Professional Documents
Culture Documents
Tamponade Kordis
Uploaded by
Muhammad Aprianto Ramadhan0 ratings0% found this document useful (0 votes)
98 views20 pagesTamponade kordis
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentTamponade kordis
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
98 views20 pagesTamponade Kordis
Uploaded by
Muhammad Aprianto RamadhanTamponade kordis
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 20
Cardiac tamponade
Muhammad Aprianto Ramadhan
Stase Bedah
FK UGM/RSST Klaten
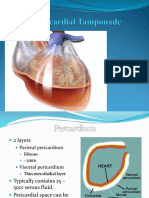
Anatomy
The pericardium, which
is the membrane
surrounding the heart,
is composed of 2 layers.
The thicker parietal
pericardium is the outer
fibrous layer; the
thinner visceral
pericardium is the inner
serous layer.
The pericardial space
normally contains 20-
50mL of fluid.
Whats happening in a cardiac
tamponade?
An increase in intrapericardial pressure and volume by 60 to 100 mL of blood and
clots in the pericardium
Disrupt ventricular filling stroke volume cardiac output SHOCK
LIFE THREATENING
BP , pulse pressure , CVP (except there is hypovolemia)
Compensatory mechanisms
Heart rate and total peripheral resistance (to maintain adequate cardiac output and blood
pressure).
increase in venomotor tone of vena cava greater increase of CVP less effective
In a normotensive patient, the earliest response to pericardial tamponade is a
progressive increase in CVP to a level greater than 15 cm H
2
O.
An increasing CVP in a hypotensive patient indicates that the normal
compensatory responses are unable to maintain an adequate cardiac output.
A simultaneous decrease in the CVP and blood pressure, which can occur
precipitously and without warning, signals decompensation and imminent
cardiac arrest.
When to suspect cardiac tamponade?
History of penetrating trauma to the chest or upper
abdomen
Rarely in blunt trauma
Shock or ongoing hypotension without obvious blood loss
Unsuccessful rescuscitation effort
Classic signs: Becks triad
Jugular venous distension
Hypotension
Muffled heart tone
Pulsus paradoxus
decrease in systolic pressure of >10 mmHg during inspiration
difficult to detect in rescuscitation practice
33%
patient
How to confirm cardiac tamponade?
Ultrasonography 98.1% sensitivity, 99.9% specificity
for pericardial effusion.
Tamponade: simultaneous presence of pericardial fluid
and diastolic collapse of the right ventricle or atrium
How to confirm cardiac tamponade?
Pericardial window
The most direct method to determine the presence of blood within
the pericardium.
Best performed in OR under GA through either the subxiphoid or
transdiaphragmatic approach.
Adequate equipment and personnel to rapidly decompress the
pericardium, explore the injury, and repair the heart should be
present.
Once the pericardium is opened and tamponade relieved,
hemodynamics usually improve dramatically and formal pericardial
exploration can ensue.
Exposure of the heart can be achieved by extending the incision to
a median sternotomy, performing a left anterior thoracotomy, or
performing bilateral anterior thoracotomies ("clamshell").
How to confirm cardiac tamponade?
Electrocardiography
Swinging heart phenomenon when
fluid accumulates to a critical extent and
cardiac tamponade ensues, cardiac
position alternates, with the heart
returning to its original position with
every other beat, and electrical alternans
may be seen.
Electrical alternans: ECG change in which
the morphology and amplitude of the P,
QRS, and ST-T wave in any single lead
alternates in every other beat
Electrical alternans, when present, is
pathognomonic for tamponade
It is much more common in chronic
pericardial effusions that evolve into a
tamponade, however, and it is rarely
seen in acute pericardial tamponade.
How to confirm cardiac tamponade
Radiography
In acute pericardial
tamponade generally is not
helpful (unless a traumatic
pneumopericardium is
present).
Because small volumes of
hemopericardium lead to
tamponade in the acute
setting, the heart typically
appears normal
This is in contrast to the
water-bottle appearance of
the heart with chronic
pericardial effusion. This
latter condition is tolerated
for a long period.
Emergency management
Fluid rescuscitation
Presence of a pneumothorax or hemothorax,
associated with penetrating cardiac trauma
tube thoracostomy.
Bedside echocardiography/sonography
Pericardiocentesis temporary relief
Refer when patients hemodynamic stabilized
Pericardiocentesis
Aspiration of 5 to 10 mL of blood may result in
dramatic clinical improvement.
