Professional Documents
Culture Documents
Prothrombin and Factor V Mutations in Women With A
Uploaded by
Alfa FebriandaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Prothrombin and Factor V Mutations in Women With A
Uploaded by
Alfa FebriandaCopyright:
Available Formats
The Ne w E n g l a nd Jo u r n a l o f Me d ic i ne
PROTHROMBIN AND FACTOR V MUTATIONS IN WOMEN WITH A HISTORY OF
THROMBOSIS DURING PREGNANCY AND THE PUERPERIUM
ANDREA GERHARDT, M.D., RÜDIGER EBERHARD SCHARF, M.D., MATTHIAS WILHELM BECKMANN, M.D., SABINE STRUVE, B.S.,
HANS GEORG BENDER, M.D., MICHAEL PILLNY, M.D., WILHELM SANDMANN, M.D., AND RAINER BERND ZOTZ, M.D.
ABSTRACT cy and the puerperium.5 Thus, venous thromboem-
Background Venous thromboembolism is a lead- bolism is an uncommon but leading cause of morbid-
ing cause of morbidity and mortality during preg- ity and mortality among women during this period.
nancy and the puerperium. However, the role of mu- During normal pregnancy, the plasma concentra-
tations in the prothrombin and factor V genes and tions and activities of several proteins involved in
other thrombophilic abnormalities as risk factors for blood coagulation and fibrinolysis change. These
thromboembolism in women during pregnancy and changes may promote coagulation, decrease antico-
the puerperium is not known. agulation, and inhibit fibrinolysis5-7 and thus may in-
Methods In a study of 119 women with a history of crease the risk of thromboembolic events, especially
venous thromboembolism during pregnancy and the
puerperium and 233 age-matched normal women,
among pregnant women who have acquired or ge-
we measured the activity of antithrombin, protein C, netic risk factors for thrombosis.5,8-10
protein S, and lupus anticoagulant. We also per- Among the genetically determined changes, the
formed genetic analyses to detect the G1691A mu- mutation in the gene encoding factor V at nucleo-
tation in the factor V gene (factor V Leiden), the tide 1691 (G1691A, referred to as factor V Leiden)
G20210A mutation in the prothrombin gene, and the is the most common inherited abnormality in patients
C677T mutation in the methylenetetrahydrofolate re- with thromboembolic disease, occurring in 20 percent
ductase gene. Blood samples were obtained at least of patients with a first episode of venous thrombosis
three months post partum or after the cessation of and up to 50 percent of those with recurrent venous
lactation. thrombosis.9 A guanine-to-adenine mutation in the
Results Among the women with a history of ve- prothrombin gene, G20210A, associated with elevat-
nous thromboembolism, the prevalence of factor V
Leiden was 43.7 percent, as compared with 7.7 per- ed plasma prothrombin concentrations and an in-
cent among the normal women (relative risk of ve- creased risk of venous thrombosis, has been iden-
nous thromboembolism, 9.3; 95 percent confidence tified.11 In addition, homozygosity for a common
interval, 5.1 to 16.9); that of the G20210A prothrom- cytosine-to-thymidine mutation in the gene encoding
bin-gene mutation, 16.9 percent as compared with 5,10-methylenetetrahydrofolate reductase (MTHFR),
1.3 percent (relative risk, 15.2; 95 percent confidence C677T, is associated with high plasma homocysteine
interval, 4.2 to 52.6); and that of both factor V Leiden concentrations and venous thrombosis,12-14 although
and the G20210A prothrombin-gene mutation, 9.3 per- this association has been questioned by some inves-
cent as compared with 0 (estimated odds ratio, 107). tigators.15
Assuming an overall risk of 1 in 1500 pregnancies, the
To date, there are limited data on the role of these
risk of thrombosis among carriers of factor V Leiden
was 0.2 percent, among carriers of the G20210A pro- genetic abnormalities in causing the venous throm-
thrombin-gene mutation, 0.5 percent, and among car- boembolism associated with pregnancy and the puer-
riers of both defects, 4.6 percent, as calculated in a perium.5,8,10,16 We studied the relative risk of venous
multivariate analysis. thromboembolism associated with these genetic mark-
Conclusions The G20210A prothrombin-gene mu- ers and other thrombophilic abnormalities in preg-
tation and factor V Leiden individually are associated nant and puerperal women.
with an increased risk of venous thromboembolism
during pregnancy and the puerperium, and the risk METHODS
among women with both mutations is dispropor- Subjects
tionately higher than that among women with only
one mutation. (N Engl J Med 2000;342:374-80.) We studied 119 consecutive women with a history of venous
thromboembolism during pregnancy and the puerperium (up to
©2000, Massachusetts Medical Society.
six weeks post partum) and 233 normal women. The women with
a history of thromboembolism were referred from local hospitals
to the Düsseldorf University Medical Center (Düsseldorf, Ger-
T
HE risk of venous thromboembolism is five
times as high among pregnant women as
among nonpregnant women of similar
From the Departments of Hemostasis and Transfusion Medicine (A.G.,
age.1-3 Estimates of the incidence of preg- R.E.S., R.B.Z.), Obstetrics and Gynecology (M.W.B., S.S., H.G.B.), and
nancy-associated venous thromboembolism vary from Vascular Surgery and Kidney Transplantation (M.P., W.S.), Heinrich Heine
1 in 1000 to 1 in 2000 deliveries.4 Thromboembolic University Medical Center, Düsseldorf, Germany. Address reprint requests
to Dr. Zotz at the Institut für Haemostaseologie und Transfusionsmedizin,
complications, including pulmonary embolism, are Heinrich Heine Universität, Moorenstr. 5, D-40225 Düsseldorf, Germany,
major causes of death among women during pregnan- or at zotz@med.uni-duesseldorf.de.
374 · Febr u ar y 10 , 2 0 0 0
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2015. For personal use only. No other uses without permission.
Copyright © 2000 Massachusetts Medical Society. All rights reserved.
