Professional Documents
Culture Documents
Unlike False Labor
Uploaded by
MEi .. ÜOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Unlike False Labor
Uploaded by
MEi .. ÜCopyright:
Available Formats
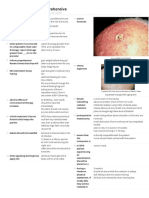
o Unlike false labor, true labor produces regular rhythmic contractions, abdominal discomfort, progressive descent of the fetus,
bloody show, and progressive effacement and dilation of the cervix. o To help a mother break the suction of her breast-feeding infant, the nurse should teach her to insert a finger at the corner of the infants mouth. o Administering high levels of oxygen to a premature neonate can cause blindness as a result of retrolental fibroplasia. o Amniotomy is artificial rupture of the amniotic membranes. o During pregnancy, weight gain averages 25 to 30 lb (11 to 13.5 kg). o Rubella has a teratogenic effect on the fetus during the first trimester. It produces abnormalities in up to 40% of cases without interrupting the pregnancy. o Immunity to rubella can be measured by a hemagglutination inhibition test (rubella titer). This test identifies exposure to rubella infection and determines susceptibility in pregnant women. In a woman, a titer greater than 1:8 indicates immunity. o When used to describe the degree of fetal descent during labor, floating means the presenting part isnt engaged in the pelvic inlet, but is freely movable (ballotable) above the pelvic inlet. o When used to describe the degree of fetal descent, engagement means when the largest diameter of the presenting part has passed through the pelvic inlet. o Fetal station indicates the location of the presenting part in relation to the ischial spine. Its described as 1, 2, 3, 4, or 5 to indicate the number of centimeters above the level of the ischial spine; station 5 is at the pelvic inlet. o Fetal station also is described as +1, +2, +3, +4, or +5 to indicate the number of centimeters it is below the level of the ischial spine; station 0 is at the level of the ischial spine. o During the first stage of labor, the side-lying position usually provides the greatest degree of comfort, although the patient may assume any comfortable position. o During delivery, if the umbilical cord cant be loosened and slipped from around the neonates neck, it should be clamped with two clamps and cut between the clamps. o An Apgar score of 7 to 10 indicates no immediate distress, 4 to 6 indicates moderate distress, and 0 to 3 indicates severe distress. o To elicit Moros reflex, the nurse holds the neonate in both hands and suddenly, but gently, drops the neonates head backward. Normally, the neonate abducts and extends all extremities bilaterally and symmetrically, forms a C shape with the thumb and forefinger, and first adducts and then flexes the extremities. o Pregnancy-induced hypertension (preeclampsia) is an increase in blood pressure of 30/15 mm Hg over baseline or blood pressure of 140/95 mm Hg on two occasions at least 6 hours apart accompanied by edema and albuminuria after 20 weeks gestation. o Positive signs of pregnancy include ultrasound evidence, fetal heart tones, and fetal movement felt by the examiner (not usually present until 4 months gestation o Goodells sign is softening of the cervix. o Quickening, a presumptive sign of pregnancy, occurs between 16 and 19 weeks gestation. o Ovulation ceases during pregnancy. o Any vaginal bleeding during pregnancy should be considered a complication until proven otherwise. o To estimate the date of delivery using Ngeles rule, the nurse counts backward 3 months from the first day of the last menstrual period and then adds 7 days to this date. o At 12 weeks gestation, the fundus should be at the top of the symphysis pubis. o Cows milk shouldnt be given to infants younger than age 1 because it has a low linoleic acid content and its protein is difficult for infants to digest.
o If jaundice is suspected in a neonate, the nurse should examine the infant under natural window light. If natural light is unavailable, the nurse should examine the infant under a white light. o The three phases of a uterine contraction are increment, acme, and decrement. o The intensity of a labor contraction can be assessed by the indentability of the uterine wall at the contractions peak. Intensity is graded as mild (uterine muscle is somewhat tense), moderate (uterine muscle is moderately tense), or strong (uterine muscle is boardlike). o Chloasma, the mask of pregnancy, is pigmentation of a circumscribed area of skin (usually over the bridge of the nose and cheeks) that occurs in some pregnant women. o The gynecoid pelvis is most ideal for delivery. Other types include platypelloid (flat), anthropoid (apelike), and android (malelike). o Pregnant women should be advised that there is no safe level of alcohol intake. o The frequency of uterine contractions, which is measured in minutes, is the time from the beginning of one contraction to the beginning of the next. o Vitamin K is administered to neonates to prevent hemorrhagic disorders because a neonates intestine cant synthesize vitamin K. o Before internal fetal monitoring can be performed, a pregnant patients cervix must be dilated at least 2 cm, the amniotic membranes must be ruptured, and the fetuss presenting part (scalp or buttocks) must be at station 1 or lower, so that a small electrode can be attached. o Fetal alcohol syndrome presents in the first 24 hours after birth and produces lethargy, seizures, poor sucking reflex, abdominal distention, and respiratory difficulty. o Variability is any change in the fetal heart rate (FHR) from its normal rate of 120 to 160 beats/minute. Acceleration is increased FHR; deceleration is decreased FHR. o In a neonate, the symptoms of heroin withdrawal may begin several hours to 4 days after birth. o In a neonate, the symptoms of methadone withdrawal may begin 7 days to several weeks after birth. o In a neonate, the cardinal signs of narcotic withdrawal include coarse, flapping tremors; sleepiness; restlessness; prolonged, persistent, high-pitched cry; and irritability. o The nurse should count a neonates respirations for 1 full minute. o Chlorpromazine (Thorazine) is used to treat neonates who are addicted to narcotics. o The nurse should provide a dark, quiet environment for a neonate who is experiencing narcotic withdrawal. o In a premature neonate, signs of respiratory distress include nostril flaring, substernal retractions, and inspiratory grunting. o Respiratory distress syndrome (hyaline membrane disease) develops in premature infants because their pulmonary alveoli lack surfactant. o Whenever an infant is being put down to sleep, the parent or caregiver should position the infant on the back. (Remember back to sleep.) o The male sperm contributes an X or a Y chromosome; the female ovum contributes an X chromosome. o Fertilization produces a total of 46 chromosomes, including an XY combination (male) or an XX combination (female). o The percentage of water in a neonates body is about 78% to 80%. o To perform nasotracheal suctioning in an infant, the nurse positions the infant with his neck slightly hyperextended in a sniffing position, with his chin up and his head tilted back slightly.
o Organogenesis occurs during the first trimester of pregnancy, specifically, days 14 to 56 of gestation. o After birth, the neonates umbilical cord is tied 1" (2.5 cm) from the abdominal wall with a cotton cord, plastic clamp, or rubber band. o Gravida is the number of pregnancies a woman has had, regardless of outcome. o Para is the number of pregnancies that reached viability, regardless of whether the fetus was delivered alive or stillborn. A fetus is considered viable at 20 weeks gestation. o An ectopic pregnancy is one that implants abnormally, outside the uterus. o The first stage of labor begins with the onset of labor and ends with full cervical dilation at 10 cm. o The second stage of labor begins with full cervical dilation and ends with the neonates birth. o The third stage of labor begins after the neonates birth and ends with expulsion of the placenta. o In a full-term neonate, skin creases appear over two-thirds of the neonates feet. Preterm neonates have heel creases that cover less than two-thirds of the feet. o The fourth stage of labor (postpartum stabilization) lasts up to 4 hours after the placenta is delivered. This time is needed to stabilize the mothers physical and emotional state after the stress of childbirth. o At 20 weeks gestation, the fundus is at the level of the umbilicus. o At 36 weeks gestation, the fundus is at the lower border of the rib cage. o A premature neonate is one born before the end of the 37th week of gestation. o Pregnancy-induced hypertension is a leading cause of maternal death in the United States. o A habitual aborter is a woman who has had three or more consecutive spontaneous abortions. o Threatened abortion occurs when bleeding is present without cervical dilation. o A complete abortion occurs when all products of conception are expelled. o Hydramnios (polyhydramnios) is excessive amniotic fluid (more than 2,000 ml in the third trimester). o Stress, dehydration, and fatigue may reduce a breast-feeding mothers milk supply. o During the transition phase of the first stage of labor, the cervix is dilated 8 to 10 cm and contractions usually occur 2 to 3 minutes apart and last for 60 seconds. o A nonstress test is considered nonreactive (positive) if fewer than two fetal heart rate accelerations of at least 15 beats/minute occur in 20 minutes. o A nonstress test is considered reactive (negative) if two or more fetal heart rate accelerations of 15 beats/minute above baseline occur in 20 minutes. o A nonstress test is usually performed to assess fetal well-being in a pregnant patient with a prolonged pregnancy (42 weeks or more), diabetes, a history of poor pregnancy outcomes, or pregnancy-induced hypertension. o A pregnant woman should drink at least eight 8-oz glasses (about 2,000 ml) of water daily. o When both breasts are used for breast-feeding, the infant usually doesnt empty the second breast. Therefore, the second breast should be used first at the next feeding. o A low-birth-weight neonate weighs 2,500 g (5 lb 8 oz) or less at birth. o A very-low-birth-weight neonate weighs 1,500 g (3 lb 5 oz) or less at birth. o When teaching parents to provide umbilical cord care, the nurse should teach them to clean the umbilical area with a cotton ball saturated with alcohol after every diaper change to prevent infection and promote drying.
o Teenage mothers are more likely to have low-birth-weight neonates because they seek prenatal care late in pregnancy (as a result of denial) and are more likely than older mothers to have nutritional deficiencies. o Linea nigra, a dark line that extends from the umbilicus to the mons pubis, commonly appears during pregnancy and disappears after pregnancy. o Implantation in the uterus occurs 6 to 10 days after ovum fertilization. o Placenta previa is abnormally low implantation of the placenta so that it encroaches on or covers the cervical os. o In complete (total) placenta previa, the placenta completely covers the cervical os. o In partial (incomplete or marginal) placenta previa, the placenta covers only a portion of the cervical os. o Abruptio placentae is premature separation of a normally implanted placenta. It may be partial or complete, and usually causes abdominal pain, vaginal bleeding, and a boardlike abdomen. o Cutis marmorata is mottling or purple discoloration of the skin. Its a transient vasomotor response that occurs primarily in the arms and legs of infants who are exposed to cold. o The classic triad of symptoms of preeclampsia are hypertension, edema, and proteinuria. Additional symptoms of severe preeclampsia include hyperreflexia, cerebral and vision disturbances, and epigastric pain. o Ortolanis sign (an audible click or palpable jerk that occurs with thigh abduction) confirms congenital hip dislocation in a neonate. o The first immunization for a neonate is the hepatitis B vaccine, which is administered in the nursery shortly after birth. o If a patient misses a menstrual period while taking an oral contraceptive exactly as prescribed, she should continue taking the contraceptive. o If a patient misses two consecutive menstrual periods while taking an oral contraceptive, she should discontinue the contraceptive and take a pregnancy test. o If a patient who is taking an oral contraceptive misses a dose, she should take the pill as soon as she remembers or take two at the nextscheduled interval and continue with the normal schedule. o If a patient who is taking an oral contraceptive misses two consecutive doses, she should double the dose for 2 days and then resume her normal schedule. She also should use an additional birth control method for 1 week. o Eclampsia is the occurrence of seizures that arent caused by a cerebral disorder in a patient who has pregnancy-induced hypertension. o In placenta previa, bleeding is painless and seldom fatal on the first occasion, but it becomes heavier with each subsequent episode. o Treatment for abruptio placentae is usually immediate cesarean delivery. o Drugs used to treat withdrawal symptoms in neonates include phenobarbital (Luminal), camphorated opium tincture (paregoric), and diazepam (Valium). o Infants with Down syndrome typically have marked hypotonia, floppiness, slanted eyes, excess skin on the back of the neck, flattened bridge of the nose, flat facial features, spadelike hands, short and broad feet, small male genitalia, absence of Moros reflex, and a simian crease on the hands. o The failure rate of a contraceptive is determined by the experience of 100 women for 1 year. Its expressed as pregnancies per 100 woman-years. o The narrowest diameter of the pelvic inlet is the anteroposterior (diagonal conjugate). o The chorion is the outermost extraembryonic membrane that gives rise to the placenta.