<<< total intrapericardial volume to just below
critical level allows compensatory mechanisms
to maintain adequate hemodynamics.
Pericardiocentesis
Blood in the pericardial space tends to be
clotted, and aspiration may not be possible.
Possible complications
production of pericardial tamponade
laceration of a coronary artery or lung
induction of cardiac dysrhythmias
Technique: Approach
Parasternal
approach
Through the left
5th or 6th
intercostal space
near the sternum.
The cardiac notch
in the left lung and
the shallower
notch in the left
pleural sac leaves
part of the
pericardial sac
exposedthe bare
area of the
pericardium
Technique: Approach
Infrasternal
approach
Passing the needle
superoposteriorly
At this site, the
needle avoids the
lung and pleurae
and enters the
pericardial cavity
Care must be taken
not to puncture
the internal
thoracic artery or
its terminal
branches.
Technique: Equipment
Surgical preparation set: gauze, antiseptic
solution (povidone iodine 10%)
Local anestethics: lidocaine 2%
16 to 18G catheter with 6 (15 cm) or more
length needle
Syringe
Three-way stopcock
Electrocardiography
CVP monitor
Technique: Procedure
Monitor tanda vital, EKG, dan CVP pasien
sebelum, selama, dan setelah prosedur.
Preparasi sebelum prosedur pada area xiphoid
dan subxiphoid (jika waktu cukup)
Anestesi lokal di tempat pungsi (jika perlu)
Tusuk kulit 1-2 cm di inferior xiphochondrial
junction kiri dengan sudut 45o
Dorong jarum hati-hati ke arah sefalad menuju
ujung skapula kiri
Jika jarum didorong terlalu jauh (myokardium),
pola cedera muncul pada monitor EKG
Pola cedera misal: perubahan ekstrem gelombang ST-
T atau membesarnya kompleks QRS
Tarik jarum sampai pola EKG sebelumnya muncul
kembali
Ketika ujung jarum memasuki perikardium,
aspirasi cairan sebanyak mungkin
Pola cedera mungkin muncul lagi saat aspirasi karena
epikardium kembali mendekat dengan perikardium.
Tarik jarum sedikit. Jika pola menetap, tarik jarum
keluar.
Setelah aspirasi selesai, cabut tabung jarum,
sambungkan ke 3-way
Jarum plastik perikardiosentesis dapat dijahit
atau diplester dan ditutup kasa kecil.
Jika gejala tamponade persisten, dapat
dilakukan dekompresi berulang.
Setelah hemodinamik pasien stabil, rujuk
unutk penanganan definitif.
References
Marx JA (ed). 2006. Rosen's Emergency
Medicine: Concepts and Clinical Practice, 6th
ed. USA: Elsevier.
Moore KL, Dalley AF, Agur AM. 2010. Clinically
Oriented Anatomy, sixth edition. USA:
Lippincott Williams & Wilkins
American College of Surgeons Committee in
Trauma. Advanced Trauma Life Support for
Doctors, Student Course Manual, 8
th
edition.