P R OT H R O MBIN AND FAC TOR V MUTAT IONS IN WOMEN WITH A H ISTORY OF TH ROMBOSIS D UR ING PR EGNANCY
many) for treatment of venous thromboembolism between Janu- with the DVV test and DVV confirm test (American Diagnostica,
ary 1990 and December 1998 and were seen again during 1999 Greenwich, Conn.).
for determination of the presence or absence of genetic risk fac- The criteria for the diagnosis of deficiencies of protein C, pro-
tors and other thrombophilic abnormalities. In both the women tein S, and antithrombin were activity levels below the lower limit
with a history of thromboembolism and the normal women, blood of normal (cutoff, 95th percentile), as determined in blood sam-
samples were obtained at least three months post partum or three ples obtained from the 233 normal women. The lower limits of
months after the cessation of lactation to rule out any pregnancy- normal were 70 percent for protein C activity, 75 percent for pro-
related alterations of coagulation and fibrinolysis. Eight of the 119 tein C activity after the exclusion of carriers of factor V Leiden,
women with a history of thromboembolism were receiving long- 55 percent for protein S activity, 65 percent for protein S activity
term oral anticoagulant therapy at the time of blood sampling; after the exclusion of normal women taking an oral contraceptive
30 of the women with a history of thromboembolism and 92 of and carriers of factor V Leiden, and 80 percent for antithrombin
the normal women were taking an oral contraceptive at this time. activity (with and without oral-contraceptive therapy).
None of the women had overt evidence of autoimmune or neo-
plastic disease. Thirteen women with a history of thromboembo- Genetic Analysis
lism had one or more pregnancy-associated complications: gesta- DNA was extracted from peripheral-blood leukocytes according
tional hypertension (3 women), immobilization due to preterm to standard protocols with the use of the Chelex system (Bio-Rad,
labor (13 women), and twin gestation (2 women). The other 106 Munich, Germany). The presence or absence of factor V Leiden
women with a history of thromboembolism had normal singleton was determined by allele-specific restriction-enzyme analysis. 22 For
pregnancies except for the occurrence of the thrombotic event. In confirmation of the genotypes, an oligonucleotide-ligation assay
four women, none of whom had pregnancy-associated complica- was performed.23 The results of the oligonucleotide-ligation assay
tions, the pregnancy resulted from in vitro fertilization and em- were in 100 percent concordance with the results of genotypic
bryo transfer. Of the 119 women with a history of thromboem- analysis, as determined by an allele-specific restriction-enzyme as-
bolism, 81 had vaginal deliveries (68 percent) and 38 delivered by say. The G20210A prothrombin-gene mutation was identified by
cesarean section (32 percent). allele-specific restriction-enzyme analysis.11 Screening for the pres-
All the women with a history of thromboembolism had an ob- ence of the C677T MTHFR polymorphism was performed by the
jectively diagnosed episode of deep venous thrombosis or pulmo- method described by Frosst et al.12
nary embolism. Deep venous thrombosis was diagnosed by Dop-
pler ultrasonography or computed tomography during pregnancy Statistical Analysis
and by venography or Doppler ultrasonography after delivery. In
The SAS statistical package (version 6.12, SAS Institute, Cary,
77 of these women (65 percent), thrombectomy was performed N.C.) was used for all statistical analyses. Depending on the type
with complete removal of the thrombus for the prevention of pul- of data, the Wilcoxon rank-sum test, chi-square analysis, or Fish-
monary embolism, thrombus extension, and the postphlebitic syn- er’s exact test (two-tailed) was used to assess the differences be-
drome. In particular, thrombectomy was performed if the throm- tween the groups. Multivariate analyses, including the calculation
bus extended into the iliac veins and the inferior caval vein or if of predictive values, were performed with the use of a stepwise
a floating thrombus was documented. The procedure was com- logistic-regression procedure. For the calculation of predictive val-
pleted with the creation of a temporary arteriovenous fistula, which ues, an incidence of 1 thromboembolic event in 1500 pregnancies
was removed three to six months later. The details and results of was assumed. The relative risk was estimated from the odds ratio.
this procedure have been reported elsewhere.17-20 Among these 77 Complete data were not available for all the women (e.g., the activ-
women, thrombectomy was performed in 39 (51 percent) during ities of protein C and protein S were not measured in women with
pregnancy and after delivery in 38 (49 percent). thromboembolism who were taking an oral anticoagulant).
The 233 normal women were recruited by the Heinrich Heine
University Blood Donation Center and matched with the women RESULTS
with a history of thromboembolism according to age. They were
from the same geographic region as the women with a history The characteristics of all the women are presented
of thromboembolism, but were unrelated to them. One hundred in Table 1. Among the 119 women with a history of
fifty-seven had previous pregnancies with no thromboembolic thromboembolism, 62 (52 percent) had deep venous
complications; 148 of these had a vaginal delivery (94 percent)
and 9 delivered by cesarean section (6 percent). thromboembolism during pregnancy (first trimester,
Personal histories to document the presence or absence of 14; second trimester, 13; third trimester, 35) and 57
thromboembolic disease were obtained from all the women with (48 percent) had thromboembolism in the postpar-
the use of a standardized questionnaire. This procedure has been tum period (vaginal delivery, 38; cesarean section,
evaluated previously.21 The study was performed in accordance with
the Helsinki Declaration, and written informed consent was given
19). In the 35 women with a history of thrombo-
by all the women. embolism during the third trimester, 11 (31 percent)
had a cesarean section followed immediately by throm-
Laboratory Tests bectomy. In 96 women, the venous thrombosis oc-
All the women were screened for inherited and acquired defects
curring during pregnancy or the puerperium was their
in blood coagulation. We determined the activities of antithrom- first thrombotic event, whereas in 23 women the ve-
bin, protein C, protein S, and lupus anticoagulant in plasma and nous thrombosis was a recurrent thrombotic event.
performed a genetic analysis to determine the presence or absence The prevalence of genetic risk factors did not differ
of factor V Leiden, the G20210A prothrombin-gene mutation, significantly between the women with a history of
and the C677T MTHFR mutation. The activities of plasma pro-
tein C and protein S were measured by a functional clotting assay thromboembolism who underwent thrombectomy
(Instrumentation Laboratory, Milan, Italy), and total protein S an- and those who did not or between the women with
tigen and free protein S antigen were measured by immunoelec- a history of thromboembolism who had no preg-
trophoresis (Boehringer Mannheim, Mannheim, Germany). Plasma nancy-associated complications and those with throm-
antithrombin activity was measured with the use of Berichrom
(Dade Behring, Liederbach, Germany). Resistance to activated pro-
boembolism who had pregnancy-associated compli-
tein C was determined with a kit (Coatest APC Resistance, Chro- cations. We therefore do not present separate analyses
mogenix, Mölndal, Sweden). Lupus anticoagulant was measured of the results.
