Professional Documents
Culture Documents
For Lab To Print
Uploaded by
elinayalOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
For Lab To Print
Uploaded by
elinayalCopyright:
Available Formats
Lab #1: MICROORGANISMS IN THE ENVIRONMENT & EFFECTIVENESS OF HAND WASHING
BACKGROUND Microorganisms are ubiquitous in almost all environments on this planet. The exposure of sterile Brain Heart Infusion (BHI) agar plates to a variety of sources including your hands will allow you to see some of the many types of microorganisms which are omnipresent in our environments. In addition, you will learn the value of proper hand washing procedures to reduce microbial numbers on your hands.
Lab #2: MICROSCOPY: INTRODUCTION AND MICROBIAL MORPHOLOGY
BACKGROUND Microscopes are common tools found in most biological and clinical laboratories. They allow visualization of organisms and/or cellular structures that are much too small to be perceived by the naked eye. Microscopes use either visible light (light microscopes) or electrons (electron microscopes) to resolve objects. Furthermore, light microscopes fall into one of several categoriesbright-field, dark-field, phase-contrast, differential interference contrast, fluorescence, and confocal. The optical system we will employ to visualize organisms and cells in this class will be a bright-field compound light microscope. Bright-field means that it will allow us to visualize dark objects against a bright field or background; and compound means that more than one lens is used to magnify the object. This exercise will acquaint you with your microscope, its use and care, and allow you to directly examine and study a variety of microorganisms such as protozoa, algae, fungi, and bacteria. Parts of the bright-field compound light microscope: 1. Ocular: Sometimes called the eyepiece, it is located at the upper end of the inclined body tube. The ocular contains lenses with a total magnification of 10x. 2. Rotating nosepiece: Holds the objective lenses and may be turned in either direction so that the magnification may be changed while viewing a specimen. 3. Objective lenses: Lenses which are closest to the object or specimen and have individual magnifying powers of 4x (scanning), 10x (low power), 40x (high-dry power), and 100x (oil-immersion). 4. Mechanical slide stage: Located below the nosepiece, this supports the specimen slide over a hole that admits light for specimen illumination.
5. Coarse focus adjustment knob: Moves the stage closer to or further away from the objective for initial focusing. 6. Fine focus adjustment knob: Permits exact focusing by moving the stage very slightly. 7. Light source: Built into the base, this illuminates the specimen by directing light up through the stage opening. 8. Condenser: Focuses light from the light source onto the specimen. The condenser can be adjusted vertically (i.e. moved up or down) in this microscope. 9. Iris diaphragm: Also known as the condenser aperture diaphragm lever, this is located on the underside of the stage and may be opened or closed to regulate the amount of light that reaches the specimen.
Lab #3: MICROSCOPY: THE WET MOUNT
BACKGROUND Microorganisms (both eukaryotic and prokaryotic) can be readily observed under a light microscope using a simple wet mount, wherein a drop of broth culture or contaminated water is placed on a microscope slide and covered with a glass cover slip. Unstained, living organisms can be viewed by altering the amount of light applied to the sample. This can be accomplished by: (1) raising/ lowering the condenser; (2) opening/ closing the iris diaphragm; or (3) increasing/ decreasing the intensity of the light at the light source. Wet mounts are very useful for observing motile organisms and produce very few, if any, artifacts. In this exercise, you will examine wetlands water samples from the Napa-Solano Marshes in American Canyon, CA. This brackish water (which is a mixture of marine and fresh water) provides habitat to an immensely diverse population of microbes and microscopic multicellular organisms. You will observe many of these organisms as you learn how manipulation of light can dramatically affect what you are able to see under the light microscope.
