Professional Documents
Culture Documents
BLS and ACLS Guidelines
Uploaded by
mirzaoctaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
BLS and ACLS Guidelines
Uploaded by
mirzaoctaCopyright:
Available Formats
Basic and Advanced Life Support
Dr. Nevine Abdel Fattah Lecturer in Chest Diseases Ain Shams University.
Adult Basic Life Support This lecture contains the guidelines for outof-hospital, single rescuer, adult basic life support (BLS). The guidelines are based on the document 2005 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment recommendations.
Adult Basic Life Support
At the end of the lesson you should be able to state and describe the Adult BLS Algorithm, focusing on Cardiac Arrest in a non drowning, non traumatic, non toxic adult collapse. Basic life support (BLS) is a specific level of pre-hospital medical care provided by trained responders, including emergency medical technicians, in the absence of advanced medical care. BLS may also include considerations of patient transport such as the protection of the cervical spine and avoiding additional injuries through splinting and immobilization.
Adult Basic Life Support
Nervous system
Adult Basic Life Support
BLS generally does not include the use of drugs or invasive skills, and can be contrasted with the provision of Advanced cardiac life support (ACLS). CPR provided in the field buys time for higher medical responders to arrive and provide ACLS. For this reason it is essential that any person starting CPR also obtains ACLS support by calling for help via radio using agency policies and procedures and/or using an appropriate emergency telephone number. An important advance in providing BLS is the availability of the automated external defibrillator or AED, which can be used to deliver defibrillation. This improves survival outcomes in cardiac arrest cases, sometimes dramatically.
Adult Basic Life Support
PERSON COLLAPSES
Check if he is unresponsive. Call Emergency number. Get AED (automatic Electric Defibrillator) Begin the ABCDs
Adult Basic Life Support
Adult Basic Life Support
Basic life support consists of the following sequence of actions:
Make sure the victim, any bystanders, and you are safe. Check the victim for a response. Gently shake his shoulders and ask loudly, Are you all right? If he responds: Leave him in the position in which you find him provided there is no further danger. Try to find out what is wrong with him and get help if needed. Reassess him regularly. If he does not respond: Shout for help. Turn the victim supine aligned position or stable side position.
Adult Basic Life Support START THE ABCDs
Airway: Open Airway.
Check Breathing
Breathing Non Breathing Check Circulation Circulation:. Monitor and check Circulation the pulse. Arrest
Breathing:
(Look, Listen &Feel)
Adult Basic Life Support
Defibrillator: An important advance in providing BLS is the availability of AED, which can be used to deliver defibrillation. improving survival outcomes in cardiac arrest cases.
Adult Basic Life Support
Airway Control:
- Chin Lift Maneuver. - Jaw thrust maneuver. - Manual clearing of mouth & throat. - Pharyngeal suctioning. - Pharyngeal intubation.
Adult Basic Life Support
Adult Basic Life Support
Open airways
Adult Basic Life Support
Airway Control:
- Esophageal obturator airway insertion. - Endotracheal intubation &Tracheobronchial suctioning. - Cricothyrotomy - transtracheal O2 jet insufflation. - Tracheotomy, bronchoscopy bronchodilatation, pleural drainage.
Adult Basic Life Support
Breathing:
Keeping the airway open, look, listen, and feel for normal breathing. Look for chest movement. Listen at the victim's mouth for breath sounds. Feel for air on your cheek. In the first few minutes after cardiac arrest, a victim may be barely breathing, taking infrequent, noisy, gasps. Do not confuse this with normal breathing. Look, listen, and feel for no more than 10 sec to determine if the victim is breathing normally. If you have any doubt whether breathing is normal, act as if it is not normal.
Adult Basic Life Support
If he is breathing normally:
Turn him into the recovery position. Send or go for help, or call for an ambulance. Check for continued breathing.
If he is not breathing normally: Ask someone to call for an ambulance or, if you are on your own, do this yourself; you may need to leave the victim. Start chest compression as follows:
Kneel by the side of the victim. Place the heel of one hand in the centre of the victims chest.
Adult Basic Life Support
Place the heel of your other hand on top of the first hand. Interlock the fingers of your hands and ensure that pressure is
not applied over the victim's ribs. Do not apply any pressure over the upper abdomen or the bottom end of the bony sternum (breastbone).
