Professional Documents
Culture Documents
Diagnostic Challenges in Cervical Lymphadenitis TB
Uploaded by
AstriTaufiRamadhani0 ratings0% found this document useful (0 votes)
48 views19 pagesDiagnostic Challenges in Cervical Lymphadenitis TB
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentDiagnostic Challenges in Cervical Lymphadenitis TB
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
48 views19 pagesDiagnostic Challenges in Cervical Lymphadenitis TB
Uploaded by
AstriTaufiRamadhaniDiagnostic Challenges in Cervical Lymphadenitis TB
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 19
Jurnal reading
DIAGNOSTIC CHALLENGES IN CERVICAL
TUBERCULOUS LYMPHADENITIS: A REVIEW
Hande Senem Deveci, Mustafa Kule, Zeynep
Altin Kule, Tulay Erden Habesoglu
North Clin Istanbul 2016;3(2):150–55
doi: 10.14744/nci.2016.20982
dr. Astri Taufi Ramadhani
Pembimbing: dr.Sahudi, Sp.B(K) KL
Tuberculosis (TB) is a common, and in many cases
lethal, infectious disease caused by various strains
of mycobacteria, usually Mycobacterium tuberculosis.
Today in developing countries tuberculosis is still a
major health problem.
Lymph node tuberculosis (LNT) is a common cause of
lymphadenopathy in areas in which TB is endemic
Pathogenesis
CTL is the result of lympho-hematogenous spread of
pulmonary tuberculosis
a hyperreaction of lymph nodes against previous
pulmonary tuberculosis
the predominant pathway of spread of the tubercle
bacilli to the cervical lymph nodes is from lung
parenchyma as the lymphatics of the right lung and
the lower lobe of the left lung normally drain to the
right supraclavicular lymph nodes and then upwards
to the right lower cervical chain
Dermographic findings
is more frequent in females and in the younger age
groups
Clinical presentation
a unilateral single or multiple painless lump, mostly
located in the posterior cervical or supraclavicular
region
The duration of lymphadenopathy at time of
presentation is typically 1–2 months, varying from 3
weeks to 8 months
Fistula formation can be seen in almost 10% of the
mycobacterial cervical lymphadenitis
night sweats, weakness, cough and fever
in HIV-positive patients the lymphadenopathies are
more commonly seen as symmetrical and multiple
Accompanying pulmonary tuberculosis is reported in
18%–42% of patients
Diagnostic tools
Hematological tests
Tuberculin skin test
Imaging techniques
Fine-needle aspiration
Culture
Molecular testing
Histopathology
Hematological tests
no specific blood test
leukocytosis, thrombocytosis, anemia, hyponatremia
and increased ALP results are associated with
chronic disease condition and these results create a
doubt about an infective condition. Also elevated
ESR show up a non-specific inflammatory response
Tuberculin skin test
Delayed-type hypersensitivity reactions against
mycobacterial antigen
positive 2–10 weeks after the mycobacterial
infection
Positive reactions (>10-mm induration) canoccur in
M. tuberculosis infections.
Suspicious reactions (5- to 9-mm induration) can
occur after BCG vaccination, M. tuberculosis infection
or nontuberculous mycobacterial infections
Negative reactions (<4-mm induration) represent a
lack of tuberculin sensitization
False-negative reactions: 20% with active
tuberculosis
like other infections, metabolic disease, malnutrition,
live virus vaccination, malignancy,
immunosuppressive drugs, newborns, elderly
people, stress, sarcoidosis and inadequate test
application
Imaging techniques
Chest radiographs do not have any diagnostic
value.
USG findings do not show diseases specific features
for CTL. It can also be used as an imaging tool for
the guided aspirations
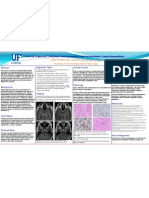
CT and MRI scans may show characteristic signs and
the localization of the CTL which may help if the
surgical excision would be planned in future.