Lab #4: ISOLATION OF PURE CULTURES SPECIAL PURPOSE MEDIA AND THE STREAK-PLATE METHOD
BACKGROUND
Bacteria occur as mixed populations in most natural environments. Therefore, the first requirement for the study of an organism and its properties is its isolation in pure culture, i.e. a culture containing only a single species. In clinical microbiology, it is often necessary to isolate and identify a specific organism from the mixed bacterial population found in feces, saliva, or body exudates to determine its presence. To accomplish this, microbiologists use a vast array of special purpose media that generally fall into one or more of the following categories: Selective media: These media are designed with a specific chemical added which will inhibit the growth of some unwanted, non-suspect groups of bacteria and enhance the growth of the organisms which are the suspected pathogens. Differential media: These media use the addition of chemical indicator substances which produce a color change in the medium and/or in a colony for certain organisms. This facilitates the differentiation between specific types of potential pathogens from other non-pathogens in a clinical isolate. Enriched media: The addition of animal blood or serum to complex media allows the growth of fastidious or low-level pathogens, which may be difficult to grow or have highly demanding or specific nutritional requirements. Since certain bacteria secrete enzymes which lyse red blood cells in different patterns surrounding their colonies, blood agar can also serve as a differential medium. In addition to the use of special purpose media, other methods employed for obtaining pure cultures of bacteria utilize dilution techniques, the most popular of which is the streak-plate method. The streak-plate is the single most common isolation technique used in both clinical and research bacteriology labs world-wide. In the streak-plate technique, an inoculation loop is used to streak a mixed inoculum many times over the surface of an agar culture medium in a pattern that progressively dilutes the bacteria to a point where single cells will develop into single colonies upon incubation.
Lab #5: THE GRAM STAIN I
BACKGROUND First developed by pathologist Hans Christian Gram in 1884, the Gram stain is one of the most useful staining procedures as it classifies bacteria into two major categories Gram-positive and Gram-negative. In the clinical diagnostic laboratory, this stain is used to identify microorganisms that are cultured from patient specimens. Briefly, the Gram stain procedure involves treatment with a primary stain (crystal violet) that stains all bacteria purple. A mordant (Grams iodine) is then applied which fixes the first stain within the cells. (A mordant is a chemical that fixes a dye in or on a substance by combining with the dye to form an insoluble compound.) A decolorizing agent (ethyl alcohol or ethyl alcohol acetone) is then used to wash the bacteria resulting in the removal of the purple color from some species but not others. A counterstain (secondary stain) of a contrasting color, safranin, is then applied to stain the decolorized bacteria red. The bacteria that retain the crystal
violet-iodine complex after decolorization appear dark blue or purple and are designated Grampositive; those that lose the crystal violet-iodine complex after decolorization and are subsequently stained red or pink by the counterstain safranin are designated Gram-negative.
Lab #7: THE ACID-FAST STAIN
BACKGROUND Like the Gram stain, the acid-fast, or Ziehl-Neelson, stain is another differential stain. It was originally developed by Franz Ziehl and Friedrich Neelson (and later modified by Joseph Kinyoun) to stain certain bacteria that were impermeable to most traditional stains, including the Gram stain. The difficulty in staining is due to the high level of lipids (e.g. mycolic acid) in the bacterial cell wall which forms a waxy, water-resistant layer. These bacteria are referred to as acid-fast because they resist decolorization with acid-alcohol after being stained with a strong solution of phenol and carbolfuchsin (primary stain). The carbolfuchsin remains in these cells after decolorization because carbolfuchsin has a higher affinity for the lipids in the cell wall than the acid-alcohol. Non-acid-fast organisms are visualized using the counterstain methylene blue. Acid-fast organisms appear red; non-acid-fast organisms appear blue. The most important acid-fast organisms (from a medical standpoint) are found in the genera Mycobacterium and Nocardia. Mycobacterium tuberculosis causes tuberculosis, and Mycobacterium leprae is the causative agent of leprosy. Nocardia asteroids can cause pulmonary infections and is one of the causative agents of mycetomaa localized, destructive infection of the feet or hands.
Lab #8: BIOCHEMICAL IDENTIFICATION OF BACTERIA
BACKGROUND Biochemical tests can be employed in the differentiation and identification of many bacterial species. In this exercise, two biochemical tests will be used to identify differences between six microbial species. The first experiment will test each organisms ability to ferment three different carbohydrates. The second will test each organisms ability to produce hydrogen sulfide gas (H2S). The ability to ferment specific carbohydrates, producing acidic, alcoholic, and/or gaseous endproducts, is a common characteristic tested and employed in the identification of particular bacterial species. Media for testing carbohydrate fermentation may be in broth form and distributed into test tubes that contain a small, inverted fermentation, or Durham tubes, that will catch any gas that may form when the broth is inoculated with the bacteria and incubated. The medium you will use will consist of nutrient broth, 0.5% of a specific carbohydrate, and the pH indicator phenol red.