Position yourself vertically above the victim's chest and, with
your arms straight, press down on the sternum 4 - 5 cm.
After each compression, release all the pressure on the chest
without losing contact between your hands and the sternum.
Repeat at a rate of about 100 times a minute (a little less than
2 compressions a second).
Compression and release should take an equal amount of time.
Adult Basic Life Support
RECOVERY POSITION
Adult Basic Life Support
Adult Basic Life Support
Breathing support:
- Mouth-to-mouth (nose) ventilation. - Mouth-to-adjunct with or without O2. - Manual bag-mask (tube) ventilation with or without O2. - Hand-triggered O2 ventilation - Mechanical ventilation
Adult Basic Life Support
Combine chest compression with rescue breaths:
After 30 compressions open the airway again using head tilt and chin lift. Pinch the soft part of the victims nose closed, using the index finger and thumb of your hand on his forehead. Allow his mouth to open, but maintain chin lift. Take a normal breath and place your lips around his mouth, making sure that you have a good seal. Blow steadily into his mouth whilst watching for his chest to rise; take about one second to make his chest rise as in normal breathing; this is an effective rescue breath. Maintaining head tilt and chin lift, take your mouth away from the victim and watch for his chest to fall as air comes out.
Adult Basic Life Support
Take another normal breath and blow into the victims mouth once more to give a total of two effective rescue breaths. Then return your hands without delay to the correct position on the sternum and give a further 30 chest compressions. Continue with chest compressions and rescue breaths in a ratio of 30:2. Stop to recheck the victim only if he starts breathing normally; otherwise do not interrupt resuscitation.
Adult Basic Life Support
If your rescue breaths do not make the chest rise as in normal breathing, then before your next attempt:
Check the victim's mouth and remove any visible obstruction. Recheck that there is adequate head tilt and chin lift. Do not attempt more than two breaths each time before returning to chest compressions.
If there is more than one rescuer present, another should take over CPR about every 2 min to prevent fatigue. Ensure the minimum of delay during the changeover of rescuers.
Adult Basic Life Support
Adult Basic Life Support
Circulation support:
- Control of external hemorrhage. - Position of shock. - Pulse checking. - Mechanical chest compressions. - Open chest direct cardiac Compressions.
Adult Basic Life Support
Chest-compression-only CPR: If you are not able, or are unwilling, to give rescue breaths, give chest compressions only. If chest compressions only are given, these should be continuous at a rate of 100 a minute. Stop to recheck the victim only if he starts breathing normally; otherwise do not interrupt resuscitation.
Adult Basic Life Support
Adult Basic Life Support
Continue resuscitation until:
Qualified help arrives and takes over, The victim starts breathing normally, or You become exhausted.
Adult Basic Life Support Algorithm
Check Responsiveness Shake and Shout
Open Airway Head tilt/chin lift
Check Breathing Look, listen and feel
2 Effective Breaths
Signs of circulation Assess 10 seconds only
Circulation Present Continue Rescue Breathing
No Circulation Compress Chest Rate of 100 per second 30 compressions to 2 breaths (30:2)
Adult Advanced Cardiac Life Support
Advanced Cardiac Life support (ACLS) is a detailed medical protocol for the provision of lifesaving cardiac care in settings ranging from the pre-hospital environment to the hospital setting.
Extensive medical knowledge and rigorous hands-on training and practice are required to master ACLS. Only qualified health care providers (doctors, nurses, emergency medical responders) can provide ACLS.
Adult Advanced Cardiac Life Support
ACLS is an extension of BLS, especially now that the use of automated external defibrillators (AEDs) in outof-hospital setting has become part of BLS. The aim of this section is to review the Adult Advanced Life support Algorithm.
Adult Advanced Life Support Algorithm
Adult Advanced Life Support Algorithm
Cardiac Arrest
Pericordial Thump if appropriate
Monitored or Witnessed Arrest!
Within 30 seconds from time of arrest. Used once only.