o The corpus luteum secretes large quantities of progesterone. o From the 8th week of gestation through delivery, the developing cells are known as a fetus. o In an incomplete abortion, the fetus is expelled, but parts of the placenta and membrane remain in the uterus. o The circumference of a neonates head is normally 2 to 3 cm greater than the circumference of the chest. o After administering magnesium sulfate to a pregnant patient for hypertension or preterm labor, the nurse should monitor the respiratory rate and deep tendon reflexes. o During the first hour after birth (the period of reactivity), the neonate is alert and awake. o When a pregnant patient has undiagnosed vaginal bleeding, vaginal examination should be avoided until ultrasonography rules out placenta previa. o After delivery, the first nursing action is to establish the neonates airway. o Nursing interventions for a patient with placenta previa include positioning the patient on her left side for maximum fetal perfusion, monitoring fetal heart tones, and administering I.V. fluids and oxygen, as ordered. o The specific gravity of a neonates urine is 1.003 to 1.030. A lower specific gravity suggests overhydration; a higher one suggests dehydration. o The neonatal period extends from birth to day 28. Its also called the first 4 weeks or first month of life. o A woman who is breast-feeding should rub a mild emollient cream or a few drops of breast milk (or colostrum) on the nipples after each feeding. She should let the breasts air-dry to prevent them from cracking. o Breast-feeding mothers should increase their fluid intake to 2 to 3 qt (2,500 to 3,000 ml) daily. o After feeding an infant with a cleft lip or palate, the nurse should rinse the infants mouth with sterile water. o The nurse instills erythromycin in a neonates eyes primarily to prevent blindness caused by gonorrhea or chlamydia. o Human immunodeficiency virus (HIV) has been cultured in breast milk and can be transmitted by an HIV-positive mother who breast-feeds her infant. o A fever in the first 24 hours postpartum is most likely caused by dehydration rather than infection. o Preterm neonates or neonates who cant maintain a skin temperature of at least 97.6 F (36.4 C) should receive care in an incubator (Isolette) or a radiant warmer. In a radiant warmer, a heat-sensitive probe taped to the neonates skin activates the heater unit automatically to maintain the desired temperature. o During labor, the resting phase between contractions is at least 30 seconds. o Lochia rubra is the vaginal discharge of almost pure blood that occurs during the first few days after childbirth. o Lochia serosa is the serous vaginal discharge that occurs 4 to 7 days after childbirth. o Lochia alba is the vaginal discharge of decreased blood and increased leukocytes thats the final stage of lochia. It occurs 7 to 10 days after childbirth. o Colostrum, the precursor of milk, is the first secretion from the breasts after delivery. o The length of the uterus increases from 2" (6.3 cm) before pregnancy to 12" (32 cm) at term. o To estimate the true conjugate (the smallest inlet measurement of the pelvis), deduct 1.5 cm from the diagonal conjugate (usually 12 cm). A true conjugate of 10.5 cm enables the fetal head (usually 10 cm) to pass.
o The smallest outlet measurement of the pelvis is the intertuberous diameter, which is the transverse diameter between the ischial tuberosities. o Electronic fetal monitoring is used to assess fetal well-being during labor. If compromised fetal status is suspected, fetal blood pH may be evaluated by obtaining a scalp sample. o In an emergency delivery, enough pressure should be applied to the emerging fetuss head to guide the descent and prevent a rapid change in pressure within the molded fetal skull. o After delivery, a multiparous woman is more susceptible to bleeding than a primiparous woman because her uterine muscles may be overstretched and may not contract efficiently. o Neonates who are delivered by cesarean birth have a higher incidence of respiratory distress syndrome. o The nurse should suggest ambulation to a postpartum patient who has gas pain and flatulence. o Massaging the uterus helps to stimulate contractions after the placenta is delivered. o When providing phototherapy to a neonate, the nurse should cover the neonates eyes and genital area. o The narcotic antagonist naloxone (Narcan) may be given to a neonate to correct respiratory depression caused by narcotic administration to the mother during labor. o In a neonate, symptoms of respiratory distress syndrome include expiratory grunting or whining, sandpaper breath sounds, and seesaw retractions. o Cerebral palsy presents as asymmetrical movement, irritability, and excessive, feeble crying in a long, thin infant. o The nurse should assess a breech-birth neonate for hydrocephalus, hematomas, fractures, and other anomalies caused by birth trauma. o When a patient is admitted to the unit in active labor, the nurses first action is to listen for fetal heart tones. o In a neonate, long, brittle fingernails are a sign of postmaturity. o Desquamation (skin peeling) is common in postmature neonates. o A mother should allow her infant to breast-feed until the infant is satisfied. The time may vary from 5 to 20 minutes. o Nitrazine paper is used to test the pH of vaginal discharge to determine the presence of amniotic fluid. o A pregnant patient normally gains 2 to 5 lb (1 to 2.5 kg) during the first trimester and slightly less than 1 lb (0.5 kg) per week during the last two trimesters. o Neonatal jaundice in the first 24 hours after birth is known as pathological jaundice and is a sign of erythroblastosis fetalis. o A classic difference between abruptio placentae and placenta previa is the degree of pain. Abruptio placentae causes pain, whereas placenta previa causes painless bleeding. o Because a major role of the placenta is to function as a fetal lung, any condition that interrupts normal blood flow to or from the placenta increases fetal partial pressure of arterial carbon dioxide and decreases fetal pH. o Precipitate labor lasts for approximately 3 hours and ends with delivery of the neonate. o Methylergonovine (Methergine) is an oxytocic agent used to prevent and treat postpartum hemorrhage caused by uterine atony or subinvolution. o As emergency treatment for excessive uterine bleeding, 0.2 mg of methylergonovine (Methergine) is injected I.V. over 1 minute while the patients blood pressure and uterine contractions are monitored.
o Braxton Hicks contractions are usually felt in the abdomen and dont cause cervical change. True labor contractions are felt in the front of the abdomen and back and lead to progressive cervical dilation and effacement. o The average birth weight of neonates born to mothers who smoke is 6 oz (170 g) less than that of neonates born to nonsmoking mothers. o Culdoscopy is visualization of the pelvic organs through the posterior vaginal fornix. o The nurse should teach a pregnant vegetarian to obtain protein from alternative sources, such as nuts, soybeans, and legumes. o The nurse should instruct a pregnant patient to take only prescribed prenatal vitamins because over-the-counter high-potency vitamins may harm the fetus. o High-sodium foods can cause fluid retention, especially in pregnant patients. o A pregnant patient can avoid constipation and hemorrhoids by adding fiber to her diet. o If a fetus has late decelerations (a sign of fetal hypoxia), the nurse should instruct the mother to lie on her left side and then administer 8 to 10 L of oxygen per minute by mask or cannula. The nurse should notify the physician. The side-lying position removes pressure on the inferior vena cava. o Oxytocin (Pitocin) promotes lactation and uterine contractions. o Lanugo covers the fetuss body until about 20 weeks gestation. Then it begins to disappear from the face, trunk, arms, and legs, in that order. o In a neonate, hypoglycemia causes temperature instability, hypotonia, jitteriness, and seizures. Premature, postmature, small-for-gestational-age, and large-forgestational-age neonates are susceptible to this disorder. o Neonates typically need to consume 50 to 55 cal per pound of body weight daily. o Because oxytocin (Pitocin) stimulates powerful uterine contractions during labor, it must be administered under close observation to help prevent maternal and fetal distress. o During fetal heart rate monitoring, variable decelerations indicate compression or prolapse of the umbilical cord. o Cytomegalovirus is the leading cause of congenital viral infection. o Tocolytic therapy is indicated in premature labor, but contraindicated in fetal death, fetal distress, or severe hemorrhage. o Through ultrasonography, the biophysical profile assesses fetal well-being by measuring fetal breathing movements, gross body movements, fetal tone, reactive fetal heart rate (nonstress test), and qualitative amniotic fluid volume. o A neonate whose mother has diabetes should be assessed for hyperinsulinism. o In a patient with preeclampsia, epigastric pain is a late symptom and requires immediate medical intervention. o After a stillbirth, the mother should be allowed to hold the neonate to help her come to terms with the death. o Molding is the process by which the fetal head changes shape to facilitate movement through the birth canal. o If a woman receives a spinal block before delivery, the nurse should monitor the patients blood pressure closely. o If a woman suddenly becomes hypotensive during labor, the nurse should increase the infusion rate of I.V. fluids as prescribed. o The best technique for assessing jaundice in a neonate is to blanch the tip of the nose or the area just above the umbilicus. o During fetal heart monitoring, early deceleration is caused by compression of the head during labor.
o After the placenta is delivered, the nurse may add oxytocin (Pitocin) to the patients I.V. solution, as prescribed, to promote postpartum involution of the uterus and stimulate lactation. o Pica is a craving to eat nonfood items, such as dirt, crayons, chalk, glue, starch, or hair. It may occur during pregnancy and can endanger the fetus. o A pregnant patient should take folic acid because this nutrient is required for rapid cell division. o A woman who is taking clomiphene (Clomid) to induce ovulation should be informed of the possibility of multiple births with this drug. o If needed, cervical suturing is usually done between 14 and 18 weeks gestation to reinforce an incompetent cervix and maintain pregnancy. The suturing is typically removed by 35 weeks gestation. o During the first trimester, a pregnant woman should avoid all drugs unless doing so would adversely affect her health. o Most drugs that a breast-feeding mother takes appear in breast milk. o The Food and Drug Administration has established the following five categories of drugs based on their potential for causing birth defects: A, no evidence of risk; B, no risk found in animals, but no studies have been done in women; C, animal studies have shown an adverse effect, but the drug may be beneficial to women despite the potential risk; D, evidence of risk, but its benefits may outweigh its risks; and X, fetal anomalies noted, and the risks clearly outweigh the potential benefits. o A patient with a ruptured ectopic pregnancy commonly has sharp pain in the lower abdomen, with spotting and cramping. She may have abdominal rigidity; rapid, shallow respirations; tachycardia; and shock. o A patient with a ruptured ectopic pregnancy commonly has sharp pain in the lower abdomen, with spotting and cramping. She may have abdominal rigidity; rapid, shallow respirations; tachycardia; and shock. o The mechanics of delivery are engagement, descent and flexion, internal rotation, extension, external rotation, restitution, and expulsion. o A probable sign of pregnancy, McDonalds sign is characterized by an ease in flexing the body of the uterus against the cervix. o Amenorrhea is a probable sign of pregnancy. o A pregnant womans partner should avoid introducing air into the vagina during oral sex because of the possibility of air embolism. o The presence of human chorionic gonadotropin in the blood or urine is a probable sign of pregnancy. o Radiography isnt usually used in a pregnant woman because it may harm the developing fetus. If radiography is essential, it should be performed only after 36 weeks gestation. o A pregnant patient who has had rupture of the membranes or who is experiencing vaginal bleeding shouldnt engage in sexual intercourse. o Milia may occur as pinpoint spots over a neonates nose. o The duration of a contraction is timed from the moment that the uterine muscle begins to tense to the moment that it reaches full relaxation. Its measured in seconds. o The union of a male and a female gamete produces a zygote, which divides into the fertilized ovum. o The first menstrual flow is called menarche and may be anovulatory (infertile). o Spermatozoa (or their fragments) remain in the vagina for 72 hours after sexual intercourse. o Prolactin stimulates and sustains milk production. o Strabismus is a normal finding in a neonate.