Certain bacteria are able to produce hydrogen sulfide via one of two pathways: (1) by the reduction of organic sulfur found in the sulfur-containing amino acids, such as cysteine and methionine; or (2) by the reduction of inorganic sulfur compounds, such as sulfate (SO42-). Since H2S gas is colorless, its production is detected by incorporating ferrous sulfate (FeSO4) into the medium. Ferrous sulfate will react with H2S to form a visible black precipitate of ferrous sulfide (FeS).
Laboratory Exercise #10: USE OF ANTIBODIES TO IDENTIFY MICROORGANISMS ENZYME-LINKED IMMUNOSORBENT ASSAY (ELISA)
BACKGROUND The enzyme-linked immunosorbent assay (ELISA) relies on antibodies to detect the presence of antigens in liquid samples. (Antigens are any agents foreign to the body that provoke an immune response, for example, viruses, parasites, fungi, bacteria, or chemicals.) Because they are antibody-based, ELISAs are called immunoassays. ELISAs can detect minute amounts of disease agents in samples, such as body fluids, before the body has had a chance to mount an immune response. Smallpox virus is an example of a disease agent that can now be detected using an ELISA. If exposure is detected and treated with vaccine within 2-3 days, patients do not develop smallpox. Other applications for ELISA include testing for West Nile virus, HIV coat protein p24, SARS virus, anthrax spores, hormones such as hCG in pregnancy tests, illegal steroids in drug tests, bacteria in food safety tests, and the presence of genetically modified organisms contaminating non-GMO food. In this exercise, you and a fellow classmate will act the part of clinical lab scientists at a local hospital, testing for the presence of West Nile virus in patient samples. Each of you will be given your own patient sample to test. [Note: Samples are not really obtained from patients and do not actually contain West Nile virus.]
Lab #11: CHEMICAL METHODS OF CONTROLLING BACTERIAL GROWTHANTIBIOTICS, ANTISEPTICS, AND DISINFECTANTS
BACKGROUND Antiseptics and Disinfectants: Chemicals that kill or prevent the growth of microorganisms are called antimicrobial agents. Disinfectants are chemical agents used on inanimate objects, whereas antiseptics are chemicals capable of being used on living tissue. Both are employed to lower the number of microorganisms and to prevent contamination and transmission of disease. The efficacy (effectiveness) of antimicrobial
agents is influenced by a variety of factors including: concentration, length of exposure, microbial characteristics, and environmental conditions (such as temperature, pH, and presence of organic material). No one chemical best fits all conditions. Antibiotics: It is very important that a physician has information regarding whether an isolated pathogenic bacterium is susceptible or resistant to available antibiotics. The hospital or clinical laboratory isolates the suspected pathogen from a clinical specimen and then determines its sensitivity to chemotherapeutic agents. Not too long ago, the standard test used by most labs was the Standardized Disk Susceptibility Test, also known as the Kirby-Bauer test. This procedure involves inoculating the organism in question on a standardized agar plate, placing small disks impregnated with various antibiotics on the inoculated surface, incubating the plates, and then observing the zones of growth inhibition surrounding the disks. The size of the zone of inhibition may be influenced by multiple factors such as: depth of the agar; rate of diffusion of the antibiotic through the agar; temperature; amount of bacterial inoculum; rate of growth of the organism; and the susceptibility of the organism to the antibiotic. Using this test, the physician can determine if the bacterial pathogen is susceptible, intermediate, or resistant to a particular antibiotic and then determine the concentration necessary to administer to the patient.
In Part A of this exercise, the antimicrobial capacity of various disinfectants and antiseptics will be assessed for two different bacterial cultures Escherichia coli and Staphylococcus aureus. In Part B of this exercise, you will carry out the Kirby-Bauer test in order to truly visualize how different antibiotics affect the growth of Escherichia coli and Staphylococcus aureus.
Laboratory Exercise #12: PHYSICAL METHODS OF CONTROLLING BACTERIAL GROWTH
BACKGROUND There are various physical methods that can be employed to either sterilize materials or at least control microbial growth. These include the use of heat, filtration, low temperatures, desiccation, osmotic pressure, and radiation. Just as with chemical methods of control, the effectiveness of any physical method may be influenced by the starting number of microbes, the environment, time of exposure, and microbial characteristics. In this exercise, the antimicrobial capacity of three different physical methodsheat, refrigeration, and high salt (osmotic pressure)will be assessed for six different bacterial organisms.