Adult Advanced Life Support Algorithm
Cardiac Arrest
Pericordial Thump if appropriate
BLS Algorithm if appropriate
Adult Advanced Life Support Algorithm
Cardiac Arrest
Pericordial Thump if appropriate
Lead positions;
BLS Algorithm if appropriate
Attach AED Monitor
Chest free of Lead wiring.
Ride Your Bike
Adult Advanced Life Support Algorithm
Cardiac Arrest
Pericordial Thump if appropriate
BLS Algorithm if appropriate
Attach AED Monitor
Assess Rhythm
+/- Check Pulse
VF/VT
Non VF/VT
Adult Advanced Life Support Algorithm
Adult Advanced Life Support Algorithm
Non VF/VT
Any rhythm other than VF/VT
Adult Advanced Life Support Algorithm
Cardiac Arrest
Pericordial Thump if appropriate
BLS Algorithm if appropriate
Attach AED Monitor
Assess Rhythm
+/- Check Pulse
VF/VT
Defibrillate x 3 As necessary
Non VF/VT
CPR immediately 1 min after AED
CPR 1 min
Adult Advanced Life Support Algorithm
Cardiac Arrest Assess Rhythm
VF/VT
Defibrillate x 3 As necessary
CPR 1 min
Adult Advanced Life Support Algorithm
Assess Rhythm +/- Check Pulse
Cardiac Arrest
Non VF/VT
CPR 3min 1 min immediately after AED
Adult Advanced Life Support Algorithm
CardiacRhythm Arrest Assess
+/- Check Pulse
VF/VT
During CPR
Correct reversible causes
If not done already:
Non VF/VT
Defibrillate x 3 As necessary
Check des, paddle position and contact. Attempt / Verify: Airway and O2 IV Access : Give Epinephrine every 3min. Consider : Amiodarone, Atropine/ Pacing & Buffers.
CPR immediately 1 min after AED
CPR 1 min
Adult Advanced Life Support Algorithm
During CPR
Correct reversible causes If not done already: Check des, paddle position and contact.
Attempt / Verify: Airway and O2
IV Access : Give Epinephrine every 3min.
Consider : Amiodarone, Atropine/ Pacing & Buffers.
Adult Advanced Life Support Algorithm
The Hs & Ts
Potential Reversible Causes Hypoxia Hpovolaemia Hypo/Hyperkalaemia and Metabolic disorders Hypothermia Tension Pneumothorax Tamponade Toxic /Therapeutic Disorders Thromboembolic and Mechanical obstruction.
Adult Advanced Life Support Algorithm
Questions?
THANK YOU
You might also like
- Pediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesFrom EverandPediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesRating: 5 out of 5 stars5/5 (2)
- Advanced Cardiac Life Support Quick Study Guide 2015 Updated GuidelinesFrom EverandAdvanced Cardiac Life Support Quick Study Guide 2015 Updated GuidelinesRating: 4 out of 5 stars4/5 (6)
- BlsDocument9 pagesBlsGhia Iane Galicia SalvaNo ratings yet
- First Aid Essentials for Life Saving (39Document64 pagesFirst Aid Essentials for Life Saving (39KBDNo ratings yet
- CPR ALS ProcedureDocument10 pagesCPR ALS ProcedureTanmoyNo ratings yet
- Basic Life Support For Adult: Evaluating ResponsivenessDocument4 pagesBasic Life Support For Adult: Evaluating ResponsivenessJulang FahmanNo ratings yet
- BLS - BSN 2023Document90 pagesBLS - BSN 2023kenyaga JobNo ratings yet
- CPR Guide for Adults, Children & BabiesDocument6 pagesCPR Guide for Adults, Children & Babiesrupali gahalian100% (2)
- BLS Guide: Adult Basic Life Support StepsDocument50 pagesBLS Guide: Adult Basic Life Support StepsVijay Krishna Murthy80% (5)
- Adult Basic Life Support: Resuscitation Council (UK)Document14 pagesAdult Basic Life Support: Resuscitation Council (UK)Agus PriyantoNo ratings yet