Thank you
You might also like
- Cardiac TemponadeDocument18 pagesCardiac TemponadeDIVYA GANGWAR100% (1)
- Cardiac Tamponade (Suryani)Document72 pagesCardiac Tamponade (Suryani)Hamdani UsmanNo ratings yet
- Valvular Heart Disease To TW FinalDocument13 pagesValvular Heart Disease To TW FinalMohammed ElSayedNo ratings yet
- Early Detection and Management of Cardiac TamponadeDocument34 pagesEarly Detection and Management of Cardiac TamponadeWiwing SetionoNo ratings yet
- Richardson2014 PDFDocument2 pagesRichardson2014 PDFJanuar Alfred PoliNo ratings yet
- Dr. Shaker's Guide to Managing Cyanotic Heart DiseaseDocument66 pagesDr. Shaker's Guide to Managing Cyanotic Heart DiseasePrasanth SankarNo ratings yet
- Pericardialdiseases 190121084846Document65 pagesPericardialdiseases 190121084846Insta GrammerNo ratings yet
- Cardiac TamponadeDocument29 pagesCardiac Tamponadeanimesh pandaNo ratings yet
- CCPACatheter Basics 07 MedicineDocument44 pagesCCPACatheter Basics 07 MedicinerinbijoyNo ratings yet
- Cardiac Tamponade: Pankaj Singh Rana Nurse Practitioner in Critical Care Swami Rama Himalayan UniversityDocument35 pagesCardiac Tamponade: Pankaj Singh Rana Nurse Practitioner in Critical Care Swami Rama Himalayan UniversityBarlonga Yhan YogaNo ratings yet
- Hypovolemic Shock Cardiogenic Shock Obstructive Shock: Prepared By: HO Tiviyah Mentor: DR Tiong Supervisor: DR Tham MinDocument29 pagesHypovolemic Shock Cardiogenic Shock Obstructive Shock: Prepared By: HO Tiviyah Mentor: DR Tiong Supervisor: DR Tham MinTeik Wei TanNo ratings yet
- 10 Tra - Cardiovascular NursingDocument21 pages10 Tra - Cardiovascular NursingJoshua Delantar100% (1)
- Congenital Heart Disease: Kriti Puri, MD Hugh D. Allen, MD Athar M. Qureshi, MDDocument30 pagesCongenital Heart Disease: Kriti Puri, MD Hugh D. Allen, MD Athar M. Qureshi, MDhari ilman toniNo ratings yet
- Cardiac TamponadeDocument43 pagesCardiac TamponadeMădălina GreereNo ratings yet
- Understanding Pericardial DiseasesDocument50 pagesUnderstanding Pericardial DiseasesRawabi rawabi1997No ratings yet
- Open Heart 1Document18 pagesOpen Heart 1mohamedNo ratings yet
- Diseases of The Pericardium 2 PDFDocument50 pagesDiseases of The Pericardium 2 PDFRawabi rawabi1997No ratings yet
- Cardiac Tamponade: Mrs. D.Melba Sahaya Sweety.D M.SC Nursing GimsarDocument23 pagesCardiac Tamponade: Mrs. D.Melba Sahaya Sweety.D M.SC Nursing GimsarD. Melba S.S ChinnaNo ratings yet
- CardioDocument32 pagesCardioFarhan AliNo ratings yet
- Anesthesia techniques for cardiac surgeryDocument179 pagesAnesthesia techniques for cardiac surgerymd.dascalescu2486No ratings yet
- Heart Failure: Zelalem T., MD Yr III Resident, PediatricsDocument65 pagesHeart Failure: Zelalem T., MD Yr III Resident, PediatricsChalie MequanentNo ratings yet
- Constrictive PericarditisDocument54 pagesConstrictive PericarditisRazib AlamNo ratings yet
- Congenital Heart DiseaseDocument55 pagesCongenital Heart DiseaseRaviNo ratings yet
- Congenital Heart Disease: Thoracic Conference Frank Nami, M.DDocument49 pagesCongenital Heart Disease: Thoracic Conference Frank Nami, M.DMarie CrystallineNo ratings yet
- Cardiovasucular Problems in Children: Niranjana Shalini. M.SC (N) Assistant ProfessorDocument79 pagesCardiovasucular Problems in Children: Niranjana Shalini. M.SC (N) Assistant ProfessorNIRANJANA SHALININo ratings yet
- Ductus Arteriosus Dependent Congenital Heart Disease: Amjad Kouatli MD. FAAP. FACCDocument28 pagesDuctus Arteriosus Dependent Congenital Heart Disease: Amjad Kouatli MD. FAAP. FACCKartik KumarasamyNo ratings yet
- Pulmonary Artery Catheterization and MonitoringDocument31 pagesPulmonary Artery Catheterization and MonitoringVhince Norben PiscoNo ratings yet