o A postpartum patient may resume sexual intercourse after the perineal or uterine wounds heal (usually within 4 weeks after delivery). o A pregnant staff member shouldnt be assigned to work with a patient who has cytomegalovirus infection because the virus can be transmitted to the fetus. o Fetal demise is death of the fetus after viability. o Respiratory distress syndrome develops in premature neonates because their alveoli lack surfactant. o The most common method of inducing labor after artificial rupture of the membranes is oxytocin (Pitocin) infusion. o After the amniotic membranes rupture, the initial nursing action is to assess the fetal heart rate. o The most common reasons for cesarean birth are malpresentation, fetal distress, cephalopelvic disproportion, pregnancy-induced hypertension, previous cesarean birth, and inadequate progress in labor. o Amniocentesis increases the risk of spontaneous abortion, trauma to the fetus or placenta, premature labor, infection, and Rh sensitization of the fetus. o After amniocentesis, abdominal cramping or spontaneous vaginal bleeding may indicate complications. o To prevent her from developing Rh antibodies, an Rh-negative primigravida should receive Rho(D) immune globulin (RhoGAM) after delivering an Rh-positive neonate. o If a pregnant patients test results are negative for glucose but positive for acetone, the nurse should assess the patients diet for inadequate caloric intake. o If a pregnant patients test results are negative for glucose but positive for acetone, the nurse should assess the patients diet for inadequate caloric intake. o Rubella infection in a pregnant patient, especially during the first trimester, can lead to spontaneous abortion or stillbirth as well as fetal cardiac and other birth defects. o A pregnant patient should take an iron supplement to help prevent anemia. o Direct antiglobulin (direct Coombs) test is used to detect maternal antibodies attached to red blood cells in the neonate. o Nausea and vomiting during the first trimester of pregnancy are caused by rising levels of the hormone human chorionic gonadotropin. o Before discharging a patient who has had an abortion, the nurse should instruct her to report bright red clots, bleeding that lasts longer than 7 days, or signs of infection, such as a temperature of greater than 100 F (37.8 C), foul-smelling vaginal discharge, severe uterine cramping, nausea, or vomiting. o When informed that a patients amniotic membrane has broken, the nurse should check fetal heart tones and then maternal vital signs. o The duration of pregnancy averages 280 days, 40 weeks, 9 calendarmonths, or 10 lunar months. o The initial weight loss for a healthy neonate is 5% to 10% of birth weight. o The normal hemoglobin value in neonates is 17 to 20 g/dl. o Crowning is the appearance of the fetuss head when its largest diameter is encircled by the vulvovaginal ring. o A multipara is a woman who has had two or more pregnancies that progressed to viability, regardless of whether the offspring were alive at birth. o In a pregnant patient, preeclampsia may progress to eclampsia, which is characterized by seizures and may lead to coma. o The Apgar score is used to assess the neonates vital functions. Its obtained at 1 minute and 5 minutes after delivery. The score is based on respiratory effort, heart rate, muscle tone, reflex irritability, and color.
o Because of the anti-insulin effects of placental hormones, insulin requirements increase during the third trimester. o Gestational age can be estimated by ultrasound measurement of maternal abdominal circumference, fetal femur length, and fetal head size. These measurements are most accurate between 12 and 18 weeks gestation. o Skeletal system abnormalities and ventricular septal defects are the most common disorders of infants who are born to diabetic women. The incidence of congenital malformation is three times higher in these infants than in those born to nondiabetic women. o Skeletal system abnormalities and ventricular septal defects are the most common disorders of infants who are born to diabetic women. The incidence of congenital malformation is three times higher in these infants than in those born to nondiabetic women. o The patient with preeclampsia usually has puffiness around the eyes or edema in the hands (for example, I cant put my wedding ring on.). o Kegel exercises require contraction and relaxation of the perineal muscles. These exercises help strengthen pelvic muscles and improve urine control in postpartum patients. o Symptoms of postpartum depression range from mild postpartum blues to intense, suicidal, depressive psychosis. o The preterm neonate may require gavage feedings because of a weak sucking reflex, uncoordinated sucking, or respiratory distress. o Acrocyanosis (blueness and coolness of the arms and legs) is normal in neonates because of their immature peripheral circulatory system. o To prevent ophthalmia neonatorum (a severe eye infection caused by maternal gonorrhea), the nurse may administer one of three drugs, as prescribed, in the neonates eyes: tetracycline, silver nitrate, or erythromycin. o Neonatal testing for phenylketonuria is mandatory in most states. o The nurse should place the neonate in a 30-degree Trendelenburg position to facilitate mucus drainage. o The nurse may suction the neonates nose and mouth as needed with a bulb syringe or suction trap. o To prevent heat loss, the nurse should place the neonate under a radiant warmer during suctioning and initial delivery-room care, and then wrap the neonate in a warmed blanket for transport to the nursery. o The umbilical cord normally has two arteries and one vein. o When providing care, the nurse should expose only one part of an infants body at a time. o Lightening is settling of the fetal head into the brim of the pelvis. o If the neonate is stable, the mother should be allowed to breast-feed within the neonates first hour of life. o The nurse should check the neonates temperature every 1 to 2 hours until its maintained within normal limits. o At birth, a neonate normally weighs 5 to 9 lb (2 to 4 kg), measures 18" to 22" (45.5 to 56 cm) in length, has a head circumference of 13" to 14" (34 to 35.5 cm), and has a chest circumference thats 1" (2.5 cm) less than the head circumference. o In the neonate, temperature normally ranges from 98 to 99 F (36.7 to 37.2 C), apical pulse rate averages 120 to 160 beats/minute, and respirations are 40 to 60 breaths/minute. o The diamond-shaped anterior fontanel usually closes between ages 12 and 18 months. The triangular posterior fontanel usually closes by age 2 months.
o In the neonate, a straight spine is normal. A tuft of hair over the spine is an abnormal finding. o Prostaglandin gel may be applied to the vagina or cervix to ripen an unfavorable cervix before labor induction with oxytocin (Pitocin). o Supernumerary nipples are occasionally seen on neonates. Theyusually appear along a line that runs from each axilla, through the normal nipple area, and to the groin. o Meconium is a material that collects in the fetuss intestines and forms the neonates first feces, which are black and tarry. o The presence of meconium in the amniotic fluid during labor indicates possible fetal distress and the need to evaluate the neonate for meconium aspiration. o To assess a neonates rooting reflex, the nurse touches a finger to the cheek or the corner of the mouth. Normally, the neonate turns his head toward the stimulus, opens his mouth, and searches for the stimulus. o Harlequin sign is present when a neonate who is lying on his side appears red on the dependent side and pale on the upper side. o Mongolian spots can range from brown to blue. Their color depends on how close melanocytes are to the surface of the skin. They most commonly appear as patches across the sacrum, buttocks, and legs. o Mongolian spots are common in non-white infants and usuallydisappear by age 2 to 3 years. o Vernix caseosa is a cheeselike substance that covers and protects the fetuss skin in utero. It may be rubbed into the neonates skin or washed away in one or two baths. o Caput succedaneum is edema that develops in and under the fetal scalp during labor and delivery. It resolves spontaneously and presents no danger to the neonate. The edema doesnt cross the suture line. o Nevus flammeus, or port-wine stain, is a diffuse pink to dark bluish red lesion on a neonates face or neck. o The Guthrie test (a screening test for phenylketonuria) is most reliable if its done between the second and sixth days after birth and is performed after the neonate has ingested protein. o To assess coordination of sucking and swallowing, the nurse should observe the neonates first breast-feeding or sterile water bottle-feeding. o To establish a milk supply pattern, the mother should breast-feed her infant at least every 4 hours. During the first month, she should breast-feed 8 to 12 times daily (demand feeding). o To avoid contact with blood and other body fluids, the nurse should wear gloves when handling the neonate until after the first bath is given. o If a breast-fed infant is content, has good skin turgor, an adequate number of wet diapers, and normal weight gain, the mothers milk supply is assumed to be adequate. o In the supine position, a pregnant patients enlarged uterus impairs venous return from the lower half of the body to the heart, resulting in supine hypotensive syndrome, or inferior vena cava syndrome. o Tocolytic agents used to treat preterm labor include terbutaline (Brethine), ritodrine (Yutopar), and magnesium sulfate. o A pregnant woman who has hyperemesis gravidarum may require hospitalization to treat dehydration and starvation. o Diaphragmatic hernia is one of the most urgent neonatal surgical emergencies. By compressing and displacing the lungs and heart, this disorder can cause respiratory distress shortly after birth. o Common complications of early pregnancy (up to 20 weeks gestation) include fetal loss and serious threats to maternal health.