Vol ume 342 Numb e r 6 · 375
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2015. For personal use only. No other uses without permission.
Copyright © 2000 Massachusetts Medical Society. All rights reserved.
The Ne w E n g l a nd Jo u r n a l o f Me d ic i ne
Prevalence of Inherited Risk Factors
TABLE 1. CHARACTERISTICS OF THE WOMEN WITH A HISTORY
OF VENOUS THROMBOEMBOLISM DURING PREGNANCY AND
The prevalence of factor V Leiden was significantly
THE PUERPERIUM AND THE NORMAL WOMEN. higher among the women with a history of throm-
boembolism than among the normal women (Tables
2 and 3). Similarly, the prevalence of the G20210A
WOMEN WITH
HISTORY OF NORMAL prothrombin-gene mutation was significantly higher
THROMBOEMBOLISM WOMEN among the women with a history of thromboembo-
CHARACTERISTIC (N=119) (N=233)
lism than among the normal women (Tables 2 and
Age at the time of thrombosis — yr NA* 3). Of the women with a history of venous throm-
Median 27
Range 13–45
boembolism who had factor V Leiden, 5 were homo-
Age at the time of blood sampling — yr zygous and 47 were heterozygous for the mutation;
Median 34 34 all of the women with the G20210A prothrombin-
Range 14–67 19–65 gene mutation were heterozygous for the mutation.
Use of oral contraceptives (current or 69 (58.0) 137 (58.8) Eleven of 118 women with a history of thrombo-
previous) — no. (%)†
Cigarette smoking (current or previous) 69 (58.0) 156 (67.0)
embolism (9.3 percent) had both factor V Leiden
— no. (%)† and the G20210A prothrombin-gene mutation (es-
Body-mass index >30 — no. (%)‡ 17 (14.3) 15 (6.4) timated odds ratio for thromboembolism during
pregnancy and the puerperium, 107). Since no nor-
*NA denotes not applicable.
mal women had this combined defect, the estimated
†The difference between the two groups was not significant.
odds ratio was calculated on the basis of the proba-
‡The relative risk of venous thromboembolism associated with a body-
mass index (the weight in kilograms divided by the square of the height in bility of a combined defect in the normal women
meters) of more than 30 was 2.3 (95 percent confidence interval, 1.0 to (7.7 percent¬1.3 percent=0.10 percent).
5.2; P=0.04).
The prevalence of the other risk factors for throm-
bophilia (deficiencies of antithrombin, protein C, and
protein S) was 24.8 percent in the women with a his-
tory of thromboembolism and 11.4 percent in the
normal women. A total of 19.3 percent of the women
with a history of thromboembolism (23 of 119) had
an antithrombin deficiency (<80 percent of normal
TABLE 2. PREVALENCE OF HEREDITARY COAGULATION DEFECTS.*
WOMEN WITH
HISTORY OF NORMAL
THROMBOEMBOLISM WOMEN
COAGULATION DEFECT (N=119) (N=233) P VALUE
% (no. with defect/total no.)
Factor V Leiden† 43.7 (52/119) 7.7 (18/233) <0.001
G20210A prothrombin-gene mutation‡ 16.9 (20/118) 1.3 (3/226) <0.001
677TT MTHFR genotype 9.6 (11/114) 9.4 (20/212) 0.95
Antithrombin deficiency (<80 percent of normal 19.3 (23/119) 2.6 (6/231) <0.001
activity)
Antithrombin deficiency (<80 percent of normal 6.7 (6/89) 1.5 (2/131) 0.06
activity) after exclusion of women taking oral
contraceptives
Protein C deficiency (<70 percent of normal activity) 14.2 (15/106) 3.9 (9/230) <0.001
Protein C deficiency (<75 percent of normal activity)§ 10.3 (6/58) 3.3 (7/212) 0.03
Protein S deficiency (<55 percent of normal activity) 12.4 (13/105) 4.8 (11/228) 0.01
Protein S deficiency (<65 percent of normal activity)¶ 7.8 (4/51) 6.6 (8/121) 0.77
*Complete data were not available for all the women. Tests for antiphospholipid antibodies were
negative in all the women.
†Among the women with factor V Leiden who had thromboembolism, five were homozygous for
the mutation; none of the normal women were homozygous for the mutation.
‡None of the women with the prothrombin G20210A mutation were homozygous for the mutation.
§Carriers of factor V Leiden were excluded from the analysis.
¶Women who were taking an oral contraceptive and carriers of factor V Leiden were excluded from
the analysis.
376 · Febr u ar y 10 , 2 0 0 0
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2015. For personal use only. No other uses without permission.
Copyright © 2000 Massachusetts Medical Society. All rights reserved.
