Professional Documents
Culture Documents
Acls Algorithms Rapid Rates
Uploaded by
Robert DwitamaCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Acls Algorithms Rapid Rates
Uploaded by
Robert DwitamaCopyright:
Available Formats
ACLS
ALGORITHMS
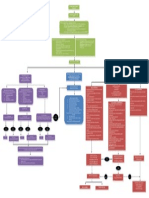
Acute Pulmonary Edema / Hypotension / Shock Algorithm
Clinical signs of hypoperfusion, congestive heart failure, acute pulmonary edema Assess ABCs Assess vitals Secure airway Review history Administer O2 Perform physical exam Start IV 12 lead ECG, chest x-ray Attach monitor, pulse oximetry and B/P Cuff
Figure 8
What is the nature of the problem?
Volume problem Includes PVR problems
Administer Fluids Blood transfusions Cause-specific interventions Consider vasopressors
Pump Problem What is the BP ?
Rate Problem
Too Slow Go to Fig 5
Too Fast Go to Fig 6
Systolic BP < 70 Signs of shock
Systolic BP 70 - 100 mmHg Signs of shock
Systolic BP 70 - 100 mmHg No Signs of shock
Systolic BP > 100 mmHg
Bradycardia Algorithm (Patient is not in Cardiac Arrest)
Assess ABCs Assess vitals Secure airway Review history Administer O2 Perform physical exam Start IV 12 lead ECG, chest x-ray Attach monitor, pulse oximetry and B/P Cuff
Figure 5
Bradycardia, either absolute (<60 BPM) or relative
Serious signs and symptoms?a,b
No
Type II second-degree AV heart block or Third-degree AV heart Block?e
Yes
No
Observe
Yes
Prepare for transvenous pacer Use TCP as a bridge device
Intervention sequence Atropine 0.5 - 1.0 mcg,d (I and IIa) TCP, if available (I) Dopamine 5 - 20 mcg/kg/min (IIb) Epinephrine 1 - 10 mcg/min (IIb) Norepinephrine 0.5 30 mcg/min (IIb)
Tachycardia Algorithm (Patient is not in Cardiac Arrest)
Assess ABCs Assess vitals Secure airway Review history Administer O2 Perform physical exam Start IV 12 lead ECG, chest x-ray Attach monitor, pulse oximetry and B/P Cuff
Figure 6
Yes Prepare for cardioversion Unstable, with serious signs or symptoms?a No
If ventricular rate > 150 BPM May give brief trial of Rx Immediate cardioversion is seldom needed for heart rates < 150 BPM
Atrial Fibrillation Atrial Flutter
Paroxysmal Supraventricular Tachycardia (PSVT)
Wide-complex tachycardia of uncertain type
Ventricular Tachycardia (VT)
Includes Electromechanical dissociation (EMD) Postdefibrillation idioventricular rhythms Pseudo - EMD Bradyasystolic rhythms Idioventricular rhythms Ventricular escape rhythms
Pulseless Electrical Activity (PEA) Algorithm (Electromechanical Dissociation [EMD])
Figure 3
Continue CPR / Intubate at once / Obtain IV Access Assess blood flow using Doppler ultrasound, endtidal CO2, echocardiography, or arterial line
Consider possible causes Hypovolemia (volume infusion) Drug overdoses - tricyclics, digitalis Hypoxia (ventilation) Beta-blockers, calcium channel blockers Cardiac tamponade (pericardiocentesis) Hyperkalemia Tension Pneumothorax Acidosis Hypothermia ( see hypothermia algorithm) Massive acute myocardial infarction Massive pulmonary embolism (surgery, lysine) Massive acute MI (go to Fig 9)
Epinephrine 1 mg IV push,a,c repeat q 3 - 5 min
If absolute bradycardia (< 60 BPM) or relative bradycardia give atropine 1 mg IV Repeat q 3 -5 min to a total of 0.03 - 0.04 mg/kg
Asystole Treatment Algorithm
Continue CPR Intubate at once Obtain IV Access Confirm asystole in more than 1 lead
Consider possible causes Hypoxia Pre-existing acidosis Hyperkalemia Drug Overdose Hypokalemia Hypothermia
Consider immediate transcutaneous pacing (TCP)a
Figure 4
Epinephrine 1mg IV push,b,c repeat q 3 - 5 min
Atropine 1 mg IV push repeat q 3 - 5 min up to a total of 0.03 - 0.04 mg/kgd,e Consider termination of efforts
Ventricular Fibrillation (VF) Figure 2 & Pulseless Ventricular Tachycardia (VT)
ABCs Perform CPR until defibrillator Arrives VF/VT present on defibrillator
Defibrillate up to 3 times if needed for persistent VF/VT 200 J, 200 - 300 J, 360 J
Rhythm after the first 3 shocks? b