You might also like
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- NCP For Acute PancreatitisDocument3 pagesNCP For Acute Pancreatitisrod navales100% (1)
- Under The RadarDocument35 pagesUnder The RadarJason M Perry50% (2)
- Prescriptions Labelling Latin Terms FA 20120222Document24 pagesPrescriptions Labelling Latin Terms FA 20120222SherazButtNo ratings yet
- Surgo Fresher's Edition 2013Document24 pagesSurgo Fresher's Edition 2013Surgo GlasgowNo ratings yet
- TgaDocument33 pagesTgavarun rajNo ratings yet
- Non-Communicable Diseases - Kuntaraf Script Online VersionDocument13 pagesNon-Communicable Diseases - Kuntaraf Script Online VersionSadiki WallaceNo ratings yet
- Laporan Kematian Pang Kim ChoonDocument17 pagesLaporan Kematian Pang Kim ChoonAfifah SelamatNo ratings yet
- BPHDocument57 pagesBPHDiannetotz MoralesNo ratings yet
- Bruxism and Prostho TreatmentDocument10 pagesBruxism and Prostho Treatmentdorasani99No ratings yet
- HAND HYGIENE MONITORING SHEET (Revised)Document3 pagesHAND HYGIENE MONITORING SHEET (Revised)lance tabinasNo ratings yet
- "Breakfast Like A King, Lunch Like A Prince and Dinner Like A PauperDocument10 pages"Breakfast Like A King, Lunch Like A Prince and Dinner Like A Pauperதுர்காதேவிNo ratings yet
- Category 3: Mammography (Digital) : 1260023072PL - Alpha - XLSX 1 of 15Document15 pagesCategory 3: Mammography (Digital) : 1260023072PL - Alpha - XLSX 1 of 15Berkant Orçun ÇangalNo ratings yet
- Andrew Austin - IEMT & Long Term Anxiety - DVD Cover PDFDocument2 pagesAndrew Austin - IEMT & Long Term Anxiety - DVD Cover PDFMichael CliftonNo ratings yet
- CertificateDocument1 pageCertificateLock DownNo ratings yet
- Term Breech TrialDocument9 pagesTerm Breech TrialAndy Tan Wei KeatNo ratings yet
- Hearing LossDocument9 pagesHearing Lossvicky singhNo ratings yet
- ECG Changes Due To Electrolyte Imbalance (Disorder) - ECG LearningDocument1 pageECG Changes Due To Electrolyte Imbalance (Disorder) - ECG LearningRadhika MNo ratings yet
- List of Licensed Private and Public Hospital 2011Document7 pagesList of Licensed Private and Public Hospital 2011TJ NgNo ratings yet
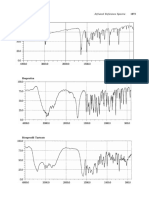
- Ibudilast: 1873 1873 JP Xvi Infrared Reference SpectraDocument53 pagesIbudilast: 1873 1873 JP Xvi Infrared Reference SpectraDiego VargasNo ratings yet
- General Review On Herbal Cosmetics: October 2011Document27 pagesGeneral Review On Herbal Cosmetics: October 2011AmirNo ratings yet
- Overview of Selected Family Therapy ModelsDocument5 pagesOverview of Selected Family Therapy ModelsErin Richardson100% (1)
- Vitiligo - New Treatment ApproachDocument7 pagesVitiligo - New Treatment Approachsawaira khanNo ratings yet
- Emergency Management of Severe BurnsDocument97 pagesEmergency Management of Severe BurnsAyu SyartikaNo ratings yet
- Learning Agility WorksheetsDocument5 pagesLearning Agility WorksheetsThiago RaydanNo ratings yet
- Remit1524932006922 1554076912502 PDFDocument21 pagesRemit1524932006922 1554076912502 PDFArthur OliveiraNo ratings yet
- 2010 Article 319 PDFDocument12 pages2010 Article 319 PDFabarmasNo ratings yet
- Biologic Width - The No Encroachment Zone: I J D ADocument8 pagesBiologic Width - The No Encroachment Zone: I J D AJinny ShawNo ratings yet
- Conscious SedationDocument65 pagesConscious SedationAjay Kumar YadavNo ratings yet
- Raheem Khan - WikipediaDocument10 pagesRaheem Khan - WikipediaRaheem MahirNo ratings yet
- Ayuspray ResearchDocument9 pagesAyuspray ResearchJay AherkarNo ratings yet