P R OT H R O MBIN AND FAC TOR V MUTAT IONS IN WOMEN WITH A H ISTORY OF TH ROMBOSIS D UR ING PR EGNANCY
TABLE 3. RELATIVE RISK OF VENOUS THROMBOEMBOLISM ASSOCIATED WITH HEREDITARY
COAGULATION DEFECTS.*
RISK FACTOR UNIVARIATE ANALYSIS MULTIVARIATE ANALYSIS†
RELATIVE RISK RELATIVE RISK
(95% CI) P VALUE (95% CI) P VALUE
Factor V Leiden 9.3 (5.1–16.9) <0.001 6.9 (3.3–15.2) <0.001
G20210A prothrombin-gene mutation 15.2 (4.2–52.6) <0.001 9.5 (2.1–66.7) 0.007
Antithrombin deficiency (<80 percent 4.7 (0.9–21.8) 0.06 10.4 (2.2–62.5) <0.001
of normal activity)‡
Protein C deficiency (<75 percent of 3.4 (1.1–10.5) 0.03 2.2 (0.8–6.1) 0.13
normal activity)§
*Univariate analyses were performed with the use of the chi-square test. Multivariate analyses were
performed with the use of the stepwise logistic-regression procedure. CI denotes confidence interval.
†All stepwise logistic-regression analyses were performed with the following variables: presence of
factor V Leiden; presence of prothrombin G20210A mutation; presence of the MTHFR 677TT geno-
type; low protein C, protein S, and antithrombin activity; body-mass index of more than 30; and use
of oral contraceptives. The P values indicate the significance of each risk factor independently.
‡Women who were taking an oral contraceptive were excluded from the univariate analysis.
§Carriers of factor V Leiden were excluded from the univariate analysis.
activity), as compared with 2.6 percent of the normal of normal activity) and the presence of factor V Lei-
women (6 of 231) (relative risk, 9.0; 95 percent con- den and the G20210A prothrombin-gene mutation
fidence interval, 3.5 to 22.7; P<0.001); a difference, could be identified as independent risk factors that
although not significant, persisted after the exclusion were predictive of thrombosis in the women with
of the women taking an oral contraceptive (Table 2). thromboembolism.
A total of 12.4 percent of the women with a history
of thromboembolism (13 of 105) and 4.8 percent of Predictors of Thrombosis in Pregnancy as Compared
with Those in the Puerperium
the normal women (11 of 228) had reduced protein
S activity (<55 percent of normal activity; relative risk, There was no significant difference in the prevalence
2.8; 95 percent confidence interval, 1.2 to 6.5; P= of factor V Leiden, the G20210A prothrombin-gene
0.01); this difference did not persist after the exclusion mutation, protein C deficiency, and protein S deficien-
of the women taking an oral contraceptive and the cy between the 62 women with a history of throm-
carriers of factor V Leiden (Table 2). A total of 14.2 boembolism during pregnancy and the 57 women
percent of the women with a history of thromboem- with a history of thromboembolism during the puer-
bolism (15 of 106) had protein C deficiency, as com- perium. There was a trend toward a higher prevalence
pared with 3.9 percent of the normal women (9 of of antithrombin deficiency among the women with
230) (relative risk, 4.0; 95 percent confidence interval, a history of venous thromboembolism in pregnancy
1.7 to 9.6; P<0.001). The difference persisted after than among the women with a history of thrombo-
the exclusion of the carriers of factor V Leiden (Table embolism during the puerperium (prevalence, 11.1
2). Among the women with a history of thromboem- percent vs. 2.3 percent; P=0.10). By contrast, the
bolism who had deficiencies of antithrombin, protein MTHFR 677TT genotype was predominantly asso-
C, and protein S, most had activity levels that ranged ciated with thrombosis in the puerperium (prevalence,
between 50 percent and 65 percent of normal activ- 30.0 percent among the women with thromboem-
ity. One woman with a history of thromboembolism bolism during the puerperium vs. 8.8 percent among
had an antithrombin activity of <50 percent, and two the women with thromboembolism during pregnan-
had a protein C activity of <50 percent, whereas none cy; P=0.04).
of the normal women had levels this low. There was no statistical difference with regard to
In a logistic-regression analysis in which adjust- the prevalence or relative risk of inherited risk factors
ments were made for age, body-mass index, and oral- between the women with a history of thromboem-
contraceptive use or nonuse (Table 3) and in which bolism who had vaginal deliveries and those who had
protein C deficiency, protein S deficiency, antithrom- cesarean deliveries.
bin deficiency, and presence of factor V Leiden,
Recurrent Venous Thromboembolism
the G20210A prothrombin-gene mutation, and the
677TT MTHFR genotype were included in the same The prevalence and relative risk of genetic risk fac-
model, only antithrombin deficiency (<80 percent tors among the women with a first episode of throm-
Vol ume 342 Numb e r 6 · 377
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2015. For personal use only. No other uses without permission.
Copyright © 2000 Massachusetts Medical Society. All rights reserved.
The Ne w E n g l a nd Jo u r n a l o f Me d ic i ne
TABLE 4. PREVALENCE AND RELATIVE RISK OF HEREDITARY COAGULATION DEFECTS IN WOMEN WITH FIRST OR RECURRENT
VENOUS THROMBOEMBOLISM AS COMPARED WITH NORMAL WOMEN.*
PREVALENCE AMONG PREVALENCE AMONG
PREVALENCE AMONG WOMEN WITH WOMEN WITH
NORMAL WOMEN FIRST EPISODE RELATIVE RISK RECURRENCE RELATIVE RISK P
CHARACTERISTIC (N=233) (N=79) (95% CI) (N=40) (95% CI) VALUE†
percent percent
Factor V Leiden 7.7 43.0 9.0 (4.7–17.4) 45.0 9.8 (4.4–21.5) 0.78
G20210A prothrombin-gene mutation 1.3 12.7 10.8 (2.9–40.3) 25.6 26.0 (6.7–98.6) 0.08
Factor V Leiden and G20210A pro- 0 7.6 69.0‡ 12.8 152.0‡ 0.37
thrombin-gene mutation
Antithrombin deficiency (<80 percent 2.6 14.1 6.2 (2.2–17.3) 30.0 16.1 (5.6–46.2) 0.04
of normal activity)
Antithrombin deficiency (<80 percent 1.5 5.0 3.4 (0.6–20.9) 10.3 7.4 (1.2–46.8) 0.40
of normal activity) after exclusion of
women taking oral contraceptives
Protein C deficiency (<70 percent of 3.9 8.5 2.3 (0.8–6.6) 26.5 8.8 (3.2–24.3) 0.01
normal activity)
Protein C deficiency (<75 percent of 3.3 5.0 1.5 (0.3–7.7) 22.2 8.4 (2.2–32.0) 0.05
normal activity)§
Protein S deficiency (<55 percent of 4.8 14.1 3.2 (1.3–8.0) 9.1 2.0 (0.5–7.5) 0.50
normal activity)
Protein S deficiency (<65 percent of 6.6 9.1 1.4 (0.4–5.7) 5.6 0.8 (0.1–7.1) 0.70
normal activity)¶
*CI denotes confidence interval.