- Basic LifeDocument33 pagesBasic LifetmschppmNo ratings yet
- First Aid Prenciples E-VerDocument54 pagesFirst Aid Prenciples E-Verapi-205902640100% (1)
- BLS Skills Lab For SimulationDocument116 pagesBLS Skills Lab For Simulationczeremar chan100% (1)
- Mod 3.1 - 4.1 - First AidDocument72 pagesMod 3.1 - 4.1 - First Aidabhishek sudheerNo ratings yet
- What Is Cardiac Arrest?: How Is CPR Performed?Document3 pagesWhat Is Cardiac Arrest?: How Is CPR Performed?Andrew PetalloNo ratings yet
- Lab 1: Basic Life SupportDocument16 pagesLab 1: Basic Life Supportj.doe.hex_87No ratings yet
- BLS AlgorithmDocument9 pagesBLS AlgorithmDr VJ GeorgeNo ratings yet
- Basic Life Support: Submitted By: Kennedy V. Velasco Bscrim 1-AlphaDocument7 pagesBasic Life Support: Submitted By: Kennedy V. Velasco Bscrim 1-AlphaProsperJuan BelieversNo ratings yet
- Chapter 5 EMERGENCY TREATMENTDocument22 pagesChapter 5 EMERGENCY TREATMENTEmmaNo ratings yet
- BLS Basics: Scene Safety, Circulation, Airway, BreathingDocument118 pagesBLS Basics: Scene Safety, Circulation, Airway, Breathingharpreet100% (1)
- Bls - Fbao - First AidDocument172 pagesBls - Fbao - First AidMaria Regina Castro Gabriel100% (1)
- Pediatric Basic Life Support: Philippine Heart Association Council On Cardio-Pulmonary ResuscitationDocument106 pagesPediatric Basic Life Support: Philippine Heart Association Council On Cardio-Pulmonary Resuscitationjitendra magarNo ratings yet
- Bls Question 1Document7 pagesBls Question 1balderas135384No ratings yet
- Basic Life SupportDocument4 pagesBasic Life Supportraven_claw25No ratings yet
- Adult BLS SequenceDocument2 pagesAdult BLS Sequencerikirdn27No ratings yet
- Masuri Prim AjutorDocument143 pagesMasuri Prim AjutorHojbota Otilia Constantina100% (1)
- CPR 1Document12 pagesCPR 1Renju JoseNo ratings yet
- CPR Program Objectives and TechniquesDocument7 pagesCPR Program Objectives and TechniquesragsyragsyNo ratings yet
- Basic Life Support HandoutDocument13 pagesBasic Life Support HandoutmdavaoNo ratings yet
- Cardiopulmonary Resuscitation: Mrs. Jenitta. G Lecturer/Asst - ProfessorDocument17 pagesCardiopulmonary Resuscitation: Mrs. Jenitta. G Lecturer/Asst - ProfessorCheran Devi100% (1)
- How To CPRDocument4 pagesHow To CPRRosi ArristaNo ratings yet
- Adult BLSDocument50 pagesAdult BLSdianNo ratings yet
- Lesson 4 A Basic Life SupportDocument49 pagesLesson 4 A Basic Life SupportJames Artajo ViajedorNo ratings yet
- Mod12 EmergencyFirst AidDocument29 pagesMod12 EmergencyFirst AidMhanna AYNo ratings yet
- Essentials of CPR: Lifesaving Steps for Cardiac EmergenciesDocument8 pagesEssentials of CPR: Lifesaving Steps for Cardiac Emergencieshiba majidNo ratings yet
- ACLSDocument78 pagesACLSKajalNo ratings yet
- BLS Algorithms and Training 2020Document22 pagesBLS Algorithms and Training 2020Ronald Aranha100% (1)
- BLS Healthcare ProvidersDocument8 pagesBLS Healthcare ProviderscmurphNo ratings yet
- LA Union: PDRRM ODocument32 pagesLA Union: PDRRM OEnash RidNo ratings yet
- 3.1 Introduction To First Aid and CPRDocument5 pages3.1 Introduction To First Aid and CPRPriyanshu BalaniNo ratings yet
- BASIC LIFE SUPPORT CPRDocument28 pagesBASIC LIFE SUPPORT CPRaefgNo ratings yet
- Cardiopulmonary Resuscitation (CPR)Document18 pagesCardiopulmonary Resuscitation (CPR)Althea Amor CambarijanNo ratings yet
