life Support and Advanced Cardiovascular Life SupportDocument90 pagesBasic Life Support and Advanced Cardiovascular Life SupportRakhshanda khan100% (1)
- AHA ACLS Written Test: Ready To Study? Start With FlashcardsDocument8 pagesAHA ACLS Written Test: Ready To Study? Start With Flashcardssally100% (1)
- Approach To ACLS RhythmDocument150 pagesApproach To ACLS RhythmChristine Bernadette Rapal Bollong100% (2)
- ACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)Document11 pagesACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)김민길100% (2)
- Acls Study Guide 2016Document2 pagesAcls Study Guide 2016nova939100% (2)
- ACLS Simulation ScenariosDocument14 pagesACLS Simulation ScenariosVanessa HermioneNo ratings yet
- DIT High Yield Questions PDFDocument13 pagesDIT High Yield Questions PDFjoshNo ratings yet
- ACLS Pretest Exam AnnotatedDocument21 pagesACLS Pretest Exam AnnotatedMOLLYNo ratings yet
- ACLS Test Sinus BradycardiaDocument1 pageACLS Test Sinus BradycardiaFiya Sahrul0% (1)
- ACLS Precourse Test AnswersDocument60 pagesACLS Precourse Test AnswersTip Piraya60% (5)
- Test 2 Review 2020Document7 pagesTest 2 Review 2020Cherie L. MilburnNo ratings yet
- LSCPR Pals Study Guide 2020Document57 pagesLSCPR Pals Study Guide 2020Juan Ma100% (1)
- ACLS Class Packet 2015Document9 pagesACLS Class Packet 2015Chi Wiin100% (3)
- 9th Edition Compendium For Update FINALDocument6 pages9th Edition Compendium For Update FINALErvina Lie100% (1)
- PALS Practice 1 Hypovolemic ShockDocument64 pagesPALS Practice 1 Hypovolemic ShockGlen LazarusNo ratings yet
- Advanced Cardiac Life Support Quick Study Guide 2015 Updated GuidelinesFrom EverandAdvanced Cardiac Life Support Quick Study Guide 2015 Updated GuidelinesRating: 4 out of 5 stars4/5 (6)
- A Simple Guide to Abdominal Aortic Aneurysm, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Abdominal Aortic Aneurysm, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Pediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesFrom EverandPediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesRating: 5 out of 5 stars5/5 (2)
- Ecg PicsDocument9 pagesEcg PicsDr. XNo ratings yet
- Hospital Equipment. Research ReportDocument6 pagesHospital Equipment. Research ReportYazan Al JabariNo ratings yet
- Basic Life Support & Medical EmergencyDocument39 pagesBasic Life Support & Medical EmergencyRoyle LolingNo ratings yet
- CPR AED PowerPointDocument106 pagesCPR AED PowerPointrajesh.880889No ratings yet
- Ec8073 Medical Electronics Question BankDocument8 pagesEc8073 Medical Electronics Question BankpurushothsathaNo ratings yet
- Тема 12 Англ Resuscitation Basic ConceptsDocument11 pagesТема 12 Англ Resuscitation Basic ConceptsMihika GuptaNo ratings yet
- Radio PillDocument41 pagesRadio PillAadhithya Priya100% (2)
- Ask Questions About C.P.RDocument5 pagesAsk Questions About C.P.RAnonymous FCOOcnNo ratings yet
- DR Sujata: Professor Dept - of Anaesthesiology &critical Care Ucms & GTB HospitalDocument53 pagesDR Sujata: Professor Dept - of Anaesthesiology &critical Care Ucms & GTB HospitalMiniNo ratings yet
- Topnotch Emergency Medicine For MoonlightersDocument129 pagesTopnotch Emergency Medicine For MoonlightersTEAM K 1920No ratings yet
- Ev Battery System: SectionDocument272 pagesEv Battery System: Sectionulisse_100% (1)
- Piis0300957220301428 PDFDocument5 pagesPiis0300957220301428 PDFDabeet MoncayoNo ratings yet
- User Manual: Shenzhen Biocare Bio-Medical Equipment Co., LTDDocument81 pagesUser Manual: Shenzhen Biocare Bio-Medical Equipment Co., LTDAnthony AkiliboyNo ratings yet
- TestDocument11 pagesTestzenagit123456100% (1)
- Mindray MEC 2000 Monitor de Paciente Manual de UsuarioDocument273 pagesMindray MEC 2000 Monitor de Paciente Manual de UsuarioPablo Libretti100% (1)
- Resusci Anne Advanced Skilltrainer - User Guide Link and Paddle VersionDocument32 pagesResusci Anne Advanced Skilltrainer - User Guide Link and Paddle VersionDani ReynaldoNo ratings yet
- IPL User ManualDocument22 pagesIPL User ManualSwandana Hersa PradikaNo ratings yet
- MEFA Day 1Document128 pagesMEFA Day 1Peter Maxwell DGNo ratings yet
- Zoll AED Plus Defibrillator - Quick User GuideDocument2 pagesZoll AED Plus Defibrillator - Quick User GuideBolawali KiNo ratings yet
- 9194 2014 Nissan Leaf Service RepairDocument16 pages9194 2014 Nissan Leaf Service RepairEngr Ko VictorNo ratings yet
- Emt National Practice ExamDocument42 pagesEmt National Practice Examdebbiemedic3557100% (12)
- Basic Life Support Field GuideDocument56 pagesBasic Life Support Field GuidelmaoheartsNo ratings yet
- Cardioline Ar600 - User ManualDocument36 pagesCardioline Ar600 - User ManualDavid SanchezNo ratings yet
- 70 2008 9621 8Document24 pages70 2008 9621 8asarolicNo ratings yet
- Ark AngelDocument172 pagesArk AngelCrina Serban67% (3)
- Emergency CartDocument23 pagesEmergency CartJennifer B. GarciaNo ratings yet
- Seca Ct3000i User ManualDocument50 pagesSeca Ct3000i User ManualLaiq Ahmed0% (1)
- DevicesDocument36 pagesDevicesKUMUTHA MALAR A/P PARMESWARANNo ratings yet