†P values are for the univariate comparison between women with a first episode of venous thromboembolism and those with a recurrent episode. In the
multivariate analysis after adjustments were made for a body-mass index of more than 30 and use of oral contraceptives, P=0.01 for the effect of antithrombin
deficiency (<80 percent of normal activity), P<0.001 for the effect of protein C deficiency (<65 percent of normal activity), and P=0.10 for the effect of the
G20210A prothrombin-gene mutation.
‡Because no normal women had this combined defect, the estimated relative risk was calculated on the basis of the probability of a combined defect in
these women. For this reason, no confidence interval is given.
§Carriers of factor V Leiden were excluded from the analysis.
¶Women who were taking an oral contraceptive and carriers of factor V Leiden were excluded from the analysis.
boembolism and among those with recurrent throm- culated in a multivariate analysis. An incidence of
boembolism, as compared with normal women, are 1 thromboembolic event in 1500 pregnancies was as-
shown in Table 4. We also compared the prevalence sumed. The probability of thrombosis among women
and relative risk of these risk factors among 79 women without any risk factor was 0.03 percent (95 percent
with a first episode of thromboembolism with those confidence interval, 0.02 to 0.04 percent); among
among the 40 women who had recurrent thrombo- those with factor V Leiden, 0.25 percent (95 per-
embolism. The presence of the G20210A prothrom- cent confidence interval, 0.2 to 0.3 percent); among
bin-gene mutation, the presence of antithrombin de- those with the G20210A prothrombin-gene muta-
ficiency, and the presence of protein C deficiency were tion, 0.5 percent (95 percent confidence interval, 0.3
associated with recurrent venous thrombotic events. to 0.8 percent); among those with antithrombin de-
Women with recurrent thromboembolism had sig- ficiency (<80 percent of normal activity), 0.4 per-
nificantly more combined defects than did women cent (95 percent confidence interval, 0.3 to 0.6 per-
with a first episode (prevalence of factor V Leiden plus cent); and among those with protein C deficiency
protein C deficiency, 14.7 percent vs. 1.4 percent, (<75 percent of normal activity), 0.1 percent (95 per-
P=0.006; prevalence of factor V Leiden plus anti- cent confidence interval, 0.04 to 0.13 percent). The
thrombin deficiency, 20 percent vs. 7.7 percent, P= combination of factor V Leiden plus the G20210A
0.05; prevalence of the G20210A prothrombin-gene prothrombin-gene mutation was associated with a
mutation plus antithrombin deficiency, 12.8 percent probability of thrombosis of 4.6 percent (95 percent
vs. 0 percent, P=0.004). confidence interval, 2.6 to 8.2 percent).
Positive Predictive Value of Hereditary Risk Factors DISCUSSION
For the carriers of hereditary risk factors, the Thromboembolic complications, including pulmo-
positive predictive values indicating the probability of nary embolism, that occur during pregnancy and the
thrombosis per pregnancy and puerperium were cal- puerperium are a major cause of maternal morbidity
378 · Febr u ar y 10 , 2 0 0 0
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2015. For personal use only. No other uses without permission.
Copyright © 2000 Massachusetts Medical Society. All rights reserved.
P R OT H R O M BIN AND FAC TOR V MUTAT IONS IN WOMEN WITH A H ISTORY OF TH ROMBOSIS D UR ING PR EGNANCY
and mortality. Our results indicate that the relative G20210A prothrombin-gene mutation, the presence
risk of venous thromboembolism among women with of protein C deficiency was associated with recurrent
the G20210A prothrombin-gene mutation is at least venous thromboembolism during pregnancy and the
as high as that among those with factor V Leiden. puerperium, particularly when it was present with
Previous studies demonstrated a relative risk of ve- other defects.
nous thromboembolism of between 3.0 and 5.0 as- The predictive value of factor V Leiden and other
sociated with the G20210A prothrombin-gene mu- inherited markers for the purpose of screening for
tation11,24-26; in contrast, we found a much higher thrombotic risk is low among pregnant women. A
relative risk of venous thromboembolism during preg- significant increase in the probability of thrombosis
nancy and the puerperium among women with this can be demonstrated only in cases in which a woman
defect. There appears to be a relation between the has a combined defect (as evidenced by a probability
presence of the G20210A prothrombin-gene muta- of 4.6 percent for women with both factor V Leiden
tion and pregnancy-related alterations in coagulation and the G20210A prothrombin-gene mutation).
or fibrinolysis that lead to thrombosis in women
who are carriers of the G20210A prothrombin-gene Supported by an institutional interdisciplinary program in vascular med-
mutation. A similar observation was recently report- icine sponsored by Hoffmann–La Roche.
ed for cerebral-vein thrombosis in women taking an REFERENCES
oral contraceptive.27
We confirmed the importance of factor V Leiden 1. Prevention of venous thrombosis and pulmonary embolism: NIH Con-
sensus Development. JAMA 1986;256:744-9.
as a risk factor for venous thromboembolism during 2. Kierkegaard A. Incidence and diagnosis of deep vein thrombosis asso-
pregnancy and the puerperium.10,16 In addition, we ciated with pregnancy. Acta Obstet Gynecol Scand 1983;62:239-43.