Fine-needle aspiration
a thin needle is inserted into an infected, swollen,
superficial lymph node.
cytological examination, acid-fast bacilli (AFB)
staining, culturing and/or molecular testing
The sensitivity and specificity of FNA cytology in the
diagnosis of tuberculous lymphadenitis are 88%
and 96%
ZN staining and microscopic evaluation is rapid,
cheap and easy. Sensitivity ranges from 46–78%
and the specificity is actually 100%
Culture
A definitive diagnosis
Isolation of mycobacterium by culture is possible in
10–69% of the cases
the long duration of culture (6–8 weeks) cause
delay in initiation of treatment and is assessed as
time-consuming
Molecular testing
After FNAs, PCR should be performed for the
samples
the positivity of PCR from FNA materials were
found 71.4%, 76.4% and 92.1% in three different
studies
Histopathologic examination and PCR of an
excisional biopsy should be recommended only for
patients in whom FNA-PCR is negative or when
there is discrepancy with the clinical impression
Histopathology
Langerhans giant cells, caseating necrosis,
granulomatous inflammation and calcification
Although it’s an invasive technique, early surgical
excision of the tuberculous lymphadenitis is considered
as an adjunct to antibiotic therapy.
surgical excision has been recommended for treatment
failure cases of tuberculosis lymphadenitis and for
patients who have discomfort from tense, fluctuant
lymph nodes
Preferred surgical method is excision of an infected
lymph node.
Conclusion
Tuberculosis (TB) is a major health concern in developing
countries. This disease is a systemic disease which may give rise
to cervical lymphadenitis as an extrapulmonary manifestation
of the disease.
The most usual signs and symptoms are the appearance of a
chronic, painless mass in the neck, which is persistent and usually
grows with time. Because of no other remarkable symptom their
diagnosis and distinction need a high index of suspicion, and
application of a variety of diagnostic modalities.
However, it is not possible or practical to apply all of the
diagnostic procedures in all patients. This would be time
consuming and expensive.
Increased ESR, leukocytosis thrombocytosis, anemia, hyponatremia and
increased ALP results put forward a non-specific inflammation or a chronic
disease status.
Chest radiographs do not have any diagnostic value. And tuberculin skin
test is also not valuable in areas where BCG vaccination is mandatory. CT
and MRI scans may show characteristic signs and the localization of the CTL
which may help if the surgical excision would be planned in future. After a
FNA, a combination of conventional techniques (such as cytology, staining,
culture) with PCR must be applied for the rapid and early diagnosis of CTL.
Therefore, the value of FNA is indisputable. The definitive diagnosis of
tuberculous lymphadenitis is done by excisional biopsy and histopathologic
examination if all other techniques fail.
You might also like
- Knot Tying ManualDocument50 pagesKnot Tying ManualAdriana Vick100% (1)
- Algorithm Syok AnafilaktikDocument1 pageAlgorithm Syok AnafilaktikAstriTaufiRamadhaniNo ratings yet
- The 2015 Bls Acls Guidelines EnaDocument36 pagesThe 2015 Bls Acls Guidelines EnaAstriTaufiRamadhaniNo ratings yet
- Berita Acara Presentasi PortofolioDocument7 pagesBerita Acara Presentasi PortofolioAstriTaufiRamadhaniNo ratings yet
- Blood PressureDocument60 pagesBlood PressureEnerolisa ParedesNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (120)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The ESC Textbook of Cardiovascular Medicine PDFDocument1,109 pagesThe ESC Textbook of Cardiovascular Medicine PDFjyothi100% (4)