VF/VT
ROSC
PEA Go to Fig 3
Asystole Go to Fig 4
VF & Pulseless VT Continue CPR Intubate / IV Access
Figure 2
Epinephrine c,d 1 mg/IV 2 mg/ETT q 3 - 5 min
Defibrillate 360 J within 30 - 60 sec Administer Rx Class IIa probable benefit f, g Defibrillate 360 J, 30 - 60 sec after Rx
You might also like
- ACLS Algorithms 2011 PDFDocument6 pagesACLS Algorithms 2011 PDFmaya_fitrianaNo ratings yet
- Advanced Cardiovascular Life Support (Acls)Document45 pagesAdvanced Cardiovascular Life Support (Acls)Erinne DefrianiNo ratings yet
- Management of Cardiac Arrhythmias in Advanced Cardiac Life Support (ACLSDocument34 pagesManagement of Cardiac Arrhythmias in Advanced Cardiac Life Support (ACLSrhezzaagxxNo ratings yet
- IABP FINAL by Mr. Adnan (13-04-2020 To 04-05-2020Document33 pagesIABP FINAL by Mr. Adnan (13-04-2020 To 04-05-2020Atia KiranNo ratings yet
- ACLS Study GuideDocument28 pagesACLS Study GuideNicole Berry100% (1)
- American Heart Association Guidelines For CPR 2015: Christopher RyalinoDocument50 pagesAmerican Heart Association Guidelines For CPR 2015: Christopher RyalinoLightNo ratings yet
- Azmi SyncopeDocument50 pagesAzmi Syncopezakiyyatul aflakhaNo ratings yet
- Cardiac Arrest Circular AlgorithmDocument6 pagesCardiac Arrest Circular Algorithmno_spam_mang80% (5)
- Icu GuidebookDocument43 pagesIcu Guidebookdrimran570100% (4)
- Think Link Ecg Notes: Normal Sinus Rhythm at 70 Beats/minDocument3 pagesThink Link Ecg Notes: Normal Sinus Rhythm at 70 Beats/minWillington CuaresmaNo ratings yet
- Saudi CPR Guidlines in EnglishDocument16 pagesSaudi CPR Guidlines in EnglishpiyushbamsNo ratings yet
- Dmergency in Cardiology Part II-dr - Erika Maharani, Sp. JP (K) (2019)Document44 pagesDmergency in Cardiology Part II-dr - Erika Maharani, Sp. JP (K) (2019)lia ancillaNo ratings yet
- Causes and Treatment of Cardiac ArrhythmiasDocument64 pagesCauses and Treatment of Cardiac ArrhythmiasBonitavanyNo ratings yet
- CPR Pitfalls in OSCEDocument35 pagesCPR Pitfalls in OSCEKrittin NaravejsakulNo ratings yet
- Advanced Cardiac Life Support (Acls) Part Ii: ACP 202 Module 6Document32 pagesAdvanced Cardiac Life Support (Acls) Part Ii: ACP 202 Module 6MoeNo ratings yet
- WI EMS Medical Guidelines BradycardiaDocument2 pagesWI EMS Medical Guidelines BradycardiaCheewin KhawprapaNo ratings yet
- Advanced Cardiac Life Support RC 275Document40 pagesAdvanced Cardiac Life Support RC 275Rika Hardiyanti PagalaNo ratings yet
- ACLS Algorithms (2011)Document6 pagesACLS Algorithms (2011)senbonsakuraNo ratings yet
- 8 Pulseless Arrest OkDocument33 pages8 Pulseless Arrest OkJulienne CaoileNo ratings yet
- Understanding Shock Types and TreatmentsDocument75 pagesUnderstanding Shock Types and TreatmentsaulianmediansyahNo ratings yet
- Pulseless VT/VF Algorithm First Impression: Sick or Not Sick? Primary SurveyDocument9 pagesPulseless VT/VF Algorithm First Impression: Sick or Not Sick? Primary SurveyBa LitNo ratings yet
- Problem 1: Julita Suhardi Emergency Medicine BlockDocument94 pagesProblem 1: Julita Suhardi Emergency Medicine BlockZhul Thaa PurpleholicNo ratings yet
- 12 Hours: Continue To Monitor: High-Risk NSTEACSDocument1 page12 Hours: Continue To Monitor: High-Risk NSTEACSMeita ReligiaNo ratings yet
- Advanced Cardiac Life Support (ACLS) : By: Diana Blum MSN Metropolitan Community College Nursing 2150Document16 pagesAdvanced Cardiac Life Support (ACLS) : By: Diana Blum MSN Metropolitan Community College Nursing 2150Vikneswara SoorianarayananNo ratings yet
- AclsDocument73 pagesAclsKamel Hady50% (2)
- ACLS Training 2016Document50 pagesACLS Training 2016Resham RanaNo ratings yet
- IABC Intra Aortic Balloon Counter Pulsation Nicvd PresentationDocument54 pagesIABC Intra Aortic Balloon Counter Pulsation Nicvd PresentationNavojit Chowdhury100% (1)
- Critical Care NursingDocument159 pagesCritical Care NursingJoy Jarin50% (2)
- ACLS AlgorithmDocument28 pagesACLS AlgorithmTommy NainggolanNo ratings yet