o Fetal embodiment is a maternal developmental task that occurs in the second trimester. During this stage, the mother may complain that she never gets to sleep because the fetus always gives her a thump when she tries. o Visualization in pregnancy is a process in which the mother imagines what the child shes carrying is like and becomes acquainted with it. o Hemodilution of pregnancy is the increase in blood volume that occurs during pregnancy. The increased volume consists of plasma and causes an imbalance between the ratio of red blood cells to plasma and a resultant decrease in hematocrit. o Mean arterial pressure of greater than 100 mm Hg after 20 weeks of pregnancy is considered hypertension. o The treatment for supine hypotension syndrome (a condition that sometimes occurs in pregnancy) is to have the patient lie on her left side. o A contributing factor in dependent edema in the pregnant patient is the increase of femoral venous pressure from 10 mm Hg (normal) to 18 mm Hg (high). o Hyperpigmentation of the pregnant patients face, formerly called chloasma and now referred to as melasma, fades after delivery. o The hormone relaxin, which is secreted first by the corpus luteum and later by the placenta, relaxes the connective tissue and cartilage of the symphysis pubis and the sacroiliac joint to facilitate passage of the fetus during delivery. o Progesterone maintains the integrity of the pregnancy by inhibiting uterine motility. o Ladins sign, an early indication of pregnancy, causes softening of a spot on the anterior portion of the uterus, just above the uterocervical juncture. o During pregnancy, the abdominal line from the symphysis pubis to the umbilicus changes from linea alba to linea nigra. o In neonates, cold stress affects the circulatory, regulatory, and respiratory systems. o Obstetric data can be described by using the F/TPAL system: o F/T: Full-term delivery at 38 weeks or longer o P: Preterm delivery between 20 and 37 weeks o A: Abortion or loss of fetus before 20 weeks o L: Number of children living (if a child has died, further explanation is needed to clarify the discrepancy in numbers). o Parity doesnt refer to the number of infants delivered, only the number of deliveries. o Women who are carrying more than one fetus should be encouraged to gain 35 to 45 lb (15.5 to 20.5 kg) during pregnancy. o The recommended amount of iron supplement for the pregnant patient is 30 to 60 mg daily. o Drinking six alcoholic beverages a day or a single episode of binge drinking in the first trimester can cause fetal alcohol syndrome. o Chorionic villus sampling is performed at 8 to 12 weeks of pregnancyfor early identification of genetic defects. o In percutaneous umbilical blood sampling, a blood sample is obtained from the umbilical cord to detect anemia, genetic defects, and blood incompatibility as well as to assess the need for blood transfusions. o The period between contractions is referred to as the interval, or resting phase. During this phase, the uterus and placenta fill with blood and allow for the exchange of oxygen, carbon dioxide, and nutrients. o In a patient who has hypertonic contractions, the uterus doesnt have an opportunity to relax and there is no interval between contractions. As a result, the fetus may experience hypoxia or rapid delivery may occur.
o Two qualities of the myometrium are elasticity, which allows it to stretch yet maintain its tone, and contractility, which allows it to shorten and lengthen in a synchronized pattern. o During crowning, the presenting part of the fetus remains visible during the interval between contractions. o Uterine atony is failure of the uterus to remain firmly contracted. o The major cause of uterine atony is a full bladder. o If the mother wishes to breast-feed, the neonate should be nursed as soon as possible after delivery. o A smacking sound, milk dripping from the side of the mouth, and sucking noises all indicate improper placement of the infants mouth over the nipple. o Before feeding is initiated, an infant should be burped to expel air from the stomach. o Most authorities strongly encourage the continuation of breast-feeding on both the affected and the unaffected breast of patients with mastitis. o Neonates are nearsighted and focus on items that are held 10" to 12" (25 to 30.5 cm) away. o In a neonate, low-set ears are associated with chromosomal abnormalities such as Down syndrome. o Meconium is usually passed in the first 24 hours; however, passage may take up to 72 hours. o Boys who are born with hypospadias shouldnt be circumcised at birth because the foreskin may be needed for constructive surgery. o In the neonate, the normal blood glucose level is 45 to 90 mg/dl. o Hepatitis B vaccine is usually given within 48 hours of birth. o Hepatitis B immune globulin is usually given within 12 hours of birth. o HELLP (hemolysis, elevated liver enzymes, and low platelets) syndrome is an unusual variation of pregnancy-induced hypertension. o Maternal serum alpha-fetoprotein is detectable at 7 weeks of gestation and peaks in the third trimester. High levels detected between the 16th and 18th weeks are associated with neural tube defects. Low levels are associated with Down syndrome. o An arrest of descent occurs when the fetus doesnt descend through the pelvic cavity during labor. Its commonly associated with cephalopelvic disproportion, and cesarean delivery may be required. o A late sign of preeclampsia is epigastric pain as a result of severe liver edema. o In the patient with preeclampsia, blood pressure returns to normal during the puerperal period. o To obtain an estriol level, urine is collected for 24 hours. o An estriol level is used to assess fetal well-being and maternal renal functioning as well as to monitor a pregnancy thats complicated by diabetes. o A pregnant patient with vaginal bleeding shouldnt have a pelvic examination. o In the early stages of pregnancy, the finding of glucose in the urine may be related to the increased shunting of glucose to the developing placenta, without a corresponding increase in the reabsorption capability of the kidneys. o A patient who has premature rupture of the membranes is at significant risk for infection if labor doesnt begin within 24 hours. o Infants of diabetic mothers are susceptible to macrosomia as a result of increased insulin production in the fetus. o To prevent heat loss in the neonate, the nurse should bathe one part of his body at a time and keep the rest of the body covered. o A patient who has a cesarean delivery is at greater risk for infection than the patient who gives birth vaginally.
o The occurrence of thrush in the neonate is probably caused by contact with the organism during delivery through the birth canal. o The nurse should keep the sac of meningomyelocele moist with normal saline solution. o If fundal height is at least 2 cm less than expected, the cause may be growth retardation, missed abortion, transverse lie, or false pregnancy. o Fundal height that exceeds expectations by more than 2 cm may be caused by multiple gestation, polyhydramnios, uterine myomata, or a large baby. o A major developmental task for a woman during the first trimester of pregnancy is accepting the pregnancy. o Unlike formula, breast milk offers the benefit of maternal antibodies. o Spontaneous rupture of the membranes increases the risk of a prolapsed umbilical cord. o A clinical manifestation of a prolapsed umbilical cord is variable decelerations. o During labor, to relieve supine hypotension manifested by nausea and vomiting and paleness, turn the patient on her left side. o If the ovum is fertilized by a spermatozoon carrying a Y chromosome, a male zygote is formed. o Implantation occurs when the cellular walls of the blastocyte implants itself in the endometrium, usually 7 to 9 days after fertilization. o Implantation occurs when the cellular walls of the blastocyte implants itself in the endometrium, usually 7 to 9 days after fertilization. o Heart development in the embryo begins at 2 to 4 weeks and is complete by the end of the embryonic stage. o Methergine stimulates uterine contractions. o The administration of folic acid during the early stages of gestation may prevent neural tube defects. o With advanced maternal age, a common genetic problem is Down syndrome. o With early maternal age, cephalopelvic disproportion commonly occurs. o In the early postpartum period, the fundus should be midline at the umbilicus. o A rubella vaccine shouldnt be given to a pregnant woman. The vaccine can be administered after delivery, but the patient should be instructed to avoid becoming pregnant for 3 months. o A 16-year-old girl who is pregnant is at risk for having a low-birth-weight neonate. o The mothers Rh factor should be determined before an amniocentesis is performed. o Maternal hypotension is a complication of spinal block. o After delivery, if the fundus is boggy and deviated to the right side, the patient should empty her bladder. o Before providing a specimen for a sperm count, the patient should avoid ejaculation for 48 to 72 hours. o The hormone human chorionic gonadotropin is a marker for pregnancy. o Painless vaginal bleeding during the last trimester of pregnancy may indicate placenta previa. o During the transition phase of labor, the woman usually is irritable and restless. o Because women with diabetes have a higher incidence of birth anomalies than women without diabetes, an alpha-fetoprotein level may be ordered at 15 to 17 weeks gestation. o To avoid puncturing the placenta, a vaginal examination shouldnt be performed on a pregnant patient who is bleeding. o A patient who has postpartum hemorrhage caused by uterine atony should be given oxytocin as prescribed.
o Laceration of the vagina, cervix, or perineum produces bright red bleeding that often comes in spurts. The bleeding is continuous, even when the fundus is firm. o Hot compresses can help to relieve breast tenderness after breast-feeding. o The fundus of a postpartum patient is massaged to stimulate contraction of the uterus and prevent hemorrhage. o A mother who has a positive human immunodeficiency virus test result shouldnt breast-feed her infant. o Dinoprostone (Cervidil) is used to ripen the cervix. o Breast-feeding of a premature neonate born at 32 weeks gestation can be accomplished if the mother expresses milk and feeds the neonate by gavage. o If a pregnant patients rubella titer is less than 1:8, she should be immunized after delivery. o The administration of oxytocin (Pitocin) is stopped if the contractions are 90 seconds or longer. o For an extramural delivery (one that takes place outside of a normal delivery center), the priorities for care of the neonate include maintaining a patent airway, supporting efforts to breathe, monitoring vital signs, and maintaining adequate body temperature. o Subinvolution may occur if the bladder is distended after delivery. o The nurse must place identification bands on both the mother and the neonate before they leave the delivery room. o Erythromycin is given at birth to prevent ophthalmia neonatorum. o Pelvic-tilt exercises can help to prevent or relieve backache during pregnancy. o Before performing a Leopold maneuver, the nurse should ask thepatient to empty her bladder. 1. Accompanied by her husband, a patient seeks admission to the labor and delivery area. The client states that she is in labor, and says she attended the hospital clinic for prenatal care. Which question should the nurse ask her first? a. Do you have any chronic illness? b. Do you have any allergies? c. What is your expected due date? d. Who will be with you during labor? 2. A patient is in the second stage of labor. During this stage, how frequently should the nurse in charge assess her uterine contractions? a. Every 5 minutes b. Every 15 minutes c. Every 30 minutes d. Every 60 minutes 3. A patient is in last trimester of pregnancy. Nurse Jane should instruct her to notify her primary health care provider immediately if she notices: a. Blurred vision b. Hemorrhoids c. Increased vaginal mucus d. Shortness of breath on exertion 4. The nurse in charge is reviewing a patients prenatal history. Which finding indicates a genetic risk factor? a. The patient is 25 years old b. The patient has a child with cystic fibrosis
c. The patient was exposed to rubella at 36 weeks gestation d. The patient has a history of preterm labor at 32 weeks gestation 5. A adult female patient is using the rhythm (calendar-basal body temperature) method of family planning. In this method, the unsafe period for sexual intercourse is indicated by; a. Return preovulatory basal body temperature b. Basal body temperature increase of 0.1 degrees to 0.2 degrees on the 2ndor 3rd day of cycle c. 3 full days of elevated basal body temperature and clear, thin cervical mucus d. Breast tenderness and mittelschmerz 6. During a nonstress test (NST), the electronic tracing displays a relatively flat line for fetal movement, making it difficult to evaluate the fetal heart rate (FHR). To mark the strip, the nurse in charge should instruct the client to push the control button at which time? a. At the beginning of each fetal movement b. At the beginning of each contraction c. After every three fetal movements d. At the end of fetal movement 7. When evaluating a clients knowledge of symptoms to report during her pregnancy, which statement would indicate to the nurse in charge that the client understands the information given to her? a. Ill report increased frequency of urination. b. If I have blurred or double vision, I should call the clinic immediately. c. If I feel tired after resting, I should report it immediately. d. Nausea should be reported immediately. 8. When assessing a client during her first prenatal visit, the nurse discovers that the client had a reduction mammoplasty. The mother indicates she wants to breast-feed. What information should the nurse give to this mother regarding breast-feeding success? a. Its contraindicated for you to breast-feed following this type of surgery. b. I support your commitment; however, you may have to supplement each feeding with formula. c. You should check with your surgeon to determine whether breast-feeding would be possible. d. You should be able to breast-feed without difficulty. 9. Following a precipitous delivery, examination of the clients vagina reveals a fourth-degree laceration. Which of the following would be contraindicated when caring for this client? a. Applying cold to limit edema during the first 12 to 24 hours b. Instructing the client to use two or more peripads to cushion the area c. Instructing the client on the use of sitz baths if ordered d. Instructing the client about the importance of perineal (Kegel) exercises 10. A client makes a routine visit to the prenatal clinic. Although shes 14 weeks pregnant, the size of her uterus approximates that in an 18- to 20-week pregnancy. Dr. Diaz diagnoses gestational trophoblastic disease and orders ultrasonography. The nurse expects ultrasonography to reveal: a. an empty gestational sac. b. grapelike clusters. c. a severely malformed fetus. d. an extrauterine pregnancy.