- Deformational PlagiocephalyDocument2 pagesDeformational PlagiocephalyfsdafaNo ratings yet
- Banco de Preguntas ReabilitacionDocument19 pagesBanco de Preguntas ReabilitacionVanessa AlcantaraNo ratings yet
- Lec 10 MidtermsDocument1 pageLec 10 MidtermsMitzi AngelaNo ratings yet
- MrsSNIGDHA 43Y FemaleDocument3 pagesMrsSNIGDHA 43Y FemalePathkind LabNo ratings yet
- Cardiology High Blood Pressure - University of Nigeria Nsukka 73rd-Inaugural-Lecture - OnwubereDocument29 pagesCardiology High Blood Pressure - University of Nigeria Nsukka 73rd-Inaugural-Lecture - OnwubereAnonymous 9QxPDpNo ratings yet
- Ourse Yllabus Section I - College and University Catalog DataDocument5 pagesOurse Yllabus Section I - College and University Catalog DatabagusNo ratings yet
- Clinically Inapparent Gallbladder Cancer Presenting With Paraneoplastic Cranial Neuropathies Aunali S Khaku, MD Lisa Aenlle MD, Irene A Malaty, MD University of Florida Department of NeurologyDocument1 pageClinically Inapparent Gallbladder Cancer Presenting With Paraneoplastic Cranial Neuropathies Aunali S Khaku, MD Lisa Aenlle MD, Irene A Malaty, MD University of Florida Department of Neurologyask1288No ratings yet
- Podcast ScriptDocument5 pagesPodcast ScriptGillian YuNo ratings yet
- REFLECTION PE & HealthDocument1 pageREFLECTION PE & HealthPenelope CarandangNo ratings yet
- LEUKOPNEADocument21 pagesLEUKOPNEAdaisyNo ratings yet
- Siraj Sir Artical IjprdDocument11 pagesSiraj Sir Artical IjprdmwdhtirahNo ratings yet
- Asia Pacific College of Advanced StudiesDocument4 pagesAsia Pacific College of Advanced StudiesRussel QuinonesNo ratings yet
- Clinical Examination Techniques in OtologyDocument44 pagesClinical Examination Techniques in OtologyDr. T. Balasubramanian100% (2)
- Breast Self ExaminationDocument40 pagesBreast Self ExaminationPrince Rener Velasco PeraNo ratings yet
- Ratio For Cmca UesDocument3 pagesRatio For Cmca UesJeralyn Delarosa GabagatNo ratings yet
- 50 Writing Task + Sample Letters PDFDocument173 pages50 Writing Task + Sample Letters PDFIrina Alexandra83% (86)
- Infectious QuestionDocument52 pagesInfectious Questionrayooona88No ratings yet
- 7 Steps To The Perfect PICO Search White PaperDocument9 pages7 Steps To The Perfect PICO Search White PaperNurkhasanah 71No ratings yet
- Home Care Referral: Clear FormDocument2 pagesHome Care Referral: Clear FormAhmad IsalNo ratings yet
- European Neonatal Ethics ConferenceDocument3 pagesEuropean Neonatal Ethics Conferencemadimadi11No ratings yet
- (Đề thi có 06 trang) Thời gian làm bài: 60 phút không kể thời gian phát đềDocument7 pages(Đề thi có 06 trang) Thời gian làm bài: 60 phút không kể thời gian phát đềĐinh MinhNo ratings yet
- Handouts CD Prof. RojasDocument6 pagesHandouts CD Prof. RojasChallen CulturaNo ratings yet
- ObesityDocument4 pagesObesityDumb PepeNo ratings yet
- Lectures DGODocument10 pagesLectures DGOnumairaNo ratings yet
- Community Medicine Preventive Social Medicine Balaram Jana.01500 1Document10 pagesCommunity Medicine Preventive Social Medicine Balaram Jana.01500 1Arfa jahanNo ratings yet
- 2021.10.27 Letter To NIHDocument14 pages2021.10.27 Letter To NIHZerohedge Janitor100% (1)
- NCP Risk For FallsDocument1 pageNCP Risk For FallsMary Joyce71% (14)
- CC Lab ActDocument3 pagesCC Lab ActTrisha IbarraNo ratings yet
- Sample Management in Clinical TrialsDocument8 pagesSample Management in Clinical TrialstheanhdbtNo ratings yet