- ME10!03!003 MMC Pathway2Document2 pagesME10!03!003 MMC Pathway2Indra WijayaNo ratings yet
- 10 Warning Signs of ImmunodeficiencyDocument24 pages10 Warning Signs of Immunodeficiencyacque100% (2)
- American Heart Association Guidelines For CPR 2015: Wanida Chongarunngamsang, MD. Faculty of Srinakarinwirot UniversityDocument49 pagesAmerican Heart Association Guidelines For CPR 2015: Wanida Chongarunngamsang, MD. Faculty of Srinakarinwirot UniversityZulkarnainBustamamNo ratings yet
- Low BP / fast pulse: Causes and management of shockDocument64 pagesLow BP / fast pulse: Causes and management of shockRachelMokNo ratings yet
- Topic: Cardiac Arrest Megacode: MD Khairulamin AS Nursing Lecturer PAPRSB Institute of Health Sciences UBDDocument38 pagesTopic: Cardiac Arrest Megacode: MD Khairulamin AS Nursing Lecturer PAPRSB Institute of Health Sciences UBDulipah100% (2)
- Cardiac ArrestDocument30 pagesCardiac ArrestTommy NainggolanNo ratings yet
- Cardiac Anesthesia PDFDocument55 pagesCardiac Anesthesia PDFvincent.chauvette100% (3)
- Maternal Collapse in Labour WardDocument114 pagesMaternal Collapse in Labour Wardedwardjohnson231080% (5)
- ACS Acute Pulmonary Edema, Emergency Arrhythmias & Heart Failure AssessmentDocument12 pagesACS Acute Pulmonary Edema, Emergency Arrhythmias & Heart Failure AssessmentviczNo ratings yet
- Emergency in Medicine 2012Document202 pagesEmergency in Medicine 2012micheal1960No ratings yet
- Updated ACLS Study Guide Pulseless VT/VF AlgorithmDocument1 pageUpdated ACLS Study Guide Pulseless VT/VF AlgorithmMaya AritonangNo ratings yet
- Advanced Cardiac Life SupportDocument28 pagesAdvanced Cardiac Life SupportAbdulrahman AlsayyedNo ratings yet
- ACLS MneumonicsDocument4 pagesACLS MneumonicsnaranothNo ratings yet
- ACLS 2005 UpdateDocument46 pagesACLS 2005 UpdateSnakeeyes NonganNo ratings yet
- Ecg in Emergency: Adi SulistyantoDocument41 pagesEcg in Emergency: Adi Sulistyantomech_pilot2203No ratings yet
- Advanced Cardiac Life SupportDocument38 pagesAdvanced Cardiac Life Supporthorosu100% (1)
- CARDIOVASCULAR EMERGENCIES GUIDEDocument47 pagesCARDIOVASCULAR EMERGENCIES GUIDEmedstudy123No ratings yet
- Exercise TestingDocument50 pagesExercise TestingGeoNo ratings yet
- ACLS CE-Part I of III - ECG Strip Interpretation W Case Scenarios SupplementalDocument80 pagesACLS CE-Part I of III - ECG Strip Interpretation W Case Scenarios SupplementalMarc Imhotep Cray, M.D.100% (2)
- Peri Arrest ArrhythmiasDocument40 pagesPeri Arrest ArrhythmiasDestiAriyaniNo ratings yet
- Life Threatening ArrhytmiaDocument41 pagesLife Threatening ArrhytmiaJanetty TjandraNo ratings yet
- Critical Care NursingDocument159 pagesCritical Care Nursinggretchen marie80% (5)
- Mechanical Ventilation: Weaning From Mechanical Ventilation Kathia Ortiz-Cantillo, MDDocument25 pagesMechanical Ventilation: Weaning From Mechanical Ventilation Kathia Ortiz-Cantillo, MDsarevNo ratings yet
- DEmergency in Cardiology Part II-dr - Erika Maharani, Sp. JP (K) (2018)Document44 pagesDEmergency in Cardiology Part II-dr - Erika Maharani, Sp. JP (K) (2018)lia ancillaNo ratings yet
- Bls (Basic Life Support) & Acls (Advanced Care Life Support) : PresenterDocument135 pagesBls (Basic Life Support) & Acls (Advanced Care Life Support) : PresenterbernarduswidodoNo ratings yet
- Guide to Canine and Feline ElectrocardiographyFrom EverandGuide to Canine and Feline ElectrocardiographyRuth WillisNo ratings yet
- Questions and Answers in Small Animal AnesthesiaFrom EverandQuestions and Answers in Small Animal AnesthesiaLesley J. SmithNo ratings yet
- EKG and ECG Interpretation: Learn EKG Interpretation, Rhythms, and Arrhythmia Fast!From EverandEKG and ECG Interpretation: Learn EKG Interpretation, Rhythms, and Arrhythmia Fast!No ratings yet
- ACLS Advanced Cardiovascular Life Support Provider Manual 2023From EverandACLS Advanced Cardiovascular Life Support Provider Manual 2023No ratings yet