Professional Documents
Culture Documents
WHONET Documentation
Uploaded by
tummalapalli venkateswara raoCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
WHONET Documentation
Uploaded by
tummalapalli venkateswara raoCopyright:
Available Formats
Need for WHONET Documentation
*T.V.Rao, C.Aher, Deepa Babin, Deepthy Sooryadas
Department of Microbiology Travancore Medical College, Kollam Kerala, India
Antibiotics are considered as strength of the Modern Medicine, and helped the humans to progress to the present stage, along with several other advances in Medicine. At present, the Antibiotics are used for needy patients and misused too when there is no need for an antibiotic prescription. Drug resistance develops naturally, but careless practices in drug supply and use are hastening it unnecessarily, we certainly need a system to document the results of antibiotic sensitivity and resistance patterns arising in our Institution, which can be documented with WHONET.
WHONET is free Windows-based database software
developed for the management and analysis of microbiology laboratory data with a special focus on the analysis of antimicrobial susceptibility test results. These tools enable microbiology laboratory to put its test results into a database and conduct analysis to support local infection control and antibiotic usage at our Hospital
The software has been developed since 1989 by the WHO Collaborating Centre for Surveillance of Antimicrobial Resistance based at the Brigham and Women's Hospital in Boston, and is used by clinical, public health, veterinary, and food laboratories in over 90 countries to support local and national surveillance programs. Laboratories can also upload files created by WHONET, to feed into national or other multi-centre surveillance networks and to strengthen our Drug policy. Such surveillance programs are now in place in many countries and part of Accreditation standards in our country.
How we can Progress with WHONET
We can enhance the local data for local needs: clinical decision support, antimicrobial use policy, infection control and outbreak detection, identifying laboratory test performance, and characterization of local microbial and resistance epidemiology And to promote local, national, regional, and global collaborations through the exchange of data and sharing of experiences. The WHONET experience suggests that pattern of drug resistance data can be collected and analysed in resource-
constrained settings, using core microbiology, if local laboratories are given appropriate support. Strengthening these laboratories is therefore a potentially cost-effective Contribution to both treating drug resistant disease and preventing its further spread. Microbiologists, Clinicians and Infection control workers may use its software to enhance monitoring of drug resistance in their hospitals and communities and to merge their files into national, regional, and global networks for surveillance of drug resistance. WHONET can also analyse stored data. From a single screen, a WHONET user selects the type of analysis to run, the species of bacteria to analyse, the subsets of isolates to include (e.g., all, isolates from urine, blood , and isolates resistant to Cephalosporins, Carbapenems or any other drug individually and from certain locations in outpatients and any wards like ICCUs Medicine, Surgery or any other speciality) Every patient in our Hospital or its community carries a complex bacterial ecosystem and each patient care unit within the centre and ultimately the centre itself may be seen as an aggregated ecosystem. Resistance genes and the strains they make resistant move through these systems, selectively accelerated by specific antimicrobial agents given to specific patients and
retarded by infection control practices. Both strategic and dayto-day management of those practices and of the selection of those agents need optimal, current information about the linkages of the resistance genes and the deployment of the strains. The Microbiology laboratory at our Hospital also needs continuing analysis of its susceptibility test and quality control results. Each laboratory tests hundreds of different combinations of bacterial species and antimicrobial agents. Variations in the usual distributions of measurements for any of the combinations, and particularly of those that impinge upon breakpoints may signal either problems in test performance or new types of resistance.