- CPR For AdultsDocument1 pageCPR For Adultsevelyn kNo ratings yet
- BLS FinalDocument47 pagesBLS Finalshouvik chowdhury100% (1)
- BLS and First Aid ReportDocument4 pagesBLS and First Aid ReportAriane Joyce AgkisNo ratings yet
- How To Do CPR On An AdultDocument25 pagesHow To Do CPR On An AdultabNo ratings yet
- C.P.R. (1)Document19 pagesC.P.R. (1)sxm2901No ratings yet
- Basic Life SupportDocument36 pagesBasic Life SupportycccaNo ratings yet
- First Aid Is An Immediate and Temporary Care Given Mapeh Lesson 3 3rd QuarterDocument3 pagesFirst Aid Is An Immediate and Temporary Care Given Mapeh Lesson 3 3rd QuarterJanix MagbanuaNo ratings yet
- How To Perform CPRDocument2 pagesHow To Perform CPRAmirul AzhanNo ratings yet
- Cardio-Pulmonary Resuscitation (CPR)Document18 pagesCardio-Pulmonary Resuscitation (CPR)Savita HanamsagarNo ratings yet
- BLS Study Guide PDFDocument12 pagesBLS Study Guide PDFPingChavez100% (1)
- Ace Personal Trainer Manual Chapter 16Document18 pagesAce Personal Trainer Manual Chapter 16Đạt NguyễnNo ratings yet
- Cardiopulmonary ResuscitationDocument38 pagesCardiopulmonary ResuscitationAgus SyaifudinNo ratings yet
- CPR PresentationDocument22 pagesCPR PresentationAlan HabalNo ratings yet
- BLS PresentationDocument36 pagesBLS PresentationRishabh MittalNo ratings yet
- BLS & AclsDocument112 pagesBLS & AclsPriya SharmaNo ratings yet
- Untrained. If You're Not Trained in CPR, Then Provide Hands-Only CPR. ThatDocument12 pagesUntrained. If You're Not Trained in CPR, Then Provide Hands-Only CPR. ThatClaire DayritNo ratings yet
- PALS Overview for BLS and Healthcare ProvidersDocument26 pagesPALS Overview for BLS and Healthcare Providersmonir61No ratings yet
- BLS Algorithms and Training 2019: (Basic Life Support)Document21 pagesBLS Algorithms and Training 2019: (Basic Life Support)Haidir MuhammadNo ratings yet
- SepsisDocument285 pagesSepsismirzaoctaNo ratings yet
- ACLS AlgorithmsDocument14 pagesACLS AlgorithmsArif KurniadiNo ratings yet
- Drip ChartDocument10 pagesDrip Chartmirzaocta100% (1)
- Panduan Pelayanan BedahDocument3 pagesPanduan Pelayanan BedahAndris PurwaningtiasNo ratings yet
- Buku AnestesiDocument33 pagesBuku AnestesiAan AnharNo ratings yet
- Thyroid Disease Anesthetic ConsiderationsDocument30 pagesThyroid Disease Anesthetic ConsiderationsmirzaoctaNo ratings yet
- Systemic Response To InjuryDocument20 pagesSystemic Response To InjurymirzaoctaNo ratings yet
- Hand Washing PDFDocument1 pageHand Washing PDFmirzaoctaNo ratings yet
- 5momentsHandHygiene A3 PDFDocument1 page5momentsHandHygiene A3 PDFDwi SurantoNo ratings yet
- Bls 2013Document12 pagesBls 2013mirzaocta100% (1)
- CV TITLEDocument3 pagesCV TITLEAdraNo ratings yet
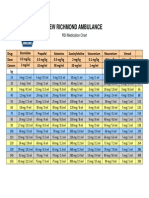
- EMS Agency Color Code Drug Doses L. L.A. County Kids: Normal Vital Signs PALS Drugs - Initial Dose MedicationDocument5 pagesEMS Agency Color Code Drug Doses L. L.A. County Kids: Normal Vital Signs PALS Drugs - Initial Dose MedicationCruz VerdeNo ratings yet
- Airway and The NurseDocument7 pagesAirway and The NursecarmenbuleandraNo ratings yet
- Phecc CPG 2021 - Far Web3Document69 pagesPhecc CPG 2021 - Far Web3James McloughlinNo ratings yet
- Advance Life SupportDocument198 pagesAdvance Life SupportPantelis PouliopoulosNo ratings yet