11. After completing a second vaginal examination of a client in labor, the nurse-midwife determines that the fetus is in the right occiput anterior position and at 1 station. Based on these findings, the nurse-midwife knows that the fetal presenting part is: a. 1 cm below the ischial spines. b. directly in line with the ischial spines. c. 1 cm above the ischial spines. d. in no relationship to the ischial spines. 12. Which of the following would be inappropriate to assess in a mother whos breast-feeding? a. The attachment of the baby to the breast. b. The mothers comfort level with positioning the baby. c. Audible swallowing. d. The babys lips smacking 13. During a prenatal visit at 4 months gestation, a pregnant client asks whether tests can be done to identify fetal abnormalities. Between 18 and 40 weeks gestation, which procedure is used to detect fetal anomalies? a. Amniocentesis. b. Chorionic villi sampling. c. Fetoscopy. d. Ultrasound 14. A client, 30 weeks pregnant, is scheduled for a biophysical profile (BPP) to evaluate the health of her fetus. Her BPP score is 8. What does this score indicate? a. The fetus should be delivered within 24 hours. b. The client should repeat the test in 24 hours. c. The fetus isnt in distress at this time. d. The client should repeat the test in 1 week. 15. A client whos 36 weeks pregnant comes to the clinic for a prenatal checkup. To assess the clients preparation for parenting, the nurse might ask which question? a. Are you planning to have epidural anesthesia? b. Have you begun prenatal classes? c. What changes have you made at home to get ready for the baby? d. Can you tell me about the meals you typically eat each day? 16. A client whos admitted to labor and delivery has the following assessment findings: gravida 2 para 1, estimated 40 weeks gestation, contractions 2 minutes apart, lasting 45 seconds, vertex +4 station. Which of the following would be the priority at this time? a. Placing the client in bed to begin fetal monitoring. b. Preparing for immediate delivery. c. Checking for ruptured membranes. d. Providing comfort measures. 17. Nurse Roy is caring for a client in labor. The external fetal monitor shows a pattern of variable decelerations in fetal heart rate. What should the nurse do first? a. Change the clients position. b. Prepare for emergency cesarean section. c. Check for placenta previa. d. Administer oxygen.
18. The nurse in charge is caring for a postpartum client who had a vaginal delivery with a midline episiotomy. Which nursing diagnosis takes priority for this client? a. Risk for deficient fluid volume related to hemorrhage b. Risk for infection related to the type of delivery c. Pain related to the type of incision d. Urinary retention related to periurethral edema 19. Which change would the nurse identify as a progressive physiological change in postpartum period? a. Lactation b. Lochia c. Uterine involution d. Diuresis 20. A 39-year-old at 37 weeks gestation is admitted to the hospital with complaints of vaginal bleeding following the use of cocaine 1 hour earlier. Which complication is most likely causing the clients complaint of vaginal bleeding? a. Placenta previa b. Abruptio placentae c. Ectopic pregnancy d. Spontaneous abortion 21. A client with type 1 diabetes mellitus whos a multigravida visits the clinic at 27 weeks gestation. The nurse should instruct the client that for most pregnant women with type 1 diabetes mellitus: a. Weekly fetal movement counts are made by the mother. b. Contraction stress testing is performed weekly. c. Induction of labor is begun at 34 weeks gestation. d. Nonstress testing is performed weekly until 32 weeks gestation 22. When administering magnesium sulfate to a client with preeclampsia, the nurse understands that this drug is given to: a. Prevent seizures b. Reduce blood pressure c. Slow the process of labor d. Increase dieresis 23. Whats the approximate time that the blastocyst spends traveling to the uterus for implantation? a. 2 days b. 7 days c. 10 days d. 14 weeks 24. After teaching a pregnant woman who is in labor about the purpose of the episiotomy, which of the following purposes stated by the client would indicate to the nurse that the teaching was effective? a. Shortens the second stage of labor b. Enlarges the pelvic inlet c. Prevents perineal edema d. Ensures quick placenta delivery 25. A primigravida client at about 35 weeks gestation in active labor has had no prenatal care and admits to cocaine use during the pregnancy. Which of the following persons must the nurse notify?
a. Nursing unit manager so appropriate agencies can be notified b. Head of the hospitals security department c. Chaplain in case the fetus dies in utero d. Physician who will attend the delivery of the infant 26. When preparing a teaching plan for a client who is to receive a rubella vaccine during the postpartum period, the nurse in charge should include which of the following? a. The vaccine prevents a future fetus from developing congenital anomalies b. Pregnancy should be avoided for 3 months after the immunization c. The client should avoid contact with children diagnosed with rubella d. The injection will provide immunity against the 7-day measles. 27. A client with eclampsia begins to experience a seizure. Which of the following would the nurse in charge do first? a. Pad the side rails b. Place a pillow under the left buttock c. Insert a padded tongue blade into the mouth d. Maintain a patent airway 28. While caring for a multigravida client in early labor in a birthing center, which of the following foods would be best if the client requests a snack? a. Yogurt b. Cereal with milk c. Vegetable soup d. Peanut butter cookies 29. The multigravida mother with a history of rapid labor who us in active labor calls out to the nurse, The baby is coming! which of the following would be the nurses first action? a. Inspect the perineum b. Time the contractions c. Auscultate the fetal heart rate d. Contact the birth attendant 30. While assessing a primipara during the immediate postpartum period, the nurse in charge plans to use both hands to assess the clients fundus to: a. Prevent uterine inversion b. Promote uterine involution c. Hasten the puerperium period d. Determine the size of the fundus 1. Answer C. When obtaining the history of a patient who may be in labor, the nurses highest priority is to determine her current status, particularly her due date, gravidity, and parity. Gravidity and parity affect the duration of labor and the potential for labor complications. Later, the nurse should ask about chronic illness, allergies, and support persons. 2. Answer B. During the second stage of labor, the nurse should assess the strength, frequency, and duration of contraction every 15 minutes. If maternal or fetal problems are detected, more frequent monitoring is necessary. An interval of 30 to 60 minutes between assessments is too long because of variations in the length and duration of patients labor.
3. Answer A. Blurred vision of other visual disturbance, excessive weight gain, edema, and increased blood pressure may signal severe preeclampsia. This condition may lead to eclampsia, which has potentially serious consequences for both the patient and fetus. Although hemorrhoids may be a problem during pregnancy, they do not require immediate attention. Increased vaginal mucus and dyspnea on exertion are expected as pregnancy progresses. 4. Answer B. Cystic fibrosis is a recessive trait; each offspring has a one in four chance of having the trait or the disorder. Maternal age is not a risk factor until age 35, when the incidence of chromosomal defects increases. Maternal exposure to rubella during the first trimester may cause congenital defects. Although a history or preterm labor may place the patient at risk for preterm labor, it does not correlate with genetic defects. 5. Answer C. Ovulation (the period when pregnancy can occur) is accompanied by a basal body temperature increase of 0.7 degrees F to 0.8 degrees F and clear, thin cervical mucus. A return to the preovulatory body temperature indicates a safe period for sexual intercourse. A slight rise in basal temperature early in the cycle is not significant. Breast tenderness and mittelschmerz are not reliable indicators of ovulation. 6. Answer A. An NST assesses the FHR during fetal movement. In a healthy fetus, the FHR accelerates with each movement. By pushing the control button when a fetal movement starts, the client marks the strip to allow easy correlation of fetal movement with the FHR. The FHR is assessed during uterine contractions in the oxytocin contraction test, not the NST. Pushing the control button after every three fetal movements or at the end of fetal movement wouldnt allow accurate comparison of fetal movement and FHR changes. 7. Answer B. Blurred or double vision may indicate hypertension or preeclampsia and should be reported immediately. Urinary frequency is a common problem during pregnancy caused by increased weight pressure on the bladder from the uterus. Clients generally experience fatigue and nausea during pregnancy. 8. Answer B. Recent breast reduction surgeries are done in a way to protect the milk sacs and ducts, so breast-feeding after surgery is possible. Still, its good to check with the surgeon to determine what breast reduction procedure was done. There is the possibility that reduction surgery may have decreased the mothers ability to meet all of her babys nutritional needs, and some supplemental feeding may be required. Preparing the mother for this possibility is extremely important because the clients psychological adaptation to mothering may be dependent on how successfully she breast-feeds. 9. Answer B. Using two or more peripads would do little to reduce the pain or promote perineal healing. Cold applications, sitz baths, and Kegel exercises are important measures when the client has a fourthdegree laceration. 10. Answer B. In a client with gestational trophoblastic disease, an ultrasound performed after the 3rd month shows grapelike clusters of transparent vesicles rather than a fetus. The vesicles contain a clear fluid and may involve all or part of the decidual lining of the uterus. Usually no embryo (and therefore no fetus) is present because it has been absorbed. Because there is no fetus, there can be no extrauterine pregnancy. An extrauterine pregnancy is seen with an ectopic pregnancy.
11. Answer C. Fetal station the relationship of the fetal presenting part to the maternal ischial spines is described in the number of centimeters above or below the spines. A presenting part above the ischial spines is designated as 1, 2, or 3. A presenting part below the ischial spines, as +1, +2, or +3. 12. Answer D. Assessing the attachment process for breast-feeding should include all of the answers except the smacking of lips. A baby whos smacking his lips isnt well attached and can injure the mothers nipples. 13. Answer D. Ultrasound is used between 18 and 40 weeks gestation to identify normal fetal growth and detect fetal anomalies and other problems. Amniocentesis is done during the third trimester to determine fetal lung maturity. Chorionic villi sampling is performed at 8 to 12 weeks gestation to detect genetic disease. Fetoscopy is done at approximately 18 weeks gestation to observe the fetus directly and obtain a skin or blood sample. 14. Answer C. The BPP evaluates fetal health by assessing five variables: fetal breathing movements, gross body movements, fetal tone, reactive fetal heart rate, and qualitative amniotic fluid volume. A normal response for each variable receives 2 points; an abnormal response receives 0 points. A score between 8 and 10 is considered normal, indicating that the fetus has a low risk of oxygen deprivation and isnt in distress. A fetus with a score of 6 or lower is at risk for asphyxia and premature birth; this score warrants detailed investigation. The BPP may or may not be repeated if the score isnt within normal limits. 15. Answer C. During the third trimester, the pregnant client typically perceives the fetus as a separate being. To verify that this has occurred, the nurse should ask whether she has made appropriate changes at home such as obtaining infant supplies and equipment. The type of anesthesia planned doesnt reflect the clients preparation for parenting. The client should have begun prenatal classes earlier in the pregnancy. The nurse should have obtained dietary information during the first trimester to give the client time to make any necessary changes. 16. Answer B. This question requires an understanding of station as part of the intrapartal assessment process. Based on the clients assessment findings, this client is ready for delivery, which is the nurses top priority. Placing the client in bed, checking for ruptured membranes, and providing comfort measures could be done, but the priority here is immediate delivery. 17. Answer A. Variable decelerations in fetal heart rate are an ominous sign, indicating compression of the umbilical cord. Changing the clients position from supine to side-lying may immediately correct the problem. An emergency cesarean section is necessary only if other measures, such as changing position and amnioinfusion with sterile saline, prove unsuccessful. Administering oxygen may be helpful, but the priority is to change the womans position and relieve cord compression. 18. Answer A. Hemorrhage jeopardizes the clients oxygen supply the first priority among human physiologic needs. Therefore, the nursing diagnosis of Risk for deficient fluid volume related to hemorrhage takes priority over diagnoses of Risk for infection, Pain, and Urinary retention. 19. Answer A. Lactation is an example of a progressive physiological change that occurs during the postpartum period.