A present WHONET helps our Hospital
Creates profile of the Bacterial Infections at our Hospital. Helps to know the Antibiograms pattern of the different isolates. Trends in MRSA, and patterns of drug resistance in several Gram negative bacterial strains. We can alert the physicians on uncommon, clinically important bacterial pathogens. Helps our faculty to present data at academic associations and in publishing papers as per editorial guidelines. However it needs greater cooperation of all Clinicians to build the system to our Hospital needs, The protocols can be integrated into the Antibiotic policy
*Email; doctortvrao@gmail.com
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Dysthymia and Cyclothymia: Understanding Mood DisordersDocument9 pagesDysthymia and Cyclothymia: Understanding Mood DisordersNatnael0% (1)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Ayurveda Tongue Analysis Dr. Rama PrasadDocument34 pagesAyurveda Tongue Analysis Dr. Rama PrasadSanjay Soni100% (2)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Nccaom Biomed Exam ContentDocument12 pagesNccaom Biomed Exam Contentapi-251021152No ratings yet
- Artificial Intelligence in Healthcare Legal and Ethical Considerations Dr.T.V.Rao MDDocument34 pagesArtificial Intelligence in Healthcare Legal and Ethical Considerations Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- H&S at Work act 1974 dutiesDocument44 pagesH&S at Work act 1974 dutiesSardar Majid80% (5)
- HOSPITAL ASSOCIATED Infections Overcoming Emerging Challenge by Dr.T.V.Rao MDDocument61 pagesHOSPITAL ASSOCIATED Infections Overcoming Emerging Challenge by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- Screening For MRSA by Dr.T.V.Rao MDDocument30 pagesScreening For MRSA by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- Biopharmaceutics & Drug Product Quality & Clinical Efficacy - FinalDocument56 pagesBiopharmaceutics & Drug Product Quality & Clinical Efficacy - Finalbimu100% (1)
- Infection Control in Burns PatietnsDocument41 pagesInfection Control in Burns Patietnstummalapalli venkateswara raoNo ratings yet
- Surgical Operation Theater StandardsDocument31 pagesSurgical Operation Theater Standardstummalapalli venkateswara raoNo ratings yet
- Influenza Teaching Current Update 2023 by Dr.T.V.Rao MDDocument100 pagesInfluenza Teaching Current Update 2023 by Dr.T.V.Rao MDtummalapalli venkateswara rao100% (1)
- MCN Test BankDocument10 pagesMCN Test BankMho Pimentel Vanguardia100% (1)
- INFECTION CONTROL TRENDS OF CHANGE by Dr.T.V.Rao MDDocument25 pagesINFECTION CONTROL TRENDS OF CHANGE by Dr.T.V.Rao MDtummalapalli venkateswara rao100% (1)
- Current Trends in Sterilisation of Operation TheatresDocument7 pagesCurrent Trends in Sterilisation of Operation Theatrestummalapalli venkateswara raoNo ratings yet
- HOSPITAL ANTIBIOGRAMS Principles Interpretation and DocumentationDocument55 pagesHOSPITAL ANTIBIOGRAMS Principles Interpretation and Documentationtummalapalli venkateswara raoNo ratings yet
- Fall Out of Neet On Medical EdcuationDocument2 pagesFall Out of Neet On Medical Edcuationtummalapalli venkateswara raoNo ratings yet
- MEDICAL ETHICS IN RESEARCH PROPOSALS (Indian Contest)Document62 pagesMEDICAL ETHICS IN RESEARCH PROPOSALS (Indian Contest)tummalapalli venkateswara raoNo ratings yet
- Need For Clinical Microbiologists by Dr.T.V.Rao MDDocument2 pagesNeed For Clinical Microbiologists by Dr.T.V.Rao MDtummalapalli venkateswara rao100% (1)
- Our Vison To Future On Diagnostic Microbiology by Dr.T.V.Rao MDDocument5 pagesOur Vison To Future On Diagnostic Microbiology by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- MDR - TB Emerging Methods in Diagnosis Dr.T.V.Rao MDDocument2 pagesMDR - TB Emerging Methods in Diagnosis Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- JOURNAL CLUB in Medicine Preparation and Presentation Dr.T.V.Rao MDDocument36 pagesJOURNAL CLUB in Medicine Preparation and Presentation Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- Streaking Culture Plates in Bacteriology by Dr.T.V.Rao MDDocument33 pagesStreaking Culture Plates in Bacteriology by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- School Hygiene by Dr.T.V.Rao MDDocument32 pagesSchool Hygiene by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- Who Is Killing Modern Medicine in IndiaDocument3 pagesWho Is Killing Modern Medicine in Indiatummalapalli venkateswara raoNo ratings yet