- A Systematic Approach To EMS Cardiac Arrest Management Improves Survival For Out of Hospital Cardiac ArrestDocument29 pagesA Systematic Approach To EMS Cardiac Arrest Management Improves Survival For Out of Hospital Cardiac ArrestMELLYNDA ANASTASYANo ratings yet
- Ground Ambulance Services in The United States - A FAIR Health White PaperDocument31 pagesGround Ambulance Services in The United States - A FAIR Health White PaperepraetorianNo ratings yet
- Medical Plan ICS 206Document2 pagesMedical Plan ICS 206Alo RioNo ratings yet
- Advanced Life Support Algorithm: Version: July 2016Document45 pagesAdvanced Life Support Algorithm: Version: July 2016Dwi RinaNo ratings yet
- Cardio Pulmonary ResuscitationDocument8 pagesCardio Pulmonary ResuscitationRuchika Kaushal71% (7)
- BLS and ACLS GuidelinesDocument46 pagesBLS and ACLS GuidelinesmirzaoctaNo ratings yet
- Aea-V 2009 EbaDocument110 pagesAea-V 2009 EbaDave JonesNo ratings yet
- Advanced Life Support Training and Assessment PDFDocument6 pagesAdvanced Life Support Training and Assessment PDFwilmaNo ratings yet
- EMS Alphabet SoupDocument3 pagesEMS Alphabet SoupCourtney0% (1)
- Agreement AmbulanceDocument3 pagesAgreement AmbulanceVIKAS PANERI100% (2)
- Emergency Medical Services Pre-Hospital Treatment Protocols: Complete Text Eighth Edition Effective 3/1/2010Document257 pagesEmergency Medical Services Pre-Hospital Treatment Protocols: Complete Text Eighth Edition Effective 3/1/2010Slaviša KovačevićNo ratings yet
- 2.1 Algoritmos AHA 2020Document22 pages2.1 Algoritmos AHA 2020Lorena Angarita RamirezNo ratings yet
- Convention Centre Detailed InfoDocument43 pagesConvention Centre Detailed InfoSaranya Saru100% (1)
- Basic Life Support and Advanced Cardiac Life Support: Knowledge of Medical Students in New DelhiDocument9 pagesBasic Life Support and Advanced Cardiac Life Support: Knowledge of Medical Students in New DelhiSriatiNo ratings yet
- Warren More Emergency Medical Services Personnel and Increased Survival After OHCADocument9 pagesWarren More Emergency Medical Services Personnel and Increased Survival After OHCAJamison ParfittNo ratings yet
- Manipal Manual of Resuscitation - 4th EditionDocument73 pagesManipal Manual of Resuscitation - 4th EditionAshlita Mendonca100% (2)
- ALS AlgorithmDocument22 pagesALS AlgorithmBookwormNo ratings yet
- Advanced Life Support Protocol Update 2006Document59 pagesAdvanced Life Support Protocol Update 2006Dennis Nabor Muñoz, RN,RM100% (3)
- Advanced Life Support-RESSU CouncilDocument30 pagesAdvanced Life Support-RESSU CouncilGigel DumitruNo ratings yet
- 25 E.D Questions With RationaleDocument12 pages25 E.D Questions With RationaleRhose Angel AzurNo ratings yet
- 3 (NCORT) Guidelines For Resuscitation Training in Ministry of Health Malaysia Hospitals & Healthcare Facilities PDFDocument66 pages3 (NCORT) Guidelines For Resuscitation Training in Ministry of Health Malaysia Hospitals & Healthcare Facilities PDFDzarrinNo ratings yet
- Charleston County Clinical Operating Guidelines: Adult & PediatricDocument207 pagesCharleston County Clinical Operating Guidelines: Adult & PediatricJohn DodsonNo ratings yet
- Erc - Sva 2021Document37 pagesErc - Sva 2021Vinícius MenegatNo ratings yet
- NZRC - All Adult Advanced Life Support Guidelines3Document79 pagesNZRC - All Adult Advanced Life Support Guidelines3stanwalksNo ratings yet