20. Answer B. The major maternal adverse reactions from cocaine use in pregnancy include spontaneous abortion first, not third, trimester abortion and abruption placentae. 21. Answer D. For most clients with type 1 diabetes mellitus, nonstress testing is done weekly until 32 weeks gestation and twice a week to assess fetal well-being. 22. Answer A. The chemical makeup of magnesium is similar to that of calcium and, therefore, magnesium will act like calcium in the body. As a result, magnesium will block seizure activity in a hyper stimulated neurologic system by interfering with signal transmission at the neuromascular junction. 23. Answer B. The blastocyst takes approximately 1 week to travel to the uterus for implantation. 24. Answer A. An episiotomy serves several purposes. It shortens the second stage of labor, substitutes a clean surgical incision for a tear, and decreases undue stretching of perineal muscles. An episiotomy helps prevent tearing of the rectum but it does not necessarily relieves pressure on the rectum. Tearing may still occur. 25. Answer D. The fetus of a cocaine-addicted mother is at risk for hypoxia, meconium aspiration, and intrauterine growth retardation (IUGR). Therefore, the nurse must notify the physician of the clients cocaine use because this knowledge will influence the care of the client and neonate. The information is used only in relation to the clients care. 26. Answer B. After administration of rubella vaccine, the client should be instructed to avoid pregnancy for at least 3 months to prevent the possibility of the vaccines toxic effects to the fetus. 27. Answer D. The priority for the pregnant client having a seizure is to maintain a patent airway to ensure adequate oxygenation to the mother and the fetus. Additionally, oxygen may be administered by face mask to prevent fetal hypoxia. 28. Answer A. In some birth settings, intravenous therapy is not used with low-risk clients. Thus, clients in early labor are encouraged to eat healthy snacks and drink fluid to avoid dehydration. Yogurt, which is an excellent source of calcium and riboflavin, is soft and easily digested. During pregnancy, gastric emptying time is delayed. In most hospital settings, clients are allowed only ice chips or clear liquids. 29. Answer A. When the client says the baby is coming, the nurse should first inspect the perineum and observe for crowning to validate the clients statement. If the client is not delivering precipitously, the nurse can calm her and use appropriate breathing techniques. 30. Answer A. Using both hands to assess the fundus is useful for the prevention of uterine inversion.
1. A postpartum patient was in labor for 30 hours and had ruptured membranes for 24 hours. For which of the following would the nurse be alert? a. Endometritis b. Endometriosis c. Salpingitis d. Pelvic thrombophlebitis
2. A client at 36 weeks gestation is schedule for a routine ultrasound prior to an amniocentesis. After teaching the client about the purpose for the ultrasound, which of the following client statements would indicate to the nurse in charge that the client needs further instruction? a. The ultrasound will help to locate the placenta b. The ultrasound identifies blood flow through the umbilical cord c. The test will determine where to insert the needle d. The ultrasound locates a pool of amniotic fluid 3. While the postpartum client is receiving herapin for thrombophlebitis, which of the following drugs would the nurse Mica expect to administer if the client develops complications related to heparin therapy? a. Calcium gluconate b. Protamine sulfate c. Methylegonovine (Methergine) d. Nitrofurantoin (macrodantin) 4. When caring for a 3-day-old neonate who is receiving phototherapy to treat jaundice, the nurse in charge would expect to do which of the following? a. Turn the neonate every 6 hours b. Encourage the mother to discontinue breast-feeding c. Notify the physician if the skin becomes bronze in color d. Check the vital signs every 2 to 4 hours 5. A primigravida in active labor is about 9 days post-term. The client desires a bilateral pudendal block anesthesia before delivery. After the nurse explains this type of anesthesia to the client, which of the following locations identified by the client as the area of relief would indicate to the nurse that the teaching was effective? a. Back b. Abdomen c. Fundus d. Perineum 6. The nurse is caring for a primigravida at about 2 months and 1 week gestation. After explaining self-care measures for common discomforts of pregnancy, the nurse determines that the client understands the instructions when she says: a. Nausea and vomiting can be decreased if I eat a few crackers before arising b. If I start to leak colostrum, I should cleanse my nipples with soap and water c. If I have a vaginal discharge, I should wear nylon underwear d. Leg cramps can be alleviated if I put an ice pack on the area 7. Thirty hours after delivery, the nurse in charge plans discharge teaching for the client about infant care. By this time, the nurse expects that the phase of postpartal psychological adaptation that the client would be in would be termed which of the following? a. Taking in b. Letting go c. Taking hold d. Resolution 8. A pregnant client is diagnosed with partial placenta previa. In explaining the diagnosis, the nurse tells the client that the usual treatment for partial placenta previa is which of the following? a. Activity limited to bed rest
b. Platelet infusion c. Immediate cesarean delivery d. Labor induction with oxytocin 9. Nurse Julia plans to instruct the postpartum client about methods to prevent breast engorgement. Which of the following measures would the nurse include in the teaching plan? a. Feeding the neonate a maximum of 5 minutes per side on the first day b. Wearing a supportive brassiere with nipple shields c. Breast-feeding the neonate at frequent intervals d. Decreasing fluid intake for the first 24 to 48 hours 10. When the nurse on duty accidentally bumps the bassinet, the neonate throws out its arms, hands opened, and begins to cry. The nurse interprets this reaction as indicative of which of the following reflexes? a. Startle reflex b. Babinski reflex c. Grasping reflex d. Tonic neck reflex 11. A primigravida client at 25 weeks gestation visits the clinic and tells the nurse that her lower back aches when she arrives home from work. The nurse should suggest that the client perform: a. Tailor sitting b. Leg lifting c. Shoulder circling d. Squatting exercises 12. Which of the following would the nurse in charge do first after observing a 2-cm circle of bright red bleeding on the diaper of a neonate who just had a circumcision? a. Notify the neonates pediatrician immediately b. Check the diaper and circumcision again in 30 minutes c. Secure the diaper tightly to apply pressure on the site d. Apply gently pressure to the site with a sterile gauze pad 13. Which of the following would the nurse Sandra most likely expect to find when assessing a pregnant client with abruption placenta? a. Excessive vaginal bleeding b. Rigid, boardlike abdomen c. Titanic uterine contractions d. Premature rupture of membranes 14. While the client is in active labor with twins and the cervix is 5 cm dilates, the nurse observes contractions occurring at a rate of every 7 to 8 minutes in a 30-minute period. Which of the following would be the nurses most appropriate action? a. Note the fetal heart rate patterns b. Notify the physician immediately c. Administer oxygen at 6 liters by mask d. Have the client pant-blow during the contractions 15. A client tells the nurse, I think my baby likes to hear me talk to him. When discussing neonates and stimulation with sound, which of the following would the nurse include as a means to elicit the best response? a. High-pitched speech with tonal variations
b. Low-pitched speech with a sameness of tone c. Cooing sounds rather than words d. Repeated stimulation with loud sounds 16. A 31-year-old multipara is admitted to the birthing room after initial examination reveals her cervix to be at 8 cm, completely effaced (100 %), and at 0 station. What phase of labor is she in? a. Active phase b. Latent phase c. Expulsive phase d. Transitional phase 17. A pregnant patient asks the nurse Kate if she can take castor oil for her constipation. How should the nurse respond? a. Yes, it produces no adverse effect. b. No, it can initiate premature uterine contractions. c. No, it can promote sodium retention. d. No, it can lead to increased absorption of fat-soluble vitamins. 18. A patient in her 14th week of pregnancy has presented with abdominal cramping and vaginal bleeding for the past 8 hours. She has passed several cloth. What is the primary nursing diagnosis for this patient? a. Knowledge deficit b. Fluid volume deficit c. Anticipatory grieving d. Pain 19. Immediately after a delivery, the nurse-midwife assesses the neonates head for signs of molding. Which factors determine the type of molding? a. Fetal body flexion or extension b. Maternal age, body frame, and weight c. Maternal and paternal ethnic backgrounds d. Maternal parity and gravidity 20. For a patient in active labor, the nurse-midwife plans to use an internal electronic fetal monitoring (EFM) device. What must occur before the internal EFM can be applied? a. The membranes must rupture b. The fetus must be at 0 station c. The cervix must be dilated fully d. The patient must receive anesthesia 21. A primigravida patient is admitted to the labor delivery area. Assessment reveals that she is in early part of the first stage of labor. Her pain is likely to be most intense: a. Around the pelvic girdle b. Around the pelvic girdle and in the upper arms c. Around the pelvic girdle and at the perineum d. At the perineum 22. A female adult patient is taking a progestin-only oral contraceptive, or minipill. Progestin use may increase the patients risk for: a. Endometriosis b. Female hypogonadism
c. Premenstrual syndrome d. Tubal or ectopic pregnancy 23. A patient with pregnancy-induced hypertension probably exhibits which of the following symptoms? a. Proteinuria, headaches, vaginal bleeding b. Headaches, double vision, vaginal bleeding c. Proteinuria, headaches, double vision d. Proteinuria, double vision, uterine contractions 24. Because cervical effacement and dilation are not progressing in a patient in labor, Dr. Smith orders I.V. administration of oxytocin (Pitocin). Why must the nurse monitor the patients fluid intake and output closely during oxytocin administration? a. Oxytoxin causes water intoxication b. Oxytocin causes excessive thirst c. Oxytoxin is toxic to the kidneys d. Oxytoxin has a diuretic effect 25. Five hours after birth, a neonate is transferred to the nursery, where the nurse intervenes to prevent hypothermia. What is a common source of radiant heat loss? a. Low room humidity b. Cold weight scale c. Cools incubator walls d. Cool room temperature 26. After administering bethanechol to a patient with urine retention, the nurse in charge monitors the patient for adverse effects. Which is most likely to occur? a. Decreased peristalsis b. Increase heart rate c. Dry mucous membranes d. Nausea and Vomiting 27. The nurse in charge is caring for a patient who is in the first stage of labor. What is the shortest but most difficult part of this stage? a. Active phase b. Complete phase c. Latent phase d. Transitional phase 28. After 3 days of breast-feeding, a postpartal patient reports nipple soreness. To relieve her discomfort, the nurse should suggest that she: a. Apply warm compresses to her nipples just before feedings b. Lubricate her nipples with expressed milk before feeding c. Dry her nipples with a soft towel after feedings d. Apply soap directly to her nipples, and then rinse 29. The nurse is developing a teaching plan for a patient who is 8 weeks pregnant. The nurse should tell the patient that she can expect to feel the fetus move at which time? a. Between 10 and 12 weeks gestation b. Between 16 and 20 weeks gestation c. Between 21 and 23 weeks gestation
d. Between 24 and 26 weeks gestation 30. Normal lochial findings in the first 24 hours post-delivery include: a. Bright red blood b. Large clots or tissue fragments c. A foul odor d. The complete absence of lochia 1. Answer A. Endometritis is an infection of the uterine lining and can occur after prolonged rupture of membranes. Endometriosis does not occur after a strong labor and prolonged rupture of membranes. Salpingitis is a tubal infection and could occur if endometritis is not treated. Pelvic thrombophlebitis involves a clot formation but it is not a complication of prolonged rupture of membranes. 2. Answer B. Before amniocentesis, a routine ultrasound is valuable in locating the placenta, locating a pool of amniotic fluid, and showing the physician where to insert the needle. Color Doppler imaging ultrasonography identifies blood flow through the umbilical cord. A routine ultrasound does not accomplish this. 3. Answer B. Protamine sulfate is a heparin antagonist given intravenously to counteract bleeding complications cause by heparin overdose. 4. Answer D. While caring for an infant receiving phototherapy for treatment of jaundice, vital signs are checked every 2 to 4 hours because hyperthermia can occur due to the phototherapy lights. 5. Answer D. A bilateral pudental block is used for vaginal deliveries to relieve pain primarily in the perineum and vagina. Pudental block anesthesia is adequate for episiotomy and its repair. 6. Answer A. Eating dry crackers before arising can assist in decreasing the common discomfort of nausea and vomiting. Avoiding strong food odors and eating a high-protein snack before bedtime can also help. 7. Answer C. Beginning after completion of the taking-in phase, the taking-hold phase lasts about 10 days. During this phase, the client is concerned with her need to resume control of all facets of her life in a competent manner. At this time, she is ready to learn self-care and infant care skills. 8. Answer A. Treatment of partial placenta previa includes bed rest, hydration, and careful monitoring of the clients bleeding. 9. Answer C. Prevention of breast engorgement is key. The best technique is to empty the breast regularly with feeding. Engorgement is less likely when the mother and neonate are together, as in single room maternity care continuous rooming in, because nursing can be done conveniently to meet the neonates and mothers needs. 10. Answer A. The Moro, or startle, reflex occurs when the neonate responds to stimuli by extending the arms, hands open, and then moving the arms in an embracing motion. The Moro reflex, present at birth, disappears at about age 3 months. 11. Answer A. Tailor sitting is an excellent exercise that helps to strengthen the clients back muscles and also prepares the client for the process of labor. The clientshould be encouraged to rest periodically during the day and avoid standing or sitting in one position for a long time.