- Hand Hygiene and Prevention of Infection inDocument22 pagesHand Hygiene and Prevention of Infection intummalapalli venkateswara raoNo ratings yet
- MDR - TB FACTS AND CONCERNS BY Dr.T.V.Rao MDDocument33 pagesMDR - TB FACTS AND CONCERNS BY Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- GRAM STAINING AND CLINICAL UTILITY by Dr.T.V.Rao MDDocument2 pagesGRAM STAINING AND CLINICAL UTILITY by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- Elizabethkingia Meningoseptica An Emerging Infection by Dr.T.V.Rao MDDocument28 pagesElizabethkingia Meningoseptica An Emerging Infection by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- 10 Options To Control Hospital Infections by Dr.T.V.Rao MDDocument17 pages10 Options To Control Hospital Infections by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- School Hygiene Preventing InfectionsDocument19 pagesSchool Hygiene Preventing Infectionstummalapalli venkateswara raoNo ratings yet
- INTERPRETATION OF ANTIBIOGRAMS Trends of Change by Dr.T.V.Rao MDDocument62 pagesINTERPRETATION OF ANTIBIOGRAMS Trends of Change by Dr.T.V.Rao MDtummalapalli venkateswara rao100% (1)
- Health Care Associated Infections Creating Drug Resistance AtlasDocument46 pagesHealth Care Associated Infections Creating Drug Resistance Atlastummalapalli venkateswara raoNo ratings yet
- MALDI-ToF in Clinical MicrobiologyDocument39 pagesMALDI-ToF in Clinical Microbiologytummalapalli venkateswara rao100% (1)
- MDR-TB An Update by Dr.T.V.Rao MDDocument43 pagesMDR-TB An Update by Dr.T.V.Rao MDtummalapalli venkateswara raoNo ratings yet
- World TB Day 2016Document33 pagesWorld TB Day 2016tummalapalli venkateswara raoNo ratings yet
- Overview and Pathophysiology of Gestational Trophoblastic Disease - PresentationDocument222 pagesOverview and Pathophysiology of Gestational Trophoblastic Disease - PresentationTanvir AhmedNo ratings yet
- Bahasa Inggris MakalahDocument6 pagesBahasa Inggris MakalahtrisnaulandariNo ratings yet
- Top Use Cases and Cutting-Edge Solutions With Generative AI in HealthcareDocument41 pagesTop Use Cases and Cutting-Edge Solutions With Generative AI in Healthcarelancet7111No ratings yet
- JC3032 AIDS Data Book 2021 enDocument468 pagesJC3032 AIDS Data Book 2021 ensonykoNo ratings yet
- Concept MapDocument2 pagesConcept Mapantherchio100% (2)
- Intermittent Asthma Case ReportDocument91 pagesIntermittent Asthma Case ReportCindy PrayogoNo ratings yet
- Postpartum Eclampsia Clinical Study (IJSRDocument3 pagesPostpartum Eclampsia Clinical Study (IJSRSulabh ShresthaNo ratings yet
- Draft 2Document84 pagesDraft 2John Gabriel SamsonNo ratings yet
- Menu Eval Plus: Fried Rice and EggDocument2 pagesMenu Eval Plus: Fried Rice and EggJasperl Niña MalabuyocNo ratings yet
- HSA1-Assessment-فورمة عمل تقريرDocument5 pagesHSA1-Assessment-فورمة عمل تقريرAhmed EzzatNo ratings yet
- Lamaran - Produksi (Yusuf)Document3 pagesLamaran - Produksi (Yusuf)Salatiga ParamedicNo ratings yet
- NitriVer® 3 Nitrite ReagentDocument16 pagesNitriVer® 3 Nitrite ReagentMark KuttinNo ratings yet
- Classroom Nutritional Status ReportDocument2 pagesClassroom Nutritional Status ReportEden PingliNo ratings yet
- Informational InterviewDocument3 pagesInformational InterviewMelissa LinkNo ratings yet
- Non-Invasive Respiratory Support in Preterm Infants 2022Document7 pagesNon-Invasive Respiratory Support in Preterm Infants 2022DraalexNo ratings yet
- Collection, Transportation, Treatment & Disposal of Laboratory WasteDocument51 pagesCollection, Transportation, Treatment & Disposal of Laboratory WasteYuresh TwayanaNo ratings yet
- Unifrax SDS FIXWOOL ADHESIVE 1400 V3.00 (GB-en) 150826Document6 pagesUnifrax SDS FIXWOOL ADHESIVE 1400 V3.00 (GB-en) 150826Muhammad Ashadul BurhanuddinNo ratings yet
- Breastfeeding TCP UfcDocument18 pagesBreastfeeding TCP UfcYana PotNo ratings yet
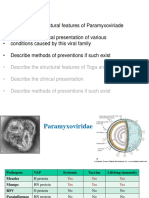
- ParamyxoviridaeDocument27 pagesParamyxoviridaeFarrah BenoitNo ratings yet
- City of Dayton Board of Zoning Appeals Staff ReportDocument36 pagesCity of Dayton Board of Zoning Appeals Staff ReportChelsea ElizabethNo ratings yet
- RP-Technik RoHS Compliance DeclarationDocument1 pageRP-Technik RoHS Compliance DeclarationModern DesignsNo ratings yet
- Zika virus knowledge and attitudesDocument3 pagesZika virus knowledge and attitudesTeguh firmansyahNo ratings yet
- Fish OilDocument44 pagesFish OilRamchandra Keny50% (2)
- Scat3: Sport Concussion Assessment Tool - 3rd EditionDocument4 pagesScat3: Sport Concussion Assessment Tool - 3rd EditionFabio da CostaNo ratings yet