3. Treffers PE, Huidekoper BL, Weenink GH, Kloosterman GJ. Epidemi-
found that factor V Leiden is a risk factor that is in- ological observations of thrombo-embolic disease during pregnancy and in
dependent of other known determinants of the risk the puerperium, in 56,022 women. Int J Gynaecol Obstet 1983;21:327-31.
of thrombosis; specifically, it is independent of the 4. Rutherford S, Montoro M, McGehee W, Strong T. Thromboembolic
disease associated with pregnancy: an 11-year review. Am J Obstet Gynecol
G20210A prothrombin-gene mutation. It is remark- 1991;164:Suppl:286. abstract.
able that as many as 9.3 percent of the women had 5. Hellgren M, Svensson PJ, Dahlbäck B. Resistance to activated protein
both the G20210A prothrombin-gene mutation and C as a basis for venous thromboembolism associated with pregnancy and
oral contraceptives. Am J Obstet Gynecol 1995;173:210-3.
factor V Leiden, leading to a disproportionately high- 6. Greer IA. Haemostasis and thrombosis in pregnancy. In: Bloom AL,
er risk than with either defect alone. Forbes CD, Thomas DP, Tuddenham EGD, eds. Haemostasis and throm-
bosis. Vol. 2. Edinburgh, Scotland: Churchill Livingstone, 1994:987-1015.
There are conflicting results regarding the role of 7. Dahlbäck B, Stenflo J. A natural anticoagulant pathway: protein C, S,
a homozygous 677TT MTHFR genotype as a risk C4b-binding protein and thrombomodulin. In: Bloom AL, Forbes CD,
factor for venous thromboembolism. Homozygosity Thomas DP, Tuddenham EGD, eds. Haemostasis and thrombosis. Vol. 1.
Edinburgh, Scotland: Churchill Livingstone, 1994:671-98.
for this polymorphism was associated with high plas- 8. Dizon-Townson DS, Nelson LM, Jang H, Varner MW, Ward K. The in-
ma homocysteine concentrations and venous throm- cidence of the factor V Leiden mutation in an obstetric population and its
bosis in some studies12-14 but not in others.15 In our relationship to deep vein thrombosis. Am J Obstet Gynecol 1997;176:883-6.
9. Bertina RM, Koeleman BP, Koster T, et al. Mutation in blood coagu-
study, the 677TT MTHFR genotype had no influence lation factor V associated with resistance to activated protein C. Nature
on the risk of venous thromboembolism, although the 1994;369:64-7.
10. Bokarewa MI, Bremme K, Blombäck M. Arg506-Gln mutation in fac-
prevalence of the 677TT MTHFR genotype in the tor V and risk of thrombosis during pregnancy. Br J Haematol 1996;92:
subgroup of women with venous thromboembolism 473-8.
during the puerperium was higher than in the sub- 11. Poort SR, Rosendaal FR, Reitsma PH, Bertina RM. A common ge-
netic variation in the 3'-untranslated region of the prothrombin gene is as-
group of women with venous thromboembolism dur- sociated with elevated plasma prothrombin levels and an increase in venous
ing pregnancy. thrombosis. Blood 1996;88:3698-703.
In the analysis of the risk associated with deficien- 12. Frosst P, Blom HJ, Milos R, et al. A candidate genetic risk factor for
vascular disease: a common mutation in methylenetetrahydrofolate reduc-
cies of antithrombin, protein C, and protein S, only tase. Nat Genet 1995;10:111-3.
antithrombin deficiency was an independent risk fac- 13. Margaglione M, D’Andrea G, d’Addedda M, et al. The methylenetet-
rahydrofolate reductase TT677 genotype is associated with venous throm-
tor for thromboembolism after adjustments were bosis independently of the coexistence of the FV Leiden and the pro-
made for the presence of factor V Leiden and oral- thrombin A20210 mutation. Thromb Haemost 1998;79:907-11.
contraceptive use. However, the number of women 14. Eichinger S, Stümpflen A, Hirschl M, et al. Hyperhomocysteinemia is
a risk factor of recurrent venous thromboembolism. Thromb Haemost
with deficiencies of protein C and protein S may be 1998;80:566-9.
too low for it to be possible to identify an influence 15. Kluijtmans LAJ, den Heijer M, Reitsma PH, Heil SG, Blom HJ, Rosen-
of each of these risk factors independently in a mul- daal FR. Thermolabile methylenetetrahydrofolate reductase and factor V Lei-
den in the risk of deep-vein thrombosis. Thromb Haemost 1998;79:254-8.
tivariate analysis. It is well known that resistance to 16. Hallak M, Senderowicz J, Cassel A, et al. Activated protein C resist-
activated protein C is associated with decreased pro- ance (factor V Leiden) associated with thrombosis in pregnancy. Am J Ob-
stet Gynecol 1997;176:889-93.
tein S activity, as determined by routine assays. We 17. Kniemeyer HW, Merckle R, Stühmeier K, Sandmann W. Chirurgische
found that resistance to activated protein C was also Therapie der akuten und embolisierenden tiefen Beinvenenthrombose —
associated with decreased protein C activity in a group Indikation, Technisches Prinzip, Ergebnisse. Klin Wochenschr 1990;68:
1208-16.
of 500 normal men and women (data not shown). 18. Kniemeyer HW, Sandmann W. Chirurgische Therapie der tiefen Venen-
In addition to antithrombin deficiency and the thrombose in Schwangerschaft und Wochenbett. Gynakologe 1990;23:91-6.
Vol ume 342 Numb e r 6 · 379
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2015. For personal use only. No other uses without permission.
Copyright © 2000 Massachusetts Medical Society. All rights reserved.