- SurgeryDocument199 pagesSurgerytaha obaidNo ratings yet
- Examination and Investigation of The Cardiovascular System (CVS)Document27 pagesExamination and Investigation of The Cardiovascular System (CVS)Jake MillerNo ratings yet
- New HematologyOncology FAE2016Document108 pagesNew HematologyOncology FAE2016omarNo ratings yet
- Cardiac Tamponad E: Pathophysiology and ManagementDocument105 pagesCardiac Tamponad E: Pathophysiology and ManagementBimaNo ratings yet
- Cardiac Tamponade and ManagementDocument42 pagesCardiac Tamponade and Managementأم حمدNo ratings yet
- ECMO (Extracorporeal Membrane Oxygenation)Document22 pagesECMO (Extracorporeal Membrane Oxygenation)dhivya singhNo ratings yet
- Model Answer -I & II سبتمبر 2015تحريريDocument12 pagesModel Answer -I & II سبتمبر 2015تحريريAmr El TaherNo ratings yet
- Department of Internal Medicine Iii Tricuspid Valve DiseasesDocument57 pagesDepartment of Internal Medicine Iii Tricuspid Valve DiseasesSuba Saravanan 12No ratings yet
- Hemodynamics Basic Concepts 1204053445109897 4Document115 pagesHemodynamics Basic Concepts 1204053445109897 4valeriesolidum100% (1)
- Congenital Heart Diseases: DR - Ankita Patel MPT (Cardio-Pulmonary)Document41 pagesCongenital Heart Diseases: DR - Ankita Patel MPT (Cardio-Pulmonary)heena solankiNo ratings yet
- CLASS 2 Low Cardiac Output Syndrome in Cardiac SurgeryDocument53 pagesCLASS 2 Low Cardiac Output Syndrome in Cardiac SurgeryjuanolivelloNo ratings yet
- Hemodynamic Monitoring Guide (39Document49 pagesHemodynamic Monitoring Guide (39Pratami Rieuwpassa IINo ratings yet
- Cardiogenic Shock and Pulmonary EdemaDocument41 pagesCardiogenic Shock and Pulmonary EdemaChristian Gallardo, MD100% (7)
- Cardiology In-Training ObjectivesDocument18 pagesCardiology In-Training ObjectiveshectorNo ratings yet
- Antman 1979Document4 pagesAntman 1979Binod KumarNo ratings yet
- Cyanotic Congenital Heart DiseasesDocument25 pagesCyanotic Congenital Heart DiseasesAlvin OmondiNo ratings yet
- Chest Pain. Surgical Treatment of Acute Coronary Syndrome (ACS)Document21 pagesChest Pain. Surgical Treatment of Acute Coronary Syndrome (ACS)Hanif ZamriNo ratings yet
- G01-Initial Assessment and Management of The Multiply Injured PatientDocument48 pagesG01-Initial Assessment and Management of The Multiply Injured Patientkosmynin86No ratings yet
- Anesthetic Management of Intracranial AneurysmsDocument66 pagesAnesthetic Management of Intracranial AneurysmsadheNo ratings yet
- 1 - PPT DR Taufik Nur Yahya SPBTKVDocument46 pages1 - PPT DR Taufik Nur Yahya SPBTKVAmry YusufNo ratings yet
- Perfusion EmergenciesDocument67 pagesPerfusion EmergenciesThulasi MuniappanNo ratings yet
- CTSU Presentation PDADocument41 pagesCTSU Presentation PDAEdwin OkonNo ratings yet
- Echocardiographic Evaluation of PericardiumDocument64 pagesEchocardiographic Evaluation of PericardiumSruthiNo ratings yet
- Bls and Acls: Deepika SelvaDocument82 pagesBls and Acls: Deepika SelvaPriyanka TNo ratings yet
- CompressedDocument73 pagesCompressedapi-667225436No ratings yet
- Hemodynamic Monitoring Riding The Waves in California Renee SmithDocument30 pagesHemodynamic Monitoring Riding The Waves in California Renee SmithSanaz NikiNo ratings yet
- Atrial Fibrillation: Key TreatmentsDocument2 pagesAtrial Fibrillation: Key TreatmentschoobiNo ratings yet
- CARDIOVASCULAR EMERGENCIES GUIDEDocument47 pagesCARDIOVASCULAR EMERGENCIES GUIDEmedstudy123No ratings yet
- Case Scenerio: DR Sourath Munir Malkani Fcps-Ii TraineDocument31 pagesCase Scenerio: DR Sourath Munir Malkani Fcps-Ii TraineSoonh ChannaNo ratings yet
- Abdominal AortaDocument41 pagesAbdominal AortaMichael IdowuNo ratings yet