12. Answer D. If bleeding occurs after circumcision, the nurse should first apply gently pressure on the area with sterile gauze. Bleeding is not common but requires attention when it occurs. 13. Answer B. The most common assessment finding in a client with abruption placenta is a rigid or boardlike abdomen. Pain, usually reported as a sharp stabbing sensation high in the uterine fundus with the initial separation, also is common. 14. Answer B. The nurse should contact the physician immediately because the client is most likely experiencing hypotonic uterine contractions. These contractions tend to be painful but ineffective. The usual treatment is oxytocin augmentation, unless cephalopelvic disproportion exists. 15. Answer A. Providing stimulation and speaking to neonates is important. Some authorities believe that speech is the most important type of sensory stimulation for a neonate. Neonates respond best to speech with tonal variations and a high-pitched voice. A neonate can hear all sound louder than about 55 decibels. 16. Answer D. The transitional phase of labor extends from 8 to 10 cm; it is the shortest but most difficult and intense for the patient. The latent phase extends from 0 to 3 cm; it is mild in nature. The active phase extends form 4 to 7 cm; it is moderate for the patient. The expulsive phase begins immediately after the birth and ends with separation and expulsion of the placenta. 17. Answer B. Castor oil can initiate premature uterine contractions in pregnant women. It also can produce other adverse effects, but it does not promote sodium retention. Castor oils is not known to increase absorption of fat-soluble vitamins, although laxatives in general may decrease absorption if intestinal motility is increased. 18. Answer B. If bleeding and cloth are excessive, this patient may become hypovolemic. Pad count should be instituted. Although the other diagnoses are applicable to this patient, they are not the primary diagnosis. 19. Answer A. Fetal attitudethe overall degree of body flexion or extensiondetermines the type of molding in the head a neonate. Molding is not influence by maternal age, body frame, weight, parity, or gravidity or by maternal and paternal ethnic backgrounds. 20. Answer A. Internal EFM can be applied only after the patients membranes have ruptures, when the fetus is at least at the -1 station, and when the cervix is dilated at least 2 cm. although the patient may receive anesthesia, it is not required before application of an internal EFM device. 21. Answer A.During most of the first stage of labor, pain centers around the pelvic girdle. During the late part of this stage and the early part of the second stage, pain spreads to the upper legs and perineum. During the late part of the second stage and during childbirth, intense pain occurs at the perineum. Upper arm pain is not common during ant stage of labor. 22. Answer D. Women taking the minipill have a higher incidence of tubal and ectopic pregnancies, possibly because progestin slows ovum transport through the fallopian tubes. Endometriosis, female hypogonadism, and premenstrual syndrome are not associated with progestin-only oral contraceptives.
23. Answer C. A patient with pregnancy-induced hypertension complains of headache, double vision, and sudden weight gain. A urine specimen reveals proteinuria. Vaginal bleeding and uterine contractions are not associated with pregnancy-induces hypertension. 24. Answer A. The nurse should monitor fluid intake and output because prolonged oxytoxin infusion may cause severe water intoxication, leading to seizures, coma, and death. Excessive thirst results form the work of labor and limited oral fluid intakenot oxytoxin. Oxytoxin has no nephrotoxic or diuretic effects. In fact, it produces an antidiuretic effect. 25. Answer C. Common source of radiant heat loss includes cool incubator walls and windows. Low room humidity promotes evaporative heat loss. When the skin directly contacts a cooler object, such as a cold weight scale, conductive heat loss may occur. A cool room temperature may lead to convective heat loss. 26. Answer D. Bethanechol will increase GI motility, which may cause nausea, belching, vomiting, intestinal cramps, and diarrhea. Peristalsis is increased rather than decreased. With high doses of bethanechol, cardiovascular responses may include vasodilation, decreased cardiac rate, and decreased force of cardiac contraction, which may cause hypotension. Salivation or sweating may gently increase. 27. Answer D. The transitional phase, which lasts 1 to 3 hours, is the shortest but most difficult part of the first stage of labor. This phase is characterized by intense uterine contractions that occur every 1 to 2 minutes and last 45 to 90 seconds. The active phase lasts 4 to 6 hours; it is characterized by contractions that starts out moderately intense, grow stronger, and last about 60 seconds. The complete phase occurs during the second, not first, stage of labor. The latent phase lasts 5 to 8 hours and is marked by mild, short, irregular contractions. 28. Answer B. Measures that help relieve nipple soreness in a breast-feeding patient include lubrication the nipples with a few drops of expressed milk before feedings, applying ice compresses just before feeding, letting the nipples air dry after feedings, and avoiding the use of soap on the nipples. 29. Answer B. A pregnant woman usually can detect fetal movement (quickening) between 16 and 20 weeks gestation. Before 16 weeks, the fetus is not developed enough for the woman to detect movement. After 20 weeks, the fetus continues to gain weight steadily, the lungs start to produce surfactant, the brain is grossly formed, and myelination of the spinal cord begins. 30. Answer A. Lochia should never contain large clots, tissue fragments, or membranes. A foul odor may signal infection, as may absence of lochia.