The Ne w E n g l a nd Jo u r n a l o f Me d ic i ne
19. Kolvenbach R, Grabitz K, Distler W, Eichwede F, Sandmann W. Die ing for coagulation factor V and resistance to activated protein C: detection
embolisierende Bein- und Beckenvenenthrombose in der Spät-Schwanger- of the genetic mutation by oligonucleotide ligation assay using a semi-
schaft: Indikation für ein simultanes, interdisziplinäres Vorgehen. Gynako- automated system. Thromb Haemost 1996;76:53-5.
loge 1991;24:305-6. 24. Cumming AM, Keeney S, Salden A, Bhavnani M, Shwe KH, Hay
20. Kniemeyer HW, Sandmann W, Schwindt C, Grabitz K, Torsello G, CRM. The prothrombin gene G20210A variant: prevalence in a U.K. anti-
Stuhmeier K. Thrombectomy with arteriovenous fistula for embolizing coagulant clinic population. Br J Haematol 1997;98:353-5.
deep venous thrombosis: an alternative therapy for prevention of recurrent 25. Hillarp A, Zöller B, Svensson PJ, Dahlbäck B. The 20210 A allele
pulmonary embolism. Clin Invest 1993;72:40-5. of the prothrombin gene is a common risk factor among Swedish outpa-
21. Frezzato M, Tosetto A, Rodeghiero F. Validated questionnaire for the tients with verified deep venous thrombosis. Thromb Haemost 1997;78:
identification of previous personal or familial venous thromboembolism. 990-2.
Am J Epidemiol 1996;143:1257-65. 26. Leroyer C, Mercier B, Oger E, et al. Prevalence of 20210 A allele of
22. Ridker PM, Hennekens CH, Lindpaintner K, Stampfer MJ, Eisenberg the prothrombin gene in venous thromboembolism patients. Thromb
PR, Miletich JP. Mutation in the gene coding for coagulation factor V and Haemost 1998;80:49-51.
the risk of myocardial infarction, stroke, and venous thrombosis in appar- 27. Martinelli I, Sacchi E, Landi G, Taioli E, Duca F, Mannucci PM. High
ently healthy men. N Engl J Med 1995;332:912-7. risk of cerebral-vein thrombosis in carriers of a prothrombin-gene mutation
23. Zotz RB, Maruhn-Debowski B, Scharf RE. Mutation in the gene cod- and in users of oral contraceptives. N Engl J Med 1998;338:1793-7.
380 · Febr u ar y 10 , 2 0 0 0
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2015. For personal use only. No other uses without permission.
Copyright © 2000 Massachusetts Medical Society. All rights reserved.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Differences in Sexual Function After Vaginal DeliveryDocument3 pagesDifferences in Sexual Function After Vaginal DeliveryAlfa FebriandaNo ratings yet
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- GMR 6939Document6 pagesGMR 6939Alfa FebriandaNo ratings yet
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Leptin rs2167270 G A (G19A) Polymorphism May Decrease The Risk of Cancer: A Case Control Study and Meta Analysis Involving 19 989 SubjectsDocument10 pagesLeptin rs2167270 G A (G19A) Polymorphism May Decrease The Risk of Cancer: A Case Control Study and Meta Analysis Involving 19 989 SubjectsAlfa FebriandaNo ratings yet
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Haplotype AnalysisDocument5 pagesHaplotype AnalysisAlfa FebriandaNo ratings yet
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- AflpDocument8 pagesAflprmiguel7No ratings yet
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Pregnancy and Postpartum Risks for Venous ThrombosisDocument6 pagesPregnancy and Postpartum Risks for Venous ThrombosisAlfa FebriandaNo ratings yet
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Magnesium OyeDocument11 pagesMagnesium Oyeade_fkuNo ratings yet
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Higado Graso Agudo en El Embarazo AJG 2017Document9 pagesHigado Graso Agudo en El Embarazo AJG 2017Fabrizzio BardalesNo ratings yet
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Poster Session IV: ObjectiveDocument2 pagesPoster Session IV: ObjectiveAlfa FebriandaNo ratings yet
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- Corticotrophin Releasing Hormone As A Useful Marker To Identify The Pre-EclampsiaDocument4 pagesCorticotrophin Releasing Hormone As A Useful Marker To Identify The Pre-EclampsiaAlfa FebriandaNo ratings yet
- CMJ 57 6 Peterlin 28051281Document6 pagesCMJ 57 6 Peterlin 28051281Alfa FebriandaNo ratings yet
- Aavs 7 1 17-23 PDFDocument7 pagesAavs 7 1 17-23 PDFAlfa FebriandaNo ratings yet
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Antenatal Care of Preeclampsia: From The Inverted Pyramid To The Arrow Model?Document4 pagesAntenatal Care of Preeclampsia: From The Inverted Pyramid To The Arrow Model?Alfa FebriandaNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Pregnancy and Postpartum Risks for Venous ThrombosisDocument6 pagesPregnancy and Postpartum Risks for Venous ThrombosisAlfa FebriandaNo ratings yet
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Haplotype AnalysisDocument5 pagesHaplotype AnalysisAlfa FebriandaNo ratings yet
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- CMJ 57 6 Peterlin 28051281Document6 pagesCMJ 57 6 Peterlin 28051281Alfa FebriandaNo ratings yet
- Single Nucleotide Polymorphisms of Follicle-Stimulating Hormone Receptor Promoter and Their Impacts To The Promoter ActivitiesDocument10 pagesSingle Nucleotide Polymorphisms of Follicle-Stimulating Hormone Receptor Promoter and Their Impacts To The Promoter ActivitiesAlfa FebriandaNo ratings yet
- Antenatal Care of Preeclampsia: From The Inverted Pyramid To The Arrow Model?Document4 pagesAntenatal Care of Preeclampsia: From The Inverted Pyramid To The Arrow Model?Alfa FebriandaNo ratings yet