- Trauma Tumpul AbdomenDocument30 pagesTrauma Tumpul AbdomendewiswahyuNo ratings yet
- ACLS SubhankarDocument87 pagesACLS SubhankarMarc Andreo MalalaNo ratings yet
- 2019 ESC/EAS Guidelines For The Management of Dyslipidaemias: Lipid Modification To Reduce Cardiovascular Risk: Supplementary DataDocument18 pages2019 ESC/EAS Guidelines For The Management of Dyslipidaemias: Lipid Modification To Reduce Cardiovascular Risk: Supplementary DataElena CosminaNo ratings yet
- Sports Facilities ResearchDocument41 pagesSports Facilities ResearchMuhammad TariqNo ratings yet
- Science 9 Quarter 1 Week 2 Sim 3Document30 pagesScience 9 Quarter 1 Week 2 Sim 3Jelly FloresNo ratings yet
- Dialog English Nurs and Patient NewDocument6 pagesDialog English Nurs and Patient NewRisma Faudiyah100% (1)
- DR Ebrahim CK Notes PDFDocument149 pagesDR Ebrahim CK Notes PDFWendy MaeNo ratings yet
- Rudolf Steiner OCCULT PHISIOLOGYDocument110 pagesRudolf Steiner OCCULT PHISIOLOGYNNo ratings yet
- VSD: Symptoms, Causes, Treatment of Ventricular Septal DefectDocument6 pagesVSD: Symptoms, Causes, Treatment of Ventricular Septal DefectFauzan Luthfi A MNo ratings yet
- Philips HD11 XE Ultrasound System Versatility and Clinical FeaturesDocument12 pagesPhilips HD11 XE Ultrasound System Versatility and Clinical FeaturesBoobeshNo ratings yet
- How Do I Know If My Activities Are of Moderate To Vigorous Intensity?Document2 pagesHow Do I Know If My Activities Are of Moderate To Vigorous Intensity?Balsc Bals BalscNo ratings yet
- General Principles of Physical ExaminationDocument35 pagesGeneral Principles of Physical Examinationjaish8904100% (4)
- Biology Class 11 NotesDocument21 pagesBiology Class 11 NotesDebasish NayakNo ratings yet
- Point-Of-Care Ultrasound in Cardiac ArrestDocument13 pagesPoint-Of-Care Ultrasound in Cardiac ArrestEgorSazhaevNo ratings yet
- Nursing MCQDocument1 pageNursing MCQNurul IslamNo ratings yet
- 01 - Kontraksi Otot JantungDocument39 pages01 - Kontraksi Otot JantungNauval Zilal FananyNo ratings yet
- ZPPSU Exercise Module for PATHFIT 2Document28 pagesZPPSU Exercise Module for PATHFIT 2Erirose ApolinarioNo ratings yet
- New Hire Med. Assessment Study GuideDocument24 pagesNew Hire Med. Assessment Study GuideNada PersonalNo ratings yet
- AtherosclerosisDocument5 pagesAtherosclerosisJoanne LagusadNo ratings yet
- (S. Abbate) Ear Acupuncture Prescriptions and Techniques PDFDocument8 pages(S. Abbate) Ear Acupuncture Prescriptions and Techniques PDFVenom VerdinNo ratings yet
- Nursing Care Plan HypertensionDocument2 pagesNursing Care Plan Hypertensionderic98% (124)
- ReleaseNotes Vitrea6.5.3Document29 pagesReleaseNotes Vitrea6.5.3Humayun KhanNo ratings yet
- Issues in Geriatric AnaesthesiaDocument11 pagesIssues in Geriatric AnaesthesiaAissyiyah Nur An NisaNo ratings yet
- Anatomy and Physiology of the Cardiovascular SystemDocument6 pagesAnatomy and Physiology of the Cardiovascular SystemDawn Santiago RNNo ratings yet
- Annotated Bibliography FinalDocument3 pagesAnnotated Bibliography Finalapi-263873257No ratings yet
- Cardiac Masses: Nick Tehrani, MDDocument77 pagesCardiac Masses: Nick Tehrani, MDNuha AL-YousfiNo ratings yet
- Exercise For Fitness: Performance Standard Content StandardDocument11 pagesExercise For Fitness: Performance Standard Content StandardPrecilla Zoleta Sosa80% (5)
- Congenital Heart Murmurs GuideDocument52 pagesCongenital Heart Murmurs GuideCristina Maria100% (1)
- PR-QRS-TwavesDocument3 pagesPR-QRS-TwavesKelly PrattNo ratings yet
- Abastract Book 2018 PDFDocument327 pagesAbastract Book 2018 PDFTatiana SchiopuNo ratings yet
- Straight Back SyndromeDocument1 pageStraight Back SyndromemisbahNo ratings yet
- Pulse PDFDocument11 pagesPulse PDFB. Vineeth ReddyNo ratings yet