You might also like
- Soap O&gDocument170 pagesSoap O&gAhmad Syahmi YZ86% (7)
- Obstetric History Taking OSCE GuideDocument17 pagesObstetric History Taking OSCE GuideSYDNIKA AIRA CARBONILLANo ratings yet
- Maternal NursingDocument16 pagesMaternal NursingJayCesarNo ratings yet
- Family Health AssessmentDocument47 pagesFamily Health Assessmentangeleigh viernesNo ratings yet
- PEDIA Nursing NCLEX Bullets Part 1Document166 pagesPEDIA Nursing NCLEX Bullets Part 1Russel Myron Adriano AdvinculaNo ratings yet
- PREPUMASTERKEY (Repaired)Document2,031 pagesPREPUMASTERKEY (Repaired)surviving nursing schoolNo ratings yet
- ATI Maternal Newborn Proctored Exam 2020Document4 pagesATI Maternal Newborn Proctored Exam 2020svetlanaNo ratings yet
- Navigating Long-Term Care - A Practical Approach for NursesFrom EverandNavigating Long-Term Care - A Practical Approach for NursesNo ratings yet
- Pregnancy Induced Hypertension (PIH)Document3 pagesPregnancy Induced Hypertension (PIH)Susan HepziNo ratings yet
- 8 Essential Concepts 4 NCLEX RN-4Document6 pages8 Essential Concepts 4 NCLEX RN-4Jot grewalNo ratings yet
- All RecallsDocument301 pagesAll RecallsFA Khan100% (2)
- Ati QuestionsDocument2 pagesAti Questionsnjames44No ratings yet
- Mark Fredderick R. Abejo RN, MAN: Maternal and Child Nursing BulletsDocument9 pagesMark Fredderick R. Abejo RN, MAN: Maternal and Child Nursing BulletsCrystal Ann Monsale TadiamonNo ratings yet
- RPS Hospital Ranchi Total Marks - 30 Question Paper Set - 1Document7 pagesRPS Hospital Ranchi Total Marks - 30 Question Paper Set - 1Tanisha Singh100% (1)
- Qualitative Research in NursingDocument13 pagesQualitative Research in NursingArnold-Samantha Arrieta0% (1)
- Newborn Care 1Document6 pagesNewborn Care 1Francine LaxaNo ratings yet
- Hesi Management of A Medical UnitDocument2 pagesHesi Management of A Medical UnitAna Bienne100% (1)
- OB Evolve Test 4Document30 pagesOB Evolve Test 4Yu Yu Chen100% (1)
- Hyperemesis Gravidarum: Bleeding Complications of PregnancyDocument6 pagesHyperemesis Gravidarum: Bleeding Complications of PregnancykirbsNo ratings yet
- CA RationaleDocument39 pagesCA RationaleSeirah Distor MartinezNo ratings yet
- Nursing BulletsDocument83 pagesNursing BulletsgilissaNo ratings yet
- PNLE NCLEX Practice Exam For Maternal and Child Health Nursing 2Document5 pagesPNLE NCLEX Practice Exam For Maternal and Child Health Nursing 2bobtaguba100% (1)
- Nursing Care of A Family Experiencing A Sudden Pregnancy ComplicationDocument5 pagesNursing Care of A Family Experiencing A Sudden Pregnancy ComplicationCrisheila Sarah PiedadNo ratings yet
- The Ultimate Review For MedicalDocument15 pagesThe Ultimate Review For MedicalJap Avila BernasNo ratings yet
- Icu 1Document3 pagesIcu 1Jillian EsquivelNo ratings yet
- Arrhythmia (Irregular Heartbeats) Symptoms, Types, and TreatmentDocument5 pagesArrhythmia (Irregular Heartbeats) Symptoms, Types, and TreatmentCyberMeow100% (1)
- Researchandplanningwritingassignment SonyarajabiDocument3 pagesResearchandplanningwritingassignment Sonyarajabiapi-361965198No ratings yet
- Chapter 40: Drugs Used in Obstetrics Test Bank: Multiple ChoiceDocument10 pagesChapter 40: Drugs Used in Obstetrics Test Bank: Multiple ChoiceNurse UtopiaNo ratings yet
- NCLEXDocument11 pagesNCLEXPrince Charles AbalosNo ratings yet
- Reviewer C AnswersDocument39 pagesReviewer C AnswersDavis WhiteNo ratings yet
- Burn 2Document4 pagesBurn 2lyn_aiNo ratings yet
- Practice Questions - Weeks 345 - 3rdedDocument5 pagesPractice Questions - Weeks 345 - 3rdedJon LevinsNo ratings yet
- Nursing Care of The Child With An Alteration in Gas Exchange/Respiratory DisorderDocument30 pagesNursing Care of The Child With An Alteration in Gas Exchange/Respiratory DisorderGlory MimiNo ratings yet
- EditDocument80 pagesEditkaye patNo ratings yet
- Antepartum 2Document3 pagesAntepartum 2Emily Davis100% (2)
- ExamDocument7 pagesExamRhabdoNo ratings yet
- Flash Cards Vocab For Exam 1. Jarvis CH 1-3, 8, 9, 12, 13http - P.quizlet - Com - Settitle Health Assessment Vocab For Exam 1Document22 pagesFlash Cards Vocab For Exam 1. Jarvis CH 1-3, 8, 9, 12, 13http - P.quizlet - Com - Settitle Health Assessment Vocab For Exam 1tipredd100% (1)
- Hesi PracticeDocument1 pageHesi Practicejustjesko0lNo ratings yet
- Blunt TraumaDocument4 pagesBlunt TraumaRebecca HughesNo ratings yet
- Asthma That Disappears Between Ages 6-8 - Bronchioles Grew & Resolved The AsthmaDocument27 pagesAsthma That Disappears Between Ages 6-8 - Bronchioles Grew & Resolved The Asthmasimonedarling100% (1)
- ATI Comprehensive: Study Online atDocument6 pagesATI Comprehensive: Study Online atVanessaMUeller100% (1)
- NCLEX Review Cardiovascular QuizDocument17 pagesNCLEX Review Cardiovascular Quizdany tesemaNo ratings yet
- Nclex PrepDocument2 pagesNclex PrepJeremy HodgesNo ratings yet
- TXTDocument356 pagesTXTJec AmracNo ratings yet
- Quiz 5 Test Bank PDFDocument37 pagesQuiz 5 Test Bank PDFOnyeka O AniyedeNo ratings yet
- NR 224 Week 1 Instuctor Unit 1 Questions and AnswersDocument7 pagesNR 224 Week 1 Instuctor Unit 1 Questions and AnswersJesse JohnsonNo ratings yet
- Chapter 001Document11 pagesChapter 001Tracy BartellNo ratings yet
- Fundamentals Quizzing TIPSDocument41 pagesFundamentals Quizzing TIPSmelissamichellleNo ratings yet
- NR442 - Community Health Nursing - Exam 1 Study GuideDocument5 pagesNR442 - Community Health Nursing - Exam 1 Study GuideJohn Mixer100% (1)
- Check My Twitter Account @nursetopia or IG @nursetopia1 For More Nursing Test Banks, Sample Exam, Reviewers, and NotesDocument5 pagesCheck My Twitter Account @nursetopia or IG @nursetopia1 For More Nursing Test Banks, Sample Exam, Reviewers, and NotesNurse UtopiaNo ratings yet
- GYNECOLOGICALNURSINGDocument4 pagesGYNECOLOGICALNURSINGSheana TmplNo ratings yet
- Alcohol Withdrawal Care PlanDocument1 pageAlcohol Withdrawal Care PlanVanessaMUellerNo ratings yet
- Chapter 30Document26 pagesChapter 30Nurse UtopiaNo ratings yet
- Ob 3Document14 pagesOb 3Princess LotusNo ratings yet
- Safety: Nclex Tips TranscriptDocument5 pagesSafety: Nclex Tips TranscriptRichard MendejaNo ratings yet
- NCLEX Pregnancy NotesDocument3 pagesNCLEX Pregnancy NotesrustiejadeNo ratings yet
- Cardiovascular System: Complications of Positive Pressure VentilationDocument5 pagesCardiovascular System: Complications of Positive Pressure VentilationjefrocNo ratings yet
- Menopause Concept MapDocument1 pageMenopause Concept MapBritanny NelsonNo ratings yet
- LP2 MAJOR EXAM 4 Files Merged 2 Files MergedDocument285 pagesLP2 MAJOR EXAM 4 Files Merged 2 Files MergedBianca ArceNo ratings yet
- 56: Neurological System: Practice QuestionsDocument36 pages56: Neurological System: Practice Questionsjutah2013No ratings yet
- Lowdermilk: Maternity & Women's Health Care, 10th EditionDocument12 pagesLowdermilk: Maternity & Women's Health Care, 10th Editionvanassa johnson100% (1)
- Explanation: MRCS Part A - Sep 2019 ExamDocument46 pagesExplanation: MRCS Part A - Sep 2019 ExamHasan ManghiNo ratings yet
- Legal Issues Emergency Medicine (Final)Document97 pagesLegal Issues Emergency Medicine (Final)GerardChanNo ratings yet
- Which Signs and Symptoms Would The Nurse Expect To Assess in A Newborn WithDocument1 pageWhich Signs and Symptoms Would The Nurse Expect To Assess in A Newborn WithjamesNo ratings yet
- 2017 Fluid and Electrolytes LECTURE NOTESDocument34 pages2017 Fluid and Electrolytes LECTURE NOTESHarley Justiniani Dela CruzNo ratings yet
- Answer: CDocument34 pagesAnswer: CLola OladapoNo ratings yet
- Funds Study Guide 29Document29 pagesFunds Study Guide 29Vin Lorenzo CampbellNo ratings yet
- OB Exam 1 ComboDocument82 pagesOB Exam 1 ComboHope RobersonNo ratings yet
- NURSING CARE OF ADULTS II: Passbooks Study GuideFrom EverandNURSING CARE OF ADULTS II: Passbooks Study GuideNo ratings yet
- Solar Heated GrillDocument2 pagesSolar Heated GrillMEi .. ÜNo ratings yet
- P PPPPP PPPPPP PP PP P PPP PPP P PPP PPPPP PPPPP PPPPPP PPPPPPPP P PPPPPDocument5 pagesP PPPPP PPPPPP PP PP P PPP PPP P PPP PPPPP PPPPP PPPPPP PPPPPPPP P PPPPPMEi .. ÜNo ratings yet
- Care For Patient With Communicable DiseaseDocument2 pagesCare For Patient With Communicable DiseaseMEi .. ÜNo ratings yet
- Communicable Diseases: Prepared By: Abigail E. Tan BSN IV C (Group 14)Document32 pagesCommunicable Diseases: Prepared By: Abigail E. Tan BSN IV C (Group 14)MEi .. ÜNo ratings yet
- High Risk PregnancyDocument5 pagesHigh Risk Pregnancygracie_greys5755No ratings yet
- Induction of Labor With Oxytocin - UpToDateDocument37 pagesInduction of Labor With Oxytocin - UpToDateMerjem DautiNo ratings yet
- Diagnosis and Management of Atypical Preeclampsia-Eclampsia: Obstetric Anesthesia Digest March 2010Document8 pagesDiagnosis and Management of Atypical Preeclampsia-Eclampsia: Obstetric Anesthesia Digest March 2010Fedrik Monte Kristo LimbongNo ratings yet
- Welcome To NCM 104: Davao Doctors College, IncDocument212 pagesWelcome To NCM 104: Davao Doctors College, IncwindloverNo ratings yet
- Wen2018Document10 pagesWen2018AkunNo ratings yet
- The Guardian Weekend 10.11.2012Document104 pagesThe Guardian Weekend 10.11.2012pardost0% (4)
- PreeclampsiaDocument4 pagesPreeclampsiairismaronNo ratings yet
- Acute Kidney Injury (Acute Renal Failure) in Pregnancy - UpToDateDocument15 pagesAcute Kidney Injury (Acute Renal Failure) in Pregnancy - UpToDateZurya UdayanaNo ratings yet
- WJD 2 196 PDFDocument8 pagesWJD 2 196 PDFMayra PereiraNo ratings yet
- Validation of The Placenta Accreta Index (PAI) - Improving The Antenatal Diagnosis of The Morbidly Adherent PlacentaDocument2 pagesValidation of The Placenta Accreta Index (PAI) - Improving The Antenatal Diagnosis of The Morbidly Adherent PlacentaOmpNo ratings yet
- Iugr FGRDocument10 pagesIugr FGRGilang Hadi FNo ratings yet
- Uterine motilityMD20.8.55 Sheet PDFDocument45 pagesUterine motilityMD20.8.55 Sheet PDFNirut SrimakamNo ratings yet
- High Risk WomenDocument17 pagesHigh Risk WomenamitNo ratings yet
- GyneDocument4 pagesGynePrincessNo ratings yet
- Hypertensive Disorder in PregnancyDocument5 pagesHypertensive Disorder in Pregnancymendato marcabanNo ratings yet
- Maternal and Child Health Is The Program of The Department of Health Created To Lessen The Death of Infants and Mother in The PhilippinesDocument18 pagesMaternal and Child Health Is The Program of The Department of Health Created To Lessen The Death of Infants and Mother in The PhilippinesNicole Marin-ChingNo ratings yet
- 052183953X Hematological123456 PDFDocument619 pages052183953X Hematological123456 PDFaliaaNo ratings yet
- Cover Kacyiru 092633Document24 pagesCover Kacyiru 092633Fulgence Umuhoza CleverstarNo ratings yet
- Maternal and Child Health Care Services: by Khaled KasimDocument70 pagesMaternal and Child Health Care Services: by Khaled KasimFahad AloufiNo ratings yet
- PreeclampsiaDocument27 pagesPreeclampsiairon100% (1)
- Normal Ecg, Infarction & Arrhythmias: Iqbal Lahmadi Departement of Internal Medicine Sintang - 2013Document98 pagesNormal Ecg, Infarction & Arrhythmias: Iqbal Lahmadi Departement of Internal Medicine Sintang - 2013Maylisa ManurungNo ratings yet