- JokohjokDocument2 pagesJokohjokAlfa FebriandaNo ratings yet
- TRF 12966Document8 pagesTRF 12966Alfa FebriandaNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Success of External Cephalic Version With Terbutaline As Tocolytic AgentDocument4 pagesSuccess of External Cephalic Version With Terbutaline As Tocolytic AgentAlfa FebriandaNo ratings yet
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- Aogs 13082Document8 pagesAogs 13082Alfa FebriandaNo ratings yet
- Meigs' Syndrome and Pseudo-Meigs' Syndrome: Report of Four Cases and Literature ReviewsDocument6 pagesMeigs' Syndrome and Pseudo-Meigs' Syndrome: Report of Four Cases and Literature ReviewsAlfa FebriandaNo ratings yet
- Endometriosis-Associated Infertility Causes and TreatmentsDocument9 pagesEndometriosis-Associated Infertility Causes and TreatmentsAlfa FebriandaNo ratings yet
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- A Rare Case of Meigs Syndrome in Pregnancy With Bilateral Ovarian MassesDocument2 pagesA Rare Case of Meigs Syndrome in Pregnancy With Bilateral Ovarian MassesAlfa FebriandaNo ratings yet
- Transfusion-Related Acute Lung Injury Risk Mitigation: An UpdateDocument10 pagesTransfusion-Related Acute Lung Injury Risk Mitigation: An UpdateAlfa FebriandaNo ratings yet
- 1 PDFDocument7 pages1 PDFAlfa FebriandaNo ratings yet
- Iron Deficiency Anaemia In...Document9 pagesIron Deficiency Anaemia In...Alfa FebriandaNo ratings yet
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Anaemia Pregnancy: (Dieckmann 1944 I960)Document13 pagesAnaemia Pregnancy: (Dieckmann 1944 I960)Alfa FebriandaNo ratings yet
- Understanding Thrombophilia Risk FactorsDocument9 pagesUnderstanding Thrombophilia Risk FactorsSeraj Abed ElmoatiNo ratings yet
- Bone Marrow Film Examination For Platelet Maturation Series: Activity No. 1Document43 pagesBone Marrow Film Examination For Platelet Maturation Series: Activity No. 1pixiedustNo ratings yet
- Blood Requisition FormDocument2 pagesBlood Requisition FormPrashant Kumar Singh100% (1)
- JPAC (/) : 3.3: Blood ProductsDocument12 pagesJPAC (/) : 3.3: Blood Productsanwar1971No ratings yet
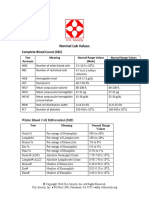
- Normal Lab Values 3 20 16 PDFDocument2 pagesNormal Lab Values 3 20 16 PDFMarian AlixandrescuNo ratings yet
- (A Unit of Shriman Enterprises), Nurpur, Pathankot Road, Jalandhar, Punjab 144012Document16 pages(A Unit of Shriman Enterprises), Nurpur, Pathankot Road, Jalandhar, Punjab 144012J KNo ratings yet
- Complications To PhlebotomyDocument4 pagesComplications To Phlebotomybenrmt67% (3)
- Blood Group: Made By:-Vedant PatelDocument18 pagesBlood Group: Made By:-Vedant PatelVedant PatelNo ratings yet
- Blood System 5 PDFDocument10 pagesBlood System 5 PDFSardar jiNo ratings yet
- BORJA Genetics Lab Exercise 6 Multiple Alleles and ABO Blood Groups in HumansDocument5 pagesBORJA Genetics Lab Exercise 6 Multiple Alleles and ABO Blood Groups in Humansbry uyNo ratings yet
- Major Non-ABO Blood Groups and Antigens (P, I, Kell, Duffy, KiddDocument1 pageMajor Non-ABO Blood Groups and Antigens (P, I, Kell, Duffy, KiddJohanna MarieNo ratings yet
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Hematology Course1Document72 pagesHematology Course1api-3703352100% (10)
- Platelet Function TestsDocument27 pagesPlatelet Function TestsTusabe FredNo ratings yet
- GPP-100 QuickguideDocument27 pagesGPP-100 QuickguideSmilja Salazar CortezNo ratings yet
- BloodbankDocument433 pagesBloodbankFait Hee95% (22)
- Daftar Harga Alkes & Reagensia E-CatalogDocument3 pagesDaftar Harga Alkes & Reagensia E-CatalogPT SNAFANo ratings yet
- Normal Erythrocyte1Document4 pagesNormal Erythrocyte1RonyArtoKapidaNo ratings yet
- HyperbilirubinemiaDocument2 pagesHyperbilirubinemiaKyla FerriolsNo ratings yet
- Microcytic Hypochromic AnaemiaDocument75 pagesMicrocytic Hypochromic AnaemiaNashita NowshinNo ratings yet
- Acog Practice Bullet In: Management of Alloimmunization During PregnancyDocument9 pagesAcog Practice Bullet In: Management of Alloimmunization During PregnancyTatiiana ZpiitiiaNo ratings yet
- 3讲义hematologyDocument96 pages3讲义hematologychongyu888xiongNo ratings yet
- CryoprecipitateDocument7 pagesCryoprecipitateBrandon BNo ratings yet
- Exchange TransfusionDocument21 pagesExchange TransfusionJOSLIN100% (2)
- Pro64-A-03 - Processing - A - CBC - CNT - SOPDocument7 pagesPro64-A-03 - Processing - A - CBC - CNT - SOPBassam AlharaziNo ratings yet
- 3 - AnemiaDocument7 pages3 - AnemiaRawabi rawabi1997No ratings yet
- Whole Blood Component Separation ProcessDocument2 pagesWhole Blood Component Separation ProcessGlenn PerezNo ratings yet
- Anemia Pathophysiology All in 1 by Francis OliverosDocument3 pagesAnemia Pathophysiology All in 1 by Francis Oliverosfrancis00090No ratings yet
- Hem311 Week 13 Lab - Reticulocyte CountDocument32 pagesHem311 Week 13 Lab - Reticulocyte CountSheine EspinoNo ratings yet
- 36, Lawrence Road, Lahore. Tel:6361417, Fax: 6315401, 5711501, Mobile: 0300-8482230Document1 page36, Lawrence Road, Lahore. Tel:6361417, Fax: 6315401, 5711501, Mobile: 0300-8482230uzairNo ratings yet
- BIOCHEMISTRY TEST LOINC CODESDocument15 pagesBIOCHEMISTRY TEST LOINC CODESSowji PNo ratings yet
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (13)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 3.5 out of 5 stars3.5/5 (2)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)